Professional Documents
Culture Documents
Thyroid Drugs
Uploaded by
John Kenneth LealOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Thyroid Drugs
Uploaded by
John Kenneth LealCopyright:
Available Formats
PHARMACOLOGY: THYROID DRUGS BY DR.
FIRMALINO
THYROID DRUGS
3. cardiovascular effect - tachycardia with increase force of heart
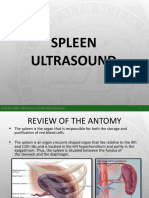
Thyroid Gland
contraction and increased cardiac output due to increase in number
Anatomy
of myocardial beta adrenergic receptors
a ductless endocrine gland
4. metabolic effect - increased metabolism of cholesterol and bile
located in anterior neck over the trachea below the thyroid
acids increased lipolysis, increased ultilization of carbohydrates
cartilage
5. Inhibition of secretion of TSH by the pituitary - Thru negative
weight = 15-20 grams
feedback to pituitary by decreased secretion of TSH
Physiology
thyroid hormones = essentiaI for growth and development
Relation of iodine to thyroid functions
regulation of energy metabolism
Iodine is necessary for thyroid hormone synthesis
If iodine intake is decreased
Synthesis of thyroid hormone
hormone production is decreased (hypothyroid state)
dependent on dietary iodine (from food, drugs, water)
TSH is increased (negative feedback from pituitary)
o
rec.
daily req. = 150-200 ug
thyroid gland hypertrophies (endemic goiter)
vascularity increased
Iodide concentrating mechanism increased
Major steps in thyroid hormone production
production of normal amount of hormone
1. Iodine trapping
2. Oxidation of iodine and Iodination of Tyrosine
3. Formation of T3 and T4 by coupling
Sources of iodine
4. Secretion
marine life sea fish / shells = as much as
200 -1000 ug/kg
5. Peripheral conversion of T4 to T3
whereas 5 kg of vegetables / fruits or 3 kg of meat or fresh water
fish provides only 100 ug iodine
1. Iodide trapping
to provide enough Iodine - other regions inject iodized oil
Is the active transport of iodide from circulation to colloid of
most practical = addition of iodide or iodate to table salt
thyroid gland
1 gram iodized salt = 100 ug iodine
iodide pump
stimulated by thyrotropin (TSH)
Clinical Diagnosis
inhibited by thiocyanate and perchlorate
1.
Hypothyroidism
autoregulated - decrease thyroid iodine will enhance uptake
2.
Hyperthyroidism
Hypothyroidism
2. Oxidation/lodination
deficiency in thyroid hormone due to iodine deficiency (endemic
Iodide is oxidized to iodine by thyroid peroxidase
goiter)
Followed by iodination of tyrosine in the thyroglobulin
congenital cretinism in children
Result =
absent or atrophic thyroid gland
o
mono iodo tyrosyl (MIT)
post thyroidectomy
o
diiodotyrosyl (DIT)
post radioactive Iodine therapy
This is blocked by PTU
myxedema when severe
3. Coupling reaction
Signs & symptoms of Hypothyroidism
Formation of T3 and T4
Cretinism, Short extremities, Mental retardation
MIT + DIT = T3 or Triiodothyronine
inactive, uncomplaining. expressionless, drowsy
DIT + DIT = T4 or Thyroxine
Puffy face, thickened lips, half open mouth, enlarged tongue
T3 is 3-5x more active than T4
Doughy, yellowish scaly skin, cool and dry to touch
Coarse, sparse, brittle hair, Thick, brittle nails
4. Secretion of thyroid hormone
Thick subcutaneous tissue, Low pitch, husky voice
T3 and T4 are synthesized and stored in the thyroglobulin
Cold intolerance, Cardiomegaly, decreased heart rate
Secretion is initiated by endocytosis of colloid from the follicular
lumen
Hyperthyroidism
The ingested thyroglobulin fuse with lysosomes containing the
resemble sympathetic hyperactivity even though epinephrine is
proteolytic enzyme resulting to release of thyroid hormone which
not elevated, Tachycardia, full pulse
then exit the cell by exocytosis
Palpitation, Lid lag/retraction, Tremor, excessive sweating,
activated by TSH by increasing activity of the lysosomal
anxiety, nervousness
enzymes
Heat intolerance, warm skin, Muscle weakness
Increased appetite, increased energy expenditure, weight loss,
5. Peripheral conversion T4 and T3
wasting
80% of T3 comes from conversion of T4 in peripheral tissues
Insomnia, restlessness, Increased bowel movement
5 deiodinase enzyme involved
this enzyme a lnhibited by PTU
2 forms
1. Diffuse toxic goiter (Grave dis.)
Transport of thyroid hormone in the blood
T3 and T4 = bound in Thyroxin binding globulin (TBG)
2. Nodular toxic goiter (Plummers dis)
Only 0.03% of total Thyroxine (T4) is free
Free T3 is 0.2-0.5%
T3 is less firmly bound
Diffuse toxic goiter (Grave dis.)
Only free form is active
Exopthalmos, Pretibial myxedema ( non pitting)
Pregnancy or estrogen administration causes increase TBG with
Young middle aged woman
increase binding, thus decrease in free form
Auto immune
Thyroid stimulating Ig G antibodies binds to TSH receptor &
Degradation and excretion
triggers increase in T4 & T3
T3 has a half life of 2 days or less
T4 half life 6-7 days
Nodular toxic goiter (Plummers dis)
in hyperthyroidism - decreased to 3-4 days
Older patients, 60 y/o above, female
in hypothyroidism - increased to 9-10 days
Arise from long standing non toxic nodular goiter
Degradation = liver
Excretion - kidney mainly, stool = 20 - 40%
TREATMENT
Actions of thyroid hormone
Thyroid Hormone
1. regulation of growth and development - increased protein
Synthethic
synthesis by controlling DNA transcription
Levothyroxine
2. calorigenic effect - increased basal metabolic rate by increasing
Liothyronine
oxygen consumption
Liotrix
PHARMACOLOGY: THYROID DRUGS BY DR. FIRMALINO
Both PTU & Methimazole can cross the placental barrier and
concentrate in fetal thyroid causing fetal hypothyroidism
But PTU is preferred for pregnant women since it is strongly
bound to protein carrier and therefore cross the placenta less
Levothyroxine
readily and is not secreted in breast milk in sufficient quantity.
Preparation of choice for replacement therapy for
hypothyroidism & suppression therapy
mechanism of action of thionamide
Characteristics Stabilily, Content uniformity, Low cost, Lack of
major action - prevents hormone synthesis by inhibiting the
allergenic foreign protein, Easy lab interpretation for monitoring
thyroid peroxidase
Long half life = 7 days
catalyzed reactions to block iodine organifications
allows once daily administration
blocks coupling or iodotyrosine
Preparation - Synthroid or Levothroid, Eltroxin (available locally
does not block iodide uptake by the gland
in the Phil), 50 or 100 ug/tab
PTU inhibits peripheral deiodination of T4 to T3 by inhibiting
deiodinase, but not Methimazole
Liothyronine
slow onset 3-4 weeks lapses before T4 is depleted
3-4X more active
short half life = 24 hours
Side effects
must be given in multiple daily doses
most common - maculopapular rash, fever
not ideal for routine replacement
Late vasculitis, hepatitis, arthralgia, lymphadenopathy, a
higher cost
lupus Iike reaction, polyserositis
difficult to monitor thru lab test
most dangerous (infrequent = 3-6%) - agranulocytosis more cardiotoxic
reversible if drug is stopped, sign = sore throat with high fever
best used as a diagnostic test in T3 suppression and short term
suppression of TSH
Anion Inhibitors
Preparation - Tertroxin , 20 ug/tab
blocks uptake of iodine by the gland thru competitive inhibition of
iodide transport
Liotrix
Agents
A mixture of levothyroxine and iodothyronine in a ratio of 4:1
1. Perchlorate - may produce aplastic anemia, mainly used as rocket
Preparation Euthyroid,
Thyrolar
fuel
2. Pertechnetate Technetium scan of thyroid
Natural Thyroid
3. Thiocyanate present in cabbage, brocolli, cauliflower considered
Fine powder from dessicated pig thyroid
as anticancer, but incidentally is also a goitrogen inhibiting thyroid
Preparation - Armour or Thyrar,
hormone causing goiter
1 grain (60 mg), or 325 mg/tab
Very toxic
used only for diagnostic purposes
Natural Thyroglobulin
Purified pig extract
Preparation - Proloid, 32.5 and 65 mg/tab
Thiocyanate in large amount may even block organification of iodine
Dose - 60-300 mg/day
this chemical is produced by enzymatic hydrolysis of certain plant
glycosides like cabbage
Antithyroid Agents
mainly used for hyperthyroidism
Iodides
4 categories
Inhibits organification (step 2)
1.Thionamides or Thiourylenes - interfere directly with thyroid
inhibits hormone release thru inhibition of thyroglobulin decreased
hormone synthesis
the size and vascularity of the gland (step 4)
2. Ionic inhibitors - block the iodide transport mechanism
Dose
3. Iodide - suppression of thyroid hormone synthesis when given in
>6 mg/day (or 6000 ug), daily req is only 150 to 200 ug
high doses
rapid improvement in thyrotoxic symptoms within 2-7 days
4. Radioactive iodine - damages and destroy the gland by ionizing
radiation
Iodides
disadvantages
Thionamides
increased lntraglandular stores of iodine which delay onset of
2 groups
thionamide therapy
1.Propylthioracil (PTU)
prevent use of radioactive iodine therapy for several weeks
2.Methimazole
should not be used alone because the gland will escape from the
iodide block in 2-8 weeks
withdrawals may produce severe exacerbation of thyrotoxicosis on
Propylthiouracil (PTU)
iodine enriched gland
rapidly absorbed
cross the placenta and cause fetal goiter
peak serum level after 1 hour
mostly excreted in the kidneys as the inactive glucoronide within
Toxicity of Iodides are reversible
24 hours
drug fever
Dosage - 100 mg every 6 hours will inhibit 60% of iodine
acneiform rash
organification for 7 hours
metallic taste
swollen salivary gland
Methimazole (Tapazole 5 mg/tab)
bleeding disorders
10x more active that PTU
mucous ulcer
completely absorbed and accumulated in the thyroid gland
anaphylaxis
slower excretion than PTU (65-70% is recovered in the urine in
conjunctivitis
48 hours)
rhinorrhea
Dosage - 15-30 mg exerts antithyroid effect for >24 hours
given single dose daily for mild to moderate hyperthyroidism
lodinated Contrast Media
for severe cases - increase dose to 60 mg/day
lpodate, lopanoic acid
may also be given in 3 divided doses every 8 hrs
Valuable in treatment of hyperthyroidism (through it is not
maintenance = 5-15 mg/day
approved by the FDA)
Pedia = 0.4 mg/kg/day w/ maintenance of 1/2 of initial dose
Rapidly inhibit the conversion of T4 and T3 in liver, kidney,
pituitary gland and brain (step s)
Carbimazole
Also inhibition of hormone release due to iodine release (step
NeoMercazole 5 mg/tab), mother drug, converted to methimazole in
4)
vivo
Relatively non-toxic - similar to iodide
15-60 mg/day initially
Useful adjunct to thyroid storm
maintenance = 15 mg/day
natural (animal origin - pigs)
desiccated thyroid
thyroglobulin
PHARMACOLOGY: THYROID DRUGS BY DR. FIRMALINO
important alternative if iodides and thionamides are
RAI
contraindicated
Advantages - easy administration, effectiveness, low expense,
May not interfere with 131 I retention as much as iodides
absence of pain
Disadvantag es - genetic damage, leukemia,
- neoplasia
Radioactive Iodine
restrict use only to patient 35 years old above
131 iodine is the only Isotope used for thyrotoxicosis
Contraindications
orally - in solution as Na 131 iodine
pregnancy - crosses the placenta,
rapidly absorbed
nursing mothers - goes out with milk
concentrated by thyroid and incorporated into storage follicles
Adrenoreceptor Blocking Agents
RAI
many signs and symptoms of thyrotoxicosis mimic those
therapeutic effect Is dependent on emission of Beta rays with
associated with sympathetic stimulation, thus agents that
an effective half life of 5 days and penetration range of 400deplete catecholamines(reserpineand guanithidine) or agents
2000 um.
like beta
Destruction or thyroid parenchyma follows within a few weeks.
evidence of thyroid destruction
blockers are useful because they impair tissue response at the
receptor site.
epithelial swelling and necrosis
Choice Propanolol
follicular disruption
end
edema
leukocytic infiltration
You might also like
- HP Color Laser Jet M477dw InventoryDocument1 pageHP Color Laser Jet M477dw InventoryJohn Kenneth LealNo ratings yet
- List of SuppliersDocument1 pageList of SuppliersJohn Kenneth LealNo ratings yet
- Scan To Network Folder Fujifilm Apeos C325Document1 pageScan To Network Folder Fujifilm Apeos C325John Kenneth LealNo ratings yet
- LiteratureDocument34 pagesLiteratureJohn Kenneth LealNo ratings yet
- Bureaucracy and The Public SectorDocument7 pagesBureaucracy and The Public SectorJohn Kenneth LealNo ratings yet
- Online Collaboration Tools (Updated)Document18 pagesOnline Collaboration Tools (Updated)John Kenneth LealNo ratings yet
- Certificate of EmploymentDocument1 pageCertificate of EmploymentJohn Kenneth LealNo ratings yet
- Event Order - A Rose For EmilyDocument3 pagesEvent Order - A Rose For EmilyJohn Kenneth LealNo ratings yet
- REVISED RPD QuestionnaireDocument3 pagesREVISED RPD QuestionnaireJohn Kenneth LealNo ratings yet
- Parent's Waiver OJTDocument1 pageParent's Waiver OJTapi-3846435100% (15)
- AuthorsDocument15 pagesAuthorsJohn Kenneth LealNo ratings yet
- A Dream Within A DreamDocument2 pagesA Dream Within A DreamAileen AblanNo ratings yet
- Minutes of The Meeting 11-27Document1 pageMinutes of The Meeting 11-27John Kenneth LealNo ratings yet
- Sculptures During Paleolithic EraDocument9 pagesSculptures During Paleolithic EraJohn Kenneth LealNo ratings yet
- Total Hours Accomplished For This WeekDocument1 pageTotal Hours Accomplished For This WeekJohn Kenneth LealNo ratings yet
- E-R Model (Microsoft Access)Document83 pagesE-R Model (Microsoft Access)John Kenneth LealNo ratings yet
- Parent's Waiver OJTDocument1 pageParent's Waiver OJTapi-3846435100% (15)
- Lesson 2 Intro To Network RevisedDocument48 pagesLesson 2 Intro To Network RevisedJohn Kenneth LealNo ratings yet
- DocumentationDocument20 pagesDocumentationJohn Kenneth LealNo ratings yet
- Wall Street 1987Document3 pagesWall Street 1987John Kenneth LealNo ratings yet
- Appendix A LogoDocument9 pagesAppendix A LogoJohn Kenneth LealNo ratings yet
- Table Relationships (Microsoft Access)Document26 pagesTable Relationships (Microsoft Access)John Kenneth LealNo ratings yet
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeFrom EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeRating: 4 out of 5 stars4/5 (5784)
- The Yellow House: A Memoir (2019 National Book Award Winner)From EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Rating: 4 out of 5 stars4/5 (98)
- Never Split the Difference: Negotiating As If Your Life Depended On ItFrom EverandNever Split the Difference: Negotiating As If Your Life Depended On ItRating: 4.5 out of 5 stars4.5/5 (838)
- Shoe Dog: A Memoir by the Creator of NikeFrom EverandShoe Dog: A Memoir by the Creator of NikeRating: 4.5 out of 5 stars4.5/5 (537)
- The Emperor of All Maladies: A Biography of CancerFrom EverandThe Emperor of All Maladies: A Biography of CancerRating: 4.5 out of 5 stars4.5/5 (271)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceFrom EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceRating: 4 out of 5 stars4/5 (890)
- The Little Book of Hygge: Danish Secrets to Happy LivingFrom EverandThe Little Book of Hygge: Danish Secrets to Happy LivingRating: 3.5 out of 5 stars3.5/5 (399)
- Team of Rivals: The Political Genius of Abraham LincolnFrom EverandTeam of Rivals: The Political Genius of Abraham LincolnRating: 4.5 out of 5 stars4.5/5 (234)
- Grit: The Power of Passion and PerseveranceFrom EverandGrit: The Power of Passion and PerseveranceRating: 4 out of 5 stars4/5 (587)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaFrom EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaRating: 4.5 out of 5 stars4.5/5 (265)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryFrom EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryRating: 3.5 out of 5 stars3.5/5 (231)
- On Fire: The (Burning) Case for a Green New DealFrom EverandOn Fire: The (Burning) Case for a Green New DealRating: 4 out of 5 stars4/5 (72)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureFrom EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureRating: 4.5 out of 5 stars4.5/5 (474)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersFrom EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersRating: 4.5 out of 5 stars4.5/5 (344)
- The Unwinding: An Inner History of the New AmericaFrom EverandThe Unwinding: An Inner History of the New AmericaRating: 4 out of 5 stars4/5 (45)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyFrom EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyRating: 3.5 out of 5 stars3.5/5 (2219)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreFrom EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreRating: 4 out of 5 stars4/5 (1090)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)From EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Rating: 4.5 out of 5 stars4.5/5 (119)
- Her Body and Other Parties: StoriesFrom EverandHer Body and Other Parties: StoriesRating: 4 out of 5 stars4/5 (821)
- Biology Ch17 - Notes - eDocument7 pagesBiology Ch17 - Notes - e陳詩淇No ratings yet
- Health Assessment (Midterm Lecture) DraftDocument8 pagesHealth Assessment (Midterm Lecture) DraftNikka Angela SalcedoNo ratings yet
- G.R. No.146891. July 30, 2002 Ruben T. Limbo, Petitioner, V. Employees Compensation Commission and Social SecurityDocument3 pagesG.R. No.146891. July 30, 2002 Ruben T. Limbo, Petitioner, V. Employees Compensation Commission and Social Securityfritzie abellaNo ratings yet
- Department of Education: Republic of The PhilippinesDocument5 pagesDepartment of Education: Republic of The PhilippinesMarc Joseph NillasNo ratings yet
- Ultrasound Spleen GuideDocument16 pagesUltrasound Spleen GuideJohn Andre RamosNo ratings yet
- APPROACH TO PANCREATIC NEUROENDOCRINE TUMORSDocument1 pageAPPROACH TO PANCREATIC NEUROENDOCRINE TUMORSRaina FujiyoshiNo ratings yet
- VPP Practical Manual Paper-IDocument135 pagesVPP Practical Manual Paper-I1kshitiz ThakurNo ratings yet
- Austin Journal of Nephrology and HypertensionDocument4 pagesAustin Journal of Nephrology and HypertensionAustin Publishing GroupNo ratings yet
- Science Test: Chapter I Respiratory and Circulatory System Term I, Semester IDocument4 pagesScience Test: Chapter I Respiratory and Circulatory System Term I, Semester IimandaNo ratings yet
- Gambaran Disfungsi Diastolik Pada Pasien 7414b2baDocument7 pagesGambaran Disfungsi Diastolik Pada Pasien 7414b2baAmelNo ratings yet
- Breast Complications in PuerperiumDocument24 pagesBreast Complications in Puerperiumvincentsharon100% (9)
- Radiation Oncology - Toxicity - RTOG - Wikibooks, Open Books For An Open WorldDocument15 pagesRadiation Oncology - Toxicity - RTOG - Wikibooks, Open Books For An Open WorldJosep GamarraNo ratings yet
- Digestive and Endocrine System: 5141 CN 111 - Anatomy and PhysiologyDocument4 pagesDigestive and Endocrine System: 5141 CN 111 - Anatomy and PhysiologyAlthea Joyce OngNo ratings yet
- BIOLOGY Form 5 Chapter 3Document62 pagesBIOLOGY Form 5 Chapter 3Lai Kee KongNo ratings yet
- Dissection Diagram The Concise FrogDocument1 pageDissection Diagram The Concise Frogapi-251077282No ratings yet
- Autonomic Nervous SystemDocument83 pagesAutonomic Nervous SystemChaudhry F MasoodNo ratings yet
- Histology NotesDocument4 pagesHistology NotesThonieroce Apryle Jey Morelos100% (2)
- Anatomy CoronaryDocument6 pagesAnatomy Coronarybri bugelNo ratings yet
- Circulatory SystemDocument30 pagesCirculatory SystemIra Lavigne De VillaNo ratings yet
- Anatomy and Physiology Lesson 2Document9 pagesAnatomy and Physiology Lesson 2Kimberly Abellar LatoNo ratings yet
- FRCEM ExamPrep GITDocument30 pagesFRCEM ExamPrep GITsk100% (1)
- SAL273Document18 pagesSAL273sumNo ratings yet
- Binondo - Activity 3 The IntegumentDocument26 pagesBinondo - Activity 3 The Integumentky knmtNo ratings yet
- Overview of Chronic Kidney Disease Complications and Indications for Starting DialysisDocument75 pagesOverview of Chronic Kidney Disease Complications and Indications for Starting DialysisIzka P RahmaniaNo ratings yet
- QirurgiaDocument132 pagesQirurgiadex menkesNo ratings yet
- Final Compre Exam Key AnswersDocument14 pagesFinal Compre Exam Key Answersmj CanilangNo ratings yet
- Thyroid Disease and Oral Health.Document6 pagesThyroid Disease and Oral Health.crookedgrange6384No ratings yet
- NCM 112 Pre Lim NotesDocument28 pagesNCM 112 Pre Lim NotesYancy TanNo ratings yet
- Netter Atlas of Human Neuroscience PDFDocument310 pagesNetter Atlas of Human Neuroscience PDFAndra Iordache67% (3)
- Case Study CholelithiasisDocument14 pagesCase Study Cholelithiasisb_faye20No ratings yet