Professional Documents
Culture Documents
Ann Oncol-2013-Montemurro-annonc - mdt287 PDF
Uploaded by
Jayjay Amburadul BuangetOriginal Description:
Original Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Ann Oncol-2013-Montemurro-annonc - mdt287 PDF
Uploaded by
Jayjay Amburadul BuangetCopyright:
Available Formats
Human epidermal growth factor receptor
2 (HER2)-positive and hormone receptor-positive
breast cancer: newinsights into molecular
interactions and clinical implications
F. Montemurro
1
*
, S. Di Cosimo
2
,
& G. Arpino
3
,
1
Unit of Investigative Clinical Oncology (INCO) and Division of Medical Oncology, Piedmont Oncology Foundation/Institute for Cancer Research and Treatment,
Candiolo;
2
Department of Medical Oncology, Fondazione IRCCS Istituto Nazionale dei Tumori, Milan;
3
Department of Clinical Medicine and Surgery,
Federico II University, Naples, Italy
Received 25 November 2012; revised 15 May 2013 and 25 June 2013; accepted 26 June 2013
Recent data showa signicant benet from combining an anti-HER-2 agent with endocrine therapy in HER2-positive and
hormone receptor (HR)-positive metastatic breast cancer. However, as the clinical outcomes achieved by these
combinations do not favourably match those with chemotherapy, clinicians still perceive HER2-positive breast cancer as
an homogeneous group and consider chemotherapy with anti-HER2 agents as the preferred treatment option,
regardless of the HR status. Indeed, in HR-positive HER2-positive tumours, chemotherapy with anti-HER2 agents is the
backbone of treatment, while endocrine therapy is commonly used in sequence when HR and HER2 are co-expressed
rather than as a real alternative. Emerging biological and clinical data challenge this paradigm, suggesting that HER2-
positive tumours are rather heterogeneous that HRs co-expression may account for part of this heterogeneity and, nally,
that chemotherapy may represent an overtreatment in selected cases. The present reviewaims to summarise the
biological features of HER2-positive breast cancer according to HR status, the role of the bi-directional cross-talk
between HER2 and HR pathways on resistance development to anti-HER2 and endocrine therapy, and nally, the novel
therapeutic strategies, including but not limited to chemotherapy, targeting these two pathways.
Key words: breast cancer, cancer metastasis, drug therapy, her2/neu, hormone receptors, resistance
introduction
Amplication and/or overexpression of the human epidermal
growth factor 2 (HER2) oncogene, which belongs to the
epidermal growth factor receptor (EGFR/HER) family, occurs in
about 15% of invasive breast cancers, and enables constitutive
activation of growth factor signalling and triggering breast
cancer cell survival, proliferation, and invasion [1, 2]. Tumours
with HER2 amplication and/or overexpressionherein after
HER2-positive breast cancerare characterised by poor clinical
prognostic features, which translate into aggressive tumour
behaviour [1] and, importantly, by experimental and clinical
resistance to endocrine therapy. Current treatment of patients
with HER2-positive disease is primarily represented by
chemotherapy combined with HER2-targeted therapy, both in
the adjuvant and in the metastatic setting [36]. This approach
has dramatically changed the natural history of HER2-positive
breast cancer and is often suggested as a rst line option of
choice for patients with metastatic disease [7].
Recent studies suggest that HER-2 positive breast cancer is
biologically and clinically heterogeneous. Analysis on 169
HER2-positive early breast cancer by the 70-gene MammaPrint
signature reported that the 22% of cases were classied as
having good prognosis, with a 10-year distant disease-free
survival (DFS) of 84%, even in the absence of (neo)adjuvant
therapy with trastuzumab and chemotherapy. Of note, the
distant DFS for HER2-positive breast cancer patients classied
as having a poor prognosis signature was 55% [8]. Therefore, a
minority of patients with HER2-positive breast cancer patients
present an excellent prognosis even in the absence of treatment.
Hormone receptor co-expression may partially account for such
heterogeneity. For example recent data from neoadiuvant
studies suggest that response to therapy with anti-HER2 agents
largely depends on HR status [9, 10].
The present review explores the biological features and
clinical behaviour of HER2-positive breast cancer according to
HR status, describes the bi-directional cross-talk between HER2
and HR pathways and its implication on resistance development
These authors equally contributed to the work.
*Correspondence to: Dr Filippo Montemurro, Unit of Investigative Clinical Oncology
(INCO) and Division of Medical Oncology, Piedmont Oncology Foundation/Institute for
Cancer Research and Treatment, Strada Provinciale 142, Km 3.95-10060 Candiolo, Italy.
Tel: +39-011-9933250; Fax: +39-011-9933275; E-mail: lippo.montemurro@ircc.it
r
e
v
i
e
w
review
Annals of Oncology 00: 110, 2013
doi:10.1093/annonc/mdt287
The Author 2013. Published by Oxford University Press on behalf of the European Society for Medical Oncology.
All rights reserved. For permissions, please email: journals.permissions@oup.com.
Annals of Oncology Advance Access published August 1, 2013
b
y
g
u
e
s
t
o
n
N
o
v
e
m
b
e
r
1
3
,
2
0
1
3
h
t
t
p
:
/
/
a
n
n
o
n
c
.
o
x
f
o
r
d
j
o
u
r
n
a
l
s
.
o
r
g
/
D
o
w
n
l
o
a
d
e
d
f
r
o
m
to anti-HER2 agents and endocrine therapy, and illustrates the
novel therapeutic strategies, including but not limited to
chemotherapy, employable in the HER2-positive and HR-
positive breast cancer patients.
immunohistochemical and genetic
subtyping of HER2-positive and
HR-positive tumours
While about 10% of estrogen receptor (ER)-positive tumours
reveal HER2 overexpression, among the subgroup revealing
HER2 amplication and/or overexpression, about half are ER
positive. ER-positive tumours overexpressing HER2 in general
express ER at a lower level compared with ER-positive tumours
of the luminal A class [11]. Of note, in HER2-positive tumours,
ER and HER2 levels are inversely correlated at both the RNA
and the protein levels [12, 13].
A number of published reports consistently indicate that
HER2-positive breast cancers show different clinical
characteristics and prognosis according to the IHC status of
HRs [1416]. For example HR co-expression seems to mitigate
adverse prognosis in HER2-positive operable breast cancer
patients. More recently, data with the PAM50 demonstrated that
up to one-third of HER-positive early breast cancer may be
intrinsically classied as luminal A or B. Of note, the HER2-
enriched subtype according to PAM 50 signature predominates
in HER2-positive and ER-negative cases (35%51%) and
predicts response to neoadjuvant trastuzumab-based
chemotherapy [17, 18].
An additional evidence that HER2-positive tumours
heterogeneity is related to the HR co-expression came from a
study integrating DNA copy number arrays, DNA methylation,
exome sequencing, messenger RNA arrays, micro RNA
sequencing and reverse-phase protein [19]. In particular, a
HER2-enriched mRNA (HER2E-mRNA) subtype/HER2-
positive group was characterised by increased expression of
tyrosine kinase (TK) receptors FGFR4, EGFR, HER2 itself
together with genes within the HER2 amplicon (i.e. GRB7). A
second group, called luminal-mRNA subtype/HER2-positive,
enriched in HR-positive tumours, showed a higher expression of
luminal genes like GATA3, BCL2 and ESR1. These two groups
presented also distinct recurrent somatic mutations and protein
expression patterns. Further studies are warranted to
prospectively conrm these ndings. Collection and analyses of
tumour tissue are also needed to dissect the role of ER pathway
in HER2 signalling and vice-versa and to identify novel
predictive biomarkers and more targeted therapeutic strategies.
differential sensitivity of HER2-positive
tumours to combinations of
chemotherapy and HER2-targeting
agents according to HR status
Since the pivotal trial published by Slamon et al., the therapeutic
platform of chemotherapy combined with HER2-targeting has
undergone a constant development through randomised trials
in the metastatic setting. Table 1 summarises the details of most
of the inuential clinical studies in the rst-line setting (details
of each trial are reported in the supplementary Appendix,
available at Annals of Oncology online). Chemotherapy and
anti-HER2 agents combination is often considered a preferred
rst-line option for most patients with HER2-positive disease
[7], regardless of HR status, based on the following evidence: (i)
retrospective analyses of patients treated in the pre-trastuzumab
era showed that, overall, HER2-positive tumours are more
chemo-sensitive than their HER2-negative counterparts,
especially when anthracycline-containing regimens are used;
[20] (ii) as single agents, both trastuzumab and lapatinb are
modestly active; [2125] (iii) pre-clinical studies have suggested
synergistic effects between trastuzumab and agents such as
paclitaxel, docetaxel, vinorelbine and platinoids; [26] and (iv)
the pivotal trial [3] and a myriad of phase II studies, including
one inuential randomised trial, [4] conrmed the cooperative
effects of chemotherapy and trastuzumab, resulting in
impressive gains in response rates (RRs), progression-free
survival (PFS) and OS.
Newer regimens with double HER2 targeting, such as the
one used in the experimental arm of the Clinical Evaluation of
Pertuzumab and Trastuzumab (CLEOPATRA) study, have
established a newer efcacy benchmark for future
developments [27].
The chemotherapy plus HER-targeting paradigm has been
translated into the management of patients with operable breast
cancer, where all randomised studies have been designed to
include this monoclonal antibody in conjunction with
chemotherapy, for treatment, again regardless of the HR status
[6, 28, 29].
However, the biological heterogeneity of HER2-positive
tumours according to HR status may have potential therapeutic
implications. A correlation between hormone-receptor levels
and endocrine responsiveness/reduced chemosensitivity is
already recognised in HER2-negative tumours [30, 31], where
increased ER and PR are associated with endocrine
responsiveness and reduced chemosensitivity and, therefore, has
therapeutic implications [32]. A recently published analysis in
patients with HER2-positive metastatic tumours, treated with
chemotherapy and trastuzumab showed that ER expression in
more than 30% of cancer cells was associated with a
signicantly lower RR to treatment, compared with the RR
observed in tumours with lower or absent ER expression [33].
However, regardless of RR, PFS of patients with ER-positive
tumours was signicantly improved when maintenance
endocrine therapy was added to trastuzumab treatment. These
results suggest that RRs with chemotherapy and trastuzumab
may be lower than those summarised in Table 1 in HER2-
positive tumours expressing high ER levels and that HER2-
inhibition may overcome the de novo endocrine resistance of
these tumours.
Data from recent neoadjuvant trials further support the
hypothesis that, in HER2-positive tumours, the HR status
inuences response to anti-HER2-based therapy. Table 2
summarises the results of three of these trials where for the rst
time the pathological complete remission rate ( pCR), a
recognised surrogate of good clinical outcome [34], were
reported according to hormone-receptor status. The
Neoadjuvant Lapatinib and/or Trastuzumab Treatment
Optimization (NEO-ALLTO) and the Neoadjuvant Study of
review
Annals of Oncology
i | Montemurro et al.
b
y
g
u
e
s
t
o
n
N
o
v
e
m
b
e
r
1
3
,
2
0
1
3
h
t
t
p
:
/
/
a
n
n
o
n
c
.
o
x
f
o
r
d
j
o
u
r
n
a
l
s
.
o
r
g
/
D
o
w
n
l
o
a
d
e
d
f
r
o
m
Pertuzumab and Herceptin in an Early Regimen Evaluation
(NEOSPHERE) trials were designed to deliver a short pre-
surgical treatment, followed by post-surgical adjuvant
chemotherapy and anti-HER2 therapy. In the German
Preoperative Adriamycin and Docetaxel (GEPAR) QUINTO
study, a full sequential anthracycline and taxane-based
chemotherapy regimen was delivered before surgery, and
trastuzumab was started concurrently with pre-operative
chemotherapy and continued after surgery to complete a year of
targeted therapy. Chemotherapy was part of the neoadjuvant
programme in all trials, with the exception of one arm of the
NEOSPHERE trial, where the association of trastuzumab and
Table 2. Rate of pathological complete response (pCR) and hormone receptor (HR) status in neo-adjuvant studies with anti-HER2 agents
Study No. of patients Regimen
a
anti-HER2 agent
a
Overall pCR
rate (%)
pCR rate according to
HR (%)
HR pos HR neg
GEPARQUINTO [87] 620 EC-Docetaxel Trastuzumab 30.3 25.8 38.7
Lapatinib 22.7 16.2 28.3
NEO-ALTTO [9] 455 Paclitaxel Trastuzumab 29.5 22.7 37.5
Lapatinib 24.7 16.1 33.7
Trastuzumab + Lapatinib 51.3 41.6 61.3
NEOSPHERE [10] 417 Docetaxel Trastuzumab 29.0 20 36.8
Pertuzumab 24.0 17.4 30
Pertuzumab + Trastuzumab 45.8 26 63.2
None Pertuzumab + Trastuzumab 16.8 5.9 29.1
a
See supplementary Appendix, available at Annals of Oncology online for details of treatments and schedule used in these studies.
pCR, pathological complete remission according to the denition given by each author for the main analysis; HR, hormone receptor; GEPAR, German
Preoperative Adriamycin and Docetaxel; NEO-ALTTO, Neoadjuvant Lapatinib and/or Trastuzumab Treatment Optimization; NEOSPHERE, Neoadjuvant
Study of Pertuzumab and Herceptin in an Early Regimen Evaluation.
Table 1. Phase III trials comparing chemotherapy HER2 targeting agents or different treatment combinations of chemotherapy and HER2 targeting agents
Study Design Treatment
a
N ORR
(%)
PFS or TTP
(months)
OS
H0648g [3] Randomised phase III, rst-line MBC Chemotherapy 234 32 4.6 20.3
Chemotherapy + Trastuzumab 235 50* 7.4* 25.1*
M7701 [4] Randomised phase II, rst-line MBC Docetaxel 94 34 6.1 22.7
Docetaxel + Trastuzumab 92 61* 11.7* 31.2*
CHAT [80] Randomised phase II, rst-line MNC Doxetaxel + Trastuzumab 110 72.7 12.8 NR
Docetaxel + Trastuzumab + Capecitabine 112 70.5 17.9*
BCIRG 007 [81] Randomised phase III, rst-line MBC Docetaxel + Trastuzumab 131 72 11.0 37.1
Docetaxel + Trastuzumab + Carboplatin 132 72 10.4 37.4
US Oncology [82] Randomised phase III, rst-line MBC Paclitaxel + Trastuzumab 98 36 7.1 32.2
Paclitaxel + Trastuzumab + Carboplatin 98 52 10.7* 35.7
HERNATA [83] Randomised phase III, rst-line
LABC or MBC
Docetaxel + Trastuzumab 143 59.9 12.4 35.7
Docetaxel + Vinorelbine 141 59.9 15.3 38.8
CLEOPATRA [27] Randomised phase III, rst line Docetaxel + Trastuzumab + Placebo 406 69.3 12.4 N.R**
Docetaxel + Trastuzumab + Pertuzumab 402 80.2* 18.5*
EGF30001 [84] Unplanned subgroup analysis of randomised
phase III trial, rst-line LABC or MBC
Paclitaxel + Placebo 37 37.8 6.3 20.6
Paclitaxel + Lapatinib 49 63.3 9.1* 26.2
EGF104535 [85] Randomised phase III trial, rst-line MBC Paclitaxel + Placebo 222 50 6.5 20.5
Paclitaxel + Lapatinib 222 69* 9.7* 27.8
TDM4450g [86] Randomised phase II trial, rst-line MBC Docetaxel + Trastuzumab 70 58 9.2 30
TDM1 67 64.2 14.2* N.R.**
*The difference was statistically signicant at the P < 0.05 level.
**The hazard ratio for overall survival was 0.64 favouring the combined arm (P = 0.005).
a
See supplementary Appendix, available at Annals of Oncology online for details of treatments and schedule used in these studies.
MBC, metastatic breast cancer; LABC, locally advanced breast cancer; ORR, overall response rate (complete + partial remission); CBR, clinical benet rate
(complete + partial remission and disease stabilisation lasting 6 months or longer); PFS, progression-free survival; TTP, time to progression; OS, overall
survival; N.R., not reached; CHAT, Capecitabine, Herceptin And Taxotere; BCIRG, breast cancer international research group; HERNATA, HERceptin plus
NAvelbine or TAxotere; CLEOPATRA, CLinical Evaluation Of Pertuzumab And TRAstuzumab.
Annals of Oncology
review
doi:10.1093/annonc/mdt287 |
b
y
g
u
e
s
t
o
n
N
o
v
e
m
b
e
r
1
3
,
2
0
1
3
h
t
t
p
:
/
/
a
n
n
o
n
c
.
o
x
f
o
r
d
j
o
u
r
n
a
l
s
.
o
r
g
/
D
o
w
n
l
o
a
d
e
d
f
r
o
m
pertuzumab was delivered pre-operatively without
chemotherapy. The NEO-ALTTO and the NEOSPHERE trials
included arms with combinations of HER2-targeting agents,
whereas the GEPARQUINTO trial compared lapatinib with
trastuzumab. Despite differences in the denition of the primary
end point, the neoadjuvant studies with trastuzumab lapatinib
and trastuzumab pertuzumab reported pCR rates ranging
from 22.7% to 30% when a single HER2-targeting agent was
given in addition to chemotherapy. The pCR rates increased to
between 45.8% and 51.3%, respectively, when pertuzumab and
lapatinib were added to trastuzumab and chemotherapy. The
NEOSPHERE study reported a pCR rate of 16.8% in the arm
with trastuzumab and pertuzumab without chemotherapy. This
nding is remarkable as it suggests that a subgroup exists for
whom anti-HER2 therapy alone may offer signicant efcacy
without the addition of chemotherapy.
Importantly, all the studies consistently showed that pCR
rates to neoadjuvant therapy were signicantly lower in ER-
positive compared with ER-negative tumours (Table 2). This
also occurred in the chemotherapy-free arm of the
NEOSPHERE trial, where treatment led to disease eradication
in about one-third of ER-negative tumours, compared with just
6% in their ER-positive counterparts. A similar observation was
made in a small study exploring the activity of exclusive dual
blockade therapy with lapatinib and trastuzumab in the
neoadjuvant setting [35]. This Translational Breast Cancer
Research Council (TBCRC) 006 trial reported an overall pCR
rate of 42% after 12 weeks of therapy in HER2-positive/ER-
negative operable and/or locally advanced breast cancer.
Interestingly, in patients with HER2-positive/ER-positive
disease, letrozole was added to lapatinib and trastuzumab,
resulting in a pCR rate of 21%. This pCR rate favourably
compares with that observed in the subset of HER2-positive/
ER-positive tumours treated in the trastuzumab/pertuzumab
arm of the NEOSPHERE trial. While this may result as being
just an additive effect, the hypothesis that endocrine therapy
may partially restore sensitivity to HER2-targeting is intriguing
and deserves further study.
Lack of long-term survival data suggests that results of
neoadjuvant trials should not impact on the way that early,
HER2-positive breast cancer is currently treated. However, the
rate of tumour response from neoadjuvant studies foster the use
of HER2-targeted therapy in combination with endocrine
therapy for advanced breast cancer patients with tumours that
co-express high-levels of HRs.
differential sensitivity of HR-positive
tumours to endocrine-therapy according
to HER2 status
In ER-positive early breast cancer, endocrine treatment reduces
the recurrence and mortality rates, regardless of the use of
chemotherapy [36]. Clinical data suggest that overexpression of
HER2 and the lesser-studied EGFR is associated with a poorer
outcome in breast cancer patients treated with endocrine
therapy [3742]. However, data are not denitive as while some
studies indicated no benet or even a potentially detrimental
effect of tamoxifen on outcomes in women with HER2-positive/
HR positive tumours, [39, 40], other studies failed to show such
effect [41, 42].
Neoadjuvant trials provide a unique platform to correlate
molecular determinants of response and resistance with the
clinical response of primary breast cancer to medical therapy.
Results in this setting show more consistently that HER2 and, to
a lesser extent, EGFR may act as mediators of resistance to
tamoxifen. In women with locally advanced, HR-positive breast
cancer randomised to neoadjuvant treatment with tamoxifen or
with the aromatase inhibitor (AI) letrozole [43], letrozole
signicantly increased RR compared with tamoxifen. However,
differences in RRs between the two drugs were most marked for
ER-positive and EGFR and/or HER2-positive tumours,
suggesting that the growth-promoting effects of these growth
factor receptors on ER-positive breast cancer can be most
effectively inhibited by potent estrogen deprivation therapy.
Dowsett et al. analysed changes in tumour proliferation
occurring in patients randomised to another AI, anastrozole,
tamoxifen or the combination of the two agents given for 3
months before surgery [44]. Similarly to the previously
described trial, the superiority of anastrozole over tamoxifen in
terms of RR was mostly observed in HER2-positive/HR-positive
tumours. Intriguingly, after 2 weeks of treatment, tamoxifen was
less effective than anastrozole in suppressing proliferation in
HER2-positive tumours compared with HER2-negative
tumours. Among patients receiving anastrozole at the end of 12
weeks of treatment, those with HER2-positive tumours showed
a signicantly lower degree of proliferation suppression than
their HER2-negative counterparts as, after an initial response,
resistance to AIs depending on HER2 signalling may rapidly
emerge. A recent follow-up of the study by Ellis et al. also
supports the idea that in HER2-positive/HR-positive tumours,
there is an estrogen-independent signalling mechanism that
leads to increased proliferation [45].
A retrospective analyses of the Arimidex, Tamoxifen, Alone
or in Combination (ATAC) and the Breast International Group
(BIG) 1 studies, two large randomised trials of adjuvant
endocrine therapy [46, 47], failed to demonstrate any
interaction between type of endocrine therapy and HER2 status
on long-term efcacy outcomes. Indeed, AIs were found to be
more effective than tamoxifen in the overall patient population,
regardless of the HER2 status. Importantly, HER2-positivity
predicted a worse clinical outcome regardless of treatment type,
conrming its role as a marker of resistance to endocrine
manipulation in general.
HR and HER bi-directional cross-talk:
implications on the development of
resistance to endocrine therapy and
anti-HER agents
Based on the above, clinically dened HER2-positive subtype of
breast cancer is not clinically and biologically homogenous.
There is increasing evidence that the ER and HER2 pathways
cross-talk and thereby synergise in tumour progression. The
following paragraphs summarise molecular evidence of such bi-
directional cross-talk and its role in differential sensitivity to
therapies.
review
Annals of Oncology
| Montemurro et al.
b
y
g
u
e
s
t
o
n
N
o
v
e
m
b
e
r
1
3
,
2
0
1
3
h
t
t
p
:
/
/
a
n
n
o
n
c
.
o
x
f
o
r
d
j
o
u
r
n
a
l
s
.
o
r
g
/
D
o
w
n
l
o
a
d
e
d
f
r
o
m
HER /ERcross-talk as a mechanism
for resistance to endocrine therapy
Aberrant signalling through the growth factor receptors
pathway has long been identied as a mediator of resistance to
endocrine manipulation in HR-positive cancer cells [48].
Clinical and laboratory evidence support a critical role for the
cross-talk between the ER and HER2 signalling pathways in
resistance to endocrine therapy [20], especially when both the
receptors are co-expressed. Mechanisms of ER signalling in
breast cancer are described in Figure 1. Estrogens, by activation
of the ER nuclear function, can increase transcription and
expression of ligands such as transforming growth factor-
(TGF) and insulin-like growth factor 1 (IGF1) [4951], that, in
turn, can trigger the growth factor receptor pathway [50, 52].
Activation of the PI3K/AKT and the p42/44 MAPK pathways
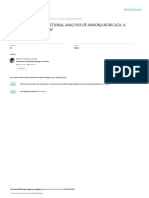
Figure 1. Mechanisms of estrogen receptor (ER) action in breast cancer. Three distinct pathways of ER regulation of gene expression are shown. First, in
classic estrogen signalling, ligand-bound ER activates gene expressioneither through direct binding of dimeric ER to specic DNA response elements,
estrogen receptor elements (EREs), in complexes that include co-activators (CoA) and histone acetyl transferases (HAT), or through proteinprotein
interactions with other transcription factors, particularly members of the activation protein 1 (Ap1) and specicity protein 1 (Sp1) familiesto facilitate
binding to serum response elements (SRE) and activation of gene transcription including genes encoding for growth factors (GFs) and receptor tyrosine
kinases (RTKs) (A). Secondly, ER can also be activated as a consequence of signalling events downstream of receptor tyrosine kinases (RTKs) such as the
epidermal growth factor receptor (EGFR), ERBB2 (also known as HER2) and the insulin-like growth factor receptor (IGFR). Phosphorylation (P) of
transcription factors (TFs) and coregulators, including components of the ER pathway that enhance gene expression on Estrogen response elements (EREs)
and other response elements (REs) by the Erk or Akt serine/threonine kinases leads to ligand-independent activation of the ER (B). Thirdly, signalling can be
mediated through non-genomic mechanisms by ER that is localised at the cell membrane or in the cytoplasm (C). Ligand binding induces the assembly of
functional protein complexes that involve other signalling molecules and that activate intracellular signalling cascades, resulting in TF activation. However, the
clinical role of membrane ER needs further investigation as its incidence in human breast cancer is very low.
Annals of Oncology
review
doi:10.1093/annonc/mdt287 | ,
b
y
g
u
e
s
t
o
n
N
o
v
e
m
b
e
r
1
3
,
2
0
1
3
h
t
t
p
:
/
/
a
n
n
o
n
c
.
o
x
f
o
r
d
j
o
u
r
n
a
l
s
.
o
r
g
/
D
o
w
n
l
o
a
d
e
d
f
r
o
m
by these receptors, may subsequently result in phosphorylation
of ER and its co-activator such as AIB1, thus leading to
enhancement of genomic ER activities, even in the absence of its
ligand, or in the presence of selective ER modulators (SERMs)
such as tamoxifen [52, 53]. Phosphorylation of co-repressors,
on the other hand, can result in their export from the nucleus,
thereby preventing regulation of ER transcriptional complexes
in the nucleus [54, 55]. Down-regulation of ER and PgR
expression has been demonstrated to occur as a result of HER-
mediated activation of the PI3K/AKT and the p42/44 MAPK
pathways [56, 57]. Thus, while receptor tyrosine kinases can
activate the transcriptional function of the ER, they can also
reduce estrogen dependence by down-regulating the expression
of the ER or estrogen-related genes, such as the PgR. This could
possibly contribute to the relative resistance to endocrine
therapies in tumours harbouring abnormalities in HER
receptors members.
Hurtado et al. [34] have recently shown that estrogen-ER and
tamoxifen-ER complexes directly repress HER2 transcription.
The Paired Box 2 transcription factor (PAX2) seems to be the
mediator of this cross-talk and its loss or deregulation causes
tamoxifen resistance by the acquisition of a HER2-driven
phenotype in the ER-positive luminal cells.
In addition to genomic signalling [58], in breast cancer
culture models, the membrane (nonnuclear) ER, bound to
either oestradiol or tamoxifen [52, 55], by triggering EGFR,
HER2, and IGFR1 [59] and their downstream pathways [60],
ultimately contribute to tamoxifen resistance development by
increasing nuclear ER gene transcription [61]. However, the
average incidence of cytoplasmic ER in nearly 3200 cases of
breast cancer was only 1.5%, strongly suggesting that its
measurement is unlikely to be of routine clinical value at the
present [62].
The following laboratory evidences suggest that inhibition of
HER pathways may delay endocrine resistance onset and that
the dual inhibition of both HER2 and ER pathways may exert
optimal antitumour activity in HR and HER2-positive breast
cancer.
In a xenograft model using MCF7 human breast cancer cells
stably transfected with HER2 (MCF7/HER2-18) [63], the
selective HER1 tyrosine kinase inhibitor getinib transiently
slowed tumour growth. However, further studies have shown
that complete inhibition of the HER pathway and its multiple
potential homo- and heterodimer pairs by combining several
anti-HER inhibitors, such as pertuzumab (a HER2-specic
monoclonal antibody that inhibits heterodimerization with
other HER members), trastuzumab and getinib, or
trastuzumab and lapatinib (a dual EGFR and HER2 TK
inhibitor) is needed to achieve the best activity in HER2-
positive/ER-positive breast tumour cells [64, 65]. Importantly,
these potent anti-HER combinations were only modestly
effective when implemented in the absence of concomitant
endocrine therapy as, in such tumours, both ER and HER2
appear to drive tumour cell survival, and both pathways should
be blocked for optimal outcome. These molecular ndings have
provided the rationale for clinical studies of endocrine therapy
and HER2-targeting agents in an attempt to block growth
factor signalling pathways and restore endocrine responsiveness
[64, 66, 67].
HER2/ERcross-talk as a mechanismfor
resistance to HER2-targeted agents
Resistance to HER2-targeting has been intensively investigated
in the last decade [68]. Until recently, there has been little
recognition of the fact that up-regulation of ER expression and/
or activity can function as an escape mechanism leading to
resistance to HER2-targeted therapy in HER2 and HR-positive
breast cancer patients. Preclinical studies show that in ER and
HER2-positive breast cancer cell lines initially sensitive to
lapatinib, enhanced ER signalling is evident upon acquisition of
resistance to lapatinib and that this resistance may be prevented
by the simultaneous inhibition of HER2 and ER signalling [69,
70]. Intriguingly, increased ER activity was also conrmed in
patients with HER2 and ER-positive metastatic breast cancers
progressing to lapatinib monotherapy [70]. An analogous
phenomenon was also documented in chronically trastuzumab
exposed patients, whose tumours revealed up-regulation of the
ER [71].
To further elucidate the potential role of the ER in the onset
of resistance to anti-HER2-targeted therapies, Wang et al.
studied different HER2-positive human breast cancer cell lines
with de novo or acquired resistance to trastuzumab, lapatinib, or
lapatinib plus trastuzumab [72]. Authors found that with
sustained HER2 inhibition, the ER functions as a key escape/
survival pathway in HER2-positive/ER-positive cells and that a
dynamic transition between HER2 and ER activity plays a role
in resistance to lapatinib-containing regimens. Thus, in HER2-
positive/ER-positive breast cancer cells, either the ER or HER2
can initially function as the major promoter of proliferation and
survival. Eventually, however, with sustained, effective HER2
inhibition using lapatinib or lapatinib + trastuzumab, the ER
becomes the primary controller of cell survival, resulting in
resistance to lapatinib, or lapatinib + trastuzumab therapy.
Findings from these studies underline the importance of dual
inhibition of both HER2 and ER to achieve the best antitumour
activity in ER-positive HER2-positive breast cancer and, if
further conrmed in the clinical setting, will provide a strong
rationale to optimise biologically targeted therapies, in selected
breast cancer patients, by completely blocking the HER
network, in conjunction with ER inhibition.
novel strategies to optimise treatment
in HER2-positive/HR-positive breast
tumours
A logical therapeutic approach in these HER2 positive and HR-
positive breast cancer is to combine target therapies to block
both ER and HER2 pathways. This hypothesis was explored in
three trials conducted in patients with locally advanced and/or
metastatic breast cancer (Table 3) [7376]. While the
Trastuzumab and Anastrozole Directed Against ER-Positive
HER2-Positive Mammary Carcinoma (TanDEM) and the
Efcacy and Safety of Letrozole Combined With Trastuzumab
in Patients With Metastatic Breast Cancer (eLEcTRA) studies
were phase III randomised trials conducted in HER2-positive/
ER-positive breast cancer patients, the EGF30008 study was
conducted in 1286 women with HR-positive breast cancer
review
Annals of Oncology
o | Montemurro et al.
b
y
g
u
e
s
t
o
n
N
o
v
e
m
b
e
r
1
3
,
2
0
1
3
h
t
t
p
:
/
/
a
n
n
o
n
c
.
o
x
f
o
r
d
j
o
u
r
n
a
l
s
.
o
r
g
/
D
o
w
n
l
o
a
d
e
d
f
r
o
m
patients not selected on the basis of their HER2 status [74].
Almost 17% of the patients had centrally conrmed HER2-
positive disease and were analysed separately as planned [75].
The three trials provided consistent results, indicating that the
combination of an anti-HER2 agent and an AI signicantly
improved RR, clinical benet rate (CBR) and PFS, compared
with endocrine therapy alone. No signicant difference on OS
estimates was observed in any of the trials, possibly due to the
inuence of crossover, the lines of treatment after progression
and to the number of events at the time of the analysis for the
primary end point PFS, when 47% and 58% of death had
occurred in the EGF30008 and TANDEM, respectively. These
trials provided a strong proof-of-concept for these
chemotherapy-free therapeutic options. However, the
complexity and redundancy of the HER network may require
more complete inhibition of the HER family receptors by
combining different anti HER2 agents with endocrine therapy
to further optimise clinical efcacy, an option currently tested in
ongoing clinical trials.
The combination of endocrine therapy and trastuzumab or
lapatinib is today an available rst-line therapeutic option in
patients with HER2-positive/HR-positive metastatic tumours
[77]. However, the comparison of RRs and PFS results between
the trials summarised in Tables 1 and 2, is a recurring argument
in favour of the use of chemotherapy-based combinations in
HER2-positive, metastatic breast cancer patients [7]. In fact, a
recent survey conducted in the United States shows that about
70% of these patients receive chemotherapy as part of rst line
treatment, with only about 10% receiving endocrine therapy and
trastuzumab [78]. Interestingly, though, about a half of patients
receiving rst-line chemotherapy and trastuzumab also received
and endocrine agent either concomitantly with chemotherapy
or added sequentially as a form of maintenance therapy.
conclusions
In the clinical practice, there is increasing recognition that
HER2-positive breast cancer patients are not a homogeneous
group. In particular, the HR status is emerging as a relevant
stratication factor with practical clinical implications. Data
from neoadjuvant studies show that HR status account for
different sensitivity to treatments. Molecular analysis provides
potential explanations for this effect, indicating that the HER
and ER pathways are strictly related in a bi-directional way.
HER2 signalling causes endocrine resistance and ER modulate
the response not only to chemotherapy, but also to HER2
targeted agents. Finally, clinical trials have conrmed the
preclinical rationale of combining endocrine therapy and anti
HER2-agents to interfere with this cross-talk.
Two important points to discuss are (i) where combinations
of endocrine agents and HER2-targeting agents can be currently
considered a reasonable rst-line option for HER2-positive/
hormone-receptor positive metastatic breast cancer patients; (ii)
what are the possible future developments of this therapeutic
approach. Given that response rates to chemotherapy plus
HER2-targeted therapy combinations typically exceed the 28%
reported for these combinations, such an approach cannot be
recommended in young patients or those with life-threatening
or symptomatic disease. However, understanding that no
treatment is curative in this setting, a therapeutic trial of this
generally well-tolerated strategy, could be considered in
postmenopausal patients with less extensive or asymptomatic
metastatic disease. Such an approach offers the possibility of
delaying initiation of a more toxic chemotherapy-based HER2-
targeted combination for 612 months, and occasionally longer.
In addition, despite lack of data from randomised trials, it seems
reasonable to offer patients maintenance endocrine therapy
with ongoing HER2 targeting once chemotherapy becomes too
toxic or its benets hit a plateau. The survey of patterns of care
published by Tripathy et al. [78] shows that these concepts are
being taken on by oncologists in the clinical practice.
We believe, however, that a real step forward would be
represented by the identication of factors other than clinical
features (i.e. age, performance status, pattern of disease) that
may dene patients where endocrine therapy combined with
HER2-targeting agents may be an elective rather than a
reasonable, option. For example high-hormone receptor
expression [33] or belonging to a luminal, rather than pure-
HER2 intrinsic subtype may represent biomarkers of reduced
efcacy of chemotherapy [79]. Patients whose tumours show
Table 3. Summary of randomised trials evaluating the addition of HER2 targeting agents to rst-line endocrine therapy with aromatase inhibitors in HER2-
positive and hormone receptor-positive breast cancer patients
Study Design Treatment
a
N ORR
(%)
CBR
(%)
PFS
(months)
OS
TANDEM [73] Randomised phase III trial, rst-line MBC Anastrozole 104 6.8 27.9 2.4 23.9
Anastrozole + Trastuzumab 103 20.3* 42.7* 4.8* 28.5
EGF30008 [75] Pre-planned subgroup analysis of a larger
randomised phase III trial, rst-line LABC or MBC
Letrozole + Placebo 108 15 29 3 32.3
Letrozole + Lapatinib 111 28* 48* 8.2* 33.3
eLEcTRA [76] Randomised phase III, closed prematurely because of
slow accrual, rst-line MBC
Letrozole 31 13 39 3.3 NR
Letrozole + Trastuzumab 26 27 65 14.1 NR
*The difference was statistically signicant at the P < 0.05 level.
a
See supplementary Appendix, available at Annals of Oncology online for details of treatments and schedule used in these studies.
TAnDEM, Trastuzumab and Anastrozole Directed Against ER-Positive HER2-Positive Mammary Carcinoma; eLEcTRA, Study of the Efcacy and Safety of
Letrozole Combined With Trastuzumab in Patients With Metastatic Breast Cancer; MBC, metastatic breast cancer; LABC, locally advanced breast cancer; ORR,
overall response rate (complete + partial remission); CBR, clinical benet rate (complete + partial remission and disease stabilisation lasting 6 months or
longer); PFS, progression-free survival; OS, overall survival; NR, not reported.
Annals of Oncology
review
doi:10.1093/annonc/mdt287 | ,
b
y
g
u
e
s
t
o
n
N
o
v
e
m
b
e
r
1
3
,
2
0
1
3
h
t
t
p
:
/
/
a
n
n
o
n
c
.
o
x
f
o
r
d
j
o
u
r
n
a
l
s
.
o
r
g
/
D
o
w
n
l
o
a
d
e
d
f
r
o
m
these features are, in our opinion, the optimal candidates for
clinical trials assessing chemotherapy-free combinations.
Despite the tremendous challenges in the research of
biomarkers that could predict treatment efcacy, large tissue-
banks have been collected in the context of neoadjuvant
randomised trials. Hopefully, these efforts will provide
candidate biomarkers that may further dene personalised
treatment strategies patients with HER2-positive breast cancer.
acknowledgements
The authors are indebted to Stefano de Angelis and Carmine de
Angelis for their help in producing the artwork for Figure 1.
funding
This manuscript had no funding.
disclosure
FM and GA are members of the speakers bureau for Roche S.p.
A. and GlaxoSmithKline S.p.A. SDC is member of the speakers
bureau for GlaxoSmithKline S.p.A. and is a Consultant for
TEVA pharmaceuticals
references
1. Slamon DJ, Clark GM, Wong SG et al. Human breast cancer: correlation of relapse
and survival with amplication of the HER-2/neu oncogene. Science 1987; 235:
177182.
2. Citri A, Yarden Y. EGF-ERBB signalling: towards the systems level. Nat Rev Mol Cell
Biol 2006; 7: 505516.
3. Slamon DJ, Leyland-Jones B, Shak S et al. Use of chemotherapy plus a
monoclonal antibody against HER2 for metastatic breast cancer that overexpresses
HER2. N Engl J Med 2001; 344: 783792.
4. Marty M, Cognetti F, Maraninchi D et al. Randomized phase II trial of the efcacy
and safety of trastuzumab combined with docetaxel in patients with human
epidermal growth factor receptor 2-positive metastatic breast cancer administered
as rst-line treatment: the M77001 study group. J Clin Oncol 2005; 23:
42654274.
5. Piccart-Gebhart MJ, Procter M, Leyland-Jones B et al. Trastuzumab after adjuvant
chemotherapy in HER2-positive breast cancer. N Engl J Med 2005; 353:
16591672.
6. Slamon D, Eiermann W, Robert N et al. Adjuvant trastuzumab in HER2-positive
breast cancer. N Engl J Med 2011; 365: 12731283.
7. Cortes J, Saura C, Bellet M et al. HER2 and hormone receptor-positive breast
cancerblocking the right target. Nature Reviews Clinical Oncology 2011; 8:
307311.
8. Knauer M, Cardoso F, Wesseling J et al. Identication of a low-risk subgroup of
HER-2-positive breast cancer by the 70-gene prognosis signature. Br J Cancer
2010; 103: 17881793.
9. Baselga J, Bradbury I, Eidtmann H et al. Lapatinib with trastuzumab for HER2-
positive early breast cancer (NeoALTTO): a randomised, open-label, multicentre,
phase 3 trial. Lancet 2012; 379: 633640.
10. Gianni L, Pienkowski T, Im YH et al. Efcacy and safety of neoadjuvant pertuzumab
and trastuzumab in women with locally advanced, inammatory, or early HER2-
positive breast cancer (NeoSphere): a randomised multicentre, open-label, phase
2 trial. Lancet Oncol 2012; 13: 2532.
11. Lal P, Tan LK, Chen B. Correlation of HER-2 status with estrogen and progesterone
receptors and histologic features in 3,655 invasive breast carcinomas. Am J Clin
Pathol 2005; 123: 541546.
12. Konecny G, Pauletti G, Pegram M et al. Quantitative association between HER-2/
neu and steroid hormone receptors in hormone receptor-positive primary breast
cancer. J Natl Cancer Inst 2003; 95: 142153.
13. Pinhel I, Hills M, Drury S et al. ER and HER2 expression are positively correlated in
HER2 non-overexpressing breast cancer. Breast Cancer Res 2012; 14: R46.
14. Blows FM, Driver KE, Schmidt MK et al. Subtyping of breast cancer by
immunohistochemistry to investigate a relationship between subtype and short and
long term survival: a collaborative analysis of data for 10,159 cases from 12
studies. PLoS Medicine 2010; 7: e1000279.
15. Garcia Fernandez A, Gimenez N, Fraile M et al. Survival and clinicopathological
characteristics of breast cancer patient according to different tumour subtypes as
determined by hormone receptor and Her2 immunohistochemistry. A single
institution survey spanning 1998 to 2010. The Breast 2012; 21: 366373.
16. Parise CA, Bauer KR, Brown MM et al. Breast cancer subtypes as dened by the
estrogen receptor (ER), progesterone receptor (PR), and the human epidermal
growth factor receptor 2 (HER2) among women with invasive breast cancer in
California, 19992004. The Breast Journal 2009; 15: 593602.
17. Gomez Pardo P, Prat A, Bianchini G et al. PAM50 intrinsic subtyping and
pathologic responses to neoadjuvant trastuzumab-based chemotherapy in HER2-
positive breast cancer. J Clin Oncol (Meeting Abstracts) 2011; 29: (Abstr 554).
18. Cheang MCU, Prat A, Fan C et al. PAM50 HER2-enriched subtype enriches for
tumor response to neoadjuvant anthracyclines/taxane and trastuzumab/taxane
containing regimens in HER2-positive breast cancer. Cancer Res 2011; 71: (Abstr
S52).
19. TCGAT. Comprehensive molecular portraits of human breast tumours. Nature
2012; 490: 6170.
20. Gennari A, Sormani MP, Pronzato P et al. HER2 status and efcacy of adjuvant
anthracyclines in early breast cancer: a pooled analysis of randomized trials. J Natl
Cancer Inst 2008; 100: 1420.
21. Vogel CL, Cobleigh MA, Tripathy D et al. Efcacy and safety of trastuzumab as a
single agent in rst-line treatment of HER2-overexpressing metastatic breast
cancer. J Clin Oncol 2002; 20: 719726.
22. Baselga J, Carbonell X, Castaneda-Soto NJ et al. Phase II study of efcacy, safety,
and pharmacokinetics of trastuzumab monotherapy administered on a 3-weekly
schedule. J Clin Oncol 2005; 23: 21622171.
23. Gomez HL, Doval DC, Chavez MA et al. Efcacy and safety of lapatinib as rst-line
therapy for ErbB2-amplied locally advanced or metastatic breast cancer. J Clin
Oncol 2008; 26: 29993005.
24. Hamberg P, Bos MM, Braun HJ et al. Randomized phase II study comparing
efcacy and safety of combination-therapy trastuzumab and docetaxel vs.
sequential therapy of trastuzumab followed by docetaxel alone at progression as
rst-line chemotherapy in patients with HER2+ metastatic breast cancer: HERTAX
trial. Clin Breast Cancer 2011; 11: 103113.
25. Inoue K, Nakagami K, Mizutani M et al. Randomized phase III trial of trastuzumab
monotherapy followed by trastuzumab plus docetaxel versus trastuzumab plus
docetaxel as rst-line therapy in patients with HER2-positive metastatic breast
cancer: the JO17360 Trial Group. Breast Cancer Res Treat 2010; 119: 127136.
26. Pegram MD, Konecny GE, OCallaghan C et al. Rational combinations of
trastuzumab with chemotherapeutic drugs used in the treatment of breast cancer.
J Natl Cancer Inst 2004; 96: 739749.
27. Baselga J, Cortes J, Kim SB et al. Pertuzumab plus trastuzumab plus docetaxel for
metastatic breast cancer. N Engl J Med 2012; 366: 109119.
28. Untch M, Gelber RD, Jackisch C et al. Estimating the magnitude of trastuzumab
effects within patient subgroups in the HERA trial. Ann Oncol 2008; 19:
10901096.
29. Romond EH, Perez EA, Bryant J et al. Trastuzumab plus adjuvant chemotherapy for
operable HER2-positive breast cancer. N Engl J Med 2005; 353: 16731684.
30. Colleoni M, Bagnardi V, Rotmensz N et al. Increasing steroid hormone receptors
expression denes breast cancer subtypes non responsive to preoperative
chemotherapy. Breast Cancer Res Treat 2009; 116: 359369.
31. Paik S, Shak S, Tang G et al. A multigene assay to predict recurrence of
tamoxifen-treated, node-negative breast cancer. N Engl J Med 2004; 351:
28172826.
32. Goldhirsch A, Wood WC, Coates AS et al. Strategies for subtypesdealing with the
diversity of breast cancer: highlights of the St. Gallen International Expert
review
Annals of Oncology
8 | Montemurro et al.
b
y
g
u
e
s
t
o
n
N
o
v
e
m
b
e
r
1
3
,
2
0
1
3
h
t
t
p
:
/
/
a
n
n
o
n
c
.
o
x
f
o
r
d
j
o
u
r
n
a
l
s
.
o
r
g
/
D
o
w
n
l
o
a
d
e
d
f
r
o
m
Consensus on the Primary Therapy of Early Breast Cancer 2011. Ann Oncol 2011;
22: 17361747.
33. Montemurro F, Rossi V, Rocca MC et al. Hormone-receptor expression and activity
of trastuzumab with chemotherapy in HER2-positive advanced breast cancer
patients. Cancer 2012; 118: 1726.
34. Cortazar P, Zhang L, Untch M et al. Meta-analysis Results from the Collaborative Trials
in Neoadjuvant Breast Cancer (CTNeoBC). Cancer Res 2012; 72: (Abstr S1-11).
35. Rimawi MF, Mayer IA, Forero A et al. Multicenter Phase II Study of Neoadjuvant
Lapatinib and Trastuzumab With Hormonal Therapy and Without Chemotherapy in
Patients With Human Epidermal Growth Factor Receptor 2-Overexpressing Breast
Cancer: TBCRC 006. J Clin Oncol 2013; 31: 17261731.
36. Davies C, Godwin J, Gray R et al. Relevance of breast cancer hormone receptors
and other factors to the efcacy of adjuvant tamoxifen: patient-level meta-analysis
of randomised trials. Lancet 2011; 378: 771784.
37. De Laurentiis M, Arpino G, Massarelli E et al. A meta-analysis on the interaction
between HER-2 expression and response to endocrine treatment in advanced
breast cancer. Clin Cancer Res 2005; 11: 47414748.
38. Arpino G, Green SJ, Allred DC et al. HER-2 amplication, HER-1 expression, and
tamoxifen response in estrogen receptor-positive metastatic breast cancer: A
southwest oncology group study. Clin Cancer Res 2004; 10: 56705676.
39. De Placido S, De Laurentiis M, Carlomagno C et al. Twenty-year results of the
Naples GUN randomized trial: predictive factors of adjuvant tamoxifen efcacy in
early breast cancer. Clin Cancer Res 2003; 9: 10391046.
40. Dowsett M, Houghton J, Iden C et al. Benet from adjuvant tamoxifen therapy in
primary breast cancer patients according oestrogen receptor, progesterone
receptor, EGF receptor and HER2 status. Ann Oncol 2006; 17: 818826.
41. Love RR, Duc NB, Havighurst TC et al. Her-2/neu overexpression and response to
oophorectomy plus tamoxifen adjuvant therapy in estrogen receptor-positive
premenopausal women with operable breast cancer. J Clin Oncol 2003; 21:
453457.
42. Berry DA, Muss HB, Thor AD et al. HER-2/neu and p53 expression versus
tamoxifen resistance in estrogen receptor-positive, node-positive breast cancer.
J Clin Oncol 2000; 18: 34713479.
43. Ellis MJ, Coop A, Singh B et al. Letrozole is more effective neoadjuvant endocrine
therapy than tamoxifen for ErbB-1- and/or ErbB-2-positive, estrogen receptor-
positive primary breast cancer: evidence from a phase III randomized trial. J Clin
Oncol 2001; 19: 38083816.
44. Dowsett M, Ebbs SR, Dixon JM et al. Biomarker changes during neoadjuvant
anastrozole, tamoxifen, or the combination: inuence of hormonal status and HER-
2 in breast cancera study from the IMPACT trialists. J Clin Oncol 2005; 23:
24772492.
45. Ellis MJ, Tao Y, Young O et al. Estrogen-independent proliferation is present in
estrogen-receptor HER2-positive primary breast cancer after neoadjuvant letrozole.
J Clin Oncol 2006; 24: 30193025.
46. Dowsett M, Allred C, Knox J et al. Relationship between quantitative estrogen and
progesterone receptor expression and human epidermal growth factor receptor 2
(HER-2) status with recurrence in the Arimidex, Tamoxifen, Alone or in
Combination trial. J Clin Oncol 2008; 26: 10591065.
47. Rasmussen BB, Regan MM, Lykkesfeldt AE et al. Adjuvant letrozole versus
tamoxifen according to centrally-assessed ERBB2 status for postmenopausal
women with endocrine-responsive early breast cancer: supplementary results from
the BIG 1-98 randomised trial. Lancet Oncol 2008; 9: 2328.
48. Chung YL, Sheu ML, Yang SC et al. Resistance to tamoxifen-induced apoptosis is
associated with direct interaction between Her2/neu and cell membrane estrogen
receptor in breast cancer. Int J Cancer 2002; 97: 306312.
49. Vyhlidal C, Samudio I, Kladde MP et al. Transcriptional activation of transforming
growth factor alpha by estradiol: requirement for both a GC-rich site and an
estrogen response element half-site. J Mol Endocrinol 2000; 24: 329338.
50. Lee AV, Cui XJ, Oesterreich S. Cross-talk among estrogen receptor, epidermal
growth factor, and insulin-like growth factor signaling in breast cancer. Clin Cancer
Res 2001; 7: 4429S4435S.
51. Umayahara Y, Kawamori R, Watada H et al. Estrogen Regulation of the Insulin-Like
Growth-Factor-I Gene-Transcription Involves An Ap-1 Enhancer. J Biol Chem
1994; 269: 1643316442.
52. Nicholson RI, Hutcheson IR, Britton D et al. Growth factor signalling networks in
breast cancer and resistance to endocrine agents: new therapeutic strategies. J
Steroid Biochem Mol Biol 2005; 93: 257262.
53. Font dM, Brown M. AIB1 is a conduit for kinase-mediated growth factor signaling
to the estrogen receptor. Mol Cell Biology 2000; 20: 50415047.
54. Hong SH, Privalsky ML. The SMRT corepressor is regulated by a MEK-1 kinase
pathway: inhibition of corepressor function is associated with SMRT
phosphorylation and nuclear export. Mol Cell Biology 2000; 20: 66126625.
55. Wu RC, Qin J, Yi P et al. Selective phosphorylations of the SRC-3/AIB1 coactivator
integrate genomic reponses to multiple cellular signaling pathways. Mol Cell 2004;
15: 937949.
56. Guo SQ, Sonenshein GE. Forkhead box transcription factor FOXO3a regulates
estrogen receptor alpha expression and is repressed by the Her-2/neu/
phosphatidylinositol 3-kinase/Akt signaling pathway. Mol Cell Biology 2004; 24:
86818690.
57. Creighton CJ, Fu X, Hennessy BT et al. Proteomic and transcriptomic proling
reveals a link between the PI3K pathway and lower estrogen-receptor (ER) levels
and activity in ER+ breast cancer. Breast Cancer Res 2010; 12: R40.
58. Levin ER, Pietras RJ. Estrogen receptors outside the nucleus in breast cancer.
Breast Cancer Res Treat 2008; 108: 351361.
59. Razandi M, Pedram A, Levin ER. Plasma membrane estrogen receptors signal to
antiapoptosis in breast cancer. Mol Endocrinol 2000; 14: 14341447.
60. Razandi M, Alton G, Pedram A et al. Identication of a structural determinant
necessary for the localization and function of estrogen receptor alpha at the
plasma membrane. Mol Cell Biology 2003; 23: 16331646.
61. Kato S, Endoh H, Masuhiro Y et al. Activation of the estrogen receptor through
phosphorylation by mitogen-activated protein kinase. Science 1995; 270:
14911494.
62. Welsh AW, Lannin DR, Young GS et al. Cytoplasmic estrogen receptor in breast
cancer. Clin Cancer Res 2012; 18: 118126.
63. Shou J, Massarweh S, Osborne CK et al. Mechanisms of tamoxifen resistance:
increased estrogen receptor-HER2/neu cross-talk in ER/HER2-positive breast
cancer. J Natl Cancer Inst 2004; 96: 926935.
64. Arpino G, Gutierrez C, Weiss H et al. Treatment of human epidermal growth factor
receptor 2-overexpressing breast cancer xenografts with multiagent HER-targeted
therapy. J Natl Cancer Inst 2007; 99: 694705.
65. Rimawi MF, Wiechmann LS, Wang YC et al. Reduced Dose and Intermittent
Treatment with Lapatinib and Trastuzumab for Potent Blockade of the HER
Pathway in HER2/neu-Overexpressing Breast Tumor Xenografts. Clin Cancer Res
2011; 17: 13511361.
66. Witters LM, Kumar R, Chinchilli VM et al. Enhanced anti-proliferative activity of the
combination of tamoxifen plus HER-2-neu antibody. Breast Cancer Res Treat
1997; 42: 15.
67. Kunisue H, Kurebayashi J, Otsuki T et al. Anti-HER2 antibody enhances the growth
inhibitory effect of anti-oestrogen on breast cancer cells expressing both oestrogen
receptors and HER2. Br J Cancer 2000; 82: 4651.
68. Rexer BN, Arteaga CL. Intrinsic and acquired resistance to HER2-targeted
therapies in HER2 gene-amplied breast cancer: mechanisms and clinical
implications. Crit Rev Oncog 2012; 17: 116.
69. Liu L, Greger J, Shi H et al. Novel Mechanism of Lapatinib Resistance in HER2-
Positive Breast Tumor Cells: Activation of AXL. Cancer Res 2009; 69:
68716878.
70. Xia W, Bacus S, Hegde P et al. A model of acquired autoresistance to a potent
ErbB2 tyrosine kinase inhibitor and a therapeutic strategy to prevent its onset in
breast cancer. Proc Natl Acad Sci U S A 2006; 103: 77957800.
71. Munzone E, Curigliano G, Rocca A et al. Reverting estrogen-receptor-negative
phenotype in HER-2-overexpressing advanced breast cancer patients exposed to
trastuzumab plus chemotherapy. Breast Cancer Res 2006; 8: R4.
72. Wang YC, Morrison G, Gillihan R et al. Different mechanisms for resistance to
trastuzumab versus lapatinib in HER2-positive breast cancers - role of estrogen
receptor and HER2 reactivation. Breast Cancer Res 2011; 13: R121.
73. Kaufman B, Mackey JR, Clemens MR et al. Trastuzumab plus anastrozole versus
anastrozole alone for the treatment of postmenopausal women with human
epidermal growth factor receptor 2-positive, hormone receptor-positive metastatic
Annals of Oncology
review
doi:10.1093/annonc/mdt287 |
b
y
g
u
e
s
t
o
n
N
o
v
e
m
b
e
r
1
3
,
2
0
1
3
h
t
t
p
:
/
/
a
n
n
o
n
c
.
o
x
f
o
r
d
j
o
u
r
n
a
l
s
.
o
r
g
/
D
o
w
n
l
o
a
d
e
d
f
r
o
m
breast cancer: results from the randomized phase III TAnDEM study. J Clin Oncol
2009; 27: 55295537.
74. Johnston S, Pippen J, Jr, Pivot X et al. Lapatinib combined with letrozole versus
letrozole and placebo as rst-line therapy for postmenopausal hormone receptor-
positive metastatic breast cancer. J Clin Oncol 2009; 27: 55385546.
75. Schwarzberg LS, Franco SX, Florance A et al. Lapatinib plus letrozole as rst-Line
therapy for HER-2+ hormone receptor-positive metastatic breast cancer.
Oncologist 2010; 15: 122129.
76. Huober J, Fasching PA, Barsoum M et al. Higher efcacy of letrozole in
combination with trastuzumab compared to letrozole monotherapy as rst-line
treatment in patients with HER2-positive, hormone-receptor-positive metastatic
breast cancer - results of the eLEcTRA trial. The Breast 2012; 21: 2733.
77. Cardoso F, Costa A, Norton L et al. 1st International consensus guidelines for
advanced breast cancer (ABC 1). The Breast 2012; 21: 242252.
78. Tripathy D, Kaufman PA, Brufsky AM et al. First-Line Treatment Patterns and
Clinical Outcomes in Patients With HER2-Positive and Hormone Receptor-Positive
Metastatic Breast Cancer From registHER. Oncologist 2013; 18: 501510.
79. Carey LA, Berry D, Ollila D et al. Clinical and translational results of CALGB 40601:
A neoadjuvant phase III trial of weekly paclitaxel and trastuzumab with or without
lapatinib for HER2-positive breast cancer. J Clin Oncol (Meeting Abstracts) 2013;
31: (Abstr 500).
80. Wardley AM, Pivot X, Morales-Vasquez F et al. Randomized phase II trial of rst-
line trastuzumab plus docetaxel and capecitabine compared with trastuzumab plus
docetaxel in HER2-positive metastatic breast cancer. J Clin Oncol 2010; 28:
976983.
81. Valero V, Forbes J, Pegram MD et al. Multicenter phase III randomized trial
comparing docetaxel and trastuzumab with docetaxel, carboplatin, and
trastuzumab as rst-line chemotherapy for patients with HER2-gene-amplied
metastatic breast cancer (BCIRG 007 study): two highly active therapeutic
regimens. J Clin Oncol 2011; 29: 149156.
82. Robert N, Leyland-Jones B, Asmar L et al. Randomized phase III study of
trastuzumab, paclitaxel, and carboplatin compared with trastuzumab and paclitaxel
in women with HER-2-overexpressing metastatic breast cancer. J Clin Oncol
2006; 24: 27862792.
83. Andersson M, Lidbrink E, Bjerre K et al. Phase III randomized study comparing
docetaxel plus trastuzumab with vinorelbine plus trastuzumab as rst-line
therapy of metastatic or locally advanced human epidermal growth factor
receptor 2-positive breast cancer: the HERNATA study. J Clin Oncol 2011; 29:
264271.
84. Di LA, Gomez HL, Aziz Z et al. Phase III, double-blind, randomized study
comparing lapatinib plus paclitaxel with placebo plus paclitaxel as rst-line
treatment for metastatic breast cancer. J Clin Oncol 2008; 26: 55445552.
85. Guan Z, Xu B, Arpornwirat W et al. Abstract P3-14-24: Overall survival benet
observed with lapatinib (L) plus paclitaxel (P) as rst-line therapy in patients with
HER2-overexpressing metastatic breast cancer (MBC). Cancer Res 2011; 70:
(Abstr P-3-14).
86. Hurvitz S, Dirix L, Kocsis J et al. Trastuzumab emtansine (T-DM1) vs trastuzumab
plus docetaxel (H+T) in previously-untreated HER2-positive metastatic breast
cancer (MBC): primary results of a randomized, multicenter, open-label
phase II study (TDM4450g/BO21976). Eur J Cancer 2011; 47: S330 (Abstr
5001).
87. Untch M, Loibl S, Bischoff J et al. Lapatinib versus trastuzumab in combination
with neoadjuvant anthracycline-taxane-based chemotherapy (GeparQuinto,
GBG 44): a randomised phase 3 trial. Lancet Oncol 2012; 13: 135144.
review
Annals of Oncology
1o | Montemurro et al.
b
y
g
u
e
s
t
o
n
N
o
v
e
m
b
e
r
1
3
,
2
0
1
3
h
t
t
p
:
/
/
a
n
n
o
n
c
.
o
x
f
o
r
d
j
o
u
r
n
a
l
s
.
o
r
g
/
D
o
w
n
l
o
a
d
e
d
f
r
o
m
You might also like
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)From EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Rating: 4.5 out of 5 stars4.5/5 (119)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaFrom EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaRating: 4.5 out of 5 stars4.5/5 (265)
- The Little Book of Hygge: Danish Secrets to Happy LivingFrom EverandThe Little Book of Hygge: Danish Secrets to Happy LivingRating: 3.5 out of 5 stars3.5/5 (399)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryFrom EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryRating: 3.5 out of 5 stars3.5/5 (231)
- Grit: The Power of Passion and PerseveranceFrom EverandGrit: The Power of Passion and PerseveranceRating: 4 out of 5 stars4/5 (587)
- Never Split the Difference: Negotiating As If Your Life Depended On ItFrom EverandNever Split the Difference: Negotiating As If Your Life Depended On ItRating: 4.5 out of 5 stars4.5/5 (838)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeFrom EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeRating: 4 out of 5 stars4/5 (5794)
- Team of Rivals: The Political Genius of Abraham LincolnFrom EverandTeam of Rivals: The Political Genius of Abraham LincolnRating: 4.5 out of 5 stars4.5/5 (234)
- Shoe Dog: A Memoir by the Creator of NikeFrom EverandShoe Dog: A Memoir by the Creator of NikeRating: 4.5 out of 5 stars4.5/5 (537)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyFrom EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyRating: 3.5 out of 5 stars3.5/5 (2219)
- The Emperor of All Maladies: A Biography of CancerFrom EverandThe Emperor of All Maladies: A Biography of CancerRating: 4.5 out of 5 stars4.5/5 (271)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreFrom EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreRating: 4 out of 5 stars4/5 (1090)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersFrom EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersRating: 4.5 out of 5 stars4.5/5 (344)
- Her Body and Other Parties: StoriesFrom EverandHer Body and Other Parties: StoriesRating: 4 out of 5 stars4/5 (821)
- Rupert SheldrakeDocument115 pagesRupert Sheldrakeamasino1100% (3)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceFrom EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceRating: 4 out of 5 stars4/5 (894)
- Cancer Self TreatmentDocument35 pagesCancer Self TreatmentRichard HoltNo ratings yet
- Effective Arguments For Medical Marijuana AdvocatesDocument22 pagesEffective Arguments For Medical Marijuana AdvocatesMPP100% (11)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureFrom EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureRating: 4.5 out of 5 stars4.5/5 (474)
- The Unwinding: An Inner History of the New AmericaFrom EverandThe Unwinding: An Inner History of the New AmericaRating: 4 out of 5 stars4/5 (45)
- The Yellow House: A Memoir (2019 National Book Award Winner)From EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Rating: 4 out of 5 stars4/5 (98)
- On Fire: The (Burning) Case for a Green New DealFrom EverandOn Fire: The (Burning) Case for a Green New DealRating: 4 out of 5 stars4/5 (73)
- Cassar Mario-Paul - Handbook of Clinical MassageDocument350 pagesCassar Mario-Paul - Handbook of Clinical MassageVlado Gon100% (2)
- Glycine - The Amino Acid That Benefits Your Entire Body - DRDocument22 pagesGlycine - The Amino Acid That Benefits Your Entire Body - DRRajib DasNo ratings yet
- Reproductive System: Facts, Symptoms & TreatmentsDocument34 pagesReproductive System: Facts, Symptoms & TreatmentsJobelyn MalisaNo ratings yet
- Obesiti 1Document22 pagesObesiti 1Rosniah Bt Zainol AbidinNo ratings yet
- HachinskiIschaemicScore SVUH MedEl ToolDocument1 pageHachinskiIschaemicScore SVUH MedEl ToolJayjay Amburadul BuangetNo ratings yet
- Diagnosis of Primary Versus Secondary Achalasia:: Reassessment of Clinical and Radiographic CriteriaDocument5 pagesDiagnosis of Primary Versus Secondary Achalasia:: Reassessment of Clinical and Radiographic CriteriaJayjay Amburadul BuangetNo ratings yet
- 06 Mrozkow PDFDocument7 pages06 Mrozkow PDFJayjay Amburadul BuangetNo ratings yet
- Biosignatures For Parkinson's Disease and AtypicalDocument13 pagesBiosignatures For Parkinson's Disease and AtypicalArnab MullickNo ratings yet
- Daftar Pustaka PDFDocument0 pagesDaftar Pustaka PDFJayjay Amburadul BuangetNo ratings yet
- Chagas Disease: American TrypanosomiasisDocument1 pageChagas Disease: American TrypanosomiasisJayjay Amburadul BuangetNo ratings yet
- 06 Mrozkow PDFDocument7 pages06 Mrozkow PDFJayjay Amburadul BuangetNo ratings yet
- BCTT 23560 Role of Pertuzumab For The Treatment of Her2 Posi PDFDocument9 pagesBCTT 23560 Role of Pertuzumab For The Treatment of Her2 Posi PDFJayjay Amburadul BuangetNo ratings yet
- Laporan PBL 2 - BHL 4 - Kelompok 9Document13 pagesLaporan PBL 2 - BHL 4 - Kelompok 9Jayjay Amburadul BuangetNo ratings yet
- Laporan PBL 2 - BHL 4 - Kelomopok 9Document13 pagesLaporan PBL 2 - BHL 4 - Kelomopok 9Jayjay Amburadul BuangetNo ratings yet
- KLPK 7Document6 pagesKLPK 7Jayjay Amburadul BuangetNo ratings yet
- KLPK 7Document6 pagesKLPK 7Jayjay Amburadul BuangetNo ratings yet
- البروفيل الديمغرافي لمرضى سرطان القولون و المستقيم بمركز مكافحة السرطان سطيفDocument14 pagesالبروفيل الديمغرافي لمرضى سرطان القولون و المستقيم بمركز مكافحة السرطان سطيفsaraNo ratings yet
- Chapter 50 Assessment of Immune FunctionDocument12 pagesChapter 50 Assessment of Immune FunctionChan SorianoNo ratings yet
- On05 6 2 01Document8 pagesOn05 6 2 01aoife123No ratings yet
- CBEDocument17 pagesCBElovtetaNo ratings yet
- Bacterial Synthesis of Nanoparticles for Biomedical ApplicationsDocument16 pagesBacterial Synthesis of Nanoparticles for Biomedical ApplicationsDibyajyoti20 Das4001No ratings yet
- Cancer Care in AyurvedaDocument7 pagesCancer Care in AyurvedaArshath JyothiNo ratings yet
- Epigenetics Source of Mental Dysfunction and The Nutrient-Based Solution William Walsh PHDDocument7 pagesEpigenetics Source of Mental Dysfunction and The Nutrient-Based Solution William Walsh PHDJorge Pita AlvarezNo ratings yet
- 2008-CE337 - The Intraoral and Extraoral ExamDocument33 pages2008-CE337 - The Intraoral and Extraoral Examyongky100% (1)
- Ancer: 1.6 MillionDocument136 pagesAncer: 1.6 MillionRichard GabrielNo ratings yet
- Genome-Wide Methylation and Expression Analyses Reveal The Epigenetic Landscape of Immune-Related Diseases For Tobacco SmokingDocument14 pagesGenome-Wide Methylation and Expression Analyses Reveal The Epigenetic Landscape of Immune-Related Diseases For Tobacco SmokingLaura AcostaNo ratings yet
- Comparison OF Bronchoalveolar Lavage Cytology and Biopsy in Lung MalignancyDocument5 pagesComparison OF Bronchoalveolar Lavage Cytology and Biopsy in Lung MalignancyDyahSavitriKusumoningtyasNo ratings yet
- Dosimetric comparison of Cyberknife vs. Linac for lung cancer SBRTDocument26 pagesDosimetric comparison of Cyberknife vs. Linac for lung cancer SBRTraheel252No ratings yet
- Antiemesis NCCNDocument79 pagesAntiemesis NCCNana salazarNo ratings yet
- Cancer Prediction Using ML - UpdatedDocument14 pagesCancer Prediction Using ML - UpdatedRAJU MAURYANo ratings yet
- Revisi Provincial Team Leader New For HabibaDocument19 pagesRevisi Provincial Team Leader New For HabibaFagi KarimNo ratings yet
- Webinar Presentations of Prof Anand Mishra and DR Pooja Ramakant From Endocrine Surgery Dept of KGMUDocument35 pagesWebinar Presentations of Prof Anand Mishra and DR Pooja Ramakant From Endocrine Surgery Dept of KGMUbobbyramakantNo ratings yet
- Pancreatic Solid LeasionsDocument24 pagesPancreatic Solid LeasionsEliza CrăciunNo ratings yet
- Bio-chemical composition and medicinal uses of soursop fruitDocument24 pagesBio-chemical composition and medicinal uses of soursop fruitAnonymous q2B8JzyT5No ratings yet
- Temozolomide Adjuvant NHSDocument5 pagesTemozolomide Adjuvant NHSSyed Touseef AhmedNo ratings yet
- Last Aid Dermatology SARPDocument7 pagesLast Aid Dermatology SARPskNo ratings yet
- Surgery For Pathological T3a, T3b and Lymph Node Positive, Prostae Cance PDFDocument11 pagesSurgery For Pathological T3a, T3b and Lymph Node Positive, Prostae Cance PDFMuhammad RifkiNo ratings yet
- SARMS Powders Prices - David FromDocument1 pageSARMS Powders Prices - David FromOld World OrderNo ratings yet
- Acute Leukaemia: Dr. Nuryanti, M.Ked (Clin - Path), SPPK Laboratory Patologi Clinic Rs GranmedDocument29 pagesAcute Leukaemia: Dr. Nuryanti, M.Ked (Clin - Path), SPPK Laboratory Patologi Clinic Rs GranmedArnita Elisabet ManurungNo ratings yet
- Tumor Markers GuideDocument23 pagesTumor Markers GuideSeptiansyah CahyoNo ratings yet