Professional Documents
Culture Documents
Masquelet JAAOS
Uploaded by
Maurinho Mnh0 ratings0% found this document useful (0 votes)
126 views9 pagesA two-stage technique uses induced biologic membranes with delayed placement of bone graft. Excellent clinical results have been reported with reconstruction of segmental bone defects >20 cm. A bioactive membrane is created via place-ment of a temporary polymethyl methacrylate spacer. The membrane appears to mature biochemically and physically 4 to 8 weeks after spacer placement.
Original Description:
Copyright
© © All Rights Reserved
Available Formats
PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentA two-stage technique uses induced biologic membranes with delayed placement of bone graft. Excellent clinical results have been reported with reconstruction of segmental bone defects >20 cm. A bioactive membrane is created via place-ment of a temporary polymethyl methacrylate spacer. The membrane appears to mature biochemically and physically 4 to 8 weeks after spacer placement.
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
126 views9 pagesMasquelet JAAOS
Uploaded by
Maurinho MnhA two-stage technique uses induced biologic membranes with delayed placement of bone graft. Excellent clinical results have been reported with reconstruction of segmental bone defects >20 cm. A bioactive membrane is created via place-ment of a temporary polymethyl methacrylate spacer. The membrane appears to mature biochemically and physically 4 to 8 weeks after spacer placement.
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
You are on page 1of 9
Induced Membrane Technique for
Reconstruction To Manage Bone
Loss
Abstract
Multiple surgeries are often required to manage segmental bone
loss because of the complex mechanics and biology involved in
reconstruction. These procedures can lead to prolonged recovery
times, poor patient outcomes, and even delayed amputation. A two-
stage technique uses induced biologic membranes with delayed
placement of bone graft to manage this clinical challenge. In the
rst stage, a polymethyl methacrylate spacer is placed in the defect
to produce a bioactive membrane, which appears to mature
biochemically and physically 4 to 8 weeks after spacer placement.
In the second, cancellous autograft is placed within this membrane
and, via elution of several growth factors, the membrane appears
to prevent graft resorption and promote revascularization and
consolidation of new bone. Excellent clinical results have been
reported, with successful reconstruction of segmental bone defects
>20 cm.
R
econstruction of large segmental
bone defects is often challeng-
ing. The goal is to achieve a func-
tional, stable extremity in an expe-
dient manner that will be well
tolerated. However, most techniques
for reconstruction of significant bone
loss are associated with lengthy heal-
ing or rehabilitation times and un-
predictable union rates, or they use
methods that are poorly tolerated.
Current management options include
intercalary bone transport and dis-
traction osteogenesis, vascularized
bone transfer, massive cancellous
autograft transfer, and synthetic
calcium-based fillers. These options
may be supplemented with the addi-
tion of demineralized bone matrix,
allograft, or bone morphogenetic
protein (BMP).
Recently, use of induced mem-
branes has shown potential as an al-
ternative reconstruction method for
large segmental bone defects. A bio-
active membrane is created via place-
ment of a temporary polymethyl
methacrylate (PMMA) spacer, and
the membrane is later filled with can-
cellous autograft.
History and Development
Traditionally, patients with signifi-
cant soft-tissue injury associated
with bone loss underwent amputa-
tion; however, limb salvage has be-
come increasingly common, with re-
ported clinical outcomes comparable
to those of amputation at short-term
follow-up.
1
As limb salvage efforts
increase, surgeons continue to strive
for successful management of large
segmental bone defects. Autogenous
bone graft remains the optimal graft
for management of these defects be-
Benjamin C. Taylor, MD
Bruce G. French, MD
T. Ty Fowler, MD
Jeremy Russell, DO
Attila Poka, MD
From the Department of
Orthopedics, Grant Medical Center
(Dr. Taylor, Dr. French, Dr. Russell,
and Dr. Poka) and the Department
of Orthopedic Surgery, Mount
Carmel Medical Center (Dr. Fowler),
Columbus, OH.
Dr. Taylor or an immediate family
member has received research or
institutional support from Synthes.
Dr. French or an immediate family
member serves as a paid consultant
to Biomet. Dr. Russell or an
immediate family member has stock
or stock options held in Orthovita.
Dr. Poka or an immediate family
member is a member of a speakers
bureau or has made paid
presentations on behalf of Stryker
and serves as a paid consultant to
Biomet. Neither Dr. Fowler nor any
immediate family member has
received anything of value from or
owns stock in a commercial
company or institution related
directly or indirectly to the subject of
this article.
J Am Acad Orthop Surg 2012;20:
142-150
http://dx.doi.org/10.5435/
JAAOS-20-03-142
Copyright 2012 by the American
Academy of Orthopaedic Surgeons.
Review Article
142 Journal of the American Academy of Orthopaedic Surgeons
cause of its osteoinductive, osteocon-
ductive, and osteogenic properties.
However, this graft has several draw-
backs and limitations, including a fi-
nite supply and risk of significant
morbidity or iatrogenic injury with
harvest.
2
In addition, outcomes asso-
ciated with massive cancellous au-
tograft of large segmental defects are
often poor due to substantial graft
resorption, even in noninfected, well-
vascularized surgical sites.
3,4
The concept of creating a mem-
brane to protect and enhance the lo-
cal environment was proposed in the
early 1960s; the initial materials
tested were nonabsorbable sub-
stances such as Teflon and polyure-
thane sponges.
5-7
Preventing graft re-
sorption while enhancing the local
biologic environment has been
achieved with porous resorbable
polymeric membranes, which not
only limit graft resorption but also
allow for increased bone healing
through neovascularization and ex-
clusion of nonosseous tissues.
7,8
Fur-
ther research on the use of these
membranes has been reported in the
periodontal and craniomaxillofacial
literature, along with techniques that
describe regeneration of periodontal
bone, a process called guided tissue
regeneration.
6
Masquelet and colleagues
9,10
devel-
oped the use of induced membrane-
assisted massive autograft for seg-
mental bony defects and successfully
managed defects 25 cm with associ-
ated severe soft-tissue injury by use
of this technique. Reported advan-
tages of this technique include pro-
tection against autograft resorption,
relative maintenance of graft posi-
tion, and prevention of soft-tissue in-
terposition.
11
This technique was dis-
covered largely by accident; the
induction of this membrane was an
unanticipated finding. Masquelet
and Begue
12
used cement spacers to
manage infected nonunions with
bone loss, and the resultant mem-
brane was initially maintained at the
time of final grafting only to limit
surgical devitalization and subse-
quent blood loss.
Basic Science Principles
The induced membrane is a unique
and potent tissue thought to be re-
sponsible for early clinical success in
managing large bone defects. The
role of the membrane in healing has
been examined in animal models, re-
sulting in improved understanding of
the structure and biologic properties
of this membrane. Histologic and
immunochemical analysis has re-
vealed that the membrane is made of
a type I collagen-heavy matrix, and
fibroblastic cells are the dominant
cell type.
11,13
The inner aspect of the
membrane is epithelial-like and com-
posed of fibroblasts, myofibroblasts,
and collagen bundles that run paral-
lel to the surface of the membrane.
12
This tissue is highly vascularized,
and the PMMA spacer causes a mild
foreign-body inflammatory response;
giant cells and macrophages were
discovered on histologic evaluation.
11
The limited inflammatory response
has been shown to decrease after the
second week following spacer im-
plantation and to disappear by 6
months following bone grafting.
14,15
The reaction produced by the
PMMA spacer is milder than that in-
duced by other membrane materials;
use of silicone spacers is often associ-
ated with intense T-cell and giant cell
reactions and formation of a vascu-
larized pseudosynovium.
11,16
The membrane contains a high
concentration of vascular endothelial
growth factor, an angiogenic factor
that has been shown to increase the
vascularity of the surrounding tis-
sue.
13
In addition, increased levels of
core-binding factor -1, a critical
transcription factor for osteoblastic
cell development, have been found in
the fibroblastic cells within the mem-
brane.
17
Further analysis of mem-
brane protein has revealed that in-
creased levels of transforming
growth factor-1 and BMP-2 are
present after implantation of the
PMMA spacer; BMP-2 production
peaks at 4 weeks postimplantation,
which suggests that an optimal time
for definitive bone grafting exists.
13
Biochemical analysis has shown that
membrane protein extract stimulates
bone marrow cell proliferation as
well as mesenchymal cell differentia-
tion to osteoblastic cell lineage.
13
Investigation of the biochemical
characteristics of the membrane con-
tinues; these characteristics have im-
plications for the development of the
induced membrane technique and
tissue engineering.
In various animal models, a fibrous
membrane was successfully formed
when a PMMA spacer was placed in
the area of the segmental bony defect
in a purely subcutaneous posi-
tion.
14,15
At 6 weeks postoperatively,
the spacer was removed, and the in-
duced membranes were noted to be 1
to 2 mm thick, well vascularized,
and nonadherent to the underlying
spacer. These membranes served to
eliminate soft-tissue interposition
into the defect and created a semi-
rigid cavity to accept bone graft. The
shape and size of the healed bone
graft is defined by the membrane. In
addition, the membrane was shown
to prevent ectopic bone formation by
maintaining the position of the
graft.
10
In models in which the spacer
was removed and was not replaced
with bone graft, limited bone forma-
tion on the internal aspect of the
membrane, but not within it, has
been reported.
12,13
This suggests that
the membrane may have inherent os-
teogenic properties; however, this
possibility has not been proved. The
membrane has been shown to main-
tain the volume of bone graft placed
in the defect, which may be the result
Benjamin C. Taylor, MD, et al
March 2012, Vol 20, No 3 143
of greater bone formation, decreased
bone resorption, and/or prevention
of soft-tissue ingrowth associated
with the use of induced mem-
branes.
11,12,14,15
Local depot delivery of antibiot-
ics via an antibiotic-impregnated
PMMA spacer can achieve antibiotic
concentration levels many times
greater than the bacterial minimum
inhibitory concentration, with negli-
gible increases in serum or plasma
levels and little systemic toxicity.
18
The selection of antibiotics that can
be used with a spacer is more limited
than that available for use via other
routes because antibiotics used with
a spacer must be thermostable to
withstand the often significant exo-
thermic reaction associated with
PMMA curing. In addition, the anti-
biotic must be hydrophilic to diffuse
into the surrounding tissues.
19
Com-
monly used antibiotics include genta-
micin, tobramycin, vancomycin, and
various cephalosporins.
18-24
Dosage for various scenarios has
not yet been fully described in the lit-
erature. However, improved clinical
outcome may be associated with the
use of two concurrent antibiotics
compared with use of a single antibi-
otic, an outcome attributed to syner-
gistic elution and antibacterial ac-
tions.
20,21
Exceeding a threshold of
8 g of antibiotics per 40 g of PMMA
is not recommended because the me-
chanical properties of the cement
may be altered such that it cannot be
formed and molded successfully.
23
Sustained local supratherapeutic
antibiotic levels can be achieved and
maintained with appropriate use of
antibiotic-impregnated cement.
25
The
contribution of antibiotics to mem-
brane formation remains largely un-
explored. Currently, it is not known
whether the presence of antibiotics
and the interaction of differing con-
centrations and chemical makeup
have an effect on membrane forma-
tion.
Surgical Technique
Reconstruction of large bone defects
using the two-stage induced mem-
brane technique is straightforward
but requires careful preoperative
planning and attention to detail to
achieve optimal results (Figure 1). In
the first stage of reconstruction, thor-
A, Preoperative AP radiograph of the forearm demonstrating signicant bone loss and fracture displacement secondary
to high-energy trauma in a 38-year-old man. Thorough irrigation and dbridement were performed followed by open
reduction and internal xation of the radius and ulna. B, Clinical photograph of the forearm demonstrating soft-tissue
coverage with a free ap and split-thickness skin graft. No signs of necrotic tissue or debris were noted at the time of
denitive soft-tissue coverage. C, Postoperative AP radiograph of the wrist demonstrating restoration of length and
alignment. The distal radioulnar joint was pinned to address instability. A large antibiotic-impregnated cement spacer
was placed into the metaphyseal defect of the distal radius. D, Postoperative AP radiograph of the wrist obtained 10
months after cement spacer removal and placement of iliac crest autograft in the induced membrane site. Full
consolidation is noted at the site of the metaphyseal defect. Revision plating was undertaken at the time of grafting
because loosened and broken screws were present in the distal articular fragment.
Figure 1
Induced Membrane Technique for Reconstruction To Manage Bone Loss
144 Journal of the American Academy of Orthopaedic Surgeons
ough and efficacious dbridement
must be performed to limit the risk
of subsequent infection by reducing
the number of microorganisms and
removing necrotic material. Ideally,
complete removal of all devitalized
bone and soft tissue is done at this
time. This material should not be re-
tained for reconstruction. The injury
is then stabilized. Various methods
of internal and external fixation can
be used in conjunction with the in-
duced membrane technique. The fix-
ation construct should be stable
enough to allow the soft tissues to
heal before the second stage of the
procedure. If possible, soft-tissue re-
pair or reconstruction should be per-
formed in a manner that will accom-
modate the secondary (ie, bone
grafting) procedure.
PMMA is mixed by hand and anti-
biotics added for local depot deliv-
ery. When a specific offending organ-
ism and its sensitivity are identified,
the appropriate antibiotic is chosen.
However, often the pathogen is un-
known or no visible infection is pres-
ent, and empiric treatment is used.
Cement should be placed into the de-
fect during later stages of polymer-
ization to allow proper sizing and
shaping of the spacer while limiting
interdigitation with cancellous bone.
The spacer should overlap the outer
cortical ends of the remaining bone
to ensure that the graft has sufficient
room to heal (Figure 2). If the condi-
tion of the soft tissue allows, the
spacer should be larger than the orig-
inal defect to permit placement of
enough bone graft for reconstruction
of the defect. The cement spacer can
be shaped into a simple block or
placed around abnormal anatomy or
a fixation device, such as an in-
tramedullary (IM) nail (Figure 3).
We recommend temporary removal
A, Intraoperative photograph
demonstrating signicant femoral bone
loss around an intramedullary (IM) nail
secondary to a high-energy gunshot
injury. B, Intraoperative photograph
demonstrating placement of a cement
spacer around the IM nail; the cortical
ends of the bone are enveloped by the
spacer to ensure that the induced
membrane is created in a similar
fashion. C, Postoperative AP radiograph
of the distal femur demonstrating
restoration of the anatomic axis of the
extremity with the IM nail and the
polymethyl methacrylate (PMMA)
spacer. The medial split-thickness skin
graft is outlined by staples. D, Postop-
erative lateral radiograph of the same
distal femur. Undisturbed comminuted
cortical fragments are visible posterior
to the PMMA spacer.
Figure 2
Benjamin C. Taylor, MD, et al
March 2012, Vol 20, No 3 145
of the cement spacer during the final
stages of polymerization, if possible,
because the exothermic reaction of
PMMA curing can be significant and
may lead to heat necrosis in the sur-
rounding bone and soft tissue. When
spacer removal is not possible, judi-
cious use of saline can limit any se-
quelae of heat necrosis. Definitive
soft-tissue coverage and spacer place-
ment should be performed during the
same surgical procedure.
The cement spacer should remain
in place for 4 to 8 weeks to allow the
membrane to fully develop biochemi-
cally and physically.
13,26
However, de-
layed soft-tissue healing or other pa-
tient variables can delay the second
stage of the procedure for several ad-
ditional weeks with no significant ev-
idence of membrane degrada-
tion.
9,10,12
The membrane is identified
and maintained, then incised care-
fully to remove the cement spacer.
The use of an osteotome and mallet
typically is required to remove the
PMMA in a piecemeal fashion (Fig-
ure 4).
If an IM nail is used for fixation, a
second membrane forms between the
cement spacer and the nail; this
membrane should also be maintained
to maximize healing and promote
corticalization of the graft. Native
cortical bone ends should then be ap-
propriately freshened with curets,
rongeurs, or osteotomes to improve
graft incorporation to native bone.
In addition, the IM canal should be
opened on either end of the defect to
improve local vascularity. However,
if an IM nail is in place, we do not
recommend nail removal or ex-
change because of the potential for
destabilization. Excellent results
have been reported with mainte-
nance of the original IM nail.
27
Cancellous autograft can be har-
vested from the anterior or posterior
iliac crest, but this is often associated
with significant risk of donor site
pain and morbidity.
2
We use
and recommend the Reamer-
Irrigator-Aspirator (RIA; Synthes,
Westchester, PA) for femoral bone
graft harvest because the biologic
content of this graft has been shown
to be equivalent or superior to that
of iliac crest graft, with volumes of
80 mL obtainable from each fe-
mur.
27,28
The biologic potential of
this IM graft has also been reported
in clinical studies; when used for re-
construction of segmental defects,
this graft has union rates equal to or
better than those associated with il-
iac crest graft as well as fewer re-
ported complications and less donor
site morbidity.
29-31
However, femoral
bone graft harvest is not without
morbidity; the harvest site should be
selected carefully on an case-by-case
basis.
Cancellous autograft can be used
with extenders (eg, cancellous al-
lograft, demineralized bone matrix)
if bone graft volume is insufficient.
Extender volume of 25% of the fi-
nal graft composition has been used
without increasing the rate of com-
plications or nonunion.
9,12
Use of
other osteoinductive materials has
not yet been thoroughly investigated;
BMP-7 is the only adjunct that has
been evaluated, and increased rates
of delayed deformity and bone graft
resorption have been reported with
its use.
12
Additional evidence-based
studies are needed before recommen-
dations can be made regarding use of
other osteoinductive materials.
The autograft is placed into the de-
fect, and the exposed ends of the na-
tive bone are enveloped with the
graft. Care must be taken to avoid
packing a large mass of graft too
tightly, especially when fixation
methods other than IM nailing are
used; a large mass of cancellous graft
packed to cortical density will not
fully revascularize or mature, leading
to poor graft consolidation.
27,31
The
membrane is then sutured over the
inlaid bone graft, creating a closed
environment (Figure 5).
Outcomes
In 2000, Masquelet et al
10
reported a
union rate of 100% in a series of 35
patients with upper and lower ex-
tremity segmental defects that mea-
sured 4 to 25 cm in length. The au-
thors found that the rate of bone
healing did not correlate with the
A, Postoperative AP radiograph
demonstrating placement of a
polymethyl methacrylate spacer
(arrows) around an intramedullary
nail to manage segmental bone
loss associated with an infraisthmal
fracture of the tibia in a 27-year-old
man. The spacer was maintained
for 10 weeks and was
subsequently replaced with
cancellous autograft. B, AP
radiograph in the same patient 24
months after hardware removal.
Complete consolidation and
corticalization of the graft are
noted.
Figure 3
Induced Membrane Technique for Reconstruction To Manage Bone Loss
146 Journal of the American Academy of Orthopaedic Surgeons
length of the defect in patients
treated with induced membranes and
external fixation. The mean time to
full weight bearing was 8.5 months.
Masquelet and Begue
12
followed this
initial study with a prospective anal-
ysis of 11 patients treated using the
same protocol but with the addition
of BMP-7. The authors reported a
91% rate of bony union in defects
that measured 5 to 18 cm. BMP-7
was added to hasten formation of
cortical bone, but local partial re-
sorption of the graft was noted in all
cases, which was an unexpected find-
ing. The authors concluded that the
full effect of adjunct BMP-7 could
not be determined, and its use could
not be recommended without addi-
tional research.
Other investigators have reported
similar results with variations of the
original technique. Stafford and Nor-
ris
27
described a series of 27 lower
extremity nonunions with segmental
bone loss treated with RIA-harvested
bone graft and either IM nailing or
plate-and-screw fixation constructs.
They reported a healing rate of 90%
at 1-year follow-up. McCall et al
31
reported on a series of 20 patients
with upper and lower extremity seg-
mental bone defects treated with the
induced membrane technique and
fixation with either IM nails or
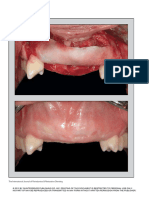
A, Intraoperative photograph of the proximal tibia demonstrating the mature induced membrane and cement spacer at
the time of spacer removal. The membrane is nonadherent to the underlying polymethyl methacrylate (PMMA) spacer.
The segmental defect was spanned with a lateral locking plate. B, Intraoperative photograph demonstrating removal of
the spacer in a piecemeal fashion while the induced membrane is carefully protected. The PMMA spacer often needs
to be removed in this manner to limit the risk of iatrogenic injury to the membrane or surrounding tissues. C, Intraop-
erative photograph demonstrating the large cavitary space created by removing the PMMA spacer. The membrane is 3
mm thick, slightly thicker than a typical induced membrane.
Figure 4
Intraoperative photograph of the proximal tibia. The mature membrane was
sutured to create a closed environment for graft consolidation. Plate xation
is shown on top of the membrane.
Figure 5
Benjamin C. Taylor, MD, et al
March 2012, Vol 20, No 3 147
plate-and-screw constructs. They
noted a bony union rate of 85% at
final follow-up; however, seven pa-
tients required additional surgery af-
ter the second stage (ie, spacer re-
moval and bone grafting) of the
procedure. Apard et al
32
reported a
bony union rate of 92% in 12 pa-
tients with segmental bone loss of
the tibia treated with induced mem-
branes and IM nailing. Full weight
bearing was permitted at 4 months
because IM nails were used instead
of external fixation, as described in
the original technique.
Injuries to the wrist and hand with
segmental bone loss caused by
trauma or infection have also been
managed with the induced mem-
brane technique. Flamans et al
33
re-
ported an 82% rate of bony union
with this technique and fixation with
pinning or plate-and-screw con-
structs. They concluded that the in-
duced membrane technique is useful
in the setting of severe bony and
soft-tissue injuries of the hand, po-
tentially avoiding acute shortening
and the need for microsurgery or
amputation. This technique has also
been used successfully for recon-
struction of devastating foot injuries,
with full weight bearing permitted by
9 months postoperatively.
34,35
Despite
encouraging early results, the level of
evidence for this technique remains
low because the current published re-
ports are either retrospective case se-
ries or small prospective noncompar-
ative studies.
Complications
Infection as a result of inadequate
dbridement or subsequent de novo
development remains the primary
complication associated with this
treatment method. Masquelet and
colleagues
9,10
emphasize the impor-
tance of methodical, thorough d-
bridement; they recommend using a
spacer without antibiotics and a
week-long regimen of oral antibiot-
ics to avoid masking inadequate d-
bridement. This treatment protocol
has the advantage of revealing infec-
tion early rather than after the sec-
ond stage of the procedure, thus
avoiding bone graft loss. Conversely,
use of antibiotic-impregnated cement
is well established in the orthopaedic
literature; this technique, in combi-
nation with adequate dbridement,
has the potential to decrease infec-
tion rates in the time between stages
of this procedure.
36
Reported rates of
septic complications leading to re-
construction failure range from zero
to 8%; most of these failures are at-
tributed to inadequate dbride-
ment.
9,12,27,31-33,35
Additional insight
into infection can be obtained at the
time of bone grafting; successful
maintenance of bone graft and treat-
ment of positive cultures with addi-
tional intravenous antibiotics have
been reported.
37
Delayed stress fracture is another
potential complication of the in-
duced membrane technique. Several
cases of delayed stress fracture have
been reported, occurring as late as 2
years after reconstruction.
9,32
This
phenomenon seems to occur before
complete corticalization of the bone,
which can take several years from
surgery to complete. An increased in-
cidence of delayed stress fractures
has been reported with use of exter-
nal fixation for definitive bony stabi-
lization compared with fixation with
IM nails or plate-and-screw con-
structs; however, head-to-head com-
parison of outcomes associated with
different fixation methods is lacking.
Future Directions
The concept of using induced mem-
branes to manage septic or aseptic
bone loss is fairly well established,
but further research is required.
Characterization of the biochemical
makeup of the membrane and the
optimal time frame for staging are
limited. Currently, analysis of only
transforming growth factor-1,
BMP-2, vascular endothelial growth
factor, and core-binding factor -1
has been performed. Further insight
into the osteoinductive factors in-
duced and the timing of their release
could potentially result in improve-
ments in outcomes by revealing a
need for supplementation with other
osteoinductive factors and by dictat-
ing optimal timing of the second
stage of the procedure. Timing of
bone graft placement remains a topic
of debate; initial biochemical analy-
sis of BMP-2 points to definitive
grafting at 4 weeks, but research on
the secretion patterns of other coex-
isting factors is lacking.
13
Much of
the clinical evidence regarding timing
of the second stage of the procedure
is highly variable; cement removal
and grafting have been performed 4
weeks to 19 months after cement im-
plantation without significant evi-
dence of membrane degradation.
12,32
Whether the induced membrane
has osteogenic qualities also remains
unknown. In animal models in which
bone graft was not placed in the de-
fect after cement spacer removal, de
novo bone formed in the periphery
of the cavity on the internal aspect of
the induced membrane, which sug-
gests that the membrane may contain
pluripotent mesenchymal cells.
38
Soft-tissue membranes that form
around joint prostheses produce
prostaglandins, which are known to
inhibit differentiation of osteoclast
precursors.
38
The effect of prosta-
glandin production has not yet been
investigated. However, it may play a
role in the ability of the membrane
to protect against significant resorp-
tion in the autograft bone.
Further investigation is needed to
determine whether PMMA is the
ideal spacer material. Data are lack-
Induced Membrane Technique for Reconstruction To Manage Bone Loss
148 Journal of the American Academy of Orthopaedic Surgeons
ing regarding the optimal chemical
makeup of the spacer, and it is possi-
ble that an alternative substance
could create a membrane that might
further improve clinical outcomes.
Masquelet and Begue
12
pointed out
that a smooth surface, such as that
produced by PMMA, leads to a
smooth membrane lining. A textured
spacer surface has the theoretic ad-
vantage of creating a membrane with
villous hyperplasia, leading to in-
creased internal surface area and po-
tentially increased vascularity as well
as improved growth factor secretion.
Analysis of bone grafts and bone
graft substitutes used in the induced
membrane model warrants further
investigation to determine which
graft will produce optimal clinical
and radiographic results. Cancellous
autograft harvested from the iliac
crest or from IM reamings is cur-
rently used, and bone substitute (eg,
demineralized bone matrix) is used
as an extender, if necessary. The
question remains whether osteoin-
ductivity and possible osteogenic
properties of the induced membrane
are enough to reconstitute the bony
defect with use of bone extenders
alone, or whether a certain ratio of
autograft is necessary for incorpora-
tion and healing. In one case report,
morcellized cancellous autograft was
augmented with a large cortical strut
autograft from the contralateral tibia
during the second stage of the in-
duced membrane procedure; rapid
incorporation of the strut was re-
ported, with full cortical reconstitu-
tion by 1 year postoperatively.
39
Use
of cortical struts with the induced
membrane technique has otherwise
not been examined. It remains to be
seen whether these grafts have the
potential to promote earlier healing
and improve early mechanical
strength.
Evaluation of the effect of different
stabilization techniques on perioper-
ative and long-term clinical out-
comes is also lacking. In the initial
description of the induced membrane
technique, external fixators were
used for limb stabilization, but other
authors have noted potential difficul-
ties with soft-tissue care as well as
pin tract complications.
31,32
In addi-
tion, stabilization of a large defect is
difficult with external fixation, and if
this method fails to maintain the axis
of the limb, both early and delayed
osteotomies may be required.
9,12
No
comparative studies exist on fixation
methods used with the induced mem-
brane model; successful results have
been reported with plate-and-screw
constructs, locked IM nailing, and
external fixators. Further research
could provide insight into optimal
construct flexibility and examine the
nuances of each fixation method.
When an IM nail is used, a second
internal membrane forms around the
exterior of the nail, potentially lead-
ing to an increase in local vascularity
and release of osteoinductive factors.
Masquelet and Begue
12
noted that
the second membrane reduces the
amount of space available for bony
reconstruction; however, the de-
crease in bone graft volume does not
seem to negatively affect clinical or
radiographic outcomes, and less
bone graft is needed for reconstruc-
tion.
Summary
Management of segmental bone de-
fects remains challenging and is often
fraught with complications and long
treatment periods. The induced
membrane technique for reconstruc-
tion of bone loss exhibits promising
early clinical and radiographic out-
comes; however, consensus and/or
evidence regarding many aspects of
the procedure are lacking. In studies
to date, the membrane appears to
eliminate local soft-tissue ingrowth
into the bone defect, prevent graft re-
sorption, and promote neovascular-
ization and corticalization of the
graft. In addition, the membrane
may have osteoinductive and weak
osteogenic capabilities. Early results
with this technique are encouraging.
This treatment method should be
considered for patients with signifi-
cant upper and/or lower extremity
bone loss.
References
Evidence-based Medicine: Levels of
evidence are described in the table of
contents. In this article, reference 1 is
a level I study. References 4 and 17 are
level II studies. References 2, 6, 12,
20, and 38 are level III studies.
References 3, 5, 7-11, 13-16, 23, 25-
28, and 30-36 are level IV studies.
References 29 and 39 are level V
expert opinion.
References printed in bold type are
those published within the past 5
years.
1. Bosse MJ, MacKenzie EJ, Kellam JF,
et al: An analysis of outcomes of
reconstruction or amputation after leg-
threatening injuries. N Engl J Med 2002;
347(24):1924-1931.
2. Ahlmann E, Patzakis M, Roidis N,
Shepherd L, Holtom P: Comparison of
anterior and posterior iliac crest bone
grafts in terms of harvest-site morbidity
and functional outcomes. J Bone Joint
Surg Am 2002;84(5):716-720.
3. Hertel R, Gerber A, Schlegel U, Cordey
J, Regsegger P, Rahn BA: Cancellous
bone graft for skeletal reconstruction:
Muscular versus periosteal bed.
Preliminary report. Injury 1994;25(suppl
1):A59-A70.
4. Weiland AJ, Phillips TW, Randolph MA:
Bone grafts: A radiologic, histologic, and
biomechanical model comparing
autografts, allografts, and free
vascularized bone grafts. Plast Reconstr
Surg 1984;74(3):368-379.
5. Gilmer WS Jr, Tooms RE, Salvatore JE:
An experimental study of the influence
of implanted polyurethane sponges upon
subsequent bone formation. Surg
Gynecol Obstet 1961;113:143-148.
6. Eickholz P, Pretzl B, Holle R, Kim TS:
Long-term results of guided tissue
regeneration therapy with non-
Benjamin C. Taylor, MD, et al
March 2012, Vol 20, No 3 149
resorbable and bioabsorbable barriers:
III. Class II furcations after 10 years.
J Periodontol 2006;77(1):88-94.
7. Meinig RP, Rahn B, Perren SM,
Gogolewski S: Bone regeneration with
resorbable polymeric membranes:
Treatment of diaphyseal bone defects in
the rabbit radius with poly(L-lactide)
membrane. A pilot study. J Orthop
Trauma 1996;10(3):178-190.
8. Gerber A, Gogolewski S: Reconstruction
of large segmental defects in the sheep
tibia using polylactide membranes: A
clinical and radiographic report. Injury
2002;33(suppl 2):B43-B57.
9. Masquelet AC: Muscle reconstruction in
reconstructive surgery: Soft tissue repair
and long bone reconstruction.
Langenbecks Arch Surg 2003;388(5):
344-346.
10. Masquelet AC, Fitoussi F, Begue T,
Muller GP: Reconstruction of the long
bones by the induced membrane and
spongy autograft [French]. Ann Chir
Plast Esthet 2000;45(3):346-353.
11. Viateau V, Bensidhoum M, Guillemin G,
et al: Use of the induced membrane
technique for bone tissue engineering
purposes: Animal studies. Orthop Clin
North Am 2010;41(1):49-56.
12. Masquelet AC, Begue T: The concept of
induced membrane for reconstruction of
long bone defects. Orthop Clin North
Am 2010;41(1):27-37.
13. Pelissier P, Masquelet AC, Bareille R,
Pelissier SM, Amedee J: Induced
membranes secrete growth factors
including vascular and osteoinductive
factors and could stimulate bone
regeneration. J Orthop Res 2004;22(1):
73-79.
14. Viateau V, Guillemin G, Bousson V,
et al: Long-bone critical-size defects
treated with tissue-engineered grafts: A
study on sheep. J Orthop Res 2007;
25(6):741-749.
15. Viateau V, Guillemin G, Calando Y,
et al: Induction of a barrier membrane to
facilitate reconstruction of massive
segmental diaphyseal bone defects: An
ovine model. Vet Surg 2006;35(5):445-
452.
16. Freund R, Wolff TW, Freund B: Silicone
block interposition for traumatic bone
loss. Orthopedics 2000;23(8):795, 799,
802, 804.
17. Viateau V, Guillemin G, Yang YC, et al:
A technique for creating critical-size
defects in the metatarsus of sheep for use
in investigation of healing of long-bone
defects. Am J Vet Res 2004;65(12):1653-
1657.
18. Cui Q, Mihalko WM, Shields JS, Ries
M, Saleh KJ: Antibiotic-impregnated
cement spacers for the treatment of
infection associated with total hip or
knee arthroplasty. J Bone Joint Surg Am
2007;89(4):871-882.
19. Joseph TN, Chen AL, Di Cesare PE: Use
of antibiotic-impregnated cement in total
joint arthroplasty. J Am Acad Orthop
Surg 2003;11(1):38-47.
20. Anagnostakos K, Kelm J, Regitz T,
Schmitt E, Jung W: In vitro evaluation of
antibiotic release from and bacteria
growth inhibition by antibiotic-loaded
acrylic bone cement spacers. J Biomed
Mater Res B Appl Biomater 2005;72(2):
373-378.
21. Hanssen AD, Spangehl MJ: Practical
applications of antibiotic-loaded bone
cement for treatment of infected joint
replacements. Clin Orthop Relat Res
2004;(427):79-85.
22. Jaeblon T: Polymethylmethacrylate:
Properties and contemporary uses in
orthopaedics. J Am Acad Orthop Surg
2010;18(5):297-305.
23. Hsieh PH, Chen LH, Chen CH, Lee MS,
Yang WE, Shih CH: Two-stage revision
hip arthroplasty for infection with a
custom-made, antibiotic-loaded, cement
prosthesis as an interim spacer. J Trauma
2004;56(6):1247-1252.
24. Kuehn KD, Ege W, Gopp U: Acrylic
bone cements: Mechanical and physical
properties. Orthop Clin North Am 2005;
36(1):29-39, v-vi.
25. Masri BA, Duncan CP, Beauchamp CP:
Long-term elution of antibiotics from
bone-cement: An in vivo study using the
prosthesis of antibiotic-loaded acrylic
cement (PROSTALAC) system.
J Arthroplasty 1998;13(3):331-338.
26. Klaue K, Knothe U, Anton C, Masquelet
AC, Perren S: Biological implementation
of autologous foreign body membranes
in consolidation of massive cancellous
bone grafts. J Bone Joint Surg Am 1997;
79(suppl II):236.
27. Stafford PR, Norris BL: Reamer-
irrigator-aspirator bone graft and bi
Masquelet technique for segmental bone
defect nonunions: A review of 25 cases.
Injury 2010;41(suppl 2):S72-S77.
28. Schmidmaier G, Herrmann S, Green J,
et al: Quantitative assessment of growth
factors in reaming aspirate, iliac crest,
and platelet preparation. Bone 2006;
39(5):1156-1163.
29. Pape HC, Tarkin IS: Reamer irrigator
aspirator: A new technique for bone
graft harvesting from the intramedullary
canal. Oper Tech Orthop 2008;19:108-
113.
30. Lowe JA, Della Rocca GJ, Murtha Y,
et al: Complications associated with
negative pressure reaming for harvesting
autologous bone graft: A case series.
J Orthop Trauma 2010;24(1):46-52.
31. McCall TA, Brokaw DS, Jelen BA, et al:
Treatment of large segmental bone
defects with reamer-irrigator-aspirator
bone graft: Technique and case series.
Orthop Clin North Am 2010;41(1):63-
73.
32. Apard T, Bigorre N, Cronier P, Duteille
F, Bizot P, Massin P: Two-stage
reconstruction of post-traumatic
segmental tibia bone loss with nailing.
Orthop Traumatol Surg Res 2010;96(5):
549-553.
33. Flamans B, Pauchot J, Petite H, et al:
Use of the induced membrane technique
for the treatment of bone defects in the
hand or wrist, in emergency [French].
Chir Main 2010;29(5):307-314.
34. Huffman LK, Harris JG, Suk M: Using
the bi-masquelet technique and reamer-
irrigator-aspirator for post-traumatic
foot reconstruction. Foot Ankle Int
2009;30(9):895-899.
35. Pelissier P, Bollecker V, Martin D,
Baudet J: Foot reconstruction with the
bi-Masquelet procedure [French]. Ann
Chir Plast Esthet 2002;47(4):304-307.
36. Sancineto CF, Barla JD: Treatment of
long bone osteomyelitis with a
mechanically stable intramedullar
antibiotic dispenser: Nineteen
consecutive cases with a minimum of 12
months follow-up. J Trauma 2008;65(6):
1416-1420.
37. Forsberg JA, Potter BK, Cierny G III,
Webb L: Diagnosis and management of
chronic infection. J Am Acad Orthop
Surg 2011;19(suppl 1):S8-S19.
38. Klaue K, Knothe U, Anton C, et al: Bone
regeneration in long-bone defects: Tissue
compartmentalisation? In vivo study on
bone defects in sheep. Injury 2009;
40(suppl 4):S95-S102.
39. Biau DJ, Pannier S, Masquelet AC,
Glorion C: Case report: Reconstruction
of a 16-cm diaphyseal defect after
Ewings resection in a child. Clin Orthop
Relat Res 2009;467(2):572-577.
Induced Membrane Technique for Reconstruction To Manage Bone Loss
150 Journal of the American Academy of Orthopaedic Surgeons
You might also like
- Regeneration of Periodontal Tissues Using Guided Tissue RegenerationDocument20 pagesRegeneration of Periodontal Tissues Using Guided Tissue RegenerationPiyusha SharmaNo ratings yet
- SCAFFOLDS COMBINED WITH STEM CELLS AND GROWTH FACTORS IN RECONSTRUCTION OF LARGE BONE DEFECTS. Rodolfo Capanna, Pietro de BiaseDocument7 pagesSCAFFOLDS COMBINED WITH STEM CELLS AND GROWTH FACTORS IN RECONSTRUCTION OF LARGE BONE DEFECTS. Rodolfo Capanna, Pietro de BiaseNuno Craveiro LopesNo ratings yet
- Review Article: Guided Bone Regeneration: A Literature ReviewDocument16 pagesReview Article: Guided Bone Regeneration: A Literature ReviewMazenShbeebNo ratings yet
- Continuing Education 1: Horizontal Alveolar Ridge Augmentation: The Importance of Space MaintenanceDocument11 pagesContinuing Education 1: Horizontal Alveolar Ridge Augmentation: The Importance of Space MaintenanceJuan Jose Sosa BerganzaNo ratings yet
- Masquelet InjuryDocument8 pagesMasquelet Injurydrets70No ratings yet
- Review Article: Guided Bone Regeneration: A Literature ReviewDocument16 pagesReview Article: Guided Bone Regeneration: A Literature ReviewGonçalo Gomes SanchesNo ratings yet
- Implant Platforn SwitchingDocument6 pagesImplant Platforn SwitchingJeary VargasNo ratings yet
- Study Material Unit 3 ScaffoldDocument4 pagesStudy Material Unit 3 ScaffoldSanjna VinodNo ratings yet
- Uided Tissue RegenerationDocument22 pagesUided Tissue RegenerationFarheen FatimaNo ratings yet
- Role of Tissue Engineering in Oral and Maxillofacial Reconstruction: Findings of The 2005 AAOMS Research SummitDocument8 pagesRole of Tissue Engineering in Oral and Maxillofacial Reconstruction: Findings of The 2005 AAOMS Research SummitRam MohanNo ratings yet
- Case Study 5Document4 pagesCase Study 5Troyee DebnathNo ratings yet
- GTR RevisitedDocument3 pagesGTR Revisitedjatt_mu_phattNo ratings yet
- Bone and Connective TissueDocument20 pagesBone and Connective TissueKarka PalmaNo ratings yet
- Techniques On Vertical Ridge Augmentation IndicatiDocument30 pagesTechniques On Vertical Ridge Augmentation IndicatiFelix SchweppeNo ratings yet
- 2011 Ghanaati Et Al Mucograft GerDocument13 pages2011 Ghanaati Et Al Mucograft GerDaniel E XêniaNo ratings yet
- Bonegraftingforimplant Surgery: Ladi Doonquah,, Pierre-John Holmes,, Laxman Kumar Ranganathan,, Hughette RobertsonDocument19 pagesBonegraftingforimplant Surgery: Ladi Doonquah,, Pierre-John Holmes,, Laxman Kumar Ranganathan,, Hughette RobertsonJason LeeNo ratings yet
- Cheng2006 PDFDocument4 pagesCheng2006 PDFPremshith CpNo ratings yet
- In Vitro Investigation of Gelatin/Polycaprolactone Nano Bers in Modulating Human Gingival Mesenchymal Stromal CellsDocument15 pagesIn Vitro Investigation of Gelatin/Polycaprolactone Nano Bers in Modulating Human Gingival Mesenchymal Stromal CellsZhongqi ZhaoNo ratings yet
- DownloadDocument10 pagesDownloadhasan nazzalNo ratings yet
- Bone Graft AssingmentDocument4 pagesBone Graft AssingmentNyein Chan AungNo ratings yet
- Review Article: Ridge Preservation Procedures After Tooth Extractions: A Systematic ReviewDocument8 pagesReview Article: Ridge Preservation Procedures After Tooth Extractions: A Systematic ReviewIka KusumawatiNo ratings yet
- 6789.9!-:/.! . !?2@80ab!c! .@8.D!Document13 pages6789.9!-:/.! . !?2@80ab!c! .@8.D!Gonçalo Gomes SanchesNo ratings yet
- Bone Regeneration in Implant Dentistry Which Are TDocument30 pagesBone Regeneration in Implant Dentistry Which Are TLEONARDO ALBERTO CRESPIN ZEPEDANo ratings yet
- Extracellular Matrix Scaffolds For Cartilage and Bone RegenerationDocument8 pagesExtracellular Matrix Scaffolds For Cartilage and Bone Regenerationduverney.gaviriaNo ratings yet
- Pi Is 1010518211000424Document6 pagesPi Is 1010518211000424Muthia FadhilaNo ratings yet
- Murray2012 ScaffoldDocument12 pagesMurray2012 ScaffoldShaliniNo ratings yet
- 1 Position Paper RegeneracionDocument22 pages1 Position Paper RegeneracionKatia AguilarNo ratings yet
- Ajtr0009 3200Document13 pagesAjtr0009 3200iam_ca2No ratings yet
- Membranes For Periodontal RegenerationDocument6 pagesMembranes For Periodontal RegenerationinventionjournalsNo ratings yet
- Polymers 03 00509 v2Document18 pagesPolymers 03 00509 v2Branko BabicNo ratings yet
- Bone Regenerative Issues Related To Bone Grafting BiomaterialsDocument9 pagesBone Regenerative Issues Related To Bone Grafting BiomaterialsOsorioGilNo ratings yet
- Journal Pre-Proof: Acta BiomaterialiaDocument45 pagesJournal Pre-Proof: Acta BiomaterialiaIndah GitaswariNo ratings yet
- Bone RegenerationDocument20 pagesBone RegenerationLigia DumaNo ratings yet
- 5 Skeletal RepairDocument123 pages5 Skeletal RepairE LNo ratings yet
- Respuesta Gingival A Las Fuerzas OrtodonticasDocument7 pagesRespuesta Gingival A Las Fuerzas OrtodonticasYeison Aguirre AponteNo ratings yet
- Wallace, Maxillary Sinus AugmentationDocument16 pagesWallace, Maxillary Sinus AugmentationChin-lungHsiehNo ratings yet
- Materials 13 00201 PDFDocument20 pagesMaterials 13 00201 PDFfiraNo ratings yet
- Guided Tissue RegenerationDocument7 pagesGuided Tissue RegenerationElenaLazarNo ratings yet
- Strietzel Et Al-2006-Journal of Biomedical Materials Research Part B - Applied BiomaterialsDocument12 pagesStrietzel Et Al-2006-Journal of Biomedical Materials Research Part B - Applied BiomaterialsDiego SiqueiraNo ratings yet
- Guided Bone Regeneration of An Atrophic Mandible With A Heterologous Bone BlockDocument6 pagesGuided Bone Regeneration of An Atrophic Mandible With A Heterologous Bone BlockGabriela Marie CruzNo ratings yet
- Techniques in Skeletal Reconstruction After Bone Resection For OsteomyelitisDocument9 pagesTechniques in Skeletal Reconstruction After Bone Resection For Osteomyelitisfabian hernandez medinaNo ratings yet
- Mandibular Reconstruction With Tissue EngineeringDocument5 pagesMandibular Reconstruction With Tissue EngineeringtamisatnamNo ratings yet
- Palatal Healing Stages After Connective Tissue GraftingDocument7 pagesPalatal Healing Stages After Connective Tissue GraftingpyrockerNo ratings yet
- Chapter VIDocument17 pagesChapter VIsteigmannNo ratings yet
- How Long Should You Wait to Reharvest Palatal TissueDocument7 pagesHow Long Should You Wait to Reharvest Palatal Tissueemi_alaNo ratings yet
- Evaluation of Healing Rates and Safety With A Bioinductive Collagen Patch For Large and Massive Rotator Cuff TearsDocument8 pagesEvaluation of Healing Rates and Safety With A Bioinductive Collagen Patch For Large and Massive Rotator Cuff TearsGuiss TlacotiaNo ratings yet
- Ep - 2019 - McGuireDocument10 pagesEp - 2019 - McGuireSamara CardenasNo ratings yet
- Tissue-Engineered Bone RegenerationDocument5 pagesTissue-Engineered Bone RegenerationElsa GonçalvesNo ratings yet
- Techniques On Vertical Ridge Augmentation: Indications and EffectivenessDocument30 pagesTechniques On Vertical Ridge Augmentation: Indications and Effectivenessrmartins76No ratings yet
- Periosteal Pocket Flap For Horizontal Bone RegenerDocument10 pagesPeriosteal Pocket Flap For Horizontal Bone RegenerViorel Ion100% (1)
- Principles of Reconstructive Surgery of Defects of The Jaws PARTDocument15 pagesPrinciples of Reconstructive Surgery of Defects of The Jaws PARTMohammedNo ratings yet
- Guided Bone Regeneration in The Oral Cavity: A Review: Rita A. Hitti and David G. KernsDocument13 pagesGuided Bone Regeneration in The Oral Cavity: A Review: Rita A. Hitti and David G. KernsAndi Muhammad FahruddinNo ratings yet
- Scaffold For Bone Tissue RegenerationDocument13 pagesScaffold For Bone Tissue RegenerationOluwasegun ModupeNo ratings yet
- Implant Reconstruction of The Bone-Grafted Maxilla: Review of The Literature and Presentation of 8 CasesDocument9 pagesImplant Reconstruction of The Bone-Grafted Maxilla: Review of The Literature and Presentation of 8 CasesRohan BhagatNo ratings yet
- Simion 2012)Document13 pagesSimion 2012)SergioNo ratings yet
- Biological Prosthetics For Hernia Repair: EditorialDocument2 pagesBiological Prosthetics For Hernia Repair: EditorialtexveerNo ratings yet
- Gholobova Et Al. - Biofabrication - 2020 - Functional Evaluation of Prevascularization in One-Stage Versus Two-Stage Tissue EngineeriDocument19 pagesGholobova Et Al. - Biofabrication - 2020 - Functional Evaluation of Prevascularization in One-Stage Versus Two-Stage Tissue EngineeriLievenNo ratings yet
- Biomaterials 1Document17 pagesBiomaterials 1Rovian RosaliaNo ratings yet
- Manuscript ARMDocument11 pagesManuscript ARMMahardika PutraNo ratings yet
- Bone Remodeling Process: Mechanics, Biology, and Numerical ModelingFrom EverandBone Remodeling Process: Mechanics, Biology, and Numerical ModelingNo ratings yet
- GTS Surgical TechniqueDocument22 pagesGTS Surgical TechniqueMaurinho MnhNo ratings yet
- Anterior Cruciate Ligament: An Anatomical Exploration in Humans and in A Selection of Animal SpeciesDocument11 pagesAnterior Cruciate Ligament: An Anatomical Exploration in Humans and in A Selection of Animal SpeciesMaurinho MnhNo ratings yet
- Art:10.1007/s00167 013 2458 3Document8 pagesArt:10.1007/s00167 013 2458 3Maurinho MnhNo ratings yet
- Mallet FingerDocument9 pagesMallet FingerMaurinho MnhNo ratings yet
- Art:10.1007/s00167 013 2449 4Document7 pagesArt:10.1007/s00167 013 2449 4Maurinho MnhNo ratings yet
- When The Koel SingsDocument15 pagesWhen The Koel SingsAlfie Paduga BeguinaNo ratings yet
- Microbial Healing of Cracks in ConcreteDocument15 pagesMicrobial Healing of Cracks in ConcreteasdasdasdasNo ratings yet
- 2nd Periodic Test (Science)Document1 page2nd Periodic Test (Science)mosarbas0950% (2)
- Characterization of Polydimethylsiloxane (PDMS) PropertiesDocument13 pagesCharacterization of Polydimethylsiloxane (PDMS) PropertiesEsteban ArayaNo ratings yet
- Presented By:-Dr. Sushma Tomar Associate Professor Department of AnatomyDocument20 pagesPresented By:-Dr. Sushma Tomar Associate Professor Department of AnatomyCristine EchaveNo ratings yet
- Zoologija VrsteDocument16 pagesZoologija VrsteДушан МарковићNo ratings yet
- LWT - Food Science and TechnologyDocument8 pagesLWT - Food Science and TechnologyAzb 711No ratings yet
- Original RT-PCR ReportDocument1 pageOriginal RT-PCR ReportVishva IyerNo ratings yet
- Adolescent Reproductive and Sexual HealthDocument42 pagesAdolescent Reproductive and Sexual HealthMuhammad Abbas WaliNo ratings yet
- Advanced Level Biology 2015 Marking SchemeDocument29 pagesAdvanced Level Biology 2015 Marking SchemeAngiee FNo ratings yet
- Protein Structure and Function Book ReviewDocument1 pageProtein Structure and Function Book ReviewBrunoNo ratings yet
- Full Essay Academic SkillsDocument3 pagesFull Essay Academic SkillsNurl AinaNo ratings yet
- Reproductive Biology and Phylogeny of Birds PDFDocument624 pagesReproductive Biology and Phylogeny of Birds PDFFabricio GZNo ratings yet
- COT TRF Science G8 - Food ChainDocument8 pagesCOT TRF Science G8 - Food ChainRAMIR BECOYNo ratings yet
- MR Spectroscopy: Technical Aspects and Clinical ApplicationsDocument5 pagesMR Spectroscopy: Technical Aspects and Clinical ApplicationsNotariana Kusuma ANo ratings yet
- Ewh Ix PDFDocument80 pagesEwh Ix PDFOR Premium FreeNo ratings yet
- 1 s2.0 S0141022999001556 MainDocument21 pages1 s2.0 S0141022999001556 MainRenata ScoralickNo ratings yet
- Lab Exercise 0ne: Carbohydrate Analysis Lab A.1 (Page 28)Document31 pagesLab Exercise 0ne: Carbohydrate Analysis Lab A.1 (Page 28)Goh Kae HorngNo ratings yet
- Chapter 5Document14 pagesChapter 5Caitlin G.No ratings yet
- Eagles and Eaglets gr2Document2 pagesEagles and Eaglets gr2vovanmtcNo ratings yet
- JCM 08 00217 v3Document23 pagesJCM 08 00217 v3Sumit BediNo ratings yet
- Organizing A TextDocument3 pagesOrganizing A TextMercedes Jimenez RomanNo ratings yet
- Botany AssignmentDocument35 pagesBotany AssignmentLakshmiNo ratings yet
- Cell Membrane: A Selective BarrierDocument23 pagesCell Membrane: A Selective BarrierHama JamalNo ratings yet
- Cell Division GizmoDocument3 pagesCell Division Gizmoapi-522847737No ratings yet
- Transport Phenomena in Nervous System PDFDocument538 pagesTransport Phenomena in Nervous System PDFUdayanidhi RNo ratings yet
- E-Portfolio Injection Study GuideDocument7 pagesE-Portfolio Injection Study Guideapi-366034042No ratings yet
- Management of PPHDocument1 pageManagement of PPH098 U.KARTHIK SARAVANA KANTHNo ratings yet
- MDU Open Elective 3rd Sem Date Sheet May 2019Document1 pageMDU Open Elective 3rd Sem Date Sheet May 2019Ratan DeshNo ratings yet
- Ssac 2104Document100 pagesSsac 2104Amrutha amrNo ratings yet