Professional Documents
Culture Documents
Fod Maps
Uploaded by
NoorAkCopyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Fod Maps
Uploaded by
NoorAkCopyright:
Available Formats
Low-FODMAP
Living
Experts Discuss
Meal-Planning
Strategies to
Help IBS Clients
Better Control
GI Distress
By Kate Scarlata, RD, LDN
iving with chronic abdominal pain, gas, bloating, diarrhea, or constipation is no walk in the
park. For clients suffering from irritable bowel
syndrome (IBS), these symptoms can greatly
impact their quality of life. And yet 76% of those
who suffer from IBS can better manage them by following
a novel dietary approach that originated in Melbourne, Australia.1 Monash University researchers call this approach the
low-FODMAP diet, known as fermentable oligo-, di-, and monosaccharides and polyols, a group of short-chain carbohydrates.
These carbohydrates can exert luminal distention via
osmotic effects and rapid fermentation, resulting in gas, pain,
36 todays dietitian march 2012
and diarrhea in sensitive individuals. Since the majority of IBS
sufferers acknowledge symptom improvement when following the low FODMAP diet, its important for RDs to be proficient
in providing dietary guidelines and strategies to clients to help
them plan menus, grocery shop, read labels, and make healthful food choices while dining out.
Research Behind FODMAPs
FODMAPs are found in everyday foods, including milk and
ice cream (lactose); apples, pears, honey, and watermelon (free
fructose); wheat, onions, garlic, and inulin (fructans); legumes
(galacto-oligosaccharides [GOS]); and prunes, sugar-free
Low FODMAP Menu
gum, and mints (polyols). FODMAPs have a cumulative impact
on gastrointestinal symptoms. Individuals may tolerate small
amounts, but symptoms can develop if they consume quantities
that surpass their threshold.
Studies have shown that ingesting FODMAPs exacerbates
symptoms in most people with IBS, while dietary restriction
of FODMAPs improves symptom control. Ong and colleagues2
from Monash University found that in those with IBS, dietary
FODMAPs induce prolonged hydrogen production in the intestine to a greater degree. More recently, researchers at Kings
College London found that the low FODMAP diet, in contrast to
standard diet therapy for IBS management, showed improved
overall symptom response in 86% of participants compared
with 49% in the standard diet group.1 Halmos and colleagues3
found that enteral formula with the highest FODMAP content created a greater risk of diarrhea, a common concern
with enteral tube feeding. Research supports the use of the
low FODMAP diet in patients whose inflammatory bowel disease is in remission but who have enduring IBS symptoms.4 In
patients with strictures, however, a low FODMAP diet is contraindicated, as the osmotic effects of the FODMAPs are likely
to be beneficial in preventing intestinal obstruction.
Breakfast
Erewhon Corn Flakes
Enriched rice milk (organic Rice Dream)
Banana
1 T sliced almonds
Lunch
Udis white bread
Sliced turkey
Lettuce or spinach leaves
Tomato
Sliced cheddar cheese
Green Valley lactose-free vanilla yogurt
1
2 cup blueberries
Baby carrots
Dinner
Grilled chicken or salmon
Baked potato with skin (butter optional)
Sauted spinach and red peppers seasoned with green
part of spring onion, salt, pepper, handful of pine nuts,
and olive oil
Kiwifruit
Balance Good Nutrition With Symptom Control
When counseling clients about menu planning, factoring in their food preferences and lifestyle behaviors likely will
help them adhere to the low FODMAP diet. The diet is somewhat restrictive but can provide adequate nutrients with careful
planning. For those with lactose intolerance, meeting calcium
and vitamin D requirements can be more challenging. Encourage consuming lactose-free milk; acceptable cheeses such as
Swiss, cheddar, feta, and mozzarella; enriched rice milk; spinach; and canned salmon for low FODMAP calcium sources. You
can suggest vitamin supplements as needed and choose those
free of FODMAP ingredients such as sorbitol and mannitol.
Fiber intake can decrease when clients follow the low
FODMAP diet so discuss low FODMAP fiber sources such as
oatmeal and rice bran as shown in Table 1 on page 38.
If clients need fiber supplements, suggest a nonfermentable
fiber choice such as Citrucel.
FODMAP-Friendly Menu Planning
When helping clients plan menus, its a good idea to
encourage them to develop a strategy and plan ahead.
For example, since most commercial meat and vegetable broths are rich in FODMAP ingredients, suggest clients
make a homemade broth by boiling water containing chicken
breasts, celery leaves, parsnips, carrots, salt, and pepper.
Save the broth and chicken for meals and side dishes during
the week. They can make risotto, chicken pot pie, chicken
salad, or chicken and rice soup. Recommend they make large
Low FODMAP Vegan Menu
Breakfast
Quinoa flakes
Enriched rice milk
3
4 cup strawberries
1 T sliced almonds
Lunch
Rice cakes with nut butter
Fruit salad with 1 cup (total) low FODMAP fruits (eg,
kiwifruit, strawberries, blueberries)
Spinach salad with lemon dressing and cherry tomatoes
Snack
Carrots and red peppers dipped in tahini
Rice milk
Handful of almonds
Dinner
Tofu and vegetable stir-fry (red peppers, zucchini,
summer squash, carrots)
Quinoa and millet saut with pine nuts
Kiwifruit or orange
march 2012 www.todaysdietitian.com 37
batches of grains such as quinoa and rice and use them
throughout the week to top salads, add to soups, or
make a pudding. Since meats and oils are free of FODMAPs, clients can include them in recipes as desired.
Using gluten-free pasta, pizza crusts, and bread instead
of wheat-based products is a simple way clients can
reduce fructans in their diet.
Clients who have functional gut disorders such as IBS
or functional bloating often self-limit their diet beyond
the low FODMAP guidelines. It may be necessary then to
create menus that include other dietary restrictions in
addition to the low FODMAP diet. The sidebars on page
37 feature a typical low FODMAP vegan and nonvegan
menu for breakfast, lunch, and dinner that you can share
with patients.
Table 1: Fiber Without FODMAPs
Food
Portion Size
Grams of Fiber
Oatmeal
4.1
Oat bran
7.2
Rice bran
6.2
Strawberries
1 cup, halves
Blueberries
1 cup
3.6
Orange
1 medium
3.1
Spinach
2 cup, cooked
2.2
Baked potato, with skin
1 medium Russet
Quinoa
1 cup, cooked
5.2
2 cup, dry
4 cup, dry
Source: USDA National Nutrient Database for Standard Reference
Safe Snacking
Once clients are armed with menu ideas, encourage them
to keep low FODMAP snacks on hand since theyre not always
available while on the go. Here are a few ideas:
Glutino pretzels and a mozzarella cheese stick
Two rice cakes spread with a layer of peanut butter
One banana and a handful of almonds
Blue Diamond Almond Nut thins and Swiss cheese
Lactose-free yogurt (Green Valley) with 1 cup of blueberries
and 1 T of almonds
Half of a sandwich using Udis white bread filled with sliced
chicken, lettuce, and tomato slices
One celery stick filled with peanut butter. Suggest clients eat
just one, as celery contains mannitol, a polyol source.
Add Flavor Not FODMAPs
Clients who like to cook often use onions and garlic to flavor
their food. But these pungent flavor enhancers arent suitable
for those following the low FODMAP diet.
For onion flavor, substitute low FODMAP choices such as
chives, scallions (green part only), and/or a dash of asafoetida powder. Found in Indian markets, asafoetida powder may
contain small amounts of wheat, so advise clients with celiac
disease to buy a wheat-free brand. For garlic lovers, suggest
they saut large garlic chunks in oil over medium heat until the
flavor permeates the oil. Remove the garlic pieces before using
the oil as a flavoring to ensure the dish remains tasty but low in
FODMAPs. Warn clients not to add chunks of garlic to a waterbased recipe and remove them because the fructans in the
garlic are water soluble and may seep into the water.
Grocery Shopping the Low FODMAP Way
Once clients plan their menus, theyll need to shop for
ingredients. Maintaining a low FODMAP pantry is key to sustaining a low FODMAP diet. Here are some tips to help clients
get started:
38 todays dietitian march 2012
2 cup, dry
Choose colorful fruits low in FODMAPs such as strawberries, bananas, blueberries, grapes, cantaloupe, pineapple,
oranges, and kiwifruit.
Select vegetables such as spinach, carrots, red bell peppers, eggplant, bok choy, tomatoes, zucchini, and potatoes.
Purchase gluten-free, all-purpose flour blends that are
free of soy. Bean flours such as Namaste Foods Perfect
Flour Blend (www.namastefoods.com) or King Arthur
Gluten-Free Multi-Purpose Flour (www.kingarthurflour.
com) also are good choices.
Select lactose-free dairy foods such as hard cheeses,
including Parmesan, cheddar, and Swiss, and Green Valley
Lactose-Free Yogurt and Lactose-Free Kefir Milk.
Select a variety of meats, fish, and poultry and hearthealthy oils, which are all FODMAP free.
Choose nuts and seeds low in FODMAPs such as walnuts,
almonds, peanuts, pecans, pine nuts, macadamia nuts, and
sesame seeds. Avoid FODMAP-rich pistachios.
Label Reading Strategies
As clients shop for low-FODMAP foods, they must learn
how to read labels. Many people assume a gluten-free product is low in FODMAPs, but thats not always the case. In fact,
many gluten-free products contain honey, pear juice, onions,
and garlic, so they arent appropriate for those following a
low FODMAP diet. Tell clients that ingredients are listed with
the most predominant ingredient first. So if honey is the last
ingredient in the list (an indication its not used to sweeten the
product), its likely a low-FODMAP food. Suggest clients avoid
products in which FODMAPs are more abundant or if multiple
FODMAPs are present. Furthermore, clients should take note
of added fiber ingredients such as inulin, often labeled as chicory root extract and fructo-oligosaccharides. Both are sources
of fructans and can trigger symptoms.
The sidebar on page 39 presents ingredients lists to illustrate a low and high FODMAP product. The bolded items are
considered FODMAP sources.
Dining Out Without Consequence
Restaurants that serve gluten-free foods may be a good
choice for clients on a low-FODMAP diet. Although the low
FODMAP diet isnt a gluten-free diet, both restrict wheat, which
is a big source of FODMAPs. Since onions and garlic added to
dishes may pose a problem, instruct patients to order foods
without these ingredients. Hidden sources of onions and garlic
include salad dressings and broth-based dishes such as risotto
and marinades.
Suggest clients follow these tips for dining out:
Bring a low-FODMAP roll, wrap, or bread to the restaurant
and order a burger, grilled fish, chicken, or beef.
Fill a thermos with lactose-free milk or rice or almond milk
to add to your cereal, oats, or coffee when dining away from
home.
Order a salad and dress it with vinegar or lemon wedges and
olive oil.
Choose brown rice or gluten-free pasta with butter and
Parmesan cheese, or a baked potato for a side dish.
Patsy Catsos, MS, RD, a Maine-based dietitian and FODMAP
diet expert, says, Many world cuisines are rice based, such as
Thai, Chinese, Japanese, and Indian. Have a look at the menu
and choose grilled or roasted beef, chicken, shrimp, or fish with
traditional seasonings. Add rice or rice noodles with an assortment of steamed or stir-fried vegetables and ask to hold the
onions. The sauces are likely to contain most of the FODMAPs
in these meals, so either find out what theyre seasoned, sweetened, and thickened with or ask for them on the side so you can
use just a little.
In a pinch, clients can go to some fast-food restaurants
that have low FODMAP options. For instance, clients can eat
oatmeal from Starbucks or McDonalds. Just use 1 tablespoon of dried cranberries or raisins, Catsos suggests. Other
low FODMAP options include Wendys baked potato, sushi, a
banana, a small fresh fruit cup, a handful of roasted nuts, tortilla chips, sliced deli meat, chicken or tuna salad, a chef salad,
hard-boiled eggs, cheese sticks, pumpkin or sunflower seeds,
and even pickles, Catsos says.
More to Come
The low FODMAP diet will continue to undergo additional
modifications as food samples are evaluated. Staying abreast of
the research is essential to provide clients with the most up-todate information. Recently, researchers have developed consumption cut-off levels for foods containing FODMAPs for those
suffering from FODMAP-induced GI distress (less than 0.5 g
per sitting as long as individuals meet FODMAP guidelines).
Monash University researchers have provided the following
recommended limits:
Excess fructose limit is less than 0.2 g per serving.
GOS and fructans limit is less than 0.2 g (less than 0.3 g for
breads/cereals) per serving.
Low FODMAP vs.
High FODMAP Label
Low FODMAP Bread: Filtered water, tapioca starch,
brown rice flour, potato starch, sunflower oil or canola
oil, egg whites, evaporated cane juice or sugar, tapioca syrup or brown rice syrup, yeast, xanthan gum, salt,
baking powder (sodium bicarbonate, cornstarch, calcium sulfate, monocalcium phosphate), mold inhibitor (cultured corn syrup, ascorbic acid), ascorbic acid
(microcrystalline cellulose, corn starch), enzymes.
High FODMAP Bread: Water, potato extract, rice starch,
rice flour, sorghum flour, organic high oleic sunflower/
safflower oil, organic evaporated cane juice, organic
honey, egg whites, organic inulin, yeast, sea salt,
organic molasses, xanthan gum.
Honey and molasses are sources of excess fructose and
inulin is a fructan, making this bread a poor choice for
followers of a low FODMAP diet.
Sugar polyol limit is less than 0.3 g per individual polyol or
less than 0.5 g per total polyols per serving.
Australian researchers are preparing a food composition
booklet called FODMAP Food Facts. This booklet should serve
as a great tool to help clients and dietitians understand the
FODMAP content of foods, make safe food choices, and stick to
limits to avoid triggering symptoms.
IBS is a common condition, and dietitians are best suited
to teach and translate the science to clients. Peter Gibson,
a professor of medicine at Monash University and leading
FODMAPs researcher, emphasizes the importance of the RDs
role: Dietary restriction of FODMAPs is an effective therapy in
the majority of patients with functional bowel symptoms. Its a
diet that should be taught by a dietitian, and it should be firstline therapy provided the dietitian is trained in the technique.
Kate Scarlata, RD, LDN, is a Boston-based dietitian in private
practice who specializes in digestive health and the author of
The Complete Idiots Guide to Eating Well With IBS.
For references, view this article on our website
at www.TodaysDietitian.com.
march 2012 www.todaysdietitian.com 39
You might also like
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryFrom EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryRating: 3.5 out of 5 stars3.5/5 (231)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)From EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Rating: 4.5 out of 5 stars4.5/5 (121)
- Grit: The Power of Passion and PerseveranceFrom EverandGrit: The Power of Passion and PerseveranceRating: 4 out of 5 stars4/5 (588)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaFrom EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaRating: 4.5 out of 5 stars4.5/5 (266)
- The Little Book of Hygge: Danish Secrets to Happy LivingFrom EverandThe Little Book of Hygge: Danish Secrets to Happy LivingRating: 3.5 out of 5 stars3.5/5 (400)
- Never Split the Difference: Negotiating As If Your Life Depended On ItFrom EverandNever Split the Difference: Negotiating As If Your Life Depended On ItRating: 4.5 out of 5 stars4.5/5 (838)
- Shoe Dog: A Memoir by the Creator of NikeFrom EverandShoe Dog: A Memoir by the Creator of NikeRating: 4.5 out of 5 stars4.5/5 (537)
- The Emperor of All Maladies: A Biography of CancerFrom EverandThe Emperor of All Maladies: A Biography of CancerRating: 4.5 out of 5 stars4.5/5 (271)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeFrom EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeRating: 4 out of 5 stars4/5 (5794)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyFrom EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyRating: 3.5 out of 5 stars3.5/5 (2259)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersFrom EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersRating: 4.5 out of 5 stars4.5/5 (344)
- Team of Rivals: The Political Genius of Abraham LincolnFrom EverandTeam of Rivals: The Political Genius of Abraham LincolnRating: 4.5 out of 5 stars4.5/5 (234)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreFrom EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreRating: 4 out of 5 stars4/5 (1090)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceFrom EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceRating: 4 out of 5 stars4/5 (895)
- Her Body and Other Parties: StoriesFrom EverandHer Body and Other Parties: StoriesRating: 4 out of 5 stars4/5 (821)
- Men's GarmentsDocument19 pagesMen's GarmentsMrs.Arthy SaravananNo ratings yet
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureFrom EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureRating: 4.5 out of 5 stars4.5/5 (474)
- The Unwinding: An Inner History of the New AmericaFrom EverandThe Unwinding: An Inner History of the New AmericaRating: 4 out of 5 stars4/5 (45)
- The Yellow House: A Memoir (2019 National Book Award Winner)From EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Rating: 4 out of 5 stars4/5 (98)
- Nutrition and Benign Prostatic Hyperplasia: ReviewDocument4 pagesNutrition and Benign Prostatic Hyperplasia: ReviewNoorAkNo ratings yet
- On Fire: The (Burning) Case for a Green New DealFrom EverandOn Fire: The (Burning) Case for a Green New DealRating: 4 out of 5 stars4/5 (73)
- 15 Minute Psych Assessment Presentation PDFDocument65 pages15 Minute Psych Assessment Presentation PDFUnedited revealations100% (1)
- 2200 Calorie Meal PlanDocument5 pages2200 Calorie Meal PlanRileShampionNo ratings yet
- NaturoPathic Medicine Study NotesDocument13 pagesNaturoPathic Medicine Study NotesNoorAkNo ratings yet
- Sibo QuestionnaireDocument2 pagesSibo QuestionnaireNoorAk0% (1)
- 4) Lumbar Spinous Push Technique (Type IV), Iliomamillary PushDocument3 pages4) Lumbar Spinous Push Technique (Type IV), Iliomamillary PushNoorAkNo ratings yet
- Menu PlanningDocument189 pagesMenu PlanningJoderick Tejada100% (4)
- The Art of Case TakingDocument41 pagesThe Art of Case Takingasyabatool100% (2)
- Weeknight Magic Vol. 1: Masha Sullivan and Anya KassoffDocument48 pagesWeeknight Magic Vol. 1: Masha Sullivan and Anya KassoffNoorAkNo ratings yet
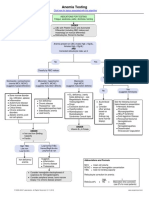
- Anemia Testing Algorithm PDFDocument1 pageAnemia Testing Algorithm PDFBilly AuNo ratings yet
- Peat Therapy 2014 01 16Document16 pagesPeat Therapy 2014 01 16NoorAkNo ratings yet
- Hydrochloric AcidDocument3 pagesHydrochloric AcidNoorAkNo ratings yet
- Melatonin Biological Basis of Its Function in Health and Disease 2006 PDFDocument303 pagesMelatonin Biological Basis of Its Function in Health and Disease 2006 PDFNoorAkNo ratings yet
- Food Sources of IronDocument5 pagesFood Sources of IrondogenvNo ratings yet
- The Faces of Low Dose Naltrexone PDFDocument116 pagesThe Faces of Low Dose Naltrexone PDFElenaMatsnevaNo ratings yet
- SIBO Summit 2016 - Key TakeawaysDocument1 pageSIBO Summit 2016 - Key TakeawaysNoorAkNo ratings yet
- Chronic Fatigue Syndrome: - A Toolkit For ProvidersDocument17 pagesChronic Fatigue Syndrome: - A Toolkit For ProvidersNoorAkNo ratings yet
- 2011-Treating Clostridium Difficile Infection With Fecal Microbiota Transplantation, Fecal Microbiota Transplantation Workgroup, Clin Gastroenterol and HepDocument6 pages2011-Treating Clostridium Difficile Infection With Fecal Microbiota Transplantation, Fecal Microbiota Transplantation Workgroup, Clin Gastroenterol and HepNoorAkNo ratings yet
- Drugs Metabolized by CYP450s PDFDocument4 pagesDrugs Metabolized by CYP450s PDFNoorAkNo ratings yet
- Athletic & Sport NutritionDocument2 pagesAthletic & Sport NutritionNoorAk100% (1)
- Hydrochloric AcidDocument3 pagesHydrochloric AcidNoorAkNo ratings yet
- 2016 Zachariae Complementary and Alternative Medicine Use Among Patients With Cancer - A Challenge in The Oncologist-Patient RelationshipDocument2 pages2016 Zachariae Complementary and Alternative Medicine Use Among Patients With Cancer - A Challenge in The Oncologist-Patient RelationshipNoorAkNo ratings yet
- 1 s2.0 S0306453016301482 MainDocument9 pages1 s2.0 S0306453016301482 MainNoorAkNo ratings yet
- Venipuncture and Blood Collection ExerciseDocument2 pagesVenipuncture and Blood Collection ExerciseNoorAkNo ratings yet
- 1 s2.0 S096007601630108X MainDocument10 pages1 s2.0 S096007601630108X MainNoorAkNo ratings yet
- Emma 3 Week OldgirlDocument3 pagesEmma 3 Week OldgirlNoorAkNo ratings yet
- 1 s2.0 S2213422015003170 MainDocument1 page1 s2.0 S2213422015003170 MainNoorAkNo ratings yet
- BF3 Pocket Guide - Final PDFDocument88 pagesBF3 Pocket Guide - Final PDFNoorAkNo ratings yet
- 10 Rules of RepertorizationDocument3 pages10 Rules of RepertorizationNoorAkNo ratings yet
- ASMDecFinal CompleteDocument24 pagesASMDecFinal CompleteNoorAk100% (1)
- Am J Clin Nutr 2000 Azaïs Braesco 1325s 33sDocument9 pagesAm J Clin Nutr 2000 Azaïs Braesco 1325s 33sNoorAkNo ratings yet
- Basic Study TipsDocument5 pagesBasic Study TipsNoorAkNo ratings yet
- Mind Map MalaysiaDocument2 pagesMind Map MalaysiaHasanNo ratings yet
- Comparison MC Donalds and Burger KingDocument12 pagesComparison MC Donalds and Burger KingLe Hoai VietNo ratings yet
- Room 3. PAG 98 Y 99Document2 pagesRoom 3. PAG 98 Y 99L Vargas ZavalaNo ratings yet
- Madrid: Júlia Cols, Claudia González and Helena IbañezDocument27 pagesMadrid: Júlia Cols, Claudia González and Helena IbañezEstel Marta Gamiz Cajal (IB1B)No ratings yet
- Tourism and Hospitality FlyerDocument2 pagesTourism and Hospitality FlyerHarsh AhujaNo ratings yet
- RPT PRE Audio Scripts T3Document4 pagesRPT PRE Audio Scripts T3Vladimir Solano GonzalesNo ratings yet
- Ob Doc & Factual Entertainment Credits: Senior/Series Producer & DirectorDocument2 pagesOb Doc & Factual Entertainment Credits: Senior/Series Producer & DirectorDani CarpanenNo ratings yet
- Synopsis Part 2Document7 pagesSynopsis Part 2swathibabuNo ratings yet
- Entreprise ManagementDocument49 pagesEntreprise ManagementNelson Perez50% (4)
- Intro Org Chart Butler SecurityDocument35 pagesIntro Org Chart Butler Securitycham sochacoNo ratings yet
- Restaurant Case StudyDocument2 pagesRestaurant Case StudySindhuja AnnNo ratings yet
- Grand TowerDocument4 pagesGrand Towerapi-27095887100% (1)
- Mcdonalds CaseDocument3 pagesMcdonalds CaseZanu Chandran M0% (1)
- Sluzbene Novine FBiH - Oglasi-55Document60 pagesSluzbene Novine FBiH - Oglasi-55edo edicNo ratings yet
- Corrosion: © 2007 Ben NurdinDocument33 pagesCorrosion: © 2007 Ben NurdinfjikjNo ratings yet
- How I Joined A CultDocument26 pagesHow I Joined A CultAnke HolstNo ratings yet
- CV. Hamdy Abd El Salam AliDocument5 pagesCV. Hamdy Abd El Salam AliBassam AhmedNo ratings yet
- Japanese Chinese Dinner MenuDocument2 pagesJapanese Chinese Dinner MenuAparna PengatNo ratings yet
- Taiwan Itinerary 2017Document8 pagesTaiwan Itinerary 2017Janelle Dela CruzNo ratings yet
- A Celebration You Enjoy-Pt3Document5 pagesA Celebration You Enjoy-Pt3izti_azrah4981No ratings yet
- Entrevista de TrabajoDocument2 pagesEntrevista de TrabajoCesar VeraNo ratings yet
- Open The "Scores" Sheet Encode Students' Names: Step 1: Step 2Document13 pagesOpen The "Scores" Sheet Encode Students' Names: Step 1: Step 2ZcharinaLykaFabellonSapunganNo ratings yet
- The Normal Distribution and Sampling Distributions: PSYC 545Document38 pagesThe Normal Distribution and Sampling Distributions: PSYC 545Bogdan TanasoiuNo ratings yet
- The Study of Coffee Shop: A Case Study of TaiwanDocument3 pagesThe Study of Coffee Shop: A Case Study of TaiwanEditor IJTSRDNo ratings yet
- CASE STUDY DominosDocument3 pagesCASE STUDY DominosHeena AroraNo ratings yet
- 3 2 5 Client HansDocument7 pages3 2 5 Client Hansapi-284582431No ratings yet
- A Foreigner in New York A Foreigner in New York: Antonio Jason Elaine PeterDocument2 pagesA Foreigner in New York A Foreigner in New York: Antonio Jason Elaine PeterGabriela GenovaNo ratings yet