Professional Documents
Culture Documents
Acute Necrotizing Pancreatitis: Treatment Strategy According To The Status of Infection
Uploaded by
Handhika Dhio SumarsonoOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Acute Necrotizing Pancreatitis: Treatment Strategy According To The Status of Infection
Uploaded by
Handhika Dhio SumarsonoCopyright:
Available Formats
ANNALS OF SURGERY
Vol. 232, No. 5, 619 626
2000 Lippincott Williams & Wilkins, Inc.
THIS MONTHS FEATURE
Acute Necrotizing Pancreatitis: Treatment
Strategy According to the Status of Infection
Markus W. Buchler, MD, Beat Gloor, MD, Christophe A. Muller, MD, Helmut Friess, MD, Christian A. Seiler, MD, and
Waldemar Uhl, MD
From the Department of Visceral and Transplantation Surgery, University of Bern, Inselspital, Switzerland
Objective
To determine benefits of conservative versus surgical treatment in patients with necrotizing pancreatitis.
Summary Background Data
Infection of pancreatic necrosis is the most important risk factor contributing to death in severe acute pancreatitis, and it is
generally accepted that infected pancreatic necrosis should
be managed surgically. In contrast, the management of sterile
pancreatic necrosis accompanied by organ failure is controversial. Recent clinical experience has provided evidence that
conservative management of sterile pancreatic necrosis including early antibiotic administration seems promising.
Methods
A prospective single-center trial evaluated the role of nonsurgical management including early antibiotic treatment in patients with necrotizing pancreatitis. Pancreatic infection, if
confirmed by fine-needle aspiration, was considered an indication for surgery, whereas patients without signs of pancreatic infection were treated without surgery.
Results
Between January 1994 and June 1999, 204 consecutive patients with acute pancreatitis were recruited. Eighty-six (42%)
Necrotizing pancreatitis (NP) represents the severe form
of human acute pancreatitis.1,2 The past decade has seen a
considerable increase in our understanding and management
of NP. The natural course of severe acute pancreatitis
progresses in two phases. The first 14 days are characterized
by the systemic inflammatory response syndrome resulting
from the release of inflammatory mediators.3,4 In patients
Correspondence: Markus W. Buchler, MD, Dept. of Visceral and Transplantation Surgery, Inselspital, University of Bern, CH-3010 Bern,
Switzerland.
E-mail: markus.buechler@insel.ch
Accepted for publication February 23, 2000.
had necrotizing disease, of whom 57 (66%) had sterile and 29
(34%) infected necrosis. Patients with infected necrosis had
more organ failures and a greater extent of necrosis compared with those with sterile necrosis. When early antibiotic
treatment was used in all patients with necrotizing pancreatitis
(imipenem/cilastatin), the characteristics of pancreatic infection changed to predominantly gram-positive and fungal infections. Fine-needle aspiration showed a sensitivity of 96%
for detecting pancreatic infection. The death rate was 1.8%
(1/56) in patients with sterile necrosis managed without surgery versus 24% (7/29) in patients with infected necrosis
( P .01). Two patients whose infected necrosis could not be
diagnosed in a timely fashion died while receiving nonsurgical
treatment. Thus, an intent-to-treat analysis (nonsurgical vs.
surgical treatment) revealed a death rate of 5% (3/58) with
conservative management versus 21% (6/28) with surgery.
Conclusions
These results support nonsurgical management, including
early antibiotic treatment, in patients with sterile pancreatic
necrosis. Patients with infected necrosis still represent a highrisk group in severe acute pancreatitis, and for them surgical
treatment seems preferable.
with NP, organ failure is common and often occurs in the
absence of infection.5 In addition to organ dysfunction,
general derangements include hypovolemia, a hyperdynamic circulatory regulation,6 fluid loss from the intravascular space, and increased capillary permeability.7 The second phase, beginning approximately 2 weeks after the onset
of the disease, is dominated by sepsis-related complications
resulting from infection of pancreatic necrosis.8,9 This is
associated with multiple systemic complications, such as
pulmonary, renal, and cardiovascular failure. In the natural
course of the disease, infection of pancreatic necrosis occurs
in 40% to 70% of patients, and it has become the most
important risk factor of death from NP.10 12 Of patients
619
620
Buchler and Others
Table 1.
Ann. Surg. November 2000
DEFINITIONS USED TO DIAGNOSE ORGAN FAILURES
Organ System
Pulmonary insufficiency
Renal insufficiency
Cardiocirculatory dysfunction
Metabolic disorders
Sepsis:* Positive blood culture/aspirate and more
than one of these clinical signs
Definition of Organ Failure
Arterial PaO2 60 mmHg (despite 4 L O2/min via nasal tube) or need for mechanical
ventilation
Serum creatinine 250 mmol/L or need for hemofiltration or hemodialysis
Mean arterial pressure 70 mmHg or need for catecholamine support
Hyperglycemia 11 mmol/L
Hypocalcemia 2 mmol/L
Coagulation disorder (prothrombin time 70%; partial thromboplastin time 45 sec)
Rectal temperature 36 or 38C
Elevated heart rate 90/min
Tachypnea (respiratory rate 20/min) or hyperventilation (PaCO2 4.3 kPa)
White cell count 4 or 12.0 109/L or presence of 10% immature neutrophils
Hyperglycemia was not used as a criterion for metabolic disorder in patients with a history of diabetes mellitus or impaired glucose tolerance. Serum creatinine 250
mmol/L was not used as a criterion for renal failure in patients with a history of chronic renal insufficiency.
* Bone RC, Balk RA, Cerra FB, et al. Definitions for sepsis and organ failure and guidelines for the use of innovative therapies in sepsis. The ACCP/SCCM Consensus
Committee. American College of Chest Physicians/Society of Critical Care Medicine. Chest 1992; 101(6):1644 1655.
who die of acute pancreatitis, more than two thirds of deaths
are due to late septic organ complications.1315
Antibiotic treatment with agents penetrating well into the
pancreas16 has been shown to prevent infection in severe
acute pancreatitis and to lower the death rate.1722 Still, the
general treatment principles in NP and particularly the role
of surgery are controversial issues. During the 1980s, according to our experience, 60% to 70% of patients with NP
were treated surgically.23 In 1991, Bradley and Allen24
introduced the concept of nonsurgical management of sterile necrosis, applying early antibiotic treatment. In 11 consecutive patients managed accordingly, there were no
deaths. In the same study, 27 patients with infected necrosis
were treated surgically using open packing, yielding a death
rate of 15%.
The promising concept of using infection as the main
parameter of surgical decision making has so far not been
adopted generally.25,26 Therefore, in a prospective singlecenter trial, we evaluated the role of nonsurgical treatment
in patients with sterile necrosis and surgical treatment in
patients with infected necrosis. In addition, we studied the
effect of early antibiotic treatment on the further course of
NP and its influence on the evolution and microbiologic
characteristics of the pancreatic infection.
PATIENTS AND METHODS
Between January 1994 and June 1999, 204 consecutive
patients with acute pancreatitis were recruited prospectively
from the Department of Visceral and Transplantation Surgery at the University of Bern. Inclusion criteria were an
elevation of serum amylase to more than three times the
upper normal limit and a typical clinical picture,27 including
abdominal pain.28 Patient stratification according to disease
severity was performed as previously published.29 NP was
defined as the appearance of pancreatic or extrapancreatic
necrosis30 on contrast-enhanced computed tomography
(CT) and a serum C-reactive protein value of more than 150
mg/L. CT was performed within 48 to 96 hours of admission and was repeated weekly in patients whose clinical
condition did not improve. On admission all patients were
treated medically according to generally accepted principles
consisting of withholding oral intake, providing pain relief,
and restoring fluid and electrolyte losses intravenously. If
vomiting had been a prominent part of the clinical picture,
a nasogastric tube was inserted. A proton pump inhibitor
was given to prevent stress ulcers, and low-molecularweight heparin (3,000 U/day) was given to prevent thrombosis. Pain treatment included the use of peridural anesthesia (n 99) or intravenous narcotic analgesics. Clinical
severity staging of acute pancreatitis was carried out using
the Ranson prognostic signs and the APACHE II scoring
system. Initially, patients were cared for in an intermediate
care unit or, in case of organ failure, in the intensive care
unit. In patients with NP, antibiotic treatment was given less
than 24 hours after CT findings of necrosis. We used imipenem/cilastatin (3 500 mg/day, intravenously) for 14
days according to the study protocol.
Endoscopic retrograde cholangiography was performed
in cases of biliary etiology, as proven by transcutaneous
ultrasonography and laboratory findings of cholestasis such as
elevated levels of serum aspartate aminotransferase, alkaline
phosphatase, or bilirubin. Papillotomy was performed if stones
or sludge were present in the common bile duct.
In patients with NP, CT-guided fine-needle aspiration
(FNA) with consecutive Gram stain and bacteriologic culture was carried out if infection of necrosis was clinically
suspected. The indication for FNA was defined during the
course of NP in the following instances:
Newly developed signs of metabolic disorders and deterioration of organ failures of lung, kidney, or the
Treatment of Necrotizing Pancreatitis
Vol. 232 No. 5
Table 2.
621
CHARACTERISTICS OF PATIENTS WITH EDEMATOUS PANCREATITIS (EP) AND
NECROTIZING PANCREATITIS (NP)
Female
Male
Mean age (range)
Biliary cause
Alcohol
Other or undefined cause
Mean serum c-reactive protein in mg/L (range)*
Mean Ranson score (range)
Mean APACHE II score (range)*
Mean hospital stay in days (range)
Hospital deaths
EP
(n 118)
NP
(n 86)
48 (41%)
70
54.2 (1796)
54 (46%)
36 (30%)
28 (24%)
81 (1205)
1.9 (07)
6.3 (116)
13 (253)
0
31 (36%)
55
56.6 (2887)
38 (44%)
32 (37%)
16 (19%)
228 (101456)
3.9 (08)
12.6 (528)
44.1 (11209)
9 (10%)
NS
.00001
.005
.01
.0001
.0012
* Peak value in the first week of disease.
cardiocirculatory system (for the definition of organ
failure, see Table 1)
Newly developed increase in blood leukocytes or fever
(38.5C) after initial response to conservative treatment.
Infection of pancreatic necrosis as proven by FNA was
regarded as an indication for surgical treatment and resulted
in surgical intervention (necrosectomy and continuous postoperative lavage of the necrotic cavities) within 24 hours.
During surgery, at least two smears for bacteriologic culture
were taken from the pancreatic necrosis and from the adjacent necrotic cavities in the retroperitoneum. Postoperative
antibiotic treatment, including antimycotic treatment, was
adapted according to the bacteriologic findings and microbiologic testing of resistance.
A complete follow-up was carried out (mean follow-up
time 35 months) after hospital discharge to determine late
consequences of edematous pancreatitis and sterile and infected pancreatic necrosis.
Data were analyzed using the Mann-Whitney or chisquare test where appropriate. P .05 was considered
significant.
RESULTS
Patient characteristics are summarized in Table 2. There
were 204 patients in the study, 125 (61%) men and 79
(39%) women. Mean age was 55.1 years (range 1796). The
cause was biliary in 92 (45%) patients, alcohol overindulgence in 68 (33%), and other or undefined in 44 (22%).
According to CT and C-reactive protein findings, there were
118 (58%) and 86 (42%) patients with edematous pancreatitis and NP, respectively.
Edematous Pancreatitis
In 118 patients, pancreatic necrosis was ruled out by CT
findings and C-reactive protein serum levels. Fifty-six pa-
tients stayed for a mean of 2.3 days (range 17) in intermediate care. No patient with edematous pancreatitis had
multiple organ failure, but in 12 patients (10%) single organ
failure was diagnosed (1 renal, 4 pulmonary insufficiency, 3
cardiocirculatory insufficiency, 4 metabolic disorders). Endoscopic retrograde cholangiopancreatography was performed early (in the first 24 48 hours) in 54 patients with
biliary etiology, and papillotomy and stone retrieval were
performed in 38 of those patients. In addition, endoscopic
retrograde cholangiopancreatography was carried out before
hospital discharge in 31 patients with an unknown cause and
to exclude tumor-induced acute pancreatitis. Laparoscopic
cholecystectomy was done in 35 patients a median of 8.6
days after admission (range 219), and open cholecystectomy was performed in 19 patients a median of 9 days after
admission (range 219). There were no hospital deaths, and
the mean hospital stay was 13 days (range 253).
Follow-Up
Hospital readmission occurred in seven patients (6%)
after a mean of 8.3 months for the following reasons:
recurrent acute pancreatitis (n 4), duodenal obstruction
(n 1), and pancreatic pseudocyst (n 1).
Necrotizing Pancreatitis
Eighty-six patients were staged as having NP based on
CT findings and C-reactive protein levels. The mean Ranson score was 3.9 (range 0 8) and APACHE II scoring was
12.6 (range 528) (P .01 vs. edematous pancreatitis) (see
Table 2). Endoscopic retrograde cholangiography was carried out in 58 patients, and papillotomy and stone removal
were performed in 20 of those patients. Again, endoscopy
was performed in the first 24 to 48 hours in 38 patients with
biliary etiology and later in 20 patients with a cause other
than gallstones. Single and multiple organ failure occurred
622
Buchler and Others
Ann. Surg. November 2000
Table 3.
ORGAN FAILURE IN PATIENTS WITH PANCREATITIS
Necrotizing Pancreatitis (n 86)
Acute Pancreatitis
No. of patients with organ failures
No. of patients with single organ failure
No. of patients with multiple organ failure
Pulmonary insufficiency
Renal insufficiency
Cardiocirculatory insufficiency
Metabolic disorders
Sepsis
EP
(n 118)
NP
(n 86)
SPN
(n 57)
IPN
(n 29)
12 (10%)
12 (10%)
0
4 (3%)
1 (1%)
3 (3%)
4 (3%)
0
62 (72%)
32 (37%)
30 (35%)
54 (63%)
11 (13%)
20 (23%)
22 (26%)
9 (10%)
.00001
.00001
.00001
.00001
.0017
.00001
.00001
.006
35 (61%)
25 (44%)
10 (18%)
27 (47%)
3 (5%)
5 (9%)
13 (23%)
1 (2%)
27 (93%)
7 (24%)
20 (69%)
27 (93%)
8 (28%)
15 (52%)
9 (31%)
8 (28%)
.015
NS
.00001
.00001
.01
.00001
NS
.01
EP, edematous pancreatitis; IPN, infected pancreatic necrosis; NP, necrotizing pancreatitis; SPN, sterile pancreatic necrosis.
in 32 and 30 patients, respectively (P .00001 vs. edematous pancreatitis) (Table 3).
Sterile Necrosis
Data on gender, age, cause, C-reactive protein levels,
Ranson score, APACHE II score, length of hospital stay,
and hospital death rate are given in Table 4. The severity,
based on the Ranson and APACHE II scores in the first
week of the disease, was similar between sterile and infected necrosis. However, necrosis was considerably more
extended in patients with infected necrosis (Table 5).
In the group with sterile necrosis, 56/57 patients were
managed conservatively. In a woman with chronic lymphatic leukemia and sterile necrosis and early multiple
organ failure (renal, pulmonary, cardiocirculatory, and metabolic), the study protocol was violated despite a negative
FNA because of severe, rapid deterioration while receiving
Table 4.
intensive care treatment. Surgical necrosectomy was carried
out on day 11 after onset of symptoms. Intraoperative cultures were negative. After surgery, renal function and respiratory parameters improved. On day 18 an infection with
methicillin-resistant Staphylococcus aureus and Candida
albicans occurred, and the patient died on day 25 of septic
multiple organ failure. Of the 56 patients managed conservatively, one patient with severe chronic alcohol disease
died on day 13 of severe respiratory distress syndrome, not
responding to resuscitation. Autopsy revealed massive necrosis retroperitoneally and severe diffuse lung injury. The
death rate in patients with sterile necrosis managed without
surgery was therefore 1.8% (1/56).
Fifteen patients (15/57; 26%) fulfilled the criteria for
FNA. In these patients, 18 FNAs were performed, showing
negative Gram stain as well as negative culture results
(Table 6). The first FNA in these patients was performed on
day 12 (range 4 22) after onset of symptoms.
CHARACTERISTICS OF PATIENTS WITH STERILE AND INFECTED NECROSIS
Female
Male
Mean age (range)
Biliary cause
Alcohol
Other or undefined cause
Mean serum c-reactive protein in mg/L (range)*
Mean Ranson score (range)
Mean APACHE II score (range)*
Mean hospital stay in days (range)
Surgical treatment (%)
Hospital deaths
IPN, infected pancreatic necrosis; SPN, sterile pancreatic necrosis.
* Peak value in the first week of disease.
SPN
(n 57)
IPN
(n 29)
20
37
56.1 (2887)
22 (39%)
23
12
222 (112343)
3.8 (08)
12.2 (528)
23.5 (1185)
1 (2%)
2 (3.5%)
11
18
57.6 (2975)
16 (55%)
9
4
231 (101456)
4.2 (07)
13.2 (622)
84.8 (22209)
27 (93%)
7 (24%)
NS
NS
NS
NS
.001
.0001
.01
Treatment of Necrotizing Pancreatitis
Vol. 232 No. 5
Table 5. MAXIMUM EXTENT OF
NECROSIS ACCORDING TO COMPUTED
TOMOGRAPHY FINDINGS
Extent of Necrosis
30% of the pancreas
3050% of the pancreas
50% of the pancreas
623
Table 7. TREATMENT RESULTS IN
PATIENTS WITH INFECTED NECROSIS
AND SURGICAL TREATMENT (n 27)
SPN
(n 57)
IPN
(n 29)
32 (56%)
16 (28%)
9 (16%)
3 (10%)
3 (10%)
23 (80%)
.00001
NS
.00001
IPN, infected pancreatic necrosis; SPN, sterile pancreatic necrosis.
Time of onset of pain until infection in days
Day of first surgical intervention
Duration of lavage (days)
Reoperation
Additional interventional procedure
Complications
Bleeding
Pancreatic fistula
Burst abdomen
Pseudocyst
20.8 (1048)
21.7 (1049)
37.6 (10124)
6 (22%)
3 (11%)
12 (44%)
2 (7%)
8 (29%)
1 (4%)
1 (4%)
Follow-Up
Values are mean and range or number of patients percentage.
During the study period, 11 patients (19%) were readmitted to the hospital after a mean of 6.9 months for various
pancreatitis-related complications such as recurrent pancreatitis (n 4), pancreatic pseudocyst (n 4), duodenal
obstruction (n 2), and splenic vein thrombosis (n 1).
One patient initially classified as and treated for sterile
necrosis was now found to suffer from infected necrosis.
This patient was readmitted after being at home for 14 days
and subsequently underwent necrosectomy and postoperative lavage of the retroperitoneal cavity. The patient recovered after the second hospital admission. In four patients a
pseudocyst was treated with a cystojejunostomy after a
mean of 4.25 months (range 2 6). In none of them was the
pseudocyst infected.
Of eight monocultures diagnosed in the preoperative FNA,
seven were confirmed by intraoperative cultures. In the
eighth, intraoperative culture results showed a polymicrobial infection. The result of 18 polymicrobial infections
found by FNA was confirmed in 17 by intraoperative cultures. In the remaining one, intraoperative culture revealed
gram-negative infection only. Thus, 92% (24/26) of the
FNA findings were correct with regard to the microbiologic
differentiation. Overall, 27 of 28 patients (96%) were correctly diagnosed as having infected necrosis.
Infected Necrosis
FNA Results
In 27 patients with NP, preoperative CT-guided FNA
revealed infected pancreatic necrosis. The first FNA was
performed a mean of 17 days (range 3 48) after onset of
symptoms. In one patient with infected necrosis, contrastenhanced CT demonstrated air in the necrotic areas, indicating infection. This patient underwent surgery without a
prior FNA. In another patient who subsequently died, FNA
was negative despite pancreatic infection, and the patient
was managed conservatively. In 26 patients both preoperative FNA and intraoperative culture results were available.
Table 6. PATIENTS UNDERGOING SINGLE
OR MULTIPLE FINE-NEEDLE
ASPIRATIONS
Number of
Aspirations
Sterile Necrosis
(15 patients)
Infected Necrosis
(28 patients)
1
2
3
3
12
3
0
0
16
6
5
1
Surgical Treatment
A total of 27 patients with infected necrosis underwent
necrosectomy and subsequent continuous lavage of the necrotic cavity by means of double-lumen drainage tubes.23
Treatment parameters of these patients are outlined in Table
7 and bacteriologic results are summarized in Table 8. There
were 18 patients with polymicrobial and 10 patients with
monomicrobial infection. Different fungus species were
found in eight patients (29%), or 17% of all positive cultures. In one patient with rapidly progressing multiple organ
Table 8. BACTERIOLOGIC FINDINGS IN
28 PATIENTS WITH INFECTED NECROSIS
Germ
Number of positive cultures (n
47) (% of all positive cultures)
Staphylococcus spp.
Candida
Enterococcus
Escherichia coli
Klebsiella spp.
Streptococcus spp.
Pseudomonas aeruginosa
Morganella morgani
Bacteroides fragilis
17 (36%)
8 (17%)
6 (13%)
5 (11%)
4 (9%)
3 (6%)
2 (4%)
1 (2%)
1 (2%)
Intraoperative culture results of 27 patients undergoing surgery and fine-needle
aspiration result from one patient who had a fine-needle aspiration only.
624
Buchler and Others
failure, infection was proven by FNA on day 15, but the
patient died that same day before surgery was performed.
Another patient who had three FNAs with negative results
responded to intensive care unit treatment and conservative
management. Back on a regular ward, he suddenly was
found dead in his bed. Autopsy revealed multiple septic
pulmonary emboli and infected pancreatic necrosis. Thus,
only 27 of 29 patients with infected pancreatic necrosis
underwent surgery.
The death rate in patients with infected necrosis was 24%
(7/29). Causes of death were nonresponding multiple organ
failure (n 4), myocardial infarction/insufficiency (n 2),
and multiple septic pulmonary emboli (n 1).
Follow-Up
During the study period, seven patients (32%) were readmitted to the hospital after a mean of 4 months (range
1.5 6) for various pancreatitis-related complications: persistent pancreatic fistula (n 3), recurrent pancreatitis (n
1), pancreatic pseudocyst (n 1), pancreatic abscess (n
1), and chronic pain (n 1). The patient with the abscess
was successfully treated by a percutaneous drainage procedure. Two of the patients readmitted because of a fistula
were managed conservatively; one patient was treated surgically. The pancreatic pseudocyst was surgically drained
with a cystojejunostomy. All seven patients recovered and
were discharged home.
Intent-to-Treat Analysis
Analysis of the patients in an intent-to-treat manner (nonsurgical vs. surgical treatment) showed that 3/58 (5%) died
while receiving conservative management (1 patient with
sterile necrosis, 2 patients with infected necrosis) and 6/28
(21%) died after surgery (5 with infected necrosis, 1 with
sterile necrosis) (P .05). This intent-to-treat analysis
seems necessary because in the patients whose NP was
managed without surgery, two died in whom infection of
necrosis was not diagnosed in a timely fashion.
DISCUSSION
The concept of conservative treatment of severe acute
pancreatitis originates from several sources. First, we
learned that an episode of severe acute pancreatitis
progresses in two phases. The first 10 to 14 days are
characterized by a systemic inflammatory response syndrome maintained by the release of various inflammatory
mediators.3,4 The production of such mediators in large
amounts may lead to distant organ failure, and surgery does
not seem to be the appropriate intervention at that stage of
the disease. Second, intensive care treatment has improved
significantly during the past decade, and patients with severe acute pancreatitis are best managed there.31 Third,
septic complications in the second phase of the disease can
be reduced and delayed by using appropriate antibiot-
Ann. Surg. November 2000
ics.16,21,22,32 Fourth, one previous study provided evidence
that conservative management is feasible in patients with
sterile necrosis.24
Our study demonstrates and confirms that conservative
treatment of sterile necrosis using early antibiotics is safe
and effective. Of 56 patients with sterile NP managed without surgery, 1 patient died of severe respiratory distress
syndrome. Recent prospective controlled trials have demonstrated that the prevalence of pancreatic infection in NP
could be lowered significantly to 10% to 43% if antibiotics
with proven efficacy in acute pancreatitis were given early.17,19,33 Our trial supports this by showing an infection
rate of 34% in NP, which is lower than the prevalence data
of up to 70% from the 1980s observed in patients not
receiving antibiotic treatment prophylactically.8,34,35 Pancreatic infection is regarded as the main risk factor for death
in patients with acute pancreatitis,9 and preventing this risk
factor seems to represent a major step forward in the management of NP. This statement is further supported by the
data from several contemporary randomized studies that
have been subjected to meta-analysis, showing an improvement in outcome associated with antibiotic treatment.21,22,32
Consequently, a significant body of clinicians use antibiotic
prophylaxis in the initial treatment of patients with predicted severe disease.36 Ruling out infection in NP and
thereby preventing surgical measures, which are still standard approaches for infected necrosis, might reduce hospital
expenses considerably in the future. Data from other groups
argue for surgical treatment in sterile necrosis, particularly
in patients with ongoing multiple organ failure or local
complications such as an inflammatory enlargement of the
pancreas causing obstruction of the gastrointestinal tract or
common bile duct.25,26 Our trial demonstrates that 33 of 35
patients with sterile necrosis and organ failure responded
well to intensive care treatment including mechanical ventilation, catecholamine treatment for cardiocirculatory failure, and hemodialysis for renal failure. However, in our
series one patient with early multiple organ failure not
responding to intensive care died after surgical necrosectomy for sterile necrosis. It can be presumed that if antibiotic treatment is successful in preventing infection, surgery
in NP might not be able to achieve a better goal than
conservative treatment. Thus, in the event of rapidly progressing multiple organ failure in sterile necrosis, surgical
measures might not overcome this problem, just as conservative treatment does not in the rare cases of so-called
fulminant pancreatitis.37
In our study, severity staging showed no differences
between patients with sterile and infected necrosis. This
finding may be explained by the fact that Ranson and
APACHE II scores were obtained during the first week of
the disease process. The Ranson criteria, by definition, are
recorded in the initial 48 hours. The APACHE II score was
calculated daily and the maximum score in the first week
was taken for statistical analysis. However, infection of
peripancreatic or pancreatic necrosis was diagnosed after a
Vol. 232 No. 5
mean of 21 days. It seems likely that this is why patients
with infected necrosis, despite the initially documented
equal severity of disease, stayed considerably longer in the
hospital and had more organ failures that occurred after the
first week in the hospital. Others have reported similar
results,1 but some have not.5
The reason for the difference in the prevalence of organ
failure, especially in the subgroup of patients with sterile
necrosis, might arise from different criteria for classifying
patients and defining organ failure. Also, in patients with
infected necrosis, contrast-enhanced CT revealed more patients with extended necrosis compared with those with
sterile necrosis. It cannot be determined from our trial
whether our result (i.e., more extensive necrosis in the
patients with infected necrosis) is the cause of the occurrence of infection or whether infection is the cause of the
extended necrosis. Several authors consider extended necrosis (i.e., necrosis of 50% of the pancreas) to be a risk
factor for infection.2,23,38,39 A recent paper demonstrated
that in patients with sterile necrosis, the extent of necrosis
correlated with the frequency of organ failure, whereas
infected necrosis was associated with organ failure irrespective of the extent of necrosis,1 supporting the concept that
infection is the major determinant for the outcome.
The present death rate of 10% in patients with NP closely
parallels the one described by Branum et al,40 who described
50 patients with NP treated with surgery; 12% of them died.
Similar to the results of Bradley and Allen,24 we found a higher
death rate in patients with infected necrosis. However, in two
patients with infected necrosis who ultimately died, the infection was not diagnosed in time and therefore no surgery was
performed. In an intent-to-treat analysis, these deaths were
shifted to the patients with sterile necrosis, thereby rendering
insignificant the difference in death rate between patients with
infected and sterile necrosis.
In this series patients with sterile necrosis were discharged home after a mean of 23.5 days; only three patients
stayed longer than 2 months (see Table 4). None of these
three was readmitted to the hospital for persistent pain or
pancreatitis. According to a recent report,41 it might be
possible that return to work in these patients could be
hastened by performing surgery at 4 weeks if the patient
remains symptomatic.
A second major finding of our trial was that early antibiotic treatment of NP changes the spectrum of bacteria in
patients in whom infection develops. Bacterial translocation
from the gut has been demonstrated to be the main cause of
infection in NP.42 45 Therefore, the bacterial spectrum of
infection has been described as primarily gram-negative and
in part anaerobic. After we administered antibiotics with a
dominant efficacy against gram-negative germs and anaerobes (imipenem/cilastatin), the bacteria in more than half of
our patients with pancreatic infection were found to be
gram-positive. In addition, we found eight patients (29%)
infected with fungus. In a series of 57 patients with NP,
Grewe et al46 described 7 (12%) with fungal infection.
Treatment of Necrotizing Pancreatitis
625
These patients were treated with a mean of four different
antibiotics for a mean of 23 days. Such findings raise the
question of the duration of primary antibiotic treatment (14
days in our trial) and of the need to use agents effective
against gram-positive bacteria and fungi concomitantly or
consecutively. In addition, it is likely that these secondary
infections do not originate in the gut but rather are hospitalacquired, entering the pancreas by means of hematogenous
routes from venous or urinary catheters, tracheal tubes, and
so forth. This argument of nosocomial infection is supported by the time when infection occurred in our trial (later
than 20 days); in earlier studies, approximately 40% of
infections with gram-negative germs occurred within 2
weeks after admission.8,17,19,47 The question of additional
primary or secondary anti gram-positive and antifungal
treatments in NP must be addressed in future clinical trials.
Surgery remains the gold standard in the treatment of
infected pancreatic necrosis,48 and necrosectomy and continuous closed lavage was successful in 67% of our patients
with infected necrosis. However, 22% needed a secondary
intervention and 11% an additional interventional procedure, and the complication rate was 44%. Fernandez-del
Castillo et al41 recently described 64 patients treated surgically and found a single surgical procedure to be sufficient
in 69%. In the present study, infection of necrotic tissue
occurred a mean of 21 days after onset of the disease, and
surgery was performed during the 24 hours after its diagnosis. More than 3 weeks after the onset of the disease, the
demarcation between viable and necrotic tissue is easier to
assess than earlier in the disease process. This approach
decreases the bleeding risk and minimizes the surgeryrelated loss of vital tissue leading to surgery-induced endocrine and exocrine pancreatic insufficiency.49 The same
policy of delaying surgery until demarcation of pancreatic
necrosis is far advanced has been reported by others.41
Recently, considerable interest has been generated in the
nonsurgical management of infected necrosis using truly conservative or interventional measures. Single-center reports in
so far small patient groups have demonstrated that even in
infected necrosis, some patients recover with nonsurgical management.50 It is important to differentiate between infected
necrosis and pancreatic abscess, a condition that has been
shown to respond to interventional treatment.51 Nevertheless,
there might be patients with infected necrosis without multiple
organ failure who would respond to nonsurgical measures
including antibiotics, and future trials need to define this population. To extend this argument, at least from a theoretical
point of view it might be possible that in our group of patients
classified as having sterile necrosis, some might have been
infected and did not undergo FNA because of a silent clinical
course, responding well to conservative management. Indeed,
one patient originally classified as having sterile necrosis was
readmitted to the hospital with infected necrosis 14 days after
the primary discharge.
In summary, the data from our study support the concept of
using conservative treatment for sterile NP versus surgery for
626
Buchler and Others
infected necrosis, an approach that could improve the clinical
success rate in NP in terms of the death rate of the past.
References
1. Isenmann R, Rau B, Beger HG. Bacterial infection and extent of
necrosis are determinants of organ failure in patients with acute necrotizing pancreatitis. Br J Surg 1999; 86:1020 1024.
2. Reber HA, McFadden DW. Indications for surgery in necrotizing
pancreatitis. West J Med 1993; 159(6):704 707.
3. Norman J. The role of cytokines in the pathogenesis of acute pancreatitis. Am J Surg 1998; 175(1):76 83.
4. Gloor B, Reber HA. Effects of cytokines, and other inflammatory mediators on human acute pancreatitis. J Int Care Med 1998; 13(6):305312.
5. Tenner S, Sica G, Hughes M, et al. Relationship of necrosis to organ failure
in severe acute pancreatitis. Gastroenterology 1997; 113(3):899903.
6. Beger HG, Bittner R, Buchler M, et al. Hemodynamic data pattern in
patients with acute pancreatitis. Gastroenterology 1986; 90(1):74 79.
7. Knoefel WT, Kollias N, Warshaw AL, et al. Pancreatic microcirculatory changes in experimental pancreatitis of graded severity in the rat.
Surgery 1994; 116(5):904 913.
8. Beger HG, Bittner R, Block S, Buchler M. Bacterial contamination of
pancreatic necrosis. A prospective clinical study. Gastroenterology
1986; 91(2):433 438.
9. Uhl W, Schrag HJ, Wheatley AM, Buchler MW. The role of infection
in acute pancreatitis. Dig Surg 1994; 11:214 219.
10. Gerzof SG, Banks PA, Robbins AH, et al. Early diagnosis of pancreatic infection by computed tomography-guided aspiration. Gastroenterology 1987; 93(6):13151320.
11. Beger HG, Rau B, Mayer J, Pralle U. Natural course of acute pancreatitis. World J Surg 1997; 21(2):130 135.
12. Bassi C, Falconi M, Girelli F, et al. Microbiological findings in severe
pancreatitis. Surg Res Comm 1989; 5:1 4.
13. Bradley EL. Antibiotics in acute pancreatitis. Current status and future
directions. Am J Surg 1989; 158(5):472 477.
14. Buchler M, Uhl W, Beger HG. Complications of acute pancreatitis and
their management. Curr Opin Gen Surg 1993:282286.
15. Schmid SW, Uhl W, Friess H, et al. The role of infection in acute
pancreatitis. Gut 1999; 45(2):311.
16. Buchler M, Malfertheiner P, Friess H, et al. Human pancreatic tissue
concentration of bactericidal antibiotics. Gastroenterology 1992;
103(6):19021908.
17. Luiten EJ, Hop WC, Lange JF, Bruining HA. Controlled clinical trial
of selective decontamination for the treatment of severe acute pancreatitis. Ann Surg 1995; 222(1):57 65.
18. Pederzoli P, Bassi C, Vesentini S, Campedelli A. A randomized
multicenter clinical trial of antibiotic prophylaxis of septic complications in acute necrotizing pancreatitis with imipenem. Surg Gynecol
Obstet 1993; 176(5):480 483.
19. Sainio V, Kemppainen E, Puolakkainen P, et al. Early antibiotic treatment
in acute necrotising pancreatitis. Lancet 1995; 346(8976):663 667.
20. Schwarz M, Isenmann R, Meyer H, Beger HG. [Antibiotic use in
necrotizing pancreatitis. Results of a controlled study]. Dtsch Med
Wochenschr 1997; 122(12):356 361.
21. Powell J, Miles R, Siriwardena A. Antibiotic prophylaxis in the initial
management of severe acute pancreatitis. Br J Surg 1998; 85:582587.
22. Golub R, Siddiqi F, Pohl D. Role of antibiotics in acute pancreatitis: a
meta-analysis. J Gastrointest Surg 1998; 2:496 503.
23. Beger HG, Buchler M, Bittner R, et al. Necrosectomy and postoperative local lavage in necrotizing pancreatitis. Br J Surg 1988; 75(3):
207212.
24. Bradley EL, Allen K. A prospective longitudinal study of observation
versus surgical intervention in the management of necrotizing pancreatitis. Am J Surg 1991; 161(1):19 25.
25. Rau B, Pralle U, Uhl W, et al. Management of sterile necrosis in
instances of severe acute pancreatitis. J Am Coll Surg 1995; 181(4):
279 288.
Ann. Surg. November 2000
26. Rattner DW, Legermate DA, Lee MJ, et al. Surgical debridement of
symptomatic pancreatic necrosis is beneficial irrespective of infection.
Am J Surg 1992; 163:105110.
27. Levitt MD, Eckfeldt JH. Diagnosis of acute pancreatitis. In: Go VLW,
Dimagno EP, Gardner JD, et al, eds. The Pancreas: Biology, Pathobiology, and Disease. New York: Raven Press; 1993:613 635.
28. Uhl W, Buchler MW, Malfertheiner P, et al. A randomized, doubleblind, multicenter trial of octreotide in moderate to severe acute
pancreatitis. Gut 1999; 45:97104.
29. Buchler M, Malfertheiner P, Uhl W, et al. Gabexate mesylate in human
acute pancreatitis. Gastroenterology 1993; 104:11651170.
30. Sakorafas GH, Tsiotos GG, Sarr MG. Extrapancreatic necrotizing
pancreatitis with viable pancreas: a previously underappreciated entity.
J Am Coll Surg 1999; 188(6):643 648.
31. Sigurdsson GH. Intensive care management of acute pancreatitis. Dig
Surg 1994; 11:231241.
32. Wyncoll D. The management of severe acute necrotizing pancreatitis:
an evidence-based review of the literature. Intensive Care Med 1999;
25:146 156.
33. Bassi C, Falconi M, Talamini G, et al. Controlled clinical trial of
pefloxacin versus imipenem in severe acute pancreatitis. Gastroenterology 1998; 115:15131517.
34. Rattner DW, Warshaw AL. Surgical intervention in acute pancreatitis.
Crit Care Med 1988; 16(1):89 95.
35. Frey CF, Bradley EL, Beger HG. Progress in acute pancreatitis. Surg
Gynecol Obstet 1988; 167(4):282286.
36. Powell JJ, Campbell E, Johnson CD, Siriwardena AK. Survey of
antibiotic prophylaxis in acute pancreatitis in the UK and Ireland. Br J
Surg 1999; 86(3):320 322.
37. Farthmann EH, Lausen M, Schoffel U. Indications for surgical treatment of
acute pancreatitis. Hepatogastroenterology 1993; 40(6):556562.
38. Reber HA, Truman HS. Surgical intervention in necrotizing pancreatitis. Gastroenterology 1986; 91:479 481.
39. McFadden DW, Reber HA. Indications for surgery in severe acute
pancreatitis. Int J Pancreatol 1994; 15(2):8390.
40. Branum G, Galloway J, Hirchowitz W, et al. Pancreatic necrosis:
results of necrosectomy, packing, and ultimate closure over drains.
Ann Surg 1998; 227:870 877.
41. Fernandez-del Castillo C, Rattner DW, Makary MA, et al. Debridement and closed packing for the treatment of necrotizing pancreatitis.
Ann Surg 1998; 228:676 684.
42. Moody FG, Haley-Russell D, Muncy DM. Intestinal transit and bacterial translocation in obstructive pancreatitis. Dig Dis Sci 1995;
40:1798 1804.
43. Runkel NS, Moody FG, Smith GS, et al. The role of the gut in the development of sepsis in acute pancreatitis. J Surg Res 1991; 51(1):1823.
44. Widdison AL, Karanjia ND, Reber HA. Routes of spread of pathogens
into the pancreas in a feline model of acute pancreatitis. Gut 1994;
35:1306 1310.
45. Widdison AL, Alvarez C, Chang YB, et al. Sources of pancreatic
pathogens in acute pancreatitis in cats. Pancreas 1994; 9:536 541.
46. Grewe M, Tsiotos GG, Luque de-Leon E, Sarr MG. Fungal infection
in acute necrotizing pancreatitis. J Am Coll Surg 1999; 188:408 414.
47. Beger HG. Surgical management of necrotizing pancreatitis. Surg Clin
North Am 1989; 69:529 549.
48. Gloor B, Uhl W, Buchler MW. Changing concepts in the surgical
management of acute pancreatitis. Baillie`res Clin Gastroenterol 1999;
13:303315.
49. Aultman DF, Bilton BD, Zibari GB, et al. Nonoperative therapy for
acute necrotizing pancreatitis. Am Surg 1997; 63:1114 1117.
50. Freeny PC, Hauptmann E, Althaus SJ, et al. Percutaneous CT-guided
catheter drainage of infected acute necrotizing pancreatitis: techniques
and results. Am J Roentgenol 1998; 170(4):969 975.
51. Bradley EL. A clinically based classification system for acute pancreatitis. Arch Surg 1993; 128:586 590.
You might also like
- Top Trials in Gastroenterology & HepatologyFrom EverandTop Trials in Gastroenterology & HepatologyRating: 4.5 out of 5 stars4.5/5 (7)
- Clinical Pancreatology: For Practising Gastroenterologists and SurgeonsFrom EverandClinical Pancreatology: For Practising Gastroenterologists and SurgeonsJuan Enrique Dominguez-MunozNo ratings yet
- Clinical-Liver, Pancreas, and Biliary TractDocument8 pagesClinical-Liver, Pancreas, and Biliary TractKirsten HartmanNo ratings yet
- Pancreatic ®stula After Pancreatic Head ResectionDocument7 pagesPancreatic ®stula After Pancreatic Head ResectionNicolas RuizNo ratings yet
- General Surgery: Ruptured Liver Abscess: A Novel Surgical TechniqueDocument3 pagesGeneral Surgery: Ruptured Liver Abscess: A Novel Surgical TechniqueRahul SinghNo ratings yet
- Liver, Pancreas and Biliary Tract Problems: Research JournalDocument13 pagesLiver, Pancreas and Biliary Tract Problems: Research JournalElaine Frances IlloNo ratings yet
- Impact of Postoperative Morbidity On Long-Term Survival After OesophagectomyDocument10 pagesImpact of Postoperative Morbidity On Long-Term Survival After OesophagectomyPutri PadmosuwarnoNo ratings yet
- Management of Infected Pancreatic Necrosis 65Document4 pagesManagement of Infected Pancreatic Necrosis 65zahir_jasNo ratings yet
- Systematized Management of Postoperative Enterocutaneous Fistulas. A 14 Years ExperienceDocument5 pagesSystematized Management of Postoperative Enterocutaneous Fistulas. A 14 Years ExperienceYacine Tarik AizelNo ratings yet
- Effect of Antibiotic Prophylaxis On Acute Necrotizing Pancreatitis: Results of A Randomized Controlled TrialDocument7 pagesEffect of Antibiotic Prophylaxis On Acute Necrotizing Pancreatitis: Results of A Randomized Controlled TrialKirsten HartmanNo ratings yet
- 72-Manuscript Word File (STEP 1) - 98-3-10-20180605Document5 pages72-Manuscript Word File (STEP 1) - 98-3-10-20180605Hamza AhmedNo ratings yet
- Early Use of TIPS in Cirrhosis and Variceal BleedingDocument10 pagesEarly Use of TIPS in Cirrhosis and Variceal Bleedingray liNo ratings yet
- Song 2017Document8 pagesSong 2017Patricia BezneaNo ratings yet
- Research Article Challenges Encountered During The Treatment of Acute Mesenteric IschemiaDocument9 pagesResearch Article Challenges Encountered During The Treatment of Acute Mesenteric IschemiaDyah RendyNo ratings yet
- Diagnosis and Proper Treatment of Renal Abscesses Remains A Challenge For PhysiciansDocument6 pagesDiagnosis and Proper Treatment of Renal Abscesses Remains A Challenge For PhysiciansDevraj ChoudhariNo ratings yet
- Abdominal Sepsis Prognostic FactorDocument6 pagesAbdominal Sepsis Prognostic FactorPrasojo JojoNo ratings yet
- Jurnal: Acute PancreatitisDocument11 pagesJurnal: Acute Pancreatitisahmad fachryNo ratings yet
- Jurnal DhaDocument11 pagesJurnal DhasiydahNo ratings yet
- Indicación RelaparotomiaDocument6 pagesIndicación RelaparotomiaJohnHarvardNo ratings yet
- Acute Appendicitis in Adults ManagementDocument16 pagesAcute Appendicitis in Adults ManagementPriscila Tobar AlcántarNo ratings yet
- Acute Appendicitis in AdultsDocument19 pagesAcute Appendicitis in Adultsdimi firmatoNo ratings yet
- Colitis Induced ChemotherapyDocument11 pagesColitis Induced Chemotherapyhandris yanitraNo ratings yet
- EchografyDocument6 pagesEchografyMiha ElaNo ratings yet
- Early Ercp and Papillotomy Compared With Conservative Treatment For Acute Biliary PancreatitisDocument6 pagesEarly Ercp and Papillotomy Compared With Conservative Treatment For Acute Biliary PancreatitisRT_BokNo ratings yet
- Cleveland Clinic Journal of Medicine 2013 BARON 354 9Document6 pagesCleveland Clinic Journal of Medicine 2013 BARON 354 9Stephanie PlascenciaNo ratings yet
- Jurnal Ebn PerikarditisDocument13 pagesJurnal Ebn Perikarditistino prima dito100% (1)
- Analysis of Antibiotics Selection in Patients Undergoing Appendectomy in A Chinese Tertiary Care HospitalDocument5 pagesAnalysis of Antibiotics Selection in Patients Undergoing Appendectomy in A Chinese Tertiary Care HospitalYuanico LiraukaNo ratings yet
- Management of Acute Upper Gastrointestinal Bleeding: Urgent Versus Early EndosDocument5 pagesManagement of Acute Upper Gastrointestinal Bleeding: Urgent Versus Early EndossamuelNo ratings yet
- Management of Acute Upper Gastrointestinal Bleeding: Urgent Versus Early EndosDocument5 pagesManagement of Acute Upper Gastrointestinal Bleeding: Urgent Versus Early EndosCarolina Ormaza GiraldoNo ratings yet
- Elterman 2014Document3 pagesElterman 2014Ana Luisa DantasNo ratings yet
- Early Management of Acute Pancreatitis-A Review of The Best Evidence. Dig Liver Dis 2017Document32 pagesEarly Management of Acute Pancreatitis-A Review of The Best Evidence. Dig Liver Dis 2017América FloresNo ratings yet
- PimpaleDocument6 pagesPimpaleMariano BritoNo ratings yet
- Modern Management of Pyogenic Hepatic Abscess: A Case Series and Review of The LiteratureDocument8 pagesModern Management of Pyogenic Hepatic Abscess: A Case Series and Review of The LiteratureAstari Pratiwi NuhrintamaNo ratings yet
- Acute Pyelonephritis in Adults: A Case Series of 223 PatientsDocument6 pagesAcute Pyelonephritis in Adults: A Case Series of 223 PatientsshiaNo ratings yet
- Liver A BSC DrainDocument8 pagesLiver A BSC DrainAngelica AmesquitaNo ratings yet
- Apendisitis MRM 3Document8 pagesApendisitis MRM 3siti solikhaNo ratings yet
- (The Clinics - Surgery) Steve Behrman MD FACS, Ron Martin MD FACS - Modern Concepts in Pancreatic Surgery, An Issue of Surgical Clinics, 1e (2013, Elsevier)Document197 pages(The Clinics - Surgery) Steve Behrman MD FACS, Ron Martin MD FACS - Modern Concepts in Pancreatic Surgery, An Issue of Surgical Clinics, 1e (2013, Elsevier)Yee Wei HoongNo ratings yet
- Organ-Specific InfectionsDocument4 pagesOrgan-Specific InfectionsMin dela FuenteNo ratings yet
- 260-Article Text-875-1-10-20220728Document4 pages260-Article Text-875-1-10-20220728hasan andrianNo ratings yet
- US en EndometritisDocument7 pagesUS en EndometritisRubí FuerteNo ratings yet
- Management of Infected Pancreatic Necrosis: State of The ArtDocument9 pagesManagement of Infected Pancreatic Necrosis: State of The ArtSares DaselvaNo ratings yet
- 1 s2.0 S001650850862925X MainDocument2 pages1 s2.0 S001650850862925X MainMirza RisqaNo ratings yet
- Outcome and Clinical Characteristics in Pleural Empyema: A Retrospective StudyDocument7 pagesOutcome and Clinical Characteristics in Pleural Empyema: A Retrospective StudylestarisurabayaNo ratings yet
- Journal Reading Acute Pancreatitis SurgeryDocument17 pagesJournal Reading Acute Pancreatitis Surgeryimanda rahmatNo ratings yet
- Appropriate Antibiotics For Peritonsillar Abscess - A 9 Month CohortDocument5 pagesAppropriate Antibiotics For Peritonsillar Abscess - A 9 Month CohortSiti Annisa NurfathiaNo ratings yet
- PylonefritisDocument8 pagesPylonefritissintaNo ratings yet
- Cholelithiasis: Causative Factors, Clinical Manifestations and ManagementDocument6 pagesCholelithiasis: Causative Factors, Clinical Manifestations and ManagementmusdalifahNo ratings yet
- Wja 3 1Document12 pagesWja 3 1Atuy NapsterNo ratings yet
- Cholangitis: Causes, Diagnosis, and ManagementDocument10 pagesCholangitis: Causes, Diagnosis, and ManagementDianaNo ratings yet
- Manejo Del ResangradoDocument13 pagesManejo Del ResangradoRudy J CoradoNo ratings yet
- Multiple Episodes of Hypoglycemia Secondary To An Insulinoma Case ReportDocument4 pagesMultiple Episodes of Hypoglycemia Secondary To An Insulinoma Case ReportmiguelNo ratings yet
- 1 PBDocument3 pages1 PBMartynaNo ratings yet
- New England Journal Medicine: The ofDocument10 pagesNew England Journal Medicine: The ofPablo BarraganNo ratings yet
- Critical Apprisal of A Prospective StudyDocument7 pagesCritical Apprisal of A Prospective StudyVK LabasanNo ratings yet
- The Clinical Outcomes and Predictive Factors For.24Document5 pagesThe Clinical Outcomes and Predictive Factors For.24KeziaNo ratings yet
- CasAre There Risk Factors For Splenic Rupture During Colonoscopy CaseDocument6 pagesCasAre There Risk Factors For Splenic Rupture During Colonoscopy Caseysh_girlNo ratings yet
- Etiology, Treatment Outcome and Prognostic Factors Among Patients With Secondary Peritonitis at Bugando Medical Centre, Mwanza, TanzaniaDocument13 pagesEtiology, Treatment Outcome and Prognostic Factors Among Patients With Secondary Peritonitis at Bugando Medical Centre, Mwanza, Tanzaniayossy aciNo ratings yet
- Complications of Pancreatic SurgeryDocument5 pagesComplications of Pancreatic Surgeryhenok seifeNo ratings yet
- Acute Colonic Pseudo-ObstructionDocument4 pagesAcute Colonic Pseudo-ObstructionJosé Luis Navarro Romero100% (1)
- Pill in Pocket NEJMDocument8 pagesPill in Pocket NEJMn2coolohNo ratings yet
- Marketing FinalDocument15 pagesMarketing FinalveronicaNo ratings yet
- Benevisión N15 Mindray Service ManualDocument123 pagesBenevisión N15 Mindray Service ManualSulay Avila LlanosNo ratings yet
- (500eboard) Version Coding Model 140 As of MY 1995Document1 page(500eboard) Version Coding Model 140 As of MY 1995Saimir SaliajNo ratings yet
- Appendix - Pcmc2Document8 pagesAppendix - Pcmc2Siva PNo ratings yet
- An Exploration of The Ethno-Medicinal Practices Among Traditional Healers in Southwest Cebu, PhilippinesDocument7 pagesAn Exploration of The Ethno-Medicinal Practices Among Traditional Healers in Southwest Cebu, PhilippinesleecubongNo ratings yet
- FMC Derive Price Action GuideDocument50 pagesFMC Derive Price Action GuideTafara MichaelNo ratings yet
- Vendor Information Sheet - LFPR-F-002b Rev. 04Document6 pagesVendor Information Sheet - LFPR-F-002b Rev. 04Chelsea EsparagozaNo ratings yet
- Plaza 66 Tower 2 Structural Design ChallengesDocument13 pagesPlaza 66 Tower 2 Structural Design ChallengessrvshNo ratings yet
- Soft Ground Improvement Using Electro-Osmosis.Document6 pagesSoft Ground Improvement Using Electro-Osmosis.Vincent Ling M SNo ratings yet
- Carriage RequirementsDocument63 pagesCarriage RequirementsFred GrosfilerNo ratings yet
- Psychological Contract Rousseau PDFDocument9 pagesPsychological Contract Rousseau PDFSandy KhanNo ratings yet
- Pt3 English Module 2018Document63 pagesPt3 English Module 2018Annie Abdul Rahman50% (4)
- ISO 9001 2015 AwarenessDocument23 pagesISO 9001 2015 AwarenessSeni Oke0% (1)
- User S Manual AURORA 1.2K - 2.2KDocument288 pagesUser S Manual AURORA 1.2K - 2.2KEprom ServisNo ratings yet
- School of Mathematics 2021 Semester 1 MAT1841 Continuous Mathematics For Computer Science Assignment 1Document2 pagesSchool of Mathematics 2021 Semester 1 MAT1841 Continuous Mathematics For Computer Science Assignment 1STEM Education Vung TauNo ratings yet
- Lecturenotes Data MiningDocument23 pagesLecturenotes Data Miningtanyah LloydNo ratings yet
- Objective & Scope of ProjectDocument8 pagesObjective & Scope of ProjectPraveen SehgalNo ratings yet
- DQ Vibro SifterDocument13 pagesDQ Vibro SifterDhaval Chapla67% (3)
- 3 Carbohydrates' StructureDocument33 pages3 Carbohydrates' StructureDilan TeodoroNo ratings yet
- DarcDocument9 pagesDarcJunior BermudezNo ratings yet
- Dynamics of Machinery PDFDocument18 pagesDynamics of Machinery PDFThomas VictorNo ratings yet
- Turning PointsDocument2 pagesTurning Pointsapi-223780825No ratings yet
- Manual s10 PDFDocument402 pagesManual s10 PDFLibros18No ratings yet
- Leigh Shawntel J. Nitro Bsmt-1A Biostatistics Quiz No. 3Document6 pagesLeigh Shawntel J. Nitro Bsmt-1A Biostatistics Quiz No. 3Lue SolesNo ratings yet
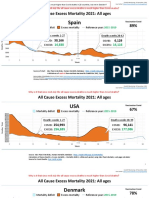
- Countries EXCESS DEATHS All Ages - 15nov2021Document21 pagesCountries EXCESS DEATHS All Ages - 15nov2021robaksNo ratings yet
- Report On GDP of Top 6 Countries.: Submitted To: Prof. Sunil MadanDocument5 pagesReport On GDP of Top 6 Countries.: Submitted To: Prof. Sunil MadanAbdullah JamalNo ratings yet
- Dokumen - Pub - Bobs Refunding Ebook v3 PDFDocument65 pagesDokumen - Pub - Bobs Refunding Ebook v3 PDFJohn the First100% (3)
- Dalasa Jibat MijenaDocument24 pagesDalasa Jibat MijenaBelex ManNo ratings yet
- Application Activity Based Costing (Abc) System As An Alternative For Improving Accuracy of Production CostDocument19 pagesApplication Activity Based Costing (Abc) System As An Alternative For Improving Accuracy of Production CostM Agus SudrajatNo ratings yet
- Hole CapacityDocument2 pagesHole CapacityAbdul Hameed OmarNo ratings yet