Professional Documents
Culture Documents
The Neurologic System
Uploaded by
Justine Jake L. Ella0 ratings0% found this document useful (0 votes)
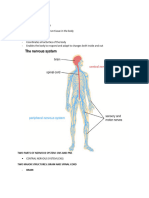
98 views12 pagesThe nervous system is composed of neurons with cell bodies that contain genetic material and organelles. Neurons have dendrites that receive signals and axons that transmit signals away from the cell body. There are three main types of neurons - sensory neurons that transmit peripheral signals to the central nervous system, motor neurons that carry signals from the central nervous system, and interneurons that connect sensory and motor neurons. The nervous system is protected and supported by glial cells in the central nervous system like oligodendrocytes and astrocytes, and Schwann cells and satellite cells in the peripheral nervous system. Nerve impulses are transmitted through changes in ion concentrations along the neuron membrane in a process called action potential.
Original Description:
Some concepts and quick browsing
Copyright
© © All Rights Reserved
Available Formats
DOCX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentThe nervous system is composed of neurons with cell bodies that contain genetic material and organelles. Neurons have dendrites that receive signals and axons that transmit signals away from the cell body. There are three main types of neurons - sensory neurons that transmit peripheral signals to the central nervous system, motor neurons that carry signals from the central nervous system, and interneurons that connect sensory and motor neurons. The nervous system is protected and supported by glial cells in the central nervous system like oligodendrocytes and astrocytes, and Schwann cells and satellite cells in the peripheral nervous system. Nerve impulses are transmitted through changes in ion concentrations along the neuron membrane in a process called action potential.
Copyright:
© All Rights Reserved
Available Formats
Download as DOCX, PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
98 views12 pagesThe Neurologic System
Uploaded by
Justine Jake L. EllaThe nervous system is composed of neurons with cell bodies that contain genetic material and organelles. Neurons have dendrites that receive signals and axons that transmit signals away from the cell body. There are three main types of neurons - sensory neurons that transmit peripheral signals to the central nervous system, motor neurons that carry signals from the central nervous system, and interneurons that connect sensory and motor neurons. The nervous system is protected and supported by glial cells in the central nervous system like oligodendrocytes and astrocytes, and Schwann cells and satellite cells in the peripheral nervous system. Nerve impulses are transmitted through changes in ion concentrations along the neuron membrane in a process called action potential.
Copyright:
© All Rights Reserved
Available Formats
Download as DOCX, PDF, TXT or read online from Scribd
You are on page 1of 12
The Neurologic System
Anatomy and Physiology
NERVOUS SYSTEM
COMPOSED OF:
1)Cell Body -contains large vesicular nucleus with one nucleoli and a
rough endoplasmic reticulum.
- contain DNA and genetic content that is present in other cells of the
body. Function of procedures DNA associated with Protein Synthesis
Parts:
a.Mitochondria
b.Organelle - lacks centrioles and centrosome which are important in cell
division.
2) Dendrites- branch type structures with synapses
- conduction of information is towards the body.
3) Axon- long efferent processes
- projects from cell body
- carries impulses away from the cell body.
a. Afferent ( sensory ) neurons - transmit information from peripheral to CNS
b. Efferent ( motor ) neurons - carry information away from the CNS
c. Interneuron ( internutia ) - connects the sensory and motor neurons
SUPPORTING STRUCTURES OF PNS:
Satellite
Schwann cells
Glial cells
Functions:
-Protection
-Provision of nutrition
-Support
-Conduction of impulses
- Insulation
1. Schwann cells - responsible for the formation of myelin sheath for myelination
PNS -covering the axon
More covering C fibers (dull pain)
Small covering E and B fibers (sharp and throbbing pain)
2. Nodes of Ranvier -accelerates transmission of impulses
-unmyelinated
Na - major component of ECF
Saltatory Conduction
- allowing to jump from node to node through ECF
- Salthe- latin word meaning tojump
- Process of jumping impulses from node to node with the used of ECF
Satellite Cells
- secretes the basement membrane that protects the body from the diffusion of large
molecule.
SUPPORTING STRUCTURES OF CNS:
1. Glial Cells
2. Oligodendroglial cells
-produces myelin sheath in the CNS
-reach out several process and from multi myelin sheath
-velocity of nerve conduction
3. Astroglia
-encapsulating the CNS
-main source of blood brain barrier
-maintain chemical environment of neurons -ex. glucose
-provides transport mechanism for exchange of O2,CO2 metabolism
-creates a special scar tissue called gliosis
4. Microglia cells
-small phagocytic cells responsible for cleaning up debris after cellular
damage, infection or cell death
5. Ependymal cells
-form the living of neural tube cavity
-abundant in choroids plexus-produce CSF
Metabolism Activity of the Brain:
10sec. -brain can survive
4-6 min. -cell death occur
Na and K- major ions of the brain
NERVE IMPULSE
Action Potential
-potential of the neuron to conduct by changing ion contents
-concentrates more on depolarization and repolarization
3 PHASES:
a. Resting phase- undisturbed period of action potential during which nerve do not
transmit impulses
(+ )charge- inside
(- ) charge- outside
Large fibers- needs 90m volts.
Smaller fibers- needs 40-60m volts.
b. Threshold Potential K+ leaks out
- concentration of Na should be equal to or above 60m volts or more.
-if below , the gate is closed
c. Repolarization
- the Na channels immediately closed but potassium channel open, not to allow
Na inside but for K to go outside by itself.
3 STIMULUS:
1. Adequate stimulus
-kind of physical or chemical change when the receptor is sensitive.
- 90 m volts.
2. Minimal stimulus
- is at least change that can excite the receptor
- 40-60 m volts.
3. Subminimal stimulus
-kind of physical chemical change below the threshold level that fails to excite
SYNAPTIC TRANSMISSION
Synapse - point of continuity that permits transmitter or transmission of activity from
one neuron to another.
2 types:
Electrical Synapse
- permits the passage of current carrying ions through small opening called
gap junction
- allow action potential to pass quickly and directly from one neuron to
another
Chemical Synapse
- Most Common
- involves special presynaptic and postsynaptic structures separated by a
synaptic junction
NEUROTRANSMITTERS
- communicates messages
- potentiate,terminate or modulate a specific action and can either excite or inhibit cell
activity.
- maybe in a form of peptides.
- stored and manufactured in the synaptic vesicles
- small molecules that incorporate a positively charge nitrogen atoms.
THE CENTRAL NERVOUS SYSTEM
Anatomy of the Brain
Three major parts:
1. Cerebrum
a. Frontal- the largest lobe the major functions are concentration, abstract
thought, information storage and motor function.
b. Parietal- a predominantly sensory lobe. The primary sensory cortex
which analyze sensory informations and relays the interpretations of this information
to the thalamus and other cortical areas
c. temporal- contains the auditory receptive areas and also contains vital
area called the interpretive area.
d. occipital- the posterior lobe of the cerebral hemisphere, is responsible
for visual interpretation
e. Central or Insula
Hipocampus essential role in the process of memory.
Corpus Callosum
- The thick connection of nerve fibers that connects the two hemispheres of the brain
and is responsible for the transmission of information from one side of the brain
to the other.
Basal Ganglia
- Basal ganglia are masses of nuclei located deep in the cerebral hemispheres that
are responsible for control of fine motor movements, including those of the hands and
lower extremities.
Diencephalon:
a. Thalamus
b. Hypothalamus
Pituitary Gland
- Pituitary gland is located in the sella turcica at the base of the brain and is connected
to the hypothalamus. It is the common site for the brain tumors in adults; frequently
they are detected by the physical signs and symptoms that can be traced to the
pituitary, such as hormonal imbalance or visual disturbances secondary to pressure or
optic chiasm.
Limbic system
2. Brain stem
- The brain stem consists of the midrabrain, pons and medulla oblongata.
- The midbrain connects the pons and the cerebellum with the cerebral hemispheres.
- The pons is situated in front of the cerebellum between the midbrain and the medulla
and is a bridge between the two halves of the cerebellum.
- The medulla oblongata contains motor fibers from the brain to the spinal cord and
sensory fibers from spinal cord to the brain.
Reticular formation
3. Cerebellum
- Cerebellum is separated from the cerebral hemispheres by a fold of dura mater,
tentorium cerebelli. The cerebellum has both the excitatory and inhibitory actions and
is largely responsible for coordination of movement.
The brain is contained in the rigid skull, which protects it from injury. The
major bones of the skull are the frontal, temporal, parietal, and occipital bones. These
bones join at the suture lines.
Skull
- is a bony structure which serves as the general framework for a head. The skull
attempts to protect the brain, acting as a form of natural helmet.
2 sets of bones in the skull
a. cranium
- is that part of the skull that holds and protects the brain in the large cavity called the
cranial vault.
b. Facial bone - holds the eye in anterior position and allows facial
muscles to show our feelings.
The meninges (fibrous connective tissue)
- Provide protection, support and nourishment to the brain and spinal cord. The layers
of the meninges are the dura, arachnoid and pia mater.
a. Dura mater-the outermost layer; covers the brain and the spinal cord. It is rough,
thick, inelastic,fibrous and gray.
Layers of Dura mater:
-periosteal layer- attach to the inner surface of the skull.
-meningeal layer- forms the outermost covering of the brain continues as the dura
mater of the spinal cord.
Four extensions of the dura :
falx cerebri
tentorium
falx cerebelli
diaphragm sellae
Epidural space
- located between the dura mater and the skull in the cranium.
b. Arachnoid
- the middle membrane; an extremely thin, delicate membrane that loosely
resembles a spider web.
- appears white, contains choroid plexus.
Subdural space
- located in between the dura mater and arachnoid layer.
c. Pia mater
- the innermost membrane; a thin transparent layer that hugs the brain closely and
extends into every fold of the brains surface.
Subarachnoid space
- in between the arachnoid and the pia mater.
CEREBROSPINAL FLUID
- a clear and odorless fluid with a specific gravity of 1.007, is produced in the
ventricles and is circulated around the brain and the spinal cord through the
ventricular system.
clear fluid that occupies the subarachnoid space (the space between the skull and
cortex of the brain).
- It acts as a "cushion" or buffer for the cortex.
- provides a supporting and protective fluid in which the brain and the spinal cord float.
- helps maintain a constant ionic environment that serves as a medium for diffusion of
nutrients, electrolytes and metabolic end products into the extracellular fluid
surrounding CNS neurons and glia.
- CSF occupies the ventricular system of the brain and the spinal cord. CSF is mainly
produced by the choroid plexus, but also by the epindymal lining of the brain's
ventricles.
- 500 ml CSF is produced normally per day, 150 ml stays in the circulation and 350 ml
is reabsorbed in the arachnoid villi.
CEREBRAL CIRCULATION
- Receives approximately 15% of the cardiac output or 750ml per min. In contrast to
other organs that may tolerate decreases in the blood flow because of their adequate
collateral circulation,the brain lacks additional collateral blood flow result in irreversible
tissue damage when blood flow is occluded for even short periods of time.
BLOOD BRAIN BARRIER
- Barrier present in circulating blood and brain tissues that protects the CNS.
Function of BBB:
- Primarily regulate and maintain an optimal and stable chemical environment for
neurons.
There are three brain barriers, namely:
1. Blood-brain
2. Blood-CSF
3. Brain-CSF
Two types:
1. Physical Barriers- it includes tight junctions of the endothelial cells lining the
capillaries, pores of the capillaries of the choroid plexuses, the basement membrane
(ependymal cells) next to the choroid plexuses, and the pial-glial membrane.
2. Physiologic Process (Transport System)- Metabolic wastes, such as urea, toxins,
proteins and most drugs are prevented from entering the brain tissue.
Certain events can increase the permeability of the blood-brain barrier.
Dilutional hyponatremia
Acute hypertension
High doses of some anesthetics
Vasodilation
Hypercarbia
SPINAL CORD
- portion of the CNS that is protected by the vertebral column and encased in the
vertebral canal.
- extends from foramen magnum of the skull, where it is continuous with the medulla
oblongata to 2
nd
lumbar vertebra; filum terminale to 1
st
coccygeal vertebra.
- Average length about 42-45 cm.
The blood supply is from the anterior spinal artery and from a succession
of small arteries which enter the spinal canal through the intervertebral foramina;
these branches are derived.
-Consist of gray matter in form of H enclosed within white matter.
Inner column of gray matter contains:
1. ) 2 anterior horns- contain efferent (motor) nerve fibers.
2. ) 2 Posterior horns- connect the afferent (sensory) nerve fib
White matter -Consist of:
Ascending tract (sensory pathway)- posterior spinal cord
Descending tract (motor pathway)- anterior spinal cord
Fissures: Consist of:
Ventral sulcus- divides front portion into lateral halves
Dorsal sulcus- divides back portion into lateral halves
Membranes of Spinal cord:
1. Pia Mater
2. Arachnoid Mater
3. Dura mater
Functions of Spinal Cord:
1. Important center of reflex for the trunk and limbs.
2. Consists of the principal conducting paths to and from the higher centers in the
brain.
3. Provide neuron and synapse network to produce involuntary responses to sensory
stimulation. Also allows for control of the no. of pain impulses that pass through the
spinal cord on their way to the brain.
4. Carries sensory information to, and motor information from the brain.
VERTEBRAL COLUMN
- a flexible series of vertebrae, surrounds and protects the spinal cord.
Ligaments hold the vertebrae together.
Consists of the following:
cervical 8 pairs
thoracic 12 pairs
lumbar 5 pairs
sacral 5 pairs
coccygeal 1 pair
total= 31 pairs
Spinal Nerves
- The spinal cord is composed of 31 pairs of spinal nerves: 8 cervical, 12
thoracic, 5 lumbar, 5 sacral and 1 coccygeal. Each spinal nerve has
ventral root and a dorsal root.
- The dorsal roots are sensory and transmit sensory impulses from specific
areas of the body known as dermatomes to the dorsal ganglia. The
sensory fiber maybe somatic, carrying information about pain,
temperature, touch and position sense (proprioception) from the tendons,
joints, and body surfaces; or visceral, carrying information from the internal
organ.
- The ventral roots are motor and transmit impulses from the spinal cord to
the body. These fibers are also either somatic or visceral. The visceral
fibers include autonomic fibers that control the cardiac muscles and
glandular secretions.
AUTONOMIC NERVOUS SYSTEM
Part of the PNS that coordinates involuntary activities
Has two division:
(1) Sympathethic Nervous System,
(2) Parasympathetic Nervous System
ANS has also two neurons:
(1) Preganglionic neuron- located in the brain or spinal cord and it's axon extends to
the autonomic ganglia
(2) Postganglionic neuron- located in the autonomic ganglia, it's axon synapses with
the target tissue and innervates the effector organ.
The hypothalamus is the major subcortical center for the regulation on visceral and
somatic activities with an inhibitory-excitatory role in the ANS.
1. SENSORY (AFFERENT) DIVISIONS
- relay messages about internal and external body environmental changes
to the CNS through specific receptors.
2 Specific Receptors:
a. Somatic- carry impulses from the skin, skeletal muscle joints and tendons to the
CNS.
b. Visceral- carry impulses involuntary muscles and glands to CNS.
2. EFFERENT (MOTOR) DIVISION
- transmitted in response to the stimuli the CNS has received from the afferent
division.
SENSORY SYSTEM FUNCTION
Integrating Sensory Impulse
The thalamus integrates all sensory impulses except olfaction. It plays a
role in the conscious awareness of pain and the recognition of variation in temperature
and touch. The thalamus is responsible for the sense of movement and position and
the ability to recognize the size, shape, and quality of objects.
Receiving Sensory Impulses
Sensory impulses enter the spinal cord by way of the posterior root. These
axons convey sensations of heat, cold, and pain and enter the posterior gray column
of the cord, where they make connections with the cells of secondary neurons. Pain
and temperature fibers cross immediately to the opposite side of the cord and course
upward to the thalamus. Fibers carrying sensations of touch, light pressure, and
localization do not connect immediately with the second neuron but ascend to the
cord for a variable distance before entering the gray matter and completing this
connection. The axon of the secondary neuron crosses the cord and proceeds to the
thalamus.
Position and vibratory sensation are produced by stimuli arising muscle,
joints, and bones. These stimuli are conveyed, uncrossed, all the way to the brain
stem by the axon of the primary neuron. In the medulla, synaptic connections are
made with cells of secondary neurons, whose axons cross the opposite side and then
proceed to the thalamus.
SENSORY LOSSES
Destruction of a nerve results in total loss of sensation in its area of
distribution. Transection of the spinal cord yields complete anaesthesia below the
level of injury. Selective destruction or degeneration of the posterior columns of the
spinal cord is responsible for a loss of position and vibratory sense in segments distal
to the lesion, without loss of touch, pain, or temperature perception. A lesion, such as
cysts, in the center of the spinal cord causes dissociation of sensation-loss of pain at
the level of lesion. this occurs because the fibers carrying pain and temperature cross
within the cord immediately on entering; thus, any lesion that divides the cord
longitudinally divides these fibers. Other sensory fibers ascend to the cord for variable
distances, some even to the medulla , before crossing, thereby by-passing the lesion
and avoiding destruction.
DIAGNOSTIC TESTS
Glasgow Coma Scale
Is a numeric expression of cognition, behavior and neurologic function
Provides objective measurements of 3 essential components of neurologic
examination:
Spontaneity of eye opening
Best verbal response
Best motor response
The total of the 3 scores ranges from 3 to 15, with 3 being the most severe
and 15 being normal. A score of 8 or less indicates coma.
The ff. criteria may render the GCS invalid:
The client is based on the clients ability to respond and
communicate.
Eyes are swollen closed.
The client is unable to communicate English.
The client has a hearing loss.
The client is blind.
The client is aphasic.
The client is paralyzed or hemiplegic.
Non-Invasive Test of Structure
X-ray
Definition
A skull x-ray is a series of pictures of the bones of the skull. The
nasal sinuses can also be viewed on a skull X-ray.
Skull x-rays have largely been replaced by CT scans.
X-ray are a form of radiation, like light or radio waves, that are
focused into a beam, much like a flashlight beam.
Spinal X-ray studies
Show fractures, dislocations, compressions, curvature,
erosion, narrowed spinal cord and degenerative process.
A skull x-ray may be done to:
Find fractures
Find a metallic foreign object stuck in the skull
Check the nasal sinuses
Check problems on a babys head, such as an odd shaped
skull.
How to Prepare:
Before the X-ray test, ask the patient if she is pregnant. If a
skull X-ray is absolutely necessary, a lead apron will be placed
over the abdomen to shield the baby from exposure to the X-
rays.
Remove any metal from the body.
Some clients with neurologic disorders require nursing support
through an X-ray study.
Client has a suspected spinal fractures, the neck is
immobilized prior to moving the client to make the X-ray films.
Nurses should document thick or heavy hair.
Risk
A slight risk of damage to cells or tissue from being exposed to
any radiation. However the risk from the X-rays is usually very
low compared with the potential benefits of the test.
Computed Tomography
Definition
Computed tomography scanning, also called CT scan, CAT scan, or
computerized axial tomography, is a diagnostic tool that provides views of
internal body structures using x rays.
In the field of mental health, a CT scan may be used when a patient seeks
medical help for symptoms that could possibly be caused by a brain
tumor.
These symptoms may include headaches, emotional abnormalities, or
intellectual or memory problems. In these cases, a CT scan may be
performed to "rule out" a tumor, so that other tests can be performed in
order to establish an accurate diagnosis.
Description
Computed tomography, is a combination of focused x-ray beams and the
computerized production of an image. Introduced in the early 1970s, this
radiologic procedure has advanced rapidly and is now widely used,
sometimes in the place of standard x rays.
Advantages
CT completely eliminates the superimposition of images of
structures outside the area of interest.
Because of the inherent high-contrast resolution of CT,
differences between tissues that differ in physical density by
less than 1% can be distinguished.
Data from a single CT imaging procedure consisting of either
multiple contiguous or one helical scan can be viewed as
images in the axial, coronal, or sagittal planes, depending on
the diagnostic task.
Patient Preparation
Before a CT Scan, make sure that the client has given informed consent.
Explain that fasting usually is not required but ask whether or not the client
becomes nauseated easily.
Explain that a contrast agent is usually given.
Because the contrast material is iodine- based, ask about any allergies to
iodine or contrast dyes.
If the CT Scan is of the clients head, remove any objects from hair (wigs,
barrettes, earrings, hair pins) before test begins.
Explain the clients role during the scan.
- The client is positioned supine, and the body part to be scanned is
placed into the doughnut shaped ring of the scanner.
- The technician moves the table from a control room to direct
the study to different areas.
- The client can expect to hear mechanical noises coming from the
scanner.
- Emphasize that the client must remain still during the scan.
- If sedation is needed, tell the client to avoid alcohol and caffeine the
day of the scan, avoid eating 2 hrs prior to the scan, and avoid driving 12
hrs after the scan.
After the test, assess the client for reactions to the contrast agent,
hematoma, at the injection site, and the quality of pulses in the limb used
for injection and contrast agent.
The client may resume normal activities unless additional diagnostic tests
are planned.
Tell the client to expect diuresis from the dye. Encourage the intake of
plenty of fluids to flush the dye and prevent nephrotoxic injury.
Risks
Radiation exposure from a CT scan is similar to, though higher than, that
of a conventional x ray.
Although this is a risk to pregnant women, the risk for other adults is
minimal and should produce no effects.
Severe contrast reactions are rare, but they are a risk of many CT
procedures.
Magnetic Resonance Imaging
Is a non-invasive test that uses powerful magnetic fields and radio
frequency pulse to produce the image.
It does not use ionizing radiation such as X-rays.
This test involves altering hydrogen ions; the magnetic field causes the
hydrogen nuclei (protons) to align small magnets in the field.
Advantages
It can detect disorders in white matter pathways caused by
loss of myelin, as in multiple sclerosis.
Can evaluate cerebral infarction within hours of event.
Is the scan of choice for congenital malformations and spinal
cord lesions.
MRI with contrast material delineates blood flow through
cerebral blood vessels in more detail than is possible with CT.
Nursing Interventions
Teach the client and family about the purpose of the test, what
the client will hear and feel during the examination, and the
clients role during the test.
Client should remove all metal-containing objects.
Client may eat and may take prescribed medications before
the examination.
If contrast material is to be used, ask whether the client tends
to become nauseated and adjust the intake of food and fluids.
Non-Invasive Test of Function
Positron Emission Tomography
Definition
Positron emission tomography (PET) is a highly specialized imaging
technique using short-lived radio labeled substances to produce extremely
high resolution images of the body's biological function.
Description
PET is used in conjunction with compounds that closely resemble a
natural substance used by the body, such as a simple sugar (glucose, for
example), labeled with a radioactive atom and injected into the patient.
Cancer cells are highly metabolic, so they are easily seen on the PET
scan.
Three Primary Uses:
Determines the amount of blood flow to specific body tissues.
Revealing how adequately tissues use blood or nutrients, such as oxygen.
Mapping specific receptors, such as medications and neurotransmitters.
Advantages
It can measure the cerebral blood flow, cerebral glucose metabolism, and
oxygen extraction.
It can diagnose stroke, brain tumors and epilepsy and can chart the
progress of Alzheimers disease, Parkinsons disease, head injury,
schizophrenia, and bipolar disorder.
Disadvantage
PET is highly expensive.
Precaution
In some cases, patients may be allergic to the radioactive agents used for
PET.
Preparation
The radiopharmaceutical is given by intravenous injection or inhaled as a
gas a few minutes before the PET procedure.
During the scan, the patient lies comfortably; the only discomfort involved
may be the pinprick of a needle used to inject the radiopharmaceutical.
Nursing Intervention
Educate the client and family about the purpose of the test, what the client
will hear and feel, and the clients role during the test.
Instruct the patient to fast for 4 hours before the scan.
If the client is diabetic, it is preferred that the blood glucose level be below
150 g/dl.
Clients who are agitated may require sedation before the scan.
Single Photon Emission Computed Tomography
Definition
Is a 3 dimensional imaging technique that uses radionuclides and
instruments to detect single photons.
It is a perfusion study that captures a moment cerebral blood flow at
the time of injection of a radionuclide.
Advantages
Is considered experimental and investigational for all other
cardiac indications and non-cardiac indications.
Has a far greater sensitivity for detecting silent ischemia than
ECG.
Clinical studies indicate that SPECT is more accurate at
detecting acute ischemia than CT scan.
Has proved useful in distinguishing recurrent brain tumor from
radiation necrosis.
Disadvantage
It cannot detect hemorrhage in order to rule out use of
thrombolysis.
Nursing Intervention
Premenopausal women are advised to practice effective
contraception before and several days after testing.
Breastfeeding women are instructed to stop nursing for the
period of time recommended by the nuclear medicine dept.
Patients are monitored during and after the procedure for
allergic reactions to the radiopharmaceutical agent.
The patient is asked if he/she is claustrophobic.
Electroencephalography
Definition
EEG is a neurological diagnostic procedure that records the changes
in electrical potentials (brain waves) in the brain.
Purpose
Is an important aid in the diagnosis and management of epilepsy and
other seizure disorders.
Is also useful in monitoring brain wave activity and in the determination of
brain death.
Precautions
It should be administered, monitored, and interpreted only by a specially
trained health professional.
It is important to recognize that diagnosis should not be based on the EEG
alonethe EEG represents an adjunct to the neurological history,
examination, and other specialized studies.
Is an extremely sensitive instrument, and tracings can be greatly
influenced by the actions and the physiologic status of the patient.
It is important that the patient be properly prepared physically and
psychologically in order to obtain an accurate and reliable record.
Medications such as anticonvulsants, tranquilizers, stimulantsincluding
coffee, tea, cola drinksand alcohol should be withheld for at least 2448
hours prior to the test.
Inasmuch as hypoglycemia affects brain wave patterns, the patient is told
not to withhold any meals.
Nursing Interventions
The patient be deprived of sleep on the night before the EEG.
Antiseizure agents, tranquilizers, stimulants and depressants should be
withheld 24 t0 48 hours before EEG.
Coffee, tea, chocolate, and cola drinks are omitted in the meal before the
tests.
end
Patient should be informed that the standard EEG takes 45 to 60 minutes,
12 hours for a sleep EEG.
The patient is assured that the procedure does not cause an electric shock
and that the EEG is a diagnostic test, not a form of treatment.
Sedation is not advisable.
The nurse needs to check the physicians prescription regarding the
administration of antiseizure medication prior to testing.
Transcranial Doppler
It is a noninvasive technique that is helpful in assessing vasospasm,
altered cerebral blood flow found in occlusive vascular disease or stroke,
and other cerebral pathology.
It also uses the same noninvasive techniques as carotid flow studies
except that it records the blood flow velocities of the basal artery can be
measured through thin areas of the temporal and occipital bones of the
skull.
A hand-held Doppler probe emits a pulsed beam; the signal is reflected
by the moving blood cells within the blood vessels.
end
Nursing Intervention
The nurse should describe first the procedure to the patient.
Inform the patient that this is a noninvasive test, that a hand-held
transducer will be placed over the neck and the orbits of the eyes, and that
some type of water-soluble jelly is used on the transducer.
Invasive Test of Function
Electromyography
Is obtained by inserting needle electrodes into the skeletal muscles.
The electrical potentials are shown on an oscilloscope and is amplified.
Advantages
An EMG is useful in determining the presence of neuromuscular disorders
and myopathies.
It helps distinguish weakness due to neuropathy from weakness resulting
from other causes.
end
Nursing Interventions
Explain the procedure.
Warn the patient to expect a sensation similar to that of an intramuscular
injection.
Lumbar Puncture
The insertion of a hollow needle beneath the arachnoid membrane of the
spinal cord in the lumbar region to withdraw cerebrospinal fluid for
diagnostic purposes or to administer medication.
Advantages:
to obtain CSF for examination
to measure and reduce CSF pressure
to determine the presence or absence of blood in the CSF
to detect subarachnoid block
to administer antibiotics intrathecally (into the spinal canal) in
certain cases of infection.
Disadvantage
A Lumbar puncture may be risky in the presence of an
intracranial mass lesion because intracranial pressure is
decreased by the removal of CSF, and the brain may
herniated downward through the tentorium and the foramen
magnum.
During the Procedure
A lumbar puncture procedure may be performed on an outpatient basis or
as part of your stay in a hospital. Procedures may vary depending on your condition
and your physician's practices. Generally, a lumbar puncture follows this process:
1. Explain the procedure to the patient.
2. Tell the patient to remove any clothing, jewelry, or other objects
that may interfere with the procedure.
2. Provide the gown.
3. Remind the patient to empty the bladder prior to the start of
the procedure.
end
The patient may experience discomfort during a lumbar puncture. The
physician will use all possible comfort measures and complete the
procedure as quickly as possible to minimize any discomfort or pain.
Myelography
Is an x-ray of the subarachnoid space taken after the injection of a
contrast agent into the spinal subarachnoid space through a lumbar
puncture.
It helps to evaluate the spinal cord and nerve roots for suspected
compression. Pressure on these delicate structures causes pain or other
symptoms.
DISADVANTAGES
Headache is a common complication of myelography.
Rare complications of myelography include injury to the nerve roots from
the needle or from bleeding into the spaces around the roots. Inflammation
of the delicate covering of the spinal cord, called arachnoiditis, or
infections, can also occur.
Seizures are another very uncommon complication reported after
myelography
CLIENT PREPARATION
Patients should be well-hydrated at the time they are undergoing a
myelogram.
All food and fluid intake should be stopped approximately four hours
before the procedure.
Certain medications may need to be stopped for one to two days before
myelography is performed.
Patients who smoke may be asked to stop the day before the test.
Nursing Interventions
The nurse clarifies the explanation given by the physician and answers
questions.
The patient is informed about what to expect during the procedure and
should be aware that changes in position may be made during the
procedure.
The meal that normally would be eaten before the procedure is omitted.
end
After myelography, the patient lies in bed with the head of the bed
elevated 30 to 45 degrees.
The patient is encouraged to drink liberal amounts of fluid for rehydration
and replacement of CSF and to decrease the incidence of post-lumbar
puncture headache.
The blood pressure, pulse, respiratory rate, and temperature are
monitored, as well as the patients ability to void.
Cerebral Angiography
Definition
An angiography is an x-ray of the arteries. The arteries are not normally
seen in an x-ray, so a special material, called contrast dye, is injected into
one or more arteries to make them visible.
It is frequently performed before craniotomy to assess the patency and
adequacy of the cerebral circulation and to determine the site, size, and
nature of the pathologic processes.
Most cerebral angiograms are performed by threading a catheter through
the femoral artery in the groin and up to the desired vessel.
Alternatively, direct puncture of the carotid or vertebral artery or retrograde
injection of a contrast agent into the brachial artery may be performed.
Advantages
Can detect aneurism, AVM, major vessel displacement
vascular occlusion or thrombi.
Helpful in assessing the patency and adequacy of cerebral
circulation before conducting craniotomy.
Disadvantage
Potential complications includes temporary or permanent neurologic
deficit, anaphylaxis, bleeding or hematoma at the IV site, and impaired
circulation in the extremity distal to the injection site.
Preprocedure
Obtain an informed consent.
Educate the client about the purpose of the test, what the client will
experience, and the clients role in the procedure.
Before the test, the client may not take anything by mouth for 4 to 6 hours
but should be kept well hydrated. IV fluids may be prescribed. Encourage
hydration 2 days before the test.
After the groin is shaved and prepared, local anesthetic is administered.
Mark the peripheral pulses.
Document the neurologic status of the client.
The clients should remove any metal items from the head, such as
barrettes and earrings.
Report allergies to iodine. Often patients with allergy to iodine also have
allergies to radiopaque contrast media that may cause severe reaction.
Tell the patient to expect some discomfort when the catheter is inserted.
Additionally, the sensation of a warm, flushed feeling and metallic taste
should be expected when the dye is injected.
Caution the patient to lie still during the procedure.
Postprocedure
Monitor neurologic status and vital signs frequently until stable.
Maintain bed rest 12 24 hours as prescribed.
The extremity to which the contrast medium was injected is
kept straight and immobilized for about 8 hours.
Apply sandbags and a pressure dressings to the injection site
as prescribed.
Nursing Interventions
The patient should be well hydrated, and clear liquids are usually
permitted up to the time of a regular arteriogram or DSA.
Before going to the x-ray department, the patient is instructed to void.
The patient is instructed to remain immobile during the angiogram process
and is told to expect a brief feeling of warmth in the face, behind the eyes,
or in the jaw, teeth, tongue, and lips, and a metallic taste when the
contrast agent is injected.
Neurologic Disorders
Cerebrovascular Accident
A focal neurological deficit due to a local disturbance in blood supply to the
brain ( WHO )
Its onset is usually abrupt but may extend over a few hours or longer.
Pathophysiology
Interruption of the blood supply to the brain deprives it of oxygen and
nutrients resulting in the death of brain tissues.
Risks Factors for Stroke
Medical Conditions
Hypertension (30% to 40% risk reduction with treatment): goal BP is lower
than 140/90; if renal insufficiency or heart failure, less than 130/85; if
diabetic, less than 130/80
Cardiac disorderscongenital heart disease, valvular conditions,
endocarditis
Atrial fibrillation (risk reduction is 68% with oral anticoagulant therapy; 21%
with aspirin therapy for nonvalvular causes)
Diabetes mellitus (44% risk reduction in hypertensive diabetics with
controlled BP)
Hyperlipidemia (20% to 30% risk reduction with those with known coronary
heart disease [CHD] on statin therapy): goal LDL is less than 160 mg/dL if
one or no risk factor; less than 130 if two or fewer risk factors or 10-year
CHD risk is less than 20%; less than 100 if two or fewer risk factors and
10-year CHD risk greater than 20%
Carotid stenosis
Prior history of TIA or stroke
Elevated homocysteine level in blood
Behaviors
Cigarette smoking (50% risk reduction in 1 year; return to baseline in 5
years)
Alcohol abuse
Physical inactivity
Cocaine use (hemorrhagic stroke)
Nonmodifiable factors
Increasing age - risk doubles for each decade over age 50
Gender - men are at greater risk than women
Heredity - increased risk with family history of stroke
Ethnic background - Blacks and Hispanics at higher risk than Whites
Types of Strokes
Ischemic ( Thrombotic, Embolic )
Partial or complete occlusion of a cerebral blood flow to an area of the
brain
Hemorrhagic
Leakage of blood from a blood vessel and hemorrhage into brain tissue,
causing edema, compression of brain tissue, and spasm of adjacent blood vessels.
Ischemic Stroke: Causes
1. Cerebral thrombosis atheroma where a plaque of hard fatty
degenerative nature forms on the inner wall of the artery, impedes blood
flow and clot forms
2. Cerebral Embolism Pieces of clot breaking off, moves to the
bloodstream and lodge in a vessel blocking the passage of blood.
3. Cerebral ischemia loss of adequate blood supply due to narrowing of
either the carotid or vertebral artery.
Hemorrhagic Stroke ( Types )
1. Epidural
2. Subdural
3. Subarachnoid
4. Intracerebral
Hemorrhagic stroke ( Causes )
Ruptured or leaking aneurysms
Arteriovenous malformations
Use of anticoagulants
Hypertension
Clinical Findings
Internal Carotid
Contralateral hemiparesis
Dysphasia with dominant side involvement
Blindness
Agnosia(inability to recognize)
Hemianopia
Cranial nerve deficits
Contralateral anosognosia(unaware of disability)
Middle cerrebral artery
Contralateral arm and leg weakness or paralysis
Homonymous hemianopia
Eye deviation to the opposite side
Dysphagia or aphasia on dominant side
Contralateral sensory impairment
Apraxia with non-dominant involvement (non-purposeful movement)
Clinical findings
Anterior cerebral artery
Contralateral paralysis leg, foot and arm
Bladder incontinence
Sensory deficit
Akinetic mutism( not moving and speaking )
Eye deviation towards affected side
Gait impairment
Mood disturbance
Vertebral-basilar system
Variations in LOC
Hemianopia
Possible quadriplegia
Eye muscle paralysis
Nystagmus
Diplopia
Dysarthria(poor articulation)
Ataxia( incoordination )
Vertigo
Diagnostic Tests
History and examination
CT scan
Arteriogram
Medical Management
Close observation and monitoring of hemodynamic parameters
Management of increased ICP
Anticoagulant therapy heparin, thrombolytics
Recombinant tissue plasminogen activator -Alteplase therapy
Nursing Management
Care during the acute phase ( first 24 to 48 hours )
Maintain patent airway:
O2 therapy started soon
Positioning to facilitate drainage
Suctioning
Elevate head of bed 30 degrees
Chest physiotherapy
VS monitoring
Respiratory pattern
Decreased PR indicates increased icp
Increased temperature
LOC
Pupil response
On Mannitol drip
I and O monitoring
Electrolyte balance
Personal hygiene
Passive ROM
Post Acute Care
Maintain clear airway to prevent hypoxia
O2 therapy humidified
Tracheostomy care
Deep breathing
Chest physiotherapy
Preventing Falls and Other Injuries
Maintain bed rest during acute phase (24 to 48 hours after onset of stroke)
with head of bed slightly elevated and side rails in place.
Administer oxygen as ordered during acute phase to maximize cerebral
oxygenation.
Frequently assess respiratory status, vital signs, heart rate and rhythm,
and urine output to maintain and support vital functions.
When patient becomes more alert after acute phase, maintain frequent
vigilance and interactions aimed at orienting, assessing, and meeting the
needs of the patient.
Try to allay confusion and agitation with calm reassurance and presence.
Assess patient for risk for fall status.
Surgical Management
Craniotomy - surgical opening of the skull to gain access to intracranial
structures to remove a tumor, relieve increased intracranial pressure
(ICP), evacuate a blood clot, stop hemorrhage, or remove epileptogenic
tissue. Craniotomy may be performed by means of burr holes (made with
a drill or hand tools) or by making a bony flap.
Craniectomy is excision of a portion of the skull.
Cranioplasty is repair of a cranial defect by means of a plastic or metal
plate.
Preoperative Management
Diagnostic findings, surgical procedure, and expectations are reviewed
with the patient.
Presurgical shampoo with an antimicrobial agent may be ordered. Shave
and prep are performed in the operating room.
Depending on primary diagnosis, corticosteroids may be ordered
preoperatively to reduce cerebral edema.
Depending on the type and location of lesion, anticonvulsants may be
ordered to reduce risk of seizures.
The patient is prepared for the use of intraoperative antibiotics to reduce
risk of infection, and urinary catheterization to assess urinary volume
during operative period.
If cerebral edema develops, intraoperative or postoperative osmotic
diuretic (mannitol) or corticosteroids may be ordered for its treatment.
Neurologic assessment is performed to evaluate and record the patient's
neurologic baseline and vital signs for postoperative comparison.
Family and patient are made aware of the immediate postoperative care
and where the physician will contact the family after surgery.
Supportive care is given as needed for neurologic deficits.
Postoperative Management
Respiratory status is assessed by monitoring rate, depth, and pattern of
respirations. A patent airway is maintained.
Vital signs and neurologic status are monitored, using GCS; findings are
documented.
Arterial and central venous pressure (CVP) are monitored, possibly with a
pulmonary Swan-Ganz catheter for accurate assessment of hemodynamic
status.
Pharmacologic agents may be prescribed to control increased ICP.
Incisional and headache pain may be controlled with mild analgesic
(codeine and acetaminophen) or low dose opioids (morphine sulfate or
fentanyl/Duragesic), as prescribed. Monitor response to medications.
Position head of bed at 15 to 30 degrees, or per clinical status of patient,
to promote venous drainage. Determining appropriate position of head of
bed is patient-dependent and should be adjusted based on observed
changes in the patient's clinical response and ICP to positioning. A
decrease in CPP is observed with raising the head of the bed to lower
ICP.
Turn side-to-side every 2 hours; positioning restrictions will be ordered by
the physician.
CT scan of the brain is performed if patient's status deteriorates.
Oral fluids are provided after swallow reflex and bowel sounds have
returned. Intake and output are monitored. Speech therapy may be
ordered for bedside swallow study or radiographic swallow study.
Signs of infection are monitored by checking craniotomy site, ventricular
drainage, nuchal rigidity, or presence of CSF (fluid collection at surgical
site).
Periorbital edema is controlled by such measures as elevation of head of
bed and cold compresses. Removal of surgical dressing and increase in
activity will assist in the resolution of periorbital edema.
Autoimmune Disorders
Multiple Sclerosis
A demyelinating disease disease that results in the destruction of the CNS
myelin.
Etiology:
Link between prevalence of MS and geographic location.
Northern Europe, Great Britain, So. Australia, New Zealand
20-40 years old
Common in women
Whites / Caucasian
Cause
Unknown
Autoimmune: associated with the dysfunctional T lymphocytes.
Triggered by viral infection.
Clinical Manifestation
Prediliction to optic nerve, preventricular white matter, brainstem,
cerebellum and spinal cord white matter.
Cranial nerve dysfunction blurred central vision, faded colors, blind
spots, diplopia, dysphagia, facial weakness, numbness and pain.
Motor dysfunction weakness, paralysis, spasticity, abnormal gait
Sensory dysfunction paresthesias, Lhermitts sign ( electric shock-like
sensation radiating down the spine.
Cerebellar function dysarthria, tremor, incoordination, atax ia, vertigo
Bowel and bladder dysfunction fecal urgency, constipation, urinary
frequency, hesitancy, nocturia
Cognitive dysfunction decreased short term memory, short attention
span
Diagnostic Test
CSF analysis increased protein, lymphocytes and IgG
Evoked potentials- prolonged impulse conduction
MRI demostrates white matter lesions
Therapeutic Management
Pharmacologic Therapy
Corticosteroid
Interferon beta and glatiramer acetate
Diazepam, stool softeners
Nursing Care
Avoid precipitation of exacerbation
Avoid fatigue, stress, infection, overheating, chilling.
Establish regular program of exercise with rests.
Provide balance diet
Physical and speech therapy
Promote safety
Promote bladder and bowel control
Provide education and emotional support
Myasthenia Gravis
A disorder of transmission at the neuromuscular juncion that affects
communication between the motor neuron and the innervated muscle cell.
Etiology:
More common in women than in men
Heredofamilial disease
20-30 years old
Causes
Autoimmune disease caused by antibody-mediated loss of acetylcholine
receptors in neuromuscular junction.
Thymoma
Diagnostic Tests
Tensilon Test anti-cholinesterase test ( edrophonium )
Administered IV-decreases breakdown of ACh in the
neuromuscular junction.
(+) MG- improvement in muscle strength
(-) MG no improvement or even deterioration
CT on thymus
Therapeutic Management
Drug Therapy
Anticholinesterase drugs pyridostigmine, neostigmine
Corticosteroids
Immunosuppresant drugs azathioprine
Plasmapheresis
Thymectomy
Complications
Myasthenia Crisis experience of a sudden exacerbation of symptoms
and weakness.
Occurs when muscle weakness becomes severe enough to
compromise ventilation
Occurs during period of infection, stress and pregnancy
Medications increasing incidence:
Quinidine, aminoglycosides, beta adrenergic
receptor blockers, calcium channel blockers,
magnesium sulfate, citrate
Weakness, dyspnea, dysphagia, restlessness,
difficulty speaking
Cholinergic Crisis
Cholinergic paralysis with sustained depolarization of motor
end plates due to overmedication of Anti acetylcholinesterase
Fasciculation, abdominal cramping, diarrhea, vomiting,
nausea, salivation
Nursing Care
Monitor patient to avoid progression to complications.
Administer medications as ordered.
Plan short periods of activity
Encourage normal ADL and divertional activities.
Provide emotional and educational support.
Be prepared with atropine.
Guillain-Barre Syndrome
An acquired inflammatory disease that results in demyelination of the
peripheral nerves with relative sparing of the axon.
Progressive ascending paralysis that is usually reversible.
Etiology:
Altered immune response directed against a component of
myelin in the peripheral nerve.
Viral infection
GI tract infection of camylobacter jejuni
Clinical Manifestation
Muscle weakness that develops in a matter of hours to 10 days.
Distal lower extremities are affected first
Patient may fall, develop footdrop and then be unable t walk.
Paresthesias
Respiratory muscle paralysis usually the last symptom.
Diagnostic Tests
CSF analysis increased protein level
EEG slowing in motor and sensory conduction velocity.
Therapeutic Management
Plasma exchange
IV Ig
Nursing care:
Monitor for respiratory paralysis
Prevent complication of immobility.
Nutritional support
AMYOTROPHIC LATERAL SCLEROSIS
Degeneration of upper motor neurons (nerves leading from the brain to
medulla or spinal cord) and lower motor neurons (nerves leading from the
spinal cord to the muscles of the body).
Results in progressive loss of voluntary muscle contraction and functional
capacity, involving the legs, feet, arms and hands, and those that control
swallowing and breathing.
Cause is unknown. Usually affects men in the fifth or sixth decade of life.
Clinical Manifestations
Progressive weakness and wasting of muscles of arms, trunk, and legs
Fasciculations and signs of spasticity
Progressive difficulty swallowing (drooling, regurgitation of liquids through
nose), speaking (nasal and unintelligible), and, ultimately, breathing
Cranial nerve deficits (bulbar symptoms) are present in 20% of cases
(prevalence increases with age), along with dysarthria, voice deterioration,
and dysphagia (Patients with bulbar presentation have poorer prognosis;
these symptoms also have a profound impact on quality of life due to
nutritional risk factors, aspiration, and respiratory complications.)
Diagnostic Tests
Electromyography to evaluate denervation and muscle atrophy
Nerve conduction study to evaluate nerve pathways
Pulmonary function tests to evaluate respiratory function
Barium swallow to evaluate ability to achieve various phases of swallow
MRI, CT to rule out other disorders
Laboratory tests: creatine kinase, heavy metal screen, thyroid function
tests, CSF evaluation to rule out other causes of muscle weakness
Therapeutic Management
There is no cure for ALS; nor is there a proven therapy that will prevent or
reverse the course of the disorder.
Riluzole (Rilutek), the first drug that has been shown to prolong the
survival of ALS patients, was recently approved by the FDA, but its effects
are limited.
Most treatment is palliative and symptomatic.
Baclofen (Lioresal) to control spasticity.
Diazepam (Valium) to control fasciculations.
Antidepressants, sleep medications.
Feeding gastrostomy.
Mechanical ventilation eventually becomes necessary.
Monitor vital capacity frequently. Document pattern, and report any
decrease below patient's baseline.
Position patient upright, suction upper airway, and perform chest physical
therapy to enhance respiratory function.
Encourage use of incentive spirometer to exercise respiratory muscles.
Assess for signs of hypoxia, such as tachypnea, hypopnea, restlessness,
poor sleep, and excessive fatigue.
Establish the wishes of the patient in terms of life-support measures;
obtain copy of advance directive for chart, if applicab
Provide suctioning and routine care of a patient with artificial airway and
mechanical ventilation.
Degenerative Disorders
Alzheimers Disease
Characterized by cortical atrophy and loss of neurons, particularly in the
parietal and frontal lobes.
Etiology:
Genetics autosomal dominant pattern
Identified in familial cases on chromosome 21 which includes
beta amyloid precursor protein.
Age: rarely develops before age 40.
Diagnostic Test
No biochemical markers or tests.
Confirmed only by microscopic examination of tissue obtained from
biopsy.
Therapeutic Management
Primarily symptomatic and supportive
Drug therapy
For mood and sleep disorders
constipation
Nursing Care
Counselling, planning and education of patient and family.
Diet and exercise
Avoid fatigue, overstimulation
Enhance memory by using calendars, clocks posted schedule
and notebooks
Changes should be attempted slowly.
Meals should not be forced and served in calm surroundings.
Ensure safe environment
Care for the family and caregivers
Parkinsons Disease
Parkinson's disease is a chronic, progressive neurologic disease affecting
the brain centers responsible for control and regulation of movement.
It is characterized by tremor, bradykinesia, rigidity, and postural
abnormalities.
It is the second most common neurodegenerative disease.
A deficiency of dopamine, due to degenerative changes in the substantia
nigra of the brain, is thought to be responsible for the symptoms of
Parkinson's disease.
Etiology may be related to a virus; genetic susceptibility; toxicity from
pesticides, herbicides, methyl-phenyl-tetrahydropyridine, or welding fumes;
repeated head injuries, or other unknown cause.
Clinical Manifestations
Bradykinesia (slowness of movement), loss of spontaneous movement
and delay in initiating movements
Resting (pill-rolling) tremor of 4 to 5 Hz. The tremor may be worse
on one side of the body affecting the limbs and sometimes involves the
head, neck, face, and jaw.
Rigidity in performance of all movements. Rigidity is always present but
increases during movement. May lead to sensations of pain, especially in
the arms and shoulders.
Micrographia (change in handwriting, with the script becoming smaller)
Problems with speech, breathing, swallowing, and sexual function.
Autonomic disorders sleeplessness, salivation, sweating, orthostatic
hypotension, dizziness.
Depression, dementia.
Masklike facies secondary to rigidity.
Gait difficulties characterized by a decreased or nonexistent arm swing;
short, shuffling steps (festination); difficulty in negotiating turns; and
sudden freezing spells (inability to take the next step).
Poor balance when moving abruptly or suddenly changing body position.
May lead to falls.
Verbal fluency may be impaired.
Finger tapping responses are slowed.
Diagnostic tests
Observation of clinical symptoms; may do imaging studies to rule out other
disorders.
Physical examination of upper extremity elbow flexion/extension reveals
rigidity on extension.
Sensorimotor assessment of grip reveals abnormally high grip forces and
longer than normal to complete object lift, particularly with lighter loads.
Favorable response to a single dose of levodopa helps confirm the
diagnosis.
Therapeutic Management
Pharmacologic
Anticholinergics, including trihexyphenidyl (Artane), benztropine
(Cogentin), NS procyclidine (Kemadrin) to reduce transmission of
cholinergic pathways, which are thought to be overactive when dopamine
is deficient. These medications are most effective in controlling tremor, but
are known to cause confusion and hallucinations.
Amantadine (Symmetrel), originally an antiflu medication, blocks the
reuptake of dopamine or increases the release of dopamine by neurons in
the brain, thereby increasing the supply of dopamine in the synapses.
Widely used as an early monotherapy, its effect may be augmented by
drug-free days.
Levodopa, a dopamine precursor, combined with carbidopa, a
decarboxylase inhibitor, to inhibit destruction of L-dopa in the bloodstream,
making more available to the brain.
The combination of levodopa-carbidopa (Sinemet) usually is used. The
addition of carbidopa prevents levodopa from being metabolized in the
gut, liver, and other tissues, and allows more to get to the brain.
Bromocriptine (Parlodel), pergolide (Permax), pramipexole (Mirapex), and
ropinirole (Requip) are dopaminergic agonists that activate dopamine
receptors in the brain.
Use of the monoamine oxidase inhibitor selegiline or deprenyl (Eldepryl)
boosts the effect of Sinemet when levodopa becomes less effective.
Tolcapone (Tasmar) and entacapone (Comtan) are in a new drug class
(COMT inhibitors) for adjunct treatment.
They prolong the duration of symptom relief by blocking the action of an
enzyme that breaks down levodopa before it reaches the brain. Must be
taken with levodopa.
SPINAL CORD INJURIES
is a traumatic injury to the spinal cord that may vary from a mild cord
concussion with transient numbness to immediate and complete
tetraplegia.
most common sites are the cervical areas C5, C6, and C7, and the junction
of the thoracic and lumbar vertebrae, T12 and L1
Mechanism are same with H.I. (causes compression, tension, and
shearing)
Classification
1.) COMPLETE
2.) INCOMPLETE
COMPLETE
ALL MOTOR, SENSORY, AND VASOMOTOR FUNCTIONS ARE
ABSENT BEVOLUNTARY LOW THE LEVEL OF INJURY
LOSS OF REFLEX FUNCTION IN ISOLATED SEGMENT OF THE
CORD.
INCOMPLETE
SOME DEGREE OF EITHER VOLUNTARY MOTOR, SENSORY, AND
VASOMOTOR FUNCTIONS ARE ABSENT BELOW LEVEL OF INJURY
CONDITION ASSOCIATED WITH SCI
1. SPINAL SHOCK
- A CONDITION IN WHICH THERE IS AN IMMEDIATE, COMPLETE LOSS OF
ALL REFLEXES , MOTOR, SENSORY AND AUTONOMIC ACTIVITY BELOW
LEVEL OF INJURY
- DANGER IS HYPOTENSION AND BRADYCARDIA
- last few days or weeks after injury- implication??
- Signs of recovery: - what happens after spinal shock??? neurologic level
- Return of anal reflex
- Flaccid paralysis becoming spastic
- Gradual return of autonomic function
- Reflex bowel and bladder contraction
2. AUTONOMIC DYSREFLEXIA (HYPERREFLEXIA)
CHARACTERIZED BY EXCESSIVE AUTONOMIC RESPONSES TO
STIMULI
COMMON WITH C. & HIGH T. SPINAL CORD LESION --- when will this
occur?
STIMULI : DISTENDED BLADDER
Manifestation of hyperreflexia
SEVERE HPN (300/160 mmHg)
Rupture of blood vessel
Severe throbbing/ pounding headache
Profuse sweating above the level of the lesion
Flushing of skin above level of lesion
Nasal stuffiness, pilomotor spasm
Blurred vision, nausea, bradycardia
Management of Hyperreflexia
Monitor BP
Elevate HOB to a sitting position
Notify AP
Check possible sources of irritation (fecal impaction) topical anes. 10
15 mins.
Relieve urinary obstruction (FBC)
IF BP doesnt subside
HYDRALAZINE (Apresoline)
Nsg. Resp.: Observe AEG 3 4 hrs
SURGERY (chordotomy or poudendal nerve resection)
3. SPINAL AUTOMATISM
Spinal reflex activities occurring automatically after S.C. severance
BP and Temp fall markedly and respond poorly to reflex stimuli
4. SPASTICITY and MUSCLE SPASM
INCREASED TONE OR CONTRACTION OF MUSCLE
DEVELPS 2 WEEKS SEVERAL MONTHS
Flaccidity ----- SPASM
May become a source of DISAPPOINTMENT
This is only a REFLEX RESPONSE
DIAGNOSTICS
Detailed Neuro. Exam DERMATOME & PLEXUSES
X-Ray, CT SCAN, MRI
ECG
MEDICAL MGt
Prevent further injury
Keep patient in extended position
Position: flat, neck immobilized with a neck collar
Intubation and mechanical intubation
Maintenance of vertebral alignment: Stryker turning frame,
Crutchfield tongs, Halo brace
DVT prophylaxis
Diet: Low-calcium, high protein
IV therapy
GI decompression
Activity: Bed rest, passive ROM exercises
Laboratories
Indwelling catheter
AEDs
High dose corticosteroids (methylprednisolone)
NURSING INTERVENTION
Promote adequate breathing
Improve mobility
Dont turn without turning frame
Promote adaptation to disturbed sensory perception
Maintain skin integrity
Promote urinary elimination
Improve bowel function
Provide comfort measure
Monitor and manage potential complication
Promote home and community based care
INCOMPLETE SCI
CENTRAL CORD SYNDROME
Motor deficit more marked in the upper extremities compared
to lower extremities
Sensory loss more pronounced in the upper extremities
Bowel/ bladder dysfunction is variable or function preserved
Cause:
Injury or edema to central cord
ANTERIOR CORD SYNDROME
Loss of pain, temperature, and motor function is noted below level of
lesion
Light touch, position and vibration intact
Cause:
Acute disk herniation or hyperflexion; injury to
anterior spinal artery , which supplies the anterior
2/3 of SC
BROWN-SEQUARD SYNDROME (LATERAL CORD SYNDROME)
IPSILATERAL PARALYSIS OR PARESIS IS NOTED
IPSILATERAL LOSS OF TOUCH, PRESSURE, & VIBRATION
CONTRALATERAL LOSS OF PAIN & TEMPERATURE
CAUSE:
TRANSVERSE HEMISECTION OF THE CORD;
USUALLY BY KNIFE OR MISSILE INJURY,
UNILATERAL ARTICULAR PROCESS, ACUTE
RUPTURED DISK
Trigeminal Neuralgia Tic douloureux
Is sudden, excruciating, recurrent paroxysm of sharp, stabbing pains in the
sensory distribution of one or more of the three branches of the 5
th
cranial
nerve
Characterized by presence of TRIGGER ZONE
Avoidance of certain acts are important clue for trigeminal
Affects more women than men; middle or late life ***
Unknown cause
Trauma, past infections, vascular compression, neoplasm,
and MS
Management
CARBAMAZEPINE (Tegretol)
Drug of choice - reduce transmission of impulse
Taken with meals - Mon. serum for toxicity
(3- 14mcg/ml)
GABAPENTIN (Neurontin) and Baclofen (Lioresal)
Similar to GABA - derivative of GABA (SC
axn)
PHENYTOIN (Dilantin) ***
If pain is uncontrolled - 10 20 mcg/ml
ALCOHOL OR PHENOL INJECTION
Temporary pain relief for months (nerve regeneration)
Given before retrogasserian rhizotomy
Surgical Management
Microvascular Decompression (J.P.)
Application of non-absorbent sponge (plastic device) in
between blood vessel and T. nerve
Pos.: Relieves pain & preserves normal sensation
Neg.: Craniotomy
Percutaneous Radiofrequency Trigeminal Gangliolysis
Thermal destruction of the gasserian ganglion (partial
destruction)
Patient awake during the procedure
Surgical procedure of choice
Neg.: Loss of sensation in the affected branch
Pos.: Touch and proprioceptive fxn is intact
Trigeminal Rhizotomy
Nursing Management
Teach what to expect after surgical procedure
1
st
Branch loss of corneal reflex (proper care)
2
nd
& 3
rd
Branch loss of sensation
Teach to avoid hot and food or fluids
Regular check-up with dentist
Take food on the unaffected side
Prevent complication of medication
AEDs causes BM suppression, regular monitoring of blood
count is imperative before and during TX
Teach patient early indication of potential blood problem
Preventing pain
Identify aggravating factor
Perform hygiene task during pain free moments
Cotton pads and room temperature water
Mouthwash instead of brushing
Soft Foods and fluids at room temperature
Chew on unaffected side
Address anxiety, depression and insomnia ***
BELLS PALSY
Most common type of peripheral facial paralysis
Unilateral paralysis of the facial muscle without evidence of pathologic
cause
Inflammation of the 7
th
cranial nerve
People of increasing age and at 3
rd
trimester preg. Is at high risk
Possible etio are: Vascular ischemia, viral disease, autoimmune disease
Manifestation
Bells phenomena
Drooping of the mouth
Flattening of the nasolabial folds
Widening of palpebral fissure
Slight lag in closing the eyes
Increased lacrimation
Speech difficulties
Painful sensation in the face, behind the ear and in the eyes ****
Management
Analgesics ***
Corticosteroid therapy (prednisone)
Physiotherapy
HEAT APPLICATION
GENTLE MASSAGE
ELECTRICAL STIMULATION**
Corneal protection
Surgical Exploration
Tumor is suspected
Decompression of the facial nerve
Surgical treatment of paralyzed face ( spinal accessory XI or
hypoglossal XII)
Nursing Management
Reassure patient that NO STROKE has occurred (3 5 weeks)
Protect involved eye
ARTIFICIAL TEARS
EYE PATCH
EYE OINTMENT AT BEDTIME
TEACH PATIENT TO MANUALLY CLOSE PARALYZED
EYELID
USE OF WRAP-AROUND SUNGLASSES OR GOGGLES
(MAINTAIN MOISTURE)
MENIERS DISEASE
Relatively common, chronic disorder in the inner ear
Characterized by recurring episodes of vertigo, associated with tinnitus
and deafness
Exact cause is not clear but is associated with degeneration of tiny
cochlear hair cells
Assessment may be done through caloric testing and
electronystagmography (ENG)
Manifestation
Severe rotational type of vertigo
Nausea and vomiting
Diaphoresis
Tinnitus
Hearing loss
Feeling of pressure in the ear
Brief loss of consciousness and nystagmus may occur
Intervention
BED REST most effective during acute episodes
SQ atropine sulfate as soon as possible
Diazepam IV slowly
Advise AEG not to read and avoid bright light
Long-term med interv.:
Antihistamine (meclizine (Antivert))
Suppress vestibular system
Diuretic therapy (acetazolamide (diamox) and chlorothiazide
(diuril))
Dietary management
Low salt & rule out allergies
Relieves pressure in the endolymphatic
PERIPHERAL NERVE INJURY
CARPAL TUNNEL SYNDROME
Progressive medical condition in which the median nerve is
compressed in the carpal tunnel
ENTRAPMENT NEUROPATHY
Etiology: IDIOPATHIC
Risk Factor: 1. Congenital Predisposition
2. Disease or injury
3. Arm use and environmental factor
Manifestation:
- Paresthesia usually appears at sleep or at night
- Muscle weakness
- Increasing pain
- Increase sweating
- Muscle wasting and weakness
Diagnosis: 1. History
2. P.E.
3. Diagnostic Procedure
a. Phulins Maneuver
b. Electrodiagnostic test
Treatment: 1. Aspirin, ibuprofen, or napronex
2. Steroid injection
3. Oral prednisone
4. Vit. B 12
5. Surgery
Indication:
- Severe & long duration
- Muscle atrophy
- Progressive sensory loss in the finger
Procedure: TRANSVERSE CARPAL LIGAMENT
TRANSECTION
Nursing Intervention:
1. Rest hands and wrist for 2 weeks
2. Splinting of wrist and hands mild and
short duration
3. Ice packs
4. Health education for prevention
NEURAL DISTURBANCE
HEAD INJURY
2/3 OF DEATH FROM VEHICULAR ACCIDENT
PROMPT INTERVENTION MINIMIZES DEVLP OF 2
O
PROBLEMS
TREATMENT OF HYPOXIA & ACID-BASE IMBALANCE DECREASES
MORTALITY
INTRACRANIAL MASS LESIONS MAY FOLLOW INITIAL TRAUMA
SEVERE CEREBRAL SWELLING OFTEN FOLLOW BRAIN INJURY
AEGS WITH H.I. OFTEN HAVE OTHER MAJOR INJURIES
NECK FRACTURES ARE TO BE EXPECTED
MECHANISM OF HEAD INJURY
CAUSED BY SUDDEN FORCE
ACCELERATION
DECELERATION
DERFORMATION
ROTATIONAL FORCE
CATEGORIES OF HEAD TRAUMA
BLUNT TRAUMA
Complex, with several head structures involved
PENETRATING
Depends on the velocity of object (low velocity and high
velocity)
Infection (complication)
COUP INJURY
COUNTRECOUP INJURY
NOTE: H.I. MAY ALSO BE CLASSIFIED AS PRIMARY AND SECONDARY
A.)PRIMARY HEAD INJURY
SCALP INJURIES
SKULL INJURIES
BRAIN INJURIES
FOCAL INJURY
DIFFUSE INJURY
SCALP INJURY
SUPERFICIAL
ALONE IS MINOR
COVER AND APPLY PRESSURE --- EXCEPT???
SKULL INJURIES
OFTEN WITH BRAIN INJURY
CAUSES ABRASION AND LACERATION OF BRAIN TISSUE
3 TYPES:
LINEAR no Tx needed
DEPRESSED surgery
BASILAR base of frontal and temporal lobes,
diagnosis???
CLINICAL SIGNS
INTRACRANIAL CSF FISTULA
CSF OR OTHER DRAINAGE FROM EAR OR NOSE
VARIOUS CRANIAL NERVE INJURIES
BLOOD BEHIND THE EARDRUM
PERIORBITAL ECCHYMOSIS
BATTLES SIGN
BRUSIE OVER THE MASTOID
Mgt: DIAMOX, LUMBAR DRAIN, CRANIECTOMY,
CRANIOPLASTY
BRAIN INJURY
FOCAL INJURY
SMALL HEMORRHAGES OF THE CORTICAL SURFACES
MAY CAUSE SECONDARY BRAIN DAMAGE
DIFFUSE INJURY
TEMPORARY LOSS OF NEUROLOGIC FUNCTION
WITHOUT STRUCTURAL DAMAGE
DIFFUSE AXONAL INJURY
SHEARING OF AXONS IN THE W.M.
IMMEDIATE COMATOSE & MAY NOT AWAKEN
B.) SECONDARY
HEMORRHAGE
INFECTION
SECONDARY BRAIN SWELLING AND EDEMA
CAROTID ARTERY OCCLUSION
HEMORRHAGE
EPIDURAL, SUBDURAL, & INTRACEREBRAL
A. EPIDURAL HEMATOMA (EXTRADURAL)
- involves extracerebral blood vessels, middle meningeal
artery and vein
ASSESSMENT: - ACUTE MANIFESTATION?
Classical Sign:
1. unconsciousness immediately after head trauma
2. Awakens & quite lucid Dx criteria
3. Later, lapses to come
CONSIDERED A MEDICAL EMERGENCY!
SUBDURAL HEMATOMA (SDH)
COLLECTION OF BLOOD BETWEEN DURA AND ARACHNOID
BLOOD IS NOT REABSORBED BUT BECOMES ORGANIZED OR
ENCAPSULATED BY THE DURA
BLOOD CLOTS AND THEN LATER ON LYSES (HIGH OSMOTIC
CHARACTER) --- H2o fr. SAS --- increase ICP
3 categories: ACUTE & SUBACUTE and CHRONIC
Acute = 24 48 hrs Subacute = 48 2 weeks
Chronic = 3 weeks months
SDH MANIFESTATION
Acute & Subacute SDH
Changes in LOC
Pupillary signs
Hemiparesis
Chronic SHD
Seen freq. in the elderly
Devlp from minor H.I.
Person seems to recover, then, neurologic signs progressively
develop
HEADACHE prominent Symptom
LOC most predominant assessment finding
Focal or lateralizing symptom (hemiparesis)***
INTRACEREBRAL HEMATOMA
OCCUR LESS OFTEN THAN EPIDURAL OR SDH, AND CAUSE
DIRECTLY BY BRAIN TISSUE BLEEDING
ASSESSMENT FINDING SAME WITH EPIDURAL AND SDH
hemiplegia more common than hemiparesis
Additional secondary head trauma
BRAIN SWELLING AND EDEMA
ASSOCIATED WITH SERIOUS HEAD INJURIES
INFECTION
OPEN HEAD INJURIES
MENINGITIS AND BRAIN ABSCESS
Classification
Mild (GCS 13 to 15, with loss of consciousness to 15 minutes)
Moderate (GCS 9 to 12, with loss of consciousness for up to 6 hours)
Severe (GCS 3 to 8, with loss of consciousness greater than 6 hours)
Diagnostic Evaluation
CT scan to identify and localize lesions, edema, bleeding.
Skull and cervical spine films to identify fracture, displacement.
Neuropsychological tests during rehabilitation phase to determine
cognitive deficits.
CBC, coagulation profile, electrolyte levels, serum osmolarity, ABG values,
and other laboratory tests to monitor for complications and guide
treatment.
MANAGEMENT/ TREATMENT
EMERGENCY AND ACUTE CARE
AIRWAY
100 % OXYGEN
MAINTENANCE OF CIRCULATION
MEASURES TO REDUCE ICP
CSF DRAINAGE
If disconnected, clamp nearest the head
Check for leakage
Avoid pressure or kinking
Clamp drainage tubing when moving or turning the
patient
OSMOTHERAPY
Dehydrate the brain; MANNITOL
FBC!; I & O!; may be combined with fluid restrction
STEROIDS
HYPERVENTILATION
HYPOTHERMIA
BARBITURATES
Tx FOR OTHER COMPLICATION
HYPONATREMIA - < 130 Meq/L ????
FLUID RESTRICTION < 800 mL
HYPERNATREMIA POLYURIA, sp. Gravity = 1.000 -1.006
HYPERMETABOLIC STATE 1 2 yrs. Prophylactic meds
POST-TRAUMATIC SEIZURE
STRESS ULCERS (C.U.)
NURSING INTERVENTION
MAINTAIN THE AIRWAY
MAINTAINING FLUID AND ELECTROLYTE BALANCE
POVIDING ADEQUATE NUTRITION
PREVENTING INJURIES
MONITOR BODY TEMPERATURE
MAINTANING SKIN INTEGRITY
ASSESS AL BODY SURFACE Q 8HRS
TURN Q 2 4 HRS
PROVIDE SKIN CARE Q 4 HRS.
IMPROVE COGNITIVE FUNCTION
PREVENTING SLEEP PATERN DISTURBANCE
PREVENTING INJURY
OBSERVE FOR RESTLESSNESS
AVOID BLADDER DISTENTION
PADDED SIDE RAILS, HANDS WRAPPED IN MITTS
AVOID RESTRAINTS AS MUCH AS POSSIBLE
AVOID USING NARCOTICS FOR RESTLESSNESS
DECREASE ENVIROBNMENTAL STIMULI
PROVIDE ADEQUATE LIGHTING TO PREVENT VISUAL
HALLUCINATION
DO NOT DISRUPT SLEEP/WAKE CYCLES
SEIZURE DISORDER
epilepsy
THE SACRED DISEASE fr. GREEK to take hold or seize
Are paroxysmal neurologic disorders causing recurrent episodes of
seizures
SEIZURE a paroxysmal, uncontrolled, abnormal discharge of
electrical activity in the brains gray matter.
Classification of seizures
General seizures
Diffuse
Begins bilaterally
Partial seizures (focal epilepsy)
Begin in one localized area
A. Generalized seizures (1/3)
GRAND MAL (10%)
Sudden loss of consciousness
Tonic phase - 30 60 seconds
Clonic phase
Entire grand mal = 2 5 min
Post grand mal:
Unresponsive
Post-ictal sleep, general fatigue,
depression, confusion, and headache
PETIT MAL (absence)
MINOR MOTOR (akinetic, myoclonic, and atonic)
GRAND MAL
Sudden loss of consciousness
Tonic phase - 30 60 seconds
Clonic phase
Entire grand mal = 2 5 min
Post grand mal:
Unresponsive
Post-ictal sleep, general fatigue,
depression, confusion, and headache
Petit mal (absence) seizure
Usually begin during childhood and primarily limited to childhood and early
adolescence
Consist of brief periods of altered consciousness lasting from 5 to 30
seconds
Diminish or disappear after puberty
May develop grand mal or partial seizure
MINOR MOTOR SEIZURES
MYOCLONIC
Involuntary jerking contraction of major muscles
Person may be thrown to the floor
AKINETIC
Momentary loss of muscle movement
ATONIC
Total loss of muscle tone, person fall to the floor
B. Partial seizures
PARTIAL MOTOR SEIZURE
Focus in the region of the brains motor cortex
Convulsive twitching in an upper extremity (most common)
Jacksonian march (central spread)
PARTIAL SENSORY SEIZURES
Parietal numbness and tingling
Occipital bright, flashing lights
Temporal difficulty with speaking/ total speech arrest
PARTIAL SEIZURES WITH COMPLEX SYMPTOMATOLOGY
Psychomotor seizures or partial complex seizures
Frequently begins with an aura
have an impairment (but not a loss) of consciousness with
simple partial features, automatisms, or impairment of
consciousness only.
Simple partial seizures can progress to complex partial seizures, and
complex partial seizures can secondarily become generalized.
STATUS EPILEPTICUS
IS A STATE IN WHICH A PERSON HAS CONTINUOUS SEIZURES OR
SEIZURES IN RAPID SUCCESSION LASTING AT LEAST 30 MINUTES.
ETIOLOGY OF SEIZURES
The etiology may be unknown or due to one of the following:
Trauma to head or brain resulting in scar tissue or cerebral atrophy
Tumors
Cranial surgery
Metabolic disorders (hypocalcemia, hypoglycemia/hyperglycemia,
hyponatremia, anoxia)
Drug toxicity, such as theophylline (Theo-Dur), lidocaine (Xylocaine),
penicillin
CNS infection
Circulatory disorders
Drug withdrawal states (alcohol, barbiturates)
Congenital neurodegenerative disorders
ASSESSMENT
HISTORY
P.E.
SKULL X-RAYS
EEG
CT SCAN
LP
MRI
INTERVENTION
ELIMINATING FACTORS THAT MAY CAUSE OR PRECIPITATE
SEIZURES
IMPROVING THE PERSONS PHYSICAL AND MENTAL HEALTH
SPECIFIC MEDICAT TREATMENT
SURGICAL TREATMENT
MEDICAL TREATMENT
Anticonvulsants or antiepileptic drugs (AEDs)
Most effective method of controlling seizures that have no
treatable cause
High doses of a single drug are more preferred than smaller
doses of several drugs
SURGICAL INTERVENTION
CRITERIA
FAILURE OF MEDICAL APPROACH
LOCALIZATION AND IDENTIFICATION OF A FOCUS OF
ABNORMAL DISCHARGE THAT IS EASILY ACCESSIBLE
SURGICALLY AND IS LOCATED IN DISPENSIBLE CORTEX
Patient is kept awake during surgery, (alert and cooperative).
temporal lobectomy, extratemporal resection, corpus callosotomy,
hemispherectomy
Nursing Intervention
Assess neurologic and respiratory status
Maintain a patent airway
Monitor and record V/S, I/O, neurovital signs, and laboratory studies
Administer medication as prescribed
Maintain seizure precautions
Protect the patient from injury during seizure activity
Observe and record seizure activity
Assess postictal state
Encourage the patient to express feelings about powerlessness
Maintain the patients diet
Individualize home care instructions
Know about the disorder and its implications
Follow instructions for medication use and be aware of
possible adverse effects
Recognize signs and symptoms of seizure onset
Avoid drinking alcohol
Promote safe environment
Wear a medical identification bracelet
Identify and time seizure activity
Prevent injury during seizure activity
MENINGITIS
Inflammation of the meninges that surround the brain and the spinal cord.
Classified as Septic and Aseptic
Neisseria meningitidis (most common)
Haemophilus influenzae and streptococcus pneumoniae ((causative
agents)
Neisseria and Streptococcus pneumoniae,most common cause (
Lippincott)
Pathophysiology
Infecting organism gains entry through bloodstream (2
0
infection) or direct
extension
Infecting organism produce an inflammatory response
Meningeal vessels becomes hyperemic and increasingly permeable
Blood cells (neutrophils) migrate to SAS, producing exudate
Exudate formation causes meningeal irritation and increased ICP
Clinical Manifestations
Initial/ Classic: fever, headache
Systemic infection
Fever, tachycardia, chills and petechial rash
Meningeal Irritation
Nuchal rigidity - early sign
Positive Kernigs sign
Positive Brudzinskis sign
Photophobia
Neurologic signs
Decrease in consciousness
Cranial nerve palsies (ptosis, diplopia, facial
weakness, tinnitus, vertigo, and deafness)
Focal neurologic deficits (ataxia and motor
weakness)
Seizures
Other Signs
Petechial or purpuric rash to large area of ecchymosis from coagulopathy,
especially with N. meningitidis.
Disorientation and memory impairment
Behavioral manifestation
Other signs f Increase ICP
Fulminating infection (10 % of Meningococcal meningitis)
Signs of septicemia
Fever
Extensive purpuric lesion over face and
extrinmities
Shock
DIC
Diagnostic Evaluation
LP: elevated CSF pressure; cloudy, turbid, or clear in appearance; normal
or increased protein; glucose decreased or normal; culture and sensitivity
test; presence of polysaccharide antigen (supports bacterial meningitis)
Cultures: identify source of infection in blood, urine, and nose and throat
secretions
X-rays: assess for fractures, abscesses, or signs of infection in chest, skull
and sinuses
WBC count: elevated
Prevention
Vaccination: meningococcal meningitis (MCV4)
Antimicrobial prophylaxis for people in close contact with meningococcal
patients
Rifampicin (Rifadin), Ciprofloxacin hydrochloride (Cipro), or
ceftriaxone sodium (Rocephin)
Vaccination as an adjunct to antibiotic (H. influenzae and S. pneumoniae)
Medical Management
A.) Early antibiotic therapy
- Penicillin ( ampicillin and piperacillin)
- Cephalosporin (ceftriaxone sodium,
cefotaxime sodium)
- Vancomycin hydrochloride alone or
with rifampicin **
B.) Dexamethasone
- given 15 to 20 minutes before 1
st
dose of
antibiotic (q 6 hrs for 4 days)
C.) Fluid volume expanders DHN and shock
D.) Phenytoin (dilantin)
E.) Meaures for increased ICP
F.) Diuretic, Isolation, and seizure precaution
Nursing Management
Provide continuous or on-going neurological assessment, monitor Vital
signs
Pulse oximetry and ABG is monitored
Take measure to address Fever immediatey
Monitor body weight, serum electrolytes, and urine volume, specific
gravity, and osmolality
Protect the patient from injury (seizure precaution)
Prevent complication secondary to immobility
Institute droplet precautions until 24 hours after the initiation of antibiotic
therapy (isolation technique)
Report meningococcal meningitis to local health authority
Brain Abscess
Localized collection of pus within the parenchyma of the brain and spinal
cord
Relatively rare, complication encountered by immuno-compromised
patients
Pathophysiology
Direct invasion from intracranial trauma or surgery
Spread of infection from nearby sites (sinuses, ears, and teeth)
Spread of infection from other organs(lung abscess, infective endocarditis)
Clinical Manifestation
HEADACHE worse in the morning (prevailing symptom)
Vomiting
Focal neurologic signs (depends on the location of abscess)
Change in mental status
Fever may or may not be present
Diagnostics
CT SCAN
MRI
Useful to obtain images of the Brain Stem and posterior fossa
Medical Management
Antimicrobial therapy & Surgical incision or aspiration
Penicilin G (20 million U) and Chloramphenicol (4-6 g/day
given IV in divided doses)
Given preoperatively and postoperatively
Corticosteroids
Antiseizure medications (phenytoid, phenobarbital)
Nursing Management
Focus is on Ongoing assessment
Blood laboratory test result , blood glucose and serum potassium levels
Patient safety is a key nursing responsibility
Encephalitis
Acute inflammatory process of the brain tissue.
HERPES SIMPLEX VIRUS ENCEPHALITIS
Herpes Simplex virus (HSV) is the most common cause of acute
encephalitis (HSV 1)
PATHO:
- Infxn of buccal mucosa --- retrograde spread along trigeminal nerve --- to
brain
- Latent virus in brain tissue is reactivated
Clinical Manifestation
Inflammation and necrosis in the T F L (temporal, frontal and limbic
system)
Initial : FEVER, HEADACHE, CONFUSION, and
BEHAVIORAL ABNORMALITIES
Focal neurologic symptoms (within 7 days, last 14 21 days)
Behavioral changes
Focal seizures
Dysphasia
Hemiparesis
Altered LOC
Diagnostics
EEG
CSF
High opening pressure
Low glucose and high protein levels
Viral cultures are almost always negative
PCR (polymerase chain reaction)
Identifies DNA bands of the HSV (3
rd
and 10
th
day
of Sx onset)
NEUROIMAGING
MRI is the neuroimaging study of choice
Medical Management
ACYCLOVIR (Zovirax) medication of choice
Continued for 3 weeks (prevent relapse)
Slow administration (over 1 hour)
Usual dose is decrease in patient with Hx of renal insufficiency
FOSCARNET SODIUM (Foscavir)
- in rare cases of acyclovir resistance
Nursing Management
ON Going Neurological Assessment
Comfort measure for headache:
Dimming of lights
Limiting noise
Administering analgesics
Use opioid medication cautiously mask signs
Initiate injury prevention and safety
Monitor for renal complication (labs and I & O)
Fungal Encephalitis
Occur rarely in healthy people
COMPROMISED IMMUNE SYSTEM
Common agents:
Cryptococcus neoformans
Histoplasma capsulatum
Aspergillus
Candida Albicans
PATHO:
- Fungal Spores enters the body via inhalation
- Initially through the lungs and bloodstream
- CNS --- Meningitis Encephalitis brain abscess
- also causes abscess of the SC = SC compression
Clinical Manifestation
Common: Fever, malaise, headache, nuchal rigidity, lethargy and mental
status changes
Symptom of increase ICP from hydrocephalus
Assessment and Diagnostics
Presence of a compromised immune system and history of living or travel
to certain areas
Elevated WBC and ANEMIA
Fungal antibodies in serum
Neuroimaging CT scan and MRI
CSF :
Elevated WBC, and protein
Culture of fungi
Medical Management
ANTIFUNGAL AGENTS
Specific period or indefinite period (maintenance dose)
AMPOTHERICIN B (Abelcet, AmBisome, Amphocin, Amphotec, Fungizone,
and Fungizone IV)
- standard antifungal treatment
- dose high enough without causing renal toxicity
FLUCONAZOLE (diflucan) or flucytosine (5-FC, 5- fluorocytosine,
Ancobon)
- may be administered in conjunction with ampothericin B
- causes transient increase in liver enzyme
- S/E: Nausea, abdominal pain, headache, dizziness, rash, reversible
alopecia
Nursing management
On Going assessment
Provide patient comfort:
Administering non-opioid analgesics
Limiting environmental stimuli
Positioning
Give diphenhydramine (Benadryl) and acetaminophen
(Tylenol) approx. 30 mins before amphothericin B (fever, chills
and body aches)
Monitor creatinine and blood urea nitrogen
Provide support to patient and family to cope up with work up
???
You might also like
- Chapter 6Document22 pagesChapter 6Marlop CasicasNo ratings yet
- Neural Mechanisms of Salivary Gland SecretionDocument247 pagesNeural Mechanisms of Salivary Gland SecretionMassimo Baudo100% (1)
- Disaster Nursing PowerpointDocument199 pagesDisaster Nursing PowerpointJustine Jake L. Ella100% (2)
- Pages From (Susan O'Sullivan, Raymond Siegelman) National Phy (BookFi - Org) - 3Document1 pagePages From (Susan O'Sullivan, Raymond Siegelman) National Phy (BookFi - Org) - 3drng480% (1)
- Pathology of The Nervous System PDFDocument17 pagesPathology of The Nervous System PDFAnaNo ratings yet
- Psychoanalytic Reflections On A Changing WorldDocument299 pagesPsychoanalytic Reflections On A Changing WorldMichael LazarusNo ratings yet
- Microbiology Burton's Chapter 16Document74 pagesMicrobiology Burton's Chapter 16Whenzhie Villaverde PampoNo ratings yet
- Lesson 4 - Virus InfectionDocument72 pagesLesson 4 - Virus Infectionpc.bhcNo ratings yet
- Entre The Microcosmos of Life - : Introduntion To BiochemistryDocument48 pagesEntre The Microcosmos of Life - : Introduntion To BiochemistryEINSTEIN2DNo ratings yet
- MicrosDocument4 pagesMicrosTalla CaboteNo ratings yet
- Lecture 2 Microbial Growth and NutritionDocument35 pagesLecture 2 Microbial Growth and NutritionMaria Florida ClementeNo ratings yet
- Characteristics of VirusDocument13 pagesCharacteristics of VirusTimmygreyNo ratings yet
- Professionalism: Workplace EthicsDocument45 pagesProfessionalism: Workplace Ethicsprecious maningasNo ratings yet
- Microbiology 1 PDFDocument5 pagesMicrobiology 1 PDFRaven CocjinNo ratings yet
- Laboratory-Activity-1 - Microscopy 2Document5 pagesLaboratory-Activity-1 - Microscopy 2Khate CyrelleNo ratings yet
- Microbiology Lecture 1 - Structure, Classification and MorphologyDocument4 pagesMicrobiology Lecture 1 - Structure, Classification and MorphologyAldwin BagtasNo ratings yet
- Cardiovascular Health 2016Document1 pageCardiovascular Health 2016Jeremy KurnNo ratings yet
- Table of Communicable Diseases PDFDocument12 pagesTable of Communicable Diseases PDFkayekristine2001No ratings yet
- Rubric For Collaborative Lesson Plan Writing: Score 4 (Exemplary) 3 (Proficient) 2 (Developing) 1 (Needs Improvement)Document3 pagesRubric For Collaborative Lesson Plan Writing: Score 4 (Exemplary) 3 (Proficient) 2 (Developing) 1 (Needs Improvement)Nikki CrystelNo ratings yet
- Ursing Care of Client With CancerDocument51 pagesUrsing Care of Client With CancerJimmelyn PalosNo ratings yet
- CNS - Limbic SystemDocument46 pagesCNS - Limbic SystemsarvinaNo ratings yet
- Chapter 1-What Is Organizational BehaviourDocument21 pagesChapter 1-What Is Organizational BehaviourMaryrose M. AmulNo ratings yet
- Chapter 3 & 4 The Anatomy of The Nervous System and Neural TransmissionDocument47 pagesChapter 3 & 4 The Anatomy of The Nervous System and Neural Transmissionjohn rey adizNo ratings yet
- Midterm Psych Module 7Document14 pagesMidterm Psych Module 7Ladybelle GototosNo ratings yet
- The Limbic System: Juan Enrique Toro Perez UWO Fellow Neurology Residents Neurosciences Review Tutor: Jorge BurneoDocument54 pagesThe Limbic System: Juan Enrique Toro Perez UWO Fellow Neurology Residents Neurosciences Review Tutor: Jorge BurneoJuan Enrique Toro PerezNo ratings yet
- PsychopharmacologyDocument53 pagesPsychopharmacologypujarze4100% (1)
- Study Guide QuestionsDocument4 pagesStudy Guide QuestionszaidaNo ratings yet
- Kharkov National Medical University: Head of Microbiology, Virology and Immunology DepartmentDocument35 pagesKharkov National Medical University: Head of Microbiology, Virology and Immunology DepartmentAnisaFajarKumala100% (1)
- Antipsychotic or Neuroleptic DrugsDocument12 pagesAntipsychotic or Neuroleptic Drugscamile buhanginNo ratings yet
- 03 Adaptive Immune SystemDocument14 pages03 Adaptive Immune SystemEnea NastriNo ratings yet
- Pharma Mod 11Document12 pagesPharma Mod 11ANGELA SHANE AGUSTINNo ratings yet
- KIM Neuroanatomy PDFDocument47 pagesKIM Neuroanatomy PDFRida TarrarNo ratings yet
- Pathogenesis of InfectionDocument8 pagesPathogenesis of InfectionCardion Rayon Bali UIN MalangNo ratings yet
- Degenerative Neurological DisordersDocument61 pagesDegenerative Neurological DisordersMarites Santos AquinoNo ratings yet
- Premidterms NotesDocument4 pagesPremidterms NotesRenee Andrei Concepcion MozarNo ratings yet
- Infectious Disorders HandoutsDocument35 pagesInfectious Disorders Handoutsfebie pachecoNo ratings yet
- Anatomy & Physiology Syllabus For Community CollegesDocument312 pagesAnatomy & Physiology Syllabus For Community CollegesRenz EspinosaNo ratings yet
- Surgical Principles From MbbsBasicDocument47 pagesSurgical Principles From MbbsBasicbasic100% (5)
- Part 1 Neurological DisordersDocument80 pagesPart 1 Neurological DisordersshanikaNo ratings yet
- Limbic SystemDocument11 pagesLimbic SystemStd DlshsiNo ratings yet
- Bacterial Cell Structure 1) Capsule: Spirillum (Spiral) - Mycoplasmas Are BacteriaDocument4 pagesBacterial Cell Structure 1) Capsule: Spirillum (Spiral) - Mycoplasmas Are BacteriaTLCRNo ratings yet
- Cardiovascular SystemDocument8 pagesCardiovascular SystemHannah Grace CorveraNo ratings yet
- Parasitic InfectionsDocument27 pagesParasitic InfectionsYsabelle GutierrezNo ratings yet
- Diencephalon-Ppt For BioDocument7 pagesDiencephalon-Ppt For BioLipi UpadhyayNo ratings yet
- Human Nervous-SystemDocument32 pagesHuman Nervous-SystemhwzeeeNo ratings yet
- Cardiac Dysfunction in Neurocritical Care.Document14 pagesCardiac Dysfunction in Neurocritical Care.Angela Moreira ArteagaNo ratings yet
- Urinary System Lecture NotesDocument8 pagesUrinary System Lecture NotesBettina ColobongNo ratings yet
- Anatomy Exam Notes CNSPDFDocument60 pagesAnatomy Exam Notes CNSPDFBerk SonmezNo ratings yet
- The Human Brain: Anatomy, Functions, and InjuryDocument53 pagesThe Human Brain: Anatomy, Functions, and InjuryFaraida Jilzani ArsadNo ratings yet
- Nursing Informatics in The Health Care Profession by Juvy CarameDocument23 pagesNursing Informatics in The Health Care Profession by Juvy CarameJUVY CARAMENo ratings yet
- Respiratory System Anatomy and PhysiologyDocument19 pagesRespiratory System Anatomy and PhysiologyKBDNo ratings yet
- Trigeminal and Facial NerveDocument121 pagesTrigeminal and Facial NerveFadilaNo ratings yet
- Limbic SystemDocument4 pagesLimbic SystemAyu NurdiyanNo ratings yet
- (Surg2) 5.1b Introduction To Anesthesia-Part 2Document16 pages(Surg2) 5.1b Introduction To Anesthesia-Part 2AlloiBialbaNo ratings yet
- Overview of Nervous SystemDocument63 pagesOverview of Nervous SystemMAHARANI100% (1)
- Anatomy / Physio of The EarDocument58 pagesAnatomy / Physio of The EarRA100% (1)
- Lect. 1 Organization of The Nervous System 54Document74 pagesLect. 1 Organization of The Nervous System 54nopporn2520No ratings yet
- Anti InfectivesDocument126 pagesAnti Infectiveseunice lachicaNo ratings yet
- Who Moved The Cheese PresentationDocument5 pagesWho Moved The Cheese PresentationP Sthapitanonda PesquedaNo ratings yet
- Module 10 - The Nervous SystemDocument8 pagesModule 10 - The Nervous SystemAngela FelixNo ratings yet
- Nervous SystemDocument69 pagesNervous SystemZekiah MagsayoNo ratings yet
- Nervous SystemDocument125 pagesNervous SystemGIRLLYN BURZONNo ratings yet
- See Pharma Schedule For Medicines To Be Given (Oral and Parenteral)Document9 pagesSee Pharma Schedule For Medicines To Be Given (Oral and Parenteral)Justine Jake L. EllaNo ratings yet
- Gastro Intestinal DisordersDocument14 pagesGastro Intestinal DisordersJustine Jake L. Ella100% (1)
- Maternity NursingDocument10 pagesMaternity NursingJustine Jake L. Ella100% (7)
- ScabiesDocument2 pagesScabiesJustine Jake L. EllaNo ratings yet
- Review of The Nervous SystemDocument38 pagesReview of The Nervous SystemNan'EsiPessehNo ratings yet
- Central and Peripheral Nervous System, Spinal Cord and Spinal NervesDocument4 pagesCentral and Peripheral Nervous System, Spinal Cord and Spinal NervesDaniel DanielNo ratings yet
- Pathology Questions Mcqs in WordDocument109 pagesPathology Questions Mcqs in WordP D SpencerNo ratings yet
- Group 10: Peripheral Nervous System (PNS)Document24 pagesGroup 10: Peripheral Nervous System (PNS)Tara DolotaNo ratings yet
- The Electrodiagnosis of Cervical and Lumbosacral RadiculopathyDocument22 pagesThe Electrodiagnosis of Cervical and Lumbosacral RadiculopathyelkarnetilNo ratings yet
- AnatomyDocument84 pagesAnatomyKumar M V ScNo ratings yet
- Thorax Anatomy..Document21 pagesThorax Anatomy..Dungani AllanNo ratings yet
- Who TRMDocument250 pagesWho TRMDaniel Giraldo Toro100% (1)
- Anatomy - Nervous System - Spinal Cord and Motor and Sensory PathwaysDocument43 pagesAnatomy - Nervous System - Spinal Cord and Motor and Sensory PathwaysYAMINIPRIYAN100% (1)
- Chapter 17 Biology 2nd Year - Prof. Ijaz Ahmed Khan Abbasi (Lecturer Biology PGC) Notes - MDCAT by FUTURE DOCTORS - Touseef Ahmad Khan - 03499815886Document36 pagesChapter 17 Biology 2nd Year - Prof. Ijaz Ahmed Khan Abbasi (Lecturer Biology PGC) Notes - MDCAT by FUTURE DOCTORS - Touseef Ahmad Khan - 03499815886Suffa Academy100% (3)
- Anatomy of Brachial Plexus: DR - Sadiq Wadood Siddiqui JR3 Department of AnatomyDocument53 pagesAnatomy of Brachial Plexus: DR - Sadiq Wadood Siddiqui JR3 Department of AnatomySadiq Wadood SiddiquiNo ratings yet
- Notes Ha LabDocument9 pagesNotes Ha LabGomo gomoNo ratings yet
- Test, Questions and Clinical - Cases in NeurologyDocument111 pagesTest, Questions and Clinical - Cases in NeurologyPurwa Rane100% (1)
- Cauda Equina SyndromeDocument15 pagesCauda Equina SyndromeAdhi Surya NegaraNo ratings yet
- Lecture Notes in NeuroanatomyDocument752 pagesLecture Notes in NeuroanatomyDenver NcubeNo ratings yet
- إعلام عملي - 1Document37 pagesإعلام عملي - 1Mohammed AliNo ratings yet
- Coordination and Control: Animation 12.1: Neuron Source & Credit: Nichd - NihDocument37 pagesCoordination and Control: Animation 12.1: Neuron Source & Credit: Nichd - Nihwardah nooriNo ratings yet
- Anatomy and Physiology Chapter 19 Neurological SystemDocument38 pagesAnatomy and Physiology Chapter 19 Neurological SystemBrantNo ratings yet
- Electrodiagnosisofcervical Radiculopathy: Kevin Hakimi,, David SpanierDocument12 pagesElectrodiagnosisofcervical Radiculopathy: Kevin Hakimi,, David Spanierkashif mansoorNo ratings yet
- Anatomy - Spinal Cord & Spinal NervesDocument32 pagesAnatomy - Spinal Cord & Spinal Nervesعهد زبنNo ratings yet
- Abdomen and ThoraxDocument7 pagesAbdomen and ThoraxchadNo ratings yet
- G7 Autonomic-NervousDocument54 pagesG7 Autonomic-NervousYna EstabilloNo ratings yet
- (ANA) 5.06 Organization of The Nervous SystemDocument19 pages(ANA) 5.06 Organization of The Nervous SystemAdrian MaterumNo ratings yet
- 615d57d2d1f66a1941cfb64d-1633507463-CENTRAL AND PERIPHERAL NERVOUS SYSTEMDocument71 pages615d57d2d1f66a1941cfb64d-1633507463-CENTRAL AND PERIPHERAL NERVOUS SYSTEMJana Marie AngwaniNo ratings yet
- Review - Pelvic Nerves - From Anatomy and Physiology To Clinical ApplicationsDocument17 pagesReview - Pelvic Nerves - From Anatomy and Physiology To Clinical ApplicationsNovi RobiyantiNo ratings yet
- USG Spinal InjectionDocument19 pagesUSG Spinal InjectionIgor HermandoNo ratings yet
- Current Mental Health Status in Asia (Autosaved)Document57 pagesCurrent Mental Health Status in Asia (Autosaved)Susan MaglaquiNo ratings yet
- Zanki Neuro BoldedDocument25 pagesZanki Neuro Boldedsmian08No ratings yet
- Nervous SystemDocument8 pagesNervous SystemNicah FranciscoNo ratings yet