Professional Documents
Culture Documents
Mte (2014)
Uploaded by
TommysOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Mte (2014)
Uploaded by
TommysCopyright:
Available Formats
reviews Annals of Oncology
Annals of Oncology 25: 564–577, 2014
doi:10.1093/annonc/mdt433
Published online 26 November 2013
Factors influencing adherence to cancer treatment in
older adults with cancer: a systematic review
M. T. E. Puts1*, H. A. Tu1,2, A. Tourangeau1, D. Howell1,3, M. Fitch1,4, E. Springall5 & S. M. H. Alibhai6,7
1
Lawrence S. Bloomberg Faculty of Nursing; 2Institute of Health Policy, Management and Evaluation, University of Toronto, Toronto; 3Princess Margaret Hospital, University
Health Network, Toronto; 4Odette Cancer Centre, Sunnybrook Health Sciences Centre, Toronto; 5Gerstein Science Information Centre, University of Toronto Libraries,
Toronto; 6Toronto General Hospital, University Health Network, Toronto, Canada; 7Department of Medicine and Institute of Health Policy, Management, and Evaluation,
University of Toronto, Toronto, Canada
Received 4 September 2013; accepted 6 September 2013
Background: Cancer is a disease that mostly affects older adults. Treatment adherence is crucial to obtain optimal out-
comes such as cure or improvement in quality of life. Older adults have numerous comorbidites as well as cognitive and
sensory impairments that may affect adherence. The aim of this systematic review was to examine factors that influence
adherence to cancer treatment in older adults with cancer.
Patients and Methods: Systematic review of the literature published between inception of the databases and February
2013. English, Dutch, French and German-language articles reporting cross-sectional or longitudinal, intervention or obser-
vational studies of cancer treatment adherence were included. Data sources included MEDLINE, EMBASE, PsychINFO,
Cumulative Index to Nursing and Allied Health (CINAHL), Web of Science, ASSIA, Ageline, Allied and Complementary
Medicine (AMED), SocAbstracts and the Cochrane Library. Two reviewers reviewed abstracts and abstracted data using
standardized forms. Study quality was assessed using the Mixed Methods Appraisal Tool 2011.
Results: Twenty-two manuscripts were identified reporting on 18 unique studies. The quality of most studies was good.
Most studies focused on women with breast cancer and adherence to adjuvant hormonal therapy. More than half of the
studies used data from administrative or clinical databases or chart reviews. The adherence rate varied from 52% to 100%.
Only one qualitative study asked older adults about reasons for non-adherence. Factors associated with non-adherence
varied widely across studies.
Conclusion: Non-adherence was common across studies but little is known about the factors influencing non-adher-
ence. More research is needed to investigate why older adults choose to adhere or not adhere to their treatment regimens
taking into account their multimorbidity.
Key words: systematic review, geriatric oncology, non-adherence, cancer treatment, aged
introduction in quality of life. Cancer medication non-adherence has been
shown to lead to decreased survival [4–7], higher recurrence/
Cancer is a disease that mostly affects older adults. It is esti- treatment failure rates [8–10] and health care costs [4–9, 11, 12].
mated that 70% of all incident cases and over 82% of deaths due Adherence is a multidimentional phenomenon, and according to
to cancer occur in persons aged ≥60 years in Canada [1]. This is the WHO, is influenced by patient-related factors, therapy-related
similar to other Western developed countries [1, 2]. With an factors, condition-related factors, health system factors and social
aging population, there will be a significant increase in the economic factors [3].
number of older adults being diagnosed with cancer [1, 2]. In addition to cancer, older persons often have other medical
Treatment adherence is defined by the World Health conditions. In 2006, 88% of Canadian older adults had at least
Organization (WHO) (2003) as “the extent to which a person’s one medical condition, and 65% had two or more conditions
behaviour—taking medication, following a diet and/or executing [13]. With increasing age, the number of chronic conditions
lifestyle changes, corresponds with agreed recommendation from increases. For the treatment of these chronic conditions, older
a health care provider” [3]. Cancer treatment adherence is crucial adults usually take multiple medications. Older adults take, on
to obtain optimal health outcomes, such as cure or improvement average, 6.5 medications per day [14]. Multimorbidity in the
older population increases treatment complexity (e.g. conflicting
treatments, drug interactions) [15–17]. An increasing number
*Correspondence to: Dr Martine Puts, Lawrence S. Bloomberg Faculty of Nursing,
University of Toronto, 155 College Street, Suite 130, Toronto, Canada M5T1P8,
of prescribed medications are associated with decreasing medi-
Tel: +1-416-978-6059, fax: +1-416-978-8222; E-mail: martine.puts@utoronto.ca cation adherence in the general older population as well as in
© The Author 2013. Published by Oxford University Press on behalf of the European Society for Medical Oncology.
All rights reserved. For permissions, please email: journals.permissions@oup.com.
Downloaded from https://academic.oup.com/annonc/article-abstract/25/3/564/148605
by guest
on 28 May 2018
Annals of Oncology reviews
older adults who are prescribed oral chemotherapy and/or hor- mean/median age of <65 years but reported on results for a sub-
monal therapy [18–23]. Research findings suggest that in the group of which the mean/median age is ≥65, the publication
general older population, up to 50% are non-adherent to medi- was considered eligible for inclusion.
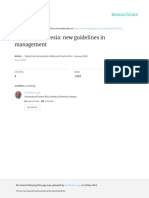
cation recommendations [19, 24], which can consequently have The studies were selected in a two-step process (Figure 1).
serious complications for the health status of an older adult. First, an initial selection based on titles and abstracts was com-
Although there have been narrative/expert reviews of adher- pleted independently by two reviewers (MP and HAT). In case
ence to medication in the general older adult population [19], of uncertainty, the abstract was included for full-text review (in-
and several narrative and systematic reviews of adherence to cluding abstracts that were addressing adherence but no age for
oral antineoplastic agents for cancer patients across age groups the study population was reported). Second, the full-text articles
[18, 25–32], there has been no systematic review of the factors were retrieved and reviewed independently by the same
influencing adherence to all forms of active cancer treatment that reviewers. In case of disagreement between the two reviewers or
focused specifically on older adults with cancer. Furthermore, uncertainty, the other members of the research team were pro-
most of the reports of these reviews did not specify the search vided the full-text article for consensus decision-making. For all
strategy, inclusion and exclusion criteria, the results of the search articles that referred to additional publications for more details
strategy, setting and sample of studies, or did not assess the on study methods, those publications were retrieved and
quality of included studies, and it is not clear if the data abstrac- reviewed to complement the data abstraction and quality assess-
tion for the review was done by one or more researchers. ment of the eligible study publication. In articles, where no age
Moreover, many included only studies published in English while for the study population was reported in the full text, the study
ignoring studies published in other languages. Therefore, the ob- authors were then contacted to obtain the details on the study
jective of this systematic review was to synthesize all studies to age. If no response was received after at least three attempts, the
address the research question ‘What factors influence adherence article was not included in the final selection as no paper indi-
to active cancer treatment in older adults aged 65 and over diag- cated that the study population were older adults.
nosed with cancer?’
Data abstraction
We have used the PRISMA statement for guiding the data ab-
materials and methods straction and reporting of this systematic review [33]. Data were
search strategy and selection criteria abstracted using the data abstraction form that had been devel-
oped for this systematic review by the research team. Data ab-
This review was based on a systematic, comprehensive search of
straction was completed independently by the same reviewers,
10 databases from inception of each database until February
who carried out the article selection (MP and HAT). The
2013, including the Cochrane Central Register of Controlled
abstracted information included study design, aim of study, lo-
Trials, MEDLINE, EMBASE, Cumulative Index to Nursing and
cation of study, sampling method and sample size, response
Allied Health (CINAHL), Allied and Complementary Medicine
rate, source of data, characteristics of included study participants
(AMED), Psych-INFO, Ageline, Sociological Abstracts, Web of
including age, sex, cancer type, cancer stage, setting (country),
Science, and Applied Social Sciences Index and Abstracts
date of diagnosis, comorbid conditions, cancer treatment
(ASSIA) databases. Eligible studies were searched using key
(surgery, chemotherapy, radiation, hormonal treatment, tar-
words/medical subject headings (MeSHs) such as medication ad-
geted therapy/biological agents), definition of treatment adher-
herence, guideline adherence, compliance, treatment preferences,
ence, factors influencing the cancer treatment adherence and
medication management, and perceptions of medication AND
details of statistical analysis. If any aspect of the study design
neoplasms/cancer AND Aged, 65 and over, elderly, older adult
and conduct was unclear, the study authors were contacted. A
(see supplementary Appendix 1, available at Annals of Oncology
meta-analysis was not possible as studies were heterogeneous
online, for the complete search strategy used in MEDLINE). A
with respect to adherence definitions, cancer treatments, study
similar search strategy was used in the remaining nine databases.
populations, methods and outcomes.
In addition, we reviewed the reference lists of previous reviews to
Although the International Society for Pharmacoeconomics
identify potentially eligible studies. The literature search was con-
and Outcomes Research workgroup Medication Compliance
ducted by an experienced university librarian (ES).
and Persistence in 2008 published definitions for both adher-
Inclusion criteria: Publications were included if reporting on
ence/compliance (synonyms) and persistence [34], in this
factors influencing adherence to any active cancer treatment (i.
review we chose to use the definitions of adherence/persistence
e. chemotherapy, surgery, radiation therapy, hormonal therapy
as provided by the study authors in the manuscript, as many of
and therapy with molecular-targeted agents and any combina-
the included studies were published before these definitions and
tions of these treatments) in older patients aged ≥65, being diag-
might have used these terms interchangeably.
nosed with cancer. Study designs could include cross-sectional,
prospective, controlled interventional or observational studies,
or qualitative studies that assessed the factors influencing cancer quality assessment
treatment adherence of older adults (≥65) with cancer. Articles Both qualitative and quantitative studies were included. Pluye
written in English, French, Dutch and German were eligible. et al. [35] have developed a scoring system to assess the meth-
Exclusion criteria: Publications focusing on cancer patients odological quality of each individual study called the Mixed
younger than 65 years of age, editorials and review articles were Methods Assessment Tool (MMAT) that can be used for mixed
ineligible. However, if a study included participants with a methods research and mixed studies reviews (MSRs). The
Volume 25 | No. 3 | March 2014 doi:10.1093/annonc/mdt433 |
Downloaded from https://academic.oup.com/annonc/article-abstract/25/3/564/148605
by guest
on 28 May 2018
reviews Annals of Oncology
Potentially relevant citations identified and screened for retrieval (N = 15,056):
Bibliographic databases (N = 15,055) plus 1 article in press identified by experts in the field
Citations excluded based on abstract and title review (N = 14,494). Reasons:
Not about adherence to active cancer treatment (N = 13,036)
Mean/median age study population <65 years or no age reported (N = 197)
Editorial/Review/case study (N = 257)
Duplicate publication (N = 1,004)
Citations included based on abstract and title review (N = 558)
Studies excluded (N = 536). Reasons:
Editorial/Review/case study (N = 44)
Mean/median age study population<65 years or no age reported (N = 321)
Not about adherence to active cancer treatment (N = 171)
Relevant citations for inclusion (N = 22 manuscripts) reporting on 18 unique studies
Figure 1. Flow chart of study selection.
authors tested the reliability and efficacy of this system and two other manuscripts, authors used data from the same pro-
found that agreement between reviewers was moderate to excel- spective observational cohort study [41, 47]. One author pub-
lent for the MMAT criteria and it was easy to use [35]. The 2011 lished three manuscripts using the same clinical chart database,
MMAT scoring system contains five types of mixed methods but the populations were not completely overlapping (different
study components or primary studies in a MSR context each age inclusion criteria and time periods of the data collected)
with its own set of methodological quality criteria based on the [42–44]. Thus, a total of 18 unique studies were included. All
existing published criteria. For each item, the answer categories included manuscripts were written in English. The percentage
were ‘yes’, ‘no’, ‘can’t tell’ followed by comments. The five types identified below refers to the percentage of the total of 18 studies
of mixed methods study components or primary studies in the result sections.
included in the MMAT are (i) qualitative; (ii) quantitative, ran-
domized, controlled trials; (iii) quantitative non-randomized; quality assessment
(iv) quantitative descriptive and (v) mixed methods. Two
reviewers (MP and HU) scored the quality of included studies The quality was good for most studies, see supplementary
independently. No study was excluded based on the quality as- Table S1, available at Annals of Oncology online. Ten studies
sessment. (56%) used data from several administrative and clinical data-
bases or chart reviews [36, 37, 39, 40, 42–44, 46, 49, 50, 52, 53,
55]. In three studies (17%), data from clinical trials were used
[45, 48, 51, 54]. In three other studies (17%), data were collected
results using prospective observational studies [38, 41, 47, 56]. One
We screened 15 056 titles and abstracts for eligibility in the first study (6%) used a retrospective observational study design [57].
step, from which we selected 558 for full-text review (see One study used a qualitative study design [53]. Of those eight
Figure 1, for an overview of the selection and the reasons for studies that did not use administrative databases/clinical data-
exclusions). In total, 21 manuscripts were included in this bases/chart reviews, only three studies reported the response
review [36–57] reporting on 18 unique studies. In two manu- rate [38, 41, 47, 53], and thus the extent of selection bias cannot
scripts, authors used data from the same clinical trial [51, 54]. In be evaluated for the majority of studies. For the prospective
| Puts et al. Volume 25 | No. 3 | March 2014
Downloaded from https://academic.oup.com/annonc/article-abstract/25/3/564/148605
by guest
on 28 May 2018
Annals of Oncology reviews
observational studies, the method of how the follow-up was con- therapy without treatment completion [51] and being pre-
ducted was described for all studies. For six studies (33%), it was scribed at least six cycles of it should be at least one of the three
not clear how much missing data there were and/or how the cyclophosphamide methotrexate 5-fluorouracil drugs [54]. The
investigators dealt with the missing data in the analyses [37, 38, persistence rate varied between 51% [50] and 91.7% [43].
40, 45, 46, 57]. For three studies (17%), the data analysis
methods were not described in sufficient detail [48, 53, 56]. which factors are associated with treatment (non-)
adherence and (non-)persistence in older adults
characteristics of included studies with cancer?
The characteristics of the included studies are described in sup- We used the WHO classification of five factors influencing ad-
plementary Table S2, available at Annals of Oncology online. Of herence to describe the diverse range of factors that were exam-
the 18 studies included, 11 (61%) were conducted in the United ined in the 18 studies included in this review (Table 1).
States, two in Switzerland (6%), one in the UK (6%), one in
Germany (6%), one in Ireland (6%), one in France (6%) and patient-related factors. Patient-related factors associated with
one in Hong Kong (6%). greater non-adherence and non-persistence were older than 75
The sample size of the included studies ranged from 25 [55] years of age [36, 37, 39, 50], older than 84 [49, 52], black race
to 22 160 patients [49]. [36], non-White race [52], being unmarried [36], having
Most studies (61%) included participants with breast cancer dementia/Parkinson disease [37], denial of cancer diagnosis/
[36–38, 41–44, 46, 47, 49–52, 54, 57]; other studies included psychiatric illness/alcohol dependency [43, 44], change in
colon cancer [39], head and neck cancer [40], bladder cancer normal daily routines [53], not understanding treatment
[45], carcinoma of the oral cavity [48], prostate cancer [55] or a (appointment) instructions [53, 55, 56] or forgetting the
mixed population [53, 56]. The majority (56%) focused on exam- treatment [56]. Patient-related factors associated with greater
ining (non-)adherence/ (non-)persistence to adjuvant hormonal adherence and persistence were younger age [38], being
therapy [37, 38, 41–44, 46, 47, 49, 50, 52, 57], adjuvant chemo- unmarried [46], excellent communication abilities [38], having
therapy/molecular targeted therapy [36, 39, 51, 54], radiation no comorbidities [40] and having a Charlson Comorbidity
treatments [40, 45], chemotherapy/molecular targeted therapy in Score of ≥3 / or increasing Charlson Comorbidity Scores
the context of advanced disease [53], chemotherapy/molecular (meaning adherence increased for each additional point on the
targeted therapy for both adjuvant and advanced disease[56], Charlson Comorbidity Score) [46, 52].
hormone treatment in the context of advanced disease [55] and a
combination of chemotherapy and surgery [48]. therapy-related factors. Negative or neutral beliefs about the
In 10 studies (non-)adherence was studied [36, 38, 39, 41, 45, value of the treatment were associated with greater non-
47, 48, 52, 55–57], in two studies non-persistence [37, 49] and in adherence and non-persistence [41, 43], as well as lack of
two other studies [46, 51, 54] both (non-)adherence and (non-) immediate treatment effect and misconceptions about the
persistence were studied. In three studies, treatment completion/ treatment effect [48], therapy-related side-effects [43–45, 47, 51,
discontinuation/non-use was studied (without defining it as 53–56], the treatment equipment itself (e.g. comfort of the mask
either as non-adherence or non-persistence) [40, 50, 53]. One needed for treatment radiation) [45], use of antidepressants at
study had three different publications [42–44], in which a differ- the time of cancer drug treatment initiation [37], higher
ent aspect of adherence and persistence was studied in each. number of drug prescriptions [47, 49], having received breast-
conserving surgery without radiation [50] or mastectomy [51,
how were non-adherence and 52]. Factors associated with greater adherence and persistence
non-persistence defined? were having positive views about the treatment [47], not having
The definition of non-adherence varied substantially between chemo while receiving radiation [40], and having had surgery
studies, ranging from having received less than four cycles of before radiation [40].
anthracycline chemotherapy [36], having received less than five
cycles of chemotherapy within 9 months of diagnosis [39], condition-related factors. Condition-related factors associated
missing one or more medication injections [55], self-reported with greater non-adherence and non-persistence are (number
intake of the medication [38, 41, 47], a medication possession of ) hospitalizations [36, 39, 45], having positive lymph nodes
rate (MPR) of <80% [46, 49, 52, 57], <80% of doses expected [41], lymph node-negative disease [51, 54], Estrogen Receptor
recorded by the microelectronic monitoring system (MEMS) (ER) indeterminate status [50], hormone receptor-positive
[51], <80% of doses expected recorded in medication calendars tumours [54] and cancer recurrence [39]. Factors associated
[54] and <100% of expected doses recorded in medication with greater adherence were early-stage disease [38], ER+ status
diaries [56]. The rate of adherence varied between 52% [40] and [38] and regional cancer stage [46].
100% [57].
Similarly, the definition of non-persistence also varied greatly health system factors. Factors associated with greater non-
between studies ranging from having 45 days of gap between adherence included having follow-up appointments with a
refills [49], discontinuation of >60 days [50], ≥90 days between general practitioner instead of an oncologist [42], prescription for
refills [46], having 180 consecutive days of no tamoxifen supply cancer treatment provided by a non-oncologist [49], receiving
after the first prescription [37], taking the medication <36 misinformation about the treatment from the physician [43, 44],
months [44], taking the treatment <5 years [43], coming off long waiting times in the clinics and having to travel long
Volume 25 | No. 3 | March 2014 doi:10.1093/annonc/mdt433 |
Downloaded from https://academic.oup.com/annonc/article-abstract/25/3/564/148605
by guest
on 28 May 2018
reviews Annals of Oncology
distances to clinics [55]. Factors associated with greater adherence fill the prescription at the pharmacy by themselves or having
were a higher number of physicians involved in care [38] and visual or hearing impairment—were associated with cancer treat-
having seen an oncologist before the start of treatment [52]. ment adherence. In addition, only one study examined the
impact of economic factors such as co-payments on adherence
social economic factors. Factors associated with non-adherence and persistence [46]. In Canada, 5% of all seniors lived in poverty
and non-persistence included insurance reasons [43] and co- in 2010 [59]. In addition, the ‘out-of-pocket’ costs for cancer
payments of ≥$30 USD [49]. treatment in Ontario, Canada, are substantial, despite having a
universal health care system with almost all medications covered
by the public health plan. Longo et al. [60, 61] reported that ‘out-
discussion of-pocket’ costs for cancer treatment including transportation
To our knowledge, this is the first systematic review focusing on were on average $585 per month in 2003, and 20% of the studied
adherence to all active cancer treatments in older adults diag- sample reported that this financial burden was problematic.
nosed with cancer. The reviewed studies represented a diverse Although seniors in various jurisdictions might be eligible for
range of cancer treatments; however, most focused on adjuvant publicly funded medication coverage, plans could require co-pay-
hormonal therapy for women with early-stage breast cancer. ments, payment of dispensing fees or only partial coverage of
Studies used very different definitions of both adherence and per- costs. In older adults with comorbidities, these additional costs
sistence which affected the adherence and persistence rates could add to a significant financial burden that potentially
reported as well as factors associated with adherence and persist- impacts adherence to cancer treatment. Therefore, this needs to
ence. The WHO has described five groups of factors (patient- be examined in future studies.
related factors, therapy-related factors, condition-related factors, More than half of the included studies abstracted data from
health system factors and social economic factors) that influence administrative and clinical databases and/or charts using claim
treatment adherence and in our review we found evidence sup- codes and prescription refill data. Although this provides an es-
porting each of these groups of factors affecting adherence in this timate of when the prescriptions were filled, in most of these
population. studies it was not examined or not possible to examine if the
Factors associated with non-adherence were not all consistent patient actually took the medication according to the treatment
across all studies conducted. For example, some studies reported plan prescribed. Only the study by Regnier Denois et al. [53] ex-
that an age of ≥75 years were associated with non-adherence plicitly asked older adults how they managed their capecitabine
[36, 37, 39, 50], whereas many studies found no association treatment. Using a qualitative study design, they reported that
between age and adherence [38, 42, 46, 47, 49, 51, 54, 57]. changes in regular routine (e.g. being out of town for family
Similarly, some studies had conflicting findings about other visits) are an important time when non-adherence to treatment
factors, for example some reported that being unmarried, occurs. Furthermore, they showed that that the treatment dosing
having several comorbidities or having lymph node-negative schedules are being changed by older adults for convenience
disease were associated with higher adherence and persistence reasons (e.g. not before meals on an empty stomach but several
[40, 46], while others reported the same factors being associated hours later), which might impact treatment efficacy and safety.
with greater non-adherence and non-persistence [36, 51,54]. It is important that a patient understands the reasons for the
These differences may be due to the different methods of data treatment and the treatment itself. This should be addressed in
collection as some of these studies used administrative databases patient education sessions by health care providers before and
[36, 40, 46], while the other study used data collected within a during cancer treatment. Several studies showed that patients’
clinical trial [51, 54]. Another possibility is that the study popu- beliefs about the value of treatment was an important factor
lation within the clinical trial was more motivated to complete influencing adherence and persistence [41, 43, 44, 48, 53] as well
the treatment compared with the general older cancer popula- is the level of understanding of the treatment instructions [43,
tion included in the administrative databases and therefore, 44, 53, 55, 56]. However, only the study by Barron et al. [37]
factors influencing adherence rates are different. For several included a proxy measure for dementia/Parkinson disease
other factors, there were more consistent findings across studies. (based on prescription information). No other study included a
Specifically, hospitalizations, therapy-related side-effects and no measure of cognitive functioning of the older adults or a
visit to a medical oncologist before and during treatment were measure of health literacy. Cognitive impairment and low health
negatively associated with adherence and persistence [36, 39, literacy are common in older adults in the oncology setting [62,
42–45, 47, 49, 51, 52, 56]. The latter finding may be particularly 63], yet it is unclear whether this impacts cancer treatment ad-
important since it has been reported that there is a referral bias herence [64–67]. These are important factors and need to be
of non-oncologist physicians not referring older adults with included in future studies investigating adherence to active
cancer to a medical oncologist [58]. cancer treatments in older adults.
What is surprising is that only a few studies examined factors Another important issue is comorbidity. In half the included
that are known to affect cancer treatment decisions for patients, studies, it was not reported what type(s) or how many other
their families and their health care providers. This includes chronic health conditions the older adults with cancer had [42–
factors such as the number of hospital visits required for the treat- 45, 47, 48, 51, 53–57], and only a few studies included the mean
ment and travel time to the hospital, which was included in only number of prescriptions taken [41, 46, 47, 52]. The three studies
one study [55]. Furthermore, no study examined classic geriatric [38, 46, 52] that did find any association between the number of
factors—such as whether the ability to travel to the cancer treat- comorbid conditions and adherence/persistence showed confl-
ment centre alone to receive the cancer treatment or the ability to icting findings. In these studies, adjuvant hormonal therapy in
| Puts et al. Volume 25 | No. 3 | March 2014
Downloaded from https://academic.oup.com/annonc/article-abstract/25/3/564/148605
by guest
on 28 May 2018
Annals of Oncology
Volume 25 | No. 3 | March 2014
Table 1. Factors associated with adherence and persistence to active cancer treatment in older adults diagnosed with cancer
Author, Which cancer Definition of non- Measurement of Adherence /persistence rate Statistical analysis Which variables were Factors associated with Factors associated with
publication treatments were adherence used or non-adherence/ used to examine included in the statistical non-adherence (−) or non-persistence (−) or
date included in the adherence/non-persistence non-persistence factors associated analysis? higher adherence (+) higher persistence (+)
(reference) study? used or persistence with non-
adherence /non-
persistence
Barcenas et al. Chemotherapy Non-adherence: having Claim codes in the Adherence rate: 83% Logistic regression Age at diagnosis, race, Age >75 years (−), black NA
[36] received one to three administrative analysis marital status, race (−), unmarried
cycles of anthracyclines. databases educational level, status (−), two different
Adherent: having poverty level, SEER SEER-regions (−), those
received four or more region, year of diagnosis, diagnosed in 2000 or
cycles of anthracyclines lymph node earlier (−), number of
involvement, tumour hospitalizations (more
size, tumour grade, PR hospitalizations had
and ER receptor status, larger impact on non-
surgery type, Charlson adherence) (−)
comorbidity index,
radiation therapy and
number of
hospitalizations
Barron et al. Tamoxifen Tamoxifen non-persistence Prescription refill Persistence rate: 77.9% at 1 Cox proportional Variables in univariate Age >75 compared with
[37] (hormonal was defined as 180 data year of treatment and hazard analysis with p < 0.1 45–54 years (−), using
therapy) consecutive days of no 64.8% at 3.5 years of regression were selected in the antidepressant
tamoxifen supply after treatment analysis multivariable model and medication at tamoxifen
the index date (=first included age, types of initiation (−), and
prescription) without prescription drug usage, having dementia/
alternative hormonal number of having Parkinson disease (−),
therapy during that time dementia/Parkinson greater than one
disease, mean number pharmacological agents
of pharmacological per month a year before
agents per month tamoxifen initiation (+)
Demissie et al. Tamoxifen Women who were taking Self-report during Adherence: 85% at 21 Logistic regression All study variables were No factor was associated
[38] (hormonal tamoxifen were classified a telephone months after surgery for analysis included in one model with discontinuation of
therapy) at the second follow-up follow-up breast cancer follow-up and then removed if not tamoxifen. Age
interview as either still interview, contributing. Two (younger age +), stage 2
doi:10.1093/annonc/mdt433 |
taking tamoxifen (yes) or questions not models were run: (+), ER positive status
no longer taking specified tamoxifen use at follow- (+) and number of
tamoxifen (no) up as outcome, and physicians (higher
tamoxifen number +) and excellent
discontinuation at ability (+) to
reviews
follow-up as outcome communicate were all
(n = 26, model associated with
underpowered) tamoxifen use
Dobie et al. Chemotherapy Adherence: having received Adherence rate using a Logistic regression Race, age, sex, ethnicity, older age (−), female (−),
[39] 5 months/cycles (one conservative definition analysis marital status, location readmission to hospital
Continued
Downloaded from https://academic.oup.com/annonc/article-abstract/25/3/564/148605
by guest
on 28 May 2018
Table 1. Continued
reviews
| Puts et al.
Author, Which cancer Definition of non- Measurement of Adherence /persistence rate Statistical analysis Which variables were Factors associated with Factors associated with
publication treatments were adherence used or non-adherence/ used to examine included in the statistical non-adherence (−) or non-persistence (−) or
date included in the adherence/non-persistence non-persistence factors associated analysis? higher adherence (+) higher persistence (+)
(reference) study? used or persistence with non-
adherence /non-
persistence
cycle a month) of Claim codes in the and full study sample: of residence, and age- (−), recurrence of cancer
chemotherapy within 9 administrative 78% and race-specific (−) were associated with
months of diagnosis databases household income and lower chemotherapy
(liberal definition) and SEER registry were completion rates
having received 6 included in all models
months/cycles (one cycle plus variables with
a month) of P < 0.09 or those that
chemotherapy within 9 significantly improved
months of diagnosis model fit
(conservative definition)
Fesinmeyer Radiation Complete course of Claim codes in the 70.4 of surgical patients and Logistic regression Each model included the For oral cavity tumours:
et al. [40] therapy (RT) radiation: at least 30 administrative 52% of nonsurgical analysis, a receipt of surgery surgery within 30 days
treatments for those who databases patients completed RT separate model relative to radiation before RT (+), Charlson
did not have surgery without interruptions/ was calculated (yes/no and within 30 of 0(+), not chemo (+).
before RT, at least 25 gaps for each of the days), tumour stage, For pharynx: surgery
treatments for those who five tumour comorbidity, age, sex, within 30 days of RT (+)
had prior surgery. An sites (larynx, race, urban versus rural and no chemo (+) and
interruption or gap was nasal cavity, residence regional tumour (+). For
defined as lapses of >4 oral cavity, laryngeal: surgery within
but <31 days between RT pharynx and 30 days of RT (+), no
treatments salivary gland) chemo (+), local
tumours (+) and
Charlson of 0 (+). For
nasal cavity or salivary
gland tumour: surgery
within 30 days (+)
Fink et al. Tamoxifen Self-reported no longer Self-reported use Adherence: 83% at 1 year Logistic regression Predictors that were Decision balance scale
[41]a (hormonal taking tamoxifen, during and 79% at 2 years of analysis significant in univariate score (having neutral or
therapy) regardless of reason for telephone treatment analyses were selected negative beliefs about
stopping at 3, 6, 15 and interviews for inclusion as well as the value of tamoxifen
Volume 25 | No. 3 | March 2014
27 months after breast confounders not further (−)) and number of
cancer surgery specified positive nodes (−)
Guth et al. Hormonal Patients were divided into Data were collected Of the 325, 287 initiated Logistic regression Only univariate analysis Location of follow-up (GP
[42]b therapy subgroups: those who from the charts endocrine therapy and analysis was conducted follow-up (−))
did not initiate therapy of follow-up One hundred and
Annals of Oncology
(including those for consultations ninety-one of 287
whom therapy was not during which (66.6%) completed 5-
recommended/ was patients were year therapy. Of the 96
recommended but never asked about the who discontinued
began/refused) and those treatments therapy, 31 were non-
who initiated therapy adherent (10.8%)
Downloaded from https://academic.oup.com/annonc/article-abstract/25/3/564/148605
by guest
on 28 May 2018
Annals of Oncology
Volume 25 | No. 3 | March 2014
(into discontinuation
due to death/breast
recurrence and/or distant
metastasis, serious
medical reasons other
than breast cancer,
therapy adverse effects,
and other reasons)
Guth et al. Hormonal Patients were divided in Data were collected Non-persistence rate 37/400 Descriptive NA Of the 37 who were non-
[43]b therapy subgroups: those who from the charts (9.3%) analysis persistent, 24
did not initiate therapy of follow-up discontinued because of
(including those for consultations side-effects, and 13 for
whom therapy was not during which other reasons including
recommended/ was patients were lack of motivation (5),
recommended but never asked about the lack of faith in therapy
began/refused) and those treatments (2), misinformation by
who initiated therapy physician (2), errors
(including those who regarding length of
completed 5 year therapy (1), insurance
therapy, those who reasons (1), denial of
completed >5 years, and cancer diagnosis (1) and
those who discontinued alcohol dependency/
due to drug-related side- psychiatric illness (2)
effects and those who
discontinued for other
reasons such as death/
recurrence/other serious
medical reasons than
breast cancer)
Guth in press Hormonal A patient was classified as Data were collected In the 80+ group, 87% were Descriptive NA Of those in the 80+ non-
et al. [44]b therapy compliant when she from the charts compliant and in the 60– analysis persistent, 13% were
started with the of follow-up 79 group 95.5% were non- persistent due to
treatment. consultations compliant. In the group side-effects and 4% for
A patient was classified during which 80+, 83% were other reasons (2 lack of
as persistent when they patients were persistence and in the motivation). Of those
took their medication for asked about the group 60–79 88% were aged 60–79, 7% were
at least 36 months treatments persistent. non-persistent due to
side-effects and 5% due
doi:10.1093/annonc/mdt433 |
to other reasons (nine
lack of motivation
/resistance, one
misinformation by
physician, and two
reviews
alcohol dependency/
psychiatric disease. In
the older group,
medications were more
often discontinued by
Continued
Downloaded from https://academic.oup.com/annonc/article-abstract/25/3/564/148605
by guest
on 28 May 2018
Table 1. Continued
reviews
| Puts et al.
Author, Which cancer Definition of non- Measurement of Adherence /persistence rate Statistical analysis Which variables were Factors associated with Factors associated with
publication treatments were adherence used or non-adherence/ used to examine included in the statistical non-adherence (−) or non-persistence (−) or
date included in the adherence/non-persistence non-persistence factors associated analysis? higher adherence (+) higher persistence (+)
(reference) study? used or persistence with non-
adherence /non-
persistence
the physician for serious
side-effects
Hoskin et al. Radiation No definition provided Not described Non-adherence rate is 17/ Descriptive NA Seventeen patients were
[45] therapy 322 analysis non-adherent: three
refused to wear the mask
needed for the
treatment, one was
hospitalized for reasons
not related to treatment,
one was hospitalized for
adverse effects of
treatment and for ten no
reason was defined
Kimmick et al. Hormonal Prescription rate: at least Using prescription Rate of prescription fill was Logistic regression Age, race, comorbidity, Marital status (non- Marital status (non-married
[46] therapy one pharmacy filled fill and refill 64% and 70% for those analysis number of prescription married (+). +), Charlson
prescription for a data with hormone receptor- medications, stage, comorbidity index of 3
hormonal therapy agent positive tumours. The hormone receptor compared with 0 (+),
within 1 year of mean MPR was 0.75. status, type of surgery, having a regional stage
diagnosis. Adherence rate: 60% had adjuvant chemo compared with local
Adherence: a Medication a MPR of >80% during received, RT received, stage (+).
Possession Ratio (MPR) the first year after the urban or rural residence,
>80%. MPR is defined as initial prescription. The type of hospital. A
the total days covered by persistence rate was 80% separate model for
the medication/total days adherence and
needing the medication. persistence was
Non-persistence = a gap calculated
of ≥90 days between
medication refills
Lash et al. Tamoxifen Self-reported Self-reported use After 5 years, 100 women Cox proportional Age, sex, estrogen receptor More prescription
[47]a (hormonal discontinuation of of tamoxifen (31%) had stopped hazard (ER) status, presence of medications at baseline
therapy) tamoxifen, regardless of during taking Tamoxifen, 16 of regression tamoxifen side-effects, (−), new medication
Volume 25 | No. 3 | March 2014
reason for stopping at 3, telephone those had restarted in analysis and number of during follow-up (−).
6, 15, 27, 29, 51 and 63 interviews the 5 year period prescription drugs Severe side-effects at
months after breast baseline and during
cancer surgery follow-up (−). Positive
views of tamoxifen (+)
Annals of Oncology
Lau et al. [48] Chemotherapy No definition was provided Not reported Twenty-five of 36 (69.4%) Not reported, NA For two patients who
and surgery were adherent seems received only one cycle
descriptive the reasons are lack of
analysis only immediate treatment
effect, for nine patients
who had completed
chemo but refused the
Downloaded from https://academic.oup.com/annonc/article-abstract/25/3/564/148605
by guest
on 28 May 2018
Annals of Oncology
Volume 25 | No. 3 | March 2014
surgery they had a
misconception that after
chemo and they had
been told their tumour
had shrunk, because
they were no longer in
pain they could wait and
perhaps avoid the
surgery altogether.
Neugut et al. Aromatase Non-persistence: a supply Using prescription Of those aged ≥65 , 24.7% Logistic regression All study variables (out of A co-payment of $30–89.99 A co-payment of $30–89.99
[49] inhibitors gap of minimum 45 days refill data were non-persistent and analysis pocket costs, number of and $90 and more (−) and $90 and more (−).
(hormonal and with no subsequent 8.9% were non-adherent other prescriptions, type Age 84 and over (−),
therapy) refills before the end of over the 2-year study of specialist, age, race, prescription of AI
the study period. Non- period marital status, income, written by primary care
adherence: a Medication region of United States, specialist or different
Possession Ratio of less and comorbidities) were specialist (−), and
80% included. Two models increased number of
were calculated: one for prescriptions (−)
adherence and one for
persistence
Owusu et al. Tamoxifen Tamoxifen discontinuation Prescription refill Forty-nine percent Cox proportional All variables that were Aged 75–80 or aged ≥80
[50] (hormonal was operationalized as data discontinued Tamoxifen hazard significant predictors of compared to those <70
therapy) ever discontinuing before the 5 year regression tamoxifen years, ER indeterminate
tamoxifen for >60 days completion analysis discontinuation at status vs. ER+ (−),
during the initial 5-year P < 0.10 were included having received a breast-
tamoxifen prescription in model which conserving surgery
included age at without radiation (−)
diagnosis, race, lymph
node involvement,
estrogen and
progesterone receptor
status, and primary
therapy received
Partridge et al. Chemotherapy/ Non-persistence: coming off MEMS Eighty-three of patients Logistic regression Age, ethnicity, Node-negative disease (−), The 26 (17%) who did not
[51]c molecular- therapy without were persistent. Average analysis performance status, received mastectomy (−) complete the protocol:
targeted completing the protocol adherence across all tumour size, hormone 17 had toxicity/adverse
therapy specified treatment. cycles was 78% receptor status effects or complications,
doi:10.1093/annonc/mdt433 |
Non-adherence, if fewer 5 withdrew from the
than 80% of doses study and 2 had disease
expected were recorded progression/ relapse and
by the MEMS. A missed 2 died
dose of capecitabine was
reviews
defined as no redosing
within 20 h of the
previous dose, when
another dose was
planned as per protocol.
A dosing violation was
Continued
Downloaded from https://academic.oup.com/annonc/article-abstract/25/3/564/148605
by guest
on 28 May 2018
Table 1. Continued
reviews
| Puts et al.
Author, Which cancer Definition of non- Measurement of Adherence /persistence rate Statistical analysis Which variables were Factors associated with Factors associated with
publication treatments were adherence used or non-adherence/ used to examine included in the statistical non-adherence (−) or non-persistence (−) or
date included in the adherence/non-persistence non-persistence factors associated analysis? higher adherence (+) higher persistence (+)
(reference) study? used or persistence with non-
adherence /non-
persistence
defined as taking a dose
<8 h or >16 h but <20 h
from the previous dose.
Partridge et al. Tamoxifen Adherence: the proportion Prescription refill The overall adherence rate Logistic regression All variables were included Age 85 and older (−), non-
[52] (hormonal of eligible days during data during the first year was analysis in multivariable model White race (−), having
therapy) the 365 days following 87%. Seventy-seven which included age, had a mastectomy (−),
the first tamoxifen percent had filled race, surgery, visit to having seen a seen a
prescription. Patients prescriptions to cover oncologist in past year, medical oncologist
with ≥80% days covered ≥80% of the year and Charlson Comorbidity before starting
is adherent. were classified as Score, other prescription tamoxifen (+),
adherent drug use, number of increasing Charlson
outpatient services use scores (+).
and days hospitalized in
the first year
Regnier Chemotherapy/ Patient reported non-use of Focus group and Rate is NR, the majority of NA NA Patients reported that a
Denois molecular- treatment individual patients indicated that change in their daily
et al. [53] targeted interviews they never had forgotten routine (such as outing
therapy their treatment in town, visiting friends
or going on holiday) was
associated with
forgetting their
medication (−), side-
effects (−), not
understanding the
prescription (−). Timing
of dosages was adjusted
for convenience reasons
Ruddy et al. chemotherapy/ Persistence with CMF: Self-report using Sixty-five percent were Logistic regression The significant univariate Non-adherence was not Node negativity (−) and
[54]c molecular being prescribed six medication persistent with CMF. analysis variables were entered in modelled due to the hormone receptor
targeted cycles of at least one of calendars and Adherence with a stepwise forward small number of patients positive tumours (−),
Volume 25 | No. 3 | March 2014
therapy the three CMF drugs. case-report cyclophosphamide was model predicting who were classified as fatigue (−)and febrile
Adherence to oral forms filled out 95% persistence which non-adherent neutropenia (−)
cyclophosphamide was by study included only node
calculated using the investigators status and hormone
number of doses taken receptor status. A
Annals of Oncology
according to the separate model was
medication calendars constructed to examine
divided by the number of which grade 3 and 4
doses prescribed. side-effects were
Non-adherent was <80% associated with
of expected doses (11 or persistence, the final
model included fatigue,
Downloaded from https://academic.oup.com/annonc/article-abstract/25/3/564/148605
by guest
on 28 May 2018
Annals of Oncology
Volume 25 | No. 3 | March 2014
fewer of the 14 doses per vomiting and febrile
cycle) neutropenia
Shaheen et al. Luteinizing Non-compliance: missing 1 Data collected Fifty-six perecnt were Descriptive NA Reasons for missing
[55] hormone- or more injections. from chart adherent, and 24% had a analysis appointments were
releasing Delay: more than 2 delay for one or more patients were confused
hormone weeks after the scheduled injections about the treatment,
agonist time for the injection long waiting times in
(LHRH) clinics, having to travel a
long distance to the
clinic, clinic was closed
due to holidays, and
pain and bleeding at
injection site
Winterhalder Chemotherapy/ Adherence: fully adherent Self-reported Ninety-one percent were Not reported Not reported. The reasons for making
et al. [56] molecular- to recommended dosage intake of fully adherent. The mistakes included
targeted and intake interval for capecitabine adherence rate among forgetting treatment
therapy the duration of treatment using diaries those with no adverse (n = 9), side-effects
which were effects was 95%, and for (n = 4), and
completed daily those with three or more misunderstanding
side-effects the instructions (n = 3)
adherence was 66.7%) There was a trend that
those with less adverse
events were more
adherent (only P = 0.07
provided)
Ziller et al. Tamoxifen and A patient was adherent Self-reported Self-reported adherence Logistic regression Only univariate models There was no significant
[57] anastrazole when self-reported and if adherence 100%, MPR adherence analysis were calculated. Factors predictor for adherence
(hormonal an MPR of ≥80% was measured using 80% for tamoxifen and examined included age, to tamoxifen or
therapy) achieved a questionnaire 69% for anastrazole job training, family risk, anastrazole.
(questions not using prescription having children,
specified). information from charts tolerability to treatment,
Prescription medication interruption,
checks were side-effects and quality
doi:10.1093/annonc/mdt433 |
done using the of life
charts.
a
These two publications used data from the same prospective observational cohort study.
b
In these three publications part of the study sample selected from the clinical database is overlapping.
reviews
c
These two publications used data from the same companion study of a randomized clinical trial.
RT, radiation therapy; MEMS, microelectronic monitoring system; NA, not applicable; NR, not reported; CMF, cyclophosphamide methotrexate 5-fluorouracil.
Downloaded from https://academic.oup.com/annonc/article-abstract/25/3/564/148605
by guest
on 28 May 2018
reviews Annals of Oncology
women with early-stage breast cancer was examined, and two of 5. Mazzeo F, Duck L, Joosens E et al. Nonadherence to imatinib treatment in patients
these studies used administrative databases [46, 52]. Further re- with gastrointestinal stromal tumors: the ADAGIO study. Anticancer Res 2011; 31
(4): 1407–1409.
search is needed to examine how comorbidities and treatments
6. Hershman DL, Shao T, Kushi LH et al. Early discontinuation and non-adherence to
for other chronic conditions affect adherence to active cancer
adjuvant hormonal therapy are associated with increased mortality in women with
treatment particularly for older adults with other cancers breast cancer. Breast Cancer Res Treat 2011; 126(2): 529–537.
beyond early-stage breast cancer, and with other treatments 7. McCowan C, Shearer J, Donnan PT et al. Cohort study examining tamoxifen
than hormonal treatment in the adjuvant settings. adherence and its relationship to mortality in women with breast cancer. Br J
Although there have been previous reviews on adherence to Cancer 2008; 99(11): 1763–1768.
some cancer treatments [18, 25–32], these have not focused on 8. Srokowski TP, Fang S, Duan Z et al. Completion of adjuvant radiation therapy
all forms of active cancer treatment adherence in the older among women with breast cancer. Cancer 2008; 113: 22–29.
population. Strengths of this review include the systematic 9. Ibrahim AR, Eliasson L, Apperley JF et al. Poor adherence is the main reason for
methodology used to identify all relevant articles using two in- loss of CCyR and imatinib failure for chronic myeloid leukemia patients on long-
term therapy. Blood 2011; 117(14): 3733–3736.
dependent reviewers, inclusion of multiple databases and four
10. Allemani C, Storm H, Voogd AC et al. Variation in ‘standard care’ for breast cancer
languages, and not excluding studies based on the quality assess- across Europe: A EUROCARE-3 high resolution study. Eur J Cancer 2010; 46:
ment criteria. This review also has several limitations. Of great- 1528–1536.
est importance is that the findings are limited by the scientific 11. Darkow T, Henk HJ, Thomas SK et al. Treatment interruptions and non-adherence
quality of the studies included. Additionally, we were unable to with imatinib and associated healthcare costs: a retrospective analysis among
conduct a meta-analysis due to the heterogeneity of the studies managed care patients with chronic myelogenous leukaemia. Pharmacoeconomics
included with regard to assessment methods used, study popu- 2007; 25: 481–496.
lations and outcomes. 12. Marin D, Bazeos A, Mahon FX et al. Adherence is the critical factor for
achieving molecular responses in patients with chronic myeloid leukemia who
In conclusion, non-adherence in older adults with cancer
achieve complete cytogenetic responses on imatinib. J Clin Oncol 2010; 28:
was common yet little is known about factors influencing 2381–2388.
non-adherence in this population, especially for cancer treat- 13. The Chief Public Health Officer. The Chief Public Health Officer’s annual report on
ments than other hormonal therapy and among older men with the state of Public Health in Canada 2010: growing older-adding life to years. The
cancer. Further studies exploring how older adults manage their Chief Public Health officer. Ottawa, Canada: Public Health Canada 2010.
cancer treatments are needed, including other forms of cancer 14. Canadian Institute for Health Information. Drug use among seniors on public drug
treatment such as radiation therapy, chemotherapy and molecu- programs in Canada 2002 to 2008. Ottawa, ON: CIHI. 1-7-2012 2010.
lar-targeted therapy. Cancer treatment risks and benefits are not 15. Mangin D, Heath I, Jamoulle M. Beyond diagnosis: rising to the multimorbidity
the same for the older and younger population [68–74] and this challenge. BMJ 2012; 344: e3526.
can affect adherence and persistence in older adults with cancer. 16. Salisbury C. Multimorbidity: redesigning health care for people who use it. Lancet
2012; 380: 7–9.
With the expected increase of the older adult population around
17. Ritchie CS, Kvale E, Fisch MJ. Multimorbidity: an issue of growing importance for
the world, and with the preference of both providers and oncologists. J Oncol Pract 2011; 7: 371–374.
patients for oral agents [26], it is important to understand how 18. Banning M. Adherence to adjuvant therapy in post-menopausal breast cancer
older adults manage their treatments at home as well as how patients: a review. Eur J Cancer Care 2012; 21(1): 10–19.
cancer treatment adherence is influenced by the treatments for 19. Banning M. Older people and adherence with medication: a review of the literature.
other chronic conditions and age-related changes in functioning Int J Nurs Stud 2008; 45: 1550–1561.
for the older population. 20. Hughes CM. Medication non-adherence in the elderly: how big is the problem?
Drugs Aging 2004; 21: 793–811.
21. Schuz B, Marx C, Wurm S et al. Medication beliefs predict medication adherence
funding in older adults with multiple illnesses. J Psychosom Res 2011; 70: 179–187.
This work was supported by a University of Toronto Connaught 22. Pound P, Britten N, Morgan M et al. Resisting medicines: a synthesis of qualitative
studies of medicine taking. Soc Sci Med 2005; 61: 133–155.
New Researcher Award awarded to Dr M. Puts.
23. Mishra SI, Gioia D, Childress S et al. Adherence to medication regimens among
low-income patients with multiple comorbid chronic conditions. Health Soc Work
disclosure 2011; 36: 249–258.
24. Schlenk EA, Dunbar-Jacob J, Engberg S. Medication non-adherence among older
The authors have declared no conflict of interest. adults: a review of strategies and interventions for improvement. J Gerontol Nurs
2004; 30: 33–43.
25. Verbrugghe M, Verhaeghe S, Lauwaert K et al. Determinants and associated
references factors influencing medication adherence and persistence to oral anticancer drugs:
A systematic review. Cancer Treat Rev 2013; 39: 610–621.
1. Canadian Cancer Society’s Steering Committee on Cancer statistics. Canadian
26. Given BA, Spoelstra SL, Grant M. The challenges of oral agents as antineoplastic
Cancer Statistics 2013. Canadian Cancer Society. Toronto, Canada: Canadian
treatments. Semin Oncol Nurs 2011; 27: 93–103.
Cancer Society 2013.
27. Spoelstra SL, Given CW. Assessment and measurement of adherence to oral
2. Smith BD, Smith GL, Hurria A et al. Future of cancer incidence in the United
antineoplastic agents. Semin Oncol Nurs 2011; 27: 116–132.
States: burdens upon an aging, changing nation. J Clin Oncol 2009; 27:
2758–2765. 28. Ruddy K, Mayer E, Partridge A. Patient adherence and persistence with oral
anticancer treatment. CA Cancer J Clin 2009; 59: 56–66.
3. Sabata E; on behalf of the WHO. Adherence to long-term therapies: Evidence for
action. Geneva: World Health Organization 2003. 29. Foulon V, Schoffski P, Wolter P. Patient adherence to oral anticancer drugs: an
emerging issue in modern oncology. Acta Clin Belg 2011; 66: 85–96.
4. Ganesan P, Sagar TG, Dubashi B et al. Nonadherence to imatinib adversely affects
event free survival in chronic phase chronic myeloid leukemia. Am J Hematol 30. Barton D. Oral agents in cancer treatment: the context for adherence. Semin Oncol
2011; 86(6): 471–474. Nurs 2011; 27: 104–115.
| Puts et al. Volume 25 | No. 3 | March 2014
Downloaded from https://academic.oup.com/annonc/article-abstract/25/3/564/148605
by guest
on 28 May 2018
Annals of Oncology reviews
31. Palmieri FM, Barton DL. Challenges of oral medications in patients with advanced 53. Regnier DV, Poirson J, Nourissat A et al. Adherence with oral chemotherapy:
breast cancer. Semin Oncol Nurs 2007; 23: S17–S22. results from a qualitative study of the behaviour and representations of patients
32. Hohneker J, Shah-Mehta S, Brandt PS. Perspectives on adherence and and oncologists. Eur J Cancer Care 2011; 20(4): 520–527.
persistence with oral medications for cancer treatment. J Oncol Pract 2011; 7: 54. Ruddy KJ, Pitcher BN, Archer LE et al. Persistence, adherence, and toxicity with
65–67. oral CMF in older women with early-stage breast cancer (Adherence Companion
33. Moher D, Liberati A, Tetzlaff J et al. Preferred reporting items for systematic Study 60104 for CALGB 49907). Ann Oncol 2012; 23(12): 3075–3081.
reviews and meta-analyses: the PRISMA statement. Int J Surg 2010; 8: 336–341. 55. Shaheen JA, Amin M, Harty JI. Patient compliance in treatment of prostate cancer
34. Cramer JA, Roy A, Burrell A et al. Medication compliance and persistence: with luteinizing hormone-releasing hormone (LHRH) agonist. Urology 1993; 42(5):
terminology and definitions. Value Health 2008; 11: 44–47. 533–535.
35. Pace R, Pluye P, Bartlett G et al. Testing the reliability and efficiency of the pilot 56. Winterhalder R, Hoesli P, Delmore G et al. Self-reported compliance with
Mixed Methods Appraisal Tool (MMAT) for systematic mixed studies review. Int J capecitabine: findings from a prospective cohort analysis. Oncology 2011; 80(1–2):
Nurs Stud 2012; 49: 47–53. 29–33.
36. Barcenas CH, Zhang N, Zhao H et al. Anthracycline regimen adherence in older 57. Ziller V, Kalder M, Albert U-S et al. Adherence to adjuvant endocrine therapy in
patients with early breast cancer. Oncologist 2012; 17: 303–311. postmenopausal women with breast cancer. Ann Oncol 2009; 20(3): 431–436.
37. Barron TI, Connolly RM, Bennett K et al. Early discontinuation of tamoxifen—A 58. Townsley C, Pond GR, Peloza B et al. Analysis of treatment practices for elderly
lesson for oncologists. Cancer 2007; 109: 832–839. cancer patients in Ontario, Canada. J Clin Oncol 2005; 23: 3802–3810.
38. Demissie S, Silliman RA, Lash TL. Adjuvant tamoxifen: predictors of use, side 59. Persons in low-income after tax 2006–2010. Ottawa, Canada: Statistics Canada.
effects, and discontinuation in older women. J Clin Oncol 2001; 19: 322–328. 2013.
39. Dobie SA, Baldwin LM, Dominitz JA et al. Completion of therapy by 60. Longo CJ, Deber R, Fitch M et al. An examination of cancer patients’ monthly
Medicare patients with stage III colon cancer. J Natl Cancer Inst 2006; 98(9): ‘out-of-pocket’ costs in Ontario, Canada. Eur J Cancer Care (Engl) 2007; 16:
610–619. 500–507.
40. Fesinmeyer MD, Mehta V, Tock L et al. Completion of radiotherapy for local and 61. Longo CJ, Fitch M, Deber RB et al. Financial and family burden associated with
regional head and neck cancer in medicare. Arch Otolaryngol Head Neck Surg cancer treatment in Ontario, Canada. Support Care Cancer 2006; 14:
2009; 135: 860–867. 1077–1085.
41. Fink AK, Gurwitz J, Rakowski W et al. Patient beliefs and tamoxifen discontinuance 62. Retornaz F, Monette J, Batist G et al. Usefulness of frailty markers in the
in older women with estrogen receptor–positive breast cancer. J Clin Oncol 2004; assessment of the health and functional status of older cancer patients referred for
22(16): 3309–3315. chemotherapy: a pilot study. J Gerontol A Biol Sci Med Sci 2008; 63: 518–522.
42. Guth U, Huang DJ, Schotzau A et al. Target and reality of adjuvant endocrine 63. Puts MT, Monette J, Girre V et al. Are frailty markers useful for predicting
therapy in postmenopausal patients with invasive breast cancer. Br J Cancer treatment toxicity and mortality in older newly diagnosed cancer patients? Results
2008; 99(3): 428–433. from a prospective pilot study. Crit Rev Oncol Hematol 2011; 78: 138–149.
43. Guth U, Myrick ME, Schotzau A et al. Drug switch because of treatment-related 64. Amalraj S, Starkweather C, Nguyen C et al. Health literacy, communication, and
adverse side effects in endocrine adjuvant breast cancer therapy: How often and treatment decision-making in older cancer patients. Oncology (Williston Park)
how often does it work? Breast Cancer Res Treat 2011; 129(3): 799–807. 2009; 23: 369–375.
44. Guth U, Myrick ME, Kandler C et al. The use of adjuvant endocrine breast cancer 65. McCarthy DM, Waite KR, Curtis LM et al. What did the doctor say? Health literacy
therapy in the oldest old. Breast 2013; 22(5): 863–868. and recall of medical instructions. Med Care 2012; 50: 277–282.
45. Hoskin PJ, Rojas AM, Saunders MI et al. Carbogen and nicotinamide in locally 66. Zamora H, Clingerman EM. Health literacy among older adults: a systematic
advanced bladder cancer: early results of a phase-III randomized trial. Radiother literature review. J Gerontol Nurs 2011; 37: 41–51.
Oncol 2009; 91(1): 120–125. 67. Ngoh LN. Health literacy: a barrier to pharmacist-patient communication and
46. Kimmick G, Anderson R, Camacho F et al. Adjuvant hormonal therapy use among medication adherence. J Am Pharm Assoc 2009; 49: e132–e146.
insured, low-income women with breast cancer. J Clin Oncol 2009; 27(21): 68. Papamichael D, Audisio R, Horiot JC et al. Treatment of the elderly colorectal
3445–3451. cancer patient: SIOG expert recommendations. Ann Oncol 2009; 20: 5–16.
47. Lash TL, Fox MP, Westrup JL et al. Adherence to tamoxifen over the five-year 69. Biganzoli L, Wildiers H, Oakman C et al. Management of elderly patients with
course. Breast Cancer Res Treat 2006;99(2): 215–220. breast cancer: updated recommendations of the International Society of Geriatric
48. Lau FW, Choi KT, Wei WI et al. Induction chemotherapy for oral cancers in a non- Oncology (SIOG) and European Society of Breast Cancer Specialists (EUSOMA).
compliant patient population. Asian J Surg 1994; 17(3): 277–282. Lancet Oncol 2012; 13(4): e148–e160.
49. Neugut AI, Subar M, Wilde ET et al. Association between prescription co-payment 70. Aapro M, Bernard-Marty C, Brain EG et al. Anthracycline cardiotoxicity in the
amount and compliance with adjuvant hormonal therapy in women with early- elderly cancer patient: a SIOG expert position paper. Ann Oncol 2011; 22:
stage breast cancer. J Clin Oncol 2011; 29(18): 2534–2542. 257–267.
50. Owusu C, Buist DS, Field TS et al. Predictors of tamoxifen discontinuation among 71. Droz J-P, Balducci L, Bolla M et al. Background for the proposal of SIOG guidelines
older women with estrogen receptor-positive breast cancer. J Clin Oncol 2008; 26 for the management of prostate cancer in senior adults. Critical Rev Oncol/
(4): 549–555. Hematol 2010; 73(1): 68–91.
51. Partridge AH, Archer L, Kornblith AB et al. Adherence and persistence with oral 72. Hurria A, Browner IS, Cohen HJ et al. Senior adult oncology: Clinical practice
adjuvant chemotherapy in older women with early-stage breast cancer in CALGB guidelines in oncology. JNCCN 2012; 10(2): 162–209.
49907: adherence companion study 60104. J Clin Oncol 2010; 28(14): 73. Balducci L. Pharmacology of antineoplastic medications in older cancer patients.
2418–2422. Oncology (Williston Park) 2009; 23: 78–85.
52. Partridge AH, Wang PS, Winer EP et al. Nonadherence to adjuvant tamoxifen therapy 74. Extermann M. Geriatric oncology: an overview of progresses and challenges.
in women with primary breast cancer. J Clin Oncol 2003; 21(4): 602–606. Cancer Res Treat 2010; 42: 61–68.
Volume 25 | No. 3 | March 2014 doi:10.1093/annonc/mdt433 |
Downloaded from https://academic.oup.com/annonc/article-abstract/25/3/564/148605
by guest
on 28 May 2018
You might also like
- CR - RamirezDocument4 pagesCR - RamirezTommysNo ratings yet
- The Role of Obesity and Related Metabolic Disturbances in Cancers ofDocument18 pagesThe Role of Obesity and Related Metabolic Disturbances in Cancers ofTommysNo ratings yet
- Lalkhen 2011Document5 pagesLalkhen 2011TommysNo ratings yet
- Ehlinger (2010)Document6 pagesEhlinger (2010)TommysNo ratings yet
- Branski (2011)Document7 pagesBranski (2011)TommysNo ratings yet
- AJCC Breast Cancer Staging SystemDocument50 pagesAJCC Breast Cancer Staging SystemLucan MihaelaNo ratings yet
- Surgical Management of Intracerebral HemorrhageDocument10 pagesSurgical Management of Intracerebral HemorrhageTommysNo ratings yet
- Chronic Inflammation Causes, Features and EffectsDocument24 pagesChronic Inflammation Causes, Features and EffectsTommys100% (1)
- WCSQ Full PaperDocument15 pagesWCSQ Full PaperTommysNo ratings yet
- Service Evaluation, Audit and Research: What Is The Difference?Document2 pagesService Evaluation, Audit and Research: What Is The Difference?TommysNo ratings yet
- Andrew (2015)Document13 pagesAndrew (2015)TommysNo ratings yet
- Mun (2001)Document10 pagesMun (2001)TommysNo ratings yet
- Atresia EsofagusDocument7 pagesAtresia EsofagusTommysNo ratings yet
- Appleton (2006)Document6 pagesAppleton (2006)TommysNo ratings yet
- Periprosthetic Fractures in Total Knee ArthroplastyDocument6 pagesPeriprosthetic Fractures in Total Knee ArthroplastyTommysNo ratings yet
- Skin Flap Dr. BrotoDocument17 pagesSkin Flap Dr. BrotoTommysNo ratings yet
- Festing 2002Document15 pagesFesting 2002TommysNo ratings yet
- CaffeineDocument9 pagesCaffeineTommysNo ratings yet
- Surviving Sepsis Campaign: International Guidelines For Management of Severe Sepsis and Septic Shock: 2016Document56 pagesSurviving Sepsis Campaign: International Guidelines For Management of Severe Sepsis and Septic Shock: 2016TommysNo ratings yet
- Ni Hms 79693Document17 pagesNi Hms 79693TommysNo ratings yet
- Yuwono (2014) - Coffee PowderDocument5 pagesYuwono (2014) - Coffee PowderTommysNo ratings yet
- Fredholm1982 Chronic Caffeine in RatsDocument4 pagesFredholm1982 Chronic Caffeine in RatsTommysNo ratings yet
- Branski (2011)Document7 pagesBranski (2011)TommysNo ratings yet
- Jurnal Trauma KepalaDocument7 pagesJurnal Trauma KepalaTommysNo ratings yet
- DDDT 8 1923 PDFDocument6 pagesDDDT 8 1923 PDFTommysNo ratings yet
- Green Hal GHDocument12 pagesGreen Hal GHTommysNo ratings yet
- Yuwono (2017) - Coffee ReviewDocument3 pagesYuwono (2017) - Coffee ReviewTommysNo ratings yet
- Coffee StatisticsDocument5 pagesCoffee StatisticsTommysNo ratings yet
- Emergency Management of Severe Burns Manual: February 2012Document3 pagesEmergency Management of Severe Burns Manual: February 2012TommysNo ratings yet
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeFrom EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeRating: 4 out of 5 stars4/5 (5784)
- The Little Book of Hygge: Danish Secrets to Happy LivingFrom EverandThe Little Book of Hygge: Danish Secrets to Happy LivingRating: 3.5 out of 5 stars3.5/5 (399)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceFrom EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceRating: 4 out of 5 stars4/5 (890)
- Shoe Dog: A Memoir by the Creator of NikeFrom EverandShoe Dog: A Memoir by the Creator of NikeRating: 4.5 out of 5 stars4.5/5 (537)
- Grit: The Power of Passion and PerseveranceFrom EverandGrit: The Power of Passion and PerseveranceRating: 4 out of 5 stars4/5 (587)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureFrom EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureRating: 4.5 out of 5 stars4.5/5 (474)
- The Yellow House: A Memoir (2019 National Book Award Winner)From EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Rating: 4 out of 5 stars4/5 (98)
- Team of Rivals: The Political Genius of Abraham LincolnFrom EverandTeam of Rivals: The Political Genius of Abraham LincolnRating: 4.5 out of 5 stars4.5/5 (234)
- Never Split the Difference: Negotiating As If Your Life Depended On ItFrom EverandNever Split the Difference: Negotiating As If Your Life Depended On ItRating: 4.5 out of 5 stars4.5/5 (838)
- The Emperor of All Maladies: A Biography of CancerFrom EverandThe Emperor of All Maladies: A Biography of CancerRating: 4.5 out of 5 stars4.5/5 (271)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryFrom EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryRating: 3.5 out of 5 stars3.5/5 (231)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaFrom EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaRating: 4.5 out of 5 stars4.5/5 (265)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersFrom EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersRating: 4.5 out of 5 stars4.5/5 (344)
- On Fire: The (Burning) Case for a Green New DealFrom EverandOn Fire: The (Burning) Case for a Green New DealRating: 4 out of 5 stars4/5 (72)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyFrom EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyRating: 3.5 out of 5 stars3.5/5 (2219)
- The Unwinding: An Inner History of the New AmericaFrom EverandThe Unwinding: An Inner History of the New AmericaRating: 4 out of 5 stars4/5 (45)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreFrom EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreRating: 4 out of 5 stars4/5 (1090)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)From EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Rating: 4.5 out of 5 stars4.5/5 (119)
- Her Body and Other Parties: StoriesFrom EverandHer Body and Other Parties: StoriesRating: 4 out of 5 stars4/5 (821)
- Shear Stress ProblemsDocument5 pagesShear Stress ProblemsNoven VillaberNo ratings yet
- Huntersvsfarmers 131204084857 Phpapp01Document1 pageHuntersvsfarmers 131204084857 Phpapp01Charles BronsonNo ratings yet
- Why The Bollard Pull Calculation Method For A Barge Won't Work For A Ship - TheNavalArchDocument17 pagesWhy The Bollard Pull Calculation Method For A Barge Won't Work For A Ship - TheNavalArchFederico BabichNo ratings yet
- SG LO2 Apply Fertilizer (GoldTown)Document2 pagesSG LO2 Apply Fertilizer (GoldTown)Mayiendlesslove WhiteNo ratings yet
- Why Delegate Authority and Empower EmployeesDocument5 pagesWhy Delegate Authority and Empower EmployeesHarold MaribojocNo ratings yet
- Concepts in Enterprise Resource Planning: Chapter Six Human Resources Processes With ERPDocument39 pagesConcepts in Enterprise Resource Planning: Chapter Six Human Resources Processes With ERPasadnawazNo ratings yet
- Speech ExamplesDocument6 pagesSpeech Examplesjayz_mateo9762100% (1)
- Material SelectionDocument99 pagesMaterial SelectionRaj Bindas100% (8)
- Self Improvement Books To ReadDocument13 pagesSelf Improvement Books To ReadAnonymous oTtlhP67% (3)
- Cau Truc To HopDocument1,258 pagesCau Truc To Hopkhôi trươngNo ratings yet
- CAT Álogo de Peças de Reposi ÇÃO: Trator 6125JDocument636 pagesCAT Álogo de Peças de Reposi ÇÃO: Trator 6125Jmussi oficinaNo ratings yet
- Cobas B 123 POC System: Instructions For Use, Version 13.0 Software Version 4.17Document354 pagesCobas B 123 POC System: Instructions For Use, Version 13.0 Software Version 4.17zelNo ratings yet
- Banking DictionaryDocument499 pagesBanking DictionaryVanessa Jenkins100% (4)
- QUIZ - FinalsDocument5 pagesQUIZ - FinalsFelsie Jane PenasoNo ratings yet
- Computer Programmer or Software Developer or C++ or Visual BasicDocument6 pagesComputer Programmer or Software Developer or C++ or Visual Basicapi-77734404No ratings yet
- Export Promoting InstitutesDocument21 pagesExport Promoting InstitutesVikaskundu28100% (1)
- Real Estate Merger Motives PDFDocument13 pagesReal Estate Merger Motives PDFadonisghlNo ratings yet
- Bus 102 QuestionsDocument4 pagesBus 102 Questionsali2aliyuNo ratings yet
- Hofa Iq Limiter Manual enDocument8 pagesHofa Iq Limiter Manual enDrixNo ratings yet
- AeroCRS 5.95-Premier AirlinesDocument1 pageAeroCRS 5.95-Premier AirlinesmohamedNo ratings yet
- Marc Sans, Barcelona ActivaDocument17 pagesMarc Sans, Barcelona ActivaPromoting EnterpriseNo ratings yet
- E No Ad Release NotesDocument6 pagesE No Ad Release NotesKostyantinBondarenkoNo ratings yet
- Module 2 - Introduction To A Web-AppDocument17 pagesModule 2 - Introduction To A Web-AppJASPER WESSLYNo ratings yet
- Create Config Files Python ConfigParserDocument8 pagesCreate Config Files Python ConfigParserJames NgugiNo ratings yet
- Uuee 17-2020Document135 pagesUuee 17-2020Tweed3ANo ratings yet
- Philippine Constitutional Commissions Powers and FunctionsDocument36 pagesPhilippine Constitutional Commissions Powers and Functionssharlica1990No ratings yet
- GT2-71D Amplifier Unit Data SheetDocument3 pagesGT2-71D Amplifier Unit Data SheetKenan HebibovicNo ratings yet
- Igpu GHZ Cache RM Igpu GHZ CachermDocument2 pagesIgpu GHZ Cache RM Igpu GHZ CachermbuzzbsodNo ratings yet
- App Form BLIDocument8 pagesApp Form BLIPaulo LuizNo ratings yet
- Ty Btech syllabusIT Revision 2015 19 14june17 - withHSMC - 1 PDFDocument85 pagesTy Btech syllabusIT Revision 2015 19 14june17 - withHSMC - 1 PDFMusadiqNo ratings yet