Professional Documents
Culture Documents
Open Reduction and Internal Fixation of Posterior Malleolar Fractures Using The Posterolateral Approach
Uploaded by
jmhinos4833Original Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Open Reduction and Internal Fixation of Posterior Malleolar Fractures Using The Posterolateral Approach
Uploaded by
jmhinos4833Copyright:
Available Formats
FOOT AND ANKLE
Open reduction and internal fixation of
posterior malleolar fractures using the
posterolateral approach
S. M. Verhage, Aims
F. Boot, Involvement of the posterior malleolus in fractures of the ankle probably adversely affects
I. B. Schipper, the functional outcome and may be associated with the development of post-traumatic
J. M. Hoogendoorn osteoarthritis. Anatomical reduction is a predictor of a successful outcome.
The purpose of this study was to describe the technique and short-term outcome of
From Medisch patients with trimalleolar fractures, who were treated surgically using a posterolateral
Centrum approach in our hospital between 2010 and 2014.
Haaglanden, The
Patients and Methods
Hague, The The study involved 52 patients. Their mean age was 49 years (22 to 79). There were 41 (79%)
Netherlands AO 44B-type and 11 (21%) 44C-type fractures. The mean size of the posterior fragment was
27% (10% to 52%) of the tibiotalar joint surface.
Results
Reduction was anatomical in all patients with a residual step in the articular surface of ≤ 1 mm.
In nine of the C-type fractures (82%), the syndesmosis was stable after fixation of the
posterior fragment and a syndesmosis screw was not required. Apart from one superficial
wound infection, there were no wound healing problems. At a mean radiological follow-up
of 34 weeks (seven to 131), one patient with a 44C-type fracture had widening of the
syndesmosis which required further surgery.
Conclusion
We conclude that the posterolateral surgical approach to the ankle gives adequate access to
the posterior malleolus, allowing its anatomical reduction and stable fixation: it has few
complications.
S. M. Verhage, MD, Resident
Surgery, Secretariaat Surgery
Take home message: Fixation of the posterior malleolus in trimalleolar fractures can be
F. Boot, MD, Resident
Emergeny Medicine, easily done via the posterolateral approach whereby anatomical reduction and stable
Secretariaat Surgery
fixation can be reached due to adequate visualisation of the fracture.
MC Haaglanden, locatie
Westeinde, Lijnbaan 32, 2512
VA, The Hague, The Cite this article: Bone Joint J 2016;98-B:812–17.
Netherlands,
The treatment of fractures of the ankle which to posterior (A to P) screw fixation of the pos-
I. B. Schipper, MD, PhD,
Professor of Trauma Surgery, involve the posterior malleolus remains con- terior malleolus are that anatomical reduction
Secretariaat Surgery
troversial. Although there is some recent evi- is more difficult due to the interposition of soft
J. M. Hoogendoorn, MD,
PhD, Orthopaedic Trauma dence that a fracture of the posterior malleolus tissue or loose bony fragments, that it is hard
Surgeon, Secretariaat Surgery
will result in an increased incidence of post- to assess reduction satisfactorily using an
Leiden University Medical
Center, Albinusdreef 2, 2333 traumatic osteoarthritis (OA) and therefore a image intensifier, and that the fixation of small
ZA, Leiden, The Netherlands.
worse functional outcome, there is no agree- or comminuted fragments is technically diffi-
Correspondence should be sent ment as to how such fractures should be cult. Incomplete reduction leads to a residual
to Mr S. M. Verhage; e-mail:
sanverhage@hotmail.com treated.1-3 Usually the posterior malleolus is step in the articular surface.2,6 A recently pub-
only fixed if the fragment exceeds 25% of the lished cohort study from our hospital showed a
©2016 The British Editorial
Society of Bone & Joint articular surface or if there is instability of the persisting articular step of > 1 mm in 42% of
Surgery ankle joint after fixation of the medial and lat- 131 cases after percutaneous reduction and A
doi:10.1302/0301-620X.98B6.
36497 $2.00 eral malleoli.4,5 to P screw fixation of the posterior malleolus.2
It has recently been shown that anatomical We favour open, anatomical reduction of
Bone Joint J
2016;98-B:812–17. reduction is an important predictor of a suc- posterior malleolar fragments using a postero-
Received 11 May 2015; cessful functional outcome.1-6 The disadvan- lateral approach with the patient in a prone
Accepted after revision 8
February 2016 tages of percutaneous reduction with anterior position. In this article we describe the
812 THE BONE & JOINT JOURNAL
OPEN REDUCTION AND INTERNAL FIXATION OF POSTERIOR MALLEOLAR FRACTURES USING THE POSTEROLATERAL APPROACH 813
Table I. Basic characteristics (n = 52)
Age (yrs) 49
Men n, (%) 11 (21)
Follow-up (wks, mean, range) 34 (7 to 131)
ASA 1 n, (%) 20 (39)
ASA 2 n, (%) 25 (48)
ASA 3 n, (%) 7 (13)
Diabetes Mellitus n, (%) 4 (8)
Body Mass Index (mean) 29 (22 to 50)
Smoking n, (%) 16 (31)
ASA, American Society of Anesthesiologists
Fig. 1
Radiographs showing trimalleolar fracture, Lauge-
Hansen type SE4.
Table II. Fracture characteristics (n = 52)
Fracture subluxation n, (%) 40 (77)
Size of posterior fragment (%) 27
Medial malleolar fracture n, (%) 43 (83)
Supination-External Rotation stage 3 n, (%) 2 (4)
Supination-External Rotation stage 4 n, (%) 38 (73)
Pronation-Abduction stage 3 n, (%) 1 (2)
Pronation-External Rotation stage 3 n, (%) 1 (2)
Pronation-External Rotation stage 4 n, (%) 10 (19)
AO-type B3 n, (%) 41 (79)
AO-type C2 n, (%) 5 (10)
AO-type C3 n, (%) 6 (12)
AO, Arbeitsgemeinschaft für Osteosynthesefragen
Fig. 2
Photograph showing posterolateral incision.
technique and its short-term outcome in 52 patients with a radiographs by two of the authors (SV, JH). Reduction was
trimalleolar fracture who were treated using this approach. considered anatomical if any displacement was ≤ 1 mm.
Ethical approval for the study was not deemed to be
Patients and Methods required by the local ethical committee.
Between 2010 and 2014, 52 patients with a trimalleolar Technique. The illustrated example shows a patient with a
fracture of the ankle were treated at our level one trauma trimalleolar fracture, type AO 44B3 or Lauge-Hansen supi-
centre using the posterolateral approach to reduce and fix nation-external rotation 4 (Fig. 1) of the left ankle. The
the posterior malleolus. There were 11 men and 41 women patient is prone for the operation. The distal part of the
with a mean age of 49 years (22 to 79). A total of 40 lower leg is placed on a foam cushion with the knee slightly
patients (77%) had a fracture subluxation. Baseline charac- flexed to allow maximal dorsiflexion of the ankle during
teristics of these patients and their fractures are shown in reduction. A longitudinal incision is made between the lat-
Tables I and II. eral border of the Achilles tendon and the medial border of
The size of the posterior malleolar fragment was calcu- the fibula (Fig. 2). Fixation of the fibular fracture before
lated as the percentage of the tibiotalar surface area fixation of the posterior malleolar fracture has its advan-
involved. The anteroposterior (AP) diameter of the frag- tages and disadvantages. Fixation of the fibula first will, in
ment was measured on the lateral radiograph, or CT scan if most cases, lead to an adequate reduction of the posterior
available, and divided by the total AP diameter of the tibi- malleolar fracture. Sometimes, however, its fixation will
otalar articular surface. limit the movement of the posterior malleolar fracture and
The mean size of the posterior malleolar fragment was therefore interfere with reduction. In our opinion, dissec-
27% (10% to 52%) of the joint surface (Table II). There tion of both fractures and careful anatomical reduction of
was comminution of the fragment in 16 patients (31%). An both is the best strategy. Here, we describe the fixation of
external fixator was used prior to definitive reconstruction the fibular fracture first.
in 22 patients (42%) due to soft tissue swelling and/or blis- During blunt subcutaneous dissection onto the peroneal
tering. The mean follow-up was 34 weeks (seven to 131). tendon, care is taken to avoid injury to the sural nerve. The
The congruency of the joint (step-off) and the quality of posterior aspect of the fibula is easily reached through the
reduction and fixation of the lateral, medial and posterior interval just lateral to the peroneal tendon. After debriding
malleoli was assessed on the post-operative and follow-up the fracture, it can be reduced and fixed using lag screws
VOL. 98-B, No. 6, JUNE 2016
814 S. M. VERHAGE, F. BOOT, I. B. SCHIPPER, J. M. HOOGENDOORN
Fig. 3 Fig. 5
Photograph showing lag screws placed to reduce the Radiograph and photograph showing placement of temporary Kirsch-
fracture of the fibula. ner wires followed by a buttress plate.
Fig. 4 Fig. 6
Photograph showing medial retraction of the mus- Post-operative radiographs of the fixed trimalleolar fracture.
cle belly of flexor hallucis longus; this will show the
posterior fracture.
and/or a buttress plate (Fig. 3). The belly of flexor hallucis layers after confirmation of reduction (Fig. 6). Post-
longus is bluntly dissected off the interosseus membrane operatively a cast or bandage is retained for a maximum of
and the lateral side of the tibia through the interval medial two weeks: non-weight-bearing continues for six weeks.
to the peroneal tendon. Particular care is taken to avoid
injury to the peroneal artery and its smaller branches. By Results
retracting the muscle belly medially, the posterior aspect of In 12 patients (23%), the fragment was fixed using lag
the tibia can be seen. The periosteum is incised to expose screws only: in 40 (77%) it was fixed using a buttress plate.
the posterior malleolar fracture (Fig. 4). It is important not After fixation, 50 ankles (96%) were found to be stable
to damage the posterior inferior tibiofibular ligament when clinically tested (Cotton test):7 no additional syndes-
(PITFL) at this stage. The posterior malleolar fragment is mosis screws were needed in these patients, even in those
almost always displaced in a craniolateral direction by trac- with AO type 44C fractures. A syndesmosis screw was
tion from the PITFL. Loose fragments can be removed by required in two patients (4%).
levering the fragment distally. After maximal dorsiflexion Post-operative radiographs showed an anatomical reduc-
of the ankle, a dental pick or bone tamp can be used to tion with a congruent ankle joint in all cases. There was one
reduce the posterior fragment. An anatomical reduction is superficial wound infection, which was successfully treated
almost always achieved and is held temporarily by Kirsch- with antibiotics. Two patients (4%) suffered from a tempo-
ner (K-) wires. When anatomical reduction is confirmed on rary numbness in the distribution of the lateral sural cuta-
image intensification, fixation is undertaken using either neous nerve. This resolved unremarkably in both within a
lag screws or a slightly prebent three-hole buttress plate few weeks. Congruency was lost in one patient with an AO-
(Fig. 5). Placement of a lag screw through the most distal type 44C fracture, and a syndesmosis screw was introduced
hole of the plate can help to close any possible gaps. By five days post-operatively which stabilised the ankle joint.
slightly internally rotating the lower leg, the medial malle- Congruency was maintained after all other patients bore
olus can be approached and fixed. The incision is closed in weight. One patient had a pulmonary embolus post-opera-
THE BONE & JOINT JOURNAL
OPEN REDUCTION AND INTERNAL FIXATION OF POSTERIOR MALLEOLAR FRACTURES USING THE POSTEROLATERAL APPROACH 815
larger than 25% or 10%, respectively. Mingo-Robinet et
al5 suggest in a retrospective study involving 45 trimalleolar
fractures, that anatomical reduction, and not size of the
fragment, was the most important determinant of outcome.
In 2013 we conducted a retrospective study of 131
patients, in whom outcome was assessed using the American
College of Foot and Ankle Surgeons (AOFAS) score, at a
mean of 6.9 years (2.5 to 15.9) after internal fixation of a tri-
malleolar fracture of the ankle. Patients with a persistent
articular step of > 1 mm after fixation of the posterior malle-
olus were significantly more likely to develop post-traumatic
OA than those with no articular step (46% versus 25%,
p = 0.02). This was the case in patients with medium-sized
posterior malleolar fragments (5% to 25% of the articular
Fig. 7a Fig. 7b surface) as well as in those with large (> 25%) fragments.
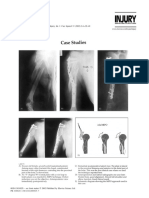
Pre-operative radiographs of AO-44C2 fracture with posterior fragment. The size of the fragment (larger than 25% of the involved
articular surface) was the leading indication for fixation of
tively but recovered fully following six months of anticoag- the posterior malleolus. In the sub-group of patients (24
ulation. One patient had a second injury within six months patients) who underwent fixation of the posterior fragment,
which caused a further trimalleolar fracture which was sim- the functional outcome was no better than in the sub-group
ilarly treated. without fixation. There was a persistent articular step of > 1
In 15 patients (29%), the medial and lateral hardware mm in ten (42%) of the fixed posterior malleolar fragments,
was removed at a later date after consolidation of the frac- compared with 46 (55%) of those in whom the posterior
ture. All material used to fix the posterior malleolus was malleolar fragment was not fixed. In the study period, nearly
left in place. all posterior fragments which were fixed were reduced by lig-
A total of four patients developed post-traumatic osteo- amentotaxis and fixation was undertaken percutaneously in
arthritis in this follow-up period as a result of cartilage an AP direction.2 The results of this retrospective study
damage of the tibial plafond and talus on lateral or mortise strengthened us in our belief to strive for an anatomical,
radiographs. One patient with grade three OA8 of the ankle open reduction.
joint underwent prosthetic replacement two years after the Similar results have been published in a recent Chinese
initial trauma. study which described 102 patients with a trimalleolar frac-
ture.3 Mean follow-up was 2.8 years (0.5 to 8.5 years). In
Discussion all, 42 patients underwent fixation of the posterior frag-
In recent years increased attention has been paid to the ment, 23 of them posterior to anterior fixation. Fixation of
importance of anatomical reduction and internal fixation the posterior fragment was performed if fragment was
of the posterior malleolus.4-6,9,10 around or larger than 25% of the involved articular surface
It is assumed that a congruent ankle joint without a step as measured on plain lateral radiographs. Functional out-
in the articular surface is needed to achieve a good func- come was assessed by the AOFAS score and osteoarthritis
tional outcome in patients who undergo surgical treatment was assessed on plain radiographs. A persistent articular
for a fracture of the ankle. Inadequate reduction of the pos- step of > 1 mm was seen in 24 (24%) patients and this cor-
terior malleolar fragment with a persistent articular step related with a worse functional outcome.3 In the fixation
diminishes the tibiotalar articular surface and leads to group a persistent articular step of >1 mm was seen in 14
altered biomechanics in the ankle joint. A change in peak (33%) patients.
pressure distribution probably plays an important role in Anatomical reduction and fixation of the posterior
the development of post-traumatic OA.1,11 There is no con- malleolar fragment also reconstructs the fibular notch and
sensus about the main cause of post-traumatic OA after a the syndesmosis. Cadaver studies show that this technique
fracture of the ankle.12 is biomechanically superior to the use of syndesmosis
According to the AO guidelines,13 a posterior malleolar screws in injuries proximal to the syndesmosis.9 In AO type
fragment is usually only reduced and fixed if it involves > 44C fractures, even small posterior malleolar fragments
25% of the tibiotalar articular surface or when there is per- can be fixed. Syndesmosis screws are not needed if the syn-
sistent instability after fixation of the medial and lateral desmosis is clinically stable after fixation.10
malleoli.13 The recommendations are partially based on In Figures 7 to 9, we present a case (AO-44C2 fracture)
biomechanical studies.11 Clinical studies are not consistent with a relatively small posterior fragment, shown on pre-
in the recommendation of the size of posterior fragment operative CT scans with comminution and several intra-
that requires fixation. De Vries et al14 and Langenhuijsen et articular fragments (Fig. 8). The fibula was dislocated.
al15 recommend fixation of posterior fragments which are After fixation of the posterior fragment with a buttress
VOL. 98-B, No. 6, JUNE 2016
816 S. M. VERHAGE, F. BOOT, I. B. SCHIPPER, J. M. HOOGENDOORN
Fig. 8a Fig. 8b
Radiograph and CT scan showing comminution of the posterior fragment with several
intra-articular fracture fragments. The fibula is rotated out of its notch on the tibia.
Fig. 9a Fig. 9b Fig. 9c
Post-operative CT-scans (a and b) and radiograph (c) showing adequate reduction of the syndesmosis.
plate the joint was congruent and the fibula was reduced assessing articular congruency.16 Another limitation is
(Fig. 9). The syndesmosis was stable. that only trimalleolar fractures which were fixed using a
One patient developed an incongruent ankle and a syn- posterolateral approach are included. There are no data
desmosis screw was introduced at a further operation. This available on unfixed posterior malleolar fragments or
emphasises the need for adequate clinical testing at the end those treated with ‘anterior to posterior’ percutaneous
of the operation. When there is any doubt about the stabil- fixation.
ity of the ankle after fixation of the posterior malleolar Little has been published on the subject of the technique
fragment there should be a low threshold for using a syn- of reduction and fixation for these fractures. Traditionally
desmosis screw. an indirect reduction technique by ligamentotaxis or percu-
There are several limitations to this study. First, it is ret- taneous reduction using a Weber clamp followed by percu-
rospective with data gathered from the notes. This aim was taneous screw fixation in an AP direction is used.17,18 This
to describe the technical advantages of the posterolateral technique does not lead to anatomical reduction of the frag-
approach with better radiological outcome and the study ment in many patients. The correct positioning of the screw
was not designed to report functional outcome. Secondly, in smaller fragments can be difficult. In recent years, several
the size of posterior fragment and articular step in the ankle authors have recommended the posterolateral approach
joint was measured on plain radiographs in most patients with the patient in a prone position with open reduction of
because this is daily practice world-wide. CT scans were the posterior malleolar fragment followed by internal fixa-
not available for most patients. In our opinion, measure- tion with lag screws and/or a buttress plate, reporting few
ment on a plain radiograph is not as good as measurement complications and a good functional outcome.2,3,10,19-21 We
by CT scans. Future studies should only use CT scans when confirm these findings in this study.
THE BONE & JOINT JOURNAL
OPEN REDUCTION AND INTERNAL FIXATION OF POSTERIOR MALLEOLAR FRACTURES USING THE POSTEROLATERAL APPROACH 817
This technique gives an adequate view of the fracture, an 6. Berkes MB, Little MTM, Lazaro LE, et al. Articular congruity is associated with
anatomical reduction in most cases and sound fixation of short-term clinical outcomes of operatively treated SER IV ankle fractures. J Bone
Joint Surg [Am] 2013;95-A:1769–1775.
the posterior malleolar fragment.19,20 Another advantage is 7. Mizel MS. Technique tip: a revised method of the Cotton test for intra-operative eval-
that small fragments are easier to fix and small intra-artic- uation of syndesmotic injuries. Foot Ankle Int 2003;24:86–87.
ular fragments can be removed from the site of the fracture. 8. Kellgren JH, Lawrence JS. Radiological assessment of osteoarthrosis. Ann Rheum
Dis 1957;16:494–502.
There has, as yet, been no prospective study to investigate
9. Gardner MJ, Brodsky A, Briggs SM, Nielson JH, Lorich DG. Fixation of poste-
the functional and radiological outcome after anatomical rior malleolar fractures provides greater syndesmotic stability. Clin Orthop Relat Res
reduction and fixation of medium-sized posterior malleolar 2006;447:165–171.
fragments (those involving between 5% and 25% of the 10. Miller AN, Carroll EA, Parker RJ, Helfet DL, Lorich DG. Posterior malleolar sta-
bilization of syndesmotic injuries is equivalent to screw fixation. Clin Orthop Relat Res
articular surface). Whether anatomical reduction and fixa- 2010 Apr;468:1129–1135.
tion of these fragments leads to a better functional outcome 11. Fitzpatrick DC, Otto JK, McKinley TO, Marsh JL, Brown TD. Kinematic and con-
and a reduced rate of post-traumatic OA therefore remains tact stress analysis of posterior malleolus fractures of the ankle. J Orthop Trauma
2004;18:271–278.
unknown. We are currently involved in two multicentre,
12. Odak S, Ahluwalia R, Unnikrishnan P, Hennessy M, Platt S. Management of
randomised trials, which are attempting to answer this posterior malleolar fractures. A systematic review. J Foot Ankle Surg 2016;55:140–
question (the POSTFIX and POSTFIX-C trials). 145.
13. No authors listed. AO Foundation. www2.aofoundation.org (date last accessed 04
Author contributions: May 2016).
S. M. Verhage: Data collection, Data analysis, Writing the paper.
F. Boot: Data collection, Data analysis, Writing the paper. 14. De Vries JS, Wijgman AJ, Sierevelt IN, Schaap GR. Long-term results of ankle
I. B. Schipper: Data analysis, Writing and correcting the paper. fractures with a posterior malleolar fragment. J Foot Ankle Surg 2005;44:211–217.
J. M. Hoogendoorn: Data analysis, Performed surgeries, Writing the paper. 15. Langenhuijsen JF, Heetveld MJ, Ultee JM, Steller EP, Butzelaar RM. Results
No benefits in any form have been received or will be received from a commer- of ankle fractures with involvement of the posterior tibial margin. J Trauma
cial party related directly or indirectly to the subject of this article. 2002;53:55–60.
16. Verhage SM, Rhemrev SJ, Keizer SB, Quarles van Ufford HM, Hoogendoorn
This article was primary edited by J. Scott and first proof edited by A. C. Ross
JM. Interobserver variation in classification of malleolar fractures. Skeletal Radiol
2015;44:1435–1439.
References 17. Tornetta P 3rd, Ricci W, Nork S, Collinge C, Steen B. The posterolateral
approach to the tibia for displaced posterior malleolar injuries. J Orthop Trauma
1. van den Bekerom MP, Haverkamp D, Kloen P. Biomechanical and clinical evalu- 2011;25:123–126 .
ation of posterior malleolar fractures. A systematic review of the literature. J Trauma
2009;66:279–284. 18. Talbot M, Steenblock TR, Cole PA. Posterolateral approach for open reduction and
internal fixation of trimalleolar ankle fractures. Can J Surg 2005;48:487–490.
2. Drijfhout van Hooff CC, Verhage SM, Hoogendoorn JM. Influence of fragment
size and postoperative joint congruency on long-term outcome of posterior malleolar 19. Forberger J, Sabandal PV, Dietrich M, et al. Posterolateral approach to the dis-
fractures. Foot Ankle Int 2015;36;673–678. placed posterior malleolus: functional outcome and local morbidity. Foot Ankle Int
3. Xu HL, Li X, Zhang DY, et al. A retrospective study of posterior malleolus fractures. 2009;30:309–314.
Int Orthop 2012;36:1929–1936. 20. O’Connor TJ, Mueller B, Ly TV, et al. “A to P” screw vs posterolateral plate for
4. McDaniel WJ, Wilson FC. Trimalleolar fractures of the ankle. An end result study. posterior malleolus fixation in trimalleolar ankle fractures. J Orthop Trauma
Clin Orthop Relat Res 1977;122:37–45. 2015;29:151–156.
5. Mingo-Robinet J, López-Durán L, Galeote JE, Martinez-Cervell C. Ankle frac- 21. Ruokun H, Ming X, Zhihong X, et al. Postoperative radiographic and clinical
tures with posterior malleolar fragment: management and results. J Foot Ankle Surg assessment of the treatment of posterior tibial plafond fractures using a posterior lat-
2011;50:141–145. eral incisional approach. J Foot Ankle Surg 2014;53:678–682.
VOL. 98-B, No. 6, JUNE 2016
You might also like
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryFrom EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryRating: 3.5 out of 5 stars3.5/5 (231)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)From EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Rating: 4.5 out of 5 stars4.5/5 (119)
- Never Split the Difference: Negotiating As If Your Life Depended On ItFrom EverandNever Split the Difference: Negotiating As If Your Life Depended On ItRating: 4.5 out of 5 stars4.5/5 (838)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaFrom EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaRating: 4.5 out of 5 stars4.5/5 (265)
- The Little Book of Hygge: Danish Secrets to Happy LivingFrom EverandThe Little Book of Hygge: Danish Secrets to Happy LivingRating: 3.5 out of 5 stars3.5/5 (399)
- Grit: The Power of Passion and PerseveranceFrom EverandGrit: The Power of Passion and PerseveranceRating: 4 out of 5 stars4/5 (587)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyFrom EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyRating: 3.5 out of 5 stars3.5/5 (2219)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeFrom EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeRating: 4 out of 5 stars4/5 (5794)
- Team of Rivals: The Political Genius of Abraham LincolnFrom EverandTeam of Rivals: The Political Genius of Abraham LincolnRating: 4.5 out of 5 stars4.5/5 (234)
- Shoe Dog: A Memoir by the Creator of NikeFrom EverandShoe Dog: A Memoir by the Creator of NikeRating: 4.5 out of 5 stars4.5/5 (537)
- The Emperor of All Maladies: A Biography of CancerFrom EverandThe Emperor of All Maladies: A Biography of CancerRating: 4.5 out of 5 stars4.5/5 (271)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreFrom EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreRating: 4 out of 5 stars4/5 (1090)
- Her Body and Other Parties: StoriesFrom EverandHer Body and Other Parties: StoriesRating: 4 out of 5 stars4/5 (821)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersFrom EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersRating: 4.5 out of 5 stars4.5/5 (344)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceFrom EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceRating: 4 out of 5 stars4/5 (890)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureFrom EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureRating: 4.5 out of 5 stars4.5/5 (474)
- Practical Visual Inspection of WeldsDocument40 pagesPractical Visual Inspection of WeldsAmit Sharma100% (1)
- The Unwinding: An Inner History of the New AmericaFrom EverandThe Unwinding: An Inner History of the New AmericaRating: 4 out of 5 stars4/5 (45)
- The Yellow House: A Memoir (2019 National Book Award Winner)From EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Rating: 4 out of 5 stars4/5 (98)
- Book Splint Cast (Ghips)Document293 pagesBook Splint Cast (Ghips)babac88100% (2)
- On Fire: The (Burning) Case for a Green New DealFrom EverandOn Fire: The (Burning) Case for a Green New DealRating: 4 out of 5 stars4/5 (73)
- Anatomy VivaDocument126 pagesAnatomy VivaBayar A. AhmedNo ratings yet
- Wheel Horse by YearDocument14 pagesWheel Horse by YearNeil SmallwoodNo ratings yet
- PRECOMMISSIONING and COMMISSIONING PROCEDURE FOR CARD ACCESS CONTROL SYSTEMDocument3 pagesPRECOMMISSIONING and COMMISSIONING PROCEDURE FOR CARD ACCESS CONTROL SYSTEMHumaid ShaikhNo ratings yet
- Tank Cleaning ConsiderationsDocument1 pageTank Cleaning ConsiderationsAdele PollardNo ratings yet
- Fabrication and Installation of Vertical Steel Pressure ShaftDocument23 pagesFabrication and Installation of Vertical Steel Pressure ShaftPasan RajasingheNo ratings yet
- Peaditrician All IndiaDocument66 pagesPeaditrician All IndiaGIRISH JOSHINo ratings yet
- Ukite 2011Document123 pagesUkite 2011pikacu19650% (2)
- Chapter 11 Blood Specimen Handling: Phlebotomy, 5e (Booth)Document35 pagesChapter 11 Blood Specimen Handling: Phlebotomy, 5e (Booth)Carol Reed100% (2)
- RADIO 250 (8) LEC 11 Introduction To Interventional RadiologyDocument4 pagesRADIO 250 (8) LEC 11 Introduction To Interventional Radiologyjmhinos4833No ratings yet
- 10.1016@s0020 13830200064 5Document27 pages10.1016@s0020 13830200064 5jmhinos4833No ratings yet
- 10.1016@s0020 13830200064 5 3Document27 pages10.1016@s0020 13830200064 5 3jmhinos4833No ratings yet
- 10.1016@s0020 13830200065 7Document12 pages10.1016@s0020 13830200065 7jmhinos4833No ratings yet
- 10.1016@s0020 13830200064 5 2Document27 pages10.1016@s0020 13830200064 5 2jmhinos4833No ratings yet
- 1 s2.0 S1877056818302299 MainDocument7 pages1 s2.0 S1877056818302299 MainPablo MirandaNo ratings yet
- Radiographic Measurements of Normal Elbows: Clinical Relevance To Olecranon FracturesDocument4 pagesRadiographic Measurements of Normal Elbows: Clinical Relevance To Olecranon Fracturesjmhinos4833No ratings yet
- THE Congenital Discoid Meniscus: From The Departnzent of Orihopaedic Surgery, University of Si AndrewsDocument12 pagesTHE Congenital Discoid Meniscus: From The Departnzent of Orihopaedic Surgery, University of Si Andrewsjmhinos4833No ratings yet
- 1 s2.0 S1877056812001089 MainDocument6 pages1 s2.0 S1877056812001089 Mainjmhinos4833No ratings yet
- DYMAX International Orthopedic Instruments CatalogDocument61 pagesDYMAX International Orthopedic Instruments Catalogjmhinos4833No ratings yet
- 10.1016@s0020 13830200062 1Document1 page10.1016@s0020 13830200062 1jmhinos4833No ratings yet
- Fluoroscopic Analysis of The Kinematics of Deep Exion in Total Knee ArthroplastyDocument4 pagesFluoroscopic Analysis of The Kinematics of Deep Exion in Total Knee Arthroplastyjmhinos4833No ratings yet
- A Biomechanical Evaluation OF THE Gamma Nail: From The Hospitalfor Joint Diseases, New YorkDocument6 pagesA Biomechanical Evaluation OF THE Gamma Nail: From The Hospitalfor Joint Diseases, New Yorkjmhinos4833No ratings yet
- Z. Al-Aubaidi, A. Fette - Orthopedic Surgery-Intech (2012) PDFDocument232 pagesZ. Al-Aubaidi, A. Fette - Orthopedic Surgery-Intech (2012) PDFjmhinos4833No ratings yet
- DYMAX International Orthopedic Instruments CatalogDocument61 pagesDYMAX International Orthopedic Instruments Catalogjmhinos4833No ratings yet
- Depliant RadiusDocument2 pagesDepliant Radiusjmhinos4833No ratings yet
- Laxo Tenso Contractura Relief ExercisesDocument32 pagesLaxo Tenso Contractura Relief Exercisesjmhinos4833No ratings yet
- Endobutton CL Ultra Fixation DeviceDocument2 pagesEndobutton CL Ultra Fixation Devicejmhinos48330% (1)
- Techniques in Hand Upper Extremity Surgery (B-Ok - Xyz) - 2Document76 pagesTechniques in Hand Upper Extremity Surgery (B-Ok - Xyz) - 2jmhinos4833No ratings yet
- The Posterolateral Approach To The Tibia For Displaced Posterior Malleolar InjuriesDocument4 pagesThe Posterolateral Approach To The Tibia For Displaced Posterior Malleolar Injuriesjmhinos4833No ratings yet
- RADIO 250 (8) LEC 09 Musculoskeletal RadiologyDocument4 pagesRADIO 250 (8) LEC 09 Musculoskeletal Radiologyjmhinos4833No ratings yet
- CalcaneoPDF - Js ViewerDocument158 pagesCalcaneoPDF - Js Viewerjmhinos4833No ratings yet
- Broach TrialDocument1 pageBroach Trialjmhinos4833No ratings yet
- Intraoperative Estimation of Tip-Apex Distance: James Robert Berstock, MBCHB, Mrcs and Oliver James Bradford, MBCHB, MrcsDocument1 pageIntraoperative Estimation of Tip-Apex Distance: James Robert Berstock, MBCHB, Mrcs and Oliver James Bradford, MBCHB, Mrcsjmhinos4833No ratings yet
- Exsanguination of The Upper LimbDocument2 pagesExsanguination of The Upper Limbjmhinos4833No ratings yet
- RADIO 250 (8) LEC 09 Musculoskeletal RadiologyDocument4 pagesRADIO 250 (8) LEC 09 Musculoskeletal Radiologyjmhinos4833No ratings yet
- (RADIO 250) LEC 11 Pediatric RadiologyDocument10 pages(RADIO 250) LEC 11 Pediatric Radiologyjmhinos4833No ratings yet
- Carbon Steel Alloys Steel, Pipe Dimension With Weight Test Pressures According To ANSI B36, 10 For ASTM A53/A 106/API 5L/A335/ SpecificationDocument6 pagesCarbon Steel Alloys Steel, Pipe Dimension With Weight Test Pressures According To ANSI B36, 10 For ASTM A53/A 106/API 5L/A335/ SpecificationsanjibkrjanaNo ratings yet
- Idioma Extranjero I R5Document4 pagesIdioma Extranjero I R5EDWARD ASAEL SANTIAGO BENITEZNo ratings yet
- Ascha_ASJ19_Nonsurgical Management of Facial Masculinization and FeminizationDocument15 pagesAscha_ASJ19_Nonsurgical Management of Facial Masculinization and Feminizationallen.515No ratings yet
- Research Journal DNA PolymeraseDocument12 pagesResearch Journal DNA PolymeraseMauhibahYumnaNo ratings yet
- Spring Creek Sun August 27Document24 pagesSpring Creek Sun August 27amoses88No ratings yet
- Solution Manual For Safety Health and Environmental Concepts For The Process Industry 2nd EditionDocument8 pagesSolution Manual For Safety Health and Environmental Concepts For The Process Industry 2nd EditionRobert Hornback100% (34)
- Cyclopropane, Ethynyl - (Cas 6746-94-7) MSDS: CyclopropylacetyleneDocument5 pagesCyclopropane, Ethynyl - (Cas 6746-94-7) MSDS: CyclopropylacetyleneMiMi JoyNo ratings yet
- Rhodes-Solutions Ch2 PDFDocument16 pagesRhodes-Solutions Ch2 PDFOscar GarzónNo ratings yet
- MBBS Final Part-I (Winter Session) Time Table (Jan 2023)Document1 pageMBBS Final Part-I (Winter Session) Time Table (Jan 2023)crystal mindNo ratings yet
- Mechanical Engineering Paper 1 SummaryDocument20 pagesMechanical Engineering Paper 1 SummaryK.v.SinghNo ratings yet
- Mind Map Burn & BleedingDocument2 pagesMind Map Burn & BleedingUlfia KhoirinnissaNo ratings yet
- Annotated Bibliography For Elder AbuseDocument6 pagesAnnotated Bibliography For Elder Abuseapi-302577490No ratings yet
- International Journal of Academic Research Vol. 4. No. 4. July, 2012Document5 pagesInternational Journal of Academic Research Vol. 4. No. 4. July, 2012Sulaiman MukmininNo ratings yet
- P Hazz Er Enforcer Us A ManualDocument23 pagesP Hazz Er Enforcer Us A ManualArif TjoeripNo ratings yet
- Oral Dislocation Rehabilitation Program - FirstDocument2 pagesOral Dislocation Rehabilitation Program - FirstPriyaki SebastianNo ratings yet
- Metals and Metallurgy: Theodore L. Brown H. Eugene Lemay, Jr. and Bruce E. BurstenDocument43 pagesMetals and Metallurgy: Theodore L. Brown H. Eugene Lemay, Jr. and Bruce E. BurstenDheeraj KumarNo ratings yet
- Optimize soil preparation with a versatile mini tillerDocument2 pagesOptimize soil preparation with a versatile mini tillerRickson Viahul Rayan C100% (1)
- Final Final PosterDocument1 pageFinal Final Posterapi-486056653No ratings yet
- Vitamin D DeficinyDocument11 pagesVitamin D DeficinyسالمNo ratings yet
- Manual NSD70D EnglishDocument155 pagesManual NSD70D Englishnarvis1No ratings yet
- MAstering IATFDocument20 pagesMAstering IATFGyanesh_DBNo ratings yet
- NTTM632 Anand Informatica-ETL Lead ResumeDocument8 pagesNTTM632 Anand Informatica-ETL Lead ResumeMohammed JawadNo ratings yet