Professional Documents
Culture Documents
41 Yugandar Etal
Uploaded by
editorijmrhs0 ratings0% found this document useful (0 votes)
12 views4 pagesIJMRHS
Copyright
© © All Rights Reserved
Available Formats
PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentIJMRHS
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
12 views4 pages41 Yugandar Etal
Uploaded by
editorijmrhsIJMRHS
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
You are on page 1of 4
731
Yugandar et al., Int J Med Res Health Sci. 2014;3(3):731-734
International Journal of Medical Research
&
Health Sciences
www.ijmrhs.com Volume 3 Issue 3 Coden: IJMRHS Copyright @2014 ISSN: 2319-5886
Received: 9
th
Apr 2014 Revised: 16
th
May 2014 Accepted: 26
th
May 2014
Case report
A PRODIGIOUS LICHEN PLANUS PIGMENTOSUS: THE WOLFS ISOTOPIC RESPONSE
*Yugandar I
1
, Shiva Kumar
2
, Sai Prasad
3
, Srilakshmi P
1
, Akshaya N
1
, Abhiram R
1
, Sujalalitha K
1
, Meghana GB
1
1
Postgraduate Students,
2
Professor, Department of DVL, P.E.S. Institute of Medical Sciences and Research,
Kuppam, Andhra Pradesh, India
3
Associate Professor, Department of Pathology, S V Medical College, Tirupati, Andhra Pradesh, India
*Corresponding author email:dryugandar@gmail.com
ABSTRACT
Lichen planus is a pruritic, benign, papulosquamous, inflammatory dermatosis of unknown etiology that affects
either or all of the skin, mucous membrane, hair and nail. In its classic form, it presents with violaceous, scaly,
flat-topped, polygonal papules. A female patient aged 43 years with a history of pruritic eruptions for a period of
one month over the right armpit and back of the right chest (C
8
, T
1
, T
2
, T
3
Dermatomes). She had a history of
herpes zoster in the same localization, which had been treated with topical and oral acyclovir two months prior to
this visit. This variant may represent as an example of the Wolfs isotopic response. We presented our case
because of its rarity as a Dermatomal distribution of lichen planus pigmentosus (LPP) and its appearance in the
area of healed herpes zoster as an isotopic response. The case well highlights this unusual condition and
represents the first case reported in Indian dermatology literature to our best of knowledge. The clinical and
histological features of this case are described here.
Keywords: Herpes, Koebner phenomenon, Lichen planus pigmentosus, Unilateral, Wolfs isotope response,
Zosteriform
INTRODUCTION
The term lichenoid is used by clinicians to describe
a flat-topped, shiny, papular eruption resembling
lichen planus or by histopathologists to describe a
type of tissue reaction consisting principally of basal
cell liquefaction and a band-like inflammatory cell
infiltrate in the papillary dermis.
1
The term lichen is derived from the Greek verb to
lick
2
. However, the use of the term is adapted to a
noun in both Greek and Latin for a symbiotic form of
plant life. The dermatosis, lichen planus was first
described by Erasmus Wilson in 1869.
3
Lichen planus pigmentosus (LPP) variant of Lichen
Planus, it is a chronic pigmentary disorder that shows
diffuse or reticulated hyper pigmented, dark brown
macules on the sun-exposed areas such as the face,
neck and other flexural folds.
4
Clinically, it is
different from classical lichen planus by the presence
of dark brown macules.
LPP was first described by Bhutani et al.
5
The Wolfs
isotopic response, as defined by Wolf et al., describes
the occurrence of a new skin disorder exactly at the
site of another, unrelated, and already healed skin
disease. Several types of cutaneous lesions have been
described occurring within cleared cutaneous herpes
zoster, or, less frequently, herpes simplex lesions.
6
A
viral origin, an immunologic origin, a vascular origin
and a neural origin are possible pathogenetic
mechanism of isotopic response. The isotopic
response induce Koebner phenomenon.
DOI: 10.5958/2319-5886.2014.00427.5
732
Yugandar et al., Int J Med Res Health Sci. 2014;3(3):731-734
It is not a type of cancer. It has been recognized that
there is an association between LP and cancer,
although the association is rare. One case of LPP has
been reported in association with Bazex syndrome,
head and neck cancer.
7
CASE REPORT
A 43 year old female, House wife reported to our
department with a one month history of pruritic
eruptions over the back of the chest. She also gave
history of two months duration of herpes zoster, had
been received topical and oral acyclovir. Following it,
she developed multiple pruritic skin eruptions over
same localization.
No history of similar skin lesion in the past or in
family members. She had no history of systemic
complaints. The physical examinations were within
normal limits. Laboratory investigations revealed
normal values.
On cutaneous examination, there were multiple
unilaterally distributed dark brown, flat macules of
variable sizes distributed diffusely over Right
Dermatomes C
8
, T
1
, T
2
, T
3
. It was distributed from
the right armpit to back of the chest, but it never
crossed midline of the body. Few were Violaceous.
(Fig 1, 2) Hair, nail and oral mucosa were not
involved.
A differential diagnosis of post inflammatory
hyperpigmentation, Erythema dyschromicum
perstans, fixed drug eruptions and LPP were
considered. Advised full thickness Punch biopsy.
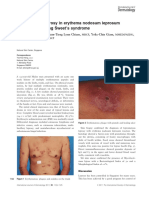
Fig 1: Dark brown, flat macules of variable sizes over
back of chest (right side)
Fig 2: Pigmentary eruptions over Right Dermatomes C
8,T 1,T 2,T 3.
Histopathological examination from one of the
papules on skin under hematoxylin and eosin staining
(H & E) showed epidermal atrophy, lamellar
keratinisation and local basal cell vacuolization.
Superficial dermis shows Pigment incontinency,
mononuclear and lymphocyte cell infiltrate. Civatte
bodies also identified (Fig: 3, 4, 5). Histology
confirmed diagnosis of LPP.
Fig 3: Atrophic Epidermis with mild keratinisation.
Blunting of Rete Ridges, Melanin pigment and few
perivascular lymphocytes in superficial dermis. (H&E
Low Power)
Fig 4: Atrophic Epidermis with absence of Rete Ridges
and presence of Melanin Pigment. (H&E stain, 200)
733
Yugandar et al., Int J Med Res Health Sci. 2014;3(3):731-734
Fig 5: Basal cell vacuolar degeneration,Pigment
incontinence, Perivascular Lymphohistiocytic infiltrate
and Civatte bodies at DEJ. (H&E stain 200)
DISCUSSION
Lichen planus is an idiopathic inflammatory disease
of the skin and mucous membrane. It is characterized
by 6 Ps": planar (flat-topped), purple, polygonal,
pruritic, papules, and plaques. In addition to the
classical appearance, about 20 different variants are
described.
LPP is characterized by mottled or reticulated hyper
pigmented, dark brown macules on the sun exposure
skin areas, varies from slate grey to brownish black, it
is mostly diffuse. The macular hyper pigmentation
involves chiefly the face, neck and upper limbs.
Striking predominance of pigmentary lesions at
intertriginous sites, especially the axillae.
1
The
mucous membranes, palms and soles are usually not
involved. The duration at presentation ranged from 2
months to 21 years in one series.
8
The cause of LPP is unknown, but an immunologic
mechanism mediates its development, as well as that
of lichen planus. Based on the distinctive
lymphocytic inflammatory response of the lichenoid
reactions, cell mediated immunity seems to play a
pivotal role in triggering the clinical expression of the
disease.
9
In our case it was induced Koebner
phenomenon by Preceding Herpes infection.
Histopathology of LPP shows atrophic epidermis,
basal hydropic degeneration, hypergranulosis,
Perivascular Lymphohistiocytic infiltration, pigment
incontinence, irregular elongation of rete ridges
appeared saw tooth pattern and multiple apoptotic
cells i.e. Civatte bodies present in dermoepidermal
junction. Few melanophages are also seen.
Our case showed lamellar keratinisation, local basal
cell vacuolization. Superficial dermis shows Pigment
incontinence, mononuclear and lymphocyte cell
infiltrate. Civatte bodies also identified.
No effective treatment is available. In the references,
Tacrolimus ointment could have a beneficial role in
the treatment of LPP.
10
Topical agents include
hydroquinone, which is the most commonly used
agents, often in combination with retinoic acid,
corticosteroids, azelaic acid, Kojic acid, and glycolic
acid in case facial LPP along with photoprotection.
Other drugs used with inconsistent results are
griseofulvin, Prednisolone, etretinate and
chloroquine.
11
Our patient advised betamethasone
ointment along with sun protection.
There have been only a few reports in the
dermatology literature. Lutz et al also described a
zosteriform pattern of lichen planus developing at the
site of healed herpes zoster.
12
Shemer et al reported a
case of zosteriform lichen planus at the site of healed
herpes zoster.
13
Cho s reported a case of LPP
presenting in zosteriform pattern.
14
Laskaris G.C et al
reported a case of LPP of the Oral Mucosa.
15
CONCLUSION
LPP is an uncommon variant of lichen planus, for
which no definite etiology, no precipitating factors
are known and no effective treatment is available.
Many cases go away within two years. About 1 in 5
will have a Second outbreak.
We describe a case of a rare variant of LPP with a
past history of herpes zoster; this abnormal
presentation can be mistaken for other common
inflammatory dermatosis. To the best of our
knowledge, is the first case report of LPP with a past
history of Herpes zoster in Indian Literature. So we
suggest that the title name Bizarre or Unusual or
Zosteriform or Prodigious Lichen Planus
Pigmentosus because of variable etiology or
presentation or treatment.
ACKNOWLEDGEMENT
We gratefully acknowledge the help of the Principal,
PESIMSR, Kuppam, the professor and head,
department of DVL, PESIMSR, Kuppam
Conflict of interest: Nil
REFERENCES
1. Breathnach SM. Lichen Planus and Lichenoid
Disorders. In: Burns T, Breathnach S, Cox N,
734
Yugandar et al., Int J Med Res Health Sci. 2014;3(3):731-734
Griffiths C, editors. Rooks Textbook of
Dermatology. 8
th
ed. Wiley-Blackwell; 2010:
41.1- 41.28.
2. Kanwar AJ, De D. Lichen planus in children.
Indian J Dermatol Venereol Leprol 2010;76:366-
72
3. Neerja Puri, Asha Puri. A study on lichen planus
in children. Our Dermatol Online 2013; 4(3):
303-05
4. Jong Keun Seo, Hyun Jae Lee, Deborah Lee,
Joon Hee Choi,Ho-Suck Sung. A case of linear
lichen planus pigmentosus. Ann Dermatol 2010;
22(3):323-25
5. Bhutani L, Bedi T, Pandhi R. Lichen planus
pigmentosus. Dermatologica 1974; 149: 43-50
6. Aylin Turel, Serap ozturkcan, M.Turhan Sahin,
Peyker Turkdog an. Wolfss Isotopic Response:
A Case of Zosteriform Lichen Planus. J Dermatol
2002; 29: 33942
7. Sassolas B, Zagnoli A, Leroy JP, Guillet G.
Lichen planus pigmentosus associated with
acrokeratosis of Bazex. Clin Exp Dermatol.
January 1994; 19(1):70-73
8. Kanwar AJ, Dogra S, Handa S. A study of 124
Indian patients with lichen planus pigmentosus.
Clin Exp Dermatol 2003; 28: 481-85
9. Jong Keun Seo, Hyun Jae Lee, Deborah Lee,
Joon Hee Choi, Ho-Suck Sung. A Case of Linear
Lichen Planus Pigmentosus. Ann Dermatol 2010;
22(3): 323
10. Ru-zhi Zhang, Wen-yuan Zhu. One case of
unilateral linear lichen planus pigmentosus. The
Open Dermatology Journal 2012; 6; 25-28
11. Kanwar AJ, Dogra S, Handa S. A study of 124
Indian patients with lichen planus pigmentosus.
Clin Exp Dermatol 2003; 28: 481-85
12. Lutz ME, Perniciaro C, Lim KK. Zosteriform
lichen planus without evidence of herpes simplex
virus or varicella-zoster virus by polymerase
chain reaction. Report of two cases. Acta Derm
Venereol 1997; 77: 491-92
13. Shemer A, Weiss G, Trau H. Wolfs isotopic
response: A case of zosteriform lichen planus on
the site of healed herpes zoster. JEADV 2001; 15:
445-47
14. Cho S, Whang KK. Lichen planus pigmentosus
presenting in zosteriform pattern. J Dermatol
1997, 24(3):193-97
15. Laskaris GC, Papavasiliou SS, Bovopoulou OD,
Nicolis GD. Lichen planus pigmentosus of the
Oral Mucosa: A Rare Clinical Variety.
Dermatologica 1981;162:6163
You might also like
- Clinical Cases in PsoriasisFrom EverandClinical Cases in PsoriasisJashin J. WuNo ratings yet
- Prurigo Nodularis of HydeDocument12 pagesPrurigo Nodularis of HydeAugusto MonjardimNo ratings yet
- Liken PlanusDocument6 pagesLiken PlanusAmirahShalehaNo ratings yet
- Leprosy: An Overview of Pathophysiology: Restu Wulandari I11110062 Pembimbing Dr. Teguh Aly'Ansyah SP - KKDocument26 pagesLeprosy: An Overview of Pathophysiology: Restu Wulandari I11110062 Pembimbing Dr. Teguh Aly'Ansyah SP - KKrestuwulandari94No ratings yet
- Ciclosporin Therapy For Canine Generalized Discoid LupusDocument6 pagesCiclosporin Therapy For Canine Generalized Discoid LupusPatrícia StancuNo ratings yet
- Childhood Lichen Planus With Palmoplantar InvolvementDocument3 pagesChildhood Lichen Planus With Palmoplantar InvolvementSabriadi NursalNo ratings yet
- Lichen Planus/lupus Erythematosus Overlap With Hypothyroidism: A Case ReportDocument3 pagesLichen Planus/lupus Erythematosus Overlap With Hypothyroidism: A Case ReportcuribepNo ratings yet
- TP LeprosyDocument4 pagesTP LeprosyZarina RobledoNo ratings yet
- Erosive Lichen Planus: A Case ReportDocument4 pagesErosive Lichen Planus: A Case ReportNuningK93No ratings yet
- (2017) BELOUSOVA, Irena E. Mycosis Fungoides Manifesting As Giant Cell Lichenoid DermatitisDocument3 pages(2017) BELOUSOVA, Irena E. Mycosis Fungoides Manifesting As Giant Cell Lichenoid DermatitisCassandra VérasNo ratings yet
- 80-Article Text-153-1-10-20161118Document4 pages80-Article Text-153-1-10-20161118Rania SalwanabilaNo ratings yet
- Parakeratosis Variegata: A Possible Role of Environmental Hazards?Document4 pagesParakeratosis Variegata: A Possible Role of Environmental Hazards?Ega AihenaNo ratings yet
- Ten N Sjs ReviewDocument5 pagesTen N Sjs ReviewNantini GopalNo ratings yet
- Leprosy Written ReportDocument7 pagesLeprosy Written Reportnicah05No ratings yet
- 17.pityriasis RoseaDocument5 pages17.pityriasis RoseahaidarTRVNo ratings yet
- Childhood Leprosy: Facts, Myths and Mysteries: Jayamini SeneviratneDocument7 pagesChildhood Leprosy: Facts, Myths and Mysteries: Jayamini SeneviratneDhanasree VijayanNo ratings yet
- UntitledDocument3 pagesUntitledShintaNo ratings yet
- 494 PDFDocument6 pages494 PDFranz ibonkNo ratings yet
- Oral Leukoerythroplakia A Case ReportDocument6 pagesOral Leukoerythroplakia A Case ReportArdelvie YoandaNo ratings yet
- Vesicubullous Diseases & Mucocutaneous DisordersDocument23 pagesVesicubullous Diseases & Mucocutaneous Disordersshahlaraib001No ratings yet
- My LepraeDocument19 pagesMy LepraeDayana PrasanthNo ratings yet
- Itchy Bumps With New-Onset Bullae: Syed H. Mahmood BS - Anthony Van Vreede MD - David Mehregan MDDocument2 pagesItchy Bumps With New-Onset Bullae: Syed H. Mahmood BS - Anthony Van Vreede MD - David Mehregan MDAna MariaNo ratings yet
- Case Report: Subcorneal Pustular Dermatosis in Childhood: A Case Report and Review of The LiteratureDocument6 pagesCase Report: Subcorneal Pustular Dermatosis in Childhood: A Case Report and Review of The LiteratureIrsalinaHusnaAzwirNo ratings yet
- EN + EosinofiliaDocument3 pagesEN + EosinofiliaAna Flavia BaptistaNo ratings yet
- Palmoplantar Lichen Planus: A Rare Presentation of A Common DiseaseDocument3 pagesPalmoplantar Lichen Planus: A Rare Presentation of A Common DiseaseiwakiwakNo ratings yet
- Leprosy ManualDocument16 pagesLeprosy ManualMikee Laceda NamquiNo ratings yet
- Lupus Vulgaris of External NoseDocument3 pagesLupus Vulgaris of External NosejalalfaizNo ratings yet
- Dermacase. Pityriasis Rosea.Document3 pagesDermacase. Pityriasis Rosea.Brenda Ruth PanjaitanNo ratings yet
- PDM Os4Document3 pagesPDM Os4Erdinawira RizkianiNo ratings yet
- Sporothrix and M LepraeDocument6 pagesSporothrix and M LepraeVictor Juris AnonuevoNo ratings yet
- MH 2 PDFDocument13 pagesMH 2 PDFNurul FajriNo ratings yet
- Oral Lichen Planus - A Case ReportDocument2 pagesOral Lichen Planus - A Case ReportNoormanNo ratings yet
- De Novo Histoid Leprosy With Borderline Tuberculoi PDFDocument5 pagesDe Novo Histoid Leprosy With Borderline Tuberculoi PDFNelsi Mellisa DewiNo ratings yet
- Erosive Lichen Planus of The Oral Cavity: A CaseDocument5 pagesErosive Lichen Planus of The Oral Cavity: A CaseFuad HasanNo ratings yet
- Pi Is 0190962214011566Document2 pagesPi Is 0190962214011566LewishoppusNo ratings yet
- Scrofuloderma: A Common Type of Cutaneous Tuberculosis. A Case ReportDocument5 pagesScrofuloderma: A Common Type of Cutaneous Tuberculosis. A Case ReportIndah IndrianiNo ratings yet
- Pemphigoid Vegetans in Childhood: A Case Report and Short Review of LiteratureDocument11 pagesPemphigoid Vegetans in Childhood: A Case Report and Short Review of LiteratureCata santaNo ratings yet
- Lupus Er Ythematosus: EpidemiologyDocument55 pagesLupus Er Ythematosus: EpidemiologyJelena BajagicNo ratings yet
- Pityriasis AlbaDocument7 pagesPityriasis AlbaAri Kurniawan100% (1)
- Document 4Document14 pagesDocument 4karthiksekaranNo ratings yet
- TEN and SJSDocument8 pagesTEN and SJSreyhanrrNo ratings yet
- Leprosy JEADVDocument9 pagesLeprosy JEADVAna BeatrizNo ratings yet
- Liken Planus & Lichen Sclerosus Et Atropichus, Granuloma AnulareDocument29 pagesLiken Planus & Lichen Sclerosus Et Atropichus, Granuloma AnulareroserosannaNo ratings yet
- Dermatology D. Azr Lec2 Mon 18.10.2010: Papulosquamous DiseasesDocument9 pagesDermatology D. Azr Lec2 Mon 18.10.2010: Papulosquamous DiseasesMohamed Al-zichrawyNo ratings yet
- Leprosy: CharacteristicsDocument10 pagesLeprosy: Characteristicsanon-374466No ratings yet
- 1793-Article Text-19545-2-10-20190508 PDFDocument5 pages1793-Article Text-19545-2-10-20190508 PDFRezkyRamadhaniSyarifNo ratings yet
- Volltext PDFDocument5 pagesVolltext PDFJhonnie Gaona CardonaNo ratings yet
- Buffalo LeprosyDocument4 pagesBuffalo LeprosyALTAF HUSAINNo ratings yet
- Lichen Striatus On AdultDocument4 pagesLichen Striatus On Adultmustafa566512345No ratings yet
- Leprosy ManualDocument12 pagesLeprosy ManualArumNo ratings yet
- Erythema MultiformeDocument5 pagesErythema MultiformeNicco MarantsonNo ratings yet
- Lepromatous Leprosy in Erythema Nodosum Leprosum Reaction Mimicking Sweet's SyndromeDocument2 pagesLepromatous Leprosy in Erythema Nodosum Leprosum Reaction Mimicking Sweet's SyndromeAstri MelistriNo ratings yet
- Isolated Lichen Planus of The Lip: S Ign S, Syn Drom Es and Diagnos EsDocument7 pagesIsolated Lichen Planus of The Lip: S Ign S, Syn Drom Es and Diagnos EsPedrito PerezNo ratings yet
- Current Status of Leprosy: Epidemiology, Basic Science and Clinical PerspectivesDocument9 pagesCurrent Status of Leprosy: Epidemiology, Basic Science and Clinical PerspectivesYolan Sentika NovaldiNo ratings yet
- Original Article Blaschkoian Lichen PlanusDocument6 pagesOriginal Article Blaschkoian Lichen PlanusiwakiwakNo ratings yet
- Pi Is 0190962208009328Document2 pagesPi Is 0190962208009328Nabhya MaheshwariNo ratings yet
- Caz de Toxoplasmoza CutanataDocument7 pagesCaz de Toxoplasmoza Cutanatacatalina criceaNo ratings yet
- Skin Lichen Planus, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsFrom EverandSkin Lichen Planus, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsNo ratings yet
- Inflammatory Dermatopathology: A Pathologist's Survival GuideFrom EverandInflammatory Dermatopathology: A Pathologist's Survival GuideNo ratings yet
- Ijmrhs Vol 4 Issue 3Document263 pagesIjmrhs Vol 4 Issue 3editorijmrhsNo ratings yet
- Ijmrhs Vol 3 Issue 4Document294 pagesIjmrhs Vol 3 Issue 4editorijmrhsNo ratings yet
- Ijmrhs Vol 3 Issue 2Document281 pagesIjmrhs Vol 3 Issue 2editorijmrhsNo ratings yet
- Ijmrhs Vol 4 Issue 2Document219 pagesIjmrhs Vol 4 Issue 2editorijmrhsNo ratings yet
- Ijmrhs Vol 4 Issue 4Document193 pagesIjmrhs Vol 4 Issue 4editorijmrhs0% (1)
- Ijmrhs Vol 3 Issue 3Document271 pagesIjmrhs Vol 3 Issue 3editorijmrhsNo ratings yet
- Ijmrhs Vol 2 Issue 4Document321 pagesIjmrhs Vol 2 Issue 4editorijmrhsNo ratings yet
- 48 MakrandDocument2 pages48 MakrandeditorijmrhsNo ratings yet
- Ijmrhs Vol 1 Issue 1Document257 pagesIjmrhs Vol 1 Issue 1editorijmrhsNo ratings yet
- Ijmrhs Vol 2 Issue 2Document197 pagesIjmrhs Vol 2 Issue 2editorijmrhsNo ratings yet
- 37poflee EtalDocument3 pages37poflee EtaleditorijmrhsNo ratings yet
- Ijmrhs Vol 3 Issue 1Document228 pagesIjmrhs Vol 3 Issue 1editorijmrhsNo ratings yet
- Ijmrhs Vol 2 Issue 3Document399 pagesIjmrhs Vol 2 Issue 3editorijmrhs100% (1)
- Ijmrhs Vol 2 Issue 1Document110 pagesIjmrhs Vol 2 Issue 1editorijmrhs100% (1)
- 40vedant EtalDocument4 pages40vedant EtaleditorijmrhsNo ratings yet
- Williams-Campbell Syndrome-A Rare Entity of Congenital Bronchiectasis: A Case Report in AdultDocument3 pagesWilliams-Campbell Syndrome-A Rare Entity of Congenital Bronchiectasis: A Case Report in AdulteditorijmrhsNo ratings yet
- 47serban Turliuc EtalDocument4 pages47serban Turliuc EtaleditorijmrhsNo ratings yet
- 45mohit EtalDocument4 pages45mohit EtaleditorijmrhsNo ratings yet
- Pernicious Anemia in Young: A Case Report With Review of LiteratureDocument5 pagesPernicious Anemia in Young: A Case Report With Review of LiteratureeditorijmrhsNo ratings yet
- 41anurag EtalDocument2 pages41anurag EtaleditorijmrhsNo ratings yet
- Recurrent Cornual Ectopic Pregnancy - A Case Report: Article InfoDocument2 pagesRecurrent Cornual Ectopic Pregnancy - A Case Report: Article InfoeditorijmrhsNo ratings yet
- 31tushar EtalDocument4 pages31tushar EtaleditorijmrhsNo ratings yet
- 36rashmipal EtalDocument6 pages36rashmipal EtaleditorijmrhsNo ratings yet
- 38vaishnavi EtalDocument3 pages38vaishnavi EtaleditorijmrhsNo ratings yet
- 35krishnasamy EtalDocument1 page35krishnasamy EtaleditorijmrhsNo ratings yet
- 33 Prabu RamDocument5 pages33 Prabu RameditorijmrhsNo ratings yet
- 34tupe EtalDocument5 pages34tupe EtaleditorijmrhsNo ratings yet
- 28nnadi EtalDocument4 pages28nnadi EtaleditorijmrhsNo ratings yet
- Lesson One Hospital DepartmentDocument4 pagesLesson One Hospital DepartmentIkhsan QusayNo ratings yet
- Candela GentleMAX Pro Treatment GuidelinesDocument1 pageCandela GentleMAX Pro Treatment Guidelinesfuture medical100% (1)
- Principles of Topical Treatments in DermatologyDocument18 pagesPrinciples of Topical Treatments in DermatologyAnonymous OlS0WZwNo ratings yet
- 20 Lecture Oral Mucosa Vesiculo-Bullous DiseaseDocument10 pages20 Lecture Oral Mucosa Vesiculo-Bullous Diseaseمازن كريم حمودNo ratings yet
- Konda Article PE PDFDocument51 pagesKonda Article PE PDFAnonymous O6EvmX7No ratings yet
- MNAH Pricelist 2015Document147 pagesMNAH Pricelist 2015First LastNo ratings yet
- Pembahasan Seminar Part 2 Agustus 2017Document971 pagesPembahasan Seminar Part 2 Agustus 2017Kemal Fikar MuhammadNo ratings yet
- Inventory Override Report 09.07.2023 03.14 PMDocument48 pagesInventory Override Report 09.07.2023 03.14 PMapotek zapemporiumNo ratings yet
- Lakme Products Price List PDF 2021Document11 pagesLakme Products Price List PDF 2021fefwNo ratings yet
- Fellowship Course in Homo Dermatology 290613Document5 pagesFellowship Course in Homo Dermatology 290613Vishakha PawarNo ratings yet
- Top 100 Ayurvedic Doctors in Ahmedabad PDFDocument42 pagesTop 100 Ayurvedic Doctors in Ahmedabad PDFocr useNo ratings yet
- Approach in Clinical Dermatology (Notes)Document4 pagesApproach in Clinical Dermatology (Notes)Codillia CheongNo ratings yet
- Prescription: Hydroquinone 1 % Tretinoin 0.05 % Kojic Acid 0.05 % Hydrocortisone 0.05%Document9 pagesPrescription: Hydroquinone 1 % Tretinoin 0.05 % Kojic Acid 0.05 % Hydrocortisone 0.05%dumral831No ratings yet
- PDT PDFDocument10 pagesPDT PDFTg CNo ratings yet
- Ebook Advances in Cosmetic Surgery Volume 1 2018 PDF Full Chapter PDFDocument67 pagesEbook Advances in Cosmetic Surgery Volume 1 2018 PDF Full Chapter PDFlinwood.kraft180100% (26)
- Lesions PPT NewDocument37 pagesLesions PPT NewDeb SharmaNo ratings yet
- Superficial and Deep Perivascular DermatitisDocument55 pagesSuperficial and Deep Perivascular DermatitisMarnie RoviraNo ratings yet
- Harga Emina NewDocument4 pagesHarga Emina NewZidni IlmaNo ratings yet
- Homeopathic Management of Ring WormDocument3 pagesHomeopathic Management of Ring WormEditor IJTSRDNo ratings yet
- Beautyzen Skin Care Series: Daftar HargaDocument4 pagesBeautyzen Skin Care Series: Daftar HargaAgus Andika PutraNo ratings yet
- Treatment For CelluliteDocument5 pagesTreatment For CelluliteAreejNo ratings yet
- PROCESS - How To Properly Cleanse Your FaceDocument3 pagesPROCESS - How To Properly Cleanse Your FaceYamig00ps KyanmAaaaNo ratings yet
- Thanakha PresentationDocument12 pagesThanakha Presentationheinthaw22100% (1)
- Sarowar Dermatology BookDocument13 pagesSarowar Dermatology Booktejbirsingh2013No ratings yet
- Contact DermatitisDocument2 pagesContact DermatitisMIR SARTAJNo ratings yet
- Alergia BavsvebsiDocument16 pagesAlergia BavsvebsiNana OkujavaNo ratings yet
- Eruption: Petechiae EcchymosesDocument3 pagesEruption: Petechiae EcchymosesTeddy WibowoNo ratings yet
- Ve Siculo Bull Ous DiseasesDocument73 pagesVe Siculo Bull Ous DiseasesAARYANo ratings yet
- Melanocytic TumorsDocument170 pagesMelanocytic TumorsOlteanu Dragos-Nicolae100% (1)
- Allure Readers' Choice Awards 2023 Meet The 68 Winning Product AllureDocument1 pageAllure Readers' Choice Awards 2023 Meet The 68 Winning Product AlluremajozeladamuaNo ratings yet