Professional Documents
Culture Documents
Cushing's Syndrome in Children
Uploaded by
stbmi1230 ratings0% found this document useful (0 votes)
33 views45 pagesCushing's Syndrome
Copyright
© © All Rights Reserved
Available Formats
PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCushing's Syndrome
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
33 views45 pagesCushing's Syndrome in Children
Uploaded by
stbmi123Cushing's Syndrome
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
You are on page 1of 45
Cushings syndrome in children
due to adrenal tumors
Department of Endocrine Surgery Department of Endocrine Surgery
SGPGIMS, Lucknow
INDIA
Agenda
Introduction
Presentation of illustrative cases
Review of literature
Introduction
Functioning Adrenal Tumors
Cortex Medulla
Hormone Cortisol Androgens Aldosterone Catecholamines
Disease Cushings
syndrome
Virilization/
Precocity
Conns
syndrome
Pheochromocytoma
Functioning Adrenocortical Tumors in
Children & Adolescents- Unique features
Rare (0.2% of all pediatric neoplasms)
Fascinating spectrum of clinical features
Need careful biochemical evaluation
High proportion of malignancy in infancy
Difficult to predict biological behavior Difficult to predict biological behavior
Difficult to predict malignancy on Histopathology
Surgeons handling these cases should be well versed with
endocrine physiology and their aberrations
Surgery remains the mainstay of treatment
Offers cure in benign tumors
Best means of palliation in malignant cases
Multidisciplinary approach involving Pediatricians, Pediatric
Endocrinologists, Surgeons, Pathologists, Geneticists
Algorithm of hormonal evaluation in a clinically
suspected case of Cushings syndrome
Screening test
Overnight DST
Confirmatory test
Low dose DST
No hypercortisolism
Cortisol suppressed
Cortisol not suppressed
Cortisol suppressed
No Cushings
syndrome
ACTH
Pituitary origin/
Cortisol not suppressed
ACTH
Pituitary origin/
Ectopic ACTH production
High
Adrenal origin
Low
High dose DST
Pituitary origin
Ectopic ACTH
production
Cortisol
suppressed
Cortisol
not suppressed
DST= Dexamethasone suppression test
Illustrative Cases Illustrative Cases
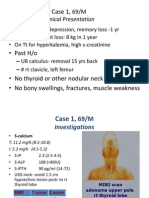
Case 1 Case 1
9 years/ boy
c/o-
Progressive weight
gain- 1 year
(10 kg in one year)
Examination
Weight- 35 kg
Height- 115.3 cm
BP- 124/80 mm Hg
Examination
Differential Diagnosis
Cushings syndrome, cause?-
ACTH independent-
Adrenal adenoma/ carcinoma Adrenal adenoma/ carcinoma
ACTH dependent-
Pituitary tumor (Cushings disease)
Ectopic ACTH secreting tumor
Hormonal profile
Hormone Value Normal range Inference
LDDST
1015 nmol/L
<50 Confirmation of
Cushings syndrome
HDDST
859.7 nmol/L
<50 Non pituitary origin
ACTH 21.50 pg/ml 4- 50 ACTH ACTH 21.50 pg/ml 4- 50 ACTH
independence
Testosterone 0.56 nmol/L 0- 2.8 Not elevated
Interpretation- ACTH independent Cushings
syndrome due to adrenal pathology
CECT Abdomen
Homogeneous soft tissue lesion (3.4x3.1x3.5cm) in
left suprarenal region s/o left adrenal mass
Left adrenalectomy
12-Sep-2007
Findings-
Tumor in body of
adrenal- 4x3.5x2 cm
Weight- 26 gms
No adhesions/ No adhesions/
metastases/ ascites
Cut section- Fleshy
and homogeneous
Specimen split open
Histopathology
Mitosis
AFIP Criteria for malignancy in
Pediatric ACC
Gross-
Tumor weight- >400
gm
Tumor size- >10.5 cm
IVC invasion
Microscopic-
Capsular invasion
Vascular invasion
Tumor necrosis
IVC invasion
Periadrenal infiltration
>15 mitoses/ 20 hpf
Atypical mitotic figures
0- absent, 1-present
0-2- benign, 3- indeterminate, 4-9- malignant
Wieneke JA et al. Am J Surg Pathol. 2003;27:867-81
Histopathology
Gross
Size- 4 cm
Weight- 26 gms
No periadrenal infiltration
Mitosis <15/20 hpf
No atypical mitosis
No necrosis
No capsular or vascular invasion
Score- 0/9
Impression- Adenoma
Post operative Course
Uneventful
Postoperative stress doses of steroids
Discharged on physiological doses (advice for stress doses)
Plan- Test for recovery of HPA axis after 3 months
Value Normal Value Normal
Basal 75.7 nmol/L 110-540
60-min after ACTH 322.9 nmol/L >540
Interpretation- HPA axis not recovered
Steroids continued
Preoperative
35 kg/ 115.3 cm
2 weeks
postoperative
8 months
postoperative
22.7 kg/ 122 cm
3 months
postoperative
Preoperative
35 kg/ 115.3 cm
2 weeks
postoperative
8 months
postoperative
22.7 kg/ 122 cm
3 months
postoperative
Case 2 Case 2
6 months/girl
Referred as a case of
right adrenal mass
with c/o-
Diarrhea- 4 months
Weight gain- 2 months
Irritable with sleep- 2
months
Growth rate
General Examination
Length- 56.5 cm
Weight- 9.5 kg
BMI- 29.8 kg/m
2
BP- 120/44 mm Hg
Buffalo hump
BP- 120/44 mm Hg
Perianal excoriation
present
Examination
Moon facies
Hormonal Profile
Hormone Value Normal range Inference
LDDST
>1380 nmol/l
<50 Confirmatory of
Cushings syndrome
ACTH 18.2 pg/ml 4-50 ACTH independent
DHEAS 6.44 mol/L 0.8-8.99 Normal
Testosterone
8.7 nmol/L
Undetectable Hyperandrogenemia
Interpretation- Cushings syndrome with
Hyperandrogenemia due to adrenal pathology (?malignant)
USG abdomen
Right adrenal mass-
Well defined, hypoechoic with cystic areas
37 x 30 mm
CECT abdomen
Right adrenal mass-
27 x 38 mm
Heterogeneous
Solid cystic areas
Right adrenalectomy
15-Apr-2011
Well encapsulated right adrenal mass- 4 x 4 x 3 cm
Weight- 25 gms
No adhesions/ metastases/ ascites
Cut section- fleshy, variegated appearance
Histopathology
Normal Adrenal
Histopathology
Gross
Size- 4 cm
Weight- 25 gms
No periadrenal infiltration
Mitosis <15/20 hpf
No atypical mitosis
No necrosis
No capsular or vascular invasion
Score- 0/9
Impression- Adenoma
Postoperative course
Uneventful
Postoperative stress doses of steroids
Discharged on physiological doses of
Steroids (advice for stress doses)
9/7/2014 Cushing's syndrome in children
Preoperative
3-months postoperative
3-months follow up
Hormones Value Normal range
Testosterone 10.42 nmol/L Undetectable
Cortisol
Basal
389 nmol/L 110-540
60-min after ACTH 715 nmol/L >540
HPA axis recovered
Exogenous steroids stopped
Imaging (USG abdomen and Chest X
Ray)- normal
Preoperative
3 months
1-year postoperative
Adrenal tumour in children
Review Review
Epidemiology
Rare (Incidence- 1-2/ million per year)
Usually sporadic
May be a part of hereditary May be a part of hereditary
syndromes
Allolio et al. Clin Endocrinol. 2004;60:273-87.
Sutter JA et al. Pediatr Endocrinol Rev. 2006;4:32-9.
Phan AT. Hematol Oncol Clin North Am. 2007;21:489-507.
Presentation
Michalkiewicz et
al, 2004
Sutter and
Grimberg, 2006
Virilization 55.1% 50-84%
Mixed 29.2%
Cushings 5.5% 15-40%
Feminization 7%
Hyperaldosteronism 1-4%
Non functional 10.2%
Evaluation
Clinical-
History
Examination
Biochemical & Hormonal Biochemical & Hormonal
Imaging
Genetic profile if indicated and feasible
Staging systems
McFarlane/ Sullivan 1978/ AJCC 2002
UICC/ WHO (TNM) 2004
IPACTR 2004
ENSAT 2008
COG 2011
Treatment
Surgery-
Treatment of choice (whenever possible)
Adjuvant medical management (in advanced
stages/ unresectable tumors)- stages/ unresectable tumors)-
Mitotane (M)-
Narrow therapeutic window
Significant CNS, GI toxicity
Cytotoxic chemotherapy
EDP (Etoposide, Doxorubicin, Cisplatin)
Streptozotocin (Sz)
Radioresistant
Ongoing and Future research
Trials-
Berrutti, 2005- (M+EDP)
Khan, 2000- (M+Sz)
Ongoing International trials- Ongoing International trials-
FIRM-ACT- M+Sz vs. M+EDP
Adiuvo- adjuvant M vs. follow-up only
IGF I & IGF II receptor antagonists
mTOR antagonists
Take home message
Rare entity
Varied presentations
Complex hormonal interplay
Needs expertise in evaluation and Needs expertise in evaluation and
management
Multidisciplinary approach
Surgery offers the only chance of cure
Regular follow up
THANK YOU
9/7/2014 Cushing's syndrome in children
THANK YOU
You might also like
- Endo RadiologyDocument245 pagesEndo Radiologystbmi123No ratings yet
- Intrathyroidal Parathyroid AdenomaDocument60 pagesIntrathyroidal Parathyroid Adenomastbmi123No ratings yet
- Insulin OmaDocument42 pagesInsulin Omastbmi123No ratings yet
- Hypervitaminosis D After ParathyroidectomyDocument8 pagesHypervitaminosis D After Parathyroidectomystbmi123No ratings yet
- Endocrine Imaging 11th PGES CourseDocument119 pagesEndocrine Imaging 11th PGES Coursestbmi123No ratings yet
- Adrenal LymphomaDocument23 pagesAdrenal Lymphomastbmi123No ratings yet
- Case 2Document22 pagesCase 2stbmi123No ratings yet
- Case 4Document24 pagesCase 4stbmi123No ratings yet
- Adrenocortical Tumors in ChildrenDocument31 pagesAdrenocortical Tumors in Childrenstbmi123No ratings yet
- Case 3Document18 pagesCase 3stbmi123No ratings yet
- Case 1Document18 pagesCase 1stbmi123No ratings yet
- ER Case1Document36 pagesER Case1stbmi123No ratings yet
- Case 3Document15 pagesCase 3stbmi123No ratings yet
- ER Case 2Document13 pagesER Case 2stbmi123No ratings yet
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeFrom EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeRating: 4 out of 5 stars4/5 (5794)
- Shoe Dog: A Memoir by the Creator of NikeFrom EverandShoe Dog: A Memoir by the Creator of NikeRating: 4.5 out of 5 stars4.5/5 (537)
- The Yellow House: A Memoir (2019 National Book Award Winner)From EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Rating: 4 out of 5 stars4/5 (98)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceFrom EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceRating: 4 out of 5 stars4/5 (895)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersFrom EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersRating: 4.5 out of 5 stars4.5/5 (344)
- The Little Book of Hygge: Danish Secrets to Happy LivingFrom EverandThe Little Book of Hygge: Danish Secrets to Happy LivingRating: 3.5 out of 5 stars3.5/5 (399)
- Grit: The Power of Passion and PerseveranceFrom EverandGrit: The Power of Passion and PerseveranceRating: 4 out of 5 stars4/5 (588)
- The Emperor of All Maladies: A Biography of CancerFrom EverandThe Emperor of All Maladies: A Biography of CancerRating: 4.5 out of 5 stars4.5/5 (271)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaFrom EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaRating: 4.5 out of 5 stars4.5/5 (266)
- Never Split the Difference: Negotiating As If Your Life Depended On ItFrom EverandNever Split the Difference: Negotiating As If Your Life Depended On ItRating: 4.5 out of 5 stars4.5/5 (838)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryFrom EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryRating: 3.5 out of 5 stars3.5/5 (231)
- On Fire: The (Burning) Case for a Green New DealFrom EverandOn Fire: The (Burning) Case for a Green New DealRating: 4 out of 5 stars4/5 (73)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureFrom EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureRating: 4.5 out of 5 stars4.5/5 (474)
- Team of Rivals: The Political Genius of Abraham LincolnFrom EverandTeam of Rivals: The Political Genius of Abraham LincolnRating: 4.5 out of 5 stars4.5/5 (234)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyFrom EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyRating: 3.5 out of 5 stars3.5/5 (2259)
- The Unwinding: An Inner History of the New AmericaFrom EverandThe Unwinding: An Inner History of the New AmericaRating: 4 out of 5 stars4/5 (45)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreFrom EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreRating: 4 out of 5 stars4/5 (1090)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)From EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Rating: 4.5 out of 5 stars4.5/5 (120)
- Her Body and Other Parties: StoriesFrom EverandHer Body and Other Parties: StoriesRating: 4 out of 5 stars4/5 (821)
- 2010 Bandelow ExtendedDocument16 pages2010 Bandelow ExtendedRian YupitaNo ratings yet
- c17 Microbiology Tortora TestbankDocument18 pagesc17 Microbiology Tortora Testbankwhitewave25No ratings yet
- SodiumDocument1 pageSodiumyoyoyoNo ratings yet
- Precautions - Isolation Precautions - Guidelines Library - Infection Control - CDCDocument6 pagesPrecautions - Isolation Precautions - Guidelines Library - Infection Control - CDCKomite PPI RSUDPCNo ratings yet
- The Benefits of ChocolateDocument2 pagesThe Benefits of ChocolateHanna FairussaniaNo ratings yet
- SeizureDocument10 pagesSeizureRomeo ReyesNo ratings yet
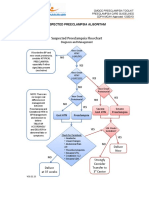
- Suspected Preeclampsia AlgorithmDocument1 pageSuspected Preeclampsia Algorithmmisstina.19876007100% (1)
- Theories of NeurosisDocument170 pagesTheories of NeurosisemilvulcuNo ratings yet
- Management of Tinea Corporis, Tinea CrurisDocument10 pagesManagement of Tinea Corporis, Tinea CrurisRansidelenta Vistaprila ElmardaNo ratings yet
- Night Float Survival GuideDocument23 pagesNight Float Survival GuideNunu Mir100% (5)
- Closed Fracture OsDocument23 pagesClosed Fracture OsDiana Lita SNo ratings yet
- Caroline Stone. Osteopathic ApproachDocument54 pagesCaroline Stone. Osteopathic ApproachIoan Andra100% (5)
- PharmacogeneticsDocument8 pagesPharmacogeneticskangaroocherryNo ratings yet
- Otitis MediaDocument34 pagesOtitis MediaEdson Reinier Joseph EnriquezNo ratings yet
- Complications in Dentoalveolar Surgery PDFDocument37 pagesComplications in Dentoalveolar Surgery PDFmirfanulhaqNo ratings yet
- Wurzel 2016Document8 pagesWurzel 2016prolanis pkmmulyoharjoNo ratings yet
- Threats of Vector-Borne Zoonotic Disease in Europe: Dogs, Drosophilids, and Oriental Eye WormDocument3 pagesThreats of Vector-Borne Zoonotic Disease in Europe: Dogs, Drosophilids, and Oriental Eye WormGustavo AndresNo ratings yet
- Dnrle Influenza NCPDocument3 pagesDnrle Influenza NCPEna RodasNo ratings yet
- Low-Cost Breath AnalyzerDocument20 pagesLow-Cost Breath AnalyzeradnanNo ratings yet
- وسيلة منصوريDocument126 pagesوسيلة منصوريhouda houdaNo ratings yet
- Assesment Preop - Rohemi 28.09.21Document27 pagesAssesment Preop - Rohemi 28.09.21Reza Devianto HambaliNo ratings yet
- ParkinsonDocument12 pagesParkinsonStephanie NieNo ratings yet
- Psychodynamic Treatment For DepressionDocument20 pagesPsychodynamic Treatment For DepressionRenzo GonzalesNo ratings yet
- 1 s2.0 S1526054219300235 MainDocument4 pages1 s2.0 S1526054219300235 MainBruno SantosNo ratings yet
- People Running PowerPoint TemplatesDocument16 pagesPeople Running PowerPoint TemplatesPutri Aulia AmaraNo ratings yet
- Drug Information of SilodosinDocument8 pagesDrug Information of SilodosinSomanath BagalakotNo ratings yet
- 2016 Opioid Presribing Rate Part DDocument104 pages2016 Opioid Presribing Rate Part DJennifer EmertNo ratings yet
- Cellulitis Talk Jan 2018Document16 pagesCellulitis Talk Jan 2018Ramsyifa VirzanisdaNo ratings yet
- Bile Duct DilatedDocument4 pagesBile Duct DilatedAmit GauravNo ratings yet
- Paper. Stem Cells Applications in Regenerative Medicine andDocument25 pagesPaper. Stem Cells Applications in Regenerative Medicine andMike NundweNo ratings yet