Professional Documents
Culture Documents
J Infect Dis. 1999 Dinarello S294 304
Uploaded by
nikuCopyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
J Infect Dis. 1999 Dinarello S294 304
Uploaded by
nikuCopyright:
Available Formats
S294
Cytokines as Endogenous Pyrogens
Charles A. Dinarello
Department of Medicine, Division of Infectious Diseases, University of
Colorado Health Sciences Center, Denver
Cytokines are pleiotropic molecules mediating several pathologic processes. Long before the
discovery of cytokines as immune system growth factors or as bone marrow stimulants, investigators
learned a great deal about cytokines when they studied them as the endogenous mediators of fever.
The terms granulocytic or endogenous pyrogen were used to describe substances with the
biologic property of fever induction. Today, we recognize that pyrogenicity is a fundamental biologic
property of several cytokines and hence the clinically recognizable property of fever links host
perturbations during disease with fundamental perturbations in cell biology. In this review, the
discoveries made on endogenous pyrogens are revisited, with insights into the importance of the
earlier work to the present-day understanding of cytokines in health and in disease.
Historical Overview
Financial support: NIH (AI-15614).
Reprints or correspondence: Dr. Charles A. Dinarello, University of Colorado Health Sciences Center, Division of Infectious Diseases, B168, 4200 E.
9th Ave., Denver, CO 80262.
The Journal of Infectious Diseases 1999;179(Suppl 2):S294304
q 1999 by the Infectious Diseases Society of America. All rights reserved.
00221899/99/79S20003$02.00
/ 9d5b$$fe24
01-13-99 07:35:41
jinfa
UC: J Infect
Downloaded from http://jid.oxfordjournals.org/ by guest on September 26, 2015
The concept that fever is associated with leukocytic infiltrates dates back to the 19th century. This subject, as well as
the role of fever in history, has been reviewed by Atkins [1
4]. Fifty years have elapsed since an endotoxin-free pyrogenic
material derived from leukocytes was described by Beeson.
Those studies were done with activated leukocytes derived
from sterile peritonitis in the rabbit. Because most of these
cells were granulocytes, the pyrogenic material was originally
called granulocytic or leukocytic pyrogen. (Herein, the term
endogenous pyrogen [EP] will be used throughout for granulocytic or leukocytic pyrogen.) On incubation for a few hours
in saline, the pyrogenic activity was spontaneously released
from cells that had infiltrated into the peritoneal cavity. Therefore, these cells had been activated in vivo and released the
pyrogenic protein on ex vivo short-term culture. The biologic
assay for this material is highly consistent and is simply a rapid
rise in rectal temperature, reaching peak elevation within 50
60 min after intravenous bolus injection into rabbits. This assay
is the hallmark of EPs. It is quantitative by the maximal rise
in temperature (fever peak), and it is qualitative in that peak
fever occurring after 90 min or biphasic fevers are characteristic
of bacterial products such as endotoxin.
Initially, little was known about the chemical nature of EP
except that it was a heat-labile protein (destroyed at 907C),
which, when injected into the peripheral circulation, acted on
the thermoregulatory center of the hypothalamus to elicit fever.
Patrick Murphy and the late Barry Wood were the first to report
on the physical characteristics of a purified form of an EP from
rabbit acute peritoneal exudate cells. This rabbit EP had a
molecular weight of 14,000 15,000 and a neutral isoelectric
point (pI 7) on polyacrylamide gels [5].
For many years, it had been assumed that EP was a single
molecule, but in 1974, two distinct EPs from human monocytes
were characterized: Both had molecular weights in the range
of 15,000. However, one had a pI of 5 and the other a pI of
6.8 7.0 [6]. Unlike the EP from the acute granulocytic exudate
cell, EP from monocytes required stimulation in vitro, and there
was no significant EP activity until 12 24 h after incubation.
Therefore, it was concluded that the monocyte EP was synthesized de novo, whereas EP from neutrophils activated in the
peritoneal exudate had been synthesized in vivo. In addition
to the 15,000-molecular-weight EP, there was also a human
monocyte derived EP with a molecular weight of 38,000. Subsequently, rabbit EP was also found in these two charged forms
[7]. Although an explanation for this molecular heterogeneity
was unclear at that time, these findings introduced the concept
that there was more than one chemically distinct EP.
The pI 7 form of EP from human monocytes was purified
to homogeneity in 1977 [8]. Purified human EP and purified
rabbit EP had nearly identical specific activities: 25 50 ng/kg
injected intravenously produced a monophasic fever peak of
0.6 1.07C in rabbits. It was later found that EP possessed
additional distinctive biologic properties apart from its ability
to evoke fever. The concept that EP possessed other properties
was derived from the work of Kampschmidt and coworkers
[9, 10], who showed that the acute-phase inducing properties
of leukocytic endogenous mediator (LEM) were not separable
from EP activity. Thus, by the mid-1970s, EPs were well on
the way to being thoroughly defined molecules in terms of both
chemical characterization and identification of nonpyrogenic
biologic properties. It is obvious from todays viewpoint that
this was the birth of cytokine biology, with EP being the
first cytokine to be described.
Before the immunologists had entered the field, a great deal
had been published on EP. For example, the late Phyllis Bodel
had reported an intracellular form of EP and production from
a murine macrophage line (PD388D) and a human lymphoma
cell (U937). These studies evolved years later, only to be re-
JID 1999;179 (Suppl 2)
Cytokines as Endogenous Pyrogens
/ 9d5b$$fe24
01-13-99 07:35:41
jinfa
genic peak with an acidic pI coincided with LAF activity. It was
very clear by this time (1980) that the heterogeneity of EPs was
also a property of LAF. Subsequent reports supported that concept
[1518]. We continued to study the nonpyrogenic biologic activities of EP through each stage of purification, confirming the molecular heterogeneity of EP and LAF [19]. During this same time,
researchers working on LAF had also noted the molecular heterogeneity of LAF.
Other products of activated macrophages with lymphocyteactivating properties were described; these factors, along with
EP, LEM, and LAF, were incorporated into the interleukin
nomenclature. Although the factors were designated interleukin-1 (IL-1), it was unclear at the time whether they represented
a single molecule or several different molecules; at least four
different pI values and several molecular weights were ascribed
to EP before the term IL-1 was introduced. A rapid expansion
of studies on IL-1, with the use of in vitro lymphocyte assays,
took place (reviewed in [20]). However, such studies, including
chemical characterization, had been done 5 10 years earlier
in the case of EP [5, 8, 21, 22].
What was the explanation for the molecular heterogeneity
of EP and LAF? It was not until the cloning of mouse IL-1
[23] and human IL-1 [24] in 1984 that the molecular heterogeneity was resolved. Both IL-1s were first synthesized as precursors with molecular weights of 31,000 but without signal peptides. Each had different primary sequences. The N-terminus
of mouse IL-1 had been identified, and the mature mouse IL1 was acidic (pI 5). Later, when the N-terminus of human
IL-1 was identified [25], the mature IL-1 had a pI of 7. Therefore, the initial description of two isoelectric points for human
EP represented two separate gene products: IL-1a for that with
a pI of 5 and IL-1b for that with a pI of 7. What explained
the 38,000-molecular-weight EP? The precursor for human IL1a is as active as mature IL-1a, whereas the precursor for IL1b is as much as 500-fold less active than the mature IL-1b.
It is therefore likely that the large-molecular-weight EP was
human precursor IL-1a.
The realization that IL-1 possessed a broad spectrum of
biologic activities involving the pathogenesis of acute-phase
responses spread rapidly, with confirmation of earlier studies on
EP and LEM. Experiments with recombinant IL-1 (discussed
below) have demonstrated that IL-1 indeed causes fever [26]
and mediates many components of the acute-phase response.
However, the term interleukin is somewhat inappropriate
for IL-1, because, like interferon (IFN), tumor necrosis factor
(TNF), and IL-6, IL-1 is produced by many different (nonleukocytic) cells and acts on many nonleukocytic targets. It may
be more appropriate to consider these polypeptides as a special
class of substances called cytokines and to denote those cytokines that are intrinsically pyrogenic as EPs or pyrogenic cytokines to differentiate them from other cytokines that are not
intrinsically pyrogenic.
To date, the following cytokines are intrinsically pyrogenic
in that they produce a rapid-onset fever by acting directly on
UC: J Infect
Downloaded from http://jid.oxfordjournals.org/ by guest on September 26, 2015
peated with use of non-EP assays. Thus, investigators working
on the biology and physical nature of EPs and LEMs had
established many of the concepts that are canonical for cytokines today.
In 1972, Gery and Waksman [11] described a product that
was present in the supernatants of stimulated macrophages that
augmented the activation of T lymphocyte responses to either
mitogens or specific antigens. Early reports on the chemical
nature of lymphocyte-activating factor (LAF) indicated a striking similarity to EP. In 1976 1977, it became clear to those
of us working on the characterization of EPs that LAF was
remarkably similar to EP, not only at the biochemical level but
also in terms of cellular sources, kinetics of production, and
spectrum of agents inducing synthesis. In fact, during this time,
we had made neutralizing antibodies to human EP [12] that
also neutralized human LAF. These antibodies were then purified [12] by a series of absorption steps but maintained their
ability to neutralize both the pyrogenic and LAF activities of
monocyte supernatants.
In 1977, we found that homogeneous preparations of human
EP with a pI of 6.8 7.0 were obtainable [8]. At that time,
silver stains for polyacrylamide gels were not available as a
criterion for purity. We developed a method that had a greater
criterion of purity than did silver staining. That method was
radioactive tagging using Bolton-Hunter reagent (BH). This
reagent covalently links a chemical group to primary amino
groups (primarily lysines and arginines). The advantage of radioactive tagging with BH was that unlike other radioactive
tagging methods, BH was gentle and biologic activity was
unaffected. Since we could assume that proteins with molecular
weights of 15,000 have ample lysines and arginines, we
tagged EP with BH and followed radioactivity. Since BH is
linked to 125I, gamma counting was used to follow the molecule,
providing us with the least quenching of any radionuclide.
Contaminating proteins were easily recognized, and the coelution of radioactivity with pyrogenicity identified EP. After four
steps of purification using specific immunoabsorption, we could
repeatedly purify EP, which had a single band on SDS-PAGE
as determined by radioactive counts, whereas other parts of the
gel were without radioactivity [8]. However, to produce pure
EP, we had lost almost 95% of the biologic units (fever units)
present in the starting material. At this time, we also used a
new methodology to confirm purity: high-pressure liquid chromatography. This method also demonstrated the purity of our
BH-labeled preparations. Interestingly, with use of BH-labeled
EP, aggregation often takes place, and we observed trimerization of BH-tagged EP.
During this same time, Lanny Rosenwasser, working in the
laboratory of Alan Rosenthal, had developed an LAF-like assay.
When purified, human EP was highly active in the LAF assay, and
we concluded that EP and LAF were the same molecule. We
published our results in 1979 [13]. In 1980, similar evidence was
published by Patrick Murphy and coworkers [14]. The Murphy
study used rabbit EP with pIs in the 5.0 range. In fact, each pyro-
S295
S296
Dinarello
/ 9d5b$$fe24
01-13-99 07:35:41
jinfa
The acute-phase response is a systemic, generalized reaction,
although most disease processes that induce it are localized.
There has been considerable speculation that the role of acutephase proteins is to help contain pathogens and their toxins
and to inactivate microbial proteases and highly reactive O2
metabolites. More than one leukocyte product is now identified
as mediating acute-phase hepatic protein synthesis. IL-1, TNF,
IL-6, IL-11, oncostatin M, ciliary neurotrophic factor, cardiotropin-1, and leukemic inhibitory factor possess the ability to
stimulate the hepatocyte to increase gene expression for various
acute-phase proteins as well as to suppress the synthesis of
several household proteins. These latter proteins include
lipoprotein lipase, albumin, and cytochrome P450 . The ability
of these cytokines to suppress gene expression for these commonly produced molecules accounts, in part, for the altered
lipid and drug metabolism states observed in patients with acute
or chronic infections or inflammatory diseases.
EPs and the Thermoregulatory Center
There are still no data demonstrating that EPs produced in
peripheral tissues and reaching the brain via the systemic circulation actually penetrate the blood-brain barrier and enter the
brain tissue itself. It seems more likely that EPs have their
major effect on the rich vascular network close to the cluster
of neurons in the preoptic/anterior hypothalamus. These sites,
called the circumventricular organs or organum vasculosum
laminae terminalis (OVLT), possess little if any blood-brain
barrier. Ablation of the OVLT prevents fever after a peripheral
injection of EP but has no effect when EP is injected directly
into brain tissue [30, 31]. Thus, it is likely that endothelial cells
lining the OVLT either offer no resistance to the movement
of EPs into the brain or release arachidonic acid metabolites
themselves when they encounter EPs from the circulation. Metabolites of cyclooxygenase may then diffuse the few millimeters into the preoptic/anterior hypothalamic region and initiate
fever. Alternatively, prostaglandin E2 (PGE2) and other prostaglandins may be produced by the endothelial cells, which, in
turn, induce a neurotransmitter-like substance that acts to raise
the set-point. This explanation is actually likely, since prostaglandins are not suitable as neurotransmitters. PGE2 is known
to increase levels of cyclic AMP, which has neurotransmitter
properties in brain tissue and has been implicated in fever
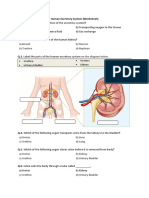
[31a]. Figure 1 is a scheme showing the likely events leading
to the synthesis of EPs and their ability to produce fever.
Endothelium as a Target for EPs
In view of the role of the OVLT in the initiation of fever
after systemic injection of EPs, it is important to note that two
of the EPs discussed herein (IL-1 and TNF) have profound
effects on endothelial cell function. IL-1 and TNF activate
human endothelial cells in vitro to synthesize and release PGI2
and PGE2 . A 10-fold increase in PGI2 release follows exposure
UC: J Infect
Downloaded from http://jid.oxfordjournals.org/ by guest on September 26, 2015
the hypothalamus without the requirement for the formation of
another cytokine: IL-1a, IL-1b, TNF-a, TNF-b, IFN-a, and
IL-6. Humans have been injected with IFN-a, IL-1b, IL-1a,
and TNF-a in clinical trials for treatment of cancers; in each
case, there has been rapid onset of fever, typical for EP activity
described in animals. Human sensitivity to the pyrogenic properties of these cytokines is in the range of 10 1000 ng/kg. The
intravenous route produces a rapid onset of fever, within 30
min, whereas subcutaneous administration takes slightly
longer.
The term EP today often refers to IL-1, because IL-1 was
the first to be endogenously purified and characterized as both
a pyrogenic and lymphocyte-activating molecule. IL-6 and
TNF also possess these biologic properties; however, these
have biologic and physical characteristics that clearly distinguish them from IL-1. For example, in the rabbit assay, 50- to
100-fold more IL-6 than IL-1 is needed for a monophasic fever
[27]. Thus, purified EP could not have been IL-6, because the
specific activity was too high. In addition, the pI of IL-6 is
6.2, and the molecular weight 20,000. Although the specific
activity of TNF is nearly the same as that for IL-1 (50 ng/kg),
TNF must be a trimer for biologic activity and hence would
not have been purified in the molecular weight range of 15,000.
Furthermore, antibodies used to purify EP did not contain antiTNF activity [28]. In the days before the isolation and purification of EP, most experiments were, in fact, carried out with a
mixture of pyrogenic cytokines, and certainly the crude leukocyte supernatants and serum from febrile animals contained
such a mixture of IL-1, TNF, and IL-6. From a clinical standpoint, during most febrile diseases, several pyrogenic cytokines
are produced and likely contribute to the febrile response.
These now include a family of cytokines that use the cell
signaling apparatus gp130. Cytokines using this receptor are
pyrogenic, and currently they include IL-6, IL-11, oncostatin
M, ciliary neurotrophic factor [29], cardiotropin-1, and leukemic inhibitory factor.
Although fever is primarily associated with infectious diseases, the febrile response is, in fact, a prominent component
of many inflammatory and immunologically mediated diseases
and frequently accompanies certain malignancies. However,
fever is hardly an isolated event. Increases in the total and
relative numbers of circulating young neutrophils often occur.
In addition, many febrile illnesses are accompanied by an increase in the synthesis of a variety of hepatic acute-phase proteins. These include antiproteases, haptoglobin, several complement components, fibrinogen, ceruloplasmin, and ferritin.
There can also be 100- or 1000-fold increases in special acutephase proteins such as C-reactive protein and serum amyloid
A protein. The dramatic increase in the rate of synthesis of these
proteins occurs despite the fact that hepatic albumin synthesis is
markedly reduced; indeed, the host is often in negative nitrogen
balance. In general, the onset of fever accompanied by these
hematologic and metabolic changes is frequently referred to as
the acute-phase response.
JID 1999;179 (Suppl 2)
JID 1999;179 (Suppl 2)
Cytokines as Endogenous Pyrogens
S297
to 1 U/mL IL-1 [32]. Although these two arachidonate metabolites increase blood flow, IL-1 and TNF also orchestrate a
cascade of cellular and biochemical events that lead to vascular
congestion, clot formation, and cellular infiltration. One way
in which IL-1 and TNF initiate these events is by stimulating
the plasma membrane of endothelial cells so that neutrophils,
monocytes, and lymphocytes adhere avidly to them [33]. IL-1
activates cultured vascular endothelial cells in 1 h at relatively low concentrations by inducing the expression of intercellular adhesion molecule 1 [34]. This molecule interacts with
the leukocyte-glycoprotein complex designated leukocyte function antigen.
IL-1 and TNF-induced increases in procoagulant activity
on the endothelial cell surface serve to increase coagulation.
There is also evidence that IL-1 and TNF induce the production
of a plasminogen activator inhibitor. These events lead to activation of factor VIII and thrombin in the initiation of clotting.
Taken together, these effects of IL-1 and TNF lead to decreased
blood flow in vessels and increased accumulation of leukocytes
and platelets. Since IL-1 is a stimulator of thromboxane release
from neutrophils, activated neutrophils adhering to endothelial
cells are likely to increase platelet aggregation. Thromboxane
release from adherent neutrophils may also contribute to fever,
since thromboxane levels in the third cerebral ventricle rise
with the early increase in EP-mediated fever [35]. IL-1 stimulates the release of platelet-activating factor from endothelial
/ 9d5b$$fe24
01-13-99 07:35:41
jinfa
cells [36], which, in turn, may affect the subsequent release of
arachidonic acid metabolites. These IL-1 and TNF-induced
effects on vascular tissue make the endothelial surface in the
OVLT a prime site of action of EPs in the initiation of fever.
IL-1 as an EP
Several groups of investigators have purified IL-1 to homogeneity, using T cell stimulation as a biologic marker, and have
shown that the isolated material produces typical EP fever.
Pacak and Siegert [37] found that purified rabbit EP from
peritoneal cells possessed potent LAF activity, and Saklatvala
et al. [38] showed that homogeneous pig IL-1 of either the
acidic or the alkaline form (also known as catabolin) was a
potent EP for rabbits. In an independent study, Van Damme
et al. [25] purified supernatant from human mononuclear cells
stimulated with concanavalin A and obtained a homogeneous
material with a molecular weight of 22,000. When this material
was sequenced, the results matched the polypeptide sequence
of human IL-1b. Hanson and Murphy [39] purified rabbit IL1 with a pI of 5 to a single band and showed that it produced
typical EP fever. It was also demonstrated that both EP-induced
fever and LAF activity were associated with three pI values
for IL-1 and that each one yielded a single band on SDSPAGE. Other investigators demonstrated that purified human
monocyte IL-1 with a pI of 7 evoked fever in endotoxin-resis-
UC: J Infect
Downloaded from http://jid.oxfordjournals.org/ by guest on September 26, 2015
Figure 1. Scheme for pathogenesis of fever. IL, interleukin; TNF, tumor necrosis factor; IFN, interferon; PG, prostaglandin; CNTF, ciliary
neurotrophic factor.
S298
Dinarello
/ 9d5b$$fe24
01-13-99 07:35:41
jinfa
mL 4 h after IL-1 administration (baseline, 50 pg/mL), and
after a dose of 300 ng/kg, the mean level was 8000 pg/mL. In
another study, infusion of 30 ng/kg IL-1a induced elevated IL6 levels within 2 h [54]. These elevations in IL-6 are associated
with a rise in C-reactive protein and a decrease in albumin. In
two studies, one with IL-1a [55] and one with IL-1b [56], a
rapid increase in circulating IL-1 receptor antagonist and TNFsoluble receptors (p55 and p75) was observed following a 30min intravenous infusion.
TNF as an EP
TNF is a macrophage product that has a direct cytotoxic
effect on certain tumor cells. Human TNF has been cloned and
shares significant amino acid homology with another macrophage product, cachectin [57]. Originally, cachectin was characterized as an endotoxin-induced macrophage product that
mediated severe weight loss, in part through its ability to inhibit
lipoprotein lipase. TNF also shares many biologic properties
with IL-1. For example, recombinant IL-1 and recombinant
TNF both stimulate synovial cell production of PGE and collagenase, endothelial cell procoagulant activity, and release of
platelet-activating factor. Both molecules are cytotoxic for certain tumor cells, and both induce hepatic acute-phase proteins.
In addition, lymphocyte activation, cytotoxicity for insulinproducing beta cells, and release of adrenocorticotropic hormone are also shared properties of both IL-1 and TNF. It is
remarkable, therefore, that the amino acid sequences of TNF
and either form of IL-1 share no discernible regions of significant homology. The receptors for TNF are distinct from those
for IL-1.
For the assessment of the biologic activities of these distinct
cytokines, it is highly important to note that TNF produces the
typical EP fever pattern in rabbits and C3H/HeJ mice. The rapid
rise in body temperature that occurs in rabbits after intravenous
injection of TNF is indistinguishable from that produced by
either form of recombinant IL-1. The fever curves and peak
temperature elevations are nearly superimposable. In terms of
specific activities, human recombinant TNF and IL-1 are similar: Either factor at 50 200 ng/kg produces monophasic fever
in rabbits. Recombinant human TNF is highly pyrogenic in
humans at doses of 100 ng/kg. Humans receiving recombinant
IL-1a or IL-1b for bone marrow transplant or for protection
of bone marrow stem cells during chemotherapy also manifest
fever at doses of 40 100 ng/kg. The fever induced in these
humans is rapid and is associated with generalized malaise and
joint pain.
Recombinant TNF injected into rabbits at a dose of 10 mg/
kg (50 times the minimal pyrogenic dose) evokes a second
fever peak after 3 4 h. At this time, circulating IL-1 is detected
in the plasma; this finding suggests that in large doses, TNF
induces IL-1 in vivo. Incubation of TNF with either human
blood monocytes or cultured human endothelial cells induces
IL-1 in vitro [28, 58]. The amount of TNF that induces IL-1
UC: J Infect
Downloaded from http://jid.oxfordjournals.org/ by guest on September 26, 2015
tant mice [40]. In the latter study, the N-terminal amino acid
sequence of the purified IL-1 matched that of human monocyte
IL-1b [41].
Because IL-1 and other recombinant cytokines are expressed
in Escherichia coli, considerable caution must be used to exclude the involvement of contaminating endotoxin in the isolated product. Endotoxin evokes fever in rabbits at concentrations as low as 1 ng/kg [42]. Since endotoxin present in these
recombinant IL-1 preparations (30 60 pg/mg) represents
0.0000002 of the protein, the amount injected is 0.0001 of
the minimal pyrogenic dose of endotoxin for rabbits. Moreover,
the EP fever produced by such a preparation is unaffected by
polymyxin B, which blocks the pyrogenic effect of E. coli
endotoxin. Finally, this fever is also elicited by IL-1 in C3H/
HeJ endotoxin-resistant mice.
In humans, IL-1 appears to be the most potent cytokine. Although the systemic effects of IL-1 have been studied in animals,
there are now data on the effects of and sensitivity to IL-1 in
humans. IL-1a or IL-1b has been injected into patients with
various solid tumors or as part of a reconstitution strategy in bone
marrow transplantation. Acute toxicities of either IL-1a or IL-1b
were greater after intravenous than after subcutaneous injection;
subcutaneous injection was associated with significant local pain,
erythema, and swelling [43, 44]. Chills and fever were observed
in nearly all patients, even in the 1-ng/kg dose group [45]. The
febrile response increased in magnitude with increasing doses
[4648], and chills and fever were abated with indomethacin
treatment [49]. In patients receiving IL-1a [50, 51] or IL-1b [46,
47], nearly all subjects experienced significant hypotension at
doses of 100 ng/kg. Systolic blood pressure fell steadily and
reached a nadir of 90 mm Hg 35 h after the infusion of IL1. At doses of 300 ng/kg, most patients required intravenous
pressors. By comparison, in a trial of 16 patients given IL-1b
from 4 to 32 ng/kg subcutaneously, there was only one episode
of hypotension at the highest dose level. These results suggest
that the hypotension is probably due to induction of NO, and
elevated levels of serum nitrate have been measured in patients
with IL-1induced hypotension [48].
At 30 100 ng/kg IL-1b, patients exhibited a sharp increase
in cortisol levels 2 3 h after the injection. Similar increases
were noted in patients given IL-1a. In 13 of 17 patients given
IL-1b, there was a fall in serum glucose level within the first
hour of administration, and in 11 patients, the glucose level
fell to 70 mg/100 mL [52]. In addition, there were increases
in adrenocorticotropic hormone and thyroid-stimulating hormone but a decrease in testosterone [48]. No changes were
observed in coagulation parameters, such as prothrombin time,
partial thromboplastin time, or fibrinogen degradation products.
This latter finding is to be contrasted to TNF-a infusion into
healthy humans, which results in a distinct coagulopathy syndrome [53].
Not unexpectedly, IL-1 infusion into humans significantly
increased circulating IL-6 levels in a dose-dependent fashion
[48]. At a dose of 30 ng/kg, the mean IL-6 level was 500 pg/
JID 1999;179 (Suppl 2)
JID 1999;179 (Suppl 2)
Cytokines as Endogenous Pyrogens
/ 9d5b$$fe24
01-13-99 07:35:41
jinfa
IL-6 as an EP
IL-6 is the term given to a polypeptide cytokine that was
initially isolated from fibroblasts and called IFN-b2. On close
examination, this IFN had little intrinsic antiviral activity but
rather possessed other biologic activities. This molecule was
cloned, and its entire cDNA-derived amino acid sequence was
published in 1986 [64]. Other investigators had isolated a polypeptide that stimulated B cell growth, hybridoma growth, and
hepatic acute-phase protein synthesis. When the B cell stimulating factor had been cloned, it revealed identity with IFN-b2
[65]. The recombinant molecule also possessed the acute-phase
protein inducing properties [66], and the molecule was renamed IL-6. Later, it was shown that IL-6 produced typical
EP fever when injected into rabbits and that there was a positive
correlation in humans with burns between fever and IL-6 levels
[67, 68].
In general, IL-6 fever in rabbits requires concentrations between 50- and 100-fold greater than that required for IL-1.
There are no known studies of IL-6 administration in humans.
There have been multiple reports of IL-6 levels in a variety of
human diseases and in various human body fluids such as
plasma, cerebrospinal fluid, and joint fluids. IL-6 gene expression is under the control of many exogenous pyrogens but also
IL-1 and TNF [69]. In fact, IL-1 and particularly IL-1 plus
TNF are very potent stimulators of IL-6 gene expression and
protein translation. Therefore, IL-6 is often elevated in conditions in which IL-1 and TNF have been synthesized.
Unlike IL-1 and TNF, IL-6 does not seem to possess proinflammatory properties. The acute-phase inducing properties of
IL-6 may be viewed as antiinflammatory, since most acutephase hepatic proteins are either oxygen scavengers or antiproteases. One of the most potent proinflammatory properties of
IL-1 is its ability to induce gene expression for cyclooxygenase,
thus resulting in large amounts of prostaglandin synthesis. IL6 does not stimulate PGE formation through increased cyclooxygenase gene expression [69a]. The fever due to IL-6 is reduced
by cyclooxygenase inhibitors, suggesting that cyclooxygenase
products are induced by IL-6; however, a clear distinction must
be made between the ability of IL-6 to transiently induce prostaglandins from cell surface signal transduction and induction
of the cyclooxygenase genes, resulting in prolonged (days)
prostaglandin synthesis. It is this latter property of IL-1 and
TNF that distinguishes them from IL-6 as proinflammatory
cytokines.
IFNs as EPs
IL-1, TNF, and other cytokines are often produced by the
same cells and induced by the same stimulators; all possess
high specific activities (at the picogram- or nanogram-per-milliliter level) in a variety of biologic assays. The case for the
multiple biologic activities of IL-1 has also existed with regard
to the IFNs, which were initially described as antiviral sub-
UC: J Infect
Downloaded from http://jid.oxfordjournals.org/ by guest on September 26, 2015
production in vitro ranges from 50 to 200 ng/mL, and the
kinetics of TNF disposition indicate that such a concentration
would be reached in vivo. The induction of IL-1 by TNF takes
place in the presence of polymyxin B, which blocks endotoxin
effects in a variety of assays. In addition, heating of TNF to
707C for 30 min reduces its capacity to induce IL-1 in vitro
as well as in vivo. Trypsin treatment also destroys the IL-1
inducing property of TNF. Thus, it is unlikely that endotoxin
accounts for these biologic properties of TNF. The amount of
endotoxin in the recombinant TNF used in these studies was
measured at 50 pg/mg (as determined by limulus testing
and gas chromatography mass spectrometry) far below the
minimal pyrogenic level used in vivo or the IL-1 inducing
concentration in vitro.
TNF, like IL-1, is defined as an EP because of its ability to
act directly on the hypothalamus. When incubated with rabbit
hypothalamic slices in vitro, TNF increases PGE2 production
within 30 min; this property is shared with IL-1. TNF is also
an endogenous inducer of IL-1. This property implicates TNF
in the pathogenesis of endotoxin fever, since endotoxin stimulates large amounts of TNF in vivo. The role that in vivo levels
of TNF play in inducing IL-1 remains to be clarified. At present,
it is clear that the pathogenesis of fever requires consideration
of both IL-1 and TNF levels following the injection of a variety
of exogenous pyrogens. Recent studies indicate that TNF-b, a
lymphokine also known as lymphotoxin, shares considerable
(78%) homology with TNF. Recombinant lymphotoxin also
manifests EP activity and induces IL-1 both in vivo and in
vitro (unpublished data).
TNF has also been crystallized, revealing that this molecule is normally found as a trimer in nature. This explains
the various molecular weights reported for TNF bioactivity
in years that preceded its molecular cloning. The monomer
of TNF has a molecular weight of 17,000, but unlike IL-1,
this monomer does not contain any methionine. The signal
peptide for TNF is clearly identified, and in human peripheral
blood mononuclear cells, 90% of the TNF synthesized
following stimulation by endotoxin is secreted, whereas in
these same cells, only 60% of the IL-1b and 10% of the IL1a is found in the culture supernatant after 24 h of incubation
[59 61].
The tertiary structure of TNF in the trimer form appears
to be critical for biologic activity. Monomeric TNF may be
detectable by a variety of RIAs or ELISAs, but it does not
have biologic activity. This discrepancy has been reported
in body fluids for several disease processes. The biologic
activity of TNF is most often measured by its cytotoxic
effects on a number of susceptible cells. Two structurally
distinct polypeptides form the external part of the TNF receptor. The TNF trimer cross-links these two receptor molecules, and this cross-linking triggers signal transduction [62,
63]. Antibodies to the TNF receptor polypeptides have been
produced, and these antibodies signal TNF biologic activity
when cross-linked by anti-F(ab*)2 .
S299
S300
Dinarello
/ 9d5b$$fe24
01-13-99 07:35:41
jinfa
hypothalamic minces in vitro (unpublished data). There have
been several reports that IFN-g stimulates IL-1 production in
vitro from human and animal macrophages and monocytes.
This property is shared with IFN-a, but these findings are
apparently due to the ability of IFNs to augment endotoxininduced IL-1 and TNF production rather than to stimulate their
production directly [77 79]. When caution to remove endotoxins from the in vitro culture medium is taken, neither IFNg nor IFN-a induces IL-1 or TNF production. Removal of
endotoxins from tissue culture media is done by ultrafiltration
[80]. Most commercial culture media contain a small amount
of endotoxin (0.5 1 ng/mL). Hence, IFNs may appear to induce IL-1 in vitro, but closer examination reveals an augmentation of endotoxin-induced cytokine production. No data are
available on whether IFN-g induces the production of IL-1 or
TNF in vivo. One difficulty in working with animal models of
IFN fever is the known species specificity of the IFNs. As has
been stated, large doses are required to produce fever in rabbits
or mice, whereas humans develop fever at considerably lower
doses.
Production of Fever by IL-2
Cell-derived IL-2 or recombinant IL-2 infusions induce fever
in humans at doses of 104 U/kg [81]. The fever begins 3 4 h
after the infusion and is associated with chills and headache.
Levels of C-reactive protein, adrenocorticotropic hormone,
prolactin, and growth hormone also become elevated [82]. In
the peripheral circulation, the half-life of recombinant IL-2 is
brief (25 min); thus, by the time of the onset of fever, levels
of IL-2 may be low [82]. These findings suggest that IL-2
causes fever by an indirect mechanism rather than by a direct
effect on the hypothalamus as a true EP. IL-2 induces TNF
and IFN-g from human mononuclear cells in vitro [83], and
these molecules could in turn mediate IL-2 fever. Mier et al.
[84] demonstrated that the biologic responses to recombinant
IL-2 and natural IL-1 are readily distinguishable in rabbits. IL1 induces elevated C-reactive protein concentrations, whereas
IL-2, at comparable doses (weight per kilogram), has no effect
on acute-phase responses. However, it has recently been demonstrated that large doses of IL-2 (100 1000 U/mL) induce IL1 production from human mononuclear cells and large granular
lymphocytes in vitro [83, 85]. Therefore, high-dose IL-2 therapy may induce acute-phase responses because of the ability
of this molecule to stimulate IL-1.
Cell Sources of EPs
The original cell source of an EP was the acute exudative
granulocyte described by Beeson. Attention was focused on
this cell, and the first purification of an EP was accomplished
by Murphy et al. [5] from rabbit acute-exudate cells. Because
its pI was 7, this EP was IL-1b. Subsequently, EP activity was
found in extracts of different tissues (spleen, liver, kidney,
UC: J Infect
Downloaded from http://jid.oxfordjournals.org/ by guest on September 26, 2015
stances. IFNs were the first cytokines administered to humans.
Although IFNs had other biologic properties, fever was a prominent effect, especially when the early, semipurified preparations were given to humans. There was considerable speculation (and some evidence) to the effect that IFN caused fever
because it was contaminated with endotoxins and that these
and other contaminants stimulated IL-1 production, which mediated the fever [70, 71]. The availability of recombinant IFN
enabled investigators to confirm that IFNs possess several biologic activities in addition to antiviral activity; these include
important effects, such as an increase in natural killer activity
and an enhanced expression of class I and class II major histocompatibility complex antigens.
Since the early days of clinical IFN trials, fever has been
the major side effect encountered [70 72]. In fact, this effect
of IFN has been consistently reported in subsequent trials with
recombinant IFN-a. Recombinant human IFN-a injected into
humans at a dose of 104 105 U/kg (equivalent to 0.1 1 mg/
kg) results in chills and fever developing within 2 h [73]. The
fever following administration of recombinant IFN is not due to
contaminating endotoxin. Moreover, since IFN is recombinant
protein, the fever it evokes is not due to other human proteins
that frequently contaminated the leukocyte-derived IFN used
in early trials.
Injected intravenously into rabbits, recombinant IFN-a induces monophasic fevers that peak 80 90 min after the injection [74]. In the rabbit, IFN-a fever is not comparable with
those produced by TNF or IL-1. Recombinant IFN-a, which
also produces fever in the endotoxin-resistant C3H/HeJ mouse,
is not affected by polymyxin B, and endotoxin (detected by
the limulus test) is not sufficient to account for the fever. The
amount of human recombinant IFN-a required to produce a
17C fever in rabbits (50 mg/kg) is significantly greater than
that of human recombinant TNF or human recombinant IL-1.
The established species specificity of the IFNs may explain
why IFN-a is pyrogenic in humans at doses of 1 mg/kg (similar
to those of TNF and IL-1 injected into humans) but is 100fold less pyrogenic in rabbits. Also, the rate of rise and time
of peak elevation in IFN fever differ from these parameters in
IL-1 or TNF fever. Nevertheless, it is clear that IFN-a is an
EP and induces fever via the same mechanism as that shown for
other EPs: synthesis of brain prostaglandins [74]. Recombinant
IFN-a stimulates PGE2 production from hypothalamic minces
in vitro, and third-cerebroventricular levels of PGE2 are elevated after injection [74]. These properties are observed with
two other EPs, IL-1 and TNF.
IFN-b shares significant amino acid homology with IFN-a
but is less pyrogenic for humans [70]. By itself, neither IFNa nor IFN-b induces IL-1 in vitro; however, IL-1 induces IFNb [25]. IFN-g can also be pyrogenic in humans. In phase I
and phase II clinical trials, recombinant human IFN-g has
caused fever [75, 76]. IFN-g is distinct from IFN-a or IFNb, with 17% amino acid homology. Unlike IFN-a, IFN-g
does not directly stimulate prostaglandin synthesis from rabbit
JID 1999;179 (Suppl 2)
JID 1999;179 (Suppl 2)
Cytokines as Endogenous Pyrogens
/ 9d5b$$fe24
01-13-99 07:35:41
jinfa
late-acute rabbit exudate neutrophil was the major cell producing IL-1. In that study, immunocytochemical staining
proved that at the single-cell level, the early-exudate neutrophil was producing IL-1. This was supported by elevated
mRNA levels coding for IL-1b in these cells [99]. Thus, these
studies are highly consistent with the acute, young exudate
neutrophil releasing IL-1b, since IL-1a is not easily secreted
by cells unless there is a significant injury to the cell (such as
death, which occurs later).
By means of Northern hybridization, human IL-1b and IL1a mRNAs have been detected in a variety of human tissues,
including cultured keratinocytes [100], vascular endothelium
[101], vascular smooth-muscle cells [102], and a variety of
leukemic cells [103, 104]. In addition, IL-1 activity as measured
on T cells has been found in supernatants from Epstein-Barr
virus infected B cell lines [105], monocyte leukemia cells
[22], histiocytic lymphoma cells, and freshly isolated large
granular lymphocytes (natural killer cells) [106]. Some of these
tissues have also been examined for synthesis of IL-1 protein
by means of specific immunoprecipitation of [35S]methioninelabeled cells. Clearly, these methods, although they are specific
for identifying IL-1, do not allow for the conclusion that the
IL-1 derived from the labeled cells is as pyrogenic as the IL1 purified from monocytes/macrophages. Could these tissues
produce IL-1 like molecules that are sufficiently related structurally to be detected by Northern hybridization or immunoprecipitation methods but that still differ in biologic potency from
IL-1 derived from the monocyte/macrophage? Although this
situation would not be unusual, we doubt that such structural
differences would account for major differences in pyrogenicity. In fact, EP activity has been demonstrated in IL-1 derived
from keratinocytes [107], U937 cells [41, 108], and renal mesangial cells [109]. Another consideration is that the amount of
EP activity per cell of these specialized tissues may be smaller
than that from the monocyte/macrophage.
Measurement of EPs in Human Diseases
Measurement of EPs in the circulation can now be accomplished with the use of several specific RIAs and ELISAs for
IL-1b, IL-1a, TNF-a, and IL-6. However, circulating cytokines should be measured in the plasma rather than the serum,
since blood leukocytes can be a source of the cytokines, and
release from these sources may take place during the clotting
and separation procedures. We recommend using EDTAtreated plasma with additional protease-inhibiting substances
[110].
In general, the measurement of circulating cytokines is, in
fact, the measurement of the amount of cytokine that is available to measure. The affinity for any cytokine to its receptor
is 100-fold greater than the affinity for any antibody. A similar
case exists for the binding of cytokines to their soluble receptors. Therefore, cytokines binding to cell surface receptors, for
example, endothelial cells, would take place and be removed
UC: J Infect
Downloaded from http://jid.oxfordjournals.org/ by guest on September 26, 2015
muscle, lung, and heart), and it became clear that cells other
than the granulocyte were sources of EP [86]. In 1967, the
mononuclear phagocyte [87 89] and various tissues were
shown to produce EPs; the stimulated monocyte/macrophage
produced more pyrogenic material than did a comparably stimulated neutrophil. The magnitude of the difference between the
amount of EP activity from human monocytes and that from
granulocytes varied between 10- to 15-fold [90] and 50-fold
[6]. Thereafter, doubts were raised concerning the ability of
blood neutrophils to produce molecules with EP activity [90]
or, specifically, IL-1 (as assayed on T cells) [91]. Recent evidence again points to the human granulocyte as a source of
IL-1 [92]. The macrophage contamination of these neutrophil
preparations is low enough not to account for the IL-1 activity.
Although the amount of IL-1 released by the neutrophil preparations is low (10- to 50-fold less than that released by an
activated macrophage), mRNA detection with synthetic oligonucleotides to the rabbit IL-1a sequence supports the notion
that these cells are synthesizing IL-1 de novo rather than releasing IL-1 that might have been absorbed onto their surface.
Others have purified IL-1 from bovine neutrophils [93] and
from human peripheral blood neutrophils [94].
The most convincing data on the neutrophil as a source of
IL-1 is derived from studies using the rabbit exudate cell, the
same cell that Beeson described as the source of EP. Rabbit
exudate neutrophils were used to make a cDNA library. By
use of oligonucleotides coding for the amino acid sequence of
a purified IL-1 like factor from rabbit neutrophils [95], a
cDNA was isolated and sequenced [96]. This cDNA coded for
the 268 amino acid sequence, which had 74% homology with
human IL-1b and 71% amino acid homology with murine IL1b. Therefore, there is no question that the most pyrogenic
cytokine, IL-1b, is encoded and produced by activated rabbit
neutrophils.
To reconcile these data with those of Murphy, it is important
to make the distinction between the rabbit acute-exudate neutrophil and the monocyte. In Murphys studies, the harvested
cells of the rabbit exudate required a stimulant [90]. However,
the EPs from the earlier studies were already stimulated in vivo
to produce EP spontaneously. The need to stimulate the cells
in Murphys study suggests that neither the granulocytes nor
monocytes were activated. Thus, the need to stimulate EP production underscores that there are two different cell types.
Under conditions of stimulation with staphylococci, EP is preferentially synthesized by the monocytes. When rabbit blood
neutrophils were used [91], it was necessary to stimulate EP
production, and hence, this favors the source of EP as being
monocytes.
A study by Goto et al. [97] demonstrated that rabbit acuteexudate cells infiltrating 3 9 h into the inflammatory process
are the source of the IL-1 like molecule. A similar conclusion
was reached by Sheng et al. [98], who used rat peritoneal acuteexudate cells. Consistent with this observation is the study by
Ohkawara et al. [99], which showed that the early- rather than
S301
S302
Dinarello
References
1. Atkins E. Pathogenesis of fever. Physiol Rev 1960; 40:580 646.
2. Atkins E, Feldman JD, Francis L, Hursh E. Studies on the mechanism of
fever accompanying delayed hypersensitivity: the role of the sensitized
lymphocyte. J Exp Med 1972; 135:1113 32.
3. Atkins E. Fever: the old and the new. J Infect Dis 1984; 149:339 48.
4. Atkins E. Fever: historical perspectives and evolution of modern views.
J Rheumatol 1985; 24(suppl):1 5.
5. Murphy PA, Chesney PJ, Wood WB Jr. Further purification of rabbit
leukocyte pyrogen. J Lab Clin Med 1974; 83:310 22.
6. Dinarello CA, Goldin NP, Wolff SM. Demonstration and characterization
of two distinct human leukocytic pyrogens. J Exp Med 1974; 139:
1369 81.
7. Cebula TA, Hanson DF, Moore DM, Murphy PA. Synthesis of four
endogenous pyrogens by rabbit macrophages. J Lab Clin Med 1979;
94:95 105.
8. Dinarello CA, Renfer L, Wolff SM. Human leukocytic pyrogen: purification and development of a radioimmunoassay. Proc Natl Acad Sci
USA 1977; 74:4624 7.
9. Merriman CR, Pulliam LA, Kampschmidt RF. Comparison of leukocytic
pyrogen and leukocytic endogenous mediator. Proc Soc Exp Biol Med
1977; 154:224 7.
10. Kampschmidt RF. Leukocytic endogenous mediator/endogenous pyrogen. In:
Powanda MC, Canonico PG, eds. Physiologic and metabolic responses of
the host. Amsterdam: Elsevier/North Holland, 1981:5574.
11. Gery I, Waksman BH. Potentiation of the T-lymphocyte response to
mitogens. II. The cellular source of potentiating mediator(s). J Exp
Med 1972; 136:143 55.
12. Dinarello CA, Renfer L, Wolff SM. Production of antibody against human
leukocytic pyrogen. J Clin Invest 1977; 60:465 72.
13. Rosenwasser LM, Dinarello CA, Rosenthal AS. Adherent cell function
in murine T-lymphocyte antigen recognition. IV. Enhancement of murine T-cell antigen recognition by human leukocytic pyrogen. J Exp
Med 1979; 150:709 14.
/ 9d5b$$fe24
01-13-99 07:35:41
jinfa
14. Murphy PA, Simon PL, Willoughby WF. Endogenous pyrogens made by
rabbit peritoneal exudate cells are identical with lymphocyte-activating
factors made by rabbit alveolar macrophages. J Immunol 1980; 124:
2498 501.
15. Dinarello CA, Rosenwasser LJ. Lymphocyte activating property of human leukocytic pyrogen. In: Hadden J, Chedid L, Mullen D, Spreafico
F, eds. Advances in immunopharmacology. Oxford: Pergamon Press,
1981:419 25.
16. Lachman LB. Interleukin-1; release from LPS-stimulated mononuclear
phagocytes. In: Nowotny A, ed. Beneficial effects of endotoxin. New
York: Plenum, 1983:283 305.
17. Gordon AH, Parker ID. A pyrogen derived from human white cells which
is active in mice. Br J Exp Pathol 1980; 61:534 9.
18. Sztein MB, Vogel SN, Sipe JD, et al. The role of macrophages in the
acute-phase response: SAA inducer is closely related to lymphocyte
activating factor and endogenous pyrogen. Cell Immunol 1981; 63:
164 76.
19. Beer DJ, Dinarello CA, Rosenwasser LJ, Rocklin RE. Cell-cell interactions in the expression of histamine-induced suppressor cell activity.
In: Dixon FJ, Meischer PA, eds. VIII International Symposium on
Immunopathology. New York: Academic Press, 1982:77 92.
20. Dinarello CA. Interleukin-1. Rev Infect Dis 1984; 6:51 95.
21. Root RK, Nordlund JJ, Wolff SM. Factors affecting the quantitative
production and assay of human leukocytic pyrogen. J Lab Clin Med
1970; 75:679 93.
22. Lachman LB. Human interleukin 1: purification and properties. Fed Proc
1984; 42:2639 45.
23. Lomedico PT, Gubler R, Hellmann CP, et al. Cloning and expression of
murine interleukin-1 cDNA in Escherichia coli. Nature 1984; 312:
458 62.
24. Auron PE, Webb AC, Rosenwasser LJ, et al. Nucleotide sequence of
human monocyte interleukin 1 precursor cDNA. Proc Natl Acad Sci
USA 1984; 81:7907 11.
25. Van Damme J, De Ley M, Opdenakker G, Billiau A, De Somer P.
Homogeneous interferon-inducing 22K factor is related to endogenous
pyrogen and interleukin-1. Nature 1985; 314:266 8.
26. Dinarello CA, Cannon JG, Mier JW, et al. Multiple biological activities
of human recombinant interleukin 1. J Clin Invest 1986; 77:1734 9.
27. Dinarello CA, Cannon JG, Mancilla J, Bishai I, Lees J, Coceani F.
Interleukin-6 as an endogenous pyrogen: induction of prostaglandin
E2 in brain but not in peripheral blood mononuclear cells. Brain Res
1991; 562:199 206.
28. Dinarello CA, Cannon JG, Wolff SM, et al. Tumor necrosis factor
(cachectin) is an endogenous pyrogen and induces production of interleukin 1. J Exp Med 1986; 163:1433 50.
29. Shapiro L, Zhang XX, Rupp RG, Wolff SM, Dinarello CA. Ciliary neurotrophic factor is an endogenous pyrogen. Proc Natl Acad Sci USA
1993; 90:8614 8.
30. Blatteis CM, Bealer SL, Hunter WS, Llanos QJ, Ahokas RA, Mashburn
TA Jr. Suppression of fever after lesions of the anteroventral third
ventricle in guinea pigs. Brain Res Bull 1983; 11:519 26.
31. Stitt JT. Evidence for the involvement of the organum vasculosum laminae terminalis in the febrile response of rabbits and rats. J Physiol
1985; 368:501 11.
31a. Dascombe MJ. Cyclic nucleotides and fever. In: Milton AS, ed. Pyretics
and antipyretics. Heidelberg, Germany: Springer-Verlag, 1982: 219
55.
32. Rossi V, Breviario F, Ghezzi P, Dejana E, Mantovani A. Prostacyclin
synthesis induced in vascular cells by interleukin-1. Science 1985; 229:
174 6.
33. Bevilacqua MP, Pober MS, Wheeler ME, Cotran RS, Gibrone MA Jr.
Interleukin 1 acts on cultured human vascular endothelium to increase
the adhesion of polymorphonuclear leukocytes, monocytes, and related
leukocyte cell lines. J Clin Invest 1985; 76:2003 11.
UC: J Infect
Downloaded from http://jid.oxfordjournals.org/ by guest on September 26, 2015
from the circulation. In addition, IL-1 and TNF are removed
from the circulation via the distal tubule, where they bind
to uromodulin. There are also carrier proteins, such as a2macroglobulin, that bind IL-1 and IL-6. The extraction procedure appears to facilitate this binding interaction. When IL-1b
is extracted using chloroform, it becomes measurable. After
extraction with chloroform, IL-1b can be detected in the circulation of human volunteers receiving endotoxin [111, 112].
Measurements of TNF-a and IL-6 are more reliable than the
measurement of IL-1b. In fact, the best correlations of disease
activity (including fever) are with the cytokine IL-6. In sepsis,
rheumatoid arthritis, inflammatory bowel disease, and acute
coronary syndromes, the levels of IL-6 are higher in patients
with worsening disease. Although one can also make associations with elevated circulating levels of IL-1b in rheumatoid
arthritis [113], measuring IL-6 levels is more reliable. This is
because the amount of IL-6 compared with IL-1b or TNF-a
is at least 1 log greater. Nevertheless, IL-6 levels fall dramatically in septic patients being treated with IL-1 receptor antagonist [114] and in rheumatoid arthritis patients being treated with
anti TNF-a antibodies [115]. Therefore, similar to findings in
animal studies [116], IL-6 appears to be under the influence
of IL-1 and TNF.
JID 1999;179 (Suppl 2)
JID 1999;179 (Suppl 2)
Cytokines as Endogenous Pyrogens
/ 9d5b$$fe24
01-13-99 07:35:41
jinfa
55. Tilg H, Atkins MB, Dinarello CA, Mier JW. Induction of circulating
interleukin-10 by interleukin-1 and interleukin-2, but not interleukin6 immunotherapy. Cytokine 1995; 7:734 9.
56. Bargetzi MJ, Lantz M, Smith CG, et al. Interleukin-1 beta induces interleukin-1 receptor antagonist and tumor necrosis factor binding proteins. Cancer Res 1993; 53:4010 3.
57. Beutler B, Cerami A. Cachectin and tumor necrosis factor as two sides
of the same biological coin. Nature 1986; 320:584 8.
58. Bachwich PR, Chensue SW, Larrick JW, Kunkel SL. Tumor necrosis
factor stimulates interleukin-1 and prostaglandin E2 production in resting macrophages. Biochem Biophys Res Commun 1986; 136:94 101.
59. Endres S, Ghorbani R, Kelley VE, et al. The effect of dietary supplementation with n-3 polyunsaturated fatty acids on the synthesis of interleukin-1 and tumor necrosis factor by mononuclear cells. N Engl J Med
1989; 320:265 71.
60. Lonnemann G, Endres S, Van der Meer JW, Cannon JG, Koch KM,
Dinarello CA. Differences in the synthesis and kinetics of release of
interleukin 1 alpha, interleukin 1 beta, and tumor necrosis factor from
human mononuclear cells. Eur J Immunol 1989; 19:1531 6.
61. Schindler R, Mancilla J, Endres S, Ghorbani R, Clark SC, Dinarello CA.
Correlations and interactions in the production of interleukin-6 (IL-6),
IL-1, and tumor necrosis factor (TNF) in human blood mononuclear
cells: IL-6 suppresses IL-1 and TNF. Blood 1990; 75:40 7.
62. Engelmann H, Aderka D, Rubinstein M, Rotman D, Wallach D. A tumor
necrosis factor binding protein purified to homogeneity from human
urine protects cells from tumor necrosis factor toxicity. J Biol Chem
1989; 264:11974 80.
63. Novick D, Engelmann H, Wallach D, Rubinstein M. Soluble cytokine
receptors are present in normal human urine. J Exp Med 1989; 170:
1409 14.
64. Zilberstein A, Riggieri R, Korn JH, Revel M. Structure and expression of
cDNA and genes for human interferon-beta-2, a distinct species inducible
by growth-stimulatory cytokines. EMBO J 1986;5:252937.
65. Kawano M, Hirano T, Matsuda T, et al. Autocrine generation and requirement of BSF-2/IL-6 for human multiple myelomas. Nature 1988; 332:
83 5.
66. Gauldie J, Richards C, Harnish D, Lansdorp P, Baumann H. Interferon
b2/B-cell stimulatory factor type 2 shares identity with monocytederived hepatocyte-stimulating factor and regulates the major acute
phase protein response in liver cells. Proc Natl Acad Sci USA 1987;
84:7251 6.
67. Van Oers MHJ, Van Der Heyden AAPAM, Aarden LA. Interleukin 6
(IL-6) in serum and urine of renal transplant recipients. Clin Exp
Immunol 1988; 71:314 9.
68. Nijsten MW, De Groot ER, ten Duis HJ, Klasen HJ, Hack CE, Aarden
LA. Serum levels of interleukin-6 and acute phase responses [letter].
Lancet 1987; 2:921.
69. Van Damme J, Opdenakker G, Simpson RJ, et al. Identification of the
human 26-kD protein, interferon b2 (IFN-b2), as a B cell hybridoma/
plasmacytoma growth factor induced by interleukin 1 and tumor necrosis factor. J Exp Med 1987; 165:914 9.
69a. Bunning RAD, Russell RGG, Van Damme J. Independent induction of
interleukin-6 and prostaglandin E2 by interleukin-1 in human articular
chondrocytes. Biochem Biophys Res Commun 1990; 166:1163 70.
70. Biliau A, Heine JW, Van Damme J, Heremans H, De Somer P. Tolerability of pure fibroblast interferon in man. Ann NY Acad Sci 1980; 350:
374 5.
71. Biliau A. Pharmacokinetic and pharmacological aspects of interferon
therapy in man. Acta Microbiol Acad Sci Hung 1981; 28:257 62.
72. Bocci V. Possible causes of fever after interferon administration. Biomedicine 1980; 32:159 62.
73. Horning SJ, Levine JF, Miller RA, Rosenberg SA, Merigan TC. Clinical
and immunologic effects of recombinant leukocyte A interferon in
eight patients with advanced cancer. JAMA 1982; 247:1718 22.
UC: J Infect
Downloaded from http://jid.oxfordjournals.org/ by guest on September 26, 2015
34. Dustin ML, Rothlein R, Bhan AK, Dinarello CA, Springer TA. Induction
by IL-1 and interferon-g: tissue distribution, biochemistry, and function of a natural adherence molecule (ICAM-1). J Immunol 1986; 137:
245 54.
35. Coceani F, Bishai I, Dinarello CA, Fitzpatrick FA. Prostaglandin E2 and
thromboxane B2 in cerebrospinal fluid of afebrile and febrile cat. Am
J Physiol 1983; 244:R785 93.
36. Dejana E, Breviario F, Erroi A, et al. Modulation of endothelial cell
functions by different molecular species of interleukin 1. Blood 1987;
69:695 9.
37. Pacak F, Siegert R. Chemical characterization of a rabbit leukocytic
pyrogen. Eur J Biochem 1982; 127:375 80.
38. Saklatvala J, Sarsfield SJ, Townsend Y. Pig interleukin 1: purification of
two immunologically different leukocyte proteins that cause cartilage
resorption, lymphocyte activation, and fever. J Exp Med 1985; 162:
1208 22.
39. Hanson DF, Murphy PA. Demonstration of interleukin 1 activity in apparently homogeneous specimens of the pI 5 form of rabbit endogenous
pyrogen. Infect Immun 1984; 45:483 90.
40. Dinarello CA, Bernheim HA, Cannon JG, et al. Purified, 35S-met, 3Hleu-labeled human monocyte interleukin-1 with endogenous pyrogen
activity. Br J Rheumatol 1985; 24(suppl):59 64.
41. Knudsen PJ, Dinarello CA, Strom TB. Purification and characterization
of a unique human interleukin 1 from the tumor cell line U937. J
Immunol 1986; 136:3311 6.
42. Wolff SM, Mulholland JH, Ward SB. Quantitative aspects of the pyrogenic
response of rabbits to endotoxin. J Lab Clin Med 1965;65:26876.
43. Kitamura T, Takaku F. A preclinical and phase I clinical trial of IL-1. J
Exp Med 1989; 7:170 7.
44. Laughlin MJ, Kirkpatrick G, Sabiston N, Peters W, Kurtzberg J. Hematopoietic recovery following high-dose combined alkylating-agent chemotherapy and autologous bone marrow support in patients in phase
I clinical trials of colony stimulating factors: G-CSF, GM-CSF, IL-1,
IL-2, and M-CSF. Ann Hematol 1993; 67:267 76.
45. Tewari A, Buhles WC Jr, Starnes HF Jr. Preliminary report: effects of
interleukin-1 on platelet counts. Lancet 1990; 336:712 4.
46. Nemunaitis J, Appelbaum FR, Lilleby K, et al. Phase I study of recombinant interleukin-1b in patients undergoing autologous bone marrow
transplantation for acute myelogenous leukemia. Blood 1994; 83:
3473 9.
47. Crown J, Jakubowski A, Gabrilove J. Interleukin-1: biological effects in
human hematopoiesis. Leuk Lymphoma 1993; 9:433 40.
48. Smith JW2, Urba WJ, Curti BD, et al. The toxic and hematologic effects
of interleukin-1 alpha administered in a phase I trial to patients with
advanced malignancies. J Clin Oncol 1992; 10:1141 52.
49. Iizumi T, Sato S, Iiyama T, et al. Recombinant human interleukin-1
beta analogue as a regulator of hematopoiesis in patients receiving
chemotherapy for urogenital cancers. Cancer 1991; 68:1520 3.
50. Smith JW, Urba WJ, Curti BD, et al. The toxic and hematologic effects
of interleukin-1 alpha administered in a phase I trial to patients with
advanced malignancies. J Clin Oncol 1992; 10:1141 52.
51. Smith JW, Longo D, Alford WG, et al. The effects of treatment with
interleukin-1a on platelet recovery after high-dose carboplatin. N Engl
J Med 1993; 328:756 61.
52. Crown J, Jakubowski A, Kemeny N, et al. A phase I trial of recombinant
human interleukin-1b alone and in combination with myelosuppressive
doses of 5-fluorouracil in patients with gastrointestinal cancer. Blood
1991; 78:1420 7.
53. van der Poll T, Bueller HR, ten Cate H, et al. Activation of coagulation
after administration of tumor necrosis factor to normal subjects. N
Engl J Med 1990; 322:1622 7.
54. Tilg H, Trehu E, Atkins MB, Dinarello CA, Mier JW. Interleukin-6
(IL-6) as an anti-inflammatory cytokine: induction of circulating IL-1
receptor antagonist and soluble tumor necrosis factor receptor p55.
Blood 1994; 83:113 8.
S303
S304
Dinarello
/ 9d5b$$fe24
01-13-99 07:35:41
jinfa
97.
98.
99.
100.
101.
102.
103.
104.
105.
106.
107.
108.
109.
110.
111.
112.
113.
114.
115.
116.
identification as rabbit interleukin-1b. Biochem Biophys Res Commun
1988; 150:1237 43.
Goto F, Nakamura S, Goto K, Yoshinaga M. Generation of an interleukin1 like lymphocyte-stimulating factor at inflammatory sites: correlation
with the infiltration of polymorphonuclear leukocytes. Br J Exp Pathol
1984; 65:521 32.
Sheng YJ, Bird J, Pompidou A, Florentin I, Giroud JP. Rat and human
polymorphonuclear leukocyte derived lymphocyte stimulatory factors.
Biomed Pharmacother 1984; 38:304 8.
Ohkawara S, Goto K, Mori S, et al. Interleukin-1 production by polymorphonuclear leukocytes during the course of acute inflammation in rabbits. Dermatologica 1989; 179:84 90.
Bell TV, Harley CB, Stetsko D, Sauder DN. Expression of mRNA homologous to interleukin 1 in human epidermal cells. J Invest Dermatol
1987; 88:375 9.
Libby P, Ordovas JM, Birinyi LK, Auger KR, Dinarello CA. Inducible
interleukin-1 gene expression in human vascular smooth muscle cells.
J Clin Invest 1986; 78:1432 8.
Libby P, Ordovas JM, Auger KR, Robbins AH, Birinyi LK, Dinarello
CA. Endotoxin and tumor necrosis factor induce interleukin-1 gene
expression in adult human vascular endothelial cells. Am J Pathol
1986; 124:179 85.
Rambaldi A, Torcia M, Bettoni S, et al. Modulation of cell proliferation
and cytokine production in acute myeloblastic leukemia by interleukin1 receptor antagonist and lack of its expression by leukemic cells.
Blood 1991; 78:3248 53.
Cozzolino F, Torcia M, Aldinucci D, et al. Production of interleukin-1
by bone marrow myeloma cells. Blood 1989; 74:380 7.
Scala G, Kuang YD, Hall RE, Muchmore AV, Oppenheim JJ. Accessory
cell function of human B cells. I. Production of both interleukin 1-like
activity and an interleukin 1 inhibitory factor by an EBV-transformed
human B cell line. J Exp Med 1984; 159:1637 52.
Scala G, Allavena P, Djeu JY, et al. Human large granular lymphocytes
are potent producers of interleukin-1. Nature 1984; 309:56 9.
Sauder DN. Biologic properties of epidermal cell thymocyte-activating
factor (ETAF). J Invest Dermatol 1985; 85(suppl 1):176S 9S.
Bodel P, Ralph P, Wenc K, Long JC. Endogenous pyrogen production
by Hodgkins disease and human histiocytic lymphoma cell lines in
vivo. J Clin Invest 1980; 65:514 8.
Lovett DH, Sterzel RB, Ryan JL, Atkins E. Production of an endogenous
pyrogen by glomerular mesangial cells. J Immunol 1985; 134:670 2.
Cannon JG, Van der Meer JW, Kwiatkowski D, et al. Interleukin-1 beta
in human plasma: optimization of blood collection, plasma extraction,
and radioimmunoassay methods. Lymphokine Res 1988; 7:457 67.
Granowitz EV, Santos A, Poutsiaka DD, et al. Circulating interleukin-1
receptor antagonist levels during experimental endotoxemia in humans.
Lancet 1991; 338:1423 4.
Cannon JG, Tompkins RG, Gelfand JA, et al. Circulating interleukin-1
and tumor necrosis factor in septic shock and experimental endotoxin
fever. J Infect Dis 1990; 161:79 84.
Eastgate JA, Symons JA, Wood NC, Grinlinton FM, di Giovine FS, Duff
GW. Correlation of plasma interleukin 1 levels with disease activity
in rheumatoid arthritis. Lancet 1988; 2:706 9.
Fisher CJJ, Slotman GJ, Opal SM, et al. Initial evaluation of human
recombinant interleukin-1 receptor antagonist in the treatment of sepsis
syndrome: a randomized, open-label, placebo-controlled multicenter
trial. Crit Care Med 1994; 22:12 21.
Elliott MJ, Maini RN, Feldmann M, et al. Randomised double-blind
comparison of chimeric monoclonal antibody to tumour necrosis factor
alpha (cA2) versus placebo in rheumatoid arthritis. Lancet 1994; 344:
1105 10.
Fantuzzi G, Dinarello CA. The inflammatory response in interleukin1b deficient mice: comparison with other cytokine-related knock-out
mice. J Leukoc Biol 1996; 59:489 93.
UC: J Infect
Downloaded from http://jid.oxfordjournals.org/ by guest on September 26, 2015
74. Dinarello CA, Bernheim HA, Duff GW, et al. Mechanisms of fever induced
by recombinant human interferon. J Clin Invest 1984;74:90613.
75. Lane HC, Fauci AS. Immunologic reconstitution in the acquired immunodeficiency syndrome. Ann Intern Med 1985; 103:714 8.
76. Kurzrock R, Quesada JR, Rosenblum MG, Sherwin SA, Gutterman JU. Phase
I study of iv administered recombinant gamma interferon in eight patients
with advanced cancer. Cancer Treat Res 1986;70:135764.
77. Dinarello CA, Ikejima T, Warner SJ, et al. Interleukin 1 induces interleukin 1. I. Induction of circulating interleukin 1 in rabbits in vivo and
in human mononuclear cells in vitro. J Immunol 1987; 139:1902 10.
78. Ghezzi P, Dinarello CA. IL-1 induces IL-1. III. Specific inhibition of IL1 production by IFN-gamma. J Immunol 1988; 140:4238 44.
79. Schindler R, Ghezzi P, Dinarello CA. IL-1 induces IL-1. IV. IFN-g
suppresses IL-1 but not lipopolysaccharide-induced transcription of
IL-1. J Immunol 1990; 144:2216 22.
80. Schindler R, Dinarello CA. A method for removing interleukin-1 and tumor
necrosis factorinducing substances from bacterial cultures by ultrafiltration
with polysulfone. J Immunol Methods 1989;116:15965.
81. Lotze MT, Matory YL, Rayner AA, et al. Clinical effects and toxicity
of interleukin-2 in patients with cancer. Cancer 1986; 58:2764 72.
82. Atkins MB, Gould JA, Allegretta M, et al. Phase I evaluation of recombinant interleukin-2 in patients with advanced malignant disease. J Clin
Oncol 1986; 4:1380 91.
83. Nedwin GE, Svdersky LP, Bringman TS, Palladino MA Jr, Goeddel
DV. Effect of interleukin 2, interferon-gamma, and mitogens on the
production of tumor necrosis factors alpha and beta. J Immunol 1985;
135:2492 7.
84. Mier JW, Souza LM, Allegretta M, Boone T, Bernheim HA, Dinarello CA.
Dissimilarities between purified human interleukin-1 and recombinant human interleukin-2 in the induction of fever, brain prostaglandin, and acutephase protein synthesis. J Biol Response Modif 1985;4:3545.
85. Mier JW, Vachino G, Van der Meer JW, et al. Induction of circulating
tumor necrosis factor (TNF alpha) as the mechanism for the febrile
response to interleukin-2 (IL-2) in cancer patients. J Clin Immunol
1988; 8:426 36.
86. Snell ES, Atkins E. The presence of endogenous pyrogen in normal rabbit
tissues. J Exp Med 1965; 121:1019 38.
87. Atkins E, Bodel P, Francis L. Release of an endogenous pyrogen in vitro
from rabbit mononuclear cells. J Exp Med 1967; 126:357 84.
88. Bodel P, Atkins E. Release of endogenous pyrogen by human monocytes.
N Engl J Med 1967; 276:1002 13.
89. Hahn HH, Char DC, Postel WB, Wood WB Jr. Studies on the pathogenesis of fever. XV. The production of endogenous pyrogen by peritoneal
macrophages. J Exp Med 1967; 126:385 94.
90. Hanson DF, Murphy PA, Windle BE. Failure of rabbit neutrophils to
secrete endogenous pyrogen when stimulated with staphylococci. J
Exp Med 1980; 151:1360 71.
91. Windle BE, Murphy PA, Cooperman S. Rabbit polymorphonuclear leukocytes do not secrete pyrogens of interleukin 1 when stimulated by
endotoxin, polyinosine:polycytosine, or muramyl dipeptide. Infect Immun 1983; 39:1142 6.
92. Tiku K, Tiku ML, Skosey JL. Interleukin 1 production by human polymorphonuclear neutrophils. J Immunol 1986; 136:3677 85.
93. Canning PC, Neill JD. Isolation and characterization of interleukin-1
from bovine polymorphonuclear leukocytes. J Leukoc Biol 1989; 45:
21 8.
94. Goh K, Furusawa S, Kawa Y, Negishi-Okitsu S, Mizoguchi M. Production
of interleukin-1 alpha and beta by human peripheral polymorphonuclear
neutrophils. Int Arch Allergy Appl Immunol 1989;88:297303.
95. Goto F, Goto K, Ohkawara S, et al. Purification and partial sequence of rabbit
polymorphonuclear leukocyte-derived lymphocyte proliferation potentiating
factor resembling IL-1 beta. J Immunol 1988;140:11538.
96. Mori S, Goto F, Goto K, et al. Cloning and sequence analysis of a cDNA
for lymphocyte proliferation potentiating factor of rabbit neutrophils:
JID 1999;179 (Suppl 2)
You might also like
- The Yellow House: A Memoir (2019 National Book Award Winner)From EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Rating: 4 out of 5 stars4/5 (98)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceFrom EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceRating: 4 out of 5 stars4/5 (895)
- Hyperalgesia in The Setting of AnxietyDocument1 pageHyperalgesia in The Setting of AnxietynikuNo ratings yet
- Curriculum Vitae: ExperienceDocument2 pagesCurriculum Vitae: ExperiencenikuNo ratings yet
- Sunita Apticon15Document3 pagesSunita Apticon15nikuNo ratings yet
- Scott Reuschel TANDEM LABS - Regulated Bioanlysis For The Pharmaceutical IndustryDocument33 pagesScott Reuschel TANDEM LABS - Regulated Bioanlysis For The Pharmaceutical IndustrynikuNo ratings yet
- Following OvulationDocument1 pageFollowing OvulationnikuNo ratings yet
- Balram Jadhav CVDocument3 pagesBalram Jadhav CVnikuNo ratings yet
- Synopsis EditedDocument8 pagesSynopsis EditednikilNo ratings yet
- PKCDocument52 pagesPKCnikuNo ratings yet
- Genome Mapping: Paul H DearDocument7 pagesGenome Mapping: Paul H DearvidpoohNo ratings yet
- CytokininDocument7 pagesCytokininPablo AlbanNo ratings yet
- Overdose Dan ToxikasiDocument44 pagesOverdose Dan ToxikasiRandi N. FarizaNo ratings yet
- ELSI Working Group 1st ReportDocument9 pagesELSI Working Group 1st ReportnikuNo ratings yet
- NeuropeptidesDocument36 pagesNeuropeptidesnikuNo ratings yet
- Chrono 3Document9 pagesChrono 3nikuNo ratings yet
- Systemic Target Single ExposureDocument10 pagesSystemic Target Single ExposurenikuNo ratings yet
- Chrono 4Document27 pagesChrono 4nikuNo ratings yet
- Management PoisoningDocument6 pagesManagement PoisoningatifdocNo ratings yet
- Pharmacologic Activity of Phosphodiesterases and Their InhibitorsDocument15 pagesPharmacologic Activity of Phosphodiesterases and Their InhibitorsnikuNo ratings yet
- Hyperalgesia in The Setting of AnxietyDocument1 pageHyperalgesia in The Setting of AnxietynikuNo ratings yet
- Chrono 2Document5 pagesChrono 2nikuNo ratings yet
- Teach Tox SlidesDocument23 pagesTeach Tox SlidesnikuNo ratings yet
- Systemin Target Repeated ExposureDocument11 pagesSystemin Target Repeated ExposurenikuNo ratings yet
- Pro Kinase CDocument9 pagesPro Kinase CnikuNo ratings yet
- Week2PostHoc 03Document22 pagesWeek2PostHoc 03nikuNo ratings yet
- United States: (12) Patent Application Publication (10) Pub. No.: US 2013/0052239 A1Document22 pagesUnited States: (12) Patent Application Publication (10) Pub. No.: US 2013/0052239 A1nikuNo ratings yet
- NIH Public Access: Author ManuscriptDocument24 pagesNIH Public Access: Author ManuscriptnikuNo ratings yet
- United States: (12) Patent Application Publication (10) Pub. No.: US 2011/0206766 A1Document20 pagesUnited States: (12) Patent Application Publication (10) Pub. No.: US 2011/0206766 A1nikuNo ratings yet
- Us 20100323011Document15 pagesUs 20100323011nikuNo ratings yet
- NPP 2009222 ADocument12 pagesNPP 2009222 AnikuNo ratings yet
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeFrom EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeRating: 4 out of 5 stars4/5 (5794)
- The Little Book of Hygge: Danish Secrets to Happy LivingFrom EverandThe Little Book of Hygge: Danish Secrets to Happy LivingRating: 3.5 out of 5 stars3.5/5 (399)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaFrom EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaRating: 4.5 out of 5 stars4.5/5 (266)
- Shoe Dog: A Memoir by the Creator of NikeFrom EverandShoe Dog: A Memoir by the Creator of NikeRating: 4.5 out of 5 stars4.5/5 (537)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureFrom EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureRating: 4.5 out of 5 stars4.5/5 (474)
- Never Split the Difference: Negotiating As If Your Life Depended On ItFrom EverandNever Split the Difference: Negotiating As If Your Life Depended On ItRating: 4.5 out of 5 stars4.5/5 (838)
- Grit: The Power of Passion and PerseveranceFrom EverandGrit: The Power of Passion and PerseveranceRating: 4 out of 5 stars4/5 (588)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryFrom EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryRating: 3.5 out of 5 stars3.5/5 (231)
- The Emperor of All Maladies: A Biography of CancerFrom EverandThe Emperor of All Maladies: A Biography of CancerRating: 4.5 out of 5 stars4.5/5 (271)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyFrom EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyRating: 3.5 out of 5 stars3.5/5 (2259)
- On Fire: The (Burning) Case for a Green New DealFrom EverandOn Fire: The (Burning) Case for a Green New DealRating: 4 out of 5 stars4/5 (73)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersFrom EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersRating: 4.5 out of 5 stars4.5/5 (344)
- Team of Rivals: The Political Genius of Abraham LincolnFrom EverandTeam of Rivals: The Political Genius of Abraham LincolnRating: 4.5 out of 5 stars4.5/5 (234)
- The Unwinding: An Inner History of the New AmericaFrom EverandThe Unwinding: An Inner History of the New AmericaRating: 4 out of 5 stars4/5 (45)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreFrom EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreRating: 4 out of 5 stars4/5 (1090)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)From EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Rating: 4.5 out of 5 stars4.5/5 (121)
- Her Body and Other Parties: StoriesFrom EverandHer Body and Other Parties: StoriesRating: 4 out of 5 stars4/5 (821)
- Retinoid Receptors and Therapeutic Applications of RAR/RXR ModulatorsDocument23 pagesRetinoid Receptors and Therapeutic Applications of RAR/RXR ModulatorsAKellyNMNo ratings yet
- 155:411 Introduction To Biochemical Engineering Fall 2012 Exam 1 October 10, 2012 From 5:00-8:00 P.MDocument2 pages155:411 Introduction To Biochemical Engineering Fall 2012 Exam 1 October 10, 2012 From 5:00-8:00 P.Mmanthan2120% (1)
- Confidential 1 Pr110 WatermarkDocument51 pagesConfidential 1 Pr110 WatermarkMarissa AldeNo ratings yet
- Nutrition Answers FinalDocument9 pagesNutrition Answers FinalelizabethNo ratings yet
- DLP - Tomatom. Science 10. q3 - DNA REPLICAtionDocument10 pagesDLP - Tomatom. Science 10. q3 - DNA REPLICAtionalchristian tomatomNo ratings yet
- MS MLPA Protocol One Tube MSP v008Document19 pagesMS MLPA Protocol One Tube MSP v008Sp PpvNo ratings yet
- Evolution-History and EvidenceDocument19 pagesEvolution-History and Evidencekatexxx100% (1)
- General Biology 1 Summative Assessment Week 1-4Document2 pagesGeneral Biology 1 Summative Assessment Week 1-4Cherrina Aguila100% (1)
- Human Excretory SystemDocument2 pagesHuman Excretory SystemVio ElenaNo ratings yet
- Lec 2 Part 2Document34 pagesLec 2 Part 2Ahmed JamalNo ratings yet
- Cytogenetics Transes Topic 16Document5 pagesCytogenetics Transes Topic 16Dianne NolascoNo ratings yet
- Sysoeva Chemical Composition Andbiological Activity of Triterpenes and Steroids of Chaga MushroomDocument8 pagesSysoeva Chemical Composition Andbiological Activity of Triterpenes and Steroids of Chaga MushroomMachfud FauziNo ratings yet
- Lecture 7Document68 pagesLecture 7Gay TonyNo ratings yet
- Usman Public School System: 1 Monthly Test Mid-Term 2018 - 2019Document3 pagesUsman Public School System: 1 Monthly Test Mid-Term 2018 - 2019Huzaifa KhanNo ratings yet
- OPfr4 2Document13 pagesOPfr4 26E Rivera Cervantes Osiris MargaritaNo ratings yet
- J Zool Syst Evol Res - 2020 - Khan - Molecular Phylogeny of Eremias SPP From Pakistan Contributes To A BetterDocument18 pagesJ Zool Syst Evol Res - 2020 - Khan - Molecular Phylogeny of Eremias SPP From Pakistan Contributes To A BettershakeeNo ratings yet
- Daftar Pustaka PembahasanDocument2 pagesDaftar Pustaka PembahasanMaryam Fathiya RinthaniNo ratings yet
- Green Life Cycle Science Butterfly Graphic OrganizerDocument1 pageGreen Life Cycle Science Butterfly Graphic OrganizerAlexia SalvadorNo ratings yet
- Rocafort Et Al., 2020 Apoplastic Effector Proteins of Plant-Associated Fungi and Oomycetes PDFDocument11 pagesRocafort Et Al., 2020 Apoplastic Effector Proteins of Plant-Associated Fungi and Oomycetes PDFJuan Muñoz CuellarNo ratings yet
- Week 2 - Text 1. Ecosystems and Human InterferencesDocument2 pagesWeek 2 - Text 1. Ecosystems and Human Interferences458 269 Cinta Alivia AthaNo ratings yet
- Biology Navneet Practice Paper - 240102 - 221900Document27 pagesBiology Navneet Practice Paper - 240102 - 221900deepak hutthyNo ratings yet
- Clinical Radio Biology - Previous Examination Papers Updated 040108Document12 pagesClinical Radio Biology - Previous Examination Papers Updated 040108sawiHijau100% (3)
- Anatomi TumbuhanDocument30 pagesAnatomi TumbuhanMEISYI DSNo ratings yet
- TuberculosisDocument16 pagesTuberculosisjojolim18100% (1)
- HSA. Past Papers With Answer SDocument33 pagesHSA. Past Papers With Answer SAaron Baker100% (1)
- Els Reviewer 2nd QuarterDocument8 pagesEls Reviewer 2nd QuarterKaezzy Yen RequermeNo ratings yet
- Acinetobacter BaumanniiDocument12 pagesAcinetobacter BaumanniiGIST (Gujarat Institute of Science & Technology)No ratings yet
- XXXDocument134 pagesXXXrhlzuraNo ratings yet
- Ijms 23 03754Document14 pagesIjms 23 03754Benyam ZenebeNo ratings yet
- CHAPTER 16 MicroparaDocument46 pagesCHAPTER 16 MicroparaKathlyn LopeñaNo ratings yet