Professional Documents
Culture Documents
(RADIO 250) LEC 07 Musculoskeletal Radiology
Uploaded by
William PinzonOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
(RADIO 250) LEC 07 Musculoskeletal Radiology
Uploaded by
William PinzonCopyright:
Available Formats
RADIO 250: ICC in Radiology and Nuclear Medicine
LEC 07: MUSCULOSKELETAL RADIOLOGY
Exam 01| Radiology Consultants | August 28, 2013
OUTLINE
I. General Anatomy
II. Trauma
A. Clinical
B. Long Bone Fractures
C. Salter-Harris
D. Avulsion
E. Stress
F. Pathologic
G. Absence/Displacement of
Fat Pad
H. Pelvic Fractures
I. Healing of Fractures
III. Bone Infection
A. Septic Arthritis
B. Osteomyelitis
C. TB Arthritis
D. Potts Disease
IV. Arthritides
A. Joint Space Changes
B. Subchondral Bone Changes
C. Periarticular Soft Tissue
Changes
V. Bone Tumors
VI. Cases
Figure 2. Sagittal section of bone showing the different layers
C. Anatomy of the Knee
For higher learning! This is what was lectured to 2015 last year, versus what
was lectured to us na parang overview and general concepts. Na-preformat
na rin e, so might as well upload it :))
I. GENERAL ANATOMY
A. Anatomy of Long Bones
Diaphysis shaft
Epiphysis one end of the long bone
Metaphysis growth plate region
o Fracture in this area will halt bone development
Articular cartilage coats joint surfaces, acts as a friction and
shock absorber
Figure 3. X-ray of knee on PA showing patella and tibiofemoral joint space;
lateral view showing the patellofemoral joint space
Things to Remember
In reading basic x-rays of appendicular bones, assess the following:
Are the cortical outlines intact?
Are the joint spaces maintained?
Are there lytic or sclerotic changes?
Are the soft tissues unremarkable?
D. Anatomy of the Spine
Figure 1. X-ray film and drawing of a long bone showing the epiphysis,
metaphysis and diaphysis.
NICE TO KNOW
Growth balls
o Filled with pituitary glands of horses
o Have it done on or before age 15
B. Layers in Bones
Medulla marrow cavity
Endosteum lining marrow cavity
Cortex dense bone
Periosteum
o Covers bone and not cartilage
o Fibrous layer
o Osteogenic layer with bone cells and blood vessels for
nourishment and repair
Figure 4. Normal radiograph of cervical spine in PA and lateral. Note that
vertebral bodies and intervening IV disc spaces are usually even in all
segmental levels. Other structures seen are the pedicles, which are an
important site for metastasis, and the posterior elements which include the
spinous process
Things to Remember
In reading basic x-rays of the spine, assess the following:
Are the vertebral bodies, their pedicles and posterior elements
intact?
Are the intervertebral disc spaces maintained?
Are there lytic or sclerotic changes?
Are the alignment and curvature maintained?
Are the soft tissues unremarkable?
II. TRAUMA
A. Clinical
Clinical assessment:
1. Bone Deformity
2. Instability/ Crepitations
BLESSIE, KARINA, JOW, TATO
UPCM 2016 7: XVI, Walang Kapantay!
1 of 11
RADIO 250
LEC 07: MUSCULOSKELETAL RADIOLOGY
3. Point Tenderness
To adequately assess trauma through radiograph, two views should
be requested: AP and lateral
1. Fracture at shaft includes joints at both ends
2. Fracture at epiphysis/metaphysic get details of adjacent joint
and soft tissue
B. Long Bone Fractures
Break in bone/cartilage
Fracture Nomenclature
Degree
Location
Type
Position
Alignment
Apposition
Complete, incomplete as well as open/ closed
proximal, middle ,distal third
spiral, oblique, transverse, comminuted, impacted
relation of distal to proximal segment
anterior, posterior, medial or lateral angulation (give
the degree)
proportion to proximal shaft; say if overlapping
Rotation
Internal or external
Figure 8. Supracondylar (metaphyseal) fracture. Complete oblique fracture of
the mid shaft or diaphysis of the right ulna
Type
Spiral fracture: slightly angulated fracture relative to the long axis,
meaning the angle of the fracture line is less than 45 degrees with
the axis of the bone
Oblique fracture: more angulated, meaning more than 45 degrees
with the axis of the bone
Transverse fracture: perpendicular to the axis of the bone
Degree
Complete
Both cortices are involved
Involves the complete cortex, may it be displaced or undisplaced
Figure 9. Left, spiral fracture. Right, oblique fracture
Figure 5. L, a complete transverse fracture of the mid-diaphysis of the
femure. R, bilateral complete oblique fractures of the distal radial and ulnar
diaphysis.
Incomplete
Break in only one side; break in the continuity in the cortical
outline
A common example of an incomplete fracture found in the
pediatric age group is a greenstick fracture
Does not extend across entire width of bone; Stable
Figure 10. Transverse fracture.
Other more complex fracture types include:
Comminuted fracture: more than two fragments produced from
the same bone
Segmental fracture: isolated segment of the involved bone
Figure 6. Incomplete fracture of the distal diaphysis of the radius.
Location
Epiphysis, diaphysis, or metaphysis
Figure 11. Comminuted (2L), Segmental fracture (2R).
Figure 7. Mid shaft (diaphyseal) fracture. Complete transverse fracture of the
diaphyseal or mid shaft aspect of the right radius
BLESSIE, KARINA, JOW, TATO
Alignment
relation of the distal fractured segment relative to the more
proximal segment of the bone; anterior, posterior, medial or
lateral angulation (give the degree)
UPCM 2016 7: XVI, Walang Kapantay!
2 of 11
RADIO 250
LEC 07: MUSCULOSKELETAL RADIOLOGY
Usually it has normal x-ray in almost 90% of cases but the
abnormality usually sets in after 10-20 days and presents as
periosteal reaction or even just a minor break.
Figure 12. Fractures can be a) with no deviation between the proximal and
distal fractured segments; b) lateral deviation of the distal fractured
segment with the proximal, or; c) a medially-displaced fractured segment
relative to the proximal segment.
Figure 16. Stress fracture.
Apposition
F. Pathologic Fracture
Abnormal mineralization
Normal to minimal stress
Usually abnormal from the start
Metabolic diseases, Metastasis
Figure 13. With regards to apposition of the displaced fractured segments,
displacement can be a) of the shaft width; b) one full shaft width; c)
overlapping, or; d) distracted, if the segments are fully separated but in the
same axis
C. Salter-Harris Classification
One of the most commonly used classification of fractures
especially for the pediatric age
Used for fractures in relation to extension to the epiphyseal plate
Figure 17. Pathologic fracture.
G. Absence/Displacement of Fat Pad
absence of fat pad can indicate presence of hemarthrosis or
hematoma formation
displacement of fat pad usually seen in supracondylar fractures
o Usually, it forms triangular hypodensity beside the bone
involved due to presence of hematoma or blood above the
periosteum.
Figure 14. Different types of Salter-Harris fracture. Type 1 growth plate
only; Type 2 -- growth plate plus the metaphyseal extension; Type 3 growth
plate plus the epiphyseal region; Type 4 is epiphyseal and metaphyseal
involvement and; Type V is a crushed growth plate.
Figure 18. Left, absence of fat pad. Right, displacement of fat pad
H. Pelvic Fractures
D. Avulsion Fracture
fragment of bone pulled away at the site of ligament or tendon
attachment
Also known as chip fracture
Figure 15. Avulsion fracture.
E. Stress Fracture
produced in bones with normal mineralization but with exposure
to repetitive prolonged stress or muscular action to bones that
have not accomodated itself to such action
BLESSIE, KARINA, JOW, TATO
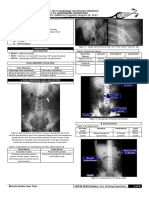
Figure 19. X-ray showing fracture of pubic rami & an oblique fracture of
sacrum
Open Book/Straddle Pelvic Injury
UPCM 2016 7: XVI, Walang Kapantay!
3 of 11
RADIO 250
LEC 07: MUSCULOSKELETAL RADIOLOGY
Figure 20. X-ray films showing opening of pubic symphysis & fracture of the
sacroiliac joints causing anterior compression.
Hip Dislocation
Posterior more common
Figure 23. Impacted fracture through the neck of the right femur
Avascular Necrosis
Could be due to loss of blood supply and common chronic steroid
use
The more proximal the fracture is, the higher the chances of AVN
Figure 21. X-ray film showing a fracture of the posterior rim of the
acetabulum. The femoral head is displaced superiorly.
Proximal Femoral Fracture
Figure 24. Avascular Necrosis
I. Healing of Fractures
Figure 22. Femoral fractures can either be subcapital, which is just below the
head; transcervical which is the anatomic neck; intertrochanteric which is
between the greater and lesser trochanters, and; subtrochanteric which is
below the trochanters.
Figure 25. Diagram of the different phases of the physiology of fracture
healing
INJURY
2 WEEKS
3 MONTHS
6 MONTHS
Figure 26. Diagram showing the different phases of the radiology of fracture
healing. From periosteal callus, it becomes periosteal and endosteal callus.
Figure 22.5. Proximal femoral fracture
Impacted Femoral Head
BLESSIE, KARINA, JOW, TATO
Remodelling
Callus
o immature (fiber) bone replaced by adult (lamellar) bone which
is stronger
Stress initiates remodeling
o Cortical bone and medullary bone continuous
When Fracture is Healed
Clinical union
o No tenderness and bear weight/use the extremity
o Earlier than disappearance of fracture line
UPCM 2016 7: XVI, Walang Kapantay!
4 of 11
RADIO 250
LEC 07: MUSCULOSKELETAL RADIOLOGY
Amount of callus is guide when to remove cast depending on
location
o Solid & mature callus with continuous margins in L.E.
Trabecular pattern across fracture
10 to 12 days between onset of clinical symptoms & radiographic
bone changes
Bone scan very sensitive (almost 80% of cases will be positive in
24 hours and as high as 90% of cases in 72 hours of infection)
The initial manifestation of acute osteomyelitis is usually swelling
of the overlying soft tissue of the area involved.
Further progression usually after 10-12 days will show minimal
periosteal reaction which will progress to further destruction of
the bone shown as areas of lysis of the involved bone.
Figure 27. Left, film showing poor healing of fracture, note misalignment.
Right, good healing of fracture; note trabecular pattern
Signs and Types of Non-Union
Smooth margins of the fracture
No peripheral callus at expected time
Ends undergo increasing sclerosis
Pseudoarthrosis
Figure 28. Picture showing the different types of non-union: hypertrophic
(elephant foot and horse hoof), oligotrophic, atrophic, infected.
Subluxation vs. Dislocation
Figure 31. Bone scan of osteomyelitis
Figure 32.Osteomyelitis
Subacute and Chronic Osteomyelitis
Involucrum & sequestrum formation
o Sequestra -> Avascular areas of dense bone surrounded by
zones of rarefaction or lucency
o Involucrum -> Shell of bone that surrounds & encloaks
sequestrum
Thickened bone with wavy sclerotic cortex & lucent areas
Medullary cavity may not be apparent
Reactivation Soft tissue swelling,new areas of periosteal newbone formation, development of sharply defined radiolucent
cavities
Figure 29. Drawing showing subluxation and dislocation.
Figure 30. X-ray films showing Boehlers angle.
Figure 33. Involucrum and Sequestra
III. INFECTION
A. Osteomyelitis
Acute osteomyelitis
Subacute and chronic osteomyelitis
Tuberculous osteomyelitis
Acute Osteomyelitis
For the initial days of infection, a radiograph wouldnt be of help
much except possibly on the soft tissue swelling.
BLESSIE, KARINA, JOW, TATO
Figure 34. In this film, chronicity was manifested as a thick periosteal
reaction as well as intense sclerosis of the bony segment
UPCM 2016 7: XVI, Walang Kapantay!
5 of 11
RADIO 250
LEC 07: MUSCULOSKELETAL RADIOLOGY
Figure 35.Thickened bone with wavy sclerotic cortex; medullary cavity may
not be apparent
B. Septic Arthritis
Figure 40-41. TB arthritis of the (L) hip joint and (R) knees
E. Infectious Spondylitis
Hematogenous
End plate -> disc -> end plate
Posterior elements rarely involved by infection
Confined to one interspace
Subacute infection
Paraspinous soft-tissue masses not as large as seen with
tuberculosis
Earliest sign is decrease disc height
Often has sclerotic margin
Figure 36.Septic arthritis at distal joint
Figure 37. Septic arthritis of the knees (irregular breaks of the cortex) with
soft tissue swelling
Figure 42.Infectious spondylitis
C. Bone Abscess
Brodies abscess
Sharply outlined area of rarefaction or lucency in metaphysis
surrounded by irregular dense sclerosis
Thickened overlying cortex
Figure 43. Radiographic findings: narrowing disc space, erosion and
destruction of the vertebral endplates, small paravertebral soft tissue mass
Figure 38. Septic arthritis of the knees (irregular breaks of the cortex) with
soft tissue swelling
D. Tuberculous Spondylitis/Potts Disease
Spread beneath paraspinous ligaments
Greater tendency than infectious spondylitis to spread along spine
Irregular erosions or smooth, saucerized defects of anterior
borders of vertebral bodies
Extensive paravertebral soft-tissue masses with calcifications
Bony ankylosis indistinct outlines of contiguous vertebrae with
no intervening disc spaces
Gibbus deformity seen as a sharp portion
Figure 39. Periosteal reaction to Brodies abscess
D. TB Arthritis
Insidious and has time to remodel, hence it is considered benign
Figure 44. Potts disease; irregular erosions of anterior portions of vertebral bodies
BLESSIE, KARINA, JOW, TATO
UPCM 2016 7: XVI, Walang Kapantay!
6 of 11
RADIO 250
LEC 07: MUSCULOSKELETAL RADIOLOGY
Figure 48. Joint space widening on Xray
Figure 45.Potts disease; mixed lytic sclerotic changes in the vertebral bodies
and extensive paravertebral soft tissue mass
Joint Space Narrowing
Destruction of articular cartilage by proteolytic enzymes, pannus
affecting cartilage nutrition, or by wear-and- tear
Early in pyogenic arthritis (7 to 10 days from onset of disease)
Late in TB arthritis, Rheumatoid Arthritis (RA), Osteoarthritis (OA)
Figure 46.Potts disease; Gibbus deformity
Figure 49. OA is usually associated with osteophyte formation and with
subchondral sclerosis.
Figure 47.Potts disease; myelogram
Pyogenic spondylitis
Subacute infection
Confined to one interspace
Smaller paraspinous softtissue masses
Tuberculous spondylitis
Chronic infection
Multiple disc level involvement
Extensive paravertebral soft-tissue
masses with calcifications
IV. ARTHRITIDES
A. Joint Space Changes
Joint Space Widening
Joint effisuion or inflammatory exudates
Early pyogenic arthritis
Figure 50. RA showing symmetric bilateral joint space narrowing
Obliteration/Ankylosis
Further destruction and narrowing of the joint space can lead to
ankylosis or obliteration of the joint space
Complete destruction of articular cartilage with bridging of bone
trabeculae at the ends of bone
Rheumatoid arthritis, pyogenic arthritis
Figure 50. In RA there is symmetric ankylosis of both acetabulofemoral joint
space in an axial direction
BLESSIE, KARINA, JOW, TATO
UPCM 2016 7: XVI, Walang Kapantay!
7 of 11
RADIO 250
LEC 07: MUSCULOSKELETAL RADIOLOGY
TB arthritis, Rheumatoid arthritis
Figure 55. RA causing periarticular osteoporosis shown on Xray
Figure 51. In pyogenic arthritis, this joint space ankylosis is usually coupled
with severe sclerosis
Subchondral Sclerosis/Eburnation
Increase in density of the subchondral surface of bone due to
hypervascularity
Osteoarthritis
B. Subchondral Bone Changes
Central Erosion
from destruction by proteolytic enzymes of the bacteria
pyogenic arthritis
Figure 56. Sclerosis is the high opacity changes indicated by the arrows
Spur Formation
Due to capsular traction at the peripheral margins of the joint
Figure 52. Central erosion here in the subchondral bone of the 2nd
metacarpal bone (L) as well as the distal middle phalanx (R). Both are with
surrounding soft tissue swelling.
Peripheral Erosions Eventually Becoming Central
Bone destruction by pannus formation
TB arthritis, Rheumatoid arthritis
Figure 53. RA starting at the periphery, gradually eating into the bone
Periarticular Erosion
Gout (Punched-out defects)
Monosodium urate crystal deposition
Figure 57. Soft tissue swelling at the distal portions of the fingers (Heberdens
nodes). Xray of this would show the osteophyte formation. Seen at the
periarticular portions of the bones with associated joint space narrowing, soft
tissue swelling and subchondral sclerosis. Eburnation is the degeneration of
bone into a hard, ivorylike mass, such as occurs at articular surfaces of bones
in osteoarthritis.
Figure 54. Periarticular erosions on the other hand usually can be seen in
gouty arthritis. Here we have well-defined periarticular erosions often
described as rat-bitten erosions. Further progression of the disease will show
the well-defined erosions almost involving all bones. Lastly as the disease
becomes chronic we can see that there is almost complete absence of the
bones due to erosions, now with early tophi or tophaceous formation
Cyst Formation
more pronounced in larger joints
osteoarthritis
Periarticular Osteoporosis
Local demineralization of bone adjacent to the involved joint
Response to hyperemia provoked by synovial inflammation or
secondary to disuse
BLESSIE, KARINA, JOW, TATO
UPCM 2016 7: XVI, Walang Kapantay!
8 of 11
RADIO 250
LEC 07: MUSCULOSKELETAL RADIOLOGY
Figure 61. OA and RA characteristic location in the hand.
Figure 58. Cyst formation seen as round lucencies in the larger joints
C. Periarticular Soft Tissue Changes
Soft Tissue Swelling
Pyogenic arthritis, rheumatoid arthritis (characteristically
fusiform)
Often earliest sign
Accumulation of synovial inflammatory tissue
Increase in intra-articular fluid
Capsular distention
Surrounding soft tissue edema
Figure 62. In OA, we have a superior displacement of the femoral head on the
left with joint space narrowing and subchondral sclerosis. On the right side,
the findings are not so overt compared to the left showing asymmetry of
findings. In TB arthritis, similarly, there is unilateral involvement of the knee
joint. In fact, given a unilateral arthritis or a single joint of involvement,
infection must be ruled out prior to any other forms of arthritides. In RA,
there is axial displacement of the femoral head bilaterally with narrowing of
the joints in a symmetric fashion. There is less sclerosis here in this film
compared to OA.
V. BONE TUMORS
Few benign and malignant tumors have pathognomonic
radiographic findings
Most of the radiographic findings are suggestive of the
aggressiveness of the tumor rather than indicating whether a
mass is benign or malignant
Figure 59. Changes in the periarticular soft tissue usually presents as soft
tissue swelling in most cases. This can be seen in pyogenic arthritis and
rheumatoid arthritis (characteristically fusiform). Often earliest sign, this is
usually secondary to accumulation of synovial inflammatory tissue as seen on
this picture as well as Increase in intra-articular fluid leading to capsular
distention and surrounding soft tissue edema. On radiograph this is seen as a
symmetric soft tissue density surrounding the joints of involvement.
Soft Tissue Masses
Gouty arthritis Tophi
Often contain flecks of calcification
Margins of the joints of the foot , hand , bursae (olecranon bursa)
Figure 60. Presence of soft tissue masses in arthritis can be seen in gouty
arthritis in the form of tophi. This often presents as flecks of calcifications in
the surrounding soft tissue on xray as seen in the left hand xray with
periarticular erosions. Further erosions and crystal deposition can lead to
tophi formation as seen.
A. Diagnostic Criteria
Age of patient
Location of lesion
Specific bone
Cortical integrity
Behavior of Lesion/ characteristics of internal margin
Periosteal new-bone formation
Tumor matrix calcification
Soft tissue and joint changes
Age of Patient
Infant Metastatic neuroblastoma
1st and 2nd decade Ewings tumor
2nd and 3rd decade Osteosarcoma and Ewings tumor
After 40 year old Metastatic carcinoma, Multiple myeloma, and
Chondrosarcoma
Location of Lesion
Epiphyses GCT, Chondroblastoma
Metaphyses Most benign and malignant bone tumors;
metabolic activity
Diaphysis Tumors of bone marrow origin such as Ewings tumor,
Non Hogdkins lymphoma, & Multiple myeloma
D. Distribution of Joint Involvement
OSTEOARTHRITIS
RHEUMATOID
ARTHRITIS
LOCATION
DISTAL JOINTS
PROXIMAL JOINTS
# JOINTS INVOLVED POLYARTICULAR
POLYARTICULAR
SYMMETRY
ASYMMETRICAL
SYMMETRICAL
*MONOARTICULAR: TB ARTHRISTIS, JUVENILE RA
BLESSIE, KARINA, JOW, TATO
UPCM 2016 7: XVI, Walang Kapantay!
9 of 11
RADIO 250
LEC 07: MUSCULOSKELETAL RADIOLOGY
Osteoblastic - increased density seen in Blastic Metastasis,
osteosarcoma and Pagets Disease)
Mixed combination of lytic and blastic patterns usually seen
in mixed metastasis
Figure 63. Giant cell tumor and aneurysmal bone cyst located at the
epiphyseal areas.
Specific Bone
Posterior elements of the vertebra Osteoblastoma
Tibia Adamantinoma
Sternum rarely benign
Patella more often benign
Cortical Integrity
Figure 64. In terms of cortical integrity, we can have either thinning,
thickening, expansion and destruction. In GCT, we have thinning, expansion
and destruction. In OF, we have thickening of the cortex as seen on this film.
Figure 66. X ray films showing the different types of lesions.
Periosteal Reaction
Lamellar periosteal reaction
o Eosinophilic granuloma
o Single layer of new bone thicker than 1 mm of uniform density
o Hallmark of a benign process
Layered or laminated periosteal reaction
o Several parallel concentric layers of periosteal new bone
o onionskin reaction
o Implies a more aggressive process
o Ewings tumor
Figure 65. In NOF, we have a well-defined defect in the proximal tibia, both
cortical thinning and expansion. In osteosarcoma of the left femur presenting
with this calcified mass, we have cortical thickening expansion and
destruction. In fibrous dysplasia, which is increase in fibrous matrix of bone
with expansion in the process, we can have both thickening and expansion of
the bone.
Behavior of Lesion
The behavior of the lesion can be observed using the tumorbone interface also known as the transition zone.
Relates to the aggressiveness of a tumor
Osteolytic - lucencies
o Geographic solitary, >1cm, well-demarcated lesions
o Moth-eaten multiple, poorly marginated, small or
moderately sized (2-5mm) lucencies with a punched out
pattern (aka moth eaten)
o Permeative Numerous tiny pinhole-size lucencies (>1mm)
BLESSIE, KARINA, JOW, TATO
Figure 67. Lamellar periosteal reaction (L); Onionskin (R)
Hair-on-end periosteal reaction
o Bony spicules perpendicular or divergent from the cortex
Sunburst periosteal reaction
o Difference with Hair-on-end depends on how much bone is
involved in the process (rad.washington.edu)
UPCM 2016 7: XVI, Walang Kapantay!
10 of 11
RADIO 250
LEC 07: MUSCULOSKELETAL RADIOLOGY
Case 2: Rheumatoid arthritis periarticular osteopenia and
narrowing of the radioulnar, radiocarpal, intercarpal,
carpometacarpal joints (ulnar deviation)
Figure 68. Hair on end (L), Sunburst appearance (R)
Tumor Matrix
Chondroid - punctate, popcorn like, arcs of calcific density
Osteoid - cloud like, amorphous, homogenous opacity
Case 3. Acute osteomyelitis thick amorphous periosteal reaction
of the proximal thirds of the radius and ulna with lytic changes seen
as well as gross overlying soft tissue swelling
VII. METABOLIC DISEASES
Osteogenesis Imperfecta
Acromegaly
Figure 69. Chondrosarcoma (Chondroid), Osteosarcoma/blastoma (Osteoid)
VI. CASES
Osteoporosis
Case 1: Complete transverse fracture of the mid diaphysis of the left
femur with lateral deviation of the distal fractured segment and
overlying soft tissue swelling
END
BLESSIE, KARINA, JOW, TATO
UPCM 2016 7: XVI, Walang Kapantay!
11 of 11
You might also like
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceFrom EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceRating: 4 out of 5 stars4/5 (895)
- Never Split the Difference: Negotiating As If Your Life Depended On ItFrom EverandNever Split the Difference: Negotiating As If Your Life Depended On ItRating: 4.5 out of 5 stars4.5/5 (838)
- (RADIO 250) LEC 03 Genitourinary and KUB ImagingDocument7 pages(RADIO 250) LEC 03 Genitourinary and KUB ImagingWilliam PinzonNo ratings yet
- (RADIO 250) LEC 06 Chest RadiologyDocument10 pages(RADIO 250) LEC 06 Chest Radiologyjmhinos4833No ratings yet
- (RADIO 250) LEC 01 Introduction To Radiology + Radioprotection PDFDocument4 pages(RADIO 250) LEC 01 Introduction To Radiology + Radioprotection PDFjmhinos4833No ratings yet
- (RADIO 250) LEC 10 Radiation OncologyDocument3 pages(RADIO 250) LEC 10 Radiation OncologyWilliam PinzonNo ratings yet
- (RADIO 250) LEC 08 Introduction To Interventional RadiologyDocument4 pages(RADIO 250) LEC 08 Introduction To Interventional RadiologyWilliam PinzonNo ratings yet
- (RADIO 250) LEC 12 Abdominal RadiologyDocument8 pages(RADIO 250) LEC 12 Abdominal RadiologyWilliam PinzonNo ratings yet
- (RADIO 250) LEC 11 Nuclear MedicineDocument7 pages(RADIO 250) LEC 11 Nuclear MedicineWilliam Pinzon100% (1)
- ACLS 2013 Pocket Brain Book 5thDocument85 pagesACLS 2013 Pocket Brain Book 5thWilliam PinzonNo ratings yet
- The Yellow House: A Memoir (2019 National Book Award Winner)From EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Rating: 4 out of 5 stars4/5 (98)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeFrom EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeRating: 4 out of 5 stars4/5 (5794)
- Shoe Dog: A Memoir by the Creator of NikeFrom EverandShoe Dog: A Memoir by the Creator of NikeRating: 4.5 out of 5 stars4.5/5 (537)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaFrom EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaRating: 4.5 out of 5 stars4.5/5 (266)
- The Little Book of Hygge: Danish Secrets to Happy LivingFrom EverandThe Little Book of Hygge: Danish Secrets to Happy LivingRating: 3.5 out of 5 stars3.5/5 (400)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureFrom EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureRating: 4.5 out of 5 stars4.5/5 (474)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryFrom EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryRating: 3.5 out of 5 stars3.5/5 (231)
- Grit: The Power of Passion and PerseveranceFrom EverandGrit: The Power of Passion and PerseveranceRating: 4 out of 5 stars4/5 (588)
- The Emperor of All Maladies: A Biography of CancerFrom EverandThe Emperor of All Maladies: A Biography of CancerRating: 4.5 out of 5 stars4.5/5 (271)
- The Unwinding: An Inner History of the New AmericaFrom EverandThe Unwinding: An Inner History of the New AmericaRating: 4 out of 5 stars4/5 (45)
- On Fire: The (Burning) Case for a Green New DealFrom EverandOn Fire: The (Burning) Case for a Green New DealRating: 4 out of 5 stars4/5 (74)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersFrom EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersRating: 4.5 out of 5 stars4.5/5 (345)
- Team of Rivals: The Political Genius of Abraham LincolnFrom EverandTeam of Rivals: The Political Genius of Abraham LincolnRating: 4.5 out of 5 stars4.5/5 (234)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreFrom EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreRating: 4 out of 5 stars4/5 (1090)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyFrom EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyRating: 3.5 out of 5 stars3.5/5 (2259)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)From EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Rating: 4.5 out of 5 stars4.5/5 (121)
- Her Body and Other Parties: StoriesFrom EverandHer Body and Other Parties: StoriesRating: 4 out of 5 stars4/5 (821)
- The Science and Physiology of Flexibility and StretchingDocument45 pagesThe Science and Physiology of Flexibility and Stretchingandikhg1971100% (1)
- Prosthetic Alignment of TTDocument11 pagesProsthetic Alignment of TTanjelikaNo ratings yet
- Activity Mobility ExerciseDocument27 pagesActivity Mobility ExerciseMary SutingcoNo ratings yet
- Common Injuries of The Musculoskeletal SystemDocument4 pagesCommon Injuries of The Musculoskeletal SystemJoniele Angelo AninNo ratings yet
- Upper Limb ChartDocument6 pagesUpper Limb ChartDianeLumintooNo ratings yet
- The Woman's Set KriyaDocument9 pagesThe Woman's Set KriyaAvi MagiNo ratings yet
- Skeleton WorksheetDocument4 pagesSkeleton WorksheetNalendra UjiNo ratings yet
- HVT With Lumbar Disc HerniationDocument12 pagesHVT With Lumbar Disc HerniationSheena McLennanNo ratings yet
- Injuries From Ultimate Frisbee: Wisconsin Medical Journal Wisconsin Medical JournalDocument5 pagesInjuries From Ultimate Frisbee: Wisconsin Medical Journal Wisconsin Medical JournalDiana Malena RodriguezNo ratings yet
- Yoga Preparatory MovementsDocument20 pagesYoga Preparatory MovementsnkbarwakhtNo ratings yet
- Physio Pretest Q-150Document30 pagesPhysio Pretest Q-150Deepa Seira50% (2)
- Cranial CavityDocument23 pagesCranial Cavityamae85No ratings yet
- Dr. Niranjan Murthy H L: Asst. Prof., Dept. of Physiology Sree Siddhartha Medical College & Hospital, TumkurDocument29 pagesDr. Niranjan Murthy H L: Asst. Prof., Dept. of Physiology Sree Siddhartha Medical College & Hospital, Tumkurnirilib100% (6)
- Lowerlimb (LEG) : Chary Jaztine L. MangacopDocument15 pagesLowerlimb (LEG) : Chary Jaztine L. MangacopChary JaztineNo ratings yet
- Skeletal Muscle AnatomyDocument6 pagesSkeletal Muscle Anatomyydnic alykPNo ratings yet
- Dermoneuromodulation Treatment Manual: Self-Published June 2007 by Diane Jacobs, PTDocument57 pagesDermoneuromodulation Treatment Manual: Self-Published June 2007 by Diane Jacobs, PTXavier De Haro MiretNo ratings yet
- 40th Annual Percivall Pott Scientific MeetingDocument26 pages40th Annual Percivall Pott Scientific MeetingAlex Mulligan100% (1)
- B.P.Ed. Third Semester (CBS) Examination Sports Medicine Physiotherapy and Rehabilitation (Elective Course)Document6 pagesB.P.Ed. Third Semester (CBS) Examination Sports Medicine Physiotherapy and Rehabilitation (Elective Course)Devashish SahasrabudheNo ratings yet
- Part1 WHOStandardAccupuncturePointLocationsDocument39 pagesPart1 WHOStandardAccupuncturePointLocationsJiman Ryu100% (1)
- Autopsy of MR PickleDocument9 pagesAutopsy of MR Pickleapi-309178195No ratings yet
- Rehabilitation of The Elbow: Melanie StevensDocument27 pagesRehabilitation of The Elbow: Melanie StevensMelanie StevensNo ratings yet
- Closed Fracture of Left Femoral Neck: Case ReportDocument31 pagesClosed Fracture of Left Femoral Neck: Case Reporttari nurulNo ratings yet
- Nursing Care of Patient With Musculoskeletal DisordersDocument11 pagesNursing Care of Patient With Musculoskeletal Disordersjashwanee100% (2)
- Tema 4 - Standing, Sitting PosDocument18 pagesTema 4 - Standing, Sitting PosAndreea ProdescuNo ratings yet
- LDDDDocument21 pagesLDDDIvha RifaiNo ratings yet
- Basic Taekwondo Techniques and TerminologyDocument111 pagesBasic Taekwondo Techniques and TerminologyGabriel FariaNo ratings yet
- Carti Bone Juice BrocherDocument4 pagesCarti Bone Juice BrocherOs MohamedNo ratings yet
- Hegedus 2012Document16 pagesHegedus 2012jose perezNo ratings yet
- Assesssment For Quality of Movement - SifaDocument7 pagesAssesssment For Quality of Movement - Sifasrimliati2906No ratings yet
- Mandibular MovementsDocument36 pagesMandibular MovementsRagini ShravanNo ratings yet