Professional Documents
Culture Documents
Deep Peri-Implantitis Two Cases Treated With Implant Apicoectomywith Follow-Up of at Least 7 Years
Uploaded by
matias112Original Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Deep Peri-Implantitis Two Cases Treated With Implant Apicoectomywith Follow-Up of at Least 7 Years
Uploaded by
matias112Copyright:
Available Formats
Oral Surgery ISSN 1752-2471
ORIGINAL ARTICLE
Deep peri-implantitis: two cases treated with implant apicoectomy
with follow-up of at least 7 years
D. Kalyvas1, M. Tarenidou1, G. Zorogiannidis2, E. Tsetsenekou1 & A. Grous3
1
Oral Surgery, Dental School, Oral and Maxillofacial Surgery, University of Athens, Athens, Greece
General private practitioner, Athens, Greece
3
Private Prosthodontist, Athens, Greece
2
Key words:
implant apicoectomy, peri-implantitis,
radiolucency
Correspondence to:
Professor D Kalyvas
Oral Surgery
Dental School
Oral and Maxillofacial Surgery
University of Athens
str. Thivon 2, Goudi
11567 Athens
Greece
Tel.: + 0030-210-8233608
email: demkal@dent.uoa.gr
Accepted: 21 October 2014
doi:10.1111/ors.12140
Abstract
Aim: Deep periimplantitis is a lesion located in the periapical region of an
osseointegtated implant. The aim of this study was to present 2 cases of this
feature treated with apicoectomy.
Materials and methods: Two cases of deep periimplantitis located in the
maxillary premolar region are presented in this report. Both the lesions
were situated in the apical segment of otherwise osseointegrated and long
(15 mm) implants. They were treated with surgical debridement,
apicoectomy, bone substitute and antibiotics.
Results: Bone overheating, proximity to periapical lesions or previous
inflammation seem to be the three possible causes of the lesions in the cases
presented. The follow-up period of 7 and 10 years indicates that implant
apicoectomy is a safe and reliable treatment choice.
Conclusions: The treatment of choice for deep periimplantitis is implant
apicoectomy, unless the implant is mobile, where implant removal is
preferable.
Clinical relevance
apex resection with a follow-up period of 7 and 10
years.
Scientic rationale for study
Deep peri-implantitis is a lesion defined as a bone loss
limited to the apical segment of an otherwise
osseointegrated implant. The radiolucent lesion
usually appears shortly after implant insertion and is
accompanied by symptoms of pain, tenderness,
swelling and/or the presence of a fistulous tract. The
aetiology and mechanism of this lesion are multifactorial. Most commonly, factors such as bone overheating or periapical inflammation of, either an
adjacent tooth, or a previously extracted tooth at the
implant site, are implicated. Several methods have
been proposed to treat deep peri-implantitis. Among
these, implant apicoectomy seems to be an effective
treatment with long-term results and few complications, if any. The aim of this article is to present two
cases of deep peri-implantitis treated with implant
200
Principal ndings
It is noted that in both cases, the maxillary premolar
region is involved. Additionally, both the affected
implants were 15 mm long, which suggests that a possible cause of deep peri-implantitis in these cases was
bone overheating during implant placement. However,
in the first case, there is no dental record for the
extracted tooth 15 and, therefore, the remaining
inflammatory cells or bacteria from a periapical lesion
cannot be excluded as a possible cause. As far as the
second case is concerned, the lesion can also be attributed to the fact that the implant at site 14 was placed in
close proximity to the root of tooth 13 and its periapical
lesion.
The peri-implantitis in both cases was treated with
amoxicillin 500 mg 3 6, surgical debridement,
Oral Surgery 8 (2015) 200--207.
2014 The British Association of Oral Surgeons and John Wiley & Sons Ltd
Deep peri-implantitis
Kalyvas et al.
apicoectomy and use of bone substitute. During the 7
years and 10 years follow-up period, there are no
clinical signs, symptoms or radiographic findings.
Practical implications
In order to treat deep peri-implantitis, several
approaches have been proposed. They include surgical
debridement (curettage), implant detoxification,
guided tissue regeneration, apical resection and
implant removal. Undoubtedly, implant removal is the
preferable treatment for mobile implants. Implant
apicoectomy appears to be an effective treatment
method. The uncomplicated follow-up period of 7 and
10 years points out this approach as a treatment of
choice.
Introduction
Deep peri-implantitis is a lesion defined as a bone
loss limited to the apical segment of an otherwise
osseointegrated implant. Other terms used to
describe this lesion are localized osteomyelitis1,
endodontic implantitis2, apical periimplantitis3,4,
periapical implant lesion512, retrograde periimplantitis1315, periradicular lesion1620 and periapical
radiolucencies21. We believe that the term deep
periimplantitis stands better for the inflammatory
nature and the origin of the lesion. Deep periimplantitis can present as an apical radiolucency
associated with an integrated implant. Accompanying
signs and symptoms can include pain, swelling, tenderness and the presence of a sinus tract (Table 1).
The first cases were described by McAllister et al.21 in
1992 and Sussman and Moss1 in 1993. Reiser and
Nevins (1995)7 defined this complication as implant
periapical lesion and suggested its aetiology, classification (into inactive and infective lesions) and treatment.
Sussman (1998)26 proposed a classification in case types
1 (implant to tooth) and 2 (tooth to implant).
The prevalence of deep peri-implantitis varies
between 0.26% and 1.8%7,14. There is a higher incidence for implants in the maxilla (3:1), and the predominant sites are the maxillary central incisor and
first premolar areas (Table 1)14. Most of the implicated
implants are 12 mm long or more. The overall failure
rate is higher for machined implants. There is one
retrospective study14 reporting a higher incidence of
deep peri-implantitis for TiUnite (Nobel BioCare,
Gteborg, Sweden) implants (8/80) rather than for
machined implants (2/459), but the numbers included
are very small.
Oral Surgery 8 (2015) 200--207.
2014 The British Association of Oral Surgeons and John Wiley & Sons Ltd
The aetiology and mechanism of this lesion are
unknown, and there are many theories as to how the
lesion arises. Most commonly, factors such as bone
overheating or periapical inflammation of, either an
adjacent tooth, or a previously extracted tooth at the
implant site, are implicated. Several methods have
been proposed to treat deep peri-implantitis. Among
these, implant apicoectomy seems to be an effective
treatment with long-term results and few complications, if any. The aim of this article is to present two
cases of deep peri-implantitis treated with implant apex
resection with a follow-up period of 7 and 10 years.
Case report no. 1
A 52-year-old woman with no significant medical
history appeared with a fused-to-metal crown at tooth
14 and a cantilever at the site of the missing tooth 15,
which had been extracted 3 years before. There is no
record for the missing tooth 15 and the reason for its
extraction. The tooth 14 was extracted due to periodontal infection and class 3 mobility. The patient had
two implants placed by drilling at sites 14 and 15 on
July 1999, 5 months after the extraction of the tooth 14
(Fig. 1). The implant type was Lifecore Restore
machined, and their diameter and length were
3.3 11.5 mm and 3.75 15 mm, respectively.
According to our protocol, 1 g of amoxicillin was
administered 1 h preoperatively and for 4 days postoperatively. On August 2000, a fistula was noted
(Fig. 2). There was also mild pain at palpation. Radiographically, there was a radiolucency around the apex
of the implant at site 15 and a gutta-percha cone
inserted in the fistula pointed at the apex of this
implant (Fig. 3). The peri-implantitis was treated with
amoxicillin 500 mg 3 6, surgical debridement,
apicoectomy and use of bone substitute (BioOss
(Geistlich Pharma North America Inc., Princeton, USA)
granules 0.251 mm) (Figs. 46). During the 7 years
follow-up period, there are no clinical signs, symptoms
or radiographic findings (Fig. 7).
Case report no. 2
A 44-year-old man with no significant medical history,
except from the fact that he is a heavy smoker (40
cigarettes/day), appeared with an implant-tooth
retained restoration. After clinical and radiographic
examination, the extraction of implants and teeth
was decided, except from teeth 13 and 27, which
were endodontically treated and used to retain the
provisional restoration. In November 1996, 5 months
after the extractions, he had six Lifecore (Lifecore
201
202
Mohamed et al.18
Kalyvas et al. (2009)
a. 15
b. 14
22
a. 14
b. 24
c. 44
d. 24
45
43
12
Quirynen et al.24
Tseng et al.12
Bousdras et al.25
Tzm et al.8
12
36
Flanagan4
Oh et al.6
a. 24, 25
b. 25
c. 43
Implant site
46, 47
a. 42
b. 46
c. 46
d. 45
13
Chaffee et al.22
Brisman et al.23
Ayangco and Sheridan
Authors
a. 13 months after placement
b. 12 months after placement
4 months
a. 3 months later
b. 3 weeks later
c. 2 weeks later
d. 6 days later
6 months after prosthesis
1 month after prosthesis
5 years after implant placement
10 weeks post-operatively
At uncovery surgery
35 days later
a. 6 weeks later
b. After 4 months and after 4 weeks
c. After 4 months
d. 2 weeks later
a. 18 months after prosthesis
b. 9 months after prosthesis
c. 1 month after
Time of appearance
Table 1 Signs, symptoms and aetiology of deep peri-implantitis
a. Fistula, pain at palpation
b. Pain at percussion
c. Pain, swelling, stula, pus secretion
d. Swelling
Pockets, loss of osseointegration
Pain
7 mm probing depth with pus formation,
periapical stula
a. Fistula, mild pain at palpation
b. Halitosis, stula, mild pain at palpation
None
Pain
a. Fistula
b. Fistula, implant mobility
c.
d. Mild pain at palpation, erythema and
swelling.
Pain
Fistula, implant mobility
a. Swelling, stula
b. Tenderness upon touching
c. Pain
Clinical signs, symptoms
a. Lifecore Restore 3.75 15 mm
b. Lifecore Restore 3.75 15 mm
Not reported
4.0 13 mm Osseotite
Brnemark system
3.75 13 mm
a. 15 mm MkIII
b. 13 mm MkII
c. 13 mm MkII
d. 13 mm MkIII
ITI
3.75 18 mm MkIII
3.25 13 mm
4.25 10 mm
3.3 10 mm
5 10 mm (Root formed implants)
a. Bone overheating (possibly ET 15)
b. EP 13
Proximity to 21 (EP)
endodontic pathology (EP) 11
a. ET 14
b. ET 24
c. ET 44
d. Proximity to 23, EP 25, or ET 24.
Proximity 45 to 44, EP 44
ET 12
Remaining root of 36
EP 45
a. ET 42
b. ET 46 or EP 45
c. Proximity of 46 to 45, EP 45
d. ET 45
a. Extracted tooth (ET) 24
b. ET 25
c. ET 43
a. 4 15 mm
b. 4 13 mm
c. 4 13 mm (Brnemark system
implants)
a.
b.
c.
d.
Aetiology
Implant type
Deep peri-implantitis
Kalyvas et al.
2014 The British Association of Oral Surgeons and John Wiley & Sons Ltd
Oral Surgery 8 (2015) 200--207.
Deep peri-implantitis
Kalyvas et al.
Figure 1 Panoramic X-ray of the rst case.
Figure 3 Gutta-percha cone pointing the apex of the implant.
Figure 2 Clinical aspect of the stula.
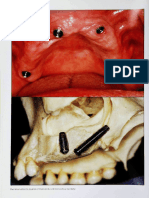
Figure 4 Intraoperative aspect of the lesion.
Biomedical, Minnesota, USA) implants placed by drilling in his upper jaw at sites 14, 12, 21, 23, 24 and 26
(Fig. 8). The implants diameter and length were
3.75 15 mm for the sites 14, 12, 21, 23 and
3.75 13 mm for the sites 24, 26. According to our
protocol, 1 g of amoxicillin was administered 1 h
preoperatively and for 4 days post-operatively. In July
1997, the teeth 13 and 27 were extracted. In November
1997, the patient presented with a complaint of halitosis and pain at palpation. Clinical examination
revealed a draining fistula (Figs. 9, 10). The treatment
was amoxicillin 500 mg 3 8, apicoectomy of the
implant at site 14 and tissue regeneration with BioOss
and Guidor (Sunstar Americas, Chicago, USA) membrane (Fig. 11). During the 10 years follow-up period,
there are no clinical signs, symptoms or radiographic
findings (Fig. 12).
Oral Surgery 8 (2015) 200--207.
2014 The British Association of Oral Surgeons and John Wiley & Sons Ltd
Discussion
The most frequent sites of deep peri-implantitis commonly appears are adjacent to sites of endodontic
pathology or the extraction sites of endodontically
treated teeth.
The aetiology of the lesion remains unclear. There
are a number of theories that have been presented in
the literature, including bone necrosis following overheating during surgical procedure, translocation of
bacteria from adjacent teeth, undiagnosed pathology at
the extraction sites (remaining inflammatory cells,
granuloma, presence of residual root fragments, fenestration of the vestibular alveolar bone, proximity to an
infected maxillary sinus) bacterial contamination of
the implant surface during placement, premature
loading leading to bone micro-fractures, poor bone
quality.
203
Deep peri-implantitis
Kalyvas et al.
Figure 5 The removed part of the implant and the periapical lesion.
Figure 7 Post-operative X-ray taken after a 7 years period of follow-up.
Figure 8 Panoramic X-ray after the implant placement.
Figure 6 The surgical eld after the apicoectomy of the implant.
As mentioned before, according to Sussman, when
an implant insertion results in devitalisation of a tooth
(e.g. due to insufficient distance, bone overheating and
cutting off the blood supply to the pulp), it can cause an
endodontic pathology that consequently may infect
the implant (pathway 1). A periapical lesion from a
nearby devitalised tooth (pathway 2) can encroach
upon the implant and contaminate it (e.g. reactivation
of a dormant periapical lesion or removal of the periapical endodontic seal). As far as the inactive lesion is
concerned, it is usually caused by placing implants that
are shorter than the drilled cavity or by a heat-induced
aseptic bone necrosis.
It was suggested that dental implants do not possess
the ability to withstand any bacterial challenge during
the first stage of osseointegration and that bacteria or
endotoxins can travel through marrow spaces and
contaminate an adjacent implant19. However, there is a
204
debate regarding if and when bacteria are present in
periradicular lesions. Even in the absence of viable
bacteria, surfaces from clinically ailing or failing
implants have been shown to be contaminated with
endotoxin, which apparently can prevent biologic
repair. Presumably, the presence of endotoxins could
induce deep peri-implantitis, when their origin is the
apex of the extracted tooth or the adjacent failed root
canal treatment19. On the other hand, Flanagan
believes that the bone at the implant site may contain
residual encapsulated bacteria, which are activated by
the implant osteotomy, reinstating the infection at the
apex of the implant4. Additionally, it is proposed that
apical entrapment of gingival epithelial cells during the
placement phase of treatment may be a cause of deep
peri-implantitis and that a small perforation of the cortical bone at the apical end of the osteotomy could
provide a path of least resistance for an infectious
process and a fistula formation4.
Oral Surgery 8 (2015) 200--207.
2014 The British Association of Oral Surgeons and John Wiley & Sons Ltd
Kalyvas et al.
Figure 9 Clinical aspect of the stula.
Deep peri-implantitis
Figure 11 The surgical eld after the apicoectomy of the implant.
Figure 12 Post-operative X-ray after a 10 years period.
Figure 10 Gutta-percha pointing the origin of the inammation. The relation with the adjacent non-healed extraction socket is a matter of radiographic projection.
It is noted that in both cases, the maxillary premolar
region is involved. This is consistent with the observations of Quirynen et al. (2005)14, as well as the data
presented in Table 1. Additionally, both the affected
implants were 15 mm long, which suggests that a possible cause of deep peri-implantitis in these cases was
bone overheating during implant placement. The bone
at the apical part of the prepared implant site may not
be adequately cooled with saline irrigation during
drilling when the site walls are as deep as 15 mm.
However, in the first case, there is no dental record for
the extracted tooth 15 and, therefore, the remaining
inflammatory cells or bacteria from a periapical lesion
cannot be excluded as a possible cause. As far as the
second case is concerned, the lesion can also be attribOral Surgery 8 (2015) 200--207.
2014 The British Association of Oral Surgeons and John Wiley & Sons Ltd
uted to the fact that the implant at site 14 was placed in
close proximity to the root of tooth 13 and its periapical
lesion.
In order to treat deep peri-implantitis, several
approaches have been proposed. They include surgical
debridement (curettage), implant detoxification,
guided tissue regeneration, apical resection and
implant removal (Table 2). There are no randomised
control trials available for none of the treatment
options. According to Oh et al., implant removal is the
preferable treatment for mobile implants6. Otherwise,
surgical intervention, that is, the removal of inflamed
granulation tissue, is indicated. Detoxification is the
disinfection of the implant surface by chemical means,
such as citric acid, chlorhexidine gel, tetracycline
and/or hydrogen peroxide13. However, because of the
rough surfaces on some implants, the mechanical
management of contaminated implant surfaces is difficult. In addition, Shabahang et al. report that the results
205
Deep peri-implantitis
Kalyvas et al.
Table 2 Treatment of deep peri-implantitis
Authors
Ayangco and Sheridan
Chaffee et al.22
Brisman et al.23
Flanagan4
Oh et al.6
Quirynen et al.24
Tseng et al.12
Bousdras et al.25
Tzm et al.8
Kalyvas et al. (2009)
Mohamed et al.18
13
Treatment
Follow-up
a. Antibiotics, debridement, detoxication with tetracycline paste
b. Debridement, detoxication with tetracycline paste, amoxicillin 500 mg 3 7
c. Debridement, detoxication with tetracycline paste
Debridement, Guided Bone Regeneration, amoxicillin 500 mg 3 10, endodontic treatment of
45, 14 months later retreatment of 45
a. Implant removal
b. Implant removal
c. Implant removal
d. Drainage, clindamycin 300 mg 4 2 and 150 mg 4 7, surgical debridement
Penicillin 500 mg 4 7 and hydrocodone, debridement, placement of calcium hydroxide paste
Implant removal, apicoectomy of adjacent tooth, new implant 3 months later
a. Doxycycline 100 mg 10, debridement
b. Antibiotics, debridement, GBR
c. Implant removal
d. Implant removal
Implant removal, GBR, new implant 4 months later
Metronidazole 400 mg 3 7, debridement and apicoectomy, chlorhexidine mouthwash
Endodontic treatment of 11, surgical debridement, apicoectomy of 11, GBR, amoxicillin
500 mg 4 10, chlorhexidine mouthwash
a. Amoxicillin 500 mg 3 8, apicoectomy and tissue regeneration
b. Amoxicillin 500 mg 3 8, apicoectomy and tissue regeneration
a. Debridement and detoxication
b. Xenograft and platelet-rich brin
a. 8 months
b. 1 year
c. 8 years
18 months
of their experimental study indicated that detoxification of the implant surface did not have a positive
impact on the amount of osseointegration19. Therefore,
implant apicoectomy appears to be an effective treatment method. Balshi et al.5 report that 38 of 39 (97.4%)
resected implants remained stable and functional. The
follow-up time averaged 4.54 years, whereas the
longest exceeded 15 years.
Conclusion
3.
4.
5.
In conclusion, as both cases have a long follow-up
period (7 and 10 years), the implant apicoectomy can
be considered as a safe and reliable treatment with
long-term success.
6.
Conflict of interest
7.
The authors confirm that they have no conflict of
interest.
8.
References
1. Sussman HI, Moss SS. Localized osteomyelitis secondary to endodontic-implant pathosis. A case report.
J Periodontol 1993;64:30610.
2. Laird BS, Hermsen MS, Gound TG, Al Salleeh F,
Byarlay MR, Vogt M et al. Incidence of endodontic
implantitis and implant endodontitis occurring with
206
9.
11 months
a. 1 year
b. 3 years
Regular recall
2 years
6 months
a.
b.
a.
b.
7 years
10 years
4 months (loading)
1 year
single-tooth implants: a retrospective study. J Endod
2008;34(11):131624.
Dahlin C, Nikfarid H, Alsen B, Kashani H. Apical periimplantitis: possible predisposing factors, case reports
and surgical treatment suggestions. Clin Implant Dent
Relat Res 2009;11(3):2227.
Flanagan D. Apical (retrograde) peri-implantitis: a case
report of an active lesion. J Oral Implantol
2002;28(2):926.
Balshi SF, Wolfinger GJ, Balshi TJ. A retrospective
evaluation of a treatment protocol for dental implant
periapical lesions: long-term results of 39 implant
apicoectomies. Int J Oral Maxillofac Implants
2007;22:26772.
Oh T, Yoon J, Wang H. Management of the implant
periapical lesion: a case report. Implant Dent
2003;12:416.
Reiser GM, Nevins M. The implant periapical lesion:
etiology, prevention, and treatment. Compend Contin
Educ Dent 1995;16:768, 770, 772 passim.
Tzm TF, Senimen M, Ortakoglu K, zdemir A,
Aydin C, Keles M. Diagnosis and treatment of a large
periapical implant lesion associated with adjacent
natural tooth: a case report. Oral Surg Oral Med Oral
Pathol Oral Radiol Endod 2006;101:1328.
Jalbout ZN, Tarnow DP. The implant periapical lesion:
four case reports and review of the literature. Pract
Proced Aesthet Dent 2001;13(2):10712.
Oral Surgery 8 (2015) 200--207.
2014 The British Association of Oral Surgeons and John Wiley & Sons Ltd
Kalyvas et al.
10. Penarrocha-Diago M, Boronat-Lopez A, Garcia-Mira B.
Inflammatory implant periapical lesion: etiology, diagnosis, treatment presentation of 7 cases. J Oral
Maxillofac Surg 2009;67(1):16873.
11. Scarano A, Di Domizio P, Petrone G, Iezzi G, Piatelli A.
Implant periapical lesion: a clinical and histologic
report. J Oral Implantol 2000;26:10913.
12. Tseng C, Chen YM, Pang I, Weber H. Peri-implant
pathology caused by periapical lesion of an adjacent
natural tooth: a case report. Int J Oral Maxillofac
Implants 2005;20:6325.
13. Ayangco L, Sheridan PJ. Development and treatment
of retrograde periimplantitis involving a site with a
history of failed endodontic and apicoectomy procedures. Int J Oral Maxillofac Implants 2001;16:412
17.
14. Quirynen M, Vogels R, Alsaadi G, Naert I, Jacobs R, van
Steenberghe D. Predisposing conditions for retrograde
peri-implantitis, and treatment suggestions. Clin Oral
Implants Res 2005;16:599608.
15. Zhou W, Han C, Li D, Li Y, Song Y, Zhao Y. Endodontic
treatment of teeth induces retrograde periimplantitis.
Clin Oral Implants Res 2009;20(12):132632.
16. Bretz WA, Matuck AN, De Oliveira G, Moretti AJ, Bretz
WA. Treatment of retrograde peri-implantitis: clinical
report. Implant Dent 1997;6(4):28790.
17. Ataullah K, Chee LF, Peng LL, Lung KHH. Management
of retrograde periimplantitis: a clinical case report.
J Oral Implantol 2006;32(6):30812.
Oral Surgery 8 (2015) 200--207.
2014 The British Association of Oral Surgeons and John Wiley & Sons Ltd
Deep peri-implantitis
18. Mohamed JB, Alam NM, Singh G, Chandrasekaran SC.
The management of retrograde peri-implantitis: a case
report. J Clin Diagn Res 2012;6(9):16002.
19. Shabahang S, Bohsali K, Boyne PJ, Caplanis N, Lozada
J, Torabinejad M. Effect of teeth with periradicular
lesions on adjacent dental implants. Oral Surg Oral Med
Oral Pathol Oral Radiol Endod 2003;96:3216.
20. Steiner DR. The resolution of a periradicular lesion
involving an implant. J Endod 2008;34(3):3305.
21. McAllister BS, Masters D, Meffert RM. Treatment of
implants demonstrating periapical radiolucencies. Pract
Periodontics Aesthet Dent 1992;4:3741.
22. Chaffee NR, Lowden K, Tiffee JC, Cooper LF. Periapical
abscess formation and resolution adjacent to dental
implants: a clinical report. J Prosthet Dent 2001;85:
10912.
23. Brisman DL, Brisman AS, Moses MS. Case reports.
Implant failures associated with asymptomatic
endodontically treated teeth. J Am Dent Assoc
2001;132:1915.
24. Quirynen M, Gijbels F, Jacobs R. An infected jawbone
site compromising successful osseointegration. Periodontol 2000 2003;33:12944.
25. Bousdras V, Aghabeigi B, Hopper C, Sindet-Pedersen S.
Management of apical bone loss around a mandibular
implant: a case report. Int J Oral Maxillofac Implants
2006;21:43944.
26. Sussman HI. Periapical implant pathology. J Oral
Implantol 1998;24:1338.
207
You might also like
- Selection of Collagen Membranes For Bone RevisionDocument16 pagesSelection of Collagen Membranes For Bone Revisionmatias112No ratings yet
- PLA PGA and Its Copolymers in Alveolar Bone RegenerationDocument8 pagesPLA PGA and Its Copolymers in Alveolar Bone Regenerationmatias112No ratings yet
- Evaluation of Guided Bone Regeneration and or Bone Grafts in The Treatment of Ligature-Induced Peri-Implantitis DefectsDocument6 pagesEvaluation of Guided Bone Regeneration and or Bone Grafts in The Treatment of Ligature-Induced Peri-Implantitis Defectsmatias112No ratings yet
- Ameloblastoma in Maxilla-Case of ReportDocument6 pagesAmeloblastoma in Maxilla-Case of Reportmatias112No ratings yet
- Calvarial Bone Grafting For Three-Dimensi Reconstruction of Severe Maxillary Defects: A CDocument11 pagesCalvarial Bone Grafting For Three-Dimensi Reconstruction of Severe Maxillary Defects: A Cmatias112No ratings yet
- Content Server RDocument13 pagesContent Server Rmatias112No ratings yet
- An Alternative Alar Cinch Suture PDFDocument11 pagesAn Alternative Alar Cinch Suture PDFmatias112No ratings yet
- Fractures of Pelvis and Acetabulum 3rd EditionDocument847 pagesFractures of Pelvis and Acetabulum 3rd Editionmatias112100% (1)
- A Cost-Consequences Analysis of The Effect OfPregabalin in The Treatment of PeripheralNeuropathic Pain in Routine Medical Practice inDocument12 pagesA Cost-Consequences Analysis of The Effect OfPregabalin in The Treatment of PeripheralNeuropathic Pain in Routine Medical Practice inmatias112No ratings yet
- Incidence of Complications of Inferior Alveolar Nrve BlockDocument6 pagesIncidence of Complications of Inferior Alveolar Nrve Blockmatias112No ratings yet
- Shoe Dog: A Memoir by the Creator of NikeFrom EverandShoe Dog: A Memoir by the Creator of NikeRating: 4.5 out of 5 stars4.5/5 (537)
- The Yellow House: A Memoir (2019 National Book Award Winner)From EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Rating: 4 out of 5 stars4/5 (98)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeFrom EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeRating: 4 out of 5 stars4/5 (5794)
- The Little Book of Hygge: Danish Secrets to Happy LivingFrom EverandThe Little Book of Hygge: Danish Secrets to Happy LivingRating: 3.5 out of 5 stars3.5/5 (400)
- Grit: The Power of Passion and PerseveranceFrom EverandGrit: The Power of Passion and PerseveranceRating: 4 out of 5 stars4/5 (588)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureFrom EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureRating: 4.5 out of 5 stars4.5/5 (474)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryFrom EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryRating: 3.5 out of 5 stars3.5/5 (231)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceFrom EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceRating: 4 out of 5 stars4/5 (895)
- Team of Rivals: The Political Genius of Abraham LincolnFrom EverandTeam of Rivals: The Political Genius of Abraham LincolnRating: 4.5 out of 5 stars4.5/5 (234)
- Never Split the Difference: Negotiating As If Your Life Depended On ItFrom EverandNever Split the Difference: Negotiating As If Your Life Depended On ItRating: 4.5 out of 5 stars4.5/5 (838)
- The Emperor of All Maladies: A Biography of CancerFrom EverandThe Emperor of All Maladies: A Biography of CancerRating: 4.5 out of 5 stars4.5/5 (271)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaFrom EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaRating: 4.5 out of 5 stars4.5/5 (266)
- On Fire: The (Burning) Case for a Green New DealFrom EverandOn Fire: The (Burning) Case for a Green New DealRating: 4 out of 5 stars4/5 (74)
- The Unwinding: An Inner History of the New AmericaFrom EverandThe Unwinding: An Inner History of the New AmericaRating: 4 out of 5 stars4/5 (45)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersFrom EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersRating: 4.5 out of 5 stars4.5/5 (345)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyFrom EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyRating: 3.5 out of 5 stars3.5/5 (2259)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreFrom EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreRating: 4 out of 5 stars4/5 (1090)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)From EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Rating: 4.5 out of 5 stars4.5/5 (121)
- Her Body and Other Parties: StoriesFrom EverandHer Body and Other Parties: StoriesRating: 4 out of 5 stars4/5 (821)
- Compensated Dengue Shock Syndrome (A97.2) and Obesity (E.661)Document3 pagesCompensated Dengue Shock Syndrome (A97.2) and Obesity (E.661)NyomanGinaHennyKristiantiNo ratings yet
- Simple Solutions Protocols Prepared by Peggy ParkerDocument7 pagesSimple Solutions Protocols Prepared by Peggy ParkerRichard E. Hadi100% (2)
- UntitledDocument2 pagesUntitledsomaticayurvedaNo ratings yet
- Master Radiology Notes UrologyDocument106 pagesMaster Radiology Notes UrologySafwan ShaikhNo ratings yet
- Mercola: 60 Dangers of The Hepatitis B VaccineDocument5 pagesMercola: 60 Dangers of The Hepatitis B VaccineJonathan Robert Kraus (OutofMudProductions)No ratings yet
- Enfermedades de Tranms. AlimentariaDocument8 pagesEnfermedades de Tranms. AlimentariaAlejandra Dominguez RazoNo ratings yet
- 02 Biological Classification Ncert Master For Neet-UgDocument5 pages02 Biological Classification Ncert Master For Neet-UgRiya VermaNo ratings yet
- (3)Document20 pages(3)Muhammad Hadi ArwaniNo ratings yet
- Emcare IV Cannulation WorkbookDocument29 pagesEmcare IV Cannulation WorkbookAnca MartinoviciNo ratings yet
- JOHANNSON, Lisa - I Healed My Vulvodynea NaturallyDocument44 pagesJOHANNSON, Lisa - I Healed My Vulvodynea NaturallyMariana de Oliveira100% (1)
- Mycoviro MidtermsDocument14 pagesMycoviro MidtermsJoseline SorianoNo ratings yet
- Dermatology Treatment GuidelinesDocument33 pagesDermatology Treatment GuidelinesYoga YogaNo ratings yet
- HIV Case (Week 2) - Antao, Alvarez, Hasan, Sanaani, UsmanDocument15 pagesHIV Case (Week 2) - Antao, Alvarez, Hasan, Sanaani, UsmanNUR-HATHI SANAANINo ratings yet
- IPC Policy 4 PDFDocument128 pagesIPC Policy 4 PDFgary ann jimenez100% (1)
- Subject PredicateDocument69 pagesSubject PredicateyuldaNo ratings yet
- Pelvic Inflammatory Disease: Dr. Indah Meyliza, M. KesDocument13 pagesPelvic Inflammatory Disease: Dr. Indah Meyliza, M. KesIndah MeylizaNo ratings yet
- DR L M KhanDocument9 pagesDR L M KhanHomoeopath Aamir Saleem100% (4)
- NarcolepsyDocument36 pagesNarcolepsyridemypony22No ratings yet
- Causes and Risk Factors of Stis: Sexually Transmitted Diseases GuideDocument12 pagesCauses and Risk Factors of Stis: Sexually Transmitted Diseases GuideCabiomilaNo ratings yet
- Third Molar Surgery and Associated ComplicationsDocument10 pagesThird Molar Surgery and Associated ComplicationsBasil JacobNo ratings yet
- Q - COVID-19 Ag - IFU - EN ES (A2) - 20200308 (1) (Final) PDFDocument2 pagesQ - COVID-19 Ag - IFU - EN ES (A2) - 20200308 (1) (Final) PDFRoja AhmadNo ratings yet
- BMBL-5th EditionDocument421 pagesBMBL-5th EditionBryan OngNo ratings yet
- Post Dural Puncture HeadacheDocument3 pagesPost Dural Puncture HeadachecignalNo ratings yet
- The Antibacterial Activity of Leaf Extracts of Ocimum Gratissimum and Sida AcutaDocument6 pagesThe Antibacterial Activity of Leaf Extracts of Ocimum Gratissimum and Sida AcutaInternational Organization of Scientific Research (IOSR)No ratings yet
- Deoxyribo Virus and RibovirusDocument5 pagesDeoxyribo Virus and RibovirusAlyssa MercadoNo ratings yet
- ManuscriptDocument13 pagesManuscriptMegbaruNo ratings yet
- Mls 044: Clinical Bacteriology Session 9: Antimicrobial Agents - Mechanisms of Action and ResistanceDocument5 pagesMls 044: Clinical Bacteriology Session 9: Antimicrobial Agents - Mechanisms of Action and ResistanceJJ AngNo ratings yet
- LEPTOSPIROSIS Power Point PresDocument22 pagesLEPTOSPIROSIS Power Point PresAlex Guevarra100% (1)
- 7 Etiology of Periodontal DiseaseDocument37 pages7 Etiology of Periodontal Diseaseceudmd3dNo ratings yet
- Infection & Specific Wound InfectionsDocument39 pagesInfection & Specific Wound InfectionsAhmed ShorshNo ratings yet