Professional Documents
Culture Documents
Nej Me 0902632
Uploaded by
Sylvia PertiwiOriginal Description:
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Nej Me 0902632
Uploaded by
Sylvia PertiwiCopyright:
Available Formats
The
n e w e ng l a n d j o u r na l
of
m e dic i n e
edi t or i a l s
Optimal Management of Acute Coronary Syndromes
L. David Hillis, M.D., and Richard A. Lange, M.D. In the United States, more than a million people are hospitalized annually with unstable angina or myocardial infarction without ST-segment elevation, so-called acute coronary syndromes. For these patients, several treatments have proved to be effective in reducing the incidence of death, infarction or reinfarction, and recurrent ischemia. These treatments include intensive medical therapy and coronary angiography followed by revascularization, if indicated.1,2 Given the sheer number of medical interventions that are now available for these conditions, knowing which therapy to administer and when to do so is confusing for many physicians. The studies by Giugliano et al.3 and Mehta et al.4 in this issue of the Journal provide information that physicians can use to further refine their treatment of such patients. The initial evaluation of patients with acute coronary syndromes should focus on an assessment of the risk of a cardiac ischemic event (death, myocardial infarction, or recurrent ischemia) in the ensuing days, weeks, and months, as well as the risk of a bleeding complication from intensive medical therapy or an invasive cardiac procedure. During the past 10 years, two risk-assessment algorithms have been developed for determining whether a patient is at high risk or at relatively low risk for having an ischemic event. With this information in hand, a treatment strategy can be individually tailored, thereby reducing the occurrence of such an event. The first of these algorithms, the Thrombolysis in Myocardial Infarction (TIMI) risk score,5 uses seven easily assessed variables to identify patients with acute coronary syndromes who are at risk for death, myocardial infarction, or recurrent ischemia within 14 days after hospitalization. These variables are an age of more than 65 years, three or more risk factors for atheroscleron engl j med 360;21
sis, known coronary artery disease, two or more episodes of anginal chest pain in the 24 hours before hospitalization, the use of aspirin in the 7 days before hospitalization, ST-segment deviation of 0.05 mV or more, and elevated serum markers for myocardial necrosis (troponin or creatine kinase MB). Patients with three or more of the seven variables are considered to be at high risk, whereas those with no more than two of the variables are considered to be at low risk.6 The second algorithm, the Global Registry of Acute Coronary Events (GRACE) risk model,7 uses eight variables to predict whether a patient will die or have a myocardial infarction in the hospital or in the next 6 months. These variables are age, Killip class (a classification of the severity of heart failure with myocardial infarction), systolic arterial pressure, ST-segment deviation, cardiac arrest during presentation, serum creatinine concentration, elevated serum markers for myocardial necrosis, and heart rate. Each variable is assigned a numerical score on the basis of its specific value, and the eight scores are added to yield a total score, which is applied to a reference nomogram to determine the patients risk. The GRACE application tool is available at www.outcomes-umassmed. org/grace. A comparison of the TIMI and GRACE risk algorithms concluded that either can be used effectively to predict the rates of death or myocardial infarction for a year after hospitalization for acute coronary syndromes.8 Although serum markers for myocardial necrosis make up only one of the TIMI or GRACE risk variables, the presence of this variable alone identifies a patient as being high risk.9 However, although elevated serum markers indicate myocardial necrosis, they provide no insight into its cause. In some patients, myocardial necrosis is caused by disorders other than coronary artery
nejm.org may 21, 2009
2237
The New England Journal of Medicine Downloaded from nejm.org on March 5, 2013. For personal use only. No other uses without permission. Copyright 2009 Massachusetts Medical Society. All rights reserved.
The
n e w e ng l a n d j o u r na l
of
m e dic i n e
Table 1. Treatment Strategies for Patients with Acute Coronary Syndromes.* Therapy Low-risk patient Antianginal drug1,2 Beta-blocker Nitroglycerin Diltiazem or verapamil Lipid-lowering drug1,2 Statin Antiplatelet drug1,2 Aspirin Clopidogrel Anticoagulant drug1,2 Unfractionated heparin High-risk patient Antianginal drug1,2 Beta-blocker Nitroglycerin Diltiazem or verapamil Lipid-lowering drug1,2 Statin Antiplatelet drug1-3,11,12,15 Aspirin Clopidogrel Glycoprotein IIb/IIIa inhibitor (eptifibatide, tirofiban, or abciximab) Anticoagulant drug1,2,6,14,15 Unfractionated heparin Enoxaparin Immediately Immediately 25 days; discontinue after successful PCI During hospitalization (up to 8 days); discontinue after successful PCI Up to 72 hr; discontinue after successful PCI Death or myocardial infarction Myocardial infarction, recurrent ischemia (as compared with unfractionated heparin) Bleeding Immediately Immediately At time of PCI Indefinitely 12 mo 1224 hr after PCI Death, myocardial infarction Myocardial infarction, recurrent ischemia Myocardial infarction Before hospital discharge Indefinitely Recurrent ischemia Immediately Immediately Immediately During hospitalization, possibly indefinitely During hospitalization, possibly indefinitely During hospitalization, possibly indefinitely Death, myocardial infarction, recurrent ischemia Not studied Myocardial infarction, recurrent ischemia Immediately 25 days Death or myocardial infarction Immediately Immediately Indefinitely 112 mo Death, myocardial infarction Myocardial infarction, recurrent ischemia Before hospital discharge Indefinitely Recurrent ischemia Immediately Immediately Immediately During hospitalization, possibly indefinitely During hospitalization, possibly indefinitely During hospitalization, possibly indefinitely Recurrent ischemia Not studied Myocardial infarction, recurrent ischemia Initiation Duration Reduced Incidence with Drug or Therapy versus Placebo
Bivalirudin Invasive management1,2,4,13 Coronary angiography followed by revascularization (if appropriate)
Immediately
Up to 3680 hr after hospitalization; within 24 hr in very highrisk patients
Myocardial infarction, recurrent ischemia
* PCI denotes percutaneous coronary intervention. This drug should be avoided in patients with decompensated heart failure, hypotension, or hemodynamic instability. The choice of unfractionated heparin, enoxaparin, or bivalirudin should be made on the basis of the patients risk assessment. This benefit assumes that bivalirudin is used as monotherapy, as compared with a combination of heparin and a glycoprotein IIb/IIIa inhibitor.
2238
n engl j med 360;21
nejm.org
may 21, 2009
The New England Journal of Medicine Downloaded from nejm.org on March 5, 2013. For personal use only. No other uses without permission. Copyright 2009 Massachusetts Medical Society. All rights reserved.
editorials
disease (e.g., pulmonary embolism, decompensated heart failure, severe hypertension or tachycardia, anemia, and sepsis). During evaluation of a patient with a possible acute coronary syndrome, the presence of elevated serum markers should be assessed in conjunction with other variables to provide insight into its most likely cause. Independent of this initial risk assessment, the patients general medical and cognitive status, anticipated life expectancy, personal preferences, and risk of treatment-related complications should be evaluated. Since intensive medical therapy and invasive management are associated with bleeding complications, the patients risk of such events should be assessed before these therapies are administered. Female sex, older age, renal insufficiency, low body weight, tachycardia, high or low systolic arterial pressure, low hematocrit, and a history of diabetes mellitus predict an increased risk of major bleeding, often due to the administration of excessive doses of antiplatelet or anticoagulant agents.10 The bleeding risk can be estimated with the tool available at www. crusadebleedingscore.org. Once the risk status of a patient with an acute coronary syndrome is established, treatment is initiated1,2,11-15 (Table 1). Regardless of the patients level of risk, antianginal medications, antiplatelet therapy (aspirin and clopidogrel), and a statin should be administered unless contraindicated.1 Patients who are deemed to be at low risk should receive unfractionated heparin; more intensive (and expensive) antiplatelet or anticoagulant therapy does not further reduce the risk of an ischemic cardiac event but does increase the risk of bleeding.6 Routine coronary angiography and revascularization are not beneficial in such patients and should be reserved for those with recurrent ischemia despite intensive medical therapy.12 In contradistinction, patients who are deemed to be at high risk should receive antianginal medications, antiplatelet therapy (aspirin and clopidogrel), a statin, anticoagulant therapy,1,5,14 and coronary angiography, followed by revascularization, if indicated (Table 1).1,6,12 In addition, glycoprotein IIb/IIIa inhibitors, which provide maximal platelet inhibition, reduce ischemic cardiac events in such patients.1,2,11 The study by Giugliano et al. and other studies15 demonstrate that glycoprotein IIb/IIIa inhibitors should be initiated at the time of angiography; their routine
administration 12 to 24 hours before the procedure carries an increased risk of bleeding and no improvement in outcome. High-risk patients with acute coronary syndromes benefit from coronary angiography and revascularization (if appropriate), in that the incidence of subsequent ischemic cardiac events is reduced.1,2,13 The question arises: Should angiography be performed within hours after presentation or can it be delayed for several days to allow medical therapy to stabilize the recently ruptured arterial plaque, thereby reducing the risk of procedure-related complications? According to the study by Mehta et al., in most patients, the use of early invasive therapy (within 24 hours after hospitalization) is no better at preventing death, myocardial infarction, or stroke than delayed invasive therapy (median time, 50 hours), although early therapy is associated with a modest decrease in the occurrence of recurrent ischemia. In contrast, in the third of patients who were considered to be at very high risk (GRACE risk score, >140, which corresponds to an estimated incidence of in-hospital death or myocardial infarction of >20%), an early invasive strategy was superior to a delayed strategy in reducing the incidence of death, myocardial infarction, or stroke. The treatment of patients with acute coronary syndromes is optimal when the intensity of therapy, both medical and nonmedical (coronary angiography and revascularization), is tailored to the patients risk of an ischemic cardiac event or a treatment-related complication. In patients who are considered to be at high risk, optimal therapy results in a substantial decrease in rates of myocardial infarction and recurrent ischemia (by 20 to 40%) and a modest decrease in the rate of death (by approximately 10%). The magnitude of benefit correlates with the patients level of risk.
No potential conflict of interest relevant to this article was reported. From the Department of Medicine, University of Texas Health Science Center, San Antonio.
1. Anderson JL, Adams CD, Antman EM, et al. ACC/AHA 2007
guidelines for the management of patients with unstable angina/non ST-elevation myocardial infarction: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines (Writing Committee to Revise the 2002 Guidelines for the Management of Patients With Unstable Angina/Non ST-Elevation Myocardial Infarction): developed in collaboration with the American College of Emergency Physicians, the Society for Cardiovascular Angiography and Interventions, and the Society of Thoracic Surgeons: endorsed by the American Association of Cardiovascular and Pulmonary Reha-
n engl j med 360;21
nejm.org
may 21, 2009
2239
The New England Journal of Medicine Downloaded from nejm.org on March 5, 2013. For personal use only. No other uses without permission. Copyright 2009 Massachusetts Medical Society. All rights reserved.
The
n e w e ng l a n d j o u r na l
of
m e dic i n e
bilitation and the Society for Academic Emergency Medicine. Circulation 2007;116(7):e148-e304. [Erratum, Circulation 2008; 117(9):e180.] 2. Bassand JP, Hamm CW, Ardissino D, et al. Guidelines for the diagnosis and treatment of non-ST-segment elevation acute coronary syndromes. Eur Heart J 2007;28:1598-660. 3. Giugliano RP, White JA, Bode C, et al. Early versus delayed, provisional eptifibatide in acute coronary syndromes. N Engl J Med 2009;360:2176-90. 4. Mehta SR, Granger CB, Boden WE, et al. Early versus delayed invasive intervention in acute coronary syndromes. N Engl J Med 2009;360:2165-75. 5. Antman EM, Cohen M, Bernink PJ, et al. The TIMI risk score for unstable angina/non-ST elevation MI: a method for prognostication and therapeutic decision making. JAMA 2000;284:835-42. 6. Sabatine MS, Antman EM. The Thrombolysis in Myocardial Infarction risk score in unstable angina/non-ST-segment elevation myocardial infarction. J Am Coll Cardiol 2003;41:Suppl S: 89S-95S. 7. Eagle KA, Lim MJ, Dabbous OH, et al. A validated prediction model for all forms of acute coronary syndrome: estimating the risk of 6-month postdischarge death in an international registry. JAMA 2004;291:2727-33. 8. de Arajo Gonalves P, Ferreira J, Aguiar C, Seabra-Gomes R. TIMI, PURSUIT, and GRACE risk scores: sustained prognostic value and interaction with revascularization in NSTE-ACS. Eur Heart J 2005;26:865-72. 9. Morrow DA, Cannon CP, Rifai N, et al. Ability of minor elevations of troponins I and T to predict benefit from an early in-
vasive strategy in patients with unstable angina and non-ST elevation myocardial infarction: results from a randomized trial. JAMA 2001;286:2405-12. 10. Subherwal S, Bach RG, Chen AY, et al. Baseline risk of major bleeding in non-ST-segment elevation myocardial infarction: the CRUSADE (Can Rapid risk stratification of Unstable angina patients Suppress ADverse outcomes with Early implementation of the ACC/AHA guidelines) bleeding score. Circulation 2009 March 30 (Epub ahead of print). 11. Boersma E, Harrington RA, Moliterno DJ, et al. Platelet glycoprotein IIb/IIIa inhibitors in acute coronary syndromes: a meta-analysis of all major randomised clinical trials. Lancet 2002;359:189-98. [Erratum, Lancet 2002;359:2120.] 12. Cannon CP, Weintraub WS, Demopoulos LA, et al. Comparison of early invasive and conservative strategies in patients with unstable coronary syndromes treated with the glycoprotein IIb/ IIIa inhibitor tirofiban. N Engl J Med 2001;344:1879-87. 13. Mehta SR, Cannon CP, Fox KA, et al. Routine vs selective invasive strategies in patients with acute coronary syndromes: a collaborative meta-analysis of randomized trials. JAMA 2005; 293:2908-17. 14. Stone GW, McLaurin BT, Cox DA, et al. Bivalirudin for patients with acute coronary syndromes. N Engl J Med 2006;355: 2203-16. 15. Stone GW, Ware JH, Bertrand ME, et al. Antithrombotic strategies in patients with acute coronary syndromes undergoing early invasive management: one-year results from the ACUITY trial. JAMA 2007;298:2497-506.
Copyright 2009 Massachusetts Medical Society.
Antiplatelet Therapy and Vascular-Access Patency
Charmaine E. Lok, M.D. Current predictions estimate that by the year 2020, more than 750,000 people in the United States alone will have end-stage renal disease and over 500,000 will require hemodialysis.1 The success of hemodialysis depends on a well-functioning vascular access, which may be considered the patients lifeline. However, creating and maintaining a vascular access are challenging and costly. In the first year of hemodialysis, care of the vascular access represents the leading cause of hospitalizations; overall costs are over $1 billion annually.2,3 The Dialysis Access Consortium (DAC) Study Group has taken the lead in advancing clinical knowledge of dialysis access dysfunction and clinical approaches to its management.4,5 In this issue of the Journal, Dixon et al.,5 of the DAC Study Group, report the results from a randomized, placebo-controlled trial of the effect of twicedaily extended-release dipyridamole (200 mg) and aspirin (25 mg) on graft patency in 649 patients undergoing hemodialysis. The primary study outcome was the loss of primary unassisted graft
2240
patency, defined as the first occurrence of graft thrombosis or performance of a radiologic or surgical procedure to facilitate graft patency. Patients who received dipyridamole plus aspirin had an absolute risk reduction of 5 percentage points (with an adjusted relative risk reduction of 18%) in the rate of loss of primary unassisted graft patency (adjusted hazard ratio for active treatment vs. placebo, 0.82; 95% confidence interval [CI], 0.68 to 0.98). The median cumulative (overall) graft patency was 22.5 months (95% CI, 20.0 to 28.2) in the placebo group and did not differ significantly in the active-treatment group, nor were there any significant differences between the two groups in the rate of bleeding or any other adverse events. This large and rigorous study evaluating graft outcomes has several important implications. The preferred vascular access for hemodialysis is an autogenous fistula, typically created at the wrist (radiocephalic fistula) or elbow (brachiocephalic or brachiobasilic fistula). Although functioning fistulas are associated with superior pa-
n engl j med 360;21
nejm.org
may 21, 2009
The New England Journal of Medicine Downloaded from nejm.org on March 5, 2013. For personal use only. No other uses without permission. Copyright 2009 Massachusetts Medical Society. All rights reserved.
You might also like
- Lectures CoasDocument74 pagesLectures CoasSylvia PertiwiNo ratings yet
- Tools in Family AssessmentDocument52 pagesTools in Family AssessmentDinda Ulfa Dinda100% (3)
- DR Rendra - Managemen Kedaruratan Bedah Pada DOGADocument58 pagesDR Rendra - Managemen Kedaruratan Bedah Pada DOGASylvia PertiwiNo ratings yet
- DHFDocument23 pagesDHFSylvia PertiwiNo ratings yet
- MalariaDocument49 pagesMalariaSylvia PertiwiNo ratings yet
- Path o PhysiologyDocument2 pagesPath o PhysiologySylvia PertiwiNo ratings yet
- Daftar Pustaka: Medical Students and Faculty - Edisi Keempat - Baltimore-PhiladelpiaDocument2 pagesDaftar Pustaka: Medical Students and Faculty - Edisi Keempat - Baltimore-PhiladelpiaSylvia PertiwiNo ratings yet
- Limfoma PPT MonceDocument65 pagesLimfoma PPT MonceSylvia PertiwiNo ratings yet
- Developmental Status of 1-Year-Old Infants Fed Breast MilkDocument8 pagesDevelopmental Status of 1-Year-Old Infants Fed Breast MilkSylvia PertiwiNo ratings yet
- Acute Intestinal Disease Caused by SalmonellaDocument20 pagesAcute Intestinal Disease Caused by SalmonellaSylvia PertiwiNo ratings yet
- Buku CHFDocument59 pagesBuku CHFSylvia PertiwiNo ratings yet
- Dr. Harun Hudari, SpPD: Opportunistic Fungal Infection GuideDocument43 pagesDr. Harun Hudari, SpPD: Opportunistic Fungal Infection GuideSylvia PertiwiNo ratings yet
- Path o PhysiologyDocument2 pagesPath o PhysiologySylvia PertiwiNo ratings yet
- BacteriologyDocument63 pagesBacteriologySylvia PertiwiNo ratings yet
- Blok 10 Lipoprotein & DyslipidemiaDocument60 pagesBlok 10 Lipoprotein & DyslipidemiaSylvia PertiwiNo ratings yet
- Nej Me 0902632Document4 pagesNej Me 0902632Sylvia PertiwiNo ratings yet
- GD1. IntroDocument29 pagesGD1. IntroSylvia PertiwiNo ratings yet
- Life CycleDocument10 pagesLife CycleSylvia PertiwiNo ratings yet
- Ancient pyramid lies in Mexican jungleDocument2 pagesAncient pyramid lies in Mexican jungleEgun NofiantoNo ratings yet
- Congenital Heart DefectsDocument23 pagesCongenital Heart DefectsSylvia PertiwiNo ratings yet
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeFrom EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeRating: 4 out of 5 stars4/5 (5784)
- The Yellow House: A Memoir (2019 National Book Award Winner)From EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Rating: 4 out of 5 stars4/5 (98)
- Never Split the Difference: Negotiating As If Your Life Depended On ItFrom EverandNever Split the Difference: Negotiating As If Your Life Depended On ItRating: 4.5 out of 5 stars4.5/5 (838)
- Shoe Dog: A Memoir by the Creator of NikeFrom EverandShoe Dog: A Memoir by the Creator of NikeRating: 4.5 out of 5 stars4.5/5 (537)
- The Emperor of All Maladies: A Biography of CancerFrom EverandThe Emperor of All Maladies: A Biography of CancerRating: 4.5 out of 5 stars4.5/5 (271)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceFrom EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceRating: 4 out of 5 stars4/5 (890)
- The Little Book of Hygge: Danish Secrets to Happy LivingFrom EverandThe Little Book of Hygge: Danish Secrets to Happy LivingRating: 3.5 out of 5 stars3.5/5 (399)
- Team of Rivals: The Political Genius of Abraham LincolnFrom EverandTeam of Rivals: The Political Genius of Abraham LincolnRating: 4.5 out of 5 stars4.5/5 (234)
- Grit: The Power of Passion and PerseveranceFrom EverandGrit: The Power of Passion and PerseveranceRating: 4 out of 5 stars4/5 (587)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaFrom EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaRating: 4.5 out of 5 stars4.5/5 (265)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryFrom EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryRating: 3.5 out of 5 stars3.5/5 (231)
- On Fire: The (Burning) Case for a Green New DealFrom EverandOn Fire: The (Burning) Case for a Green New DealRating: 4 out of 5 stars4/5 (72)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureFrom EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureRating: 4.5 out of 5 stars4.5/5 (474)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersFrom EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersRating: 4.5 out of 5 stars4.5/5 (344)
- The Unwinding: An Inner History of the New AmericaFrom EverandThe Unwinding: An Inner History of the New AmericaRating: 4 out of 5 stars4/5 (45)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyFrom EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyRating: 3.5 out of 5 stars3.5/5 (2219)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreFrom EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreRating: 4 out of 5 stars4/5 (1090)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)From EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Rating: 4.5 out of 5 stars4.5/5 (119)
- Her Body and Other Parties: StoriesFrom EverandHer Body and Other Parties: StoriesRating: 4 out of 5 stars4/5 (821)
- Ultrasound ImagingDocument11 pagesUltrasound ImagingFikret Baz100% (1)
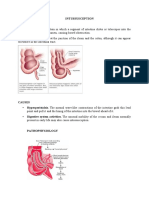
- INTUSSUSCEPTIONDocument3 pagesINTUSSUSCEPTIONS GNo ratings yet
- Basic Principles of Psychiatric NursingDocument5 pagesBasic Principles of Psychiatric NursingJo C Cuilan100% (1)
- BSSP Course DescriptionsDocument3 pagesBSSP Course DescriptionsJilliane LagusNo ratings yet
- TramadolDocument2 pagesTramadolJordanne EtisNo ratings yet
- CrohnsDocument19 pagesCrohnsLauren LevyNo ratings yet
- Ramos vs. CADocument20 pagesRamos vs. CAWilfredNo ratings yet
- The Benefits of ExerciseDocument3 pagesThe Benefits of ExerciseAtet KurniadiNo ratings yet
- How To Prevent Flatulence (Aerophagy)Document7 pagesHow To Prevent Flatulence (Aerophagy)krishnaNo ratings yet
- Nursing Test Bank QuestionDocument97 pagesNursing Test Bank QuestionADEDIRAN ABIONANo ratings yet
- Administration of An Oxytocin Receptor Antagonist Attenuates SexualDocument7 pagesAdministration of An Oxytocin Receptor Antagonist Attenuates SexualAtlamaltaNo ratings yet
- PNI Psychosocial Factors that Impact Immune SystemDocument23 pagesPNI Psychosocial Factors that Impact Immune SystemAnn Michelle TarrobagoNo ratings yet
- Chocolate Milk Argument Essay SamplesDocument3 pagesChocolate Milk Argument Essay Samplesapi-349881433100% (4)
- EVOLUTION OF CARD REPERTORYDocument7 pagesEVOLUTION OF CARD REPERTORYRahul RamanNo ratings yet
- 290 297Document12 pages290 297YASMINDPNo ratings yet
- Peptic UlcerDocument4 pagesPeptic UlcerEris Abdul AzizNo ratings yet
- The Soulmate DietDocument24 pagesThe Soulmate DietShana MarieNo ratings yet
- Biomedical Waste ManagementDocument14 pagesBiomedical Waste ManagementdivyeshkpatelNo ratings yet
- Neonatal Resuscitation AlgorithmDocument1 pageNeonatal Resuscitation Algorithmpalembang2015No ratings yet
- William Boericke. Homoeopat PDFDocument475 pagesWilliam Boericke. Homoeopat PDFAbhishek Kumar Upadhyay100% (1)
- DR Miller Cost of Rhinoplasty InfographicDocument1 pageDR Miller Cost of Rhinoplasty Infographick8xcqsrxmqNo ratings yet
- Practical Radiotherapy Planning, Fourth EditionDocument477 pagesPractical Radiotherapy Planning, Fourth EditionMehtap Coskun100% (12)
- HYper and Hypo TGDocument43 pagesHYper and Hypo TGRiajoy AsisNo ratings yet
- Health & Nutrition Classification of FoodDocument10 pagesHealth & Nutrition Classification of Foodg20kpNo ratings yet
- Ocular Trauma: State of Illinois Trauma Nurse Specialist ProgramDocument38 pagesOcular Trauma: State of Illinois Trauma Nurse Specialist ProgramMayuha SaidNo ratings yet
- Development Economics II Summary: Health, Calories, and ProductivityDocument9 pagesDevelopment Economics II Summary: Health, Calories, and Productivityshabrina larasatiNo ratings yet
- Catalogo FS 07-09-2023Document10 pagesCatalogo FS 07-09-2023narciso javier Avila BejaranoNo ratings yet
- HAAD Exam For Nurses Questions 2018Document46 pagesHAAD Exam For Nurses Questions 2018Asif Newaz100% (6)
- DSM OcdDocument2 pagesDSM Ocdnmyza89No ratings yet
- STEM Immersion Reflections in Physical Therapy, Nursing, and Medical TechnologyDocument4 pagesSTEM Immersion Reflections in Physical Therapy, Nursing, and Medical TechnologyLeonard Cyren LigutomNo ratings yet