Professional Documents
Culture Documents
Benefit CKD
Uploaded by
Ibnu ZakiCopyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Benefit CKD
Uploaded by
Ibnu ZakiCopyright:
Available Formats
REVIEW
Benets in Nutritional Interventions in Patients With CKD Stage 3-4
Philippe Chauveau, MD, and Michel Aparicio, MD, PhD
The efcacy and safety of protein-restricted diets in chronic kidney disease (CKD) is still a matter of debate. However, several studies have clearly demonstrated the benecial effects of such diets on the outcome of patients with stage 3-4 CKD. This point has been conrmed by 4 recent studies. In 2009, a meta-analysis showed that protein restriction signicantly delayed the time to renal death with a substantial economic benet for the health service. Although toxicity of urea has since long been considered as negligible, an experimental model in rats has shown a direct role of urea in the development of oxidative stress and insulin resistance, which are among the leading mechanisms of cardiovascular complications in CKD. These latter results conrm an interest in studying reduction in blood urea levels as observed in patients kept on a low-protein diet (LPD) or on a supplemented very-low protein diet (SVLPD). A reduction in proteinuria, which is associated to a LPD, has the following prognostic value: the more important the reduction in proteinuria, slower is the decline in renal function. This effect, which is additive to the one of an angiotensin-converting enzyme inhibitor (ACEI), is higher with SVLPD than with conventional LPD. Safety of a reduced protein intake has been conrmed by the study on the long-term outcomes (11 years) of patients already on SVLPD. The difference between these results and those from the extended follow-up of the modication of diet in renal disease (MDRD) study, in which no recommendations were made after the completion of the trial, conrms the importance of a close nutritional survey of patients with CKD who are put on a protein-restricted diet. 2011 by the National Kidney Foundation, Inc. All rights reserved.
ORE THAN 100 YEARS after the initial publication on the prescription of dietary protein restriction in patients with chronic kidney disease (CKD), this topic remains a matter of debate and controversy, as shown by a recent editorial of Alp Ikizler entitled dietary restriction in CKD: the debate continues.1 Several cases involving meta-analysis have clearly shown that protein restriction prescribed to stable patients with CKD resulted in a signicant delay in renal death without any detrimental effect, as long as patients were being carefully followed up.2 Many nephrologists are still reluctant to prescribe such a diet on account of a potential impairment of nutritional status; however,
Department of Nephrology, Centre Hospitalier Universitaire and University Bordeaux II, Bordeaux, France. Address reprint requests to Philippe Chauveau, Department of Nephrology, Centre Hospitalier Universitaire and University Bordeaux II, Bordeaux, France. E-mail: ph.chauveau@gmail.com 2011 by the National Kidney Foundation, Inc. All rights reserved. 1051-2276/$36.00 doi:10.1053/j.jrn.2010.11.005
such complications do not seem to have ever been conrmed in the literature. In 2007, Fouque and Aparicio reported the eleven reasons to control the protein intake in patients with CKD.3 In the present review, we report recent studies and new guidance concerning the positive effects of the restriction of protein intake in patients with CKD.
Delay in Renal Replacement Therapy
Studies in the 5/6 nephrectomized rats model have constantly demonstrated that, in comparison with high or normal protein intake, low-protein diet (LPD) and supplemented very-low protein diet (SVLPD) have benecial effects on decrease in renal function.4 The results of clinical studies in human beings are controversial. Most of them included few patients in open studies. The effect of LPD on the rate of decrease of glomerular ltration is also controversial and varies according to the measurement of renal function, that is, slope of decline of plasma creatinine or isotopic
Journal of Renal Nutrition, Vol 21, No 1 (January), 2011: pp 2022
20
NUTRITIONAL INTERVENTIONS IN PATIENTS WITH CKD
21
methods. When the criterion used is renal death or time to renal replacement therapy (RRT), most studies showed a positive effect of protein restriction. In a meta-analysis, which included more than 1,400 patients from 7 controlled studies, Fouque and Aparicio observed that a reduction of 0.2 g protein/kg/day was associated with a reduced renal death of 49%.3 In 2009, another meta-analysis included more than 2,000 patients, and the relative risk of renal death was 0.68 in favor of a reduction in protein intake.5 In 2007, Brunori et al. demonstrated in a randomized study that, for patients aged .70 years, SVLPD delayed the initiation of dialysis without any negative consequence on morbidity and mortality, the mean delay in the SVLPD group was 10.7 months.6 On the basis of this study, an economic evaluation showed that the rst year economic benet for the health service per patient was V21,800.7 In comparison with LPD, SVLPD seems to have an additive effect; Chang et al. studied 120 patients who were trained for 6 months on a LPD (0.6 g/kg/day) and then switched to a SVLPD. Glomerular ltration rate (GFR) decline (estimated using the modication of diet in renal disease [MDRD] formula) during the SVLPD period was signicantly lower in patients with and without diabetes.8
explain these data ndings, the authors propose that urea can alter the function of cytosolic, nuclear, and mitochondrial proteins that are involved in the regulation of mitochondrial ROS production. According to them, reduction of serum urea to its lowest achievable level in addition to a judicious use of antioxidant supplements should be proposed to patients with CKD to stem the production of ROS and their deleterious consequences.
LPD and Proteinuria
One of the less controversial issues concerning LPD in CKD is that in proteinuric patients with or without diabetes, restriction in protein intake is associated with reduction of proteinuria. According to the series, the mean reduction in proteinuria ranges from 20% to 37%. Patients with reduction higher than 50% exhibit a higher reduction of GFR decline. LPD confers an additive effect with an ACE inhibitor or ARB.11 It has been recently demonstrated by Bellizzi et al. that SVLPD had a higher effect on proteinuria as compared with LPD alone.12
Nutritional Safety and Long-term Outcomes
It had been suggested that reduction in protein intake could be associated with an increased risk of malnutrition and that LPD and SVLPD could have detrimental effects before RRT and could also have an effect on morbidity and mortality after patients were put on RRT. This remains true in patients without counseling or on standard nutritional survey. Approximately 50% of patients, who started RRT in the United States between 2005 and 2007, exhibited low serum albumin level. In contrast, among all LPD or SVLPD clinical studies, very few cases of malnutrition have been reported. Nine months after completion of the MDRD study, the mean albuminemia level was 42 g/L, whereas in the Bordeaux cohort of 239 patients, only 2 stopped for malnutrition13 and the mean albuminemia level at the start of RRT was 39 g/L. After the initiation of RRT, patients who were previously on SVLPD rapidly increased their protein intake and maintained an adequate calories intake at least during the rst year. In 2009, we examined the long-term outcomes of patients who were included between 1985 and 2000. The survival rate of dialysis patients was comparable with those of the
Insulin Resistance and Oxidative Stress
The increased level of oxidative stress and insulin resistance (IR), which are common in patients with CKD, seem to play a crucial role in the pathogenesis of several complications, particularly atherosclerosis, which is the leading cause of death in uremic patients.9 These abnormalities are observed in dialyzed patients as well as in patients with mild or moderate CKD. A recent article10 suggested that an increased level of urea, which has since long been considered to have negligible toxicity, could be the link between these 2 abnormalities. In a mouse model of CKD induced by 5/6 nephrectomy, DApolito et al. reported increased reactive oxygen species (ROS) production, IR, and increased expression of IR-associated adipokines in visceral adipose tissue. Urea infusion in normal animals induced abnormalities similar to that observed in uremic animals. The impairment of insulin sensitivity was corrected by antioxidant therapy, thereby leading the authors to conclude that IR resulted from urea-induced ROS. To
22
CHAUVEAU AND APARICIO
renal diseases: a meta-analysis. Ann Intern Med 124:627-632, 1996 3. Fouque D, Aparicio M: Eleven reasons to control the protein intake of patients with chronic kidney disease. Nat Clin Pract Nephrol 3:383-392, 2007 4. Gao X, Wu J, Dong Z, et al: A low-protein diet supplemented with ketoacids plays a more protective role against oxidative stress of rat kidney tissue with 5/6 nephrectomy than a low-protein diet alone. Br J Nutr 103:608-616, 2010 5. Fouque D, Laville M: Low protein diets for chronic kidney disease in non diabetic adults. Cochrane Database Syst Rev 3: CD001892, 2009. 6. Brunori G, Viola BF, Parrinello G, et al: Efcacy and safety of a very-low-protein diet when postponing dialysis in the elderly: a prospective randomized multicenter controlled study. Am J Kidney Dis 49:569-580, 2007 7. Scalone L, Borghetti F, Brunori G, et al: Cost-benet analysis of supplemented very low-protein diet versus dialysis in elderly CKD5 patients. Nephrol Dial Transplant 25:907-913, 2010 8. Chang JH, Kim DK, Park JT, et al: Inuence of ketoanalogs supplementation on the progression in chronic kidney disease patients who had training on low-protein diet. Nephrology (Carlton) 14:750-757, 2009 9. Rigalleau V, Gin H: Carbohydrate metabolism in uraemia. Curr Opin Clin Nutr Metab Care 8:463-469, 2005 10. DApolito M, Du X, Zong H, et al: Urea-induced ROS generation causes insulin resistance in mice with chronic renal failure. J Clin Invest 120:203-213, 2010 11. Chauveau P, Combe C, Rigalleau V, et al: Restricted protein diet is associated with decrease in proteinuria: consequences on the progression of renal failure. J Ren Nutr 17: 250-257, 2007 12. Bellizzi V, Di Ioro BR, De Nicola L, et al: Very low protein diet supplemented with ketoanalogs improves blood pressure control in chronic kidney disease. Kidney Int 71:245-251, 2007 13. Chauveau P, Couzi L, Vendrely B, et al: Long-term outcome on renal replacement therapy in patients who previously received a keto acid-supplemented very-low-protein diet. Am J Clin Nutr 90:969-974, 2009 14. Menon V, Kopple JD, Wang X, et al: Effect of a very lowprotein diet on outcomes: long-term follow-up of the Modication of Diet in Renal Disease (MDRD) Study. Am J Kidney Dis 53:208-217, 2009
age-matched patients of the French national registry. The outcome of patients who underwent grafting could be favorably compared with that of the entire cohort of patients who underwent grafting in Bordeaux during the same period.13 These results are in contradiction with those of an extended follow-up of the MDRD study by Menon et al. conducted in 2009,14 in which no recommendations were made after the completion of the trial and no information on medical management and clinical course was available. This conrms that close nutritional survey during the diet, education of the patient and his family, close nutritional counseling when the patient starts RRT, and motivation of the medical staff throughout the patients history from CKD to dialysis and transplantation represent the cornerstone of success of a program of dietary prescription in patients with CKD.
Conclusion
LPD or SVLPD are associated with many benecial effects in patients with CKD stages 3-4. To avoid malnutrition, the nephrology unit should be able to provide nutritional support and education. In these ideal conditions of agreement between the patients and the staff, after an educational program, nutritional therapy with LPD is considered to be nutritionally safe.
References
1. Ikizler TA: Dietary protein restriction in CKD: the debate continues. Am J Kidney Dis 53:189-191, 2009 2. Pedrini MT, Levey AS, Lau J, et al: The effect of dietary protein restriction on the progression of diabetic and nondiabetic
You might also like
- Nutrients 08 00773Document22 pagesNutrients 08 00773Ibnu ZakiNo ratings yet
- Nutrition in Sick PatientsDocument50 pagesNutrition in Sick PatientsIbnu ZakiNo ratings yet
- Nutrition Management in The Intensive Care UnitDocument17 pagesNutrition Management in The Intensive Care UnitIbnu ZakiNo ratings yet
- 2-3 AnatomicalDocument11 pages2-3 AnatomicalIbnu ZakiNo ratings yet
- 05 - 203perkembangan Terkini Diagnosis Dan Penatalaksanaan Imflammatory Bowel Disease PDFDocument6 pages05 - 203perkembangan Terkini Diagnosis Dan Penatalaksanaan Imflammatory Bowel Disease PDFrisda aulia putriNo ratings yet
- 7418 PiDocument2 pages7418 PiIbnu ZakiNo ratings yet
- Shoe Dog: A Memoir by the Creator of NikeFrom EverandShoe Dog: A Memoir by the Creator of NikeRating: 4.5 out of 5 stars4.5/5 (537)
- The Yellow House: A Memoir (2019 National Book Award Winner)From EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Rating: 4 out of 5 stars4/5 (98)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeFrom EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeRating: 4 out of 5 stars4/5 (5794)
- The Little Book of Hygge: Danish Secrets to Happy LivingFrom EverandThe Little Book of Hygge: Danish Secrets to Happy LivingRating: 3.5 out of 5 stars3.5/5 (400)
- Grit: The Power of Passion and PerseveranceFrom EverandGrit: The Power of Passion and PerseveranceRating: 4 out of 5 stars4/5 (588)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureFrom EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureRating: 4.5 out of 5 stars4.5/5 (474)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryFrom EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryRating: 3.5 out of 5 stars3.5/5 (231)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceFrom EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceRating: 4 out of 5 stars4/5 (895)
- Team of Rivals: The Political Genius of Abraham LincolnFrom EverandTeam of Rivals: The Political Genius of Abraham LincolnRating: 4.5 out of 5 stars4.5/5 (234)
- Never Split the Difference: Negotiating As If Your Life Depended On ItFrom EverandNever Split the Difference: Negotiating As If Your Life Depended On ItRating: 4.5 out of 5 stars4.5/5 (838)
- The Emperor of All Maladies: A Biography of CancerFrom EverandThe Emperor of All Maladies: A Biography of CancerRating: 4.5 out of 5 stars4.5/5 (271)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaFrom EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaRating: 4.5 out of 5 stars4.5/5 (266)
- On Fire: The (Burning) Case for a Green New DealFrom EverandOn Fire: The (Burning) Case for a Green New DealRating: 4 out of 5 stars4/5 (74)
- The Unwinding: An Inner History of the New AmericaFrom EverandThe Unwinding: An Inner History of the New AmericaRating: 4 out of 5 stars4/5 (45)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersFrom EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersRating: 4.5 out of 5 stars4.5/5 (345)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyFrom EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyRating: 3.5 out of 5 stars3.5/5 (2259)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreFrom EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreRating: 4 out of 5 stars4/5 (1090)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)From EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Rating: 4.5 out of 5 stars4.5/5 (121)
- Her Body and Other Parties: StoriesFrom EverandHer Body and Other Parties: StoriesRating: 4 out of 5 stars4/5 (821)
- Dengue (Break Bone Fever) - FAQ, DPH-TAMIL NADU, IndiaDocument3 pagesDengue (Break Bone Fever) - FAQ, DPH-TAMIL NADU, IndiaDr.SagindarNo ratings yet
- How To Treat Varicose VeinsDocument2 pagesHow To Treat Varicose VeinsTee VillanuevaNo ratings yet
- TrandolaprilDocument28 pagesTrandolaprilYeyenJaejoongNo ratings yet
- Dialysis Products Catalog PDFDocument52 pagesDialysis Products Catalog PDFAFRIANSYAHNo ratings yet
- Internal Fixation ToolsDocument22 pagesInternal Fixation ToolsChandan Kumar ChoubeyNo ratings yet
- WaterDocument26 pagesWaterKisna Bhurtel100% (1)
- The Work of Hanna KroegerDocument261 pagesThe Work of Hanna Kroegerohaiadios100% (7)
- Seminar HD-RSUD Sleman 2019Document36 pagesSeminar HD-RSUD Sleman 2019herkamaya100% (1)
- Acute Pain NCPDocument2 pagesAcute Pain NCPfaye-pamatmat-257080% (5)
- NCP DM Group 6Document4 pagesNCP DM Group 6Jeffrey Calicdan BucalaNo ratings yet
- JCI-Sentinel Event AlertDocument3 pagesJCI-Sentinel Event AlertDewi Ratna SariNo ratings yet
- (PDF) Download Complete Works of William Shakespeare PDF Ebook by William Shakespeare - Stepor EbookDocument2 pages(PDF) Download Complete Works of William Shakespeare PDF Ebook by William Shakespeare - Stepor EbookAnonymous kJ78MwD4O50% (2)
- Core Practical 9 Antimicrobial Properties of Plants Writing FrameDocument6 pagesCore Practical 9 Antimicrobial Properties of Plants Writing FrametiaNo ratings yet
- MOST Assign1 VitaminsDocument6 pagesMOST Assign1 VitaminsbubblingbrookNo ratings yet
- The Kessler Psychological Distress Scale (K10)Document2 pagesThe Kessler Psychological Distress Scale (K10)octavianNo ratings yet
- Anti Neoplastic AgentsDocument116 pagesAnti Neoplastic AgentsAbii KetiNo ratings yet
- Care of The Chronically Ill and The Older PersonDocument8 pagesCare of The Chronically Ill and The Older PersonAnne Con100% (1)
- Tammy, 2011. Drug Interaction PDFDocument14 pagesTammy, 2011. Drug Interaction PDFdyahNo ratings yet
- Design Consideration in Reducing Stress in RPDDocument11 pagesDesign Consideration in Reducing Stress in RPDAnkit NarolaNo ratings yet
- Haad Exam 7Document22 pagesHaad Exam 7MallikarjunNo ratings yet
- Analysis of Synthetic CannabinoidsDocument13 pagesAnalysis of Synthetic CannabinoidsLuděk SpurnýNo ratings yet
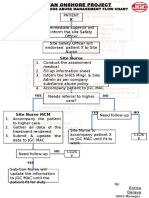
- Alcohol and Drug Abuse Flow ChartDocument1 pageAlcohol and Drug Abuse Flow Chartboen jaymeNo ratings yet
- Supraventricular TachycardiaDocument5 pagesSupraventricular TachycardialjubodragNo ratings yet
- Milieu TherapyDocument2 pagesMilieu Therapysivagiri.pNo ratings yet
- Carmin WentworthDocument4 pagesCarmin Wentworthapi-356549360No ratings yet
- MEDIWAYSDocument79 pagesMEDIWAYSRaj KumarNo ratings yet
- Kleihauer TestDocument3 pagesKleihauer Testteo2211No ratings yet
- Double Burden of Malnutrition 2017Document31 pagesDouble Burden of Malnutrition 2017Gîrneţ AlinaNo ratings yet
- 14 WartsprotocolDocument9 pages14 WartsprotocolLakshmi Deepak INo ratings yet
- CNS Stimulants 2010Document38 pagesCNS Stimulants 2010Neal KirkNo ratings yet