Professional Documents
Culture Documents
Content Server
Uploaded by
Nuryadi HermitaOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Content Server
Uploaded by
Nuryadi HermitaCopyright:
Available Formats
195
Review
Chronic thromboembolic pulmonary
http://econtent.hogrefe.com${contentReq.requestUri} - Deviprasad K <deviprasad@nes.co.in> - Monday, December 19, 2016 9:51:48 PM - EBSCO Publishing IP Address:140.234.255.9
hypertension a diagnostic and
therapeutic update
Hans Stricker
Angiology, Ospedale La Carit, Locarno, Switzerland
Summary: Chronic thromboembolic pulmonary hypertension (CTEPH), an important cause of severe pulmonary hypertension, is still underdia-
gnosed, mainly due to the insufcient use of V/Q scannning in patients with pulmonary hypertension. This article reviews the current diagnostic
approach and discusses the therapeutic options in this particular form of pulmonary hypertension. Every patient with CTEPH should undergo
an evaluation in a specialised centre with experience in pulmonary arterial endarteriectomy (PEA) as the potentially curative surgical tech-
nique. Partly unresolved questions regard the status of the recently described percutaneous transluminal pulmonary angioplasty and the best
medical treatment in patients with inoperable or recurrent/persistent pulmonary hypertension after PEA.
Key words: Chronic thromboembolic pulmonary hypertension, diagnosis, therapy, pulmonary thrombarteriectomy, riociguat
Introduction Denition
Chronic thromboembolic pulmonary hypertension (CTEPH) CTEPH is defined as precapillary pulmonary hyperten-
has been classified as a separate entity (group 4) within the sion by invasive right heart catheterisation with a mean
realm of pulmonary hypertension, although it shares some pulmonary artery pressure at rest 25 mm Hg and a
important similarities with pulmonary artery hyperten- mean pulmonary arterial wedge pressure 15 mm Hg
sion (PAH) at the level of small vessel changes. The main and documented chronic/organised flow-limiting
reasons for this are the potential curability which is unique thromboemboli in the elastic pulmonary arteries (main,
for patients suffering from pulmonary hypertension, and lobar, segmental, subsegmental) after at least 3 months
an apparently evident pathophysiological mechanism with of effective anticoagulation [1]. Risk factors for the de-
its history of venous thromboembolism. Several reviews velopment of CTEPH are inadequate anticoagulation,
on this topic were recently published [13], which include recurrent thromboembolism and occlusion of proximal
the findings discussed at the last World Symposium on pulmonary arteries. The condition is associated with lu-
Pulmonary Hypertension in Nice 2013. The aim of this ar- pus anticoagulants and/or antiphospholipid antibodies,
ticle is to review the pathophysiological characteristics, the and with elevated FVIII in blood plasma [5]. Other risk
diagnostic work-up and the current therapeutic options of factors include splenectomy, ventriculoatrial shunts, in-
the disease. fected pacemakers, chronic inflammatory conditions,
non-O blood groups, thyroid replacement, and malig-
nancy [6].
Epidemiology
The incidence of CTEPH after a documented venous Pathogenic mechanisms
thromboembolism varies by a factor of 20 among the stud-
ies (from 0.4 to 9.1, (1)) but seems to be <1% if only the After an episode of acute pulmonary embolism, complete
cases after a documented pulmonary embolism are con- resolution may be achieved in 708 5% of all patients 6 to
sidered. The difference in data may be due to referral bias, 12 months after initial PE diagnosis with partial resolution
the difficulty distinguishing between acute PE and CTEPH in the vast majority of the remaining patients [rev. in 7].
on imaging, and a specific patient history of the acute From V/Q scintigraphic studies, we know that the resolu-
event. In a large European registry, only 3 out of 4 patients tion of thrombi appears to reach a plateau after 3 months
with CTEPH reported a history of PE [4]. of adequate treatment [rev. in 7]. The exact mechanisms
2016 Hogrefe Vasa (2016), 45 (3), 195 199
DOI 10.1024/0301-1526/a000525
196 H. Stricker: CTEPH update
why thromboemboli will eventually be transformed in fi- In summary, the mechanisms depicted above in patients
brotic tissue that encroaches the lumen of the pumonary after acute pulmonary embolism could represent a continu-
vessels in up to 30% of patients is not known. Among the um of events that may, in rare instances, result in the clinical
factors for poor thrombus clearance, abnormal genetic entity of CTEPH, which would then be the final stage of that
variants of fibrinogen, predisposing pulmonary endotheli- which Klok et al. called a post-PE syndrome [7].
http://econtent.hogrefe.com${contentReq.requestUri} - Deviprasad K <deviprasad@nes.co.in> - Monday, December 19, 2016 9:51:48 PM - EBSCO Publishing IP Address:140.234.255.9
al cell abnormalities, impairments in the angiogenesis pro-
cess, and bacterial infection of fresh thrombi have been
suggested to play a role [7]. Classic thrombophilia includ-
ing antithrombin deficiency, protein C deficiency, protein Symptoms
S deficiency, factor V Leiden, and plasminogen deficiency
is not found more frequently in patients with CTEPH than The median age of patients with CTEPH is 63 years [4];
in patients with pulmonary embolism who do not develop although patients with CTEPH can present at any age, it is
CTEPH, and anomalies in circulating plasmatic fibrinolyt- rare in childhood. Both sexes are equally affected. CTEPH
ic factors are not involved [8, 9]. Besides the territories is less frequent than pulmonary artery hypertension
with unresolved thromboemboli, the development of (PAH). In a recently published report from the Swiss Regis-
CTEPH is characterised by involvement of the small pul- try, CTEPH was diagnosed roughly half as frequently as
monary arteries though a remodelling, which includes in- PAH (in 249 vs. 549 patients or 45%); interestingly, the
timal thickening, medial hypertrophy, and plexiform le- quote increased when comparing the diagnoses in the
sions, not only in areas that are affected but also in those years from 2000 to 2004 with those from 2009 to 2012
that are spared by thromboembolic occlusion. It is by this (from 35% to 58%, p=0.01), which could be the result of a
type of pulmonary arteriopathy that CTEPH closely re- qualitatively improved diagnostic work-up by better ad-
sembles the histopathology of patients with idiopathic herence to guidelines recommending V/Q scanning [10].
PAH with the occurrence of in situ thrombosis caused by a Symptoms of dyspnoea, fatigue, chest pain, syncope, pe-
dysfunctional endothelium that loses the anticoagulant ripheral oedema, and palpitations are unspecific, and di-
properties which usually prevent the intravascular clotting agnosis is often delayed. After a documented episode of
of blood material. Due to this distal pulmonary vascular pulmonary embolism, a period of honeymoon with ab-
remodelling specific for CTEPH, pulmonary artery pres- sence of symptoms is typically seen, after which dyspnoea
sure rises disproportionally to what could have been ex- reappears. Haemoptysis occurs more frequently in CTEPH
pected by the amount of areas with unresolved thrombi. compared with idiopathic PAH (4.8% versus 0.6%) [11].
Support for this hypothesis is provided by the lack of cor-
relation between pulmonary artery pressure and the de-
gree of angiographic pulmonary vascular bed obstruction,
by the progress of pulmonary hypertension without recur- Diagnosis
rent embolism, and by the higher pulmonary vascular re-
sistance in CTEPH patients compared to those with acute Given the unspecific nature of the symptoms, more common
PE and a similar obstruction index [7]. A large burden of pathologic conditions are frequently diagnosed. Conse-
small vessel arteriopathy constitutes the main limit in quently, if simple diagnostic techniques such as chest radi-
haemodynamic improvement after pulmonary thromben- ography or pulmonary function tests do not support clinical
darterectomy and offers the rationale for pulmonary vaso- settings such as COPD, asthma or deconditioning, pulmo-
dilator therapy in some CTEPH patients with prevalent nary hypertension should be considered. The subsequent
distal disease [6]. diagnostic work-up includes echocardiography and meas-
urement of BNP levels as a biomarker for right heart dys-
function. In fact, normal N-terminal proBNP together with
non-suspect ECG have been proposed as a means to exclude
CTEPH 6 months after a pulmonary embolism [12]. If echo-
cardiography suggests pulmonary hypertension, the subse-
quent diagnostic measures will follow in a step-wise fashion
[13]. Ventilation/perfusion scanning (V/Q scanning, Fig. 1)
with a negative predictive value of 98%, a sensitivity rate
of 96% and specificity rate of 90% for the detection of
CTEPH, is essential in distinguishing pulmonary hyperten-
sion from CTEPH. Ensuing right-heart catheterisation, ide-
ally combined with pulmonary angiography which is needed
to evaluate operability, will confirm pulmonary hyperten-
sion and assess its gravity. Computed tomographic pulmo-
nary angiography (Fig. 2) is widely used to provide confirma-
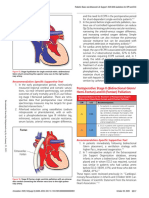
Figure 1. Pulmonary ventilation/perfusion scintigraphy. The perfusion
of the patient shows patchy central and wedge-shaped peripheral de- tory information, but this technique cannot be used to
fects of both lungs. exclude CTEPH (contrarily to V/Q scanning) or to be a sub-
Vasa (2016), 45 (3), 195 199 2016 Hogrefe
H. Stricker: CTEPH update 197
stitute for invasive angiography, due to a low 51% sensitivity
in diagnosing CTEPH. V/Q scanning is reportedly under-
used in the diagnostic work-up of pulmonary hypertension
(3), and efforts have to be made to improve adherence to di-
agnostic guidelines.
http://econtent.hogrefe.com${contentReq.requestUri} - Deviprasad K <deviprasad@nes.co.in> - Monday, December 19, 2016 9:51:48 PM - EBSCO Publishing IP Address:140.234.255.9
Catheter-based selective pulmonary angiography (Fig. 3)
is considered the gold-standard diagnostic tool for confir-
mation of CTEPH. It can be used to assess the extent and
distribution of disease which are essential data that can
provide the patients eligibility for PEA. Typical angio-
graphic defects represent organised and recanalised
thrombi following an acute thromboembolic event. These
include pulmonary artery webs or bands, intimal irregu-
larities, abrupt narrowing of the pulmonary arteries, proxi-
mal obstruction and pouch defects, and are very distinct
from those observed in acute PE.
Among newer diagnostic techniques magnetic reso-
nance pulmonary angiography may have a role in the func-
tional assessment of the right heart and the pulmonary
circulation and could play a role in pre- and post-operative
assessment of right ventricular function in the future, but Figure 2. CT- pulmonary angiography. This 70-year-old patient was di-
more expertise is needed for this technique confined to agnosed with pulmonary hypertension (mean pulmonary artery pres-
sure of 43 mmHg, pulmonary vascular resistance of 363 DS/cm5) as a
only a few centres. consequence of a supposed pulmonary embolism nine months earlier.
The angiographic reconstruction shows abrupt vessel narrowing, int-
raluminal bands, irregular vascular wall thickening and dilated central
pulmonary arteries.
Treatment
CTEPH is associated with a dismal prognosis in the ab- Prior to the intervention, angiography is currently the
sence of specific intervention. Especially in the presence gold standard for the anatomical assessment of pulmonary
of signs and symptoms of right heart failure the average artery obstructions, which together with right-heart cath-
survival is poor, as demonstrated in a study where it was eterisation is essential for distinguishing proximal, opera-
found to be only 1.7 years after diagnostic catheterisation; ble CTEPH from distal disease. Most patients will have
in contrast, without heart failure, patients lived on average
4.7 years. If the mean pulmonary artery pressure meas-
ured >50 mmHg, the 2-year survival was 20% [14].
All patients should receive life-long anticoagulation in
order to prevent recurrent venous thromboembolism.
Formally, the new direct oral anticoagulants have not
been tested, and until more data are available, it may be
prudent for patients to be anticoagulated with vitamin K
antagonists.
Surgical treatment
Pulmonary endarterectomy (PEA) is the treatment of choice
and has the potential to cure some of the patients with
CTEPH. It is a surgically demanding technique and requires
experience for the assessment of operability as well as tech-
nical skills for its performance. There are only a few centres
worldwide with a case load >1000 interventions and its deli-
cate postoperative surveillance necessary to obtain a periop-
erative mortality <5% [15]. An expert centre is by definition
one that performs at least 20 PEA operations per year with a
Figure 3. Pulmonary angiography (Courtesy of Diagnostic Radiology,
mortality rate of <10%. Recent guidelines recommend that
Uniklinik Giessen). The preoperative angiography of the index patient
expert centres should aim at improved mortality rates (<7%) shows constrictive bands and abrupt vessel narrowing in one of the
and early haemodynamic improvements after PEA [16]. examined lobar arteries.
2016 Hogrefe Vasa (2016), 45 (3), 195 199
198 H. Stricker: CTEPH update
haemodynamic abnormalities at rest, but in selected cas- tients with inoperable CTEPH or with persistent/recurrent
es, patients with markedly increased pulmonary vascular pulmonary hypertension after PEA, treated with Riociguat
resistance upon exercise have shown to benefit from surgi- or placebo for 16 weeks (CHEST-1), followed by an open
cal intervention [15]. It must be underscored that patients trial (CHEST-2). After 16 weeks, the 6 minute walking test
should be evaluated only by an expert team in PEA before significantly increased by 46 meters (primary endpoint),
http://econtent.hogrefe.com${contentReq.requestUri} - Deviprasad K <deviprasad@nes.co.in> - Monday, December 19, 2016 9:51:48 PM - EBSCO Publishing IP Address:140.234.255.9
operations may be withheld. Temporal delay to evaluation and also the secondary endpoints NT-proBNP, PVR and
of operability can result in a negative outcome, and medi- WHO-class improved significantly [19]. This agent subse-
cal bridging while postponing a specific assessment is not quently to the positive results of the trial has been licensed
recommended [15]. as the first specific medical treatment for non-operable
The operation is performed in deep hypothermic circu- CTEPH and for persistent pulmonary hypertension after
latory arrest. Dissection of pulmonary arteries of both PEA. Importantly, riociguat cannot be combined with
lungs are performed as distally as possible to minimise PDE5-inhibitors [20], whereas a combination with en-
postoperative residual pulmonary hypertension. Perioper- dothelin antagonists or prostanoids is possible.
ative complications include lung reperfusion injury in
<10% of patients, characterised by pulmonary oedema
and treated by ECMO, and neurocognitive impairment
due to prolonged circulatory arrest. Operative mortality Conclusions
correlates with preoperative pulmonary vascular resist-
ance (PVR) but there are no upper limits of PVR, pulmo- CTEPH, an important cause of severe pulmonary hyperten-
nary artery pressure or parameters of right heart insuffi- sion, is still underdiagnosed, and the use of V/Q scanning as
ciency that preclude surgery. Up to 30% of the patients part of the diagnostic approach in patients with pulmonary
may present with postoperative residual/persistent pul- hypertension is essential. Every patient with CTEPH should
monary hypertension, which negatively influences prog- undergo evaluation in a specialised centre with a large expe-
nostic outcomes. Those patients may be candidates for rience in PEA. Partly unresolved questions regard the status
medical treatment [15]. of BPA and the best medical treatment in patients with inop-
erable or recurrent/persistent PH after PEA.
Percutaneous transluminal pulmonary
angioplasty (BPA)
References
The feasibility of balloon dilatation of obstructed pulmo-
nary arteries was first demonstrated in 2001, and the safe- 1. Lang IM, Madani M. Update on chronic thromboembolic pul-
monary hypertension. Circulation 2014; 130 (6): 508 18.
ty and efficacy have been shown in a Japanese study which
2. Androulakis E, Lioudaki E, Christophides T, et al. Chronic
included 70 mostly elderly patients; however, critical rep- thromboembolic pulmonary arterial hypertension: a review of
erfusion pulmonary oedema and vessel injuries may be an the literature and novel therapeutic approaches. Expert Rev
issue [17]. Further studies including the results of long- Respir Med 2015; 9: 351 9.
3. Kim NH, Delcroix M, Jenkins DP, et al. Chronic thromboembolic
term outcomes are needed in order to resolve uncertain-
pulmonary hypertension. J Am Coll Cardiol 2013; 62 (25 Suppl):
ties in the approach of CTEPH by this technique. D92 9.
4. Pepke-Zaba J, Delcroix M, Lang I, et al. Chronic thromboem-
bolic pulmonary hypertension (CTEPH): results from an inter-
national prospective registry. Circulation 2011; 124: 1973 81.
Medical treatment 5. Wilkens H, Lang I, Blankenburg T, et al. [Chronic thromboem-
bolic pulmonary hypertension--a position paper]. Dtsch Med
Recently published data from a registry revealed that more Wochenschr 2014; 139 (Suppl 4): S155 65.
than one third of patients are treated with specific drugs for 6. LeVarge BL, Channick RN. Chronic thromboembolic pulmonary
hypertension: evolution in management. Curr Opin Pulm Med
pulmonary hypertension, irrespective of their operability
2014; 20: 400 8.
[4]. They include endothelin antagonists (Bosentan), pros- 7. Klok FA, van der Hulle T, den Exter PL, et al. The post-PE syn-
tanoids (epoprostenol, treprostinil), and PDE5-inhibitors drome: a new concept for chronic complications of pulmonary
(sildenafil, tadalafil, vardenafil). The results from various embolism. Blood Rev 2014; 28: 221 6.
8. Wolf M, Boyer-Neumann C, Parent F, et al. Thrombotic risk fac-
studies with bosentan were analysed in a meta-analysis
tors in pulmonary hypertension. Eur Respir J 2000; 15: 395 9.
with an improvement of haemodynamics and probably of 9. OlmanMA, Marsh JJ, Lang IM, et al. Endogenous brinolytic
exercise parameters [18]. The data for prostanoids have also system in chronic large-vessel thromboembolic pulmonary
shown an improvement of haemodynamics, exercise capac- hypertension. Circulation 1992; 86: 1241 8.
10. Mueller-Mottet S, Stricker H, Domeninghetti G, et al. Long-
ity (epoprostenol, treprostinil), and survival (treprostinil),
term data from the Swiss pulmonary hypertension registry.
whereas PDE5-inhibitors, although well tolerated and with Respiration 2015; 89: 127 40.
positive influence on certain paraclinical parameters, lack 11. Lang IM, Simonneau G, Pepke-Zaba JW, et al. Factors associ-
well-designed studies with respect to survival [2]. ated with diagnosis and operability of chronic thromboembol-
ic pulmonary hypertension: a case-control study. Thromb Hae-
Riociguat is a novel drug, which stimulates soluble gua-
most 2013; 110: 83 91.
nylate cyclase (sGC). The CHEST study included 261 pa-
Vasa (2016), 45 (3), 195 199 2016 Hogrefe
H. Stricker: CTEPH update 199
12. Klok FA, Tesche C, Rappold L, et al. External validation of a tematic review and meta-analysis. Thromb Res 2010; 126:
simple non-invasive algorithm to rule out chronic thromboem- e51 6.
bolic pulmonary hypertension after acute pulmonary embo- 19. Ghofrani HA, DArmini AM, Grimminger F et al. Riociguat for the
lism. Thromb Res 2015; 135: 796-801. treatment of chronic thromboembolic pulmonary hyperten-
13. DArmini AM. Diagnostic advances and opportunities in chron- sion. N Engl J Med 2013; 369: 319 29.
20. Bayer Pharma AG. Adempas (riociguat) EU Summary of Prod-
http://econtent.hogrefe.com${contentReq.requestUri} - Deviprasad K <deviprasad@nes.co.in> - Monday, December 19, 2016 9:51:48 PM - EBSCO Publishing IP Address:140.234.255.9
ic thromboembolic pulmonary hypertension. Eur Respir Rev
2015; 24: 253 62. uct Characteristics 2014. www.ema.europa.eu/docs/en_GB/
14. Riedel M, Stanek V, Widimsky J, et al. Longterm follow-up of document_library/EPAR_-_Product_Information/hu-
patients with pulmonary thromboembolism. Late prognosis man/002737/WC500165034.pdf.
and evolution of hemodynamic and respiratory data. Chest
Submitted: 20.08.2015
1982; 81: 151 158.
Accepted after revision: 10.11.2015
15. Jenkins D. Pulmonary endarterectomy: the potentially curative
There are no conicts of interest existing.
treatment for patients with chronic thromboembolic pulmo-
nary hypertension. Eur Respir Rev 2015; 24: 263 271. Correspondence address
16. Kim NH, Mayer E. Chronic thromboembolic pulmonary hyper- Dr. Hans Stricker, MD
tension: the evolving treatment landscape. Eur Respir Rev Angiology
2015; 24: 173 177. Ospedale La Carit
17. Yanagisawa R, Kataoka M, Inami T, et al. Safety and efcacy of Via allOspedale 1
percutaneous transluminal pulmonary angioplasty in elderly 6600 Locarno
patients. Int J Cardiol 2014; 175: 285 9. Switzerland
18. Becattini C, Manina G, Busti C, et al. Bosentan for chronic
thromboembolic pulmonary hypertension: ndings from a sys- hans.stricker@eoc.ch
2016 Hogrefe Vasa (2016), 45 (3), 195 199
Copyright of Vasa: Zeitschrift fr Gefaesskrankheiten is the property of Hogrefe AG and its
content may not be copied or emailed to multiple sites or posted to a listserv without the
copyright holder's express written permission. However, users may print, download, or email
articles for individual use.
You might also like
- Critical Care NursingDocument10 pagesCritical Care Nursingianecunar100% (10)
- CTEPH and Klippel Trenaunay SyndromeDocument6 pagesCTEPH and Klippel Trenaunay SyndromeAndreiSefNo ratings yet
- HTP Por Tep Cronico Tto Respiratory Medicine 2021Document12 pagesHTP Por Tep Cronico Tto Respiratory Medicine 2021Gustavo GomezNo ratings yet
- RG 220078Document17 pagesRG 220078Andiie ResminNo ratings yet
- Technegas Specs Flyer v1 20181025Document2 pagesTechnegas Specs Flyer v1 20181025Renaoval AchillesNo ratings yet
- 1 s2.0 S1053077021005723 PDFDocument13 pages1 s2.0 S1053077021005723 PDFangelicaNo ratings yet
- Pulmonary Hypertension in Cardiac SurgeryDocument14 pagesPulmonary Hypertension in Cardiac SurgeryinaNo ratings yet
- Austin Journal of Anesthesia and AnalgesiaDocument3 pagesAustin Journal of Anesthesia and AnalgesiaAustin Publishing GroupNo ratings yet
- Najah PosterDocument1 pageNajah PosterDl Al-azizNo ratings yet
- Echocardiographic Evaluation of Pericardial Effusion and Cardiac TamponadeDocument10 pagesEchocardiographic Evaluation of Pericardial Effusion and Cardiac TamponadeGustiTiballaNo ratings yet
- Modern Invasive Hemodynamic Assessment of Pulmonary HypertensionDocument11 pagesModern Invasive Hemodynamic Assessment of Pulmonary HypertensionfabiolaNo ratings yet
- Ecocardiografia Monitoreo Hemodinamico en Critico..Document12 pagesEcocardiografia Monitoreo Hemodinamico en Critico..cositaamorNo ratings yet
- Anaesthesia in Dogs and Cats With Cardiac DiseaseDocument19 pagesAnaesthesia in Dogs and Cats With Cardiac DiseaseALEJANDRA MADRIGALNo ratings yet
- Clinical Update On Pulmonary Hypertension: Salim Yaghi, Anastasia Novikov, Theo TrandafirescuDocument7 pagesClinical Update On Pulmonary Hypertension: Salim Yaghi, Anastasia Novikov, Theo TrandafirescuIs DGNo ratings yet
- 4 Arterial, Central Venous, and Pulmonary Artery CathetersDocument12 pages4 Arterial, Central Venous, and Pulmonary Artery CathetersToujours ÁmeNo ratings yet
- Pulmonary Hypertension: Annals of Internal MedicinetDocument16 pagesPulmonary Hypertension: Annals of Internal MedicinetAlicia TGNo ratings yet
- HEMOPTISISDocument6 pagesHEMOPTISISJufrialdy AldyNo ratings yet
- Pulmonary Hypertension Feb 2006Document6 pagesPulmonary Hypertension Feb 2006lucasNo ratings yet
- Acute DyspneaDocument37 pagesAcute Dyspneaisnaira imamNo ratings yet
- Journal Pulmonary HypertensionDocument8 pagesJournal Pulmonary HypertensionFirman SyahNo ratings yet
- Aca 21 116Document7 pagesAca 21 116FreddyNo ratings yet
- Infographics Pulmonary EdemaDocument1 pageInfographics Pulmonary EdemaSwag MasterNo ratings yet
- Advanced Management of Intermediate High Risk Pulmonary EmbolismDocument8 pagesAdvanced Management of Intermediate High Risk Pulmonary EmbolismcastillojessNo ratings yet
- Journal Reading Transcatheter Aortic Valve Replacement Under Monitored Anesthesia Care Versus General Anesthesia With IntubationDocument23 pagesJournal Reading Transcatheter Aortic Valve Replacement Under Monitored Anesthesia Care Versus General Anesthesia With IntubationTomy SandriyaNo ratings yet
- New Pharmacologic Therapies For AHFDocument9 pagesNew Pharmacologic Therapies For AHFDaniel HernandezNo ratings yet
- Monitoring Fluid ResponsivenessDocument7 pagesMonitoring Fluid Responsivenessvaleria SepviNo ratings yet
- Jim 2020 001291.fullDocument7 pagesJim 2020 001291.fullAlessioNavarraNo ratings yet
- Perioperative Management of Pulmonary Hypertensive Crisis: AsktheexpertDocument2 pagesPerioperative Management of Pulmonary Hypertensive Crisis: AsktheexpertGede AdiNo ratings yet
- HRT 08900369Document2 pagesHRT 08900369Gonzalo Cedrés Di MarcoNo ratings yet
- Cpap Vs Vni - PasquinaDocument8 pagesCpap Vs Vni - PasquinaMelina AlcaineNo ratings yet
- Hepatology - 2004 - Colle - Diagnosis of Portopulmonary Hypertension in Candidates For Liver Transplantation A ProspectiveDocument9 pagesHepatology - 2004 - Colle - Diagnosis of Portopulmonary Hypertension in Candidates For Liver Transplantation A ProspectiveYasin DeveliogluNo ratings yet
- Hemodynamics 3443434Document12 pagesHemodynamics 3443434lolopoponakerNo ratings yet
- Chest Tube Drainage of The Pleural SpaceDocument10 pagesChest Tube Drainage of The Pleural SpaceFernandaNo ratings yet
- Eco DopplerDocument8 pagesEco DopplerClaudia IsabelNo ratings yet
- Masip NIV EHJ 2018Document12 pagesMasip NIV EHJ 2018Assessoria da Gerência Geral HEHANo ratings yet
- Invasive ProcedureDocument12 pagesInvasive ProcedureAngelica PabelloNo ratings yet
- Casco Vs CNAFDocument9 pagesCasco Vs CNAFScott JonesNo ratings yet
- Alternatives To Swan Ganz CatheterDocument12 pagesAlternatives To Swan Ganz CatheterJhonatan AndradeNo ratings yet
- Hepatopulmonary Syndrome (HPS)Document2 pagesHepatopulmonary Syndrome (HPS)Cristian urrutia castilloNo ratings yet
- 1 FullDocument4 pages1 FullMuli YamanNo ratings yet
- Acute Respiratory Distress Syndrome PDFDocument14 pagesAcute Respiratory Distress Syndrome PDFayuNo ratings yet
- Pengaruh Positive End Expiratory Pressure Terhadap Nilaicentral Venous PressureDocument14 pagesPengaruh Positive End Expiratory Pressure Terhadap Nilaicentral Venous PressureRahmatSutopoNo ratings yet
- Parte 4 (49-55)Document7 pagesParte 4 (49-55)biasilvacarvalho98No ratings yet
- Paper 7, Corrado 2017Document8 pagesPaper 7, Corrado 2017NITIN SENTHILKUMARNo ratings yet
- Termodiluicao PulmonarDocument7 pagesTermodiluicao PulmonarKarina ResendeNo ratings yet
- Hoeper 2016Document14 pagesHoeper 2016riyad saksakNo ratings yet
- Breathing Problems and Thoracic TraumaDocument16 pagesBreathing Problems and Thoracic TraumaVlad ZecaNo ratings yet
- MainDocument11 pagesMainDhonz R AdiwaramanNo ratings yet
- Acute Respiratory Distress Syndrome - NursingDocument14 pagesAcute Respiratory Distress Syndrome - NursingyellowbyunsNo ratings yet
- Cateter Arteria Pulmonar 2011Document7 pagesCateter Arteria Pulmonar 2011jerodriguez82No ratings yet
- Norepinephrine in Septic Shock: When and How Much?: ReviewDocument6 pagesNorepinephrine in Septic Shock: When and How Much?: ReviewCielo Rodriguez DezaNo ratings yet
- Riphah International University: Cardiopulmonary Physical TherapyDocument6 pagesRiphah International University: Cardiopulmonary Physical Therapykhalid.zainabNo ratings yet
- Breathing Problems and Thoracic TraumaDocument16 pagesBreathing Problems and Thoracic TraumaLory cNo ratings yet
- Anesthetic Management For Cardiopulmonary BypassDocument16 pagesAnesthetic Management For Cardiopulmonary BypassAhmet PinarbasiNo ratings yet
- Monitoring of Total Positive End Expiratory Pressure During Mechanical Ventilation by Artificial Neural NetworksDocument10 pagesMonitoring of Total Positive End Expiratory Pressure During Mechanical Ventilation by Artificial Neural NetworksRespiratory Care ZoneNo ratings yet
- DynaMed Plus - Pulmonary Embolism (PE)Document85 pagesDynaMed Plus - Pulmonary Embolism (PE)Gamer MadaNo ratings yet
- 20171200.0-00009 WWWWDocument16 pages20171200.0-00009 WWWWNataliaMaedyNo ratings yet
- Young Man With Cardiac Arrest Secondary To Undiagnosed Mediastinal MassDocument4 pagesYoung Man With Cardiac Arrest Secondary To Undiagnosed Mediastinal MassPxPPxH ChanNo ratings yet
- Intervensi Pulmo Konas Perpari-1Document32 pagesIntervensi Pulmo Konas Perpari-1Rivani KurniawanNo ratings yet
- Monitoring Mechanical Ventilation Using Ventilator WaveformsFrom EverandMonitoring Mechanical Ventilation Using Ventilator WaveformsNo ratings yet
- HEPALISA - 4 Page - PMDDocument4 pagesHEPALISA - 4 Page - PMDHoD MicrobiologyNo ratings yet
- Book Eczema PsoriazisDocument457 pagesBook Eczema Psoriazisdaniel bNo ratings yet
- HIFUDocument1 pageHIFUKaye RabadonNo ratings yet
- CNS DrugsDocument57 pagesCNS DrugsHussein Al-jmrawiNo ratings yet
- Argumentative Text (Graphic Organizer) - LauretaDocument1 pageArgumentative Text (Graphic Organizer) - LauretaPaul Vincent LauretaNo ratings yet
- Sexually Transmitted DiseasesDocument76 pagesSexually Transmitted Diseasessomaya abdulhakimNo ratings yet
- Stroke Hemoragic: Sebagai Salah Satu Tugas Mata Kuliah TIK Akademi Keperawatan (Akper) SawerigadingDocument10 pagesStroke Hemoragic: Sebagai Salah Satu Tugas Mata Kuliah TIK Akademi Keperawatan (Akper) SawerigadingMade Serly KrisdayantiNo ratings yet
- Cefotaxime 1Document3 pagesCefotaxime 1DidikNo ratings yet
- 2 Months Well Child CheckDocument3 pages2 Months Well Child CheckJanelleNo ratings yet
- Era University / Era College of Nursing: Lesson Plan On-Breast GynecomastiaDocument8 pagesEra University / Era College of Nursing: Lesson Plan On-Breast GynecomastiaShreya SinhaNo ratings yet
- Patient EducationDocument14 pagesPatient EducationJ Therese NorrellNo ratings yet
- Upper GI Endoscopy Referral Form - InHealth GroupDocument2 pagesUpper GI Endoscopy Referral Form - InHealth GroupAbdullahi AhmedNo ratings yet
- Oet Writing Sample 01 EnglishDocument52 pagesOet Writing Sample 01 EnglishMuhammad Ahmad RazaNo ratings yet
- What Are The Biological Agents That Can Be Utilized For Bioterrorism?Document30 pagesWhat Are The Biological Agents That Can Be Utilized For Bioterrorism?anukriti shrivastavaNo ratings yet
- Effects of Smoking & What Is Passive Smoking?Document9 pagesEffects of Smoking & What Is Passive Smoking?天天No ratings yet
- Placenta Previa ManagementDocument28 pagesPlacenta Previa ManagementAhsan AuliyaNo ratings yet
- Important MCQDocument23 pagesImportant MCQFarrukh Ali KhanNo ratings yet
- Patofisiologi VenaDocument5 pagesPatofisiologi VenaNisa AriyantiiNo ratings yet
- Impact of Covid 19 On EnvironmentDocument20 pagesImpact of Covid 19 On EnvironmentRamkishan JaiswarNo ratings yet
- Protocol TPEDocument19 pagesProtocol TPEPatricia TamasNo ratings yet
- NLEP-Bsc NSG pt-IVDocument6 pagesNLEP-Bsc NSG pt-IVSree LathaNo ratings yet
- Report of Mr. SAURABH SHIVAJI WAGHMAREDocument1 pageReport of Mr. SAURABH SHIVAJI WAGHMAREShivaniNo ratings yet
- ReportDocument4 pagesReportRancho AmithNo ratings yet
- Sas 15 MCN Lec 2Document3 pagesSas 15 MCN Lec 2Jhoanna Marie VillaverdeNo ratings yet
- Changes in Preventive Care Benefits Due To Health Care ReformDocument3 pagesChanges in Preventive Care Benefits Due To Health Care Reformv4meetNo ratings yet
- An Observational Study Use of Systemic Antibiotics For Endodontic Infections TreatmentDocument17 pagesAn Observational Study Use of Systemic Antibiotics For Endodontic Infections TreatmentAthenaeum Scientific PublishersNo ratings yet
- Fluid and Electrolyte Therapy During Vomiting and DiarrheaDocument22 pagesFluid and Electrolyte Therapy During Vomiting and Diarrheafernin96No ratings yet
- Philippine CPG-2013-uti in Adults-Part1 PDFDocument82 pagesPhilippine CPG-2013-uti in Adults-Part1 PDFVirginia AbalosNo ratings yet
- ASTHMA & COPD (Emphysema, CB) (CHAP 20)Document10 pagesASTHMA & COPD (Emphysema, CB) (CHAP 20)Abegail QuintoNo ratings yet
- RCL Employment Medical Examination Form A (New-Returning) Revised 2015-03Document2 pagesRCL Employment Medical Examination Form A (New-Returning) Revised 2015-03Ahmad ShodiqNo ratings yet