Professional Documents
Culture Documents
Tarnow 2000
Uploaded by
Edu Edu0 ratings0% found this document useful (0 votes)
68 views4 pagesBone loss around implants has been well documented in the literature. Lateral bone loss measured from the crest of bone to the implant surface. Crestal bone loss for implants with a greater than 3 mm distance between them was 0. Mm. Selective utilization of smaller diameter implants may be beneficial when multiple implants are placed in the esthetic zone.
Original Description:
Original Title
Tarnow 2000 (1)
Copyright
© © All Rights Reserved
Available Formats
PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentBone loss around implants has been well documented in the literature. Lateral bone loss measured from the crest of bone to the implant surface. Crestal bone loss for implants with a greater than 3 mm distance between them was 0. Mm. Selective utilization of smaller diameter implants may be beneficial when multiple implants are placed in the esthetic zone.
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
68 views4 pagesTarnow 2000
Uploaded by
Edu EduBone loss around implants has been well documented in the literature. Lateral bone loss measured from the crest of bone to the implant surface. Crestal bone loss for implants with a greater than 3 mm distance between them was 0. Mm. Selective utilization of smaller diameter implants may be beneficial when multiple implants are placed in the esthetic zone.
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
You are on page 1of 4
Volume 71 Number 4
The Effect of Inter-Implant Distance on
the Height of Inter-Implant Bone Crest*
D.P. Tarnow, S.C. Cho, and S.S. Wallace
546
Background: The biologic width around implants has been
well documented in the literature. Once an implant is uncovered,
vertical bone loss of 1.5 to 2 mm is evidenced apical to the
newly established implant-abutment interface. The purpose of
this study was to evaluate the lateral dimension of the bone loss
at the implant-abutment interface and to determine if this lat-
eral dimension has an effect on the height of the crest of bone
between adjacent implants separated by different distances.
Methods: Radiographic measurements were taken in 36
patients who had 2 adjacent implants present. Lateral bone loss
was measured from the crest of bone to the implant surface. In
addition, the crestal bone loss was also measured from a line
drawn between the tops of the adjacent implants. The data were
divided into 2 groups, based on the inter-implant distance at
the implant shoulder.
Results: The results demonstrated that the lateral bone loss
was 1.34 mm from the mesial implant shoulder and 1.40 mm
from the distal implant shoulder between the adjacent implants.
In addition, the crestal bone loss for implants with a greater than
3 mm distance between them was 0.45 mm, while the implants
that had a distance of 3 mm or less between them had a cre-
stal bone loss of 1.04 mm.
Conclusions: This study demonstrates that there is a lateral
component to the bone loss around implants in addition to the
more commonly discussed vertical component. The clinical sig-
nicance of this phenomenon is that the increased crestal bone
loss would result in an increase in the distance between the base
of the contact point of the adjacent crowns and the crest of
bone. This could determine whether the papilla was present or
absent between 2 implants as has previously been reported
between 2 teeth. Selective utilization of implants with a smaller
diameter at the implant-abutment interface may be benecial
when multiple implants are to be placed in the esthetic zone so
that a minimum of 3 mm of bone can be retained between them
at the implant-abutment level. J Periodontol 2000;71:546-549.
KEY WORDS
Dental implants; dental implantation; bone loss; alveolar bone;
papilla.
* Department of Implant Dentistry, New York University College of Dentistry, New York, NY.
T
he existence of the biologic width
around teeth has been documented
in the literature. It was a study by
Gargiulo et al.
1
in 1961 that gave us a
dimensional understanding of this physio-
logic attachment apparatus. The average
distance from the base of the sulcus to the
crest of the bone was found to be 2.04 mm.
The epithelial attachment averaged 0.97
mm and the connective tissue attachment
averaged 1.07 mm in length. Another
cadaver study by Vacek et al.
2
in 1994 con-
rmed the consistency of these dimensions
while showing the connective tissue attach-
ment to average 0.77 mm and the epithe-
lial attachment to average 1.14 mm.
The presence of a biologic width around
implants has also been investigated. Multiple
research groups have veried that a biologic
width also exists around implants.
3-8
This is
true for implants of all shapes after uncov-
ering (stage 2) surgery. For 1-piece non-sub-
merged implants
4,7,8
or 2-stage implants
used with a single-stage non-submerged pro-
tocol, the biologic width will form at the time
of implant placement. This phenomenon is
not related to loading and it will occur
whether the implant is unloaded or loaded.
7
The biologic rationale is that the bone
exposed to the oral cavity will always cover
itself with periosteumand connective tissue.
Additionally, connective tissue will always
cover itself with epithelium. If a chronic irri-
tant, such as bacteria, reaches the implant-
abutment interface through screw-access
channels,
9-12
or if the abutment is removed
after initial healing,
6
the bone will resorb to
create a distance from this chronically
exposed or irritated area. Tarnowet al.
13
have
previously histologically documented a sim-
ilar bone response to subgingival crown
preparations that violate the attachment
apparatus on human teeth.
9046_IPC_AAP_553150 4/20/00 3:19 PM Page 546
J Periodontol April 2000 Tarnow, Cho, Wallace
Two-stage implants are usually placed at or near
the crest of bone. Once they are uncovered, an implant-
abutment interface is established and the bone resorbs
about 1.5 to 2.0 mm apically.
8
This vertical bone loss
has been well researched. The purpose of this paper
was to evaluate the lateral bone loss at the implant-
abutment connection and to see if this lateral dimen-
sion has an effect on the height of the crest of bone
between 2 implants separated by different distances.
MATERIALS AND METHODS
Thirty-six patients were utilized for this radiographic
study. These patients were part of a longitudinal study
conducted at the New York University Department of
Implant Dentistry on machined titaniumimplants. Radi-
ographic measurements were taken at a minimum of
1 and a maximum of 3 years after implant exposure.
Only areas with 2 adjacent implants were utilized for this
study. All radiographs were taken with a parallel tech-
nique utilizing a customized XCP bite block as a posi-
tioning index for consistency and reproducibility of the
radiographic images. The radiographs were computer
scanned, imaged, and magnied for measurement. Fig-
ure 1 illustrates the measurements taken for this study.
The lateral distances from the crest of the inter-
implant bone to the implants were recorded (A and B
in Fig. 1). In addition, the radiographs were divided
into 2 groups: those where the inter-implant distance
(D in Fig. 1) was 3 mm or less, and those where the
inter-implant distance was greater than 3 mm.
RESULTS
The lateral distance from the implant to the crest of the
ridge was 1.34 mm (SD = 0.36 mm) for A and 1.40
mm (SD = 0.60) for B. The crestal bone loss (C) for
implants with a 3 mm or less distance between them
(as measured by D) was 1.04 mm, while the crestal
bone loss (C) for implants that were more than 3.0
mm apart was 0.45 mm. These data are presented in
Table 1.
DISCUSSION
These ndings demonstrate two important facts. The
rst is that there is a lateral component to the bone loss
after abutment connection of a 2-stage implant. The
second is that this lateral component of bone loss can
result in greater inter-implant crestal bone loss if the
two implants are not spaced more than 3 mm apart
(measurement D). The lateral dimension of the defect
is readily observed in Figures 2 and 3.
547
Figure 1.
Radiographic measurements recorded. A and B represent the lateral
distance (bone loss) from the implant to bone crest; C, vertical crestal
bone loss; and D, the distance between implants at the implant-
abutment interface.
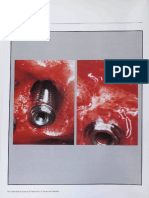
Figure 2.
Inter-implant distance greater than 3 mm. Lateral bone loss from
adjacent implants (A and B from Figure 1) does not overlap, with
minimal resultant crestal bone loss (C from Figure 1).
Table 1.
Recorded Data for Lateral and Crestal Bone
Loss (see Figure 1)
Bone Loss (mm)
Lateral A (n = 36) B (n = 36)
Mean 1.34 1.40
SD () 0.36 0.60
Bone Loss (mm)
Crestal D C
3 mm (n = 25) 1.04
>3 mm (n = 11) 0.45
9046_IPC_AAP_553150 4/20/00 3:19 PM Page 547
Inter-Implant Distance in the Alveolar Bone Crest Volume 71 Number 4
In 1978 Waerhaug
14
demonstrated that there was a
1.78 mm distance between plaque on teeth and the
surrounding bone. In addition, in 1984 Tal
15
examined
the presence or absence of intrabony defects when
roots were at different distances apart. It is interesting
to note that the minimum distance between roots for
2 separate angular defects to be present on adjacent
teeth was 3.l mm. In other words, the lateral aspect of
each angular defect appears to be at least 1.55 mm
on each root. This distance correlates with the present
nding of 1.34 mm and 1.40 mm of bone loss (Fig.
1A and B, respectively) in the lateral direction from an
implant to the crest of bone.
Separating the data into 2 groups, with the inter-
implant distance of the rst group being 3 mm or less
and that of the second group being greater than 3 mm,
was based on the hypothesis that 2 adjoining implants
with 3 mm or less of separation should have increased
inter-implant bone loss as a result of the horizontal
distance that bone will be lost on each side of the inter-
implant crest. The scatter graph shown in Figure 4
demonstrates the clear trend of increased crestal bone
loss as the inter-implant distance decreases.
CONCLUSIONS
This paper demonstrates that there is a lateral com-
ponent to the bone loss around implants once the bio-
logic width has formed.
The clinical signicance of this phenomenon is that
the increased crestal bone loss results in an increase
in the distance between the base of the contact point
of the adjacent crowns and the crest of bone. This
could determine whether the papilla will be present or
absent between 2 implants, as has been reported by
Tarnow et al.,
16
between 2 teeth. In that study, a small
difference of 1 mm was clinically signicant. When the
distance from the contact point to the crest was 5 mm,
the papilla was almost always present. When this dis-
tance increased to 6 mm, the papilla completely lled
the embrasure space in only 55% of the observed
cases.
It is commonly observed that it is more difcult to
maintain or create a papilla between 2 adjacent
implants than it is to maintain or create the papilla
between an implant and a natural tooth. This may indi-
cate that the selective utilization of implants with a
smaller diameter at the implant-abutment interface
may be benecial when multiple implants are to be
placed in the esthetic zone so that a minimum of 3
mm of bone can be retained between them at the
implant-abutment level. It may also indicate that wide-
bodied implants adjacent to one another may be of
limited use in the esthetic zone, since they would dimin-
ish the inter-implant distance and potentially lead to
increased crestal resorption. Measurements are pres-
ently underway to evaluate whether the papillae are
affected by this crestal resorption between adjacent
implants.
REFERENCES
1. Gargiulo AW, Wentz FM, Orban B. Dimensions and rela-
tions of the dentogingival junction in humans. J Peri-
odontol 1961;32:261-267.
2. Vacek JS, Gher ME, Assad DA, Richardson AC,
Giambarresi LI. The dimensions of the human den-
togingival junction. Int J Periodontics Restorative Dent
1994;14:155-165.
3. Berglundh T, Lindhe J, Ericsson I, Marinello CP, Liljen-
berg B, Thomsen P. The soft tissue barrier at implants
and teeth. Clin Oral Implants Res 1991;2:81-90.
4. Buser D, Weber HP, Donath K, Fiorellini JP, Paquette
DW, Williams RC. Soft tissue reactions to non-submerged
unloaded titanium implants in beagle dogs. J Periodon-
tol 1992;63:226-236.
548
Figure 3.
Inter-implant distance 3 mm or less. Lateral bone loss from adjacent
implants (A and B from Figure 1) overlap, with resultant increase in
crestal bone loss (C from Figure 1).
Figure 4.
Relationship between crestal bone loss and inter-implant distance (see
Figure 1).
9046_IPC_AAP_553150 4/20/00 3:20 PM Page 548
J Periodontol April 2000 Tarnow, Cho, Wallace
5. Abrahamsson I, Berglundh T, Wennstrom J, Lindhe J.
The peri-implant hard and soft tissues at different implant
systems. Clin Oral Implants Res 1996;7:212-219.
6. Abrahamsson I, Berglundh T, Lindhe J. The mucosal
barrier following abutment disconnection. An experi-
mental study in dogs. J Clin Periodontol 1997;24:568-
572.
7. Cochran DL, Hermann JS, Schenk RK, Higgenbottom
FL, Buser D. Biologic width around titanium implants. A
histometric analysis of the implanto-gingival junction
around unloaded and loaded non-submerged implants in
the canine mandible. J Periodontol 1997;68:186-198.
8. Hermann JS, Cochran DL, Nummikoski PV, Buser D.
Crestal bone changes around titanium implants. A radi-
ographic evaluation of unloaded non-submerged and
submerged implants in the canine mandible. J Peri-
odontol 1997;68:1117-1130.
9. Berglundh T, Lindhe J, Marinello C, Ericsson I, Liljenberg
B. Soft tissue reaction to de novo plaque formation on
implants and teeth. An experimental study in the dog.
Clin Oral Implants Res 1992;3:1-8.
10. Traversy MC, Birek P. Fluid and microbial leakage of
implant-abutment assembly in vitro. J Dent Res 1992:
71(Spec. Issue):54(Abstr. 1909).
11. Quirynen M, van Steenberghe D. Bacterial colonization
of the internal part of 2-stage implants. Clin Oral
Implants Res 1993;4:158-161.
12. Jansen VK, Conrads G, Richter E. Microbial leakage and
marginal t of the implant-abutment interface. Int J Oral
Maxillofac Implants 1997;12:527-540.
13. Tarnow D, Stahl SS, Magner A, Zamzock J. Human gin-
gival attachment responses to subgingival crown place-
ment. Marginal remodeling. J Clin Periodontol 1986;
13:563-569.
14. Waerhaug J. Healing of the dento-epithelial junction fol-
lowing subgingival plaque control. II: As observed on
extracted teeth. J Periodontol 1978;49:119-134.
15. Tal H. Relationship between the interproximal distance
of roots and the prevalence of intrabony pockets. J Peri-
odontol 1984;55:604-607.
16. Tarnow DP, Magner AW, Fletcher P. The effect of the
distance from the contact point to the crest of bone on
the presence or absence of the interproximal dental
papilla. J Periodontol 1992;63:995-996.
Send reprint requests to: Dr. Dennis Tarnow, 205 E. 64th
Street, Suite 402, New York, NY 10021. Fax: 212/754-6753.
Accepted for publication August 19, 1999.
549
9046_IPC_AAP_553150 4/20/00 3:20 PM Page 549
You might also like
- Peri-Implant Soft Tissue and Marginal Bone Adaptation On Implant With Non-Matching Healing Abutments: micro-CT AnalysisDocument5 pagesPeri-Implant Soft Tissue and Marginal Bone Adaptation On Implant With Non-Matching Healing Abutments: micro-CT AnalysisOswaldo VillaNo ratings yet
- Palaska 2014Document10 pagesPalaska 2014Marco TeixeiraNo ratings yet
- RetrieveDocument13 pagesRetrieveBruno MañonNo ratings yet
- CatalogoDocument7 pagesCatalogoIsabela Campos SánchezNo ratings yet
- Micromotion Analysis of Different Implant Configuration, Bone Density, and Crestal Cortical Bone Thickness in Immediately Loaded Mandibular Full ADocument7 pagesMicromotion Analysis of Different Implant Configuration, Bone Density, and Crestal Cortical Bone Thickness in Immediately Loaded Mandibular Full ABagis Emre GulNo ratings yet
- Cohen 2019Document12 pagesCohen 2019Jarvin Miguel Buitrago GalindezNo ratings yet
- Crestal Bone Changes On Platform - Switched Implants and Adjacent Teeth When The Tooth-Implant Distance Is Less Than 1.5 MMDocument10 pagesCrestal Bone Changes On Platform - Switched Implants and Adjacent Teeth When The Tooth-Implant Distance Is Less Than 1.5 MMJuanOso Gutierrez ArayaNo ratings yet
- Ultrasonic Versus Drills Implant Site Preparation: A Histologic Analysis in Bovine RibsDocument4 pagesUltrasonic Versus Drills Implant Site Preparation: A Histologic Analysis in Bovine RibsAnusha BorraNo ratings yet
- The Platform Switching Concept-A Myth or Fact: A Literature ReviewDocument5 pagesThe Platform Switching Concept-A Myth or Fact: A Literature ReviewChifa MusrataNo ratings yet
- Sugical Management of Long Bone Fracture by String of Pearl Locking PlateDocument8 pagesSugical Management of Long Bone Fracture by String of Pearl Locking PlateInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- Influence of Implant Positions and Occlusal Forces On Peri-Implant Bone Stress in Mandibular Two-Implant Overdentures A 3-Dimensional Finite Element AnalysisDocument10 pagesInfluence of Implant Positions and Occlusal Forces On Peri-Implant Bone Stress in Mandibular Two-Implant Overdentures A 3-Dimensional Finite Element AnalysisJavier MaldonadoNo ratings yet
- Effect of Thread Size On The Implant Neck Area Preliminary Results at 1 Year of FunctionDocument6 pagesEffect of Thread Size On The Implant Neck Area Preliminary Results at 1 Year of FunctionSergio Lamas RamirezNo ratings yet
- FAI.2007.0529Document7 pagesFAI.2007.0529milenabogojevskaNo ratings yet
- Ijomi 2017 Vol 32 P 1296 1307Document12 pagesIjomi 2017 Vol 32 P 1296 1307John MacioNo ratings yet
- Zero bone loss around implants possible with soft tissue augmentationDocument4 pagesZero bone loss around implants possible with soft tissue augmentationmarwaNo ratings yet
- Immediate One-Stage Postextraction Implant: A Human Clinical and Histologic Case ReportDocument6 pagesImmediate One-Stage Postextraction Implant: A Human Clinical and Histologic Case ReportBagis Emre GulNo ratings yet
- (2010 Weng) Influence of Microgap Location and Configuration On Peri-Implant Bone Morphology in Nonsubmerged Implants - An Experimental Study in DogsDocument8 pages(2010 Weng) Influence of Microgap Location and Configuration On Peri-Implant Bone Morphology in Nonsubmerged Implants - An Experimental Study in Dogsyena1010No ratings yet
- Anemark 1969-2-2 (02-07)Document6 pagesAnemark 1969-2-2 (02-07)Carolina Dávila RamírezNo ratings yet
- Archives of Oral Biology: ReviewDocument8 pagesArchives of Oral Biology: Reviewformula marolisNo ratings yet
- Australian Dental Journal - 2018 - Spencer - Implant Based Rehabilitation Options For The Atrophic Edentulous JawDocument8 pagesAustralian Dental Journal - 2018 - Spencer - Implant Based Rehabilitation Options For The Atrophic Edentulous JawAswathi RaghuthamanNo ratings yet
- Abuhussein2010 PDFDocument8 pagesAbuhussein2010 PDFJimmy Bryan Caparachini GuerreroNo ratings yet
- Guided Tissue Regeneration For Implants Placed Into Extraction Sockets and For Implant Dehiscences - Surgical Techniques and Case ReportDocument17 pagesGuided Tissue Regeneration For Implants Placed Into Extraction Sockets and For Implant Dehiscences - Surgical Techniques and Case ReportEugenioNo ratings yet
- Reconstrução de Severa Reabsorção Maxilar Com Distração OsteogenicaDocument7 pagesReconstrução de Severa Reabsorção Maxilar Com Distração OsteogenicaNelson UzunNo ratings yet
- Right To PrivacyDocument6 pagesRight To PrivacymelovebeingmeNo ratings yet
- (2008 Weng) Influence of Microgap Location and Configuration On The Periimplant Bone Morphology in Submerged Implants. An Experimental Study in DogsDocument7 pages(2008 Weng) Influence of Microgap Location and Configuration On The Periimplant Bone Morphology in Submerged Implants. An Experimental Study in Dogsyena1010No ratings yet
- Lib artRetroCliEvalTSVDocument12 pagesLib artRetroCliEvalTSVSaravanan MaxNo ratings yet
- Biologic Width and ImplantsDocument8 pagesBiologic Width and ImplantsShruti Maroo - RathiNo ratings yet
- OsseointegrationDocument58 pagesOsseointegrationnakul ware100% (5)
- Clinical Outcomes of Ultrashort Sloping Shoulder Implant Design A Survival AnalysisDocument7 pagesClinical Outcomes of Ultrashort Sloping Shoulder Implant Design A Survival AnalysisBagis Emre GulNo ratings yet
- Tarrson Family Endowed Chair in PeriodonticsDocument54 pagesTarrson Family Endowed Chair in PeriodonticsRobins DhakalNo ratings yet
- W5 TarnowDocument4 pagesW5 TarnowAdit VekariaNo ratings yet
- 1 s2.0 S1991790219308700 MainDocument6 pages1 s2.0 S1991790219308700 MainRonin ZxxNo ratings yet
- Alveolar Bone Preservation Subsequent To Miniscrew Implant Placement in A Canine ModelDocument9 pagesAlveolar Bone Preservation Subsequent To Miniscrew Implant Placement in A Canine ModelSamuel OtavioNo ratings yet
- Detolla 2000Document5 pagesDetolla 2000guptaamitalwNo ratings yet
- Influence of Thin Mucosal Tissues On Crestal Bone Stability Around Implants With Platform Switching: A 1-Year Pilot StudyDocument6 pagesInfluence of Thin Mucosal Tissues On Crestal Bone Stability Around Implants With Platform Switching: A 1-Year Pilot StudyPedro Maria Crizul BarretoNo ratings yet
- Jpis 42 105Document5 pagesJpis 42 105Jean Pierre Alcántara VigoNo ratings yet
- Articulo en Inglés 2Document8 pagesArticulo en Inglés 2Luis Ramirez BenaventeNo ratings yet
- TMP 50 FDDocument8 pagesTMP 50 FDFrontiersNo ratings yet
- Alargamento Coronario en Zonas EsteticasDocument9 pagesAlargamento Coronario en Zonas EsteticasCamila BórquezNo ratings yet
- 1 s2.0 S199179021930460X MainDocument6 pages1 s2.0 S199179021930460X MainPanaite TinelaNo ratings yet
- The Influence of Soft Tissue Thickness On Crestal Bone ChangesDocument9 pagesThe Influence of Soft Tissue Thickness On Crestal Bone ChangesFrancisco VargasNo ratings yet
- Ellis 1991Document9 pagesEllis 1991Harshitha RajannaNo ratings yet
- Upper Extremity Amputations and Prosthetics: Steven A. Ovadia, MD Morad Askari, MDDocument7 pagesUpper Extremity Amputations and Prosthetics: Steven A. Ovadia, MD Morad Askari, MDprovaNo ratings yet
- Marzadori2018 PDFDocument9 pagesMarzadori2018 PDFMel LlerenaNo ratings yet
- Analysis of Strain at Selected Bone Sites of A Cantilevered Implant-Supported ProsthesisDocument7 pagesAnalysis of Strain at Selected Bone Sites of A Cantilevered Implant-Supported ProsthesisMR GOKCHENNo ratings yet
- Three-Dimensional Bone and Soft Tissue Requirements For Optimizing Esthetic Results in Compromised Cases With Multiple ImplantsDocument10 pagesThree-Dimensional Bone and Soft Tissue Requirements For Optimizing Esthetic Results in Compromised Cases With Multiple ImplantsYu Yu Victor Chien100% (1)
- Aaid Joi D 14 00023Document6 pagesAaid Joi D 14 00023MohamedAtefNo ratings yet
- Biologic width significance for implant dentistryDocument8 pagesBiologic width significance for implant dentistryaakanksha bhardwajNo ratings yet
- The Effect of SplintingDocument8 pagesThe Effect of SplintingVictor Manuel RevelloNo ratings yet
- JIAP January 2010 - Summers' Technique Modification For Sinus Floor Elevation Using A Connective Tissue Graft. A Case Report.Document4 pagesJIAP January 2010 - Summers' Technique Modification For Sinus Floor Elevation Using A Connective Tissue Graft. A Case Report.Dr. Silviu Andrei ConstantinescuNo ratings yet
- Ijomi 15 193 PDFDocument4 pagesIjomi 15 193 PDFBagis Emre GulNo ratings yet
- Flap SurgeryDocument128 pagesFlap SurgerycoldmailhotmailNo ratings yet
- ReviewDocument6 pagesReviewArchana SrinivasanNo ratings yet
- 2-Referencias y Tecnicas Usadas en Clasificacion Hueso Alveolar - SeriwatanachaiDocument5 pages2-Referencias y Tecnicas Usadas en Clasificacion Hueso Alveolar - SeriwatanachaimnhjrtbnzbNo ratings yet
- Biologic Width: Understanding and Its Preservation: Review ArticleDocument6 pagesBiologic Width: Understanding and Its Preservation: Review ArticleMedstudNo ratings yet
- A New Definition ofDocument16 pagesA New Definition ofDiverse AnunturiNo ratings yet
- J Jds 2019 12 003Document6 pagesJ Jds 2019 12 003aDITYA GUJARENo ratings yet
- Histologic Comparison of Biologic Width Around Teeth Versus Implants: The Effect On Bone PreservationDocument5 pagesHistologic Comparison of Biologic Width Around Teeth Versus Implants: The Effect On Bone PreservationPaul CerdaNo ratings yet
- Short ImplantsFrom EverandShort ImplantsBoyd J. TomasettiNo ratings yet
- Orthodontically Driven Corticotomy: Tissue Engineering to Enhance Orthodontic and Multidisciplinary TreatmentFrom EverandOrthodontically Driven Corticotomy: Tissue Engineering to Enhance Orthodontic and Multidisciplinary TreatmentFederico BrugnamiNo ratings yet
- Soft tissue cephalometric norms for North Indians using Legan and Burstone analysisDocument5 pagesSoft tissue cephalometric norms for North Indians using Legan and Burstone analysisjoseph nNo ratings yet
- Content ServerDocument9 pagesContent ServerZAIDA BERNAL BECERRANo ratings yet
- chard I Iedel, Seattle, Wash.: The HuronDocument17 pageschard I Iedel, Seattle, Wash.: The Huronjoseph nNo ratings yet
- Arnett - Soft Tissue Cephalometric AnalysisDocument15 pagesArnett - Soft Tissue Cephalometric AnalysisVicente Contreras100% (1)
- Soft Tissue Cephalometric Norms For Orthognathic SurgeryDocument6 pagesSoft Tissue Cephalometric Norms For Orthognathic Surgeryjoseph nNo ratings yet
- Joseph R. Jarabak-A Living LegendDocument2 pagesJoseph R. Jarabak-A Living Legendjoseph n100% (1)
- Autism Spectrum Disorders: An Update on Oral Health ManagementDocument12 pagesAutism Spectrum Disorders: An Update on Oral Health Managementjoseph nNo ratings yet
- 10 1093ejocjq028Document9 pages10 1093ejocjq028joseph nNo ratings yet
- "Are We Similar To Caucasians" - Orthognathic Surgery For North IndiansDocument7 pages"Are We Similar To Caucasians" - Orthognathic Surgery For North Indiansjoseph nNo ratings yet
- CONSENSO JBMR. Diagnosis and Management of Osteonecrosis of The Jaw.Document21 pagesCONSENSO JBMR. Diagnosis and Management of Osteonecrosis of The Jaw.joseph nNo ratings yet
- Funato PDFDocument12 pagesFunato PDFjoseph nNo ratings yet
- Interdisciplinary Treat Planning ChapterDocument56 pagesInterdisciplinary Treat Planning ChapterJulio César Huayllasco de la Cruz0% (1)
- Mock-Ups Help With Demanding PatientsDocument4 pagesMock-Ups Help With Demanding Patientsjoseph nNo ratings yet
- CoachmanDocument10 pagesCoachman881971100% (3)
- Interdisciplinary Management of Anterior Dental EstheticsDocument11 pagesInterdisciplinary Management of Anterior Dental Estheticsjoseph nNo ratings yet
- Managing Bone FracturesDocument2 pagesManaging Bone FracturesMa. Ferimi Gleam BajadoNo ratings yet
- General Surgery 2002Document50 pagesGeneral Surgery 2002Breyner De Jesus García RodríguezNo ratings yet
- Pathology Reporting of Breast Cancer A GuideDocument52 pagesPathology Reporting of Breast Cancer A Guidewht36No ratings yet
- Prone PositionDocument7 pagesProne PositionLyka Lhianne IbañezNo ratings yet
- Collagen Film DressingDocument2 pagesCollagen Film DressingRadiika BalamuruganNo ratings yet
- AOMSI MC2022 ScheduleDocument10 pagesAOMSI MC2022 ScheduleDarain ShahidNo ratings yet
- Acute Urinary RetentionDocument28 pagesAcute Urinary RetentionJuan JoséNo ratings yet
- Investigation On Gastrointestinal Tract A ReviewDocument6 pagesInvestigation On Gastrointestinal Tract A ReviewHafidz Ma'rufNo ratings yet
- NCLEX Drugs CalculationDocument3 pagesNCLEX Drugs CalculationajhienngNo ratings yet
- Lec Framework Care of MotherDocument27 pagesLec Framework Care of MotherRica ParcasioNo ratings yet
- Colon Interposition For Esophageal ReconstructionDocument11 pagesColon Interposition For Esophageal ReconstructionDelcu MarinicaNo ratings yet
- Fourniers Gangrene of The External Genitalia: Plastic Reconstruction by Thin Skin GraftDocument7 pagesFourniers Gangrene of The External Genitalia: Plastic Reconstruction by Thin Skin GraftIJAR JOURNALNo ratings yet
- GUIDE INTENSIVE CARE SOCIETY WEANINGDocument4 pagesGUIDE INTENSIVE CARE SOCIETY WEANINGdeliejoyceNo ratings yet
- 1 PBDocument8 pages1 PBMahathir Harry PermanaNo ratings yet
- Tabel KodingDocument82 pagesTabel KodingfaisaldanyaniNo ratings yet
- Set PedDocument11 pagesSet PedechaNo ratings yet
- Nuclear Cardiology: Dr. Tarek HiderDocument31 pagesNuclear Cardiology: Dr. Tarek HiderMuneeb JanNo ratings yet
- Case Study 39-Year-Old Women Diagnosed As Solitary Rectal Ulcer SyndromeDocument5 pagesCase Study 39-Year-Old Women Diagnosed As Solitary Rectal Ulcer SyndromeInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- Secure Your Family Against Uncertainties, With A Plan That Adjusts To Your NeedsDocument25 pagesSecure Your Family Against Uncertainties, With A Plan That Adjusts To Your Needsroxcox216No ratings yet
- CABGDocument41 pagesCABGJasmin Jacob100% (2)
- DiastologiaDocument10 pagesDiastologiaReinaldo Pacheco VásquezNo ratings yet
- Neurologica L Assessment: Lijo Joseph Msc. Nursing Ist YrDocument38 pagesNeurologica L Assessment: Lijo Joseph Msc. Nursing Ist YrBibi Renu100% (2)
- Chapter 8 Self-Assessment Q&ADocument5 pagesChapter 8 Self-Assessment Q&Apblinder1319No ratings yet
- Histology of The Upper GITDocument43 pagesHistology of The Upper GITBenedict OkotNo ratings yet
- Psychological Interventions To Reduce Postoperative Pain and Opioid Consumption: A Narrative Review of LiteratureDocument38 pagesPsychological Interventions To Reduce Postoperative Pain and Opioid Consumption: A Narrative Review of LiteraturedrsubramanianNo ratings yet
- Process of Rapifd PrototypingDocument3 pagesProcess of Rapifd Prototypingpooja rohondiaNo ratings yet
- Vascular Supply To The BrainDocument38 pagesVascular Supply To The BrainGhea Putri HendrianiNo ratings yet
- New England Journal Medicine: The ofDocument11 pagesNew England Journal Medicine: The ofnenda nurfendaNo ratings yet
- Lumbar Hernia: Anatomical Basis and Clinical AspectsDocument5 pagesLumbar Hernia: Anatomical Basis and Clinical AspectsAlejandra PereyraNo ratings yet
- Levo-Milri 2021Document7 pagesLevo-Milri 2021Fer AlmazanNo ratings yet