Professional Documents
Culture Documents
Case 9: Deep Vein Thrombosis
Uploaded by
introvoyz0410 ratings0% found this document useful (0 votes)
736 views5 pages- L.J., a 70-year-old retired bus driver, was admitted with right deep vein thrombosis (DVT). He has a history of smoking, pneumonia, atrial fibrillation, and previous DVTs.
- He reported swelling in his right leg that progressed over two months. A Doppler study confirmed a thrombus in his right leg vein.
- He was admitted to begin treatment with bed rest, heparin therapy, and monitoring to prevent pulmonary embolism complications.
Original Description:
Cardiovascular disorders: Deep Vein Thrombosis Case Study
Copyright
© © All Rights Reserved
Available Formats
DOCX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this Document- L.J., a 70-year-old retired bus driver, was admitted with right deep vein thrombosis (DVT). He has a history of smoking, pneumonia, atrial fibrillation, and previous DVTs.
- He reported swelling in his right leg that progressed over two months. A Doppler study confirmed a thrombus in his right leg vein.
- He was admitted to begin treatment with bed rest, heparin therapy, and monitoring to prevent pulmonary embolism complications.
Copyright:
© All Rights Reserved
Available Formats
Download as DOCX, PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
736 views5 pagesCase 9: Deep Vein Thrombosis
Uploaded by
introvoyz041- L.J., a 70-year-old retired bus driver, was admitted with right deep vein thrombosis (DVT). He has a history of smoking, pneumonia, atrial fibrillation, and previous DVTs.
- He reported swelling in his right leg that progressed over two months. A Doppler study confirmed a thrombus in his right leg vein.
- He was admitted to begin treatment with bed rest, heparin therapy, and monitoring to prevent pulmonary embolism complications.
Copyright:
© All Rights Reserved
Available Formats
Download as DOCX, PDF, TXT or read online from Scribd
You are on page 1of 5
Case 9: Deep Vein Thrombosis
- L.J., 70 y/o retired bus driver admitted with Right DVT
- Has 48 pack year smoking history, quitted 2 years ago
- Has had pneumonia several times and frequent episodes of A-fib
- 2 previous episodes of DVT and was diagnosed with rheumoid arthritis 3 years ago
- HPI: 2 mos ago he began experiencing SOB on exertion and noticed swelling of his R foreleg that
became progressively worse until it involved his thigh to the groin
- SO: wife, who brought LJ to the hospital when he c/o increasingly severe pain in his leg
- Doppler study indicated a probable thrombus vein extending distally to the lower leg
- Admitted for bed rest and to initiate heparin therapy
- Lab values : PT 12.4, INR 1.11, PTT 25 sec, Hgb 13.3 g/dl Hct 38.9, cholesterol 206 mg/dl. BMP is
normal
Deep Vein Thrombosis
description
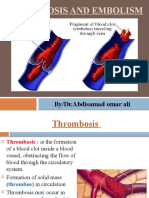
A blood clot (thrombus) that forms inside a deep vein. It may partially or completely block blood
flow, or it could break off and travel to the lung. Deep vein thrombosis often occurs in the lower
legs (calves). Less often it occurs in the arm or pelvis.
causes
Pooling of blood in the vein, which triggers blood-clotting mechanisms. The pooling may occur
after prolonged bed rest, following surgery, or from long-lasting illness, such as heart attack,
stroke, or bone fracture.
risk increases with
Persons over 60.
Obesity.
Smoking.
Surgery and surgery recovery.
Cancer, heart failure, stroke, and polycythemia.
Bed rest for an extended time, burns, or injuries.
Blood disorders that increase the risk of blood clots.
Signs and Symptoms
Oedema
Calf pain
Tenderness
Swelling
Increased skin temperature
Engorgement of superficial leg veins
Slight fever
Positive Homans sign (discomfort in calf muscles on forced dorsiflexion
Initial assessment by observation and examination
Observation
Observe and record skin colour. Compare with unaffected side.
Is the area swollen? Compare with unaffected side.
Is oedema present?
Is the area painful? Check for pain at rest or on movement.
Is the area reddened? Compare with unaffected side.
Are any wounds present? If so, how long have they been present? Have they been
treated? By whom?
Physical examination
Check and record presence of distal pulses on the affected limb and compare with the
unaffected side.
Check and record heart rate, respiratory rate and depth, blood pressure and
temperature.
Is the area hot? Compare with unaffected side.
Palpate the area for pain or tenderness. Compare with the unaffected side.
Check for range of movement of proximal and distal joints. Does this increase pain?
Can the patient walk normally on the affected limb(s)?
Information to be collected during history taking
Information to be collected verbally
History of present problem:
How long has it been present?
When did it start?
Is it constant or intermittent?
Is it worse today than usual?
Is there any previous history of same or similar problem?
Is there any recent history of injury to the affected area?
Has there been any recent long distance travel (>4 hours) in last 4 weeks?
Has there been any previous surgery especially orthopaedic, pelvic or abdominal?
Is the area painful? If so, does anything relieve the pain or make it worse?
Has any medication been taken to relieve the problem?
Immediate management and investigations
Patients with suspected DVT are nursed on a stretcher-trolley, in a bed or
in a chair. Elevate the affected leg with some flexion of the knee (to
encourage venous drainage) and support it on a pillow in the position most
comfortable for the patient. Take a history (Boxes 11.2 and 11.3), measure
vital signs, gain intravenous (IV) access and take bloods for full blood count
(FBC), urea, electrolytes and clotting screen. In addition, oxygen
saturation may be measured and oxygen given if required. Measurement
of calf circumferences to provide a baseline for further evaluation may be
carried out 10 cm below the tibial tuberosity. A swelling of 3 cm greater
than the asymptomatic side is a relative indicator of DVT but is not
definitive. Application of graded compression stockings can reduce postthrombotic
syndrome by up to 60% (Gorman et al 2000). Explain
procedures to the patient and assess their potential for early discharge.
The principle of managing patients with a DVT is early initiation of
effective anticoagulant therapy with the aim of preventing further progression of the
thrombosis to the proximal veins and, thereby,
pulmonary embolism. Given that diagnosis on the basis of clinical features
is often inconclusive, management of suspected DVT is based on the
results obtained from one or more objective diagnostic investigations. To
support this, clinical risk factors (Box 11.1) are also assessed and taken into
account, as confirmation rates of DVT rise with the number of factors
present. Identification of an underlying cause, if present, will also guide the
treatment and prevention of further episodes (Gorman et al 2000).
The standard radiographic investigation for DVT is contrast
venography (Gorman et al 2000) but the painful, invasive nature of this
procedure, its technical difficulty and the time taken for completion make
it inappropriate for use in acute settings. Technological advances in recent
years have led to the introduction of non-invasive ultrasonography as a
first-line investigation for DVTs. Known as pulsed Doppler ultrasound,
this technique measures the velocity of moving objects (such as red blood
cells) in comparison to other objects.
Rapid, effective anticoagulant therapy is important in the initial
management of DVT. Treatment usually starts with an intravenous dose
of heparin (5000 units) followed by subcutaneous low molecular weight
heparin (LMWH) for 5 days. LMWH has been shown to be at least as
effective as the traditionally used unfractionated heparin in preventing
recurrent venous thromboembolism. In addition, it significantly reduces
the occurrence of major haemorrhage during initial treatment and
reduces overall mortality at the end of the patients follow-up period (van
den Belt et al 2000). Oral warfarin is usually started on day 1 with the dose
determined by algorithm.
The Wells clinical prediction guide for DVT (Anand et al 1998)
Clinical feature Score
Active cancer (treatment ongoing or within 6 months or palliative) 1
Paralysis, paresis or plaster of Paris on lower leg 1
Recently bedridden >3 days or major surgery within 4 weeks 1
Localised tenderness along distribution of deep vein system 1
Calf diameter >3 cm larger than the asymptomatic leg* 1
Pitting oedema 1
Entire swollen leg 1
Collateral superficial veins (non-varicose) 1
Alternative diagnosis (as likely or greater than that of DVT) 2
Adding the scores with a total as follows indicates probability of DVT:
0 = low probability = 3% frequency of DVT
12 = medium probability = 17% frequency of DVT
3+ = high probability = 75% frequency of DVT
*Measured 10 cm below tibial tuberosity
Ongoing assessment and treatment
Gorman et al (2000) suggest that the patients activated partial
thromboplastin time (aPTT) is checked every 6 hours until the target of
1.52.5 is reached or according to a heparin algorithm. Once reached, this
should be checked daily to maintain this range. Platelet count should also
be measured at the start of treatment and on day 5 to rule out
thrombocytopenia. Duration of treatment for DVT varies from 3 to 12
months depending upon the risk of recurrence of thrombosis.
Many patients who are referred with DVT can be discharged once
initial investigations and treatment have been completed. Pout et al (1999)
give an example of how a nurse-led outpatient clinic has successfully been
introduced to treat patients with daily doses of LMWH. This approach has
been adopted in other centres with the aim of improving the service to
patients and relieving pressure on individual MAUs
COMPLICATION
Pulmonary Embolism
2. Symptoms: dyspnea (73%), pleuritic pain (66%), cough (37%), leg pain or swelling (27%), hemoptysis
(13%), lightheadedness, loss of consciousness.
3. Signs: tachypnea (~80%), tachycardia (~80%), rales (51%), S4, loud P2, elevated JVP, fever.
4. Work-up: Always think of PE in patients with new or unexplained dyspnea and/or hypoxemia. Studies
should include:
CXR: abnormal in 84% but non-specific: atelectasis, effusion, basilar opacity, elevated diaphragm,
Westermarks sign (focal decreased pulmonary vessel perfusion), Hamptons hump (peripheral wedge
shaped density).
ECG: sinus tachycardia, S1Q3T3, right axis-deviation, RBBB, T wave inversions of V1-4, a-fib/flutter.
ABG: mean PaO2 70mmHg, < 60 (25%), < 80 (74%). Normal ABG does not rule out PE if clinical
suspicion high.
D-Dimer: if ELISA test available, a low result has an extremely high negative predictive value.
Spiral CT, V/Q Scan, LE doppler ultrasound. Echo can be useful in massive PE.
Treatment
Unfractionated heparin:
Low molecular weight heparin (enoxaparin): preferred treatment for ease of use; dose at 1mg/kg q12h
SQ. Continue for ~5 days, until INR is therapeutic (2.0-3.0) on warfarin. Relative contraindication if CrCl <
30 ml/min or weight > 120 kg. Can follow anti-factor Xa levels if available.
Warfarin: start when patient is stable (which may be on admission).
Thrombolytics: consider in massive PE with hemodynamic compromise (call pulmonary consult). Stop
heparin and dose tPA at 100 mg IV over 2 hours. Can use up to 14 days after initial onset of PE. Obtain
consent, review exclusion criteria, monitor frequently for neuro changes, and know full tPA protocol if you
are going to proceed to thrombolysis.
IVC filter: in patients who develop PE while anticoagulated, or in patients in whom anticoagulation is
contraindicated (recent surgery, CVA). Not effective as long-term treatment.
Start hypercoagulability workup when appropriate (i.e., when common risk factors are absent).
You might also like
- Case Presentation DVTDocument26 pagesCase Presentation DVTimad mokalledNo ratings yet
- Deep Vein ThrombosisDocument33 pagesDeep Vein ThrombosisWisnu Cahyo100% (1)
- Deep Vein ThrombosisDocument22 pagesDeep Vein ThrombosisEznal MahidinNo ratings yet
- Deep Vein ThrombosisDocument12 pagesDeep Vein ThrombosisJohn Jacob100% (1)
- Deep Vein ThrombosisDocument13 pagesDeep Vein Thrombosisusmle prepNo ratings yet
- Acute AppendicitisDocument2 pagesAcute AppendicitisnasibdinNo ratings yet
- Dengue FeverDocument26 pagesDengue FeverathulpjoseNo ratings yet
- Thrombosis and EmbolismDocument20 pagesThrombosis and EmbolismSAKARIYE MAXAMEDNo ratings yet
- Deep Vein ThrombosisDocument9 pagesDeep Vein ThrombosisitdocNo ratings yet
- Approach To The Diagnosis and Therapy of Lower Extremity Deep Vein ThrombosisDocument14 pagesApproach To The Diagnosis and Therapy of Lower Extremity Deep Vein ThrombosisWidi HadianNo ratings yet
- Disseminated Intravascular CoagulationDocument2 pagesDisseminated Intravascular CoagulationGerardLum100% (1)
- A Simple Guide to Hypovolemia, Diagnosis, Treatment and Related ConditionsFrom EverandA Simple Guide to Hypovolemia, Diagnosis, Treatment and Related ConditionsNo ratings yet
- Cervical Cancer Case StudyDocument5 pagesCervical Cancer Case StudyIke Ace Evbuomwan100% (1)
- Thyroid CaseDocument53 pagesThyroid CaseKenisha HutsonNo ratings yet
- Deep Vein ThrombosisDocument3 pagesDeep Vein ThrombosisAnonymous cwRgUKv2MQ100% (1)
- BurnsDocument80 pagesBurnsmarNo ratings yet
- Upper and Lower GI Bleeding Differential DiagnosesDocument3 pagesUpper and Lower GI Bleeding Differential DiagnosesKEn PilapilNo ratings yet
- Case Study Tonsil It IsDocument16 pagesCase Study Tonsil It IsMuhammad FarhanNo ratings yet
- HyphemaDocument19 pagesHyphemaLiyanti RinceNo ratings yet
- Bronchial AsthmaDocument40 pagesBronchial Asthmasamson bd mokuntil100% (1)
- Management of Heart FailureDocument62 pagesManagement of Heart Failureapi-13265958No ratings yet
- Deep Vein ThrombosisDocument42 pagesDeep Vein ThrombosisNsklm100% (7)
- Syndrome of Inappropriate Secretion of Anti Diuretic HormoneDocument39 pagesSyndrome of Inappropriate Secretion of Anti Diuretic Hormonefarmasi_hmNo ratings yet
- Acute Rheumatic FeverDocument50 pagesAcute Rheumatic Feversunaryo lNo ratings yet
- AtherosclerosisDocument56 pagesAtherosclerosisJohn Matley Caampued100% (8)
- Glasgow Coma ScaleDocument2 pagesGlasgow Coma ScaleAlas CuatroNo ratings yet
- Hepatic EncephalopathyDocument16 pagesHepatic Encephalopathyjh_ajjNo ratings yet
- Total Thyroidectomy - EdittedDocument55 pagesTotal Thyroidectomy - EdittedPrisicilla Doydora Pat67% (3)
- Aortic Valve StenosisDocument4 pagesAortic Valve StenosisYrag NoznipNo ratings yet
- Ascites: Pathogenesis and Clinical ApproachDocument34 pagesAscites: Pathogenesis and Clinical ApproachPooja ShashidharanNo ratings yet
- Fluid and Electrolyte Management of The Surgical PatientDocument28 pagesFluid and Electrolyte Management of The Surgical PatientAndri Feisal NasutionNo ratings yet
- EDEMADocument36 pagesEDEMAGeetanjali MiglaniNo ratings yet
- Nephrotic SyndromeDocument61 pagesNephrotic SyndromeRanah Julia Garchitorena AyoNo ratings yet
- Benign Tumors of The StomachDocument55 pagesBenign Tumors of The Stomachapi-19641337No ratings yet
- Physiology of PleuraDocument16 pagesPhysiology of PleuraMohamedSalah100% (2)
- Thyroid Case SheetDocument6 pagesThyroid Case SheetHanisha VasireddyNo ratings yet
- Case Study-Acute Urinary RetentionDocument10 pagesCase Study-Acute Urinary RetentionArthadian De Peralta75% (4)
- Slide Ortho Tibia and FibulaDocument25 pagesSlide Ortho Tibia and Fibulaleonard0% (1)
- Neonatal JaundiceDocument48 pagesNeonatal Jaundicelordoftheweb100% (22)
- Deep Vein Thrombosis (DVT)Document13 pagesDeep Vein Thrombosis (DVT)Vijay AnandNo ratings yet
- Malignant MelanomaDocument31 pagesMalignant MelanomakityamuwesiNo ratings yet
- Hemoptysis 1216302404643775 8Document33 pagesHemoptysis 1216302404643775 8abdul sahidNo ratings yet
- PretermDocument11 pagesPretermAlma Gobaleza100% (2)
- Glaucoma Case StudyDocument5 pagesGlaucoma Case StudyEdgel QuidolesNo ratings yet
- SLE Case PresentationDocument29 pagesSLE Case PresentationBlesson JohnNo ratings yet
- Anaesthesia in Emergency Laparotomy: Speaker:P.Shravani Moderator:Dr.K.Vinay Assistant ProfessorDocument52 pagesAnaesthesia in Emergency Laparotomy: Speaker:P.Shravani Moderator:Dr.K.Vinay Assistant ProfessorSanthi Swetha PudhotaNo ratings yet
- Case StudyDocument21 pagesCase StudyLuige AvilaNo ratings yet
- Intestinal ObstructionDocument21 pagesIntestinal ObstructionBheru LalNo ratings yet
- Hematological Alterations: Disseminated Intravascular Coagulation (DIC)Document16 pagesHematological Alterations: Disseminated Intravascular Coagulation (DIC)jhommmmmNo ratings yet
- Mumps: Causes, Incidence, and Risk FactorsDocument6 pagesMumps: Causes, Incidence, and Risk FactorsRan SisonNo ratings yet
- Deep Vein ThrombosisDocument15 pagesDeep Vein ThrombosisAngela TenorioNo ratings yet
- EmpyemaDocument52 pagesEmpyemaDivara Syauta100% (3)
- SinusitisDocument30 pagesSinusitisAbdiqani MahdiNo ratings yet
- Blood DyscrasiaDocument4 pagesBlood DyscrasiaEm Hernandez Arana100% (1)
- Chronic Obstructive Pulmonary DiseaseDocument18 pagesChronic Obstructive Pulmonary DiseaseMaryam BajwaNo ratings yet
- Kuliah Thrombosis 2015 NNDocument39 pagesKuliah Thrombosis 2015 NNBeladiena Citra SiregarNo ratings yet
- Nursing Care PlanDocument12 pagesNursing Care Planzsazsageorge86% (21)
- Deep Venous ThrombosisDocument7 pagesDeep Venous ThrombosisUzma KhanNo ratings yet
- Deep Vein ThrombosisDocument38 pagesDeep Vein ThrombosisvincentthedyNo ratings yet
- MeningococcemiaDocument1 pageMeningococcemiaintrovoyz041No ratings yet
- Lymph Angio Leio Myomato SisDocument2 pagesLymph Angio Leio Myomato Sisintrovoyz041No ratings yet
- Malaria: Ovale, and P. MalariaeDocument1 pageMalaria: Ovale, and P. Malariaeintrovoyz041No ratings yet
- Meningitis PLUS: Goetz: Textbook of Clinical Neurology, 1st EdDocument1 pageMeningitis PLUS: Goetz: Textbook of Clinical Neurology, 1st Edintrovoyz041No ratings yet
- NephRotic SyndromeDocument2 pagesNephRotic Syndromeintrovoyz041No ratings yet
- Neurosyphilis: Mandell: Principles and Practice of Infectious Disease, 5 Ed, PP 2476-2489. Uptodate 2002Document1 pageNeurosyphilis: Mandell: Principles and Practice of Infectious Disease, 5 Ed, PP 2476-2489. Uptodate 2002Drashua AshuaNo ratings yet
- PheochromocytomaDocument2 pagesPheochromocytomaintrovoyz041No ratings yet
- Pneumo CoccusDocument1 pagePneumo Coccusintrovoyz041No ratings yet
- PE The BasicsDocument2 pagesPE The Basicsintrovoyz041No ratings yet
- MyocarditisDocument1 pageMyocarditisintrovoyz041No ratings yet
- Prostate Cancer: Pearls and Myths From The UrologistsDocument2 pagesProstate Cancer: Pearls and Myths From The Urologistsintrovoyz041100% (1)
- RhabdomyolysisDocument2 pagesRhabdomyolysisintrovoyz041No ratings yet
- Polymyositis, DermatomyositisDocument2 pagesPolymyositis, Dermatomyositisintrovoyz041No ratings yet
- Sepsis and Activated Protein C How Does It Work?Document2 pagesSepsis and Activated Protein C How Does It Work?introvoyz041No ratings yet
- Red Cell AplasiaDocument2 pagesRed Cell Aplasiaintrovoyz041No ratings yet
- SingultusDocument2 pagesSingultusintrovoyz041No ratings yet
- Varicella Infection What Kind of Virus Is It? How Does It Get Around?Document2 pagesVaricella Infection What Kind of Virus Is It? How Does It Get Around?introvoyz041No ratings yet
- RV InfarctDocument2 pagesRV Infarctintrovoyz041No ratings yet
- But What Is The TTKG in A Type IV RTA? See BelowDocument2 pagesBut What Is The TTKG in A Type IV RTA? See Belowintrovoyz041No ratings yet
- Factitious DisorderDocument6 pagesFactitious Disorderayu yuliantiNo ratings yet
- RND Systems Bcells BRDocument16 pagesRND Systems Bcells BRchernishovadoNo ratings yet
- Symptoms of Mind Control Electronic Harassment and Organized StalkingDocument6 pagesSymptoms of Mind Control Electronic Harassment and Organized StalkingKalista Pearson100% (1)
- Lecture 21 - HypersensitivityDocument25 pagesLecture 21 - Hypersensitivityapi-3703352100% (2)
- Endocarditis InfecciosaDocument12 pagesEndocarditis InfecciosaJavier Agustín Holloway Sahli100% (1)
- HIV/AIDS in The PhilippinesDocument5 pagesHIV/AIDS in The PhilippinesRop RabinoNo ratings yet
- Bloody Easy 3 TransfusionDocument78 pagesBloody Easy 3 TransfusionSushilNo ratings yet
- Assessment Nursing Diagnosis Background Knowledge Planning Intervention Rationale EvaluationDocument6 pagesAssessment Nursing Diagnosis Background Knowledge Planning Intervention Rationale EvaluationMaye ArugayNo ratings yet
- Evaluation Performa For Case StudyDocument2 pagesEvaluation Performa For Case StudyBobby TiwariNo ratings yet
- 2006 Feb Inpatient Quality IndicatorsDocument1 page2006 Feb Inpatient Quality IndicatorsJPNo ratings yet
- Biochemistry-Module 10 (Electrolytes)Document11 pagesBiochemistry-Module 10 (Electrolytes)Rommel BaraquielNo ratings yet
- Jinoob KCDocument6 pagesJinoob KCAshok NarayananNo ratings yet
- 10.blood Vessels & HeartDocument4 pages10.blood Vessels & Heartharips motupalliNo ratings yet
- 'OET' SAMPLE READING NEW DR TANJIM OVEE 2020Document19 pages'OET' SAMPLE READING NEW DR TANJIM OVEE 2020AHMED TANJIMUL ISLAMNo ratings yet
- Hospital Management System Software, College and School Management System Software, Hotel Management System Software Are Product of Msys TechnosoftDocument2 pagesHospital Management System Software, College and School Management System Software, Hotel Management System Software Are Product of Msys TechnosoftmsystechnosoftNo ratings yet
- SLIDE03 FluidElectrolyteImbalanceDocument57 pagesSLIDE03 FluidElectrolyteImbalanceGrace Amato-Moore100% (1)
- Wound Care Procedure StudentsDocument2 pagesWound Care Procedure StudentsJan Philippe BelandoNo ratings yet
- JCC Stemi CompleteDocument36 pagesJCC Stemi Completeb aNo ratings yet
- Ref Sonographic Evaluation of Thyroid Size 2019Document5 pagesRef Sonographic Evaluation of Thyroid Size 2019Daniel Alejandro CastrilloNo ratings yet
- Stok 03082022Document22 pagesStok 03082022Andika SulistiawanNo ratings yet
- Jurnal HDDocument11 pagesJurnal HDerlinrevNo ratings yet
- How To Get Electives at AKU (Experience)Document15 pagesHow To Get Electives at AKU (Experience)FarazNo ratings yet
- Biology: Advanced Subsidiary Unit 1: Molecules, Diet, Transport and HealthDocument28 pagesBiology: Advanced Subsidiary Unit 1: Molecules, Diet, Transport and HealthTamanna AdibaNo ratings yet
- Treatment Dysarthria EfficacyDocument12 pagesTreatment Dysarthria EfficacySwathi GeethaNo ratings yet
- Case Presentation of DepressionDocument39 pagesCase Presentation of DepressionHeden Collado100% (1)
- Salmonellosis: Odsigue, Clarissa Rama, Alea Albert Rosales, Joy SybilDocument36 pagesSalmonellosis: Odsigue, Clarissa Rama, Alea Albert Rosales, Joy SybilAleya Albert RamaNo ratings yet
- Corona Virus Worksheet Secondary School Reading Comprehension Exercises - 123313Document2 pagesCorona Virus Worksheet Secondary School Reading Comprehension Exercises - 123313Tamara OliveiraNo ratings yet
- E Portfolio Contemporary Nursing PresentationDocument6 pagesE Portfolio Contemporary Nursing Presentationapi-663116972No ratings yet
- Differential Diagnosis of Neck SwellingsDocument24 pagesDifferential Diagnosis of Neck SwellingsDrArish Mahmood100% (3)
- Dr. Jaime Cruz vs. Agas Jr. Medical Hygiene - G.R No. 204095, June 15, 201 5Document4 pagesDr. Jaime Cruz vs. Agas Jr. Medical Hygiene - G.R No. 204095, June 15, 201 5Marianne Shen PetillaNo ratings yet