Professional Documents
Culture Documents
AV Fistula CCF
Uploaded by
Drshah ShahOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
AV Fistula CCF
Uploaded by
Drshah ShahCopyright:
Available Formats
Hemodialysis International 2011; 15:104107
Case Report
High-output heart failure secondary to
arteriovenous fistula
Adam B. STERN, Philip J. KLEMMER
UNC Kidney Center, Division of Nephrology and Hypertension, Chapel Hill, NC, USA
Abstract
In the hemodialysis patient population, a surgically created arteriovenous stula is the preferred
vascular access option. Development of high-output heart failure may be an underappreciated complication in patients who have undergone this procedure. When a large proportion of arterial blood is
shunted from the left-sided circulation to the right-sided circulation via the stula, the increase in
preload can lead to increased cardiac output. Over time, the demands of an increased workload may
lead to cardiac hypertrophy and eventual heart failure. Patients may present with the usual signs of
high-output heart failure including tachycardia, elevated pulse pressure, hyperkinetic precordium,
and jugular venous distension. Typically, the AV stula is quite large and is likely located in the upper
arm, more proximal to the heart. Routine access ow monitoring should demonstrate blood ows
(Qa) 42000 ML/min. Echocardiogram may reveal either a low or high left ventricular ejection fraction, and right-heart catheterization demonstrates an elevated cardiac output with a low to normal
systemic vascular resistance. When addressing the problem of high-output heart failure, the
nephrologist is faced with the dilemma of preventing progression of heart failure at the expense
of loss of vascular access. Nevertheless, treatment should be directed at correcting the underlying
problem by surgical banding or ligation of the stula.
Key words: hemodialysis, arteriovenous stula, vascular access, heart failure
CASE PRESENTATION
A 38-year-old Hispanic female developed end-stage renal
disease (ESRD) due to idiopathic collapsing focal segmental glomerulosclerosis. The diagnosis was established
by kidney biopsy in 2007. In spite of immunosuppressive
therapy, she progressed rapidly to ESRD. In 10/08, a left
upper arm brachial-basilic vein transposition arteriovenous fistula was created. The fistula was accessed on
postoperative day 46 for the initiation of hemodialysis.
Additional medical problems included hypertension,
remote nephrolithiasis, and recent history of a positive
PPD. There was no history of diabetes. She did not use
Correspondence to: A. B. Stern, MD, UNC Kidney Center,
Division of Nephrology and Hypertension, CB 7155, Chapel
Hill, NC 27599-7155, USA.
Email: adam_stern@med.unc.edu
104
tobacco products, alcohol, or illicit drugs. There was no
family history of kidney or heart disease.
The patient tolerated hemodialysis for 312 hours thrice
weekly without complication for approximately 1 year. In
October 2009, she began to experience difficulty with
maintaining a consistent dry weight. At the end of treatments, she frequently became hypotensive and would
experience muscle cramping. When her dry weight was
increased to compensate for her symptoms, she developed shortness of breath, orthopnea, and paroxysmal
nocturnal dyspnea on her nondialysis days. There were
no changes in medications, dialysis prescription, or dietary salt intake. Her estimated dry weight was 58 kg with
an average interdialytic weight gain of 3.6 kg.
In her 13th month of dialysis, the patient experienced
heavy substernal chest pressure and shortness of breath.
On presentation to the emergency department, she was
noted to be hypertensive (164/102 mmHg) and tachycardic
r 2011 The Authors
Hemodialysis International r 2011 International Society for Hemodialysis
DOI:10.1111/j.1542-4758.2010.00518.x
High-output heart failure
(105 bpm). Hemoglobin saturation was 97% on ambient
air. Physical examination was significant for jugular
venous distension, bibasilar pulmonary rales, trace lower
extremity edema, and hyperkinetic precordium. Her
arteriovenous fistula was hypertrophied and extended
from the left elbow to the left axilla with a strong thrill
and bruit. Her hands were equally warm. The hemoglobin was 10.4 g/dL, troponin I level was 0.194 ng/ML
(0.00.034), which had risen from the normal range 1
week before admission. The CK-MB was 1.2 ng/ML (0.0
6.0). Pro-BNP was 99,400 pg/ML (0178). A PA and
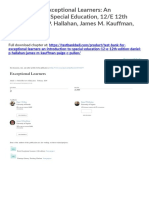
lateral chest X-ray revealed cardiomegaly with septal
thickening, peri-bronchial cuffing, bilateral pleural effusions, and Kerley B lines, all suggestive of pulmonary
edema (see Figure 1). Her chest pain was relieved with
intravenous morphine. Intravenous heparin, a b-blocker,
aspirin, and a statin were initiated. The patient was
admitted for presumed acute coronary syndrome.
On the day following admission, a transthoracic echocardiogram was notable for moderate left ventricular dilation with an estimated left ventricular ejection fraction
of 35%. It also suggested severe pulmonary hypertension
with elevations in both right atrial and central venous
pressures. There was normal right ventricular contractile
performance. The patients symptoms improved with intravenous furosemide and hemodialysis.
Figure 1 PA chest X-ray at the time of presentation demonstrating cardiomegaly, peri-bronchial cuffing, bilateral pleural
effusions, and Kerley B lines.
Hemodialysis International 2011; 15:104107
On hospital day #2, the patient underwent left and
right heart catheterization. Left heart catheterization did
not reveal significant obstructive coronary artery disease.
Right heart catheterization showed high cardiac output
(fick 9.92 L/min, thermodilution 10.87 L/min) and lownormal systemic vascular resistance (830.6 dyne sec cm).
There was evidence of pulmonary hypertension (45/
22 mmHg) with normal pulmonary vascular resistance
(1.92 Wood units).
The patient was referred to a surgeon for fistula banding. A 6 mm Goretex graft was interposed in the proximal
portion of the fistula, effectively increasing resistance and
decreasing blood flow. The fistula remained patent following this procedure. Despite this intervention, the patients symptoms did not improve over the following
month. She was referred back to the surgeon for a ligation procedure. Postligation, her symptoms improved. An
echocardiogram performed 1 week after ligation continued to demonstrate severe left ventricular dysfunction
with an ejection fraction of 2025%. At 6 months, the
echocardiogram showed a modest improvement in left
ventricular function with an estimated ejection fraction of
4550%. The patient remained asymptomatic.
DISCUSSION
Surgical creation of an arteriovenous fistula has been advocated as the preferred vascular access among patients
with ESRD.1,2 This approach has been used effectively
since the 1960s.3An association between arteriovenous
fistulas used for hemodialysis and the development of
high-output heart failure was first reported in the early
1970s.4,5 The incidence of high-output heart failure in
this group of patients, however, has not been well defined. Heart failure itself is a well-recognized comorbidity
among dialysis patients, and half of all deaths in the dialysis population are attributable to cardiovascular disease.6 In one series of 299 incident hemodialysis patients
with normal left ventricular ejection fractions, 25% subsequently developed congestive heart failure over a period of 41 months.7 The contribution of a high-output AV
shunt to this morbidity is not clear.
The normal range cardiac index in the adult is 2.5
4.2 L/min/m2. Patients with cardiac indices below this
range have systolic dysfunction. When the cardiac index
is above this range, a patient may develop high-output
heart failure as a consequence of supraphysiologic cardiac
output. Specifically, after the creation of an arteriovenous
fistula, blood is shunted from the high-pressure arterial
side to the low-pressure venous side. This diversion of
blood back to the right-sided circulation reduces overall
105
Stern and Klemmer
systemic arterial blood flow. The counterregulatory
response is an increase in cardiac output mediated
by the sympathetic nervous system and circulating
catecholamines. Initially, the heart increases cardiac output via an increase in heart rate and stroke volume. With
time, excess cardiac stimulation leads to left ventricular hypertrophy, reduction in LVEF, and eventual heart
failure.8
Several data requirements are needed in order to diagnose high-output heart failure secondary to an AV fistula.
First and foremost is the index of suspicion on the part of
the clinician. Despite their physiologic differences, the
signs and symptoms of low-output and high-output heart
failure are quite similar. Dyspnea on exertion, fatigue, and
fluid retention are the hallmarks of both. On physical
exam, the clinician may note tachycardia, jugular venous
distention, basilar rales, pleural effusions, and peripheral
edema. Notable differences in the physical exam may
be the presence of a hyperkinetic precordium and
wide pulse pressure in the high output state. Because of
the increase in venous return to the right atrium, a rightsided S3 gallop may be noted on inspiration. Access
should be hypertrophied, located in the upper arm, with
high (>2000 ML/min) access flow rates. Some patients
may have signs or symptoms of vascular steal syndrome
in the hand of the access side. The early development of
steal symptoms in the hand may actually lead to early
surgical intervention, thereby preventing incipient highoutput heart failure.
When heart failure is suspected, a standard transthoracic echocardiogram should document left ventricular
function. Contractility may vary from being supraphysiologic initially to being decreased over the course of time.
Left ventricular dilation occurs to maintain adequate
stoke volume in the face of low ejection fraction. Pulmonary hypertension always occurs as a consequence
of excess central blood volume and high preload hemodynamics. In addition, because of volume expansion in
the central circulation, serum levels of ANP and BNP may
rise dramatically. Definitive proof a high-output state requires right heart catheterization. High cardiac output,
low-normal systemic vascular resistance, and pulmonary
hypertension with normal pulmonary vascular resistance
are characteristic findings.
Once that the diagnosis of heart failure has been made,
the clinician must prove that it is a consequence of increased blood flow through the fistula. Other causes of
high-output heart failure (see Table 1) need to be excluded. Hemodialysis access flow (Qa) can be determined
routinely by the noninvasive ultrasound dilution technique. In general, the Qa is greater in an upper arm access
106
(0.81.9 L/min) versus a lower arm access (0.451.3 L/
min).9 Therefore, it is not surprising that the incidence of
high-output heart failure seems to be more common in
patients with upper arm accesses, specifically with Qa
42.0 L/min.10 One proposed method of determining the
contribution of the hemodialysis access to the overall cardiac output is to measure the ratio of access flow to cardiac output (Qa:CO). Although unproven in prospective
trials, a Qa:CO 40.3 may be a risk factor for the development of high-output heart failure.9 Alternatively, the
NicoladoniBranham sign can be elicited by brief manual
compression of the AV fistula.11 The response to this diagnostic maneuver is an immediate decrease in pulse rate
and an increase in blood pressure, which occur as a result
of the sudden restoration of normal blood flow to the
systemic circulation coincident with the occlusion of the
AV fistula. Although not originally described, the widened pulse pressure may narrow with fistula occlusion.
This maneuver maybe performed at the bedside or during
heart catheterization or echocardiogram.
High-output heart failure presents a difficult treatment
dilemma to the nephrologist. Ideally, one would prefer to
treat the symptoms and prevent progression of heart failure while simultaneously preserving adequate vascular
access. Because these two goals are often not always mutually compatible, the fistula may need to be surgically
ligated, resulting in the loss of access.12 Alternatively,
banding techniques may be used to constrict the fistula in
one or more places, thus partially reducing the Qa. While
these techniques were originally developed to treat ischemic steal syndrome, they may prove effective in the
management of high-output heart failure. Banding is accomplished by surgical positioning of a circumferential
polytetrafluroethylne band adjacent to the arterial
anastomosis, which reduces blood inflow.13 Alternatively,
hemoclips may be applied downstream to the venous
supply to further increase resistance. Another technique,
described as an inflow reduction procedure, is performed
in upper arm fistulas by ligating the brachial artery anastomosis and attaching a synthetic graft from the cephalic
vein to the smaller diameter distal radial artery.14 The
recently described MILLER procedure, which uses an
Table 1 Etiology of high-output heart failure
AV fistula (congenital or acquired)
Anemia
Thyrotoxicosis
Cirrhosis
Beriberi
Pregnancy
Hemodialysis International 2011; 15:104107
High-output heart failure
endovascular balloon to serve as a guide for band placement, is an effective therapy for the steal syndrome that
can be performed in an outpatient interventional radiology suite.15 This method could prove useful for the treatment of high-output heart failure as well.
Over one half of annual deaths among dialysis patients
occur as a consequence of cardiovascular disease. The
high burden of morbidity and mortality in these patients
cannot be fully explained by traditional Framingham risk
factors. As such, fistula-related high-output heart failure
may represent an under diagnosed reason for potentially
reversible heart failure in hemodialysis patients. A high
index of suspicion on the part of the nephrologist and
dialysis staff is critical for successful diagnosis and treatment of this disorder.
Manuscript received November 2010; revised November
2010.
REFERENCES
1 Polkinghorne K.R. Vascular access and all-cause mortality: A propensity score analysis. J Am Soc Nephrol. 2004;
15:477486.
2 Dhingra RK, Young EW, Hulbert-Shearon TE, Leavey SF,
Port F. Type of vascular access and mortality in US hemodialysis patients. Kidney Int. 2001; 60:14431451.
3 Brescia MJ, Cimino JE, Appel K, Hurwich BJ. Chronic
hemodialysis using venipuncture and a surgically created
arteriovenous fistula. N Engl J Med. 1966; 275:1089
1092.
4 Ahearn DJ, Maher JF. Heart failure as a complication of
hemodialysis arteriovenous fistula. Ann Intern Med. 1972;
77:201204.
5 George CR, May J, Schieb M, Benson RE, Evans RA.
Heart failure due to an arteriovenous fistula for haemodialysis. Med J Aust. 1973; 1:696698.
Hemodialysis International 2011; 15:104107
6 US Renal Data System (USRDS). Annual Data Report. Volume 2, ESRD, Ch 6. Bethesda, MD: National Institutes of
Health; 2009, p. 277.
7 Harnett JD, Foley RN, Kent GM, Barre PE, Murray D,
Parfrey PS. Congestive heart failure in dialysis patients:
Prevalence, incidence, prognosis and risk factors. Kidney
Int. 1995; 47:884890.
8 MacRae JM, Pandeya S, Humen DP, Krivitski N, Lindsay
RM. Arteriovenous fistula-associated high-output cardiac
failure: A review of mechanisms. Am Jf Kid Dis. 2004;
43:e1722.
9 Winjen E, Keuter XH, Planken NR, et al. The relationship
between access flow and different types of vascular access with systemic hemodynamics in hemodialysis patients. Artif Organs. 2005; 29:960964.
10 Basile C, Lomonte C, Vernaglione L, Casucci F,
Antonelli M, Losurdo N. The relationship between the
flow of arteriovenous fistula and cardiac output in haemodialysis patients. Nephrol Dial Transplant. 2008;
23:282287.
11 Reis GJ, Hirsh AT, Come PC. Detection and treatment of
high-output cardiac failure resulting from a large hemodialysis fistula. Catheterization Cardiovasc Diagn. 14:263
265.
12 Young PR Jr, Rohr MS, Marterre WF Jr. High-output cardiac failure secondary to a brachiocephalic arteriovenous
hemodialysis fistula: Two cases. Am Surg. 1998; 64:239
241.
13 Suding PN, Wilson SE. Strategies for management of ischemic steal syndrome. Semin Vasc Surg. 2007; 20:184
188.
14 Chelma ES, Morsey M, Anderson L, Whitemore A. Inflow reduction by distalization of anastomosis treats efficiently high-inflow high-cardiac output vascular access
for hemodialysis. Semin Dial. 20:6872.
15 Goel N, et al. Minimally invasive limited ligation endoluminal-assisted revision (miller) for treatment of dialysis access-associated steal syndrome. Kid Int. (2006);
70:765770.
107
You might also like
- 364 FullDocument12 pages364 FullDesi HutapeaNo ratings yet
- Pediatrics 1997 Seikaly 879 84 PDFDocument8 pagesPediatrics 1997 Seikaly 879 84 PDFDrshah ShahNo ratings yet
- PHEX Analysis in 118 Pedigrees Reveals New Genetic CluesDocument11 pagesPHEX Analysis in 118 Pedigrees Reveals New Genetic CluesDrshah ShahNo ratings yet
- Transient Enalparil PLOS OneDocument11 pagesTransient Enalparil PLOS OneDrshah ShahNo ratings yet
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeFrom EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeRating: 4 out of 5 stars4/5 (5794)
- The Little Book of Hygge: Danish Secrets to Happy LivingFrom EverandThe Little Book of Hygge: Danish Secrets to Happy LivingRating: 3.5 out of 5 stars3.5/5 (400)
- Shoe Dog: A Memoir by the Creator of NikeFrom EverandShoe Dog: A Memoir by the Creator of NikeRating: 4.5 out of 5 stars4.5/5 (537)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceFrom EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceRating: 4 out of 5 stars4/5 (895)
- The Yellow House: A Memoir (2019 National Book Award Winner)From EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Rating: 4 out of 5 stars4/5 (98)
- The Emperor of All Maladies: A Biography of CancerFrom EverandThe Emperor of All Maladies: A Biography of CancerRating: 4.5 out of 5 stars4.5/5 (271)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryFrom EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryRating: 3.5 out of 5 stars3.5/5 (231)
- Never Split the Difference: Negotiating As If Your Life Depended On ItFrom EverandNever Split the Difference: Negotiating As If Your Life Depended On ItRating: 4.5 out of 5 stars4.5/5 (838)
- Grit: The Power of Passion and PerseveranceFrom EverandGrit: The Power of Passion and PerseveranceRating: 4 out of 5 stars4/5 (588)
- On Fire: The (Burning) Case for a Green New DealFrom EverandOn Fire: The (Burning) Case for a Green New DealRating: 4 out of 5 stars4/5 (74)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureFrom EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureRating: 4.5 out of 5 stars4.5/5 (474)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaFrom EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaRating: 4.5 out of 5 stars4.5/5 (266)
- The Unwinding: An Inner History of the New AmericaFrom EverandThe Unwinding: An Inner History of the New AmericaRating: 4 out of 5 stars4/5 (45)
- Team of Rivals: The Political Genius of Abraham LincolnFrom EverandTeam of Rivals: The Political Genius of Abraham LincolnRating: 4.5 out of 5 stars4.5/5 (234)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyFrom EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyRating: 3.5 out of 5 stars3.5/5 (2259)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreFrom EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreRating: 4 out of 5 stars4/5 (1090)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersFrom EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersRating: 4.5 out of 5 stars4.5/5 (344)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)From EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Rating: 4.5 out of 5 stars4.5/5 (121)
- Her Body and Other Parties: StoriesFrom EverandHer Body and Other Parties: StoriesRating: 4 out of 5 stars4/5 (821)
- Chapter VIII Drug StudyDocument21 pagesChapter VIII Drug StudyDylan Angelo AndresNo ratings yet
- Essay - Child DevelopmentDocument2 pagesEssay - Child DevelopmentTina AroraNo ratings yet
- Immune System ProjectDocument21 pagesImmune System ProjectAvinash BobadeNo ratings yet
- Case 4-2021: A 70-Year-Old Woman With Dyspnea On Exertion and Abnormal Findings On Chest ImagingDocument12 pagesCase 4-2021: A 70-Year-Old Woman With Dyspnea On Exertion and Abnormal Findings On Chest ImagingBruno ConteNo ratings yet
- TNBDocument21 pagesTNBAhmad FauziNo ratings yet
- Gordon's Functional Health PatternsDocument2 pagesGordon's Functional Health PatternsKara GloriaNo ratings yet
- Kenny's Boards 2 ReviewsDocument254 pagesKenny's Boards 2 ReviewsHuguette Marie NseleNo ratings yet
- Detailed Lesson Plan BPPDocument8 pagesDetailed Lesson Plan BPPDa Real SoroteNo ratings yet
- Endocrine SystemDocument10 pagesEndocrine SystemPeej Reyes100% (1)
- The Zombie FilesDocument6 pagesThe Zombie FilesVincent TomasinoNo ratings yet
- 11 Acute SinusitisDocument41 pages11 Acute SinusitisAshwin ParchaniNo ratings yet
- Pubmed 1 & Ovid 2Document7 pagesPubmed 1 & Ovid 2Adam PrabataNo ratings yet
- OsteomyelitisDocument29 pagesOsteomyelitisAishath Samha HussainNo ratings yet
- 2011 SLE 1st BankDocument222 pages2011 SLE 1st BankEmad Hajali100% (1)
- Ebook Essentials of Psychiatry in Primary Care Behavioral Health in The Medical Setting PDF Full Chapter PDFDocument67 pagesEbook Essentials of Psychiatry in Primary Care Behavioral Health in The Medical Setting PDF Full Chapter PDFcharles.johnson573100% (27)
- 4 641377LHDocument12 pages4 641377LHGuna SoundariNo ratings yet
- Introduction PeDocument25 pagesIntroduction PeRodelJohnMarmolNo ratings yet
- Return To Work FormDocument1 pageReturn To Work Formair2212No ratings yet
- Opportunistic MycosesDocument6 pagesOpportunistic MycosesJullana Rondina EscondeNo ratings yet
- Healing WonderDocument31 pagesHealing WonderRussiel DagohoyNo ratings yet
- NV L2K Forms-10-9-17Document3 pagesNV L2K Forms-10-9-17LeaNo ratings yet
- Novilyn C. Pataray BSN - Ii Pharyngitis: St. Paul College of Ilocos SurDocument1 pageNovilyn C. Pataray BSN - Ii Pharyngitis: St. Paul College of Ilocos SurCharina AubreyNo ratings yet
- Unit 6Document5 pagesUnit 6Bình HồNo ratings yet
- Polya Urn ModelDocument2 pagesPolya Urn ModelParmenNo ratings yet
- Example of Nursing Care Plan (Pathophysiology)Document5 pagesExample of Nursing Care Plan (Pathophysiology)Elizabeth ZamoraNo ratings yet
- Acute AbdomenDocument14 pagesAcute AbdomenSaha DirllahNo ratings yet
- Test Bank For Exceptional Learners An Introduction To Special Education 12 e 12th Edition Daniel P Hallahan James M Kauffman Paige C PullenDocument31 pagesTest Bank For Exceptional Learners An Introduction To Special Education 12 e 12th Edition Daniel P Hallahan James M Kauffman Paige C PullenPeter Fleming100% (30)
- Fever of Unknown Origin Most Frequent Causes in AdDocument6 pagesFever of Unknown Origin Most Frequent Causes in AdDanteNo ratings yet
- Herbal Medicine Natural Remedies 150 Herbal Remedies To Heal Common Ailments (PDFDrive)Document296 pagesHerbal Medicine Natural Remedies 150 Herbal Remedies To Heal Common Ailments (PDFDrive)Fathi Adan100% (19)
- Rating The Risk Factors For Breast Cancer: ReviewDocument9 pagesRating The Risk Factors For Breast Cancer: ReviewPratamasari InsaniNo ratings yet