Professional Documents
Culture Documents
Trans Pulmopatho Colored
Uploaded by
2012Original Description:
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Trans Pulmopatho Colored
Uploaded by
2012Copyright:
Available Formats
OS 213 Dr.
Nelia Tan-Liu
Pulmonary Pathology Lab Module 1 Exam 1
Lecture Outline: Common Bacterial Agents in Pnuemonia
I. Bacterial Pneumonia • Strep pneumoniae
II. Viral Pneumonia • Hemo influenzae
III. Fungal Pneumonia
IV. Tuberculosis
• Staph aureus
V. Bronchiectasis • Klebs pneumoniae
VI. Chronic Bronchitis • Escherichia coli
VII. Adult Respiratory Distress Syndrome • Pseudomonas spp.
4 Stages of Inflammation in Bacterial Pneumonia
Bacterial Pneumonia 1. CONGESTION
• lung is heavy, boggy, and red
Case Discussion: • It is characterized by vascular
A case of a 32 year old male who presented with engorgement, intra-alveolar fluid
productive cough, fever and malaise for 8 days. with few neutrophils, and often the
Patient began to experience dyspnea 1 day prior to presence of numerous bacteria
consult. Chest x-ray showed a diffuse infiltrate
between the right middle and right lower lobes. 2. STAGE OF RED HEPATIZATION
• characterized by massive confluent
Questions: exudation with red cells (congestion)
Differentiate lobar pneumonia from and neutrophils and fibrin filling the
bronchopneumonia based on the gross alveolar spaces
features. • On gross examination, the lobe now
Enumerate common bacterial agents appears distinctly red, firm, and
isolated in pneumonia. airless with a liver-like consistency,
Enumerate the Stages of Inflammation in hence the term hepatization.
Bacterial Pneumonia
Enumerate four possible complications of
pneumonia.
Differentiate transudate from exudate
Name other etiologic agents that can give
rise to pulmonary abscesses
Lobar Pneumonia vs Bronchopneumonia
• Lobar pneumonia
o A widespread fibrinosuppurative
consolidation of large areas and
even whole lobes of the lung.
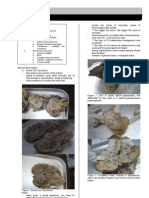
Figure 3. Photomicrograph showing intra-alveolar infiltration by
Figure 1. acute inflammatory cells (neutrophils)
Gross picture of lung
showing consolidation of .
a large portion of a lobe 3. STAGE OF GREY HEPATIZATION
or an entire lobe
• Progressive disintegration of red
cells and the persistence of
fibrinosuppurative exudate giving
the gross appearance of a grayish
brown, dry surface
• Bronchopneumonia
o Consolidated areas of acute
suppurative inflammation.
o Consolidation may be patchy
through one lobe but is more
often multilobar and frequently
bilateral and basal because of the
tendency of secretions
Figure 2.
Gross picture of lung
Figure 4. Slide showing grey hepatization
showing patchy
consolidation of the lung
4. STAGE OF RESOLUTION
• Final stage
• The consolidated exudate within the
alveolar spaces undergoes
January 22, 2009 | Thursday Page 1 of 8
Cielo & Co
OS 213 Dr. Nelia Tan-Liu
Pulmonary Pathology Lab Module 1 Exam 1
progressive enzymatic digestion to oimplies significant alteration in the
produce granular, semifluid debris normal permeability of small blood
that is resorbed, ingested by vessels in the area of injury
macrophages, or coughed up. Etiologic Agents Causing Pulmonary Abscesses
• Pleural fibrinous reaction to the • Staph aureus
underlying inflammation often • Gram negative organisms
present in the early stages if the • Anaerobic organisms:
consolidation extends to the surface o Bacteroides
(pleuritis), may similarly resolve. o Fusobacterium
• More often, it undergoes o Peptococcus
organization, leaving fibrous
thickening or permanent adhesions.
Viral Pneumonia
Questions:
Name the common viral agents causing
interstitial pneumonia.
Differentiate viral from bacterial pneumonia
based on predominant histologic pattern.
Describe cytopathic effects in pneumonia
caused by:
o Respiratory Syncytial Virus
o Cytomegalovirus
o Measles
Enumerate three bacterial agents that can
Figure 5. Slide showing fibrotic areas with chronic inflammation present as interstitial pneumonia.
Common Viral Agents Causing Interstitial
Four Possible Complications of Pneumonia Pneumonia:
• Microabscesses/ abscess • Resiratory Syncytial virus
• Empyema • Adenovirus
• Pleural effusion • Rhinovirus
• Bacteremia/ Sepsis • Rubeola
• Varicella
Viral vs Bacterial Pneumonia (Histology)
• The predominant histological pattern in viral
pneumonia is the interstitial nature of the
inflammatory reaction– inflammation is
virtually localized within the walls of the
alveoli.
Figure 6. Gross and microscopic pictures of abscess formation (1st two
pictures), and empyema
Transudate vs Exudate
• Transudate
o fluid with low protein count; sp gr of
< 1.012
o an ultrafiltrate of blood plasma that
results from osmotic or hydrostatic
imbalance across the vessel wall
without an increase in vascular
permeability
• Exudate
o inflammatory extravascular fluid that
has a high protein concentration,
cellular debris, and an sp gr of >
1.020 Figure 7. Interstitial Pneumonitis
January 22, 2009 | Thursday Page 2 of 8
Cielo & Co
OS 213 Dr. Nelia Tan-Liu
Pulmonary Pathology Lab Module 1 Exam 1
• The alveolar septa are widened and In Fungal Pneumonia, pulmonary damage results
edematous and usually have a from:
mononuclear inflammatory infiltrate of vascular occlusion by the fungus, resulting
lymphocytes, histiocytes, and occasionally in ischemic necrosis, or
plasma cells. direct invasion by and host reaction to the
• In acute cases, neutrophils may also be organism
present.
• The alveoli may be free from exudate, but
in many patients there are intra-alveolar
proteinaceous material, a cellular exudate,
and characteristically pink hyaline
membranes lining the alveolar walls, similar
to those seen in hyaline membrane disease
of infants.
Book Notes: (Robbins Patho)
VIRAL AND MYCOPLASMAL PNEUMONIA (PRIMARY
ATYPICAL PNEUMONIA):
• The term primary atypical pneumonia was initially
applied to an acute febrile respiratory disease
characterized by patchy inflammatory changes in
the lungs, largely confined to the alveolar septa
Figure 8. A lung showing diffuse consolidation and vascular
and pulmonary interstitium.
thrombosis with infarction
• The term atypical denotes the lack of alveolar
exudate, but a much more accurate designation
is interstitial pneumonitis.
• The pneumonitis is caused by a variety of
organisms, the most common being Mycoplasma
pneumoniae. Other etiologic agents are viruses,
including influenza virus types A and B, the
respiratory syncytial viruses, adenovirus,
rhinoviruses, rubeola, and varicella viruses;
Chlamydia (psittacosis); and Coxiella burnetti (Q
fever). [33] In some cases, the cause cannot be
determined.
• Any one of these agents may cause merely an
upper respiratory tract infection, recognized as
the common cold, or a more severe lower
respiratory tract infection.
• The circumstances that favor such extension of
the infection are often mysterious but include
malnutrition, alcoholism, and underlying
debilitating illnesses.
Figure 9. Close-up view, post-fixation
Cytopathic Effects in Pneumonia
• RSV: formation of syncytial cells
• CMV: abnormal inclusions or structural
changes
• Measles: multinucleate giant cells with
eosinophilic nuclear and cytoplasmic
inclusion bodies (Warthin-Finkeldey cells)
• NB: All of these produce essentially similar
morphologic patterns (interstitial
inflammatory reaction)
Bacterial Agents That Can Present as Interstitial
Pneumonia
• Mycoplasma pneumoniae
• Chlamydia trachomatis
• Coxiella burnetti
Cielo: GREETINGS!!! Wohoooooo!!! Heheheh
Fungal Pneumonia Let’s vote in the SR Referendum
Figure 10. Fungal elements occluding a large pulmonary vessel
this Jan 26-31!!!
Note: Mu sisses, hello!!! Namiss ko kayo ngayong weekend!
Clingy! Hahahah!!! Yung mga mag-e-Entertainment
Committee, hanap na kayo sa O-bar please… We’re on a
January 22, 2009 | Thursday very tight schedule. Bwahaha!! Me-an hello!!! Engkly
Page 3 of 8
pagaling ka! Bismark, tnx sa inputs. Bispren! Burger! Burger!!
Cielo & Co
HAPPY BIRTHDAY FIFIFOFUHM!!!!
LABSHYUUU Mu 2012!! Good Luck 2013 Apps!!!
OS 213 Dr. Nelia Tan-Liu
Pulmonary Pathology Lab Module 1 Exam 1
Differentiate Langhans’ type from other
types of giant cells.
Definitive Diagnostic Modality for TB
Culture and isolation
Recent diagnostics involve PCR for
mycobacterial nucleic acids in sputum and
gastric lavages
Gross Facets of TB
Cavitations with casseous material
Fibrosis/Fibrocalcific scars
Hilar lymphadenopathies
Hemorrhage
Consolidation
Bronchial erosions
Pleural effusion
Fibrous pleuritis
Figure 11. Section taken from an invasive pulmonary aspergillosis.
(methenamine silver stain)
Questions:
Enumerate 3 conditions leading to an
immunocompromised state.
Enumerate other fungal agents that may
cause pneumonia.
Conditions Leading to an Immunocompromised
State:
• HIV-AIDS Figure 12. Pulmonary TB (Ghon complex)
• Chronic steroid use
• Malignancies
Fungal Agents that may Cause Pneumonia
• Histoplasma capsulatum Huge tuberculous
• Blastomyces dermatidis cavity
• Coccidioides immitis
Tuberculosis
Case Discussion:
This is the case of a 56 year old Filipino male who
had 2 months history of recurrent febrile episodes in
the afternoon, productive cough and weight loss.
One week prior to consult, patient began to have
blood-tinged sputum and dyspneic episodes. Early tuberculous cavity formed by caseous (cheese-like) necrosis
Initial chest x-ray showed hilar lymphadenopathies,
Figure 13. Pulmonary TB with Cavitations
bilateral apical cavitations, and minimal pleural
effusion on the right.
Important Histologic Feature of TB Granuloma
Questions: • A focus of chronic inflammation consisting of
Give the definitive diagnostic modality for microscopic aggregate of macrophages that
tuberculosis. are transformed into epithelium-like cells
Discuss the different gross facets of surrounded by a collar of mononuclear
tuberculosis. WBCs
Enumerate the important histologic features Figure 14. TB
of a TB granuloma Granuloma
January 22, 2009 | Thursday Page 4 of 8
Cielo & Co
OS 213 Dr. Nelia Tan-Liu
Pulmonary Pathology Lab Module 1 Exam 1
The right portion of this bronchiole shows epithelial erosion. There is
exudate in the lumen.
Acute inflammatory cells, especially PMNs, are present, although
evidence of chronic inflammation is also likely to be present.
Questions:
Langhans’ Type vs Other Types of Giant Cells What is your diagnosis?
• Langhans: nuclei are arranged in U-shaped What are the underlying conditions
pattern associated with this condition? What
• Other giant cells: irregular distribution of processes are necessary for its
nuclei development?
What type of inflammatory cells is present?
Figure 15. Compare with asthma.
Langhans’ Giant
Cells
Diagnosis: Bronchiectasis
Underlying Conditions Associated with
Bronchiectasis:
• Bronchiectasis is caused by conditions that
predispose to chronic necrotizing infections
and consequent destruction of muscle and
elastic support tissue of bronchi and
bronchioles.
• The most common conditions are:
a. Bronchial obstruction (tumors; foreign
bodies), diffuse obstructive airway
diseases (atopic asthma; chronic
bronchitis)
Bronchiectasis b. Congenital or hereditary conditions
(congenital bronchiectasis; cystic
Case Discussion: fibrosis)
A case of a 20 year old patient who presented with c. Necrotizing or suppurative pneumonias
recurrent fever and productive cough. Sputum
gradually became copious, foul and purulent. Initial Processes Necessary for the Development of
PE includes bronchial breath sounds on the Bronchiectasis:
peripheral lung fields; and bibasal crackles. • Persistent obstruction
• Superimposed infection
Definition
• Bronchiectasis is the permanent dilation of Type of Inflammatory Cells Present
bronchi and bronchioles and is secondary to • Acute inflammatory cells, especially PMNs,
cycles of obstruction and infection.
are present, although evidence of chronic
inflammation is also likely to be present.
Figure 16. Cut section of the left lung.
Note the inflamed left main stem
bronchus. It gives rise to branches in the Compare with Asthma
v
left lower lobe that have been opened to • By comparison, in asthma, the inflammatory
demonstrate that they extend nearly to cells are composed of CD4+ lymphocytes,
the pleural surface in this specimen. eosinophils, mast cells, and a few
The diameters of the two opened neutrophils.
bronchial branches in the lower lobe are
each greater than the diameter of the
bronchus from which they originate,
indicating the severity of bronchial Chronic Bronchitis
dilation.
Case Discussion:
A case of a 62 year old chain-smoker who presented
with persistent cough with daily sputum production
for almost 10 months each year since 1999.
Figure 17. Section Occasionally, patient spat blood-tinged sputum, but
from a bronchiole. no consult was done until patient had dyspnea,
There is marked fever, and palpitations. Initial PE revealed cyanosis,
inflammation of the dynamic precordium and diffuse crackles on both
bronchi and lungs.
bronchiolar walls. The
inflammatory cells
are seen as dark blue Definition
nuclei under the
mucosal lining.
January 22, 2009 | Thursday Page 5 of 8
Cielo & Co
OS 213 Dr. Nelia Tan-Liu
Pulmonary Pathology Lab Module 1 Exam 1
• Chronic bronchitis, per se is defined
clinically. It is present in any patient who has
persistent cough with sputum production for
at least 3 months in at least 2 consecutive
years.
• In simple chronic bronchitis, patients have a
productive cough but no physiologic
evidence of airflow obstruction.
Questions:
• Some individuals may demonstrate • What is your diagnosis? Bases?
hyperreactive airways with intermittent
bronchospasm and wheezing. This condition
• How does the mucous gland hyperplasia in
is called chronic asthmatic bronchitis. this case differ from that in a typical case of
asthma?
• Finally, some patients, especially heavy
• What is the Reid Index?
smokers, develop chronic airflow
obstruction, usually with evidence of
Diagnosis and Basis for It
associated emphysema, and are classified
as showing obstructive chronic bronchitis. • Chronic bronchitis is a clinical definition: a
persistent cough with sputum production for
at least three months in two consecutive
years.
• Characteristic features supporting this
diagnosis are hypersecretion of mucous in
the large airways, chronic inflammation of
the airways (predominantly lymphocytes)
and hypertrophy of the submucosal glands
in the trachea and bronchi.
Mucous Gland Hyperplasia in Chronic Bronchitis
(as compared to that in Asthma)
• In typical allergic asthma, which also has
mucous gland hyperplasia, the bronchial
wall has an inflammatory infiltrate in which
eosinophils are prominent.
• There is also hypertrophy and hyperplasia of
smooth muscle cells in asthma.
Reid Index
• The ratio of the thickness of the mucous
Figure 18. Trachea and Main Bronchi. The trachea in the mid-upper gland layer to the thickness of the wall
field is hyperemic, and the bifurcation and main stem bronchi contain between the epithelium and the cartilage.
mucopurulent exudate. The underlying epithelium is also inflamed. • The normal ratio is 0.4.
This picture may occur in chronic bronchitis and a superimposed
• It is increased in chronic bronchitis.
infection. However, one may also see this picture as part of an acute
inflammatory process in a patient dying of acute pneumonia.
Remember that chronic bronchitis is a clinical term.
Adult Respiratory Distress Syndrome
Case Discussion:
A case of a 52 year old diabetic, with a history of
cerebral infarct and with left-sided residuals, who
was diagnosed to have community acquired
pneumonia on admission. Patient was admitted for 6
days and was apparently improved on discharge. At
home, patient developed high grade fever, body
malaise and recurrence of productive cough.
Home medications were continued and consult was
done only 5 days later. Patient already presented
Figure 19. Bronchial Wall. These are changes typical of chronic with difficulty of breathing and was subsequently re-
bronchitis. The bronchial epithelium is partially denuded in some admitted. At the wards, patient was hypotensive,
regions but squamous metaplasia is present in others. The basement tachypneic and febrile. Intubation was done due to
membrane is thickened (white arrow) and the mucosal vessels are sudden respiratory distress and cyanosis. Chest x-
engorged and dilated (thin black arrows). A moderate number of ray showed diffuse bilateral alveolar infiltration.
plasmacytes and lymphocytes (thick black arrow) are present in the Despite resuscitative efforts, patient demised on the
submucosa and the gland layer which is markedly enlarged and 2nd hospital day.
composes almost half of the wall thickness of the bronchus. Majority of
the galnds January
are mucous 22, 2009 | The
in character. Thursday
glands and ducts are dilated Page 6 of 8
and filled with mucinous secretion containing desquamated cells and Cielo & Co
inflammatory cells.
OS 213 Dr. Nelia Tan-Liu
Pulmonary Pathology Lab Module 1 Exam 1
Book Notes: (Robbins Patho) Questions
ADULT RESPIRATORY DISTRESS SYNDROME What is your histologic diagnosis?
(DIFFUSE ALVEOLAR DAMAGE)
Can the exact etiology be determined by the
• ARDS and its many synonyms ( including adult
microscopic findings alone?
respiratory failure, shock lung, diffuse alveolar
damage, acute alveolar injury, and traumatic wet What is/are the likely cause(s) in this case?
lungs) are descriptive terms for a syndrome What other conditions can cause these
caused by diffuse alveolar capillary damage. findings?
• It is characterized clinically by the rapid onset of Enumerate the composition of the hyaline
severe life-threatening respiratory insufficiency, membrane seen in the histologic sections.
cyanosis, and severe arterial hypoxemia that is What pathologic finding is central to the
refractory to oxygen therapy and that may development of ARDS?
progress to extrapulmonary multisystem organ
failure.
Histologic Diagnosis
• ARDS is a well-recognized complication of • Diffuse alveolar damage, representing the
numerous and diverse conditions, including both
direct injuries to the lungs and systemic usual underlying pathologic change of the
disorders. Direct lung injuries causing ARDS clinically defined Adult Respiratory Distress
include diffuse pulmonary and other viral Syndrome.
infections, oxygen toxicity, inhalation of toxins
and other irritants, and aspiration of gastric Can the exact etiology be determined by the
contents. Systemic conditions causing ARDS microscopic findings alone?
include septic shock, shock associated with • No. The morphologic changes are non-
trauma, hemorrhagic pancreatitis, burns,
specific.
complicated abdominal surgery, narcotic
overdose and other drug reactions, • Diffuse Alveolar Damage is best viewed as
hypersensitivity reactions to organic solvents, the pathologic end-result of acute alveolar
hemodialysis, and cardiac surgery involving injury caused by a variety of insults and
extracorporeal pumps. In many cases, a initiated by different mechanisms.
combination of the foregoing conditions is
present (e.g., shock, oxygen therapy, and
Likely cause in this case
sepsis).
• Sepsis, diffuse pulmonary infections, gastric
aspiration, and mechanical trauma are
responsible for more than 50% of cases of
ARDS.
Other Conditions that can Cause These Findings
• Injuries:
o pulmonary contusion
\ o near drowning
o fat embolism
o burns
o ionizing radiation
• Inhaled irritants
o oxygen toxicity
o smoke
o irritant gasses and chemicals
Figure 20. Lung Section, scanning view. Sections of the lungs show • Chemical injury
diffused infiltration by inflammatory cells with loss of alveolar o heroin or methadone overdose
architecture. There are areas revealing collection of pink amorphous o aspirin
material and hyalinized deposits. Most areas have necrotic debris with o barbiturate overdose
admixed neutrophils. o paraquat
• Hematologic conditions
o multiple transfusions
o DIC
• Pancreatitis
• Uremia
• Cardiopulmonary bypass
• Hypersensitivity reactions
o organic solvents
o drugs
Composition of the Hyaline Membrane
• The waxy hyaline membranes lining the
Figure 21. Lung Section, HPO alveolar walls consist of fibrin-rich edema
fluid mixed with the cytoplasmic and lipid
remnants of necrotic epithelial cells.
January 22, 2009 | Thursday Page 7 of 8
Cielo & Co
OS 213 Dr. Nelia Tan-Liu
Pulmonary Pathology Lab Module 1 Exam 1
Pathologic Finding Central to Development of
ARDS
• Diffuse damage to the alveolar capillary
walls. Neutrophils are thought to play an
important role in the pathogenesis of acute
lung injury and ARDS. In contrast, the
respiratory distress in newborns is initiated
by deficiency in pulmonary surfactant.
January 22, 2009 | Thursday Page 8 of 8
Cielo & Co
You might also like
- Physical Security Audit Checklist PDFDocument3 pagesPhysical Security Audit Checklist PDFHendrawan StbNo ratings yet
- Community Acquired Pneumonia: Ang Gobonseng, Ed Gerard R. MedclerkDocument66 pagesCommunity Acquired Pneumonia: Ang Gobonseng, Ed Gerard R. MedclerkRyn Anfone100% (2)
- 6th Central Pay Commission Salary CalculatorDocument15 pages6th Central Pay Commission Salary Calculatorrakhonde100% (436)
- 6th Central Pay Commission Salary CalculatorDocument15 pages6th Central Pay Commission Salary Calculatorrakhonde100% (436)
- Dialectical Behavior Therapy With Adolescents - Settings, Treatments, and DiagnosesDocument254 pagesDialectical Behavior Therapy With Adolescents - Settings, Treatments, and DiagnosesAlguém100% (2)
- Abnormal Chest FindingsDocument5 pagesAbnormal Chest FindingsAbishek Prince100% (1)
- PATHOLOGIC CHANGES. Grossly, The Lungs Are Characteristically Stiff, Congested and Heavy. Microscopically, The Following Features Are EvidentDocument6 pagesPATHOLOGIC CHANGES. Grossly, The Lungs Are Characteristically Stiff, Congested and Heavy. Microscopically, The Following Features Are EvidentIsak ShatikaNo ratings yet
- PneumoniaDocument21 pagesPneumoniaZunaira RaheenNo ratings yet
- Etiology: 1. Compare Lobar Pneumonia With Lobular Pneumonia On The ListDocument3 pagesEtiology: 1. Compare Lobar Pneumonia With Lobular Pneumonia On The Listselam kalayuNo ratings yet
- Pathology Paru Azham HandoutDocument11 pagesPathology Paru Azham HandoutKiky Martha A.No ratings yet
- Pulmonary Diseases ExplainedDocument23 pagesPulmonary Diseases ExplainedVratin ModiNo ratings yet
- Image Session of Respiratory System IDocument31 pagesImage Session of Respiratory System IZain Ul AbidinNo ratings yet
- Chronic Obstructive Pulmonary DiseaseDocument6 pagesChronic Obstructive Pulmonary Diseaseshamae justinianoNo ratings yet
- LO Week 5 Tutorial 2Document7 pagesLO Week 5 Tutorial 2Hizkia MarlissaNo ratings yet
- Pneumonia Types and PathologyDocument35 pagesPneumonia Types and Pathologysuheel raiNo ratings yet
- DurdonaDocument12 pagesDurdonaAbdumalik KarshievNo ratings yet
- The Lung Pathology Lab Encoded PDFDocument85 pagesThe Lung Pathology Lab Encoded PDFJustinNo ratings yet
- Pulmonary InfectionDocument9 pagesPulmonary InfectionlalaNo ratings yet
- Lung Abscess Symptoms, Causes and TreatmentDocument40 pagesLung Abscess Symptoms, Causes and Treatmentghhh100% (1)
- 长沙医学院 国际教育学院 Pathology (病理学)Document57 pages长沙医学院 国际教育学院 Pathology (病理学)Ichsan FajriNo ratings yet
- AutopsyDocument29 pagesAutopsyAkshita Amit AgarwalNo ratings yet
- (Materi Dr. Heny) PneumoniaDocument86 pages(Materi Dr. Heny) PneumoniaFathiyah SalsabilaNo ratings yet
- Bronchial Pneumonia: Lecturer: Sir Raynell Gordon Presenter: Miracle CambridgeDocument18 pagesBronchial Pneumonia: Lecturer: Sir Raynell Gordon Presenter: Miracle CambridgemiracleNo ratings yet
- Non Tuberculous Infections (Updated)Document54 pagesNon Tuberculous Infections (Updated)ZijieNo ratings yet
- Pneumonia I Pathophysiology and Clin PresentationDocument10 pagesPneumonia I Pathophysiology and Clin PresentationsunilsohanlalgurjarNo ratings yet
- Div Clsis An Update Onvestigation DivDocument4 pagesDiv Clsis An Update Onvestigation DivAshwinNo ratings yet
- Section 3-7 Slides + CommentsDocument9 pagesSection 3-7 Slides + CommentsNkgivgNo ratings yet
- ReviewerDocument7 pagesReviewerAyessa CortesNo ratings yet
- THE So-Called Middle Lobe Syndrome: LeegaardDocument3 pagesTHE So-Called Middle Lobe Syndrome: LeegaardHari PrasadNo ratings yet
- 2013 July Chest Section PDFDocument171 pages2013 July Chest Section PDFsebsbie admasNo ratings yet
- Lobar Pneumonia: Deevon M. Cariaga FEU-NRMF Institute of MedicineDocument12 pagesLobar Pneumonia: Deevon M. Cariaga FEU-NRMF Institute of MedicinedeevoncNo ratings yet
- The Radiology AssistantDocument30 pagesThe Radiology AssistantIcha IchaNo ratings yet
- International Journal of Health Sciences and Research: Tuberculous Epiglottitis - A Rare Case ReportDocument5 pagesInternational Journal of Health Sciences and Research: Tuberculous Epiglottitis - A Rare Case ReportAmikIndrayani1994No ratings yet
- PneumoniaDocument120 pagesPneumoniaSaklenali LoniNo ratings yet
- COPD: Chronic Obstructive Pulmonary Disease ExplainedDocument15 pagesCOPD: Chronic Obstructive Pulmonary Disease ExplainedMary Grace AgataNo ratings yet
- Practical 4 PathologyDocument13 pagesPractical 4 PathologyVINCENTNo ratings yet
- Pulmonary Disease Management GuideDocument5 pagesPulmonary Disease Management GuideCharisa Antonette HuelvaNo ratings yet
- PatomekanismeDocument18 pagesPatomekanismeEdwin Pasha Jr.No ratings yet
- Lung AbscessDocument20 pagesLung AbscessSAMOEINo ratings yet
- Schematic Diagram OF BronchopneumoniaDocument11 pagesSchematic Diagram OF BronchopneumoniaanGel1115No ratings yet
- Interstitial Lung DiseaseDocument15 pagesInterstitial Lung DiseaseLea MonzerNo ratings yet
- Lab 2.medDocument121 pagesLab 2.medFYMNo ratings yet
- Disorders of LungsDocument54 pagesDisorders of LungsAsna FasilNo ratings yet
- Laracas Lezel M. BSN3B - Medical SurgicalDocument14 pagesLaracas Lezel M. BSN3B - Medical SurgicalLezel LaracasNo ratings yet
- Pneumonia in Sheep and GoatDocument32 pagesPneumonia in Sheep and Goataliabh2006100% (5)
- Patho PTBDocument3 pagesPatho PTBRenalyn Domingo JoseNo ratings yet
- Bubonic PlagueDocument9 pagesBubonic PlagueХристинаГулеваNo ratings yet
- Ast 2Document17 pagesAst 2AbuAbdullah KhanNo ratings yet
- Asthm 2Document34 pagesAsthm 2AbuAbdullah KhanNo ratings yet
- BronchiectasisDocument24 pagesBronchiectasisMuhammad HaziqNo ratings yet
- Frimpong PPDocument16 pagesFrimpong PPJack frimpongNo ratings yet
- Lung Abscess Handout PDFDocument3 pagesLung Abscess Handout PDFTansanee MalivalayaNo ratings yet
- Pulmonary Tuberculosis: PGI Leichel Ann N. AlbertoDocument82 pagesPulmonary Tuberculosis: PGI Leichel Ann N. AlbertoLeichel AlbertoNo ratings yet
- Pathology of pneumonia and lung disordersDocument61 pagesPathology of pneumonia and lung disordersIngeNo ratings yet
- 621 FullDocument18 pages621 FullG LekNo ratings yet
- Pneumonia Diagnosis and TreatmentDocument6 pagesPneumonia Diagnosis and TreatmentIsabel CastilloNo ratings yet
- Bronchial Gland Signs of Chronic BronchitisDocument4 pagesBronchial Gland Signs of Chronic BronchitisZiyan NafisahNo ratings yet
- Respiratory Disorders Part 4 Complete HoDocument3 pagesRespiratory Disorders Part 4 Complete HoLie CellNo ratings yet
- Disorders of Respiratory Function - Infections and Neoplasms - 2020Document17 pagesDisorders of Respiratory Function - Infections and Neoplasms - 2020Cres Padua QuinzonNo ratings yet
- PneumoniaDocument33 pagesPneumoniarabeccabeckybonbonNo ratings yet
- Renal Pathology GuideDocument71 pagesRenal Pathology GuideSuha AbdullahNo ratings yet
- 5 MED II 1 - PneumoniaDocument11 pages5 MED II 1 - PneumoniaDeann RoscomNo ratings yet
- Respiratory Disease, Any of The Diseases and Disorders That Affect HumanDocument26 pagesRespiratory Disease, Any of The Diseases and Disorders That Affect HumanAryan RajNo ratings yet
- PCAP UpdatesDocument60 pagesPCAP Updates2012No ratings yet
- SCOPING DOCUMENT For WHO Treatment Guidelines On Pain Related ToDocument10 pagesSCOPING DOCUMENT For WHO Treatment Guidelines On Pain Related To2012No ratings yet
- Boards SyllabusDocument14 pagesBoards Syllabus2012No ratings yet
- Boards SyllabusDocument14 pagesBoards Syllabus2012No ratings yet
- Cancer Pain Relief Who 1998Document86 pagesCancer Pain Relief Who 19982012100% (1)
- The Division of Plastic SurgeryDocument36 pagesThe Division of Plastic Surgery2012No ratings yet
- Fa Step 1 ScheduleDocument5 pagesFa Step 1 ScheduleDinesh DalviNo ratings yet
- General Recommendation ImmunizationDocument69 pagesGeneral Recommendation Immunization2012No ratings yet
- ADA Summary of Guidelines 2011Document7 pagesADA Summary of Guidelines 2011IffatNaeemNo ratings yet
- CEBM Levels of EvidenceDocument2 pagesCEBM Levels of Evidence2012100% (2)
- Review Lectures Forlu6: Basic Eye Exam Common Opd Complaints Common Er Cases PharmacologyDocument110 pagesReview Lectures Forlu6: Basic Eye Exam Common Opd Complaints Common Er Cases Pharmacologyupmed2012block9No ratings yet
- American Diabetes Association (ADA) gUIDELINESDocument43 pagesAmerican Diabetes Association (ADA) gUIDELINESSamuel Rudolf Maranatha JulioNo ratings yet
- USMLEboardswhatworked 2008Document32 pagesUSMLEboardswhatworked 20082012No ratings yet
- Diseases of The Anus Rev#1CDocument77 pagesDiseases of The Anus Rev#1C2012No ratings yet
- Review of The Evidence For Herbal Medications and NutraceuticalsDocument5 pagesReview of The Evidence For Herbal Medications and Nutraceuticals2012No ratings yet
- Clin Tox Oral Vs IV ActylcysteineDocument19 pagesClin Tox Oral Vs IV Actylcysteine2012No ratings yet
- Organ Transplantation, Immunology and RejectionDocument2 pagesOrgan Transplantation, Immunology and Rejection2012No ratings yet
- Test Blueprint For Final Exam 2008-2009 For 75 PtsDocument3 pagesTest Blueprint For Final Exam 2008-2009 For 75 Pts2012No ratings yet
- Art of Med Trans Feb 28Document9 pagesArt of Med Trans Feb 282012No ratings yet
- Patho Lab Trans - ButchDocument6 pagesPatho Lab Trans - Butch2012No ratings yet
- CSAP Full 2002Document125 pagesCSAP Full 20022012No ratings yet
- Pharma EvaluationDocument1 pagePharma Evaluation2012No ratings yet
- Renal Patho Lab 2 PART 1 ColoredDocument8 pagesRenal Patho Lab 2 PART 1 Colored2012No ratings yet
- Glomerulonephritis Block A TransDocument7 pagesGlomerulonephritis Block A Trans2012No ratings yet
- OS 214 - Renal Module - Imaging of The KUBDocument9 pagesOS 214 - Renal Module - Imaging of The KUB2012No ratings yet
- Trans Glomerularpatho FinalDocument16 pagesTrans Glomerularpatho Final2012100% (1)
- 434 OS 212 PictoTrans - Cutaneous SymptomatologyDocument51 pages434 OS 212 PictoTrans - Cutaneous Symptomatology2012No ratings yet
- Laccase Mediator Pretreatment of Wheat StrawDocument15 pagesLaccase Mediator Pretreatment of Wheat StrawMeyerling RandfordNo ratings yet
- Greek God and Goddess ListDocument3 pagesGreek God and Goddess Listapi-359276609No ratings yet
- Fall ProtectionDocument5 pagesFall ProtectionAamir AliNo ratings yet
- Acute Atelectasis Prevention & TreatmentDocument9 pagesAcute Atelectasis Prevention & TreatmentmetabolismeproteinNo ratings yet
- Electric Vehicle BatteryDocument15 pagesElectric Vehicle BatteryTotal Acess100% (1)
- Read The Following Text. A Day in The Life of Paula Radcliffe - Marathon RunnerDocument2 pagesRead The Following Text. A Day in The Life of Paula Radcliffe - Marathon RunnerAldo JimenezNo ratings yet
- Breading Guide To All FoodDocument1 pageBreading Guide To All FoodInno EspinaNo ratings yet
- Weekly Home Learning Plan: Grade 8 - Quarter 2. Week 7Document3 pagesWeekly Home Learning Plan: Grade 8 - Quarter 2. Week 7Danmer Jude TorresNo ratings yet
- Employment Law Lubs 3915Document4 pagesEmployment Law Lubs 3915ogunsatoNo ratings yet
- Funda PharmaDocument9 pagesFunda PharmaShiangNo ratings yet
- State-of-the-Art Reactor Consequence Analyses (SOARCA) ReportDocument200 pagesState-of-the-Art Reactor Consequence Analyses (SOARCA) ReportKingba OlayemiNo ratings yet
- M96SC05 Oleo StrutDocument6 pagesM96SC05 Oleo Strutchaumont12345No ratings yet
- Makalah ThoughtDocument5 pagesMakalah Thoughtifa safiraNo ratings yet
- Thalassemia WikiDocument12 pagesThalassemia Wikiholy_miracleNo ratings yet
- Auxiliary Range: CLR - High Speed Trip Lockout RelayDocument2 pagesAuxiliary Range: CLR - High Speed Trip Lockout Relaydave chaudhuryNo ratings yet
- Agri & Food Processing - Biscuit Manufacturing UnitDocument6 pagesAgri & Food Processing - Biscuit Manufacturing Unitvijayind2006No ratings yet
- Nabertherm RHTH Tube Furnace SOPDocument4 pagesNabertherm RHTH Tube Furnace SOPIyere PatrickNo ratings yet
- Lit Crit TextDocument8 pagesLit Crit TextFhe CidroNo ratings yet
- Coffee Master Program Flashcards - QuizletDocument23 pagesCoffee Master Program Flashcards - QuizletmuuayliiNo ratings yet
- Chemistry Code No. 1/2 Set: 3 Time Allowed: 3 Hours Maximum Marks: 100 General InstructionsDocument5 pagesChemistry Code No. 1/2 Set: 3 Time Allowed: 3 Hours Maximum Marks: 100 General InstructionsShalini KumariNo ratings yet
- Brian Cody Mcgonegal ResumeDocument2 pagesBrian Cody Mcgonegal Resumeapi-348833348No ratings yet
- Safety Audit Format Gs ManmadDocument3 pagesSafety Audit Format Gs ManmadsunilNo ratings yet
- Chapter 3 NotesDocument10 pagesChapter 3 Notesmjamie12345No ratings yet
- Kluge 2004 MetabolaDocument42 pagesKluge 2004 MetabolaBlah BlahNo ratings yet
- Experienced Waiter ResumeDocument3 pagesExperienced Waiter ResumeArchford ManyereNo ratings yet
- Intermediate Alloy Steels Properties and SpecificationsDocument15 pagesIntermediate Alloy Steels Properties and Specificationsanon_558118723100% (1)
- Caregiving Learning Activity SheetDocument7 pagesCaregiving Learning Activity SheetJuvy Lyn Conda100% (5)
- CN LSHC The Future of Pharmacy en 031120Document8 pagesCN LSHC The Future of Pharmacy en 031120marina_netNo ratings yet