Professional Documents
Culture Documents
5
Uploaded by
Ni Wayan Ana Ps0 ratings0% found this document useful (0 votes)
10 views4 pagesPRES dan eklampsia
Copyright
© © All Rights Reserved
Available Formats
PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentPRES dan eklampsia
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
10 views4 pages5
Uploaded by
Ni Wayan Ana PsPRES dan eklampsia
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
You are on page 1of 4
OBSTETRICS
Posterior reversible encephalopathy syndrome (PRES) in pregnancy:
A diagnostic challenge to obstetricians
U. KRISHNAMOORTHY
1
, P. K. SARKAR
1
, Y. NAKHUDA
2
& P. D. MULLINS
3
Departments of
1
Obstetrics and Gynaecology,
2
Radiology and
3
Medicine, Acute Unit, Burnley General Hospital,
East Lancashire Hospitals NHS Trust, UK
Summary
Post-partum clinical presentation with seizures and focal neurological decit has a wide differential diagnosis. Two cases of
the rare condition Posterior Reversible Encephalopathy Syndrome (PRES) associated with pregnancy are presented with
complete recovery following multidisciplinary care. One of the cases was associated with Factor VII deciency in pregnancy
and the other with twin gestation and psoas abcess.
Keywords
Posterior reversible encephalopathy syndrome, PRES, eclampsia, factor VII deciency, psoas abcess
Case report 1
A 22-year-old primigravida with singleton gestation and
uneventful antenatal period presented with spontaneous
labour at 39 weeks gestation. Emergency caesarean
section was performed under epidural anaesthesia for
secondary arrest. A baby boy weighing 3,780 g was
delivered in good condition. She had an uneventful
recovery and went home on the third postoperative day.
Blood pressure (BP) was normal throughout this period.
Five days later, she was readmitted with headache,
epigastric pain, vomiting and BP of 171/97 mmHg.
Neurological assessment found her to be unresponsive
revealing a Glasgow coma score of 6/15. Intravenous
labetalol at a dose of 50 mg was administered for BP
control. Prolonged grand mal seizure lasting approxi-
mately 4 min occurred after admission. Diagnosis of
eclampsia was made and airway secured by endotracheal
intubation after rapid sequence induction. Intravenous
magnesium sulphate as 4 g bolus followed by main-
tenance infusion of 4 g/h was started.
Non-enhanced cranial computerised tomogram (CT)
was normal. After 36 h of stability, the decision was made
to extubate. Following extubation, BP abruptly increased
to 187/115 mmHg and she sustained an episode of grand
mal seizure lasting 2 min necessitating further 4 g bolus
magnesium sulphate and maintenance infusion was con-
tinued. Within an hour she sustained four further episodes
of grand mal convulsions 510 min apart. Repeat bolus of
4 g magnesium sulphate was administered besides 100 mg
labetalol. Although repeat intubation was not required,
magnesium sulphate infusion was continued for a further
48 h.
Neurological assessment revealed weakness of the right
lower limb and repeat cranial CT was normal. In view of
recurrent convulsive episodes despite magnesium sulphate,
differential diagnoses were considered. Phaeochromocyto-
ma was ruled out by normal levels of urinary metanephrine
and normetanephrine. Normal results of a lumbar punc-
ture that was performed following correction of coagulo-
pathy with transfusion of fresh frozen plasma helped
exclude iatrogenic meningitis secondary to epidural anaes-
thesia. Clear cerebrospinal uid under no tension ruled out
subarachnoid haemorrhage.
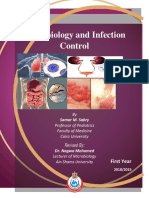
At this point, magnetic resonance imaging (MRI) of the
brain was performed (Figure 1). Axial T2 (Fig. 1a) and
uid attenuated inversion recovery MR (FLAIR) (Fig. 1b)
sequence demonstrated subcortical white matter hyperin-
tensity lesions in occipital and parietal lobes in keeping with
focal oedema. Diffusion-weighted imaging (DWI) axial
image (Fig. 1c) demonstrated isointensity, whereas corre-
sponding apparent diffusion coefcient (ADC) map image
(Fig. 1d) revealed hyperintensity (Fig. 1d) in the region of
interest, conrming diagnosis of posterior reversible
encephalopathy syndrome (PRES).
Anticoagulation with therapeutic doses of heparin was
recommended by physicians, but this was deferred as
coagulation studies showed prolonged international nor-
malised ratio (INR) of 1.8 and prothrombin time (PT) of
23. Mechanical thromboprophylaxis only was therefore
provided. There was no neurological decit when she was
allowed home 12 days later and she was maintained on oral
This article is not subject to United States copyright laws.
Correspondence: U. Krishnamoorthy, 7 Hawthorn Road, Bamford, Rochdale, Lancashire OL11 5JG, UK. E-mail: ukrishnamoorthy@hotmail.com
Journal of Obstetrics and Gynaecology, April 2009; 29(3): 192194
ISSN 0144-3615 print/ISSN 1364-6893 online
DOI: 10.1080/01443610802716026
labetalol at a dose of 200 mg twice daily. Further
coagulation prole and thrombophilia screen performed
in view of deranged coagulation prole revealed reduced
factor VII levels that stayed consistently low when repeated
after 3 months, conrming deciency of factor VII. She
remained well at 6 months follow-up, when all drug
therapy was eventually withdrawn.
Case report 2
A 35-year-old woman with no signicant background
medical history was booked for antenatal care in her third
pregnancy. The rst pregnancy was a spontaneous rst
trimester miscarriage and the second was an uneventful
term vaginal delivery. Booking and serial ultrasound scans
conrmed a dichorionic, diamniotic twin pregnancy with
progressive growth along the 50th percentile. At 34 weeks
gestation, pre-term labour with spontaneous rupture of
membranes proceeded to normal vaginal delivery of live
twins in good condition. She had epidural analgesia and
her BP throughout was normal. She was discharged home,
after an uneventful recovery, on the third day.
Ten days later she was re-admitted with complaints of
right iliac fossa pain, epigastric pain, headache, vomiting
and diplopia followed by grand mal seizures at presenta-
tion. Eclampsia was diagnosed as BP was elevated at 160/
90 mmHg. Intravenous magnesium sulphate was started as
bolus followed by maintenance infusion and intravenous
labetalol as in Case report 1. Three further episodes of
recurrent seizures necessitated a further bolus of magne-
sium sulphate. Neurological assessment revealed disorien-
tation, bilateral lower limb weakness and exaggerated
reexes. She was pyrexial with temperature of 38.58C,
3 g of proteinuria was noted and blood tests revealed
leucocytosis and elevated C-reactive protein levels.
Cranial CT and lumbar puncture were reported normal.
MRI of the brain (Figure 2) showed bilateral symmetrical
vasogenic oedema with predominant involvement of sub-
cortical white matter in the posterior parietal and occipital
lobes. MR venography ruled out suspicion of venous sinus
thrombosis. DWI MRI, to exclude ischaemia as the cause of
oedema, showed no infarction, and a diagnosis of posterior
reversible encephalopathy syndrome (PRES) was made.
Gradual improvement was noted on labetalol, magnesium
sulphate and therapeutic doses of heparin. Incidentally, an
abdominal CT scan performed due to persistent right iliac
fossa pain revealed a small right-sided psoas abscess
(4 63 cm) which resolved with intravenous antibiotics.
Within 2 weeks, there was complete resolution of clinical
and radiological features and oral labetalol only at a dose of
200 mg twice daily was continued. She was well at 6 months
review and the labetalol was stopped.
Discussion
PRES was rst described in 1996 as a usually reversible
neurological syndrome with a variety of presenting
symptoms ranging from headache, altered mental status,
seizures and vision loss, to loss of consciousness (Hinchey
et al. 1996). The term describes a potentially reversible
imaging appearance and symptomatology that is shared by
a diverse array of associated conditions (McKinney et al.
2007) (Table I).
Figure 1. Axial MRI images of the brain. Axial T2 (a) and FLAIR
(b) images demonstrate bilateral symmetrical high signal intensity
area with predominant involvement of subcortical white matter in
the right parieto-occipital region (arrowed). Diffusion weighted
(DWI) MRI axial image (c) demonstrates signal iso-intensity in the
same area. Apparent diffusion coefcient (ADC) image (d)
demonstrates increased signal intensity due to increased water
mobility signifying vasogenic oedema.
Figure 2. (a) Axial T2 and (b) axial FLAIR (uid-attenuated inversion recovery) T2 MRI images demonstrating bilateral symmetrical high
signal intensity areas (arrows), with predominant involvement of sub-cortical white matter in the posterior parietal and occipital lobes.
PRES in pregnancy 193
Classical MRI brain appearance in PRES is as follows:
reversible parieto-occipital white matter oedema on FLAIR
MR; areas of abnormal T2 signal; normal DWI and
increased ADC values (McKinney et al. 2007; Finocchi
et al. 2005). Reversible, vasogenic oedema of PRES has
different appearances compared with those of irreversible,
cytotoxic oedema present in brain infarction (Fujiwara
et al. 2005). Hypothesis suggests that endothelial dysfunc-
tion and a state of hyperperfusion leads to breakdown in the
blood-brain barrier and extravasation of uid resulting in
cortical and/or sub-cortical oedema (McKinney et al.
2007). PRES triggered by transient hypercoagulable state
and successfully treated with anticoagulant therapy using
heparin has been reported (Yano et al. 2005).
Factor VII deciency is a rare hereditary coagulation
disorder with an incidence estimated at 1 in 500,000 (Rizk
et al. 1999). Case report 1 is the rst report of PRES in
pregnancy associated with factor VII deciency. Hae-
mostatic dysfunction consequent upon clotting factor
deciency may be the pathogenesis besides endothelial dys-
function caused by eclampsia. PRES associated with sepsis,
dural puncture and regional anaesthesia have been reported
(Bartynski et al. 2006; Servillo et al. 2008). Case report 2 is
the rst report of PRES in association with twin gestation
and psoas abscess. Hypercoagulable twin pregnant state
besides underlying sepsis could be precipitating factors.
An opportunistic recent survey of 120 obstetricians in
the North West Region in March 2008 revealed paucity of
awareness of condition. PRES although rare is presently a
well acknowledged association of pregnancy, pre-eclampsia
and eclampsia. Obstetricians and other healthcare profes-
sionals involved in the care of pregnant women need to be
aware of this rare but increasingly reported syndrome of
PRES. Advances in the eld of radiology and increasing
expertise in the eld accounts for the rising diagnoses of
PRES. Prompt diagnosis facilitating appropriate treatment
is associated with good outcome, reversibility of clinico-
radiological variabilities and prevents progression to
irreversible brain damage (Finocchi et al. 2005). Appro-
priate MR imaging with DWI and ADC on all cases of
maternal convulsions when CT scan reveals normal
ndings is recommended by the authors, so that pregnancy
associated PRES is diagnosed and treated in a timely
manner.
Declaration of interest: The authors report no conicts
of interest. The authors alone are responsible for the
content and writing of the paper.
References
Bartynski WS, Boardman JF, Zeigler ZR et al. 2006.
Posterior reversible encephalopathy syndrome in infection,
sepsis, and shock. American Journal of Neuroradiology 27:
21792190.
Finocchi V, Bozzao A, Bonamini M et al. 2005.
Magnetic resonance imaging in posterior reversible
encephalopathy syndrome: Report of three cases and
review .of literature. Archives of Gynaecology and Obstetrics
271:7985.
Fujiwara Y, Higaki H, Yamada T et al. 2005. Two cases of
reversible posterior leukoencephalopathy syndrome, one with
and the other without pre-eclampsia. Journal of Obstetric and
Gynaecological Research 31:520526.
Hinchey J, Chaves C, Appignani B et al. 1996. A reversible
posterior leukoencephalopathy syndrome. New England Journal
of Medicine 334:494500.
Mckinney AM, Short J, Truwit LC et al. 2007. Posterior reversible
encephalopathy syndrome: Incidence of atypical regions of
involvement and imaging ndings. American Journal of Radi-
ology 189:904912.
Rizk DE, Castella A, Shaheen H et al. 1999. Factor VII deciency
detected in pregnancy: a case report. American Journal of
Perinatology 16:223226.
Servillo G, Apicella E, Striano P. 2008. Posterior reversible
encephalopathy syndrome (PRES) in the parturient with
preeclampsia after inadvertent dural puncture. International
Journal of Obstetric Anesthesia 17:8889.
Yano Y, Kario K, Fukunaga T et al. 2005. A case of reversible
posterior leukoencephalopathy syndrome caused by transient
hypercoagulable state induced by infection. Hypertension
Research 28:619623.
Table I. Recognised conditions associated with PRES.
Hypertension
Pre-eclampsia
Eclampsia
Systemic lupus erythematosus
Immunosuppressive medications (e.g. cyclosporine)
Anti-neoplastic agents
Severe hypercalcemia
Thrombocytopenic syndromes
Henoch Scho nlein purpura
Haemolytic uraemic syndrome
Amyloid angiopathy
Various causes of renal failure
Regional anaesthesia
Infection/sepsis
Drugs: cocaine, methamphetamine
Sources: McKinney et al. (2007); Servillo et al. (2008).
194 U. Krishnamoorthy et al.
You might also like
- Quinn Et A Predictores de Composicion de Leche 2012Document8 pagesQuinn Et A Predictores de Composicion de Leche 2012Adriana CavazosNo ratings yet
- Content ServerDocument5 pagesContent ServerNi Wayan Ana PsNo ratings yet
- Ibnt 06 I 3 P 377Document2 pagesIbnt 06 I 3 P 377Ni Wayan Ana PsNo ratings yet
- ObsosDocument6 pagesObsosNi Wayan Ana PsNo ratings yet
- Content ServerDocument3 pagesContent ServerNi Wayan Ana PsNo ratings yet
- Content ServerDocument4 pagesContent ServerNi Wayan Ana PsNo ratings yet
- Pi Is 0002937814008084Document8 pagesPi Is 0002937814008084snrarasatiNo ratings yet
- Content ServerDocument4 pagesContent ServerNi Wayan Ana PsNo ratings yet
- The Role of Honey in The Management of Wounds: DiscussionDocument4 pagesThe Role of Honey in The Management of Wounds: DiscussionNi Wayan Ana PsNo ratings yet
- Cervical Stitch (Cerclage) For Preventing Pregnancy Loss: Individual Patient Data Meta-AnalysisDocument17 pagesCervical Stitch (Cerclage) For Preventing Pregnancy Loss: Individual Patient Data Meta-AnalysisNi Wayan Ana PsNo ratings yet
- The Hypercoagulable State in Thalassemia: Hemostasis, Thrombosis, and Vascular Biology Clinical Trials and ObservationsDocument9 pagesThe Hypercoagulable State in Thalassemia: Hemostasis, Thrombosis, and Vascular Biology Clinical Trials and ObservationsNi Wayan Ana PsNo ratings yet
- Cerebrovascular Accident in B-Thalassemia Major (B-TM) and B-Thalassemia Intermedia (b-TI)Document3 pagesCerebrovascular Accident in B-Thalassemia Major (B-TM) and B-Thalassemia Intermedia (b-TI)Ni Wayan Ana PsNo ratings yet
- The Causes of CancerDocument11 pagesThe Causes of CancerShailNo ratings yet
- 2Document10 pages2Ni Wayan Ana PsNo ratings yet
- Title of The Presentation: Your SubtitleDocument2 pagesTitle of The Presentation: Your SubtitleNi Wayan Ana PsNo ratings yet
- Using Antimicrobial Surgihoney To Prevent Caesarean Wound InfectionDocument5 pagesUsing Antimicrobial Surgihoney To Prevent Caesarean Wound InfectionNi Wayan Ana PsNo ratings yet
- Do Clear Cell Ovarian Carcinomas Have Poorer Prognosis Compared To Other Epithelial Cell Types? A Study of 1411 Clear Cell Ovarian CancersDocument7 pagesDo Clear Cell Ovarian Carcinomas Have Poorer Prognosis Compared To Other Epithelial Cell Types? A Study of 1411 Clear Cell Ovarian CancersNi Wayan Ana PsNo ratings yet
- P ('t':'3', 'I':'668636885') D '' Var B Location Settimeout (Function ( If (Typeof Window - Iframe 'Undefined') ( B.href B.href ) ), 15000)Document10 pagesP ('t':'3', 'I':'668636885') D '' Var B Location Settimeout (Function ( If (Typeof Window - Iframe 'Undefined') ( B.href B.href ) ), 15000)Ni Wayan Ana PsNo ratings yet
- 1391283400Document7 pages1391283400Ni Wayan Ana PsNo ratings yet
- Clinical Characteristics of Clear Cell Carcinoma of The OvaryDocument6 pagesClinical Characteristics of Clear Cell Carcinoma of The OvaryNi Wayan Ana PsNo ratings yet
- Passage and Passanger Image Collection (Ana)Document16 pagesPassage and Passanger Image Collection (Ana)Ni Wayan Ana PsNo ratings yet
- 416 1391 1 PBDocument5 pages416 1391 1 PBNi Wayan Ana PsNo ratings yet
- 07 DJMCJ v7 I1 151 Nazia Akhter Obstructed LabourDocument4 pages07 DJMCJ v7 I1 151 Nazia Akhter Obstructed LabourDewi Rahmawati SyamNo ratings yet
- Chemotherapy For Recurrent and Metastatic Cervical CancerDocument5 pagesChemotherapy For Recurrent and Metastatic Cervical CancerNi Wayan Ana PsNo ratings yet
- Skrining CMVDocument10 pagesSkrining CMVNi Wayan Ana PsNo ratings yet
- Distosia Ncbi (Ana)Document8 pagesDistosia Ncbi (Ana)Ni Wayan Ana PsNo ratings yet
- Cytokeratin 7 and Cytokeratin 19 Expressions in Oval Cells and Mature Cholangiocytes As Diagnostic and Prognostic Factors of CholestasisDocument6 pagesCytokeratin 7 and Cytokeratin 19 Expressions in Oval Cells and Mature Cholangiocytes As Diagnostic and Prognostic Factors of CholestasisNi Wayan Ana PsNo ratings yet
- Liver Disease Pediatric PatientDocument14 pagesLiver Disease Pediatric PatientNi Wayan Ana PsNo ratings yet
- Jurnal GastroenterohepatologiDocument18 pagesJurnal GastroenterohepatologiRarasRachmandiarNo ratings yet
- CMV Primer Non PrimerDocument3 pagesCMV Primer Non PrimerNi Wayan Ana PsNo ratings yet
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeFrom EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeRating: 4 out of 5 stars4/5 (5794)
- The Little Book of Hygge: Danish Secrets to Happy LivingFrom EverandThe Little Book of Hygge: Danish Secrets to Happy LivingRating: 3.5 out of 5 stars3.5/5 (400)
- Shoe Dog: A Memoir by the Creator of NikeFrom EverandShoe Dog: A Memoir by the Creator of NikeRating: 4.5 out of 5 stars4.5/5 (537)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceFrom EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceRating: 4 out of 5 stars4/5 (895)
- The Yellow House: A Memoir (2019 National Book Award Winner)From EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Rating: 4 out of 5 stars4/5 (98)
- The Emperor of All Maladies: A Biography of CancerFrom EverandThe Emperor of All Maladies: A Biography of CancerRating: 4.5 out of 5 stars4.5/5 (271)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryFrom EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryRating: 3.5 out of 5 stars3.5/5 (231)
- Never Split the Difference: Negotiating As If Your Life Depended On ItFrom EverandNever Split the Difference: Negotiating As If Your Life Depended On ItRating: 4.5 out of 5 stars4.5/5 (838)
- Grit: The Power of Passion and PerseveranceFrom EverandGrit: The Power of Passion and PerseveranceRating: 4 out of 5 stars4/5 (588)
- On Fire: The (Burning) Case for a Green New DealFrom EverandOn Fire: The (Burning) Case for a Green New DealRating: 4 out of 5 stars4/5 (73)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureFrom EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureRating: 4.5 out of 5 stars4.5/5 (474)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaFrom EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaRating: 4.5 out of 5 stars4.5/5 (266)
- The Unwinding: An Inner History of the New AmericaFrom EverandThe Unwinding: An Inner History of the New AmericaRating: 4 out of 5 stars4/5 (45)
- Team of Rivals: The Political Genius of Abraham LincolnFrom EverandTeam of Rivals: The Political Genius of Abraham LincolnRating: 4.5 out of 5 stars4.5/5 (234)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyFrom EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyRating: 3.5 out of 5 stars3.5/5 (2259)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreFrom EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreRating: 4 out of 5 stars4/5 (1090)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersFrom EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersRating: 4.5 out of 5 stars4.5/5 (344)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)From EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Rating: 4.5 out of 5 stars4.5/5 (121)
- Her Body and Other Parties: StoriesFrom EverandHer Body and Other Parties: StoriesRating: 4 out of 5 stars4/5 (821)
- Anti-HSV-2 IgG Herpes Simplex Virus Type 2Document2 pagesAnti-HSV-2 IgG Herpes Simplex Virus Type 2ElenaNo ratings yet
- Varicose Veins Diagnosis and TreatmentDocument7 pagesVaricose Veins Diagnosis and Treatmenthossein kasiriNo ratings yet
- Disruptive Behavioral DisorderDocument5 pagesDisruptive Behavioral Disorderapi-228136529100% (1)
- Medical Examination Report: A. Examinee DetailsDocument4 pagesMedical Examination Report: A. Examinee DetailsMohammed Bilal ShaikNo ratings yet
- Rogelio Ramos Vs CADocument28 pagesRogelio Ramos Vs CAAnonymous FBDGfUqHENo ratings yet
- Asthma - Discharge Care For Adults - EnglishDocument2 pagesAsthma - Discharge Care For Adults - EnglishMalik Khuram ShazadNo ratings yet
- Careers in Biomedical ScienceDocument24 pagesCareers in Biomedical ScienceEncik LaLaNo ratings yet
- Tabel Perbandingan MSC Dan EksosomDocument5 pagesTabel Perbandingan MSC Dan EksosomRaisha FathimaNo ratings yet
- A Trauma and Systems ChangeDocument80 pagesA Trauma and Systems Changemarco0082No ratings yet
- A 25-Year-Old Man With New-Onset Seizures PDFDocument8 pagesA 25-Year-Old Man With New-Onset Seizures PDFMr. LNo ratings yet
- Long COVIDDocument8 pagesLong COVIDSMIBA MedicinaNo ratings yet
- EU Digital COVID Certificate Certificat Digital European COVIDDocument2 pagesEU Digital COVID Certificate Certificat Digital European COVIDDespre FotografieNo ratings yet
- AXA - Sales Brochure Qatar - ALL - ENDocument10 pagesAXA - Sales Brochure Qatar - ALL - ENAhmad MuhammadNo ratings yet
- 1mg PrescriptionDocument2 pages1mg PrescriptionSankalp IN GamingNo ratings yet
- Rad 3 PDFDocument5 pagesRad 3 PDFjovanaNo ratings yet
- 7 Rights of Medication AdminstrationDocument5 pages7 Rights of Medication Adminstrationpgreenbaum5377No ratings yet
- Studi Kasus: Kehamilan Dengan: Dengan Katub Jantung Prostetik Mekanik Dan Penggunaan AntikoagulanDocument10 pagesStudi Kasus: Kehamilan Dengan: Dengan Katub Jantung Prostetik Mekanik Dan Penggunaan AntikoagulanMonyet...No ratings yet
- Guidance Document - Nutritional Care & Support For TB Patients in India PDFDocument107 pagesGuidance Document - Nutritional Care & Support For TB Patients in India PDFekalubisNo ratings yet
- Global Impact of The First Year of COVID-19 VaccinationDocument10 pagesGlobal Impact of The First Year of COVID-19 VaccinationRoel PlmrsNo ratings yet
- الميكروبيولوجى والتحكم فى العدوىDocument115 pagesالميكروبيولوجى والتحكم فى العدوىmahmoud salahNo ratings yet
- SupervisorsDocument1 pageSupervisorsBOOKREADER_NOW100% (2)
- Biological Products: by Randy NavaretteDocument9 pagesBiological Products: by Randy Navaretteapi-550314322No ratings yet
- Roleplay Discharge PlanningDocument3 pagesRoleplay Discharge PlanningAnonymous KQKONmD9H100% (1)
- Fee Paying FreshDocument3 pagesFee Paying FreshQuame HazyNo ratings yet
- Rizal As A Doctor PDFDocument17 pagesRizal As A Doctor PDFIan CortadoNo ratings yet
- Sample CollectionDocument41 pagesSample Collectionsoumen100% (1)
- Conrad Munashe Mashazhike: 58 Tembisa Section - +27 68 225 5504 - 25 May 2022Document3 pagesConrad Munashe Mashazhike: 58 Tembisa Section - +27 68 225 5504 - 25 May 2022Nathi MashazhikeNo ratings yet
- Drug Study - AlleyahDocument10 pagesDrug Study - AlleyahLorenzo, Alleyah Jaira D.No ratings yet
- Factfile 1: Mental Health and EmploymentDocument4 pagesFactfile 1: Mental Health and Employmenttony_jameson-allenNo ratings yet
- Medical TechnologistDocument2 pagesMedical Technologistapi-307429612No ratings yet