Professional Documents
Culture Documents
Fraktur Femur
Uploaded by
Yusuf BrilliantOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Fraktur Femur
Uploaded by
Yusuf BrilliantCopyright:
Available Formats
The Journal of TRAUMA Injury, Infection, and Critical Care
Changes in the Management of Femoral Shaft Fractures in Polytrauma Patients: From Early Total Care to Damage Control Orthopedic Surgery
Hans-Christoph Pape, MD, Frank Hildebrand, MD, Stephanie Pertschy, MD, Boris Zelle, MD, Rayeed Garapati, MD, Kai Grimme, MD, and Christian Krettek, MD
Background: The optimal treatment of major fractures in patients with blunt multiple injuries continues to be discussed. The aim of this study is to investigate the clinical course of polytrauma patients treated at a Level I trauma center within the last two decades regarding the effect of changes in the management of their femoral shaft fracture. Methods: In a retrospective cohort study performed at a Level I trauma center, the patients injuries and clinical outcomes were studied. Adult blunt polytrauma patients were included if a femoral shaft fracture eligible for intramedullary stabilization was stabilized (including external fixation) primarily < 8 hours after primary admission. Patients were separated according to the management strategies for the femur fracture (I intramedullary nailing [IIMN]; I external fixation [IEF]; I plate osteosynthesis [Iplate]) followed during a certain time period: (1) early total care (ETC) (January 1, 1981December 31, 1989) and early (< 24 hours) definitive stabilization; (2) intermediate (INT) (January 1, 1990 December 31, 1992) change in the protocol; or (3) damage control orthopedic surgery (DCO) (January 1, 1993December 31, 2000), early (< 24 hours) temporary stabilization, and secondary conversion to intramedullary nailing in patients at risk of organ failure. Results: The patient groups were comparable regarding age, gender distribution, and the mechanism of injury. Primary external fixation was performed significantly more frequent in the INT (23.9%) and DCO (35.6%) groups compared with the ETC group (16.6%) (p 0.02 ETC vs. DCO). Plating of the femur was almost abolished in the 1990s (DCO, 6.8%; ETC, 23.4%). In the subgroups categorized to IEF (ETC, 41.1 points; INT, 37.1 points; DCO, 39.1 points), the general injury severity was higher in comparison with the IIMN group (ETC, 38.3%; INT, 36.1%; DCO, 35.8%). Thoracic or abdominal injuries accounted for significantly higher numbers of patients submitted to IEF in the INT (13.6%, p 0.03) and DCO (17.3%, p 0.01) groups, compared with the ETC (8.1%) group. A higher incidence of reamed nailing was present in the ETC group compared with the other groups (ETC, 96.1%; INT, 73.7%; DCO, 13.5%). No significant differences in the incidence of local complications were found. The incidence of multiple organ failure decreased significantly from the ETC to the DCO period regardless of the type of treatment of the femoral fracture. Moreover, there was a significantly higher incidence of acute respiratory distress syndrome (ARDS) when IIMN (15.1%) and IEF (9.1%) in the DCO subgroup were compared. Conclusion: A significant reduction in the incidence of general systemic complications regardless of the type of femur fixation used was found when comparing the time periods of 1981 to 1989 (ETC), 1990 to 1992 (INT), and 1993 to 2000 (DCO). The change in treatment protocols to external fixation and from reamed to unreamed nailing was not associated with an increased rate of local complications (pin-track infections, delayed unions, nonunions). Among other causes for the improved general outcome during the most recent time period (DCO), an increase in the frequency of air rescue, a change from reamed to unreamed nailing, and an increased awareness toward thoracic and abdominal injuries may have played a role. Even during the DCO era, IMN was associated with a higher rate of ARDS than IEF. In view of a lower complication rate despite higher injury severity compared with the ETC period, the introduction of DCO appears to be an adequate alternative for patients at high risk of developing posttraumatic systemic complications such as ARDS and multiple organ failure. Key Words: Blunt multiple trauma, Damage control orthopedics, Major fractures, Femoral shaft fractures, Operative treatment.
J Trauma. 2002;53:452462.
he immediate and complete definitive operative care of all fractures represents the optimal treatment for the patient with multiple orthopedic injuries. The benefits of this approach have been demonstrated in numerous studies within the past two decades.1 4 However, certain exceptions have been discussed in the past few years, where the principle of early total care may not
be beneficial (head and chest trauma, high Injury Severity Score [ISS] predisposing to posttraumatic complications, borderline patients).5 8 In these, the surgical burden may even increase the risk of postoperative complications.9 11 For these patients, the concept of initial temporary fixation and secondary conversion to a definitive procedure has recently
From the Department of Orthopaedics and Trauma Surgery, Hannover Medical School (H.-C.P., F.H., S.P., B.Z., K.G., C.K.), Hannover, Germany, and Department of Orthopaedics, Mount Sinai School of Medicine (R.G.), New York, New York. Address for reprints: Hans-Christoph Pape, MD, Department of Trauma Surgery, Hannover Medical School, Carl Neubergstr. 1, 30625 Hannover, Germany; email: pape.hans-christoph@mh-hannover.de. DOI: 10.1097/01.TA.0000025660.37314.0F
Submitted for publication September 24, 2001. Accepted for publication January 9, 2002. Copyright 2002 by Lippincott Williams & Wilkins, Inc. This work was scheduled for presentation at the 61st Annual Meeting of the American Association for the Surgery of Trauma, which was canceled because of the terrorist attacks of September 11, 2001.
452
September 2002
Influence of Damage Control Orthopedics after Blunt Polytrauma
been advocated, and the term damage control orthopedic surgery was coined.12 It was derived from trauma patients with abdominal and pelvic injuries, where initial hemorrhage control and secondary planned revision for definitive care has been shown to improve the postoperative course.1315 In our department, the concepts of treating femoral shaft fractures in polytrauma patients have changed substantially during the past decade. We reviewed the posttraumatic clinical course after these injuries regarding our management protocols.
PATIENTS AND METHODS
Patients
This is a retrospective investigation derived from a database that contains the records of 4,628 trauma patients treated between January 1, 1975, and December 31, 2000, at our institution. The database involves ongoing data collection on admissions for multiple injuries to our unit. It was collected retrospectively before 1992 and a prospective data collection was performed thereafter. Twice-daily entries of clinical and physiologic parameters and organ function scores during the first 3 weeks of admission to intensive care are performed. All injuries are classified by the trauma physician, who also routinely calculates the ISS. Outcome events, and major complications during the course, are also recorded on an ongoing basis. The patients were treated according to similar protocols regarding early intubation and ventilation, and aggressive resuscitation.16
Fig. 1. Hannover protocol for fracture management of the femur in patients with multiple injuries. OR, operating room; ETC, early total care; DCO, damage control orthopedic; Ex. Fix., external fixation. (Reprinted from The American Journal of Surgery, Volume 183, Pape H-C, Giannoudis P, Krettek C, The timing of fracture treatment in polytrauma patients: relevance of damage control orthopaedic surgery, pp. 622 629, 2002, with permission from Excerpta Medica Inc.)
hour chest radiograph. The diagnosis was made regardless of the presence or absence of rib fractures.22 The diagnosis of shock was made when the systolic blood pressure dropped below 90 mm Hg despite volume treatment and catecholamine infusions. Pin-track infection and wound infection were diagnosed according to Greens criteria.23
Treatment Protocols
The trauma protocol used at our institution foresees that a long bone fracture is classified as an emergency that has to be stabilized acutely (at least 8 hours) either by internal operations or by external fixation. Thus, a patient who is in critical condition because of another associated injury may undergo laparotomy or craniotomy first and then be submitted to stabilization of the long bone fracture.17 A patient who is highly unstable during this procedure may undergo external fixation parallel to the abdominal/cranial operation or may be transferred to the intensive care unit (ICU), where an external fixateur is then placed (Fig. 1).18 We do not place a patient on the intensive care unit before the operative procedure for improvement of the general condition, but without stabilization of the fracture.
Inclusion Criteria
The inclusion criteria for all patients were as follows: age 19 to 65 years, blunt multiple trauma, ISS of 18 or more, presence of a femoral shaft fracture eligible for intramedullary stabilization, and primary surgery begun at 8 hours after admission, including external fixation for major fractures.
Data Collection
From the database, demographic data were used. In addition, clinical parameters of organ function and therapy reflecting the posttraumatic course were documented (incidence of acute respiratory distress syndrome [ARDS], ICU complications).
Definitions
The severity of injury was categorized preoperatively using the ISS.19 The initial neurologic state was evaluated according to the Glasgow Coma Scale score.20 Primary surgery was defined as an operative intervention within 24 hours posttrauma. Multiple organ failure was defined according to the criteria of Moore et al.21 Lung contusion was defined as a parenchymal pulmonary lesion diagnosed on initial chest computed tomographic scan (lung contusion) or by radiologic findings on the 24Volume 53 Number 3
Group Distribution
Three different time periods were identified: 1. Early total care (ETC) (patients treated between January 1, 1981, and December 31, 1989). The protocol for the treatment of the femoral shaft fracture was early ( 24 hours) definitive stabilization. 2. Intermediate period (INT) (patients treated between January 1, 1990, and December 31, 1992). During this period, a change in the usual protocol for the treatment of the femoral shaft fracture in patients with multiple 453
The Journal of TRAUMA Injury, Infection, and Critical Care
Table 1 Patient Demographics
Time Periods 19811989, ETC (%) 19901992, INT (%) 19932000, DCO (%) p Value*
No. of patients Mean age (yr) Sex (M/F) Mechanism MVC Pedestrian Motorcyclist Other Mean rescue time (min) Type of rescue system Helicopter Ambulance
235 32.7 127/108 177 (75.3) 027 (11.5) 028 (11.9) 003 (1.3) 068 039 (16.6) 196 (83.4)
88 33.1 46/42 57 (64.7) 14 (15.9) 13 (14.8) 04 (4.5) 52 42 (47.7) 46 (52.3)
191 29.9 102/89 153 (80.1) 019 (9.9) 017 (8.9) 002 (1.1) 048 121 (63.4) 070 (36.6)
NS NS NS NS NS NS NS 0.01 0.03
MVC, motor vehicle crash. * The p value indicates the comparison of the rescue systems between the ETC period and the DCO period.
injuries at risk of posttraumatic complications occurred from early ( 24 hours) definitive stabilization toward early temporary fixation. 3. Damage control orthopedic surgery (DCO) (patients treated between January 1, 1993, and December 31, 2000). The usual protocol for the treatment of the femoral shaft fracture in patients with multiple injuries at risk of posttraumatic complications was early ( 24 hours) temporary stabilization, followed by secondary conversion to intramedullary nailing. Moreover, three subgroups were identified according to the type of femur fixation: IIMN (intramedullary instrumentation within 8 hours after admission), IEF (IIIMN) (external fixation within 8 hours after admission), and Iplate (plate osteosynthesis within 8 hours after admission).
RESULTS
Patients were included if they were injured between January 1, 1981, and December 31, 2000; 514 patients fulfilled the inclusion criteria and were included in the study. The demographic data demonstrate comparable patient groups regarding age, gender distribution, and mechanism of injury. The mean rescue time indicates a tendency toward a more rapid primary admission to our unit in the INT and DCO groups compared with ETC patients. This difference was not significant. There was a significant difference in the ratio between patients rescued by helicopter versus ambulances between the ETC period and the DCO period (Table 1).
Patients Who Were Excluded or Who Were Managed Nonoperatively
During the entire study period, nonoperative management of the femoral shaft occurred in 13 patients, all of whom were admitted in extremis. During the ETC period, all eight patients died within 24 hours after admission, six from their severe head injuries and two from a contralateral traumatic 454
hemipelvectomy. During the INT period, the one who had his femur not stabilized also died of cerebral herniation. During the DCO period, two of three patients who did not undergo femoral stabilization died of head injury hours after admission to the ICU; one patient who had been rolled over had crush injuries of his thoracic and abdominal organs and died hours after admission to the ICU. The mean ISS in these patients was 67. We have therefore felt that the small number of patients and the overall severity of their injuries does not provide useful information for the general treatment of these fractures. According to our database, 11 patients were excluded because the time interval between admission and the beginning of the first surgical intervention exceeded 8 hours. Among these were five patients during the ETC period (mean ISS, 41 points; three died from head trauma), three patients during the INT period (mean ISS, 48 points; two died from their severe chest injuries 24 hours), and three patients during the DCO period (mean ISS, 51 points; two died from head trauma 24 hours). Table 2 lists the group distribution regarding the type of femur fixation. The percentage of primary intramedullary fixations was comparable during all three time periods. Primary external fixation was performed significantly more frequently in the INT and DCO groups compared with the ETC group. Plating of the femur was almost abolished in the period from 1993 to 2000 (Table 2). There were significantly higher mean injury severities of the head and the chest compared with the other anatomic regions. These occurred in IEF patients in all time periods. All other Abbreviated Injury Scale values demonstrated no statistically significant differences between the subgroups or between the time periods. The general injury severity was higher in patients categorized to IEF in comparison with the IIMN group. There was a trend toward lower ISS in those patients submitted to IIMN in the years 1993 to 2000 comSeptember 2002
Influence of Damage Control Orthopedics after Blunt Polytrauma
Table 2 Group Distribution*
Time Periods Patient Subgroups 19811989, ETC (%) 19901992, INT (%) 19932000, DCO (%) p Value
IIMN IEF, IIIMN Iplate
141 (60) 039 (16.6) 055 (23.4)
36 (40.9) 21 (23.9) 31 (35.2)
110 (57.6) 068 (35.6) 013 (6.8)
NS 0.02 0.003
* The p values in the table indicate the comparison between ETC and DCO. The p values between groups INT and DCO are 0.05 for the IIMN patients, 0.04 for the IEF patients, and 0.02 for I plate patients.
pared with the previous time periods. This trend was statistically significant at p 0.05 between the ETC and DCO groups. A similar trend occurred in the group experiencing plate osteosynthesis (Table 3). The percentages of patients in whom the indications for external fixation were head injury or hemorrhagic
shock did not change during the different time periods. Thoracic or abdominal injuries accounted for significantly higher numbers of patients submitted to IEF in the INT and DCO groups, compared with the ETC group (Table 4). The general techniques for intramedullary stabilization did not change during the three time periods. The numbers of
Table 3 Injury Severity*
ETC INT DCO p Value
AIS head IIMN IEF, IIIMN Iplate AIS face IIMN IEF, IIIMN Iplate AIS thorax IIMN IEF, IIIMN Iplate AIS abdomen IIMN IEF, IIIMN Iplate AIS extremity IIMN IEF, IIIMN Iplate AIS external IIMN IEF, IIIMN Iplate ISS IIMN IEF, IIIMN Iplate
2.1 2.9 2.3 0.8 0.4 0.8 3.8 4.1 2.8 1.2 1.1 1.4 3.9 4.2 3.4 0.7 0.3 0.4 38.3 41.1 38.4
2.2 3.0 2.4 0.4 0.6 0.8 3.4 4.0 2.9 1.3 1.0 1.2 3.7 4.4 2.8 0.4 0.5 0.3 36.1 37.1 34.1
2.1 2.9 2.2 0.6 0.6 0.4 2.6 3.8 3.4 1.4 1.2 1.7 3.9 4.3 3.0 0.6 0.7 0.5 35.8 39.1 33.1
NS NS NS NS NS NS 0.02 NS 0.05 NS NS NS NS NS NS NS NS NS 0.05 NS 0.05
* The p values in the table indicates differences between ETC and DCO. Indicates p values below 0.05 in comparison between group IIMN and the other subgroups.
Table 4 Indications for External Fixation
ETC n (%) INT n (%) DCO n (%) p Value
Head injury Shock Thoracic/abdominal injury Others
10 (4.2) 09 (3.8) 19 (8.1) 01 (0.4)
04 (4.5) 05 (5.7) 12 (13.6) 0
14 (7.3) 12 (6.3) 33 (17.3) 09 (4.7) 0.03 DCO vs. INT, p
NS NS * 0.01 DCO vs. ETC).
* Statistically significant differences between the DCO group and the other groups (p
Volume 53 Number 3
455
The Journal of TRAUMA Injury, Infection, and Critical Care
Table 5 Specifics of Fracture Treatment
ETC INT DCO p Value
IMN antegrade IMN retrograde Percentage of reamed IMN Mean duration of EF (days)
175/180 005/180 96.1 3.8
51/57 6/57 73.7 4.1
152/178 26/178 13.5 4.6 0.05 DCO vs. INT, p
NS NS * NS 0.005 DCO vs. ETC).
* Statistically significant differences between the DCO group and the other groups (p
antegrade/retrograde nailings and the mean duration of EF were comparable. There was a higher incidence of reamed nailing in the ETC group compared with the other groups (Table 5). Table 6 documents no significant differences in the incidence of local complications, infections, or hardware failure despite the treatment changes over the years. As demonstrated in Table 7, there was no significant change in the hospital stay between the subgroups. The incidence of postinjury multiple organ failure (MOF) decreased significantly from the ETC to the DCO period, regardless of the type of treatment of the femoral fracture. Moreover, there was a significantly higher incidence of MOF in comparing IIMN and IEF in the DCO subgroup. A similar distribution occurred regarding the incidence of ARDS (Table 7). The patients listed in Table 7 in subgroup IEF are the ones in whom conversion to an intramedullary device was performed later.
Patients in Whom No Conversion to an Intramedullary Device Was Performed
The distribution of patients where the external fixateur was left in place differs between the three time periods. Of 22 patients (mean ISS, 52 points) in whom no conversion to an intramedullary device was performed, 13 belonged to the ETC group, 2 belonged to the INT group, and 7 belonged to the DCO group. Of the 13 patients in the ETC group (mean ISS, 55 points), all had developed ARDS and 6 developed MOF (7 deaths). During the INT period, one patient developed MOF and one developed ARDS (two deaths). Of nine patients during the DCO period (mean ISS, 63 points), five developed MOF and two developed ARDS (seven deaths).
Statistical Analysis
Data were tested for normal distribution. Differences between groups were compared by two-way analysis of vari-
Table 6 Postoperative Local Complications
ETC INT DCO p Value
Pin-track infection Wound infection Osteomyelitis Hardware failure EF IMN/Plate Delayed union Nonunion
2/39 5/235 2/235 3/39 3/196 1/235 1/235
3/21 2/88 0/88 1/21 1/67 1/88 1/88
4/68 3/191 1/191 5/68 1/123 2/191 1/191
NS NS NS NS NS NS NS
Table 7 Postoperative Course
ETC (%) INT (%) DCO (%) p Value*
Hospital stay IIMN IEF, IIIMN Iplate MOF IIMN IEF; IIIMN Iplate ARDS IIMN IEF, IIIMN Iplate
14.6 15.1 14.2
5 2 1
13.7 14.7 12.9
5 4 3
13.9 13.4 15.8
4 3 4
NS NS NS 0.03 0.03 0.02 0.003 0.002 0.001
51 (21.7) 39 (16.6) 46 (19.6) 77 (32.7) 38 (16.2) 45 (19.1)
17 (19.3) 14 (15.9) 17 (19.3) 20 (22.7) 10 (11.4) 14 (15.9)
31 (16.2) 22 (11.5) 8 (4.2) 29 (15.1) 15 (7.8) 4 (2.1)
* p values indicate significant differences between ETC and DCO. Indicates a significant (p 0.05) difference between IIMN vs. IEF.
456
September 2002
Influence of Damage Control Orthopedics after Blunt Polytrauma
ance with repeated measurement design. Means were tested by post hoc analysis using the Fishers least significance difference test. Values of p 0.05 were considered significant. Proportions were evaluated using the Yates statistics. Before drawing any meaningful conclusions from these results, it must be considered that the investigation summarizes a long period during which sustained changes in the general management have occurred. Among the known factors, an improvement in rescue system organization and in the education of rescue physicians may be relevant. Since the late 1980s, a standardized training course has been required for rescue physicians in Germany. It includes intubation and placement of a chest tube at the scene of the accident. There has also been an improvement in the initial and perioperative monitoring of patients with multiple injuries. The systemic or pulmonary volume status and blood flow can be quantified by invasive or noninvasive techniques. Both may aid in assessing the true volume requirements if these are clouded by chest trauma or other trauma-related pathologic conditions. It is also evident that the modes of prevention and treatment of postinjury organ failure in the ICU have improved. Early enteral feeding, sophisticated volume replacement, and substantial technical improvements of artificial ventilators may play an important role. These and other changes can partially explain why the general rate of complications has decreased over the past two decades.27 To improve the reliability of the present study, only those patients admitted primarily were enrolled. Thus, the influence of different treatment protocols and rescue conditions from other facilities was excluded. Moreover, a minimum Injury Severity Score of 18 was selected to focus on those patients prone to have a higher risk of developing posttraumatic complications. Previous studies have also investigated general changes in the management of patients with multiple injuries and provided interesting results.16 We therefore feel that, despite a long period of investigation, certain conclusions can be drawn from this study. The first main result outlined abovethe improvement in the treatment of patients with multiple injuriesmay be adequately explained in the previous paragraphs. The second main result may indicate that the change in treatment of the femoral shaft fracture has contributed to this positive development. It can be suspected from the fact that within the last observation period (DCO), IIMN patients demonstrated a higher number of postoperative systemic complications compared with IEF patients, even though in IIMN patients the injury severity was lower. It is likely that the surgical burden from external fixation (operation time, associated blood loss, intraoperative temperature loss) is lower than that from intramedullary nailing. However, no other clinical studies are available that compare the surgical burden from external fixation with that from intramedullary nailing. Inflammatory parameters have been shown to be more sensitive than clinical measurements in determining the surgical burden.28 Proinflammatory markers are known to be pathologically elevated early after trauma29,30 and have also been demonstrated to represent markers of the severity of the surgeryinduced stress response.31 Previous measurements of inflammatory parameters revealed that the changes associated with 457
DISCUSSION
The question of optimal timing of definitive fracture stabilization represents a continuing challenge to all physicians involved in the care of severely injured patients. It would be ideal to perform a prospective randomized trial in groups of patients that sustained identical injuries, underwent identical rescue conditions, presented with comparable injury severities and injury distributions, and were treated favorably in a single trauma center. Court-Brown criticized previous retrospective studies8 in that the patient groups were not comparable and suggested that a prospective study should be performed.24 However, even if the goals discussed above were achievable, several factors continued to be uncontrolled, namely, the influence of age, gender differences, and differences in rescue conditions. Moreover, the impact of a surgical procedure has been discussed to be clinically relevant, especially in those patients who have a high risk of developing posttraumatic complications (e.g., high ISS, severe singleorgan injury).25 The unavailability of a sufficiently high patient number meeting the inclusion criteria within an acceptable period of time appears to be a major obstacle.26 In this light, the aim of the current retrospective study was to investigate whether the changes in the treatment of femur shaft fractures affected the clinical course in patients with multiple blunt injuries. The first main result indicates that the incidence of posttraumatic systemic complications decreased significantly within the study period in three patient groups that underwent different types of treatment for a femoral shaft fracture, although demonstrating similar demographic data, Injury Severity Scores, and rescue conditions. This tendency occurred regardless of the type of fracture fixation. The second main result demonstrates that in patients submitted to IEF, the incidence of posttraumatic local and systemic complications was comparable with those assigned to IIMN, even though their Injury Severity Scores were higher. The third main finding is an increased incidence of ARDS in patients during the damage control era, when they were submitted to primary intramedullary stabilization of the femur shaft when compared with external fixation. This finding was not associated with a higher mortality in this subgroup. Moreover, the relative percentage of patients who developed ARDS decreased from 54.6% (ETC) to 26.4% (DCO) when IIMN was performed and decreased from 97.4% (ETC) to 22.1% when IEF was performed. This may demonstrate that different indications for IEF were chosen over the different time periods. Volume 53 Number 3
The Journal of TRAUMA Injury, Infection, and Critical Care
IMN are comparable to those of a total hip arthroplasty and that an additive inflammatory reaction in the presence of multiple injuries can be determined.32 We are unable to comment on this issue in the current study because these parameters have not been available during the ETC period and the INT period. Also, our findings are in line with two other important recent clinical studies. Scalea et al. reviewed patients treated between July 1995 and June 1998 and assessed the feasibility of planned conversion from external fixation to intramedullary nailing of the femur. Their study reported that patients submitted to primary intramedullary stabilization usually had lower Injury Severity Scores. In addition, several clinical parameters (blood and fluid requirements) demonstrated that these patients had been in a better clinical condition before undergoing initial definitive fracture repair. Conversion from EF to IMN was not associated with local or systemic complications. Forty-three of 284 patients (15.1%) were submitted to this procedure. The authors therefore concluded that temporary EF represents a safe and viable alternative in patients at high risk for postoperative complications and organ failure. Moreover, a distinct term was coined to better describe the clinical approach (damage control orthopedic surgery).12 Another group from the same institution looked at patients treated between 1989 and 1997, and focused on medical and orthopedic problems after intramedullary fixation. They reported an infection rate of 1.7% and an acceptable number of unplanned reoperations, and also concluded that EF is a safe method for selected trauma patients.33 Beyond our main findings addressed above, we feel that the description of the treatment changes also represents important information regarding the treatment of femoral shaft fractures in polytrauma patients. First, the number of patients admitted by the primary rescue helicopter has risen within the three investigation time periods (ETC, 16.5%; INT, 47.7%; DCO, 36.6%). The mean rescue times demonstrated a tendency toward shorter rescue, but no significant changes. It is therefore conceivable that the rescue conditions have not had a major influence on the results obtained. Second, it is of note that the incidence of Iplate osteosynthesis decreased from 23.4% in the ETC group to only 6.8% among patients of the DCO group. In DCO patients, special situations were responsible for the decision as to why a plate was used instead of an intramedullary device. Four patients had open fractures in the midshaft area, in addition to multiple other injuries, and the treating surgeon placed the plate directly through the wound. Nine other patients had bisegmental fractures and were treated with a dynamic condylar screw, thus including concomitant proximal fracturesit is of note that all these fractures could also have been treated by an intramedullary device (e.g., proximal femoral nail or Gamma nail). Moreover, when determining the evidence of primary surgery in the time period between 1981 and 1989, it must be considered that the indications for IM mailing were more narrow than to date. Previously, most of 458 the biomechanical investigations demonstrating favorable properties of the intramedullary procedure were not yet available. Therefore, it appears that the indication for performing primary definitive surgery included plating more often in the ETC group than in the DCO group. The apparent similarity in the IIMN group between the ETC (60%) and the DCO (57.6%) period should be viewed in this light, and a higher number of intramedullary nailings could have been performed in the ETC period. Third, the percentage of reamed procedures decreased significantly during the three time periods (ETC, 96.1%; INT, 73.7%; DCO, 13.5%). The effect of this change on the incidence of local and systemic posttraumatic complications is difficult to evaluate. Previous clinical and experimental studies have demonstrated that there may be a certain reduction in the operative burden when an unreamed procedure is performed.34 36 Krpfl et al. demonstrated less severe fat intravasation and less associated inflammatory reactions.37 Smith et al. reported immunologic alterations after femoral nailing and measured the systemic interleukin-10 release and the class II human leukocyte antigen-DR expression on peripheral blood mononuclear cells. Reamed femoral nailing was associated with greater impairment of immune reactivity than the unreamed nailing technique.38 Our previous clinical investigations revealed a significant increase of elastase levels in central venous blood in patients during reamed compared with unreamed femoral nailing, associated with an increase in the stimulatory capacity of polymorphonuclear leukocytes.39 In contrast, De Groote et al., in a large prospective, randomized, multicenter evaluation, reported no significant differences between two patient groups submitted to either reamed or unreamed nailing. In this well-conducted study, a large number of patients were enrolled and a fair number of patients had multiple injuries.40 One may therefore wonder why the subclinical effects described above did not become apparent in this clinical study. Different rescue conditions or geographic differences could play a role. The relatively small size of Germany and the tight, overlapping rescue system may lead to admission of patients to German hospitals that are severely injured but who, because of the short rescue, may be in an apparently stable condition (borderline). These patients would then most likely have problems surviving or would truly be unstable if the geographic situation caused a longer period until definitive rescue could occur. Also, the severity of thoracic injuries may be different in various countries.41 In the current study, the higher incidence of ARDS during the DCO era in patients submitted to unreamed nailing compared with external fixation can be viewed in this light. During this era, the treating physician was thought to have carefully evaluated the clinical status. Nevertheless, a number of patients remained that developed postoperative pulmonary complications. Thus, the clinical evaluation in these patients still appears to have been performed falsely. This would then September 2002
Influence of Damage Control Orthopedics after Blunt Polytrauma
support the idea of a borderline situation where the special risk continues to be difficult to evaluate. Acute immunologic monitoring, as can be obtained since a short period of time, may be the key to further classify the clinical status in the future. However, the influence of all these effects geographic peculiarities and rescue conditions, the degree of chest trauma in various countries and its influence on the incidence of ARDS, and the difficulty in evaluating the clinical status and the possible role of inflammatory monitoring have not been well studied so far and require further investigation. Local complications have to be considered when judging the effectiveness of a certain type of fracture treatment. In this light, some authors have argued that the unreamed procedure is associated with a higher incidence of delayed unions because of a small intramedullary contact area and a smaller nail diameter.42 In contrast, opponents have claimed that the destruction of the intramedullary blood supply plays a role in terms of a delay in healing, if the reamed procedure is selected,43 and have described increased blood loss with the reamed procedure.44 Our data reveal a comparable general rate of delayed union and nonunion, as described in other studies.45 47 In addition, the change in treatment principles (ETC vs. DCO) of femoral shaft fractures did not appear to depend on the type of operation (unreamed vs. external fixation) (data not shown). The unreamed procedure was selected for various reasons, and the tendency toward less systemic effects was only one of them. Previous authors have wondered whether the placement of an external fixateur and subsequent conversion to intramedullary nailing might increase the risk of local complications. However, as demonstrated in Table 6, there were no statistically significant differences regarding wound infection, osteomyelitis, or hardware failure. Moreover, the rate of nonunions did not increase during the time period when increased use of a temporary external fixateur was performed. Fourth, there appeared to have been an increased awareness of thoracic and abdominal injuries (Table 4). These diagnoses accounted for placement of an external fixator in 8.5% of patients between 1981 and 1989 and in 17.3% between 1993 and 2000. The incidence of systemic complications in comparison between the IIMN group and the IEF group was not significantly different despite higher Injury Severity Scores in the IEF groups. It is likely that the change in the management has also contributed to the favorable results in the DCO group. In addition, this effect may have been because of our improved diagnostic abilities regarding chest injuries. Numerous studies have demonstrated that accurate grading of the severity of thoracic trauma48,49 and the prediction of later complications50,51 is difficult. Moreover, if pulmonary contusions are present, their dynamic nature is well known. The admission chest radiographs have been found to underestimate the severity of pulmonary contusion.52 Our recent investigations demonstrated that serial chest radiographs over 24 hours after admission have a Volume 53 Number 3 significantly higher diagnostic yield from an initial rate of diagnoses of pulmonary contusions of 42.3% to 93.7% of all diagnosed unilateral contusions. The development of computed tomography has helped a great deal in this respect,53 which may reflect the numbers indicated in Table 4. What effects did these changes have on the hospital course? There was no significant change in the hospital stay between the IIMN group and the IEF group. This is an unexpected finding because it may be hypothesized that the conversion to IMN would delay the overall hospital course. One possible explanation may lie in the fact that there was a tendency in the IIMN group for longer ventilation therapy that could be attributed to some selected patients who had a very long initial hospitalization period (data not shown) and may have caused an increase in the mean ICU stay. The incidences of MOF and ARDS were lower in the groups submitted to IEF despite a tendency toward a higher ISS in this treatment group. The treatment of the femoral fracture may have contributed to this favorable result, but other factors are likely to have played a role as well. Because of the retrospective nature of the study, we may have summarized groups of patients that are preselected by their clinical status. These patients may then have been correctly identified as high-risk patients and treated as such by the surgeon in charge. If this assumption was true, one may argue that the clinical impression is of higher value than some of the scoring systems used in this study. For example, the calculation of the Injury Severity Score may underestimate the clinical status if a patient is admitted with numerous open fractures but without any injuries to another body region. It may also be interesting to compare all cardiorespiratory parameters and the inflammatory mediators in these patients. However, as outlined above, these were not available in the current study. Another important factor that may be studied in the future is the indication for performing damage control orthopedic surgery. In the present study, the overall incidence of IEF ranged between 16.6% in the ETC group and 35.6% in the DCO group. This percentage is higher than in both other studies dealing with this issue.12,30 During the earlier time period investigated by Nowotarski et al. (1989 1997), 4% of patients underwent primary EF, and it increased to 15.1% of patients (19951998). This interesting finding could be because of patient selection or a worse condition of these patients at admission. In addition, it may also represent a trend toward a more frequent use of EF (i.e., a modulated indication to perform primary temporary fixation between the studies). One may then argue that future studies are necessary to investigate proper indications for DCO treatment. In view of the favorable outcome in patients submitted to DCO, this variation observed between the clinical studies is an observation with apparently negligible clinical impact. However, it is most noteworthy and encouraging for all future clinical investigations that patients collected from different time pe459
The Journal of TRAUMA Injury, Infection, and Critical Care
riods and institutions from different continents appear to have the same positive tendency toward outcome in favor of the principle of damage control orthopedic surgery. In conclusion, a significant reduction in the incidence of general systemic complications regardless of the type of femur fixation used was found in comparison between the time periods of 1981 to 1989 (ETC), 1990 to 1992 (INT), and 1993 to 2000 (DCO). Although various medical improvements may have contributed to these positive developments, several specific differences in the general management of traumatized patients might have played a role. These included an increase in the frequency of air rescue, a decrease in the number of plate osteosynthesis procedures, a change from reamed to unreamed nailing, and an increased awareness toward thoracic and abdominal injuries in the most recent time period (DCO). It is noteworthy that despite these changes toward the DCO era, IIMN was still associated with a higher risk of ARDS when compared with external fixation. No adverse effects were attributed to the treatment change from external fixation to intramedullary nailing in terms of local complications, hardware failure, local infections, or fracture healing. The introduction of DCO is likely to have had a positive impact in the treatment of the femoral shaft fracture in polytrauma patients without the risk of side effects, and it appears to be an adequate alternative for patients at high risk of posttraumatic complications.
8. Carlson DA, Rodman GH, Kaehr D, Hage J, Misinski M. Femur fractures in chest-injured patients: is reaming contraindicated? J Orthop Trauma. 1998;12:164 168. Giannoudis PV, Smith RM, Bellamy MC, Morrison JF, Dickson RA, Guillou PJ. Stimulation of the inflammatory system by reamed and unreamed nailing of femoral fractures. J Bone Joint Surg Br. 1999; 81:356 361. Townsend RN, Lheureau T, Protetch J, et al. Timing fracture repair in patients with severe brain injuries. J Trauma. 1998;44:977981. Jaicks RR, Cohn SM, Moller BA. Early fracture fixation may be deleterious after head injury. J Trauma. 1997;42:1 6. Scalea TM, Boswell SA, Scott JD, et al. External fixation as a bridge to intramedullary nailing for patients with multiple injuries and with femur fractures: damage control orthopedics. J Trauma. 2000;48:613 623. Burch JM, Ortiz VB, Richardson RJ, Lewis F. Abbreviated laparotomy and planned reoperation for critically injured patients. Ann Surg. 1992;215:476 483. Talbert S, Trooskin SZ, Scalea T, et al. Packing and reexploration for patients with nonhepatic injuries. J Trauma. 1992;33:121126. Henry SM, Tornetta P, Scalea TM. Damage control for devastating pelvic and extremity injuries. Surg Clin North Am. 1997;77:879 895. Regel G, Lobenhoffer P, Grotz M, Pape H-C, Lehmann U, Tscherne H. Treatment results of patients with multiple trauma: an analysis of 3406 cases treated between 1972 and 1991 at a German Level I Trauma Center. J Trauma. 1995;38:70 77. Tscherne H, Regel G, Pape H-C, Pohlemann T, Krettek C. Internal fixation of multiple fractures in patients with polytrauma. Clin Orthop. 1998;347:6278. Pape H-C, Giannoudis P, Krettek C. The timing of fracture treatment in polytrauma patients: relevance of damage control orthopaedic surgery. Am J Surg. 2002;183:622 629. Baker SP, ONeill B, Haddon W, Long WB. The injury severity score: a method for describing patients with multiple injuries and evaluating emergency care. J Trauma. 1974;14:187196. Teasdale G, Jennett B. Assessment of coma and impaired consciousness: a practical scale. Lancet. 1974;2:81 89. Moore FA, Moore EE, Poggetti R, et al. Gut bacterial translocation via the portal vein: a clinical perspective with major torso trauma. J Trauma. 1991;31:629 638. Pape H-C, Remmers D, Rice J, Winny M, Ebisch M, Tscherne H. Appraisal of early evaluation of blunt chest trauma: development of a standardized scoring system for initial clinical decision making. J Trauma. 2000;49:496 504. Green SA. Complications of external fixation. Clin Orthop. 1983; 180:109 114. Court-Brown CM. Invited commentary. J Orthop Trauma. 1998; 12:175176. Offner PJ, Moore EE. Risk factors for MOF and pattern of organ failure after severe trauma. In: Baue AE, Faist E, Fry M, eds. Multiple Organ Failure. New York: Springer-Verlag; 1999:30 43. Reynolds MA, Richardson JD, Spain DA, et al. Is timing of fracture fixation important for the patient with multiple trauma? Ann Surg. 1995;222:470 481. Baue AE. Are we making progress in preventing and treating MOF? In: Baue AE, Faist E, Fry M, eds. Multiple Organ Failure. New York: Springer-Verlag; 1999;656 663. Ogura H, Tanaka H, Koh T, et al. Priming, second hit priming, and apoptosis in leukocytes from trauma patients. J Trauma. 1999; 46:774 783. Roumen R, Hendrijks T, ven der Ven-Jongekrijk J, Nieuwenhuizen G, Sauerwein R, Goris RJ. Cytokine patterns in patients after major vascular surgery, hemorrhagic shock, and severe blunt trauma. Ann Surg. 218;6:769 776.
9.
10. 11. 12.
13.
14. 15.
16.
17.
18.
ACKNOWLEDGMENT
This manuscript is dedicated to the retirement of Harald Tscherne, who had the first University Chair for Unfallchirurgie in Germany since 1970. His influence vividly stimulated the development of trauma and orthopedic surgery in Germany. His concepts yielded the way for the strategies described in this manuscript. He resigned in October 2000, having fulfilled 30 years of trauma leadership in Europe.
19.
20. 21.
REFERENCES
1. Johnson KD, Cadambi A, Seibert B. Incidence of adult respiratory distress syndrome in patients with multiple musculoskeletal injuries: effect of early operative stabilization of fractures. J Trauma. 1985; 25:375381. Bone LB, Johnson KD, Weigelt J, et al. Early versus delayed stabilization of fractures. J Bone Joint Surg Am. 1989;71:336 339. Seibel R, LaDuca J, Hassett JM, et al. Blunt multiple trauma (ISS 36), femur traction, and the pulmonary failure-septic state. Ann Surg. 1985;202:283295. Pape H-C, AufmKolk M, Paffrath T, et al. Primary intramedullary fixation in polytrauma patients with associated lung contusion: a cause of posttraumatic ARDS? J Trauma. 1993;34:540 548. Nast-Kolb D, Waydhas C, Jochum M, Spannagl M, Duswald K-H, Schweiberer L. Is there a favorable time for the management of femoral shaft fractures in polytrauma? [in German]. Chirurg. 1990; 61:259 265. Pelias ME, Townsend MC, Flancbaum L. Long bone fractures predispose to pulmonary dysfunction in blunt chest trauma despite early operative fixation. Surgery. 1992;111:576 579. Schller W, Gaudernack T. Lungenkomplikationen nach Oberschenkelmarknagelung. Hefte Unfallheilkunde. 1986;182:273 278.
22.
23. 24. 25.
2. 3.
4.
26.
5.
27.
28.
6.
29.
7.
460
September 2002
Influence of Damage Control Orthopedics after Blunt Polytrauma
30. Roumen R, Redl H, Schlag G, et al. Inflammatory mediators in relation to the development of multiple organ failure in patients after severe blunt trauma. Crit Care Med. 1995;23:474 480. Baigrie RJ, Lamont PM, Dallman M, Morris PJ. The release of Il-1 precedes that of Il-6 in patients undergoing major surgery. Lymphokine Cytokine Res. 1991;10:253256. Pape H-C, Barthels M, van Griensven M, Krettek C, das Gupta R, Tscherne H. Biochemical changes following trauma and skeletal surgery of the lower extremity: quantification of the operative burden. Crit Care Med. 2000;28:34413448. Nowotarski PJ, Turen CH, Brumback RJ, Scarboro JM. Conversion of external fixation to intramedullary nailing for fractures of the shaft of the femur in multiply injured patients. J Bone Joint Surg Am. 2000;82:781788. Anwar IA, Olson SA, Battistella FD. Pulmonary consequences of reamed versus unreamed intramedullary femur fixation: a prospective randomized study. Presented at: 57th Annual Meeting of the American Association for the Surgery of Trauma, September 24 27, 1997, Waikoloa, Hawaii. Pape H-C, Dwenger A, Regel G, et al. Pulmonary damage after intramedullary femoral nailing in sheep: is there an effect of different nailing methods? J Trauma. 1992;33:574 581. Pape H-C, Regel G, Dwenger A, et al. Influences of different methods of intramedullary femoral nailing on lung function in patients with multiple trauma. J Trauma. 1993;35:709 715. Krpfl A, Davies J, Berger U, Hertz H, Schlag G. Intramedullary pressure and bone marrow fat extravasation in reamed and unreamed femoral nailing. J Orthop Res. 1999;17:261268. Smith RM, Giannoudis PV, Bellamy MC, Perry BS, Dickson RA, Guillou PJ. Interleukin-10 release and monocyte human leukocyte antigen-DR expression during femoral nailing. Clin Orthop. 2000; 73:233240. Pape HC, Regel G, Dwenger A, et al. Influences of different methods of intramedullary femoral nailing on lung function in patients with multiple trauma. J Trauma. 1993;35:709 715. De Groote R, Powell J, Buckley R, et al. A prospective randomized clinical trial comparing reamed versus unreamed intramedullary femoral nailing of femoral shaft fractures. Assessment of pulmonary dysfunction. Presented at: 14th Annual Meeting of the Orthopaedic Trauma Association; October 8 10, 1998, Vancouver, Canada. Sturm JA, Lackner C, Sittaro N, Grimme K, Pape H-C. Trauma care in Germany. J Trauma. In press. Clatworthy MG, Clark DI, Gray DH, Hardy AE. Reamed versus undreamed femoral nails. J Bone Joint Surg Br. 1998;80:485 489. Schemitsch EH, Kowalski MJ, Swiontkowski MF, Senft D. Cortical blood flow in reamed and unreamed intramedullary nailing: a fractured tibia model in sheep. J Orthop Trauma. 1994;8:373382. Tornetta P III, Tiburzi D. The treatment of femoral shaft fractures using intramedullary interlocked nails with and without intramedullary reaming: a preliminary report. J Orthop Trauma. 1997;11:89 92. Wolinsky P, McCarthy E, Shyr S, Johnson K. Reamed intramedullary nailing of the femur: 551 cases. J Trauma. 1999; 46:392399. Brumback RJ, Uwagie-Ero S, Lakatos RP, et al. Intramedullary nailing of femoral shaft fractures. J Bone Joint Surg Am. 1988; 70:14531462. Winquist RA, Hansen ST, Clawson DK. Closed intramedullary nailing of femoral shaft fractures: a report on 520 cases. J Bone Joint Surg Am. 1984;66:529 539. Fulton RL, Peter ET. The progressive nature of pulmonary contusion. Surgery. 1970;67:499 506. McGonigal M, Schwab W, Kauder W, Miller W, Grumbach K. Supplemental emergent chest computed tomography in the management of blunt torso trauma. J Trauma. 1990;30:14311435. 50. Pape H-C, Remmers D, Grotz M, et al. Levels of antibodies to endotoxin and cytokine release in patients with severe trauma: does posttraumatic dysergy contribute to organ failure? J Trauma. 1999; 46:907912. 51. Nast Kolb D, Waydhas C, Gippner-Steppat C, et al. Indicators of the posttraumatic inflammatory response correlate with organ failure in patients with multiple injuries. J Trauma. 1997;42:446 451. 52. Schild HH, Strunk H, Weber W, et al. Pulmonary contusion: CT vs plain radiograms. J Comput Assist Tomogr. 1989;13:417 420. 53. Toombs BD, Sandler SV, Lester RG. Computed tomography of chest trauma. Radiology. 1981;140:733738.
31.
32.
33.
EDITORIAL COMMENT
One of the major beneficial evolutions in trauma care over the past decade has been the concept of damage control surgery. As we have improved our understanding of the circulatory response to hemorrhage and have accordingly refined our resuscitative strategies, trauma surgeons have moved away from the concept of early definitive operative repair of intra-abdominal,1,2 vascular,3,4 and orthopedic injuries.5 Instead, it has become increasingly apparent that focusing on complete and effective resuscitation of the patient carries a much higher priority than definitive surgical repairs. To some degree, we have known this principle for a much longer time than the past decade, because relatively low priority injuries such as facial fracture fixations have been operatively addressed in a delayed manner at most trauma centers for several decades. What has changed in recent years is the broader application of this principle of delayed definitive management to injuries of all types in severely injured patients. Dr. Pape and colleagues have provided a useful retrospective view of the evolution of femoral shaft fracture management for 514 severely injured patients admitted to a single Level I German trauma center over a 26-year period. The major point of the article is that the transition from primary definitive femoral fixation (using intramedullary instrumentation) to a damage control approach (with temporary stabilization followed by secondary conversion to intramedullary nailing) has been associated with a reduction in the incidence of both multiple organ failure and ARDS. Moreover, despite the increased use of external fixation and delayed definitive repair, there was not an increase in the local complication rate. While encouraging that such improvements in outcome can be detected, it is important to note that they occurred in an environment and over a time period that has been characterized by change. For example, over this same time period, the authors noted that the use helicopter transports increased from 16.6% to 63.4%, with a corresponding decline in ambulance transports. No doubt other changes in management have occurred over this long time period, including the areas of hemodynamic monitoring and support, ventilator therapy, antibiotic agents, and nutrition, to name but a few. The specific impact of the orthopedic management on the incidence of organ failure is difficult to tease out of such a 461
34.
35.
36.
37.
38.
39.
40.
41. 42. 43.
44.
45.
46.
47.
48. 49.
Volume 53 Number 3
The Journal of TRAUMA Injury, Infection, and Critical Care
noisy background and could only be determined through the conduct a prospective, randomized, controlled clinical trail comparing damage control measures to definitive surgery. Given the overwhelming complexity such a study would present and the fact that the quality of trauma care appears to be continuously improving, it is not likely that such a study will ever be conducted. This report by Pape and colleagues may therefore be as good an analysis as we will get on the issue of the orthopedic management of femur fractures in severely injured patients. R Lawrence Reed II, MD, FACS, FCCM Professor of Surgery Loyola University Medical Center Maywood, Illinois
REFERENCES
Morris JA Jr, Eddy VA, Blinman TA, Rutherford EJ, Sharp KW. The staged celiotomy for trauma: issues in unpacking and reconstruction. Ann Surg. 1993;217:576 586. 2. Rotondo MF, Schwab CW, McGonigal MD, et al. Damage control: an approach for improved survival in exsanguinating penetrating abdominal injury. J Trauma. 1993;35:375383. 3. Reilly PM, Rotondo MF, Carpenter JP, Sherr SA, Schwab CW. Temporary vascular continuity during damage control: intraluminal shunting for proximal superior mesenteric artery injury. J Trauma. 1995;39:757760. 4. Porter JM, Ivatury RR, Nassoura ZE. Extending the horizons of damage control in unstable trauma patients beyond the abdomen and gastrointestinal tract. J Trauma. 1997;42:559 561. 5. Henry SM, Tornetta P 3rd, Scalea TM. Damage control for devastating pelvic and extremity injuries. Surg Clin North Am. 1997; 77:879 895. 1.
462
September 2002
You might also like
- Blood Supply of BrainDocument12 pagesBlood Supply of BrainSharon Rose Genita Medez100% (1)
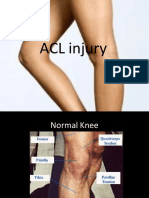
- Anterior Cruciate Ligament-Injury & ManagementDocument101 pagesAnterior Cruciate Ligament-Injury & ManagementYusuf Brilliant100% (1)
- Timing of Fixation of Major Fractures in Blunt Polytrauma: Role of Conventional Indicators in Clinical Decision MakingDocument13 pagesTiming of Fixation of Major Fractures in Blunt Polytrauma: Role of Conventional Indicators in Clinical Decision MakingArun JoyNo ratings yet
- Biomechanics of The HipDocument12 pagesBiomechanics of The HipSimon Ocares AranguizNo ratings yet
- Decision Making Pain Ramamurthy PDFDocument319 pagesDecision Making Pain Ramamurthy PDFDian wNo ratings yet
- Damage Control OrthopedicsDocument17 pagesDamage Control OrthopedicsterencedszaNo ratings yet
- Development of The Central Nervous SystemDocument39 pagesDevelopment of The Central Nervous SystemRyan SaganNo ratings yet
- Birth TraumaDocument18 pagesBirth TraumaJemmy SieNo ratings yet
- EnemaDocument4 pagesEnemaNeelofur Ibran AliNo ratings yet
- List of Hospitals in Addis Ababa (Ethiopia) : Sghk@ethionet - EtDocument7 pagesList of Hospitals in Addis Ababa (Ethiopia) : Sghk@ethionet - EtErmias AssefaNo ratings yet
- CPG Management of Severe Childhood CariesDocument46 pagesCPG Management of Severe Childhood Cariesumiraihana1No ratings yet
- Dco 5 PDFDocument10 pagesDco 5 PDFGauda GranthanaNo ratings yet
- Length of Stay Total Knee ArthroplastyDocument9 pagesLength of Stay Total Knee ArthroplastyRista MarginaNo ratings yet
- Medi 97 E0523Document9 pagesMedi 97 E0523Andrea OsborneNo ratings yet
- Surgical Treatment of Chronic Elbow Dislocation Allowing For Early Range of Motion: Operative Technique and Clinical ResultsDocument8 pagesSurgical Treatment of Chronic Elbow Dislocation Allowing For Early Range of Motion: Operative Technique and Clinical ResultsLuis Carlos HernandezNo ratings yet
- Moderator:Dr Vijay Kumar Co-Moderator:Dr Venketish All India Institute of Medical Sciences New DelhiDocument58 pagesModerator:Dr Vijay Kumar Co-Moderator:Dr Venketish All India Institute of Medical Sciences New DelhiWasim R. IssaNo ratings yet
- Boissonneault2019 PDFDocument17 pagesBoissonneault2019 PDFBangkit PrimayudhaNo ratings yet
- Art:10.1186/1471 2474 15 188Document8 pagesArt:10.1186/1471 2474 15 188indriNo ratings yet
- Clinical Outcomes of Locked Plating of Distal Femoral Fractures in A Retrospective CohortDocument9 pagesClinical Outcomes of Locked Plating of Distal Femoral Fractures in A Retrospective Cohortisnida shela arloviNo ratings yet
- Journal of Orthopaedic Surgery and ResearchDocument17 pagesJournal of Orthopaedic Surgery and ResearchRyuu RupiNo ratings yet
- Ankle Arthrodesis After Severe InfectionDocument5 pagesAnkle Arthrodesis After Severe InfectionSeagate PramonoNo ratings yet
- Complications After Free Ap Surgery: Do We Need A Standardized Classification of Surgical Complications?Document6 pagesComplications After Free Ap Surgery: Do We Need A Standardized Classification of Surgical Complications?drpuneetjindalNo ratings yet
- 08 Subasi NecmiogluDocument7 pages08 Subasi Necmiogludoos1No ratings yet
- 1 s2.0 S0737614618300017 MainDocument22 pages1 s2.0 S0737614618300017 MainJEFFERSON MUÑOZNo ratings yet
- Timing of Cranioplasty After Decompressive Craniectomy ForDocument5 pagesTiming of Cranioplasty After Decompressive Craniectomy ForjoerizalNo ratings yet
- Clinical StudyDocument7 pagesClinical StudyAldo AtjehNo ratings yet
- 152 FullDocument8 pages152 FullJuan Camilo MateusNo ratings yet
- Pi Is 0976566220304872Document11 pagesPi Is 0976566220304872rivanNo ratings yet
- Cho Vanes 2012Document17 pagesCho Vanes 2012Luiggi GordilloNo ratings yet
- Bahan ReferatDocument17 pagesBahan ReferatGisma CNo ratings yet
- Management of Pertrochanteric Fractures inDocument8 pagesManagement of Pertrochanteric Fractures inantonio dengNo ratings yet
- Augmentation Plating Leaving The Nail in Situ Is An Excellent Option For Treating Femoral Shaft Nonunion After IM Nailing: A Multicentre StudyDocument7 pagesAugmentation Plating Leaving The Nail in Situ Is An Excellent Option For Treating Femoral Shaft Nonunion After IM Nailing: A Multicentre StudytomimacagnoNo ratings yet
- Journal of Clinical Orthopaedics and TraumaDocument8 pagesJournal of Clinical Orthopaedics and TraumaandiNo ratings yet
- Wound Healing Complications in Closed and Open Calcaneal FracturesDocument6 pagesWound Healing Complications in Closed and Open Calcaneal FracturesMaryamNo ratings yet
- 2015 Inclusion of Trigger Point Dry Needling in A Multimodal Physical Therapy Program For Postoperative Shoulder Pain, A Randomized Clinical TrialDocument9 pages2015 Inclusion of Trigger Point Dry Needling in A Multimodal Physical Therapy Program For Postoperative Shoulder Pain, A Randomized Clinical TrialCarlos Meriño GuzmanNo ratings yet
- What Factors Are Associated With Elbow Stiffness After Operation of Terrible Triad InjuryDocument16 pagesWhat Factors Are Associated With Elbow Stiffness After Operation of Terrible Triad InjuryAndrea OsborneNo ratings yet
- Distal Humerus Fracture in Patients Over 70 Years of Age: Results of Open Reduction and Internal FixationDocument8 pagesDistal Humerus Fracture in Patients Over 70 Years of Age: Results of Open Reduction and Internal FixationSantiago Coba GonzálezNo ratings yet
- Intertan Nail Vs PFN ADocument7 pagesIntertan Nail Vs PFN AzubayetarkoNo ratings yet
- Jurnal IrfanDocument9 pagesJurnal IrfanrizkiNo ratings yet
- Abstracts - Final Off Print BJNDocument57 pagesAbstracts - Final Off Print BJNZieshNo ratings yet
- Fijacion Percutane Temprana TL en PolitraumaDocument6 pagesFijacion Percutane Temprana TL en PolitraumaSacha SalasNo ratings yet
- Abstracts Estes Congress 2010 WebDocument238 pagesAbstracts Estes Congress 2010 WebAna Cláudia CarriçoNo ratings yet
- Comparing Erector Spinae Plane Block With Serratus Anterio - 2020 - British JourDocument9 pagesComparing Erector Spinae Plane Block With Serratus Anterio - 2020 - British JourtasyadelizaNo ratings yet
- Nakashima2013 Article CharacterizingTheNeedForTracheDocument7 pagesNakashima2013 Article CharacterizingTheNeedForTracheCristian GiovanniNo ratings yet
- Outpatient Tympanomastoidectomy: Factors Affecting Hospital AdmissionDocument4 pagesOutpatient Tympanomastoidectomy: Factors Affecting Hospital AdmissionGuillermo StipechNo ratings yet
- Surgical Outcomes After Traumatic Open Knee Dislocation: Ó Springer-Verlag 2009Document6 pagesSurgical Outcomes After Traumatic Open Knee Dislocation: Ó Springer-Verlag 2009agus sukarnaNo ratings yet
- Pape2005 PDFDocument12 pagesPape2005 PDFantonio dengNo ratings yet
- DiniDocument10 pagesDiniMuhammad Yasdar BahriNo ratings yet
- 1 s2.0 S1877056821003029 MainDocument21 pages1 s2.0 S1877056821003029 MainAndrea OsborneNo ratings yet
- Posttrx Empyema PDFDocument6 pagesPosttrx Empyema PDFAndyGcNo ratings yet
- J Jpedsurg 2008 06 024Document1 pageJ Jpedsurg 2008 06 024afsdsaadsNo ratings yet
- Conversion VATSDocument6 pagesConversion VATSAlin Ionut BurlacuNo ratings yet
- 1471-2474-13-81 KonsulDocument7 pages1471-2474-13-81 KonsulGustan AriadiNo ratings yet
- 2013 4 Spine12876Document9 pages2013 4 Spine12876Rendy SusantoNo ratings yet
- EgyptOrthopJ50145-8454425 232904tgtDocument6 pagesEgyptOrthopJ50145-8454425 232904tgtAzmi FarhadiNo ratings yet
- Sweet Et Al. Systematic Review Clavicle and Rib FracturesDocument8 pagesSweet Et Al. Systematic Review Clavicle and Rib FracturesRut Herdianti P. EkasiwiNo ratings yet
- Open Pelvic Fracture: The Killing Fracture?Document8 pagesOpen Pelvic Fracture: The Killing Fracture?odyNo ratings yet
- Functiuonal Out5come After Sugical Tratment of Ankle Fracture Using Baird Jackon ScoreDocument4 pagesFunctiuonal Out5come After Sugical Tratment of Ankle Fracture Using Baird Jackon ScoreAxell C MtzNo ratings yet
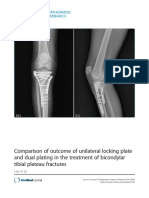
- Comparison of Outcome of Unilateral Locking Plate and Dual Plating in The Treatment of Bicondylar Tibial Plateau FracturesDocument9 pagesComparison of Outcome of Unilateral Locking Plate and Dual Plating in The Treatment of Bicondylar Tibial Plateau Fracturesana starcevicNo ratings yet
- Chest Wall Stabilization in Trauma Patients: Why, When, and How?Document12 pagesChest Wall Stabilization in Trauma Patients: Why, When, and How?Ariane YudhiantiNo ratings yet
- Injury: Serdar Onat, Refik Ulku, Alper Avci, Gungor Ates, Cemal OzcelikDocument5 pagesInjury: Serdar Onat, Refik Ulku, Alper Avci, Gungor Ates, Cemal OzcelikEdomiyas ZenebeNo ratings yet
- Resident Participation in Fixation of Intertrochanteric Hip FracturesDocument10 pagesResident Participation in Fixation of Intertrochanteric Hip FracturesSantiago MartinezNo ratings yet
- Intramedullary Nailing of Subtrochanteric Fractures: Does Malreduction Matter?Document5 pagesIntramedullary Nailing of Subtrochanteric Fractures: Does Malreduction Matter?Reza ParkerNo ratings yet
- Lberaçao Capsular Posteror CrurgcaDocument7 pagesLberaçao Capsular Posteror CrurgcaEduardo FilhoNo ratings yet
- Johannesson 2004Document13 pagesJohannesson 2004Faeyz OrabiNo ratings yet
- EjercicioDocument12 pagesEjercicioVillateAngelaNo ratings yet
- 1 s2.0 S0266435613004105 MainDocument5 pages1 s2.0 S0266435613004105 MainMr-Ton DrgNo ratings yet
- Effect of Scrotal Hitching in Reducing Scrotal Edema After Inguinoscrotal Hernia RepairDocument4 pagesEffect of Scrotal Hitching in Reducing Scrotal Edema After Inguinoscrotal Hernia RepairIOSRjournalNo ratings yet
- Case Studies of Postoperative Complications after Digestive SurgeryFrom EverandCase Studies of Postoperative Complications after Digestive SurgeryNo ratings yet
- Management of IV Fluids and Electrolyte Balance Slides PDFDocument29 pagesManagement of IV Fluids and Electrolyte Balance Slides PDFYusuf BrilliantNo ratings yet
- G Yepes 1966Document9 pagesG Yepes 1966Yusuf BrilliantNo ratings yet
- Anteriorcruciateligamentinjury 090619120341 Phpapp01 121206081353 Phpapp02Document23 pagesAnteriorcruciateligamentinjury 090619120341 Phpapp01 121206081353 Phpapp02Yusuf BrilliantNo ratings yet
- Management of Peritonitis in Critically Ill PatientDocument29 pagesManagement of Peritonitis in Critically Ill PatientYusuf BrilliantNo ratings yet
- Anatomy of Anterior Cruciate LigamentDocument60 pagesAnatomy of Anterior Cruciate LigamentYusuf BrilliantNo ratings yet
- Staph KeratinDocument9 pagesStaph KeratinYusuf BrilliantNo ratings yet
- Window Anatomy PDFDocument7 pagesWindow Anatomy PDFYusuf BrilliantNo ratings yet
- Behavioural Anchored Rating ScalesDocument1 pageBehavioural Anchored Rating ScalesYusuf BrilliantNo ratings yet
- Diagnosis HipoglikemiaDocument4 pagesDiagnosis HipoglikemiaYusuf BrilliantNo ratings yet
- How To Read A Head CT: DR Mohamed El Safwany. MDDocument60 pagesHow To Read A Head CT: DR Mohamed El Safwany. MDYusuf BrilliantNo ratings yet
- Leptospira As An Emerging PathogenDocument12 pagesLeptospira As An Emerging PathogenYusuf BrilliantNo ratings yet
- Super HumanDocument1 pageSuper HumanYusuf BrilliantNo ratings yet
- Be Careful With This Fraudster Network Malaysian InvestmentDocument14 pagesBe Careful With This Fraudster Network Malaysian InvestmentYusuf BrilliantNo ratings yet
- A Rare Cause of Endocarditis: Streptococcus PyogenesDocument3 pagesA Rare Cause of Endocarditis: Streptococcus PyogenesYusuf BrilliantNo ratings yet
- Measles Virus PathogenesisDocument12 pagesMeasles Virus PathogenesisYusuf BrilliantNo ratings yet
- Leptospira As An Emerging PathogenDocument12 pagesLeptospira As An Emerging PathogenYusuf BrilliantNo ratings yet
- Measles Virus PathogenesisDocument12 pagesMeasles Virus PathogenesisYusuf BrilliantNo ratings yet
- Drag RaceDocument1 pageDrag RaceYusuf BrilliantNo ratings yet
- Crottt Uuuh AaaahhDocument1 pageCrottt Uuuh AaaahhYusuf BrilliantNo ratings yet
- Daftar PenyakitDocument46 pagesDaftar PenyakitNindya RimaliviaNo ratings yet
- Measles Virus PathogenesisDocument12 pagesMeasles Virus PathogenesisYusuf BrilliantNo ratings yet
- Slide PosterDocument11 pagesSlide PosterYusuf BrilliantNo ratings yet
- File PetingDocument1 pageFile PetingYusuf BrilliantNo ratings yet
- Gagal Jantung 2013Document83 pagesGagal Jantung 2013Yusuf BrilliantNo ratings yet
- Diagnosis HipoglikemiaDocument4 pagesDiagnosis HipoglikemiaYusuf BrilliantNo ratings yet
- ABSTRAKS STUDI ,,,SEKSUAL - AUSTRALIA - EditDocument2 pagesABSTRAKS STUDI ,,,SEKSUAL - AUSTRALIA - EditYusuf BrilliantNo ratings yet
- New Issues in Hypertension Blood Pressure (Juli 2005)Document47 pagesNew Issues in Hypertension Blood Pressure (Juli 2005)Yusuf BrilliantNo ratings yet
- Merck Manual: OF Diagnosis and TherapyDocument22 pagesMerck Manual: OF Diagnosis and TherapyScholl_201133% (3)
- EBNDocument5 pagesEBNyanishappyNo ratings yet
- Medical Treatment For Dandruff: in This Leafl Et: 2. Before You Use Selsun ShampooDocument2 pagesMedical Treatment For Dandruff: in This Leafl Et: 2. Before You Use Selsun ShampooCharles Franklin Joseph100% (1)
- Approach To Episiotomy - UpToDateDocument13 pagesApproach To Episiotomy - UpToDatePedro Vilches Polaina100% (1)
- OxytocinDocument1 pageOxytocinSubbie OutlierNo ratings yet
- Iap Guide Book On Immunization 2009 - 2010Document175 pagesIap Guide Book On Immunization 2009 - 2010bapsamits100% (1)
- Chelation of Gadolinium Oxford 2009Document3 pagesChelation of Gadolinium Oxford 2009gasfgdNo ratings yet
- 1 Aakash Hospital BrochureDocument4 pages1 Aakash Hospital BrochureAakashNo ratings yet
- UNEP Directory March 2021Document23 pagesUNEP Directory March 2021Chris JohnNo ratings yet
- Most Common ENT Diseases in School Going Children (5-15 Years of Age) in Our HospitalDocument3 pagesMost Common ENT Diseases in School Going Children (5-15 Years of Age) in Our HospitalAnonymous izrFWiQNo ratings yet
- Nursing SchoolsDocument31 pagesNursing SchoolsKathy Claire Pecundo Ballega100% (1)
- Prema V Opalustre MIHDocument8 pagesPrema V Opalustre MIHbrigidgaffneyNo ratings yet
- Hospital Strategic Plan Presentation ExampleDocument12 pagesHospital Strategic Plan Presentation ExampleDennis DaviesNo ratings yet
- HamdardDocument4 pagesHamdardNaved Hussain100% (1)
- Teorya NG PagtanggapDocument6 pagesTeorya NG PagtanggapMaxine TaeyeonNo ratings yet
- Vital Signs Chart 3Document1 pageVital Signs Chart 3Adrian CraciunNo ratings yet
- Cristian Colceriu - Elitele României - Prof. Dr. Ștefan Florian - Cluj Contemporary ElitesDocument15 pagesCristian Colceriu - Elitele României - Prof. Dr. Ștefan Florian - Cluj Contemporary Elitescristian colceriuNo ratings yet
- HipotermiaDocument6 pagesHipotermiaThelma SamcamNo ratings yet
- CGHSDocument30 pagesCGHSDevender SharmaNo ratings yet
- Symposium Program - 2017Document16 pagesSymposium Program - 2017api-1937195310% (1)
- Fractura de EscafoidesDocument37 pagesFractura de EscafoidesCamilo Vidal100% (1)
- PCCDocument6 pagesPCCFakiha BukhariNo ratings yet
- Thesis Book - Suhasini Vasireddy - Ravi Teja - TITLE FINALDocument4 pagesThesis Book - Suhasini Vasireddy - Ravi Teja - TITLE FINALRaviteja PadiriNo ratings yet