Professional Documents
Culture Documents
Congestive Heart Failure - Dra. Deduyo
Uploaded by
Medisina101Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Congestive Heart Failure - Dra. Deduyo
Uploaded by
Medisina101Copyright:
Available Formats
CONGESTIVE HEART FAILURE CARDIOLOGY
Growing Burden of Heart Failure anything, in the middle of the night, he awaken with
increasing difficulty of breathing to the point that he has to sit
Heart Failure is one of the most common and important clinical problems in up.
Cardiology In order to be able to breathe well, drink small amount of
water in hoping that difficulty of breathing will relieve. There
One year mortality rate (NYHA IV ): 30-50% is 2-3 pillows orthopnea or in the other words the last few
Prevalence of heart failure is rising in individualized countries months, he tries to elevate his head to be able to breathre
Due to aging population, hypertension and improved survival in better and there was peripheral edema that he did not paying
CAD (post MI) attention
Most admissions usually in the ICU or even in the ward is due to Having this problem of PND and orthopnea, is this a patient in
heart failure, or any patient having ischemic disease, or necessarily failure? Is this a patient with primary pulmonary disease? Like
having hypertension, or coronary artery disease, it may be also due a COPD or we would like to know is this a patient with
to valvular heart diseases or any other diseases even primary hypertension? Is this a patient with diabetes? Or is this a
diseases such as congenital heart disease can manifest as heart patient in the process of some of episodes of on and off chest
failure in the later part of their life pain which he did not pay attention to. Is this a patient would
However, because of the aging population we were able to control be smoking before, as we would like to know if a COPD patient
hypertension, treat our patient with coronary artery disease, with having episodes of orthopnea and PND , he is also found a
necessary revascularization as angioplasty and bypass it is also the pulmonary patient and he said that yes, I was smoking
same that we end up with a heart failure sometime in their life before but I already stopped it 8 years ago
The overall estimated rate is 3-20/1,000 population and those 65 We would like to know either there is a maintenance
years of age, 10% of the age group are in the stage of heart failure medication, he tells about an ACE inhibitor, a beta blocker,
furosemide and DPPT inhibitor with an additional of
Clinical Scenario metformin
He is indeed hypertensive and indeed diabetic based on the
73 y/o, Male, 10 days productive cough of greenish yellowish
medications that he being used. Knowing that he is
phlegm
hypertensive what will have in mind is the blood pressure ba
1-2 days of increasing dyspnea on exertion and at rest
ay controlled, we took the BP it is 150/90 what will you say? Is
1 yr hx of breathlessness in doing ordinary activities in the house
the hypertension controlled? NO! He is also using 3 drugs,
2-3 pillows orthopnea
meron siyang ACE inhibitor, beta blocker may diuretic pa but
Consistent peripheral edema
despite of that they still not control
Occasional episodes of paroxysmal nocturnal dyspnea
His heart rate is 93 beats per min inspite of the beta blocker
therapy his weight is 141 lbs in other words, di naman siya
Medical History
mataba
Hypertension But we are attracted to visible neck vein at 45 degrees. What
Diabetes do we expect on the neck vein but the patient is semi
Denies having angina recumbent at 45 degrees should it be normally distended or
Stopped smoking 8 years deep, not visible. We should not feel anything, it should not be
visible. Kasi upright na siya eh, hindi bale kung nakahiga
Meds: ACE inhibitor, Beta Blocker, Furosemide, DPP4 inhibitor, because you increase venous return in to the right side of the
Metformin heart so this is but normal that at 30 degrees that jugular vein
is still visible. So this is abnormal and the next thing we do is
Physical Exam to determine, nahihirapan huminga, inuubo, ang attention
natin yung baga right? Because the chief complaint is cough,
BP: 150/90 mmHg, HR: 93 bpm, Wt: 141 lbs productive of yellowish green sputum. Do you agree that we
Neick vein distended at 45 degrees should examine the lungs, because we are interested to know
Lungs: bilateral basal crackles whether crackles are present or not and true enough there is
Heart: regular rhythm, displaced apical beat with normal S1, loud bilateral basal crackles.
S2 (+LVS3) grade 3/6 apical systolic murmur What if the crackles is one sided and this patient is having cough,
Abdomen: (+) hepatojugular reflex what is your assessment? Kung one sided lang, kaliwa o kanan, at
LE: cold, mild pedal edema inuubo yung pasyente, it could be pneumonia kung one sided yan
A typical patient 73 years old presenting with 10 days cough but I just want to emphasize that crackles of heart failure is
productive of yellowish green sputum, 1-2 days increasing BILATERAL. Although we do not stop the possibility that there will
dyspnea upon activity and worried because the difficulty of be underlying pneumonia or a community acquired pneumonia as a
breathing even felt even resting at home precipitating factor.
However in the past, there is already shortness of breath, The apical beat is displaced. Where the apical beat is displaced?
restlessness in doing the usual activity at home Pababa ba? On the side? To the side, horizontally. To the left kasi
Majority of these patients even though they know there is apex more pointed to the left. Kung nadisplaced siya, di siya
something wrong they still try to do something because what nadisplaced pakanan di ba? Papunta siya ng kaliwa. When is the
is on their mind if I stay over the more that I feel weaker apical beat displaced, sideward and downward? Remember the
Kaya pinipilit nila, not knowing that their heart is in failure. He right ventricle is the most anterior portion of the heart, pero kapag
is awakening at night with episodes of paroxysmal nocturnal left ventricle kapag yan ay nadisplace sideward and downward it
dyspnea. What does it mean? He sleeps like he dont feel means to say that there is dilatation of the ventricle with volume
Et factum estutamicistranscribit 2014 -2015
Dra.Deduyo Page 1 of 10
durumsimul in unum! medicine vade MARIE
CONGESTIVE HEART FAILURE CARDIOLOGY
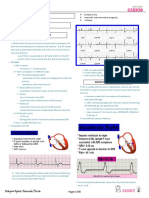
overloading, malakas ang volume inside, and form of the pressure S3 gallop Tachycardia (HR > 120 bpm)
and what you see among valvular heart diseases especially aortic
regurgitation and mitral regurgitation with volume overloading. Increased JVD > 16 cm H20 Vital capacity < 1/3 from maximum
Still the S1 is still normal, because the patient is dyspneic, there is a
loud S2 so when we say loud S2, S2 is loud all over not only the apex Hepatojugular reflex
but all valvular areas. In this condition, we usually ask the patient to
sit upright, try to split the S2 to determine which is loud, is it the A2
or the P2? Why do we want to know whether the P2 is the one that Definitive CHF = 2 major criteria or 1 major & 2 minor criteria
is loud because we are considering the possibility concomitant to
the dyspnea and those crackles there could be some degree also of Having in mind that the patient having a heart failure we will used
pulmonary hypertension as a part of the pulmonary congestion. the so called FRAMINGHAMS CRITERIA, divided into major and
And there is what we are looking for, a LVS3 GALLOP. The LVS3 minor criteria. Remember in paediatrics, if the diagnosis of the
gallop is the hallmark in the diagnosis of patient with heart patient with rheumatic fever, we also use the Jones Criteria for the
failure. diagnosis, dividing it a major and minor criteria.
S3 could be present but... (nainterrupt) S3 gallop, hindi lahat heart In major citeria. orthopnea and PND? Yes. Neck vein distention?
failure but always remember this, ano ang gagamitin ninyo Yes. Crackles? Meron. Cardiomegaly? Meron. Because the apical
stethoscope kung S3 ang hinahanap? The BELL bakit? Kasi yun ay beat is displaced so the heart is displaced, there is cardiomegaly.
LOW PITCH Acute pulmonary edema? Wala! Kasi kung pulmonary edema you
Now, every S3 is also found in patients with volume overloading, have crackles all over, e basal crackles lang ito. Hindi pa siya
with mitral regurgitation or aortic regurgitation or combination pulmonary edema.
thereof. And this patient presents apical holosystolic murmur as When you say that there is pulmonary edema, you dont need the
transmitted in the region of axilla. stethoscopeto be able to hear the crackles and your patient is
So, ano yang holosystolic murmur na yan? AR? MR? TR? Kung markedly orthopneic. Ang sound nyan parang alam mo yung
meron kang systolic murmur sa apex, and it is holosystolic, MITRAL oxygen bottle? Parang kumukulo. It is bubbling and most often the
siguro yan kasi apex yan. However, you have to do breathing to patient cough out reddish. Meron siyang hemoptysis because of the
determine whether it is affected by breathing. So it may be loud severe pulmonary congestion (wala siya pulmonary edema), meron
during breathing so it is not mitral but it is TRICUSPID. If it not lang siya bilateral basal crackles.
affected by breathing, that is a MITRAL so you do transmission, it is May S3 gallop ba? Yes. And if we are going to measure at the
transmitted to the axilla or even at the back. Why? Because the bedside the jugular venous pressure at 45 degrees kita natin yan,
flow of blood from LV to LA, and where is the left atrium? It is at the siguradong mataas ang JVP and hepatojugular reflux is positive.
back, posterior. Ang definitive niyan ay dalawa lamang, diagnosed na. So we are
In the abdomen, since we saw that there is a visibility of the neck very sure that we are dealing a patient with a heart failure.
vein, we do some pressure on the liver area. Upon pressure of the Minor criteria would be ankle edema, di natin pinakialam kasi
liver area, we bring more blood in to the right side of the heart and marami pa may edema, night cough, dyspnea in exertion meron
if there is increase pressure in the right atrium and the right siya nito, hepatomegaly,wala; pleural effusion, wala; tachycardia,
ventricle, so there will be resistance to the right atrial and right 93 lang so hindi; vital capacity is less than 1/3 from maximum
ventricular inflow, so what will be happen? There is more Even with 1 major and 1 of these minor criteria will be able to
distention, of the jugular vein. Why that is increased pressure in the consider that the patient is in failure.
right side of the heart? Because there is pulmonary congestion as
proven that there is bilateral basal crackles. Accuracy of Various HF Parameter
Since the hallmark in a patient with heart failure is that it is a low
output failure, meaning there is diminished cardiac output. So what Variable Sensitivity Specificity Accuracy
will happen in the circulation in the periphery? There will be
diminished peripheral circulation so when you tried to touch the History of HF 62 94 90
patient, will the patient feel warm? Hindi. Malamig ang pasyente
mo. And as you go more to the periphery, to the lower extremity, Dyspnea 56 53 54
lalo na siyang malamig kasi pinakahuli siya maperfuse, the lower
extremities, so it is cold. Orthopnea 47 88 72
Framingham Criteria for the Diagnosis of CHF Rales 56 80 70
Major Criteria Minor Criteria JVD 39 94 72
orthopnea & PND Ankle edema S3 20 99 66
neck vein distention Night cough Edema 67 68 68
crackles Dyspnea on exertion
Cardiomegaly Hepatomegaly
Acute pulmonary edema Pleural effusion
Et factum estutamicistranscribit 2014 -2015
Dra.Deduyo Page 2 of 10
durumsimul in unum! medicine vade MARIE
CONGESTIVE HEART FAILURE CARDIOLOGY
Most useful findings for confirming presence of HF: S3 and elevated JVD
Studies have shown that there are different variables, so these are
the most common manifestation and symptoms of the patient.
Dyspnea, orthopnea, crackles on auscultation, S3 on auscultation,
jugular venous distention and edema on inspection.
With its accuracy you will know 90% is the history of heart failure,
specificity 94%, sensitivity is 62%, so nagdududa ka pa kung failure
nga kasi there are other manifestations / diseases manifesting as
difficulty of breathing. Dyspnea as you would see, is not accurate.
Orthopnea is better, specificity is 88%, accuracy 72% and sensitivity
is only 47%. Crackles 56% sensitivity, 80% specificity, and 70%
accuracy. But your S3 gallop and jugular vein distention, seems to
be a specific and most useful finding to confirm indeed a heart
failure is present indeed in our patient.
Whenever you have a patient who is dyspneic, and orthopneic,
tingnan mo yung leeg, paupuin ninyo ang pasyente ninyo, because
it is more accurate if the patient is sitting down esoecially if there is
edema. Most patients are bothrered and worried with the presence
of edema. Pag nagcomplain ang pasyente mo, tingnan mo ang
leeg. If you see a visible jugular vein, and ask your patient how do
you sleep at night? Do you lie down flat? Or you need several
pillows to support your back or you wanted to sit upright to have a
better feeling of comfort during breathing. It is only then you will
consider heart failure.
Systolic Vs Diastolic HF
Have in this in mind, what is the vicious cycle of heart failure? The
To differentiate; an echocardiogram is necessary. Diastolic
Systolic
There are many classification of heart failure and will divide into
Impaired LV
systolic and diastolic. The symptomatic is the systolic failure. Pathophysiology Impaired LV relaxation
contractility
Diastolic failure may be present and it has been there for several
years. But the person involved will not bother to pay attention and
Normal / slightly
most of our patients give reason for a feeling of discomfort or easy Ejection Fraction < 40 %
decreased
fatigability, not knowing that there is already a beginning failure in
the form of diastolic failure.
Symptoms Pulmonary congestion Same
Pathophysiology, systolic is ejection so there is impairment in
pumping ability of left ventricle. Diastole means ventricular filling problem is malfunctioning of the left ventricle of whatever etiology
and for the blood to be fill up, for the left ventricular cavity to be fill or underlying cause is present.
up, it should be able to accommodate to relax / expand. But there is Left ventricle is not functioning normally, what will happen? The
restriction, it is easily killed off and there is impairment of the cardiac output will be reduced. If the cardiac output is reduced,
relaxation capacity of the left ventricle that is failure during there will be decreased renal perfusion. Whatever amount of blood
diastole. is ejected by the left ventricle that is the amount blood goes to the
Ejection fraction is the estimate of the amount of the cardiac output kidney. If we have diminished renal blood flow, there will be
that is being released and thrown out into a periphery. activation of the neurohormonal mechanism, there will be increase
Looking at the ejection fraction, it is less than 40%. By the way the in renin, increase in angiotensin which later on the aldosterone
NORMAL ejection fraction is around 56% to 77%. The higher the secretion will be there released by the adrenals, myocardial tissue
better. In diastolic failure, it is still normal, or maybe slightly and vascular system.
decreased. Increase in aldosterone will promote decreased potassium,
Symptoms that is pulmonary congestion on systolic failure, but in decreased magnesium and other extrarenal effect.
diastolic failure, there may not be any pulmonary congestion. Increase in aldosterone will promote sodium retention. If sodium is
In diastolic failure, you can say that they are still asymptomatic retained, potassium is secreted and you will have EDEMA and there
probably because there is impairment of relaxation, it can affect the will be excessive blood volume because of the sodium retention.
cardiac output, only thing expect to happen in patients with When there is left ventricular dysfunction, the various defense
diastolic failure is a symptom of easy fatigability. They easily got mechanisms is to compensate for the problem and one of the
tired especially if the heart rate is very fast. compensatory mechanism would be to dilate the chamber. (FRANK
To be able to differentiate, we have echocardiography. STARLINGS MECHANISM) of the heart
The Frank Starlings Law if there is reduction in the cardiac
output, there would be stretching of the myocardial fiber. In order
to increase the volume, in accordance to increase the pressure, so
Et factum estutamicistranscribit 2014 -2015
Dra.Deduyo Page 3 of 10
durumsimul in unum! medicine vade MARIE
CONGESTIVE HEART FAILURE CARDIOLOGY
that this ventricle will contract and a greater cardiac output will be The progressions from hypertension to heart failure are aggravated
release. by common comorbid risk factors like a person with left ventricular
And this mechanism will go on, dilate ng dilate ng dilate until it is hypertrophy.
overstretch. Para lang siyang tirador, hinatak mo ng hinatak, there Do you still remember when I lectured about hypertension, when
would come a time it can no longer being stretch. So, if it is the there is LVH, as a consequence of a chronic uncontrolled
purpose of trying to throw a stone far away. It does goes down. hypertension that will be reason also why this patient can go into
Cardiac output becomes reduced. complications as coronary artery diseases and heart failure
Because of neurohormonal activation, hindi lang aldosterone ang aggravated also by diabetes mellitus, aggravated by dyslipidemia,
nasesecrete, sympathetic nervous system is also activated. Ano ang renal dysfunction, obesity, and cigarette consumption.
purpose ng sympathetic nervous system? To increase the heart
rate. Ano ang purpose ng increasing the heart rate? To increase
cardiac output because the cardiac output is determined by the
heart rate and stroke volume.
Heart rate sympathetic
Yung stroke volume, increased volume because of sodium retention
compensatory mechanism
But in dealing the compensatory mechanism, pag sinabi mong to
compensate is to adapt to the situation is the very reason why the
patient becomes symptomatic. Symptomatic and with
manifestations of edema, manifestations of pulmonary congestion,
because you increase the venous return into the right side of the
heart, you also throw more blood into the pulmonary, tumataas
naman ang pressure dito sa left side, bumabalik sa pulmonary,
kawawang baga :( nagcocongest.
The pathophysiology of hypertension.
Note that blood pressure is determined by cardiac output and
peripheral resistance. So in any event that there will be increased
cardiac outpiut or increased peripheral resistance, the blood
pressure would be elevated.
If there is excess sodium intake from the diet or there is genetic
predisposition, this could itself increase sodium retention by the
kidney.
Sodium retention by the kidney would increase the fluid volume,
increase the preload. The main reason why there is increase in the
preload is because there will be increase in the output but the
outcome is hypertension. Diuretics is part of medical treatment for
patients with hypertension if there is that particular problem
Increased sympathetic nervous system activity which we have
identified could be due to the renin angiotensin aldosterone system
activity and why this is stimulated? Because there is a decrease in
the cardiac output among our patients with heart failure.
Cardiovascular continuum, concentrating on hypertension,
So whenever this is increase, sympathetic nervous system is
diabetes, coronary artery disease and this end stage of heart
increase, there will be increased contractility, increased heart rate,
failure. There are primary heart diseases that can lead also to end
increased cardiac output, vasoconstriction, on account of the
stage of heart diseases in the form of congestive heart failure.
angiotensin aldosterone contributing to the increase in fluid volume
therefore there will be increase in peripheral resistance and there
Progression of Hypertension to HF
would be hypertension.
Common Comorbid Risk Factors Beta blockers that can block the sympathetic nervous system
LVH ACE or ARB can block the RAA system and the diuretic seems to be
DM the main line for managing patients with hypertension.
Insulin resistance
Hyperlipidemia
Renal dysfunction
Obesity
Cigarette consumption
Et factum estutamicistranscribit 2014 -2015
Dra.Deduyo Page 4 of 10
durumsimul in unum! medicine vade MARIE
CONGESTIVE HEART FAILURE CARDIOLOGY
touch, also need for hospitalization in order to be able to feel
comfortable.
The worst thing that may happen is our patient may die.
And if there is hypertension, there is endothelial injury. If there is
endothelial injury, there is a change in gene expression, cytokines,
growth factors and adhesion molecules. There will be change in a The main compensatory mechanism is activated by the hormonal
lipid metabolism, and a change in redox status with the increase in system. The adrenergic system, renin angiotensin system, yun ang
free radicals that causes oxidation and further endothelial injury. maactivate and the purpose is to increase the cardiac output
What is the end result of this endothelial injury? Atherosclerosis. because the hemodynamic problem is the output is already LOW.
What is atherosclerosis? Basic lesion among patients with coronary The reason why our patient is symptomatic.
artery diseases. However, sympathetic nervous system activity seems to be more
In patients with hypertension, we expect our patients could have cardiotoxic. What if there is CAD, the more it injures the damaged
coronary artery diseases. heart and therefore more myocyte will be damage and decreased
There is increased vessel wall thickness, our heart would increase in myocardial contractility.
ventricular relative wall thickness of the heart also increases. As a Purpose of adrenergic system is to increase the heart rate, to
part of LVH, as a consequence of hypertension. improve the cardiac output, did not capilliarize kasi lalo na bumaba
nag contractility, lalo na bumaba ang cardiac output.
When there is increased heart rate, then contractility will need
more oxygen, the myocardium is in need of more oxygen once if
there is a problem in coronary, hindi naman niya maprovide yung
oxygen na yan. More damage to the myocytes.
Some patients did not have the luxury for the chest discomfort,
hindi bumigat yan. Ang unang una sintomas ng CAD ay HEART
FAILURE. More dyspneic than with chest discomfort.
With RAAS, there is vasoconstriction because of angiotensin,
volume overload because of aldosterone and increase in the wall
stress. Naiistress yung wall ng myocardium, and it will require more
oxygen that it could not be provided.
Increased wall stress could mean more hypertrophy and when a
ventricle is hypertrophied, the more it needs oxygen that cannot be
provided by a damaged coronary artery so there will be more
myocytes that will be dead, decreased myocardial contractility.
Compensatory means to adapt, the reason why our patient is we
Hypertension leads to coronary artery disease and when there is found symptomatic.
CAD, either you have unstable angina, non STEMI, ST elevation
myocardial infarction.
With the presence of hypertrophy (LVH), or any form of CAD, there
will be ventricular remodelling.
What is ventricular remodelling? There is no dilatation of the left
ventricle.
The more remodel it is, it leads to systolic failure, with each
dilatation the remodelling there is more damage, there is dilatation,
with hypetrophy, this what we expect.
Diastolic failure with both dilatation and LV damage is aggravated
by CAD, there is systolic heart failure.
Typical symptoms of a patient with a heart failure, there will
decreased tissue perfusion, the reason why patient feels cold to
Et factum estutamicistranscribit 2014 -2015
Dra.Deduyo Page 5 of 10
durumsimul in unum! medicine vade MARIE
CONGESTIVE HEART FAILURE CARDIOLOGY
If you try to look harder for the effect of adrenergic system Ano ba yung hormones that are activated with sympathetic nervous
activation, what will happen? Adrenergic system, the sympathetic system activity and RAAS activity? Renin angiotensin II,
nervous system when the heart rate is very fast affects the sympathetic norepinephrine; they have a common effect:
vasculature, the arterial blood vessel, it affects the heart. On the produce hypertrophy, apoptosis, ischemia, arrhythmia they call it
blood vessels, it has an adverse metabolic effect, and worsen the the late end fibrosis
risk (?) profile and worsens the heart failure.
Adrenergic system, sympathetic nervous system will promote more COMMON ETIOLOGIES OF HF
vasoconstriction that will further increase the afterload and CAD
Poorly controlled hypertension
therefore diminished further the cardiac output.
Complications of MI
Vasoconstriction will lead to decreased renal blood flow that would Sustained cardiac arrhythmia
promote RAA system activation and there would be fluid retention. Valvular lesions
The tachycardia, the ventricular remodelling would increase Dilated cardiomyopathy
myocardial oxygen consumnption, the remodelling would cause Myocarditis
more apoptosis or more myocyte death and it causes heart failure.
CAD and HYPERTENSION: most common
Heart failure is indeed a very fatal disease. It is the end stage of
ANY heart disease.
Never ever give a diagnosis of a heart failure alone! You have to
identify and answer the question Why the heart did goes into
failure? We said that this patient indeed is in heart failure basing
in the Framingham Criteria, you presented almost 6 major criteria
to determine to say the heart is in failure. Hindi tayo mage end dun
sa definitive, sasagutin natin yung why? Secondary to: is it CAD?
Poorly controlled hypertension?
This is what we confirmed, triple drug, poorly controlled ang
hypertension. CAD hindi pa natin nacoconfirm.
Bakit siya nagfailure? Isa lang yung alam natin, meron siyang
hypertension, hindi controlled. Is it a complication of MI? Wala
naman siya history na nagkaroon ng acute coronary syndrome. Out
yun! Sustained cardiac arrhythmia? Di ba sabi natin regular in
rhythm, so wala siyang arrhythmia. Is the patient having a valvular
heart disease? Meron siyang apical systolic murmur. Meron siyang
murmur kaya meron valvular dysfunction, meron siyang mitral
If we compare it to the most common cancers (breast CA, colon CA, regurgitation. Could it be the cause? Or a consequence of presence
prostate CA) and heart failure, in one year breast cancer is still alive of hypertension, diabetes or age of the patient? Mukha lang
(88%), prostate (75%), colon (56%) and heart failure is 67%. consequences pero hindi siya primary.
High mortality in colon CA than heart failure A 42 years old, having a history rheumatic fever and confirmed to
We follow up these people after 2 years, breast cancer survival have a rheumatic heart disease presenting this, all of them na un
because of chemotherapy (80% pa ang buhay), prostate cancer kasi may rheumatic heart disease siya, may valvular heart disease
(64%), colon cancer one half na ang namatay. Heart failure (41%). siya.
After 3 years, the breast cancer survival is still good, lalo na kung Dilated cardiomyopathy, hindi madidiagnosed at the bedside saka
ang nirerevert nila kung dilated cardiomyopathy yan, apical beat is very much
(chemotherapy) because there is specific for breast CA. Prostate displaced even to the side and down and you cannot almost feel the
cancer (55%), Colon CA (42%). Heart failure less than 1/4, so bad apical beat and the heart sound is distant. Kasi dilated siya.
All of these will need adrenergic blockade. Is there myocarditis? Paano natin malalaman na may myocarditis
yan? What is the most common? Viral etiology. Meron ba siyang
history ng flu like illness? Wala naman siyang history na ganun.
Et factum estutamicistranscribit 2014 -2015
Dra.Deduyo Page 6 of 10
durumsimul in unum! medicine vade MARIE
CONGESTIVE HEART FAILURE CARDIOLOGY
Where patients having a flu like symptoms 3 weeks prior to Which is the following not routinely ordered in the evaluation of patients with
admission or consultation and was bothered by increasing difficulty HF
of breathing, non hypertensive, non diabetic. Ang history na
natatandaan ay nagkaroon ng influenza. 1. Chest Xray
Symptoms nila difficulty of breathing 2. ECG
A 52 years old, an overseas contract worker of a rich banker in 3. Serum electrolytes and albumin
Macau, came home because I really dont feel well. Ang history lang 4. Complete Blood Count
niya ay viral infection, viral myocarditis. Do not just reject kung may 5. Urinalysis
trangkaso ka baka you may be one of it. 6. NTproBNP
CAD and hypertension seems to be the most common. Yan ung 7. Echocardiography
secondary to. 8. Coronary Angiography
Other etiologies of HF What are we going to request?
Acute pulmonary embolism Nahihirapan huminga chest xray
Pericardial diseases effusion/tamponade, constrictive pericarditis Are we going to do ECG? yes kasi hypertension and diabetic
Infiltrative disease Serum electrolytes and albumin yes because the pt. is chronically
Hyperkinetic state anemia and thyrotoxicosis taking the diuretic; we must know if nag hhypoikalemia or
hyponatremia
Acute pulmonary embolism we usually see these people who are CBC yes
bedridden, deep vein thrombosis, those having pericardial diseases, Sputum production
pericardial effusion, tamponade, constrictive pericarditis, Urinalysis yes kasi diabetic siya; prone to UTI
infiltrating diseases, hyperkinetic stages of anemia and NTpro BNP - it is a natriuretic peptide
thyrotoxicosis. Echocardiography can be distinguish a systolic or diastolic failure
or a combination thereof.
HF Differential Diagnosis Coronary angiography depends upon the ECG, baka ang etiology
niya is acute coronary disease on top of the hypertension.
Dyspneic state
COPD/asthma exacerbation Laboratory evaluation
Pulmonary embolism
Pneumonia/pulmonary infection The evaluation of laboratory is to diagnose potentially reversible
Pneumothorax causes and correctable problem
Pleural effusion To identify comorbidities
Obesity To correct abnormalities before and during the treatment and
Physical deconditioning assess the severity to be able to predict the prognosis and this is the
value of NTproBNP
Low cardiac output state
Acute myocardial infarction
Pericardial tamponade
Fluid retention state
Renal failure
Nephrotic syndrome
Liver Cirrhosis / failure
Hypoproteinemia
Deep venous thrombosis
Differential diagnosis of patients who are in heart failure because
they are dyspneic. Remember the very first case, 72 years old with
history of smoking, inuubo siya, nahihirapan siyang huminga. Baka
siya COPD di ba? Or exacerbation of asthma? Is it a pulmonary
embolism? Is there a pneumonia or pulmonary infection? Which is
present to a patient with complaint of cough productive with
yellowish greenish sputum?
Is it a pneumothorax? A pleural effusion? Physical deconditioning?
Obesity?
Low cardiac output state: myocardial infarction, pericardial
tamponade
Fluid retention state: very common is renal patients, renal failure,
nephritic syndrome, mga dinidialysis kasi nakikita natin mga uremic
(uremic effusion, uremic cardiomyopathy), liver failure,
hyperproteinemia, deep venous thrombosis
Et factum estutamicistranscribit 2014 -2015
Dra.Deduyo Page 7 of 10
durumsimul in unum! medicine vade MARIE
CONGESTIVE HEART FAILURE CARDIOLOGY
Natriuretic peptides
There are 2:
NTproBNP
BNP
Correlates well to the cardiac function and clinical presentation and
most useful in symptomatic patients
Present a diagnostic challenge
If the result is less than 100 pg/ml for BNP and less than 400 pg/ml
Chest radiograph for NTproBNP, walang heart failure
If the BNP is 100- 400 pg/ml and NTproBNP 400-2000 pg/ml ,
Chest Xray PA and Lateral should be request for patient suspected uncertain diagnosis
with heart failure and in acute dyspneic patient, may exclude other If more than 400 and more than 2000, chronic heart failure is
significant compounding diagnosis indeed present.
Remember that the Xray may lag its clinical findings by hours
May crackles ka na. Hindi pa nakita ang pneumonia, hindi pa nakita International Consensus for Optimal NTproBNP
ang congestion.
Dependent on the age of the patient
In chronic HF, it is limited by unreliable sensitivity and specificity
Ang patient natin ay 73 so 50-7, ang optimal cut off mo is 905
In one particular study, the chest Xray evidence of pulmonary
pg/ml
congestion was 53% in a full blown heart failure patient. With a
mild to moderate pulmonary capillary wedge pressure (PCWP) of Kung mas matass diyan, so we say our patient is indeed in failure.
The older the patient, the higher the cut off.
16-29 mmHg and in 39% of those markedly elevated PCWP of more
than 30 mmHg signifies that there is already pulmonary congestion
NTproBNP Testing for diagnosis or exclusion of Heart Failure
and pulmonary hypertension.
A negative chest X-ray does not exclude the diagnosis of left
ventricular function. Patient with acute dyspnea Hx, PE, CXR, ECG, measure
NTproBNP
NTproBNP less thsn 300 pg/ml, heart failure is unlikely
There are patients in the heart failure, that we say correlate it
clinically and triage different symptoms
NTproBNP is age adjusted positivity
450
750
900
1,800 heart failure is likely
NTproBNP can reach up to 20,000
Habang tumatass, prognosis is worse
Usually, malakas ito. Hindi magawa yung prognosis. Every 8-12 hrs
nirerepeat kasi tinitingnan pa yung pagbabago.
If NTproBNP level decreases, the outcome is good.
NTproBNP uses also as basis in order to admit the patient or not
Kung mababa hindi iaadmit, kung matass iaadmit.
Hindi man heart failure, pwedeng tumaas ang NTproBNP
Et factum estutamicistranscribit 2014 -2015
Dra.Deduyo Page 8 of 10
durumsimul in unum! medicine vade MARIE
CONGESTIVE HEART FAILURE CARDIOLOGY
International Consensus Statement. AJC 2008 Hypertension is another added problem arise above 90% pf the
NTproBNP / BNP levels without Acute Decompensated HF patients, so effective contol of BP needs more than 1
Acute coronary syndrome patients will have an increased value antihypertensive drug
lalo na NTproBNP signifies injury to the myocardium. Para siyang Hypercholesterolemia is also a problem, and the use of statins
troponin, which is a marker of injury in the myocardium. showed reduction in the development of atherosclerosis in the
Pulmonary embolism it is also elevated allograft heart. Saan ba kumukuha ng puso? Sa recently na
Right ventricular overload (elevated) namatay.
Obesity - decreased
Renal failure - increased Mechanical and Ventricular Assist and Replacement Device
Critical illness - increased
Chronic heart failure may be high or low is a prelude to cardiac transplant
For severe heart failure
Treatment: Purpose: place in the heart to pump but it cannot last longer ,
should be the heart should be replace
Experimental data, noong araw, beta blockers is a NO NO, but
now because of increase sympathetic nervous system activity, Ventricular Assist enable to maintain an excellent perfusion
important parcel in the treatments of patients with heart failure
besides digitalis Waiting point, holding area
But the beta blockers here are off load dose, for example, Transplant devices may be eventually use as a permanent implant
Metoprolol which we use 15 mg for hypertension, mababang Associated with increased incidence of emboli and infection
mababa lang ang dose.
Carvedilol and Bisoprolol mababang mababa lang din ang dose Cardiac myoplasty skeletal muscle assist procedure; cut latissimus dorsi
1,094 patients whose classification of heart failure, randomized the muscle, skeletal muscle and they wrap it around the heart so that skeletal
placebo of Carvedilol for 15 months, 65% showed a reduction in muscle is the one to contract
mortality so they start by monitoring
Using Bisoprolol, whose patients are more symptomatic of 3-4 ACE Inhibitor studies have shown ... activated in patients with systolic
randomized the placebo of Bisoprolol, showed 34% reduction in dysfunction without overt heart failure.
mortality
Side effects of ACE inhibitor: Cough, hyperkalemia, angioedema,
In Metoprolol using the same group of patients of 2-4 randomized
the placebo of Metoprolol activity cause less than 34%
ARB anatagonist of RAAS that can cause potentiation of bradykinin. Without
Because of this study, nawala na ang Metoprolol and Bisoprolol,
cough
Carvedilol na lang ang ginagamit.
Carvedilol, is the newer generation combination of the alpha and Lower incidence of renal insufficiency
beta blocker approved it in 1997 and it is really indicated for mild to Hyperkalemia
moderate heart failure. The rationale is because the SNS being Drug alternative to ACE due to its renal effect
activated in a symptomatic left ventricular dysfunction and its
activation increase in relation to the severity of the heart failure. Hydralazine and Isosorbide dinitrate (ISDN)
Besides Metoprolol, Diuretics, our pateient will be needing diuretics
because there is pulmonary congestion Hydralazine when you go to OB, for pregnancy induced
hypertension
ACE or ARB The use of combination of hydralazine and ISDN will reduce the
mortality and improve the symptoms of heart failure
The popularity of ACE ay medyo nag wane because of the side
In this trial, failure ang hydralazine and ISDN when it was
effect of cough, lalo na yung patient natin inuubo na siya, hindi na
compared to ACE. ACE was the on e reduce the mortality
siya pwede bigyan ng ACE.
These drugs are said recommended for patients intolerant to ACE
ARB could be a better alternative
because ARB is not available especially those who developed renal
Because the ECG of this patient showed ischemic changes, patient is insufficiency
subjected to coronary angiography. True enough, our patient has 4
Hydralazine 75-100 mg 3x a day; ISDN 30-40 mg
vessel diseases so the recommendation was a bypass.
This patient will benefit very well for the bypass because there will Calcium channel Blocker
be revascularization of the other parts of the myocardium, hindi
yung nag myocyte death na, wala tayong magagawa. First generation CCB Verapamil, Diltiazem, Nifedipine
Contraindicated in the presence of heart failure because they did
Cardiac transplantation will be the last result, increased markedly not showed improved survival and can even exacerbate the
in the 1980s due to immunosuppression. The 1 year survival is 85% symptoms of heart failure because CCB can provoke edema
and the 5 years survival is 70-75%.
First cardiac transplant Dr. Christian Baarnard Digitalis (Digoxin)
During the period of increased immunosuppression acute
rejection patients especially have heightened risk of infection Subsequent studies in well characterized cardiac dilatation have
from the cytomegalovirus systolic dysfunction have shown that digitalis compared to placebo
decreases the PCWP, increases the cardiac index, improve the
symptoms and exercise tolerance.
Et factum estutamicistranscribit 2014 -2015
Dra.Deduyo Page 9 of 10
durumsimul in unum! medicine vade MARIE
CONGESTIVE HEART FAILURE CARDIOLOGY
Able to reduce the heart rate.
The lower the heart rate, the more the patient can do some activity
Notice that if you exercise and the baseline heart rate is 100
already, do you think you can exercise longer? Of course not.
All the outlets baseline heart rate of over 50 per minute
Radiance Trial
Dati, pag nagdigitalis ka kailangan atrial fibrillation. Sinus
tachycardia, pwede ba magdigitalis? In order to reduce the heart
rate
Patients receiving digoxin who were in sinus rhythm and had an
ejection fraction of 35%
All patients continue to take ACE and diuretics
Those in digoxin treatment discontinue as 25% of ability in clinical
deterioration in comparison to those 5% of those who continue
receiving digoxin
We can use digitalis for reduction of the heart rate, not as a
treatment of cardiac arrhythmia
This trial demonstrated in the benefit of digoxin
Evolving Concept of Heart Failure Treatment to correct the myocardial
abnormality
Assist / bridge device (VAD)
Transplantation
Modify synthesis of abnormal gene products (stem cell}
Et factum estutamicistranscribit 2014 -2015
Dra.Deduyo Page 10 of 10
durumsimul in unum! medicine vade MARIE
You might also like
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeFrom EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeRating: 4 out of 5 stars4/5 (5794)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreFrom EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreRating: 4 out of 5 stars4/5 (1090)
- Never Split the Difference: Negotiating As If Your Life Depended On ItFrom EverandNever Split the Difference: Negotiating As If Your Life Depended On ItRating: 4.5 out of 5 stars4.5/5 (838)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceFrom EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceRating: 4 out of 5 stars4/5 (895)
- Grit: The Power of Passion and PerseveranceFrom EverandGrit: The Power of Passion and PerseveranceRating: 4 out of 5 stars4/5 (588)
- Shoe Dog: A Memoir by the Creator of NikeFrom EverandShoe Dog: A Memoir by the Creator of NikeRating: 4.5 out of 5 stars4.5/5 (537)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersFrom EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersRating: 4.5 out of 5 stars4.5/5 (344)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureFrom EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureRating: 4.5 out of 5 stars4.5/5 (474)
- Her Body and Other Parties: StoriesFrom EverandHer Body and Other Parties: StoriesRating: 4 out of 5 stars4/5 (821)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)From EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Rating: 4.5 out of 5 stars4.5/5 (121)
- The Emperor of All Maladies: A Biography of CancerFrom EverandThe Emperor of All Maladies: A Biography of CancerRating: 4.5 out of 5 stars4.5/5 (271)
- The Little Book of Hygge: Danish Secrets to Happy LivingFrom EverandThe Little Book of Hygge: Danish Secrets to Happy LivingRating: 3.5 out of 5 stars3.5/5 (399)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyFrom EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyRating: 3.5 out of 5 stars3.5/5 (2259)
- The Yellow House: A Memoir (2019 National Book Award Winner)From EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Rating: 4 out of 5 stars4/5 (98)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaFrom EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaRating: 4.5 out of 5 stars4.5/5 (266)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryFrom EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryRating: 3.5 out of 5 stars3.5/5 (231)
- Team of Rivals: The Political Genius of Abraham LincolnFrom EverandTeam of Rivals: The Political Genius of Abraham LincolnRating: 4.5 out of 5 stars4.5/5 (234)
- On Fire: The (Burning) Case for a Green New DealFrom EverandOn Fire: The (Burning) Case for a Green New DealRating: 4 out of 5 stars4/5 (73)
- The Unwinding: An Inner History of the New AmericaFrom EverandThe Unwinding: An Inner History of the New AmericaRating: 4 out of 5 stars4/5 (45)
- Pedia Cardiology 2Document5 pagesPedia Cardiology 2Medisina101No ratings yet
- Fire Alarm SymbolsDocument6 pagesFire Alarm Symbolscarlos vasquezNo ratings yet
- Infective Endocarditis - Dr. Payawal PDFDocument6 pagesInfective Endocarditis - Dr. Payawal PDFMedisina101No ratings yet
- Arrythmia Part 1 - Dr. Payawal PDFDocument10 pagesArrythmia Part 1 - Dr. Payawal PDFMedisina101100% (1)
- Arrythmia Part 2 - Dr. Payawal PDFDocument8 pagesArrythmia Part 2 - Dr. Payawal PDFMedisina101No ratings yet
- ECG Part 1 - Dr. Payawal PDFDocument10 pagesECG Part 1 - Dr. Payawal PDFMedisina101No ratings yet
- Coronary Artery Disease - Dra. Deduyo PDFDocument7 pagesCoronary Artery Disease - Dra. Deduyo PDFMedisina101No ratings yet
- Acute Coronary Syndrome - Dra. Deduyo PDFDocument6 pagesAcute Coronary Syndrome - Dra. Deduyo PDFMedisina101No ratings yet
- ECG Part 2 - Dr. Payawal PDFDocument4 pagesECG Part 2 - Dr. Payawal PDFMedisina101No ratings yet
- Deep Vein Thrombosis - Dr. Deduyo PDFDocument17 pagesDeep Vein Thrombosis - Dr. Deduyo PDFMedisina101No ratings yet
- Valvular Heart Diseases Part 2 - Dr. BartolomeDocument9 pagesValvular Heart Diseases Part 2 - Dr. BartolomeMedisina101No ratings yet
- Congenital Heart Diseases - Dr. BartolomeDocument12 pagesCongenital Heart Diseases - Dr. BartolomeMedisina101No ratings yet
- Diseases of The Aorta - Dr. Deduyo PDFDocument11 pagesDiseases of The Aorta - Dr. Deduyo PDFMedisina101No ratings yet
- Valvular Heart Diseases Part 1 - Dr. BartolomeDocument18 pagesValvular Heart Diseases Part 1 - Dr. BartolomeMedisina101No ratings yet
- Peripheral Vascular Medicine - Dr. Deduyo PDFDocument14 pagesPeripheral Vascular Medicine - Dr. Deduyo PDFMedisina101No ratings yet
- Cardiac Tumors Slides - Dr. BartolomeDocument81 pagesCardiac Tumors Slides - Dr. BartolomeMedisina101No ratings yet
- PEDIA - Cardio (Esguerra) PDFDocument9 pagesPEDIA - Cardio (Esguerra) PDFMedisina101No ratings yet
- Pericardial Diseases - Dr. BartolomeDocument8 pagesPericardial Diseases - Dr. BartolomeMedisina101No ratings yet
- Pedia Pulmo 3 11.03.16Document49 pagesPedia Pulmo 3 11.03.16Medisina101No ratings yet
- Pedia Pulmo I 10.4.16Document129 pagesPedia Pulmo I 10.4.16Medisina101No ratings yet
- SURGERY Lecture 4 - Breast (Dra. Fernandez)Document15 pagesSURGERY Lecture 4 - Breast (Dra. Fernandez)Medisina101100% (1)
- Cardiac Tumors - Dr. BartolomeDocument12 pagesCardiac Tumors - Dr. BartolomeMedisina101No ratings yet
- Acquired Heart DiseaseDocument44 pagesAcquired Heart DiseaseMedisina101No ratings yet
- Pedia Pulmo 2 10.18.16Document73 pagesPedia Pulmo 2 10.18.16Medisina101No ratings yet
- SURGERY Lecture 5 - Abdominal Wall, Omentum, Mesentery, Retroperitoneum (Dr. Wenceslao)Document13 pagesSURGERY Lecture 5 - Abdominal Wall, Omentum, Mesentery, Retroperitoneum (Dr. Wenceslao)Medisina101No ratings yet
- SURGERY Lecture 1 - Small Intestine (Dr. Mendoza)Document16 pagesSURGERY Lecture 1 - Small Intestine (Dr. Mendoza)Medisina101100% (1)
- Surgery II - Pancreas 2014Document20 pagesSurgery II - Pancreas 2014Medisina101No ratings yet
- SURGERY Lecture 2 - Liver & Gallbladder (Dr. Wenceslao)Document19 pagesSURGERY Lecture 2 - Liver & Gallbladder (Dr. Wenceslao)Medisina101100% (1)
- SURGERY Lecture 3 - Abdominal Hernia (Dr. Mendoza)Document12 pagesSURGERY Lecture 3 - Abdominal Hernia (Dr. Mendoza)Medisina101100% (1)
- Head and Neck SurgeryDocument15 pagesHead and Neck SurgeryMedisina101100% (1)
- SM Electrical Guidelines: General Notes:: Site HereDocument1 pageSM Electrical Guidelines: General Notes:: Site HereNathaniel DreuNo ratings yet
- Worksheet - Government Microeconomic IntervenDocument20 pagesWorksheet - Government Microeconomic IntervenNguyễn AnnaNo ratings yet
- P3 Chapter 2 End-Of-Chapter (Higher) Mark SchemeDocument3 pagesP3 Chapter 2 End-Of-Chapter (Higher) Mark SchemePaul LloydNo ratings yet
- Cwts ThesisDocument7 pagesCwts Thesisbufukegojaf2100% (2)
- Corp Given To HemaDocument132 pagesCorp Given To HemaPaceNo ratings yet
- CRISIL Mutual Fund Ranking: For The Quarter Ended September 30, 2020Document48 pagesCRISIL Mutual Fund Ranking: For The Quarter Ended September 30, 2020MohitNo ratings yet
- Components of A Rainwater Harvesting SystemDocument38 pagesComponents of A Rainwater Harvesting SystembudiperNo ratings yet
- People v. Jerry BugnaDocument1 pagePeople v. Jerry BugnaRey Malvin SG PallominaNo ratings yet
- 5754 Almg3 5754 Almg3 Almg3 Almg3 5754 Almg3 Almg3 Almg3 Almg3Document3 pages5754 Almg3 5754 Almg3 Almg3 Almg3 5754 Almg3 Almg3 Almg3 Almg3InfoNo ratings yet
- Location: Map of Naga CityDocument2 pagesLocation: Map of Naga Citycatherine boragayNo ratings yet
- Charla Krupp - How To Never Look Fat Again - Over 1,000 Ways To Dress Thinner - Without Dieting!-Grand Central Publishing (2010) PDFDocument316 pagesCharla Krupp - How To Never Look Fat Again - Over 1,000 Ways To Dress Thinner - Without Dieting!-Grand Central Publishing (2010) PDFben0% (1)
- Streptococcus Pneumoniae Staphylococci Faculty: Dr. Alvin FoxDocument32 pagesStreptococcus Pneumoniae Staphylococci Faculty: Dr. Alvin Foxdanish sultan100% (1)
- 1stweek Intro Quanti Vs QualiDocument18 pages1stweek Intro Quanti Vs QualiHael LeighNo ratings yet
- Banco de Oro (Bdo) : Corporate ProfileDocument1 pageBanco de Oro (Bdo) : Corporate ProfileGwen CaldonaNo ratings yet
- Knopp2017 Article OnceACheaterAlwaysACheaterSeriDocument11 pagesKnopp2017 Article OnceACheaterAlwaysACheaterSeriAnda F. CotoarăNo ratings yet
- Absenteeism in Public Sector: Presented byDocument25 pagesAbsenteeism in Public Sector: Presented byPravin Rathod50% (2)
- Lord You Know All Things, You Can Do All Things and You Love Me Very MuchDocument4 pagesLord You Know All Things, You Can Do All Things and You Love Me Very Muchal bentulanNo ratings yet
- Elasticity, Plasticity Structure of Matter: by DR R. HouwinkDocument9 pagesElasticity, Plasticity Structure of Matter: by DR R. HouwinkKhlibsuwan RNo ratings yet
- Polymer LedDocument14 pagesPolymer LedNaveenNo ratings yet
- Eaton BECOPAD P Range TechnicalDataSheet enDocument4 pagesEaton BECOPAD P Range TechnicalDataSheet enEsteban Fernando Meza IbacetaNo ratings yet
- Comparative Study of Financial Statements of Company, Oil and Gas.Document105 pagesComparative Study of Financial Statements of Company, Oil and Gas.Ray Brijesh AjayNo ratings yet
- QM SyllabusDocument2 pagesQM SyllabusSanthosh Chandran RNo ratings yet
- OSCE Pediatric Dentistry Lecture-AnswersDocument40 pagesOSCE Pediatric Dentistry Lecture-AnswersR MNo ratings yet
- TQM Assignment 3Document8 pagesTQM Assignment 3ehte19797177No ratings yet
- (VOLKSWAGEN) Manual de Taller Volkswagen Jetta 1999 2006Document4 pages(VOLKSWAGEN) Manual de Taller Volkswagen Jetta 1999 2006Carlos AntonioNo ratings yet
- Pre-Feasibility Report: at Plot No. 15/B-3, Jigani Industrial Area Anekal Taluk, Bangalore South District Karnataka byDocument41 pagesPre-Feasibility Report: at Plot No. 15/B-3, Jigani Industrial Area Anekal Taluk, Bangalore South District Karnataka by12mchc07No ratings yet
- AdEasy Adenoviral Vector SystemDocument43 pagesAdEasy Adenoviral Vector SystemDaniel PintoNo ratings yet
- ASNT QuestionsDocument3 pagesASNT Questionsshabbir626100% (1)