Professional Documents
Culture Documents
Geriatrics Restraints
Uploaded by
Rinkish DalliahOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Geriatrics Restraints
Uploaded by
Rinkish DalliahCopyright:
Available Formats
GERONTOLOGY UPDATE
Restraints and Alternatives
Cindy Gatens, MN RN CRRN-A The use of physical restraints in older adults is associated with poor outcomes: functional decline, cardiovascular stress, decreased peripheral circulation, incontinence, muscle atrophy, pressure ulcers, infections, agitation, social isolation, loss of selfesteem, serious injuries, and even death. However, physical and chemical restraints are sometimes necessary to protect the patient, staff, and others from harm. To address concerns about the improper use of restraints (and seclusion) the Centers for Medicare & Medicaid Services (CMS) published their final rule regulations for hospitals effective January 8, 2007. The regulations included additional expectations for staff education, face-toface evaluations, formal noticegiven upon admissionof patients rights and freedom from inappropriate use of restraint and seclusion, and reporting of death due to restraint and seclusion. According to CMS regulations, a restraint is any manual method, physical or mechanical device, material, or equipment that immobilizes the ability of a patient to move his or her arms, legs, body, or head freely...or a drug or medication when it is used as a restriction to manage the patients freedom of movement and is not a standard treatment or dosage for the patients condition (Department of Health and Human Services, CMS, 2006). Although CMS agrees that restraining may be an appropriate part of a patients plan of care, they strongly advocate that restraints only be used when absolutely necessary and when other measures have been unsuccessful. Hospitals have responded by attempting to reduce restraint use and increase alternatives. Rehabilitations nurses who care for the elderly have the opportunity to creative devise creative care plans that manage patient behaviors without using restraints. Older patients with dementia have the highest risk for being restrained when hospitalized. Elderly patients with impaired memory, judgement, and comprehension often have difficulty adapting to the hospital setting. At particular risk for restraint use are patients whose behavior (i.e., confusion, agitation, impulsivity) is judged to be unsafe (i.e., contributing to falls or interfering with treatment or medical devices). Other hospitalized elderly at risk are those who have experienced stroke or brain injury with cognitive deficits resulting in impulsivity, wandering, confusion, impaired judgement, agitation, and aggression. Many rehabilitation facilities have significantly reduced the number of restraint episodes or become restraint free by relying on various alternative measures for preventing and managing problematic behaviors. 8 ARNNetwork
Confusion
The rehabilitation nurses comprehensive assessment addressing the cause of confusion must include any physiologic, pharmacologic, emotional, and environmental factors that may be responsible for an individuals unsafe behavior. This data can provide information about safety risk and also can help define strategies for restraint-free management and care. Knowing the older adults premorbid behavior and function is essential for personalizing care. Any behavior that precipitates a decision to restrain a patient should first trigger an investigation aimed at recognizing and eliminating the cause of the behavior (e.g., recognize that a common reason for bed exit is the need to toilet; anticipate the need by putting the patient on a toileting schedule). A medication review of the side effects and medication effects on cognition is also important. Avoid medications that can aggravate acute confusion in the elderly (e.g., hypnotics, sedatives, antianxiety agents, tricyclic antidepressants, other medications with anticholinergic side effects). Look for other medical conditions that could cause confusion such as infection, dehydration, and pain. Potential restraint-free interventions for managing patients with confusion include maximizing structure and consistency (e.g., memory book, calendar, consistent routines), frequent reorientation, a room near the nursing station, opportunities for exercise and ambulation, toileting schedules, lower bedrails (or use of half rails if ambulatory), implementation of wheelchair and bed exit alarms, discontinuation of lines and tubes if possible, low bed, if appropriate, abdominal binder, long sleeve clothing (or knit sleeve to limit access to lines and tubes), environmental exit alarms that alert an attempted elopement, and continuous observation or family staying with patient, if appropriate.
Agitation and Aggression
It is important to be aware of staff behaviors that may trigger agitation and aggression. Modify behavior by moving and speaking quietly, slowly, and directly, staying relaxed, safely positioning self, redirecting patient to a less stimulating or frustrating activity, discontinuing an activity, not arguing with a patient about behavior, being flexible, and modifying treatment interventions. The environment should be modified by minimizing stimulation (e.g., lights, noise, visitors), maximizing consistency, providing safe motion, activity, and verbalization, providing clear expectations of interactions and treatment, scheduling rest periods, facilitating safety by removing items that could cause injury, arranging for constant observation, or involving family (if calming and reassuring to patient). In todays healthcare climate, rehabilitation nurses are asked to make critical clinical decisions, predicting and anticipating patient behaviors that put both patients and staff at risk for injury. As clinicians and educators, we have a responsibility to be advocates for our elderly patients. Temporary restraints may be an appropriate part of a patients personalized plan of care, but we must strongly advocate that restraints should be used only when absolutely necessary and when other alternatives to avoid restraint have been unsuccessful.
Reference
Department of Health and Human Services, Centers for Medicare & Medicaid Services. (2006). Federal Register, 42 CFR Part 482, Medicare and Medicaid Programs; Hospitals Conditions of Participation: Patients Rights; Final Rule retrieved August 11, 2007 from http://www.cms.hhs.gov/quarterlyproviderupdates/downloads/CMS3018N.pdf.
Suggested Resources
American Geriatrics Society. (1991). AGS Position Statement: Restraint Use retrieved August 11, 2007 from www.americangeriatrics.org/products/positionpapers/restraintsupdatePF.shtml. Markwell, S. (2005). Long-term restraint reduction. Journal Nursing Care Quality, 20(3), 253260. Morris, K. (2007). Issues and answers: Restraint use. Ohio Nurses Review, 82(4), 1415. Sullivan-Marx, E. M. (2001). Achieving restraint-free care of acutely confused older adults, Journal of Gerontological Nursing, 27(4), 5661.
Impulsivity
Restraint-free interventions for impulsivity include cuing the patient to stop, think, and act, verbally reviewing steps before beginning an activity, having the patient rehearse the steps to complete a task, identifying and intervening immediately with impulsive behaviors, reviewing and rehearsing how to appropriately engage in a behavior, completing frequent checks, activating and explaining the bed and wheelchair exit alarms, Cindy Gatens is a clinical nurse specialist at the Ohio State University Medical Center in initiating low bed, if appropriate, placing patient Columbus, OH. in a common area where staff can frequently visualize patient and behaviors, arranging for constant observation, or asking family to stay with patient, if appropriate.
October/November 2007
You might also like
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryFrom EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryRating: 3.5 out of 5 stars3.5/5 (231)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)From EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Rating: 4.5 out of 5 stars4.5/5 (121)
- Grit: The Power of Passion and PerseveranceFrom EverandGrit: The Power of Passion and PerseveranceRating: 4 out of 5 stars4/5 (588)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaFrom EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaRating: 4.5 out of 5 stars4.5/5 (266)
- The Little Book of Hygge: Danish Secrets to Happy LivingFrom EverandThe Little Book of Hygge: Danish Secrets to Happy LivingRating: 3.5 out of 5 stars3.5/5 (400)
- Never Split the Difference: Negotiating As If Your Life Depended On ItFrom EverandNever Split the Difference: Negotiating As If Your Life Depended On ItRating: 4.5 out of 5 stars4.5/5 (838)
- Shoe Dog: A Memoir by the Creator of NikeFrom EverandShoe Dog: A Memoir by the Creator of NikeRating: 4.5 out of 5 stars4.5/5 (537)
- The Emperor of All Maladies: A Biography of CancerFrom EverandThe Emperor of All Maladies: A Biography of CancerRating: 4.5 out of 5 stars4.5/5 (271)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeFrom EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeRating: 4 out of 5 stars4/5 (5794)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyFrom EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyRating: 3.5 out of 5 stars3.5/5 (2259)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersFrom EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersRating: 4.5 out of 5 stars4.5/5 (344)
- Team of Rivals: The Political Genius of Abraham LincolnFrom EverandTeam of Rivals: The Political Genius of Abraham LincolnRating: 4.5 out of 5 stars4.5/5 (234)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreFrom EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreRating: 4 out of 5 stars4/5 (1090)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceFrom EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceRating: 4 out of 5 stars4/5 (895)
- Her Body and Other Parties: StoriesFrom EverandHer Body and Other Parties: StoriesRating: 4 out of 5 stars4/5 (821)
- IBSC-CP-C Candidate Handbook PDFDocument15 pagesIBSC-CP-C Candidate Handbook PDFJuan Manuel Tiscareño GarciaNo ratings yet
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureFrom EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureRating: 4.5 out of 5 stars4.5/5 (474)
- The Unwinding: An Inner History of the New AmericaFrom EverandThe Unwinding: An Inner History of the New AmericaRating: 4 out of 5 stars4/5 (45)
- Drug and Alcohol Awareness ClassDocument71 pagesDrug and Alcohol Awareness ClassRinkish DalliahNo ratings yet
- The Yellow House: A Memoir (2019 National Book Award Winner)From EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Rating: 4 out of 5 stars4/5 (98)
- On Fire: The (Burning) Case for a Green New DealFrom EverandOn Fire: The (Burning) Case for a Green New DealRating: 4 out of 5 stars4/5 (73)
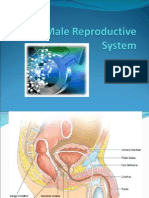
- Male Reproductive SystemDocument49 pagesMale Reproductive SystemRinkish Dalliah50% (2)
- Cardiac Catheterization and AngiographyDocument80 pagesCardiac Catheterization and Angiographyspider_mechNo ratings yet
- Peripheral Vascular Disease NursingDocument13 pagesPeripheral Vascular Disease NursingCatlyn Chatpman100% (1)
- Trans GenerationalDocument7 pagesTrans Generationallara_2772No ratings yet
- ACLS Supplementary Material PDFDocument74 pagesACLS Supplementary Material PDFsmbawasainiNo ratings yet
- Explosive FirepowerDocument15 pagesExplosive FirepowerTS100% (1)
- Post TestDocument9 pagesPost TestPradnya Paramitha100% (2)
- NutritionDocument22 pagesNutritionAsrar ZakNo ratings yet
- Health As A Multifactorial PhenomenonDocument2 pagesHealth As A Multifactorial PhenomenonJan Jamison Zulueta100% (9)
- Biogas Safety Fact SheetDocument68 pagesBiogas Safety Fact SheetKayne HerrimanNo ratings yet
- 04 ICP MonitoringDocument42 pages04 ICP MonitoringRinkish Dalliah100% (1)
- Prevención de RecaídasDocument10 pagesPrevención de RecaídasJean Paul CastroNo ratings yet
- Interventions For ClientsDocument68 pagesInterventions For ClientsRinkish DalliahNo ratings yet
- 77 Ijh Nac Chapter 4Document23 pages77 Ijh Nac Chapter 4Rinkish DalliahNo ratings yet
- 24 A MaleDocument27 pages24 A MaleRinkish DalliahNo ratings yet
- WOQOL Measuring QV MentalDocument15 pagesWOQOL Measuring QV MentalpenfoNo ratings yet
- 14MCSR PregnancyDocument69 pages14MCSR PregnancyRinkish DalliahNo ratings yet
- Fetal SkullDocument11 pagesFetal SkullRinkish DalliahNo ratings yet
- 14MCSR PregnancyDocument69 pages14MCSR PregnancyRinkish DalliahNo ratings yet
- Introduction HivDocument2 pagesIntroduction HivRinkish DalliahNo ratings yet
- Fam Nursing AssessmentDocument1 pageFam Nursing AssessmentRinkish DalliahNo ratings yet
- WaterDocument13 pagesWaterHoppy KishnaNo ratings yet
- HNELHD CG 12 04 Warfarin Age Adjusted Dosing in AdultsDocument5 pagesHNELHD CG 12 04 Warfarin Age Adjusted Dosing in AdultsAnonymous 4txA8N8etNo ratings yet
- Final Programme A4 - IPOS 2023 - CompressedDocument60 pagesFinal Programme A4 - IPOS 2023 - CompressedFlorinaNo ratings yet
- Steroid Use in The Elderly: Postgraduate MedicineDocument8 pagesSteroid Use in The Elderly: Postgraduate MedicineValdi DwiramaNo ratings yet
- Pub105961487 PDFDocument164 pagesPub105961487 PDFTriandini SanusiNo ratings yet
- Complex Regional Pain Syndrome Concise Guidance 1Document6 pagesComplex Regional Pain Syndrome Concise Guidance 1roooNo ratings yet
- Epilepsy PDFDocument15 pagesEpilepsy PDFMohamedErrmaliNo ratings yet
- 3-Introduction To Medicinal Chemistry-And Physicochemical PropertiesDocument39 pages3-Introduction To Medicinal Chemistry-And Physicochemical PropertiesKevin ChapleyNo ratings yet
- SW 3400 Group Portfolio Part IIDocument5 pagesSW 3400 Group Portfolio Part IIapi-687461513No ratings yet
- 6.10.16 Gabrielle Lees Lecture PDFDocument46 pages6.10.16 Gabrielle Lees Lecture PDFRicardo LunaNo ratings yet
- Product CatalogueDocument27 pagesProduct CatalogueHemang M. GajjarNo ratings yet
- 473 eDocument9 pages473 eAzmi FarhadiNo ratings yet
- Form 2 Chapter 2Document7 pagesForm 2 Chapter 2Sue Suraya NazaNo ratings yet
- Patient Details History Discussion and MDT PlanDocument2 pagesPatient Details History Discussion and MDT PlanRogers ByebwaNo ratings yet
- Hydroxychloroquine PDFDocument2 pagesHydroxychloroquine PDFsbsreddy100% (1)
- Blood Warmer ValidationDocument5 pagesBlood Warmer ValidationulgenyNo ratings yet
- Get Big Diet by Jacob WilsonDocument5 pagesGet Big Diet by Jacob WilsonYoel OrueNo ratings yet
- Personality Stability, Development, and ChangeDocument24 pagesPersonality Stability, Development, and ChangeLouNo ratings yet
- Devil's Claw Powerpoint Presentation EditedDocument17 pagesDevil's Claw Powerpoint Presentation EditedMunyaNo ratings yet
- In The Clinic - OsteoporosisDocument16 pagesIn The Clinic - OsteoporosisRoberto López MataNo ratings yet
- Mcinnes2005 Mutismo SelectivoDocument10 pagesMcinnes2005 Mutismo SelectivoCamila SiebzehnerNo ratings yet