Professional Documents
Culture Documents
IV Complications
Uploaded by
mara5140100%(5)100% found this document useful (5 votes)
22K views76 pagesInfiltration is the process in which a substance enters or infuses into another substance or a surrounding area. Extravasation is the actual unintentional escape or leakage of material from a vessel into the surrounding tissue. The use of warm compresses to treat infiltration has become controversial.
Original Description:
Original Title
iv complications
Copyright
© Attribution Non-Commercial (BY-NC)
Available Formats
PPT, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentInfiltration is the process in which a substance enters or infuses into another substance or a surrounding area. Extravasation is the actual unintentional escape or leakage of material from a vessel into the surrounding tissue. The use of warm compresses to treat infiltration has become controversial.
Copyright:
Attribution Non-Commercial (BY-NC)
Available Formats
Download as PPT, PDF, TXT or read online from Scribd
100%(5)100% found this document useful (5 votes)
22K views76 pagesIV Complications
Uploaded by
mara5140Infiltration is the process in which a substance enters or infuses into another substance or a surrounding area. Extravasation is the actual unintentional escape or leakage of material from a vessel into the surrounding tissue. The use of warm compresses to treat infiltration has become controversial.
Copyright:
Attribution Non-Commercial (BY-NC)
Available Formats
Download as PPT, PDF, TXT or read online from Scribd
You are on page 1of 76
IV Complications
Infiltration and Extravasation:
Definitions and Misc. Info
Infiltration: the process in which a substance
enters or infuses into another substance or a
surrounding area. Infiltration may be an
intentional or unintentional process
Extravasation: the actual unintentional escape
or leakage of material from a vessel into the
surrounding tissue
Vesicant: an agent that is irritating and causes
blistering
Infiltration and Extravasation:
Etiology
1 of 2
Puncture of distal vein wall during
venipuncture
Puncture of any portion of the vein wall by
mechanical friction from the catheter/needle
cannula
Dislodgement of the catheter/needle cannula
from the intima of the vein
Poorly secured IV device
Poor vein or site selection
Infiltration and Extravasation:
Etiology
2 of 2
Improper cannula size
High delivery rate or pressure of the infusate
Over manipulation of the IV device, the site,
or both
Irritating infusate that inflames the intima of
the vein and causes it to weaken
Infiltration and Extravasation:
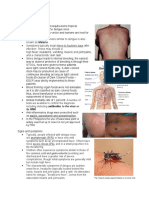
Signs and Symptoms
1 of 2
Pain at or near the insertion site
Swelling proximal to or distal to the IV site
Puffiness of the dependent part of limb or
body
Taut, rigid skin around IV site
Blanching and coolness of skin around IV site
Damp or wet dressing
Slowed infusion rate
Infiltration and Extravasation:
Signs and Symptoms
2 of 2
No back flow of blood into IV tubing when
clamp is full opened and solution container is
lowered below IV site
No back flow of blood into IV tubing when
tubing is pinched above cannula hub
Infusion stops running
The infusion continues to infuse when
pressure is applied to the vein above the tip of
the cannula
Infiltration and Extravasation:
Interventions
The use of warm compresses to treat infiltration
has become controversial. It has been found that
cold compresses may be better for some
infiltrated infusates and warm compresses may
be more effective for others. It has also been
documented that elevation of the infiltrated
extremity may be painful for the patient. To act
in the best interest of the patient, following IV
infiltration, consult with the physician for order
regarding compresses and elevation.
Infiltration and Extravasation:
Clinical Criteria
1 of 3
No symptoms
Skin blanched
Edema <1 inch in any direction
Cool to touch
With or without pain
Skin blanched
Edema 1-6 inches in any direction
Cool to touch
With or without pain
Infiltration and Extravasation:
Clinical Criteria
2 of 3
Skin blanched, translucent
Gross edema >6 inches in any direction
Cool to touch
Mild-moderate pain
Possible numbness
Skin blanched, translucent
Infiltration and Extravasation:
Clinical Criteria
3 of 3
(continued from previous slide)
Deep pitting tissue edema
Circulatory impairment
Moderate-severe pain
Infiltration or any amount of blood product,
irritant, or vesicant
Catheter and Needle
Displacement:
Definitions and Misc. Info
Displacement: cannula has shifted from it's
intended placement site in the vein, or is
inadvertently removed from the vein.
Catheter and Needle
Displacement
Etiology
1 of 1 secured after
Cannula was inadedaquatly
insertion
Tape around site becomes loose or detaches
from the skin
Insertion pulled out during transportation or
movement of the client
Catheter and Needle
Displacement
Preventative Interventions
1 of
Explain to the patient 1 insertion their role
prior
in caring for the IV
Appropriate securing of IV line
Frequent assessment of site to ensure patency
IF THE SITE BECOMES DISLODGED,
THE SITE MUST BE MOVED!
Occlusion and Loss of Patency:
Definitions and Misc. Info
Occlusion: occurs when there is some type of
blockage that interferes with the passage of
infusate into the vein. It can occur at any
point within the vein, the cannula, or the
tubing.
Occlusion and Loss of Patency
Etiology
Tubing may be kinked or bent
Transition from electric pump to gravity flow
Not saline-locking the site when infusate runs
out
Fibrin sheath formation around and over the
tip of a cannula
Too large of a cannula
Occlusion and Loss of Patency
Signs and Symptoms
Slowed rate of infusion even if clamp is
opened or height of infusate is raised
Infusion stops infusing
Infusion site pain (with normal appearance)
Blood backs up from the cannula into the IV
tubing
Occlusion and Loss of Patency:
Interventions
For prevention, flush routinely, especially
with intermittent infusion devices
Pinch the IV tubing open and closed or gently
milk it
If the above doesn't work, attempt to irrigate
the line with normal saline
Phlebitis:
Definitions and Misc. Info
Phlebitis: The inflammation of a vein
Inflammation: part of the body's normal
immune response to any type of injury or
invasion
Suppurative phlebitis: phlebitis in which pus
accumulates in the tissue
Phlebitis:
Etiology
Bacterial: Pathogenic organisms can gain
access and stimulate inflammation.
Chemical: caused by irritating or vesicant
solutions.
Mechanical: physical trauma from the skin
puncture and movement of the cannula into
the vein during insertion; any subsequent
manipulation and movement of the cannula;
clotting; or excessively large cannula.
Phlebitis:
Signs and Symptoms
Erythema at the site
Pain or burning at the site and along the
length of the vein
Warmth over the site
Edema at the site
Vein hard, red, and cord like
Slowed infusion rate
Temperature elevation on degree or more
above the baseline
Phlebitis:
Grading Criteria
1 of 2
Erythema at access site with or without pain
No symptoms
Pain at access site with erythema and/or
edema
Pain at access site with erythema and/or
edema
Streak formation
Palpable venous cord
Phlebitis:
Grading Criteria
2 of 2
Pain at access site with erythema and/or
edema
Phlebitis:
Preventative Interventions
Infusion container should be hung 36 inches
higher than the IV site
Clip body hair around the IV site, but DO
NOT SHAVE IT! Shaving may encourage
bacterial contamination.
Insertion should be performed with aseptic
technique
Phlebitis:
Interventions
At the first sign of phlebitis, the IV must be
discontinued and the cannula removed. If the
site shows fever and drainage, contact the
physician.
Warm compresses may be used, according to
agency protocol
Thrombosis and
Thrombophlebitis:
Definitions and Misc. Info
Thrombosis: the formation of a clot
Thrombophlebitis: the inflammation of a
vessel due to the development of a thrombus
Deep Vein Thrombosis (DVT): inflammation
of the larger deeper veins of the extremities
Venous Stasis: the condition wherein blood
flow is inhibited or stopped due to a clot
formation
Thrombosis and
Thrombophlebitis:
Etiology
Usually the sequela1ofof 1
phlebitis, meaning it is
a consequence of it. A clot forms when the
blood vessel becomes traumatized.
Thrombosis and
Thrombophlebitis
Signs and Symptoms
Slowed or stopped 1 of 2 rate
infusion
Aching or burning sensation at the infusion
site
Elevation in temperature on degree or more
above baseline
Skin warm and red around IV site
Cording of the infusion vein
Thrombosis and
Thrombophlebitis
Signs and Symptoms
Malaise 2 of 2
Swelling and edema of the extremity
Diminished arterial pulses
Pallor
Thrombosis and
Thrombophlebitis:
Interventions
1 ofand2 restarted elsewhere
IV must be discontinued
immediately
Physician should be consulted as to whether the
extremity should be elevated and warm, moist
compresses applied.
Physician may order antiembolic stockings
and/or the use of sequential compression devices
(SCDs)
Anticoagulants and anti-inflammatories and a
balanced routine of active and passive activity
and rest
Hematoma:
Definitions and Misc. Info
Hematoma: the accumulation of clotted blood
in the tissue interstices
Ecchymosis: a black and blue skin
discoloration
Hematoma:
Etiology
Faulty venipuncture technique, where the
cannula passes through the distal vein wall
Infiltration following cannulation of a vein
Flow control clamp for infusion is opened
before tourniquet is removed
Vessel rupture due to large cannula
Inadequate pressure applied following a
blood sampling stick or the discontinuation of
an infusion or heparin/saline lock.
Hematoma:
Signs and Symptoms
Ecchymosis over and around insertion area
Pain at the site
Swelling and hardness at the insertion site
Inability to advance the cannula all the way
into the vein during insertion
Inability to flush the IV line
Hematoma:
Interventions
IV line discontinued, and a 2X2 inch gauze
pressure dressing applied
Alcohol should not be used when removing
the cannula because it enhances bleeding and
may cause stinging
Once bleeding has stopped, the extremity
may be elevated and warm moist compresses
applied, depending on the severity
Venous Spasm:
Definitions and Misc. Info
Venous spasm: a sudden involuntary
movement or contraction of a vessel wall as a
result of trauma or irritation; usually painful.
Cramp: a strong, painful spasm
Venous Spasm:
Etiology
Administration of an irritating infusate with a
high osmolarity or a high or low pH
Delivery of cold or viscous infusates
For some patients, entrance of IV cannula,
especially if cannula is too large
Too rapid infusion of infusate
Venous spasm:
Signs and Symptoms
Slowed infusion rate
Stopped infusion rate
Severe pain from the IV site radiating up the
extremity
Blanching over the IV site
Redness over and around the IV site
Venous Spasm:
Interventions
Prevention: use a large vein and a small-
gauge cannula so that blood flow is
unrestricted and allows for dilution of the
infusate; administer fluids at room
temperature
Once it occurs:
− Decrease infusion rate
− Apply warm compress if infusate is cold
− Pharmacist should be contacted about adding a
buffer if infusate is irritating
Vessel Collapse:
Definitions and Misc. Info
Vessel collapse: the walls of a vein or artery
retract abnormally
Vessel Collapse:
Etiology
Decreased circulation, as seen with excessive
blood or fluid loss and shock
Vessel Collapse:
Signs and Symptoms
Inability to see a vein
Inability to feel a vein
Loss of vessel elasticity
Vessel feels flat or flaccid
Reduced or stopped infusion flow
Vessel Collapse:
Interventions
Restart the IV elsewhere, preferably in a larger vein
If patient is in shock a physician may need to insert
a central line
− Stay with patient
− Provide reassurance
− Assist with central venous cannulation
− Keep the patient warm
− Lower head and elevate legs to promote venous
return
− Carefully monitor vital signs
Cellulitis:
Definitions and Misc. Info
Cellulitis: the diffuse inflammation and
infection of cellular and subcutaneous tissue.
It is bacterial in nature.
Peau d'orange: site feels warm and the skin
has the roughened appearance of an orange
peel
Cellulitis:
Etiology
Invasion and multiplication of bacteria into
the IV site
Cellulitis:
Signs and Symptoms
1 of 2
Tenderness
Pain
Warmth
Edema
Induration
Red streaking on skin
Peau d'orange
Vesicles
Cellulitis:
Signs and Symptoms
2 of 2
Abscess formation with pus
Ulceration
Fever
Chills
Malaise
Cellulitis:
Interventions
Discontinue IV and start elsewhere
Physician may need to incise and drain an abscess
Limb may be elevated to reduce edema
Cool compresses to promote comfort often
alternated with war, moist compresses to promote
circulation
Sterile dressings should be used
Antibiotics, analgesics, and antipyretics are
generally administered
Nerve, Tendon, Ligament and
Limb Damage:
Etiology
Incorrect insertion and placement of the IV
cannula, or improper securing and
stabilization of the cannula and IV line after
insertion
Nerve, Tendon, Ligament and
Limb Damage:
Signs and Symptoms
Tingling
Numbness
Loss of sensation
Loss of movement
Cyanosis
Pallor
Deformity
Paralysis
Nerve, Tendon, Ligament and
Limb Damage:
Interventions
Prevent damage by properly placing the IV
line
Frequently assess the extremity in which the
IV is placed
Contamination and Infection:
Definitions and Misc. Info
Contamination: the introduction of
microorganisms or particulate matter into a
normally sterile environment
Contamination and Infection:
Breaks in asepsis during the manufacture,
packaging, and storage of infusates,
medications, and delivery systems
Break in asepsis during setup and
administration of infusion therapy
Contamination and Infection:
Signs and Symptoms
Chills
Malaise
Fever
Elevated leukocyte count
Normal appearance of IV site
Contamination and Infection:
Interventions
IV must be discontinued and move to another
site with fresh equipment
Cannula, connection sites, tubing, and
infusate should be cultured
Sepsis:
Definitions and Misc. Info
Sepsis: the (usually) febrile disease process
that results from the presence of
microorganisms or their toxic products in the
circulatory system.
Sepsis:
Etiology
Most often attributed to Staphylococcus
aureus and S. epidermidis, the Candida
albicans yeast, and the coliform species
Escherichiea, Enterobacter, and Klebsiella.
Sepsis:
Signs and Symptoms
Chills
1 of 2
Malaise
Altered mental status
Fever
Tachycardia
Tachypnea
Leukocytosis
Hypotension
Flushing
Sepsis:
Signs and Symptoms
2 of 2
S/S of Toxic Shock Syndrome:
− Malaise with generalized myalgia and arthralgia
− Vertigo
− Nausea with vomiting
− Edema of hands and feet
− Desquamation of hands and feet
Sepsis:
Interventions
Keep patient flat with legs elevated
Provide oral fluids
Keep warm
Medications as necessary to support blood
pressure, circulation, and promote comfort
Conserve strength
Administer oxygen
Analgesics and antipyretics may be given
Hypersensitivity: Info
Hypersensitivity: the profound physiologic
response of the body to an antigen
Allergy: acquired abnormal immune response
to an allergen following sensitization
Hypersensitivity:
Certain people are especially drug sensitive;
others are simply allergic to some specific
medications
Hypersensitivity:
Signs and Symptoms
1 of 5
Facial edema
Generalized edema
Erythema along veins
Palpitations
Hypotension
Cardiac arrest
Dysphagia
Gastric cramping
Hypersensitivity:
Signs and Symptoms
2 of 5
Intestinal cramping
Nausea
Vomiting
Flushing
Red flare
Rash
IV site edema
Pruritis
Hypersensitivity:
Signs and Symptoms
3 of 5
Urticaria (hives)
Agitation
Anxiety
Confusion
Disorientation
Headache
Paresthesias
Vertigo
Hypersensitivity:
Signs and Symptoms
4 of 5
Nasal congestion
Rhinorrhea (runny nose)
Cough
Sensation of tightness in throat
Mucous membrane edema
Wheezing
Bronshospasm
Respiratory obstruction
Hypersensitivity:
Signs and Symptoms
5 of 5
Respiratory arrest
Watery eyes
Scratchy throat
Tinnitus
Buzzing sound in ears
Throbbing sensation in ears
Tingling/numbness in fingers and /or toes
Hypersensitivity:
Interventions
At the first indication of a hypersensitivity
reaction, the nurse must either discontinue the
infusion and keep the vein open with normal
saline or, if the reaction is mild, slow th IV to a
KVO rate until further orders can be obtained.
NEVER REMOVE THE CANNULA! Vital
signs are to be taken and the physician notified.
The nurse must stay with the patient, reassure
him, and keep him warm. Emergency equipment
must be readily available. Emergency drugs are
administered according to agency policy and
physician orders.
Embolism:
Definition and Misc. Info
Embolus: an aggregate of undissolved material
in the blood that is carried by circulatory flow.
Endogenous embolus: clotted blood, tissue
particles, tumor cell mass, or fat globules
Exogenous embolus: particulate matter, liquids,
gaseous material.
Ischemia: obstruction of a vessel due to
embolus.
Infarction: an area of necrosis following the
loss of blood supply.
Embolism:
Etiology
Blood clot
Air embolism: through severed IV lines,
tubings that are not primed with infusate,
vented infusion containers that are allowed to
run dry, or disconnected and loose tubing
junctions
Catheter embolism: a portion of the catheter
breaks off
Any small, particulate matter that can enter
the bloodstream from the IV site
Embolism:
Signs and Symptoms
1 of 2
Dyspnea
Tachypnea
Cardiac arrhythmia
Hypotension
Diaphoresis
Anxiety
Substernal pressure
Embolism:
Signs and Symptoms
2 of 2
Chest pain with inhalation and exhalation
Localized decreased breath sounds
Pleural friction rub
Cough (often with hemoptysis)
Embolism:
Interventions
1 of 2
Blood clot
− Low dose heparin or oral anti-coagulants
− Plan activity and movement
− Promote comfort and gas exchange by elevating
the head of the bed, assisting with coughing and
deep breathing, administering analgesics, and
maintaining a restful environment
Embolism:
Interventions
2 of 2
Air embolism
− Mostly preventative and supportive
Catheter embolism
− Apply tourniquet above IV site
− Prepare for surgery
Speed Shock:
Definitions and Misc. Info
Speed shock: the systemic reaction to the
rapid or excessive infusion of medication or
infusate into the circulation
Speed shock:
Etiology
Flow control clamp is inadvertently left
completely open
EID (electronic infusion device) programmed
incorrectly
Speed Shock:
Signs and Symptoms
Flushing of head and neck
Feeling of apprehension
Hypertension
Pounding headache
Dyspnea
Chest pain
Chills
Loss of consciousness
Cardiac arrest
Speed Shock:
Interventions
Best intervention is prevention. Do not give a
medication without reading and following the
manufacturer's guidelines.
When it occurs:
− Slow or stop infusion
− Notify physician
− Observe for cardiac arrest
You might also like
- 2018 ESMO Handbook of Interpreting Oncological Study PublicationsDocument219 pages2018 ESMO Handbook of Interpreting Oncological Study PublicationsAlex Lugli100% (1)
- PICC Line Instruction SheetDocument1 pagePICC Line Instruction Sheetmara5140100% (3)
- Chart of Commonly Transfused Blood ProductsDocument2 pagesChart of Commonly Transfused Blood Productsmara5140100% (8)
- Easy ECG GuideDocument17 pagesEasy ECG GuideDr.Chinmay Kulkarni83% (12)
- SITXWHS004 Assessment 1 - ProjectDocument18 pagesSITXWHS004 Assessment 1 - Projectaarja stha100% (1)
- Reaching OutDocument353 pagesReaching OutDebayan NandaNo ratings yet
- Complications of IV TherapyDocument16 pagesComplications of IV TherapyFayeTolentinoNo ratings yet
- Multiple Injuries: Physical Examination and Review of SystemsDocument5 pagesMultiple Injuries: Physical Examination and Review of SystemsTarquin Tomada100% (1)
- Definition and FocusDocument20 pagesDefinition and FocusAbdul Azis G. CamidNo ratings yet
- Clinical Nursing Malpractice Case StudiesDocument3 pagesClinical Nursing Malpractice Case StudiesPaul RichardNo ratings yet
- Deep Vein ThrombosisDocument3 pagesDeep Vein ThrombosisAnonymous cwRgUKv2MQ100% (1)
- Emergency Disaster NursingDocument21 pagesEmergency Disaster NursingJoy Jarin100% (1)
- NursingDocument98 pagesNursingLAWRENCE MARI SANTELLA0% (1)
- Complications of Labor and DeliveryDocument8 pagesComplications of Labor and DeliveryMox SwanNo ratings yet
- Parenteral InjectionsDocument7 pagesParenteral InjectionsNashleyah AnayatinNo ratings yet
- Acute Burns Case StudyDocument6 pagesAcute Burns Case StudyErica MeyersNo ratings yet
- Drug Name Generic Name Classification Mechanism of Action Indication Contra Indication/precautions Adverse Effect Dosage Nursing InterventionsDocument4 pagesDrug Name Generic Name Classification Mechanism of Action Indication Contra Indication/precautions Adverse Effect Dosage Nursing InterventionsTedd CamilingNo ratings yet
- Medical Surgical Nursing Nclex Questions7Document7 pagesMedical Surgical Nursing Nclex Questions7dee_day_8No ratings yet
- Concept MapDocument1 pageConcept MapSheryl Ann Barit PedinesNo ratings yet
- Rheumatic Joint Disease Study GuideDocument18 pagesRheumatic Joint Disease Study Guidechalinsammy1No ratings yet
- Discharge PlanDocument5 pagesDischarge PlanrraksNo ratings yet
- Diabetes InsipidusDocument8 pagesDiabetes InsipidusNader Smadi100% (5)
- Gestational Conditions 1Document19 pagesGestational Conditions 1MrLarry Dolor100% (1)
- Case Study Chapter 20 (Oct 16th)Document2 pagesCase Study Chapter 20 (Oct 16th)Anz MingNo ratings yet
- Oc Ob Set ADocument10 pagesOc Ob Set AmatrixtrinityNo ratings yet
- 1Document28 pages1joanneisrael12100% (1)
- DiverticulosisDocument49 pagesDiverticulosisJewelyn Alafriz AngelesNo ratings yet
- Buergers Disease Concept MapDocument1 pageBuergers Disease Concept MapElmer Dizon100% (1)
- DigoxinDocument2 pagesDigoxinNinoska Garcia-Ortiz100% (2)
- InsulinDocument6 pagesInsulinJorelle-Nickolai RodriguezNo ratings yet
- Automatic Intravenous Piggyback NPSDocument5 pagesAutomatic Intravenous Piggyback NPSRafaela CarolineNo ratings yet
- Medical Surgical Nursing ReviewDocument16 pagesMedical Surgical Nursing ReviewArda LynNo ratings yet
- Risk Factors: CholelithiasisDocument10 pagesRisk Factors: CholelithiasisRoyster CabralNo ratings yet
- Transient Ischemic Attack Precipitating Factors Predisposing FactorsDocument6 pagesTransient Ischemic Attack Precipitating Factors Predisposing FactorsYosef OxinioNo ratings yet
- DULNUANDocument2 pagesDULNUANJB tindonganNo ratings yet
- Case Study EvaluationDocument6 pagesCase Study EvaluationKristy HimmlerNo ratings yet
- ALTERED POST PARTUM Complications Nursing Lecture and Care PlanDocument13 pagesALTERED POST PARTUM Complications Nursing Lecture and Care PlanKristelle Joy Capili SicatNo ratings yet
- Pathophysiology LectureDocument73 pagesPathophysiology LectureJoyyNo ratings yet
- Community Health Nursing & FUNDA ComprehesiveDocument29 pagesCommunity Health Nursing & FUNDA Comprehesivegracetano50No ratings yet
- Impaired SwallowingDocument2 pagesImpaired SwallowingfaizaNo ratings yet
- NCM 112 Lecture NotesDocument5 pagesNCM 112 Lecture NotesSureen RegularNo ratings yet
- Concept Map Leukemia PDFDocument7 pagesConcept Map Leukemia PDFMichael AmandyNo ratings yet
- Classification of Burns Based On Depth CharacteristicsDocument2 pagesClassification of Burns Based On Depth CharacteristicsmexelleNo ratings yet
- Complication of IV TherapyDocument3 pagesComplication of IV TherapyRayl RsNo ratings yet
- AnticholinergicsDocument5 pagesAnticholinergicskman0722100% (1)
- Med Trans ReviewerDocument1 pageMed Trans ReviewerDenise CerdaNo ratings yet
- NCP CvaDocument3 pagesNCP CvaRachel Anne Cabral EvangelistaNo ratings yet
- Fundamentals of Nursing NCLEX Practice Questions Quiz 1Document39 pagesFundamentals of Nursing NCLEX Practice Questions Quiz 1Regine Mae Encinada100% (1)
- Chapter 5Document21 pagesChapter 5Nurse UtopiaNo ratings yet
- IMCI UpdatedDocument5 pagesIMCI UpdatedMalak RagehNo ratings yet
- Pharma Cards.Document19 pagesPharma Cards.Brent NicholsNo ratings yet
- Ca QuizDocument7 pagesCa Quizvicson_4No ratings yet
- Pharma 031513 - 100Document16 pagesPharma 031513 - 100Patrieze Aleck EspinaNo ratings yet
- Practice Test Questions Downloaded From FILIPINO NURSES CENTRALDocument23 pagesPractice Test Questions Downloaded From FILIPINO NURSES CENTRALFilipino Nurses CentralNo ratings yet
- Personal Philosophy PaperDocument10 pagesPersonal Philosophy Paperapi-354302626No ratings yet
- Far Eastern University: Institute of NursingDocument3 pagesFar Eastern University: Institute of Nursingshendae cosmianoNo ratings yet
- Pnle 1-Foundation of Professional NSG PracticeDocument19 pagesPnle 1-Foundation of Professional NSG Practiceshiela maeNo ratings yet
- Gordon's Typology of 11 Functional Health PatternDocument12 pagesGordon's Typology of 11 Functional Health PatternJ. ishtelleNo ratings yet
- IV InsertionDocument9 pagesIV InsertionSharmaine Grace FlorigNo ratings yet
- ArcherReview Self AssessmentDocument17 pagesArcherReview Self AssessmentGodwin KyeremehNo ratings yet
- Cardiogenic Shock NclexDocument81 pagesCardiogenic Shock NclexKrishna SapkotaNo ratings yet
- Complications of Intravenous TherapyDocument29 pagesComplications of Intravenous TherapyKrizia BonillaNo ratings yet
- ROT ExamDocument6 pagesROT ExamIan CarodanNo ratings yet
- CL Module9 PDFDocument27 pagesCL Module9 PDFO.r. CadzNo ratings yet
- Neonatal Infusion Therapy - HandoutDocument9 pagesNeonatal Infusion Therapy - HandoutAde PurnaNo ratings yet
- Intravenous Therapy Is Treatment That Infuses Intravenous Solutions, Medications, Blood, or BloodDocument5 pagesIntravenous Therapy Is Treatment That Infuses Intravenous Solutions, Medications, Blood, or BloodShehada Marcos BondadNo ratings yet
- Table of Commonly Used IV SolutionsDocument3 pagesTable of Commonly Used IV Solutionsmara514081% (16)
- Care of Clients With Hiv InfectionDocument32 pagesCare of Clients With Hiv Infectionmara5140No ratings yet
- Path Physiologies of The Cardiovascular SystemDocument34 pagesPath Physiologies of The Cardiovascular Systemmara5140No ratings yet
- Musculoskeletal Disorders Care of Client With Fall 2005Document41 pagesMusculoskeletal Disorders Care of Client With Fall 2005mara5140100% (3)
- Cancer IntroDocument29 pagesCancer Intromara5140No ratings yet
- Test 4 OutlineDocument13 pagesTest 4 Outlinemara5140No ratings yet
- Arnons NotesDocument63 pagesArnons Notesmara5140100% (1)
- Rheumatoid Arthritis and GoutDocument21 pagesRheumatoid Arthritis and Goutmara5140100% (1)
- ShockDocument7 pagesShockmara5140No ratings yet
- Fourth Semester FinalDocument14 pagesFourth Semester Finalmara5140No ratings yet
- Test 2 OutlineDocument7 pagesTest 2 Outlinemara5140No ratings yet
- Abg InterpretationDocument14 pagesAbg Interpretationmara5140100% (7)
- Test 3 OutlineDocument3 pagesTest 3 Outlinemara5140No ratings yet
- Aortic Aneurysm-: NUR2744 Test 3 OutlineDocument10 pagesAortic Aneurysm-: NUR2744 Test 3 Outlinemara5140No ratings yet
- Endocarditis: Vegetation Around The Valves Sub Acute and Acute StagesDocument15 pagesEndocarditis: Vegetation Around The Valves Sub Acute and Acute Stagesmara5140No ratings yet
- Test 4 OutlineDocument13 pagesTest 4 Outlinemara5140No ratings yet
- Rheumatic FeverDocument21 pagesRheumatic FeverUmar Azlan50% (2)
- Boiron - DDR 2018 - GB PDFDocument218 pagesBoiron - DDR 2018 - GB PDFRicardoMadeiraNo ratings yet
- اخلاق طبابتDocument230 pagesاخلاق طبابتAziz Ahmad NaseriNo ratings yet
- Implementing Telemedicine Services During COVID-19: Guiding Principles and Considerations For A Stepwise ApproachDocument25 pagesImplementing Telemedicine Services During COVID-19: Guiding Principles and Considerations For A Stepwise ApproachlauNo ratings yet
- NegOr Q4 MAPEH7 Module4a v2Document12 pagesNegOr Q4 MAPEH7 Module4a v2fauralaurenceNo ratings yet
- CL489F Physiotherapy Reassessment ReportDocument4 pagesCL489F Physiotherapy Reassessment ReportnaeemullahNo ratings yet
- CBT For KidsDocument34 pagesCBT For KidsJelena VisekrunaNo ratings yet
- MastoiditisDocument3 pagesMastoiditisPrincess GyasiNo ratings yet
- Coronary Drug Eluting Stents Nonclinical and Clinical StudiesDocument89 pagesCoronary Drug Eluting Stents Nonclinical and Clinical Studiesdudde niranjanNo ratings yet
- Drug Formulary HospitalDocument98 pagesDrug Formulary HospitalahmshmNo ratings yet
- Nominal Roll N035 1bnm10jDocument2 pagesNominal Roll N035 1bnm10jsubiNo ratings yet
- Hili MallDocument7 pagesHili Mallvenkatesh snkNo ratings yet
- Startup StoryDocument1 pageStartup StorybmeghabNo ratings yet
- Literature Review On UTIDocument31 pagesLiterature Review On UTINishchal Dhakal0% (1)
- A New Biotech Out of Dana-Farber Wants To Join The Long Non-Coding RNA Party, With Help From Bob Langer - Endpoints NewsDocument1 pageA New Biotech Out of Dana-Farber Wants To Join The Long Non-Coding RNA Party, With Help From Bob Langer - Endpoints NewsAakanksha bansalNo ratings yet
- f2 Home-Sci Simplified Notes SPDocument20 pagesf2 Home-Sci Simplified Notes SPmicah isabokeNo ratings yet
- Ticket Ticket: Medical FacultyDocument6 pagesTicket Ticket: Medical Facultyhealer sruthyNo ratings yet
- Assessment Test Descriptions PyDocument19 pagesAssessment Test Descriptions PyDewa Ayu VeronicaNo ratings yet
- Intussusception - A Case ReportDocument3 pagesIntussusception - A Case ReportAgustinus HuangNo ratings yet
- Use of Alcohol Containing Caps ForDocument6 pagesUse of Alcohol Containing Caps ForGaby FernandezNo ratings yet
- Irene Gee Regidor BSED-English Conditions of Developmental Delay 1. Mental RetardationDocument3 pagesIrene Gee Regidor BSED-English Conditions of Developmental Delay 1. Mental RetardationAliana CabalunaNo ratings yet
- MLP Registration FormDocument6 pagesMLP Registration FormDoll JonesNo ratings yet
- A Broader View of PsychopathyDocument9 pagesA Broader View of PsychopathyMAN HIM HONo ratings yet
- Exercise Science Honours 2016Document22 pagesExercise Science Honours 2016asdgffdNo ratings yet
- A Bump Start.Document3 pagesA Bump Start.Speech & Language Therapy in PracticeNo ratings yet
- Caused by The .: Dengue Dengue Fever Is ADocument2 pagesCaused by The .: Dengue Dengue Fever Is AEdrese AguirreNo ratings yet
- Guidance For Industry: Clinical Pharmacology Data To Support A Demonstration of Biosimilarity To A Reference ProductDocument18 pagesGuidance For Industry: Clinical Pharmacology Data To Support A Demonstration of Biosimilarity To A Reference ProductBrian WilliamsNo ratings yet