Professional Documents
Culture Documents
Chapter 210: Cardiovascular Laboratory Service
Uploaded by
ABDULWAHAB ABDULWAHABOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Chapter 210: Cardiovascular Laboratory Service
Uploaded by
ABDULWAHAB ABDULWAHABCopyright:
Available Formats
Department of Veterans Affairs PG-18-9: Space Planning Criteria
Veterans Health Administration November 29, 2011
Washington, DC 20420 Revised: October 03, 2016
CHAPTER 210: CARDIOVASCULAR LABORATORY SERVICE
1 PURPOSE AND SCOPE .............................................................................................210-2
2 DEFINITIONS ..............................................................................................................210-2
3 OPERATING RATIONALE AND BASIS OF CRITERIA ..............................................210-4
4 INPUT DATA STATEMENTS ......................................................................................210-5
5 SPACE CRITERIA ......................................................................................................210-6
6 PLANNING AND DESIGN CONSIDERATIONS .......................................................210-13
7 FUNCTIONAL RELATIONSHIPS ..............................................................................210-15
8 FUNCTIONAL DIAGRAM ..........................................................................................210-16
Chapter 210: Cardiovascular Laboratory Service - Page 1 of 16
Department of Veterans Affairs PG-18-9: Space Planning Criteria
Veterans Health Administration November 29, 2011
Washington, DC 20420 Revised: October 03, 2016
1 PURPOSE AND SCOPE
This document outlines Space Planning Criteria for Chapter 210: Cardiovascular
Laboratory Service. It applies to all medical facilities in Department of Veterans Affairs
(VA).
2 DEFINITIONS
Accessible: A site, building, facility, or portion thereof that complies with provisions
outlined in the Architectural Barriers Act of 1968 (ABA).
Architectural Barriers Act (ABA): A set of standards developed to insure that all buildings
financed with federal funds are designed and constructed to be fully accessible to
everyone. This law requires all construction, renovation, or leasing of sites, facilities,
buildings, and other elements, financed with federal funds, to comply with the
Architectural Barriers Act Accessibility Standards (ABAAS). The ABAAS replaces the
Uniform Federal Accessibility Standards (UFAS).
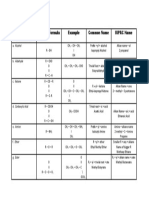
Blood Gas Analysis: A test which analyzes arterial blood for oxygen, carbon dioxide, and
bicarbonate content in addition to blood pH. It is used to test the effectiveness of
respiration.
Cardiac Catheterization (Cardiac Cath): A cardiac procedure where a thin plastic tube
(catheter) is inserted into an artery or vein in the arm or leg. The catheter is then
advanced into the chambers of the heart, or into the coronary arteries. This procedure is
performed to obtain diagnostic information about the patient’s heart and blood vessels. It
may also be used to provide therapeutic interventions in certain types of heart conditions.
Cardiac Stress Test: A cardiac stress test is a medical test performed to evaluate the
ability for arterial blood flow to the myocardium (heart muscle) to increase during the
stress of physical exercise, compared to blood flow while at rest. As an exercise test,
results also reflect overall physical fitness. This test is ordered as a screening procedure
for heart disease. It takes approximately 30 minutes, usually including 6-9 minutes of
treadmill walking. Electrodes are placed on the chest so that the EKG is monitored during
the entire exam, while the physician monitors the patient’s blood pressure.
Cardiac Stress Test – Nuclear: This test follows the same procedure as the Cardiac
Stress Test, with the addition of a nuclear scan. To scan the heart with a nuclear camera,
a small amount of nuclear substance is injected into the patient, which acts as a tracer.
This allows the tracking of blood cells as they circulate from the arteries to the heart
muscle. Nuclear images are taken with a nuclear medicine camera after the exercise
phase as well as at rest for comparison.
Cardiology: The study of the heart and its functions.
Clinic Stop: A clinic stop is one encounter of a patient with a healthcare provider. Per
these criteria, the clinic stop is the workload unit of measure for space planning. One
individual patient can have multiple Clinic Stops in a single visit or in one day.
Echocardiogram (ECHO): A diagnostic test which uses ultrasound waves to make
images of the heart chambers, valves, and surrounding structures. It can measure
cardiac output and is a sensitive test for pericarditis and inflammation around the heart.
Electrocardiogram (EKG): A test that records the electrical activity of the heart, shows
abnormal rhythms (arrhythmias or dysrhythmias), and detects heart muscle damage.
Full-Time Equivalent (FTE): A staffing parameter equal to the amount of time assigned to
one full time employee. It may be composed of several part-time employees whose total
Chapter 210: Cardiovascular Laboratory Service - Page 2 of 16
Department of Veterans Affairs PG-18-9: Space Planning Criteria
Veterans Health Administration November 29, 2011
Washington, DC 20420 Revised: October 03, 2016
time commitment equals that of a full-time employee. One FTE equals 40 hours per
week.
Functional Area: The grouping of rooms and spaces based on their function within a
clinical service. Typical Functional Areas within VA Space Criteria are: Reception Area,
Patient Area, Support Area, Staff and Administrative Area, and Education Area.
Healthcare Planning Module: Methodology used to create a VISN Strategic Plan which
defines how and where high-cost services should be delivered in each market.
Holter Monitor: A device which measures the heart rhythm during a 24 hour period of
time while the patient records their symptoms and activities in a diary. A small portable
EKG device is worn by the patient. After the test is complete, a correlation is made
between the symptoms (or activities) recorded and the EKG pattern that was obtained
simultaneously.
Input Data Statements: A set of questions designed to elicit information about the
healthcare project in order to create a Program for Design (PFD) based on the criteria
parameters set forth in this document. Input Data Statements could be Mission,
Workload, or Staffing related, based on projections and data provided by the VHA or the
VISN about the estimated model of operation for the facility. This information is
processed through mathematical and logical operations in VA-SEPS.
Invasive Cardiology: Procedures that include all invasive cardiac related services such as
Cardiac Catheterization, Therapeutic Cardiovascular Procedures, Electrophysiology (EP)
and Pacemaker Implantation.
Non-Invasive Cardiology: Procedures that do not penetrate the skin or invade the body,
except for minor needle punctures. Non-Invasive procedures include EKG, Holter
Monitoring, Echocardiography, Vascular Testing, Ultrasound, and Nuclear Cardiography.
Pacemaker Implants: An “artificial pacemaker” is a small, battery-operated device that
helps the heart beat in a regular rhythm. Some devices are permanent (internal) and
some are temporary (external).
Picture Archiving and Communication System (PACS): The digital capture, transfer, and
storage of diagnostic images. A PACS system consists of: workstations for interpretation,
image/data producing modalities, a web server for distribution, printers for file records,
image servers for information transfer and holding, and an archive of off-line information.
A computer network is needed to support digital imaging devices.
Program for Design (PFD): A space program generated either manually or by VA-SEPS
based on criteria set forth in this document and specific information entered about
mission, workload projections, and staffing levels authorized.
Provider: An individual who examines, diagnoses, treats, prescribes medication and
manages the care of patients within his or her scope of practice as established by the
governing body of a healthcare organization.
Room Efficiency Factor: A factor that provides flexibility in the utilization of a room to
account for patient delays, scheduling conflicts, and equipment maintenance. Common
factors are in the 75% to 85% range. A room with 80% room efficiency provides a buffer
to assume that this room would be available 20% of the time beyond the planned
operational practices for this room. This factor may be adjusted based on the actual
and/or anticipated operations and processes of the room/department at any particular
facility.
SEPS (VA-SEPS): Acronym for Space and Equipment Planning System, a digital tool
Chapter 210: Cardiovascular Laboratory Service - Page 3 of 16
Department of Veterans Affairs PG-18-9: Space Planning Criteria
Veterans Health Administration November 29, 2011
Washington, DC 20420 Revised: October 03, 2016
developed by the Department of Defense (DOD) and the Department of Veterans Affairs
to generate a Program For Design (PFD) and an Equipment List for a VA healthcare
project based on specific information entered in response to Input Data Questions. VA-
SEPS incorporates the propositions set forth in all VA space planning criteria chapters.
VA-SEPS has been designed to aid healthcare planners in creating a space plan based
on a standardized set of criteria parameters.
Tilt Table Test: A test which involves placing the patient on a table with a foot-support.
The table is tilted in various directions and the blood pressure and pulse are measured
and symptoms are recorded with the patient in diverse positions.
Ultrasound: High frequency sound waves which are utilized to determine the size and
shape of organs based on the differential rates of reflection. In addition, images can be
observed in real time to reveal motion, and can include coloration of arterial and venous
blood flow.
Workload: Workload is the anticipated number of clinic stops that is processed through a
department/service area. The total workload applied to departmental operational
assumptions will determine overall room requirements by modality.
3 OPERATING RATIONALE AND BASIS OF CRITERIA
A. Workload projections or planned services/modalities for a specific VA project are
provided by the VA Office of Policy and Planning and the VISN Support Services
Center (VSSC). These utilization projections are generated by a methodology based
upon the expected veteran population in the respective market/service area.
Healthcare planners working on VA projects will utilize and apply the workload based
criteria set forth herein for identified services and modalities to determine room
requirements for each facility.
B. Space planning criteria have been developed on the basis of an understanding of the
activities involved in the functional areas of the Cardiovascular Laboratory Service
and its relationship with other services of a medical facility. These criteria are
predicated on established and/or anticipated best practice standards, as adapted, to
provide environments supporting the highest quality health care for veterans.
C. These criteria are subject to modification relative to development in equipment,
medical practice, vendor requirements, and planning and design. The selection of the
size and type of Cardiovascular Laboratory Service equipment is determined by
anticipated medical needs.
D. Room Capacity should be based on:
Formula 1:
Operating days per year X Hours of operation per day = Number of annual
clinic stops
Minutes per clinic stop / 60 minutes
The general planning model for VA facilities assumes 250 Operating Days per Year
and 8 Hours of Operation per Day. Room capacity will fluctuate as operating days per
year and/or hours of operation are modified. For example, additional capacity may be
generated by extending the hours of operation per day within the same physical
setting.
The Room Efficiency Factor applied to Cardiovascular Laboratory Service is 80%.
Example: Annual Clinic Stops for Cardiology (Stop Code 303) based upon an
Chapter 210: Cardiovascular Laboratory Service - Page 4 of 16
Department of Veterans Affairs PG-18-9: Space Planning Criteria
Veterans Health Administration November 29, 2011
Washington, DC 20420 Revised: October 03, 2016
average 45 minutes per clinic stop, including set-up, testing time, and clean-up:
250 operating days per year x 8 hours per day = 2,667 annual clinic
stops
45 minutes per clinic stop / 60 minutes
At 100% utilization, this results in a maximum capacity of 2,667 clinic stops per year.
However, 100% utilization is not realistic to achieve and is not a design standard.
Apply the Room Efficiency Factor:
2,667 x 80% = 2,133 annual clinic stops.
TABLE 1: WORKLOAD PARAMETER CALCULATION
MINIMUM
AVERAGE ANNUAL ANNUAL
LENGTH WORKLOAD WORKLOAD
OF CLINIC ROOM CAPACITY TO
CLINIC STOP STOP EFFICIENCY OF ONE GENERATE
CODE DESIGNATION (minutes) FACTOR ROOM* A ROOM**
Stop Code 107
20 80% 4,800 1,440
EKG
Stop Code 303
45 80% 2,133 640
Cardiology
Stop Code 311
30 80% 3,200 960
Pacemaker
Stop Code 334
75 80% 1,280 384
Cardiac Stress Test
* Based on Operating Criteria assumed in Item D above.
** Minimum annual workload to generate a room is equal to 30% of the annual
workload capacity of one room.
4 INPUT DATA STATEMENTS
A. Mission Input Data Statements
1. Is a Patient Check-In Kiosk authorized? (M)
2. Is a Cardiovascular Laboratory Service Residency Program authorized? (M)
a. How many Intern FTE positions are authorized? (S)
b. How many Resident FTE positions are authorized? (S)
c. How many Fellow FTE positions are authorized? (S)
B. Workload Input Data Statements
1. How many annual EKG clinic stops (Stop Code 107) are projected? (W)
2. How many annual Cardiology clinic stops (Stop Code 303) are projected? (W)
3. How many annual Pacemaker clinic stops (Stop Code 311) are projected? (W)
4. How many annual Cardiac Stress Test clinic stops (Stop Code 334) are
projected? (W)
C. Staffing Input Data Statements
1. How many EKG Technician FTE positions, greater than two, are authorized? (S)
2. How many Nurse FTE positions are authorized? (S)
3. How many Physician FTE positions are authorized? (S)
4. How many Nurse Manager FTE positions are authorized? (S)
5. How many Nurse Practitioner FTE positions are authorized? (S)
Chapter 210: Cardiovascular Laboratory Service - Page 5 of 16
Department of Veterans Affairs PG-18-9: Space Planning Criteria
Veterans Health Administration November 29, 2011
Washington, DC 20420 Revised: October 03, 2016
6. How many Technician FTE positions are authorized? (S)
7. How many Administrative FTE positions are authorized? (S)
D. Miscellaneous Input Data Statements
1. How many Holter Monitor Rooms are authorized? (Misc)
2. How many Echocardiograph Rooms are authorized? (Misc)
3. How many Stress Echocardiograph Rooms are authorized? (Misc)
4. How many Tilt Table Testing Rooms are authorized? (Misc)
5. How many Cardiac CT / MRI Rooms are authorized? (Misc)
5 SPACE CRITERIA
For functional descriptions of key spaces refer to the Design Guide for Cardiovascular
Laboratory Service.
A. FA 1: Reception Area:
1. Waiting (WTG02) ....................................................................... 45 NSF (4.2 NSM)
Provide one if the projected number of Exam / Procedure / Testing Rooms (of all
types) is one; provide WTG04 if the projected number of Exam / Procedure /
Testing Rooms (of all types) is two; provide WTG06 if the projected number of
Exam / Procedure / Testing Rooms (of all types) is three; provide WTG08 if the
projected number of Exam / Procedure / Testing Rooms (of all types) is four;
provide WTG10 if the projected number of Exam / Procedure / Testing Rooms (of
all types) is five; provide WTG12 if the projected number of Exam / Procedure /
Testing Rooms (of all types) is six; provide WTG14 if the projected number of
Exam / Procedure / Testing Rooms (of all types) is seven; provide WTG16 if the
projected number of Exam / Procedure / Testing Rooms (of all types) is eight;
provide WTG18 if the projected number of Exam / Procedure / Testing Rooms (of
all types) is nine; provide WTG20 if the projected number of Exam / Procedure /
Testing Rooms (of all types) is ten; provide WTG22 if the projected number of
Exam / Procedure / Testing Rooms (of all types) is eleven; provide WTG24 if the
projected number of Exam / Procedure / Testing Rooms (of all types) is twelve;
provide WTG26 if the projected number of Exam / Procedure / Testing Rooms (of
all types) is thirteen; provide WTG28 if the projected number of Exam / Procedure
/ Testing Rooms (of all types) is fourteen; provide WTG30 if the projected number
of Exam / Procedure / Testing Rooms (of all types) is fifteen; provide WTG32 if
the projected number of Exam / Procedure / Testing Rooms (of all types) is
sixteen; provide WTG34 if the projected number of Exam / Procedure / Testing
Rooms (of all types) is seventeen; provide WTG36 if the projected number of
Exam / Procedure / Testing Rooms (of all types) is eighteen; provide WTG38 if
the projected number of Exam / Procedure / Testing Rooms (of all types) is
nineteen; provide WTG40 if the projected number of Exam / Procedure / Testing
Rooms (of all types) is twenty.
The Cardiovascular Laboratory Service Exam / Procedure / Testing Rooms are:
a. Pacemaker ICD Interrogation Room,
b. EKG Testing Room,
c. Cardiology Exam Room,
d. Holter Monitor Room,
e. Echocardiograph Room,
f. Stress Echocardiograph Room,
g. Stress Testing Treadmill Room,
h. Tilt Table Testing Room, and
Chapter 210: Cardiovascular Laboratory Service - Page 6 of 16
Department of Veterans Affairs PG-18-9: Space Planning Criteria
Veterans Health Administration November 29, 2011
Washington, DC 20420 Revised: October 03, 2016
i. Cardiac CT / MRI Rooms.
WTG02: Allocated NSF accommodates one bariatric chair @ 14 NSF, one
accessible space @ 10 NSF, and circulation; total two people.
WTG04: Allocated space accommodates two standard chairs @ 9 NSF each, one
bariatric chair @ 14 NSF, one accessible space @ 10 NSF, and circulation; total
four people.
WTG06: Allocated space accommodates four standard chairs @ 9 NSF each, one
bariatric chair @ 14 NSF, one accessible space @ 10 NSF, and circulation; total
six people.
WTG08: Allocated space accommodates six standard chairs @ 9 NSF each, one
bariatric chair @ 14 NSF, one accessible space @ 10 NSF, and circulation; total
eight people.
WTG10: Allocated space accommodates eight standard chairs @ 9 NSF each,
one bariatric chair @ 14 NSF, one accessible space @ 10 NSF, and circulation;
total ten people.
WTG12: Allocated space accommodates ten standard chairs @ 9 NSF each, one
bariatric chair @ 14 NSF, one accessible space @ 10 NSF, and circulation; total
twelve people.
WTG14: Allocated space accommodates twelve standard chairs @ 9 NSF each,
one bariatric chair @ 14 NSF, one accessible space @ 10 NSF, and circulation;
total fourteen people.
WTG16: Allocated space accommodates twelve standard chairs @ 9 NSF each,
two bariatric chairs @ 14 NSF each, two accessible spaces @ 10 NSF each, and
circulation; total sixteen people.
WTG18: Allocated space accommodates fourteen standard chairs @ 9 NSF each,
two bariatric chairs @ 14 NSF each, two accessible spaces @ 10 NSF each, and
circulation; total eighteen people.
WTG20: Allocated space accommodates sixteen standard chairs @ 9 NSF each,
two bariatric chairs @ 14 NSF each, two accessible spaces @ 10 NSF each, and
circulation; total twenty people.
WTG22: Allocated space accommodates eighteen standard chairs @ 9 NSF
each, two bariatric chairs @ 14 NSF each, two accessible spaces @ 10 NSF
each, and circulation; total twenty-two people.
WTG24: Allocated space accommodates twenty standard chairs @ 9 NSF each,
two bariatric chairs @ 14 NSF each, two accessible spaces @ 10 NSF each, and
circulation; total twenty-four people.
WTG26: Allocated space accommodates twenty standard chairs @ 9 NSF each,
three bariatric chairs @ 14 NSF each, three accessible spaces @ 10 NSF each,
and circulation; total twenty-six people.
WTG28: Allocated space accommodates twenty-two standard chairs @ 9 NSF
each, three bariatric chairs @ 14 NSF each, three accessible spaces @ 10 NSF
each, and circulation; total twenty-eight people.
WTG30: Allocated space accommodates twenty-four standard chairs @ 9 NSF
each, three bariatric chairs @ 14 NSF each, three accessible spaces @ 10 NSF
Chapter 210: Cardiovascular Laboratory Service - Page 7 of 16
Department of Veterans Affairs PG-18-9: Space Planning Criteria
Veterans Health Administration November 29, 2011
Washington, DC 20420 Revised: October 03, 2016
each, and circulation; total thirty people.
WTG32: Allocated space accommodates twenty-six standard chairs @ 9 NSF
each, three bariatric chairs @ 14 NSF each, three accessible spaces @ 10 NSF
each, and circulation; total thirty-two people.
WTG34: Allocated space accommodates twenty-eight standard chairs @ 9 NSF
each, three bariatric chairs @ 14 NSF each, three accessible spaces @ 10 NSF
each, and circulation; total thirty-four people.
WTG36: Allocated space accommodates twenty-eight standard chairs @ 9 NSF
each, four bariatric chairs @ 14 NSF each, four accessible spaces @ 10 NSF
each, and circulation; total thirty-six people.
WTG38: Allocated space accommodates thirty standard chairs @ 9 NSF each,
four bariatric chairs @ 14 NSF each, four accessible spaces @ 10 NSF each, and
circulation; total thirty-eight people.
WTG40: Allocated space accommodates thirty-two standard chairs @ 9 NSF
each, four bariatric chairs @ 14 NSF each, four accessible spaces @ 10 NSF
each, and circulation; total forty people.
2. Reception (RCP02) ............................................................... 260 NSF (24.2 NSM)
Provide one for the Cardiovascular Laboratory Service.
Allocated NSF accommodates two Receptionist FTEs, patient privacy area, and
circulation.
3. Kiosk, Patient Check-In (RCHK2) .......................................... 105 NSF (9.8 NSM)
Provide one if a Patient Check-in Kiosk is authorized.
Allocated NSF accommodates two display kiosks, patient privacy area and
circulation.
4. Workstation, Patient Education (CLSC1) ............................... 40 NSF (3.8 NSM)
Provide one for the Cardiovascular Laboratory Service.
This space is intended to be used for medical information resource material for
patients and visitors. Locate accessible to waiting.
5. Toilet, General (TNPG1) ........................................................... 60 NSF (5.6 NSM)
Provide two for the Cardiovascular Laboratory Service.
Allocated NSF accommodates one accessible toilet @ 25 NSF, one wall-hung
lavatory @ 12 NSF, ABA clearances, and circulation. One for male and one for
female.
B. FA 2: Non-Invasive Cardiology Patient Area:
1. EKG Testing Room (OPEC1) ............................................... 150 NSF (14.0 NSM)
Provide one for every increment of 4,800 annual EKG clinic stops (Stop Code
107) projected; minimum annual workload projected to provide a room is 1,440
(see Table 1).
2. Exam Room, Cardiology (EXRC1) ....................................... 120 NSF (11.2 NSM)
Provide one for every increment of 2,133 annual Cardiology clinic stops (Stop
Code 303) projected; minimum annual workload projected to provide a room is
640 (see Table 1).
Chapter 210: Cardiovascular Laboratory Service - Page 8 of 16
Department of Veterans Affairs PG-18-9: Space Planning Criteria
Veterans Health Administration November 29, 2011
Washington, DC 20420 Revised: October 03, 2016
3. Pacemaker ICD Interrogation Room (EXRC2) .................... 120 NSF (11.2 NSM)
Provide one for every increment of 3,200 annual Pacemaker clinic stops (Stop
Code 311) projected; minimum annual workload projected to provide a room is
960 (see Table 1).
4. Holter Monitor Room (OPHM1) ............................................ 150 NSF (14.0 NSM)
Provide one per each Holter Monitor Room authorized.
5. Echocardiograph Room (OPPE1)........................................ 150 NSF (14.0 NSM)
Provide one per each Echocardiograph Room authorized.
6. Stress Echocardiograph Room (OPPE2)............................ 300 NSF (27.9 NSM)
Provide one per each Stress Echocardiograph Room authorized.
7. Stress Testing Treadmill Room (OPTM1) ........................... 300 NSF (27.9 NSM)
Provide one for every increment of 1,280 annual Cardiac Stress Test clinic stops
(Stop Code 334) projected; minimum annual workload projected to provide a
room is 384 (see Table 1).
8. Tilt Table Testing Room (OPTM2) ....................................... 180 NSF (16.8 NSM)
Provide one per each Tilt Table Testing Room authorized.
9. Consult Room (OFDC2) ....................................................... 120 NSF (11.2 NSM)
Provide two for the Cardiovascular Laboratory Service.
10. Reading Room, ECHO (XVC01) ........................................... 160 NSF (14.9 NSM)
Minimum NSF; provide an additional 40 NSF for every increment of four
Echocardiograph and Stress Echocardiograph Rooms greater than four.
11. Reading Station, EKG (XVC01) ............................................ 120 NSF (11.2 NSM)
Provide one if at least one EKG Testing Room is generated.
12. Toilet, Patient (TPG01) ............................................................. 60 NSF (5.6 NSM)
Minimum one for Non-Invasive Cardiology; provide an additional one for every
increment of six Pacemaker ICD Interrogation Rooms, EKG Testing Rooms,
Cardiology Exam Rooms, Holter Monitor Rooms, Echocardiograph Rooms, Stress
Echocardiograph Rooms, Stress Testing Treadmill Rooms, Tilt Table Testing and
Consult Rooms greater than six.
Allocated NSF accommodates one accessible toilet @ 25 NSF, one accessible
wall-hung lavatory @ 13 NSF, ABA clearances, and circulation.
C. FA 3: Non-Invasive Cardiology Support Area:
1. Utility Room, Clean (UCCL1) ............................................... 120 NSF (11.2 NSM)
Provide one for Non-Invasive Cardiology.
2. Utility Room, Soiled (USCL1) .............................................. 120 NSF (11.2 NSM)
Provide one for Non-Invasive Cardiology.
3. Workroom, Event / Holter Monitor (OPHM1) ...................... 160 NSF (14.9 NSM)
Minimum NSF; provide an additional 80 NSF per each additional EKG FTE
Technician position authorized greater than two.
Chapter 210: Cardiovascular Laboratory Service - Page 9 of 16
Department of Veterans Affairs PG-18-9: Space Planning Criteria
Veterans Health Administration November 29, 2011
Washington, DC 20420 Revised: October 03, 2016
4. Storage,
Non-Invasive Cardiology Supplies (SRSE1) ...................... 120 NSF (11.2 NSM)
Minimum NSF; provide an additional 40 NSF for every increment of four
Pacemaker ICD Interrogation Rooms, EKG Testing Rooms, Cardiology Exam
Rooms, Holter Monitor Rooms, Echocardiograph Rooms, Stress Echocardiograph
Rooms, Stress Testing Treadmill Rooms, and Tilt Table Testing Rooms greater
than four.
5. Storage, ICD Equipment (SRSE1) ....................................... 120 NSF (11.2 NSM)
Minimum NSF; provide an additional 40 NSF for every increment of eight
Pacemaker ICD Interrogation Rooms, EKG Testing Rooms, Cardiology Exam
Rooms, Holter Monitor Rooms, Echocardiograph Rooms, Stress Echocardiograph
Rooms, Stress Testing Treadmill Rooms, and Tilt Table Testing Rooms greater
than eight.
6. Storage, Equipment (SRE01) ............................................... 160 NSF (14.9 NSM)
Minimum NSF; provide an additional 40 NSF for each increment of four
Pacemaker ICD Interrogation Rooms, EKG Testing Rooms, Cardiology Exam
Rooms, Holter Monitor Rooms, Echocardiograph Rooms, Stress Echocardiograph
Rooms, Stress Testing Treadmill Rooms, and Tilt Table Testing Rooms greater
than four.
7. Alcove, Crash Cart (RCA01) .................................................... 20 NSF (1.9 NSM)
Provide one for Non-Invasive Cardiology.
8. Alcove, Wheelchair / Stretcher (SRLW1) ................................ 60 NSF (5.6 NSM)
Minimum one; provide an additional one for each increment of eight Pacemaker
ICD Interrogation Rooms, EKG Testing Rooms, Cardiology Exam Rooms, Holter
Monitor Rooms, Echocardiograph Rooms, Stress Echocardiograph Rooms,
Stress Testing Treadmill Rooms, and Tilt Table Testing Rooms greater than eight.
9. Housekeeping Aides Closet (HAC) (JANC1) .......................... 60 NSF (5.6 NSM)
Provide one for Non-Invasive Cardiology.
D. FA 4: Invasive Cardiology Patient Area:
1. Cardiac CT / MRI Room (XCMRI) ......................................... 400 NSF (37.2 NSM)
Provide one per each Cardiac CT / MRI Room authorized.
2. Toilet, Patient (TPG01) ............................................................. 60 NSF (5.6 NSM)
Provide one if one or more Cardiac CT / MRI Rooms is authorized.
Allocated NSF accommodates one accessible toilet @ 25 NSF, one accessible
wall-hung lavatory @ 13 NSF, ABA clearances, and circulation.
The following rooms formerly located in this Functional Area are now located in PG-
18-9: 286 Inpatient Surgical / Endovascular Services and Ambulatory Surgical
Service; Functional Area 6: Inpatient Surgical Facility Endovascular Service Patient
Area:
Cardiac Catheterization Laboratory,
Control Room, Cardiac Catheterization,
Procedure Room, Electrophysiology,
Control Room, Electrophysiology,
Transesophageal, Echocardiograph,
Storage, TEE Probe, and
Scrub / Gowning Area.
Chapter 210: Cardiovascular Laboratory Service - Page 10 of 16
Department of Veterans Affairs PG-18-9: Space Planning Criteria
Veterans Health Administration November 29, 2011
Washington, DC 20420 Revised: October 03, 2016
E. FA 5: Invasive Cardiology Support Area:
1. Alcove, Crash Cart (RCA01) .................................................... 20 NSF (1.9 NSM)
Provide one for Invasive Cardiology.
2. Alcove, Wheelchair / Stretcher (SRLW1) ................................ 60 NSF (5.6 NSM)
Provide one for Invasive Cardiology.
3. Storage, Clean Linen (LCCL1) ................................................. 80 NSF (7.5 NSM)
Provide one for Invasive Cardiology.
4. Housekeeping Aides Closet (HAC) (JANC1) .......................... 60 NSF (5.6 NSM)
Provide one for Invasive Cardiology.
The following rooms formerly located in this Functional Area are now located in PG-
18-9: 286 Inpatient Surgical / Endovascular Services and Ambulatory Surgical
Service; Functional Area 6: Inpatient Surgical Facility Endovascular Service Patient
Area or Functional Area 9: Inpatient Surgical Facility Support Area:
Instrument Room,
System Component Room,
Viewing Room,
Supply Room, Sterile,
Surgical Facility Clean Core Area,
Equipment Cleaning Room,
Digital Quality Control Area – PACS,
Digital Archival Storage Room – PACS,
Medication Room,
Utility Room, Clean,
Utility Room, Soiled,
Lounge, Staff,
Locker Room, Male Staff,
Toilet / Shower, Male Staff,
Locker Room, Female Staff,
Toilet / Shower, Female Staff.
F. FA 6: Invasive Cardiology Prep and Recovery Area:
The following rooms formerly located in this Functional Area are now located in PG-
18-9: 286 Inpatient Surgical / Endovascular Services and Ambulatory Surgical
Service; Functional Area 3: Inpatient Surgical Facility Pre-Operative Holding / Phase
II Recovery Patient Area:
Recovery Room, Patient Prep,
Recovery Cubicle, Patient Prep,
Toilet, Prep / Recovery Patient,
Nurse Station,
Alcove, Nourishment Station,
Alcove, Crash Cart, and
Storage, Equipment
G. FA 7: Staff and Administrative Area:
1. Office,
Cardiovascular Laboratory Service Chief (OFA09) ............. 100 NSF (9.3 NSM)
Provide one for the Cardiovascular Laboratory Service.
2. Waiting (WTG03) ....................................................................... 80 NSF (7.5 NSM)
Provide one for the Cardiovascular Laboratory Service.
Chapter 210: Cardiovascular Laboratory Service - Page 11 of 16
Department of Veterans Affairs PG-18-9: Space Planning Criteria
Veterans Health Administration November 29, 2011
Washington, DC 20420 Revised: October 03, 2016
Allocated space accommodates one standard chair @ 9 NSF, one bariatric chair
@ 14 NSF, one accessible space @ 10 NSF, and circulation; total three people.
3. Workstation, Secretary (OFA07) ............................................. 56 NSF (5.3 NSM)
Provide one for the Cardiovascular Laboratory Service.
4. Workstation, Physician (OFA07) ............................................. 56 NSF (5.3 NSM)
Provide one per each Physician FTE position authorized.
5. Office, Nurse Manager (OFA09) ............................................ 100 NSF (9.3 NSM)
Provide one per each Nurse Manager FTE position authorized.
6. Workstation, Nurse Practitioner (OFA07) ............................... 56 NSF (5.3 NSM)
Provide one per each Nurse Practitioner FTE position authorized.
7. Workstation, Nurse (OFA07) .................................................... 56 NSF (5.3 NSM)
Provide one per each Nurse FTE position authorized.
8. Workstation, Technician (OFA07) ........................................... 56 NSF (5.3 NSM)
Provide one per each Technician FTE position authorized.
9. Workstation, Administration (OFA07)..................................... 56 NSF (5.3 NSM)
Provide one per each Administrative Clerk FTE position authorized.
10. Conference Room (CFR01) .................................................. 240 NSF (22.3 NSM)
Provide one for the Cardiovascular Laboratory Service.
Allocated NSF accommodates six conference chairs @ 7.5 NSF each, two 5’-0” x
2’-0” tables at 10 NSF each, one credenza @ 8 NSF, and circulation; total six
people.
11. Workroom, Cardiology Team (WRCH1) .............................. 120 NSF (11.2 NSM)
Provide one for the Cardiovascular Laboratory Service.
12. Copier / Printer Room (RPR01) ............................................... 80 NSF (7.5 NSM)
Provide one for the Cardiovascular Laboratory Service.
13. Storage, Forms / Literature (SRS01) ....................................... 80 NSF (7.5 NSM)
Provide one for the Cardiovascular Laboratory Service.
14. Toilet, Staff (TNPG1) ................................................................. 60 NSF (5.6 NSM)
Provide one for the Cardiovascular Laboratory Service.
Allocated NSF accommodates one accessible toilet @ 25 NSF, one wall-hung
lavatory @ 12 NSF, ABA clearances, and circulation.
H. FA 8: Education Area:
The spaces below provide programming of educational spaces at department /
service level.
1. Office, Residency Program Director (OFA09) ...................... 100 NSF (9.3 NSM)
Provide one if a Cardiovascular Laboratory Service Residency Program is
authorized.
2. Workstation, Intern / Resident / Fellow (OFA07).................... 56 NSF (5.3 NSM)
Provide one per each Intern, Resident, and Fellow FTE position authorized if a
Cardiovascular Laboratory Service Residency Program is authorized.
3. Training Room, Resident (CFR01) ...................................... 240 NSF (22.3 NSM)
Provide one if a Cardiovascular Laboratory Service Residency Program is
authorized.
Chapter 210: Cardiovascular Laboratory Service - Page 12 of 16
Department of Veterans Affairs PG-18-9: Space Planning Criteria
Veterans Health Administration November 29, 2011
Washington, DC 20420 Revised: October 03, 2016
Allocated NSF accommodates six conference chairs @ 7.5 NSF each, two 5’-0” x
2’-0” tables at 10 NSF each, one credenza @ 8 NSF, and circulation; total six
people.
6 PLANNING AND DESIGN CONSIDERATIONS
A. Net-to-Department Gross factor (NTDG) for Cardiovascular Laboratory Service is
1.50. This number, when multiplied by the programmed Net Square Feet (NSF) area,
determines the Departmental Gross Square Feet (DGSF).
B. Consider grouping clinician workspaces into a team room for multidisciplinary
interaction.
C. Separation of inpatient and outpatient traffic should be considered to the greatest
extent possible. Provide Reception Check-in for outpatient separate from inpatient
circulation when both patient types utilize the same departmental facilities.
D. Standardization of rooms and modular design should be considered to allow flexibility
to adapt to new technologies and respond to changes in patient volumes.
E. Connection to ancillary services, such as lab and pharmacy, should be considered.
F. The waiting room should be connected to the patient entrance corridor and be under
the visual control of Reception / Check-in. This space can be shared between
adjacent services where appropriate.
G. Design should accommodate patient privacy and confidentiality in all areas, and in
reception and patient care areas in particular. This includes visual and auditory
considerations.
H. Where possible, the department should be configured to limit the mix of patient and
service functions, and to maintain clear separation of clean and dirty functions to
avoid cross contamination. For example, Clean and Soiled Utility rooms can be
located at alternate ends of a department.
I. Corridors should be designed to a minimum of 8 feet clear width to accommodate
passage of equipment or beds and two stretchers and/or wheelchairs. In non-patient
areas and outpatient clinical spaces, corridors may be a minimum of 5 feet in clear
width.
J. Administration and support areas should be located and designed to maximize staff
and space efficiency, and reduce staff travel distances.
K. Plan for locating high volume services closer to patient waiting or building access
points to decrease patient travel time/distance and increase staff responsiveness.
Services with longer duration procedure times or low volume generation can be less
centrally located.
L. Sharing of patient and staff support areas among adjacent services should be
considered for efficient utilization of staff. For example, centralized check-in/check-out
can reduce the total number of FTE’s required to provide this function over multiple
service lines.
M. During design, NSF for Staff Lounge and Lockers may be combined with an adjacent
department(s).
N. Verify room sizes and equipment layouts with equipment vendors prior to finalizing
room layouts.
Chapter 210: Cardiovascular Laboratory Service - Page 13 of 16
Department of Veterans Affairs PG-18-9: Space Planning Criteria
Veterans Health Administration November 29, 2011
Washington, DC 20420 Revised: October 03, 2016
O. Refer to Department of Veterans Affairs (VA) Office of Construction and Facilities
Management Technical Information Library (www.cfm.va.gov/til/) for additional
technical criteria.
P. Refer to Design Guide for Cardiovascular Laboratory for a detailed discussion of
functional and design considerations.
Chapter 210: Cardiovascular Laboratory Service - Page 14 of 16
Department of Veterans Affairs PG-18-9: Space Planning Criteria
Veterans Health Administration November 29, 2011
Washington, DC 20420 Revised: October 03, 2016
7 FUNCTIONAL RELATIONSHIPS
Relationship of Cardiovascular Laboratory Service to services listed below:
TABLE 2: FUNCTIONAL RELATIONSHIP MATRIX
SERVICES RELATIONSHIP REASON
ICU 3 C, I
MS&N Patient Care Units 3 C, I
Patient Prep and Recovery 1 C, I
Emergency Department 3 C, I
Main Entrance 3 H
Cardiovascular Labs N
Endoscopy 1 A
Ambulatory Surgery/ Minor Procedure 1 A
Radiology 1 C, I
Diagnostic Testing 1 C, I
Pulmonary Clinic / Testing 1 A, G, H
Cardiology Clinic / Testing N
Digestive Disease Clinic/Testing N
Neurology Clinic/Testing N
Ventilator Storage N
Respiratory Therapy N
Pharmacy 5 B
Laboratory 5 B
Social Work / Case Management 5 H
PT/OT N
Food Service / Kitchen 5 B
Sterile Processing Department (SPD) 3 C
Staff On-Call Rooms 3 C
Linen Storage 5 B
Waste Management 5, X B, E, F
Loading Dock 5 B, D
Legend:
Relationship: Reasons:
1. Adjacent A. Common use of resources
2. Close / Same Floor B. Accessibility of supplies
3. Close / Different Floor Acceptable C. Urgency of contact
4. Limited Traffic D. Noise or vibration
5. Connection Needed E. Presence of odors or fumes
X. Not Applicable F. Contamination hazard
Y. Separation Desirable G. Sequence of work
H. Patient convenience
I. Frequent contact
J. Need for security
K. Closeness inappropriate
L Interference
Chapter 210: Cardiovascular Laboratory Service - Page 15 of 16
Department of Veterans Affairs PG-18-9: Space Planning Criteria
Veterans Health Administration November 29, 2011
Washington, DC 20420 Revised: October 03, 2016
8 FUNCTIONAL DIAGRAM
Chapter 210: Cardiovascular Laboratory Service -Page 16 of 16
You might also like
- Radiesthesia and The Major ArcanaDocument72 pagesRadiesthesia and The Major ArcanaStere Stere67% (3)
- VPP - ZetasizerDocument11 pagesVPP - ZetasizerprathimaNo ratings yet
- Operation Theater Policies and Procedures ManualDocument33 pagesOperation Theater Policies and Procedures ManualVikram92% (101)
- Textbook of Urgent Care Management: Chapter 35, Urgent Care Imaging and InterpretationFrom EverandTextbook of Urgent Care Management: Chapter 35, Urgent Care Imaging and InterpretationNo ratings yet
- Vyntus CPX Essays Diagnostic Special Edition PDFDocument48 pagesVyntus CPX Essays Diagnostic Special Edition PDFLajoskaNo ratings yet
- Monitoring Temperature and HumidityDocument27 pagesMonitoring Temperature and HumidityCyprian Cypu100% (1)
- IHFG Part B Clinical Information UnitDocument16 pagesIHFG Part B Clinical Information Unitkamil EliaNo ratings yet
- Critical Care ApplicationDocument36 pagesCritical Care ApplicationMonique ReyesNo ratings yet
- Guidebook Kidney DialysisDocument88 pagesGuidebook Kidney Dialysisunfriendly.gy2268No ratings yet
- Decision Trees QuestionsDocument2 pagesDecision Trees QuestionsSaeed Rahaman0% (1)
- 2013 ElectricalGuide Final030414Document32 pages2013 ElectricalGuide Final030414احمدعليNo ratings yet
- TS-qualification-controlled Road Vehicles PDFDocument18 pagesTS-qualification-controlled Road Vehicles PDFHassan Houdoud100% (1)
- Chapter 316: Dialysis CenterDocument16 pagesChapter 316: Dialysis CenterAnonymous oUoJ4A8xNo ratings yet
- SP Chapter 233Document14 pagesSP Chapter 233nishaNo ratings yet
- Department of Veterans Affairs VA Space Planning Criteria (316) Washington, D.C. 20402 March 2008 (SEPS Version 1.6)Document15 pagesDepartment of Veterans Affairs VA Space Planning Criteria (316) Washington, D.C. 20402 March 2008 (SEPS Version 1.6)saish11No ratings yet
- SP Chapter 316Document21 pagesSP Chapter 316Niña TolentinoNo ratings yet
- CVP MonitoringDocument36 pagesCVP MonitoringFlorence SanchezNo ratings yet
- Guidance For Industry-Diagnostic ECG Guidance (Including Non-Alarming ST Segment Measurement) - 1998Document11 pagesGuidance For Industry-Diagnostic ECG Guidance (Including Non-Alarming ST Segment Measurement) - 1998boyu wangNo ratings yet
- Chapter 214: Clinical Services AdministrationDocument14 pagesChapter 214: Clinical Services AdministrationAhmad Gamal Elden MAhanyNo ratings yet
- 130 Cardiac Investigation Unit: Draft 1.1 - 28 June 2018Document22 pages130 Cardiac Investigation Unit: Draft 1.1 - 28 June 2018ahmadgce04No ratings yet
- PCCL Standards2015Document20 pagesPCCL Standards2015ummimalikihamidNo ratings yet
- Dgnucmed 02Document17 pagesDgnucmed 02mahmoudNo ratings yet
- Methodology: Real Time Intensive Cardiac Care (Rticc)Document8 pagesMethodology: Real Time Intensive Cardiac Care (Rticc)Asad MemonNo ratings yet
- Standard OperatingDocument30 pagesStandard OperatingAgustinAjenoNo ratings yet
- 1 BEtextDocument34 pages1 BEtextSergio MontesNo ratings yet
- Cost Analysis of Cath Lab Procedures Done at A Tertiary Care Hospital of North IndiaDocument9 pagesCost Analysis of Cath Lab Procedures Done at A Tertiary Care Hospital of North IndiaIJAR JOURNALNo ratings yet
- Avs Tech Guide PDFDocument24 pagesAvs Tech Guide PDFPaoNuNo ratings yet
- NCIR - HL7 - 2.5.1 - Guide - VXU - ACK - 10.3.1 LatestDocument166 pagesNCIR - HL7 - 2.5.1 - Guide - VXU - ACK - 10.3.1 LatestUsama SarwatNo ratings yet
- PNNL Washington CEF UseCaseTestPlans - FinalDocument204 pagesPNNL Washington CEF UseCaseTestPlans - FinalBach Vu CongNo ratings yet
- DH AI Rad Companion Chest CT Whitepaper 2Document18 pagesDH AI Rad Companion Chest CT Whitepaper 2titelcosminelNo ratings yet
- New Zealand Early Warning Score Vital Sign Chart User Guide 2017Document19 pagesNew Zealand Early Warning Score Vital Sign Chart User Guide 2017Darma YantieNo ratings yet
- PHIN Laboratory Result ELR v231Document86 pagesPHIN Laboratory Result ELR v231anujaks_rlbNo ratings yet
- Ultra-Low Power Design of Wearable Cardiac Monitoring SystemsDocument7 pagesUltra-Low Power Design of Wearable Cardiac Monitoring SystemsJubin JainNo ratings yet
- PrehospitalCTASParamedicGuide December312016 Version2.0 PDFDocument98 pagesPrehospitalCTASParamedicGuide December312016 Version2.0 PDFSaifullah RachmanNo ratings yet
- RPT - 220 - Use of Water Equivalent Diameter For Calculating Patient Size and Size-Specific Dose Estimates (SSDE) in CTDocument23 pagesRPT - 220 - Use of Water Equivalent Diameter For Calculating Patient Size and Size-Specific Dose Estimates (SSDE) in CTJavier CarrascoNo ratings yet
- Use of Water Equivalent Diameter For Calculating Patient Size and Size-Specific Dose Estimates (SSDE) in CT-annotatedDocument28 pagesUse of Water Equivalent Diameter For Calculating Patient Size and Size-Specific Dose Estimates (SSDE) in CT-annotatedJuly ArgoNo ratings yet
- TED SSI Protocol PDFDocument47 pagesTED SSI Protocol PDFaberNo ratings yet
- Whole Body and Hip DXA Bone Density Most Operations Manual: Able of OntentsDocument45 pagesWhole Body and Hip DXA Bone Density Most Operations Manual: Able of OntentsDima ShvetsNo ratings yet
- Te 1540 Web PDFDocument68 pagesTe 1540 Web PDFEdis ĐedovićNo ratings yet
- HeartBeat Rate and Temperature Monitoring Device 1 EDITEDDocument57 pagesHeartBeat Rate and Temperature Monitoring Device 1 EDITEDFeddy Micheal FeddyNo ratings yet
- Robust Classification of Cardiac Arrhythmia Using Machine LearningDocument9 pagesRobust Classification of Cardiac Arrhythmia Using Machine LearningIJRASETPublicationsNo ratings yet
- Clinical MonitoringDocument42 pagesClinical Monitoringibrahim kademogluNo ratings yet
- Oxy ReportDocument83 pagesOxy ReportPride Sikipa0% (1)
- FDA GuidanceDocument29 pagesFDA GuidanceAlison BurdettNo ratings yet
- Hospital Del Dia - EeuuDocument10 pagesHospital Del Dia - EeuuIsaac AnguloNo ratings yet
- Ewquickguide 2 EdDocument188 pagesEwquickguide 2 EdStanley Wu TaiNo ratings yet
- U.S. Food & Drug Administration 10903 New Hampshire Avenue: Silver Spring, MD 20993Document9 pagesU.S. Food & Drug Administration 10903 New Hampshire Avenue: Silver Spring, MD 20993Lâm Hoàng Thiên VũNo ratings yet
- Ctas Pre HospitalDocument97 pagesCtas Pre HospitalHani Tri HandokoNo ratings yet
- RACECARS Trial Overview For EMS and 911 2021-02-16Document54 pagesRACECARS Trial Overview For EMS and 911 2021-02-16Robby MartinNo ratings yet
- Specification and Acceptance Testing of Radiotherapy Treatment Planning SystemsDocument68 pagesSpecification and Acceptance Testing of Radiotherapy Treatment Planning Systemsjiar001No ratings yet
- Indicadores Post RCPDocument14 pagesIndicadores Post RCPFernando Martinez AguilarNo ratings yet
- Lumify Reimbursement GuideDocument12 pagesLumify Reimbursement Guidecrazyballerman808No ratings yet
- E-Health Management SystemDocument85 pagesE-Health Management Systemwalid youssefNo ratings yet
- E Monitoring For Raised Intracranial Pressure and Vasospasm PDF 11262109074Document51 pagesE Monitoring For Raised Intracranial Pressure and Vasospasm PDF 11262109074jiovannaescalanteNo ratings yet
- CARESCAPECentral StationBrochureUSJB64765USApr2019Document14 pagesCARESCAPECentral StationBrochureUSJB64765USApr2019Trịnh Quang ThắngNo ratings yet
- ABS Advisory On Structural Health Monitoring The Application of Sensor-Based ApproachesDocument24 pagesABS Advisory On Structural Health Monitoring The Application of Sensor-Based ApproachesinnovativekarthiNo ratings yet
- Final Document: Global Harmonization Task ForceDocument30 pagesFinal Document: Global Harmonization Task Forcechitti poluriNo ratings yet
- Intellegent Systems For BiomechanicsDocument5 pagesIntellegent Systems For BiomechanicsSrinivas RaghavanNo ratings yet
- Differential GPS Measurement of Overhead Conductor Sag: Software ImplementationDocument30 pagesDifferential GPS Measurement of Overhead Conductor Sag: Software ImplementationbogdanNo ratings yet
- Cancer Study Protocol Web ReadyDocument31 pagesCancer Study Protocol Web ReadyclaudiorafaelroncaNo ratings yet
- The Measurement and The Monitoring of The Central Hemodynamics Using Non-Invasive and Minimally-Invasive DataDocument145 pagesThe Measurement and The Monitoring of The Central Hemodynamics Using Non-Invasive and Minimally-Invasive Dataadh30No ratings yet
- Implementation of a Remote and Automated Quality Control Programme for Radiography and Mammography EquipmentFrom EverandImplementation of a Remote and Automated Quality Control Programme for Radiography and Mammography EquipmentNo ratings yet
- Dosage Calculations, CH 10 ProblemsDocument1 pageDosage Calculations, CH 10 ProblemsJacqueline GreerNo ratings yet
- Industrial Attachment ReportDocument34 pagesIndustrial Attachment ReportOtsile Charisma Otsile Saq100% (1)
- NACH FormDocument2 pagesNACH FormShreyas WaghmareNo ratings yet
- Interventional Cardiology and SurgeryDocument19 pagesInterventional Cardiology and SurgeryDEV NANDHINI RNo ratings yet
- AD Oracle ManualDocument18 pagesAD Oracle ManualAlexandru Octavian Popîrțac100% (2)
- Eaton Current Limiting FusesDocument78 pagesEaton Current Limiting FusesEmmanuel EntzanaNo ratings yet
- Profile of RespondentsDocument36 pagesProfile of RespondentsPratibha SharmaNo ratings yet
- TestDocument233 pagesTestye rightNo ratings yet
- Figs Taste Scale of Selected Varieties From Hawaiifruit-Net PDFDocument4 pagesFigs Taste Scale of Selected Varieties From Hawaiifruit-Net PDFHanafizar Hanafi Napi AtanNo ratings yet
- ECO-321 Development Economics: Instructor Name: Syeda Nida RazaDocument10 pagesECO-321 Development Economics: Instructor Name: Syeda Nida RazaLaiba MalikNo ratings yet
- CR-7iA CR-4iA Installation and Setup Guide (B-83774JA-1 01)Document1 pageCR-7iA CR-4iA Installation and Setup Guide (B-83774JA-1 01)lidiia.pavlkukNo ratings yet
- Theory of Accounts On Business CombinationDocument2 pagesTheory of Accounts On Business CombinationheyNo ratings yet
- Scenario of Shale Gas Exploration in IndiaDocument24 pagesScenario of Shale Gas Exploration in IndiaManish TiwariNo ratings yet
- הרצאה- אנמיה וטרומבוציטופניהDocument87 pagesהרצאה- אנמיה וטרומבוציטופניהliatfurmanNo ratings yet
- Management of AsthmaDocument29 pagesManagement of AsthmaAbdullah Al ArifNo ratings yet
- All About 304 Steel (Properties, Strength, and Uses)Document7 pagesAll About 304 Steel (Properties, Strength, and Uses)ZebNo ratings yet
- Ulangan Tengah Semester: Mata Pelajaran Kelas: Bahasa Inggris: X Ak 1 / X Ak 2 Hari/ Tanggal: Waktu: 50 MenitDocument4 pagesUlangan Tengah Semester: Mata Pelajaran Kelas: Bahasa Inggris: X Ak 1 / X Ak 2 Hari/ Tanggal: Waktu: 50 Menitmirah yuliarsianitaNo ratings yet
- Cooking VocabularyDocument2 pagesCooking VocabularyDANIELANo ratings yet
- Listes de Produits GAURAPADDocument1 pageListes de Produits GAURAPADBertrand KouamNo ratings yet
- Eim s2000 Series Brochure PDFDocument16 pagesEim s2000 Series Brochure PDFHumbertoOtaloraNo ratings yet
- Celgene V Actavis AbraxaneDocument131 pagesCelgene V Actavis AbraxaneiphawkNo ratings yet
- PaperDocument21 pagesPaperAnonymous N2TkzrNo ratings yet
- Fermentation Media: Agustin Krisna WardaniDocument27 pagesFermentation Media: Agustin Krisna WardaniYosiaNo ratings yet
- Potential Prospect 1.7Document6 pagesPotential Prospect 1.7Joshua M. GenoviaNo ratings yet
- Naming Alcohols, Aldehydes. EtcDocument1 pageNaming Alcohols, Aldehydes. Etcim_mikezNo ratings yet
- Amp. 100 Watt ExtractedDocument6 pagesAmp. 100 Watt ExtractedJosue CórdovaNo ratings yet
- 13 Unit 5 PainDocument4 pages13 Unit 5 PainAndres SalazarNo ratings yet
- GCU 0103 Computer PlatformsDocument5 pagesGCU 0103 Computer PlatformsArani NavaratnarajahNo ratings yet