Professional Documents
Culture Documents
Marcadores de Vulnerabilidad en El Espectro Esquizofrenico
Uploaded by
Oscar Alejandro Cardenas QuinteroCopyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Marcadores de Vulnerabilidad en El Espectro Esquizofrenico
Uploaded by
Oscar Alejandro Cardenas QuinteroCopyright:
Available Formats
Psychiatr Clin N Am 25 (2002) 837853
Vulnerability markers in the schizophrenia
spectrum: implications for phenomenology,
genetics, and the identication
of the schizophrenia prodrome
Kristin S. Cadenhead, MD*
Department of Psychiatry, University of California, San Diego,
9500 Gilman Drive, La Jolla, CA 92093-0810, USA
The history of the schizophrenia spectrum and
schizotypal personality disorder
The schizophrenia spectrum describes what is most likely a continuum
of illnesses that include the more severe Kraepelinean schizophrenia,
schizophrenia-related personality disorders, and the relatively mild and
nonclinical phenotypic decits observed in family members of schizophrenia patients. For nearly a century, nonpsychotic psychopathology, which
seems to be a subsyndromal form of schizophrenia symptoms, has been
observed in family members of schizophrenia patients [15] and individuals
with no family history of schizophrenia [6,7]. The concept of the schizophrenia spectrum of disorders rst emerged from early observations of family
members of schizophrenia patients. Bleuler [1] described these relatives as
odd or eccentric without the overt psychotic symptoms of a schizophrenia
patient and labeled them latent schizophrenics. Robert Knight [8] used the
term borderline states to describe individuals who resided on the border
between neurosis and psychosis. Kretschmer [9] described a temperamental
predisposition to schizophrenia, or schizoid personality, often seen in relatives of schizophrenia patients. Rado [10] coined the term schizotype to
describe a group of patients who seemed to have a schizophrenia phenotype
* E-mail address: Kcadenhead@ucsd.edu (K.S. Cadenhead).
Financial support provided by the National Institute of Mental Health grants MH-01124,
MH18399, MH51129, and MH-42228, a NARSAD Young Investigator Award, and the
Department of Veterans Aairs VISN 22 Mental Illness Research Education and Clinical
Center (MIRECC).
0193-953X/02/$ - see front matter 2002, Elsevier Science (USA). All rights reserved.
PII: S 0 1 9 3 - 9 5 3 X ( 0 2 ) 0 0 0 2 1 - 7
838
K.S. Cadenhead / Psychiatr Clin N Am 25 (2002) 837853
that was present throughout life and represented a genetic predisposition to
schizophrenia. Later, Meehl [11] used the term schizotaxia to describe a
neural integrative defect that by the unusual processes of social learning
develops into the schizotype personality structure proposed by Rado.
Kety et al [12] described signs and symptoms of borderline schizophrenia based on clinical observations of family members of schizophrenia
patients and descriptions of patients who displayed magical or psychoticlike thinking and transient psychoses [7]. Because many of the natural
relatives of schizophrenia patients were raised with their aected family
member, it was hard to ascertain to what extent their symptoms, syndromes,
and diagnoses were inuenced by genetic versus environmental factors. In
their seminal Danish adoption study, Kety et al provided some of the rst
genetic evidence that supported the spectrum concept of schizophrenia by
nding increased rates of latent, borderline, and uncertain schizophrenia, as per DSM-II, in family members of schizophrenia patients. In a replication of their early study, Kety et al [3] reported an 8.2% prevalence rate
of latent schizophrenia in biologic relatives of chronic schizophrenia adoptees. Kendler et al [2] applied DSM-III criteria to Ketys sample and found
an increased prevalence of schizotypal personality disorder (SPD) in relatives of schizophrenia spectrum adoptees. A surprising nding in Kendlers
study was that the prevalence of SPD was highest in biologic relatives of
schizotypal adoptees [13].
Schizotypal personality disorder rst appeared in DSM-III after research
began to show that not all individuals described as borderline were related
to schizophrenia as initially described [14,15]. Spitzer et al [16] divided borderlines into borderline personality disorder, as described by Gunderson
and Singer [17], and SPD using information from Kety et als [12] study
of relatives of schizophrenics and clinical data regarding prodromal
signs and symptoms from psychiatric outpatients. Despite this division,
subsequent studies reported considerable overlap or comorbidity of the two
groups [18]. Pope [19] and others [20] suggested that the positive symptoms
noted in some SPD individuals might reect aective disorders or borderline
personality disorder rather than schizophrenia spectrum disorder. Other
investigators have subdivided the criteria for SPD into two psychopathologic dimensions that correspond to the psychotic and decit symptoms
observed in schizophrenia: cognitive/perceptual (ideas of reference, paranoia, odd speech, unusual perceptions, odd behavior, or appearance) and
social/interpersonal (few friends, inappropriate or constricted aect,
social anxiety) [21].
Siever [22] has suggested that the psychotic-like and social decit
symptoms describe two distinct aspects of schizotypy with dierent modes
of genetic transmission and corresponding distinct underlying neuropathologic substrates. Sievers [22] model proposes that when both sets of symptoms and decits occur in the same individual, the result is schizophrenia.
Consistent with Sievers hypothesis, Kendlers [23] monozygotic twin study
K.S. Cadenhead / Psychiatr Clin N Am 25 (2002) 837853
839
demonstrated that the positive and negative schizotypy were independently
heritable. More recently, three factor models of schizotypal symptoms have
been dened using psychometric scales, clinical SPD populations, or relatives of schizophrenia patients [2428]. Depending on the means of symptom assessment and population used, the factor structure varies. Whereas
most of the models identify positive and negative dimensions, the third proposed factor has included disorganization, oddness, or social impairment.
The question as to which specic clinical criteria best dene a schizophrenia phenotype has been addressed through genetic and long-term follow-up
studies in individuals believed to be at risk for schizophrenia. Family studies
[2,29,30] have found increased rates of SPD in biologic relatives of schizophrenia patients using DSM-III criteria and have emphasized the social
decit or negative criteria as being the better discriminators of relatedness
to schizophrenia [17,31]. There is also some evidence of a genetic link between
other cluster A personality disorders (paranoid and schizoid) and schizophrenia, although the data tend to be less conclusive [3237]. Long-term
follow-up of individuals believed to be at risk for schizophrenia has shown
that the SPD criteria that are most predictive of a later diagnosis of schizophrenia are magical thinking, suspiciousness or paranoid ideation, and
social isolation [38]. The empirically based diagnostic criteria for SPD continue to be rened with the goal of establishing criteria that identify individuals who are genotypically linked to schizophrenia (DSM-IV).
The prevalence of SPD is generally believed to be 3% in the general
population while family-genetic studies have determined that 10% to 15%
of relatives of schizophrenic patients have an increased risk of SPD
[2,3,30,32,3941]. Relatively few studies have assessed the relatives of individuals diagnosed with SPD [13,33,36,4246]. Most of the SPD family studies have found that 4% to 5% of the relatives of SPD subjects have
schizophrenia [33,36,43,46,47] and an even greater number (9%18%) meet
criteria for SPD, which suggests that a genetic vulnerability for SPD may be
transmitted independently. The rate of schizophrenia in siblings of a person
with schizophrenia also is higher if a parent is diagnosed with SPD [13].
Kendler [2,13] has suggested that SPD may be a more common phenotypic
expression of a genetic diathesis to the schizophrenia-related disorders than
is chronic schizophrenia itself.
The DSM-IV diagnostic criteria for schizotypal personality disorder
dene a heterogeneous group of individuals with a mix of social/interpersonal, perceptual, and disorganized symptoms who may or may not have a family history of schizophrenia and be at risk for developing schizophrenia. It
is possible that SPD is genetically identical to schizophrenia but is a milder
phenotype because of less penetrance, protective factors, or the lack of nongenetic factors such as viral or toxic insults. What is more likely is that
only a subset of SPD subjects is genetically identical or closely linked to
schizophrenia. The identication of vulnerability markers in SPD subjects
and relatives of schizophrenic patients has become increasingly important
840
K.S. Cadenhead / Psychiatr Clin N Am 25 (2002) 837853
because it provides a means of assessing phenotypic traits of the schizophrenia spectrum that may not be grossly evident clinically [48,49]. It is possible
that vulnerability markers can identify trait-linked abnormalities that are
common to the nonpsychotic schizophrenia spectrum disorders and potentially identify more homogeneous subgroups that are linked to specic pathophysiologic processes [50]. Because these schizophrenia spectrum groups
may have some genetic vulnerability to schizophrenia but do not have many
of the confounding variables (chronic illness, medication eects, and multiple hospitalizations) seen in schizophrenic patients, this research can provide
important information regarding the core decits of schizophrenia spectrum
subjects that are directly related to functional outcome. Since individuals
with SPD do not usually manifest the more generalized decits of chronic
schizophrenia patients, the study of this population may add insight into the
primary (versus generalized) decits of schizophrenia patients.
Vulnerability markers in the schizophrenia spectrum
Abnormalities of attention, cognition, and information processing in
schizophrenia patients have long been recognized [51]. Psychophysiologic
and neuropsychological measures of information processing have been used
to quantify these cognitive abnormalities and may represent vulnerability
markers that are possible endophenotypes for schizophrenia spectrum illness [52]. The neurobiologic measures may assess traits that are tied closer
to brain function than are the clinical diagnostic categories for schizophrenia spectrum illness that probably represent relatively remote and variable
aspects of genes that predispose to schizophrenia [53]. If vulnerability
markers could be used in conjunction with clinical criteria to better identify
individuals who are at risk for developing psychosis (see later section), it
may be possible to intervene early in the course of prodromal schizophrenia
and perhaps prevent some of the devastating eects of the illness.
Measures of central inhibition
Researchers have hypothesized that the observed attention and cognitive
abnormalities of schizophrenia spectrum subjects are secondary to decits
in inhibitory functioning that cause sensory inundation by external and
internal stimuli [55]. Schizophrenia patients, their relatives, and SPD subjects have decits when assessed in various psychophysiologic paradigms,
including prepulse inhibition (PPI) of the startle response [5557], P50
event-related potential suppression [5860], and the antisaccade (AS) task
[6163]. These three tasks have been designed to study central inhibition.
Prepulse inhibition of the startle response
Prepulse inhibition of the startle response is an operational measure of
sensorimotor gating in which weak prestimuli are presented at brief intervals
K.S. Cadenhead / Psychiatr Clin N Am 25 (2002) 837853
841
(eg, 100 msec) before a startle-eliciting stimulus, which reduces the magnitude of the response [55,64]. In humans, PPI is quantied by assessing the
reduction in the magnitude of the blink reex component of the startle
response to startle eliciting stimuli versus trials that also include a prepulse
stimulus. PPI is a stable neurobiologic marker with high reliability across
repeated test sessions [65]. Schizophrenia patients [55,6669], SPD subjects
[56,57], and clinically unaected relatives of schizophrenia patients have
reduced PPI [57] when compared to normal comparison subjects, which suggests that PPI is potentially a useful endophenotype in the study of schizophrenia spectrum disorders [70]. The use of nonmedicated SPD subjects is
particularly important because there is some evidence from between-subjects
schizophrenia studies that atypical versus typical neuroleptic treatment may
improve PPI [67,69]. Consistent with the data in patients, in an animal model
of schizophrenia-linked PPI decits, PPI decits induced in rats by apomorphine or phencyclidine (PCP) are reversed by neuroleptic medication [71].
Although the heritability of PPI has not been assessed denitively, aective modulation of the startle response seems to be at least partially under
genetic control because monozygotic (but not dizygotic) twins show similar
changes in startle magnitude in this paradigm [72]. Sibling pairs (one with
schizophrenia, one without schizophrenia) from a recent PPI family study
[57] show relatively high PPI correlations (n 13 pairs, R 0.66), which
adds support to the notion that PPI is a heritable vulnerability trait. Preliminary work has shown evidence of high PPI heritability in mice [73,74], and
Joober et al [75] have reported a series of overlapping quantitative trait loci
mediating startle and PPI in mice, which suggests that mammalian PPI is
under genetic inuence.
P50 event-related potential suppression
In the conditioning-testing P50 paradigm [76], two rapid auditory click
stimuli are presented 500 msec apart and the P50 event-related potential
response to both clicks is assessed. In normal subjects there is suppression
of the second P50 wave that is believed to be related to the activation of
inhibitory processing and circuitry by the rst P50 stimulus. Normal P50
gating is present by late adolescence [77,78]. P50 suppression is a stable trait
[79,80] with high heritability. Schizophrenia patients [48,8183], SPD subjects [58], and relatives of schizophrenia patients [60,84,85] all have reduced
P50 suppression compared to normal comparison subjects. The nding of
P50 suppression decits in SPD subjects and relatives of schizophrenia
patients suggests that the P50 paradigm assesses trait markers for schizophrenia spectrum illness. P50 suppression has been linked with a genetic
marker at the locus of the alpha-7 subunit of the nicotinic receptor in a
study of schizophrenia kindreds [48]. This linkage nding is the rst one
to link a candidate endophenotype of information processing decits in
schizophrenia to a specic chromosomal region. As in the PPI literature,
it seems that atypical antipsychotic medications may at least partially
842
K.S. Cadenhead / Psychiatr Clin N Am 25 (2002) 837853
reverse the P50 suppression decits of schizophrenia patients [8689]. Studies of SPD subjects, rst break and nonmedicated schizophrenia patients,
and relatives of schizophrenia patients are essential.
Antisaccade paradigm
The antisaccade task is a measure of saccadic inhibition that requires subjects to look in the opposite direction of a computer-generated cue. Schizophrenia patients, their nonpsychotic rst-degree biologic relatives, and SPD
subjects generate an increased proportion of antisaccade errors [61,63,90].
Poor antisaccade performance correctly identied 70% of schizophrenia
patients and 25% to 50% of these patients nonpsychotic rst-degree relatives in three samples [91].
Convergence and divergence across inhibitory measures
in schizotypal subjects
In a recent study [92], the question was asked whether the decits in
inhibition observed in SPD subjects on measures of PPI, P50, and antisaccade are present in all SPD subjects or if distinct subgroups of SPD subjects
can be identied on the basis of their performance on these measures. The
authors also questioned whether it was possible to dene an endophenotype
using measures of inhibitory functions within a population of SPD subjects
for use in future genetic studies [70]. The results of this study suggest that the
inhibitory decits measured by the P50 and antisaccade paradigms are signicantly correlated and are present in a signicant subgroup of subjects
with SPD, whereas the PPI paradigm seems to identify a distinct subgroup
of subjects. The relationship between P50 and antisaccade performance has
been reported in schizophrenia patients and their relatives, and a composite P50/AS phenotype has been linked to a marker on chromosome 22q
in these families [93]. The use of multiple neurobiologic measures that dene
separate phenotypes and diering neural substrates within schizophrenia
spectrum populations also may provide a means of reducing the heterogeneity characteristic of clinically dened samples. When compared with
clinically dened phenotypes, neurobiologic measures also may assess specic brain function more directly and provide simpler, empirically derived
phenotypes.
The convergence and divergence in performance on the various measures
of inhibitory functioning suggest that there may be overlap in the modulatory neural circuitry responsible for central inhibition on the three tasks.
There also may be important dierences in SPD subjects performance that
may provide insight into separate neurophysiologic substrates that are
implicated in schizophrenia spectrum disorders. Further work using animal
models, functional neuroimaging, or brain mapping may provide clues to the
similar and diering inhibitory functions. Vulnerability markers could be
K.S. Cadenhead / Psychiatr Clin N Am 25 (2002) 837853
843
used not only in genetic analyses [70] but also as predictive variables in studies of individuals at risk for the later development of psychotic illness [94].
Prodromal schizophrenia: the study of individuals at risk for psychosis
Schizophrenia is a devastating disease that often emerges during late adolescence or early adulthood, a crucial phase of psychological and social
development. Although many treatments for schizophrenia are eective,
they are also limited and palliative. The idea of intervening in the prodromal
stages of schizophrenia has been advocated for more than 70 years [95].
Clinical research has shown that the longer the duration of untreated psychosis, the poorer the treatment response, which suggests that early intervention may greatly improve the outcome of the illness [94,96,97]. It is
also possible that if intervention occurs before the onset of decit symptoms
and cognitive decline, these processes can be prevented or respond to current
treatments [94,98]. The use of vulnerability markers along with clinical symptoms and genetic risk may help researchers to improve the predictive power
of identifying individuals at risk for schizophrenia for early intervention.
Most research into the symptoms that precede the rst episode of schizophrenia has been retrospective in nature, reconstructing the prodromal
changes reported by schizophrenic patients and their relatives [99101]. In
a literature review that outlined the observed stages of psychosis, Docherty
[100] described early stages in which the person becomes overwhelmed easily
and withdraws socially (overextension and restricted consciousness). The
disinhibition stage, characterized by symptoms such as ideas of reference,
may follow a transition event in which decompensation may be promoted. Psychotic disorganization is the stage in which cognitive disorganization may be prominent along with the development of hallucinatory
phenomena. The nal stage of psychotic resolution includes prominent psychotic organization with the development of an organized delusional system
and denial of illness.
Most studies have noted prodromal periods to last anywhere from a few
days to 5 years [99101]. The symptoms most often reported in the early
stages of the prodrome include reduced concentration and attention,
reduced drive and motivation, anergia, depressed mood, sleep disturbance,
anxiety, social withdrawal, suspiciousness, deterioration in role functioning,
and irritability [102]. Many prodromal symptoms are nonspecic in nature,
but it has been suggested that certain symptoms, such as disturbance of
selective attention, perceptual abnormalities, and other attenuated forms
of psychotic symptoms, have some specicity for psychosis [103105].
Davidson et al [106] reported that decits in social functioning, organizational ability, and intellectual functioning were the strongest predictors of
schizophrenia in a group of Israeli men who received draft board tests and
were later hospitalized for schizophrenia. In further analysis of the draft
board study, Weiser et al [107] report that adolescents with a schizophrenia
844
K.S. Cadenhead / Psychiatr Clin N Am 25 (2002) 837853
spectrum personality disorder have an odds ratio of 21.5 of developing
schizophrenia. Weiser et al noted that although the odds ratio for schizophrenia spectrum personality disorders is signicant, it is not strong enough
to recommend prophylactic treatment with antipsychotic medication.
Several research groups [102,108110] in the past decade have designed
programs to identify and treat individuals in the prodromal stage of schizophrenia to test the hypothesized benet of early intervention. Falloon
[109] designed a public health initiative in Buckingham, England to detect
and treat psychosis in the prodromal phase. The investigators worked
closely with all 16 family practitioners in that community of 30,000 people
and educated them in recognizing DSM-III-R prodromal symptoms of
schizophrenia between 1984 and 1988. The family practitioners referred
potential cases to a mental health team, who then evaluated the patients.
Individuals who were regarded as being in the prodromal phase were
provided with an educational seminar in which they were told that the
features they were displaying were possible signs of an impending schizophrenia and that treatment might ameliorate their current symptoms. The
treatment included crisis intervention with stress management and help
with coping strategies. Regular assessments were performed in which issues
such as chronic stress, conict, and problem solving were addressed. Neuroleptic medication was used in low doses for short periods to address target
symptoms such as sleep disturbance, agitation, muddled thinking, or preoccupation with an odd idea.
During the course of the study, the annual incidence rate of schizophrenia was 0.75 per 100,000 compared to 7.4 per 100,000 10 years earlier, which
suggested a reduction in new cases of schizophrenia. Falloons study demonstrates the potential benet of early detection and intervention. It also demonstrated that it is possible to identify potential patients in the context of a
primary health care setting. Falloons study also suggested that the hypothetical deterioration process underlying psychosis may not be as resistant
to treatment as once believed [111]. Falloon reported that the benets of
educating people about schizophrenia and other major mental disorders
were greater than the very rare deleterious eects. It was also noted in Falloons [109] report that measures of information processing may soon be
able to dierentiate those persons most vulnerable to the disorder and alleviate the concern of those considered vulnerable solely on phenomenologic
grounds.
McGorry et al [102,112] established the Early Psychosis Prevention
and Intervention Centre (EPPIC) in Melbourne, Australia. One component
of the EPPIC program is the Personal Assistance and Crisis Evaluation
(PACE) service, designed to identify and treat individuals in the prodromal
phase of schizophrenia [102]. Yung et al [102] used two dierent strategies to
identify people with at-risk mental states. The rst strategy involved identifying people who demonstrated state or symptomatic indications of an
impending psychosis. Because many features (ie, anxiety, depression, poor
K.S. Cadenhead / Psychiatr Clin N Am 25 (2002) 837853
845
role functioning) of at-risk mental states are vague and nonspecic and lead
to a high incidence of false-positive results in their preliminary studies, only
symptoms with specicity for the development of psychosis were used [102].
The state group included individuals who had attenuated forms of psychotic symptoms, including at least one of the following symptoms: ideas
of reference, odd beliefs or magical thinking, perceptual disturbance, odd
thinking and speech, paranoid ideation, odd behavior or appearance (from
DSM-IV criteria for schizotypal personality disorder). The symptoms had
to occur with a frequency of at least several times per week, and the change
in mental state had to be present for at least 1 week. Individuals who had
transient psychotic symptoms (hallucinations, delusions, thought disorder)
that resolved within 1 week were also included in the state group.
The second strategy was a modication of the genetic high-risk approach
[113] that involved combining trait-risk factors for psychotic disorders with
state-risk factors. They chose family history of any psychotic disorder or
SPD in any rst-degree relative, as a trait marker, combined with the presence of an at-risk mental state. In this group, at-risk mental states also could
include anxiety or depression as long as it was of sucient severity or duration to indicate a marked deterioration in functioning. Yung et al [102] also
included the risk factor of age by including individuals between age 16 and
30 who are at maximum risk of becoming psychotic. These strategies for
selecting subjects were used to maximize the risk of transition to psychosis
within a short time to study the process in detail. The outcome measure
in this study was the development of psychosis. Yung et al [102] noted that
selecting the exact onset point for psychosis is dicult and must be dened
arbitrarily. In their study, the presence of hallucinations, delusions, or formal thought disorder at least several times per week for longer than 1 week
was dened as psychosis onset consistent with the criteria outlined by
Larsen et al [114].
During the rst 16 months of their study, Yung et al [102] received 119
referrals. Most of their referrals came from primary care physicians, school
counselors, and youth workers and from education of the general public
about the program. Subjects were excluded from participation if they did
not speak English, had a previous psychotic episode of longer than a week
(treated or untreated), or had previous treatment with a neuroleptic for
3 weeks or longer (precluding the ability to detect transition to psychosis).
Seventy-three of the original 119 referrals were not excluded and attended
the appointment. Of those, 49 met intake criteria and 24 did not. Those
individuals who met intake criteria were followed in the PACE clinic, which
is located in a primary care setting that promotes the health of adolescents.
The site of the PACE clinic was chosen to avoid the stigmatizing eects of
being seen in a psychiatric facility. All subjects were oered clinical service
and research involvement. The clinical component included such things
as supportive therapy, relaxation training, and monitoring for impending
psychosis. Neuroleptic agents were used in one case that demonstrated a
846
K.S. Cadenhead / Psychiatr Clin N Am 25 (2002) 837853
high suicide risk, but in general the initial approach to treatment with
medication was more conservative than that described by Falloon et al [115].
Yung et al [102] were mindful of ethical issues when dealing with this
population. In the PACE clinic they did not emphasize the risk of transition
to psychosis or schizophrenia because they did not know what the risk or
transition rate was and they did not want to prematurely stigmatize or
worry the patients and their families. The need for intervention was explained in terms of the presenting problems. Of the rst 20 people recruited
into the study, 8 (40%) became psychotic within the rst 6 months. In a
recent presentation of clinical trial data, McGorry et al [116] reported that
of 60 patients who met criteria for at-risk mental states, 32 were assigned to
a treatment group who received ripseridone, 1 to 2 mg/d, antidepressants,
and anxiolytics in combination with cognitive behavioral therapy. The control group of 28 patients received basic support, antidepressants, and anxiolytic medications. 12.5% of the treatment group and 36% of the control
group converted to psychosis.
The Cologne Early Recognition Project included outpatients who were
examined with the Bonn Scale for the Assessment of Basic Symptoms to
identify individuals in the schizophrenia prodrome. This prospective study
included 110 patients with and 50 without prodromal symptoms. At follow-up, 79 patients (77 who had had prodromal symptoms and 2 who had
not) had developed schizophrenia. Although the sensitivity (0.98) and the
negative predictive (0.96) values were high, the specicity (0.59) and positive
predictive values (0.7) of prodromal symptoms were lower, and the false
positive rate was 20.6%. When specic criteria from the Bonn scale were
analyzed, thought interference, disturbances of receptive language, and visual distortions were able to predict schizophrenia with a probability up to
91%, with false-positive rates between 1.9% and 7.5%.
The studies by Falloon, McGorry, and Yung [102,109,110] and recent
programs developed by McGlashan [94], Tsuang [98], Larsen [117], and
Cornblatt [108] demonstrate the feasibility of identifying individuals in the
community at risk for psychosis. Preliminary data from the various sites
report that 30% to 40% of the at-risk population converts to psychosis within the rst few years [118]. The development of these programs provides education to primary care providers, teachers, and school counselors about the
prodromal forms of mental illness. These studies also demonstrate that it
may be possible to intervene earlier in the course of schizophrenia and prevent some of the devastating eects of the illness.
The CARE (Cognitive Assessment and Risk Evaluation) program was
established at University of California, San Diego, in 2000. The primary aim
of the CARE program is to identify and assess adolescents and young adults
between the ages of 12 and 30 who are experiencing changes in their
thoughts, behavior, or emotions that might put them at risk for developing
schizophrenia. Individuals who have low-grade psychotic symptoms or meet
criteria for schizotypal personality disorder are included, as are individuals
K.S. Cadenhead / Psychiatr Clin N Am 25 (2002) 837853
847
with a family history of schizophrenia who have had a recent deterioration
in functioning. All participants in the CARE program receive an extensive
clinical assessment and undergo a battery of psychophysiologic, neurocognitive, and information processing measures that have shown promise as
potential vulnerability markers for schizophrenia spectrum illness. The
CARE program is a longitudinal study that follows all participants on a
monthly basis over a 2- to 5-year period to assess their clinical status and
potential conversion to psychosis.
If neurobiologic markers can be identied with adequate sensitivity, specicity, and predictive validity for the later development of psychosis, these
markers could be used in conjunction with clinical assessment in determining which individuals are at risk for schizophrenia and who would benet
from early treatment. The identication of abnormalities in information
processing in the prodromal phase of schizophrenia also will increase our
understanding of neurodevelopmental processes in individuals at risk for
psychosis.
Summary
A continuum of symptoms between normality and overt psychosis has
been documented in relatives of schizophrenia patients, SPD, and individuals who may be in the early stages of a psychotic illness with subsyndromal symptoms. The empirically derived criteria for SPD have been
rened to dene a clinical phenotype that is linked to schizophrenia. The
clinical SPD symptoms dene a heterogeneous group of individuals who are
often comorbid for Axis I and II disorders, may or may not have a family
history of schizophrenia, and are at risk for developing schizophrenia themselves. SPD subjects have similar abnormalities to those observed in schizophrenia patients on various psychophysiologic paradigms designed to study
central inhibition, including P50 event-related potential suppression, PPI of
the startle response, and the antisaccade task. Because SPD subjects do not
have many of the confounding variables observed in schizophrenia patients
(ie, medication eects), these paradigms might represent vulnerability markers that are possible endophenotypes for schizophrenia spectrum illness.
Questions still remain as to whether SPD is genotypically linked to
schizophrenia but has genes of lesser penetrance, fewer aected genes, lack
of a second hit, or perhaps protective factors. It is also possible that SPD,
like schizophrenia, is a common nal pathway that can come about because of several etiologic factors that aect crucial neurodevelopmental periods. Future directions in SPD work might include the use of vulnerability
markers to essentially subtype schizophrenia spectrum patients and create
simpler endophenotypes to understand the phenomenologic and neurobiologic substrate. The use of vulnerability markers along with clinical symptoms may help to improve the predictive power for identifying individuals
848
K.S. Cadenhead / Psychiatr Clin N Am 25 (2002) 837853
at risk for schizophrenia for early intervention. Finally, genetic studies have
yet to be performed in SPD.
References
[1] Bleuler E. Dementia praecox; or, the group of schizophrenias. Monograph series on
schizophrenia; no. 1. New York: International Universities Press; 1964.
[2] Kendler KS, Gruenberg AM, Kinney DK. Independent diagnoses of adoptees and
relatives as dened by DSM-III in the Provincial and national samples of the Danish
adoption study of schizophrenia. Arch Gen Psychiatry 1994;51:45668.
[3] Kety S, Wender P, Jacobsen L, Ingraham L, Jansson L, Faber B, et al. Mental illness in
the biological and adoptive relatives of schizophrenic adoptees: replication of the
Copenhagen study in the rest of Denmark. Arch Gen Psychiatry 1994;51:44255.
[4] Kraepelin E. Dementia praecox: the clinical roots of the schizophrenia concept.
Translations of seminal European contributions on schizophrenia. Cambridge (UK):
Cambridge University Press; 1987. p. 1324.
[5] Rosano A. A study of heredity in insanity in light of the mendelian theory. American
Journal of Insanity 1911;1:21134.
[6] Deutsch H. Some forms of emotional disturbance and their relationship to schizophrenia.
Psychoanal Q 1944;11:30121.
[7] Hoch PH, Cattell JP. The diagnosis of pseudoneurotic schizophrenia. Psychiatr Q 1959;
33:1743.
[8] Knight RP. Borderline states. Bull Menninger Clin 1953;17:12.
[9] Kretschmer E. Die rolle der vererbung und der konstitution in der aetiologie der seelischen
stoerungen. Nederlandsch Tijdschrift voor Psychologie 1938;5:388400.
[10] Rado S. Dynamics and classication of disordered behavior. Am J Psychiatry 1953;110:
40626.
[11] Meehl PE. Schizotaxia, schizotypy, schizophrenia. Am Psychol 1962;17:82738.
[12] Kety SS, Rosenthal D, Wender PH, Schulsinger F. Mental illness in the biological and
adoptive families of adopted schizophrenics. Am J Psychiatry 1971;128:3026.
[13] Kendler KS, Walsh D. Schizotypal personality disorder in parents and the risk for
schizophrenia in siblings. Schizophr Bull 1995;21:4752.
[14] Grinker R, Werble B, Drue R. The borderline syndrome. New York: Basic Books, Inc;
1968.
[15] Kernberg O. Borderline personality organization. J Am Psychoanal Assoc 1967;15:64185.
[16] Spitzer RL, Endicott J, Gibbon M. Crossing the border into borderline personality
and borderline schizophrenia: the development of criteria. Arch Gen Psychiatry 1979;36:
1724.
[17] Gunderson JG, Singer MT. Dening borderline patients: an overview. Am J Psychiatry
1975;132:110.
[18] George A, Solo PM. Schizotypal symptoms in patients with borderline personality
disorders. Am J Psychiatry 1986;143:2125.
[19] Pope HG, Jonas JM, Cohen BM, Lipinski JF. Failure to nd evidence of schizophrenia in
rst-degree relatives of schizophrenic probands. Am J Psychiatry 1982;139:8268.
[20] Keefe RS, Silverman JM, Siever LJ, Cornblatt BA. Rening phenotype characterization
in genetic linkage studies of schizophrenia. Soc Biol 1991;38:197218.
[21] Siever LJ, Gunderson JG. The search for a schizotypal personality: historical origins and
current status. Compr Psychiatry 1983;24:199212.
[22] Siever LJ, Kalus OF, Keefe RS. The boundaries of schizophrenia. Psychiatr Clin North
Am 1993;16:21744.
[23] Kendler KS, Ochs AL, Gorman AM, Hewitt JK. The structure of schizotypy: a pilot
multitrait twin study. Psychiatry Res 1991;36:1936.
K.S. Cadenhead / Psychiatr Clin N Am 25 (2002) 837853
849
[24] Battaglia M, Cavallini MC, Macciardi F, Bellodi L. The structure of DSM-III-R
schizotypal personality disorder diagnosed by direct interviews. Schizophr Bull 1997;23:
8392.
[25] Battaglia M, Fossati A, Torgersen S, Bertella S, Bajo S, Maei C, et al. A psychometricgenetic study of schizotypal disorder. Schizophr Res 1999;37:5364.
[26] Bergman AJ, Silverman JM, Harvey PD, Smith CJ, Siever LJ. Schizotypal symptoms in
the relatives of schizophrenia patients: an empirical analysis of the factor structure.
Schizophr Bull 2000;26:57786.
[27] Reynolds CA, Raine A, Mellingen K, Venables PH, Mednick SA. Three-factor model of
schizotypal personality: invariance across culture, gender, religious aliation, family
adversity, and psychopathology. Schizophr Bull 2000;26:60318.
[28] Venables PH, Rector NA. The content and structure of schizotypy: a study using
conrmatory factor analysis. Schizophr Bull 2000;26:587602.
[29] Baron M, Gruen R, Asnis L, Kane JM. Familial relatedness of schizophrenia and
schizotypal states. Am J Psychiatry 1983;140:143742.
[30] Onstad S, Skre I, Edvardsen J, Torgersen S, Kringlen E. Mental disorders in rst-degree
relatives of schizophrenics. Acta Psychiatr Scand 1991;83:4637.
[31] Kendler KS, Masterson CC, Ungaro R, Davis KL. A family history study of
schizophrenia-related personality disorders. Am J Psychiatry 1984;141:4247.
[32] Baron M, Gruen R, Rainer JD, Kane J, Asnis L, Lord S. A family study of schizophrenic
and normal control probands: implications for the spectrum concept of schizophrenia.
Am J Psychiatry 1985;142:44755.
[33] Battaglia M, Bernardeschi L, Franchini L, Bellodi L. A family study of schizotypal
disorder. Schizophr Bull 1995;21:3345.
[34] Kety SS. Mental illness in the biological and adoptive relatives of schizophrenic adoptees:
ndings relevant to genetic and environmental factors in etiology. Am J Psychiatry 1983;
140:7207.
[35] Maier W, Lichtermann D, Minges J, Heun R. Personality disorders among the relatives
of schizophrenia patients. Schizophr Bull 1994;20:48193.
[36] Thaker G, Adami H, Moran M, Lahti A, Cassady S. Psychiatric illnesses in families of
subjects with schizophrenia-spectrum personality disorders: high morbidity risks for
unspecied functional psychoses and schizophrenia. Am J Psychiatry 1993;150:6671.
[37] Varma SL, Zain AM, Singh S. Psychiatric morbidity in the rst-degree relatives of
schizophrenic patients. Am J Med Genet 1997;74:711.
[38] Fenton W, McGlashan T. Risk of schizophrenia in character disordered patients. Am
J Psychiatry 1989;146:12804.
[39] Frangos E, Athanassenas G, Tsitourides S, Katsanou N, Alexandrakou P. Prevalence of
DSM III schizophrenia among the rst-degree relatives of schizophrenic probands. Acta
Psychiatr Scand 1985;72:3826.
[40] Gershon ES, DeLisi LE, Hamovit J, Nurnberger JI Jr., Maxwell ME, Schreiber J, et al.
A controlled family study of chronic psychoses: schizophrenia and schizoaective disorder. Arch Gen Psychiatry 1988;45:32836.
[41] Lowing PA, Mirsky AF, Pereira R. The inheritance of schizophrenia spectrum disorders:
a reanalysis of the Danish adoptee study data. Am J Psychiatry 1983;140:116771.
[42] Battaglia M, Bellodi L. Familial risks and reproductive tness in schizophrenia. Schizophr
Bull 1996;22:1915.
[43] Battaglia M, Gasperini M, Sciuto G, Scherillo P, Diaferia G, Bellodi L. Psychiatric disorders in the families of schizotypal subjects. Schizophr Bull 1991;17:65968.
[44] Berenbaum H, McGrew J. Familial resemblance of schizotypic traits. Psychol Med 1993;
23:32733.
[45] Ingraham LJ. Family-genetic research and schizotypal personality research. In: Raine A,
Lencz T, Mednick SA, editors. Schizotypal personality. New York: Cambridge University
Press; 1995. p. 1942.
850
K.S. Cadenhead / Psychiatr Clin N Am 25 (2002) 837853
[46] Siever LJ, Silverman JM, Horvath TB, Klar H, Coccaro E, Keefe RS, et al. Increased
morbid risk for schizophrenia-related disorders in relatives of schizotypal personality
disordered patients. Arch Gen Psychiatry 1990;47:63440.
[47] Silverman JM, Siever LJ, Horvath TB, Coccaro EF, Klar H, Davidson M, et al.
Schizophrenia-related and aective personality disorder traits in relatives of probands
with schizophrenia and personality disorders. Am J Psychiatry 1993;150:43542.
[48] Freedman R, Coon H, Myles-Worsley M, Orr-Urtreger A, Olincy A, Davis A, et al.
Linkage of a neurophysiological decit in schizophrenia to a chromosome 15 locus. Proc
Natl Acad Sci USA 1997;94:58792.
[49] Hyman SE. The NIMH perspective: next steps in schizophrenia research. Biol Psychiatry
2000;47:17.
[50] Siever LJ. Brain structure/function and the dopamine system in schizotypal personality
disorder. In: Raine A, Lencz T, Mednick SA, editors. Schizotypal personality. New York:
Cambridge University Press; 1995. p. 27286.
[51] Venables P. Input dysfunction in schizophrenia. In: Maher B, editor. Progress in experimental personality research. New York: Academic Press; 1964. p. 141.
[52] Bra DL. Psychophysiological and information processing approaches to schizophrenia.
In: Charney DS, Nestler E, Bunney BS, editors. Neurobiological foundation of mental
illness. New York: Oxford University Press; 1999. p. 25871.
[53] Tsuang MT. Recent advances in genetic research on schizophrenia. J Biomed Sci 1998;5:
2830.
[54] Bra DL. Information processing and attention dysfunctions in schizophrenia. Schizophr
Bull 1993;19:23359.
[55] Bra DL, Grillon C, Geyer MA. Gating and habituation of the startle reex in
schizophrenic patients. Arch Gen Psychiatry 1992;49:20615.
[56] Cadenhead K, Geyer M, Bra D. Impaired startle prepulse inhibition and habituation
in schizotypal personality disordered patients. Am J Psychiatry 1993;150:18627.
[57] Cadenhead KS, Swerdlow NR, Shafer K, Diaz M, Bra DL. Modulation of the startle
response and startle laterality in relatives of schizophrenia patients and schizotypal personality disordered subjects: evidence of inhibitory decits. Am J Psychiatry 2000;157:
16608.
[58] Cadenhead K, Light G, Geyer M, Bra D. P50 event-related-potential sensory
gating decits in schizotypal personality disordered subjects. Am J Psychiatry 2000;
157:559.
[59] Clementz B, Geyer M, Bra D. Poor P50 suppression among schizophrenia patients
and their rst-degree biological relatives. Am J Psychiatry 1998;155:16914.
[60] Waldo MC, Carey G, Myles-Worsley M, Cawthra E, Adler LE, Nagamoto HT, et al.
Codistribution of a sensory gating decit and schizophrenia in multi-aected families.
Psychiatry Res 1991;39:25768.
[61] Brenner CA, McDowell JE, Cadenhead KS, Clementz BA. Saccadic inhibition among
schizotypal personality disorder and schizophrenia subjects. Psychophysiology 2001;38:
399403.
[62] Katsanis J, Kortenkamp S, Iacono WG, Grove WM. Antisaccade performance in patients
with schizophrenia and aective disorder. J Abnorm Psychol 1997;106:46872.
[63] Ross RG, Harris JG, Olincy A, Radant A, Adler LE, Freedman R. Familial transmission
of two independent saccadic abnormalities in schizophrenia. Schizophr Res 1998;30:
5970.
[64] Kumari V, Soni W, Mathew VM, Sharma T. Prepulse inhibition of the startle response
in men with schizophrenia: eects of age of onset of illness, symptoms, and medication.
Arch Gen Psychiatry 2000;57:60914.
[65] Cadenhead KS, Carasso B, Swerdlow NR, Geyer MA, Bra DL. Prepulse inhibition and
habituation of the startle response are stable neurobiological measures in a normal male
population. Biol Psychiatry 1999;45:3604.
K.S. Cadenhead / Psychiatr Clin N Am 25 (2002) 837853
851
[66] Grillon C, Ameli R, Charney DS, Krystal J, Bra D. Startle gating decits occur across
prepulse intensities in schizophrenic patients. Biol Psychiatry 1992;32:93943.
[67] Kumari V, Soni W, Sharma T. Normalization of information processing decits in
schizophrenia with clozapine. Am J Psychiatry 1999;156:104651.
[68] Nuechterlein KH, Dawson ME. Information processing and attentional functioning in
the developmental course of schizophrenic disorders. Schizophr Bull 1984;10:160203.
[69] Weike AI, Bauer U, Hamm AO. Eective neuroleptic medication removes prepulse
inhibition decits in schizophrenia patients. Biol Psychiatry 2000;47:6170.
[70] Cadenhead K, Bra DL. Enophenotyping schizotypy: a prelude to genetic studies within
the schizophrenia spectrum. Schizophr Res 2002;54:4757.
[71] Swerdlow NR, Bra DL, Taaid N, Geyer MA. Assessing the validity of an animal model
of decient sensorimotor gating in schizophrenic patients. Arch Gen Psychiatry 1994;51:
13954.
[72] Carlson SR, Katsanis J, Iacono WG, McGue M. Emotional modulation of the startle
reex in twins: preliminary ndings. Biol Psychol 1997;46:23546.
[73] Bullock AE, Slobe BS, Vazquez V, Collins AC. Inbred mouse strains dier in the regulation
of startle and prepulse inhibition of the startle response. Behav Neurosci 1997;111:
135360.
[74] Paylor R, Crawley JN. Inbred strain dierences in prepulse inhibition of the mouse startle
response. Psychopharmacology (Berl) 1997;132:16980.
[75] Joober R, Zarate JM, Rouleau GA, Skamene E, Boksa P. Quantitative trait loci modulating the acoustic startle response and prepulse inhibition of acoustic startle. Society for
Neuroscience Proceedings 2001 (abstract).
[76] Adler LE, Pachtman E, Franks RD, Pecevich M, Waldo MC, Freedman R. Neurophysiological evidence for a defect in neuronal mechanisms involved in sensory gating in
schizophrenia. Biol Psychiatry 1982;17:63954.
[77] Freedman R, Adler LE, Waldo M. Gating of the auditory evoked potential in children
and adults. Psychophysiology 1987;24:2237.
[78] Myles-Worsley M, Coon H, Byerley W, Waldo M. Developmental and genetic inuences
on the P50 sensory gating phenotype. Biol Psychiatry 1996;39:28995.
[79] Boutros NN, Overall J, Zouridakis G. Test-retest reliability of the P50 mid-latency
auditory evoked response. Psychiatry Res 1991;39:18192.
[80] Waldo MC, Graze K, de Gra Bender S, Adler LE, Freedman R. Premenstrual mood
changes and gating of the auditory evoked potential. Psychoneuroendocrinology 1987;12:
3540.
[81] Clementz BA, Geyer MA, Bra DL. P50 suppression among schizophrenia and normal
comparison subjects: a methodological analysis. Biol Psychiatry 1997;41:103544.
[82] Freedman R, Adler LE, Waldo MC, Pachtman E, Franks RD. Neurophysiological evidence for a defect in inhibitory pathways in schizophrenia: comparison of medicated and
drug-free patients. Biol Psychiatry 1983;18:53751.
[83] Judd LL, McAdams L, Budnick B, Bra DL. Sensory gating decits in schizophrenia:
new results. Am J Psychiatry 1992;149:48893.
[84] Siegel C, Waldo M, Mizner G, Adler LE, Freedman R. Decits in sensory gating in
schizophrenic patients and their relatives: evidence obtained with auditory evoked
responses. Arch Gen Psychiatry 1984;41:60712.
[85] Young D, Waldo M, Rutledge J, Freedman R. Heritability of inhibitory gating of the P50
auditory-evoked potential in monozygotic and dizygotic twins. Neuropsychobiology 1996;
33:1137.
[86] Light GA, Geyer MA, Clementz BA, Cadenhead KS, Bra DL. Normal P50 suppression
in schizophrenia patients treated with atypical antipsychotic medications. Am J Psychiatry
2000;157:76771.
[87] Nagamoto HT, Adler LE, Hea RA, Grith JM, McRae KA, Freedman R. Gating of
auditory P50 in schizophrenics: unique eects of clozapine. Biol Psychiatry 1996;40:1818.
852
K.S. Cadenhead / Psychiatr Clin N Am 25 (2002) 837853
[88] Nagamoto HT, Adler LE, McRae KA, Huettl P, Cawthra E, Gerhardt G, et al. Auditory
P50 in schizophrenics on clozapine: improved gating parallels clinical improvement
and changes in plasma 3-methoxy-4- hydroxyphenylglycol. Neuropsychobiology 1999;39:
107.
[89] Yee CM, Nuechterlein KH, Morris SE, White PM. P50 suppression in recent-onset
schizophrenia: clinical correlates and risperidone eects. J Abnorm Psychol 1998;107:
6918.
[90] Fukushima J, Morita N, Fukushima K, Chiba T, Tanaka S, Yamashita I. Voluntary
control of saccadic eye movements in patients with schizophrenic and aective disorders.
J Psychiatr Res 1990;24:924.
[91] McDowell JE, Myles-Worsley M, Coon H, Byerley W, Clementz BA. Measuring liability
for schizophrenia using optimized antisaccade stimulus parameters. Psychophysiology
1999;36:13841.
[92] Cadenhead K, Light G, Geyer M, McDowell J, Bra D. Neurobiological measures in
schizotypal personality disorder: beginning to dene a phenotype? Am J Psychiatry
2002;159:86971.
[93] Myles-Worsley M, Coon H, McDowell J, Brenner C, Ho M, Lind B, et al. Linkage
of a composite inhibitory phenotype to a chromosome 22q locus in eight Utah families.
Am J Med Genet 1999;88:54450.
[94] McGlashan TH. Early detection and intervention of schizophrenia: rationale and
research. Br J Psychiatry 1998;172(Suppl):36.
[95] Sullivan HS. The onset of schizophrenia. Am J Psychiatry 1994;151:1359.
[96] Lieberman JA, Alvir JM, Woerner M, Degreef G, Bilder RM, Ashtari M, et al.
Prospective study of psychobiology in rst-episode schizophrenia at Hillside Hospital.
Schizophr Bull 1992;18:35171.
[97] Vaglum P. Earlier detection and intervention in schizophrenia: unsolved questions.
Schizophr Bull 1996;22:34751.
[98] Tsuang MT, Stone WS, Seidman LJ, Faraone SV, Zimmet S, Wojcik J, et al. Treatment
of nonpsychotic relatives of patients with schizophrenia: four case studies. Biol Psychiatry
1999;45:14128.
[99] Beiser M, Erickson D, Fleming JA, Iacono WG. Establishing the onset of psychotic
illness. Am J Psychiatry 1993;150:134954.
[100] Docherty JP, Van Kammen DP, Siris SG, Marder SR. Stages of onset of schizophrenic
psychosis. Am J Psychiatry 1978;135:4206.
[101] Hafner H. Onset and course of the rst schizophrenic episode. Kao Hsiung I Hsueh Ko
Hsueh Tsa Chih 1998;14:41331.
[102] Yung AR, Phillips LJ, McGorry PD, McFarlane CA, Francey S, Harrigan S, et al.
Prediction of psychosis: a step towards indicated prevention of schizophrenia. Br J
Psychiatry 1998;172(Suppl):1420.
[103] Bowers MB Jr, Freedman DX. Psychedelic experiences in acute psychoses. Arch Gen
Psychiatry 1966;15:2408.
[104] Chapman J. The early symptoms of schizophrenia. Br J Psychiatry 1966;112:22551.
[105] Klosterkotter J, Hellmich M, Steinmeyer EM, Schultze-Lutter F. Diagnosing schizophrenia in the initial prodromal phase. Arch Gen Psychiatry 2001;58:15864.
[106] Davidson M, Reichenberg A, Rabinowitz J, Weiser M, Kaplan Z, Mordehai M.
Behavioral and intellectual markers for schizophrenia in apparently healthy male adolescents. Am J Psychiatry 1999;156:132835.
[107] Weiser M, Reichenberg A, Rabinowitz J, Kaplan Z, Mark M, Bodner E, et al. Association
between nonpsychotic psychiatric diagnoses in adolescent males and subsequent onset of
schizophrenia. Arch Gen Psychiatry 2001;58:95964.
[108] Cornblatt B, Obuchowski RS, Goldman RS, Bergman A, Smith C, Baruch-Feldman C,
et al. This Hillside RAPP Clinic: intervention during the schizophrenia prodrome. Biol
Psychiatry 1998;43:84S.
K.S. Cadenhead / Psychiatr Clin N Am 25 (2002) 837853
853
[109] Falloon IR, Coverdale JH, Laidlaw TM, Merry S, Kydd RR, Morosini P. Early
intervention for schizophrenic disorders: implementing optimal treatment strategies in
routine clinical services. OTP Collaborative Group. Br J Psychiatry 1998;172(Suppl):338.
[110] McGorry P. Preventive strategies in early psychosis: Verging on reality. [editorial]. Br J
Psychiatry 1998;172(Suppl):12.
[111] McGlashan TH. Early detection and intervention in schizophrenia: editors introduction.
Schizophr Bull 1996;22:1979.
[112] McGorry PD, Edwards J, Mihalopoulos C, Harrigan SM, Jackson HJ. EPPIC: an evolving
system of early detection and optimal management. Schizophr Bull 1996;22:30526.
[113] Cornblatt B, Obuchowski M. Update of high-risk research: 19871997. Int Rev Psychiatry
1997;9:43747.
[114] Larsen TK, McGlashan TH, Moe LC. First-episode schizophrenia: I. Early course
parameters. Schizophr Bull 1996;22:24156.
[115] Falloon IR. Early intervention for rst episodes of schizophrenia: a preliminary exploration. Psychiatry 1992;55:415.
[116] McGorry P, Phillips L, Yung A, Francey S, Velakoulis D, Brewer W, et al. The
identication of predictors of psychosis in a high risk group. Schizophr Res 1999;36:
4950.
[117] Larsen T, Joa I. Identifying persons prodromal to rst episode schizophrenia: the TOPPOrihect. Curr Opin Psychiatry 1999;12:207.
[118] Larsen TK, Friis S, Haahr U, Joa I, Johannessen JO, Melle I, et al. Early detection and
intervention in rst-episode schizophrenia: a critical review. Acta Psychiatr Scand 2001;
103:32334.
You might also like
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeFrom EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeRating: 4 out of 5 stars4/5 (5795)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreFrom EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreRating: 4 out of 5 stars4/5 (1091)
- Never Split the Difference: Negotiating As If Your Life Depended On ItFrom EverandNever Split the Difference: Negotiating As If Your Life Depended On ItRating: 4.5 out of 5 stars4.5/5 (838)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceFrom EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceRating: 4 out of 5 stars4/5 (895)
- Grit: The Power of Passion and PerseveranceFrom EverandGrit: The Power of Passion and PerseveranceRating: 4 out of 5 stars4/5 (588)
- Shoe Dog: A Memoir by the Creator of NikeFrom EverandShoe Dog: A Memoir by the Creator of NikeRating: 4.5 out of 5 stars4.5/5 (537)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersFrom EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersRating: 4.5 out of 5 stars4.5/5 (345)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureFrom EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureRating: 4.5 out of 5 stars4.5/5 (474)
- Her Body and Other Parties: StoriesFrom EverandHer Body and Other Parties: StoriesRating: 4 out of 5 stars4/5 (821)
- The Emperor of All Maladies: A Biography of CancerFrom EverandThe Emperor of All Maladies: A Biography of CancerRating: 4.5 out of 5 stars4.5/5 (271)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)From EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Rating: 4.5 out of 5 stars4.5/5 (121)
- The Little Book of Hygge: Danish Secrets to Happy LivingFrom EverandThe Little Book of Hygge: Danish Secrets to Happy LivingRating: 3.5 out of 5 stars3.5/5 (400)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyFrom EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyRating: 3.5 out of 5 stars3.5/5 (2259)
- The Yellow House: A Memoir (2019 National Book Award Winner)From EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Rating: 4 out of 5 stars4/5 (98)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaFrom EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaRating: 4.5 out of 5 stars4.5/5 (266)
- Pediatric Drug Dosage - All in One PDFDocument15 pagesPediatric Drug Dosage - All in One PDFHuang Hasjim33% (9)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryFrom EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryRating: 3.5 out of 5 stars3.5/5 (231)
- Team of Rivals: The Political Genius of Abraham LincolnFrom EverandTeam of Rivals: The Political Genius of Abraham LincolnRating: 4.5 out of 5 stars4.5/5 (234)
- On Fire: The (Burning) Case for a Green New DealFrom EverandOn Fire: The (Burning) Case for a Green New DealRating: 4 out of 5 stars4/5 (74)
- The Unwinding: An Inner History of the New AmericaFrom EverandThe Unwinding: An Inner History of the New AmericaRating: 4 out of 5 stars4/5 (45)
- Neuroimaging Clinics of North America 2015 #2 PDFDocument173 pagesNeuroimaging Clinics of North America 2015 #2 PDFYully gunawan100% (1)
- DIALOGUEDocument6 pagesDIALOGUEAlexis Angel DiMaria Muñoz QNo ratings yet
- Poultry Diseases and Their TreatmentDocument159 pagesPoultry Diseases and Their TreatmentAbubakar Tahir Ramay67% (12)
- Histeria Por Vacunación Mass Psychogenic Illness After Vaccination 2003Document6 pagesHisteria Por Vacunación Mass Psychogenic Illness After Vaccination 2003Oscar Alejandro Cardenas QuinteroNo ratings yet
- Depresion en El Anciano en APS NejmDocument3 pagesDepresion en El Anciano en APS NejmOscar Alejandro Cardenas QuinteroNo ratings yet
- Depresion PostpartoDocument6 pagesDepresion PostpartoOscar Alejandro Cardenas QuinteroNo ratings yet
- Depresion y Ejercicio NejmDocument2 pagesDepresion y Ejercicio NejmOscar Alejandro Cardenas QuinteroNo ratings yet
- Depression As An Evolutionary Strategy For Defense Against InfectionDocument14 pagesDepression As An Evolutionary Strategy For Defense Against InfectionOscar Alejandro Cardenas Quintero100% (2)
- A Case of Nonconvulsive Status Epilepticus Presenting As Dissociative FugueDocument2 pagesA Case of Nonconvulsive Status Epilepticus Presenting As Dissociative FugueOscar Alejandro Cardenas QuinteroNo ratings yet
- Cjp-June-05 - GEDocument2 pagesCjp-June-05 - GEOscar Alejandro Cardenas QuinteroNo ratings yet
- Differential Typology of Delusions in Major Depression and Schizophrenia. A Critique To The Unitary Concept of PsychosisDocument8 pagesDifferential Typology of Delusions in Major Depression and Schizophrenia. A Critique To The Unitary Concept of PsychosisOscar Alejandro Cardenas QuinteroNo ratings yet
- Diagnosis and Clinical Features of Major Neuropsychiatric Disorders in HIV InfectionDocument9 pagesDiagnosis and Clinical Features of Major Neuropsychiatric Disorders in HIV InfectionOscar Alejandro Cardenas QuinteroNo ratings yet
- V71I12 - A Breakthrough in Schizophrenia GeneticsDocument2 pagesV71I12 - A Breakthrough in Schizophrenia GeneticsOscar Alejandro Cardenas QuinteroNo ratings yet
- Kapur (2003) Psychosis As A State of Aberrant SalienceDocument11 pagesKapur (2003) Psychosis As A State of Aberrant SalienceOscar Alejandro Cardenas QuinteroNo ratings yet
- Kapur (2003) Psychosis As A State of Aberrant SalienceDocument11 pagesKapur (2003) Psychosis As A State of Aberrant SalienceOscar Alejandro Cardenas QuinteroNo ratings yet
- RESUMEDocument3 pagesRESUME9460No ratings yet
- Professional PhilosophyDocument8 pagesProfessional Philosophyapi-450228862No ratings yet
- Analisis Pelaksanaan Retensi Dan Penyimpanan Dokumen Rekam Medis Inaktif Filing Rawat Jalan Di Rumah Sakit Bhayangkara Semarang Tahun 2016Document11 pagesAnalisis Pelaksanaan Retensi Dan Penyimpanan Dokumen Rekam Medis Inaktif Filing Rawat Jalan Di Rumah Sakit Bhayangkara Semarang Tahun 2016Haris ArisNo ratings yet
- REV Patrick Samuel Zulu RESEARCH 2024Document51 pagesREV Patrick Samuel Zulu RESEARCH 2024xbw5vjrxdpNo ratings yet
- Bipolar 1 DisorderDocument11 pagesBipolar 1 DisorderGirlly AlcantaraNo ratings yet
- Understanding PhlebotomyDocument4 pagesUnderstanding PhlebotomyAngelo Jude CumpioNo ratings yet
- DEEP VEIN Dr. Samira BelkheirDocument43 pagesDEEP VEIN Dr. Samira BelkheirkalfNo ratings yet
- As Fluid Volume Deficit (FVD), Hypovolemia) Is ADocument2 pagesAs Fluid Volume Deficit (FVD), Hypovolemia) Is ATanya Alyssa Untalan AquinoNo ratings yet
- Diabetes MellitusDocument8 pagesDiabetes MellitusJaja RamosNo ratings yet
- Documenting Pharmaceutical Care Patient Medical Records PDFDocument3 pagesDocumenting Pharmaceutical Care Patient Medical Records PDFPuspa NurrochmawatiNo ratings yet
- ProjectDocument3 pagesProjectAnshul PaunikarNo ratings yet
- COVID Testing Labs 26042021Document167 pagesCOVID Testing Labs 26042021suresh10526_71653021No ratings yet
- Chapter 10 Syringes and NeedlesDocument15 pagesChapter 10 Syringes and NeedlesTiffany FlorentNo ratings yet
- Standard Claim Form HospitalDocument2 pagesStandard Claim Form Hospitalnpatel35No ratings yet
- Cancer Goes Viral: HPV-positive Throat and Tongue Cancers Are Taking Off in MenDocument2 pagesCancer Goes Viral: HPV-positive Throat and Tongue Cancers Are Taking Off in MenMEGA_ONENo ratings yet
- Cebu Declaration List of ParticipantsDocument6 pagesCebu Declaration List of ParticipantspuspaNo ratings yet
- Introduction To BioethicsDocument33 pagesIntroduction To BioethicsReymart BolagaoNo ratings yet
- Novilyn C. Pataray BSN - Ii Otitis Media: St. Paul College of Ilocos SurDocument1 pageNovilyn C. Pataray BSN - Ii Otitis Media: St. Paul College of Ilocos SurCharina AubreyNo ratings yet
- Actaapa 2018 21Document5 pagesActaapa 2018 21Argitya RighoNo ratings yet
- Prediction of Pulmonary Embolism in The Emergency DepartmentDocument10 pagesPrediction of Pulmonary Embolism in The Emergency DepartmenttechiemedicNo ratings yet
- Workplace Health Longterm Sickness Absence and Capability To Work PDFDocument38 pagesWorkplace Health Longterm Sickness Absence and Capability To Work PDFFuzail AyazNo ratings yet
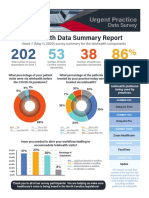
- UPDS Telehealth Data ReportDocument3 pagesUPDS Telehealth Data ReportCorey LarkinsNo ratings yet
- PDF Book UrduDocument4 pagesPDF Book UrduMuhammad KamranNo ratings yet
- Cerumen Impaction FinalDocument8 pagesCerumen Impaction FinalRose Ann Del MundoNo ratings yet
- CV - Dr. Adeel TahirDocument3 pagesCV - Dr. Adeel TahirAdeel TahirNo ratings yet
- Verminous Arteritis HandoutDocument1 pageVerminous Arteritis HandoutmarceeseamansNo ratings yet