Professional Documents
Culture Documents
Management of Diabetic Foot Lesions
Uploaded by
WasemBhatCopyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Management of Diabetic Foot Lesions
Uploaded by
WasemBhatCopyright:
Available Formats
7/15/2014 Management of diabetic foot lesions
http://www.uptodate.com/contents/management-of-diabetic-foot-lesions?topicKey=SURG%2F8175&elapsedTimeMs=3&source=search_result&searchTer 1/23
Official reprint from UpToDate
www.uptodate.com 2014 UpToDate
Authors
David K McCulloch, MD
Richard J de Asla, MD
Section Editors
John F Eidt, MD
Joseph L Mills, Sr, MD
David M Nathan, MD
Deputy Editor
Kathryn A Collins, MD, PhD, FACS
Management of diabetic foot lesions
All topics are updated as new evidence becomes available and our peer review process is complete.
Literature review current through: Jun 2014. | This topic last updated: Mar 27, 2013.
INTRODUCTION The lifetime risk of a foot ulcer for patients with diabetes (type 1 or 2) may be as high as 25
percent [1-3]. Diabetic foot ulcers are a major cause of morbidity and mortality, accounting for approximately
two-thirds of all nontraumatic amputations performed in the United States [4,5]. This observation illustrates the
importance of prompt treatment of foot ulcers in patients with diabetes. The management of diabetic foot lesions
is provided here. Evaluation and prevention of foot ulcers and the treatment of diabetes-related foot infections
(cellulitis and osteomyelitis) are discussed separately. (See "Evaluation of the diabetic foot" and "Clinical
manifestations, diagnosis, and management of diabetic infections of the lower extremities".)
WOUND CLASSIFICATION The first step in managing diabetic foot ulcers is classifying the wound.
Classification is based upon clinical evaluation of the extent of the lesion and, in some classification systems,
an assessment of the vascular status of the foot. The intensity and duration of treatment can be determined
after clinical evaluation of the ulcer. (See "Evaluation of the diabetic foot", section on 'Wound evaluation'.)
A widely used classification of diabetic foot ulcers is that proposed by Wagner [6]:
Grade 0 No ulcer in a high-risk foot
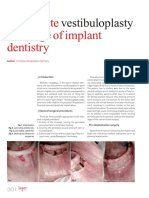
Grade 1 Superficial ulcer involving the full skin thickness but not underlying tissues (picture 1)
Grade 2 Deep ulcer, penetrating down to ligaments and muscle, but no bone involvement or abscess
formation (picture 2)
Grade 3 Deep ulcer with cellulitis or abscess formation, often with osteomyelitis (picture 3)
Grade 4 Localized gangrene (picture 4)
Grade 5 Extensive gangrene involving the whole foot
The Wagner classification is based upon clinical evaluation (depth of ulcer and presence of necrosis) alone and
does not account for the vascular status of the foot. A modified system that is frequently used by orthopedic
surgeons individually scores the components of wound depth and ischemia [7]. Other ulcer classification
systems have also been published [8-11]. The International Working Group on the Diabetic Foot proposed
classifying all ulcers according to the following categories: perfusion, extent, depth, infection, and sensation
(PEDIS) [12]. The PEDIS system is primarily used for research purposes.
The usual approach to the management of lesions of each Wagner grade is given below, followed by a
discussion of some newer approaches.
GRADE 0 LESIONS Counseling regarding preventive foot care should be given to any patient whose feet are
at risk for ulcer development, particularly patients with existing neuropathy. There are several measures that can
markedly diminish ulcer formation, such as avoiding poorly fitting shoes, walking barefoot, and smoking. This
topic is reviewed separately. (See "Evaluation of the diabetic foot", section on 'Risk factors' and "Evaluation of
the diabetic foot", section on 'Preventive foot care'.) [1]
GRADE 1 AND 2 LESIONS Extensive debridement, good local wound care, relief of pressure on the ulcer,
and control of infection (when present) are believed to be important components of therapy for grade 1 and 2 foot
ulcers [9,13,14]. There are limited data evaluating the efficacy of this standard approach, particularly the benefits
of debridement and local wound care. In a meta-analysis of the control groups from 10 trials (622 patients)
7/15/2014 Management of diabetic foot lesions
http://www.uptodate.com/contents/management-of-diabetic-foot-lesions?topicKey=SURG%2F8175&elapsedTimeMs=3&source=search_result&searchTer 2/23
evaluating standard treatment (debridement and local wound care) versus various new therapies, 24 and 31
percent of ulcers healed after 12 and 20 weeks, respectively, of standard treatment [15].
In clinical practice, measurements of a patient's ulcer size should be taken at every office visit so that
comparisons can be made and progress documented. The surface area of a healthy diabetic foot ulcer should
decrease in size at a rate of approximately one percent a day. Ulcers that do not improve should be evaluated
for ongoing soft tissue infection or osteomyelitis requiring antibiotics, insufficient vascular flow, or most
commonly, the need for more effective off-loading. (See 'Assessment for peripheral artery disease' below and
'Assess for osteomyelitis' below.)
Method of debridement Debridement of necrotic tissue is important for ulcer healing [16], although there
are few trials comparing the different methods of debridement (sharp, enzymatic, autolytic, mechanical, and
biological). The types of debridement are reviewed separately. (See "Treatment of pressure ulcers", section on
'Debridement'.)
Sharp debridement involves the use of a scalpel or scissors to remove necrotic tissue [17]. It is the most widely
used method except in certain settings, such as highly vascular ulcers or when there is significant vascular
compromise such that concerns exist as to the patient's ability to heal any new wounds created by sharp
debridement. In such settings, enzymatic debridement (topical application of proteolytic enzymes such as
collagenase) may be preferable [8]. Autolytic debridement, using a semiocclusive or occlusive (hydrogel)
dressing to cover a wound so that necrotic tissue is digested by enzymes normally present in wound tissue,
may be a good option in patients with painful ulcers.
In a systematic review of six small randomized trials, hydrogels were significantly more effective than wet to
moist saline or dry gauze in healing foot ulcers in diabetic patients [18]. However, a hydrogel combined with
good wound care (defined as sharp debridement, saline dressings, pressure relief, and control of infection) was
not significantly better than good wound care alone. Larval therapy (a form of biological debridement) showed no
significant benefit in small studies. Overall, the review was limited by the small number of trials and poor
methodological quality.
Thus, there are few data to guide choice of debridement. When surgeons with expertise in sharp debridement
are available, we prefer this method. As an alternative, we suggest application of a hydrogel since limited data
support its efficacy in promoting ulcer healing. For patients with evidence of arterial insufficiency, we suggest
referral to a vascular specialist.
Infection control The diagnosis of infection is clinical and is likely to be present if the ulcer contains obvious
purulent material or there is redness, swelling or warmth around the ulcer [19]. Cultures of the ulcer base are
taken after debridement and prior to initiation of empiric antibiotic therapy. Tissue samples taken by curettage,
rather than wound swab or irrigation, are preferable because they provide more accurate results [20]. The most
common infecting organisms are aerobic gram-positive cocci. Other frequent pathogens are aerobic gram-
negative bacilli and anaerobes, usually as a second organism [21].
In general, the limited data on antibiotic therapy of diabetic foot infections lack standardization to allow
comparison of outcomes of different regimens. On the basis of the available studies, no single drug or
combination appears to be superior to others. Empiric antibiotic therapy should cover gram-positive cocci (table
1). Subsequent antibiotic therapy should be tailored to culture and susceptibility results. It is not always
necessary to cover all microorganisms isolated from cultures. (See "Clinical manifestations, diagnosis, and
management of diabetic infections of the lower extremities", section on 'Antimicrobial therapy'.) [22]
Local wound care After debridement, ulcers should be kept clean and moist but free of excess fluids.
Moisture accelerates tissue healing. Dressings should be selected based upon wound characteristics, such as
the extent of exudate, desiccation, or necrotic tissue.
Some dressings simply provide protection, whereas others promote wound hydration or prevent excessive
moisture. Wet-to-dry saline dressings are frequently used, but some ulcers may require a moister environment.
In addition, wet-to-dry dressings will remove both nonviable and viable tissues. Thus, caution is required to avoid
damaging healthy tissue.
7/15/2014 Management of diabetic foot lesions
http://www.uptodate.com/contents/management-of-diabetic-foot-lesions?topicKey=SURG%2F8175&elapsedTimeMs=3&source=search_result&searchTer 3/23
Some dressings are impregnated with antimicrobial agents to prevent infection and enhance ulcer healing.
However, there are no clinical trial data to support their effectiveness [23]. (See "Treatment of pressure ulcers",
section on 'Dressing choices'.)
Mechanical off-loading Off-loading devices, including total contact casts, cast walkers, shoe modifications
and other devices to assist in ambulation are available to reduce or eliminate pressure in the region of the ulcer,
which is important for healing. The evidence supports the use of total contact casts and nonremovable cast
walkers for relief of pressure associated with diabetic ulcer healing [24]. A 2000 Cochrane database review
updated in 2013 evaluated 14 trials comparing various forms of pressure-relieving treatments (nonremovable,
removable) and dressings [25,26]. In five trials, the likelihood of wound healing was significantly better at 12
weeks for nonremovable, pressure-relieving casts compared with removable devices or dressings (relative risk
[RR] 1.17, 95% CI 1.01-1.36). In one trial, no significant differences were found between different types of
nonremovable pressure-relieving treatments [27].
Total contact cast A total contact cast is a padded fiberglass shell designed to take pressure off the
heel or elsewhere on the foot by averaging the pressure across the sole of the foot (ie, eliminates high and low
pressure regions by providing contact at all points) or to generally un-weight the entire foot through a total
contact fit at the calf. The most aggressive unloading is achieved by making the patient non-weight-bearing.
Disadvantages of total contact casting include expertise needed in applying the cast, inability to inspect the
wound frequently, inconvenience in activities of daily living (eg, bathing), and the risk of developing a secondary
ulcer in an ill-fitting cast (particularly in patients with neuropathy) [9]. Frequent cast changes may be needed to
avoid complications.
Based upon randomized trials, total contact casting enhances diabetic ulcer healing and is the standard for
relieving pressure from the forefoot [25-33]. As an example, in a trial of off-loading modalities in 63 diabetic
patients with superficial, noninfected, nonischemic plantar ulcers, the proportion of ulcers that were healed at 12
weeks was significantly higher in those randomly assigned to a total contact cast compared with a half-shoe or
removable cast walker (90 versus 58 and 65 percent, respectively) [30]. Patients with a total contact cast also
had faster wound healing. Another small trial found that a casting combined with Achilles tendon lengthening
resulted in significantly fewer ulcer recurrences at seven months (15 verus 59 percent) and two years (38 versus
81 percent) compared with the casting alone [34].
Total contact casts should not be used in patients with infected wounds, osteomyelitis, peripheral ischemia,
bilateral ulceration, lower extremity amputation or heel ulceration [35].
Cast walkers An alternative to total contact casting is a prefabricated brace called a cast walker that is
designed to maintain a total contact fit (figure 1). Several cast walkers (non-removable, removable) are
commercially available and provide capability to off-load the foot similar to contact casts. Cast walkers also
appear to facilitate wound healing, but a significant disadvantage is poor patient compliance if the cast walker is
removed [36].
Cast walkers appear to have a similar ability to off-load the foot compared with total contact casting.
One study compared plantar foot pressure metrics in a standard shoe, total contact cast and
prefabricated pneumatic walking brace [37]. Five plantar foot sensors were placed at the first, third, and
fifth metatarsal heads, fifth metatarsal base, and mid-plantar heel of 10 healthy male subjects who
walked at a constant speed over a distance of 280 meters. Peak pressures were significantly reduced in
the pneumatic walking brace compared with the standard shoe for all sensor locations to an equal or
greater degree compared with the total contact cast in all sensor locations.
Another study measured foot pressures using an in-shoe pressure measurement system (Novel Pedar)
in 18 healthy subjects while wearing a cast walker or total contact cast [38]. Peak foot pressures using
the cast walker were significantly reduced in the forefoot (12 versus 18 N/cm ) and foot as a whole (14
versus 19 N/cm ) compared with a fiberglass total contact cast, but no differences were found for the
heel or midfoot.
These studies suggest these prefabricated products are at least as good as total contact casting for off-loading
2
2
7/15/2014 Management of diabetic foot lesions
http://www.uptodate.com/contents/management-of-diabetic-foot-lesions?topicKey=SURG%2F8175&elapsedTimeMs=3&source=search_result&searchTer 4/23
the foot and equalizing foot pressures when the foot anatomy is normal, but data are not available demonstrating
these effects for patients with diabetic foot deformities.
Cast walkers have been used for the treatment of neuropathic plantar ulcers but these devices, thus far, have
not been found to be superior to total contact casting in randomized trials. In one trial, the rate of ulcer healing
was significantly higher in those randomly assigned to total contact casting compared with a half-shoe or
removable cast walker [30]. Another trial that randomly assigned 48 patients to total contact casting or a
removable cast walker (ie, Stabil-D), found no difference in the number of days to achieve healing (35 versus
39 days) [39].
Therapeutic shoes After healing of the ulcer is achieved, extra-depth and -width shoes with orthotic
inserts are often prescribed to prevent recurrent ulceration [25]. However, in one trial, 400 diabetic patients with
a history of foot ulcer were randomly assigned to wear therapeutic shoes or their usual footwear for two years
[40]. The risk of re-ulceration was not found to be different between the groups. Non-prescription rocker sole
shoes (figure 2) may also offload the foot [41,42]. In a non-randomized prospective study of 92 patients with
healed diabetic foot ulcers, the first-year annual rate of foot ulcer relapse was significantly lower in patients who
used stock diabetic shoes (rocker sole) compared with those who wore their usual footwear (15 versus 60
versus percent) [42]. In the United States, reimbursement from insurance carriers can be expected for at least
one pair of shoes and/or shoe inserts, provided the design of the shoe/insert meets qualifying guidelines.
Wedge shoes (eg, Darco International), also called half shoes, are available as a forefoot wedge and heel wedge
shoes to off-load the forefoot and heel, respectively (figure 3). These shoes may be useful under certain
circumstances. For example, plantar heel ulcers are particularly difficult to heel because of an inability to
adequately off-load this region; the heel wedge shoe can be useful to achieve this goal.
The disadvantage of wedge shoes is that most patients, especially elderly patients or those with proprioception
abnormalities may not be able to maintain their balance, and some patients find walking in them difficult, if not
impossible.
Knee walkers Knee walkers are ambulatory assist devices that may be indicated for anyone with a lower
extremity issue where weight bearing needs to be avoided (figure 4). These devices are becoming more popular
in the treatment of diabetic ulcer as a means to off-load the foot. There are no trials evaluating the effectiveness
of these devices in healing diabetic foot ulcers.
Summary Debridement, good local wound care, and relief of pressure on the ulcer are believed to be
important components of therapy for grade 1 and 2 foot ulcers [9]. This treatment program does not require
hospitalization. Close monitoring is required, and hospitalization for bed rest and intravenous antibiotic therapy
is advisable if the ulcer does not improve. (See "Clinical manifestations, diagnosis, and management of diabetic
infections of the lower extremities".)
GRADE 3 LESIONS Before deciding upon appropriate management of deep ulcers, it is important to evaluate
for substantial peripheral vascular disease or bony involvement. A brief review is found here. These topics are
discussed in detail separately. (See "Evaluation of the diabetic foot", section on 'Physical signs of peripheral
artery disease' and "Evaluation of the diabetic foot", section on 'Signs of infection'.)
Assessment for peripheral artery disease Assessment of the adequacy of the circulation is an important
component of the evaluation of all wounds, and particularly wounds found in patients with diabetes. Symptoms
of claudication or extremity pain at rest, and physical findings of diminished or absent pulses, cool temperature,
pallor on elevation, or dependent rubor should raise suspicion about the presence of peripheral artery disease.
Noninvasive vascular studies including ankle-brachial index, pulse volume recordings and duplex
ultrasonography should be obtained to confirm the diagnosis. (See "Evaluation of the diabetic foot", section on
'Physical signs of peripheral artery disease'.)
The ankle-brachial index is a measurement of the ratio of blood pressure at the ankle to that in the brachial
artery that correlates with the presence and severity of arterial occlusive disease [43]. In patients with diabetes,
the blood vessels may be incompressible and ankle-brachial index values misleading. Segmental volume
plethysmography and toe-brachial index values are more reliable for determining the severity of disease. The
noninvasive diagnosis of lower extremity peripheral artery disease is reviewed in detail elsewhere. (See
7/15/2014 Management of diabetic foot lesions
http://www.uptodate.com/contents/management-of-diabetic-foot-lesions?topicKey=SURG%2F8175&elapsedTimeMs=3&source=search_result&searchTer 5/23
"Noninvasive diagnosis of arterial disease".)
Assess for osteomyelitis Osteomyelitis is likely to be present if bone can be seen at the floor of a deep
ulcer, or if it can be easily detected by probing the ulcer with a sterile, blunt stainless steel probe. Other signs
that suggest osteomyelitis are an ulcer size larger than 2 x 2 cm and an otherwise unexplained elevation in the
erythrocyte sedimentation rate. (See "Clinical manifestations, diagnosis, and management of diabetic infections
of the lower extremities", section on 'Diagnosis of underlying osteomyelitis'.)
Radiologic tests Radiologic tests may be useful if the diagnosis of osteomyelitis remains uncertain. The
diagnosis is clear if osteomyelitis is visible on plain radiographs. However, radiologic changes occur late in the
course of osteomyelitis and negative radiographs do not exclude it. Other imaging techniques that may be
useful in selective cases include radionuclide bone imaging, magnetic resonance imaging and imaging with
indium-labeled leukocytes.
Bone biopsy If clinical and radiographic assessments fail to provide a diagnosis, then bone biopsy can
be considered. Bone biopsy does carry the risk of inoculating an otherwise uninfected bone if the biopsy is
obtained through an infected soft tissue bed. (See "Approach to imaging modalities in the setting of suspected
osteomyelitis".)
Treatment The treatment of grade 3 lesions includes debridement, infection control, local wound care, and
relief of pressure. The presence of osteomyelitis or peripheral artery disease warrants additional therapy [44].
Coordination of care among providers is important for keeping rates of amputation as low as possible. This was
illustrated in a study of 10 Department of Veterans Affairs (VA) medical centers in which increased rates of
amputation were seen in programs with the lowest scores for availability of clinical protocols, educational
seminars, discharge planning and quality of care meetings [45].
Antimicrobial therapy Whether it is important to make a definitive diagnosis of osteomyelitis and
whether patients with osteomyelitis should always be treated by hospitalization, intravenous antimicrobial drug
therapy, and surgical debridement of bone are debated [46]. Some authors have suggested that osteomyelitis is
present in as many as two-thirds of diabetic patients who have foot ulcers [47], but this figure is much higher
than is generally believed and may reflect bias in the severity of the cases studied. Surgical removal of infected
bone may be necessary if the ulcer is not healing. A short period of hospitalization, with surgical debridement,
including culture of material obtained from deep in the ulcer and bone biopsy, is often helpful in choosing
antibiotic therapy [48]. Parenteral antibiotic therapy based upon the culture results has traditionally been given
for four to six weeks in patients with osteomyelitis. The optimal regimen and when to transition to oral therapy
are dependent upon the clinical features of each case. (See "Clinical manifestations, diagnosis, and
management of diabetic infections of the lower extremities", section on 'Antimicrobial therapy'.)
Mechanical off-loading Mechanical off-loading relieves pressure on the ulcer and enhances healing.
Total contact casting and cast walkers are alternatives to prolonged bed rest for the relief of pressure and allow
for continued ambulation. (See 'Mechanical off-loading' above.)
Revascularization Revascularization plays an important role in the management of diabetic foot ulcers
in patients with documented peripheral artery disease (to avoid the need for amputation) [9]. In patients with
diabetes, foot ulcers, and critical limb ischemia, revascularization, when possible, is associated with a lower
incidence of amputation. As an example, in a longitudinal study of 564 patients with diabetes, foot ulcers (in 85
percent of subjects), and critical limb ischemia (defined as ankle-pressure <70 mmHg), angioplasty (PTA) or
bypass grafting (BPG) was performed in 74.5 and 20.6 percent, respectively [49]. Neither procedure was
possible in the remaining 4.9 percent. Among patients who received PTA, BPG, or no revascularization,
amputations were ultimately performed in 8.2, 21.2, and 59.2 percent, respectively.
GRADE 4 AND 5 LESIONS Patients with these more advanced lesions require urgent hospital admission
and surgical consultation, and amputation may sometimes be required. (See "Clinical manifestations,
diagnosis, and management of diabetic infections of the lower extremities".)
ADVANCED THERAPIES Several approaches have been reported that may improve ulcer healing, such as
vacuum-assisted wound closure, the use of custom-fit semipermeable polymeric membrane dressings, cultured
human dermis, and application of products such as platelet-derived growth factors and platelet releasate [50-52].
7/15/2014 Management of diabetic foot lesions
http://www.uptodate.com/contents/management-of-diabetic-foot-lesions?topicKey=SURG%2F8175&elapsedTimeMs=3&source=search_result&searchTer 6/23
Negative pressure wound therapy Negative pressure wound therapy (NPWT), also called vacuum-assisted
closure (VAC), involves the application of controlled subatmospheric pressure to the surface of the wound.
NPWT enhances wound healing by increasing wound perfusion, reducing edema, reducing the local bacterial
burden and increasing the formation of granulation tissue. The indications, contraindications, and uses of
negative pressure wound therapy systems are discussed in detail separately. (See "Negative pressure wound
therapy".)
Randomized trials have found that NPWT reduces time to closure of diabetic foot ulcers, and wounds following
diabetic foot surgery [53-58]. In this patient population, NPWT also decreases length of hospitalization,
complication rates, and cost [59-61].
One multicenter trial randomized 342 patients with diabetic foot ulcers (stage 2 or 3 Wagner ulcers, and
adequate vascular perfusion) to negative pressure wound therapy or moist wound therapy (ie, hydrogel,
alginate) [54]. All ulcers were debrided (as needed) within two days of randomization, and the majority of
the patients also received off-loading therapy. The primary endpoint was wound closure. A significantly
greater percentage of patients treated with negative pressure wound therapy achieved wound closure
within the 16 week timeframe of the study compared with alternative medical therapy (43 versus 29
percent). The negative pressure wound therapy group also demonstrated significantly fewer amputations
compared with the alternate medical therapy group (4 versus 10 percent).
Another multicenter trial followed 162 diabetic patients for 16 weeks following partial foot amputation [53].
The percentage of patients with healed wounds (56 versus 39 percent) and time to complete closure (42
versus 84 days) were significantly improved in patients randomized to vacuum-assisted wound closure
group compared with the control group.
Skin substitutes Human skin equivalents have been studied in diabetic patients with noninfected,
nonischemic chronic plantar ulcers [51,62-65]. In one study of 208 patients, weekly application of the cultured
skin equivalent (Graftskin) for four weeks improved the healing rate compared with usual care (complete wound
healing in 56 and 38 percent of patients, respectively) [62]. Bioengineered skin substitutes (Dermagraft, Apligraf)
are also available for the treatment of nonhealing diabetic foot ulcers [63,64].
Growth factors A platelet-derived growth factor gel preparation (becaplermin) is approved by the US Food
and Drug Administration as an adjuvant therapy for diabetic foot ulcers [66]. It promotes cellular proliferation and
angiogenesis and thereby improves wound healing. However, its use has been limited by high cost and by post-
marketing reports of an increased rate of mortality secondary to malignancy in patients treated with three or
more tubes of becaplermin (3.9 versus 0.9 in controls per 1000 person years) [67]. In another trial, local
application of human epidermal growth factor was shown to promote healing of diabetic foot ulcers [68].
Hyperbaric oxygen therapy Hyperbaric oxygen therapy, as a component of diabetic ulcer management,
may be associated with improved healing but the indications for hyperbaric oxygen in the treatment of
nonhealing diabetic foot ulcers remain uncertain. Several metaanalyses of these trials have concluded that
hyperbaric oxygen therapy in the treatment of diabetic foot ulcers may offer a benefit; however, each noted that
the methodologic quality of the included studies was poor and there was a potential for bias [69-73]. The
available trials are limited by small sample size and heterogeneity of the wounds being treated (eg, ulcer size,
ulcer depth, microbial environment, presence of ischemia) [74-83]. No conclusions could be drawn regarding
specific indications for or timing of therapy.
A pooled analysis found significantly improved wound healing (OR 9.99, 95% CI 3.97-25.1), and decreased risk
of amputation (OR 0.24, 95% CI 0.14-0.43) [70]. A later metaanalysis found similar results [73]. As an example
of these effects, in one of the larger trials that included 70 patients with severely ischemic foot ulcers (Wagner
grades 3 and 4), the amputation rate was 9 percent in the treatment group and 33 percent in the control [74]. In
another trial that included 94 patients, a significantly increased incidence of complete healing (Wagner 2 though
4 ulcers) was achieved in the hyperbaric oxygen therapy group (52 versus 29 percent) compared with a placebo
group [81].
Therapies that combine hyperbaric oxygen therapy with known mediators of wound healing may augment the
effects of hyperbaric oxygen. Activation and mobilization of endothelial progenitor cells (EPCs) are impaired in
7/15/2014 Management of diabetic foot lesions
http://www.uptodate.com/contents/management-of-diabetic-foot-lesions?topicKey=SURG%2F8175&elapsedTimeMs=3&source=search_result&searchTer 7/23
patients with diabetes. These cells are known to play an important role in wound healing by participating in the
formation of new blood vessels in areas of hypoxia [84-87]. Hyperoxia effectively improves EPC mobilization, but
does not specifically target to a specific site which may, in part, explain the nonuniform improvement in diabetic
foot wounds with hyperbaric oxygen therapy alone [88]. However, in a murine model of diabetes,
coadministration of the chemokine stromal cell-derived factor-1 alpha (SDF-1 alpha) resulted in homing of
activated EPCs into the wound site [89]. These data suggest that combining hyperbaric oxygen therapy with
administration of SDF-1 alpha may be synergistic. Other combination therapies (eg, fibroblast growth factor) are
also being studied [90,91].
Other agents Small trials have shown some promise for other topical agents. In a randomized study,
application of .05 percent tretinoin solution for 10 minutes a day followed by iodine gel for four weeks resulted in
complete resolution of 46 percent of the ulcers in the treatment group (n = 13) compared with 18 percent in the
control group (n = 11) [92]. In addition, electrical stimulation near the ulcer may also help slowly healing ulcers
[93,94].
INFORMATION FOR PATIENTS UpToDate offers two types of patient education materials, The Basics and
Beyond the Basics. The Basics patient education pieces are written in plain language, at the 5 to 6 grade
reading level, and they answer the four or five key questions a patient might have about a given condition. These
articles are best for patients who want a general overview and who prefer short, easy-to-read materials. Beyond
the Basics patient education pieces are longer, more sophisticated, and more detailed. These articles are
written at the 10 to 12 grade reading level and are best for patients who want in-depth information and are
comfortable with some medical jargon.
Here are the patient education articles that are relevant to this topic. We encourage you to print or e-mail these
topics to your patients. (You can also locate patient education articles on a variety of subjects by searching on
patient info and the keyword(s) of interest.)
Beyond the Basics topics (see "Patient information: Diabetes mellitus type 1: Overview (Beyond the
Basics)" and "Patient information: Diabetes mellitus type 2: Overview (Beyond the Basics)" and "Patient
information: Foot care in diabetes mellitus (Beyond the Basics)")
SUMMARY AND RECOMMENDATIONS
The treatment of diabetic foot ulcers begins with a comprehensive assessment of the ulcer and the
patient's overall medical condition. Evidence of underlying neuropathy, bony deformity, and peripheral
artery disease should be actively sought. The wound is classified upon initial presentation and with each
follow-up visit using a standardized system to document the examination, plan treatment, and follow the
progress of healing. (See 'Introduction' above and 'Wound classification' above.)
Adequate debridement, proper local wound care, relief of pressure on the ulcer by mechanical off-loading,
and control of infection (when present) are important components of therapy. Dressings are selected
based upon wound characteristics. (See 'Local wound care' above.)
Several methods are available to achieve mechanical off-loading and include total contact casts, cast
walkers, wedge shoes, and bedrest. (See 'Mechanical off-loading' above.)
Few data are available comparing methods of debridement (sharp, enzymatic, autolytic, mechanical, and
biological). In the absence of such data, we suggest surgical (sharp) debridement rather than another
method (Grade 2C). If a surgeon with clinical expertise in sharp debridement is not available, we suggest
autolytic debridement with hydrogels (Grade 2C). (See 'Method of debridement' above.) Alternatively, the
patient can be referred to a facility with appropriate surgical expertise in the management of diabetic foot
problems.
For managing extensive open wounds following debridement for infection or necrosis, or partial foot
amputation, we suggest negative pressure wound therapy (Grade 2A). All necrotic tissue or infected
bone (osteomyelitis) must be removed from the wound prior to using this device. (See 'Negative pressure
wound therapy' above and "Negative pressure wound therapy", section on 'Contraindications'.)
th th
th th
7/15/2014 Management of diabetic foot lesions
http://www.uptodate.com/contents/management-of-diabetic-foot-lesions?topicKey=SURG%2F8175&elapsedTimeMs=3&source=search_result&searchTer 8/23
In patients with Wagner grade 3 and higher ulcers with critical limb ischemia, we recommend
revascularization (Grade 1B). Revascularization should also be performed in patients with any degree of
limb ischemia and a nonhealing ulcer. (See 'Grade 3 lesions' above.)
Patients with Wagner grade 4 and 5 ulcers require immediate surgical consultation. (See 'Grade 4 and 5
lesions' above.)
Use of UpToDate is subject to the Subscription and License Agreement.
REFERENCES
1. Boulton AJ, Armstrong DG, Albert SF, et al. Comprehensive foot examination and risk assessment: a
report of the task force of the foot care interest group of the American Diabetes Association, with
endorsement by the American Association of Clinical Endocrinologists. Diabetes Care 2008; 31:1679.
2. National Diabetes Data Group. Diabetes in America, 2nd Edition, National Institutes of Health,
Washington, D.C p.409.
3. American Diabetes Association. Clinical Practice Recommendations: foot care in patients with diabetes
mellitus. Diabetes Care 1996; 19:S23.
4. Ramsey SD, Newton K, Blough D, et al. Incidence, outcomes, and cost of foot ulcers in patients with
diabetes. Diabetes Care 1999; 22:382.
5. Gregg EW, Sorlie P, Paulose-Ram R, et al. Prevalence of lower-extremity disease in the US adult
population >=40 years of age with and without diabetes: 1999-2000 national health and nutrition
examination survey. Diabetes Care 2004; 27:1591.
6. O'Neal, LW, Wagner, FW. The Diabetic Foot, Mosby, St Louis 1983. p.274.
7. Brodsky JW. Outpatient diagnosis and care of the diabetic foot. Instr Course Lect 1993; 42:121.
8. Frykberg RG, Zgonis T, Armstrong DG, et al. Diabetic foot disorders. A clinical practice guideline (2006
revision). J Foot Ankle Surg 2006; 45:S1.
9. Khanolkar MP, Bain SC, Stephens JW. The diabetic foot. QJM 2008; 101:685.
10. Oyibo SO, Jude EB, Tarawneh I, et al. A comparison of two diabetic foot ulcer classification systems: the
Wagner and the University of Texas wound classification systems. Diabetes Care 2001; 24:84.
11. Lavery LA, Armstrong DG, Harkless LB. Classification of diabetic foot wounds. J Foot Ankle Surg 1996;
35:528.
12. Schaper NC. Diabetic foot ulcer classification system for research purposes: a progress report on criteria
for including patients in research studies. Diabetes Metab Res Rev 2004; 20 Suppl 1:S90.
13. Cardinal M, Eisenbud DE, Armstrong DG, et al. Serial surgical debridement: a retrospective study on
clinical outcomes in chronic lower extremity wounds. Wound Repair Regen 2009; 17:306.
14. Armstrong DG, Lavery LA, Nixon BP, Boulton AJ. It's not what you put on, but what you take off:
techniques for debriding and off-loading the diabetic foot wound. Clin Infect Dis 2004; 39 Suppl 2:S92.
15. Margolis DJ, Kantor J, Berlin JA. Healing of diabetic neuropathic foot ulcers receiving standard treatment.
A meta-analysis. Diabetes Care 1999; 22:692.
16. Lebrun E, Tomic-Canic M, Kirsner RS. The role of surgical debridement in healing of diabetic foot ulcers.
Wound Repair Regen 2010; 18:433.
17. Steed DL, Donohoe D, Webster MW, Lindsley L. Effect of extensive debridement and treatment on the
healing of diabetic foot ulcers. Diabetic Ulcer Study Group. J Am Coll Surg 1996; 183:61.
18. Edwards J, Stapley S. Debridement of diabetic foot ulcers. Cochrane Database Syst Rev 2010;
:CD003556.
19. Joseph WS, Lipsky BA. Medical therapy of diabetic foot infections. J Vasc Surg 2010; 52:67S.
20. Lipsky BA. Medical treatment of diabetic foot infections. Clin Infect Dis 2004; 39 Suppl 2:S104.
21. Lipsky BA, Pecoraro RE, Larson SA, et al. Outpatient management of uncomplicated lower-extremity
infections in diabetic patients. Arch Intern Med 1990; 150:790.
7/15/2014 Management of diabetic foot lesions
http://www.uptodate.com/contents/management-of-diabetic-foot-lesions?topicKey=SURG%2F8175&elapsedTimeMs=3&source=search_result&searchTer 9/23
22. Lipsky BA, Berendt AR, Cornia PB, et al. 2012 Infectious Diseases Society of America clinical practice
guideline for the diagnosis and treatment of diabetic foot infections. Clin Infect Dis 2012; 54:e132.
23. Bergin SM, Wraight P. Silver based wound dressings and topical agents for treating diabetic foot ulcers.
Cochrane Database Syst Rev 2006; :CD005082.
24. Cavanagh PR, Bus SA. Off-loading the diabetic foot for ulcer prevention and healing. J Vasc Surg 2010;
52:37S.
25. Spencer S. Pressure relieving interventions for preventing and treating diabetic foot ulcers. Cochrane
Database Syst Rev 2000; :CD002302.
26. Lewis J, Lipp A. Pressure-relieving interventions for treating diabetic foot ulcers. Cochrane Database Syst
Rev 2013; :CD002302.
27. Katz IA, Harlan A, Miranda-Palma B, et al. A randomized trial of two irremovable off-loading devices in the
management of plantar neuropathic diabetic foot ulcers. Diabetes Care 2005; 28:555.
28. Mueller, MJ, Diamond, JE, Sinacore, DR, et al. Total contact casting in treatment of diabetic plantar
ulcers: controlled clinical trial. Diabetes Care 1989; 12:384.
29. Caravaggi C, Faglia E, De Giglio R, et al. Effectiveness and safety of a nonremovable fiberglass off-bearing
cast versus a therapeutic shoe in the treatment of neuropathic foot ulcers: a randomized study. Diabetes
Care 2000; 23:1746.
30. Armstrong DG, Nguyen HC, Lavery LA, et al. Off-loading the diabetic foot wound: a randomized clinical
trial. Diabetes Care 2001; 24:1019.
31. Nabuurs-Franssen MH, Huijberts MS, Sleegers R, Schaper NC. Casting of recurrent diabetic foot ulcers:
effective and safe? Diabetes Care 2005; 28:1493.
32. Piaggesi A, Macchiarini S, Rizzo L, et al. An off-the-shelf instant contact casting device for the
management of diabetic foot ulcers: a randomized prospective trial versus traditional fiberglass cast.
Diabetes Care 2007; 30:586.
33. Piaggesi A, Viacava P, Rizzo L, et al. Semiquantitative analysis of the histopathological features of the
neuropathic foot ulcer: effects of pressure relief. Diabetes Care 2003; 26:3123.
34. Mueller MJ, Sinacore DR, Hastings MK, et al. Effect of Achilles tendon lengthening on neuropathic plantar
ulcers. A randomized clinical trial. J Bone Joint Surg Am 2003; 85-A:1436.
35. Lavery LA, Vela SA, Lavery DC, Quebedeaux TL. Total contact casts: pressure reduction at ulcer sites
and the effect on the contralateral foot. Arch Phys Med Rehabil 1997; 78:1268.
36. Armstrong DG, Lavery LA, Kimbriel HR, et al. Activity patterns of patients with diabetic foot ulceration:
patients with active ulceration may not adhere to a standard pressure off-loading regimen. Diabetes Care
2003; 26:2595.
37. Baumhauer JF, Wervey R, McWilliams J, et al. A comparison study of plantar foot pressure in a
standardized shoe, total contact cast, and prefabricated pneumatic walking brace. Foot Ankle Int 1997;
18:26.
38. Pollo FE, Brodsky JW, Crenshaw SJ, Kirksey C. Plantar pressures in fiberglass total contact casts vs. a
new diabetic walking boot. Foot Ankle Int 2003; 24:45.
39. Faglia E, Caravaggi C, Clerici G, et al. Effectiveness of removable walker cast versus nonremovable
fiberglass off-bearing cast in the healing of diabetic plantar foot ulcer: a randomized controlled trial.
Diabetes Care 2010; 33:1419.
40. Reiber GE, Smith DG, Wallace C, et al. Effect of therapeutic footwear on foot reulceration in patients with
diabetes: a randomized controlled trial. JAMA 2002; 287:2552.
41. Brown D, Wertsch JJ, Harris GF, et al. Effect of rocker soles on plantar pressures. Arch Phys Med
Rehabil 2004; 85:81.
42. Busch K, Chantelau E. Effectiveness of a new brand of stock 'diabetic' shoes to protect against diabetic
foot ulcer relapse. A prospective cohort study. Diabet Med 2003; 20:665.
43. Fowkes FG. The measurement of atherosclerotic peripheral arterial disease in epidemiological surveys. Int
J Epidemiol 1988; 17:248.
44. Pecoraro RE, Reiber GE, Burgess EM. Pathways to diabetic limb amputation. Basis for prevention.
Diabetes Care 1990; 13:513.
45. Wrobel JS, Charns MP, Diehr P, et al. The relationship between provider coordination and diabetes-related
7/15/2014 Management of diabetic foot lesions
http://www.uptodate.com/contents/management-of-diabetic-foot-lesions?topicKey=SURG%2F8175&elapsedTimeMs=3&source=search_result&searchTe 10/23
foot outcomes. Diabetes Care 2003; 26:3042.
46. Eckman MH, Greenfield S, Mackey WC, et al. Foot infections in diabetic patients. Decision and cost-
effectiveness analyses. JAMA 1995; 273:712.
47. Newman LG, Waller J, Palestro CJ, et al. Unsuspected osteomyelitis in diabetic foot ulcers. Diagnosis
and monitoring by leukocyte scanning with indium in 111 oxyquinoline. JAMA 1991; 266:1246.
48. Mushlin AI, Littenberg B. Diagnosing pedal osteomyelitis: testing choices and their consequences. J Gen
Intern Med 1994; 9:1.
49. Faglia E, Clerici G, Clerissi J, et al. Long-term prognosis of diabetic patients with critical limb ischemia: a
population-based cohort study. Diabetes Care 2009; 32:822.
50. Blackman JD, Senseng D, Quinn L, Mazzone T. Clinical evaluation of a semipermeable polymeric
membrane dressing for the treatment of chronic diabetic foot ulcers. Diabetes Care 1994; 17:322.
51. Marston WA, Hanft J, Norwood P, et al. The efficacy and safety of Dermagraft in improving the healing of
chronic diabetic foot ulcers: results of a prospective randomized trial. Diabetes Care 2003; 26:1701.
52. Margolis DJ, Kantor J, Santanna J, et al. Effectiveness of platelet releasate for the treatment of diabetic
neuropathic foot ulcers. Diabetes Care 2001; 24:483.
53. Armstrong DG, Lavery LA, Diabetic Foot Study Consortium. Negative pressure wound therapy after partial
diabetic foot amputation: a multicentre, randomised controlled trial. Lancet 2005; 366:1704.
54. Blume PA, Walters J, Payne W, et al. Comparison of negative pressure wound therapy using vacuum-
assisted closure with advanced moist wound therapy in the treatment of diabetic foot ulcers: a multicenter
randomized controlled trial. Diabetes Care 2008; 31:631.
55. McCallon SK, Knight CA, Valiulus JP, et al. Vacuum-assisted closure versus saline-moistened gauze in
the healing of postoperative diabetic foot wounds. Ostomy Wound Manage 2000; 46:28.
56. Eginton MT, Brown KR, Seabrook GR, et al. A prospective randomized evaluation of negative-pressure
wound dressings for diabetic foot wounds. Ann Vasc Surg 2003; 17:645.
57. Ford CN, Reinhard ER, Yeh D, et al. Interim analysis of a prospective, randomized trial of vacuum-
assisted closure versus the healthpoint system in the management of pressure ulcers. Ann Plast Surg
2002; 49:55.
58. Etoz, A, Ozgenel, Y, Ozcan, M. The use of negative pressure wound therapy on diabetic foot ulcers.
Wounds 2004; 16:264.
59. Philbeck, TE, Schroeder, WJ, Whittington, KT. Vacuum-assisted closure therapy for diabetic foot ulcers:
clinical and cost analysis. Home Health Consultant 2001; 8:1.
60. Armstrong DG, Lavery LA, Abu-Rumman P, et al. Outcomes of subatmospheric pressure dressing
therapy on wounds of the diabetic foot. Ostomy Wound Manage 2002; 48:64.
61. Andros G, Armstrong DG, Attinger CE, et al. Consensus statement on negative pressure wound therapy
(V.A.C. Therapy) for the management of diabetic foot wounds. Ostomy Wound Manage 2006; Suppl:1.
62. Veves A, Falanga V, Armstrong DG, et al. Graftskin, a human skin equivalent, is effective in the
management of noninfected neuropathic diabetic foot ulcers: a prospective randomized multicenter clinical
trial. Diabetes Care 2001; 24:290.
63. Edmonds M, Bates M, Doxford M, et al. New treatments in ulcer healing and wound infection. Diabetes
Metab Res Rev 2000; 16 Suppl 1:S51.
64. Barber C, Watt A, Pham C, et al. Influence of bioengineered skin substitutes on diabetic foot ulcer and
venous leg ulcer outcomes. J Wound Care 2008; 17:517.
65. Kirsner RS, Warriner R, Michela M, et al. Advanced biological therapies for diabetic foot ulcers. Arch
Dermatol 2010; 146:857.
66. Wieman TJ, Smiell JM, Su Y. Efficacy and safety of a topical gel formulation of recombinant human
platelet-derived growth factor-BB (becaplermin) in patients with chronic neuropathic diabetic ulcers. A
phase III randomized placebo-controlled double-blind study. Diabetes Care 1998; 21:822.
67. http://www.regranex.com/ (Accessed on October 07, 2010).
68. Tsang MW, Wong WK, Hung CS, et al. Human epidermal growth factor enhances healing of diabetic foot
ulcers. Diabetes Care 2003; 26:1856.
69. Kranke P, Bennett M, Roeckl-Wiedmann I, Debus S. Hyperbaric oxygen therapy for chronic wounds.
Cochrane Database Syst Rev 2004; :CD004123.
7/15/2014 Management of diabetic foot lesions
http://www.uptodate.com/contents/management-of-diabetic-foot-lesions?topicKey=SURG%2F8175&elapsedTimeMs=3&source=search_result&searchTe 11/23
70. Goldman RJ. Hyperbaric oxygen therapy for wound healing and limb salvage: a systematic review. PM R
2009; 1:471.
71. Roeckl-Wiedmann I, Bennett M, Kranke P. Systematic review of hyperbaric oxygen in the management of
chronic wounds. Br J Surg 2005; 92:24.
72. Wang C, Schwaitzberg S, Berliner E, et al. Hyperbaric oxygen for treating wounds: a systematic review of
the literature. Arch Surg 2003; 138:272.
73. Liu R, Li L, Yang M, et al. Systematic review of the effectiveness of hyperbaric oxygenation therapy in the
management of chronic diabetic foot ulcers. Mayo Clin Proc 2013; 88:166.
74. Faglia E, Favales F, Aldeghi A, et al. Adjunctive systemic hyperbaric oxygen therapy in treatment of
severe prevalently ischemic diabetic foot ulcer. A randomized study. Diabetes Care 1996; 19:1338.
75. Duzgun AP, Satir HZ, Ozozan O, et al. Effect of hyperbaric oxygen therapy on healing of diabetic foot
ulcers. J Foot Ankle Surg 2008; 47:515.
76. Kessler L, Bilbault P, Ortga F, et al. Hyperbaric oxygenation accelerates the healing rate of nonischemic
chronic diabetic foot ulcers: a prospective randomized study. Diabetes Care 2003; 26:2378.
77. Abidia A, Laden G, Kuhan G, et al. The role of hyperbaric oxygen therapy in ischaemic diabetic lower
extremity ulcers: a double-blind randomised-controlled trial. Eur J Vasc Endovasc Surg 2003; 25:513.
78. Doctor N, Pandya S, Supe A. Hyperbaric oxygen therapy in diabetic foot. J Postgrad Med 1992; 38:112.
79. Lin, TF, Chen, et al. The vascular effects of hyperbaric oxygen therapy in treatment of early diabetic foot.
Undersea Hyperb Med 2001; 28(suppl):63.
80. Hammarlund C, Sundberg T. Hyperbaric oxygen reduced size of chronic leg ulcers: a randomized double-
blind study. Plast Reconstr Surg 1994; 93:829.
81. Lndahl M, Katzman P, Nilsson A, Hammarlund C. Hyperbaric oxygen therapy facilitates healing of
chronic foot ulcers in patients with diabetes. Diabetes Care 2010; 33:998.
82. Zamboni WA, Wong HP, Stephenson LL, Pfeifer MA. Evaluation of hyperbaric oxygen for diabetic
wounds: a prospective study. Undersea Hyperb Med 1997; 24:175.
83. Baroni G, Porro T, Faglia E, et al. Hyperbaric oxygen in diabetic gangrene treatment. Diabetes Care 1987;
10:81.
84. Brem H, Tomic-Canic M. Cellular and molecular basis of wound healing in diabetes. J Clin Invest 2007;
117:1219.
85. Silvestre JS, Lvy BI. [Diabetes and peripheral arterial occlusive disease: therapeutic potential and pro-
angiogenic strategies]. Ann Cardiol Angeiol (Paris) 2006; 55:100.
86. Capoccia BJ, Robson DL, Levac KD, et al. Revascularization of ischemic limbs after transplantation of
human bone marrow cells with high aldehyde dehydrogenase activity. Blood 2009; 113:5340.
87. Hung SC, Pochampally RR, Chen SC, et al. Angiogenic effects of human multipotent stromal cell
conditioned medium activate the PI3K-Akt pathway in hypoxic endothelial cells to inhibit apoptosis,
increase survival, and stimulate angiogenesis. Stem Cells 2007; 25:2363.
88. Berendt AR. Counterpoint: hyperbaric oxygen for diabetic foot wounds is not effective. Clin Infect Dis
2006; 43:193.
89. Gallagher KA, Liu ZJ, Xiao M, et al. Diabetic impairments in NO-mediated endothelial progenitor cell
mobilization and homing are reversed by hyperoxia and SDF-1 alpha. J Clin Invest 2007; 117:1249.
90. Efrati S, Gall N, Bergan J, et al. Hyperbaric oxygen, oxidative stress, NO bioavailability and ulcer
oxygenation in diabetic patients. Undersea Hyperb Med 2009; 36:1.
91. Nakada T, Saito Y, Chikenji M, et al. Therapeutic outcome of hyperbaric oxygen and basic fibroblast
growth factor on intractable skin ulcer in legs: preliminary report. Plast Reconstr Surg 2006; 117:646.
92. Tom WL, Peng DH, Allaei A, et al. The effect of short-contact topical tretinoin therapy for foot ulcers in
patients with diabetes. Arch Dermatol 2005; 141:1373.
93. Baker LL, Chambers R, DeMuth SK, Villar F. Effects of electrical stimulation on wound healing in patients
with diabetic ulcers. Diabetes Care 1997; 20:405.
94. Peters EJ, Lavery LA, Armstrong DG, Fleischli JG. Electric stimulation as an adjunct to heal diabetic foot
ulcers: a randomized clinical trial. Arch Phys Med Rehabil 2001; 82:721.
Topic 8175 Version 15.0
7/15/2014 Management of diabetic foot lesions
http://www.uptodate.com/contents/management-of-diabetic-foot-lesions?topicKey=SURG%2F8175&elapsedTimeMs=3&source=search_result&searchTe 12/23
7/15/2014 Management of diabetic foot lesions
http://www.uptodate.com/contents/management-of-diabetic-foot-lesions?topicKey=SURG%2F8175&elapsedTimeMs=3&source=search_result&searchTe 13/23
GRAPHICS
Wagner grade 1 ulcer
Foot from a diabetic patient showing a superficial ulcer (Wagner grade
1) that involves the full thickness of the skin but no underlying
tissues. This lesion healed quickly with rest and local foot care.
Courtesy of David McCulloch, MD.
Graphic 70998 Version 1.0
7/15/2014 Management of diabetic foot lesions
http://www.uptodate.com/contents/management-of-diabetic-foot-lesions?topicKey=SURG%2F8175&elapsedTimeMs=3&source=search_result&searchTe 14/23
Wagner grade 2 ulcer
Foot from a diabetic patient with a penetrating neuropathic ulcer that
is not associated with abscess formation or bone involvement
(Wagner grade 2). The toes have been pulled anteriorly because the
anterior tibial muscles are unopposed due to motor neuropathy-
induced weakness of the intrinsic foot muscles. This promotes
subluxation of the proximal interphalangeal-metatarsal joints, resulting
in a claw toe appearance (arrow) and in increased pressure on the
metatarsal heads, predisposing to ulcer formation at this site.
Courtesy of David McCulloch, MD.
Graphic 51991 Version 2.0
7/15/2014 Management of diabetic foot lesions
http://www.uptodate.com/contents/management-of-diabetic-foot-lesions?topicKey=SURG%2F8175&elapsedTimeMs=3&source=search_result&searchTe 15/23
Wagner 3 foot ulcer
The patient presented with a fluctuant eschar on the plantar surface
of the foot. The abscess was unroofed and drained and, following
debridement, exposed bone was apparent at the base of the wound.
Courtesy of Paul Thottingal, MD.
Graphic 71315 Version 1.0
7/15/2014 Management of diabetic foot lesions
http://www.uptodate.com/contents/management-of-diabetic-foot-lesions?topicKey=SURG%2F8175&elapsedTimeMs=3&source=search_result&searchTe 16/23
Wagner grade 4 ulcer
Foot from a diabetic patient with a Wagner grade 4 ulcer that extends
to the deep layers with signs of local infection, cellulitis, and necrosis.
This lesion healed completely after an extensive hospital stay
involving excision of necrotic tissue but no amputation.
Courtesy of David McCulloch, MD.
Graphic 63780 Version 3.0
7/15/2014 Management of diabetic foot lesions
http://www.uptodate.com/contents/management-of-diabetic-foot-lesions?topicKey=SURG%2F8175&elapsedTimeMs=3&source=search_result&searchTe 17/23
Oral agents for empiric treatment of mild to moderate diabetic foot
infections
SINGLE-drug regimens with activity against streptococci and
staphylococci (MSSA)
Cephalexin or
Dicloxacillin or
Amoxicillin-clavulanate or clindamycin
TWO-drug regimens with activity against streptococci and MRSA
Clindamycin* or
Linezolid or
Penicillin or cefazolin or dicloxacillin
PLUS
Trimethoprim-sulfamethoxazole or doxycycline
TWO-drug regimens with activity against streptococci, MRSA, aerobic
gram-negative bacilli and anaerobes
Trimethoprim-sulfamethoxazole
PLUS
Amoxicillin-clavulanate
-OR-
Clindamycin
PLUS
Ciprofloxacin or levofloxacin or moxifloxacin
Antibiotic dosing for adults
Cephalexin 500 mg every 6 hours
Dicloxacillin 500 mg every 6 hours
Clindamycin 300 to 450 mg every 6 to 8 hours
Linezolid 600 mg every 12 hours
Penicillin V potassium 500 mg every 6 hours
Trimethoprim-sulfamethoxazole (co-
trimoxazole)
2 double-strength tablets (trimethoprim 160 mg
and sulfamethoxazole 800 mg per tablet) every
12 hours
Doxycycline 100 mg orally every 12 hours
Amoxicillin-clavulanate 875/125 mg every 12 hours
Ciprofloxacin 750 mg every 12 hours
Levofloxacin 750 mg every 24 hours
Moxifloxacin 400 mg every 24 hours
7/15/2014 Management of diabetic foot lesions
http://www.uptodate.com/contents/management-of-diabetic-foot-lesions?topicKey=SURG%2F8175&elapsedTimeMs=3&source=search_result&searchTe 18/23
MSSA: methicillin-susecptible staphylococcus aureus; MRSA: methicillin-resistant staphylococcus
aureus.
* Check susceptibility testing.
Many of these agents require adjustment of the dose in the setting of renal dysfunction.
Data courtesy of authors with additional data from: Lipsky BA, et al. 2012 Infectious Diseases
Society of America clinical practice guideline for the diagnosis and treatment of diabetic foot
infections. Clin Infect Dis 2012; 54:e132.
Graphic 69671 Version 4.0
7/15/2014 Management of diabetic foot lesions
http://www.uptodate.com/contents/management-of-diabetic-foot-lesions?topicKey=SURG%2F8175&elapsedTimeMs=3&source=search_result&searchTe 19/23
Removable cast walker
Graphic 64409 Version 1.0
7/15/2014 Management of diabetic foot lesions
http://www.uptodate.com/contents/management-of-diabetic-foot-lesions?topicKey=SURG%2F8175&elapsedTimeMs=3&source=search_result&searchTe 20/23
Rocker sole shoe
Graphic 86276 Version 1.0
7/15/2014 Management of diabetic foot lesions
http://www.uptodate.com/contents/management-of-diabetic-foot-lesions?topicKey=SURG%2F8175&elapsedTimeMs=3&source=search_result&searchTe 21/23
Wedge shoes
Graphic 53678 Version 1.0
7/15/2014 Management of diabetic foot lesions
http://www.uptodate.com/contents/management-of-diabetic-foot-lesions?topicKey=SURG%2F8175&elapsedTimeMs=3&source=search_result&searchTe 22/23
Knee walker
Graphic 73730 Version 1.0
7/15/2014 Management of diabetic foot lesions
http://www.uptodate.com/contents/management-of-diabetic-foot-lesions?topicKey=SURG%2F8175&elapsedTimeMs=3&source=search_result&searchTe 23/23
Di scl osures: David K McCulloch, MD Nothing to disclose. Richard J de Asla, MD Nothing to disclose. John F Eidt, MD
Grant/Research Support: Medtronic CEC (drug eluting balloon). Joseph L Mills, Sr, MD Nothing to disclose. David M Nathan, MD
Nothing to disclose. Kathryn A Collins, MD, PhD, FACS Nothing to disclose.
Contributor disclosures are reviewed f or conf licts of interest by the editorial group. When f ound, these are addressed by vetting
through a multi-level review process, and through requirements f or ref erences to be provided to support the content. Appropriately
ref erenced content is required of all authors and must conf orm to UpToDate standards of evidence.
Conflict of interest policy
Disclosures
You might also like
- Authetication FormDocument3 pagesAuthetication FormWasemBhatNo ratings yet
- (David Weinstock) NeuroKinetic Therapy An InnovatDocument151 pages(David Weinstock) NeuroKinetic Therapy An Innovatsitti fatimah azzahra. m100% (2)
- Achilles Exercise ProtocolDocument2 pagesAchilles Exercise ProtocolkjdgfkjasdhgakjhNo ratings yet
- Achilles Exercise ProtocolDocument2 pagesAchilles Exercise ProtocolkjdgfkjasdhgakjhNo ratings yet
- Scapular Dysfunction Floor or Wall AngelsDocument4 pagesScapular Dysfunction Floor or Wall AngelsWasemBhatNo ratings yet
- Physiotherapy Information For Achilles TendinopathyDocument6 pagesPhysiotherapy Information For Achilles TendinopathyWasemBhatNo ratings yet
- Normative Values For Isometric Muscle Force by Handheld DynamometerDocument14 pagesNormative Values For Isometric Muscle Force by Handheld DynamometerWasemBhatNo ratings yet
- Top Consultancies in MumbaiDocument6 pagesTop Consultancies in MumbaiWasemBhatNo ratings yet
- Assessment Screening Tools PDFDocument5 pagesAssessment Screening Tools PDFWasemBhatNo ratings yet
- Gulf Careers1 PDFDocument1 pageGulf Careers1 PDFWasemBhatNo ratings yet
- Gulf Careers 2Document18 pagesGulf Careers 2WasemBhatNo ratings yet
- Musculoskeletal Complaints, Physical Activity and Health-Related Quality of Life Among Patients With The Ehlers-Danlos Syndrome Hypermobility Type, Disability and Rehabilitation, Informa HealthcareDocument1 pageMusculoskeletal Complaints, Physical Activity and Health-Related Quality of Life Among Patients With The Ehlers-Danlos Syndrome Hypermobility Type, Disability and Rehabilitation, Informa HealthcareWasemBhatNo ratings yet
- Top Consultancies in MumbaiDocument6 pagesTop Consultancies in MumbaiWasemBhatNo ratings yet
- Ace Business Solutions: Most non-IT SkillsDocument5 pagesAce Business Solutions: Most non-IT SkillsSatya Vardhan PinnojuNo ratings yet
- Joint Hypermobility SyndromeDocument21 pagesJoint Hypermobility SyndromeWasemBhatNo ratings yet
- BMTC Bus Pass FormDocument1 pageBMTC Bus Pass FormWasemBhat33% (3)
- Overview of Geriatric Rehabilitation - Program Components and Settings For RehabilitationDocument37 pagesOverview of Geriatric Rehabilitation - Program Components and Settings For RehabilitationWasemBhat0% (1)
- SampleSize WebDocument2 pagesSampleSize WebHolyxNo ratings yet
- Reliability & Validity of Handheld Dynamometer For Dynamic Muscle Assessment StrengthDocument14 pagesReliability & Validity of Handheld Dynamometer For Dynamic Muscle Assessment StrengthWasemBhatNo ratings yet
- Strength Norms Obtained Dynamometry 20-79Document7 pagesStrength Norms Obtained Dynamometry 20-79WasemBhatNo ratings yet
- Overview of Geriatric Rehabilitation - Program Components and Settings For RehabilitationDocument37 pagesOverview of Geriatric Rehabilitation - Program Components and Settings For RehabilitationWasemBhat0% (1)
- Sample Size DeterminationDocument7 pagesSample Size DeterminationWasemBhatNo ratings yet
- Prosthetic For FootDocument2 pagesProsthetic For FootWasemBhatNo ratings yet
- CSP Physiotherapy Works MSK June 2013Document2 pagesCSP Physiotherapy Works MSK June 2013WasemBhatNo ratings yet
- A Simple Questionnaire To Detect HypermobilDocument2 pagesA Simple Questionnaire To Detect HypermobilWasemBhatNo ratings yet
- Poster Guidelines and FormatDocument3 pagesPoster Guidelines and FormatWasemBhatNo ratings yet
- Science Fair Paper Writing GuideDocument6 pagesScience Fair Paper Writing GuideWasemBhatNo ratings yet
- Abbreviations Used in Most HospitalDocument11 pagesAbbreviations Used in Most HospitalWasemBhatNo ratings yet
- Test & MeasurmentDocument5 pagesTest & MeasurmentWasemBhatNo ratings yet
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeFrom EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeRating: 4 out of 5 stars4/5 (5794)
- Shoe Dog: A Memoir by the Creator of NikeFrom EverandShoe Dog: A Memoir by the Creator of NikeRating: 4.5 out of 5 stars4.5/5 (537)
- The Yellow House: A Memoir (2019 National Book Award Winner)From EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Rating: 4 out of 5 stars4/5 (98)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceFrom EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceRating: 4 out of 5 stars4/5 (895)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersFrom EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersRating: 4.5 out of 5 stars4.5/5 (344)
- The Little Book of Hygge: Danish Secrets to Happy LivingFrom EverandThe Little Book of Hygge: Danish Secrets to Happy LivingRating: 3.5 out of 5 stars3.5/5 (399)
- Grit: The Power of Passion and PerseveranceFrom EverandGrit: The Power of Passion and PerseveranceRating: 4 out of 5 stars4/5 (588)
- The Emperor of All Maladies: A Biography of CancerFrom EverandThe Emperor of All Maladies: A Biography of CancerRating: 4.5 out of 5 stars4.5/5 (271)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaFrom EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaRating: 4.5 out of 5 stars4.5/5 (266)
- Never Split the Difference: Negotiating As If Your Life Depended On ItFrom EverandNever Split the Difference: Negotiating As If Your Life Depended On ItRating: 4.5 out of 5 stars4.5/5 (838)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryFrom EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryRating: 3.5 out of 5 stars3.5/5 (231)
- On Fire: The (Burning) Case for a Green New DealFrom EverandOn Fire: The (Burning) Case for a Green New DealRating: 4 out of 5 stars4/5 (73)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureFrom EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureRating: 4.5 out of 5 stars4.5/5 (474)
- Team of Rivals: The Political Genius of Abraham LincolnFrom EverandTeam of Rivals: The Political Genius of Abraham LincolnRating: 4.5 out of 5 stars4.5/5 (234)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyFrom EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyRating: 3.5 out of 5 stars3.5/5 (2259)
- The Unwinding: An Inner History of the New AmericaFrom EverandThe Unwinding: An Inner History of the New AmericaRating: 4 out of 5 stars4/5 (45)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreFrom EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreRating: 4 out of 5 stars4/5 (1090)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)From EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Rating: 4.5 out of 5 stars4.5/5 (120)
- Her Body and Other Parties: StoriesFrom EverandHer Body and Other Parties: StoriesRating: 4 out of 5 stars4/5 (821)
- Mdindia Healthcare Services (Tpa) Pvt. LTD.: Claim FormDocument4 pagesMdindia Healthcare Services (Tpa) Pvt. LTD.: Claim FormShubakar ReddyNo ratings yet
- Pbibliografia HipnoterapiaycancerDocument5 pagesPbibliografia HipnoterapiaycancerAnonymous 8XPmSvNo ratings yet
- Summary For The Case Study On MastectomyDocument2 pagesSummary For The Case Study On MastectomyNishi SharmaNo ratings yet
- MJMHS 0150Document8 pagesMJMHS 0150Dasana SunnyNo ratings yet
- Pediatric Transplant Rating InstrumentDocument10 pagesPediatric Transplant Rating InstrumentcoxalfonsoNo ratings yet
- Hyperemesis Gravidarum: Kelompok 5 Andi Cipta Andi Salma Vadhila Nur Alia Resmi Julita Putri RismayantiDocument7 pagesHyperemesis Gravidarum: Kelompok 5 Andi Cipta Andi Salma Vadhila Nur Alia Resmi Julita Putri RismayantiChayeol ParkNo ratings yet
- Fixed Orthodontic Retainers: A ReviewDocument5 pagesFixed Orthodontic Retainers: A ReviewhelmysiswantoNo ratings yet
- Mod 6 CommunicationDocument43 pagesMod 6 CommunicationAhmad FarooqNo ratings yet
- Flabby RidgeDocument4 pagesFlabby RidgeBrijesh MaskeyNo ratings yet
- Ambuja Cement Foundation Visit ReportDocument5 pagesAmbuja Cement Foundation Visit ReportRavisinh ValaNo ratings yet
- Estrope, Czryn Gylsy O. - Prescription Interpretation and Analysis in PHARM 201Document3 pagesEstrope, Czryn Gylsy O. - Prescription Interpretation and Analysis in PHARM 201Czryn Gylsy EstropeNo ratings yet
- HealinginzionDocument139 pagesHealinginzionShoshannahNo ratings yet
- sp500 CompaniesDocument38 pagessp500 CompaniesWayne De FranceNo ratings yet
- Dwnload Full Foundations of Maternal Newborn and Womens Health Nursing 7th Edition Murray Test Bank PDFDocument35 pagesDwnload Full Foundations of Maternal Newborn and Womens Health Nursing 7th Edition Murray Test Bank PDFroxaneblyefx100% (13)
- Up-To-Date at The Age of Implant Dentistry: VestibuloplastyDocument3 pagesUp-To-Date at The Age of Implant Dentistry: VestibuloplastyDemmy WijayaNo ratings yet
- Capp Mdi With SpacerDocument1 pageCapp Mdi With SpacerHopeton SinclairNo ratings yet
- 6 The Comparison of The Effects of Clinical Pilates Exercises With and Without Childbirth Training On Pregnancy and Birth ResultsDocument28 pages6 The Comparison of The Effects of Clinical Pilates Exercises With and Without Childbirth Training On Pregnancy and Birth Resultseamaeama7No ratings yet
- Pqa Executive Fellow Q ADocument3 pagesPqa Executive Fellow Q Aapi-407904109No ratings yet
- PsychologicaldisorderprojectDocument4 pagesPsychologicaldisorderprojectapi-280442205No ratings yet
- WHO Surgical Safety Checklist: InstructionsDocument3 pagesWHO Surgical Safety Checklist: InstructionsireneNo ratings yet
- Disruption of Radiologist WorkflowDocument6 pagesDisruption of Radiologist WorkflowChrisNo ratings yet
- Castaneda Goals EssayDocument2 pagesCastaneda Goals Essayapi-510502557No ratings yet
- Neurexan Patient Flyer ANG May 2010 7311Document2 pagesNeurexan Patient Flyer ANG May 2010 7311Waqar GhoryNo ratings yet
- Aesthetic Medicine Training CourseDocument8 pagesAesthetic Medicine Training Coursedrdahabra3No ratings yet
- Implementing Rules & Regulations of Republic Act No. 8972Document15 pagesImplementing Rules & Regulations of Republic Act No. 8972Katherine EvangelistaNo ratings yet
- Induction of Labour Guide 2013 149 Induction of Labour GuidelineDocument14 pagesInduction of Labour Guide 2013 149 Induction of Labour GuidelineSyah Sembung WasisoNo ratings yet
- Anti-Obesity MedicationsDocument33 pagesAnti-Obesity MedicationsJorge Luis Alva AlonsoNo ratings yet
- Reasons For Extraction of Primary Teeth in Jordan-A Study.: August 2013Document5 pagesReasons For Extraction of Primary Teeth in Jordan-A Study.: August 2013Mutia KumalasariNo ratings yet
- LLM Medical Law Dissertation TopicsDocument4 pagesLLM Medical Law Dissertation TopicsBuyCollegePapersOnlineSingapore100% (1)
- Press Release Avantha PHSDocument2 pagesPress Release Avantha PHSSatvinder Deep SinghNo ratings yet