Professional Documents
Culture Documents
A&P2E1 StudyGuide
Uploaded by
fatimajafar2003Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
A&P2E1 StudyGuide
Uploaded by
fatimajafar2003Copyright:
Available Formats
3/26/2010
Page 1
Anatomy and Physiology II Exam 1 Review
1.
Mix and Match the endocrine gland location with their name
from the mix and match list
2.
What glands produce steroid hormones and what glands produce
protein type hormones? Which gland produces amino acid
hormones that are fat soluble and cross cell membranes.
What glands produce fat soluble hormones and what is
the significance of hormones being fat soluble?
Gland
Hypothalamus
Pituitary
Pineal
Thyroid
Parathyroid
Thymus
Adrenal
Pancreas
Digestive System
Testes / Ovaries
3.
Hormone Type
Peptide
Protein
Peptide
Amino acid
Amino acid
Peptide
Peptide
Steroids
Amino acid
Protein
Protein & Peptide
Steroid (One Protein
in ovaries)
Fat Soluble
No
No
No
No
(T3 & T4)Yes
No
No
Yes
No
No
No
Steroid Yes
Protein No
Both nerves and hormones produce signals that control body
function. Contrast the signals from nerves and hormones
with respect to their speed and how long the affects of the
signal last.
Hormones: Responses take longer then to nerve signals,
duration is also longer. Used for slow responses like
onset of puberty.
Nerve signals: Responses are rapid, duration is very short
like a pain signal. Used for rapid response with a
short duration.
4.
Explain in detail how protein or steroid type hormones work
at the cellular level.
Steroid:
Fat soluble and readily crosses cell membranes.
Produced by:
o Adrenal cortex
o Testes
o Ovaries
o The thyroid hormones (T3 & T4) also work like steroid
hormones
3/26/2010
Page 2
work:
Move across cell membrane and into nucleus of cell
Bond with protein receptors in nucleus
The steroid-protein complex then bonds with regulatory
segments on the DNA and acts by turning genes on/off.
This causes them to control the synthesis of proteins.
Protein (also amino acid & peptide):
Long chains of amino acids, not fat soluble
Produced by:
o Anterior pituitary
o Pancreas
o Digestive System
o Ovaries(one only)
How work:
o Hormone bonds to G-protein receptor site on cell
membrane
o Adenylate cyclase is activated, convertes ATP to CAMP. NOTE: cyclic guanosine monophosphate (C-GMP) is
another secondary messenger used by some hormones.
o C-AMP activates Kinase A
o Kinase A catalyzes the addition of phosphates to
enzymes, activating the enzyme in the cell
o The activated enzyme changes the cell functions
o The enzyme calmodulin is also activated and it
converts the C-AMP back to ATP, aiding in stopping the
effect of the hormone.
5.
How
o
o
o
For the following hormones, know where they are produced,
the target tissues they affect, what effects they have, and
how they are regulated. Know the hormone related diseases
and their symptoms.
Pituitary gland and Hypothalamus gland interaction
Anterior
Pituitary
Gland
hGH
Hypothalamus
Release
Trigger
GHRH
Hypothalamus
Inhibition
Trigger
GHIH
FSH + LH
GnRH
GnRH
Tissue
And
Effect
Blood sugar
levels,
protein
synthesis,
etc.
Body
maturation,
follicle
development
in ovaries,
sperm
production
in testes
Diseases
Dwarfism,
Giantism,
Acromegaly
3/26/2010
PRL
Page 3
PRH
PIH
Initiates
milk
production
in women,
unclear in
men
Other pituitary gland hormones
Pituitary
TSH (anterior)
ACTH (anterior)
MSH (anterior)
Oxytocin/OT
(Posterior)
ADH (Posterior)
Effect
Thyroid increases
production of T3& T4
hormones
Adrenal cortex gland
to release
glucocorticoids
(cortisol,
cortisone, and
corticosterone)
Melanocytes increase
productivity of
melanin
Contracts uterus
during birth,
contracts mammary
glands during breast
feeding
Causes body to
retain water (blood
plasma).
Notes
Triggered by UV
exposure.
Disease:
Diabetes Insipidus
3/26/2010
Page 4
[gland] Hormone
[pineal]
Melatonin
Effect
High levels help
you go to sleep
Releaes
Night: Darkness
reduces the
levels of
norepinephrine,
reducing the
inhabitation of
melatonin
[Thyroid]
T3& T4
basal metabolic
rate & O2 usage
cellular
metabolism
growth &
development
use of glucose
for ATP creation
protein
synthysis
actions of
epinephrine &
norepinephrine
through up
regulation of
beta receptors
blood Ca++ and
HPO42- lvls
Activity of
osteocytes (bone
production)
Activity of
osteoclasts (bone
Trigger: Low
blood levels of
T3 & T4
1. Hypothalamus
releases TRH
2. Pituitary
releases TSH
3. Thyroid
releases T3 & T4
Effect: blood
lvl of T3 & T4
[Thyroid]
Calcitonin (CT)
blood lvls of
Ca++
Inhibition
Day:
Photoreceptors
on eyes cause
the sympathetic
nervous system
to produce
norepinehrine,
inhibiting the
release of
melatonin
Trigger: High
blood lvl of T3
& T4
1. Hypothalamus
inhibits release
of TRH
2. Pituitary
inhibits release
of TSH
3. Thyroid
reduces
releasing T3 &
T4
Effect: blood
lvl of T3 & T4
Blood lvls of
Ca++
Disease/Notes
Cretinism,
Myxedema,
Graves disease,
Goiter
T3 =
triiodothyronine
(3 iodine)
T4 =
Tetraiodothyronine
(4 iodine)
3/26/2010
[Parathyroid]
Parathyroid (PTH)
[Thymus] Thymosin,
Thymic hormonal
factor (THF), Thymic
factor (TF), and
Thymopoietin
[Adrenal Cortex Mineralocorticoid
group]
Page 5
breakdown)
blood Ca++ and
Blood lvls of Ca+
2+
HPO4 lvls
Activity of
osteocytes (bone
production)
Activity of
osteoclasts (bone
breakdown)
reabsorption of
Ca++ and Mg++ in
the kidney
Promotes the
formation of
hormone
calcitriol from
Vitamin D in the
kidneys.
Calcitriol
increases the
absorption of Ca+
+, HPO 2-, and Mg++
4
in the gut.
All of these
hormones promote
the maturation
and development
of immune system
cells (i.e. Tcells and Bcells).
Triggers the
Trigger:
reabsorption of
Angiotensin II
++
Na from the
blood lvls of
Ca++
Trigger:
Low Angiotensin
II
Hypoparathyroidism
3/26/2010
Aldosterone
Page 6
urine to the
blood in the
kidneys.
Cl- and HCO3- are
reabsorbed due to
the osmotic
gradient created
by moving the
ions above. This
increases blood
pressure.
H+ excretion to
the urine is
promoted,
preventing blood
acidosis.
Steps:
1. Low blood
pressure reduces
the filtration
rate at the
kidneys, reducing
urine levels of
Cl2. Low lvls of Clin the urine
trigger the
juxtaglomerular
apparatus
(located in the
distal convoluted
tubule of the
kidney) to
release rennin.
3. Renin causes
the plasma
protein
angiotensinogen
to form
angiotensin I
4. Angiotensin I
moves through the
blood to the
lungs where the
enzyme
angiotensin
converting enzyme
(ACE) converts it
to angiotensin II
5. Angiotensin II
Other
aldosterone
release
mechanisms:
- High blood K+
or low blood Na+
can also trigger
aldosterone
release
- Low blood K+ or
high blood Na+
can inhibit
aldosterone
release.
3/26/2010
Page 7
triggers
aldosterone
release from the
adrenal cortex
and causes
vasoconstriction
increasing the
blood pressure.
6. Increased
blood pressure
increases the
filtration rate
at the kidneys
increasing the
amount of Cl- in
the urine and
hence reducing
the release of
rennin.
[Adrenal cortex
protein
Trigger: Low
Glucocorticoid group] catabolism in
blood lvls of
Cortisol
muscle to
glucocorticoids
(hydrocortisone),
increase blood
1. Hypothalamus:
Corticosterone,
amino acid lvls
releases CRH
Cortisone
for production of 2. Pituitary:
enzymes
releases ACTH
use of amino
3. Adrenal
acids or lactic
cortex: releases
acids in liver to glucocorticoids
make glucose
Effect: Blood
(i.e.
lvls of
gluconeogenesis
glucocorticoids
making of glucose increase
from other then
Trigger: High
blood lvls of
glucocorticoids
1. Hypothalamus:
inhibits release
of CRH
2. Pituitary:
inhibits release
of ACTH
Effect: Blood
lvls of
glucocorticoids
decrease
NOTE: CRH is also
released in
response to
emotional or
physical stressors
that take the body
away from
homeostasis
(general
adaptation
syndrome). Reduces
the bodies immune
response to deal
with some
immediate
3/26/2010
glycogens)
lipolysis
break down of
triglycerides and
release of fatty
acids
blood glucose
lvls
sensitivity of
blood vessels to
compounds that
cause
vasoconstriction
inflammatory
response
number of mast
cells
reduce
histamine release
capillary
permeability
phagocytosis of
dead and foreign
cells
connective
tissue formation
immune response
[Adrenal cortex
In Men causes the
Androgen group]
development of
Dehydroepiandosterone secondary sex
(DHEA)
characteristics.
Androgens are male
In Women DHEA is
sex hormones, two
converted into
main are testosterone estrogen by
Page 8
stressor. Explains
how stressors
increase disease.
Treatment uses:
1. Hydrocortisone
(cortisol) is used
to treat chronic
inflammation.
2. Glucocorticoids
are used to reduce
the immune
response in
patients that have
had an organ
transplant,
reduces the
rejections.
It is unclear how
DHEA is regulated
but its release
appears to be
triggered by ACTH
Disease:
Addisons disease,
Cushings
syndrome,
Hyperglycemia,
Osteoporosis,
Poor wound
healing,
Mood swings
Congenital adrenal
hyperplasia
3/26/2010
Page 9
various body
tissues and can
be an important
source of
estrogen in post
menopausal women.
May also
contribute to sex
drive in women.
In prepuberty
boys and girls
will cause growth
spurts and growth
of pubic hair
[Adrenal medulla]
Same effect as
Stimulated by the
epinephrine
the sympathetic
sympathetic
(adrenaline)
nervous system
preganglionic
norepinephrine (NE)
nerves when the
sympathetic
nervous system is
activated. Most
(80%) of the
hormone released
is epinephrine
[Pancreas Islets of Increases blood
Low blood sugar
Langerhans Alpha
sugar lvl by
lvl stimulates
cells]
causing the liver the release of
Glucagon
to convert
glucagons
glycogen to
glucose
Promotes the
formation of
glucose in the
liver from amino
from the testes and
dehydroepiandosterone
produced by the
adrenal cortex
High blood sugar
lvl inhibits the
release of
glucagons
3/26/2010
Page 10
acids and lactic
acid
(gluconeogenesis)
[Pancreas Islets of Decreases blood
High blood sugar
Langerhans Beta
sugar lvls by
lvls stimulates
cells]
causing the liver insulin release
Insulin
to convert
glucose to
glycogen
Accelerates
facilitated
diffusion of
glucose into
cells,
particularly
skeletal muscle
Increases
movement of amino
acids into cells
and promotes
protein synthesis
Increases
synthesis of
fatty acids
Low blood sugar
lvls inhibits
insulin release
Other factors
which may cause
insulin release:
1. Acetylcholine
from
parasympathetic
vegas nerve
stimulates the
release of insulin
2. Food high in
carbohydrates
raise blood sugar
triggering insulin
release
3. Food high in
proteins increase
blood levels of
the amino acids,
arginine and
leucine,
triggering insulin
release.
4. hGH and ACTH
stimulate insulin
release because
they raise blood
sugar lvls.
Diseases:
Diabetes mellitus
(Type I & Type II)
3/26/2010
[Pancreas Islets of Inhibits the
Langerhans Delta
secretion of
cells]
insulin and
Somatostatin
glucagons
Slows the
absorption of
nutrients from
the gut
Overall reduces
digestion
[Pancreas Islets of Inhibits release
Langerhans F-cells] of somatostatin
Pancreatic
Causes
polypeptide
contraction of
the gallbladder
and secretion of
pancreatic
digestive enzymes
Overall increases
digestion
[Eicosanoids]
Many effects, act
Prostaglandins
somewhat similar
to
neurotransmitters
Page 11
Low lvls of
pancreatic
polypeptide
increase the
release of
somatostatin
High lvls of
pancreatic
polypeptide
inhibit the
release of
somatostatin
Acute
hypoglycemia
Fasting
Exercise
Diets high in
protein
High blood
glucose
High
somatostatin
Some are released
when tissues are
damaged or
irritated,
triggering the
nerve signals
that cause pain
Asprin and
Ibuprofen
inhibit
prostaglandins
Note: Usually the
release triggers
override the
inhibitory effect
of somatostatin
3/26/2010
Page 12
Hormone Related Diseases
Hormone
Dwarfism
Disease
hGH
Giantism
hGH
Acromegaly
hGH
Diabetes insipidus ADH
Cretinism
T3 & T4
Myxedema
T3 & T4
Graves Disease
T3 & T4
Goiter
T3 & T4
Details
Hyposecretion of hGH before puberty. Causes person to be
short.
Hypersecretion of hGH before puberty. Causes person to be
tall.
Hypersecretion of hGH after puberty. Causes bones to enlarge
in diameter because they can no longer grow in length.
Brain damage causes low ADH lvls or the kidney receptors for
ADH do not respond.
SxS: This causes the person to produce large amounts of dilute
urine, dehydrating the body.
Low T3/T4 lvls during development causes mental retardation
and dwarfism
Low T3/T4 in adults causes the following:
SxS:
Edema of the face
Slow heart beat, low body temp, low metabolic rate
Dry skin and hair
Muscular weakness
Mental dullness
An autoimmune disease where immunoglobulins mimic the actions
of TSH.
SxS:
Exophtyalmos (eyes protrude)
Thyroid gland 2x-3x normal size
Increased metabolic rate
Increased heart rate
Weight loss despite a good appetite
Insomnia
No heat tolerance (i.e. body overheats easily)
Excessive growth of the thyroid gland usually caused by a diet
low in iodine
3/26/2010
Page 13
Hypoparathyroidism PTH
Addisons Disease
Glucocorticoid
group of the
Adrenal cortex
hormones
Cushings Syndrome Glucocorticoid
group of the
Adrenal cortex
hormones
Congenital adrenal Androgen group
Low blood PTH lvl due to parathyroid dmg, causes blood calcium
lvls to be abnormally low. This reduces extracellular Ca++ to
the point that skeletal muscle can depolarize and contract. It
causes tetany (i.e. sustained contraction) in skeletal muscle
because most of the calcium for contractions is stored in the
sarcoplasmic reticulum. In smooth muscle and cardiac muscle it
can cause depolarization and contraction, but it reduces the
force of contractions because most of the calcium that causes
muscle contractions come from outside the cell. These effects
can cause serious heart arrhythmia to occur.
Hyposecretion of glucocoticoids which causes the following
SxS:
Mental dullness
Anorexia
Nausea
Weight loss
Hypoglycemia
Muscle weakness
Low aldosterone
ACTH may be high due to a lack of negative feedback and it may
mimic the effects of melanin stimulating hormone, increasing
skin pigmentation
Hypersecretion of glucocorticoids which causes the following
Sxs:
Fat redistribution: fat puffy face and thin spindly arms and
legs due to muscle catabolism
Buffalo hump on back
Large pendulous hanging abdomen
Flushed facial skin
Hyperglycemia
Osteoporosis
Poor wound healing
Mood swings
Hypersecretion of DHEA which causes the following SxS in
3/26/2010
hyperplasia
Page 14
of the adrenal women:
cortex
Deep voice
hormones
Baldness
Atrophy of the breast
Infrequent menstruation
This disease has little effect on adult men. In boys it causes
early development of secondary sex characteristics.
Diabetes mellitus
Insulin
A disease caused by improper regulation of insulin with the
following SxS:
High blood sugar
High sugar in the urine
Excessive thirst (polydipsia)
Excessive eating (polyphagia)
Diabetes mellitus
Insulin
Autoimmune disease that leads to the destruction of beta
Type I
cells. Usually occurs in young people. Because glucose doesnt
AKA Juvenile onset
move into the cells, cells burn fatty acids raising the levels
of blood ketones causing ketoacidosis (low blood pH).
Treatment inject insulin
Insulin shock too much insulin injected, blood sugar lvl
drops too low.
Diabetes mellitus
Insulin
Person has the proper amount of insulin in the blood stream,
Type II
but the target cells in the body are less sensitive to insulin
AKA Adult onset
due to down regulation.
This type of diabetes represents 90% of cases and usually can
be controlled by exercise and loss of weight
3/26/2010
Page 15
You might also like
- Curriculum Vitae 2020 2Document87 pagesCurriculum Vitae 2020 2api-325315995No ratings yet
- CH 45 Guided ReadingDocument7 pagesCH 45 Guided ReadingmharirajNo ratings yet
- AP-2 Lab Report - Lab 01 The Endrocine SystemDocument15 pagesAP-2 Lab Report - Lab 01 The Endrocine Systemrcdunfee86% (7)
- Endocrine ReviewDocument9 pagesEndocrine ReviewSpencer ThomasNo ratings yet
- Hippa TestDocument2 pagesHippa Testfatimajafar2003No ratings yet
- New Triorigin Sequence of Endocrine OrgansDocument4 pagesNew Triorigin Sequence of Endocrine OrgansЕвгений ТополовскийNo ratings yet
- Hormonal Responses To ExerciseDocument38 pagesHormonal Responses To ExercisesajjadNo ratings yet
- Fazio Log YeDocument31 pagesFazio Log YeBianca NegrutNo ratings yet
- Endocrinology Excerpts: Hypothalamic-Pituitary-Adrenal AxisDocument9 pagesEndocrinology Excerpts: Hypothalamic-Pituitary-Adrenal AxisKiana TehraniNo ratings yet
- 17.2 Hormones Anatomy and PhysiologyDocument14 pages17.2 Hormones Anatomy and PhysiologyPrincess RuthNo ratings yet
- Uqs EndoDocument60 pagesUqs EndoNida BatoolNo ratings yet
- The Stress ResponseDocument9 pagesThe Stress ResponseRaditya PradiptaNo ratings yet
- Endocrine System: Pituitary Gland and HypothalamusDocument9 pagesEndocrine System: Pituitary Gland and HypothalamusRohan Sahu0% (1)
- 08 Biomedik - Sistem Endokrin &hormonDocument43 pages08 Biomedik - Sistem Endokrin &hormonqueenraaa16No ratings yet
- Endocrine GlandDocument4 pagesEndocrine Glandakash_zizouNo ratings yet
- HormonesDocument55 pagesHormonesAvinashNo ratings yet
- NOTES Endocrinology ToxicologyDocument52 pagesNOTES Endocrinology ToxicologyRenz Gerard AmorNo ratings yet
- System Glands Hormone: NeurotransmittersDocument6 pagesSystem Glands Hormone: NeurotransmittersShaheryar HasanNo ratings yet
- Endocrine Glands Are Glands of TheDocument9 pagesEndocrine Glands Are Glands of ThextinebadzNo ratings yet
- 1 - Endocrine 1 (Introduction) - MedicineDocument36 pages1 - Endocrine 1 (Introduction) - MedicineBHUWAN BASKOTANo ratings yet
- Review Chapter 16 EndocrineDocument11 pagesReview Chapter 16 EndocrineAkul MunjalNo ratings yet
- Hormones CompleteDocument30 pagesHormones CompleteAqsa NoorNo ratings yet
- Endocrine Gland - Wikipedia, The Free EncyclopediaDocument5 pagesEndocrine Gland - Wikipedia, The Free EncyclopediakbhattacNo ratings yet
- Androgens: Laksmi Indreswari, MD Biochemistry LaboratoryDocument15 pagesAndrogens: Laksmi Indreswari, MD Biochemistry LaboratoryMustika Ayu FitrianiNo ratings yet
- Endocrine SystemDocument41 pagesEndocrine SystemMerrin EncarnacionNo ratings yet
- Endocrine GlandsDocument13 pagesEndocrine GlandsJoan GalarceNo ratings yet
- Endocrine SystemDocument22 pagesEndocrine SystemLen Len Ochinang OchinangNo ratings yet
- SAQ 2nd Week (Thyroid Gland)Document15 pagesSAQ 2nd Week (Thyroid Gland)Josephine BediakoNo ratings yet
- Lec 2Document9 pagesLec 2Imran HussainNo ratings yet
- Endocrine SystemDocument61 pagesEndocrine Systemhiteshsirvi0000No ratings yet
- Clinton Hackney Anatomy & Physiology II BctcsDocument65 pagesClinton Hackney Anatomy & Physiology II BctcsJack HolthouseNo ratings yet
- Hormones & Hormones AntagonistsDocument27 pagesHormones & Hormones AntagonistsVarsha Shende KhobragadeNo ratings yet
- The Endocrine System: Presented By, MD Nasir Uddin Mahmood, Product Executive, Opsonin Pharma LimitedDocument24 pagesThe Endocrine System: Presented By, MD Nasir Uddin Mahmood, Product Executive, Opsonin Pharma LimitedMd Nasir Uddin Mahmood100% (2)
- Chapt 8 AnswersDocument6 pagesChapt 8 AnswershulsercNo ratings yet
- Module 9 The Endocrine SystemDocument15 pagesModule 9 The Endocrine SystemMisha WilliamsNo ratings yet
- Endocrine System: Dr. Victor J. SamillanDocument45 pagesEndocrine System: Dr. Victor J. SamillanBruno MoraNo ratings yet
- Anabolic Extreme - Blood TestsDocument2 pagesAnabolic Extreme - Blood Testsandrewa_6No ratings yet
- Thyroid Physiology - Function TestDocument42 pagesThyroid Physiology - Function TestAbhishekNo ratings yet
- Dulutalias - Chapter18-THE ENDOCRINE SYSTEMDocument10 pagesDulutalias - Chapter18-THE ENDOCRINE SYSTEMGwen Valerie DulutaliasNo ratings yet
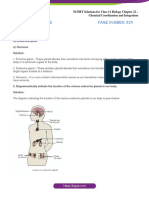
- Ncert Solutions June6 For Class 11 Biology Chapter 22 Chemical Coordination and IntegrationDocument8 pagesNcert Solutions June6 For Class 11 Biology Chapter 22 Chemical Coordination and Integrationginnisingh524No ratings yet
- 1-Endocrine 1Document23 pages1-Endocrine 1محمد عليNo ratings yet
- Endocrine System ReviewDocument16 pagesEndocrine System Reviewarjohnson83No ratings yet
- HormonesDocument29 pagesHormonesCandy Chieng67% (3)
- Drugs Used in Disorders of Endocrine System Ppt. Book (Lectures 1-6)Document467 pagesDrugs Used in Disorders of Endocrine System Ppt. Book (Lectures 1-6)Marc Imhotep Cray, M.D.100% (1)
- Pituitary HormonesDocument75 pagesPituitary HormonesRinkiNo ratings yet
- EndocrineDocument7 pagesEndocrineKharrel YballeNo ratings yet
- Human Endocrene SystemDocument11 pagesHuman Endocrene SystemmaroonblekiNo ratings yet
- Pituitary and ThyroidDocument54 pagesPituitary and ThyroidSaif AliNo ratings yet
- DelaCruz AlbertBryan Activity#7 MED3Document4 pagesDelaCruz AlbertBryan Activity#7 MED3AlbertNo ratings yet
- HormonesDocument25 pagesHormonesmirzauzairbaig84No ratings yet
- BBT221 Lecture 6Document41 pagesBBT221 Lecture 6Al Sabri Bhuiyan 1812098042No ratings yet
- ArooosaDocument20 pagesArooosaMudassir FarooqNo ratings yet
- Chemistry ReviewerDocument8 pagesChemistry ReviewerprnfbmsdqnNo ratings yet
- Endocrine Test 8 NotesDocument9 pagesEndocrine Test 8 NotesHayden ShulerNo ratings yet
- Hormone ActionDocument9 pagesHormone ActionGaurav Kamblen'chaNo ratings yet
- Endocrine System 13 معدلDocument11 pagesEndocrine System 13 معدلhanaalhadidi567No ratings yet
- Hormones 080623Document83 pagesHormones 080623Rao Asad MubeenNo ratings yet
- M.Prasad Naidu MSC Medical Biochemistry, Ph.D.Research ScholarDocument32 pagesM.Prasad Naidu MSC Medical Biochemistry, Ph.D.Research ScholarM.PRASAD NAIDUNo ratings yet
- Chemical Co - OrdinationDocument21 pagesChemical Co - OrdinationManinder KaurNo ratings yet
- HBB 2102 Endocrine System Student NotesDocument8 pagesHBB 2102 Endocrine System Student Notesjordanmusyoki19No ratings yet
- Hormones: Hormonal Control Nervous ControlDocument5 pagesHormones: Hormonal Control Nervous Controlvaibhav trivediNo ratings yet
- Random Endocrine NotesDocument7 pagesRandom Endocrine Noteskep1313No ratings yet
- Dimensional Analysis MethodDocument17 pagesDimensional Analysis Methodfatimajafar2003No ratings yet
- CH 1 Math ReviewDocument29 pagesCH 1 Math Reviewfatimajafar2003No ratings yet
- Inserting IVDocument1 pageInserting IVfatimajafar2003No ratings yet
- RRD #1 Intro, Genetics, Intracellular Functions Fa16Document26 pagesRRD #1 Intro, Genetics, Intracellular Functions Fa16fatimajafar2003No ratings yet
- PT Cakra Medika Utama: Price List Boditech Med Inc (I-Chroma)Document2 pagesPT Cakra Medika Utama: Price List Boditech Med Inc (I-Chroma)raditNo ratings yet
- 123 Sur HypoparathyroidismDocument3 pages123 Sur HypoparathyroidismHurryNo ratings yet
- Determinacija Spola 2014Document27 pagesDeterminacija Spola 2014Krampus TrećiNo ratings yet
- Anatomy and Physiology of Adrenal GlandDocument26 pagesAnatomy and Physiology of Adrenal GlandYAMINIPRIYANNo ratings yet
- Male Reproductive SystemDocument8 pagesMale Reproductive SystemShayu ShaNo ratings yet
- Thyroidectomy - : An Operation To Remove All or Part of The Thyroid GlandDocument20 pagesThyroidectomy - : An Operation To Remove All or Part of The Thyroid GlandCindy Babsa-ay MaslagNo ratings yet
- TIRADS ClassificationDocument1 pageTIRADS ClassificationkristwibowoNo ratings yet
- Endocrine GlandsDocument3 pagesEndocrine Glandsdan 123No ratings yet
- Thyroid QuizDocument3 pagesThyroid QuizĐặng Quỳnh ANNo ratings yet
- Sidney H. Ingbar (Editor), Sidney C. Werner (Editor) by Lippincott Williams & Wilkins PublishersDocument10 pagesSidney H. Ingbar (Editor), Sidney C. Werner (Editor) by Lippincott Williams & Wilkins Publishersbyrock66No ratings yet
- Oxford Handbook of Endocrinology & Diabetes-Oxford University Press - 4th Edition) (2022)Document1,130 pagesOxford Handbook of Endocrinology & Diabetes-Oxford University Press - 4th Edition) (2022)Sa7arNo ratings yet
- Histology of The EyelidDocument7 pagesHistology of The EyelidshmirtbNo ratings yet
- Skin Functions and LayersDocument23 pagesSkin Functions and LayersAnis Samrotul Lathifah100% (2)
- Science 10 - Q3 - Summative TestDocument1 pageScience 10 - Q3 - Summative Testzenaida a academiaNo ratings yet
- Endocrine System: A & P-Ii Unit VDocument25 pagesEndocrine System: A & P-Ii Unit VAsad KHANNo ratings yet
- Kuliah HyperthyroidDocument18 pagesKuliah HyperthyroidFreddyNo ratings yet
- Hypopituitarism - ThomasDocument40 pagesHypopituitarism - ThomasguidanceNo ratings yet
- Science6 Q2 W2 1Document9 pagesScience6 Q2 W2 1Matt The idkNo ratings yet
- Shashikant PDFDocument4 pagesShashikant PDFAacharya Shashikant VashishthNo ratings yet
- Adrenal Gland Disorders: Addison's DiseaseDocument4 pagesAdrenal Gland Disorders: Addison's DiseaseyoussraselimNo ratings yet
- Animal Endocrine SystemDocument9 pagesAnimal Endocrine SystemAaron ZNo ratings yet
- ACE's Essentials of Exercise Science For Fitness ProfessionalsDocument18 pagesACE's Essentials of Exercise Science For Fitness ProfessionalsHArsh AroraNo ratings yet
- Tyroid Drug - ppt3Document15 pagesTyroid Drug - ppt3nurliah armandNo ratings yet
- Endocrin E Diseases: by Group 3Document53 pagesEndocrin E Diseases: by Group 3Ash AshNo ratings yet
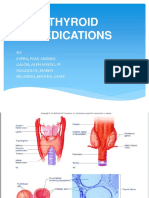
- Thyroid MedicationsDocument20 pagesThyroid MedicationsBlueberry CincoNo ratings yet
- Physioex Lab Report: Pre-Lab Quiz ResultsDocument13 pagesPhysioex Lab Report: Pre-Lab Quiz ResultsIvana FNo ratings yet
- Physioex Lab Report: Pre-Lab Quiz ResultsDocument3 pagesPhysioex Lab Report: Pre-Lab Quiz ResultssmitNo ratings yet
- CR EndokrinDocument14 pagesCR EndokrinFajar SutrisnaNo ratings yet