Professional Documents
Culture Documents
Laryngeal Morphological Changes Due
Uploaded by
Lilia ScutelnicOriginal Description:
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Laryngeal Morphological Changes Due
Uploaded by
Lilia ScutelnicCopyright:
Available Formats
Rev. Med. Chir. Soc. Med. Nat., Iai 2012 vol. 116, no.
INTERNAL MEDICINE - PEDIATRICS
ORIGINAL PAPERS
LARYNGEAL MORPHOLOGICAL CHANGES DUE
TO GASTROESOPHAGEAL REFLUX DISEASE
M. D. Cobzeanu1 , Monica Voineag2, V. L. Drug3, Anca Ciubotaru4,
B. M. Cobzeanu1 , O. D. Palade1
University of Medicine and Pharmacy Grigore T. Popa - Iasi
Faculty of Medicine
1. Discipline of ENT
3. Discipline of Medical Semiolgy IGH
4. University of Arts George Enescu - Iasi
2. ENT Outpatients Siegen, Germany
LARYNGEAL MORPHOLOGICAL CHANGES DUE TO GASTROESOPHAGEAL REFLUX DISEASE (GERD) (Abstract): Chronic laryngitis may have life impact on professional voice users. Besides smoking and excessive alcohol intake, GERD is a determining
factor in the etiology of dysphonia. Aim: To evaluate the laryngeal alteration due to GERD
in professional voice users. Material and methods: The study included 96 vocal professionals (teachers, actors, singers and priests), 58 males and 38 females, with a mean age of 38.3
7.5 years, presented for chronic laryngeal symptoms. The patients filled out a standardized
questionnaire and were examined laryngoscopically. Results: Laryngeal changes were scaled
0 (absence) to 7 (maximum) arytenoid edema (5.071.08), interarytenoid edema
(6.181.12), vocal folds edema (5.671.04), ventricular bands edema (4.960.97), laryngeal
edema 4.120.83). Conclusions: Laryngoscopic changes may suggest the concomitance of
GERD in professional voice users with dysphonia. Keywords: GERD, DYSPHONIA, VOCAL PROFESSIONALS.
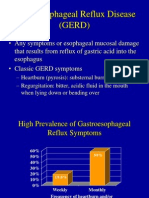
Even though most otolaryngologists are
aware of the pathology induced by gastroesophageal reflux disease (GERD), this
relationship was more intensely studied
during the last two decades (13, 14). Otolaryngologists have become extremely cautious
when performing the clinical ENT examination and look for reflux signs (rashes, edema
in the arytenoid mucosa and interarytenoidian area) even when they prescribe treatment
for chronic laryngitis. According to the most
recent surveys, laryngopharyngeal reflux
(LPR) displays a complex spectrum of
pathological signs (1, 2, 3, 5).
Reflux laryngitis occurs as a result of a
backward flow of acid and other stomach
contents into the esophagus to the larynx,
resulting in a chemical burn of the lining.
The diagnosis of LPR is based on a
combination of symptoms and findings in
the larynx during physical examination (4,
7, 8).
The opening of the esophagus sits behind the arytenoids in the posterior part of
the larynx, and that is why these areas are
the most affected by reflux. The larynx
shows signs of irritation and inflammation,
as evidenced by the presence of redness
1011
M.D. Cobzeanu et al.
(erythema) and swelling (edema) of the
arytenoids, interarytenoid region (the area
between the arytenoids, also referred to as
the posterior glottis, or, incorrectly, as the
posterior commissure), and the post-cricoid
region (the area behind the arytenoids that
separates the larynx from the esophageal
opening).
In severe cases, the reflux material can
contact other parts of the larynx causing
erythema and edema of the folds.
The presence of edema of the true vocal
cords is highly suggestive of LPR, even in
the absence of laryngeal erythema (6, 9, 10,
11).
Any activity that increases intraabdominal pressure may exacerbate the
symptoms of LPR. Such activities may
include weight lifting, sit-ups, abdominal
crunches, sexual intercourse, running,
dancing, aerobics, public speaking, acting,
and singing.
Reflux-related symptoms and clinical
presentation have been identified in 4 to10% of all the patients seen by otolaryngologists (15, 16, 17), and most likely, asthese estimates are not accurate, the percentage could be even much higher. Re-garding the patients with laryngeal pathology, LPR is related with these conditions
or represents an etiological factor in approximately 50% of the cases (11, 13).
The most common symptoms and clinical presentations of the reflux laryngitis
are:
- morning hoarseness
- the voice warms in more than 20-30
minutes
- halitosis
- throat clearing
- oral dryness
- white tongue
- globus faringeus
1012
dysphagia
regurgitations of the gastric content
recurrent cough
laryngospasm,
complication of asthma
acute upper airways infection in children.
In addition to longer vocal warm up
time, the vocal professionals and actors
may also suffer other interferences in their
vocal practice frequent throat clearing,
abundant expectoration, especially during
the first 10-20 minutes of vocal training
(16).
Some authors noticed that LPR patients
do not present esophagitis-related changes,
so dyspepsia and heartburn are usually
absent (8, 12, 17).
The prevalence of esophagitis is relatively low, as the esophageal mucosa of the
distal esophagus has its own antacid protection mechanisms which include the following:
peristalsis (quickly pushing the acid off the
surface of the esophageal mucosa)
structure of the mucosa (tolerating the
intermittent contact with the gastric acid)
capacity of the saliva to neutralize the acid
However, the larynx and the pharynx do
not have such protective mechanisms, thus
exposure to acid and pepsin may cause
substantial changes at this level, whereas
the esophagus may not be affected at all.
According to the preliminary data reported
by Axford (14), the lining of the larynx has
a cell defense mechanism which is different
from the esophageal mucosa and there are
specific differences in the expression of the
MUC genes and carbonic anhydrase in the
larynx and pharynx (1, 3, 8).
If the mucosa is affected, either directly
or through secondary mechanisms, changes
in the laryngeal mucosa may result. Thus, it
Laryngeal morphological changes due to gastroesophageal reflux disease
may be directly affected by the contact
with the laryngeal lining with acid and
pepsin, which results in mucosal lesions.
Alternatively, the irritation of the distal
esophagus by the gastric acid may activate
a reflex mediated by the vagus nerve,
which leads to chronic cough and throat
clearing, affecting the larynx lining as well
(16, 17).
The bile reflux may also affect the larynx. Additionally, according to recent surveys, there are a lot of question marks concerning the pathophysiology of reflux laryngitis. Some authors consider that the
decrease in salivary epidermal growth factor may be associated with reflux laryngitis
(14, 15, 17).
The aim of this research study was to
evaluate the laryngeal alterations due to
gastroesophageal reflux disease in professional voice users
(chronic dysphonia)
- absence of laryngeal benign or malignant lesions
- no drug treatment that could alter the
esophageal motor function or acid secretion
(anticholinergics, sedatives, prostaglandins,
calcium channel blockers, potassium, antibiotics, NSAIDs)
- symptomatic GERD
Exclusion criteria:
- active smokers
- chronic alcohol intake
- upper airways infections during the
last month (before inclusion in the research
study)
- prior history of anti-reflux surgery
- asthma
Statistical analysis
Statistical analysis was performed using
SPSS 16.0, on Windows XP Professional
platform.
MATERIAL AND METHODS
Selection of patients groups
The cases included in the research study
were selected among the patients of the Sf.
Spiridon Emergency Hospital Iasi, ENT
Department. As study material, we used a
group of 96 vocal professionals (teachers,
actors, singers, priests) diagnosed with
chronic laryngitis between 2008 and 2010.
All patients filled out a standardized questionnaire and patient meeting the clinical
criteria of gastroesophageal reflux disease
were included in the study. A written informed consent was obtained from all patients. The control group included 54 age-,
sex- and profession- matched ENT patients
with no laryngeal complaints (16,17).
Selection criteria:
- vocal professionals (teachers, actors,
singers, priests)
- dysphonia for at least 3 months
RESULTS
This research survey included 58 males
and 38 females, aged between 21 and 60
years, mean age 38.3 years (7.56) and
median age 39 years.
The most affected professionals considering laryngeal changes - were teachers
(37.5%), followed by singers (28.12%).
There was no statistically significant difference between priests and actors, considering that priests are a male-only category.
The analysis of laryngeal changes revealed the prevalence of changes in the true
vocal folds, as well as in the interarytenoid
area (p<0.001), closely followed by changes at arytenoid level, false vocal folds, and
laryngeal mucosa in general (table I).
Diagnostic sensitivity of laryngoscopy
for laryngeal changes was of over 50% for
8 of the 10 laryngeal signs suspected to
occur following the action of the reflux.
1013
M.D. Cobzeanu et al.
Interarytenoid and arytenoid edema followed by vocal folds edema and erythema
were the changes with the highest sensitivity (83-97%).
TABLE I
Laryngeal changes (flexible endoscopic laryngoscopy)
Research group
Laryngeal change
Control group
SD
SD
Arytenoid edema/ erythema
5.07
1.08
1.15
0.92
Interarytenoid edema/ erythema
6.18*
1.12
0.93
0.89
Vocal folds edema/ erythema
5.67*
1.04
0.98
0.91
Ventricular bands edema/ erythema
4.96
0.97
0.87
0.73
Laryngeal edema/ erythema
4.12
0.83
0.77
0.69
-arithmetic mean
SD-standard deviation
Specificity was highest in the patients
with true vocal folds and ventricular bands
erythema, followed by ventricular bands
edema and laryngeal erythema (90-94%).
DISCUSSION
According to our findings, laryngeal
changes were more common at the level of
the vocal and interarytenoid folds
(p<0.001), followed by arytenoid area and
ventricular bands both before, as well as
after treatment. Interarytenoid and arytenoid edemas, followed by edema and erythema of the vocal folds were found to be
the changes with the highest sensitivity (83
- 97%) (16, 17).
Despite numerous studies on reflux
symptoms, those mentioned above as well
as many others (16, 17), there is no objective data to support the significance of the
various patient complaints and changes (as
a result of the performed tests) in terms of
diagnosis. This issue arose as there has not
been any consensus as regards normal
among the groups of patients included in
the survey. Interdisciplinary debates (most
1014
*p<0.001
particularly, otorhinolaryngology and gastroenterology), as well as multicentric surveys are necessary to accurately determine
the sensitivity and specificity of the results
frequently associated with laryngopharyngeal reflux, as well as the impact of
LPR on the quality of life and general
health status.
CONCLUSIONS
Patients presenting with laryngeal reflux symptoms must be treated in multidisciplinary way (otolaryngologist/gastroenterologist). The positive diagnostic requires
modern and accurate testing methods: flexible endoscopic laryngoscopy, pH monitoring, esophageal impedance study, upper
gastro intestinal endoscopy (UGIE).
Because there is no consensus on diagnosis and treatment, this condition is frequently either over diagnosed (resulting in
various invasive, useless and expensive
tests, as well as the application of inefficient treatment plans), or under diagnosed
(resulting in the progression of symptoms
because of the lack of adequate treatment).
Laryngeal morphological changes due to gastroesophageal reflux disease
REFERENCES
1. Book DT, Rhees JS, Toohill RJ, Smith TL. Perpectives in laryngopharyngeal reflux: an international
survey. Laryngoscope 2002; 112: 1399-1406.
2. Lenderking WR, Hillson E, Crawley JA, Moore D, Berzon R, Pashos CL. The clinical charactheristics and impact of laryngopharyngeal reflux disease on health-related quality of life. Value Health
2003; 6: 560-565.
3. Carrau RL, Khdir A, Crawkley JA, Hillson EM, Davis JK, Pashos CL. The impact of laryngopharyngeal reflux on patient-reported quality of life. Laryngoscope. In press.
4. Halum SL, Postma GN, Johnston, Belafsky PC, Koufman JA. Patients with isolated laryngopharyngeal reflux are not obese. Laryngoscope 2005; 115(6): 1042-1045.
5. Koufman JA, Amin MR, Panetti M. Prevalence of reflux in 113 consecutive patients with laryngeal
and voice disorders. Otolaryngol Head Neck Surg 2000; 123: 385-388.
6. Book DT, Rhee JS, Toohill RJ, Smith TL. Perspective in laryngopharyngeal reflux: an international
survey. Laryngoscope 2002; 112(8 pt 1): 1399-1406.
7. Vaezi MF. Ear, nose, and throat manifestations of gastroesophageal reflux disease. Clin Perspect
Gastroeneterol 2002; 5(6): 324-328.
8. Siupsinskiene N, Adamonis K, Toohill RJ. Quality of life in laryngopharyngeal reflux patients.
Laryngoscope 2007; 117: 480-4.
9. Roy N, Merril RM, Thibeault S, Parsa RA, Gray SD, Smith EM. Prevalence of voice disorders in
teachers and the general population. J Speech Lang Hear Res 2004; 47(2): 281-293.
10. Smit CF, van Leeuwen JA, Mathus-Vliegen LM et al. Gastropharyngeal and gastroesophageal reflux
in globus and hoarseness. Arch Otolaryngol Head Neck Surg 2000; 126: 827-830.
11. Johnston N, Bulmer D, gill GA, et al. cell biology of laryngeal epithelial defenses in health and disease: further studies. Ann Otol Rhinol Laryngol 2003; 112: 481-491.
12. Adhami T, Goldblum JR, Richter JE, Vaezi MF. The role of gastric and duodenal agents in laryngeal
injury: an experimental canine model. Am J Gastroenterol 2004; 99(11): 2098-2106.
13. Shaker R, Bardan E, Gu C et al. Intrapharyngeal distribution of gastric acid refluxate. Laryngoscope
2003; 113: 1182-1191.
14. Axford SE, Sharp N, Ross PE, et al. Cell biology of laryngeal epithelial defenses in health and disease: preliminary studies. Ann Otol Rhinol Laryngol 2001; 110: 1099-1108.
15. Galli J, Calo L, Agostino S et al. Bile reflux as possible risk factor in laryngopharyngeal inflammatory and neoplastic lesions. Acta Otorhinolaryngol Ital 2003; 23: 377-382.
16. Monica Voineag, V. Costinescu, M. D. Cobzeanu. Management of pharyngolaryngeal reflux at voice
professionals. Analele Universitatii Dunarea de Jos Galati, Medicina 2011; XVII(2): 77-83.
17. Voineag M. A. Diagnosis and Treatment of Dysphonias Caused by the Gastroesophageal Reflux
Disease (Case of Vocal Professionals). PhD Thesis, 2011.
1015
You might also like
- The Prevalence and Risk FactorsDocument17 pagesThe Prevalence and Risk FactorsLilia ScutelnicNo ratings yet
- ActivityStability of Human PepsinDocument4 pagesActivityStability of Human PepsinLilia ScutelnicNo ratings yet
- Association of Laryngopharyngeal PDFDocument8 pagesAssociation of Laryngopharyngeal PDFLilia ScutelnicNo ratings yet
- Videostroboscopy in Laryngopharengeal RefluxDocument5 pagesVideostroboscopy in Laryngopharengeal RefluxLilia ScutelnicNo ratings yet
- The Prevalence of Laryngeal PathologyDocument7 pagesThe Prevalence of Laryngeal PathologyLilia ScutelnicNo ratings yet
- English Today Vol.1 Varianta 2 PDFDocument93 pagesEnglish Today Vol.1 Varianta 2 PDFDan CelacNo ratings yet
- 0003489414532777Document10 pages0003489414532777Lilia ScutelnicNo ratings yet
- 0 GERD Abstractbook 11FINAL 67833Document174 pages0 GERD Abstractbook 11FINAL 67833Lilia ScutelnicNo ratings yet
- 2007, Vol.40, Issues 5, The Professional VoiceDocument269 pages2007, Vol.40, Issues 5, The Professional VoiceLamia Bohliga100% (1)
- Laryngopharyngeal Reflux, DR A HaddadDocument35 pagesLaryngopharyngeal Reflux, DR A HaddadLilia ScutelnicNo ratings yet
- Interpreting Bravo PH StudiesDocument16 pagesInterpreting Bravo PH StudiesLilia ScutelnicNo ratings yet
- Campaign 1 - English For The Military StudentDocument160 pagesCampaign 1 - English For The Military StudentLilia ScutelnicNo ratings yet
- Characterization of Laryngopharyngeal Reflux in PDFDocument5 pagesCharacterization of Laryngopharyngeal Reflux in PDFLilia ScutelnicNo ratings yet
- Anatomy of Reflux A Growing Health Problem PDFDocument10 pagesAnatomy of Reflux A Growing Health Problem PDFLilia ScutelnicNo ratings yet
- Laryng Reflux 090825 1Document13 pagesLaryng Reflux 090825 1Syafiq IshakNo ratings yet
- Cell Biology of Laryngeal...Document11 pagesCell Biology of Laryngeal...Lilia ScutelnicNo ratings yet
- Laryngitis From RefluxDocument6 pagesLaryngitis From RefluxLilia ScutelnicNo ratings yet
- Anatomy of Reflux A Growing Health Problem PDFDocument10 pagesAnatomy of Reflux A Growing Health Problem PDFLilia ScutelnicNo ratings yet
- Posterior Commissure of The Human Larynx Revisited PDFDocument8 pagesPosterior Commissure of The Human Larynx Revisited PDFLilia ScutelnicNo ratings yet
- Acoustical Voice Measurements Did Change After Treatment inDocument7 pagesAcoustical Voice Measurements Did Change After Treatment inLilia ScutelnicNo ratings yet
- Anatomy of Reflux A Growing Health Problem PDFDocument10 pagesAnatomy of Reflux A Growing Health Problem PDFLilia ScutelnicNo ratings yet
- Acid Reflux Treatment For Hoarseness (Review)Document17 pagesAcid Reflux Treatment For Hoarseness (Review)Lilia ScutelnicNo ratings yet
- Abnormal Endoscopic Pharyngeal and LaryngealDocument7 pagesAbnormal Endoscopic Pharyngeal and LaryngealLilia ScutelnicNo ratings yet
- Acid Reflux Treatment For Hoarseness (Review) PDFDocument17 pagesAcid Reflux Treatment For Hoarseness (Review) PDFLilia ScutelnicNo ratings yet
- Gastroesophageal Reflux Disease (GERD)Document37 pagesGastroesophageal Reflux Disease (GERD)CraciunElenaNo ratings yet
- Sulcus Vocalis AutosomnalDocument6 pagesSulcus Vocalis AutosomnalLilia ScutelnicNo ratings yet
- 1larynxma 121125054402 Phpapp01Document73 pages1larynxma 121125054402 Phpapp01Lilia ScutelnicNo ratings yet
- Etiology of Vocal Fold Palsy 20060927Document43 pagesEtiology of Vocal Fold Palsy 20060927Lilia ScutelnicNo ratings yet
- Sulcus Vocalis 20070808Document38 pagesSulcus Vocalis 20070808Lilia ScutelnicNo ratings yet
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeFrom EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeRating: 4 out of 5 stars4/5 (5794)
- Shoe Dog: A Memoir by the Creator of NikeFrom EverandShoe Dog: A Memoir by the Creator of NikeRating: 4.5 out of 5 stars4.5/5 (537)
- The Yellow House: A Memoir (2019 National Book Award Winner)From EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Rating: 4 out of 5 stars4/5 (98)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceFrom EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceRating: 4 out of 5 stars4/5 (895)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersFrom EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersRating: 4.5 out of 5 stars4.5/5 (344)
- The Little Book of Hygge: Danish Secrets to Happy LivingFrom EverandThe Little Book of Hygge: Danish Secrets to Happy LivingRating: 3.5 out of 5 stars3.5/5 (399)
- Grit: The Power of Passion and PerseveranceFrom EverandGrit: The Power of Passion and PerseveranceRating: 4 out of 5 stars4/5 (588)
- The Emperor of All Maladies: A Biography of CancerFrom EverandThe Emperor of All Maladies: A Biography of CancerRating: 4.5 out of 5 stars4.5/5 (271)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaFrom EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaRating: 4.5 out of 5 stars4.5/5 (266)
- Never Split the Difference: Negotiating As If Your Life Depended On ItFrom EverandNever Split the Difference: Negotiating As If Your Life Depended On ItRating: 4.5 out of 5 stars4.5/5 (838)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryFrom EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryRating: 3.5 out of 5 stars3.5/5 (231)
- On Fire: The (Burning) Case for a Green New DealFrom EverandOn Fire: The (Burning) Case for a Green New DealRating: 4 out of 5 stars4/5 (73)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureFrom EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureRating: 4.5 out of 5 stars4.5/5 (474)
- Team of Rivals: The Political Genius of Abraham LincolnFrom EverandTeam of Rivals: The Political Genius of Abraham LincolnRating: 4.5 out of 5 stars4.5/5 (234)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyFrom EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyRating: 3.5 out of 5 stars3.5/5 (2259)
- The Unwinding: An Inner History of the New AmericaFrom EverandThe Unwinding: An Inner History of the New AmericaRating: 4 out of 5 stars4/5 (45)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreFrom EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreRating: 4 out of 5 stars4/5 (1090)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)From EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Rating: 4.5 out of 5 stars4.5/5 (121)
- Her Body and Other Parties: StoriesFrom EverandHer Body and Other Parties: StoriesRating: 4 out of 5 stars4/5 (821)
- Chapter 2: Demand, Supply & Market EquilibriumDocument15 pagesChapter 2: Demand, Supply & Market EquilibriumRaja AfiqahNo ratings yet
- Full Download Test Bank For Microbiology The Human Experience First Edition First Edition PDF Full ChapterDocument36 pagesFull Download Test Bank For Microbiology The Human Experience First Edition First Edition PDF Full Chapterscalp.downcast.c7wgo100% (20)
- AIX CommandsDocument8 pagesAIX CommandsKamal KantNo ratings yet
- Orpiano Vs TomasDocument2 pagesOrpiano Vs TomasDotsNo ratings yet
- Daily Hora ChartDocument2 pagesDaily Hora ChartkalanemiNo ratings yet
- Evaluation Sheet For RankingDocument6 pagesEvaluation Sheet For RankingSonny MatiasNo ratings yet
- Types of Communicative StrategyDocument46 pagesTypes of Communicative StrategyMyra Bolinas100% (1)
- Cohort 2 Assignment Essay FinalDocument4 pagesCohort 2 Assignment Essay Finalapi-652640066No ratings yet
- Unit 9Document3 pagesUnit 9LexNo ratings yet
- Tugas Week 6 No 8.23Document5 pagesTugas Week 6 No 8.23Mikael MuhammadNo ratings yet
- Psychological Science1Document23 pagesPsychological Science1Jatin RaghavNo ratings yet
- The AmazonsDocument18 pagesThe AmazonsJoan Grace Laguitan100% (1)
- Form No. 61: (See Proviso To Clause (A) of Rule 114C (1) )Document1 pageForm No. 61: (See Proviso To Clause (A) of Rule 114C (1) )Vinayak BhatNo ratings yet
- Personal Entrepreneurial Competencies (Pecs) Self-Rating QuestionnaireDocument3 pagesPersonal Entrepreneurial Competencies (Pecs) Self-Rating QuestionnaireMESIE JEAN PARAL100% (3)
- The Wall Dramaturgical PacketDocument24 pagesThe Wall Dramaturgical PacketMarilo CostaNo ratings yet
- Cost ContingenciesDocument14 pagesCost ContingenciesbokocinoNo ratings yet
- Synonyms & Antonyms of Mop: Save Word To Save This Word, You'll Need To Log inDocument6 pagesSynonyms & Antonyms of Mop: Save Word To Save This Word, You'll Need To Log inDexterNo ratings yet
- Mercado Vs Manzano Case DigestDocument3 pagesMercado Vs Manzano Case DigestalexparungoNo ratings yet
- Incremental and TwiceDocument12 pagesIncremental and TwiceAgung KaryawinaraNo ratings yet
- Artificial Neural NetworkDocument16 pagesArtificial Neural NetworkSahil ChopraNo ratings yet
- (After The Reading of The Quote) : For The Entrance of The Philippine National Flag!Document4 pages(After The Reading of The Quote) : For The Entrance of The Philippine National Flag!JV DeeNo ratings yet
- Principles of Learning: FS2 Field StudyDocument8 pagesPrinciples of Learning: FS2 Field StudyKel Li0% (1)
- Day 4 - 10.7-8 Notes HandoutDocument4 pagesDay 4 - 10.7-8 Notes HandoutRusherNo ratings yet
- Week 006 - Module Sample Works of Well-Known WritersDocument13 pagesWeek 006 - Module Sample Works of Well-Known WritersLeona April DarriguezNo ratings yet
- Create and Open Input Dialog Box - MATLAB InputdlgDocument4 pagesCreate and Open Input Dialog Box - MATLAB InputdlgwhytheritoNo ratings yet
- ViShNu-Virachita Rudra StotramDocument6 pagesViShNu-Virachita Rudra StotramBhadraKaaliNo ratings yet
- Online Sales of New Cars: StudyDocument29 pagesOnline Sales of New Cars: StudyIson StudiosNo ratings yet
- Taylor Scientific ManagementDocument2 pagesTaylor Scientific ManagementworkingfolksNo ratings yet
- DLP IN LitDocument9 pagesDLP IN LitLotis VallanteNo ratings yet
- A Skunk, A Weasel and A Rat!Document174 pagesA Skunk, A Weasel and A Rat!WalliveBellair100% (1)