Professional Documents
Culture Documents
Bazo Errante 2016 REVISED Ijtra1601084
Uploaded by
luisalfredo_montesCopyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Bazo Errante 2016 REVISED Ijtra1601084
Uploaded by
luisalfredo_montesCopyright:
Available Formats
International Journal of Technical Research and Applications e-ISSN: 2320-8163,
www.ijtra.com Volume 4, Issue 1 (January-February, 2016), PP. 120-123
WANDERING SPLEEN - A CASE REPORT
MOHD MUBARIK NAQASH 1, ARIF NABI BHAT 2, SAJAD AHMAD SALATI3, SHAMS-UL-BARI4
1
ASSOCIATE PROF , 2SENIOR RESIDENT INTERNAL MEDICINE, 3ASSISTANT PROF SURGERY,
4
ASSISTANT PROF GENERAL SURGERY
1
INTERNAL MEDICINE, SKIMS MEDICAL COLLEGE BEMINA
2
SKIMS MEDICAL COLLEGE BEMINA
3
UNAIZAH COLLEGE OF MEDICINE, QASSIM UNIVERSITY, KSA
4
SKIMS MEDICAL COLLEGE BEMINA.
1,2,4
SRINAGAR, J&K, INDIA
1
mubarikn@rediffmail.com
Abstract: Wandering spleen is a rare clinical entity in
which the spleen is attached by a long vascular pedicle and
can be found in any part of the abdomen or pelvis. It can
be complicated by torsion leading to a surgical abdominal
emergency. A case of a patient with wandering spleen is
reported here that presented with chronic abdominal pain.
Keywords: Wandering Spleen, Pedicle, Torsion, Abdominal
Pain.
I. INTRODUCTION
The spleen develops from the mesoderm in the dorsal
mesogastrium. It lies in the left hypochondrium behind the
stomach, and is approximately 12 cm long and 7 cm wide1.
The spleen is fixed in position by the lieno-renal and
gastrosplenic ligaments; the phrenico-colic ligament provides
additional support. The ligaments are embryological
condensations that take place in the peritoneum, and
congenital peritoneal anomalies may result in splenic
displacement.
Wandering spleen, also known as displaced, ectopic, drifting,
floating spleen or splenoptosis is a rare condition defined as a
huge, single spleen in an abdominal position rather than its
anatomical site, owing to laxity of its pedicles and absence of
ligamentous attachments 2. The spleen can be found in any part
of the abdomen or pelvis because of the length of its pedicle.
The abnormally fixed spleen can twist on its vascular pedicle,
creating ischemia that may progress to infarction if not
promptly treated 3.
Clinical presentation of wandering spleen is varied and the
diagnosis is often elusive. The presence of a wandering spleen
can give rise to symptoms similar to those of other common
abdominal diseases like intermittent abdominal pain of
varying severity, acute abdomen secondary to haemorrhagic
splenic infarction due to torsion of the vascular pedicle, the
presence of a palpable mass that can be located anywhere
from the left hypochondrium to the pelvis 2.. Early
preoperative diagnosis is difficult without radiological aids.
Laboratory tests can support the diagnosis by revealing
thrombocytopenia (secondary to congestive hypersplenism),
increased creatine phosphokinase (CPK) and leucocytosis.
The usual treatment is fixation of the spleen (splenopexy),
except in cases of infarction where there is no evidence of
blood flow to the spleen after detorsion. In such cases
splenectomy should be considered.
We report a case of wandering spleen in a 45 years old male
that presented with chronic abdominal pain. This is the first
case of its kind reported from the Kashmir valley.
II. CASE REPORT
A 45 year old multiparous female, with no underlying
co-morbidity got admitted in the department of internal
medicine of our hospital for the evaluation of abdominal
fullness and pain for the last few years. The pain was describe
as intermittent, self-relieving, dragging in nature, in the left
hypochondrium and generally between 4-6/10 on Visual
Analogue Pain Scale. This was associated with early
postprandial fullness and occasional nausea. The patient used
to take over the counter antacids, antispasmodics, protein
pump inhibitors but without any permanent relief of her
symptoms. The patient was referred by a local medical
practitioner to our hospital for full evaluation and treatment.
On general physical examination, she was of normal body
built, afebrile and had stable vital signs. Abdominal
examination revealed a mobile mildly tender mass, spanning
over the left lumbar area, left iliac fossa and the hypogastrium.
Rest of the general and the systematic examination revealed
no apparent abnormality. On investigation, hemogram
revealed haemoglobin of 10gms/dl, total leukocyte count of
3790/dl (with a differential of 66.3% polymorphs, 26.9%
lymphocytes, 5.5% monocytes) and platelet count of
70,000/cc. Coagulation profile and the bio-chemical
investigations were within normal limits.
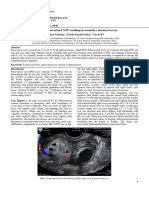
Ultrasonography (USG) of the abdomen with a curve linear
transducer (5MHz) showed that the spleen was not in its usual
site, and was located in the left lumbar region extending to left
iliac fossa measuring about 19.3 cm in size. Spleen appeared
to change position on changing the position of patient during
the scan. Splenic vein was 8mm. No features of chronic liver
disease were seen as also rest of the structures were also
normal and the diagnosis of wandering spleen was made
(Figure-1). Contrast Enhanced Helical Computed Tomography
120 | P a g e
International Journal of Technical Research and Applications e-ISSN: 2320-8163,
www.ijtra.com Volume 4, Issue 1 (January-February, 2016), PP. 120-123
(CECT) of abdomen showed spleen enlarged in size
measuring about 19.3cm and located in ectopic location
extending from the left lumbar region to the hypogastrium
with no detectable splenenculi. The diagnosis of wandering
spleen was hence confirmed (Figure-2). Splenectomy was
planned in view of the features of hypersplenism. Informed
consent was secured and anti-Pneumococcal, Hemophilus
Influenza-B and anti-meningococcal vaccines were
administered in the pre-operative phase. Open splenectomy
after gaining access into abdomen through a lower transverse
abdominal incision. She had an uncomplicated postoperative
period and was discharged with an advice of regular follow
up. Histological examination of the splenic specimen revealed
normal splenic tissue.
III. DISCUSSION
Wandering spleen is a rare entity and reported in both the
genders and only about 500 cases have been reported in
literature till date 4. Van Horne, a Dutch physician, is credited
in literature with describing this condition in 1667 after
performing an autopsy. In 1875, Martin, a German
obstetrician was first to perform the first splenectomy for a
wandering spleen 5.
The usual occurrence is at 20 to 40 years of age and is more
frequent in women of reproductive age group 4. The incidence,
based on several large series of splenectomies, is less than
0.5%. Wandering spleen is most often as a result of congenital
anomaly in the of development of dorsal mesogastrium, but
acquired factors may have a role in certain instances.
Congenital form occurs due to failure of the development of
dorsal mesogastrium, when the lesser sac is formed. However,
the acquired anomalies have been described and are attributed
to laxity of the ligaments due to weakness of the abdominal
wall, multiple pregnancies, hormonal changes, or increase in
the size of the spleen. The acquired form mostly occurs in
multiparous females as the ligaments which are holding the
spleen in its position become lax and such spleens are usually
enlarged. The spleen in our patient was palpated as a
significantly enlarged, mobile, mildly tender and ectopically
located lump spanning over left lumbar quadrant, left iliac
fossa and hypogastrium.
The condition in adults may be most detected incidentally as
an asymptomatic lump or in imaging studies undertaken for a
different indication or the patient may report with chronic
gastrointestinal complaints or with an acute abdominal
emergency 5. Complications related to torsion or compression
of abdominal organs by the spleen or the pedicles are reported
in literature. The most common presentation in children is an
acute surgical abdomen occurring due to infarction from
torsion of the splenic pedicle. The triad of a firm ovoid mass
with a notched edge, tender movements of the mass except
when the mass is moved toward the left upper quadrant and
resonance to percussion in the left upper quadrant has been
described to point towards the diagnosis of a wandering
spleen. Ben Aly A et al have reported one instance of familial
wandering spleen where two sisters presenting with acute
torsion of a spleen within a 3-year interval 6.
Haematological and biochemical investigations may be nonspecific. Laboratory tests may reveal elevated inflammatory
markers and evidence of hypersplenism or functional asplenia
.Splenomegaly is usually a result of torsion of the pedicle and
splenic sequestration. Complications of wandering spleen
include infarction, gangrene, splenic abscess, variceal
haemorrhage, colonic volvulus, gut obstruction and pancreatic
necrosis 7-8.
The diagnosis can be confirmed by imaging studies including
Duplex USG, nuclear scintigraphy, computed tomography and
magnetic resonance imaging. Doppler sonographic helps in
evaluation of organ blood flow. CT findings of wandering
spleen include absence of spleen in the left upper quadrant and
a soft tissue mass resembling spleen elsewhere in the
abdomen. Radio-isotopic scanning (technetium 99 sulfur
colloid scan) allows the assessment of location as well as the
functioning of spleen.
Arteriography allows definitive
evaluation of the splenic vasculature and features of left-sided
portal hypertension 5.
If significant torsion of the splenic pedicle occurs, the torted
pedicle may mimic bowel intussusceptions in appearance. The
most specific sign of splenic torsion is a "whirl-like" (or
'whorled') appearance of splenic vessels and surrounding fat
usually noted at the splenic hilum 9.
Definitive treatment for wandering spleen is surgical, since
conservative/ non-operative treatment has been found to be
associated with a complication rate as high as 65% 5.
Splenopexy is the treatment of choice for a non-infarcted
wandering-spleen. Splenectomy is ideally reserved for patients
presenting with acute abdomen and splenic infarction or
thrombosis or with hypersplenism and patients in whom
splenopexy is technically infeasible. Subtotal splenectomy and
splenic auto-transplantation may be of limited value .Our
patient also had an enlarged spleen (hypersplenism), thus
splenectomy was preferred to splenopexy by the operating
surgeon to avoid any postoperative complications. Recently
laparoscopic procedures have been introduced for splenic
surgery and it has shown to offer the benefits of minimally
invasive surgery 10-11.
Anti-Pneumococcal,
Hemophilus
influenza
and
meningococcal vaccines are indicated before elective
splenectomy and shortly after nonelectivesplenectomy11.
Significant morbidity and mortality rates seem to be
considerably less and are limited primarily to patients
presenting initially with acute abdominal findings 4.
IV- ACKNOWLEDGMENTS
The authors thank the patient to allow the case history and
images for publication for academic purposes.
121 | P a g e
International Journal of Technical Research and Applications e-ISSN: 2320-8163,
www.ijtra.com Volume 4, Issue 1 (January-February, 2016), PP. 120-123
FIG 1 : USG SHOWING SPLEEN IN ECTOPIC LOCATION
EXTENDING FROM LEFT LUMBAR REGION TO LEFT ILIAC
FOSSA MEASURING 19.3 CM. SPLEEN CHANGED THE
POSITION ON CHANGE OF POSTURE
FIG 2: CECT SCAN SHOWING ECTOPIC AND
ENLARGED SPLEEN EXTENDING FROM THE LEFT
LUMBAR REGION INTO THE PELVIS
122 | P a g e
International Journal of Technical Research and Applications e-ISSN: 2320-8163,
www.ijtra.com Volume 4, Issue 1 (January-February, 2016), PP. 120-123
REFERENCES
1.
Singh I. Essentials of anatomy. New Delhi. Jaypee
Brothers Medical Publishers Ltd; 2002,P283-4.
2.
Desai DC, Hebra A, Davidoff AM, Schnaufer L.
Wandering Spleen: A Challenging diagnosis. South Med J
1997; 90(4):439-43.
3.
Anthony McBrearty, Etain McGuinness, and Adrian
Neill. Wandering spleen: a potential abdominal catastrophe.
Clin Case Rep. 2013 Oct; 1(1): 4243. doi: 10.1002/ccr3.9.
4.
Sharma A, Salerno G. A torted wandering spleen: a
case report. J Med Case Rep. 2014 1; 8:133. doi:
10.1186/1752-1947-8-133.
5.
Dahiya N, Karthikeyan D, Vijay S, Kumar T, Vaid M.
Wandering spleen : Unusual presentation and course of events.
Indian J Radiol Imaging 2002;12:359-62
6.
Ben Ely A, Seguier E, Lotan G, Strauss S, Gayer G.
Familial wandering spleen: a first instance. J Pediatr Surg.
2008; 43(5):E23-5. doi: 10.1016/j.jpedsurg.2007.12.077.
7.
Llorens Marina CI, Cedeno A, Lugo-Vicente H,
Chapel C, Rivera G, Diaz A. Wandering spleen torsion causing
acute abdominal pain in a child: case report and review of
literature. Bol Asoc Med P R. 2014; 106(1):57-9.
8.
Lin CH, Wu SF, Lin WC, Chen AC. Wandering
spleen with torsion and gastric volvulus. J Formos Med Assoc.
2005; 104(10):755-8.
9.
Priyadarshi RN, Anand U, Kumar B, Prakash V.
Torsion in wandering spleen: CT demonstration of whirl sign.
Abdom Imaging. 2013; 38(4):835-8. doi: 10.1007/s00261-0129944-9.
10. Schaarschmidt K, Lempe M, Kolberg-Schwerdt A,
Schlesinger F, Hayek I, Jaeschke U. The technique of
laparoscopic retroperitoneal splenopexy for symptomatic
wandering spleen in childhood. J Pediatr Surg.2005;40:5757
11. Benevento A, Boni L, Dionigi G, Ferrari A, Dionigi
R. Emergency laparoscopic splenectomy for "wandering"
(pelvic) spleen: case report and review of the literature on
laparoscopic approach to splenic diseases. Surg Endosc. 2002;
16(9):1364-5. Epub 2002 Jun 6
123 | P a g e
You might also like
- Radical Disciple 1Document4 pagesRadical Disciple 1Milton LucasNo ratings yet
- Successful Treatment of A 14-Year-Old Patient With Intestinal Malrotation With Laparoscopic Ladd Procedure: Case Report and Literature ReviewDocument5 pagesSuccessful Treatment of A 14-Year-Old Patient With Intestinal Malrotation With Laparoscopic Ladd Procedure: Case Report and Literature ReviewHendry JohannesNo ratings yet
- Primitive Mesenteric Clamp Syndrome: Unusual Cause of Upper Gastrointestinal ObstructionDocument5 pagesPrimitive Mesenteric Clamp Syndrome: Unusual Cause of Upper Gastrointestinal ObstructionIJAR JOURNALNo ratings yet
- JCDR 9 PD26Document2 pagesJCDR 9 PD26ceciliaNo ratings yet
- Gi 1Document3 pagesGi 1Syifa' FauziyahNo ratings yet
- Acute Gastric Dilation and Ischemia Secondary To Small Bowel ObstructionDocument4 pagesAcute Gastric Dilation and Ischemia Secondary To Small Bowel ObstructionMudatsir N. MileNo ratings yet
- WWW - Vet 201508 0008Document4 pagesWWW - Vet 201508 0008Preston BoasythongNo ratings yet
- 2 5 21 861 PDFDocument3 pages2 5 21 861 PDFAhmed ZidanNo ratings yet
- 231 PDFDocument12 pages231 PDFAgus KarsetiyonoNo ratings yet
- Title: A Case Report On Left-Sided AppendicitisDocument10 pagesTitle: A Case Report On Left-Sided Appendicitishom lakshmiNo ratings yet
- Case Report AbdomenDocument5 pagesCase Report Abdomensigario hutamaNo ratings yet
- Ogilvie Syndrome After Emergency Cesarean Section: A Case ReportDocument4 pagesOgilvie Syndrome After Emergency Cesarean Section: A Case ReportIJAR JOURNALNo ratings yet
- APENDICITIS Fischers Mastery of Surgery 7th ING PDFDocument33 pagesAPENDICITIS Fischers Mastery of Surgery 7th ING PDFMichel RamirezNo ratings yet
- Surgical ArticleDocument8 pagesSurgical ArticleKevin Leo Lucero AragonesNo ratings yet
- Interpretation of Abdominal X-RayDocument5 pagesInterpretation of Abdominal X-RayWeh Loong GanNo ratings yet
- Postgrad Med J 2005 Yalamarthi 174 7Document5 pagesPostgrad Med J 2005 Yalamarthi 174 7Novendi RizkaNo ratings yet
- Bet 4 051Document3 pagesBet 4 051myway999No ratings yet
- International Journal of Pharmaceutical Science Invention (IJPSI)Document3 pagesInternational Journal of Pharmaceutical Science Invention (IJPSI)inventionjournalsNo ratings yet
- Anil Degaonkar, Nikhil Bhamare, Mandar Tilak Arterio-Enteric Fistula A Case ReportDocument6 pagesAnil Degaonkar, Nikhil Bhamare, Mandar Tilak Arterio-Enteric Fistula A Case ReportDr. Krishna N. SharmaNo ratings yet
- Hypertrophic Pyloric StenosisDocument28 pagesHypertrophic Pyloric StenosisAhmad Abu Kush100% (2)
- Bowel ObstructionDocument10 pagesBowel Obstructionenke.nwekeNo ratings yet
- Dysphagia Lusoria: A Comprehensive ReviewDocument6 pagesDysphagia Lusoria: A Comprehensive ReviewDante ChavezNo ratings yet
- A Rare Case of Colon Cancer in A Young Patient: A Case Report and Literature ReviewDocument5 pagesA Rare Case of Colon Cancer in A Young Patient: A Case Report and Literature ReviewIJAR JOURNALNo ratings yet
- A Case of Gastric Schwannoma: Sciences, Porompat, Imphal. Sciences, Porompat, Imphal. Imphal. Sciences, Porompat, ImphalDocument7 pagesA Case of Gastric Schwannoma: Sciences, Porompat, Imphal. Sciences, Porompat, Imphal. Imphal. Sciences, Porompat, ImphalFerina Nur HaqiqiNo ratings yet
- Small Intestine Obstruction in Patients Due To Phytobezoar: Case Report of Four PatientsDocument4 pagesSmall Intestine Obstruction in Patients Due To Phytobezoar: Case Report of Four PatientsInt Journal of Recent Surgical and Medical SciNo ratings yet
- Gobbur Et AlDocument4 pagesGobbur Et AleditorijmrhsNo ratings yet
- Colitis Due To Ancylostoma Duodenale: ReferencesDocument2 pagesColitis Due To Ancylostoma Duodenale: Referencesinggrit06No ratings yet
- Accessory Spleen: V. Durgesh, CH. Roja RaniDocument3 pagesAccessory Spleen: V. Durgesh, CH. Roja RaniIOSRjournalNo ratings yet
- 201 203 AbdominalDocument3 pages201 203 AbdominalManal Salah DorghammNo ratings yet
- Biloma After Laparoscopic Cholecystectomy: Case ReportDocument3 pagesBiloma After Laparoscopic Cholecystectomy: Case ReportAlpriyando Rindy AgustinusNo ratings yet
- Stomach Volvulus: Why Should We Remember It? Case ReviewDocument7 pagesStomach Volvulus: Why Should We Remember It? Case ReviewChristabella Natalia WijayaNo ratings yet
- Title: A Case Report On Left-Sided AppendicitisDocument10 pagesTitle: A Case Report On Left-Sided AppendicitispigzeniNo ratings yet
- TMP CD3Document4 pagesTMP CD3FrontiersNo ratings yet
- Ijrms-12417 CDocument5 pagesIjrms-12417 CSamuel MedinaNo ratings yet
- Case Report Hepato FinalDocument29 pagesCase Report Hepato FinalBangkit PutrawanNo ratings yet
- Surgical Treatment of Gastrointestinal Motility DisordersDocument47 pagesSurgical Treatment of Gastrointestinal Motility DisordersBolivar IseaNo ratings yet
- IntussusceptionDocument10 pagesIntussusceptionhya2284No ratings yet
- NCBI BookshelfDocument9 pagesNCBI Bookshelframzan aliNo ratings yet
- Intestinal Obstruction Due To An Obturator Hernia: A Case Report With A Review of The LiteratureDocument2 pagesIntestinal Obstruction Due To An Obturator Hernia: A Case Report With A Review of The Literaturemudasir61No ratings yet
- Case Report EndometriosisDocument4 pagesCase Report EndometriosischristinejoanNo ratings yet
- Case 22: Total Colonic Aganglionosis - Long-Segment Hirschsprung DiseaseDocument4 pagesCase 22: Total Colonic Aganglionosis - Long-Segment Hirschsprung DiseaseRahmat MuliaNo ratings yet
- Acute Appendicitis PaperDocument6 pagesAcute Appendicitis Paperapi-279084200No ratings yet
- Cystogram With Dumbbell Shaped Urinary Bladder in A Sliding Inguinal HerniaDocument12 pagesCystogram With Dumbbell Shaped Urinary Bladder in A Sliding Inguinal Hernia6281326189433No ratings yet
- Rounds: GrandDocument7 pagesRounds: GrandHưng Nguyễn KiềuNo ratings yet
- Pancreatic Pseudocyst EDITEDDocument5 pagesPancreatic Pseudocyst EDITEDLaura LatifaNo ratings yet
- Tuberculous Ileal Perforation in Post-Appendicectomy PeriOperative Period: A Diagnostic ChallengeDocument3 pagesTuberculous Ileal Perforation in Post-Appendicectomy PeriOperative Period: A Diagnostic ChallengeIOSRjournalNo ratings yet
- Soleimani 2007Document9 pagesSoleimani 2007ceciliaNo ratings yet
- Primary Aortoenteric FistulaDocument5 pagesPrimary Aortoenteric FistulaKintrili AthinaNo ratings yet
- Appendicitis: Mark W. Jones Hassam Zulfiqar Jeffrey G. DeppenDocument7 pagesAppendicitis: Mark W. Jones Hassam Zulfiqar Jeffrey G. DeppenAndi HairunNo ratings yet
- Laparoscopic Splenectomy For Pediatric Wandering Spleen - A Case ReportDocument11 pagesLaparoscopic Splenectomy For Pediatric Wandering Spleen - A Case ReportAdlyn Bea Albesa-BernaldezNo ratings yet
- Nissen Fundoplication - StatPearls - NCBI BookshelfDocument9 pagesNissen Fundoplication - StatPearls - NCBI BookshelfAndres Neira QuezadaNo ratings yet
- Pancreatic Pseudocyst EDITEDDocument5 pagesPancreatic Pseudocyst EDITEDLaura LatifaNo ratings yet
- SyedDocument3 pagesSyededitorijmrhsNo ratings yet
- TR Kelompok 4 AbdomenDocument29 pagesTR Kelompok 4 AbdomenShelly AnggrainiNo ratings yet
- Upper Gastrointestinal Endoscopy in Turkey: A Review of 5,000 CasesDocument2 pagesUpper Gastrointestinal Endoscopy in Turkey: A Review of 5,000 CasesEnderson MedeirosNo ratings yet
- Surgery Lectures EsophagusDocument22 pagesSurgery Lectures Esophagusj,007No ratings yet
- Perforated Appendicitis: Shahid Sadoughi University of Medical Sciense, Yazd, IranDocument17 pagesPerforated Appendicitis: Shahid Sadoughi University of Medical Sciense, Yazd, IranEloisamay Barrameda EspirituNo ratings yet
- Intussusception: PathophysiologyDocument8 pagesIntussusception: PathophysiologyNaufal AndaluNo ratings yet
- HematometrocolposDocument7 pagesHematometrocolposanna carmela rani montalboNo ratings yet
- Krukenberg Tumour Simulating Uterine Fibroids and Pelvic Inflammatory DiseaseDocument3 pagesKrukenberg Tumour Simulating Uterine Fibroids and Pelvic Inflammatory DiseaseradianrendratukanNo ratings yet
- Mortalidad en Los Recién Nacidos Referidos A Hospitale Terciarios. Una IntrospecciónDocument4 pagesMortalidad en Los Recién Nacidos Referidos A Hospitale Terciarios. Una Introspecciónluisalfredo_montesNo ratings yet
- Vacunaciòn AntipertussisDocument5 pagesVacunaciòn Antipertussisluisalfredo_montesNo ratings yet
- Use of Probiotics For Management of Acute.30Document9 pagesUse of Probiotics For Management of Acute.30Muhammad AL Farisi SutrisnoNo ratings yet
- Asymptomatic Mycoplasma Infection Causing Acute Demyelinating Encephalomyelitis: Case Report and Review of LiteratureDocument4 pagesAsymptomatic Mycoplasma Infection Causing Acute Demyelinating Encephalomyelitis: Case Report and Review of Literatureluisalfredo_montesNo ratings yet
- A Teaching-Learning Sequence For The Special RelativityDocument25 pagesA Teaching-Learning Sequence For The Special Relativityluisalfredo_montesNo ratings yet
- Academic Freedom and The Diminished Subject725005 - 923831530Document20 pagesAcademic Freedom and The Diminished Subject725005 - 923831530luisalfredo_montesNo ratings yet
- A Place From Where To Speak - The University And360920 - 923831531Document19 pagesA Place From Where To Speak - The University And360920 - 923831531luisalfredo_montesNo ratings yet
- Academic Freedom in Europe - Reviewing Unesco's546926 - 923831534Document26 pagesAcademic Freedom in Europe - Reviewing Unesco's546926 - 923831534luisalfredo_montesNo ratings yet
- ¿Whither ConstructivismDocument18 pages¿Whither Constructivismluisalfredo_montesNo ratings yet
- A Method Has Been Found - On Educational Research and Its Methodological Preoccupations 305633 - 906619931Document10 pagesA Method Has Been Found - On Educational Research and Its Methodological Preoccupations 305633 - 906619931luisalfredo_montesNo ratings yet
- A Cross-Cultural Comparison of Korean and American Science Teachers' Views of Evolution and The Nature of Science 453338 - 920456608Document32 pagesA Cross-Cultural Comparison of Korean and American Science Teachers' Views of Evolution and The Nature of Science 453338 - 920456608luisalfredo_montesNo ratings yet
- Theri GathaDocument26 pagesTheri GathaLalit MishraNo ratings yet
- DisasterDocument10 pagesDisasterMixsz LlhAdy100% (1)
- Phed 239 Syllabus s14-1st Half-3Document7 pagesPhed 239 Syllabus s14-1st Half-3api-249627241No ratings yet
- Upload - 00083938 - 1499831786562 BOND MAXDocument17 pagesUpload - 00083938 - 1499831786562 BOND MAXkrsrinivasarajuNo ratings yet
- CrimLaw2 Reviewer (2007 BarOps) PDFDocument158 pagesCrimLaw2 Reviewer (2007 BarOps) PDFKarla EspinosaNo ratings yet
- Item Analysis Third QuarterDocument4 pagesItem Analysis Third Quarterwhite valeNo ratings yet
- Training Needs in Facilities Management Zaharah Manaf 2005Document11 pagesTraining Needs in Facilities Management Zaharah Manaf 2005Anonymous dmYc1M4uNo ratings yet
- A Beginner Guide To Website Speed OptimazationDocument56 pagesA Beginner Guide To Website Speed OptimazationVijay KumarNo ratings yet
- B.sc. Hons. ZoologyDocument110 pagesB.sc. Hons. ZoologyHarsh Dalal0% (1)
- National Social Protection Strategy GhanaDocument95 pagesNational Social Protection Strategy GhanaSisiraPinnawalaNo ratings yet
- Kerala University PHD Course Work Exam SyllabusDocument4 pagesKerala University PHD Course Work Exam Syllabuslozuzimobow3100% (2)
- 4TH Semester B.A., LL.B B.A., LL.B (H)Document14 pages4TH Semester B.A., LL.B B.A., LL.B (H)BISTIRNA BARUANo ratings yet
- Buggy LabDocument5 pagesBuggy Labnarinyigit84No ratings yet
- Quantitative Option Strategies: Marco Avellaneda G63.2936.001 Spring Semester 2009Document29 pagesQuantitative Option Strategies: Marco Avellaneda G63.2936.001 Spring Semester 2009Adi MNo ratings yet
- Culture Shock Refers To The Feelings of Confusion and Uncertainty That You Experience When You Come Into Contact With A New CultureDocument13 pagesCulture Shock Refers To The Feelings of Confusion and Uncertainty That You Experience When You Come Into Contact With A New CultureRetno WulanNo ratings yet
- Ieo Sample Paper Class-10Document2 pagesIeo Sample Paper Class-10jairusr100% (1)
- Ed 2 Module 8 1Document5 pagesEd 2 Module 8 1Jimeniah Ignacio RoyoNo ratings yet
- Rfid: Threats, Failures, and FixesDocument43 pagesRfid: Threats, Failures, and FixesChromatonNo ratings yet
- What Is Black Box Testing?: Black Box Testing Is Done Without The Knowledge of The Internals of The System Under TestDocument127 pagesWhat Is Black Box Testing?: Black Box Testing Is Done Without The Knowledge of The Internals of The System Under TestusitggsipuNo ratings yet
- MIS ProjectDocument12 pagesMIS ProjectDuc Anh67% (3)
- Executive ReportDocument51 pagesExecutive ReportPrecelle Joy YangaNo ratings yet
- American Colonial Empire - Julian GoDocument6 pagesAmerican Colonial Empire - Julian GoBert M DronaNo ratings yet
- Volt Am Metric Determination of Ascorbic Acid in Vitamin C SupplementsDocument2 pagesVolt Am Metric Determination of Ascorbic Acid in Vitamin C SupplementshebieNo ratings yet
- 4 5 and 6 - Approaches To HR MeasurementDocument14 pages4 5 and 6 - Approaches To HR MeasurementRahul RaoNo ratings yet
- Notes-Indolence of The Filipino PeopleDocument3 pagesNotes-Indolence of The Filipino PeopleKayes MNo ratings yet
- D4213Document5 pagesD4213Ferry Naga FerdianNo ratings yet
- Gelernter, David Hillel - The Tides of Mind - Uncovering The Spectrum of Consciousness-Liveright Publishing Corporation (2016)Document263 pagesGelernter, David Hillel - The Tides of Mind - Uncovering The Spectrum of Consciousness-Liveright Publishing Corporation (2016)রশুদ্দি হাওলাদার100% (2)
- Prose: Jooprencess E. PonoDocument11 pagesProse: Jooprencess E. Ponoaye plazaNo ratings yet
- The Balance of Power in World Politics TDocument23 pagesThe Balance of Power in World Politics TVali IgnatNo ratings yet