Professional Documents
Culture Documents
Heart Failure
Uploaded by
Mita RahOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Heart Failure
Uploaded by
Mita RahCopyright:
Available Formats
Review Article
Pediatric heart failure therapy: why β1-receptor blocker, tissue
ACE-I and mineralocorticoid-receptor-blocker?
Sabine Recla1, Dorle Schmidt1, Thushiha Logeswaran1, Anoosh Esmaeili2, Dietmar Schranz1,2
1
Pediatric Heart Center, Justus-Liebig University, Giessen, Germany; 2Department of Pediatric Cardiology, Johann-Wolfgang Goethe University,
Frankfurt, Germany
Contributions: (I) Conception and design: S Recla, D Schranz; (II) Administrative support: All authors; (III) Provision of study material or patients: All
authors; (IV) Collection and assembly of data: S Recla, D Schranz; (V) Data analysis and interpretation: None; (VI) Manuscript writing: All authors;
(VII) Final approval of manuscript: All authors.
Correspondence to: Prof. Dr. Dietmar Schranz. Pediatric Heart Center, Justus-Liebig University, Feulgenstrasse 12, 35385 Giessen, Germany.
Email: Dietmar.Schranz@paediat.med.uni-giessen.de.
Abstract: Pediatric heart failure (HF) treatment lagged behind the knowledge of pharmacological
research and evidence-based clinical experience in adults. Considering the lack of prospective, double
blind randomized studies in children, the review is focused on the preferred indication of specific β1-
adrenoreceptor blockers (ARB), mineralocorticoid antagonists and tissue angiotensin-converting enzyme
inhibitors (ACE-I). Our recommendations are based on the specificity in children, the effectiveness and the
side-effect profile of HF-drugs, the receptor-physiological knowledge and the negative results of the few
pediatric HF studies with an “evidence study label”. In the interest of our pediatric patients, effective HF
treatment has not longer to be postponed by balancing between evidence-based versus pathophysiology-
based approach. At our institution, bisoprolol, lisinopril and spironolactone (BLS) are used treating HF in
patients with left-right shunt lesions, reduced ejection fraction as well as during the inter-stage after HLHS-
Hybrid approach. Chronic use of diuretics and fluid restriction is avoided, if always possible; intravascular
volume deficiency stimulates further the neurohumoral axis. Pediatric HF needs to be treated with a strategy
respecting the variable pathophysiology and the differences of receptor physiology between children and
adult patients. The personalized treatment can be easily proofed by the surrogate parameters as heart rate,
breath pattern, weight gain and image-derived parameters as well as biomarkers. Effective HF-therapy is
also the basis for novel regenerative strategies in particular for young children with “end-stage” HF avoiding
cardiac transplant or death.
Keywords: Pediatric heart failure; β1-receptor blocker; tissue ACE-inhibitor; spironolactone
Submitted Dec 21, 2018. Accepted for publication Mar 28, 2019.
doi: 10.21037/tp.2019.04.08
View this article at: http://dx.doi.org/10.21037/tp.2019.04.08
Definition of heart failure (HF) arterial coupling. Therefore, every single component or
the sum of all components can lead to an insufficient heart
HF defines a condition in which the heart is unable
function. Pediatric HF is related to genetic and metabolic
to fulfill the body’s need of blood supply. The reason abnormalities, structural diseases with volume or pressure
of this inability is either known or idiopathic. Cardiac overload, hypoxemia, arrhythmias or caused by myocardial
output is not only a sum of myocardial contractility, heart disease. Clinical symptoms are dependent on the severity of
frequency, heart rhythm, preload and afterload, but is HF, but also related to age and the cause of HF (1).
also related to contractile synchrony, interventricular New York Heart Association (NYHA) functional
interaction, as well as atrial-ventricular and ventricular- classification is not suitable to the young pediatric
© Translational Pediatrics. All rights reserved. tp.amegroups.com Transl Pediatr 2019;8(2):127-132
128 Recla et al. Medical heart failure treatment
population (2). Instead, the Ross classification was Therapy of HF in children
developed related to the symptoms of infants and young
In history, the most important aim of HF therapy was
children in term of tachypnea, feeding difficulties, growth
to improve symptoms, so bedding children in upright
problems, sweating and symptoms of exercise intolerance.
position (10) and treating dyspnea and pulmonary
Additionally, the functional class could be correlated to
congestion by diuretics (11). Continuing to the present,
neurohumoral serum markers as plasma norepinephrine
evidence-based clinical trials in children are still missing
levels (3).
and recommendations are predicated on clinician’s
experience. In contrast, HF treatment in adults is based
Pathophysiology on guidelines that are periodically reviewed and updated.
These guidelines summarize results from studies of large
Chronic HF is caused by a progressive disease; the
cohorts of homogeneous patient groups (12); consecutively,
consecutive symptoms are related to the endogenous
recommendations are based on multiple randomized
counter-reactions in term of activation of the renin-
trials with a high level of evidence (level A). Difficulty of
angiotensin-aldosterone (RAA) as well as sympathetic conducting trials with a sufficient number of pediatric
nervous system. Initially, the water-salt retention and patients result in a lack of evidence-based therapies.
vasoconstriction preserves cardiac output by the Anrep- Heterogeneous causes of HF in children in a wide range of
effect (4) and the Frank-Starling mechanism (5). In age do not allow recruiting a sufficient number of patients
acute, these mechanisms restore cardiovascular function for randomized trials. Therefore, the few published studies
with improved symptoms. However, in long-term seem to be underpowered. Moreover, the majority of drugs
sustained activation of the neurohumoral axis worsens LV used in adult population have not received a regulatory
remodeling with loss of functional cardiomyocytes and approval for use in children; 80% of children receive off-
increased interstitial cardiac fibrosis leading to subsequent label medications for treating HF (13). Neglecting the
systolic and/or diastolic dysfunction lastly to cardiac specific pediatric pharmacokinetics and pharmacodynamics,
decompensation with secondary end-organ damage (6). usually drug levels in children are inadequate or excessive,
The pathophysiology of the HF in children differs when adult doses are scaled on the on children’s body
from that in adults not at least respective to the molecular weight (14). The largest pediatric HF trial utilizing
regulation. A unique characteristic of pediatric dilated carvedilol in a multicenter randomized placebo-controlled
cardiomyopathy (DCM) is down regulation of both, β1- trial did not show any treatment effect on the end point
AR and of β2-AR, in contrast to DCM in adults where of clinical HF outcomes. The study enrolled 161 children
no change of the β2-AR expression is observed (7). and adolescents (59% DCM) comparing low- and high-
Further, molecular regulation, including the potentials dose carvedilol therapy to placebo on a background of
of cardiomyocyte proliferation is unique in children; conventional therapy (15). In consequence of this and a
these mechanisms contribute to postnatal myocardial few other published results, a recently published Cochrane
growth. Further, it could be shown, that the percentage review concluded, that there are not enough data to
of cardiomyocytes in mitosis and cytokinesis is highest recommend or discourage the use of β-blockers in children
in infancy and the number of cardiomyocytes increases with HF (16-18). The conclusion, taken only from three
until an age of 20 years (8). These results suggest an studies with a cohort of 20, 22 and 161 patients, respectively,
ability of an age-related myocardial regeneration and a might be one reason, that β-blocker are in general less used
chance for cardiac proliferation in children and still as an by pediatricians. The negative results of the carvedilol study
adolescent, if stimulated (8). Postnatally, also hemodynamic might have a lot of additional causes as the heterogeneity
factors markedly influence myocardial growth; grown- of HF in term of etiology and severity, the used dosages
up of borderline left ventricles are related to the amount reflecting a strong under-dosing of the utilized β-blocker
of intracavity blood flow. In general, pressure load led and may be the inappropriate use of unselective β-blockers
to both, myocyte hyperplasia/hypertrophy accompanied (Propranolol or Carvedilol) at least treating pediatric DCM.
by myocardial angiogenesis in contrast to only myocyte In context, that infants require in fact fourfold higher doses
hypertrophy in a later age (9). of for example carvedilol achieving similar drug exposure to
© Translational Pediatrics. All rights reserved. tp.amegroups.com Transl Pediatr 2019;8(2):127-132
Translational Pediatrics, Vol 8, No 2 April 2019 129
adult patients (19), inappropriate diuretic treatment might properties and side-effects, like bronchoconstriction and
be an additional limiting factor to establish higher and vasodilative effects. Considering the effectiveness of a
sufficient dosages of β-blockers, but even ACE-inhibitors. drug, obviously it depends on more than just receptor
In fact, the recommended standard pharmacotherapy is affinity. As mentioned before, age and disease influence the
unchanged since more than 20 years and is still consisting pharmacokinetic profile, absorption behavior, metabolism,
of diuretics, digoxin and usually (70%) an angiotensin tissue distribution and elimination as well as longevity of
converting enzyme (ACE) inhibitor. Still only 4–18% of action at the given receptors. Regarding of this acquired
pediatric patients with HF undergo therapy with β-blockers knowledge, the selective long-acting β1-Blocker bisoprolol
(20,21). Among these, more than 70% are treated with (B) seems to be the prefers β-Blocker in children with HF,
carvedilol, despite official FDA reservations considering also in consideration of the parent’s compliance, applicating
carvedilol in children (22). This current prescribing trends the drug only once per day. Combining bisoprolol with the
for chronic HF therapy in children might be even called long-acting tissue angiotensin-converting enzyme (ACE)-
therapeutic “nihilism” (23). inhibitor as lisinopril, further supports this highly important
aspect of parent’s compliance: both drugs can be applicated
once per day and with a similar dosage of 0.1–0.2 mg/kg
Child-specific HF therapy
per day (28). Considering that angiotensin II, aldosterone
Requirements for specific pediatric HF therapies need to and catecholamines mediate trophic stimuli at tissue level
be based on pathophysiology and distinctive features of and are therefore responsible for the cardiac remodeling,
molecular cardiac profile in children. The aim of pediatric the β1-blocker bisoprolol has to be combined with an ACE-
HF-therapy is inhibiting the disease process or creating Inhibitor and aldosterone-antagonist. ACE-inhibitors have
a chance for cardiac regeneration, if possible. Therefore, the properties for reverse remodeling, decreasing systemic
clinicians have not further to tailor therapeutic strategies vascular resistance and improvement of vascular compliance.
to treat their patient’s symptoms by favoring the triple The remodeling properties seem to be higher especially
D-treatment [diuretics, digitalis, diet (fluid restriction)], with ACE-inhibitors with an effective tissue penetration
but should provide therapies affecting adverse biological like Lisinopril (L) (29,30). Compared to tissue-ACE-I,
consequences of sustained neurohormonal activation. high dosages of serum ACE-I, like Captopril, are needed to
Moreover, an important complementary strategy may be inhibit myocardial Angiotensin II formation. High dosages
based on stimulating endogenous regenerative mechanisms. of serum ACE-I induce furthermore bradykinin-dependent
Considering the research results of Miyamoto side-effects, as bronchoconstriction (symptomatic with
et al. (7), the cardiotoxic effects of endogenously and/ cough), especially in young patients. To complete the
or exogenously stimulated β1-ARs have sufficiently to be neurohormonal blockade, an aldosterone antagonist, like
blocked and contrarily, the cardioprotective properties spironolactone (S), might be additionally used in a low,
of β2-ARs be preserved (24); her summary “inhibition of non-diuretic dosage, preferentially as an anti-remodeling
the already down-regulated β2-ARs may override the benefits drug (31).
of β1-AR inhibition in children limiting the efficacy of non- Considering an effective anti-congestive treatment by
specific blockade in pediatric HF” needs to be taken in account blocking the sympathetic, RAAS-, and aldosterone system,
especially treating HF caused by DCM (7). Rather, β1-AR overtreatment of diuretics should be avoided and diuretics
inhibition along with β2-AR stimulation could be useful should rather be weaned in long-term therapy, if possible.
in acute HF (25,26). Moreover, tachypnea, respiratory Inappropriate diuretic treatment forces the neurohumoral
problems and coughing are often first symptoms in axis because of intravascular and in particular intraarterial
children with HF and hence unselective β-Blockers volume depletion; averts also adequate dosages of Beta-
may worsen these symptoms, too. The β1- to β2-AR- blocker and ACE-I. Additionally, infants with advanced
affinity of bisoprolol is almost 25 times higher to β1- DCM treated by catecholamines can oftentimes not be
AR in comparison to carvedilol (27). This means that weaned due to overtreatment of diuretics which leads
carvedilol needs a much higher dosage for blocking β1- in some to the inadequate indication for cardiac assist
AR comparing to bisoprolol and contemporary blocks device. Therefore, in most of the admitted young patients
the β2-AR. Blocking β2-AR means to lose the advantages with advanced DCM, diuretic treatment needs usually
of β2-AR preservation in terms of both cardio-protective to be weaned, before an adequate B-L-S therapy can
© Translational Pediatrics. All rights reserved. tp.amegroups.com Transl Pediatr 2019;8(2):127-132
130 Recla et al. Medical heart failure treatment
Algorithm for pediatric (age!) heart failure therapy (DCM, HFrEF)
Symptoms
at rest
NO may be YES
FC I-II FC II - III FC III - IV
HFmrEF LV-EF <40 LV-EF <35 (despite Inodilator)
LVEDD (z-score >+2) LVEDD >+/– 4.5 LVEDD >+4.5
RV function (RV >45%) RV function (RV >40%) RV function (RV >40%)
HR <110
Admit patient Milrinone
YES NO Start B-L-S start B-L-S
Re-assess If diuretics necessary
consider
Re-assess Start B-L-S rASD*
NO
re-assess Are symptoms
Improved in 48–72 hrs FC IV
normal
LV-EF <25
BNP, sodium
YES age < 5yrs (Inodilator + Catechol)
consider (RV <35%)
Patient discharge rPAB**
close re-assess Consider
“SC-therapy”
“fetal” circulation
Schranz 2018 HTx +/– AD
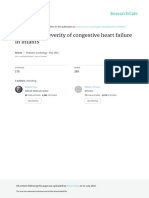
Figure 1 The figure shows our algorithm of pediatric heart failure (HF) therapy related to the clinical functional class (FC), LV-EF,
LVEDD in relation to the RV-EF (right ventricular ejection fraction). The scheme classifies the severity of heart failure with mid-
range (HFmrEF) and reduced ejection fraction (HFrEF); β-blocker therapy in terms of Bisoprolol, as a highly specific β1-selective AR-
blocker, is recommended in all FC and even considered in infants and young children with FC IV, when catecholamines are continuously
applicated in addition to PDE-3 inhibitors, as Milrinone and/or calcium sensitizer, Levosimendan (Giessen, personal experience, not
proofed in randomized controlled studies). Diuretics as a first line HF-drug is not recommended; patients with FC I and II, diuretics are
usually avoided; favoring adequate dosages of Bisoprolol (B), and the tissue angiotensin-converting inhibitor, Lisinopril (L); the combined
treatment with low-dosed Spironolactone (S) is summarized as B-L-S therapy. FC III, when the indication for diuretics might be indicated
on elevated filling pressures due to left atrial and pulmonary vein congestion, creation of a restrictive atrial septum defect (rASD) should be
considered (32*). In young children (less than 5 years) and in particular infants, a surgically performed reversible pulmonary artery banding
[rPAB; (33**)] is recommended in patients suffering left ventricular dilated cardiomyopathy (LV-DCM) with preserved right ventricular (pRV)
function and the infant or young child is considered for cardiac transplantation (HTx, LVEDD, z-value >+4.5). In case of biventricular
heart failure, resuscitation of a still patent, but constricted ductus arteriosus stenting or a surgical performed reverse Potts shunt should be
considered together with generating a left-right-shunting rASD; further with or without additional bilateral PAB (back to “fetal”, parallel
circulation); the strategy might be severe for bridging to cardiac transplant (HTx), avoiding assist device (AD) or cardiac recovery. BNP,
brain natriuretic peptide; heart rate; SC, stem cell; &, and.
be established. Considering further stimulation of the to this strategy, but in our opinion also the intermittent
neurohumoral axis by inadequate application of diuretics, application of the cytokine, erythropoietin. Furthermore,
the indication for long-term treatment should be strict erythropoietin seems to have cardioprotective effects
and not only based on the diagnosis HF (21). In case of a beyond of its stimulation of red cell production (34). Known
real indicated diuretic treatment, FC III–IV creation of a are also stem-cell mobilization and homing properties
restrictive interatrial communication should be considered leading to an increase of endothelial progenitor cells (35).
first and may be preferred over a long-term diuretic Therefore, we favor erythropoietin as a supportive therapy
treatment (Figure 1). in particular in young children with DCM.
Balanced oxygen consumption and delivery (DO 2 = Considering the regenerative potential of the
CaO2 × CO) is sine qua none of an optimized HF therapy; myocardium in children, which is inversely related to the
achieving an adequate hemoglobin level of 12–14 mg/L belongs patients age, all measures favoring regeneration should
© Translational Pediatrics. All rights reserved. tp.amegroups.com Transl Pediatr 2019;8(2):127-132
Translational Pediatrics, Vol 8, No 2 April 2019 131
be considered before cardiac transplantation. In this References
context it is important to mention, that the left and the
1. Hsu DT, Pearson GD. Heart Failure in Children Part I:
right heart do not act in isolation. Observing the nature
History, Etiology, and Pathophysiology. Circ Heart Fail
of congenital heart lesions, the importance of ventricular-
2009;2:63-70.
ventricular interaction (VVI) and the role of myocardial
2. Association NYH. Diseases of the heart and blood vessels:
proliferation properties in young children with the chance
nomenclature and criteria for diagnosis. Little, Brown, 1964.
for regeneration become obvious (8,36). In fact, VVI plays
3. Ross RD, Bollinger RO, Pinsky WW. Grading the severity
a pivotal role for heart function in human beings; the right
of congestive heart failure in infants. Pediatr Cardiol
and the left heart are strongly linked together sharing a
1992;13:72-5.
common ventricular septum, myofibers and pericardium
4. von Anrep G. On the part played by the suprarenals
(36,37). Additionally, as mentioned above, pressure overload
in the normal vascular reactions of the body. J Physiol
induces myocyte hyperplasia together with angiogenesis
1912;45:307-17.
but so far only in young children (9). Based on all of these
5. Katz AM. Ernest Henry Starling, His Predecessors, and
observations and gained knowledge, pulmonary artery
the “Law of the Heart.” Circulation 2002;106:2986-92.
banding (PAB) was introduced as a regenerative therapeutic
6. Mann DL, Bristow MR. Mechanisms and Models in
strategy in infants and young children with advanced
Heart Failure The Biomechanical Model and Beyond.
DCM provided for cardiac transplantation (32,33,38,39).
PAB was aimed to restore LV-geometry and synchrony by Circulation 2005;111:2837-49.
leftward shifting of the ventricular septum; VVI-interaction 7. Miyamoto SD, Stauffer BL, Nakano S, et al. Beta-
related preload decrease accompanied with a reduced left adrenergic adaptation in paediatric idiopathic dilated
ventricular end-diastolic volume and pressure. Along with cardiomyopathy. Eur Heart J 2014;35:33-41.
the PAB-induced pressure overload of the right ventricle, 8. Mollova M, Bersell K, Walsh S, et al. Cardiomyocyte
myocyte hyperplasia and hypertrophy are stimulated proliferation contributes to heart growth in young humans.
providing the endogenous regenerative ability of the Proc Natl Acad Sci 2013;110:1446-51.
especially young human heart. 9. Di Donato RM, Fujii AM, Jonas RA, et al. Age-dependent
ventricular response to pressure overload. Considerations
for the arterial switch operation. J Thorac Cardiovasc Surg
Conclusions 1992;104:713-22.
Treatment of life-threatening heart insufficiency in children 10. Kreidberg MB, Chernoff HL, Lopez WL. Treatment of
remains a great challenge. Lacking evidence-based clinical cardiac failure in infancy and childhood. N Engl J Med
trials and missing sufficient pediatric guidelines the 1963;268:23-30.
therapy remained almost unchanged since decades. One 11. Engle MA. When the child’s heart fails: Recognition,
chance for improvement of pediatric HF therapy might treatment, prognosis. Prog Cardiovasc Dis 1970;12:601-20.
be achieved by focusing on the current pathophysiological 12. Yancy CW, Jessup M, Bozkurt B, et al. 2017 ACC/
and pharmacological knowledge. It is hypothesized, that AHA/HFSA Focused Update of the 2013 ACCF/AHA
the target therapy should be based on the selective long- Guideline for the Management of Heart Failure: A Report
acting β1-Blocker Bisoprolol, the long-acting tissue ACE-I of the American College of Cardiology/American Heart
Lisinopril and mineralocorticoid-receptor antagonist Association Task Force on Clinical Practice Guidelines and
Spironolactone (named as BLS-therapy). the Heart Failure Society of America. J Am Coll Cardiol
2017;70:776-803.
13. Pasquali SK, Hall M, Slonim AD, et al. Off-Label Use of
Acknowledgements
Cardiovascular Medications in Children Hospitalized With
None. Congenital and Acquired Heart Disease. Circ Cardiovasc
Qual Outcomes 2008;1:74-83.
14. Rodriguez W, Selen A, Avant D, et al. Improving Pediatric
Footnote
Dosing Through Pediatric Initiatives: What We Have
Conflicts of Interest: The authors have no conflicts of interest Learned. Pediatrics 2008;121:530-9.
to declare. 15. Shaddy RE, Boucek MM, Hsu DT, et al. Carvedilol for
© Translational Pediatrics. All rights reserved. tp.amegroups.com Transl Pediatr 2019;8(2):127-132
132 Recla et al. Medical heart failure treatment
children and adolescents with heart failure: A randomized children. J Heart Lung Transplant 2013;32:1045-6.
controlled trial. JAMA 2007;298:1171-9. 29. Chrysant SG. Vascular remodeling: The role of
16. Azeka E, Franchini Ramires JA, Valler C, et al. Delisting angiotensin-converting enzyme inhibitors. Am Heart J
of infants and children from the heart transplantation 1998;135:S21-30.
waiting list after carvedilol treatment. J Am Coll Cardiol 30. Saha SA, Molnar J, Arora RR. Tissue ACE inhibitors
2002;40:2034-8. for secondary prevention of cardiovascular disease in
17. Buchhorn R, Hulpke-Wette M, Hilgers R, et al. patients with preserved left ventricular function: a pooled
Propranolol treatment of congestive heart failure in infants meta-analysis of randomized placebo-controlled trials. J
with congenital heart disease: The CHF-PRO-INFANT Cardiovasc Pharmacol Ther 2007;12:192-204.
Trial. Int J Cardiol 2001;79:167-73. 31. Masutani S, Saiki H, Kurishima C, et al. Heart Failure
18. Frobel AK, Hulpke-Wette M, Schmidt KG, et al. Beta- With Preserved Ejection Fraction in Children. Circ J
blockers for congestive heart failure in children. Cochrane 2013;77(9).
Database Syst Rev 2009;(1):CD007037. 32. Bauer A, Esmaeili A, deRosa R, et al. Restrictive atrial
19. Albers S, Meibohm B, Mir TS, et al. Population communication in right and left heart failure. Transl
pharmacokinetics and dose simulation of carvedilol in Pediatr 2019;8:133-9.
paediatric patients with congestive heart failure. Br J Clin 33. Michel-Behnke I, Pavo I, Recla S, et al. Regenerative
Pharmacol 2008;65:511-22. therapies in young hearts with structural or congenital
20. Harmon WG, Sleeper LA, Cuniberti L, et al. Treating heart disease. Transl Pediatr 2019;8:140-50.
Children With Idiopathic Dilated Cardiomyopathy (from 34. Burger D, Xenocostas A, Feng QP. Molecular basis of
the Pediatric Cardiomyopathy Registry). Am J Cardiol cardioprotection by erythropoietin. Curr Mol Pharmacol
2009;104:281-6. 2009;2:56-69.
21. Kantor PF, Lougheed J, Dancea A, et al. Presentation, 35. Heeschen C, Aicher A, Lehmann R, et al. Erythropoietin
Diagnosis, and Medical Management of Heart Failure in is a potent physiologic stimulus for endothelial progenitor
Children: Canadian Cardiovascular Society Guidelines. cell mobilization. Blood 2003;102:1340-6.
Can J Cardiol 2013;29:1535-52. 36. Friedberg MK, Redington AN. Right Versus Left
22. Moffett BS, Price JF. National Prescribing Trends for Ventricular Failure Differences, Similarities, and
Heart Failure Medications in Children. Congenit Heart Interactions. Circulation 2014;129:1033-44.
Dis 2015;10:78-85. 37. Smerup M, Nielsen E, Agger P, et al. The Three-
23. Schranz D, Voelkel NF. “Nihilism” of chronic heart failure Dimensional Arrangement of the Myocytes Aggregated
therapy in children and why effective therapy is withheld. Together Within the Mammalian Ventricular Myocardium.
Eur J Pediatr 2016;175:445-55. Anat Rec (Hoboken) 2009;292:1-11.
24. Bernstein D, Fajardo G, Zhao M. The Role of β-adrenergic 38. Schranz D, Rupp S, Müller M, et al. Pulmonary artery
Receptors in Heart Failure: Differential Regulation of banding in infants and young children with left ventricular
Cardiotoxicity and Cardioprotection. Prog Pediatr Cardiol dilated cardiomyopathy: A novel therapeutic strategy
2011;31:35-8. before heart transplantation. J Heart Lung Transplant
25. Xiao RP, Zhu W, Zheng M, et al. Subtype-specific 2013;32:475-81.
β-adrenoceptor signaling pathways in the heart and their 39. Schranz D, Akintuerk H, Bailey L. Pulmonary Artery
potential clinical implications. Trends Pharmacol Sci Banding for Functional Regeneration of End-Stage
2004;25:358-65. Dilated Cardiomyopathy in Young Children: World
26. Navaratnarajah M, Siedlecka U, Ibrahim M, et al. Impact Network Report. Circulation 2018;137:1410-2.
of combined clenbuterol and metoprolol therapy on
reverse remodelling during mechanical unloading. PloS
One 2014;9:e92909.
Cite this article as: Recla S, Schmidt D, Logeswaran T,
27. Ladage D, Schwinger RHG, Brixius K. Cardio-selective
Esmaeili A, Schranz D. Pediatric heart failure therapy: why β1-
beta-blocker: pharmacological evidence and their influence
receptor blocker, tissue ACE-I and mineralocorticoid-receptor-
on exercise capacity. Cardiovasc Ther 2013;31:76-83.
blocker? Transl Pediatr 2019;8(2):127-132. doi: 10.21037/
28. Recla S, Steinbrenner B, Schranz D. Medical therapy in
tp.2019.04.08
dilated cardiomyopathy and pulmonary arterial banding in
© Translational Pediatrics. All rights reserved. tp.amegroups.com Transl Pediatr 2019;8(2):127-132
You might also like
- Annex A. ChecklistDocument2 pagesAnnex A. ChecklistroseannurakNo ratings yet
- Ductus ArteriosoDocument17 pagesDuctus ArteriosoJohn Romero CevallosNo ratings yet
- A Review of The Mechanism of Action of Drugs Used in Congestive Heart Failure in PediatricsDocument9 pagesA Review of The Mechanism of Action of Drugs Used in Congestive Heart Failure in PediatricsFernando CardiologíaNo ratings yet
- Age-Stratified Revision of Ross Classification for Pediatric Heart FailureDocument6 pagesAge-Stratified Revision of Ross Classification for Pediatric Heart FailureCitra Eva MeilyndhaNo ratings yet
- Jurnal AnakDocument9 pagesJurnal AnakIndah IndrianiNo ratings yet
- Blood Pressure Management in Children On DialysisDocument12 pagesBlood Pressure Management in Children On DialysisinaNo ratings yet
- Brief: Pediatric Pulmonary HypertensionDocument5 pagesBrief: Pediatric Pulmonary HypertensionAudylia HartonoNo ratings yet
- Pediatric PHDocument10 pagesPediatric PHAdrian KhomanNo ratings yet
- Inotropicos en Neonatos 2Document13 pagesInotropicos en Neonatos 2Paola DiazNo ratings yet
- An Update On The Diagnosis and Treatment of Pediatric Pulmonary HypertensionDocument16 pagesAn Update On The Diagnosis and Treatment of Pediatric Pulmonary HypertensionM.m. BekkarNo ratings yet
- Bosentan en NiñosDocument8 pagesBosentan en NiñosvictorballenNo ratings yet
- International Journal of Preventive MedicineDocument14 pagesInternational Journal of Preventive MedicineireneaureliaNo ratings yet
- E351 Full PDFDocument13 pagesE351 Full PDFajes coolNo ratings yet
- HT PedDocument18 pagesHT PedLina María CañónNo ratings yet
- Epidemiology of Familial Hypercholesterolaemia CoDocument9 pagesEpidemiology of Familial Hypercholesterolaemia CoSusana RocheNo ratings yet
- Consenso IccDocument15 pagesConsenso IccMaida Martinez AngelesNo ratings yet
- Barst RJ 2011 Pulmonary Arterial Hypertension A Comparison Between Children and AdultsDocument13 pagesBarst RJ 2011 Pulmonary Arterial Hypertension A Comparison Between Children and Adultsdr.herusetiawanNo ratings yet
- Pediatric Pulmonary Hypertension: y Z X JJ (# Z # Yy ZZDocument10 pagesPediatric Pulmonary Hypertension: y Z X JJ (# Z # Yy ZZOlivia DwimaswastiNo ratings yet
- HHS Public Access: Pulmonary Hypertension in ChildrenDocument44 pagesHHS Public Access: Pulmonary Hypertension in ChildrenLina María CañónNo ratings yet
- Efek Steroid HSPDocument16 pagesEfek Steroid HSPFarida UlfaNo ratings yet
- Pi Is 0149291820302836Document15 pagesPi Is 0149291820302836John SMithNo ratings yet
- Pediatric Pulmonary Hypertension: y Z X JJ (# Z # Yy ZZDocument10 pagesPediatric Pulmonary Hypertension: y Z X JJ (# Z # Yy ZZFrancisoSilvaNo ratings yet
- Management of Heart Failure With Preserved EjectionFraction A Review PDFDocument13 pagesManagement of Heart Failure With Preserved EjectionFraction A Review PDFGharbi StrongNo ratings yet
- Hipertension Pulmonar PeditriaDocument8 pagesHipertension Pulmonar PeditriajesusgonzalezapNo ratings yet
- Epidemiology and Outcomes of Acute Decompensated Heart Failure in Critically Ill ChildrenDocument25 pagesEpidemiology and Outcomes of Acute Decompensated Heart Failure in Critically Ill ChildrenLufthi FahrezaNo ratings yet
- CHF AAPDocument11 pagesCHF AAPFajar Al-HabibiNo ratings yet
- Accepted Manuscript: YprrvDocument27 pagesAccepted Manuscript: YprrvTiara Grhanesia DenashuryaNo ratings yet
- Maternal Hemodynamics: A Method To Classify Hypertensive Disorders of PregnancyDocument23 pagesMaternal Hemodynamics: A Method To Classify Hypertensive Disorders of PregnancyaulianmediansyahNo ratings yet
- Heart Failure With Preserved Ejection Fraction - JAMA (2023)Document12 pagesHeart Failure With Preserved Ejection Fraction - JAMA (2023)cheve glzNo ratings yet
- Evaluation and Management of Elevated Blood Pressures in Hospitalized ChildrenDocument11 pagesEvaluation and Management of Elevated Blood Pressures in Hospitalized ChildrenKhaoulapediatreNo ratings yet
- Heart Failure in ChildrenDocument27 pagesHeart Failure in ChildrendenakarinaNo ratings yet
- Dulfer 2013Document9 pagesDulfer 2013Clarice PortugalNo ratings yet
- SEHGAL 2016 - A New Look at Bronchopulmonary Dysplasia - Post Capillary Pathophysiology and Cardiac DysfunctionDocument8 pagesSEHGAL 2016 - A New Look at Bronchopulmonary Dysplasia - Post Capillary Pathophysiology and Cardiac DysfunctionRafael JustinoNo ratings yet
- Jillinger, PausDocument19 pagesJillinger, PausyessiNo ratings yet
- Heart Rate Variability Alterations in Infants With Spontaneous HypertoniaDocument8 pagesHeart Rate Variability Alterations in Infants With Spontaneous HypertoniaAlexis Arce AlvarezNo ratings yet
- Pulmonary Hypertension in Bronchopulmonary DysplasiaDocument10 pagesPulmonary Hypertension in Bronchopulmonary DysplasiaIván Gustavo Magaña CeballosNo ratings yet
- Journal explores hypno-breathing for heart failure patientsDocument4 pagesJournal explores hypno-breathing for heart failure patientsedo100% (1)
- Angiogenic profile identifies pulmonary hypertension in children with Down syndromeDocument8 pagesAngiogenic profile identifies pulmonary hypertension in children with Down syndromebaba ababNo ratings yet
- ADHF ManagementDocument6 pagesADHF ManagementEsti YunitaNo ratings yet
- Congestive Heart Failure !1 Running Head: Congestive Heart FailureDocument11 pagesCongestive Heart Failure !1 Running Head: Congestive Heart Failureapi-543558169No ratings yet
- Current State of Pediatric Heart FailureDocument16 pagesCurrent State of Pediatric Heart FailureAstridcarolinaTelloNo ratings yet
- Growth indicators in children with congenital heart diseaseDocument7 pagesGrowth indicators in children with congenital heart diseasemuhammadrikiNo ratings yet
- S0022347621003152Document8 pagesS0022347621003152Vedith KumarNo ratings yet
- Rhythm Control of Atrial Fibrillation in Heart FailureDocument9 pagesRhythm Control of Atrial Fibrillation in Heart FailureUCI CONTINGENCIANo ratings yet
- Heart Failure in Patients With Metabolic Syndrome XDocument12 pagesHeart Failure in Patients With Metabolic Syndrome XErwin SiahaanNo ratings yet
- Rainer Kozlik-Feldmann, Georg Hansmann, Damien Bonnet, Dietmar Schranz, Christian Apitz, Ina Michel-BehnkeDocument7 pagesRainer Kozlik-Feldmann, Georg Hansmann, Damien Bonnet, Dietmar Schranz, Christian Apitz, Ina Michel-BehnkeHerdinadNo ratings yet
- Richardson2021 Article L-typeCalciumChannelBlockerUseDocument9 pagesRichardson2021 Article L-typeCalciumChannelBlockerUsetrikusumaNo ratings yet
- Regression of Left-Ventricular Hypertrophy in Children and Adolescents With Hypertension During Ramipril MonotherapyDocument7 pagesRegression of Left-Ventricular Hypertrophy in Children and Adolescents With Hypertension During Ramipril Monotherapy69262650irinaNo ratings yet
- HF in ElderlyDocument3 pagesHF in ElderlyHadi M.WNo ratings yet
- 2012RossClassificationarticleinPedCardiology PDFDocument7 pages2012RossClassificationarticleinPedCardiology PDFKumiko MichishigeNo ratings yet
- Update On The Use of Sildenafil in Neonatal Pulmonary Hypertension. A Narrative Review of The History, Current Administration and Future DirectionsDocument10 pagesUpdate On The Use of Sildenafil in Neonatal Pulmonary Hypertension. A Narrative Review of The History, Current Administration and Future DirectionsFer45No ratings yet
- 63. Barnes 1998. Central adiposity and hemodynamic functioning at rest andDocument9 pages63. Barnes 1998. Central adiposity and hemodynamic functioning at rest andnaiarahsanzNo ratings yet
- 10.1007@s12098 019 02884 W PDFDocument2 pages10.1007@s12098 019 02884 W PDFputri vinia /ilove cuteNo ratings yet
- Develop Med Child Neuro - 2022 - Houwen Van Opstal - Long Term Outcomes For Females With Early Onset DystrophinopathyDocument12 pagesDevelop Med Child Neuro - 2022 - Houwen Van Opstal - Long Term Outcomes For Females With Early Onset DystrophinopathyJessica CampoNo ratings yet
- CDH and Pulmonary HypertensionDocument6 pagesCDH and Pulmonary HypertensionStollery SandboxNo ratings yet
- SildenafilDocument12 pagesSildenafilrizkaNo ratings yet
- Cardiac Failure in Children Treatment ReviewDocument31 pagesCardiac Failure in Children Treatment ReviewZakaria MukallaNo ratings yet
- Essential Hypertension in Ten & Half Years Old Boy: A Case ReportDocument3 pagesEssential Hypertension in Ten & Half Years Old Boy: A Case ReportYunika ArumNo ratings yet
- Treatment of Henoch Schonlein Purpura What Evidence Do We HaveDocument8 pagesTreatment of Henoch Schonlein Purpura What Evidence Do We Haveida ayu agung WijayantiNo ratings yet
- EPO in Anemia CHFDocument10 pagesEPO in Anemia CHFAlizaPinkyNo ratings yet
- Hypertension in Children and Adolescents: New PerspectivesFrom EverandHypertension in Children and Adolescents: New PerspectivesEmpar LurbeNo ratings yet
- Daftar PustakaDocument4 pagesDaftar PustakaMita RahNo ratings yet
- Daftar PustakaDocument3 pagesDaftar PustakaEvelina Navi BraginskiyNo ratings yet
- Daftar PustakaDocument3 pagesDaftar PustakaMita RahNo ratings yet
- Daftar PustakaDocument3 pagesDaftar PustakaMita RahNo ratings yet
- Daftar PustakaDocument3 pagesDaftar PustakaEvelina Navi BraginskiyNo ratings yet
- Sensus Pasien Stase Ilmu Kesehatan Anak - Ruang BayiDocument2 pagesSensus Pasien Stase Ilmu Kesehatan Anak - Ruang BayiMita RahNo ratings yet
- 01156Document13 pages01156riskysetNo ratings yet
- MR DR Dika 21 Okt 19Document14 pagesMR DR Dika 21 Okt 19Mita RahNo ratings yet
- E383 Full PDFDocument11 pagesE383 Full PDFBarryNo ratings yet
- Autophagy and CancerDocument349 pagesAutophagy and CancerSohibun21No ratings yet
- Temu Ilmiah Reumatologi (TIR) 2023 - Perhimpunan Reumatologi IndonesiaDocument1 pageTemu Ilmiah Reumatologi (TIR) 2023 - Perhimpunan Reumatologi IndonesiabelanjayukdiNo ratings yet
- Act 1. PhobiasDocument2 pagesAct 1. PhobiasRoxanne CastilloNo ratings yet
- Eight Hallmarks of Cancer ExplainedDocument40 pagesEight Hallmarks of Cancer ExplainedArnab KalitaNo ratings yet
- Retinoblastoma Clinical and Pathological ClassificationDocument9 pagesRetinoblastoma Clinical and Pathological ClassificationSonia SaulésNo ratings yet
- Lab Value MnemonicsDocument10 pagesLab Value MnemonicsSophia CuertoNo ratings yet
- Vital Signs ChecklistDocument21 pagesVital Signs ChecklistJapsay Francisco GranadaNo ratings yet
- Data FinalDocument72 pagesData FinalAchsan KamalNo ratings yet
- Use of Local and Axial Pattern Flaps For Reconstruction of The Hard and Soft Palate PDFDocument9 pagesUse of Local and Axial Pattern Flaps For Reconstruction of The Hard and Soft Palate PDFJose Luis Granados SolerNo ratings yet
- Review Article: Guided Bone Regeneration: A Literature ReviewDocument16 pagesReview Article: Guided Bone Regeneration: A Literature ReviewGonçalo Gomes SanchesNo ratings yet
- Shaukat Khanum Memorial Cancer Hospital & Research CentreDocument2 pagesShaukat Khanum Memorial Cancer Hospital & Research CentreUsama AjmalNo ratings yet
- Heritage Health - Pre Auth FormDocument6 pagesHeritage Health - Pre Auth FormBOOKREADER_NOWNo ratings yet
- Cardiac Case Study NDDocument11 pagesCardiac Case Study NDapi-313165458No ratings yet
- Congenital Anatomic AnomaliesDocument12 pagesCongenital Anatomic Anomaliesmahparah_mumtazNo ratings yet
- College of Nursing: Pharmacology Drug StudyDocument2 pagesCollege of Nursing: Pharmacology Drug StudyChristine Pialan SalimbagatNo ratings yet
- Introduction To Emergency Medical Services (EMS)Document17 pagesIntroduction To Emergency Medical Services (EMS)ishak1863No ratings yet
- Muhammad YounasDocument4 pagesMuhammad YounasHamid IqbalNo ratings yet
- Distraksi Menonton Efektif Menurunkan Nyeri Ringan Pasien: Congestive Heart Failure (CHF)Document7 pagesDistraksi Menonton Efektif Menurunkan Nyeri Ringan Pasien: Congestive Heart Failure (CHF)Devy YahyaNo ratings yet
- Treatment of Endometriosis in Women Desiring FertilityDocument23 pagesTreatment of Endometriosis in Women Desiring FertilityVaisnavi Muthoovaloo67% (3)
- 1 - Indocyanine Green-Enhanced Fluorescence To Assess BowelDocument7 pages1 - Indocyanine Green-Enhanced Fluorescence To Assess BowelIcaro DanielNo ratings yet
- Benazepril Hydrochloride (Drug Study)Document3 pagesBenazepril Hydrochloride (Drug Study)Franz.thenurse6888100% (1)
- EMT Training at Mansion Mandiri HotelDocument4 pagesEMT Training at Mansion Mandiri Hotelyuna triazNo ratings yet
- Unconventional Fixed Partial Denture: A Simple Solution For Aesthetic RehabilitationDocument4 pagesUnconventional Fixed Partial Denture: A Simple Solution For Aesthetic RehabilitationAdvanced Research PublicationsNo ratings yet
- Child Clinical Interview Form OnlineDocument24 pagesChild Clinical Interview Form OnlineMonica Bolocan100% (3)
- DR Putu Gde Hari WangsaDocument5 pagesDR Putu Gde Hari Wangsahariwangsa23No ratings yet
- 4 - Tracheostomy Care and SuctioningDocument4 pages4 - Tracheostomy Care and SuctioningABEGAIL BALLORANNo ratings yet
- List of Consultants at KEM Hospital PuneDocument8 pagesList of Consultants at KEM Hospital PuneRitesh AkhandeNo ratings yet
- Cover Letter To The EditorDocument2 pagesCover Letter To The EditorMohamed GhaliNo ratings yet