Professional Documents
Culture Documents
Case Study Copd
Uploaded by
Irveen Joy RamirezCopyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Case Study Copd
Uploaded by
Irveen Joy RamirezCopyright:
Available Formats
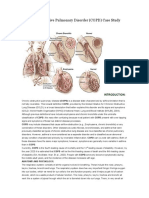
INTRODUCTION: Chronic obstructive pulmonary disease (COPD) is a disease state characterized by airflow limitation that is not fully reversible.
This newest definition COPD, provided by the Global Initiative for Chrnonic Obstructive Lung Disease (GOLD), is a broad description that better explains this disorder and its signs and symptoms (GOLD, World Health Organization [WHO] & National Heart, Lung and Blood Institute [NHLBI], 2004). Although previous definitions have include emphysema and chronic bronchitis under the umbrella classification of COPD, this was often confusing because most patient with COPD present with over lapping signs and symptoms of these two distinct disease processes. COPD may include diseases that cause airflow obstruction (e.g., Emphysema, chronic bronchitis) or any combination of these disorders. Other diseases as cystic fibrosis, bronchiectasis, and asthma that were previously classified as types of chronic obstructive lung disease are now classified as chronic pulmonary disorders. However, asthma is now considered as a separate disorder and is classified as an abnormal airway condition characterized primarily by reversible inflammation. COPD can co-exist with asthma. Both of these diseases have the same major symptoms; however, symptoms are generally more variable in asthma than in COPD. Currently, COPD is the fourth leading cause of mortality and the 12th leading cause of disability. However, by the year 2020 it is estimated that COPD will be the third leading cause of death and the firth leading cause of disability (Sin, McAlister, Man. Et al., 2003). People with COPD commonly become symptomatic during the middle adult years, and the incidence of the disease increases with age.
ANATOMY AND PHYSIOLOGY: The respiratory system consists of all the organs involved in breathing. These include the nose, pharynx, larynx, trachea, bronchi and lungs. The respiratory system does two very important things: it brings oxygen into our bodies, which we need for our cells to live and function properly; and it helps us get rid of carbon dioxide, which is a waste product of cellular function. The nose, pharynx, larynx, trachea and bronchi all work like a system of pipes through which the air is funneled down into our lungs. There, in very small air sacs called alveoli, oxygen is brought into the bloodstream and carbon dioxide is pushed from the blood out into the air. When something goes wrong with part of the respiratory system, such as an infection like pneumonia, chronic obstructive pulmonary diseases, it makes it harder for us to get the oxygen we need and to get rid of the waste product carbon dioxide. Common respiratory symptoms include breathlessness, cough, and chest pain.
The Upper Airway and Trachea
When you breathe in, air enters your body through your nose or mouth. From there, it travels down your throat through the larynx (or voicebox) and into the trachea (or windpipe) before entering your lungs. All these structures act to funnel fresh air down from the outside world into your body. The upper
airway is important because it must always stay open for you to be able to breathe. It also helps to moisten and warm the air before it reaches your lungs.
The Lungs
The lungs are paired, cone-shaped organs which take up most of the space in our chests, along with the heart. Their role is to take oxygen into the body, which we need for our cells to live and function properly, and to help us get rid of carbon dioxide, which is a waste product. We each have two lungs, a left lung and a right lung. These are divided up into lobes, or big sections of tissue separated by fissures or dividers. The right lung has three lobes but the left lung has only two, because the heart takes up some of the space in the left side of our chest. The lungs can also be divided up into even smaller portions, called bronchopulmonary segments. These are pyramidal-shaped areas which are also separated from each other by membranes. There are about 10 of them in each lung. Each segment receives its own blood supply and air supply.
COPD VERSUS HEALTHY LUNG
Air enters your lungs through a system of pipes called the bronchi. These pipes start from the bottom of the trachea as the left and right bronchi and branch many times throughout the lungs, until they eventually form little thin-walled air sacs or bubbles, known as the alveoli. The alveoli are where the important work of gas exchange takes place between the air and your blood. Covering each alveolus is a whole network of little blood vessel called capillaries, which are very small branches of the pulmonary arteries. It is important that the air in the alveoli and the blood in the capillaries are very close together, so that oxygen and carbon dioxide can move (or diffuse) between them. So, when you breathe in, air comes down the trachea and through the bronchi into the alveoli. This fresh air has lots of oxygen in it, and some of this oxygen will travel across the walls of the alveoli into your bloodstream. Traveling in the opposite direction is carbon dioxide, which crosses from the blood in the capillaries into the air in the alveoli and is then breathed out. In this way, you bring in to your body the oxygen that you need to live, and get rid of the waste product carbon dioxide.
Blood Supply
The lungs are very vascular organs, meaning they receive a very large blood supply. This is because the pulmonary arteries, which supply the lungs, come directly from the right side of your heart. They carry blood which is low in oxygen and high in carbon dioxide into your lungs so that the carbon dioxide can be blown off, and more oxygen can be absorbed into the bloodstream. The newly oxygen-rich blood then travels back through the paired pulmonary veins into the left side of your heart. From there, it is pumped all around your body to supply oxygen to cells and organs.
The Work of Breathing
The lungs are covered by smooth membranes that we call pleurae. The pleurae have two layers, a visceral layer which sticks closely to the outside surface of your lungs, and a parietal layer which line s the inside of your chest wall (ribcage). The pleurae are important because they help you breathe in and out smoothly, without any friction. They also make sure that when your ribcage expands on breathing in; your lungs expand as well to fill the extra space.
The Diaphragm and Intercostal Muscles
When you breathe in (inspiration), your muscles need to work to fill your lungs with air. The diaphragm, a large, sheet-like muscle which stretches across your chest under the ribcage, does much of this work. At rest, it is shaped like a dome curving up into your chest. When you breathe in, the diaphragm contracts and flattens out, expanding the space in your chest and drawing air into your lungs. Other muscles, including the muscles between your ribs (the intercostal muscles) also help by moving your ribcage in and out. Breathing out (expiration) does not normally require your muscles to work. This is because your lungs are very elastic, and when your muscles relax at the end of inspiration your lungs simply recoil back into their resting position, pushing the air out as they go.
The Respiratory System and Ageing
The normal process of ageing is associated with a number of changes in both the structure and function of the respiratory system. These include: 1. Enlargement of the alveoli. The air spaces get bigger and lose their elasticity, meaning that there is less area for gases to be exchanged across. This change is sometimes referred to as senile emphysema. 2. The compliance (or springiness) of the chest wall decreases, so that it takes more effort to breathe in and out. 3. The strength of the respiratory muscles (the diaphragm and intercostal muscles) decreases. This change is closely connected to the general health of the person. All of these changes mean that an older person might have more difficulty coping with increased stress on their respiratory system, such as with an infection like pneumonia, than a younger person would.
PREDISPOSING FACTORS
Cigarette smoking o The primary cause of chronic obstructive pulmonary disease (COPD) is exposure to tobacco smoke. Clinically significant COPD develops in 15% of cigarette smokers, although this number is believed to be an underestimate. Age of initiation of smoking, total pack-years, and current smoking status predict COPD mortality. People who smoke have a greater annual decline in FEV1. Overall, tobacco smoking accounts for as much as 90% of the risk. o Secondhand smoke, or environmental tobacco smoke, increases the risk of respiratory infections, augments asthma symptoms, and causes a measurable reduction in pulmonary function. Air pollution o Although the role of air pollution in the etiology of COPD is unclear, the effect is small when compared with cigarette smoking. o The use of solid fuels for cooking and heating may result in high levels of indoor air pollution and the development of COPD. Airway hyper responsiveness o Airway hyper responsiveness (i.e., Dutch hypothesis) stipulates that patients who have nonspecific airway hyperactivity and who smoke are at increased risk of developing COPD with an accelerated decline in lung function. Nonspecific airway hyperactivity is inversely related to FEV1 and may predict a decline in lung function. o The possible role of airway hyper responsiveness as a risk factor for the development of COPD in people who smoke is unclear. Moreover, bronchial hyperactivity may result from airway inflammation observed with the development of smoking-related chronic bronchitis. This may contribute to airway remodeling, leading to a more fixed obstruction as is seen in persons with COPD.
PATHOPHYSIOLOGY OF CHRONIC OBSTRUCTIVE PULMONARY DISEASE
PATIENTS PROFILE
NAME ADDRESS AGE DATE OF BIRTH OCCUPATION CIVIL STATUS
PHYSICAL EXAMINATION
Wesleyan University-Philippines College of Nursing
A CASE STUDY OF CHRONIC OBSTRUCTIVE PULMONARY DISEASE
Submitted By: Irveen Joy L. Ramirez BSN III 5
Submitted To: Sir Jeffrey Galang RN, MAN Clinical Instructor
You might also like
- Community Acquired Pneumonia, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsFrom EverandCommunity Acquired Pneumonia, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsNo ratings yet
- Case Study COPDDocument16 pagesCase Study COPDRegine Cimafranca Macalaguing100% (5)
- COPD Case ICUDocument19 pagesCOPD Case ICUKim Vizcarra100% (1)
- Anatomy and Physiology CopdDocument15 pagesAnatomy and Physiology CopdAssenav May100% (3)
- Case Presentation: Patient Chart - Mary JohnsonDocument12 pagesCase Presentation: Patient Chart - Mary Johnsonivoneeh_16100% (1)
- Nursing Care PlanDocument2 pagesNursing Care PlanAl RizkyNo ratings yet
- Process RecordingDocument1 pageProcess RecordingJuko Fernandez0% (1)
- HSNS264 A1 COPDDocument2 pagesHSNS264 A1 COPDKC Nilam100% (1)
- Abdominal Case Study CompiledDocument392 pagesAbdominal Case Study CompiledIshak IzharNo ratings yet
- CopdDocument30 pagesCopdsalmanhabeebekNo ratings yet
- The Patient and His Illness A. Pathophysiology (Book Based)Document5 pagesThe Patient and His Illness A. Pathophysiology (Book Based)Edmar Francis SabileNo ratings yet
- Ward Case PresentationDocument92 pagesWard Case PresentationSuzette Rae TateNo ratings yet
- Copd CaseDocument36 pagesCopd Casejho_No ratings yet
- I. Review of Systems System/ Organ Subjective Cues AnalysisDocument1 pageI. Review of Systems System/ Organ Subjective Cues AnalysisZmiaNo ratings yet
- Pleural EffusionDocument38 pagesPleural EffusionMela VincoNo ratings yet
- Liceo de Cagayan University College of NursingDocument23 pagesLiceo de Cagayan University College of NursingMelody Forca FranciscoNo ratings yet
- PathophysiologyDocument2 pagesPathophysiologyKarla Karina Dela CruzNo ratings yet
- NUR5703 Respiratory Advanced PathophysiologyDocument16 pagesNUR5703 Respiratory Advanced PathophysiologyLee MeyerNo ratings yet
- (Patho) PTB COPDDocument1 page(Patho) PTB COPDKyle HannahNo ratings yet
- Practice Mod 6 Case StudyDocument6 pagesPractice Mod 6 Case Studyvanessa100% (1)
- Asthma Patient Education: Check ListDocument2 pagesAsthma Patient Education: Check ListZiyad AlrajhiNo ratings yet
- Jim Nursing Essay - Chronic Obstructive Pulmonary Disease (COPD) .Document8 pagesJim Nursing Essay - Chronic Obstructive Pulmonary Disease (COPD) .SarahJaneNo ratings yet
- PnuemoniaDocument102 pagesPnuemoniaRegineCuasSulibNo ratings yet
- Running Head: Elder Assessment 1Document13 pagesRunning Head: Elder Assessment 1api-4190916620% (1)
- Chronic Obstructive Pulmonary Disease: Patient Population: ObjectivesDocument28 pagesChronic Obstructive Pulmonary Disease: Patient Population: Objectivesdoni anandaNo ratings yet
- Velez College College of Nursing: Bascon, Karl Niño D. Calunsag, Hazel Kate C. Lague, Inah Krizia ODocument7 pagesVelez College College of Nursing: Bascon, Karl Niño D. Calunsag, Hazel Kate C. Lague, Inah Krizia Oinah krizia lagueNo ratings yet
- PneumothoraxDocument45 pagesPneumothoraxWiDya EmiLiaNo ratings yet
- Opqrst SampleDocument2 pagesOpqrst SampleNunyaNo ratings yet
- Case Study of PNEUMONIADocument12 pagesCase Study of PNEUMONIAAriaNo ratings yet
- COPD Case Study ResearchDocument5 pagesCOPD Case Study ResearchErica MotoNo ratings yet
- Concept Map 2Document1 pageConcept Map 2lanrevoiceNo ratings yet
- Cap MR DDHDocument32 pagesCap MR DDHLovelle LopezNo ratings yet
- Nursing Care Plans For Lung CancerDocument7 pagesNursing Care Plans For Lung CancerThea Eya Faye100% (1)
- Oxygenation Problem Notes and Nursing InterventionsDocument7 pagesOxygenation Problem Notes and Nursing InterventionsAnna TaylorNo ratings yet
- Case Study PNEUMONIADocument40 pagesCase Study PNEUMONIAHomework PingNo ratings yet
- Chronic Obstructive Pilmonary Disease: Kreshimaricon FurigayDocument86 pagesChronic Obstructive Pilmonary Disease: Kreshimaricon FurigayKreshee Maricon100% (1)
- Journal Surg Ward BorjaDocument4 pagesJournal Surg Ward BorjaYana PotNo ratings yet
- Written Report Community Acquired Pneumonia - Medium RiskDocument14 pagesWritten Report Community Acquired Pneumonia - Medium RiskMichael LinebargerNo ratings yet
- Acute Respiratory Failure 375Document65 pagesAcute Respiratory Failure 375Ahsan Javed100% (1)
- Chronic Obstructive Pulmonary Disease: EmphysemaDocument11 pagesChronic Obstructive Pulmonary Disease: EmphysemarielNo ratings yet
- Pathophysiology of Tuberculosis: Group 5 Latosa, Selene Lee, Guk Lim, Johanna Magalona, Stephen Mendoza, ColeenDocument22 pagesPathophysiology of Tuberculosis: Group 5 Latosa, Selene Lee, Guk Lim, Johanna Magalona, Stephen Mendoza, ColeenAlexander Santiago ParelNo ratings yet
- Pneumonia Pathophysiology 3Document2 pagesPneumonia Pathophysiology 3billiam123No ratings yet
- Kap StudyDocument21 pagesKap StudyFaraz SiddiquiNo ratings yet
- Chronic Obstructive Pulmonary DiseaseDocument15 pagesChronic Obstructive Pulmonary DiseaseAlexandra T ManzanoNo ratings yet
- Benign Prostatic HyperplasiaDocument14 pagesBenign Prostatic HyperplasiaFatima Love Ariate-ArcasetasNo ratings yet
- Case Study - EmphysemaDocument6 pagesCase Study - Emphysemamackie_041992No ratings yet
- NCPDocument27 pagesNCPcuakialyannaNo ratings yet
- Acute Respiratory Distress SyndromeDocument31 pagesAcute Respiratory Distress Syndromegretchen marie100% (1)
- Geriatric For JustineDocument28 pagesGeriatric For JustineJaylord VerazonNo ratings yet
- Case Analysis On Respiratory DisordersDocument5 pagesCase Analysis On Respiratory DisordersAaron ConstantinoNo ratings yet
- CopdDocument9 pagesCopdMaria NorilynNo ratings yet
- Pneumonia Case StudyDocument3 pagesPneumonia Case StudyKayla Callahan50% (2)
- Chronic Obstructive Pulmonary DisorderDocument11 pagesChronic Obstructive Pulmonary DisorderOlivelhynn BernaldoNo ratings yet
- COPD May Include Diseases That Cause Airflow Obstruction (E.g., Emphysema, ChronicDocument13 pagesCOPD May Include Diseases That Cause Airflow Obstruction (E.g., Emphysema, Chronicmaxmay07No ratings yet
- Chronic Obstructive Pulmonary DisorderDocument15 pagesChronic Obstructive Pulmonary Disordercrabby_chicNo ratings yet
- Anatomy and Physiology CopdDocument15 pagesAnatomy and Physiology CopdAssenav MayNo ratings yet
- A Case StudyDocument23 pagesA Case StudyFritzie NagacNo ratings yet
- I.Title Chronic Obstructive Pulmonary DiseaseDocument23 pagesI.Title Chronic Obstructive Pulmonary DiseaseJessel VinluanNo ratings yet
- What Do The Lungs Do, and How Do They Function?: StructureDocument15 pagesWhat Do The Lungs Do, and How Do They Function?: StructurethenameisvijayNo ratings yet
- Anatomy and Physiology of The Respiratory SystemDocument5 pagesAnatomy and Physiology of The Respiratory SystemxoxosvwNo ratings yet
- Drug StudyDocument6 pagesDrug StudyIrveen Joy RamirezNo ratings yet
- Drug StudyDocument4 pagesDrug StudyIrveen Joy Ramirez100% (1)
- Teaching PlanDocument1 pageTeaching PlanIrveen Joy RamirezNo ratings yet
- Anti Infective AgentsDocument2 pagesAnti Infective AgentsIrveen Joy RamirezNo ratings yet
- Non Steroidal Anti InflammatoryDocument2 pagesNon Steroidal Anti InflammatoryIrveen Joy RamirezNo ratings yet
- Tri Con ExDocument1 pageTri Con ExIrveen Joy RamirezNo ratings yet
- IRVEENDocument10 pagesIRVEENIrveen Joy RamirezNo ratings yet
- Drug Study - Tetanus ToxoidDocument1 pageDrug Study - Tetanus ToxoidIrveen Joy Ramirez75% (4)
- Orthopedic Nursing Orthopedic Gadget-A Piece of Special Device Designed To Correct Deformoities or To PreserveDocument5 pagesOrthopedic Nursing Orthopedic Gadget-A Piece of Special Device Designed To Correct Deformoities or To PreserveSophia Kaye AguinaldoNo ratings yet
- Facial Lines and Wrinkles Face Reading - Crow's-Feet, Lines On Forehead, Nose, Under EyesDocument3 pagesFacial Lines and Wrinkles Face Reading - Crow's-Feet, Lines On Forehead, Nose, Under EyesUtpal KumarNo ratings yet
- Jowett OdtDocument42 pagesJowett OdtMichałNo ratings yet
- Anatomy StudyDocument124 pagesAnatomy StudyPragya ShrivastavaNo ratings yet
- Skull Connections of The Skull BonesDocument72 pagesSkull Connections of The Skull BonesBianca VaidaNo ratings yet
- Nervous System Concept MapDocument12 pagesNervous System Concept MapJo BrackenNo ratings yet
- Fascia Fundamentals E-BookDocument26 pagesFascia Fundamentals E-BookjuanNo ratings yet
- Benign Prostatic Hyperplasia: Sagittal View of Lower Urinary TractDocument1 pageBenign Prostatic Hyperplasia: Sagittal View of Lower Urinary TractLuke Rose100% (1)
- Medical and Surgical Nursing Notes For NLEDocument63 pagesMedical and Surgical Nursing Notes For NLEZhayree R.No ratings yet
- Shoulder AnatomyDocument150 pagesShoulder Anatomysrinidhi2011No ratings yet
- BRIEF 3.0 PDF Fill-In PDFDocument1 pageBRIEF 3.0 PDF Fill-In PDFSMIT SHARMANo ratings yet
- Parapharyngeal Space AnatomyDocument31 pagesParapharyngeal Space AnatomyciciNo ratings yet
- (w2) Basic Anatomical TerminologyDocument4 pages(w2) Basic Anatomical TerminologyRednaxela Mejico TarucNo ratings yet
- Ankle Block: Dr. S. Parthasarathy MD., DA., DNB, MD (Acu), Dip. Diab. DCA, Dip. Software StatisticsDocument27 pagesAnkle Block: Dr. S. Parthasarathy MD., DA., DNB, MD (Acu), Dip. Diab. DCA, Dip. Software StatisticsRajNo ratings yet
- PyelonephrolithotomyDocument2 pagesPyelonephrolithotomyJohn Bryan TuganoNo ratings yet
- Acupuncture Points - Acupuncture School Online - Learning Acupuncture and Moxibustion Courses OnlineDocument7 pagesAcupuncture Points - Acupuncture School Online - Learning Acupuncture and Moxibustion Courses Onlinecarlos coelhoNo ratings yet
- SXSXDocument27 pagesSXSXJoevany E. BigorniaNo ratings yet
- Neuro AssessmentDocument13 pagesNeuro AssessmentOrlea Francisco-Sisio100% (2)
- Class 11 Biology Chapter 20 NOTESDocument14 pagesClass 11 Biology Chapter 20 NOTESYashica PradhanNo ratings yet
- Surgery of The Auricle.52Document2 pagesSurgery of The Auricle.52Fatharani FazaNo ratings yet
- CHAPTER 12 - Coordination & ResponseDocument25 pagesCHAPTER 12 - Coordination & ResponseHAJAR LENNo ratings yet
- LKPD Describing PeopleDocument9 pagesLKPD Describing PeopleIputu ananda kiran laksamanaNo ratings yet
- Self Assessment QuestionsDocument35 pagesSelf Assessment QuestionsAli QuwarahNo ratings yet
- 100 Mcqs of AnatomyDocument13 pages100 Mcqs of Anatomydrusmansaleem100% (1)
- Trauma: Accidental Temporal Bone Fractures Classification SchemesDocument12 pagesTrauma: Accidental Temporal Bone Fractures Classification SchemesDr-Firas Nayf Al-ThawabiaNo ratings yet
- Lec8 Sem2 Hnsweek3 20110822Document9 pagesLec8 Sem2 Hnsweek3 20110822Sazter AthiraNo ratings yet
- Freelesson1endhairloss EulastversionDocument7 pagesFreelesson1endhairloss EulastversionDezant MiradzNo ratings yet
- Control and CoordinationDocument22 pagesControl and CoordinationMozibor RahmanNo ratings yet
- CH 2 Maternal AnatomyDocument70 pagesCH 2 Maternal AnatomyTengku Chairannisa PutriNo ratings yet
- Electrocardiographic Changes During Acute Mental StressDocument4 pagesElectrocardiographic Changes During Acute Mental StressVeronica JanethNo ratings yet
- Summary: The Psychology of Money: Timeless Lessons on Wealth, Greed, and Happiness by Morgan Housel: Key Takeaways, Summary & Analysis IncludedFrom EverandSummary: The Psychology of Money: Timeless Lessons on Wealth, Greed, and Happiness by Morgan Housel: Key Takeaways, Summary & Analysis IncludedRating: 5 out of 5 stars5/5 (80)
- The Obesity Code: Unlocking the Secrets of Weight LossFrom EverandThe Obesity Code: Unlocking the Secrets of Weight LossRating: 4 out of 5 stars4/5 (6)
- ADHD is Awesome: A Guide to (Mostly) Thriving with ADHDFrom EverandADHD is Awesome: A Guide to (Mostly) Thriving with ADHDRating: 5 out of 5 stars5/5 (1)
- Think This, Not That: 12 Mindshifts to Breakthrough Limiting Beliefs and Become Who You Were Born to BeFrom EverandThink This, Not That: 12 Mindshifts to Breakthrough Limiting Beliefs and Become Who You Were Born to BeRating: 2 out of 5 stars2/5 (1)
- The Age of Magical Overthinking: Notes on Modern IrrationalityFrom EverandThe Age of Magical Overthinking: Notes on Modern IrrationalityRating: 4 out of 5 stars4/5 (26)
- LIT: Life Ignition Tools: Use Nature's Playbook to Energize Your Brain, Spark Ideas, and Ignite ActionFrom EverandLIT: Life Ignition Tools: Use Nature's Playbook to Energize Your Brain, Spark Ideas, and Ignite ActionRating: 4 out of 5 stars4/5 (404)
- Summary: Outlive: The Science and Art of Longevity by Peter Attia MD, With Bill Gifford: Key Takeaways, Summary & AnalysisFrom EverandSummary: Outlive: The Science and Art of Longevity by Peter Attia MD, With Bill Gifford: Key Takeaways, Summary & AnalysisRating: 4.5 out of 5 stars4.5/5 (42)
- Raising Mentally Strong Kids: How to Combine the Power of Neuroscience with Love and Logic to Grow Confident, Kind, Responsible, and Resilient Children and Young AdultsFrom EverandRaising Mentally Strong Kids: How to Combine the Power of Neuroscience with Love and Logic to Grow Confident, Kind, Responsible, and Resilient Children and Young AdultsRating: 5 out of 5 stars5/5 (1)
- The Body Keeps the Score by Bessel Van der Kolk, M.D. - Book Summary: Brain, Mind, and Body in the Healing of TraumaFrom EverandThe Body Keeps the Score by Bessel Van der Kolk, M.D. - Book Summary: Brain, Mind, and Body in the Healing of TraumaRating: 4.5 out of 5 stars4.5/5 (266)
- Outlive: The Science and Art of Longevity by Peter Attia: Key Takeaways, Summary & AnalysisFrom EverandOutlive: The Science and Art of Longevity by Peter Attia: Key Takeaways, Summary & AnalysisRating: 4 out of 5 stars4/5 (1)
- By the Time You Read This: The Space between Cheslie's Smile and Mental Illness—Her Story in Her Own WordsFrom EverandBy the Time You Read This: The Space between Cheslie's Smile and Mental Illness—Her Story in Her Own WordsNo ratings yet
- Why We Die: The New Science of Aging and the Quest for ImmortalityFrom EverandWhy We Die: The New Science of Aging and the Quest for ImmortalityRating: 4 out of 5 stars4/5 (3)
- Cult, A Love Story: Ten Years Inside a Canadian Cult and the Subsequent Long Road of RecoveryFrom EverandCult, A Love Story: Ten Years Inside a Canadian Cult and the Subsequent Long Road of RecoveryRating: 4 out of 5 stars4/5 (44)
- Dark Psychology & Manipulation: Discover How To Analyze People and Master Human Behaviour Using Emotional Influence Techniques, Body Language Secrets, Covert NLP, Speed Reading, and Hypnosis.From EverandDark Psychology & Manipulation: Discover How To Analyze People and Master Human Behaviour Using Emotional Influence Techniques, Body Language Secrets, Covert NLP, Speed Reading, and Hypnosis.Rating: 4.5 out of 5 stars4.5/5 (110)
- Gut: the new and revised Sunday Times bestsellerFrom EverandGut: the new and revised Sunday Times bestsellerRating: 4 out of 5 stars4/5 (392)
- When the Body Says No by Gabor Maté: Key Takeaways, Summary & AnalysisFrom EverandWhen the Body Says No by Gabor Maté: Key Takeaways, Summary & AnalysisRating: 3.5 out of 5 stars3.5/5 (2)
- The Ritual Effect: From Habit to Ritual, Harness the Surprising Power of Everyday ActionsFrom EverandThe Ritual Effect: From Habit to Ritual, Harness the Surprising Power of Everyday ActionsRating: 3.5 out of 5 stars3.5/5 (3)
- The Marshmallow Test: Mastering Self-ControlFrom EverandThe Marshmallow Test: Mastering Self-ControlRating: 4.5 out of 5 stars4.5/5 (58)
- Dark Psychology: Learn To Influence Anyone Using Mind Control, Manipulation And Deception With Secret Techniques Of Dark Persuasion, Undetected Mind Control, Mind Games, Hypnotism And BrainwashingFrom EverandDark Psychology: Learn To Influence Anyone Using Mind Control, Manipulation And Deception With Secret Techniques Of Dark Persuasion, Undetected Mind Control, Mind Games, Hypnotism And BrainwashingRating: 4 out of 5 stars4/5 (1138)
- Sleep Stories for Adults: Overcome Insomnia and Find a Peaceful AwakeningFrom EverandSleep Stories for Adults: Overcome Insomnia and Find a Peaceful AwakeningRating: 4 out of 5 stars4/5 (3)
- Raising Good Humans: A Mindful Guide to Breaking the Cycle of Reactive Parenting and Raising Kind, Confident KidsFrom EverandRaising Good Humans: A Mindful Guide to Breaking the Cycle of Reactive Parenting and Raising Kind, Confident KidsRating: 4.5 out of 5 stars4.5/5 (169)
- Mindset by Carol S. Dweck - Book Summary: The New Psychology of SuccessFrom EverandMindset by Carol S. Dweck - Book Summary: The New Psychology of SuccessRating: 4.5 out of 5 stars4.5/5 (328)
- A Brief History of Intelligence: Evolution, AI, and the Five Breakthroughs That Made Our BrainsFrom EverandA Brief History of Intelligence: Evolution, AI, and the Five Breakthroughs That Made Our BrainsRating: 4.5 out of 5 stars4.5/5 (6)