Professional Documents
Culture Documents
Journal of Clinical and Diagnostic Research
Uploaded by
mutya yulindaOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Journal of Clinical and Diagnostic Research
Uploaded by
mutya yulindaCopyright:
Available Formats
JOURNAL OF CLINICAL AND DIAGNOSTIC RESEARCH
How to cite this article:
VIDYA H, NEELAM P, ANUPAMA B, SOWMYA P D. SUBHYALOID HAEMORRHAGE IN SEVERE
DIMORPHIC ANAEMIA AND THROMBOCYTOPAENIA A CASE REPORT. Journal of Clinical and
Diagnostic Research [serial online] 2010 October [cited: 2010 October 17]; 4:3201-3202.
Available from
http://www.jcdr.in/article_fulltext.asp?issn=0973709x&year=2010&volume=&issue=&page=&issn=0973-709x&id=967
Vidya H, et all, Subhyaloid haemorrhage in anaemia
CASE REPORT
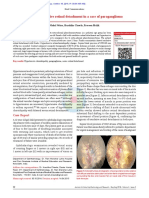
Subhyaloid Haemorrhage In Severe Dimorphic Anaemia And
Thrombocytopaenia A Case Report
VIDYA H*, NEELAM P**, ANUPAMA B***, SOWMYA P D****
ABSTRACT
We report here, a case of a 15 year old girl who presented with the complaint of reddish
discolouration of vision in the left eye. This was ascertained to be due to a subhyaloid haemorrhage
in the macular area. Haematological investigations and confirmatory bone marrow biopsy revealed
severe dimorphic anaemia with thrombocytopaenia. Following blood transfusion under the
physicians supervision, the subhyaloid haemorrhage showed signs of resolution and there was
improvement in the vision. This case report highlights the role of routine fundoscopy in all cases of
anaemia, especially as retinal findings may be present with or without visual impairment.
KEY WORDS: severe anaemia, thrombocytopaenia, subhyaloid haemorrhage, macula.
____________________________
*MS, **MS, ***DO, DNB, FMRF, ****MBBS, Department of
Ophthalmology, Yenepoya Medical College, Deralakatte,
Mangalore- 575018
Corresponding Author
Dr Vidya H,
Department of Ophthalmology
Yenepoya Medical College
Deralakatte
Introduction
intake of drugs. There was no history of melena,
nose bleeds or easy bruisibility.
The ocular manifestations of severe anaemia
include conjunctival pallor and haemorrhages,
retinal haemorrhages, tortuous retinal veins, cottonwool exudates and disc oedema, flame-shaped
retinal haemorrhages being the commonest type of
haemorrhage,
followed
by
sub-hyaloid
haemorrhage. [1] Ocular manifestations occur when
severe
anaemia
is
associated
with
thrombocytopaenia. [2] We report here, a case of
severe anaemia with thrombocytopaenia, who
presented with a subhyaloid haemorrhage which
showed signs of resolution over a period of one
week with systemic management of the condition.
Case Report
A 15 year old girl was referred for ophthalmic
examination for her complaint of reddish
discolouration of vision in the left eye. She was
admitted for polymennorhoea and menorrhagia
along with spasmodic dysmenorrhoea which was of
3 months duration. There was no ocular or head
trauma. She denied any history of the long term
3201
Mangalore- 575018
vidya_radhesh@rediffmail.com
On examination, her Best Corrected Visual Acuity
(BCVA) in the right eye was 6/6 and in the left eye,
it was 5/60. Her anterior segment findings were
unremarkable, except for conjunctival pallor.
Fundus examination showed the presence of flame
shaped haemorrhages, along with Roth spots in both
the eyes. Macula of the left eye showed sub-hyaloid
haemorrhage [Table/Fig 1]. The intraocular pressure
in both the eyes by Goldmann applanation
tonometry was 12 mmHg. She was investigated for
anaemia. Her haemoglobin level was 3.1 gm%,
platelet count was 0.71 lakh /cumm, RBC count was
0.85 million /cumm and the WBC count was 1,100
cells/ cumm. Her bleeding time, clotting time and
prothrombin time were normal. Ultrasonography of
the abdomen revealed splenomegaly.
The
peripheral blood smear report suggested features of
dimorphic anaemia, which was confirmed by bone
marrow aspiration biopsy.
Journal of Clinical and Diagnostic Research. 2010 October;(4):3201-3202
Vidya H, et all, Subhyaloid haemorrhage in anaemia
patients with thrombocytopaenia alone. [2] Our
patient
had
severe
anaemia
with
thrombocytopaenia, which were responsible for the
occurrence of retinopathy.
[Table/Fig 1]: Fundus photograph (taken on slit lamp) of
left eye showing macular subhyaloid haemorrhage
The patient was administered 3 pints of whole
blood, following which her haemoglobin level
improved to 7.4 gm% and the platelet count to 1.0
lakh / cumm. Fundus examination after a week,
showed signs of resolution of the subhyaloid
haemorrhage. BCVA in the left eye at the time of
discharge was 6/12. The patient was subsequently
lost for follow up.
Literature search on anaemic retinopathy showed
bilateral macular haemorrhage occurring in drug
induced anaemia, idiopathic thrombocytopaenic
purpura and autoimmune haemolytic anaemia.
[5],[6],[7],[8] Anaemic retinopathy is almost always
reversible with the treatment of anaemia. In our
patient, the sub-hyaloid haemorrhage showed signs
of resolution and there was improvement in the
vision with the treatment of anaemia. Surgical
intervention is required when spontaneous
resorption is insufficient [9]. This case report
highlights the need for fundus examination in all
patients with anaemia and the fact that ophthalmic
manifestations do not need any specific treatment
other than systemic management.
Discussion
Subhyaloid or preretinal macular haemorrhage is
located between the nerve fiber layer and the inner
limiting membrane. The causes for haemorrhage
include
diabetic
retinopathy,
hypertensive
retinopathy, retinal vein occlusion, ruptured
macroaneurysm, shaken baby syndrome and
valsalva retinopathy. Other causes include
autoimmune haemolytic anaemia, aplastic anaemia,
leukaemia and severe head trauma.
The factors that have been implicated in the
pathogenesis of anaemic retinopathy include anoxia,
venous stasis, angiospasm, increased capillary
permeability and thrombocytopaenia. [2] Severity
of the anaemia, increased blood viscosity as seen in
leukaemic and other myeloproliferative disorders
and periods of hypotension (especially following
severe haemorrhage), are other contributing factors
for anaemic retinopathy.
Foulds et al found a higher prevalence of anaemic
retinopathy in patients with haemoglobin levels of <
6 gm %. [3] In the study by Carraro MC, Rosetti L
and Gerli GC, retinopathy was seen in 38% of the
patients
with
concomitant
anaemia
and
thrombocytopaenia. [4] Rubenstein et al found a
44% prevalence of retinopathy in 67 patients with
anaemia and thrombocytopaenia. They found retinal
haemorrhages only in patients with anaemia and
thrombocytopaenia and no signs of retinopathy in
3202
Bibliography
[1] Duke-Elder S, Dobree JH. Disease of Retina; lx.
System of Ophthalmology. C.V. Mosby Co; 1967. pp.
37381. Chapter IV.
[2] Rubenstein
RA,
Yanoff
M,
Albert
DM.
Thrombocytopenia,
anemia,
and
retinal
hemorrhage. Am J Ophthalmol. 1968; 65:4359.
[3] Foulds WS. The ocular manifestations of blood
diseases. Trans Ophthalmol Soc UK 1963;83:345-360.
[4] Carrara MC, Rossetti L, Gerli GC. Prevalance of
retinopathy
in
patients
with
anemia
or
thrombocytopenia. Eur J Haematol 2001; 67:238244.5
[5] Belfort RN et al. Bilateral macular hemorrhage as a
complication of drug-induced anemia: a case report
.Journal of Medical Case Reports 2009 Jan 13;3:16
[6] Majji AB, Bhatia K, Mathai A. Spontaneous bilateral
peripapillary, subhyaloid and vitreous hemorrhage
with severe anemia secondary to idiopathic
thrombocytopenic purpura. Indian J Ophthalmol.
2010 MayJun; 58(3): 234236
[7] Meyer CH, Callizo J, Mennel S, Schmidt JC.
Complete resorption of retinal hemorrhages in
idiopathic thrombocytopenic purpura. Eur J
Ophthalmol. 2007;17:1289
[8] Oner A, Ozkiris A, Dogan H, Erkilic K, Karakukcu M.
Bilateral macular hemorrhage associated with
autoimmune hemolytic anemia. Retina 2005 ,
25(8):1089-1090
[9] De Maeyer K, Van Ginderdeuren R, Postelmans L,
Stalmans P, Van Calster J.Sub inner limiting
membrane haemorrhage: causes and treatment with
vitrectomy. Br J Ophthalmol 2007 Jul;91(7):850-2
Journal of Clinical and Diagnostic Research. 2010 October;(4):3201-3202
You might also like
- 2016 RetinaDocument4 pages2016 RetinaDeasy Arindi PutriNo ratings yet
- Hemorrhagic Unilateral RetinopathyDocument7 pagesHemorrhagic Unilateral RetinopathyHanna_RNo ratings yet
- Fundus Findings in Patients of Mild, Moderate and Severe Degree of Anaemia Presenting To The Tertiary Health Care CentreDocument6 pagesFundus Findings in Patients of Mild, Moderate and Severe Degree of Anaemia Presenting To The Tertiary Health Care CentreIJAR JOURNALNo ratings yet
- Issue Apr2012 Pdffiles CasereportDocument5 pagesIssue Apr2012 Pdffiles CasereportyunjaealwaysNo ratings yet
- Hematom 2Document2 pagesHematom 2omidazadmehr1375No ratings yet
- 40surekha EtalDocument3 pages40surekha EtaleditorijmrhsNo ratings yet
- HB 1Document3 pagesHB 1Putu Arimarta Irianta HerosNo ratings yet
- Spontaneous Resolution of Ophthalmologic Symptoms Following Bilateral Traumatic Carotid Cavernous FistulaeDocument6 pagesSpontaneous Resolution of Ophthalmologic Symptoms Following Bilateral Traumatic Carotid Cavernous FistulaeMaria Angelina BunawanNo ratings yet
- Oral Furosemide Therapy in Patients With Exudative Retinal Detachment Due To Hypertensive Retinopathy-IVDocument17 pagesOral Furosemide Therapy in Patients With Exudative Retinal Detachment Due To Hypertensive Retinopathy-IVnuge putriNo ratings yet
- Scurvy Masquerading As Juvenile Idiopathic Arthritis or VasculitisDocument6 pagesScurvy Masquerading As Juvenile Idiopathic Arthritis or VasculitisZach Segmuel MiñanoNo ratings yet
- Bedah Trabekulektomi 5 Fluorourasil Dengan Antivascular Endothelial Growth Factor Pada Glaukoma Neovaskular - Nikho Melga ShalimDocument12 pagesBedah Trabekulektomi 5 Fluorourasil Dengan Antivascular Endothelial Growth Factor Pada Glaukoma Neovaskular - Nikho Melga ShalimMohammed GhalumNo ratings yet
- Prop 4Document3 pagesProp 4Yuffaa AinayyaaNo ratings yet
- Bilateral Exudative Retinal Detachment in A Case of ParagangliomaDocument4 pagesBilateral Exudative Retinal Detachment in A Case of ParagangliomaDeasy Arindi PutriNo ratings yet
- Chen2014 Jurnal MataDocument3 pagesChen2014 Jurnal MatanidaNo ratings yet
- A Case Report of Evans SyndromeDocument5 pagesA Case Report of Evans SyndromecatNo ratings yet
- Exudative Retinopathy of Adults A Late S PDFDocument5 pagesExudative Retinopathy of Adults A Late S PDFInna BujorNo ratings yet
- Ophthal Notes PGDocument6 pagesOphthal Notes PGSwati TyagiNo ratings yet
- Conjunctival Folliculosis Presenting As HemolacriaDocument5 pagesConjunctival Folliculosis Presenting As HemolacriaAthenaeum Scientific PublishersNo ratings yet
- Ampiginosa 1Document5 pagesAmpiginosa 1Juan BianchiNo ratings yet
- Pi Is 0002934314012236Document3 pagesPi Is 0002934314012236olaNo ratings yet
- Case Report Diabetic Retinopaty in EnglishDocument13 pagesCase Report Diabetic Retinopaty in Englishsasha anka DilanNo ratings yet
- Journal of Oral and Maxillofacial Surgery, Medicine, and PathologyDocument4 pagesJournal of Oral and Maxillofacial Surgery, Medicine, and PathologyKharismaNisaNo ratings yet
- Respiratory and Pulmonary Medicine: ClinmedDocument3 pagesRespiratory and Pulmonary Medicine: ClinmedGrace Yuni Soesanti MhNo ratings yet
- Clinico - Hematological Analysis of Pancytopenia: A Bone Marrow StudyDocument6 pagesClinico - Hematological Analysis of Pancytopenia: A Bone Marrow StudySrinath M VNo ratings yet
- A Rare Case of Terson Syndrome With Subarachnoid HemorrhageDocument12 pagesA Rare Case of Terson Syndrome With Subarachnoid HemorrhageNinaNo ratings yet
- Oklusi Vena RetinaDocument4 pagesOklusi Vena RetinacinthyaaaNo ratings yet
- CASE REPORT COMPETITION With Identifying FeaturesDocument12 pagesCASE REPORT COMPETITION With Identifying FeaturesJoel Cesar AtinadoNo ratings yet
- Haemophilia - 2022 - Meijer - Diagnosis of Rare Bleeding DisordersDocument6 pagesHaemophilia - 2022 - Meijer - Diagnosis of Rare Bleeding Disordersyasmineessaheli2001No ratings yet
- Herpes Ophthalmicus: Review: ZosterDocument4 pagesHerpes Ophthalmicus: Review: ZosterAndika Wahyu UtomoNo ratings yet
- Prothrombin Gene Mutation G20210A, Homocysteine, Antiphospholipid Antibodies and Other Hypercoagulable States in Ocular ThrombosisDocument5 pagesProthrombin Gene Mutation G20210A, Homocysteine, Antiphospholipid Antibodies and Other Hypercoagulable States in Ocular ThrombosisDouglas NoltieNo ratings yet
- BleedingDocument4 pagesBleedingJohn Askof NyabutiNo ratings yet
- Urticarial Vasculitis Associated With Essential THDocument3 pagesUrticarial Vasculitis Associated With Essential THgugicevdzoceNo ratings yet
- Subhyaloid Hemorrhage in Cerebral Malaria: Case ReportDocument4 pagesSubhyaloid Hemorrhage in Cerebral Malaria: Case ReportFaza KahfiNo ratings yet
- Herpes Zoster OphthalmicusDocument12 pagesHerpes Zoster OphthalmicusGio Vano NaihonamNo ratings yet
- Recurrent Ischaemic Stroke Unveils Polycythaemia Vera - BMJ Case ReportsDocument9 pagesRecurrent Ischaemic Stroke Unveils Polycythaemia Vera - BMJ Case ReportsancillaagraynNo ratings yet
- Final Case - PpsDocument62 pagesFinal Case - PpsIlaiyabharathi ThulasimaniNo ratings yet
- Priapism - A Rare Presentation in Chronic Myeloid Leukemia: Case Report and Review of The LiteratureDocument5 pagesPriapism - A Rare Presentation in Chronic Myeloid Leukemia: Case Report and Review of The LiteratureSalwiyadiNo ratings yet
- 3144.full MoyamoyaDocument8 pages3144.full MoyamoyaDarren ZytkiewiczNo ratings yet
- Update On (Approach To) Anemia1 (Changes)Document39 pagesUpdate On (Approach To) Anemia1 (Changes)Balchand KukrejaNo ratings yet
- Evaluation of Hematological Parameters and Bone Marrow in Indian Patients Suffering From PancytopeniaDocument15 pagesEvaluation of Hematological Parameters and Bone Marrow in Indian Patients Suffering From PancytopeniaJUAN PABLONo ratings yet
- A Case Report On Sickle Cell Disease With Hemolyti PDFDocument4 pagesA Case Report On Sickle Cell Disease With Hemolyti PDFAlhaji SwarrayNo ratings yet
- Activity No 2 ImmunohematologyDocument3 pagesActivity No 2 ImmunohematologyAegina FestinNo ratings yet
- Matson 1961Document4 pagesMatson 1961NyimasNo ratings yet
- An Approach To Young HypertensionDocument2 pagesAn Approach To Young HypertensionNataShini RajaRatnamNo ratings yet
- RiddlesDocument44 pagesRiddlessafasayed100% (1)
- Coats Disease: Classification and Treatment: by Rishav Kansal, Bs Kiran Turaka, MD and Carol L. Shields, MDDocument3 pagesCoats Disease: Classification and Treatment: by Rishav Kansal, Bs Kiran Turaka, MD and Carol L. Shields, MDAnggie Imaniah SitompulNo ratings yet
- Masquerade SyndromesDocument10 pagesMasquerade Syndromestony_chrisNo ratings yet
- Diffuse Cavernous Hemangioma of The Spleen With Kasabach-Merritt Syndrome Misdiagnosed As Idiopathic Thrombocytopenia in A ChildDocument4 pagesDiffuse Cavernous Hemangioma of The Spleen With Kasabach-Merritt Syndrome Misdiagnosed As Idiopathic Thrombocytopenia in A ChildIndah Afriani NasutionNo ratings yet
- Retninal Vein OcclusionDocument10 pagesRetninal Vein OcclusionuhibNo ratings yet
- Supranuclear Control Ocular Motility 1800 1800Document6 pagesSupranuclear Control Ocular Motility 1800 1800Ram KumarNo ratings yet
- Case Report: Unilateral Optic Neuropathy and Acute Angle-Closure Glaucoma Following Snake EnvenomationDocument5 pagesCase Report: Unilateral Optic Neuropathy and Acute Angle-Closure Glaucoma Following Snake EnvenomationErnesErlyanaSuryawijayaNo ratings yet
- Spontaneous HyphemaDocument1 pageSpontaneous HyphemaGiovani FaustineNo ratings yet
- Central Retinal Artery OcclusionDocument9 pagesCentral Retinal Artery OcclusionAzhar Dzulhadj B. ArafahNo ratings yet
- Jurnal HifemaDocument10 pagesJurnal HifemaAndi NugrohoNo ratings yet
- Case Scenario All GroupsDocument3 pagesCase Scenario All GroupsChris P BaconNo ratings yet
- Is Episcleritis Associated To Glaucoma?Document3 pagesIs Episcleritis Associated To Glaucoma?Alvin JulianNo ratings yet
- Considerations in Managing Facial Deformities: Case Report and Review of The LiteratureDocument6 pagesConsiderations in Managing Facial Deformities: Case Report and Review of The LiteratureSukhvinder Singh RanaNo ratings yet
- Hematology FinalDocument14 pagesHematology FinalTop Music100% (1)
- Acknowledgement: Aniridia Associated With Congenital Aphakia and Secondary GlaucomaDocument3 pagesAcknowledgement: Aniridia Associated With Congenital Aphakia and Secondary GlaucomaNisrina FarihaNo ratings yet
- Antenatal Corticosteroid Therapy Before 24 Weeks.13-1Document11 pagesAntenatal Corticosteroid Therapy Before 24 Weeks.13-1mutya yulindaNo ratings yet
- Things in The ClassDocument6 pagesThings in The Classmutya yulindaNo ratings yet
- Corneal EdemaDocument1 pageCorneal EdemaLisqorinaNo ratings yet
- Daftar PustakaDocument1 pageDaftar PustakaLisqorinaNo ratings yet
- Tipikal: Golongan Nama Obat Sediaan Dosis Anjuran AntipsikosisDocument4 pagesTipikal: Golongan Nama Obat Sediaan Dosis Anjuran Antipsikosismutya yulindaNo ratings yet
- Daftar Pustaka: Cermin Dunia Kedokteran, No 151. 2006. P: 14-17Document2 pagesDaftar Pustaka: Cermin Dunia Kedokteran, No 151. 2006. P: 14-17mutya yulindaNo ratings yet
- Section 2: Diagnostic and Treatment Decisions: 2.32 Painful OphthalmoplegiaDocument14 pagesSection 2: Diagnostic and Treatment Decisions: 2.32 Painful Ophthalmoplegiamutya yulindaNo ratings yet
- Section 2: Diagnostic and Treatment Decisions: 2.32 Painful OphthalmoplegiaDocument14 pagesSection 2: Diagnostic and Treatment Decisions: 2.32 Painful Ophthalmoplegiamutya yulindaNo ratings yet
- Multi-Spot Laser Coagulation With The VISULAS 532s: A Comparative Study of 101 ProceduresDocument8 pagesMulti-Spot Laser Coagulation With The VISULAS 532s: A Comparative Study of 101 Proceduresmutya yulindaNo ratings yet
- Screening For Cervical Cancer: U.S. Preventive Services Task ForceDocument9 pagesScreening For Cervical Cancer: U.S. Preventive Services Task Forcemutya yulindaNo ratings yet
- Richter Spie06 Optoacoustic ContrastDocument10 pagesRichter Spie06 Optoacoustic Contrastmutya yulindaNo ratings yet
- Interstitial Laser Photocoagulation For Treatment of Benign Prostatic Hypertrophy: Outcomes and Cost EffectivenessDocument8 pagesInterstitial Laser Photocoagulation For Treatment of Benign Prostatic Hypertrophy: Outcomes and Cost Effectivenessmutya yulindaNo ratings yet
- 00 Diabetic Retinopathy Medical StudentsDocument7 pages00 Diabetic Retinopathy Medical StudentsBrigita De VegaNo ratings yet
- EnucleationDocument2 pagesEnucleationmutya yulindaNo ratings yet
- Vitreous Hemorrhage: Major ReviewDocument4 pagesVitreous Hemorrhage: Major Reviewmutya yulindaNo ratings yet
- Richter Spie06 Optoacoustic ContrastDocument10 pagesRichter Spie06 Optoacoustic Contrastmutya yulindaNo ratings yet
- Interstitial Laser Photocoagulation For Treatment of Benign Prostatic Hypertrophy: Outcomes and Cost EffectivenessDocument8 pagesInterstitial Laser Photocoagulation For Treatment of Benign Prostatic Hypertrophy: Outcomes and Cost Effectivenessmutya yulindaNo ratings yet
- Retinal Detachment and PeripheralDocument41 pagesRetinal Detachment and PeripheralAkhmad FauzanNo ratings yet
- Corneal EdemaDocument1 pageCorneal EdemaLisqorinaNo ratings yet
- Tubercular ScleritisDocument5 pagesTubercular Scleritismutya yulindaNo ratings yet
- 153 Swan SyndromeDocument5 pages153 Swan Syndromemutya yulindaNo ratings yet
- Vitreous HemorrhageDocument3 pagesVitreous Hemorrhagemutya yulindaNo ratings yet
- Viss CRN ProcedureDocument59 pagesViss CRN Proceduremutya yulindaNo ratings yet
- Sarkar KC and Biswas MCDocument7 pagesSarkar KC and Biswas MCDr. Shashwat BhattacharyyaNo ratings yet
- ICD 10 Training For OptometryDocument48 pagesICD 10 Training For OptometryctluvphdNo ratings yet
- Jurnal Reading Retinopati Diabetik Stase MataDocument16 pagesJurnal Reading Retinopati Diabetik Stase MatameikisirmanNo ratings yet
- DR Global Report 1Document108 pagesDR Global Report 1Quang NguyenNo ratings yet
- Diabetic Macular EdemaDocument23 pagesDiabetic Macular Edemadrvishalkulkarni2007No ratings yet
- Diabetic RetinopathyDocument12 pagesDiabetic RetinopathyGanavi R PatelNo ratings yet
- ICO International Clinical Guidelines: List of Guidelines AvailableDocument74 pagesICO International Clinical Guidelines: List of Guidelines AvailableOvidiu Rusu100% (1)
- Sush Unity OPTHALMOLOGY1700-Latest PDFDocument74 pagesSush Unity OPTHALMOLOGY1700-Latest PDFDr-Jahanzaib GondalNo ratings yet
- 1 - Perception and CoordinationDocument37 pages1 - Perception and CoordinationJek Dela CruzNo ratings yet
- FFADocument5 pagesFFASally MetwallyNo ratings yet
- MEDS 1. Diabetic Retinopathy: Practice Essentials, Pathophysiology, EtiologyDocument14 pagesMEDS 1. Diabetic Retinopathy: Practice Essentials, Pathophysiology, EtiologyVivi DeviyanaNo ratings yet
- Pathophysiology of DMDocument45 pagesPathophysiology of DMAmanuel MaruNo ratings yet
- OCT OPTOM DR Sudha Cugati 2Document76 pagesOCT OPTOM DR Sudha Cugati 2Dung Duong TrungNo ratings yet
- Intravitreal Injection of Triamcinolone Acetonide: Core MessagesDocument22 pagesIntravitreal Injection of Triamcinolone Acetonide: Core MessagesSiva LoveNo ratings yet
- Lay Forum NotesDocument7 pagesLay Forum NotesCleoGomezNo ratings yet
- Fundoscopy Ophthalmoscopy OSCE GuideDocument19 pagesFundoscopy Ophthalmoscopy OSCE GuideMohamed Anas SayedNo ratings yet
- Vitreous HemorrhageDocument7 pagesVitreous HemorrhageAndreas OctavianoNo ratings yet
- DT - Normal Eyes With Sudden Painless Loss of VisionDocument34 pagesDT - Normal Eyes With Sudden Painless Loss of VisionIzzatul Yazidah100% (1)
- Ophthalmic Manifestation of Systimic DiseaseDocument45 pagesOphthalmic Manifestation of Systimic DiseaseSarahNo ratings yet
- Prediction of Chances - Diabetic Retinopathy Using Data Mining Classification TechniquesDocument5 pagesPrediction of Chances - Diabetic Retinopathy Using Data Mining Classification Techniquesjack dawsonNo ratings yet
- ReTINAL iMAGE For BLOOD VESSEL BY USING ARTIFICIAL NEURAL NETWORKDocument5 pagesReTINAL iMAGE For BLOOD VESSEL BY USING ARTIFICIAL NEURAL NETWORKSHARMILA GHOSH,IT18 Vel Tech, ChennaiNo ratings yet
- RetinaDocument76 pagesRetinaSarahNo ratings yet
- Diabetic Macular EdemaDocument227 pagesDiabetic Macular EdemaAiGrijaDeOchiiTaiNo ratings yet
- Blurring of Vision Ii: Retinal Vascular Disorders: Dr. Jose BondocDocument15 pagesBlurring of Vision Ii: Retinal Vascular Disorders: Dr. Jose BondocRea Dominique CabanillaNo ratings yet
- Profed07-Foundation of Special and Inclusive Education-Chapter 2Document9 pagesProfed07-Foundation of Special and Inclusive Education-Chapter 2Ken100% (1)
- Diabetic Retinopathy: Dwi Lestari PohanDocument72 pagesDiabetic Retinopathy: Dwi Lestari PohanKelvin MandelaNo ratings yet
- Software Project Management: Assignment #1 (B)Document9 pagesSoftware Project Management: Assignment #1 (B)ammarNo ratings yet
- Hypertensive RetinopathyDocument46 pagesHypertensive RetinopathyAnadia RahmaNo ratings yet
- Assessing The Severity of Diabetic Retinopathy: Early Treatment Diabetic Retinopathy Study Report Number 10Document2 pagesAssessing The Severity of Diabetic Retinopathy: Early Treatment Diabetic Retinopathy Study Report Number 10Vivi DeviyanaNo ratings yet
- Kanski's Clinical Ophthalmology A Systematic Approach by John SalmonDocument20 pagesKanski's Clinical Ophthalmology A Systematic Approach by John SalmonAliNo ratings yet