Professional Documents
Culture Documents
The HIV-Infected Adult Patient in The Emergency Department, The Changing Landscape of Disease
Uploaded by
Gavin TexeirraOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
The HIV-Infected Adult Patient in The Emergency Department, The Changing Landscape of Disease
Uploaded by
Gavin TexeirraCopyright:
Available Formats
The HIV-Infected Adult Patient In February 2016
Volume 18, Number 2
The Emergency Department: The Authors
David L. Gutteridge, MD, MPH
Changing Landscape Of Disease
Department of Emergency Medicine, Icahn School of Medicine at Mount
Sinai, New York, NY
Daniel J. Egan, MD
Associate Professor, Department of Emergency Medicine, Program
Abstract Director, Emergency Medicine Residency, Mount Sinai St. Luke’s
Roosevelt, New York, NY
The care of the HIV-infected patient in the emergency department Peer Reviewers
has changed since the development of highly active antiretroviral Andy Jagoda, MD, FACEP
therapy. This therapy has resulted in longer life expectancies and Professor and Chair, Department of Emergency Medicine, Icahn School
of Medicine at Mount Sinai, New York, NY; Medical Director, Mount Sinai
increased quality of life for HIV-infected patients, and in cases of Hospital, New York, NY
treatment compliance and success, virtual elimination of AIDS- Roland C. Merchant, MD, MPH, ScD
associated opportunistic infections. As a result, the emergency cli- Associate Professor, Emergency Medicine and Epidemiology, Brown
University, Rhode Island Hospital, Providence, RI
nician is now more often confronted with adverse events related
CME Objectives
to medication and the diseases associated with aging and chronic
disease. This issue focuses on the differences in evaluation of HIV Upon completion of the article, you should be able to:
1. Describe the pathophysiology of disease processes unique to the
patients on long-term therapy and patients with medication non- initiation of and long-term treatment with antiretroviral drugs.
compliance and low CD4 counts, as well as recognition of life- 2. Recognize common side effects of antiretroviral drugs.
threatening and rare opportunistic infections. Disease processes 3. Risk stratify patients with common presentations based on their HIV
related to the effect of longstanding HIV infection, even with status and whether they are on highly active antiretroviral therapy.
4. Recognize the more common system-based diseases and problems
good control, on many organ systems are addressed. encountered in patients on highly active antiretroviral therapy.
Prior to beginning this activity, see “Physician CME Information”
on the back page.
Editor-In-Chief Daniel J. Egan, MD Eric Legome, MD Robert Schiller, MD Research Editor
Andy Jagoda, MD, FACEP Associate Professor, Department Chief of Emergency Medicine, Chair, Department of Family Medicine,
of Emergency Medicine, Program King’s County Hospital; Professor of Beth Israel Medical Center; Senior Andrea Duca, MD
Professor and Chair, Department of Emergency Medicine Residency,
Emergency Medicine, Icahn School Director, Emergency Medicine Clinical Emergency Medicine, SUNY Faculty, Family Medicine and
Residency, Mount Sinai St. Luke's Downstate College of Medicine, Community Health, Icahn School of Università Vita-Salute San Raffaele
of Medicine at Mount Sinai, Medical of Milan, Italy
Director, Mount Sinai Hospital, New Roosevelt, New York, NY Brooklyn, NY Medicine at Mount Sinai, New York, NY
York, NY Nicholas Genes, MD, PhD Keith A. Marill, MD Scott Silvers, MD, FACEP International Editors
Assistant Professor, Department of Research Faculty, Department of Chair, Department of Emergency
Associate Editor-In-Chief Peter Cameron, MD
Emergency Medicine, Icahn School Emergency Medicine, University Medicine, Mayo Clinic, Jacksonville, FL
Academic Director, The Alfred
Kaushal Shah, MD, FACEP of Medicine at Mount Sinai, New of Pittsburgh Medical Center,
Corey M. Slovis, MD, FACP, FACEP Emergency and Trauma Centre,
Associate Professor, Department of York, NY Pittsburgh, PA
Professor and Chair, Department Monash University, Melbourne,
Emergency Medicine, Icahn School Charles V. Pollack Jr., MA, MD,
Michael A. Gibbs, MD, FACEP of Emergency Medicine, Vanderbilt Australia
of Medicine at Mount Sinai, New FACEP
York, NY Professor and Chair, Department University Medical Center, Nashville, TN
Professor and Chair, Department of Giorgio Carbone, MD
of Emergency Medicine, Carolinas Ron M. Walls, MD Chief, Department of Emergency
Emergency Medicine, Pennsylvania
Editorial Board Medical Center, University of North
Hospital, Perelman School of Professor and Chair, Department of Medicine Ospedale Gradenigo,
Saadia Akhtar, MD Carolina School of Medicine, Chapel Emergency Medicine, Brigham and Torino, Italy
Hill, NC Medicine, University of Pennsylvania,
Associate Professor, Department of Philadelphia, PA Women's Hospital, Harvard Medical
Suzanne Y.G. Peeters, MD
Emergency Medicine, Associate Dean Steven A. Godwin, MD, FACEP School, Boston, MA
Michael S. Radeos, MD, MPH Emergency Medicine Residency
for Graduate Medical Education, Professor and Chair, Department Director, Haga Teaching Hospital,
Program Director, Emergency of Emergency Medicine, Assistant Assistant Professor of Emergency Critical Care Editors The Hague, The Netherlands
Medicine Residency, Mount Sinai Dean, Simulation Education, Medicine, Weill Medical College
of Cornell University, New York; William A. Knight IV, MD, FACEP Hugo Peralta, MD
Beth Israel, New York, NY University of Florida COM-
Research Director, Department of Associate Professor of Emergency Chair of Emergency Services,
Jacksonville, Jacksonville, FL Medicine and Neurosurgery, Medical
William J. Brady, MD Emergency Medicine, New York Hospital Italiano, Buenos Aires,
Professor of Emergency Medicine Gregory L. Henry, MD, FACEP Hospital Queens, Flushing, NY Director, EM Midlevel Provider Argentina
and Medicine, Chair, Medical Clinical Professor, Department of Program, Associate Medical Director,
Emergency Medicine, University Ali S. Raja, MD, MBA, MPH Neuroscience ICU, University of Dhanadol Rojanasarntikul, MD
Emergency Response Committee,
of Michigan Medical School; CEO, Vice-Chair, Emergency Medicine, Cincinnati, Cincinnati, OH Attending Physician, Emergency
Medical Director, Emergency
Medical Practice Risk Assessment, Massachusetts General Hospital, Medicine, King Chulalongkorn
Management, University of Virginia Scott D. Weingart, MD, FCCM
Inc., Ann Arbor, MI Boston, MA Memorial Hospital, Thai Red Cross,
Medical Center, Charlottesville, VA Associate Professor of Emergency
Robert L. Rogers, MD, FACEP, Thailand; Faculty of Medicine,
Calvin A. Brown III, MD John M. Howell, MD, FACEP Medicine, Director, Division of ED Chulalongkorn University, Thailand
Clinical Professor of Emergency FAAEM, FACP Critical Care, Icahn School of Medicine
Director of Physician Compliance, Assistant Professor of Emergency
Credentialing and Urgent Care Medicine, George Washington at Mount Sinai, New York, NY Stephen H. Thomas, MD, MPH
University, Washington, DC; Director Medicine, The University of Professor and Chairman, Emergency
Services, Department of Emergency
Medicine, Brigham and Women's of Academic Affairs, Best Practices, Maryland School of Medicine, Senior Research Editors Medicine, Hamad Medical Corporation
Inc, Inova Fairfax Hospital, Falls Baltimore, MD and Weill Cornell Medical College,
Hospital, Boston, MA James Damilini, PharmD, BCPS
Church, VA Alfred Sacchetti, MD, FACEP Qatar; Emergency Physician-in-Chief,
Clinical Pharmacist, Emergency
Peter DeBlieux, MD Assistant Clinical Professor, Hamad General Hospital, Doha, Qatar
Shkelzen Hoxhaj, MD, MPH, MBA Room, St. Joseph’s Hospital and
Professor of Clinical Medicine, Department of Emergency Medicine,
Chief of Emergency Medicine, Baylor Medical Center, Phoenix, AZ
Interim Public Hospital Director Thomas Jefferson University,
College of Medicine, Houston, TX
of Emergency Medicine Services, Philadelphia, PA Joseph D. Toscano, MD
Louisiana State University Health Chairman, Department of Emergency
Science Center, New Orleans, LA Medicine, San Ramon Regional
Medical Center, San Ramon, CA
Case Presentations dation is a change from prior guidelines, which
recommended therapy only for patients with
You arrive for your ED shift and are presented with 3 lower CD4 counts. The guidelines are also based
HIV-infected patients with various chief complaints. The on evidence that treatment decreases the risk of
first patient is a 28-year-old man with 1 day of right flank transmission, and that patients with undetectable
pain, nausea, vomiting, and hematuria. He had a kidney HIV viral loads are at exceedingly low risk for
stone a year ago with identical pain, and a point-of-care transmitting the virus to others.5
ultrasound shows asymmetric hydronephrosis; however, a In addition to improving life expectancy,
nonenhanced CT scan demonstrates hydronephrosis and HAART has also changed the epidemiology of
hydroureter without a stone. You wonder if the CT elimi- conditions affecting HIV-infected patients. In the
nates an impacted stone or if there is another explanation. beginning of the epidemic, HIV patients generally
The second patient is a 42-year-old HIV-infected presented with infectious complications of their
woman complaining of as many as 3 episodes a day of advanced disease. These included OIs such as Pneu-
diarrhea for the past 3 weeks. She denies pain, melena, mocystis jiroveci pneumonia and Kaposi sarcoma.
rectal bleeding, and fevers. Her laboratory test results are Now, patients more commonly present with compli-
unremarkable. You wonder if additional testing is needed cations unrelated to OIs, including cardiovascular,
and whether sending her home is appropriate. hepatic, and kidney disease, as well as HIV-related
The third patient presents because her family has malignancies and adverse effects from medication.5,6
noticed that she has been acting increasingly “sad.” She The spectrum of presenting complaints is associated
denies any suicidal or homicidal ideation, but does cor- with patient compliance with treatment. OIs are still
roborate that since initiation of an SSRI antidepressant seen in patients with undiagnosed infection present-
drug 6 months ago, she has not noticed any improvement ing with advanced disease and those with financial,
in her mood. In the absence of suicidal ideation, you won- social, or other barriers to medication compliance.
der if she can be sent home. This changing epidemiology of HIV complica-
You are reminded that caring for the HIV-infected tions poses a particular challenge for emergency cli-
patient is not so simple, and you realize quickly that you nicians, who should be familiar with these presenta-
are dealing with 3 very different presentations related to tions as well as the presentation of OIs. This issue of
the same disease and must prioritize where to begin. Emergency Medicine Practice reviews the emergency
complications of long-term HIV infection, especially
noninfectious conditions and complications common
Introduction in the HAART-adherent HIV patient.
The human immunodeficiency virus (HIV) causes a
progressive failure of the immune system, ultimately Selected Abbreviations
leading to acquired immunodeficiency syndrome
(AIDS) in the absence of treatment. Although under AIDS Acquired immunodeficiency syndrome
different nomenclature, AIDS was first described in ARV Antiretroviral
the early 1980s when clusters of patients developed AZT/ZDV Zidovudine
opportunistic infections (OIs) not seen in patients HAART Highly active antiretroviral therapy
with intact immune systems. HIV has spread to every HIV Human immunodeficiency virus
country in the world, creating a global pandemic. In NNRTI Nonnucleoside reverse transcriptase inhibitor
2012, there were 35.3 million people living with HIV NRTI Nucleoside reverse transcriptase inhibitor
worldwide and 2.3 million new diagnoses that year.1 NtRTI Nucleotide reverse transcriptase inhibitor
The development of highly active antiretroviral OI Opportunistic infection
therapy (HAART) in 1996 dramatically increased PEP Postexposure prophylaxis
life expectancy for HIV-infected patients. Due to PI Protease inhibitor
the effectiveness of HAART, by the early 2000s, life
expectancy of HIV-infected patients in developed Critical Appraisal Of The Literature
countries was equivalent to that of comparable per-
sons who were not HIV-infected.2,3 PubMed and the Cochrane Database of System-
Current guidelines from the United States atic Reviews were searched for English-language
Department of Health and Human Services recom- articles related to the management of HIV/AIDS.
mend the treatment of all HIV-infected patients Attention was focused on articles relevant to the
with antiretroviral medications (ARVs).4 These emergency clinician, those published after 1996 (to
current recommendations are based on evidence coincide with the advent of HAART), and on articles
that ARVs reduce the risk of disease progression in that discussed the effects of chronic HIV infection
all patients with CD4 T lymphocyte (CD4) count and HAART adverse events. Search terms included
< 350 cells/mm3, CD4 count 350 to 500 cells/mm3, HIV, AIDS, combination antiretroviral therapy, highly
and CD4 count > 500 cells/mm3. This recommen- active antiretroviral therapy, and immune reconstitution
Copyright © 2016 EB Medicine. All rights reserved. 2 Reprints: www.ebmedicine.net/empissues
inflammatory syndrome. Because of the large num- by several names, including acute seroconversion,
ber of articles retrieved in these searches, the initial primary HIV infection, or acute retroviral syndrome.
focus was on review articles with cross-referencing During the seroconversion syndrome, there may
primary literature cited in the bibliographies. Rel- be an acute drop in CD4 count (leading, rarely, to an
evant guidelines by the World Health Organization, OI), which typically rebounds when the body gains
the United States Department of Health and Human some control over the virus. The diagnosis of acute
Services, and the American College of Emergency seroconversion is challenging, because current rapid
Physicians were also reviewed. HIV antibody testing technology may not detect the
Now, nearly 20 years after the advent of presence of the infection. Fourth-generation tests
HAART, considerable literature exists on the subject that combine detection of the HIV antibody as well
of HIV both in terms of the OIs patients experience as the p24 antigen on the surface of HIV identify in-
and the chronic effects of longstanding illness and fection as early as 2 weeks after exposure. However,
treatment. This literature provides strong evidence with negative rapid testing and with a diagnosis of
to support the practice recommendations made in an acute HIV infection suspected, an HIV viral load
this article. must be obtained. Diagnosis is critical, as patients
with acute infection have extremely high viral loads
Epidemiology And Pathophysiology and are more infectious than those with chronic in-
fection. Additionally, identification of acute infection
In 2012, there were an estimated 1.2 million persons allows for prompt referral to an HIV clinician, allow-
in the United States aged > 12 years infected with ing initiation of ARV therapy. After the acute illness
HIV. This estimate includes approximately 160,000 is over, patients experience a period of chronic (or
persons (14%) who were unaware of their diag- latent) HIV infection without AIDS. AIDS is defined
nosis.7 The high prevalence of undiagnosed HIV by a CD4 count < 200 cells/mm3 or development
underscores the importance of routine HIV testing. of certain OIs or cancers. The average time from
Based on 2009-2010 National Hospital Ambulatory HIV infection to a CD4 count < 200 cells/mm3 is 8
Medical Care Survey data, HIV-infected patients to 10 years. Most individuals remain asymptomatic
accounted for 5 in 1000 emergency department (ED) during this chronic (or latent) phase, although many
visits. Although they had similar acuity to non–HIV- have lymphadenopathy. Considering the high in-
infected patients, they received more diagnostic test- fectivity and then clinical silence, if the diagnosis is
ing, had longer lengths of stay, and were more likely missed, emergency clinicians must maintain a high
to be admitted.8 index of suspicion for this illness in patients present-
In order to become infected with HIV, an indi- ing with typical features and risk factors for HIV
vidual must be exposed to an infected body fluid, exposure in the weeks preceding their evaluation.
typically through either direct inoculation into the Although patients may survive for years with-
bloodstream or via a disrupted mucosal barrier. As a out developing OIs, chronic infection with the virus
medium, blood carries the highest risk of infection; in the absence of HAART is not without detrimen-
however, exposure to other fluids such as semen, tal effects on the body. Infection causes a chronic
vaginal secretions, breast milk, and cerebrospinal inflammatory state, which may predispose patients
fluid also carry risk. Risk of infection is determined to numerous conditions, including coronary artery
by 2 key factors: the viral load of the source patient disease, venous thromboembolism, and chronic
and the method of exposure. Several days after obstructive pulmonary disease. Once patients begin
infection, the virus moves beyond the local site of in- treatment with HAART, measurable inflamma-
fection into the bloodstream with rapid replication. tory markers decrease, as does the risk for adverse
Approximately 75% to 90% of patients experience sequelae from the HIV infection itself. However, pa-
an acute illness during this time. Patients develop tients taking HAART are at risk for adverse medica-
a fever, with additional symptoms typical of many tion effects as well as regular age-related conditions
viral syndromes including lymphadenopathy, sore that have become more prevalent as HIV-infected
throat, and gastrointestinal symptoms (such as vom- patients live longer.
iting and diarrhea). Some more-distinctive features
include genital or mucocutaneous ulcers and a rela- Prehospital Care
tively nondescript macular rash that mimics a viral
exanthem often seen in children with viral illnesses. The primary goal for providers in the prehospital
The syndrome typically lasts for weeks, and patients care of the HIV-infected patient is safe transfer to the
seek evaluation by a medical provider, often in the receiving facility and careful attention to personal
ED. There is a notable absence of pulmonary symp- protection. Resuscitation and stabilization of the
toms during the illness, and this may help clinicians HIV-infected patient follows the same principles as a
in their diagnostic approach to the febrile patient. non–HIV-infected individual. High-risk procedures
This constellation of signs and symptoms is known for exposure to bodily fluids occur often, and the
February 2016 • www.ebmedicine.net 3 Mobile app access: www.ebmedicine.net/app
prehospital provider must take caution for his or
her own safety, strictly adhering to universal pre-
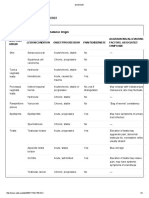
Table 1. Major Adverse Effects Of
cautions. In the event that a blood or body fluid
Antiretroviral Medications4
exposure does occur, the provider should seek Medication Adverse Effects
immediate care. Treatment with postexposure pro- Nucleoside Reverse Transcriptase Inhibitors
phylaxis (PEP) (a 28-day course of treatment with
HIV medication) is effective at decreasing rates of Abacavir Hypersensitivity reaction, Stevens-Johnson
syndrome, lactic acidosis, increased risk of
HIV acquisition.
myocardial infarction
Didanosine Stevens-Johnson syndrome, lactic acidosis,
Emergency Department Evaluation pancreatitis, peripheral neuropathy
Emtricitabine Lactic acidosis, hyperpigmentation/skin discol-
History oration
Chronic HIV infection can affect nearly every organ Lamivudine Lactic acidosis
system, highlighting the importance of a thorough
Stavudine Lactic acidosis, pancreatitis, peripheral neuropathy
history and physical examination. First, providers
should evaluate the status of the HIV infection (eg, Tenofovir* Lactic acidosis, Fanconi syndrome, accelerated
CD4 count and viral load), the treatment regimen, osteoporosis
and the patient's medication compliance. After an Zidovudine Stevens-Johnson syndrome, lactic acidosis, bone
overall sense of disease status is obtained, emer- marrow suppression
gency clinicians should focus on evaluation of the Nonnucleoside Reverse Transcriptase Inhibitors
chief complaint and its relevance to HIV infection or Delavirdine Stevens-Johnson syndrome, transaminitis
treatment taken for the HIV infection.
Initial questions for an HIV-infected patient Efavirenz Stevens-Johnson syndrome, psychosis, depression
include inquiring about the patient’s most recent Etravirine Stevens-Johnson syndrome, hypersensitivity reac-
CD4 count, viral load (or at least whether the viral tions
load is undetectable), and any recent travel history Nevirapine Stevens-Johnson syndrome, hepatic necrosis
or exposure to sick contacts. Asking about a pa- Rilpivirine Stevens-Johnson syndrome, depression
tient’s prior OIs is also important, as patients may
Protease Inhibitors
have sequelae from OIs that alter their physical
examination. If the patient is on HAART, determine Atazanavir Hyperbilirubinemia (indirect), PR interval prolon-
the specific drugs taken, the patient’s compliance, gation/atrioventricular block
and ask about the characteristic side-effect profiles Darunavir Gastrointestinal upset, sulfonamide hypersensitiv-
of some medications. (See Table 1.) These ques- ity, hepatotoxicity, Stevens-Johnson syndrome
tions help frame an understanding of the patient’s Fosamprenavir Rash, sulfonamide hypersensitivity, transaminitis
baseline HIV infection status. Indinavir Nephrotoxicity, urolithiasis
Questions related to the patient’s chief com-
Lopinavir Pancreatitis, PR and QT interval prolongation,
plaint should be guided by whether or not the transaminitis, gastrointestinal intolerance
patient is under the care of a clinician for his or her
Nelfinavir Gastrointestinal intolerance
HIV infection and is compliant with the prescribed
medication regimen. Patients unaware of their CD4 Ritonavir Gastrointestinal intolerance, metabolic syndrome,
count or viral load or who are not engaged in their paresthesia (circumoral and extremities),
asthenia
care should be considered at higher risk for OIs and
other complications of AIDS. Therefore, a thorough Saquinavir Metabolic syndrome, PR and QT interval prolon-
gation
history of these patients includes questions regard-
ing infectious symptoms such as fevers, chills, and Tipranavir Hepatotoxicity, intracranial hemorrhage, skin rash
diaphoresis. Patients compliant with treatment Integrase Inhibitors
regimens are at higher risk for conditions related to
Dolutegravir Hypersensitivity reactions
chronic infection and adverse reactions from medi-
cation. A thorough review of systems may uncover Elvitegravir Nephrotoxicity, gastrointestinal intolerance
symptoms related to chronic infection that the pa- Raltegravir Stevens-Johnson syndrome, creatine phosphoki-
tient may not have thought relevant to their present- nase elevation, pyrexia
ing complaint (eg, changes in skin, sleep, bowel or Fusion/Entry Inhibitors
bladder habits, or psychiatric disturbance).
Enfuvirtide Hypersensitivity reaction, increased incidence of
pneumonia
Physical Examination
Maraviroc Hepatotoxicity, abdominal pain, pyrexia, upper
A complete physical examination is critical for respiratory tract infections
patients with HIV. Physical examination findings *Nucleotide reverse transcriptase inhibitor.
related to specific conditions are discussed in the fol-
Copyright © 2016 EB Medicine. All rights reserved. 4 Reprints: www.ebmedicine.net/empissues
lowing sections. Because HIV has many dermatolog- Imaging
ic manifestations, a comprehensive skin examination Radiologic imaging tests should be directed at
should be included in addition to a complaint-based the patient’s complaints and immune status. The
physical examination. emergency clinician should have a low bar for imag-
ing, especially low-risk and low-cost tests (such as
Diagnostic Testing x-ray and ultrasound), where appropriate. Other
modalities such as computed tomography (CT) and
Laboratory Testing magnetic resonance imaging (MRI) should also be
In general, laboratory testing plays an important used, when appropriate. For example, an immu-
role in the screening and diagnosis of HIV-related nocompetent HIV-infected patient with headache
metabolic and infectious diseases. A study published probably does not need a CT of the brain; however,
in 2013 suggested that HIV-infected patients re- with decreasing CD4 counts, the chance of OIs or
ceived 4.5 laboratory tests per ED visit compared to malignancy in the brain increases, and neuroimag-
3.5 tests for the non–HIV-infected individual.8 These ing is indicated.
tests included complete blood count, basic metabolic
panel, and hepatic function testing. Lactic acidosis Medication Side Effects
is a complication of nucleoside reverse transcriptase
inhibitor (NRTI) use and, when acutely worsened, Highly Active Antiretroviral Therapy
is associated with higher mortality. Serum lactic The first promising antiretroviral medication against
acid measurement is appropriate in patients with HIV was the NRTI, zidovudine (AZT/ZDV), which
an anion gap metabolic acidosis or severe illness. was approved by the United States Food and Drug
HIV-infected patients are not only tested more often Administration (FDA) in 1987. In the years follow-
than noninfected patients, but are admitted more ing, several more NRTIs were developed; however,
frequently.8 Therefore, it appears that having a lower the virus’s rapid rate of mutation created drug
threshold for testing is appropriate in these patients. resistance, and mortality remained high. In 1996, the
When infectious complications are suspected, addition of protease inhibitors (PIs) revolutionized
appropriate cultures (sometimes for atypical HIV treatment. Two landmark studies demonstrated
organisms or OIs) should be ordered. If recent a 60% to 80% decrease in AIDS, associated hospital-
HIV-specific testing results are not available, the ization, and mortality in patients treated with this
emergency clinician can order a CD4 count and drug combination, HAART.11-13 In addition, non-
viral load; however, timely results are not typical- nucleoside reverse transcriptase inhibitors (NNRTI),
ly available for decision-making. CD4 counts and integrase inhibitors, fusion inhibitors, entry inhibi-
viral load results help to narrow the differential tors, and pharmacokinetic enhancers have been
diagnosis in HIV-infected patients. In cases where introduced as treatment, each directed at a different
patients have not had or do not know these val- stage of viral reproduction. Medications are often
ues, an absolute lymphocyte count may be used as administered in combination therapy through single
a surrogate for CD4 count.9 An absolute lympho- pills. This section will discuss each of these drug
cyte count < 950 cells/mm3 is associated with a classes and some of the more common adverse reac-
total CD4 count < 200 cells/mm3 (sensitivity, 76%; tions and side effects associated with each.
95% confidence interval [CI] 73%-79%; specificity,
93%; 95% CI, 87%-96%; positive likelihood ratio, Nucleoside Reverse Transcriptase Inhibitors And
10.1; 95% CI, 8.2-14).10 Nucleotide Reverse Transcriptase Inhibitors
HIV testing should be conducted in individuals The NRTIs and nucleotide reverse transcriptase in-
who might be infected with HIV if they show signs or hibitors (NtRTIs) inhibit reverse transcription of HIV
symptoms of diagnoses consistent with OIs or AIDS- RNA into DNA, thereby preventing viral replica-
related complications. Rapid HIV antibody testing is tion. These classes of medications are relatively well
available using either oral swabs or blood samples. tolerated and have a mild side-effect profile, includ-
Most currently available HIV antibody tests have sen- ing gastrointestinal upset, headache, and insomnia.
sitivities of 100% and specificities > 99%. Fourth-gen- The most severe toxic effect is dose-dependent bone
eration HIV tests identify both antibodies as well as marrow suppression, causing anemia and leukope-
the p24 antigen on the surface of HIV, which appears nia.14 Transaminitis and severe lactic acidosis have
to permit earlier diagnosis of an HIV infection. If an also been reported and are more common in patients
acute HIV infection is suspected, then measurement with liver disease.
of a viral load can help to make the diagnosis. Abacavir, one of the most commonly prescribed
NRTIs, is associated with a potentially severe hyper-
sensitivity reaction in 3% to 5% of patients. Certain
HLA alleles are susceptible to this reaction and
guidelines have been developed for screening and
February 2016 • www.ebmedicine.net 5 Mobile app access: www.ebmedicine.net/app
dosing before prescribing this medication, which re- frequent in the first 6 weeks of treatment and in pa-
duces or eliminates its occurrence.15,16 Symptoms of tients with a history of chronic hepatitis and in male
the hypersensitivity reaction include fever, rash, and patients with CD4 counts > 400/mm3.21
gastrointestinal and respiratory symptoms, which
usually occur within the first 6 weeks of drug expo- Protease Inhibitors
sure. Abacavir is also associated with an increased PIs prevent budding of the mature HIV virion from
risk of myocardial infarction in patients with risk the host membrane, making the virus largely nonin-
factors for cardiovascular disease.17 fectious. The most commonly used PIs are atazana-
For patients with liver disease who are taking vir, darunavir, lopinavir/ritonavir, and nelfinavir.
NRTIs, discontinuation of agents effective against Common side effects associated with PIs are mild
both HIV and hepatitis B virus (eg, emtricitabine, gastrointestinal upset, including nausea, diarrhea,
lamivudine, and tenofovir) can precipitate a severe and abdominal discomfort. Other potentially more
and sometimes fatal flare in hepatitis. When present- severe metabolic alterations include lipodystrophy,
ed with this clinical concern, the emergency clinician dyslipidemia, hypertriglyceridemia, and type 2
should provide supportive care and consult an infec- diabetes mellitus.22 Rarely, hypertriglyceridemia
tious disease specialist for treatment options. can precipitate pancreatitis. Atazanavir is associated
Tenofovir, another commonly prescribed NRTI, is with hyperbilirubinemia and jaundice, which may
associated with development of Fanconi syndrome in prompt patients to present to the ED; however, this
some patients.18 Patients with impaired renal function condition is not dangerous and resolves when the
prior to initiation of the drug are most at risk. Patients drug is discontinued.
with this syndrome can develop polyuria, polydipsia, Many of the PIs inhibit, and some induce,
and dehydration. Laboratory tests may demonstrate isoforms of the cytochrome P 450 enzyme system.
acidemia, hypochloremia, hypokalemia, and hypo- As a result, numerous other classes of medications
phosphatemia due to loss of bicarbonate, glucose, interact with PIs, including proton pump inhibi-
amino acids, and phosphate in the urine. Urinalysis tors, anticoagulants, HMGCoA reductase inhibi-
demonstrates glucosuria and proteinuria. Tenofovir tors, corticosteroids, antiarrhythmics, antiepileptics,
can also cause bone density loss and fractures, either antimalarials, and antidepressants. Therefore, it
alone or as part of Fanconi syndrome. The syndrome is imperative to cross-check interactions prior to
is usually avoided by stopping tenofovir at the time administering or prescribing other medications to
of abnormal creatinine measurements. patients taking PIs.4,23
Some medications in this class have less com-
mon, but important, side effects. According to Integrase Inhibitors
animal studies, AZT/ZDV may cause endothelial Integrase inhibitors, first approved by the FDA in
dysfunction leading to cardiovascular complica- 2007, prevent the incorporation of viral DNA into
tions.19 Didanosine and stavudine have been associ- the human host DNA. Examples of integrase inhibi-
ated with a rare incidence of pancreatitis, which can tors include raltegravir, dolutegravir, and elvitegra-
be fatal and has led to an FDA black box warning. vir. This class of medications is usually well toler-
ated, with side effects usually mild and including
Nonnucleoside Reverse Transcriptase Inhibitors nausea and headache.
NNRTIs also inhibit HIV reverse transcriptase. Ex-
amples of NNRTIs include nevirapine, efavirenz, etra- Fusion Inhibitors
virine, and rilpivirine. Efavirenz is associated with In order for HIV to gain entry into the host CD4 cell,
vivid dreams, nightmares, insomnia, and confusion, glycoprotein 120 on the surface of HIV must attach
which often resolve after the first several weeks of to host receptors and other glycoproteins, ultimately
treatment.20 However, more-severe neuropsychiatric allowing the cells to fuse. Currently, the only fusion
complications, including severe psychosis, have been (sometimes called entry) inhibitors available are
reported, and for this reason, efavirenz is often avoid- enfuvirtide and maraviroc. Enfuvirtide is admin-
ed in patients with a psychiatric history. Immediate istered by injection only because the acidic pH of
discontinuation of the medication is recommended if the stomach destroys the protein component of this
such severe psychosis occurs. Rarely, rilpivirine is also medication. Side effects are primarily limited to local
associated with insomnia and depression. erythema and nodules at the injection site. Rarely,
Rash, gastrointestinal upset, headache, and diz- patients develop neutropenia.
ziness are common with all medications in this class.
Infrequently (though more commonly with nevi- System-Based Disease And Medication Effects
rapine), patients can experience Stevens-Johnson
syndrome, toxic epidermal necrolysis, or erythema Cardiovascular Disease
multiforme. Nevirapine has also been associated As the life expectancy of HIV-infected patients has
with liver injury and failure, which led to an FDA increased, so have observed rates of traditional age-
black box warning in 2000. This complication is most
Copyright © 2016 EB Medicine. All rights reserved. 6 Reprints: www.ebmedicine.net/empissues
related conditions (such as cardiovascular disease) disease is not seen as frequently, but it must remain
increased among this population. A recent study on the differential in HIV-infected patients with pos-
estimated the increased relative risk of myocardial sible exposures.
infarction among HIV-infected persons to be 1.75 Today, patients with well-controlled HIV on
(95% CI, 1.51-2.02) compared to patients not HIV- HAART more commonly develop the traditional
infected.24 The pathophysiology of this increase pulmonary infections of immunocompetent pa-
involves not only traditional risk factors such as tients, of which, Streptococcus pneumonia is most
age and smoking, but also HAART. As mentioned common.29 Treatment for common pneumonias is
previously, HAART causes metabolic side effects the same as for non–HIV-infected patients, using
that also likely contribute the increased risk of car- antibiotics and fluid resuscitation or other sup-
diovascular disease.17,25-27 portive measures. Patients with immunosuppres-
sive disease are at risk for drug-resistant organ-
Pulmonary Disease isms, and the emergency clinician should con-
Prior to HAART, Pneumocystis pneumonia used to be sider expanding therapy in those patients whose
one of the most common opportunistic pulmonary disease is not well-controlled.
infections. Patients with Pneumocystis pneumonia Guidance on the disposition of HIV-infected
classically present with an indolent, nonproductive patients with pneumonia from the ED likely can
cough and exertional dyspnea. On x-ray, a perihilar mirror practice for patients without an HIV in-
or “batwing” infiltrate is seen. (See Figure 1.) Lac- fection, although there are no evidence-based
tate dehydrogenase (LDH) is typically elevated in guidelines on this topic. However, patients with
patients with Pneumocystis pneumonia, and a normal good social support who are followed closely by a
value is helpful in ruling out the disease.28 Patients primary care provider and known to be compliant
infected with HIV are at increased risk of tubercu- with treatment are likely to be good candidates for
losis (TB), (both novel infection and reactivation) outpatient treatment.30
after diagnosis with HIV because of the depletion of Chronic obstructive pulmonary disease (COPD)
TB-specific T-cells. With poorly controlled HIV infec- is an increasing concern in HIV patients. Higher
tion, the risk of TB increases. In the developed world rates of smoking in HIV-infected patients, lung in-
(where there are lower rates of TB in general), the jury from previous OIs, and drug effects are all risk
factors for the development of COPD.31 Treatment
for COPD is the same as for noninfected patients.
Figure 1. Chest X-Ray Of Pneumocystis Some data suggest that chronic HIV infection itself
jiroveci Pneumonia may also be an independent risk factor for the
disease.32 The higher risk could be related to the
chronic systemic inflammatory response present
in longstanding infection. This inflammatory state
is also associated with hypercoagulability, leading
to higher rates of venous thromboembolism and
pulmonary embolism in this population.33 The Pul-
monary Embolism Rule-out Criteria (PERC) did not
report HIV status on the participants of the study, so
it is difficult to conclude whether these criteria can
be applied to HIV-infected individuals.
Emergency clinicians should have a high index
of suspicion for concomitant conditions in the
context of a patient’s CD4 count and be prepared
to evaluate patients with laboratory and radiologic
studies, as appropriate. Imaging with chest x-ray
should be considered in all patients with HIV and
pulmonary complaints.
Renal Disease
Renal disease in HIV patients can be caused both
by the HIV infection itself as well as the nephrotox-
icity of HAART. Patients present with acute kidney
injury similar to non–HIV-infected patients, and
their treatment is the same. Nephrotoxic medica-
tions should be withheld temporarily while the
Arrows point to perihilar (“batwing”) infiltrate. patient is resuscitated.
Image courtesy of Mount Sinai St. Luke's Hospital, New York, NY.
February 2016 • www.ebmedicine.net 7 Mobile app access: www.ebmedicine.net/app
Clinical
ClinicalPathway
PathwayFor
ForEmergency Department
Management Management
Of Weakness Of Multiple
In HIV-Infected Patients
Shocks
HIV-infected patient presents with weakness
Rapidly assess for possible stroke syndrome. Perform a comprehensive physical and
neurologic examination, focusing on:
• Focal vs generalized findings
• Upper vs lower extremity asymmetry
• Cranial nerves
YES • Muscle tone and strength
• Upper and lower motor neuron findings
Is the weakness focal?
NO
Consider CNS causes Weakness is associated Weakness is Weakness is
Patient is on HAART
of unilateral weakness: with upper motor associated with generalized
• Stroke neuron findings lower motor neuron
• Tumor findings (reflexes,
• Spinal cord lesion fasciculations)
If the CD4 count is
< 200 cells/mm3:
Consider: Consider: Consider: Consider medication-
• Toxoplasmosis
• Spinal cord lesion • Guillain-Barré • Electrolyte specific effects:
• CNS lymphoma
• Spinal epidural syndrome abnormalities • Renal impairment
• Abscess
abscess • Cauda equina • Sepsis • Lactic acidosis
• Tuberculosis
• Radiculopathy • Hypothyroid • Anemia/bone marrow
(Class III)
If the CD4 count is • Adrenal insufficiency suppression
< 200 cells/mm3: If the CD4 count is • Acute coronary • Dehydration from
• HIV myelopathy < 200 cells/mm3: syndromes diarrhea
(Class III) • HIV polyneuropathy • Dehydration (Class III)
(Class III) • Myasthenia gravis
• Botulism
(Class III)
Abbreviations: CD4, CD4 T lymphocyte; CNS, central nervous system; CT, computed tomography; HAART, highly active antiretroviral therapy; HIV,
human immunodeficiency virus; MRI, magnetic resonance imaging.
Class Of Evidence Definitions
Each action in the clinical pathways section of Emergency Medicine Practice receives a score based on the following definitions.
Class I Class II Class III Indeterminate
• Always acceptable, safe • Safe, acceptable • May be acceptable • Continuing area of research
• Definitely useful • Probably useful • Possibly useful • No recommendations until further
• Proven in both efficacy and effectiveness • Considered optional or alternative treat- research
Level of Evidence: ments
Level of Evidence: • Generally higher levels of evidence Level of Evidence:
• One or more large prospective studies • Nonrandomized or retrospective studies: Level of Evidence: • Evidence not available
are present (with rare exceptions) historic, cohort, or case control studies • Generally lower or intermediate levels • Higher studies in progress
• High-quality meta-analyses • Less robust randomized controlled trials of evidence • Results inconsistent, contradictory
• Study results consistently positive and • Results consistently positive • Case series, animal studies, • Results not compelling
compelling consensus panels
• Occasionally positive results
This clinical pathway is intended to supplement, rather than substitute for, professional judgment and may be changed depending upon a patient’s individual
needs. Failure to comply with this pathway does not represent a breach of the standard of care.
Copyright © 2016 EB Medicine. 1-800-249-5770. No part of this publication may be reproduced in any format without written consent of EB Medicine.
Copyright © 2016 EB Medicine. All rights reserved. 8 Reprints: www.ebmedicine.net/empissues
Nephrolithiasis and urolithiasis are common per day).37 Etiologies include infectious diseases,
side effects of PIs, particularly indinavir (although malignancies, and medication-induced diarrhea.
few HIV-infected patients take this medication and, The pathogenesis of gastrointestinal symptoms
instead, take one of the newer PIs). PIs have poor depends on the degree of immunocompromise.
solubility and significant urinary excretion that Common pathogens that cause diarrhea in healthy
leads to stone formation. Urinalysis will most likely individuals will also do so in HIV-infected patients
demonstrate hematuria; however, stones comprised on HAART. In the pre-HAART era, Clostridium
of indinavir deposits are typically radiolucent and difficile was the most common pathogen isolated in
may be missed by standard radiologic imaging. HIV-infected patients with diarrhea; however, with
Therefore, secondary signs of obstruction, such as successful treatment with HAART, the frequency
hydroureter and perinephric stranding, may be of hospitalizations and diagnosis of AIDS are both
the only findings on imaging. Discussion with the decreased. Therefore, C difficile may not be the most
patient’s HIV provider regarding the continuation frequent infection, though it is more common in
or cessation of indinavir is advised. Treatment of HIV-infected individuals than in non–HIV-infected
nephrolithiasis and urolithiasis are the same as for individuals.38
the non–HIV-infected patient. As the CD4 count drops, the patient is at risk for
OIs such as Cryptococcus, Cytomegalovirus, microspo-
Neurologic Disease ridiosis, and Mycobacterium avium complex. In many
Evaluation of the HIV-infected patient with a cases, initiation of HAART to restore the gastroin-
neurologic complaint should be guided by the CD4 testinal immune system will help eradicate these
count. Patients with HIV infection, even if it is well- infections. Stool laboratory studies are guided based
controlled, have a slightly higher risk of cerebrovas- on the patient’s stage of disease.
cular disease due to the chronic inflammatory state, Hepatobiliary complaints are also common
accelerated atherosclerosis, and metabolic effects of in HIV-infected patients and may be caused by a
medications. The evaluation of patients with fo- variety of etiologies from infectious to infiltrative
cal neurologic deficits should follow typical stroke to medication-related problems. Co-infection with
algorithms. hepatitis C virus affects 30% to 80% of HIV patients
Rates of central nervous system OIs, such as and chronic hepatitis B virus affects 5% to 10% of
cryptococcal meningitis, toxoplasmosis, progressive patients.39,40 Co-infection with either virus increases
multifocal leukoencephalopathy, and Cytomegalovi- a patient's risk of developing chronic hepatitis 2 to 3
rus have decreased significantly with treatment ad- times compared to non–HIV-infected patients with
herence. However, if a patient with a low CD4 count hepatitis B virus or hepatitis C virus. Nearly all of
is identified, imaging and, possibly, lumbar puncture the HAART medications have potential hepatotoxic-
aimed at the identification of OI is indicated. CT ity that can be worsened by co-infection with hepati-
of the head may require contrast in order to bet- tis B virus or hepatitis C virus.41
ter identify infectious processes or central nervous Patients with hepatobiliary complaints should
system malignancy, such as lymphoma. MRI pro- be asked about their medication regimens and any
vides identification of smaller lesions and evaluates co-infections with hepatitis B virus or hepatitis C
leptomeningeal enhancement better than CT. virus. Laboratory evaluations should include trans-
HIV myelopathy may develop at the end stages aminases, bilirubin, and lipase.
of untreated disease. Patients develop lower extrem-
ity weakness associated with sensory abnormalities, Hematologic Disease
imbalance, and incontinence. Patients are hyperre- Cytopenias of all cell lines are common in HIV-
flexic, with normal imaging studies and abnormali- infected patients. Patients with an uncontrolled
ties on electrophysiologic testing. HIV infection may develop pancytopenia, as bone
The prevalence of HIV-associated dementia has marrow production is suppressed. Anemia may be
also decreased since the introduction of HAART.34 caused by a primary HIV infection or as a result of
Rates of milder neurocognitive disorders also ap- medication use. Medication-induced anemia is often
pear to decrease with longer periods of undetect- macrocytic, although in the ED evaluation, this is a
able virus.35,36 diagnosis of exclusion.
The rate of HIV-associated thrombocytopenia
Gastrointestinal And Hepatobiliary Disease increases with decreasing CD4 count. Initiation of
Gastrointestinal symptoms, especially diarrhea, are HAART, particularly AZT/ZDV, is the mainstay of
some of the most common presentations of HIV- treatment. These medications are rarely initiated in
infected patients in the ED. In a large cohort study, the ED, and patients with severe or symptomatic
40% of HIV infected adults on HAART reported at thrombocytopenia should be evaluated in consulta-
least 1 episode of diarrhea in the past month, with tion with the appropriate specialists.
3% reporting severe diarrhea (defined as > 6 stools HIV-infected patients also have higher rates
February 2016 • www.ebmedicine.net 9 Mobile app access: www.ebmedicine.net/app
of thromboembolic disease, with a large prospec- ranges from 10% to 80%, depending on the defini-
tive study estimating the rate to be 2.6 per 1000 tion of lipodystrophy.45 The most important risk
patient-years.42 The chronic inflammatory state of factor for development of this condition appears to
HIV infection appears to be a risk factor for throm- be NRTI use.46
boembolic disease. In HIV-infected patients without Prior to widespread use of HAART, endocrine
well-controlled disease, factors associated with complications of OIs were much more prevalent.
thrombotic complications include lower CD4 count, These complications included glandular infection
higher viral load, presence of OI, malignancy, and and infiltration of the pituitary, adrenal, and, rarely,
indwelling central venous catheters.43 Thrombotic thyroid glands. Although these conditions are
thrombocytopenic purpura occurs in HIV-infected much less common now because of HAART, they
patients, although its prevalence has decreased in should still be considered, especially in patients not
the HAART era. Patients with hemolytic anemia and on HAART or patients with AIDS. Glucocorticoid
thrombocytopenia should be evaluated for throm- deficiency can result from adrenal involvement, and
botic thrombocytopenic purpura.44 while it is usually subclinical, it should be consid-
ered in patients with AIDS and hypotension or criti-
Endocrine Disease cal illness. Treatment for these patients is the same as
HAART is associated with dyslipidemia and truncal for non–HIV-infected patients.
obesity. This pattern of central fat accumulation and Patients on HAART are at risk for developing
peripheral fat loss has been termed HIV-associated thyrotoxicosis in association with immune recon-
lipodystrophy syndrome. Prevalence of lipodystrophy stitution inflammatory syndrome due to autoim-
Risk Management Pitfalls For Managing HIV-Infected Patients
In The Emergency Department (Continued on page 11)
1. “I know he had long-standing HIV, but he was 4. “My patient has a history of migraines; I as-
only 42 years old, and I thought that was too sumed this headache was a migraine as well.”
young to have acute coronary syndromes.” Emergency clinicians must be careful not to
HIV and HAART are synergistic in causing anchor on prior headache diagnoses. The
cardiovascular disease. A chronic inflammatory primary goal is to rule out dangerous causes
state caused by HIV itself, as well as side of headaches, even in patients who have a
effects of HAART, may act together to cause history of benign headaches. Patients with
cardiovascular disease. If the patient has been migraines or tension headaches can still suffer
HIV-infected for an extended period of time, from meningitis, subarachnoid hemorrhage, or
acute coronary syndromes should be in the other causes of series or secondary headaches.
differential. A careful HIV history, with particular attention
to the CD4 count, and thorough neurological
2. “This patient presented with fever, generalized examination is critical in HIV-infected patients
lymphadenopathy, sore throat, and a macular presenting with headache. This process will
rash. He is concerned about HIV infection, but often help differentiate patients who will require
his rapid HIV test is negative.” imaging and further testing.
This patient has symptoms consistent with acute
seroconversion illness. Rapid testing technology 5. “My patient complained of diarrhea for the
may miss early infection, and therefore a viral past 2 weeks since starting HAART, and the
load must be sent in order to properly identify symptoms were interfering with her ability to
these patients. work. I thought it would be OK to temporar-
ily stop her medications until her primary care
3. “My patient presented with generalized weak- provider could adjust them.”
ness but recently had a high CD4 count.” Inconsistent compliance with HAART can cause
Remember that common causes of weakness in viral resistance to the medications. Therefore,
the non–HIV-infected patient are also common there are very few scenarios in which a patient
in the HIV-infected patient. For this patient, should stop HAART treatment. Stevens-Johnson
think beyond opportunistic infections and syndrome and nevirapine-associated hepatic
consider sepsis and metabolic etiologies (such as failure are indications to stop HAART. The
hypoglycemia) and derangements in potassium patient’s primary care provider or an HIV
and calcium. In the winter months, also consider medicine consultant should be involved in all
carbon monoxide poisoning. decisions to terminate HAART.
Copyright © 2016 EB Medicine. All rights reserved. 10 Reprints: www.ebmedicine.net/empissues
mune activation against the thyroid. Patients and more significant pathology. Infectious complica-
generally present months to years after starting tions (such as septic arthritis) are less common with
HAART with symptoms of Grave disease, weight improved control of the disease. As the CD4 count
loss, and tachycardia.47 drops, septic arthritis, osteomyelitis, and discitis must
Disorders of glucose metabolism are associated be considered with appropriate evaluation, including
with the use of HAART, particularly PIs. Addition- laboratory testing and imaging studies.50
ally, the disease itself is associated with an increased
incidence of diabetes as a result of chronic inflamma- Psychiatric Disease
tion leading to insulin resistance.48 Neuropsychiatric illness is prevalent and multifac-
torial in HIV-infected individuals. Direct effects of
Musculoskeletal Disease the virus, underlying mental illness, and the social
Patients with longstanding HIV infection who are on implications of an HIV diagnosis all contribute to
treatment have lower bone mineral density when com- psychiatric illness. Medication effects, notably efavi-
pared with noninfected individuals of similar age.49 renz, also contribute. Depression is one of the most
Therefore, HIV-infected patients are at increased risk common diagnoses in HIV-infected patients and is
of fracture. HIV itself, as well as antiretroviral medica- associated with decreased medication compliance.23
tions, are implicated in higher rates of avascular ne- Demoralization syndrome is similar to depres-
crosis. Benign musculoskeletal and joint complaints of sion in that patients experience a sense of hope-
pain are common in the HIV-infected patient, and the lessness or sadness. However, it is different from
emergency clinician must differentiate between these depression because it is not associated with anhe-
Risk Management Pitfalls For Managing HIV-Infected Patients
In The Emergency Department (Continued from page 10)
6. “A patient with a history of HIV infection and 9. “The patient complained of feeling 'off bal-
COPD presented with shortness of breath and ance.' She had mild ataxia, but the CT scan was
mild pleuritic chest pain. He said that the pain normal. I never expected a cerebellar lesion.”
was not characteristic of his COPD exacerba- Remember the limitations of nonenhanced
tions. Oxygen saturation was normal and his CT scans. Patients with poorly controlled HIV
lungs were clear to auscultation.” are at higher risk for central nervous system
Consider pulmonary embolism in a patient infections, including toxoplasmosis, which may
like this. HIV infection causes a chronic be missed on this type of CT scan. Patients with
inflammatory state, which is associated with a concerning history or physical examination
increased risk of venous thromboembolism. should receive additional testing when a
nonenhanced CT scan is negative.
7. “The patient frequently had loose stools, so I
thought his diarrhea was the same old thing.” 10. “He recently discontinued his tenofovir. The
Diarrhea is a frequent complaint in HIV-infected liver function tests were high. I still don't un-
patients and can often be caused by medications. derstand what happened.”
However, dangerous etiologies occur frequently, Tenofovir, emtricitabine, and lamivudine are
as well. It is important to question patients about also active against hepatitis B virus. Termination
changes in bowel movements, recent travel history, of these agents in patients with co-infection
recent antibiotic use, and previous history of can precipitate a severe and sometimes fatal
gastrointestinal infections, and to assess for infectious hepatitis flare that must be included in the
etiologies before blaming a medication side effect. differential diagnosis of this patient. Along
with evaluating other etiologies of hepatitis,
8. “There was no history of OI and he just started consultation with an HIV medicine specialist
HAART. I never thought he could have TB.” about reinitiating these medications is
Initiation of HAART treatment places patients at suggested.
risk of unmasking previously unrecognized OI.
Although it may seem counterintuitive, starting
treatment can actually be dangerous in patients
with very low CD4 counts. When these patients
present to the ED, OIs and medication side
effects should both be considered as etiologies of
their complaints.
February 2016 • www.ebmedicine.net 11 Mobile app access: www.ebmedicine.net/app
donia. Demoralization is common in patients with exposure.53 Individual states may have different
HIV and may be related to the social implications guidelines, and emergency clinicians should be
of being diagnosed with HIV. Unlike depression, aware of local regulations. The exposed patient
demoralization does not respond to antidepressants should have baseline HIV testing performed. A
and requires further evaluation and treatment by a multidrug regimen is recommended, extrapolating
psychiatrist. the success of using combination therapy in the
Mania is also a recognized complication of treatment of HIV. Randomized data on the success
HIV disease. Patients presenting to the ED with of PEP are not available; however, rates of sero-
symptoms consistent with this should be evaluated conversion remain low when therapy is initiated
for organic etiologies of their symptoms and then early with full compliance.54
referred to psychiatric services. Patients present-
ing to the ED with symptoms concerning for any Summary
mental illness should be questioned about suicidal
and homicidal ideation and admitted if either are When evaluating the HIV-infected ED patient, the
present; otherwise, they should receive prompt first step is an assessment of the status of disease.
outpatient follow-up. The differential diagnosis of a patient’s symptoms
will change significantly based on the CD4 count
Dermatologic Disease and viral load. Patients with low CD4 counts (< 200
Dermatologic complaints are common in HIV- cells/mm3) must have a complete history, review
infected patients. HAART is associated with a high of systems, and physical examination in order to
rate of drug-related skin reactions, which can lead to identify any OIs. When the CD4 count is unknown,
medication noncompliance.51 Dermatologic hyper- the absolute lymphocyte count might be a helpful
sensitivity and photosensitivity are both common surrogate. HIV-infected patients with well-controlled
with HAART. disease taking medications are living longer and are
Although treatment with HAART seems to be now experiencing side effects possibly due to the
associated with a lower risk of infectious derma- chronic inflammatory state of HIV and adverse drug
tologic conditions, rates of these infections remain reactions. It is critical to understand the organ-specif-
high.52 Folliculitis is likely the most common of ic complications of chronic HIV infection and more
these, with Staphylococcus aureus being the most common adverse medication effects. In particular,
common pathogen, particularly the methicillin-resis- patients with longstanding HIV infection are likely
tant strain. Other common infectious dermatologic at higher risk of coronary artery disease, thrombo-
complaints, including herpes zoster, human papil- embolic disease, and COPD. Commonly used HIV
lomavirus-associated warts, seborrheic dermatitis, medications carry the risk of multiple drug interac-
and molluscum contagiosum, are more common in tions, and emergency clinicians must cross-check
HIV-infected patients, with treatment considerations ED therapy and new prescriptions with the patient’s
being the same as in non–HIV-infected patients. home medication regimen.
Special Circumstances Key Points
HIV-infected patients with sexual partners, or • A thorough history should include the patient’s
patients with a sexual partner of unknown status, most recent CD4 count, CD4 nadir, viral load,
may present to the ED after sexual encounters and a list of the patient’s medications.
during which barrier methods of protection are • HAART (especially PIs) increase triglycerides
compromised, ie, condom breakage or lack of and LDL (low-density lipoprotein) and lower
condom usage. In these instances, the emergency HDL (high-density lipoprotein) levels, causing
clinician must counsel the patient regarding PEP higher risk of coronary artery disease.
and potentially initiate treatment. The ED is also a • Systemic inflammatory response associated with
frequent portal of entry for healthcare workers and chronic HIV leads to coronary artery disease, hy-
others with potential exposures to HIV through percoagulability, and venous thromboembolism.
percutaneous or mucous membrane exposure. The • Ritonavir increases bioavailability of cortico-
risk of HIV transmission depends on both the type steroids and can lead to iatrogenic Cushing
of exposure and stage of illness in the source of the syndrome.
exposure (if known). • Nonenhanced CT scans can miss nephrolithiasis
PEP is most effective when administered soon caused by radiolucent indinavir stones.
after the exposure, ideally within 2 hours. The • Laboratory-based fourth-generation rapid
United States Centers for Disease Control and HIV tests have sensitivities > 90%, even in the
Prevention recommend that PEP be initiated as acute phase.
soon as possible, preferably within 72 hours of the • HIV-infected patients with low CD4 counts are
Copyright © 2016 EB Medicine. All rights reserved. 12 Reprints: www.ebmedicine.net/empissues
at risk for several central nervous system infec- References
tions and diseases, such as progressive multifo-
cal leukoencephalopathy. Maintain a low thresh- Evidence-based medicine requires a critical ap-
old for nonenhanced CT scans of the brain. praisal of the literature based upon study methodol-
• Although diarrhea is very common in HIV-in- ogy and number of subjects. Not all references are
fected patients and may have a benign etiology, equally robust. The findings of a large, prospective,
C difficile is also very common, so dangerous randomized, and blinded trial should carry more
etiologies of diarrhea should be excluded. weight than a case report.
• Cytopenias of all cell lines are common in HIV- To help the reader judge the strength of each
infected patients. reference, pertinent information about the study are
• Demoralization syndrome presents similarly to included in bold type following the reference, where
depression but is not improved by antidepres- available. In addition, the most informative referenc-
sants. Ask patients with psychiatric complaints es cited in this paper, as determined by the authors,
about suicidal and homicidal ideation. are noted by an asterisk (*) next to the number of the
• PEP is most effective if it is administered as close reference.
to the time of exposure as possible. It is not rec-
ommended after 72 hours postexposure. 1. UNAIDS. UNAIDS fact sheet. Available at: http://www.
unaids.org/en/resources/campaigns/globalreport2013/
factsheet/. Accessed November 8, 2014. (United Nations
Case Conclusions publication)
2.* Nakagawa F, May M, Phillips A. Life expectancy living with
After reviewing the CT scan for the 28-year-old man with HIV: recent estimates and future implications. Curr Opin
flank pain and no identifiable stone, you decided to treat Infect Dis. 2013;26(1):17-25. (Systematic review)
3. Lima VD, Hogg RS, Harrigan PR, et al. Continued improve-
him presumptively. You remembered that in patients tak-
ment in survival among HIV-infected individuals with
ing indinavir, CT scans may not demonstrate the stone newer forms of highly active antiretroviral therapy. AIDS.
and may show only secondary signs. The patient had 2007;21(6):685-692. (Prospective; 2000 patients)
ongoing pain and urology was consulted. He was taken to 4. Panel on Antiretroviral Guidelines for Adults and Adoles-
the operating room for ureteral stent in the context of an cents. Department of Health and Human Services. Guide-
lines for the use of antiretroviral agents in HIV-1-infected
obstructing radiolucent stone.
adults and adolescents. Available at: http://aidsinfo.nih.
The 42-year-old woman’s laboratory test results gov/contentfiles/lvguidelines/AdultandAdolescentGL.pdf.
were notable for a leukocytosis of 14,000 cells/mm3. On Accessed August 5, 2015. (Government report)
further questioning, she said that, although she was on 5. Rodger A, Bruun T, Cambiano V, et al. HIV transmission
HAART and Pneumocystis pneumonia prophylaxis with risk through condomless sex if HIV+ partner on suppressive
ART: PARTNER Study. Paper presented at: 21st Confer-
trimethoprim-sulfamethoxazole, she had not been able to
ence on Retroviruses and Opportunistic Infections, Abstract
see a physician in over a year because of insurance prob- 153LB. March 3-6, 2014. (Prospective; 30,000 cases)
lems. She did not remember the last time she had her CD4 6.* Palella FJ Jr, Baker RK, Moorman AC, et al. Mortality in the
count or viral load checked. You decided that this patient highly active antiretroviral therapy era: changing causes
was at high risk for C difficile infection. You started of death and disease in the HIV outpatient study. J Acquir
Immune Defic Syndr. 2006;43(1):27-34. (Prospective; 7000
metronidazole and admitted her to the hospital.
patients)
Upon speaking with the third patient, you realized 7. Hall HI, An Q, Tang T, et al. Prevalence of diagnosed and un-
that she was most likely not responding to antidepressants diagnosed HIV infection – United States, 2008-2012. MMWR.
because she suffered from demoralization. She reported 2015;64(24):657-662. (CDC report)
that she had not been taking her HAART consistently 8.* Mohareb AM, Rothman RE, Hsieh YH. Emergency depart-
ment (ED) utilization by HIV-infected ED patients in the
because, “What’s the point?” While she did not require
United States in 2009 and 2010 - a national estimation. HIV
emergent psychiatric evaluation, you conferred with her Med. 2013;14(10):605-613. (Observational; 1.1 milliion pa-
and her family members, and they agreed that she would tients)
follow up with her psychiatrist to discuss her demoraliza- 9. Shapiro NI, Karras DJ, Leech SH, et al. Absolute lymphocyte
tion and to pursue therapy. You reiterated the importance count as a predictor of CD4 count. Ann Emerg Med. 1998;32(3
Pt 1):323-328. (Retrospective; 322 patients)
of HAART compliance and counseled her that therapy
10. Napoli AM, Fischer CM, Pines JM, et al. Absolute lympho-
and proper treatment for demoralization may improve her cyte count in the emergency department predicts a low CD4
mood and her compliance with treatment. count in admitted HIV-positive patients. Acad Emerg Med.
2011;18(5):565. (Retrospective; 866 patients)
11. Hammer SM, Squires KE, Hughes MD, et al. A controlled
Acknowledgement trial of two nucleoside analogues plus indinavir in persons
with human immunodeficiency virus infection and CD4
The authors wish to thank Jennifer L. Galjour, MD, cell counts of 200 per cubic millimeter or less. AIDS Clinical
MPH, Icahn School of Medicine at Mount Sinai, New Trials Group 320 Study Team. N Engl J Med. 1997;337(11):725-
York, NY, for her assistance with this issue. 733. (Prospective randomized controlled; 1056 patients)
12. Moore RD, Chaisson RE. Natural history of HIV infec-
tion in the era of combination antiretroviral therapy. AIDS.
1999;13(14):1933-1942. (Retrospective; 1000 patients)
February 2016 • www.ebmedicine.net 13 Mobile app access: www.ebmedicine.net/app
13. Gulick RM, Mellors JW, Havlir D, et al. Treatment with patients)
indinavir, zidovudine, and lamivudine in adults with human 31. Hull MW, Phillips P, Montaner JS. Changing global epide-
immunodeficiency virus infection and prior antiretroviral miology of pulmonary manifestations of HIV/AIDS. Chest.
therapy. N Engl J Med. 1997;337(11):734-739. (Prospective 2008;134(6):1287-1298. (Review)
randomized double-blind; 97 patients) 32. Crothers K, Butt AA, Gibert CL, et al. Increased COPD
14. PubChem. Compound summary for zidovudine. Available among HIV-positive compared to HIV-negative veterans.
at: http://pubchem.ncbi.nlm.nih.gov/compound/35370?fro Chest. 2006;130(5):1326-1333. (Prospective observational;
m=summary#x291. Accessed November 18, 2014. (Website) 1000 patients)
15. Martin MA, Hoffman JM, Freimuth RR, et al. Clinical 33. Rasmussen LD, Dybdal M, Gerstoft J, et al. HIV and risk of
pharmacogenetics implementation consortium guidelines venous thromboembolism: a Danish nationwide population-
for HLA-B genotype and abacavir dosing: 2014 update. Clin based cohort study. HIV Med. 2011;12(4):202-210. (Retrospec-
Pharmacol Ther. 2014;95(5):499-500. (Clinical guideline) tive; 4000 patients)
16. Mallal S, Nolan D, Witt C, et al. Association between pres- 34. Heaton RK, Clifford DB, Franklin DR Jr, et al. HIV-
ence of HLA-B*5701, HLA-DR7, and HLA-DQ3 and hyper- associated neurocognitive disorders persist in the era of
sensitivity to HIV-1 reverse-transcriptase inhibitor abacavir. potent antiretroviral therapy: CHARTER Study. Neurology.
Lancet. 2002;359(9308):727-732. (Observational; 200 patients) 2010;75(23):2087-2096. (Observational; 1555 patients)
17. Worm SW, Sabin C, Weber R, et al. Risk of myocardial infarc- 35. Heaton RK, Franklin DR Jr, Deutsch R, et al. Neurocogni-
tion in patients with HIV infection exposed to specific indi- tive change in the era of HIV combination antiretroviral
vidual antiretroviral drugs from the 3 major drug classes: the therapy: the longitudinal CHARTER study. Clin Infect Dis.
data collection on adverse events of anti-HIV drugs (D:A:D) 2015;60(3):473-480. (Cross-sectional observational; 1500
study. J Infect Dis. 2010;201(3):318-330. (Observational; 580 patients)
patients) 36. Ortiz G, Koch S, Romano JG, et al. Mechanisms of ischemic
18. Gupta SK, Anderson AM, Ebrahimi R, et al. Fanconi syn- stroke in HIV-infected patients. Neurology. 2007;68(16):1257-
drome accompanied by renal function decline with tenofovir 1261. (Retrospective; 80 patients)
disoproxil fumarate: a prospective, case-control study of 37.* Knox TA, Spiegelman D, Skinner SC, et al. Diarrhea and
predictors and resolution in HIV-infected patients. PLoS One. abnormalities of gastrointestinal function in a cohort of
2014;9(3):e92717. (Prospective case-control; 56 patients) men and women with HIV infection. Am J Gastroenterol.
19. Jiang B, Hebert VY, Zavecz JH, et al. Antiretrovirals induce 2000;95(12):3482-3489. (Cross-sectional; 600 patients)
direct endothelial dysfunction in vivo. J Acquir Immune Defic 38. Collini PJ, Kuijper E, Dockrell DH. Clostridium difficile
Syndr. 2006;42(4):391-395. (Animal study) infection in patients with HIV/AIDS. Curr HIV/AIDS Rep.
20. Cespedes MS, Aberg JA. Neuropsychiatric complications of 2013;10(5):273-282. (Review)
antiretroviral therapy. Drug Saf. 2006;29(10):865-874. (Sys- 39. Puoti M, Airoldi M, Bruno R, et al. Hepatitis B virus co-in-
tematic review) fection in human immunodeficiency virus-infected subjects.
21. Stern JO, Robinson PA, Love J, et al. A comprehensive AIDS Rev. 2002;4(1):27-35. (Systematic review)
hepatic safety analysis of nevirapine in different populations 40. Staples CT Jr, Rimland D, Dudas D. Hepatitis C in the HIV
of HIV infected patients. J Acquir Immune Defic Syndr. 2003;34 (human immunodeficiency virus) Atlanta V.A. (Veterans
Suppl 1:S21-S33. (Prospective; 3000 patients) Affairs Medical Center) Cohort Study (HAVACS): the effect
22. Fantry LE. Protease inhibitor-associated diabetes mellitus: a of coinfection on survival. Clin Infect Dis. 1999;29(1):150-154.
potential cause of morbidity and mortality. J Acquir Immune (Prospective observational; 300 patients)
Defic Syndr. 2003;32(3):243-244. (Editorial) 41. den Brinker M, Wit FW, Wertheim-van Dillen PM, et al. Hep-
23.* Venkat A, Piontkowsky DM, Cooney RR, et al. Care of the atitis B and C virus co-infection and the risk for hepatotoxic-
HIV-positive patient in the emergency department in the ity of highly active antiretroviral therapy in HIV-1 infection.
era of highly active antiretroviral therapy. Ann Emerg Med. AIDS. 2000;14(18):2895-2902. (Retrospective; 400 patients)
2008;52(3):274-285. (Systematic review) 42. Sullivan PS, Dworkin MS, Jones JL, et al. Epidemiology of
24. Triant VA, Lee H, Hadigan C, et al. Increased acute myocar- thrombosis in HIV-infected individuals. The Adult/Adoles-
dial infarction rates and cardiovascular risk factors among cent Spectrum of HIV Disease Project. AIDS. 2000;14(3):321-
patients with human immunodeficiency virus disease. J Clin 324. (Longitudinal observational; 42,000 patients)
Endocrinol Metab. 2007;92(7):2506-2512. (Prospective obser- 43. Saif MW, Bona R, Greenberg B. AIDS and thrombosis: ret-
vational; 4000 patients) rospective study of 131 HIV-infected patients. AIDS Patient
25. Giannarelli C, Klein RS, Badimon JJ. Cardiovascular Care STDS. 2001;15(6):311-320. (Retrospective; 100 patients)
implications of HIV-induced dyslipidemia. Atherosclerosis. 44. Becker S, Fusco G, Fusco J, et al. HIV-associated thrombotic
2011;219(2):384-389. (Systematic review) microangiopathy in the era of highly active antiretroviral
26. O’Cleirigh C, Valentine SE, Pinkston M, et al. The unique therapy: an observational study. Clin Infect Dis. 2004;39 Sup-
challenges facing HIV-positive patients who smoke pl 5:S267-S275. (Prospective observational; 6000 patients)
cigarettes: HIV viremia, ART adherence, engagement 45. Heath KV, Hogg RS, Chan KJ, et al. Lipodystrophy-associ-
in HIV care, and concurrent substance use. AIDS Behav. ated morphological, cholesterol and triglyceride abnormali-
2015;19(1):178-185. (Cross-sectional; 300 patients) ties in a population-based HIV/AIDS treatment database.
27. Friis-Moller N, Reiss P, Sabin CA, et al. Class of antiretroviral AIDS. 2001;15(2):231-239. (Prospective observational; 1000
drugs and the risk of myocardial infarction. N Engl J Med. patients)
2007;356(17):1723-1735. (Prospective observational; 23,437 46. Mallal SA, John M, Moore CB, et al. Contribution of nucleo-
patients) side analogue reverse transcriptase inhibitors to subcuta-
28. Smith RL, Ripps CS, Lewis ML. Elevated lactate dehydroge- neous fat wasting in patients with HIV infection. AIDS.
nase values in patients with Pneumocystis carinii pneumonia. 2000;14(10):1309-1316. (Prospective; 277 patients)
Chest. 1988;93(5):987-992. (Case control; 7 patients) 47. Crum NF, Ganesan A, Johns ST, et al. Graves disease: an
29. Benito N, Moreno A, Miro JM, et al. Pulmonary infections increasingly recognized immune reconstitution syndrome.
in HIV-infected patients: an update in the 21st century. Eur AIDS. 2006;20(3):466-469. (Correspondence)
Respir J. 2012;39(3):730-745. (Review) 48. Hadigan C, Kattakuzhy S. Diabetes mellitus type 2 and
30. Fine MJ, Auble TE, Yealy DM, et al. A prediction rule to iden- abnormal glucose metabolism in the setting of human
tify low-risk patients with community-acquired pneumonia. immunodeficiency virus. Endocrinol Metab Clin N Am.
N Engl J Med. 1997;336(4):243-250. (Retrospective; 14,000 2014;43(3):685-696. (Review)
Copyright © 2016 EB Medicine. All rights reserved. 14 Reprints: www.ebmedicine.net/empissues
49. Takhar SS, Hendey GW. Orthopedic illnesses in patients with 3. The most common cause of community-ac-
HIV. Emerg Med Clin North Am. 2010;28(2):335-342. (Review) quired pneumonia in HIV patients on HAART
50. Marquez J, Restrepo CS, Candia L, et al. Human immu-
nodeficiency virus-associated rheumatic disorders in the
is:
HAART era. J Rheumatol. 2004;31(4):741-746. (Prospective; 75 a. Pneumocystis jiroveci
patients) b. Streptococcus pneumoniae
51. Martins CR. Cutaneous drug reactions associated with c. Influenza A
newer antiretroviral agents. J Drugs Dermatol. 2006;5(10):976- d. Haemophilus influenzae
982. (Review)
52. Maurer T, Rodrigues LK, Ameli N, et al. The effect of highly
active antiretroviral therapy on dermatologic disease in a 4. Nephrolithiasis is strongly associated with
longitudinal study of HIV type 1-infected women. Clin Infect which of the following HAART medications?
Dis. 2004;38(4):579-584. (Cross-sectional; 800 patients) a. Protease inhibitors
53. Centers for Disease Control and Prevention. PEP. Available b. Reverse transcriptase inhibitors
at: http://www.cdc.gov/hiv/basics/pep.html. Accessed
July 30, 2015. (CDC website)
c. Integrase inhibitors
54. Thomas R, Galanakis C, Vezina S, et al. Adherence to post- d. Nephrolithiasis is not a known complication
exposure prophylaxis (PEP) and incidence of HIV serocon- of HAART
version in a major North American cohort. PLoS ONE. 2015;
11;10(11):e0142534. (Prospective; 3547 patients) 5. Which of the following is associated with
increased risk of cerebrovascular accidents in
CME Questions patients with HIV?
a. Progressive multifocal leukoencephalopathy
Take This Test Online! b. Atherosclerosis
c. Central nervous system lymphoma
Current subscribers receive CME credit absolutely d. Higher CD4 counts
free by completing the following test. Each issue
includes 4 AMA PRA Category 1 CreditsTM, 4 ACEP 6. Which of the following is NOT a common eti-
Category I credits, 4 AAFP Prescribed credits, and 4 ology of diarrhea in HIV-infected patients on
Take This Test Online! HAART?
AOA Category 2A or 2B credits. Monthly online test-
ing is now available for current and archived issues. a. Clostridium difficile
To receive your free CME credits for this issue, scan b. Adverse medication effect
the QR code below with your smartphone or visit c. Viral gastroenteritis
www.ebmedicine.net/E0216. d. Mycobacterium avium complex
7. Which of the following statements about hepa-
tobiliary disease in HIV infection is FALSE?
a. Co-infection with either hepatitis B or
hepatitis C increases a person’s risk of
chronic hepatitis by 2 to 3 times compared to
1. The United States Department of Health and non–HIV-infected patients.
Human Services recommends treatment with b. HIV-infected patients with hepatobiliary
HAART for which of the following groups of complaints in the ED should receive
HIV-infected patients? laboratory testing with transaminases,
a. Patients with CD4 count < 350 cells/mm3 bilirubin, and lipase.
b. Patients with CD4 count < 500 cells/mm3 c. Hepatobiliary disease in HIV patients only
without opportunistic infection occurs in the presence of co-infection with
c. Patients with CD4 count > 500 cells/mm3 hepatitis B or hepatitis C.
with previous opportunistic infection d. Co-infection with hepatitis C affects up to
d. All of the above 80% of HIV patients, depending on risk
factors.
2. Which of the following factors is NOT impli-
cated in the increased risk of cardiovascular 8. Anemia is common in patients with HIV on
disease seen in patients with HIV? HAART. This is likely secondary to which of
a. History of smoking the following?
b. A systemic inflammatory response a. Medication side effect
associated with HIV infection b. Hemolysis
c. HAART c. A response to thrombocytopenia
d. Opportunistic infection d. Disseminated intravascular coagulation
February 2016 • www.ebmedicine.net 15 Mobile app access: www.ebmedicine.net/app
9. Factors associated with thromboembolic Physician CME Information
disease include all of the following EX- Date of Original Release: February 1, 2016. Date of most recent review: January 10, 2016.
Termination date: February 1, 2019.
CEPT:
Accreditation: EB Medicine is accredited by the Accreditation Council for Continuing Medical
a. Anemia Education (ACCME) to provide continuing medical education for physicians. This activity has been
planned and implemented in accordance with the Essential Areas and Policies of the ACCME.
b. Low CD4 count
Credit Designation: EB Medicine designates this enduring material for a maximum of 4 AMA PRA
c. High viral load Category 1 Credits™. Physicians should claim only the credit commensurate with the extent of
d. Indwelling central venous catheters their participation in the activity.
ACEP Accreditation: Emergency Medicine Practice is approved by the American College of
Emergency Physicians for 48 hours of ACEP Category I credit per annual subscription.
10. A person presents after having an unex- AAFP Accreditation: This Medical Journal activity, Emergency Medicine Practice, has been
pected exposure to HIV when the condom reviewed and is acceptable for up to 48 Prescribed credits by the American Academy of
Family Physicians per year. AAFP accreditation begins July 1, 2015. Term of approval is
of his HIV-infected partner broke during for one year from this date. Each issue is approved for 4 Prescribed credits. Credit may be
claimed for one year from the date of each issue. Physicians should claim only the credit
sexual intercourse. Which of the follow- commensurate with the extent of their participation in the activity.
ing is true? AOA Accreditation: Emergency Medicine Practice is eligible for up to 48 American
a. Initiation of treatment with Osteopathic Association Category 2-A or 2-B credit hours per year.
Needs Assessment: The need for this educational activity was determined by a survey
antiretroviral medication is of medical staff, including the editorial board of this publication; review of morbidity and
contraindicated after 36 hours mortality data from the CDC, AHA, NCHS, and ACEP; and evaluation of prior activities for
emergency physicians.
postexposure.
Target Audience: This enduring material is designed for emergency medicine physicians,
b. A negative HIV viral load in the physician assistants, nurse practitioners, and residents.
exposed person excludes exposure to Goals: Upon completion of this activity, you should be able to: (1) demonstrate medical
decision-making based on the strongest clinical evidence; (2) cost-effectively diagnose and
infection. treat the most critical presentations; and (3) describe the most common medicolegal pitfalls
c. PEP is most effective within 2 hours of for each topic covered.
Discussion of Investigational Information: As part of the journal, faculty may be presenting
exposure. investigational information about pharmaceutical products that is outside Food and Drug
d. PEP is only effective within 24 hours of Administration–approved labeling. Information presented as part of this activity is intended
solely as continuing medical education and is not intended to promote off-label use of any
exposure. pharmaceutical product.
Faculty Disclosure: It is the policy of EB Medicine to ensure objectivity, balance,
independence, transparency, and scientific rigor in all CME-sponsored educational activities.
All faculty participating in the planning or implementation of a sponsored activity are expected
to disclose to the audience any relevant financial relationships and to assist in resolving
any conflict of interest that may arise from the relationship. In compliance with all ACCME
Essentials, Standards, and Guidelines, all faculty for this CME activity were asked to complete
a full disclosure statement. The information received is as follows: Dr. Gutteridge, Dr.
Egan, Dr. Galjour, Dr. Merchant, Dr. Jagoda, Dr. Shah, Dr. Damilini, Dr. Toscano, and
their related parties report no significant financial interest or other relationship with
the manufacturer(s) of any commercial product(s) discussed in this educational
presentation.
Commercial Support: This issue of Emergency Medicine Practice did not receive any
commercial support.
Earning Credit: Two Convenient Methods: (1) Go online to www.ebmedicine.net/CME and
click on the title of the article. (2) Mail or fax the CME Answer And Evaluation Form (included
with your June and December issues) to EB Medicine.
Hardware/Software Requirements: You will need a Macintosh or PC to access the online
archived articles and CME testing.
Additional Policies: For additional policies, including our statement of conflict of interest, source
of funding, statement of informed consent, and statement of human and animal rights, visit
www.ebmedicine.net/policies.
CEO: Stephanie Williford Publisher: Suzanne Verity Senior Business Analyst: Robin Wilkinson Director of Editorial: Dorothy Whisenhunt
Senior Content Editor & CME Director: Erica Scott Content Editor: Cheryl Belton Editorial Content Coordinator: Angie Wallace
Director of Operations: Robin Salet Office Manager: Kiana Collier Client Data Associate: Paige Simpson
Director of Business Development: Susan Woodard Online Marketing Manager: Marcus Snow Client Services Associate: Cory Shrider
Direct all inquiries to: Subscription Information
EB Medicine Full annual subscription: $349 (includes 12 monthly evidence-based print
Phone: 1-800-249-5770 or 1-678-366-7933 issues; 48 AMA PRA Category 1 CreditsTM, 48 ACEP Category I credits, 48 AAFP
Fax: 1-770-500-1316 Prescribed credits, and 48 AOA Category 2A or 2B CME credits; and full online
and mobile app access to searchable archives and additional CME). Call
5550 Triangle Parkway, Suite 150
1-800-249-5770 or go to www.ebmedicine.net/subscribe to subscribe.
Norcross, GA 30092
E-mail: ebm@ebmedicine.net Individual issues: $39 (includes 4 CME credits). Call 1-800-249-5770 or go to
Website: www.ebmedicine.net www.ebmedicine.net/EMPissues to order.
To write a letter to the editor, please email: Group subscriptions at discounted rates are also available.
jagodamd@ebmedicine.net Contact groups@ebmedicine.net for more information.
Emergency Medicine Practice (ISSN Print: 1524-1971, ISSN Online: 1559-3908, ACID-FREE) is published monthly (12 times per year) by EB Medicine (5550 Triangle Parkway, Suite
150, Norcross, GA 30092). Opinions expressed are not necessarily those of this publication. Mention of products or services does not constitute endorsement. This publication is
intended as a general guide and is intended to supplement, rather than substitute, professional judgment. It covers a highly technical and complex subject and should not be used
for making specific medical decisions. The materials contained herein are not intended to establish policy, procedure, or standard of care. Copyright © 2016 EB Medicine. All rights
reserved. No part of this publication may be reproduced in any format without written consent of EB Medicine. This publication is intended for the use of the individual subscriber only
and may not be copied in whole or part or redistributed in any way without the publisher’s prior written permission.
Copyright © 2016 EB Medicine. All rights reserved. 16 Reprints: www.ebmedicine.net/empissues
You might also like
- Shoe Dog: A Memoir by the Creator of NikeFrom EverandShoe Dog: A Memoir by the Creator of NikeRating: 4.5 out of 5 stars4.5/5 (537)
- The Yellow House: A Memoir (2019 National Book Award Winner)From EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Rating: 4 out of 5 stars4/5 (98)
- Ventriculoperitoneal Shunt Complications in Children An Evidence-Based Approach To Emergency Department Management PDFDocument24 pagesVentriculoperitoneal Shunt Complications in Children An Evidence-Based Approach To Emergency Department Management PDFGavin TexeirraNo ratings yet
- Conversion PDFDocument2 pagesConversion PDFGavin TexeirraNo ratings yet
- 0115 Seizures and SEDocument28 pages0115 Seizures and SEGavin TexeirraNo ratings yet
- Scrotal Masses EvaluationDocument2 pagesScrotal Masses EvaluationGavin TexeirraNo ratings yet
- ATLS Case ScenarioDocument13 pagesATLS Case ScenarioGavin Texeirra97% (38)
- 0315 DVTDocument28 pages0315 DVTGavin TexeirraNo ratings yet
- Pulmonary EmbolismDocument9 pagesPulmonary EmbolismGavin Texeirra100% (1)
- Alcohol Screening QuestionnaireDocument2 pagesAlcohol Screening QuestionnaireGavin TexeirraNo ratings yet
- Home Epley HandoutsDocument4 pagesHome Epley HandoutsGavin Texeirra100% (1)
- BPPVDocument2 pagesBPPVGavin TexeirraNo ratings yet
- MRX Software Version 7 Instructions For UseDocument326 pagesMRX Software Version 7 Instructions For UseGavin TexeirraNo ratings yet
- Endometriosis With Hemorrhagic AscitiesDocument5 pagesEndometriosis With Hemorrhagic AscitiesGavin TexeirraNo ratings yet
- Philips Heartstart MRXDocument17 pagesPhilips Heartstart MRXGavin TexeirraNo ratings yet
- Pacemaker Data Collection From DeviceDocument6 pagesPacemaker Data Collection From DeviceGavin TexeirraNo ratings yet
- The HusiaDocument144 pagesThe HusiaGavin Texeirra100% (4)
- Artigo 16Document8 pagesArtigo 16Gavin TexeirraNo ratings yet
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeFrom EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeRating: 4 out of 5 stars4/5 (5794)
- The Little Book of Hygge: Danish Secrets to Happy LivingFrom EverandThe Little Book of Hygge: Danish Secrets to Happy LivingRating: 3.5 out of 5 stars3.5/5 (400)
- Grit: The Power of Passion and PerseveranceFrom EverandGrit: The Power of Passion and PerseveranceRating: 4 out of 5 stars4/5 (588)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureFrom EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureRating: 4.5 out of 5 stars4.5/5 (474)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryFrom EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryRating: 3.5 out of 5 stars3.5/5 (231)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceFrom EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceRating: 4 out of 5 stars4/5 (895)
- Team of Rivals: The Political Genius of Abraham LincolnFrom EverandTeam of Rivals: The Political Genius of Abraham LincolnRating: 4.5 out of 5 stars4.5/5 (234)
- Never Split the Difference: Negotiating As If Your Life Depended On ItFrom EverandNever Split the Difference: Negotiating As If Your Life Depended On ItRating: 4.5 out of 5 stars4.5/5 (838)
- The Emperor of All Maladies: A Biography of CancerFrom EverandThe Emperor of All Maladies: A Biography of CancerRating: 4.5 out of 5 stars4.5/5 (271)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaFrom EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaRating: 4.5 out of 5 stars4.5/5 (266)
- On Fire: The (Burning) Case for a Green New DealFrom EverandOn Fire: The (Burning) Case for a Green New DealRating: 4 out of 5 stars4/5 (74)
- The Unwinding: An Inner History of the New AmericaFrom EverandThe Unwinding: An Inner History of the New AmericaRating: 4 out of 5 stars4/5 (45)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersFrom EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersRating: 4.5 out of 5 stars4.5/5 (345)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyFrom EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyRating: 3.5 out of 5 stars3.5/5 (2259)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreFrom EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreRating: 4 out of 5 stars4/5 (1090)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)From EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Rating: 4.5 out of 5 stars4.5/5 (121)
- Her Body and Other Parties: StoriesFrom EverandHer Body and Other Parties: StoriesRating: 4 out of 5 stars4/5 (821)
- Obstetrics Midterms Rationale 2nd Sem 2018 2019Document21 pagesObstetrics Midterms Rationale 2nd Sem 2018 2019Gene Paulo UyNo ratings yet
- AttachmentDocument39 pagesAttachmentshmlniz100% (1)
- Research Article: Oral Care of Hospitalised Older Patients in The Acute Medical SettingDocument5 pagesResearch Article: Oral Care of Hospitalised Older Patients in The Acute Medical SettingMohammed Falih HassanNo ratings yet
- Case StudyDocument3 pagesCase StudyLouel VicitacionNo ratings yet
- GenpathDocument8 pagesGenpathNatural Science BiologyNo ratings yet
- IDP 11.13.19 11.14.19 Metal Implants White Paper - 0 PDFDocument152 pagesIDP 11.13.19 11.14.19 Metal Implants White Paper - 0 PDFVivek KhakharNo ratings yet
- Evidence-Based Guideline Summary: Evaluation, Diagnosis, and Management of Facioscapulohumeral Muscular DystrophyDocument10 pagesEvidence-Based Guideline Summary: Evaluation, Diagnosis, and Management of Facioscapulohumeral Muscular DystrophyFitria ChandraNo ratings yet
- D An Introduction: Physical Medicine and RehabilitationDocument33 pagesD An Introduction: Physical Medicine and RehabilitationChadNo ratings yet
- NephrologyDocument9 pagesNephrologyEliDavidNo ratings yet
- Needle Prick Injury & PreventionDocument17 pagesNeedle Prick Injury & Preventioniman zainuddinNo ratings yet
- Nursing Nclex 2005Document39 pagesNursing Nclex 2005Hasan A AsFourNo ratings yet
- SupradynDocument5 pagesSupradynashrayagrawalNo ratings yet
- New TNMDocument157 pagesNew TNMShouvik ChowdhuryNo ratings yet
- University of Zimbabwe Dissertation TopicsDocument4 pagesUniversity of Zimbabwe Dissertation TopicsCustomWritingPaperServiceCanada100% (1)
- Nurse Shift PDFDocument11 pagesNurse Shift PDFWisnu YogaNo ratings yet
- Siobhan (2017) - Smudging of The Motor Cortex Is Related To The Severity of Low Back PainDocument7 pagesSiobhan (2017) - Smudging of The Motor Cortex Is Related To The Severity of Low Back PainLuciana AraújoNo ratings yet
- Ultrasound Thesis TopicsDocument6 pagesUltrasound Thesis Topicsdw9x1bxb100% (2)
- Editorial: Dental Caries and OsteoporosisDocument2 pagesEditorial: Dental Caries and OsteoporosisBagis Emre GulNo ratings yet
- @MBS MedicalBooksStore 2020 CompressionDocument46 pages@MBS MedicalBooksStore 2020 CompressionTaufikNo ratings yet
- BIO 211 Chapter 18 AssignmentDocument20 pagesBIO 211 Chapter 18 Assignmentf1l2o3r4e5n6No ratings yet
- Management Thoracic Pain 2019Document9 pagesManagement Thoracic Pain 2019Lotte WeggemanNo ratings yet
- Guide PDFDocument84 pagesGuide PDFbiomeditechNo ratings yet
- Standard Coding Guideline ICD-10-TM 2006Document192 pagesStandard Coding Guideline ICD-10-TM 2006api-3835927100% (1)
- Radiologi Gastrointestinal (Noted)Document52 pagesRadiologi Gastrointestinal (Noted)desak 102018084No ratings yet
- Measuring Central Venous Pressure: Elaine ColeDocument8 pagesMeasuring Central Venous Pressure: Elaine ColednllkzaNo ratings yet
- Feeling GreatDocument243 pagesFeeling GreatSunny LamNo ratings yet
- TORCHDocument32 pagesTORCHJafar NoryNo ratings yet
- Travatan (Travoprost Ophthalmic Solution) 0.004% SterileDocument7 pagesTravatan (Travoprost Ophthalmic Solution) 0.004% SterileSyed Shariq AliNo ratings yet
- Basic Math Ability Exam A Relias Graded ADocument6 pagesBasic Math Ability Exam A Relias Graded ADebs MaxNo ratings yet