Professional Documents
Culture Documents
Application PDF
Uploaded by
Reno AndriOriginal Description:
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Application PDF
Uploaded by
Reno AndriCopyright:
Available Formats
Guidelines for the Control of Gonococcal Conjunctivitis in the Northern Territory
Guidelines for the Control of
Gonococcal Conjunctivitis in
the Northern Territory
November 2005
Guidelines for the Control of Gonococcal Conjunctivitis in the Northern Territory
Prepared by the Centre for Disease Control.
1st Edition
2nd Edition
3rd Edition
August 1997
January 2003
November 2005
Further copies available from
Centre for Disease Control
Department of Health and Community Services
PO Box 40596
Casuarina NT 0811
OR
http://www.nt.gov.au/health/cdc/protocols.shtml
Comments are welcome and should be directed to the Project/
Research Officer at the above address.
Guidelines for the Control of Gonococcal Conjunctivitis in the Northern Territory
Background ..................................................................................................... 4
Clinical Picture ................................................................................................ 4
Mode of Transmission .................................................................................... 4
Incubation ........................................................................................................ 5
Period of Communicability ............................................................................. 5
Case Definition ................................................................................................ 5
Clinical features ................................................................................................. 5
Case definition................................................................................................... 5
Epidemic definition ............................................................................................ 5
Pathology tests ................................................................................................ 6
Management of Cases .................................................................................... 6
For all suspected cases .................................................................................. 6
Management of Cases in babies .................................................................... 6
Management of sporadic cases in older children or adults ........................ 7
Management of an Epidemic situation .......................................................... 7
General measures and advice for all cases and contacts........................... 9
Bibliography .................................................................................................. 10
Flow chartManagement of gonococcal conjunctivitis ........................... 11
Guidelines for the Control of Gonococcal Conjunctivitis in the Northern Territory
Background
Gonococcal conjunctivitis is a highly contagious eye infection caused by Neisseria
gonorrhoeae. It is a notifiable disease. It can arise in several different situations.
Babies of women with genital gonorrhoea can be infected at birth (neonatal
gonococcal ophthalmia). Small numbers of sporadic cases in children or adults
occur every year in the Northern Territory (NT) as a result of auto-inoculation in a
person with genital gonorrhoea. More rarely, epidemics can occur within a remote
community or over several communities and may involve dozens or even hundreds
of cases. This has occurred in central Australia 4 times in the past 25 years. A
smaller epidemic has been observed in the Top End as well.
Any case indicates the possibility of an epidemic occurring. Urgent notification is
required and investigation of the circumstances with a public health response is
essential. Sporadic cases in children raise the possibility of sexual abuse.
Clinical Picture
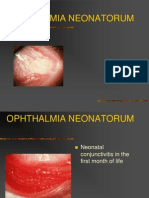
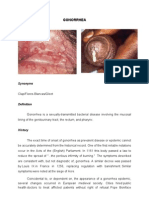
Gonococcal conjunctivitis is usually a localised, fairly severe infection of the
conjunctiva with intense inflammation and copious purulent discharge with or
without periorbital oedema. Corneal ulceration, perforation and blindness can occur
if treatment is not given promptly. It is also possible for the infection to be quite mild
and endure for several weeks or months.
Neonatal infection is a more serious clinical situation than that usually seen in older
children and adults because of its greater potential to cause corneal perforation.
Mode of Transmission
Neonatal infection (gonococcal ophthalmia neonatorum) occurs during passage of
the infant through the birth canal if the mother is infected with genital Neisseria
gonorrhoeae.
Sporadic cases occur in older children and adults where the source is usually
someone with a genital infection. This may occur where:
A person who has genital gonorrhoea who (usually) accidentally infects his
or her eyes by touching them with fingers or fomites (eg clothes, towels)
contaminated with their genital secretions.
A person becomes infected by contact with the contaminated fingers or
fomites of another person who has genital gonorrhoea.
Epidemics can arise from a person with gonococcal conjunctivitis transmitting
infection by direct, non-intimate interpersonal contact, contact with infected fomites
(eg clothes, towels) or by transmission by flies. Such epidemics usually occur in
remote communities and have been associated with increased fly numbers following
heavy rains.
4
Guidelines for the Control of Gonococcal Conjunctivitis in the Northern Territory
Incubation
Usually 2 to 7 days, but sometimes can be longer.
Period of Communicability
May extend for months in untreated people. Infectivity ceases within hours of
appropriate antibiotic therapy. Patients should be isolated / excluded from school
until 24 hours after treatment.
Case Definition
Cases may be divided into confirmed or probable. Both confirmed and probable
cases should be treated according the recommendations below and notified to the
local Centre for Disease Control (CDC)*.
Clinical features
A clinical illness usually characterised by intense inflammation of the conjunctivae,
copious purulent discharge with or without periorbital oedema. Low grade, mild
conjunctivitis lasting several weeks may also occur.
Confirmed case
Neisseria gonorrhoeae detected in a conjunctival specimen by:
Culture,
OR
A nucleic acid technique (NAT) such as Polymerase Chain Reaction (PCR)
where 2 different assays are both positive for the same specimen.
Probable case
A clinically compatible illness and either:
gram negative intracellular diplococci visible on microscopy of a conjunctival
specimen,
OR
epidemiologically linked to a laboratory confirmed case within 1 week of a
confirmed case and occurring either in the same household or same
schoolroom environment
*Note: There is a distinction made between gonococcal conjunctivitis and ophthalmia neonatorum
based on age (28 days) for notification purposes.
Guidelines for the Control of Gonococcal Conjunctivitis in the Northern Territory
Epidemic definition
At least 2 persons with a confirmed case occurring in separate households in the
same community within 1 month of each other.
Pathology tests
All suspect patients should have 2 swabs taken, 1 for microscopy, culture and
sensitivity (MC&S) and 1 for PCR for gonorrhoea and chlamydia.
For MC&S: roll the swab on a slide and let the slide air dry, place the swab
in Modified Amies or Stuarts transport medium (do not refrigerate).
For PCR place the swab in a dry tube and put in the fridge.
Management of Cases
For all suspected cases
Collect swabs as above.
Irrigate the eyes with saline solution to remove the discharge.
If the eye is very crusted it may be necessary to bathe the eyes to remove
the crusting. If so, use sterile cotton wool balls well moistened with normal
saline. Wipe from inner canthus outwards. Use a fresh ball for each wipe
and dispose of in a biohazard bag.
If possible check visual acuity, and check cornea for ulceration with
fluorescein. If either are abnormal discuss with an ophthalmologist
regarding management. Arrange immediate transfer to hospital if there
is corneal ulceration.
If the eyelids are too swollen to be able to examine the eye, discuss with an
ophthalmologist and consider immediate treatment and transfer to hospital.
Antibiotic eye drops may be of some use in addition to parenteral antibiotics
if there is corneal ulceration or staining.
See additional investigations and treatment as indicated below for babies, sporadic
cases and epidemic situations.
Management of Cases in babies
Conjunctivitis in babies less than 6 weeks old may be due to neonatal infection with
N. gonorrhoea, Chlamydia trachomatis or a range of other organisms. A test for
gonorrhoea should be done in all babies of this age with conjunctivitis.
For babies less than 2 weeks old, or with severe conjunctivitis or with corneal
ulceration:
Do investigations and eye toilet as for all suspected cases.
Give 50mg/kg of IM ceftriaxone to a maximum of 125mg immediately.
6
Guidelines for the Control of Gonococcal Conjunctivitis in the Northern Territory
Arrange immediate transfer to hospital for baby and mother.
If diagnosis is confirmed, arrange full STI check and treatment for
gonorrhoea for mother and her sexual partner(s).
For babies 2-6 weeks old without severe conjunctivitis and no sign of corneal
ulceration:
Do investigations and eye toilet as for all suspected cases.
Consult with a paediatrician regarding management as hospitalisation may
be needed (these babies may have or develop neonatally acquired
chlamydia conjunctivitis or pneumonia).
Management of sporadic cases in older children or adults
This may be diagnosed on initial clinical suspicion, but more usually will be less
severe clinically and diagnosed on receipt of the test result.
Do investigations and eye toilet as for all suspected cases.
All persons (children and adults) with confirmed or likely gonococcal
conjunctivitis should have either a low vaginal swab (either self administered
or by the clinician), or first void urine test for MC&S and gonorrhoea and
chlamydia PCR. Persons found to have genital infection should have a full
STI work up and management as per standard practice.
If there is no loss of visual acuity or corneal staining, treat with:
Ceftriaxone 50mg/kg to a maximum of 1g as a single IM or IV dose
Exclude from school or child care for 24 hours after treatment.
All members of the household, or members of same classroom for a school
age child, should be examined for conjunctivitis. If signs are present, swabs
should be taken as for all suspected cases.
Immediate treatment of household or school room contacts even if they have no
symptoms may be necessary to prevent complications in them or further
dissemination. Discuss with a senior Public Health Physician. Factors in favour of
such treatment would be:
remote location or difficulty of access to clinical care or oversight,
crowded accommodation,
sub-optimal understanding and personal practices of hygiene, or
presence of children in the household.
Management of an Epidemic situation
All members of the household where there is an affected person, and members of
same classroom for a school age child, should be examined for conjunctivitis. If
signs are present, swabs should be taken as for all suspected cases.
There is no need for genital or urine specimens in an epidemic situation.
7
Guidelines for the Control of Gonococcal Conjunctivitis in the Northern Territory
All members of the household and members of same classroom for a school age
child, should be treated regardless of whether there are clinical signs of
conjunctivitis.
Treat both children and adults:
Procaine penicillin intramuscularly (IM) as a single dose (50,000 units = 50
mg /kg (to a maximum of 1,500,000 units = 1.5g)
Using Procaine Penicillin 1,500,000 units = 1.5g/3.4ml
Weight
mg
Amount
3 kg to < 6 kg
250 mg
0.6 ml
6 kg to < 10 kg
375 mg
0.8 ml
10 kg to < 15 kg
500 mg
1.1 ml
15 kg to < 20 kg
750 mg
1.7 ml
20 kg to < 30 kg
1.0 g
2.3 ml
Greater than 30 kg
1.5 g
3.4 ml
OR
Amoxycillin plus probenecid as a single oral dose
Weight
Amoxycillin
Probenecid
3 kg to < 6 kg
500 mg
nil
6 kg to < 10 kg
1g
nil
10 kg to < 15 kg
1.5g
250 mg
15 kg to < 20 kg
2g
500 mg
20 kg or over
3g
1g
For people with hypersensitivity to penicillin (excluding immediate hypersensitivity,
i.e. anaphylactic reaction) or where the standard treatment has failed, or if infection
is known to be due to penicillinase producing Neisseria gonorrhoeae (PPNG),
treatment with ceftriaxone should be given as above. Failed treatment is defined as
no substantial decrease in discharge, conjunctival injection or peri-orbital oedema
within 24 hours of treatment.
The recommended treatment in an epidemic situation differs from sporadic cases for
the following reasons:
the potentially large numbers of people requiring treatment quickly and
easier use of and access to procaine penicillin,
cost effectiveness,
to minimise widespread use of ceftriaxone to reduce selection pressure for
resistant organisms, and
Guidelines for the Control of Gonococcal Conjunctivitis in the Northern Territory
the experience of effectiveness of the above regimes in 4 widespread
epidemics in the past 20 years,
General measures and advice for all cases and contacts
Encourage frequent washing of face and hands with warm water and soap
and using clean towels.
Provide information to all close household contacts and family members on
the importance of good hygiene as a way of preventing the spread of
infection.
Warn families to re-present if there is persisting eye infection, fevers or other
symptoms such as arthritis.
Guidelines for the Control of Gonococcal Conjunctivitis in the Northern Territory
Bibliography
1.
2.
3.
4.
5.
6.
7.
8.
9.
10.
11.
12.
13.
14.
15.
16.
17.
18.
19.
20.
21.
22.
23.
24.
Alfonso E, Friedland B, Hupp S, Olsen K, Senikowich K, Sklar VE et al. Neisseria gonorrhoeae
conjunctivitis. An outbreak during an epidemic of acute hemorrhagic conjunctivitis. JAMA
1983; 250(6):794-795.
Chandler JW. Ocular infections associated with sexually transmitted diseases and AIDS. In:
KK Holmes et al, editor. Sexually Transmitted Diseases. 3rd ed. New York: McGraw-Hill; 1999.
Coats DK, Carothers TS, Brady-McCreery K, Paysse EA. Ocular infectious diseases. In: Feigin
RD, Demmler GJ, Cherry JD, Kaplan SL, editors. Textbook of pediatric infectious diseases. 5th
ed. New York: Saunders; 2004.
Gutman LT. Gonococcal infection. In: Remington JS, Klein JO, editors. Infectious disease of
the fetus and newborn infant. 3rd ed. New York: WB Saunders; 2001.
Haimovici R, Roussel TJ. Treatment of gonococcal conjunctivitis with single-dose
intramuscular ceftriaxone. Am J Ophthalmol 1989; 107(5):511-514.
Hansen T, Burns RP, Allen A. Gonorrheal conjunctivitis an old disease returned. JAMA 1966;
195(13):1156.
Hook EW, Handsfield HH. Gonococcal infections in the adult. In: KK Holmes et al, editor.
Sexually Transmitted Diseases. 3rd ed. New York: McGraw-Hill; 1999. 451-466.
Hoosen AA, Kharsany AB, Ison CA. Single low-dose ceftriaxone for the treatment of
gonococcal ophthalmia--implications for the national programme for the syndromic
management of sexually transmitted diseases. S Afr Med J 2002; 92(3):238-240.
Isada CM, Meisler DM. Gonococcal ocular disease. In: Fraunfelder FT, Hampton Roy F,
editors. Current ocular therapy. 3rd ed. New York: WB Saunders; 2000.
Kaye G, Ziskind A, Salmon JF. Gonococcal conjunctivitis. S Afr Med J 1989; 75(11):552.
Laga M, Naamara W, Brunham RC, D'Costa LJ, Nsanze H, Piot P et al. Single-dose therapy of
gonococcal ophthalmia neonatorum with ceftriaxone. N Engl J Med 1986; 315(22):1382-1385.
Lepage P, Kestelyn P, Bogaerts J. Treatment of gonococcal conjunctivitis with a single
intramuscular injection of cefotaxime. J Antimicrob Chemother 1990; 26 Suppl A:23-27.
Mak DB, Smith DW, Harnett GB, Plant AJ. A large outbreak of conjunctivitis caused by a single
genotype of Neisseria gonorrhoeae distinct from those causing genital tract infections.
Epidemiol Infect 2001; 126(3):373-378.
Matters R, Wong I, Mak D. An outbreak of non-sexually transmitted gonococcal conjunctivitis
in Central Australia and the Kimberley region. Commun Dis Intell 1998; 22(4):52-56.
Matters R. Non-sexually transmitted gonococcal conjunctivitis. Commun Dis Intell 1981; 13:3.
McKeown DJ, Mears MP. Epidemic gonococcal conjunctivitis in Central Australia--a
manifestation of cyclical weather patterns? Med J Aust 1998; 169(7):397.
Merianos A, Condon RJ, Tapsall JW, Jayathissa S, Mulvey G, Lane JM et al. Epidemic
gonococcal conjunctivitis in central Australia. Med J Aust 1995; 162(4):178-181.
Mikru FS, Molla T, Ersumo M, Henriksen TH, Klungseyr P, Hudson PJ et al. Community-wide
outbreak of Neisseria gonorrhoeae conjunctivitis in Konso district, North Omo administrative
region. Ethiop Med J 1991; 29(1):27-35.
O'Farrell N, Blignaut P. Gonococcal conjunctivitis. S Afr Med J 1989; 76(10):580.
Rebenstein JB, Jick SL. Disorders of the conjunctiva and limbus. In: Yanoff M, Duker JS,
editors. Ophthalmology. 2nd ed. St. Louis: Mosby Inc; 2005.
Sexually transmitted diseases treatment guidelines 2002. Centers for Disease Control and
Prevention. MMWR Recomm Rep 2002; 51(RR-6):1-78.
Ullman S, Roussel TJ, Culbertson WW, Forster RK, Alfonso E, Mendelsohn AD et al. Neisseria
gonorrhoeae keratoconjunctivitis. Ophthalmology 1987; 94(5):525-531.
Wan WL, Farkas GC, May WN, Robin JB. The clinical characteristics and course of adult
gonococcal conjunctivitis. Am J Ophthalmol 1986; 102(5):575-583.
World Health Organization. Guidelines for the management of sexually transmitted infections.
2003. Geneva, World Health Organization.
10
Guidelines for the Control of Gonococcal Conjunctivitis in the Northern Territory
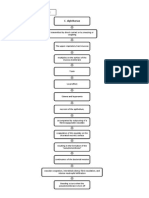
Management of gonococcal conjunctivitis
Collect swabs for
gonorrhoea and
chlamydia, MC&S &
PCR,
Clinical case
Irrigate eye
Visual Acuity
Fluorescein stain
Babies less than
2 week of age
Treat (see p 6) and arrange
hospital admission
If diagnosis confirmed
arrange full STI check for
mother and her partner
Abnormal
Normal
Consult
ophthalmologist
and consider
transfer to hospital
Babies 2-6
weeks of age
Consult with paediatrician
re management
Older children
and adults
Low vaginal swab or First
Void Urine for gonococcal
and chlamydial, MC&S &
PCR
Treat (see p 7)
Exclude from school or
child care for 24 hours
Examine household and school
room contacts for symptoms of
conjunctivitis
Notify CDC.
Discuss need for
treatment of contacts with
Public Health Physician
11
If positive full STI workup
and contact trace
Guidelines for the Control of Gonococcal Conjunctivitis in the Northern Territory
For further information contact
Centre for Disease Control Darwin
Ph: 08 89228044
Fax: 08 89228310
www.nt.gov.au/health/cdc
OR
Your regional CDC
Alice Springs
Ph: 08 89517549
Katherine Ph: 08 89739049
Nhulunbuy Ph
Tennant Creek
08 89870357
Ph
12
08 89624250
You might also like
- Clinical Management Review 2023-2024: Volume 2: USMLE Step 3 and COMLEX-USA Level 3From EverandClinical Management Review 2023-2024: Volume 2: USMLE Step 3 and COMLEX-USA Level 3No ratings yet
- Guidelines For The Control of Gonococcal Conjunctivitis in The Northern TerritoryDocument2 pagesGuidelines For The Control of Gonococcal Conjunctivitis in The Northern TerritoryDenden RoraNo ratings yet
- 420 052 Guideline DiphtheriaDocument12 pages420 052 Guideline DiphtheriaLeo RinaldiNo ratings yet
- Diphtheria how to recognize the disease, how to keep from catching it, how to treat those who do catch itFrom EverandDiphtheria how to recognize the disease, how to keep from catching it, how to treat those who do catch itNo ratings yet
- Name: Carlo M. Yao Bachelor of Science in NursingDocument33 pagesName: Carlo M. Yao Bachelor of Science in Nursingcarlo24_briggsNo ratings yet
- Neonatal Sepsis, Opthalmia Neonatarum & HIV/AIDSDocument15 pagesNeonatal Sepsis, Opthalmia Neonatarum & HIV/AIDSSAKSHI RANANo ratings yet
- Diphtheria HandoutsDocument8 pagesDiphtheria HandoutsRachelle Mae DimayugaNo ratings yet
- Measles Management Guidelines - 091222-1Document14 pagesMeasles Management Guidelines - 091222-1Tushar AmbedareNo ratings yet
- Meningococalmeningitis: Presented by Class 6 B Community Medicine DepartmentDocument41 pagesMeningococalmeningitis: Presented by Class 6 B Community Medicine DepartmentMohamed AhmedNo ratings yet
- Ophthalmia NeonatorumDocument17 pagesOphthalmia NeonatorumIndranil DuttaNo ratings yet
- By-Dr. Samarjeet Kaur JR-II BRD Med. College GKPDocument17 pagesBy-Dr. Samarjeet Kaur JR-II BRD Med. College GKPSamarjeet Kaur100% (1)
- Infections of The Newborn - 2Document17 pagesInfections of The Newborn - 2rat5fNo ratings yet
- Jurnallll 3Document15 pagesJurnallll 3RiestaKierantiNo ratings yet
- Role of Family Physician in Management of Neonatal Conjunctivitis or Ophthalmia NeonatorumDocument20 pagesRole of Family Physician in Management of Neonatal Conjunctivitis or Ophthalmia NeonatorumAbdulla1999 AshrafNo ratings yet
- Keratoconjuctivitis FR2006Document27 pagesKeratoconjuctivitis FR2006mrezasyahliNo ratings yet
- CDC Diphtheria Surveillance WorksheetDocument6 pagesCDC Diphtheria Surveillance WorksheetLuna WhiteNo ratings yet
- Chapt 19.3 PDFDocument98 pagesChapt 19.3 PDFkasunswiftNo ratings yet
- OPTHALMIA NEONATORUM: Is An Eye Infection That Occurs at Birth or During The First MonthDocument4 pagesOPTHALMIA NEONATORUM: Is An Eye Infection That Occurs at Birth or During The First Monthcharuz_092823No ratings yet
- Dacryocystitis: Continuing Education ActivityDocument8 pagesDacryocystitis: Continuing Education Activityerna utamiNo ratings yet
- Gonorrhea 1Document26 pagesGonorrhea 1Alessandra Franchesca CortezNo ratings yet
- Neonatal InfectionsDocument19 pagesNeonatal InfectionsA B Siddique RiponNo ratings yet
- Microlife GP - FINAL - Oct 2012Document2 pagesMicrolife GP - FINAL - Oct 2012HeartofEnglandNo ratings yet
- Jurnal Nirza MataDocument15 pagesJurnal Nirza MataRozans IdharNo ratings yet
- Update MonkeypoxDocument14 pagesUpdate MonkeypoxMary Grace PedrozoNo ratings yet
- Clinical Management Protocol PDFDocument7 pagesClinical Management Protocol PDFAJEET KUMAR PANDEYNo ratings yet
- B1692 Virtual Management of Confirmed Monkeypox CasesDocument19 pagesB1692 Virtual Management of Confirmed Monkeypox CaseschaandNo ratings yet
- Infectious Diseases GuideDocument30 pagesInfectious Diseases GuideSarahNo ratings yet
- Opthalmia UmDocument23 pagesOpthalmia Umnanu-jenuNo ratings yet
- Viral Conjunctivitis AlgorithmDocument8 pagesViral Conjunctivitis AlgorithmRobert Selvin MNo ratings yet
- Peds InfectiousDocument8 pagesPeds InfectiousMohammad RammalNo ratings yet
- Chickenpox & ChlamydialDocument5 pagesChickenpox & ChlamydialEliezah RodriguezNo ratings yet
- Patofisiologi DifteriDocument11 pagesPatofisiologi DifteriicorrrNo ratings yet
- Meningococcemia: N F S LDocument45 pagesMeningococcemia: N F S LMarky Roque100% (1)
- Guidelines For The Management of Corneal Ulcer WHODocument36 pagesGuidelines For The Management of Corneal Ulcer WHOichalledhaNo ratings yet
- GonorrheaDocument22 pagesGonorrheaSharah Londonio100% (1)
- 420 063 Guideline MeaslesDocument25 pages420 063 Guideline MeaslesJerome ProfetanaNo ratings yet
- New VPD Orientation SlidesDocument31 pagesNew VPD Orientation Slidesapi-209888269No ratings yet
- Journal Reading - Nurul Nadifa Erza - 2010221012 - Insight Into ScabiesDocument24 pagesJournal Reading - Nurul Nadifa Erza - 2010221012 - Insight Into ScabiesNurul Nadifa ErzaNo ratings yet
- Diseases, Syndromes & Health Events Under SurveillanceDocument61 pagesDiseases, Syndromes & Health Events Under SurveillanceGina BoligaoNo ratings yet
- Communicable Disease Lectures 2Document2 pagesCommunicable Disease Lectures 2Sheana TmplNo ratings yet
- What Is PlagueDocument3 pagesWhat Is Plagueanon_959000253No ratings yet
- 09conjunctival Infections 13-12-07Document55 pages09conjunctival Infections 13-12-07ari rujatiNo ratings yet
- Neonatal InfectionDocument19 pagesNeonatal InfectionLekshmi ManuNo ratings yet
- Neonatal Infection (Group Assignment)Document12 pagesNeonatal Infection (Group Assignment)AMOS MELINo ratings yet
- Sexually Transmitted Infections and PregnancyDocument19 pagesSexually Transmitted Infections and PregnancyBeyins TiuNo ratings yet
- National AND: Dengue ControlDocument26 pagesNational AND: Dengue ControlFranz Anthony Quirit GoNo ratings yet
- Monkey PoxDocument29 pagesMonkey PoxMalavika A GNo ratings yet
- Measles: Investigative GuidelinesDocument17 pagesMeasles: Investigative GuidelinesDennis DennisNo ratings yet
- Annexure-XX Clinical Management Protocol: (Novel Influenza A H1N1)Document3 pagesAnnexure-XX Clinical Management Protocol: (Novel Influenza A H1N1)Ramadi PrameelaNo ratings yet
- Bacterial Keratitis: Signs and SymptomsDocument4 pagesBacterial Keratitis: Signs and Symptoms]]]100% (1)
- Conjunctivitis - Diagnosis & DDXDocument7 pagesConjunctivitis - Diagnosis & DDXNabillaMerdikaPutriKusumaNo ratings yet
- Gastroenteritis Infection Prevention and Control SOPDocument9 pagesGastroenteritis Infection Prevention and Control SOPM Ukrio Zefri ZonNo ratings yet
- Mumps Clinical Diagnosis Fact Sheet 508Document2 pagesMumps Clinical Diagnosis Fact Sheet 508Andrea DelgadoNo ratings yet
- Chapter 5 Bacterial Diseases of Ruminants 2020Document30 pagesChapter 5 Bacterial Diseases of Ruminants 2020JAD IMADNo ratings yet
- And Treatment Blepharokeratoconjunctivitis in Children: DiagnosisDocument5 pagesAnd Treatment Blepharokeratoconjunctivitis in Children: DiagnosislordaponkNo ratings yet
- Conjunctivitis (H10)Document3 pagesConjunctivitis (H10)unit cdc pkd raubNo ratings yet
- Corneal Atlas 2011Document20 pagesCorneal Atlas 2011Wentao Liu100% (3)
- East Africa University Bosaso, Puntland Somalia Faculty of Medicine Communicable Disease MR Buruj Ali SaladDocument42 pagesEast Africa University Bosaso, Puntland Somalia Faculty of Medicine Communicable Disease MR Buruj Ali SaladShaimaa AbdulkadirNo ratings yet
- 29 Nursing Management of Communicable DiseaseDocument79 pages29 Nursing Management of Communicable DiseaseMonika SanaaNo ratings yet
- Azygos Venos System 2Document17 pagesAzygos Venos System 2Fazil Omar BelwaelNo ratings yet
- Peds Shelf NotesDocument88 pagesPeds Shelf Notesskeebs23100% (8)
- Mirzi S. Turbolencia,: Curriculum VitaeDocument2 pagesMirzi S. Turbolencia,: Curriculum VitaeChester KyleNo ratings yet
- Nicom CompetencyDocument2 pagesNicom Competencyapi-258141893No ratings yet
- Grammar and VocabularyDocument2 pagesGrammar and Vocabularythiên bình trầnNo ratings yet
- Level 1 HospitalDocument2 pagesLevel 1 Hospitaljoyrena ochondra100% (2)
- Kinesiologia E Chiropratica-Migraines - The Applied Kinesiology and Chiropractic PerspectiveDocument5 pagesKinesiologia E Chiropratica-Migraines - The Applied Kinesiology and Chiropractic PerspectiveFernando BernardesNo ratings yet
- Claim IntimationDocument2 pagesClaim IntimationSyed's Way PoolNo ratings yet
- Periodic Medical ExaminationDocument4 pagesPeriodic Medical ExaminationAndreeaRedheadNo ratings yet
- Teorya NG PagtanggapDocument6 pagesTeorya NG PagtanggapMaxine TaeyeonNo ratings yet
- Respiratory Therapist, NICU/ICUDocument5 pagesRespiratory Therapist, NICU/ICUapi-77517256No ratings yet
- Autohemoterapia en Urticaria CrónicaDocument2 pagesAutohemoterapia en Urticaria CrónicaCristobal CarrascoNo ratings yet
- AmfepramoneDocument3 pagesAmfepramone18.10.1986No ratings yet
- Management of Status Asthmatic Us in ChildrenDocument7 pagesManagement of Status Asthmatic Us in Childrenjshq1971No ratings yet
- Oncology Scope of ServicesDocument2 pagesOncology Scope of ServicesJaisurya SharmaNo ratings yet
- 7 ImunisasiDocument85 pages7 ImunisasiElfa RiniNo ratings yet
- Blood ComponentDocument33 pagesBlood Componentmatrixtrinity100% (1)
- Easy Oral Motor Exercises To TryDocument4 pagesEasy Oral Motor Exercises To TryAzryanty Mohamad ArifinNo ratings yet
- MAPEH Reaction PaperDocument4 pagesMAPEH Reaction Papergellijimenez100% (1)
- 9 - DR Arun Bhatt - Schedule YDocument27 pages9 - DR Arun Bhatt - Schedule Yvivek100% (1)
- Hospital and NurseDocument7 pagesHospital and NurseArselia RumambiNo ratings yet
- Lesson 21 PDFDocument4 pagesLesson 21 PDFShirmayne TangNo ratings yet
- Neuro Tract Lesions Ps230114Document16 pagesNeuro Tract Lesions Ps230114সোমনাথ মহাপাত্রNo ratings yet
- Can Rotation PlanDocument18 pagesCan Rotation PlanMadhuNo ratings yet
- Business Plan For CTDocument12 pagesBusiness Plan For CTapi-310212918100% (2)
- USA Physician DirectoryDocument265 pagesUSA Physician Directorysonukarma321No ratings yet
- Critical Care/Intensive Care Unit Experience Internal Medicine INM.M INM.S CourseDocument11 pagesCritical Care/Intensive Care Unit Experience Internal Medicine INM.M INM.S CourseAmer Moh SarayrahNo ratings yet
- Ebp Powerpoint PresentationDocument40 pagesEbp Powerpoint Presentationapi-383379774No ratings yet
- A Neonate With Precordial Pulsations.Document5 pagesA Neonate With Precordial Pulsations.Jose Maria LloredaNo ratings yet