Professional Documents
Culture Documents
Inhalation Injury
Uploaded by
Alya Putri Khairani0 ratings0% found this document useful (0 votes)
22 views2 pagesbb
Copyright
© © All Rights Reserved
Available Formats
DOCX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this Documentbb
Copyright:
© All Rights Reserved
Available Formats
Download as DOCX, PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
22 views2 pagesInhalation Injury
Uploaded by
Alya Putri Khairanibb
Copyright:
© All Rights Reserved
Available Formats
Download as DOCX, PDF, TXT or read online from Scribd
You are on page 1of 2
Inhalation Injury
Dependent on the chemical properties, the
concentration of the chemical, and the duration of
contact with skin or mucous membranes. Care for
children with chemical injuries includes obtaining a
thorough history of the accident with the type and
duration of contact and rinsing the affected area with
copious amounts of water until a bum center consult
can be obtained, as well as frequent assessment of
the affected area. Inhalation injury, often called
smoke inhalation, is a condition associated with
exposure to the heat and toxic fumes produced by
fire conditions in a closed space. Complete and
incomplete combustion of materials commonly found
in the everyday environment produces extreme heat,
toxic fumes, and a reduction in the environmental
oxygen concentration, often reducing it to 16% or
less. The identification of a person who has sustained
an inhalation injury is often difficult. Clinically, a
person who is at risk has the following
characteristics:
Burned in a closed space or standing upright
as theirclothing burned
Burns of the face or neck
Singed eyebrows, nasal hairs, and hairline or
facial hair
Carbon particles in the mouth or nose or
carbonaceous sputum
Brassy cough, hoarseness, or stridor
Significant serum carboxyhemoglobin level
(greater than 15%)9
These children warrant close observation and
immediate intervention if respiratory distress
develops. Early or prophylactic intervention,
particularly in young children, is essential for
survival. The inhalation injury produced by fire
conditions has four components. First, thermal injury
occurs in the upper airways because of exposure to
high environmental temperatures and superheated
gases. Direct heat damage is usually limited to the
upper airway because the moist mucous membranes
act as a heat exchanger, lowering the temperature of
the inhaled gases before they cross the vocal cords.
In fire conditions, the upper airway extracts excess
heat from inhaled gases. This protects the lower
airway (below the vocal cords) from thermal damage.
The sole exception to this is the inhalation of steam.
Steam has a heat-carrying capacity that is
approximately 400 times the capacity of ambient air.
This allows the steam to pass through the vocal cords
with little heat loss in the upper airway, thus creating
thermal burns below the vocal cords. The exposure to
hot gases produces diffuse edema throughout the
upper airway, resulting in airway obstruction. The
edema rapidly advances and peaks at about 6 to 12
hours after injury. Extensive burns of the head and
neck or hot liquid aspiration can produce such
massive edema in local tissues that the airway is
compromised. Although not a true inhalation injury,
these injuries may present with similar clinical signs
and symptoms. Suspicion of aspiration or extensive
head or neck bums is treated by protecting the
airway with an endotracheal tube (ETT) until the
edema resolves. Because of the small comparative
size of children's airways, intervention in the form of
endotracheal intubation is often required. Another
aspect of inhalation injury occurs when carbon
monoxide (CO) combines with the hemoglobin
molecule to reduce the oxygen-carrying capacity of
red blood cells. CO is a clear, colorless, odorless gas
produced by the incomplete combustion of organic
materials, such as wood, paper, cotton, gasoline, and
others. Incomplete combustion occurs because
insufficient oxygen is available in fire conditions.
Depending on the carboxyhemoglobin levels, the
child may experience symptoms ranging from mild
intellectual dysfunction to apnea and cardiac arrest
(Table 29-2). The binding of CO to hemoglobin can be
reversed by the administration of 100% oxygen.
Experiments attempting to quantify the elimination
half-life of CO by nonrebreathing face mask or by ETT
intubation demonstrate a range of 26 to 146
minutes. Hyperbaric oxygen (HEO) therapy may also
be indicated for the child with CO poisoning, although
its use remains controversial. A child undergoing HBO
treatment is put into a hyperbaric chamber and is
exposed to 100% oxygen at a pressure higher than
atmospheric pressure. This method has shown to aid
in displacing CO from the hemoglobin molecule, thus
providing increased amounts of available oxygen and
reversing the toxic effects of CO. Another sequela of
inhalation injury is hypoxia caused by exposure to
fire conditions wherein environmental oxygen is
rapidly consumed by combustion. This results in
environmental oxygen concentrations that reduce the
FT02 , so Pa02 levels of 50 to 60 mmHg are
commonplace. Combined with CO exposure, the
reduced FI02 worsens the tissue hypoxia and its
consequences. The inhalation of toxic gases from the
fire may produce a chemical pneumonitis. The
combustion of commonly found materials liberates
toxic gases, which can include hydrogen sulfide,
hydrogen cyanide, hydrogen chloride, acrolein,
mustard gas, nerve gas, and many others. When
these gases come in contact with the epithelium
lining the tracheobronchial tree, they form corrosi ve
acids that destroy the cilia and underlying tissue.
Toxic materials also adhere to soot particles that are
inhaled, providing an additional source of toxic
exposure and debris that must be cleared. Toxins are
absorbed into the general circulation, where they can
have systemic effects (e.g., production of hydrogen
cyanide, which causes immediate respiratory
dysfunction). The initial response of the lung is
bronchorrhea followed by a sloughing of necrotic
tissues. The increased debris formation plus the loss
of the cilia results in atelectasis. The clinical
symptoms may present hours to 7 days later. There
are three time periods following injury when the
damage caused by these toxic agents occur.
Immediately after the exposure to fire conditions,
hypoxia associated with decreased environmental
oxygen concentrations, CO poisoning, and airway
edema from exposure to hot gases
develops. During the 24 to 48 hours following injury,
pulmonary edema is associated with the toxicity of
inhaled gases and fluid resuscitation. After 48 hours,
the effects of atelectasis and pneumonia become
evident as a clinical picture similar to acute
respiratory distress syndrome (ARDS) develops. The
presence of skin involvement further complicates the
management of inhalation injury. Skin damage that
involves more than 25% TBSA results in diffuse
capillary leak throughout the body, including the
lung. The increase in interstitial water surrounding
the alveoli reduces effective gas exchange and
increases the patient's volume requirements.
Inhalation injury can increase the body's fluid
requirement up to 37% over calculated fluid
resuscitation needs. The assessment of fluid balance
becomes increasingly complicated, and pulmonary
edema is a common complication. The treatment of
pulmonary edema is usually reduction of the infused
fluid volume in increments until symptoms disappear.
Full-thickness, circumferential surface burns of the
neck and chest wall can compromise pulmonary
function even further. When inelastic eschar
surrounds the chest, a corsetlike effect is created.
Edema continues to occur in the burn wound,
compressing the tissues of the chest wall inward and
compromising the vital capacity. Relief is provided by
escharotomies (incisions through the eschar) that
allow the chest wall to expand. Escharotomies to
relieve chest compression are usually performed
within the first 24 hours after injury, but extensions
of the escharotomies may need to be done as the
edema continues through the emergent phase.
Surviving the initial inhalation injury is not the end of
the child's pulmonary problems. The child may
develop ARDS following hypoxic or hypovolemic
insult or as a component of septic shock associated
with bacteremia from wound debridement,
intravascular lines, urinary tract infections, or
pneumonia. The long-term sequelae of inhalation
injury include bronchiolitis obliterans, cylindrical
bronchiectasia, and tracheal stenosis associated with
prolonged intubation or tracheostomy. Children
whose respiratory units are destroyed at a young age
have a better prognosis for long-term respiratory
function than do school-age children or adolescents.
As the young child grows after the injury, the
remaining respiratory units can increase in surface
area more than would normally be expected to
compensate for the units that were destroyed
Circumferential Burns
Full-thickness circumferential burns of the torso or
extremity
present a special problem for the child. As mentioned
earlier, circumferential burns to the torso may
impede a
child's ability to ventilate. Similarly, circumferential
areas
of full-thickness bums to extremities are nonelastic
and
produce a tourniquet effect that diminishes blood
flow to the
affected area. As edema occurs in the affected area
and the
tissue cannot stretch, the child experiences
numbness and
tingling distal to the injured area, loss of motor
function and
sensation, and severe pain. Release of pressure must
occur
and requires surgical intervention by escharotomy or
fasciotomy. An escharotomy involves an incision
through the burned tissue down to the subcutaneous
fat
layers to restore blood supply. A fasciotomy is
necessary
when the escharotomy has not restored adequate
perfusion
and the injury has extended into the muscle. This
procedure
involves a deeper incision through the fascia
covering the
muscle compartments and allows the expansion of
compressed
or edematous areas of muscle.
The best time to perform an escharotomy varies and
is
based on frequent assessment of the affected area,
distal
circulation, sensory motor function, and pulses, as
well as
respiratory effort and peak inspiratory pressures with
torso
bums. If an escharotomy is performed, blood loss
may be a
problem as circulation is restored and is monitored. If
the
escharotomy is performed too late, necrosis of the
entire
extremity distal to the injury site, compartment
syndrome,
and gangrene can develop.
You might also like
- Uric Acid and Its MetabolismDocument3 pagesUric Acid and Its MetabolismAlya Putri KhairaniNo ratings yet
- Inhalation InjuryDocument2 pagesInhalation InjuryAlya Putri KhairaniNo ratings yet
- Chapter 3 A Neuro Disorders Public H ChallengesDocument71 pagesChapter 3 A Neuro Disorders Public H ChallengesAnna Francesca AbarquezNo ratings yet
- Leptospira SP.: Leptospira Are Spiral Bacteria (Spirochaete) in The Family of LeptospiraceaeDocument3 pagesLeptospira SP.: Leptospira Are Spiral Bacteria (Spirochaete) in The Family of LeptospiraceaeAlya Putri KhairaniNo ratings yet
- Colorectal CacinomaDocument2 pagesColorectal CacinomaAlya Putri KhairaniNo ratings yet
- Iccu / Cicu: Patients Heart Attacks Unstable Angina Cardiac DysrhythmiaDocument4 pagesIccu / Cicu: Patients Heart Attacks Unstable Angina Cardiac DysrhythmiaAlya Putri KhairaniNo ratings yet
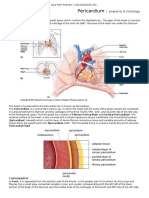
- Pericardium:: AnatomyDocument4 pagesPericardium:: AnatomyAlya Putri KhairaniNo ratings yet
- Normal X RayDocument6 pagesNormal X RayAlya Putri KhairaniNo ratings yet
- Community Nutrition & Physician's ResponsibilityDocument16 pagesCommunity Nutrition & Physician's ResponsibilityAlya Putri KhairaniNo ratings yet
- Bleeding: Blood VesselDocument2 pagesBleeding: Blood VesselAlya Putri KhairaniNo ratings yet
- Hypersensitivity Type IDocument3 pagesHypersensitivity Type IAlya Putri KhairaniNo ratings yet
- Inhalation InjuryDocument2 pagesInhalation InjuryAlya Putri KhairaniNo ratings yet
- Colorectal CacinomaDocument2 pagesColorectal CacinomaAlya Putri KhairaniNo ratings yet
- Renal Regulation of PotassiumDocument5 pagesRenal Regulation of PotassiumAlya Putri KhairaniNo ratings yet
- Function of SinusesDocument1 pageFunction of SinusesAlya Putri KhairaniNo ratings yet
- Congenital Syphilis Causes and TreatmentDocument4 pagesCongenital Syphilis Causes and TreatmentAlya Putri Khairani100% (1)
- Kinesiology of Shoulder Complex MusclesDocument7 pagesKinesiology of Shoulder Complex MusclesAlya Putri KhairaniNo ratings yet
- Histogenesis and Cell Types in Bone FormationDocument6 pagesHistogenesis and Cell Types in Bone FormationAlya Putri KhairaniNo ratings yet
- Clobetasol Propionate and Urea CreamDocument4 pagesClobetasol Propionate and Urea CreamAlya Putri KhairaniNo ratings yet
- Anatomy of Oral RegionDocument6 pagesAnatomy of Oral RegionAlya Putri KhairaniNo ratings yet
- Hemolytic Anemia: MorphologyDocument10 pagesHemolytic Anemia: MorphologyAlya Putri KhairaniNo ratings yet
- How Tetanus or Dental Caries Can Cause Cardiovascular DiseaseDocument3 pagesHow Tetanus or Dental Caries Can Cause Cardiovascular DiseaseAlya Putri KhairaniNo ratings yet
- Diagnosing and Managing Systemic Lupus ErythematosusDocument3 pagesDiagnosing and Managing Systemic Lupus ErythematosusAlya Putri KhairaniNo ratings yet
- Influenza: Laboratory FindingsDocument6 pagesInfluenza: Laboratory FindingsAlya Putri KhairaniNo ratings yet
- Staging of HerniaDocument1 pageStaging of HerniaAlya Putri KhairaniNo ratings yet
- Leptospira SP.: Leptospira Are Spiral Bacteria (Spirochaete) in The Family of LeptospiraceaeDocument3 pagesLeptospira SP.: Leptospira Are Spiral Bacteria (Spirochaete) in The Family of LeptospiraceaeAlya Putri KhairaniNo ratings yet
- Failure To ThriveDocument3 pagesFailure To ThriveAlya Putri KhairaniNo ratings yet
- Herpes VirusesDocument6 pagesHerpes VirusesAlya Putri KhairaniNo ratings yet
- Conversion DisorderDocument2 pagesConversion DisorderAlya Putri KhairaniNo ratings yet
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeFrom EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeRating: 4 out of 5 stars4/5 (5784)
- The Yellow House: A Memoir (2019 National Book Award Winner)From EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Rating: 4 out of 5 stars4/5 (98)
- Never Split the Difference: Negotiating As If Your Life Depended On ItFrom EverandNever Split the Difference: Negotiating As If Your Life Depended On ItRating: 4.5 out of 5 stars4.5/5 (838)
- Shoe Dog: A Memoir by the Creator of NikeFrom EverandShoe Dog: A Memoir by the Creator of NikeRating: 4.5 out of 5 stars4.5/5 (537)
- The Emperor of All Maladies: A Biography of CancerFrom EverandThe Emperor of All Maladies: A Biography of CancerRating: 4.5 out of 5 stars4.5/5 (271)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceFrom EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceRating: 4 out of 5 stars4/5 (890)
- The Little Book of Hygge: Danish Secrets to Happy LivingFrom EverandThe Little Book of Hygge: Danish Secrets to Happy LivingRating: 3.5 out of 5 stars3.5/5 (399)
- Team of Rivals: The Political Genius of Abraham LincolnFrom EverandTeam of Rivals: The Political Genius of Abraham LincolnRating: 4.5 out of 5 stars4.5/5 (234)
- Grit: The Power of Passion and PerseveranceFrom EverandGrit: The Power of Passion and PerseveranceRating: 4 out of 5 stars4/5 (587)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaFrom EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaRating: 4.5 out of 5 stars4.5/5 (265)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryFrom EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryRating: 3.5 out of 5 stars3.5/5 (231)
- On Fire: The (Burning) Case for a Green New DealFrom EverandOn Fire: The (Burning) Case for a Green New DealRating: 4 out of 5 stars4/5 (72)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureFrom EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureRating: 4.5 out of 5 stars4.5/5 (474)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersFrom EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersRating: 4.5 out of 5 stars4.5/5 (344)
- The Unwinding: An Inner History of the New AmericaFrom EverandThe Unwinding: An Inner History of the New AmericaRating: 4 out of 5 stars4/5 (45)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyFrom EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyRating: 3.5 out of 5 stars3.5/5 (2219)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreFrom EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreRating: 4 out of 5 stars4/5 (1090)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)From EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Rating: 4.5 out of 5 stars4.5/5 (119)
- Her Body and Other Parties: StoriesFrom EverandHer Body and Other Parties: StoriesRating: 4 out of 5 stars4/5 (821)
- Occupational Lung DiseaseDocument31 pagesOccupational Lung DiseaseRapid Medicine100% (2)
- Atelectasis: Contraction Atelectasis (Or Cicatrization Atelectasis)Document10 pagesAtelectasis: Contraction Atelectasis (Or Cicatrization Atelectasis)Gan BangNo ratings yet
- Assessment of The Thorax and Lungs 2014Document9 pagesAssessment of The Thorax and Lungs 2014alphabennydelta4468No ratings yet
- PositioningDocument97 pagesPositioningzixdiddy100% (1)
- Ineffective Airway ClearanceDocument6 pagesIneffective Airway Clearanceapi-252726911No ratings yet
- Procedure Demonstration On Postural DrainageDocument15 pagesProcedure Demonstration On Postural DrainageParth VasaveNo ratings yet
- Ebook Cardiovascular and Pulmonary Physical Therapy Evidence To Practice 5Th Edition Frownfelter Test Bank Full Chapter PDFDocument24 pagesEbook Cardiovascular and Pulmonary Physical Therapy Evidence To Practice 5Th Edition Frownfelter Test Bank Full Chapter PDFEdwardStephensMDeqik100% (10)
- Poisoning, DrowningDocument24 pagesPoisoning, DrowningThilaga RamNo ratings yet
- Ko 2020Document48 pagesKo 2020npr00No ratings yet
- Respiratory Distress of The NewbornDocument3 pagesRespiratory Distress of The Newbornsarguss14100% (1)
- ACI14 Suction 2-2Document46 pagesACI14 Suction 2-2Muhamad Ibnu HasanNo ratings yet
- Askep Sistem PernapasanDocument12 pagesAskep Sistem Pernapasanirlin ritiNo ratings yet
- AtelectasisDocument2 pagesAtelectasisiMaibelle BelleNo ratings yet
- Oxygen InsufficiencyDocument70 pagesOxygen InsufficiencydaisyNo ratings yet
- Postural DrainageDocument7 pagesPostural DrainageBiway RegalaNo ratings yet
- Alveolar Recruitment Maneuvers Under General AnesthesiaDocument12 pagesAlveolar Recruitment Maneuvers Under General AnesthesiaBetzaBarriosNo ratings yet
- PhysioEx 9,1: Exercise 7 Activity 3: PEX-07-03Document7 pagesPhysioEx 9,1: Exercise 7 Activity 3: PEX-07-03mishael_baig100% (8)
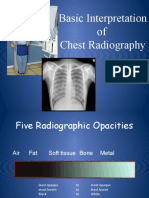
- Basic Interpretation of CXRDocument84 pagesBasic Interpretation of CXRAbdiqani Mohamed AdanNo ratings yet
- Oropharyngeal and Nasopharyngeal Suctioning (Rationale)Document3 pagesOropharyngeal and Nasopharyngeal Suctioning (Rationale)Jemina Rafanan Racadio100% (2)
- Summary of Learning-Pulmo Hour-Tantoco, Justin LareeDocument1 pageSummary of Learning-Pulmo Hour-Tantoco, Justin LareeJustin TantocoNo ratings yet
- Laryngeal ObstructionDocument2 pagesLaryngeal Obstructionajirah02No ratings yet
- Postpartum NCPDocument20 pagesPostpartum NCPireneNo ratings yet
- Pneumonia Nursing Care Plans - 10 Nursing Diagnosis - NurseslabsDocument34 pagesPneumonia Nursing Care Plans - 10 Nursing Diagnosis - NurseslabsMenard Velasco100% (1)
- PEEP Reduces Post-Op Lung ComplicationsDocument6 pagesPEEP Reduces Post-Op Lung ComplicationsTeodorNo ratings yet
- Pulmonary TB RadiologyDocument45 pagesPulmonary TB RadiologyArina Windri RivartiNo ratings yet
- Practise Questions Keith & Moore 5th Edition - Should ReadDocument113 pagesPractise Questions Keith & Moore 5th Edition - Should ReadAmirsalar Eslami83% (6)
- Infantile Lobar Emphysema : OF TWO Cases WithDocument4 pagesInfantile Lobar Emphysema : OF TWO Cases WithparahNo ratings yet
- Test Bank Clinical Manifestations and Assessment of Respiratory Disease Mid PartDocument24 pagesTest Bank Clinical Manifestations and Assessment of Respiratory Disease Mid Partweekup035No ratings yet
- Interpreting Chest FilmsDocument122 pagesInterpreting Chest Filmsgeorgen1No ratings yet
- CSDocument74 pagesCSSimina ÎntunericNo ratings yet