Professional Documents
Culture Documents
OXYGENATION
Uploaded by
Jo Marchianne Pigar0%(1)0% found this document useful (1 vote)
119 views8 pagesThis document summarizes key aspects of respiration and gas exchange. It discusses that oxygen is necessary for cellular function while carbon dioxide is a waste product. The four main components of respiration are ventilation, alveolar gas exchange, oxygen and carbon dioxide transport, and tissue diffusion. The respiratory system has upper and lower parts, and oxygen diffuses from the alveoli into the blood while carbon dioxide diffuses in the opposite direction. Various factors can affect respiratory function and gas exchange.
Original Description:
Original Title
OXYGENATION.docx
Copyright
© © All Rights Reserved
Available Formats
DOCX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentThis document summarizes key aspects of respiration and gas exchange. It discusses that oxygen is necessary for cellular function while carbon dioxide is a waste product. The four main components of respiration are ventilation, alveolar gas exchange, oxygen and carbon dioxide transport, and tissue diffusion. The respiratory system has upper and lower parts, and oxygen diffuses from the alveoli into the blood while carbon dioxide diffuses in the opposite direction. Various factors can affect respiratory function and gas exchange.
Copyright:
© All Rights Reserved
Available Formats
Download as DOCX, PDF, TXT or read online from Scribd
0%(1)0% found this document useful (1 vote)
119 views8 pagesOXYGENATION
Uploaded by
Jo Marchianne PigarThis document summarizes key aspects of respiration and gas exchange. It discusses that oxygen is necessary for cellular function while carbon dioxide is a waste product. The four main components of respiration are ventilation, alveolar gas exchange, oxygen and carbon dioxide transport, and tissue diffusion. The respiratory system has upper and lower parts, and oxygen diffuses from the alveoli into the blood while carbon dioxide diffuses in the opposite direction. Various factors can affect respiratory function and gas exchange.
Copyright:
© All Rights Reserved
Available Formats
Download as DOCX, PDF, TXT or read online from Scribd
You are on page 1of 8
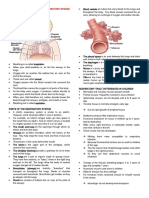
Oxygen – a clear, odorless gas that constitutes approximately A.
PULMONARY VENTILATION – first process of the
21% of the air we breathe, is necessary for proper functioning respiratory system, ventilation of the lungs, is
of all living cells. Absence of oxygen can lead to cellular, accomplished through the act of breathing.
tissue, and organism death. a. Inspiration (inhalation) – air flows into the lungs
b. Expiration (exhalation) – air moves out of the lungs
Respiration – is the process of gas exchange between the
individual and the environment. Factors:
4 COMPONENTS: Clear airways
1. Ventilation or breathing, the movement of air in and 1. An intact central nervous system and respiratory
out of the lungs as we inhale and exhale center
2. Alveolar-capillary gas exchange, which involves the 2. An intact thoracic cavity capable of expanding
diffusion of oxygen and carbon dioxide between the and contracting
alveoli and the pulmonary capillaries 3. Adequate pulmonary compliance and recoil.
3. Transport of oxygen and carbon dioxide between the
medulla and pons – respiratory centers; control breathing
tissues and the lungs
4. Movement of oxygen and carbon dioxide between severe head injury, opiates or barbiturates – affect the
the systemic capillaries and the tissues. respiratory centers
4 PROCESSES of the respiratory system: intrapleural pressure (pressure in the pleural cavity
surrounding the lungs) – always slightly negative in relation
1. pulmonary ventilation
to atmospheric pressure; it creates the suction that holds the
2. alveolar gas exchange transport of oxygen
visceral pleura and the parietal pleura together as the chest
3. carbon dioxide
cage expands and contracts.
4. systemic diffusion.
intrapulmonary pressure (pressure within the lungs) -
Respiratory System
always equalizes with atmospheric pressure; inspiration
A. Upper Respiratory (mouth, nose, pharynx, and occurs when the diaphragm and intercostal muscles contract,
larynx compose the upper respiratory system) increasing the size of the thoracic cavity.
B. Lower respiratory (trachea and lungs, with the
COPD – reduce this elasticity result in forced expirations and
bronchi, bronchioles, alveoli, pulmonary capillary
may impair the body’s ability to expel carbon dioxide.
network, and pleural membranes)
tidal volume – 500 mLof air is inspired and expired with each
Sneeze reflex – initiated by irritants in nasal passages; large
breath
volume of air rapidly exits through the nose and mouth during
a sneeze, helping to clear nasal passages. Lung compliance - the expansibility or stretchability of lung
tissue, plays a significant role in the ease of ventilation; for
Cough reflex – (vagus nerve) triggered by irritants in the
normal inspiration
larynx, trachea, or bronchi; foreign particles are then swept
upward toward the larynx and throat by cilia, tiny hairlike Atelectasis - collapse of a portion of the lung
projections on the epithelial cells
lung recoil – the continual tendency of the lungs to collapse
Mucous blanket – traps pathogens and microscopic away from the chest wall; for normal expiration
particulate matter
Surfactant – a lipoprotein produced by specialized alveolar
respiratory membrane (alveolar/ capillary membrane) - gas cells, acts like a detergent, reducing the surface tension of
exchange occurs between the air on the alveolar side and the alveolar fluid
blood on the capillary side; not more than 0.0004 mm thick
pleura – outer surface of the lungs is covered by a thin, double
layer of tissue B. ALVEOLAR GAS EXCHANGE - the second phase of
the respiratory process—the diffusion of oxygen from the
A. parietal pleura – lines the thorax and surface of the alveoli and into the pulmonary blood vessels.
diaphragm
B. visceral pleura – covers external surface of the Diffusion – is the movement of gases or other particles from
lungs an area of greater pressure or concentration to an area of
lower pressure or concentration
pleural fluid - a serous lubricating solution; prevents friction
during the movements of breathing and serves to keep the
layers adherent through its surface tension.
partial pressure - the pressure exerted by each individual RESPIRATORY REGULATION - includes both neural
gas in a mixture according to its concentration in the mixture and chemical controls to maintain the correct
of oxygen PO2 concentrations of oxygen, carbon dioxide, and hydrogen
ions in body fluids.
a. in the alveoli - 100 mmHg
b. in the venous blood of the pulmonary arteries –
Emphysema - oxygen concentrations, not carbon
60 mmHg.
dioxide concentrations, play a major role in regulating
PCO2 respiration
a. alveoli – 40 mHg Stimulus of response : carbon dioxide – detected by the
b. pulmonary capillaries - 45 mmHg carotid bodies
Carbon dioxide retention : decrease oxygenation
C. TRANSPORT OF OXYGEN AND CARBON DIOXIDE –
third part of the respiratory process involves the transport ASTHMA & COPD – they are given low-flow
of respiratory gases. concentration of oxygen (2-3 liters per minute)
97% combines loosely with hemoglobin Factors
hemoglobin - oxygen-carrying red pigment in the red blood 1. Age
cells (RBCs) 2. Environment
3. Lifestyle
oxyhemoglobin - the compound of oxygen and hemoglobin
4. Health status
Factors affect the rate of oxygen transport from the lungs to 5. Medication
the tissues: 6. Stress
1. Cardiac output ( damage to the heart muscle, ALTERATION IN RESPIRATORY FUNCTION
blood loss, or pooling of blood in the peripheral 1. Patency (open airway)
blood vessels ) - diminishes the amount of
2. The movement of air into or out of the lungs
oxygen delivered to the tissues
3. The diffusion of oxygen and carbon dioxide
2. No. of erythrocytes and blood hematocrit
between the alveoli and the pulmonary
a. Erythrocyte – red blood cell
capillaries
i. Men - 5 million per cubic milliliter
4. The transport of oxygen and carbon dioxide via
of blood
the blood to and from the tissue cells.
ii. Women - 4.5 million per cubic
milliliter Conditions Affecting the Airway
b. Hematocrit – percentage of the blood that
Lower airway obstruction - Stridor,a harsh, high-
is erythrocytes
pitched sound, may be heard during inspiration
i. Men – 40% to 54%
The client may have altered arterial blood gas levels,
ii. Women – 36% to 40%
restlessness, dyspnea, and adventitious breath
3. Exercise
sounds
Carbon dioxide
Conditions Affecting Movement of Air
a. 65% - carried inside the RBC as
Breathing patterns - refers to the rate, volume, rhythm, and
bicarbonate (HO3)
relative ease or effort of respiration
b. 30% - carbhemoglobin (also known as
carbaminohemoglobin Eupnea – normal respiration; is quiet, rhythmic, and effortless
c. 5% - in plasma and as carbonic acid (the
compound formed when carbon dioxide Tachypnea - rapid respiration; seen with fevers, metabolic
combines with water). acidosis, pain, and hypoxemia.
Bradypnea - abnormally slow respiratory rate, which may be
D. SYSTEMIC DIFFUSION – fourth process of respiration is seen in clients who have taken drugs such as morphine or
diffusion of oxygen and carbon dioxide between the sedatives, who have metabolic alkalosis, or who have
capillaries and the tissues and cells down to a increased intracranial pressure
concentration gradient similar to diffusion at the alveolar
capillary level Apnea - is the absence of any breathing
Hypoventilation - inadequate alveolar ventilation, may be
Shock – reduced blood flow states
caused by either slow or shallow breathing, or both; may lead
to increased levels of carbon dioxide (hypercarbia or nail becomes swollen and the ends of the fingers and toes
hypercapnia) or low levels of oxygen (hypoxemia). increase in size.
Hyperventilation - is the increased movement of air into and
out of the lungs; the rate and depth of respirations increase
and more CO2 is eliminated than is produced
Kussmaul’s breathing – by which the body
attempts to compensate for increased metabolic acids by
blowing off acid in the form of CO2; particular type of
hyperventilation that accompanies metabolic acidosis
Irregular rhythms:
1. Cheyne-Stokes respirations - marked rhythmic
waxing and waning of respirations from very deep to
very shallow with short periods of apnea commonly
caused by chronic diseases, increased intracranial
pressure, and drug overdose.
2. Biot’s (cluster) respirations - shallow breaths
interrupted by apnea; may be seen in clients with
central nervous system disorders.
Orthopnea – is the inability to breathe easily unless sitting
upright or standing.
Dyspnea – difficulty breathing or the feeling of being short of
breath (SOB)
Conditions Affecting Diffusion
Hypoxemia – reduced oxygen levels in the blood,may be
caused by conditions that impair diffusion at the alveolar-
capillary level such as pulmonary edema or atelectasis
(collapsed alveoli) or by low hemoglobin levels.
Hypoxia – insufficient oxygen anywhere in the body
Causes: pulmonary edema, anemia, heart failure,
embolism – thrombus is dislodged
amniotic fluid embolism (AFE) is a rare childbirth
(obstetric) emergency in which amniotic fluid enters
the blood stream of the mother to trigger a serious
reaction.
Cyanosis -bluish discoloration of the skin, nail beds, and
mucous membranes due to reduced hemoglobin-oxygen Anxiety related to ineffective airway clearance and
saturation; may be present with hypoxemia or hypoxia feeling of suffocation
Fatigue related to ineffective breathing pattern
1. Circumoral – lips Fear related to chronic disabling respiratory illness
2. Peripheral – distal Powerlessness related to inability to maintain
3. Central - trunk independence in self-care activities because of
The blood must contain about 5 g or more of ineffective breathing pattern
unoxygenated hemoglobin per 100 mL of blood, and Insomnia related to orthopnea and required O2 therapy
the surface blood capillaries must be dilated. Social Isolation related to activity intolerance and
The cerebral cortex can tolerate hypoxia for only 3 to inability to travel to usual social activities.
5 minutes before permanent damage occurs.
Clubbing - The angle between the nail and the base of the
nail increases to more than 180 degrees; as a result of long-
term lack of oxygen in the arterial blood supply; base of the
PROMOTING OXYGENATION INCENTIVE SPIROMETRY
Interventions by the nurse to maintain the normal Incentive spirometers - also referred to as sustained
respirations of clients include: maximal inspiration devices (SMIs); measure the flow of air
inhaled through the mouthpiece; designed to mimic natural
1. Positioning the client to allow for maximum chest
sighing or yawning by encouraging the client to take long,
expansion
slow, deep breaths.
2. Encouraging or providing frequent changes in
position to:
3. Encouraging deep breathing and coughing
4. Encouraging ambulation 1. Improve pulmonary ventilation.
2. Counteract the effects of anesthesia or
5. Implementing measures that promote comfort, such
as giving pain medications. hypoventilation.
3. Loosen respiratory secretions.
semi-Fowler’s or high Fowler’s position – allows maximum 4. Facilitate respiratory gaseous exchange.
chest expansion in clients who are confined to bed, 5. Expand collapsed alveoli.
particularly those with dyspnea.
A. Flow-oriented - consists of one or more clear plastic
1. Deep breathing and coughing – facilitate respiratory
chambers containing freely movable colored balls or
functioning
disks. The ball or disks are elevated as the client
Expectorate – spit out inhales. The longer the inspiratory flow is
maintained, the larger the volume, so the client is
2. Hydration – maintains the moisture of the respiratory encouraged to take slow deep breaths. This type of
mucous membranes. spirometer does not measure the specific volume of
Humidifiers – are devices that add water vapor to air inhaled.
inspired air B. Volume-oriented - measure the inhalation volume
maintained by the client.
3. Medications
a) Bronchodilators - including sympathomimetic PERCUSSION, VIBRATION, AND POSTURAL DRAINAGE
drugs and xanthines, reduce bronchospasm, (PVD)
opening tight or congested airways and
facilitating ventilation
b) Anti-inflammatory drugs - such as Percussion - called clapping, is forceful striking of the skin
glucocorticoids; work by decreasing the edema with cupped hands; should produce a hollow, popping sound;
and inflammation in the airways and allowing a avoided over the breasts, sternum, spinal column, and
better air exchange. kidneys.
Bronchodilators first before anti-inflammatory Vibration - is a series of vigorous quivering produced by
hands that are placed flat against the client’s chest wall; used
c) Leukotriene modifiers - suppress the effects of
after percussion to increase the turbulence of the exhaled air
leukotrienes on the smooth muscle of the
and thus loosen thick secretions; often done alternately with
respiratory tract; cause bronchoconstriction,
percussion.
mucous production, and edema of the
respiratory tract. Postural drainage - is the drainage by gravity of secretions
d) Expectorants - help “break up” mucus, making from various lung segments.
it more liquid and easier to expectorate
The sequence for PVD is usually as follows:
(Guaifenesin)
digitalis glycosides act directly on the heart to 1. Positioning
improve the strength of contraction and slow the 2. Percussion
heart rate 3. Vibration
Beta-adrenergic stimulating agents such as 4. Removal of secretions by coughing or suction
dobutamine similarly increase cardiac output, thus
improving O2 transport Each position is usually assumed for 10 to 15 minutes.
Beta-adrenergic blocking agents such as CLRT – continuous lateral rotational therapy
propranolol affect the sympathetic nervous system to
reduce the workload of the heart.
MUCUS CLEARANCE DEVICES (MCD)
is used for clients with excessive secretions such as
cystic fibrosis, COPD, and bronchiectasis
The Flutter MCD
is a small, handheld device with a hard plastic
mouthpiece at one end and a perforated cover at the
other end.
Inside the device is a steel ball that sits in a circular
cone shape
Client inhales slowly and then, keeping the cheeks 2. Face Mask
firm, exhales fast through the device, causing the cover the client’s nose and mouth may be used
steel ball to move up and down for oxygen inhalation
This movement causes vibrations that loosen mucus i. simple face mask - delivers oxygen
from the airways and assist its movement up the concentrations from 40% to 60% at liter
airways to be expectorated flows of 5 to 8 L/min
ii. partial rebreather mask - delivers
OXYGEN THERAPY oxygen concentrations of 40% to 60%
at liter flows of 6 to 10 Lper minute
Supplemental oxygen is indicated for clients who have
iii. nonrebreather mask - delivers the
hypoxemia due to the reduced ability for diffusion of oxygen
highest oxygen concentration
through the respiratory membrane, hyperventilation, or
possible—95% to 100%—by means
substantial loss of lung tissue due to tumors or surgery other than intubation or mechanical
Oxygen is supplied in two ways in health care facilities ventilation, at liter flows of 10 to 15
L/min
1. by portable systems (cylinders or tanks) – dry, iv. Venturi mask - delivers oxygen
dehydrate the respiratory mucous membranes concentrations varying from 24% to
2. from wall outlets. 40% or 50% at liter flows of 4 to 10
Humidifying devices L/min
1. blue adapter delivers a 24%
essential adjunct of oxygen therapy, particularly for concentration of oxygen at 4
liter flows over 4 Lper minute L/min
provide 20%-4-% humidity 2. green adapter delivers a 35%
prevent mucous membranes from drying and concentration of oxygen at 8
becoming irritated and loosen secretions for easier L/min
expectoration.
Limitations of masks include difficulty in achieving a proper fit
OXYGEN DELIVERY SYSTEMS and poor tolerance by some clients who may complain of
feeling hot or “smothering.”
A. Low-flow systems - deliver oxygen via small-bore
tubing. Include nasal cannulas, face masks, oxygen
tents, and transtracheal catheters
B. High-flow systems - supply all the oxygen required
during ventilation in precise amounts, regardless of
the client’s respirations. The high-flow system used
to deliver a precise and consistent FiO2
1. Cannula (nasal prongs)
low concentration of oxygen (24% to 45%) at
flow rates of 2 to 6 L/min
the most common and inexpensive device used
to administer oxygen.
Does not interfere with the client’s ability to eat
or talk
Portable, permits some freedom of movement,
and is well tolerated by the client
2 styles: mustache and pendant
3. Face tent
can replace oxygen masks when masks are
poorly tolerated by clients
30% to 50% concentration of oxygen at 4 to 8
L/min
4. Transtracheal Catheter
is placed through a surgically created tract in
the lower neck directly into the trachea
cleans the catheter two to four times per day
greater than 1 L/min should be humidified, and are used to keep the upper air passages open when
high flow rates, as much as as 15 to 20 L/min, they may become obstructed by secretions or the
can be administered tongue
5. Noninvasive Positive Pressure Ventilation (NPPV) - these airways are easy to insert and have a low risk
require mechanical assistance to maintain adequate of complications
breathing sizes vary and should be appropriate to the size and
include acute and chronic respiratory failure, age of the client.
pulmonary edema, COPD, and obstructive the airway should be well lubricated with water
sleep apnea soluble gel prior to inserting.
i. CPAP - continuous positive airway o Oropharyngeal airways stimulate the gag
pressure reflex and are only used for clients with
ii. BiPap - bilevel positive airway altered levels of consciousness (e.g.,
pressure the pressure delivered during because of general anesthesia, overdose,
exhalation is less than the pressure or head injury).
delivered during inhalation. o Nasopharyngeal airways are tolerated
Cannula better by alert clients. They are inserted
through the nares, terminating in the
To deliver a relatively low concentration of oropharynx. When caring for a client with a
oxygen when only minimal O2 support is nasopharyngeal airway, provide frequent
required oral and nares care, repositioning the
To allow uninterrupted delivery of oxygen while airway in the other naris every 8 hours or as
the client ingests food or fluid ordered to prevent necrosis of the mucosa.
Face Mask Endotracheal Tubes
To provide moderate O2 support and a higher
concentration of oxygen and/or humidity than is
provided by cannula
Face Tent
To provide high humidity
To provide oxygen when a mask is poorly
tolerated
To provide a high flow of O2 when attached to a
Venturi system
ARTIFICIAL AIRWAYS - are inserted to maintain a patent air most commonly inserted in clients who have had
passage for clients whose airway has become or maybe come general anesthetics or for those in emergency
obstructed. situations where mechanical ventilation is required.
An endotracheal tube is inserted by an
4 common types: anesthesiologist, primary care provider, certified
1. Oropharyngeal nurse anesthetist (CRNA), or respiratory therapist
2. Nasopharyngeal with specialized education
3. Endotracheal It is inserted through the mouth or the nose and into
4. Tracheostomy the trachea with the guide of a laryngoscope. The
tube terminates just superior to the bifurcation of the
Oropharyngeal and Nasopharyngeal Airways trachea into the bronchi
the client is unable to speak while it is in place.
Tracheostomy. SUCTIONING - aspirating secretions through a catheter
connected to a suction machine or wall suction outlet.
Clients who need airway support due to a temporary
or permanent condition may have a tracheostomy 1. Oropharyngeal and nasopharyngeal suctioning
A tracheostomy is an opening into the trachea removes secretions from the upper respiratory tract.
through the neck. 2. Nasotracheal suctioning provides closer access to
tube is usually inserted through this opening and an the trachea and requires sterile technique
artificial airway is created
Either be:
need to be suctioned and cleaned as often as every
1 to 2 hours. a) whistle-tipped catheter - is less irritating to
2 techniques: respiratory tissues, although the open-tipped
o traditional open surgical method - done catheter may be more effective for removing thick
in the operating room, and a surgical mucous plugs
incision is made in the trachea just below b) open tipped
the larynx.
o percutaneous insertion - can be done at Yankauer device or oral suction tube, -is used to suction
the bedside in a critical care unit the oral cavity
may be plastic, silicone, or metal, and cuffed,
uncuffed, or fenestrated.
COMPONENTS:
outer cannula - is inserted into the trachea and a flange
that rests against the neck and allows the tube to be
secured in place with tracheostomy tapes/twill ties or
Velcro collars
obturator - used to insert the outer cannula and is then
removed; kept at the client’s bedside in case the tube Lifespan consideration (Suctioning)
becomes dislodged and needs to be reinserted.
inner cannula - inserted and locked into place inside the
outer cannula; removed for cleaning and the outer
cannula remains in place to maintain a patent airway
Low-pressure cuffs - commonly used to distribute a low,
even pressure against the trachea, thus decreasing the risk of
tracheal tissue necrosis
Lifespan consideration (Tracheostomy or Endotracheal)
Clients with long-term tracheostomies may use a “heat
moisture exchange device known as a ‘Swedish nose’
Lifespan consideration (Tracheostomy Care)
CHEST TUBES AND DRAINAGE SYSTEMS
a) Pneumothorax - air collects in the pleural space
b) Hemothorax - is the accumulation of blood in the
pleural space
c) Pyothorax - puss
d) pleural effusion - exists when there is excessive
fluid in the pleural space
Heimlich valve
may be used for ambulatory clients
a one-way flutter valve that allows air to escape
from the chest cavity, but prevents air from
reentering
not designed to collect fluid
Pneumostat
a one-way valve
a small built-in collection chamber
exclusively for clients with a pneumothorax who
usually have small amounts of fluid
NOTE: STEPS, NURSING INTERVENTIONS BASA NALA
BOOK DAMO HAHA
-sherlock :<
You might also like
- NCM 116 Lab Midterm ActivityDocument2 pagesNCM 116 Lab Midterm ActivityEula Dannah Alyssha EboraNo ratings yet
- NCM 112-Mod3Document19 pagesNCM 112-Mod3Samantha BolanteNo ratings yet
- September 13 - NCM 112 (Mam G)Document2 pagesSeptember 13 - NCM 112 (Mam G)Aaron DayloNo ratings yet
- RESPIRATORY SYSTEM Nclex Iloilo 4Document27 pagesRESPIRATORY SYSTEM Nclex Iloilo 4Barangay Centro SurNo ratings yet
- UNIT 1 (MS 1) Care of Clients With Problems in OxygenationDocument10 pagesUNIT 1 (MS 1) Care of Clients With Problems in OxygenationElle MirandaNo ratings yet
- Pediatric Nursing - QuizDocument13 pagesPediatric Nursing - QuizChy ChyNo ratings yet
- Airway CareDocument68 pagesAirway CareJesus Mario LopezNo ratings yet
- Oxygen TherapyDocument3 pagesOxygen Therapymarie100% (3)
- Post Op Worksheet FinalDocument5 pagesPost Op Worksheet FinalRiza Angela BarazanNo ratings yet
- NCM 112 OXYGENATION - HandoutDocument9 pagesNCM 112 OXYGENATION - Handoutissaiahnicolle100% (1)
- Chapter 44-Activity and ExerciseDocument4 pagesChapter 44-Activity and ExerciseollietonkNo ratings yet
- Case Studies On Major Concepts: Cellular AberrationDocument38 pagesCase Studies On Major Concepts: Cellular AberrationJek Dela CruzNo ratings yet
- A. The Sum of All Chemical Reactions in The Organisms, That Produce Energy or Synthesize Organic MatterDocument5 pagesA. The Sum of All Chemical Reactions in The Organisms, That Produce Energy or Synthesize Organic MatterShane Aileen AngelesNo ratings yet
- Rhea TestDocument3 pagesRhea Testerma090308No ratings yet
- NORMAL OB-emergency-assessmentDocument3 pagesNORMAL OB-emergency-assessmentJo Hn VengzNo ratings yet
- M Vanguardia-McnpDocument11 pagesM Vanguardia-Mcnpmark OrpillaNo ratings yet
- NCM 112 Lecture Notes (Respiratory System and Its Diseases)Document9 pagesNCM 112 Lecture Notes (Respiratory System and Its Diseases)Kyle FernandezNo ratings yet
- Angelito L. Ramos Jr. RN Clinical InstructorDocument68 pagesAngelito L. Ramos Jr. RN Clinical Instructorraymondblade18100% (17)
- Skill Performance Evaluation - Measuring Intake and OutputDocument2 pagesSkill Performance Evaluation - Measuring Intake and OutputLemuel Que100% (1)
- Finals Rle 2015Document13 pagesFinals Rle 2015AnnaAlfonsoNo ratings yet
- 60 91 EndocrineDocument34 pages60 91 EndocrineYaj CruzadaNo ratings yet
- Prelim Exam NCM 103Document10 pagesPrelim Exam NCM 103Zhyraine Iraj D. CaluzaNo ratings yet
- July 2012 Pnle Pearls of Success Part 6: Medical and Surgical Health NursingDocument7 pagesJuly 2012 Pnle Pearls of Success Part 6: Medical and Surgical Health NursingNicole OrtegaNo ratings yet
- CHN Notes SummaryDocument6 pagesCHN Notes SummaryVIKTORIA SARAH DIZONNo ratings yet
- Compre F&EDocument6 pagesCompre F&EArcon AlvarNo ratings yet
- Compt - Appraisal Prelim 2 Glenda CasundoDocument19 pagesCompt - Appraisal Prelim 2 Glenda CasundoJoanne Bernadette AguilarNo ratings yet
- PNLE IV For Care of Clients With Physiologic and Psychosocial Alterations (Part 2)Document23 pagesPNLE IV For Care of Clients With Physiologic and Psychosocial Alterations (Part 2)ASDF ASDFNo ratings yet
- Toprank Cardio Hema Post TestDocument5 pagesToprank Cardio Hema Post TestJoyce ObraNo ratings yet
- CHN ExamDocument16 pagesCHN ExamGlenn Daryll SantosNo ratings yet
- Management of Patients With Gastric and Duodenal DisordersDocument7 pagesManagement of Patients With Gastric and Duodenal DisordersintotheunknownNo ratings yet
- Nursing RLEDocument19 pagesNursing RLEPatricia AdiaoNo ratings yet
- Test Your Nursing Knowledge: CA1 Module 3 ActivitiesDocument6 pagesTest Your Nursing Knowledge: CA1 Module 3 ActivitiesEsmareldah Henry SirueNo ratings yet
- First Semester 2020-2021 Study Guide: University of The CordillerasDocument13 pagesFirst Semester 2020-2021 Study Guide: University of The CordillerasJonalyn EtongNo ratings yet
- RESEARCH LM - Toprank ReviewDocument34 pagesRESEARCH LM - Toprank ReviewAnna Mateo De LeonNo ratings yet
- Medsurg 3Document22 pagesMedsurg 3eyesontheskyNo ratings yet
- Periop QuizesDocument9 pagesPeriop QuizesAnonymous ZQ4gHahzNo ratings yet
- C. Delay Hanging The Blood and Notify The HCPDocument31 pagesC. Delay Hanging The Blood and Notify The HCPmyNo ratings yet
- F&E ExamDocument3 pagesF&E ExamDino PringNo ratings yet
- NCM 112 MidtermDocument25 pagesNCM 112 MidtermJan Charlie Sophia100% (1)
- CHN MidtermsDocument31 pagesCHN MidtermsVince LeonidaNo ratings yet
- Chapter 39 - Assessment and Management of Patients With Hepatic DisordersDocument6 pagesChapter 39 - Assessment and Management of Patients With Hepatic DisordersMichael BoadoNo ratings yet
- OxygenationDocument191 pagesOxygenationShane Damian100% (3)
- FundamentsDocument57 pagesFundamentsGela CiluomNo ratings yet
- TB and LeprosyDocument39 pagesTB and LeprosyCharise Ligores100% (1)
- Evolution of Nursing Research and Role of The Nurse in ResearchDocument3 pagesEvolution of Nursing Research and Role of The Nurse in ResearchAlmer OstreaNo ratings yet
- Fundamentals of Nursin Final Examination-Answer Keys (March 18,2013Document13 pagesFundamentals of Nursin Final Examination-Answer Keys (March 18,2013marsan12No ratings yet
- CVP - Nursing Performance ChecklistDocument3 pagesCVP - Nursing Performance ChecklistJoy Jarin75% (4)
- Nursing Department: Care To Learn, Learn To Care Embracing World Class StandardsDocument13 pagesNursing Department: Care To Learn, Learn To Care Embracing World Class Standardsmalinda0% (2)
- 8 Irrigating A ColostomyDocument5 pages8 Irrigating A ColostomyAnn Jalover PerezNo ratings yet
- Handouts CHNDocument23 pagesHandouts CHNJames Eugene CaasiNo ratings yet
- Nursing - BAG-TECHNIQUEDocument23 pagesNursing - BAG-TECHNIQUENiño PaoloNo ratings yet
- Nle Tips For OrthopedicDocument2 pagesNle Tips For OrthopedicCharie OcampoNo ratings yet
- Funda Test DrillDocument32 pagesFunda Test DrillNurseRiemNo ratings yet
- Practice Questions (F & E)Document5 pagesPractice Questions (F & E)pbiluanNo ratings yet
- Competency Appraisal - Diagnostic TestsDocument7 pagesCompetency Appraisal - Diagnostic TestsMj BrionesNo ratings yet
- P.A. 1Document6 pagesP.A. 1SamSarah BongolanNo ratings yet
- Administering Enema POWERPOINT GIVING ENEMA TO PATIENT, FOR PATIENT WITH GASTROINTESTINAL DISORDERS .. LECTURES, PRINCIPLES AND PROCEDURESDocument14 pagesAdministering Enema POWERPOINT GIVING ENEMA TO PATIENT, FOR PATIENT WITH GASTROINTESTINAL DISORDERS .. LECTURES, PRINCIPLES AND PROCEDURESPb0% (1)
- Ncma 113Document4 pagesNcma 113Wonie booNo ratings yet
- M7 RespiratoryDocument6 pagesM7 RespiratoryNel joy PaurilloNo ratings yet
- 04 OxygenationDocument4 pages04 Oxygenationbunso padillaNo ratings yet
- Hand WashingDocument4 pagesHand WashingJo Marchianne PigarNo ratings yet
- Final SHS Chapter IiiDocument4 pagesFinal SHS Chapter IiiJo Marchianne PigarNo ratings yet
- MCN RLE Worksheet No.3Document4 pagesMCN RLE Worksheet No.3Jo Marchianne PigarNo ratings yet
- Final SHS Chapter IiDocument19 pagesFinal SHS Chapter IiJo Marchianne PigarNo ratings yet
- Final SHS Chapter IDocument9 pagesFinal SHS Chapter IJo Marchianne PigarNo ratings yet
- Excretory System FINALDocument3 pagesExcretory System FINALJo Marchianne PigarNo ratings yet
- Endocrine SystemDocument5 pagesEndocrine SystemJo Marchianne PigarNo ratings yet
- MCN RLE Worksheet 2Document5 pagesMCN RLE Worksheet 2Jo Marchianne PigarNo ratings yet
- ReferencesDocument2 pagesReferencesJo Marchianne PigarNo ratings yet
- Disbursement VoucherDocument1 pageDisbursement VoucherJo Marchianne PigarNo ratings yet
- Worksheet #3Document43 pagesWorksheet #3Jo Marchianne PigarNo ratings yet
- PBCDocument1 pagePBCJo Marchianne PigarNo ratings yet
- Moral ValuesDocument7 pagesMoral ValuesJo Marchianne PigarNo ratings yet
- 1.1.c-Technology and Society in The Bronze AgesDocument13 pages1.1.c-Technology and Society in The Bronze Agestwinkledreampoppies50% (2)
- Data For InformaticsDocument2 pagesData For InformaticsJo Marchianne PigarNo ratings yet
- Change TheoryDocument1 pageChange TheoryJo Marchianne PigarNo ratings yet
- Drug StudiesDocument4 pagesDrug StudiesJo Marchianne PigarNo ratings yet
- Upper Respiratory System DisordersDocument7 pagesUpper Respiratory System DisordersJo Marchianne PigarNo ratings yet
- DRUG StudiesDocument7 pagesDRUG StudiesJo Marchianne PigarNo ratings yet
- She Was A: 1. Health Perception - Health Management PatternDocument9 pagesShe Was A: 1. Health Perception - Health Management PatternJo Marchianne PigarNo ratings yet
- History Taking GuideDocument2 pagesHistory Taking GuideJo Marchianne PigarNo ratings yet
- MMDSTDocument4 pagesMMDSTJo Marchianne PigarNo ratings yet
- Hematology Part-IiDocument7 pagesHematology Part-IiJo Marchianne PigarNo ratings yet
- Ligaments of ShoulderDocument12 pagesLigaments of ShoulderJo Marchianne PigarNo ratings yet
- Physical and Developmental Disorders of The Gastrointestinal SystemDocument10 pagesPhysical and Developmental Disorders of The Gastrointestinal SystemJo Marchianne PigarNo ratings yet
- Lower Respiratory DisordersDocument4 pagesLower Respiratory DisordersJo Marchianne PigarNo ratings yet
- HEMATOLOGYDocument10 pagesHEMATOLOGYJo Marchianne Pigar100% (8)
- MCN WorksheetDocument5 pagesMCN WorksheetJo Marchianne PigarNo ratings yet
- Data For InformaticsDocument3 pagesData For InformaticsJo Marchianne PigarNo ratings yet
- Cls-Progression Stage 8 - 2024 - Paper-2 (S)Document18 pagesCls-Progression Stage 8 - 2024 - Paper-2 (S)king100% (1)
- 5 6082340175571059112Document5 pages5 6082340175571059112Inukaicchi TakumichiNo ratings yet
- Functional Anatomy of The Respiratory System NoseDocument5 pagesFunctional Anatomy of The Respiratory System NoseEjie Boy IsagaNo ratings yet
- 03 Life Processes Chapter Wise Important QuestionsDocument17 pages03 Life Processes Chapter Wise Important Questionsmm8871100% (1)
- Pure Bio ANSWERDocument17 pagesPure Bio ANSWERlohbernard168No ratings yet
- Paediatric Booklet by Win Nursing CoachingDocument116 pagesPaediatric Booklet by Win Nursing CoachingAkshya YadavNo ratings yet
- LIFE PROCESSES - Question BankDocument15 pagesLIFE PROCESSES - Question BankMISHKA KHANDELWALNo ratings yet
- Respiratory Distress in The Newborn: Pediatrics in Review October 2014Document16 pagesRespiratory Distress in The Newborn: Pediatrics in Review October 2014turigauNo ratings yet
- Dioxido de CloroDocument12 pagesDioxido de CloroEli De La CruzNo ratings yet
- Exchange Surfaces Summary SheetDocument1 pageExchange Surfaces Summary Sheetrobgardner1No ratings yet
- Respiratory System - ReviewerDocument8 pagesRespiratory System - ReviewerEva Marie GaaNo ratings yet
- Spanish GlossaryDocument62 pagesSpanish GlossaryAnna CabedoNo ratings yet
- Mechanism of Gas ExchangeDocument8 pagesMechanism of Gas ExchangeCHANON KIATKAWINWONGNo ratings yet
- Bio Science Study Material EM For Website-1Document73 pagesBio Science Study Material EM For Website-1Prabhakar ReddyNo ratings yet
- University of Guyana School of Medicine Med 1106 - Physiology I DR Kalima ThompsonDocument66 pagesUniversity of Guyana School of Medicine Med 1106 - Physiology I DR Kalima ThompsonKNo ratings yet
- NCERT Exemplar Solution Class 10 Science Chapter 6Document28 pagesNCERT Exemplar Solution Class 10 Science Chapter 6REJEENo ratings yet
- Breathing Is A Mechanical Process Where Oxygen Is Inhaled by Lungs andDocument9 pagesBreathing Is A Mechanical Process Where Oxygen Is Inhaled by Lungs andJamesShallowNo ratings yet
- Surfactant (Physiology)Document28 pagesSurfactant (Physiology)MaadaNo ratings yet
- NCPDocument7 pagesNCPRuth MontebonNo ratings yet
- Pediatric Pneumonia - Practice Essentials, Background, PathophysiologyDocument1 pagePediatric Pneumonia - Practice Essentials, Background, PathophysiologyShiferaw TesfayeNo ratings yet
- Inhalational Poisoning: Patricio, Roselene P. Ricarte, Viaka Faye Salvatus, JonnaDocument44 pagesInhalational Poisoning: Patricio, Roselene P. Ricarte, Viaka Faye Salvatus, JonnaRose PatricioNo ratings yet
- Marieb 2015 11th 0321919009 SampleDocument31 pagesMarieb 2015 11th 0321919009 SampleJoe Chill100% (1)
- Nervous System QuizDocument8 pagesNervous System QuizGee ZNo ratings yet
- A&P Chapter 15 Respiratory SystemDocument21 pagesA&P Chapter 15 Respiratory SystemKarl RobleNo ratings yet
- Respiratory SystemDocument4 pagesRespiratory SystemAlloiza CaguiclaNo ratings yet
- Pathophysiology Acute Respiratory FailureDocument2 pagesPathophysiology Acute Respiratory FailureKimberly Regacho88% (8)
- Bacterial PneumoniaDocument6 pagesBacterial PneumoniaIrsa SevenfoldismNo ratings yet
- Ventilator System ServoDocument54 pagesVentilator System ServoRoshield RandasanNo ratings yet
- Chapter 7Document138 pagesChapter 7Bëar MëNo ratings yet
- HK 3940 Human Physiology Final Exam Fall 2007: Name: Id#Document9 pagesHK 3940 Human Physiology Final Exam Fall 2007: Name: Id#rijzNo ratings yet