Professional Documents
Culture Documents
Persistent Fetal Vasculature
Uploaded by
dewishinta12Original Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Persistent Fetal Vasculature
Uploaded by
dewishinta12Copyright:
Available Formats
Artigo Original | Original Article
Persistent fetal vasculature: ocular features, management of cataract and outcomes
Persistncia da vasculatura fetal: caractersticas oftalmolgicas, manuseio da catarata e resultados cirrgicos
Marcia Beatriz Tartarella1, Rodrigo Ueno Takahagi1, Ana Paula Braga2, Joo Borges Fortes Filho3
ABSTRACT
RESUMO
Purposes: To describe ocular features, management of cataract and functional
outcomes in patients with persistent fetal vasculature.
Methods: Retrospective, descriptive case series of patients with persistent fetal
vasculature. Data were recorded from the Congenital Cataract Section of Federal
University of So Paulo, Brazil from 2001 to 2012. All patients were evaluated for
sex, age at diagnosis, systemic findings, laterality, age at surgery, and initial and
final follow-up visual acuities. Follow-up and complications after cataract surgery
were recorded. Ultrasound was performed in all cases and ocular eco-Doppler
was performed in most.
Results: The study comprised 53 eyes from 46 patients. Age at diagnosis ranged
from 5 days of life to 10 years-old (mean 22.7 months). Twenty-seven patients
were male (58.7%). Persistent fetal vasculature was bilateral in 7 patients (15.2%).
Forty-two eyes (79.2%) had combined (anterior and posterior forms) PFV presentation, 5 eyes (9.4%) had only anterior persistent fetal vasculature presentation
and 6 eyes (11.3%) had posterior persistent fetal vasculature presentation. Thirtyeight eyes (71.7%) were submitted to cataract surgery. Lensectomy combined
with anterior vitrectomy was performed in 18 eyes (47.4%). Phacoaspiration with
intraocular lens implantation was performed in 15 eyes (39.5%), and without lens
implantation in 5 eyes (13.2%). Mean follow-up after surgery was 44 months. Postoperative complications were posterior synechiae (3 cases), retinal detachment
(2 cases), phthisis (3 cases), posterior capsular opacification (8 cases), inflammatory
pupillary membrane (5 cases), glaucoma (4 cases), intraocular lens implantation
displacement (1 case) and vitreous hemorrhage (2 cases). Complications were
identified in 19 (50%) of the 38 operated eyes. Visual acuity improved after cataract
surgery in 83% of the eyes.
Conclusions: Patients with persistent fetal vasculature have variable clinical presentation. There is an association of persistent fetal vasculature with congenital
cataract. Severe complications are related to cataract surgery in patients with
persistent fetal vasculature, but 83% of the operated eyes improved visual acuity.
Objetivos: Descrever as caractersticas oftalmolgicas, o tratamento da catarata
e os resultados funcionais em pacientes com o diagnstico de persistncia da vasculatura fetal.
Mtodos: Estudo retrospectivo e descritivo de srie de casos de pacientes com persistncia da vasculatura fetal. Dados foram obtidos dos arquivos do Setor de Catarata
Congnita da Universidade Federal de So Paulo, Brasil, durante o perodo entre 2001
a 2012. Todos os pacientes foram avaliados quanto ao sexo, idade ao diagnstico,
achados sistmicos, lateralidade, idade cirurgia e acuidade visual inicial e final ao
seguimento. Complicaes aps a cirurgia da catarata foram analisadas. Ultrassom
foi realizado em todos os casos e eco-Doppler foi realizado na maioria dos pacientes.
Resultados: O estudo incluiu 53 olhos de 46 pacientes. Idade ao diagnstico variou
de 5 dias de vida at 10 anos (mdia 22,7 meses). Vinte e sete pacientes eram masculinos (58,7%). A persistncia da vasculatura fetal foi bilateral em 7 pacientes (15,2%).
Quarenta e dois olhos (79,2%) apresentaram formas combinadas (anterior e posterior)
da persistncia da vasculatura fetal, 5 olhos (9,4%) tinham somente a forma anterior
da persistncia da vasculatura fetal e 6 olhos (11,3%) tinham a forma posterior de
apresentao da persistncia da vasculatura fetal. Trinta e oito olhos (71,7%) foram
operados de catarata. Lensectomia com vitrectomia anterior foi realizada em 18 olhos
(47,4%). Facoaspirao com implante de lente intraocular foi realizada em 15 olhos
(39,5%) e sem implantao de lente em 5 olhos (13,2%). O seguimento mdio aps
cirurgia foi de 44 meses. Complicaes ps-operatrias foram: sinquias posteriores (3
casos), descolamento da retina (2 casos), atrofia do globo ocular (3 casos), opacificao
da cpsula posterior (8 casos), membrana pupilar inflamatria (5 casos), glaucoma
(4 casos), deslocamento da lente implantada (1 caso) e hemorragia vtrea (2 casos).
Complicaes foram identificadas em 19 (50%) dos 38 olhos operados. Acuidade visual
melhorou aps a cirurgia da catarata em 83% dos olhos.
Concluses: Pacientes com persistncia da vasculatura fetal tem apresentaes clnicas
variveis. Existe uma associao da persistncia da vasculatura fetal com catarata
congnita. Complicaes graves so associadas com a cirurgia da catarata nesses
pacientes, mas 83% dos olhos operados melhoraram a acuidade visual nesse estudo.
Keywords: Persistent hyperplastic primary vitreous/pathology; Cataract/congenital; Ophthalmologic surgical procedures
Descritores: Persistncia do vtreo primrio hiperplsico/patologia; Catarata/congnito; Procedimentos cirrgicos oftalmolgicos
INTRODUCTION
Persistent fetal vasculature (PFV) is a congenital developmental
anomaly of the eye resulting from failure of the embryological
primary vitreous and hyaloid vasculature to regress. PVF typically
presents unilaterally without association with systemic findings, but
sometimes PFV may be associated with rare systemic syndromes as
Walker-Warburg anencephaly, oculo-dento-osseous dwarfism, oculopalato-cerebral dwarfism, Patau syndrome, or others(1,2). Bilateral cases
account for less than 10% of the cases(3). Persistent fetal vasculature
can be classified as anterior, posterior and combined forms, according
to the affected intraocular structures. This heterogeneity of clinical
presentation makes PFV a challenge to surgical management(4).
Persistent fetal vasculature is related to congenital cataract(5,6).
However, surgeries for cataract in patients with PFV are more difficult
to perform and are related to higher rates of postoperative complications as: retinal detachment, hyphema, intraocular hemorrhage,
glaucoma, secondary opacification of the visual axis and extensive
inflammatory response with pupillary block(7-10).
Submitted for publication: November 14, 2012
Accepted for publication: March 17, 2013
Funding: No specific financial support was available for this study.
Study performed at Universidade Federal de So Paulo.
Physician, Department of Ophthalmology, School of Medicine, Universidade Federal de Sao Paulo,
Sao Paulo (SP), Brazil.
Orthoptist, Department of Ophthalmology, Universidade Federal de So Paulo, So Paulo (SP), Brazil.
3
Physician, Department of Ophthalmology, School of Medicine, Universidade Federal do Rio Grande
do Sul, Porto Alegre (RS), Brazil.
1
Disclosure of potential conflicts of interest: M.B.Tartarella, None; R.U.Takahagi, None; A.P.Braga,
None; J.B.Fortes Filho, None.
Correspondence address: Joo Borges Fortes Filho. Hospital de Clnicas de Porto Alegre. Rua
Ramiro Barcelos, 2350 - Porto Alegre (RS) - 90035-903 - Brazil
E-mail: jbfortes@prorop.com.br
Arq Bras Oftalmol. 2013;76(3):185-8
185
Persistent fetal vasculature: ocular features, management of cataract and outcomes
This study aims to describe ocular features, management of
cataract and visual acuity (VA) outcomes of patients with PFV after
cataract surgery.
METHODS
Study design
A retrospective, noncomparative and descriptive case series of
patients with PFV were recorded from the files of Congenital Cataract
Section of Federal University of So Paulo, Brazil during the period
from 2001 to 2012.
Patients and ophthalmological examination
All patients were evaluated for sex, age at diagnosis, associated
systemic abnormalities, laterality, biomicroscopic examination,
ocular axial length (contact A-scan measurements), initial and final
follow-up VA, and intraocular pressure. Age at surgery, follow-up period and complications after cataract surgery were recorded. Indirect
ophthalmoscopy and A- and B-scan ultrasonography were performed in all patients in order to evaluate components of anterior and
posterior forms of PVF. Ocular eco-Doppler was performed in most
patients to assess vascular blood flow. Persistent fetal vasculature was
classified according to the structural ocular involvement as anterior,
posterior or combined form(11).
Surgical techniques used for cataract extraction
Lensectomy by 25 gauge bimanual vitrectomy technique was
performed through the pars plicata or limbal approaches. The
nucleus and cortex were aspirated in the bag. Anterior vitrectomy
for removal of the PFV was performed in all cases operated by this
technique. Endodiathermy was used if bleeding or in patients when
the eco-Doppler examination disclosed vascular blood flow inside
the fibrovascular stalk.
Phacoaspiration with or without intraocular lens implantation
(IOL) was performed through limbal incision, lens aspiration and IOL
in the bag implantation. Posterior capsulorhexis, anterior vitrectomy
and fibrovascular stalk management were performed via pars plana
with 25 gauge vitrectomy system. Endodiathermy of permeable fi
brovascular stalk was performed when necessary.
All surgeries were performed under general anesthesia by the
same author (MBT).
Criteria for surgery indication and main outcomes evaluated
Surgery was indicated in cases with VA of 20/150 or less in eyes
with no macular involvement. Exclusion criteria included microph
thalmia and eyes with no light perception.
Postoperative VA and rate of postoperative complications were
obtained. Visual acuity was assessed with age-appropriated tests such
as the Teller Acuity Cards, Lea-Gratings Visual Chart, Snellen Chart, or
Sweep VEP (Sweep Visual Evoked Potentials). Postoperative corrected
distance VA results were compared, when possible, with preoperative
values and classified as: no-change; improvement or deterioration.
Ethics
The authors certify that the study protocol was approved by the
Ethics Committee and that the protocol for the research project is
conforming to the provisions of the Declaration of Helsinki in 1995
(as revised in Edinburgh 2000). Authors declare no financial support
or relationships that may pose a conflict of interest.
RESULTS
The study group comprised 53 eyes from 46 patients. Age at diagnosis ranged from 5 days of life to 10 years-old (mean 22.7 months).
186
Arq Bras Oftalmol. 2013;76(3):185-8
Twenty-seven patients were male (58.7%). Persistent fetal vasculature was bilateral in 7 patients (15.2%) and unilateral in 39 patients
(84.8%). Among the bilateral cases one patient was diagnosed as
Patau syndrome and one patient had juvenile rheumatoid arthritis.
In the entire group the initial VA varied from non-light perception
to 20/50.
Forty-two eyes (79.2%) had combined (anterior and posterior
forms) PFV presentation, 5 eyes (9.4%) had only posterior PFV
presentation and 6 eyes (11.3%) had predominantly anterior PFV
presentation.
Thirty-eight eyes (71.7%) were submitted to cataract surgery.
Age at surgery ranged from one month-age to 4 years (mean 14
months). Initial VA in the operated group of patients varied from light
perception (31 eyes) to 20/150. There was no indication for surgery
in patients with no-light perception and severe microphthalmia.
Lensectomy combined with anterior vitrectomy was performed in 18
eyes (47.4%). Phacoaspiration with IOL implantation was performed
in 15 eyes (39.5%), and without IOL implantation in 5 eyes (13.2%).
Fifteen eyes were not submitted to cataract surgery including one
patient presenting unilateral PFV with VA of 20/50 in the affected eye.
Mean follow-up after surgery was 44 months. Postoperative complications were posterior synechiae (3 cases), retinal detachment
(2 cases), phthisis bulbi (3 cases), posterior capsular opacification
(8 cases), inflammatory pupillary membrane (5 cases), glaucoma (4
cases), IOL displacement (1 case) and vitreous hemorrhage (2 cases).
Those complications were identified in 19 (50%) of the 38 operated
eyes.
Final corrected distance VA was obtained in 36 eyes and VA im
proved after surgery in 83% of eyes. Three eyes (8.3%) developed
phthisis bulbi after surgery and showed no-light perception. A total
of 12 eyes (33%) had final VA under 20/200. Seventeen eyes (47%)
showed VA between 20/200 and 20/40. Three eyes (8.3 %) achieved
20/40 or better.
None of the 15 non-operated eyes improved VA and, in this
group, a total of 6 eyes decreased VA during the follow up period of
the study.
DISCUSSION
This study reported predominance of unilateral cases and both
anterior and posterior PFV presentation. These findings are in agree
ment with some previous published studies(10,11). Some authors
discuss that most cases of unilateral congenital cataracts are due
to different presentations of PFV(5,7), and that minimal fetal vascular
remnants were found in 100% of a case series of 31 patients operated
for unilateral congenital cataract(5).
Cataract surgery in patients with PFV presents different degrees
of difficulty, and initial surgical plan may change depending on the pre
and intraoperative conditions. Ocular eco-Doppler findings showing
extensive blood flow from the optic nerve to the posterior face of the
lens is a predictive factor of possible intraoperative hemorrhage. The
surgeon must be aware of the situation and be prepared with endocoagulation instruments and techniques to deal with the situation.
Intraocular hemorrhage is a common cause of bad prognosis and
poor outcomes in this PFV cases.
Membranous cataract or fibrovascular plaques at pupillary site or
in the retrolental space may need further surgical manipulation with
the use of micro-scissors to create a clear visual axis.
Some eyes with PFV and cataract are associated with variable
degrees of microphthalmia. In these cases, the visual improvement
after cataract surgery may be limited. Early surgical intervention with
microsurgical 25 gauge lensectomy or phacoaspiration techniques
combined with anti-amblyopic therapy resulted in favorable visual
outcome in many operated eyes(10).
Nineteen eyes (50%) presented postoperative complications in
our study. Severe complications as retinal detachment and phthisis
Tartarella MB, et al.
bulbi occurred in 5 eyes (13%) leading to loss of vision in those eyes.
All these five eyes presented microphthalmia, combined form of
PFV, a large stalk with internal blood flow and posterior retinal folds.
Literature report with modern closed chamber cataract surgery in
PFV showed a complication rate of 27%(8).
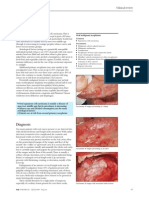
Figure 1. Patient with cataract affecting the visual axis and persistent fetal vasculature.
Figure 2. Ultrasound image of patient with persistent fetal vasculature in combined
(anterior and posterior forms) presentation. Width of the stalk determines poor prognosis
for visual acuity recovery after cataract surgery.
The prognosis after cataract surgery seems to be linked to the
presentation forms of the PFV and associated preoperative ocular
features. Anatomical results depend on the fibrovascular stalk width,
presence of blood flow inside the stalk, type of presentation (anterior,
posterior or combined form of PFV) and associated microphthalmia.
Those variables are associated with the higher incidence of postoperative complications. Visual and functional results depend on age
of lens opacity occurrence (congenital or latter acquired cataract
formation), age at surgery and presence of major or minor macular
involvement.
In our study 82% of the included eyes had initial VA of light perception and final corrected distance VA improved after surgery in
83% of the eyes despite the high rate of complications while none of
the 15 non-operated eyes improved VA. Specific circumstances and
clinical variables, as the occurrence of glaucoma after surgery and
poor adhesion to occlusive therapy with severe amblyopia, may have
also affected the final VA in those children.
New studies concerning cumulative factors that could predict
prognosis for each case are necessary to help ophthalmologists to
decide whether to perform surgery. Among the main pre-operatory
clinical variables are: lens and vitreous opacities affecting the visual
axis (Figure 1), width and occurrence of blood flow inside de stalk
detected by eco-Doppler (Figures 2 and 3), retrolental vascularized
plaque also detected by eco-Doppler (Figure 4), form of PFV presen
tation with major or minimal macular involvement (Figure 5), presence of microphthalmia and patients age at surgery.
The surgeon and patients parents must be aware of severe
postoperative complications after cataract surgery in eyes with PFV
thus causing in some cases poor VA or unfavorable outcomes. Early
diagnosis, early surgery and prompt anti-amblyopic therapy after
cataract surgery are important factors to be considered as functional
prognostic factors.
CONCLUSIONS
Our study related that patients with persistent fetal vasculature
had variable clinical presentations and there is a clear association
of persistent fetal vasculature with congenital cataract. Although
severe complications are related to cataract surgery in patients with
persistent fetal vasculature our study disclosed that more than 80% of
the operated eyes improved visual acuity despite high occurrence of
intra and postoperative complications. Eco-Doppler can help in order
to predict intraoperative hemorrhage and poor visual prognosis in
severe forms of persistent fetal vasculature.
In spite of the limitations of this study regarding its retrospective
and noncomparative design we observed visual acuity improvement
in 83% of the eyes after cataract surgery and anti-amblyopic therapy
in a mean postoperative follow-up of 44 months.
Figure 3. Eco-Doppler showing vascularized stalk from persistent fetal vasculature. Width and vascularization inside the stalk determines poor
prognosis for visual acuity recovery after cataract surgery.
Arq Bras Oftalmol. 2013;76(3):185-8
187
Persistent fetal vasculature: ocular features, management of cataract and outcomes
Figure 4. Eco-Doppler showing retrolental vascularized plaque from persistent fetal vasculature.
Figure 5. Persistent fetal vasculature in predominantly posterior presentation. Left: Major macular involvement suggests poor visual prognosis after
cataract removal. Right: Minor macular involvement indicates better visual acuity after cataract removal.
REFERENCES
1. Alexandrakis G, Scott IU, Flynn HW Jr, Murray TG, Feuer WJ. Visual acuity outcomes
with and without surgery in patients with persistent fetal vasculature. Ophthalmology. 2000;107(6):1068-72.
2. Dhir L, Quinn AG. Persistent fetal vasculature and spontaneous hyphema in a patient
with Klippel-Trnaunay-Weber syndrome. J AAPOS 2010;14(2):190-2.
3. Kumar A, Jethani J, Shetty S, Vijayalakshmi P. Bilateral persistent fetal vasculature: a
study of 11 cases. J AAPOS. 2010;14(4):345-8.
4. Sisk RA, Berrocal AM, Feuer WJ, Murray TG. Visual and anatomic outcomes with
or without surgery in persistent fetal vasculature. Ophthalmology. 2010;117(11):
2178-83.e1-2.
5. Mllner-Eidenbck A, Amon M, Moser E, Klebermass N. Persistent fetal vasculature
and minimal fetal vascular remnants: a frequent cause of unilateral congenital cataracts. Ophthalmology. 2004;111(5):906-13.
6. Mllner-Eidenbck A, Amon M, Hauff W, Klebermass N, Abela C, Moser E. Surgery in
unilateral congenital cataract caused by persistent fetal vasculature or minimal fetal
188
Arq Bras Oftalmol. 2013;76(3):185-8
vascular remnants: age-related findings and management challenges. J Cataract
Refract Surg. 2004;30(3):611-9.
7. Paysse EA, McCreery KM, Coats DK. Surgical management of the lens and retrolenti
cular fibrotic membranes associated with persistent fetal vasculature. J Cataract
Refract Surg. 2002;28(5):816-20. Comment in J Cataract Refract Surg. 2003;29(7):
1250.
8. Vasavada AR, Vasavada SA, Bobrova N, Praveen MR, Shah SK, Vasavada VA, et al. Out
comes of pediatric cataract surgery in anterior persistent fetal vasculature. J Cataract
Refract Surg. 2012;38(5):849-57.
9. Vasavada VA, Dixit NV, Ravat FA, Praveen MR, Shah SK, Vasavada V, et al. Intraoperative
performance and postoperative outcomes of cataract surgery in infant eyes with
microphthalmos. J Cataract Refract Surg. 2009;35(3):519-28.
10. Anteby I, Cohen E, Karshai I, BenEzra D. Unilateral persistent hyperplastic primary
vitreous: course and outcome. J AAPOS. 2002;6(2):92-9.
11. Dass AB, Trese MT. Surgical results of persistent hyperplastic primary vitreous. Oph
thalmology. 1999;106(2):280-4.
You might also like
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeFrom EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeRating: 4 out of 5 stars4/5 (5794)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreFrom EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreRating: 4 out of 5 stars4/5 (1090)
- Never Split the Difference: Negotiating As If Your Life Depended On ItFrom EverandNever Split the Difference: Negotiating As If Your Life Depended On ItRating: 4.5 out of 5 stars4.5/5 (838)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceFrom EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceRating: 4 out of 5 stars4/5 (894)
- Grit: The Power of Passion and PerseveranceFrom EverandGrit: The Power of Passion and PerseveranceRating: 4 out of 5 stars4/5 (587)
- Shoe Dog: A Memoir by the Creator of NikeFrom EverandShoe Dog: A Memoir by the Creator of NikeRating: 4.5 out of 5 stars4.5/5 (537)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureFrom EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureRating: 4.5 out of 5 stars4.5/5 (474)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersFrom EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersRating: 4.5 out of 5 stars4.5/5 (344)
- Her Body and Other Parties: StoriesFrom EverandHer Body and Other Parties: StoriesRating: 4 out of 5 stars4/5 (821)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)From EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Rating: 4.5 out of 5 stars4.5/5 (119)
- The Emperor of All Maladies: A Biography of CancerFrom EverandThe Emperor of All Maladies: A Biography of CancerRating: 4.5 out of 5 stars4.5/5 (271)
- The Little Book of Hygge: Danish Secrets to Happy LivingFrom EverandThe Little Book of Hygge: Danish Secrets to Happy LivingRating: 3.5 out of 5 stars3.5/5 (399)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyFrom EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyRating: 3.5 out of 5 stars3.5/5 (2219)
- The Yellow House: A Memoir (2019 National Book Award Winner)From EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Rating: 4 out of 5 stars4/5 (98)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaFrom EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaRating: 4.5 out of 5 stars4.5/5 (265)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryFrom EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryRating: 3.5 out of 5 stars3.5/5 (231)
- Team of Rivals: The Political Genius of Abraham LincolnFrom EverandTeam of Rivals: The Political Genius of Abraham LincolnRating: 4.5 out of 5 stars4.5/5 (234)
- On Fire: The (Burning) Case for a Green New DealFrom EverandOn Fire: The (Burning) Case for a Green New DealRating: 4 out of 5 stars4/5 (73)
- The Unwinding: An Inner History of the New AmericaFrom EverandThe Unwinding: An Inner History of the New AmericaRating: 4 out of 5 stars4/5 (45)
- Keeler Ophthalmoscope Bulb and Retinoscope Bulb ModelsDocument1 pageKeeler Ophthalmoscope Bulb and Retinoscope Bulb ModelsEDRAES17No ratings yet
- GlaucomaDocument15 pagesGlaucomapreethijojo20035582100% (5)
- Proceeding Book PVSM 2020Document150 pagesProceeding Book PVSM 2020brahmani pitanatriNo ratings yet
- Cytiotrophoblast SyncDocument2 pagesCytiotrophoblast Syncdewishinta12No ratings yet
- Terminology of Mechanical Injuries: The Birmingham Eye Trauma Terminology (BETT)Document10 pagesTerminology of Mechanical Injuries: The Birmingham Eye Trauma Terminology (BETT)febyrahmaNo ratings yet
- Anorectal Malformation PDFDocument13 pagesAnorectal Malformation PDFFrinciaNo ratings yet
- Kdigo-Gn-Guideline GN PDFDocument143 pagesKdigo-Gn-Guideline GN PDFFerry JuniansyahNo ratings yet
- 04 Approach To Stemi PDFDocument7 pages04 Approach To Stemi PDFAtikah Risya SyilfiyaniNo ratings yet
- RBHH - Oral Cancer After Prolonged Immunosupression For Multiorgan Chronic Graft Vs Host DiseaseDocument4 pagesRBHH - Oral Cancer After Prolonged Immunosupression For Multiorgan Chronic Graft Vs Host Diseasedewishinta12No ratings yet
- Circulation 2012 Jneid CIRDocument36 pagesCirculation 2012 Jneid CIRdewishinta12No ratings yet
- Emerging Patterns in Clinico-Pathological Spectrum of Oral CancerDocument5 pagesEmerging Patterns in Clinico-Pathological Spectrum of Oral Cancerdewishinta12No ratings yet
- PDFDocument70 pagesPDFranggadrNo ratings yet
- Association Between CYP1A1 Polymorphism and Oral Squamous Cell CarcinomaDocument8 pagesAssociation Between CYP1A1 Polymorphism and Oral Squamous Cell Carcinomadewishinta12No ratings yet
- A Database of Genes Involved in Oral CancerDocument3 pagesA Database of Genes Involved in Oral Cancerdewishinta12No ratings yet
- ABC - Oral CancerDocument4 pagesABC - Oral Cancerdewishinta12No ratings yet
- 1.Ch12 Oral CancerDocument24 pages1.Ch12 Oral Cancerdewishinta12No ratings yet
- Corneal Topography Measuring and Modifying The Cornea 1992Document194 pagesCorneal Topography Measuring and Modifying The Cornea 1992SmaraNo ratings yet
- Types of Amblyopia - American Academy of OphthalmologyDocument1 pageTypes of Amblyopia - American Academy of OphthalmologyIraNo ratings yet
- Eye Module ExamDocument10 pagesEye Module ExamTehniat iqbalNo ratings yet
- Eye Screening Support SystemDocument70 pagesEye Screening Support Systembereketab demmelashNo ratings yet
- SANKARA COLLEGE OF OPTOMETRY BINOCULAR VISION EXAMDocument2 pagesSANKARA COLLEGE OF OPTOMETRY BINOCULAR VISION EXAMDiwakar RaoNo ratings yet
- Case Studies PresbyopiaDocument33 pagesCase Studies PresbyopiaMalaika ZubairNo ratings yet
- Dapus MataDocument2 pagesDapus MataDita YuliantiNo ratings yet
- Artificial Eye Seminar: A Guide to Prosthetics, Conditions and HistoryDocument18 pagesArtificial Eye Seminar: A Guide to Prosthetics, Conditions and HistoryShafiyaanNo ratings yet
- Ipao Program Flyer 17novDocument1 pageIpao Program Flyer 17novapi-246252391No ratings yet
- CH42 Management of Complicated Retinal DetachmentDocument36 pagesCH42 Management of Complicated Retinal DetachmentriveliNo ratings yet
- Overcoming Challenges in OphthalmologyDocument7 pagesOvercoming Challenges in Ophthalmologyestmar valentinoNo ratings yet
- Cataract: Classsification Acquired Age Related Nuclear Cortical Posterior Sub-CapsularDocument37 pagesCataract: Classsification Acquired Age Related Nuclear Cortical Posterior Sub-CapsularBushra SherwaniNo ratings yet
- Visual Outcomes and Barriers in Children with Low VisionDocument4 pagesVisual Outcomes and Barriers in Children with Low VisionshishichanNo ratings yet
- Fficulties, Risks and Potential Complications: Diabetes and Phacoemulsification Cataract Surgery: DiDocument13 pagesFficulties, Risks and Potential Complications: Diabetes and Phacoemulsification Cataract Surgery: Dimara 11No ratings yet
- Anatomy and Function of The Eye: Henry J. KaplanDocument7 pagesAnatomy and Function of The Eye: Henry J. KaplanCucută Alexandru-DanielNo ratings yet
- Small Animal Ophthalmology - Don A Samuelson and Dennis E Brooks PDFDocument243 pagesSmall Animal Ophthalmology - Don A Samuelson and Dennis E Brooks PDFVũ.T HiềnNo ratings yet
- Retinal Detachment - Symptoms and Causes - Mayo ClinicDocument7 pagesRetinal Detachment - Symptoms and Causes - Mayo ClinicJames YuNo ratings yet
- Extirpation of Eye - DoxcDocument2 pagesExtirpation of Eye - Doxckushal NeupaneNo ratings yet
- Pub Complementary-Pediatrics PDFDocument352 pagesPub Complementary-Pediatrics PDFShimaa AbdouNo ratings yet
- Aravind Eye CareDocument29 pagesAravind Eye CareNiy MdNo ratings yet
- MCQ OphthalmoDocument62 pagesMCQ Ophthalmosafasayed100% (1)
- Ophtha SIM 2nd EdDocument250 pagesOphtha SIM 2nd EdRalphNo ratings yet
- Eye Examination: Dr. Seng Serey / Prof .Kenn Freedman Prof - Kong PisethDocument78 pagesEye Examination: Dr. Seng Serey / Prof .Kenn Freedman Prof - Kong PisethSela KHNo ratings yet
- Retinopathy of Prematurity (Rop)Document21 pagesRetinopathy of Prematurity (Rop)ArinYuniastikaEkaPutriNo ratings yet
- Aao 2019Document16 pagesAao 2019Abdul HannanNo ratings yet
- Eye RobicsDocument28 pagesEye RobicsIsmi Raudha0% (1)
- Guidelines For The Cleaning and Sterilization Of.1Document2 pagesGuidelines For The Cleaning and Sterilization Of.1Ana Mª GuaiquilNo ratings yet