Professional Documents
Culture Documents
Bruyere Case13 001-012 DS
Uploaded by
jrnataCopyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Bruyere Case13 001-012 DS
Uploaded by
jrnataCopyright:
Available Formats
Bruyere_Case13_001-012.
qxd
6/26/08
6:22 PM
Page 13-1
CAS E STU DY
13
BACTERIAL PNEUMONIA
For the Patient Case for this case study,
see the printed book.
DISEASE SUMMARY
Definitions
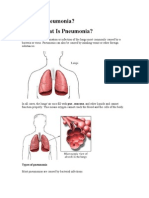
Bacterial pneumonia (from the Greek pneuma, breath) is a potentially fatal infection and
inflammation of the lower respiratory tract (i.e., bronchioles and alveoli) usually caused by
inhaled bacteria (most commonly Streptococcus pneumoniae, aka pneumococcus). The illness is frequently characterized by high fever, shortness of breath, rapid breathing, sharp
chest pain, and a productive cough with thick phlegm. Pneumonia that develops outside the
hospital setting is commonly referred to as community-acquired pneumonia. Pneumonia that
develops 48 hours or later after admission to the hospital is known as nosocomial or hospitalacquired pneumonia.
Prevalence
Approximately 4.5 million cases of community-acquired pneumonia occur annually in the
United States. The overall incidence of community-acquired pneumonia is reported to be 170
cases per 100,000 persons. Frequency estimates of nosocomial pneumonia in the United
States range from 4 to 7 episodes per 1000 hospitalizations. Approximately 25% of patients
in intensive care units develop pneumonia. Pneumonia is more prevalent during the winter
months and in colder climates. Incidence is greater in males than in females and advanced
age increases the frequency. Elderly people have a weaker immune response, a higher risk
for aspiration of bacteria, and health conditions (e.g., heart failure) that increase ones vulnerability for developing bacterial pneumonia as a complication. With advancing age, the
incidence of pneumonia increases from 94 cases per 100,000 persons aged 44 years to 280
cases per 100,000 persons older than 65 years.
Significance
Despite advances in the identification of causative microbes and the availability of new
antimicrobial drugs, pneumonia continues to be a major health problem. In addition, there
is still much controversy regarding diagnostic approaches and treatment choices.
DS13-1 Case Study 13 Bacterial Pneumonia
Bruyere_Case13_001-012.qxd
6/26/08
6:22 PM
Page 13-2
Pneumonia is the sixth leading cause of death in the United States and the most common cause of death from infectious disease. Furthermore, pneumonia is the leading cause of
death among hospital-acquired infections.
Left untreated and depending on the causative microbe and population, bacterial pneumonia has a mortality rate that may exceed 30%. Every year more than 60,000 Americans
die from pneumonia. Pneumococcal pneumonia alone accounts for an estimated 40,000
deaths yearly. The disease is a particular concern for older adults and people with chronic
illnesses or an impaired immune system, but it can also strike previously healthy, young people. Worldwide, pneumonia is a leading cause of death in children, many of whom are
younger than 1 year of age.
Bronchiectasis is a potential major complication of bacterial pneumonia. Destroyed
alveoli and bronchioles are replaced by small sacs filled with infected debris. A low-grade,
smoldering infection destroys more lung tissue with time. Bacterial pneumonia may also
cause destruction of lung tissue with subsequent scarring, a permanent decrease in gas
exchange, and a loss of respiratory reserve. The lungs also become less elastic and inflation
of the lungs requires more energy and work during the inspiratory phase of respiration.
Bacterial pneumonia can turn deadly when fluid fills the air sacs and interferes with the
ability to exchange oxygen and carbon dioxide. Circulating oxygen levels decrease (i.e.,
hypoxemia) and circulating carbon dioxide concentrations increase (i.e., hypercapnia), leading ultimately to respiratory failure and death. In some cases, microorganisms gain access
to the blooda condition known as bacteremiaspread rapidly to other organs, and cause
life-threatening sepsis or septic shock.
Causes and Risk Factors
Dozens of types of bacteria can cause pneumonia. Bacterial pneumonia is caused by an
infection of the lungs and may present as a primary disease or as secondary disease in a
debilitated individual or following a viral upper respiratory infection, such as influenza or
the common cold. Community-acquired pneumonia tends to be caused by different microorganisms than those infections acquired in the hospital. Some of the more common
causative microbes are shown in Disease Summary Table 13.1.
Pneumonia caused by Streptococcus pneumoniae remains the most common cause of all
bacterial pneumonias. High-risk groups include older adults and people with a chronic illness or compromised immune system. This type of pneumonia is a common complication of
chronic cardiopulmonary disease (e.g., heart failure) or an upper respiratory tract infection.
Mycoplasma are the smallest free-living agents of disease in man and have properties of
both bacteria and viruses. These microbes are a cause of walking pneumonia, which occurs
primarily in the summer and fall. Patients may not be sick enough to stay in bed or seek medical care and occasionally may not know that they have pneumonia. Mycoplasmal pneumonia
is common in children who attend childcare centers and among school-age children and young
adults. The disease may account for as many as one in three cases of childhood pneumonia.
Pneumonia from Haemophilus influenzae most commonly arises in the winter and early
spring and often follows an upper respiratory infection. This pneumonia is also associated
with hosts who are debilitated. Young age, old age, asthma, chronic obstructive pulmonary
disease (COPD), smoking, and a compromised immune system are risk factors.
Disease Summary Table 13.1 Common Causative Microbes of Communityand Hospital-Acquired Pneumonia
Causes of Community-Acquired
Pneumonia
Causes of Hospital-Acquired Pneumonia
Streptococcus pneumoniae
Pseudomonas aeruginosa
Mycoplasma pneumoniae
Staphylococcus aureus
Haemophilus influenzae
Klebsiella pneumoniae
Legionella pneumophila
Escherichia coli
Chlamydia pneumoniae
Enterobacter species
Moraxella catarrhalis
Serratia marcescens
Source: Porth CM. Pneumonias. In: Porth CM, ed. PathophysiologyConcepts of Altered Disease States. 7th Ed.
Philadelphia: Lippincott Williams & Wilkins, 2005:666669.
DS13-2 Case Study 13 Bacterial Pneumonia
Bruyere_Case13_001-012.qxd
6/26/08
6:22 PM
Page 13-3
Disease Summary Table 13.2 Risk Factors Associated with Specific Types
of Bacterial Pneumonia
Risk Factors for Bacterial Pneumonia
Causative Bacteria
Exposure to overcrowded institutions such as
jails, shelters for homeless people, military
training barracks, and childcare centers
Streptococcus pneumoniae, Mycoplasma
pneumoniae, Chlamydia pneumoniae
Diabetic ketoacidosis
S. pneumoniae, Staphylococcus aureus
Chronic obstructive pulmonary disease
Moraxella catarrhalis
Solid organ transplantation (primarily from
immunosuppressant drugs)
S. pneumoniae, Legionella pneumophila,
M. catarrhalis
Sickle cell disease (secondary to loss of
splenic function)
S. pneumoniae, Haemophilus influenzae
Cystic fibrosis
S. aureus, Pseudomonas aeruginosa
Gastrointestinal surgery
Escherichia coli
Source: Sharma S. Pneumoniabacterial. eMedicine website. Available at: www.emedicine.com/MED/topic1852.htm.
Date accessed: February 2007.
Legionella pneumophila infections tend to occur sporadically and in local outbreaks.
Although more than 14 types of L. pneumophila have been identified, serotype 1 accounts for
more than 80% of reported cases of legionellosis. The organism frequently is found in warm,
standing water. Legionella pneumonia was named after an outbreak in 1976 that affected
approximately 180 members of the American Legion who were staying at the same
Philadelphia hotel for an annual convention. Twenty-nine legionnaires died and the
causative microbe was not identified until the following year. These infections usually arise
in the summer and fall and bacteria may be found in the water condensed from air conditioning systems or in contaminated hospital water systems.
Although everyone is at risk, adolescents and young adults are most commonly affected
by chlamydial pneumonia. The chlamydial strain that causes pneumonia is not the same
microbe that causes sexually transmitted chlamydia.
Gram-negative pneumonias (e.g., caused by Escherichia coli, Pseudomonas, Enterobacter,
or Serratia) are observed in individuals who are debilitated, immunocompromised, or recently
hospitalized. Previous antibiotic therapy and mechanical ventilation are also risk factors.
Aspiration plays a central role in the pathogenesis of nosocomial pneumonia.
Approximately 45% of healthy subjects aspirate during sleep, and an even higher percentage
of severely ill patients aspirate routinely. The oropharynx of hospitalized patients may
become colonized with aerobic gram-negative bacteria within a few days after admission,
and nosocomial pneumonia is predominantly caused by gram-negative bacteria. Any individual with a subnormal level of consciousness (e.g., due to seizures or alcohol or drug intoxication) or central nervous system impairment (e.g., due to a stroke) may have a reduced gag
reflex that allows aspiration of stomach or oropharyngeal contents containing bacteria.
Typical causative organisms include Moraxella catarrhalis and the anaerobic organisms
Bacteroides, Peptostreptococcus, and Fusobacterium. When isolated, these bacteria are commonly part of a polymicrobial flora.
Bacterial pneumonia caused by Staphylococcus aureus is commonly observed in intravenous drug users, individuals with debilitative diseases (especially cystic fibrosis), patients
with prosthetic devices, hospitalized patients, and residents of chronic care facilities. In
patients who abuse intravenous drugs, the infection probably is spread through the blood to
the lungs from contaminated injection sites. S. aureus also is an important cause of pneumonia following infection with influenza A virus.
Patients with chronic alcoholism, diabetes mellitus, or COPD are at increased risk for
bacterial pneumonia caused by Klebsiella pneumoniae. Other risk factors that are associated
with specific types of pneumonia are shown in Disease Summary Table 13.2.
Pathophysiology
Bacteria commonly enter the respiratory tract but, due to multiple defense mechanisms, do
not normally cause pneumonia. When pneumonia does occur, it usually is the result of an
exceedingly virulent microbe, a large dose of bacteria, and/or impaired host defense
DS13-3 Case Study 13 Bacterial Pneumonia
Bruyere_Case13_001-012.qxd
6/26/08
6:22 PM
Page 13-4
Disease Summary Table 13.3 Conditions That Interfere with Primary
Respiratory Defense Mechanisms
Respiratory Defense
Mechanism
Function(s)
Factors That Impair
Function
Nasopharyngeal defenses
IgA protects against bacterial
proliferation
Sneezing removes microbes
from respiratory tract
IgA deficiency
Hay fever
Common cold
Trauma to the nose
Glottic and cough reflexes
Protect against aspiration
Reduced cough reflex due
to stroke, neuromuscular
disease, sedation, anesthesia,
tracheal intubation
Mucociliary clearance system
Removes microbes from
nasopharynx down to alveoli
Smoking
Viruses
Cold, dry air
Tracheal intubation
Alveolar macrophage
Removes microbes from alveoli
Cold, dry air
Alcohol use
Smoking
Obstruction hypoxia
IgG and IgM
Help to remove microbes from
the blood
IgG and/or IgM deficiency
Adapted with permission from Porth CM. Pneumonias. In: Porth CM, ed. PathophysiologyConcepts of Altered
Disease States. 7th Ed. Philadelphia: Lippincott Williams & Wilkins, 2005;Table 30-1:666.
mechanisms. A list of the five primary respiratory defense mechanisms and conditions that
interfere with function is shown in Disease Summary Table 13.3.
When microorganisms evade upper respiratory defense mechanisms, the alveolar
macrophage is capable of removing most infectious agents without triggering a significant
inflammatory or immune response. However, if the microbe is virulent or present in sufficiently
high numbers, it can overwhelm macrophages and result in a full-scale activation of systemic
defense mechanisms. These mechanisms include the release of multiple chemical mediators of
inflammation, infiltration of white blood cells, and activation of the immune response.
Tight adherence of some bacteria (e.g., Pseudomonas) to the tracheal lining and biofilm
of an endotracheal tube makes clearance of these microbes from the airways difficult and
accounts, in part, for their highly virulent nature.
In non-hospitalized people, bacteria reach the lung by one of four routes:
1. inhalation of microorganisms that have been released into the air when an infected individual coughs or sneezes
2. aspiration of bacteria from the upper airways
3. spread from contiguous infected sites
4. hematogenous spread
When bacteria enter the lower respiratory tract, they adhere to the walls of bronchi and
bronchioles, multiply extracellularly, and trigger inflammation. Clinical risk factors that
favor colonization of the lower airways include antibiotic therapy that alters the normal bacterial flora, diabetes, smoking, chronic bronchitis, and viral infections.
With the onset of inflammation, alveolar air spaces fill with an exudative fluid (i.e., rich
in protein). Inflammatory cells (first neutrophils during the acute phase, later macrophages
and lymphocytes during the chronic phase) subsequently invade the walls of the alveoli.
Bacterial pneumonia may be associated with significant hypoxemia and hypercapnia because
thick, inflammatory exudate (or pus) collects in the alveolar spaces and interferes with the diffusion of oxygen and carbon dioxide. Alveolar exudate tends to solidifya process known as
consolidationand expectoration of infected phlegm becomes difficult. Legionella,
Mycoplasma, and Chlamydia are examples of atypical bacterial agents in that they produce
patchy inflammatory changes in the lungs (i.e., bronchopneumonia). The remaining typical
bacterial causes of pneumonia produce widespread inflammation throughout one or more
lobes of the lung (i.e., lobar pneumonia). Disease Summary Figure 13.1 illustrates the distinguishing features of bronchopneumonia and lobar pneumonia. The term double pneumonia
is used to indicate the presence of infection and inflammation within both lungs.
DS13-4 Case Study 13 Bacterial Pneumonia
Bruyere_Case13_001-012.qxd
6/26/08
6:22 PM
Page 13-5
Lobar pneumonia
Bronchopneumonia
Trachea
Scattered areas
of consolidation
Bronchus
Horizontal
fissure
Oblique
fissure
Alveolus
Terminal
bronchus
Consolidation in
one lobe
DISEASE SUMMARY FIGURE 13.1
Distinguishing features of lobar pneumonia and bronchopneumonia. (Image provided by the
Anatomical Chart Company.)
Colonization of the pharynx and, possibly, the stomach with bacteria is the most important factor in the pathophysiology of hospital-acquired pneumonia, followed closely by aspiration of infected secretions into the lower airways. Pharyngeal colonization is promoted by
several exogenous factors: instrumentation of the upper airways with contaminated nasogastric or endotracheal tubes, contamination by dirty hands, and treatment with broadspectrum antibiotics that promote the emergence of drug-resistant bacteria. Certain patient
DS13-5 Case Study 13 Bacterial Pneumonia
Bruyere_Case13_001-012.qxd
6/26/08
6:22 PM
Page 13-6
characteristics (e.g., malnutrition, advanced age, altered consciousness, swallowing disorders, immunodeficiency) are also major contributing factors.
The role of the stomach in the pathophysiology of nosocomial pneumonia remains controversial. However, research studies suggest that elevations in gastric pH resulting from the
use of antacids, H2-receptor blockers, and enteral feeding are associated with gastric microbial overgrowth and tracheobronchial colonization.
Pneumococcal pneumonia remains the most common type of bacterial pneumonia and
its pathophysiology has been extensively studied. The initial step in the development of this
disease is the attachment of S. pneumoniae to cells of the nasopharynx and subsequent colonization. Colonization alone, however, does not cause clinical manifestations of illness
because perfectly healthy people can harbor the microbe without evidence of infection.
Factors that permit pneumococci to spread beyond the nasopharynx include the virulence of
the strain, impaired host defense mechanisms, and viral infections of the respiratory tract.
Viruses can damage respiratory tract lining cells, enhance bacterial adherence, and increase
the production of mucus, which protects pneumococci from phagocytosis. In the alveoli,
pneumococci infect type II alveolar cells and adhere to alveolar walls, causing an outpouring of fluid, red and white blood cells, and fibrin from the circulation, which, in turn, results
in consolidation of the lung. Fluid in the lower airways creates a medium for further multiplication of bacteria and aids in the spread of infection through pores of Kohn into adjacent
regions of the lung.
Diagnosis: Clinical Manifestations
and Laboratory Tests
A diagnosis of bacterial pneumonia is based primarily on chest x-ray findings, white blood cell
count, and a sputum culture together with fever (often as high as 106F), recurrent chills, cough,
shortness of breath (i.e., dyspnea), and abnormal chest sounds.
The clinical presentation of bacterial pneumonia varies from a mildly ill, ambulatory
patient to a critically ill patient with respiratory failure or septic shock. The sudden onset of
symptoms with rapid progression of the illness is typical of bacterial pneumonia. A thorough
past medical history and history of potential exposures are usually obtained. If the patient
has been healthy previously, the cause of pneumonia is usually Mycoplasma or a gram-positive
microbe. However, if the patient has been hospitalized or has a chronic illness, gram-negative
microbes are suspected.
Although not diagnostic of a particular causative agent, characteristics of the sputum
may suggest a particular pathogen. Pneumococci may cause bloody or rust-colored sputum. Patients with Pseudomonas, Haemophilus, or pneumococcal infections are known to
expectorate green sputum. Anaerobic infections typically produce foul-smelling and badtasting sputum. Klebsiella and type 3 pneumococci cause the production of thick, dark red
sputum.
Rigors or severe shaking chills may be observed with any infectious process. However,
and for reasons that are not clear, the presence of rigors suggests pneumococcal pneumonia
more often than pneumonia caused by other bacterial pathogens. Patients may complain of
non-specific symptoms that include headache, malaise, nausea, vomiting, and diarrhea.
Although these symptoms may be observed with many other systemic illnesses, their presence is suggestive of infection with Legionella species. Patients may also complain of cough,
myalgia, shortness of breath, abdominal pain, loss of appetite, and unintentional weight loss.
Sharp or stabbing chest pain worsened by deep breathing or coughing and secondary to
pleuritis is a common symptom of pneumococcal infection, but may also occur with other
types of pneumonia.
Physical examination findings vary depending on the type of microorganism, severity of
pneumonia, age of the patient, coexisting host factors, and presence of complications and
may include the following:
fever or hypothermia
rapid, shallow breathing
tachycardia or bradycardia
cyanosis
decreased breath sounds
DS13-6 Case Study 13 Bacterial Pneumonia
Bruyere_Case13_001-012.qxd
6/26/08
6:22 PM
Page 13-7
crackles (rales) with auscultation of the lungs
egophony on auscultation
pleural friction rub
dullness of the chest to percussion
altered mental status (especially confusion)
Leukocytosis (15,000 white blood cells/mm3) with a shift to the left and a predominance of neutrophils in the circulation may be observed with any bacterial infection.
However, its absence, particularly in patients who are elderly or debilitated, should not cause
the clinician to discount the possibility of a bacterial infection. Leukopenia is an ominous
sign of impending sepsis and portends a poor outcome. An assessment of the arterial blood
gases is essential to determine if hospital admission or oxygen supplementation is indicated
and may reveal hypoxemia and respiratory acidosis. A pulse oximetric finding that is 90%
indicates significant hypoxemia.
Hyponatremia and microhematuria may be associated with Legionella pneumonia.
Urinary antigen testing for Legionella serogroup 1 microbes is accurate. A Legionella serum
antibody titer of 1:128 or more is suggestive of Legionella pneumonia. The presence of
Mycoplasma and Chlamydia immunoglobulin M antibodies contribute to the diagnosis.
Chest radiographs reveal white shadows in the involved area indicative of an alveolar
inflammatory process and may also indicate the following:
a segmental or lobar opacity is observed with S. pneumoniae
cavitary lesions and bulging lung fissures are caused by K. pneumoniae and S. aureus
cavitation and pleural effusions are caused by S. aureus, anaerobic infections, and gramnegative infections
Legionella tends to affect the lower lung fields
Klebsiella tends to affect the upper lung zones
In unclear cases, high-resolution computed tomography (CT) scanning of the lungs may
aid in the diagnosis.
Sputum examination provides an accurate diagnosis in approximately 50% of patients.
A gram stain of expectorated sputum helps to distinguish bacterial from viral pneumonia
and gram-negative from gram-positive microbes. Sputum samples that result from deep
cough provide the best results. A single predominant microbe present with the gram stain
is indicative of bacterial pneumonia. Disease Summary Figure 13.2 shows a positive gram
stain in which S. pneumoniae appear in blue. Mixed flora may be observed with anaerobic
infections.
Blood cultures are positive in only approximately 40% of cases, but, when positive,
results confirm a causative agent. Cultures may require 2448 hours incubation before
results are available. When there is fluid within the pleural space, transthoracic needle aspiration (i.e., thoracentesis) with examination and culture of the fluid is performed to assist in
identification of the causative microorganism.
Distinguishing clinical features of selected types of bacterial pneumonia are listed in
Disease Summary Table 13.4.
DISEASE SUMMARY FIGURE 13.2
Gram stain showing Streptococcus pneumoniae. (Reprinted with permission from Koneman EW, Allen
SD, Janda WM, Schreckenberger PC, Winn WC Jr. Color Atlas and Textbook of Diagnostic
Microbiology. 5th Ed. Philadelphia: Lippincott Williams & Wilkins, 1997.)
DS13-7 Case Study 13 Bacterial Pneumonia
Bruyere_Case13_001-012.qxd
6/26/08
6:22 PM
Page 13-8
Disease Summary Table 13.4 Distinguishing Clinical Features of Selected
Types of Bacterial Pneumonia
Microorganism
Common Clinical Manifestations
Gram Stain Result
Staphylococcus aureus
Fever, chills, chest pain, productive
cough, yellow sputum
Streptococcus pneumoniae
Fever, chills, chest pain, productive
cough, malaise, fine crackles,
rust-colored sputum
Haemophilus influenzae
Upper respiratory symptoms, fever,
vomiting, irritability, productive cough,
dyspnea, green sputum
Klebsiella pneumoniae
Productive cough, sputum is thick and
dark red
Pseudomonas aeruginosa
Fever, chills, copious green and
foul-smelling sputum
Legionella species
Fever, vomiting, diarrhea, myalgia,
abdominal pain, malaise, weakness,
lethargy, dry cough, fatigue,
low-grade fever
Mycoplasma pneumoniae
Sore throat, headache, myalgia, malaise,
dry cough, violent coughing attacks,
fatigue, low-grade fever
Adapted with permission from Schumann L. Pneumonia. In: Copstead LEC, Banasik JL, eds. Pathophysiology.
3rd Ed. St. Louis: Elsevier Saunders, 2005;Table 23-7:635.
Disease Summary Question 1. Distinguish between rales and crackles.
Disease Summary Question 2. What causes tachypnea and tachycardia secondary
to bacterial pneumonia?
Disease Summary Question 3. What is egophony?
Disease Summary Question 4. The only signs of bacterial pneumonia in an elderly
patient are often a loss of appetite and deterioration in mental status. What causes
deterioration in mental status secondary to bacterial pneumonia?
Disease Summary Question 5. Would you expect a patient with bacterial pneumonia
to have a high, low, or normal erythrocyte sedimentation rate?
Disease Summary Question 6. Would you expect a patient with bacterial pneumonia
to have a high, low, or normal serum C-reactive protein concentration?
Disease Summary Question 7. What is meant by a shift to the left?
Appropriate Therapy
The primary goals of treatment are to eradicate the infection, reduce morbidity, and prevent
complications. The pneumonia severity of illness scoring system (PSISS) evaluates 19 different characteristics of the patient that are easily obtained. The PSISS is used to make a
decision whether patients can be safely treated in an outpatient setting and is displayed in
Disease Summary Table 13.5.
Patients in risk class I (older than 50 years but no coexisting illness or vital sign
abnormality) and risk class II (70 total points) can be treated at home with planned outpatient follow-up evaluations. Patients in risk class III (7190 total points) should be
observed in the emergency room before their disposition is decided. Patients in risk class
IV (91130 total points) and V (130 total points) are seriously ill and usually require
hospital admission.
DS13-8 Case Study 13 Bacterial Pneumonia
Bruyere_Case13_001-012.qxd
6/26/08
6:22 PM
Page 13-9
Disease Summary Table 13.5 Pneumonia Severity of Illness Scoring
System (PSISS)
Patient Characteristic
Points Assigned
Demographic Factors
Age
Males
Age in years
Females
Age in years minus 10
Nursing home resident
10
Coexisting Illnesses
Cancer
30
Liver disease
20
Heart failure
10
Cerebrovascular disease
10
Renal disease
10
Physical Examination Findings
Altered mental status
20
Respiratory rate 30 breaths/minute
20
Systolic blood pressure 90 mm Hg
20
Body temperature 95F or 104F
15
Pulse 125 beats/minute
10
Laboratory and X-Ray Findings
Arterial pH 7.35
30
Blood urea nitrogen 30 mg/dL
20
Blood sodium 130 meq/L
20
Blood glucose 250 mg/dL
10
Hematocrit 30%
10
Arterial PaO2 60 mm Hg
10
Pleural effusion
10
Adapted with permission from Chesnutt MS, Prendergast TJ. Pneumonia. In: McPhee SJ, Papadakis MA, Tierney LM Jr.,
eds. 2007 Current Medical Diagnosis and Treatment. 46th Ed. New York: McGraw-Hill, 2007;Table 9-10:254.
Since many patients are hypoxemic, the first step in the management of bacterial pneumonia is establishing adequate ventilation and oxygenation. For patients with mild dyspnea,
only supplemental low-flow oxygen administered with a nasal cannula may be required.
Patients with underlying chronic lung disease who need high oxygen concentrations may
require endotracheal intubation. Other important measures include the following:
adequate hydration to loosen secretions and help bring up phlegm
correction of serum electrolyte abnormalities
control of fever with antipyretic agents
bedrest
good pulmonary hygiene (e.g., deep breathing and coughing exercises, suction of secretions, chest physical therapy)
Early mobilization of patients with encouragement to sit, stand, and walk when tolerated
also speeds recovery.
The mainstay of pharmacotherapy for bacterial pneumonia is antibiotic treatment.
Antibiotic therapy should be initiated promptly after the diagnosis is established and appropriate specimens are obtained, especially in patients who require hospitalization. Delays in
obtaining diagnostic specimens or the results of testing should not preclude the early administration of antibiotics to acutely ill patients. The choice of pharmacotherapeutic agent(s) is
based on the severity of the patients illness, host factors (e.g., coexisting illness and age), and
the presumed or identified causative agent. Outpatients are given oral agents and, for the
most part, parenteral medications are given to hospitalized patients. A table showing preferred pharmacotherapy for many of the microorganisms that cause bacterial pneumonia is
displayed in Disease Summary Table 13.6.
DS13-9 Case Study 13 Bacterial Pneumonia
Bruyere_Case13_001-012.qxd
6/26/08
6:23 PM
Page 13-10
Disease Summary Table 13.6 Preferred Pharmacotherapy for Microorganisms
That Cause Bacterial Pneumonia
Causative Microbe
Streptococcus pneumoniae
Haemophilus influenzae
Preferred Antimicrobial Therapy
Penicillin-susceptible strains: penicillin G, amoxicillin
Penicillin-resistant strains: macrolides1, cephalosporins,
doxycycline, fluoroquinolones2, clindamycin, vancomycin,
TMP-SMX3, linezolid
Cefotaxime, ceftriaxone, cefuroxime, doxycycline,
erythromycin, TMP-SMX
Staphylococcus aureus
Methicillin-susceptible strains: nafcillin or oxacillin with
or without rifampin; gentamicin
Methicillin-resistant strains: vancomycin with or without
gentamicin; rifampin, linezolid
Klebsiella pneumoniae
Third-generation cephalosporin4 an aminoglycoside5
for severe infections
Escherichia coli
Pseudomonas aeruginosa
Anaerobes
Mycoplasma pneumoniae
Legionella species
Chlamydia pneumoniae
Moraxella catarrhalis
Third-generation cephalosporin an aminoglycoside
for severe infections
An antipseudomonal -lactam6 aminoglycoside
Clindamycin, -lactam/-lactamase inhibitor7, imipenem
Doxycycline, erythromycin
A macrolide with or without rifampin; fluoroquinolone
Doxycycline
A second8- or third-generation cephalosporin; a
fluoroquinolone
Adapted with permission from Chesnutt MS, Prendergast TJ. Pneumonia. In: McPhee SJ, Papadakis MA, Tierney LM
Jr., eds. 2007 Current Medical Diagnosis and Treatment. 46th Ed. New York: McGraw-Hill, 2007;Table 9-9:252253.
1
For example, clarithromycin or azithromycin
2
For example, gatifloxacin or levofloxacin
3
Trimethoprim-sulfamethoxazole
4
For example, ceftriaxone or ceftazidime
5
For example, gentamicin or tobramycin
6
For example, ceftazidime
7
For example, ampicillin-sulbactam or piperacillin-tazobactam
8
For example, cefaclor or cefuroxime
Disease Summary Question 8. Why are so many different antibiotics necessary to
effectively treat bacterial pneumonia today?
Serious Complications and Prognosis
Potential serious complications of bacterial pneumonia are multiple and include the following:
local destruction of lung tissue with subsequent scarring and significant loss of gas exchange
bronchiectasis
empyema (i.e., accumulation of pus in the pleural space that often requires surgery and
aspiration)
respiratory failure
dependence on mechanical ventilation
septic shock
Prognosis generally is good in the otherwise healthy patient with uncomplicated pneumonia. With appropriate treatment, most patients improve markedly within 2 weeks. Several
factors, alone or in combination, increase morbidity and mortality and include the following:
advanced age
aggressive microbes (e.g., Klebsiella, Legionella)
coexisting illness
development of respiratory failure
DS13-10 Case Study 13 Bacterial Pneumonia
Bruyere_Case13_001-012.qxd
6/26/08
6:23 PM
Page 13-11
Disease Summary Table 13.7 Thirty-Day Mortality Rates Based On PSISS
Risk Classes
PSISS Risk Class
Mortality in 30 Days, %
0.10.4
II
0.60.7
III
0.92.8
IV
8.29.3
27.031.1
Adapted with permission from Chesnutt MS, Prendergast TJ. Pneumonia. In: McPhee SJ, Papadakis MA, Tierney LM
Jr., eds. 2007 Current Medical Diagnosis and Treatment. 46th Ed. New York: McGraw-Hill, 2007;Table 9-11:254.
neutropenia or immunodeficiency state
features of sepsis
In general, the mortality rate for community-acquired bacterial pneumonia is reported to be
1% when treated in an outpatient setting, but may increase up to 25% among those who
require hospital admission. Thirty-day mortality rates are based on PSISS risk classes as
shown in Disease Summary Table 13.7.
Suggested Readings
American Lung Association. Pneumonia fact sheet. American Lung Association website.
Available at: www.lungusa.org/site/pp.asp?cdvLUK9O0E&b35692. Date accessed: April
2006.
Brashers VL. Pneumonia. In: McCance KL, Huether SE, eds. Pathophysiology: The Biologic
Basis for Disease in Adults and Children. 5th Ed. St. Louis: Elsevier Mosby, 2006:12281230.
Chesnutt MS, Prendergast TJ. Pneumonia. In: McPhee SJ, Papadakis MA, Tierney LM Jr., eds.
2007 Current Medical Diagnosis and Treatment. 46th Ed. New York: McGraw-Hill, 2007:
251260.
Lehnert P. Pneumonia. WebMD website. Available at: www.webmd.com/a-to-z-guides/
Pneumonia-Topic-Overview. Date accessed: May 2005.
Little FF. Pneumonia. MedlinePlus Medical Encyclopedia website, National Library of
Medicine and National Institutes of Health. Available at: www.nlm.nih.gov/medlineplus/ency/
article/000145.htm. Date accessed: October 2005.
Mayo Clinic staff. Pneumonia. Mayo Clinic website. Available at: www.mayoclinic.com/health/
pneumonia/DS00135. Date accessed: May 2005.
Porth CM. Pneumonias. In: Porth CM, ed. PathophysiologyConcepts of Altered Disease
States. 7th Ed. Philadelphia: Lippincott Williams & Wilkins, 2005:665669.
Schumann L. Pneumonia. In: Copstead LEC, Banasik JL, eds. Pathophysiology. 3rd Ed. St.
Louis: Elsevier Saunders, 2005:634637.
Sharma S. Pneumoniabacterial. eMedicine website. Available at: www.emedicine.com/
MED/topic1852.htm. Date accessed: February 2007.
Stephen J. Pneumoniabacterial. eMedicine website. Available at: www.emedicine.com/
EMERG/topic465.htm. Date accessed: February 2007.
Ware CJ, Botros M. Bacterial pneumonia. eMedicineHealth website. Available at: www.
emedicinehealth.com/bacterial_pneumonia/article_em. Date accessed: August 2005.
DS13-11 Case Study 13 Bacterial Pneumonia
You might also like
- Bruyere Case13 001-012 DSDocument11 pagesBruyere Case13 001-012 DSSheila May LumhodNo ratings yet
- Pneumonia-Normal Host: Pneumonia Is An Acute or Chronic Infection Involving The Pulmonary Parenchyma. MostDocument2 pagesPneumonia-Normal Host: Pneumonia Is An Acute or Chronic Infection Involving The Pulmonary Parenchyma. MostJaya Semara PutraNo ratings yet
- Pyogenic Bacterial Pneumonia and Lung Abscess: Staphylococcus Aureus, Pseudomonas AeruginosaDocument5 pagesPyogenic Bacterial Pneumonia and Lung Abscess: Staphylococcus Aureus, Pseudomonas AeruginosaVladimir Tigrero ZernaNo ratings yet
- Causes of PneumoniaDocument4 pagesCauses of Pneumoniailke akdenizNo ratings yet
- Pneumonia WrittenDocument12 pagesPneumonia WrittenFereli Joy SupanNo ratings yet
- PneumoniaDocument10 pagesPneumoniaJohn Philip M. Lacas RNNo ratings yet
- Bacterial PneumoniaDocument6 pagesBacterial PneumoniaIrsa SevenfoldismNo ratings yet
- PneumoniaDocument68 pagesPneumoniaJelmalyn Basali100% (1)
- Pneumonia Is An: ClinicalDocument13 pagesPneumonia Is An: ClinicaldfgsfsfssdNo ratings yet
- PneumoniaDocument1 pagePneumoniaJozepf AgustinNo ratings yet
- Case Study PNEUMONIADocument40 pagesCase Study PNEUMONIAHomework PingNo ratings yet
- PneumoniaDocument18 pagesPneumoniaFryam Bells100% (1)
- Gharib2001 Radiologi Pneumonia-DikonversiDocument31 pagesGharib2001 Radiologi Pneumonia-Dikonversitsamara24_No ratings yet
- Fast Facts On PneumoniaDocument6 pagesFast Facts On PneumoniaAndeariesa DarmansiusNo ratings yet
- Lec. 3 Pulmonary Infections. SaifDocument19 pagesLec. 3 Pulmonary Infections. Saifs2111110520No ratings yet
- PneumoniaDocument2 pagesPneumoniaMargaret EricksonNo ratings yet
- Final Sem ProjectDocument53 pagesFinal Sem ProjectShourendranath MondalNo ratings yet
- Chapter 1Document30 pagesChapter 1Ayro Business CenterNo ratings yet
- Clinical Presentation On PnemoniaDocument37 pagesClinical Presentation On PnemoniasreekalaNo ratings yet
- Nursing Care Management 103 Cap MRDocument9 pagesNursing Care Management 103 Cap MRkarenfaye00No ratings yet
- Pneumonia 1Document17 pagesPneumonia 1Jonathan katanaNo ratings yet
- Streptococcus Pneumoniae Is A Normal Inhabitant of The Human Upper Respiratory TractDocument2 pagesStreptococcus Pneumoniae Is A Normal Inhabitant of The Human Upper Respiratory TractJj DelacruzNo ratings yet
- PneumoniaDocument3 pagesPneumoniaEdward McSweegan, PhD100% (1)
- CommunityDocument2 pagesCommunityRonald Anthony TobiasNo ratings yet
- PneumoniaDocument55 pagesPneumoniaGlenn ValerioNo ratings yet
- Focused Reviews: Pneumococcal Vaccination StrategiesDocument12 pagesFocused Reviews: Pneumococcal Vaccination StrategiesRishi MangalNo ratings yet
- CommunityDocument2 pagesCommunityMarlowe Adlei Novedo PabloNo ratings yet
- Overview of Community-Acquired Pneumonia in Adults: Official Reprint From Uptodate ©2023 UptodateDocument40 pagesOverview of Community-Acquired Pneumonia in Adults: Official Reprint From Uptodate ©2023 UptodateHERANDY GUADALUPE SOSA ROMERONo ratings yet
- Case Study For PneumoniaDocument11 pagesCase Study For PneumoniaGabbii Cinco100% (1)
- Epidemiology, Pathogenesis, and Microbiology of CDocument5 pagesEpidemiology, Pathogenesis, and Microbiology of C5grpnfzvtkNo ratings yet
- Neumonía Adquirida en La ComunidadDocument74 pagesNeumonía Adquirida en La ComunidadHector ArandaNo ratings yet
- Lec.2 Respirotary System SaifDocument19 pagesLec.2 Respirotary System Saifs2111110520No ratings yet
- Pneumonia Is AnDocument9 pagesPneumonia Is Ansandro2000No ratings yet
- PneumoniaDocument15 pagesPneumoniaJawahir Gomez100% (1)
- Woolfrey2012 PDFDocument22 pagesWoolfrey2012 PDFJorge BarriosNo ratings yet
- Pneumonia by Kamran UOSargodhaDocument19 pagesPneumonia by Kamran UOSargodhaZeshan Haider Kazmi100% (3)
- Central Academy: Biology ProjectDocument12 pagesCentral Academy: Biology ProjectMastbleNo ratings yet
- Medical Mnemonic Sketches : Pulmonary DiseasesFrom EverandMedical Mnemonic Sketches : Pulmonary DiseasesNo ratings yet
- Pneumonia 3Document8 pagesPneumonia 3janinecasilenNo ratings yet
- Managing Community-Acquired Pneumonia During Flu Season: ReviewDocument12 pagesManaging Community-Acquired Pneumonia During Flu Season: ReviewCaerulus Fuad Abdul BaqiNo ratings yet
- 3 PneumoniaDocument17 pages3 PneumoniaMohamed Na3eemNo ratings yet
- Pneumonia With Pleural EffusionDocument24 pagesPneumonia With Pleural EffusionMund CheleNo ratings yet
- Overview of Community-Acquired Pneumonia in Adults - UpToDateDocument29 pagesOverview of Community-Acquired Pneumonia in Adults - UpToDateリダNo ratings yet
- Overview of Community-Acquired Pneumonia in AdultsDocument73 pagesOverview of Community-Acquired Pneumonia in Adultsmayteveronica1000No ratings yet
- PneumoniaDocument35 pagesPneumoniaAlina Batalà100% (1)
- Lect 8 Pneumonia PDFDocument68 pagesLect 8 Pneumonia PDFRaghad AbdullaNo ratings yet
- Pneumonia Is A Serious Infection of The Lungs in Which The AirDocument1 pagePneumonia Is A Serious Infection of The Lungs in Which The AirErdem EzerNo ratings yet
- Pneumonia: Pneumococcus. A Serious Complication of Pneumonia, Pneumococcal Meningitis, Is AssociatedDocument7 pagesPneumonia: Pneumococcus. A Serious Complication of Pneumonia, Pneumococcal Meningitis, Is AssociatedHannah YtacNo ratings yet
- Focused Reviews: Pneumococcal Vaccination StrategiesDocument12 pagesFocused Reviews: Pneumococcal Vaccination StrategiesrafaelreanoNo ratings yet
- Overview of Community-Acquired Pneumonia in AdultsDocument78 pagesOverview of Community-Acquired Pneumonia in AdultsGuardito PequeñoNo ratings yet
- Community Acquired PneumoniaDocument7 pagesCommunity Acquired PneumoniaJoshuaOng100% (1)
- Signs and Symptoms: Community-Acquired Pneumonia (CAP) Is One of SeveralDocument12 pagesSigns and Symptoms: Community-Acquired Pneumonia (CAP) Is One of SeveralJohanna Fe Tadena ClerigoNo ratings yet
- Epidemiology, Pathogenesis, and Microbiology of Community-Acquired Pneumonia in AdultsDocument19 pagesEpidemiology, Pathogenesis, and Microbiology of Community-Acquired Pneumonia in AdultsRubén RodríguezNo ratings yet
- Microbiology:: Parasites (Parasitic Pneumonia)Document5 pagesMicrobiology:: Parasites (Parasitic Pneumonia)9t6vx7psm5No ratings yet
- Fungal Lung DiseaseDocument9 pagesFungal Lung DiseaseHipsipilasNo ratings yet
- Final Case Study of Cap EditDocument50 pagesFinal Case Study of Cap EditBem Bem Kai Hinoguin100% (1)
- CommunityDocument17 pagesCommunityRosemarie GonzalesNo ratings yet
- Wae'l Hayajneh: PneumoniaDocument14 pagesWae'l Hayajneh: PneumoniaRashed ShatnawiNo ratings yet
- PNEUMONIA Pathophysiology PDFDocument5 pagesPNEUMONIA Pathophysiology PDFMariaNo ratings yet
- ClinicalCases 6 0229Document5 pagesClinicalCases 6 0229jrnataNo ratings yet
- Tracker ListDocument10 pagesTracker ListJethro MamonongNo ratings yet
- Tracker ListDocument10 pagesTracker ListJethro MamonongNo ratings yet
- Laboratory Procedure Manual: UrineDocument30 pagesLaboratory Procedure Manual: UrinejrnataNo ratings yet
- Clin Infect Dis. 2012 Katz 1256 8Document3 pagesClin Infect Dis. 2012 Katz 1256 8jrnataNo ratings yet
- WHO HSE GAR DCE 2010.2 EngDocument6 pagesWHO HSE GAR DCE 2010.2 Engangelabety88No ratings yet
- SkoliosisDocument6 pagesSkoliosisRizki Muhammad RanandaNo ratings yet
- Diagnosis and Management of Pre-Eclampsia and EclampsiaDocument24 pagesDiagnosis and Management of Pre-Eclampsia and Eclampsiasyaifuddin07051989No ratings yet
- WHO HSE GAR DCE 2010.2 EngDocument6 pagesWHO HSE GAR DCE 2010.2 Engangelabety88No ratings yet
- Cureus 0008 000000000559Document8 pagesCureus 0008 000000000559jrnataNo ratings yet
- ReferenceDocument2 pagesReferencejrnataNo ratings yet
- Nej Mo A 0706873Document10 pagesNej Mo A 0706873jrnataNo ratings yet
- Duke Embryology - Gut DevelopmentDocument10 pagesDuke Embryology - Gut DevelopmentjrnataNo ratings yet
- Guidelines For Essential Trauma CareDocument106 pagesGuidelines For Essential Trauma CareTiago Miguel CaeiroNo ratings yet
- Nej Mo A 1404446Document11 pagesNej Mo A 1404446KikiNurAqidahNo ratings yet
- Anti Sperm Antibody As A Cause of Immunological Infertility in MalesDocument4 pagesAnti Sperm Antibody As A Cause of Immunological Infertility in MalesjrnataNo ratings yet
- Pediatric PneumoniaDocument12 pagesPediatric PneumoniaKrystal Migo Denolo ContrerasNo ratings yet
- Respiratory SystemDocument69 pagesRespiratory SystemVanitas CarteNo ratings yet
- What Is PneumoniaDocument15 pagesWhat Is PneumoniaKram Simon Sapongay100% (2)
- Diagnosa IcdDocument13 pagesDiagnosa IcdAnnisa Putri AbisekaNo ratings yet
- Pneumonia - PhysiopediaDocument5 pagesPneumonia - PhysiopediaudesaoilmillNo ratings yet
- PNEUMONIADocument44 pagesPNEUMONIAReshama JamankarNo ratings yet
- Case Study District Hospital - EtdDocument7 pagesCase Study District Hospital - EtdWan AmeeramirulzamanNo ratings yet
- Acute Respiratory Infection in ChildrenDocument16 pagesAcute Respiratory Infection in ChildrenDesi Riana PurbaNo ratings yet
- What Causes PneumoniaDocument6 pagesWhat Causes PneumoniaJorge SegoviaNo ratings yet
- Pneumonia Care Concept Map NUR 101Document1 pagePneumonia Care Concept Map NUR 101Jamie Waters100% (2)
- Pneumonia: Pneumonia Is An Inflammatory Condition of The Lung. It Is Often Characterized AsDocument13 pagesPneumonia: Pneumonia Is An Inflammatory Condition of The Lung. It Is Often Characterized AsBettina Gem M. PeñalosaNo ratings yet
- Microbiology Case Study Pneumonia EpidemidimiologyDocument4 pagesMicrobiology Case Study Pneumonia EpidemidimiologyArguend0No ratings yet
- Microbial Diseases of The Respiratory SystemDocument9 pagesMicrobial Diseases of The Respiratory SystemAnaNo ratings yet
- Updated: Dec 07, 2016 Author: Justina Gamache, MD Chief Editor: Guy W Soo Hoo, MD, MPHDocument42 pagesUpdated: Dec 07, 2016 Author: Justina Gamache, MD Chief Editor: Guy W Soo Hoo, MD, MPHgita suci arianiNo ratings yet
- Practice Essentials: Pediatric Pneumonia MedicationDocument56 pagesPractice Essentials: Pediatric Pneumonia MedicationAnonymous HgX3mN1oNo ratings yet
- PNEUMONIADocument3 pagesPNEUMONIAAssasination ClassroomNo ratings yet
- Respiratory Questions by DR - OkashaDocument96 pagesRespiratory Questions by DR - Okashamohammed okashaNo ratings yet
- Daftar Penyakit Kompetensi 4ADocument12 pagesDaftar Penyakit Kompetensi 4ARoy Sandy PermanaNo ratings yet
- Catálogo Fast Track 2017Document10 pagesCatálogo Fast Track 2017rolan.olivaresNo ratings yet
- Bruyere Case13 001-012 DSDocument11 pagesBruyere Case13 001-012 DSjrnataNo ratings yet
- Case Presentation FinalDocument115 pagesCase Presentation FinalMildred ZNo ratings yet
- PneumoniaDocument18 pagesPneumoniaFryam Bells100% (1)
- Bacteria Causing Respiratory Tract Infections: Damanhour University Faculty of PharmacyDocument7 pagesBacteria Causing Respiratory Tract Infections: Damanhour University Faculty of Pharmacyزياد محمدNo ratings yet