Professional Documents
Culture Documents
Early Diagnosis of TB
Uploaded by
hollywoodd0 ratings0% found this document useful (0 votes)
30 views9 pagesread
Original Title
Early Diagnosis of Tb
Copyright
© Attribution Non-Commercial (BY-NC)
Available Formats
PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this Documentread
Copyright:
Attribution Non-Commercial (BY-NC)
Available Formats
Download as PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
30 views9 pagesEarly Diagnosis of TB
Uploaded by
hollywooddread
Copyright:
Attribution Non-Commercial (BY-NC)
Available Formats
Download as PDF, TXT or read online from Scribd
You are on page 1of 9
Early Roentgen Diagnosis of Tuberculosis
of the Hip In Children!
JOSEPH M. WINSTON, M.D.2 and JAMES S. HEWSON, M.D.3
T
HE EARLY ROENTGEN diagnosis of
tuberculosis of the hip in children has
received little attention in recent radiologic
literature. This is primarily due to the
decline of tuberculosis in this country and
the advent of the antituberculous chemo-
therapeutic agents. However, the disease
is far from eradicated; new cases are still
being seen, often after irreversible changes
have occurred.
The usual end-result of tuberculous dis-
the principal distinguishing features of
tuberculous arthritis. Since it appears
that these criteria are not widely known, re-
statement and further illustrations seem
indicated.
During the past fifteen years, there have
been seen at the Alfred 1. duPont In-
stitute 9 patients with early roentgen
changes in the hips in whom there was
microscopic proof of tuberculosis. Not
included in this series are 3 cases which
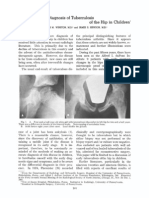
Fig. 1. A. Four-and-a-half-year-old white girl with intermittent discomfort in left hip for two and a half years.
There was a difference in density of the femoral heads. Note cupping of acetabular fossa.
B. Solid fusion eight years after onset. Lead shields the gonads.
ease of a joint has been ankylosis (1) .
There is a reasonable chance, however,
since the discovery of antibiotics, of ob-
taining a mobile joint if the disease is
recognized in its early stage. It is im-
portant, therefore, to be constantly re-
minded of the methods of making an ac-
curate diagnosis of this disease in children)
to familiarize oneself with the early diag-
nostic signs and symptoms, and to be aware
of the differential diagnosis in their pres-
ence. In 1924, Phemister (26) recorded
clinically and roentgenographically were
thought to be tuberculosis but in which
either biopsy was not performed or the
biopsy report and/or culture were negative.
Also excluded are patients with well ad-
vanced and of ten healed tuberculosis of the
hip, admitted for reconstructive surgery.
This paper will be limited to a discussion of
early tuberculosis ofthe hip in children.
Earlier literature, particularly in the
nineteen twenties and nineteen thirties, is
filled with reports of excellent results of
1 From the Departments of Radiology and Orthopedic Surgery, Hospital of the University of Pennsylvania,
Philadelphia, Penna., and Alfred 1. duPont Institute of the Nemours Foundation, Wilmington, De1. Presented
at the Forty-seventh Annual Meeting of the Radiological Society of North America, Chicago, Il1., Nov. 26-Dec. 1,
1961.
2 Now at Jeanes Hospital, Philadelphia, Penna. Instructor in Radiology, University of Pennsylvania.
3 Resident in Orthopedic Surgery, University of Pennsylvania.
241
242 JOSEPH M. WINSTON AND JAMES S. HEWSON
Fig. 2. A. Normal right hip in 2-year-old boy with a mass over the
left hip and limp of recent onset. The left hip was held in a position of flexion.
B. Generalized demineralization of hip. There is widening of the epi-
physeal plate with irregularity of the adjacent bony surfaces. Note cystic
change in the femoral neck.
C. Lateral view of left hip showing widened epiphyseal line and periosteal
reaction.
See Fig. 2, D for follow-up,
August 1962
treatment of tuberculosis of the hip.
Rollier (3), for instance, in 1930 reported
74 per cent cures, with function of the hip
joint. Not' all the cases, however, were
verified by tissue biopsy or bacteriologic
examination. In 1921, Sundt (4) stated
that in a series of 243 cases of hip disease
seen from 1903 to 1918, 29.6 per cent were
nontuberculous. Among these were cases
of congenital coxa vara, epiphysiolysis,
fracture, arthritis deformans, osteomyelitis,
syphilis, synovitis of tuberculous origin,
hysteria, and Legg-Perthes disease. Neil-
son (5) in 1923 gave a differential diagnosis
of hip conditions which had been .con-
sidered tuberculous. In 1930 O'Connor
(6), reviewing 189 cases admitted with a
tentative diagnosis of tuberculosis, found
54 that were not tuberculous. The follow-
ing year Milgram (7) reported that, of 88
cases of Legg-Perthes disease, 31 had been
diagnosed as tuberculosis on the first
admission. In addition} proved tuberculo-
sis was initially misdiagnosed in 38.. 7 per
cent of 142 patients. Those cases with an
insidious onset were incorrectly diagnosed
29 per cent of the time, those with a sudden
onset were incorrectly diagnosed 61.9 per
Vol. 79 EARLY DIAGNOSIS OF TUBERCULOSIS OF THE HIP IN CHILDREN 243
cent of the time, and at operation tuber-
culosis was apparently unrecognized 67.3
per cent of the time. The roentgen diag-
nosis of tuberculosis of the hip was missed
41.9 per cent of the time. Barr (8) re-
ported on 106 consecutive cases in children
and found that in 15 per cent the admission
diagnosis was incorrect.
PATHOGENESIS
Tuberculosis of the skeleton is a sign of
generalized disease and practically always
arises as a result of hematogenous spread
from primary foci in other regions (9,
10). In children the primary infection is
usually in the lungs and the tracheo-
bronchial lymph nodes (11). Campos
(12) found that, of 500 cases of skeletal
tuberculosis which he reviewed, 57 per cent
had normal chest roentgenograms. Six
of our patients had roentgen changes in
the chest suggestive of tuberculosis. It
is postulated that in children tuberculosis
occurs about the hips because of the
proportionately large blood supply to this
rapidly growing area. The frequency of
involvement of the metaphysis is due to the
lodging of the bacilli in the end arteries in
this region of the bone (11).
Tuberculosis of the hip in children has a
high incidence, accounting for about 20 per
cent of cases of bone and joint tuberculosis
(13). Buzby (14), in 1922, reported that
92 per cent of his cases of tuberculosis of
the hip began before ten years of age and
were always secondary to a focus elsewhere.
Ponseti (15), in 1948, analyzed 31 cases
of proved tuberculosis and found the age
of onset ranging from one to twelve years.
Tuberculosis in children may affect the
hip joint in either of two ways (15).
In young children the lesion mayat first
be para-articular, with the joint space
itself only gradually becoming involved.
The most common sites of para-articular
involvement are the femoral neck, the
ilium on the pelvic side of the acetabular
roof, and the junction of the shaft and neck.
The other type involves the joint itself.
The extra-articular foci of tuberculous
osteitis are seen more often in children and
Fig. 2. D. Same case as Fig. 2, A-C. Follow-up
approximately one year later.
very rarely in adults. In both types, it is
probable that synovial membrane and
bone are involved from the start, but in
young children the bone lesion is more
apparent initially and in the older person
the synovial lesion. Wilkinson (16) re-
ports that all patients with bone involve-
ment had synovial changes.
CLINICAL HISTORY
The usual onset of tuberculosis of the
hip is gradual and insidious. Indeed, as
reported by Iversen (17) in 1937, it often
starts without a demonstrable source.
Dsually a limp precedes pain and there
develops a stiffness of the involved hip.
The affected leg is often shorter than the
sound one (18). Muscle spasm may occur
in an attempt to splint the joint. Night
cries are provoked by the pain and sudden
discomfort following the muscle relaxation
that occurs with rest. The pain is re-
ferred either from the inner aspect of the
244
JOSEPH M. WINSTON AND JAMES S. HEWSON August 1962
Fig. 3. A. Eighteen-month-old girl with a six-month history of limp and
pain in the left lower extremity. The hip was held in external rotation. The
initial study demonstrates subluxation of the left hip. The arrow indicates
metaphyseal changes. There is evidence of periosteal production along the
shaft.
B. Periosteal production seen better on lateral projection.
C. Seven days later. Note rapid progression of destructive changes in the
metaphysis.
D. Two months later. Further changes in the femoral head and meta-
physes.
See Fig. 3, E for follow-up.
thigh to the knee, in the distribution of the
obturator nerve, or to the anterior surface
of the thigh, following the course of
the femoral nerve. The patient often
becomes worse as the day progresses.
Usually there is some lumbar lordosis on
standing erect. Typically, there are a rise
in temperature of 1 1/2 to 2
0
in the eve-
ning, some anorexia, and malaise.
Six of our 9 patients complained of a
limp and 7 presented with pain. Less fre-
quent symptoms were night cries, fever,
and lethargy.
Limitation of motion was the most fre-
quent finding on initial physical examina-
tion. In the early stages this is usually
due to reflex muscle spasm. Later it may
be the result of actual pain on motion of
the joint.
Initially the extremity is flexed at the
hips, abducted, and externally rotated.
In this position the joint capsule is re-
laxed, and the pain is relieved. As the
disease progresses, the hip becomes ad-
ducted and internally rotated as well as
flexed.
Atrophy of the muscles of the affected
limb is a constant finding. Swelling due to
Vol. 79
EARLY DIAGNOSIS OF TUBERCULOSIS OF THE HIP IN CHILDREN 245
periarticular inflammation may occur in
any area about the hip.
DIAGNOSIS
Since there is a reasonable chance of
obtaining a mobile joint if the disease is
recognized in its earliest stages, early diag-
nosis is imperative. In addition to the
clinical history and physical findings, blood
studies, skin tests, roentgen studies, and
biopsy are helpful diagnostic aids.
1. Blood Studies: The white blood
count and sedimentation rate are not
specific, but an increase in the sedimenta-
tion rate, a decreased hemoglobin and red
count, and an increased white blood count
are helpful laboratory findings.
2. Skin Test: The Mantoux skin test is
of value only if negative on repetition.
Mills et al. (19) reported that of 35 proved
cases 34 gave a positive reaction, while of
20 patients with nontuberculous disease
of the hip only 5 had positive reactions.
3. Roentgen Studies: The roentgeno-
graphic changes can be divided into
osseous, intra-articular, and peri-articular
soft-tissue.
Early roentgen changes include osteo-
porosis, rarefaction, or merely the slightest
alteration in density of the upper femur and
iliac bones. More advanced changes con-
sist of erosion of the acetabular surface,
areas of cancellous bone destruction, ab-
scesses or small cyst-like areas of bone
destruction, widening of the zone of in-
creased density of the acetabulum, hernia-
tion of the acetabulum, and periosteal
proliferation.
The primary location of the disease, ac-
cording to Badgley and Hammond (28),
was in the acetabular area in 50 per cent,
in the femoral epiphysis in 32 per cent, in
the neck of the femur in 14 per cent, and
in the greater trochanter in 4 per cent.
Dobson (21), reported on 320 cases, of
which 39.3 per cent involved the acetabu-
lum, 34.1 per cent the acetabulum and
femoral head, 19.2 per cent the head of the
femur, and 7.4 per cent the femoral neck.
Cholmeley (22) found 44 per cent located
in the acetabulum, 2 per cent in the epi-
Fig. 3. E. Same case as Fig. 3, A-D. Residual
deformity at time of follow-up study four years later.
physis, 17 per cent in the neck, and 2 per
cent in the greater trochanter.
Areas of contact of joint cartilage con-
stitute a barrier to the extension of the
disease and cause destruction to take place
first at the joint margins where there is
little or no contact or pressure.
The destruction of articular cartilage by
granulation tissue is characteristically slow
in tuberculosis owing to the lack of pro-
teolytic enzymes in the tuberculous exu-
date. Since the destruction of bone follows
the destruction of the overlying cartilage,
bone changes are first seen in the peripheral
and non-contact areas; the subchondral
bone, like the articular cartilage, is well
preserved in the regions of contact. As a
result, the main force of the destructive
lesion may manifest itself at points rela-
tively remote from weight-bearing surfaces
(10).
Tuberculosis as a primary focus in the
neck of the femur usually occurs as a
246 JOSEPH M. WINSTON AND JAMES S. HEWSON
,
,It;u!,, .
H .
i t'; 'I'
. . \\ n,' ...... ...,'
Fig. 4. A. Difference in density on two sides difficult to demonstrate
on reproductions but very apparent on films. Such a difference is easily over-
looked if films are not of excellent quality and if index of suspicion is not
high.
B. Decreased density of right hip. Note cystic changes in the acetabular
fossa.
C. Thirty months later. Note flattening of the femoral head, advanced
cystic changes in the acetabular fossa, and reaction at edge of acetabulum.
August 1962
circumscribed area of bone destruction in
the metaphysis, and characteristically ap-
pears as a wedge-shaped area upon the
under surface of the fem.oral neck just distal
to the epiphyseal line (9), in the distribu-
tion of the infero-rnesial neck artery (26),
with or without periosteal proliferation.
In the acetabular region, destruction occurs
in a posterior mediallocation (23).
Odelberg-Johnson (27), divided the bone
changes into 3 stages. In the first there is
a loss of lime salts involving the entire hip
region. The contours of the joint and the
articular cartilage are preserved in this
stage and there is some question of whether.
Shenton's line is broken. Femoral growth
is often disturbed so that the shaft involved
is narrower and the cortex thinner than on
the normal side. During the second stage,
which includes the second year of illness,
there is more pronounced bone atrophy,
with blurred spongiosa, and there are
ill-defined defects in the joint contour.
The femur is dislocated upward and
laterally, the articular cartilage becomes
destroyed, and there is more pronounced
shaft growth disturbance. In the third
stage, which occurs not before the end of
Vol. 79 EARLY DIAGNOSIS OF TUBERCULOSIS OF THE HIP IN CHILDREN
Fig. 5. A. Seven-year-old girl with limp in the left leg for one year. Note
irregularity to acetabular fossa. There is no evidence of swelling of the joint
capsule.
B. Two months later the changes in the acetabular fossa are more promi-
nent.
C. Ten months later.
D. Evidence of good healing eight years after onset of symptoms.
247
the second year, there is beginning repair,
and the destroyed areas are sharply de-
fined, with sclerotic borders. At this
stage there is an increased lime content
and the spongiosa is more distinct.
There may be an associated slight
increase in the joint space due to distention
with fluid. As mentioned above, tuber-
culous exudate does not contain proteolytic
enzymes, and cartilage therefore persists
until later stages, when it is covered with a
pannus of unhealthy granulation tissue
(13). As a result, reduction in the depth
or disappearance of the cartilage space is
characteristically of late occurrence in
tuberculous arthritis.
The articular capsule may appear
swollen, with associated thickening of the
248 JOSEPH M. WINSTON AND JAMES S. HEWSON August 1962
adjoining subcutaneous tissue. The swell-
ing may be due to inflammation of the
periarticular tissue or possibly infiltration
of soft structures or a cold abscess. There
may be widening and change in the con-
tour of the shadow of the normal obturator
internus muscle. This is due to dis-
placement of the tendon of the obturator
muscle as it passes adjacent to the ex-
panded hip capsule.
The leg may be in a position of flexion.
Subluxation is not rare and, if it has oc-
curred, further enhances the appearance
of a narrowed joint space. Dislocation is
thought to be due to a combination of
muscle spasm plus the pressure of the head
on the softened acetabulum, causing the
head to travel upward and backward, with
dislocation onto the posterior ilium.
CULTURE AND BIOPSY
The final method of diagnosis consists in
obtaining material for culture and/or
microscopic examination. Where there is
evidence of synovial effusion into the joint
or abscess formation, aspiration may be of
help (25). The aspirated fluid should be
examined microscopically, cultured, and
inoculated into guinea-pigs. Unfor-
tunately many patients will have no effu-
sion. Even when fluid is obtainable, the
results of culture are often nonconfirrn-
atory. Fluid was obtained in 5 of our 9
patients and was positive in 3. Petragnani
and Dubos preparation appeared to be the
best culture media.
Biopsy of regional lymph nodes may
yield valuable information in a relatively
high percentage of cases (24), particularly
in the period between the third and fif-
teenth months of the disease. The lymph
drainage from the hip is not to the inguinal
region, but to the iliac group and, there-
fore, if node biopsy is attempted, it must
be in the latter area. Lymph node biopsy
is now rarely necessary because of the
safety and greater accuracy of biopsy of
the affected joint itself (22).
DIFFERENTIAL DIAGNOSIS
Differential diagnosis includes Legg-
Perthes disease, nontuberculous infection,
acute and chronic arthritis, congenital
dislocation of the hip, and slipped epiphy-
sis. Legg-Perthes disease clinically may
simulate tuberculosis. Pain, limp, slight
shortening of the leg, and mild muscular
atrophy are present, although usually to a
lesser degree. There is no limitation of
extension and flexion is freer. In contrast
to tuberculosis, the general condition of the
child is good. Roentgenographically the
changes, limited mainly to the epiphysis,
consist of irregularity in density, fragmen-
tation' and compression. The femoral
neck may become shorter and broader.
At no time is there actual destruction of
the articular cortex.
In 1924, Phemister (26) recorded points
which still stand as the principal dis-
tinguishing features of tuberculous and
nontuberculous suppurative arthritis. In
pyogenic arthritis the articular cartilage
is destroyed and broken down first at the
point of contact and pressure of opposing
articular surfaces. The infectious pro-
teolytic ferments assist greatly in the
rapid removal of the necrotic cartilage.
As a result, there is early narrowing or
disappearance of the joint space, and the
earliest bone destruction occurs on the
opposing or weight-bearing portion of the
articular surfaces.
In tuberculous arthritis the articular
cartilage is not destroyed first but rather is
protected at the point of contact and pres-
sure of opposing articular surfaces. The
earliest destruction is peripheral, along the
free surfaces where tuberculous granuJlation
can grow and remove the dead tissue. The
first disappearance of the bony cortical
shadow is usually seen peripherally about
the margins of the weight-bearing portions
of the articular surface where there has
been absorption by the granulation. As a
result, reduction in the depth of the joint
space is characteristically late.
Congenital dislocation of the hip may be
confused clinically with tuberculosis. Ab-
sence of pain, tendency to favor the affected
limb, and unaltered general state are
in favor of dislocation of the hip. Roent-
Vol. 79 EARLY DIAGNOSIS OF TUBERCULOSIS OF THE HIP IN CHILDREN 249
genographically, the femoral neck is
directed above the acetabulum which may
be shallow. The epiphysis, if calcified, is
in a high position and may show flattening
owing to the abnormal pressure.
In slipped femoral epiphysis the epiphy-
seal line is wide and irregular with upward
and forward displacement of the neck on
the head of the femur. There may be
anterior bowing of the neck and new bone
may form between the lower border of the
neck and the overhanging head.
SUMMARY
An insidious onset of pain, limp, and
stiffness associated with limitation of
motion and roentgen findings of rare-
faction and the slightest alteration in
density of the upper femur and iliac bones
should make one suspicious of early tu-
berculous involvement of the hip. It is
hoped that more lesions will be recognized
early, in order that a mobile joint may
be the end-result and ankylosis the rarity.
Jeanes Hospital
Fox Chase
Philadelphia 11, Penna.
REFERENCES
1. CHOLMELEY, J. A.: Femoral Osteotomy in
Extra-articular Arthrodesis of the Tuberculous Hip.
J. Bone & Joint Surg. 38-B: 342-352, February 1956.
2. POMERANZ, M. M.: Roentgen Diagnosis of
Bone and Joint Tuberculosis. Am. J. Roentgeno1. 29:
753-762, June 1933.
3. ROLLIER, A.: Conservative Treatment in Sur-
gical Tuberculosis of the Lower Extremity. J. Bone &
Joint Surg. 12: 733-748, October 1930.
4. SUNDT, H.: Tuberculous Hip Disease and Its
Simulants. Tubercle, London 2: 289-299, 1920-1921.
5. NIELSON, A. L.: Abortive Type of Tubercu-
lous Hip Joint Disease. J.A.M.A. 80: 1442-1443,
May 19, 1923.
6. O'CONNOR, D. S.: Tuberculosis of the Hip
Joint; End Result Study. New England J. Med. 203:
636-641, Sept. 25, 1930.
7. MILGRAM, J. E.: Diagnostic Inaccuracy in
Tuberculosis of the Bone, Joint, and Bursa. J .A.M.A.
97: 232-235, July 25, 1931.
8. BARR, J. S.: Tuberculosis of the Hip in Chil-
dren. J.A.M.A. 107: 1517-1522, Nov. 7, 1936.
9. RATLIFF, A. H.: Tuberculosis of the Femoral
Neck in Childhood. J. Bone & Joint Surg. 39-A: 1365-
1373, December 1957.
10. WIDMANN, B. P., OSTRUM, H. W., AND MILLER,
R. F.: Unusual Manifestations of Bone Tuberculosis.
Radiology 32: 434--445, April 1939.
11. HATCHER, C. H., AND PHEMISTER, D. B.: The
Primary Point of Infection in Tuberculosis of the Hip
Joint. Surg., Oynec., & Obst. 65: 721-740, December
1937.
12. CAMPOS, O. P.: Bone and Joint Tuberculosis
and Its Treatment. J. Bone & Joint Surg. 37-A: 937-
966, October 1955.
13. FERGUSON, A. B.: Orthopedic Surgery in In-
fancy and Childhood. Baltimore, Williams & Wilkins
ce., 1957.
14. BUZBY, B. F.: Tuberculosis of the Hip. New
York M. J. 116: 150-153, Aug. 2, 1922.
15. PONSETI, 1.: Evolution and Treatment of
Tuberculosis of the Hip. Surg., Gynec. & Obst. 87:
257-276, September 1948.
16. Wilkinson. Cited by Stevenson. Tubercle,
London 38: 164; 355, 1957.
17. IVERSEN, S. C.; On the Infantile Coxitis and
Its Sequelae. Acta orthop, scandinav. 8: 231-292,
1937.
18. RUGH, J. T.: Diagnosis and Differential Diag-
nosis of Early Hip Joint Disease in Childhood. New
York M. J. 115: 256-258, March 1, 1922.
19. MILLS, T. J., OWEN, R., AND STRACH, E. H.:
Early Diagnosis of Bone and Joint Tuberculosis in
Children. Lancet 2: 57-59, July 14, 1956.
20. BROWN, C. J. 0.: Diagnosis and End Results
of Tuberculosis of the Hip Joint. M. J. Australia 2:
196-202, Aug. 18, 1928.
21. DOBSON, J.: Prognosis in Tuberculosis of the
Hip. Analysis of Results of Treatment and of Factors
which Influence End-Result. J. Bone & Joint Surg.
33-B: 149-159, May 1951.
22. CHOLMELEY, J. A.: Distribution and Treat-
ment of Extra-articular Foci in Tuberculous Arthritis
of Hip Joint. Brit. J. Surg. 27: 224-233, October 1939.
23. WILKINSON, M. C.: Partial Synovectomy and
Curettage in the Treatment of Tuberculosis of the Hip.
J. Bone & Joint Surg. 39-B: 66-79, February 1957.
24. SMITH, A. DE F. : The Early Diagnosis of Joint
Tuberculosis. J.A.M.A. 83: 1569-1573, Nov. 15, 1924.
25. MERCER, W.: The Management of the Tuber-
culous Hip Joint. J. Bone & Joint Surg. 36-A: 1123-
1128, December 1954.
26. PHEMISTER, D. B., AND HATCHER, C. H.:
Correlation of Pathological and Roentgenological
Findings in the Diagnosis of Tuberculous Arthritis.
Am. J. Roentgenol. 29: 736-752, June 1933.
27. ODELBERG-JOHNSON, G.: Different Types of
Tuberculosis of the Hip in Children. Acta orthop.
scandinav. 9: 197-209, 1938.
28. BADGLEY, C. E., AND HAMMOND, G.: Tuber-
culosis of the Hip; Review of 76 Patients with Proved
Tuberculous Arthritis of 77 Hips Treated By Arthro-
desis. J. Bone & Joint Surg. 24: 135-147, January
1942.
(Pro le summario in interlingua, vider le pagina 263)
You might also like
- Never Split the Difference: Negotiating As If Your Life Depended On ItFrom EverandNever Split the Difference: Negotiating As If Your Life Depended On ItRating: 4.5 out of 5 stars4.5/5 (838)
- Shoe Dog: A Memoir by the Creator of NikeFrom EverandShoe Dog: A Memoir by the Creator of NikeRating: 4.5 out of 5 stars4.5/5 (537)
- HRCT PatternsDocument5 pagesHRCT PatternshollywooddNo ratings yet
- Early Diagnosis of TBDocument9 pagesEarly Diagnosis of TBhollywooddNo ratings yet
- DX STD and Classification of TBC in ATSDocument20 pagesDX STD and Classification of TBC in ATSAeris YeapNo ratings yet
- Testicular Tumour MetastasisDocument11 pagesTesticular Tumour MetastasishollywooddNo ratings yet
- DX STD and Classification of TBC in ATSDocument20 pagesDX STD and Classification of TBC in ATSAeris YeapNo ratings yet
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeFrom EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeRating: 4 out of 5 stars4/5 (5794)
- The Yellow House: A Memoir (2019 National Book Award Winner)From EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Rating: 4 out of 5 stars4/5 (98)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceFrom EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceRating: 4 out of 5 stars4/5 (894)
- The Little Book of Hygge: Danish Secrets to Happy LivingFrom EverandThe Little Book of Hygge: Danish Secrets to Happy LivingRating: 3.5 out of 5 stars3.5/5 (399)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureFrom EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureRating: 4.5 out of 5 stars4.5/5 (474)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryFrom EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryRating: 3.5 out of 5 stars3.5/5 (231)
- Grit: The Power of Passion and PerseveranceFrom EverandGrit: The Power of Passion and PerseveranceRating: 4 out of 5 stars4/5 (587)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaFrom EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaRating: 4.5 out of 5 stars4.5/5 (265)
- On Fire: The (Burning) Case for a Green New DealFrom EverandOn Fire: The (Burning) Case for a Green New DealRating: 4 out of 5 stars4/5 (73)
- The Emperor of All Maladies: A Biography of CancerFrom EverandThe Emperor of All Maladies: A Biography of CancerRating: 4.5 out of 5 stars4.5/5 (271)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersFrom EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersRating: 4.5 out of 5 stars4.5/5 (344)
- The Unwinding: An Inner History of the New AmericaFrom EverandThe Unwinding: An Inner History of the New AmericaRating: 4 out of 5 stars4/5 (45)
- Team of Rivals: The Political Genius of Abraham LincolnFrom EverandTeam of Rivals: The Political Genius of Abraham LincolnRating: 4.5 out of 5 stars4.5/5 (234)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyFrom EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyRating: 3.5 out of 5 stars3.5/5 (2219)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreFrom EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreRating: 4 out of 5 stars4/5 (1090)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)From EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Rating: 4.5 out of 5 stars4.5/5 (119)
- Her Body and Other Parties: StoriesFrom EverandHer Body and Other Parties: StoriesRating: 4 out of 5 stars4/5 (821)