Professional Documents
Culture Documents
Nasal DD
Uploaded by
Riham Ar AbOriginal Description:
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Nasal DD
Uploaded by
Riham Ar AbCopyright:
Available Formats
61
Intranasal Drug Delivery
Daniel P. Wermeling and Jodi L. Miller
University of Kentucky, Lexington, Kentucky, U.S.A.
I. INTRODUCTION
Over half a century ago, Noah Fabricant stated, “The use of nasal medication
has never been as widespread and popular as it is today. . . . Nasal medication
actually may be considered tapping on the door of maturity. The tapping should
grow louder, for there is ample evidence to demonstrate that it will continue to
improve with the passing of time” [1]. Now, almost 60 years later, these senti-
ments still ring true. In the year 2000, there were 27 products on the U.S. market
for intranasal use, with more than half of these obtaining Food and Drug Adminis-
tration approval between 1990 and 2000. The market value of these products
was estimated to be 1.5 billion dollars [2]. With ever-increasing pharmaceutical
technology and numerous medicinal opportunities for intranasal administration,
its popularity will most likely continue.
Depending on the therapeutic intent, intranasal drugs may be targeted for
local treatment or systemic action. The majority of products currently marked in
the United States for local effects are steroidal agents for treatment and prevention
of nasal symptoms. Intranasal drugs for systemic action include treatments for
migraine headaches, calcium supplementation, vitamin B12 deficiency, and pain
relief, as well as other therapeutic indications [2]. The variety of agents currently
available is impressive; however, the list of nasal products should expand drasti-
cally over the next few years. This chapter will mainly focus on intranasal prod-
ucts designed for systemic delivery. In addition to either local or systemic effects,
agents may be intended for acute or chronic treatment. The expected duration of
treatment and therapeutic use will also impact product design.
727
Copyright © 2003 Marcel Dekker, Inc.
728 Wermeling and Miller
Nasal administration offers many benefits compared to alternate delivery
routes. Not only is the nasal cavity easily accessible, it is virtually noninvasive.
In most cases intranasal administration is well tolerated; however, depending on
the substance delivered, slight momentary irritation may occur. Owing to the
nasal cavity’s extensive vascular supply, absorption rates and onset of action for
systemic medications are comparable to injectable administration routes yet the
need for needles is eliminated. In addition, hepatic first-pass metabolism is
avoided with intranasal delivery and destruction of drugs by gastric fluid is not
a concern.
II. NASAL ANATOMY AND PHYSIOLOGY
The basic nasal structures are shown in Figure 1 [3]. The distance from the tip
of the nose to the pharyngeal wall is about 10–12 cm [4]. The nasal septum
divides the nose into two nasal cavities, each with a 2–4-mm-wide slit opening
[4]. Each cavity has a surface area of approximately 75 cm2, a volume of 7.5
mL, and contains three distinct functional regions [5]. The vestibular region is
located closest to the nasal passage opening, contains long hairs, and serves as
a filter for incoming particles [6]. The respiratory region, containing the largest
surface area, is located between the vestibular and olfactory regions [6]. The
Figure 1 Diagrammatic representation of the exposed mucosal surface of the nasal lat-
eral wall and turbinate of the human. Distribution of the four epithelial populations is also
shown. SS, squamous epithelium; TE, transitional (nonciliated, cuboidal) epithelium; RE,
respiratory epithelium; OE, olfactory epithelium; N, nares; HP, hard palate; NP, nasophar-
ynx; ST, superior turbinate; MT, middle turbinate; IT, inferior turbinate. (Modified from
Ref. [3] with permission.)
Copyright © 2003 Marcel Dekker, Inc.
Intranasal Drug Delivery 729
respiratory region is considered the most important section for delivering drugs
systemically and will be discussed in more detail below [5]. Finally, the olfactory
region is located in the uppermost portion of each cavity and opposite the septum
[5,6]. This is the region responsible for functions associated with smell.
The epithelium of the respiratory region consists of four different cell types
(Fig. 2): basal, mucus-containing goblet, ciliated columnar, and nonciliated co-
lumnar [5,7]. The ciliated columnar cell is the most predominant. The cilia beat
in a wave-like, coordinated manner to transport mucus and trapped particles to
the pharynx area for subsequent ingestion [5,6]. Cells in the respiratory region
are covered by approximately 300 microvilli, which greatly increase the surface
area of the nasal cavity [5]. The respiratory region also contains the inferior,
middle, and superior turbinates [5]. The lamina propria, below the epithelium,
houses blood vessels, nerves, and both serous and mucus secretory glands [7].
Blood is delivered to the nose from the external and internal carotid arteries
[5,8]. The lateral and medial nasal walls are directly supplied by the sphenopala-
tine artery, which is a distant branch of the external carotid [8]. These sections
of the nose are drained by the sphenopalatine foramen [5]. The anterior section
of the nose receives blood from the ophthalmic arterial branch of the internal
carotid and is drained via the facial vein [5,8]. The lamina propia contains a
dense network of capillaries, including many very permeable fenestrated capillar-
ies [4,8].
The vidian nerve provides the majority of cholinergic innervation to the
nasal cavity. When stimulated, acetylcholine is released and vasodilatation occurs
Figure 2 Schematic representation of transport routes across nasal respiratory epithe-
lium: (1) paracellular; (2) transcellular; (3) transcytotic. Goblet cells (g), ciliated columnar
cells (c), and tight junctions (tj) are presented. Basal cells (b) are located on the basal
lamina (bl) adjacent to the lamina propia (lp) with blood vessels (v). (From Ref. [48] with
permission.)
Copyright © 2003 Marcel Dekker, Inc.
730 Wermeling and Miller
[4]. Sympathetic innervation to the nose arises from the stellate ganglion [4].
Released norepinephrine acts on both α and β2 receptors and the overall result
is vasoconstriction, demonstrating dominance of the α receptor [4].
A mucus layer, resulting from nasal and lacrimal gland secretions as well
as plasma transudate, is present on the nasal passage epithelium [7–9]. The pH
of secretions ranges from 5.5 to 6.5 and from 5.0 to 6.7 in adults and children,
respectively [10]. The mucus consists of an outer viscous layer of mucus (gel)
and a watery (sol) layer located along the mucosal surface [8,9]. Glycoproteins,
particularly mucin, are responsible for the gel-like appearance of the mucus. Ly-
sozymes, enzymes, and immunoglobulins in addition to other proteins may also
be found in the mucus. Approximately 3% of the mucus consists of these proteins
while the remainder is made of 90–95% water and 1–2% salt. Each day about
1500 to 2000 mL of mucus is produced [7,8]. The epithelium is covered with a
new mucus layer approximately every 10 min [8].
Mucosal clearance is an important defense function of the nasal passage.
Clearance occurs as a combined effort of the mucus layer and cilia action. The
cilia project into the sol layer where they move in a sweeping motion back and
forth. The gel layer of the mucus, along with entrapped particles, is transported
to the nasopharyngeal area for ingestion [7]. The cilia beat at a frequency of
approximately 10–13 Hz [11,12]. This results in the movement of mucus at a
rate of approximately 5–6 mm/min and therefore clearance of particles from the
nose within 20 min [4,9].
Xenobiotic-metabolizing enzymes are present in the nasal mucosa [8,9,
13–19]. In animals, these enzymes are found in greater quantities in the olfac-
tory epithelium compared to the respiratory epithelium of the nose. In humans,
this distinction remains unclear owing to difficulty obtaining olfactory epithelium
[13,14]. In the respiratory mucosa of humans, the concentration of cytochrome
P450 enzymes is 25 pmol/mg of microsomal protein [19]. Isoforms of the P450
enzyme that have been identified in humans thus far include CYP1A, CYP2A,
and CYP2E [14]. Carboxylesterases, glutathione S-transferases, and rhodanese
enzymes have also been detected in the human nasal mucosa [20–23].
Normal physiology of the nasal passage is subject to alteration as a result
of many environmental and pathological factors. Some of these are encountered
quite frequently in the general population, including the common cold and other
respiratory viruses [24], allergic [25–30] and nonallergic rhinitis [31,32] as well
as treatment of these conditions, smoking [33,34], and the process of aging [35].
Additionally, although some conflict exists in the medical literature, estrogen is
believed to induce physiological changes in the nose [36–43]. Alterations in the
nasal cavity may also be caused by the presence of a deviated septum [44], immo-
tile cilia syndrome [45], or nasal polyps [46]. The potential effects of these modi-
fications on local drug action or systemic exposure should be taken into account
when considering intranasal administration.
Copyright © 2003 Marcel Dekker, Inc.
Intranasal Drug Delivery 731
III. INTRANASAL DRUG ABSORPTION
To reach the vascular system substances intended for systemic absorption must
first pass through the mucus layer followed by the epithelium. A review by Khan-
vilkar et al. [47] addresses the numerous issues associated with drug transfer
through mucus. The mucus does not present a major problem for small, uncharged
particles. On the other hand, some larger or charged molecules may encounter
difficulties passing through this layer. One important rate-limiting factor in the
diffusion of drug through the mucus is potential binding of solutes to mucin.
Types of interactions between foreign molecules and the mucus include electro-
static, hydrophobic, and van der Waals. In addition, the mucus’ structure is very
sensitive to its environment, meaning that alterations in pH, temperature, osmotic
pressure, etc. may induce structural changes in this layer. This dynamic nature
of the mucus may cause variations in the transfer of molecules from the delivery
site to the epithelium [47].
Once a substance passes through the mucus, it may cross the nasal mucosa
by three different mechanisms (Fig. 2) [48]. First, it may be transferred via trans-
cellular, or simple, diffusion across the membrane by way of pores or carriers
[18,49]. A second method is paracellular transport, which involves movement
through the spaces between cells and tight junctions [18]. This pathway is be-
lieved to be important for absorption of peptides and proteins [50,51]. The third
mechanism is transcytosis. This entails particle uptake into vesicles, subsequent
transfer across the cell, and, finally, deposition into the interstitial space [49].
In addition to passing through the mucus layer and penetration through the
epithelium, substances may undergo metabolism by nasal enzymes present in the
mucosa. Also, because of normal physiological mucocilliary clearance mecha-
nisms, drugs have limited absorption time in the nasal cavity. Both of these are
important factors to keep in mind for intranasal drug absorption. Furthermore, it
has also been suggested that redistribution of molecules within the nasal mucosa
is a possibility [51]. This recycling effect would be beneficial for topical agents;
however, it may affect the absorption kinetics for drugs intended for systemic
action.
Pharmacokinetic parameters following intranasal absorption will vary with
administration of different agents. Values in the literature for time to reach maxi-
mum concentration in humans range from 5 min to 4 h [52–59]. Also, bioavail-
ability with intranasal delivery greatly varies and is dependent on numerous fac-
tors such as the drug itself, formulation differences, and the delivery system, all
of which will affect nasal exposure, extent of absorption, and the pharmacokinet-
ics of each particular agent or formulation.
One last consideration for intranasal absorption is the potential transfer of
substances from the nasal cavity directly to the central nervous system (CNS).
This topic has been reviewed elsewhere in the scientific literature [56]. In rats,
Copyright © 2003 Marcel Dekker, Inc.
732 Wermeling and Miller
CNS uptake of fluorescein-isothiocyanate-labeled dextrans of differing molecular
weights (4400–40500 Da) [60], 3H-dihydroergotamine [61], and 3H-5-fluoroura-
cil [62] following intranasal and intravenous (IV) administration has been stud-
ied. Sakane et al. [60] found undetectable levels of all the dextrans studied in
the cerebrospinal fluid (CSF) after the IV dose. However, levels were detectable
for dextrans with a MW ⱕ20,000 Da in the CSF with intranasal administration.
Wang et al. [61] found comparable or greater levels of radiolabeled dihydroergo-
tamine in different regions of the brain with IV and intranasal administration
despite lower intranasal plasma radioactivity concentration-time profiles. Sakane
et al. [62] observed significantly higher ratios for CSF/plasma and cerebral
cortex/plasma concentrations with intranasal instillation as compared to IV infu-
sion. Observations from these three investigations suggest a direct pathway does
exist from the nasal cavity to the CNS.
Three potential mechanisms exist for the delivery from the nose to the
brain. First, drug that reaches the systemic circulation may then subsequently
cross the blood-brain barrier. Second, substances may cross the olfactory epithe-
lium via simple diffusion, receptor-mediated transcytosis, or paracellular trans-
port. The substance may then follow the nerve to the CNS or gain entry to the
lamina propria. From the lamina propria, drugs may enter either the lymphatic
system or systemic circulation [6]. Third, an agent may be taken up by a neuronal
cell of the olfactory nerve, undergo intracellular axonal transport, and gain entry
to the brain via the olfactory bulb [5,6]. The possibility of direct penetration into
the CNS may be desirable for some agents; however, it may be problematic for
others.
IV. CONSIDERATIONS FOR INTRANASAL PRODUCT
DESIGN
A. Drug Formulation
Many factors play a role in the absorption of substances from the nasal cavity.
These factors mostly center on the chemical attributes of a particular agent, the
excipients in the formulation, and means of delivery. Molecular weight is be-
lieved to offer the best correlation with extent of absorption [50,63]. Agents with
a molecular weight less than 1000 are absorbed to a much larger degree than
agents with molecular weights greater than 1000. For larger molecules, the addi-
tion of an adjuvant may be useful [49]. Not only is molecular weight important
in absorption, but also the molecular size and shape of an agent. Cyclic-shaped
molecules are better absorbed than those having a linear structure [49]. Particle
size is also important because spray particles less than 10 µm may bypass the
nasal cavity and be deposited in the lungs [12]. For powder formulations, a parti-
Copyright © 2003 Marcel Dekker, Inc.
Intranasal Drug Delivery 733
cle size of greater than 50 µm has been shown to provide a favorable pattern of
distribution in the nose [64].
Systemic bioavailability decreases as the hydrophilicity of an agent in-
creases [65]. Bioavailability is affected by pH and pKa factors as well [66–69].
The pH of the drug, formulation, and nasal cavity all need to be taken into ac-
count. It is generally well known that un-ionized chemical species are capable
of moving across membrane barriers more readily than ionized species, and thus,
increased absorption usually occurs. However, drug formulations should not be
extremely acidic because they may cause damage to the nasal epithelium and
surface enzymes [67,69]. Although increased absorption could result from the
structural damage, nasal integrity should not be compromised. Designing formu-
lations so the final pH is within a range of 4.5–6.5 is suggested to minimize nasal
irritation [68]. Another formulation factor to consider is osmolarity. In one study,
when the osmolarity of the solution was adjusted with mannitol greater biological
activity of the delivered agent was observed [68]. Additionally, a study in rats
demonstrated a solution of 0.462 M provided the best absorption of secretin al-
though shrinkage of epithelial cells was observed [66].
Other elements to consider when designing agents for intranasal adminis-
tration are the solution concentration and volume to be delivered. One study
focused on intranasal insulin delivery determined a higher concentration did not
produce significantly greater activity [70]. On the other hand, the initial drug
concentration has been found to influence nasal absorption [9,71]. Larger delivery
volumes allow better distribution and coverage of the nasal passage, which theo-
retically would lead to greater drug absorption. One study suggests a larger vol-
ume with a weaker concentration is preferable to a small, very concentrated vol-
ume [9,72]. Another study demonstrated higher plasma peak levels and biological
response when the total spray volume delivered per nostril (100 µL) was deliv-
ered as two separate sprays (50 µL each) [73]. The volume that can be reasonably
delivered is also limited by the size of the nasal cavity. Behl et al. [68] suggest
an upper limit of 25 mg/dose and a volume of 25–150 µL/nostril.
Since the normal physiological process of the nose, i.e., mucocilliary clear-
ance, is critical to its defense mechanisms, disruption should be avoided. Sub-
stances delivered to the nasal cavity may cause inhibition of this system or en-
hance the clearance process [7,74]. Enhancing this process in most cases would
be undesirable because the time for drug absorption would decrease. So the poten-
tial nasal physiological effects a drug or formulation excipient may have must
be considered as well. This should especially be evaluated for drugs intended for
chronic therapy so prolonged mucosal dysfunction is avoided.
Another relevant formulation issue for intranasal products is maintenance
of sterility. A very common preservative, benzalkonium chloride, has been added
to numerous nasal products [75]. Despite its popularity, reports in the literature
Copyright © 2003 Marcel Dekker, Inc.
734 Wermeling and Miller
suggest it may be associated with hypersensitivity reactions [76], mucosal swell-
ing [77,78], and decreased mucocilliary transport [75]. Since many nasal products
are multidose open systems, a preservative of some sort is necessary. An alterna-
tive for multidose packages may be delivery with a nasal spray bottle filled under
aseptic conditions and designed to prohibit contamination upon use [79]. Unit-
dose systems have an advantage over multidose because no preservative is re-
quired as long as the product undergoes sterile fill processing. The sterile fill
process may include filtration or the use of terminal sterilization procedures.
One must also keep in mind patient acceptability especially for agents in-
tended for chronic therapy [84]. Some formulations may cause transient discom-
fort upon instillation. This discomfort may be related to the drug, for example
midazolam [81], or to inactive excipients such as propylene glycol [82,83]. If a
product causes irritation or distress during application, patient compliance will
most likely be compromised.
The discussion above has focused on formulation issues related to agents
intended for systemic delivery. For local residence and effect in the nasal cavity
there are other considerations. Of course, many of the items previously presented
are important for either type of delivery. These include compatibility with the
nasal tissue, for example, and appropriate pH and osmolarity, careful choice of
a preservative if needed, and a reasonable concentration and volume for adminis-
tration. Additionally, drugs for local effect may be targeted to a specific area of
the nasal cavity rather than general distribution. An example of this is treatment
of nasal polyposis where the target area for drug disposition is the sinus mucosa
[84]. Aqueous formulations are desirable for local delivery. If the drug molecule
is highly water-insoluble, it may be necessary to use wetting agents such as poly-
sorbate 20 and sorbitan laurate to develop an aqueous suspension [84]. Using
this type of method, undissolved drug should be available at the local site of
action [84].
B. Dosage Form
Besides chemical and formulation issues, the dosage form is also important
for intranasal administration. To date, delivery of substances to the nose has
been via insufflation of powders, topical gels, sprays, drops, and nasal pledgets
[9,50,52]. One study has shown sprays to significantly increase bioavailability
even when compared to powder formulations [80]. Alternatively, powders appear
to offer many benefits such as increased chemical stability, decreased need for
preservative additions, administration of larger doses, and in some cases, greater
bioavailability and absorption [64]. The choice of dosage form and the delivery
system employed should be focused on feasibility and chemical stability, and
should compliment the expected therapeutic use. Table 1, based upon a review
Copyright © 2003 Marcel Dekker, Inc.
Intranasal Drug Delivery 735
Table 1 Important Considerations for Intranasal Dosage Forms
Dosage form Key points
Nasal drops Best for solutions
Metering of doses may be inaccurate or inconsistent
Solution spray Metered-dose actuator devices are available
Accurate dosing is feasible with spray devices
Suspension spray Metered-dose actuator devices are available
Orifice of the actuator may need modification for proper
delivery
Common dosage form for local effects
Powders May cause irritation and leave gritty sensation
Greater expense for drug development
Gels Metered-dose devices are available
Postnasal drip and anterior leakage are decreased
Used for systemic and local drug delivery
Emulsions/ointments Best for local action
Patient acceptability is low
Difficult to provide accurate dose
Source: Based on Ref. [68].
by Behl et al. [68], contains a brief list of various intranasal dosage forms along
with key considerations.
C. Delivery Device
The delivery device for a particular formulation should be based on several fac-
tors, including accuracy and dose reproducibility, cost, simple use for the patient,
physiochemical characteristics of the drug and chosen dosage form, and protec-
tion from microbial contamination [85]. Metered-dose systems are considered
the best for dose accuracy and reproducibility. Current delivery devices for liquid
and powder intranasal formulations are the following [85]:
Liquid formulations—instillation catheter, dropper, unit-dose containers,
squeeze bottle, pump spray, airless and preservative-free sprays, com-
pressed air nebulizers, and metered-dose inhalers
Powder formulations—insufflators, monodose inhalers, multidose inhalers,
and pressurized metered-dose inhalers
The delivery device and drug formulation should also be compatible with each
other to prevent leaching and absorption, which could pose a risk for toxicity
Copyright © 2003 Marcel Dekker, Inc.
736 Wermeling and Miller
and may affect dose accuracy, respectively. Additionally, a device should be
chosen on its ability to store the formulation appropriately without compromising
stability [85].
V. TECHNOLOGIES FOR MODIFIED INTRANASAL
DRUG DELIVERY
Modifications of intranasal delivery formulations primarily include the addition
of absorption enhancers to increase bioavailability and the use of bioadhesive
delivery systems to prolong drug contact time in the nasal passage for both in-
creased and sustained drug release [50]. These technologies are expanded upon
below. Absorption enhancers as well as bioadhesive systems have moved closer
to the forefront of pharmaceutical research when the nasal cavity was targeted
as a prime delivery route for proteins and peptides. These modifications attempt
to minimize the physiological barriers encountered in the nose. Barriers to drug
absorption are a limited residence time in the nasal cavity due to mucocilliary
clearance, penetration through and possible interaction with the mucus layer, pas-
sage of large molecules across the epithelial layer, and avoidance of potential
enzymatic degradation.
The broad category of absorption enhancers includes compounds that can
be divided into the following classes: surfactants, glycosides, bile salts, chelators,
fatty acid salts, fusidic acid derivatives, phospholipids, glycyrrhetinic acid deriva-
tives, cyclodextrins, glycols, cyclic peptide antibiotics, preservatives, carboxylic
acids, and O-acyl carnitine derivatives [50]. Selected enhancer agents will be
discussed in more detail below. These enhancers may improve the absorption of
substances using a variety of mechanisms such as increasing membrane fluidity,
paracellular or transcellular transport, and nasal blood flow, or decreasing mucus
layer viscosity, inhibiting proteolytic enzymes, loosening the tight junctions be-
tween epithelial cells, dissociating protein aggregation, and initiating membrane
pore formation [50]. One, or a combination, of these methods may be used to
enhance drug absorption.
Cyclodextrin and its derivatives appear to be the best-studied category of
enhancers. Cyclodextrins are cyclic oligosaccharides consisting of an inner hy-
drophobic core and an outer hydrophilic surface. This composition allows the
formation of inclusion complexes with lipophilic compounds [86]. The mecha-
nisms of action of cyclodextrins include solubilization and stabilization of pep-
tides and proteins, prevention of aggregation and proteolytic degradation, and
the opening of tight epithelial junctions [86,87]. Of the numerous cyclodextrin
derivatives, dimethyl-β-cyclodextrin has been found the most effective for im-
proving nasal bioavailability while minimizing toxic potential [80,88]. Cyclodex-
Copyright © 2003 Marcel Dekker, Inc.
Intranasal Drug Delivery 737
trins have been used successfully to increase the absorption of many substances
including, but not limited to, luteinizing hormone-releasing hormone [88], bio-
synthetic human growth hormone [89–93], ACTH(4–9) peptide analog [94], and
salmon calcitonin [95].
Enzyme inhibitors, specifically targeting aminopeptidase, have been effec-
tive in promoting the nasal absorption of a variety of peptides [50]; however,
findings of Machida et al. [96] suggest the effectiveness of recombinant human
granulocyte colony-stimulating factor was not enhanced with the addition of an
enzyme inhibitor. Also, aprotinin, camostat mesilate, and soybean trypsin inhibi-
tor were studied for their absorption enhancing effects on intranasal vasopressin
and its 1-deamino-8-d-arginine analog [97]. Only camostat mesilate, an inhibitor
of both aminopeptidase and trypsin, was found to significantly increase the bio-
logical effects. Thus, enzyme inhibitors seem to vary in their degree of effective-
ness.
Other absorption enhancers have also proven to be useful as described here
in brief detail. A medium-chain phospholipid enhanced intranasal insulin pharma-
cokinetics with minimal nasal irritation [98]. Laureth-9 also aids in the absorption
of insulin [99]. Lauroylcarnitine chloride was found beneficial in rats for increas-
ing salmon calcitonin absorption [100]. Glycyrrhetinic acid derivatives, espe-
cially carbenoxolone disodium salt, enhanced insulin uptake without nasal ir-
ritation or insulin degradation [101]. In sheep, both sodium deoxycholate and
polyoxyethylene 9-lauryl ether enhanced nasal absorption of interferon [102].
Finally, sodium taurodihydrofusidate (STDHF) was found useful in rabbits and
rats for increasing bioavailability of insulin [103]. The absorption-enhancing ef-
fect of STDHF has been shown to increase as its concentration increases and to
promote absorption independently of penetrant molecular weight [104]. Despite
its potential usefulness as an absorption enhancer, toxic effects on the nasal mu-
cosa may prevent its use therapeutically [105]. As with all components of nasal
formulations, preservation of physiological processes is desirable.
The other major modification for intranasal formulations is the use and
incorporation of bioadhesive technology. Recent reviews of this technology in
association with nasal delivery are available in the medical literature [85,106].
Bioadhesion refers to the adherence of a compound to biological material through
interfacial forces. The bioadhesive compound then remains attached for a pro-
longed period of time [106]. The term “mucoadhesion” is used when the com-
pound binds to the mucus covering of a biological tissue [85]. As described by
Illum [106], a series of steps occurs during this process. First, the bioadhesive
agent and membrane/mucus layer need to come into contact with each other.
Then, the chains of the adhesive agent penetrate into the membrane crevices or
interpenetration with mucosal chains occurs. Thus, increased residence time
within the nasal cavity allows for more complete, as well as prolonged, absorp-
Copyright © 2003 Marcel Dekker, Inc.
738 Wermeling and Miller
tion. These agents may also inhibit enzymatic activity and have demonstrated the
ability to cause alterations in the tight junctions, leading to increased substance
penetration [85].
The most common polymers used for intranasal delivery are carbopol, cel-
lulose compounds, sodium hyaluronate, polycarbophil, starch, dextran, and chito-
san [106]. These may be delivered to the nasal passage via several systems includ-
ing liquid solutions, gel, powder, and microspheres [106]. Several factors are
important for the effectiveness of a bioadhesive material. Both the chemical class
of a polymer and its polymer molecular mass are important to its bioadhesive
characteristics. Each class has a critical mass value where adhesiveness is at an
optimum level [85]. Also, penetration via the bioadhesive chain is extremely
important to its binding ability; therefore, extensive or dense cross-linking is not
desired [85]. Similar to having an optimum mass for bioadhesive properties, the
polymer concentration at the targeted interface may also affect binding ability
[85,106]. Other considerations for bioadhesive efficacy include the level of hydra-
tion and the pH of the environment. Too much hydration will cause excessive
swelling of the polymer and subsequently decrease adhesion. Also, changes in
the nasal pH may alter the bioadhesive binding effectiveness via alteration of
charge potential and interactions [85].
The most predominant polymer used for bioadhesion is chitosan. Chitosan
and its use as a delivery system has been recently reviewed by Janes et al. [107].
This polymer is obtained by deacetylation of chitin, which is naturally found
in crab and shrimp shells [108]. Chitosan is a high-molecular-weight, cationic,
hydrophilic polymer. It is biodegradable and has low toxicity [109–111]. In-
creased absorption obtained with chitosan is the result of both bioadhesion and
alteration of the tight junctions [112]. Chitosan microspheres and nanoparticles
have been used successfully in rabbits for insulin delivery [112,113]. In rats and
sheep, a solution formulation of chitosan was found to promote absorption of
insulin with little change on the nasal mucosa [109]. Chitosan microspheres have
also been studied for systemic delivery of pentazocine [110]. Intranasal pentazo-
cine bioavailability was improved with sustained blood level profiles. An addi-
tional use that has been investigated for chitosan is its ability to increase immuno-
genicity of mucosal vaccines [111]. The clearance of chitosan from the nasal
cavity in both a solution form and as microspheres was investigated in humans
[114]. The clearance half-lives of the chitosan solution and microspheres were
41 and 84 min, respectively. The half-life of clearance for the control was only
21 min. These studies substantiate chitosan’s usefulness as a bioadhesive agent.
In the same study discussed above [114], the clearance of starch micro-
spheres was also evaluated. The clearance half-life for the starch microspheres
was 68 min, which was approximately three times the value of the control group.
The starch microsphere system was studied for its impact on nasal absorption of
desmopressin in sheep [115]. Compared to the control nasal solution, the starch
Copyright © 2003 Marcel Dekker, Inc.
Intranasal Drug Delivery 739
system provided significantly shorter time to maximum concentration (Tmax),
higher maximum concentration (Cmax), increased area under the curve (AUC),
and improved bioavailability. The starch microsphere system is considered rela-
tively safe for drug delivery [116].
Carbopol formulations also appear to be effective for promoting nasal drug
exposure. Carbopol 971P, its analog Carbopol 974P, and polycarbophil were
evaluated in rabbits for intranasal pharmacokinetics of apomorphine [117]. For
all formulations, an increase in drug loading created a trend of increased Cmax
and AUC values as well as decreased Tmax. Carbopol 971P was further investi-
gated alone and in combination with apomorphine for its potential adverse effects
on ciliary beat frequency [118]. Carbopol 971P alone caused partially reversible
ciliary inhibition at 0.1 and 0.5% w/v formulations. Additionally, severe in-
flammation was observed with continued treatment. The investigators conclude
Carbopol 971P is not suitable for intranasal administration of apomorphine. An-
other report focuses on the use of Carbopol 934P for its rheological properties
[119]. It has low-viscosity-fluid characteristics, so it may be delivered via nasal
spray. Once in the nasal cavity, it transforms into a high-viscosity gel. With this
type of Carbopol 934P system, resulting pharmacokinetic parameters for propa-
nolol were favorable in beagle dogs [119]. Carbopol systems appear to be useful
bioadhesive agents; however, their nasal safety profiles should be thoroughly
investigated prior to therapeutic use.
Other bioadhesive materials have been studied as well. Carboxymethylcel-
lulose was determined to be a safe system for short-term intranasal use [120].
Also, it was found effective for providing sustained release of apomorphine in
rabbits [121]. A combination of polymethacrylic acid and polyethylene glycol
has been evaluated for its effects on intranasal budesonide delivery in rabbits
[122]. Concentrations in the blood remained constant for approximately 45 min
after administration. Another bioadhesive delivery system recently evaluated is
comprised of esterified hyaluronic acid (HYAFF) microspheres [123]. This sys-
tem was used in the formulation of influenza vaccines. Significantly increased
antibody responses (IgG and IgA) were obtained in mice, rabbits, and micropigs.
The intranasal immune response in pigs using the HYAFF system was greater
than that observed when given by intramuscular injection. Copolymers of poly
(acrylic acid) and pluronic surfactants have recently been developed [124]. This
combination utilizes both bioadhesion and thermogelling properties. Residence
time of the copolymer in rats was enhanced compared to either methodology
alone. Another system, gelatin microspheres, provided desirable absorption of
intranasal salmon calcitonin [125]. Additionally, gelatin microspheres demon-
strated usefulness for nasal administration of levodopa [126]. An initial fast re-
lease was observed followed by a slower release.
Additional systems for increasing residence time and absorption following
intranasal administration are emulsion formulations [127–129], liposome [130]
Copyright © 2003 Marcel Dekker, Inc.
740 Wermeling and Miller
and proliposome [131] formulations, and the use of nanoparticles [132,133]. Fi-
nally, a sucrose acetate isobutyrate delivery system has been utilized for intrana-
sal vaccination. The addition of this nonpolymeric high-viscosity agent resulted
in enhanced immune responses in adult horses [134].
These systems, as well as those previously addressed, demonstrate the wide
array of formulation opportunities for intranasal delivery. The main focus of these
and future systems should continue on its current path for modifications capable
of increasing absorption in addition to providing sustained release.
VI. FUTURE PROSPECTS FOR INTRANASAL
DRUG DELIVERY
Currently, the majority of intranasal products on the market are targeted toward
local relief or the prevention of nasal symptoms. The trend toward the develop-
ment of intranasal products for systemic absorption should rise considerably over
the next several years. The development of these products will be in a wide
variety of therapeutic areas from pain management to treatment for erectile dys-
function. However, the primary focus of intranasal administration, correlated with
increasing molecular scientific knowledge and methods, will be the development
of peptides, proteins, recombinant products, and vaccines. The nasal cavity pro-
vides an ideal administration site for these agents because of its accessibility,
avoidance of hepatic first-pass metabolism, and large vascular supply. Future
technologies in the intranasal arena will be concentrated on improved methods
for safe, efficient delivery systems primarily for molecular agents, but also for
numerous therapeutic categories.
REFERENCES
1. ND Fabricant. Nasal Medication. Baltimore, MD: Waverly Press, 1942, pp. 1–3.
2. J Law. Not to be sniffed at. Scrip Magazine May: 35–38, 2000.
3. JR Harkema. Comparative pathology of the nasal mucosa in laboratory animals
exposed to inhaled irritants. Environ Health Perspect 85:231–238, 1990.
4. N Mygind, A Änggård. Anatomy and physiology of the nose—pathophysiologic
alterations in allergic rhinitis. Clin Rev Allergy 2:173–188, 1984.
5. L Illum. Transport of drugs from the nasal cavity to the central nervous system.
Eur J Pharm Sci 11:1–18, 2000.
6. S Mathison, R Nagilla, UB Kompella. Nasal route for direct delivery of solutes to
the central nervous system: fact or fiction? J Drug Target 5:415–441, 1998.
7. NGM Schipper, JC Verhoef, FWHM Merkus. The nasal mucocilliary clearance:
relevance to nasal drug delivery. Pharm Res 8:807–814, 1991.
Copyright © 2003 Marcel Dekker, Inc.
Intranasal Drug Delivery 741
8. YW Chien, S Chang. Intranasal drug delivery for systemic medication. Crit Rev
Ther Drug Carr Syst 4:67–194, 1987.
9. YW Chien, KSE Su, S Chang. Nasal Systemic Drug Delivery. New York: Marcel
Dekker, 1989, pp. 1–38.
10. SS Hehar, JDT Mason, AB Stephen, N Washington, NS Jones, SJ Jackson, D Bush.
Twenty-four hour ambulatory nasal pH monitoring. Clin Otolaryngol 24:24–25,
1999.
11. GSMJE Duchateau, K Graamans, J Zuidema, FWHM Merkus. Correlation between
nasal ciliary beat frequency and mucus transport rate in volunteers. Laryngoscope
95:854–859, 1985.
12. NS Jones, S Quraishi, JDT Mason. The nasal delivery of systemic drugs. Int J Clin
Pract 51:308–311, 1997.
13. CJ Reed. Drug metabolism in the nasal cavity: relevance to toxicology. Drug Metab
Rev 25:173–205, 1993.
14. JR Thornton-Manning, AR Dahl. Metabolic capacity of nasal tissue interspecies
comparisons of xenobiotic-metabolizing enzymes. Mutat Res 380:43–59, 1997.
15. AR Dahl, JL Lewis. Respiratory tract uptake of inhalants and metabolism of xenobi-
otics. Annu Rev Pharmacol Toxicol 32:383–407, 1993.
16. J Jenner, GH Dodd. Xenobiotic metabolism in the nasal epithelia. Drug Metab Drug
Interact 6:123–148, 1988.
17. MA Sarkar. Drug metabolism in the nasal mucosa. Pharm Res 9:1–9, 1992.
18. VH Lee. Enzymatic barriers to peptide and protein absorption. Crit Rev Ther Drug
Carr Syst 5:69–97, 1988.
19. PG Gervasi, V Longo, F Naldi, G Panattoni, F Ursino. Xenobiotic-metabolizing
enzymes in the human respiratory nasal mucosa. Biochem Pharmacol 41:177–184,
1991.
20. JL Lewis, KJ Nikula, R Novak, AE Dahl. Comparative localization of carboxyles-
terase in F344 rat, beagle dog, and human nasal tissue. Anat Rec 239:55–64, 1994.
21. A Aceto, CD Ilio, S Angelucci, V Longo, PG Gervasi, G Federici. Glutathione
transferases in human nasal mucosa. Arch Toxicol 63:427–431, 1989.
22. NSR Krishna, TV Getchell, YC Awasthi, N Dhooper, ML Getchell. Age- and
gender-related trends in the expression of glutathione S-transferases in human nasal
mucosa. Ann Otol Rhinol Laryngol 104:812–822, 1995.
23. JL Lewis, CE Rhoades, PG Gervasi, WC Griffith, AR Dahl. The cyanide-metaboliz-
ing enzyme rhodanese in human nasal respiratory mucosa. Toxicol Appl Pharmacol
108:114–120, 1991.
24. B Winther. Effects on the nasal mucosa of upper respiratory viruses (common cold).
Dan Med Bull 41:193–204, 1994.
25. A Togias, RM Naclerio, D Proud, U Pipkorn, R Bascom, O Ilioupoulos, A Kagey-
Sobotka, PS Norman, LM Lichtenstein. Studies on the allergic and nonallergic nasal
inflammation. J Allergy Clin Immunol 81:782–790, 1988.
26. RM Naclerio. Pathophysiology of perennial allergic rhinitis. Allergy 52(suppl 36):
7–13, 1997.
27. AK Badhwar, HM Druce. Allergic rhinitis. Med Clin North Am 76:789–803, 1992.
28. D Wang, P Clement. Pathogenic mechanisms underlying the clinical symptoms of
allergic rhinitis. Am J Rhinol 14:325–333, 2000.
Copyright © 2003 Marcel Dekker, Inc.
742 Wermeling and Miller
29. H Klementsson. Eosinophils and the pathophysiology of allergic rhinitis. Clin Exp
Allergy 22:1058–1064, 1992.
30. R Naclerio, W Solomon. Rhinitis and inhalant allergens. JAMA 278:1842–1848,
1997.
31. G Philip, AG Togias. Nonallergic rhinitis. Eur Arch Otorhinolaryngol 252(suppl
1):S27–S32, 1995.
32. A Sanico, A Togias. Noninfectious, nonallergic rhinitis (NINAR): considerations
on possible mechanisms. Am J Rhinol 12:65–72, 1998.
33. M Englender, D Chamovitz, M Harell. Nasal transit time in normal subjects and
pathological conditions. Otolaryngol Head Neck Surg 103:909–912, 1990.
34. EJ Kaminski, OE Fanher, CJ Calandra. In vivo studies of the ciliostatic effects of
tobacco smoke. Arch Environ Health 16:188–193, 1968.
35. DR Edelstein. Aging of the normal nose in adults. Laryngoscope 106(suppl 81):
1–25, 1996.
36. A Molteni, RL Warpeha, L Brizio-Molteni, EM Fors. Estradiol receptor-binding
protein in head and neck neoplastic and normal tissue. Arch Surg 116:207–210,
1981.
37. N Hamano, N Terada, K Maesako, T Ikeda, S Fukuda, J Wakita, T Yamashita, A
Konno. Expression of histamine receptors in nasal epithelial cells and endothelial
cells—the effects of sex hormones. Int Arch Allergy Immunol 115:220–227,
1998.
38. N Hamano, N Terada, K Maesako, T Numata, A Konno. Effect of sex hormones
on eosinophilic inflammation in nasal mucosa. Allergy Asthma Proc 19:263–269,
1998.
39. B Paulsson, T Gredmark, P Burian, M Bende. Nasal mucosal congestion during
the menstrual cycle. J Laryngol Otol 111:337–339, 1997.
40. H Toppozada. The human nasal mucosa in the menopause. J Laryngol Otol 102:
314–318, 1988.
41. RL Mabry. Rhinitis of pregnancy. South Med J 79:965–971, 1986.
42. M Bende, U Hallgårde, C Sjögren, K Uvnäs-Moberg. Nasal congestion during preg-
nancy. Clin Otolaryngol 14:385–387, 1989.
43. UP Stübner, D Gruber, UE Berger, J Toth, B Marks, J Huber, F Horak. The influ-
ence of female sex hormones on nasal reactivity in seasonal allergic rhinitis. Allergy
54:865–871, 1999.
44. A Ginzel, P Illum. Nasal mucocilliary clearance in patients with septal deviation.
Rhinology 18:177–181, 1980.
45. CM Rossman, JB Forrest, RE Ruffin, MT Newhouse. Immotile cilia syndrome in
persons with and without Kartagener’s syndrome. Am Rev Respir Dis 121:1011–
1016, 1980.
46. DF Proctor. Transnasal Systemic Medications. Amsterdam: Elsevier, 1985, pp. 101.
47. K Khanvilkar, MD Donovan, DR Flanagan. Drug transfer through mucus. Adv
Drug Del Rev 28:173–193, 2001.
48. E Marttin, JC Verhoef, C Cullander, SG Romeijn, JF Nagelkerke, FWHM Merkus.
Confocal laser scanning microscopic visualization of the transport of dextrans after
nasal administration to rats: effects of absorption enhancers. Pharm Res 14:631–
637, 1997.
Copyright © 2003 Marcel Dekker, Inc.
Intranasal Drug Delivery 743
49. C McMartin, LEF Hutchinson, R Hyde, GE Peters. Analysis of structural require-
ments for the absorption of drugs and macromolecules from the nasal cavity. J
Pharm Sci 76:535–540, 1987.
50. V Agarwal, B Mishra. Recent trends in drug delivery systems: intranasal drug deliv-
ery. Ind J Exp Biol 37:6–16, 1999.
51. SP Newman, F Morén, SW Clarke. Deposition pattern of nasal sprays in man.
Rhinology 26:111–120, 1987.
52. L Illum, SS Davis. Intranasal insulin. Clin Pharmacokinet 12:30–41, 1992.
53. WAJJ Hermens, CWJ Belder, JMWM Merkus, PM Hooymans, J Verhoef, FWHM
Merkus. Intranasal administration of estradiol in combination with progesterone to
ovariectomized women: a pilot study. Eur J Obstet Gynecol Reprod Biol 43:65–
70, 1992.
54. A Adjei, D Sundberg, J Miller, A Chun. Bioavailability of leuprolide acetate follow-
ing nasal and inhalation delivery to rats and healthy humans. Pharm Res 9:244–
249, 1992.
55. A Hoffman, E Ziv. Pharmacokinetic considerations of new insulin formulations
and routes of administration. Clin Pharmacokinet 33:285–301, 1997.
56. E Cincinelli, F Savino, I Cagnazzo, P Scorcia, P Galantino. Progesterone adminis-
tration by nasal spray in menopausal women: comparison between two different
spray formulations. Gynecol Endocrinol 6:247–251, 1992.
57. N Eller, CJ Kollenz, G Hitzenberger. A comparative study of pharmacodynamics
and bioavailability of 2 different desmopressin nasal sprays. Int J Clin Pharmacol
Ther 36:139–145, 1998.
58. A Hussain, T Foster, S Hirai, T Kashihara, R Batenhorst, M Jones. Nasal absorption
of propanolol in humans. J Pharm Sci 69:1240, 1980.
59. CJ Johnson, P Olsson, M Bende, T Carlsson, PO Gunnarsson. Absolute bioavail-
ability of nicotine applied to different nasal regions. Eur J Clin Pharmacol 41:585–
588, 1991.
60. T Sakane, M Akizuki, Y Taki, S Yamashita, H Sezaki, T Nadai. Direct drug trans-
port from the rat nasal cavity to the cerebrospinal fluid: the relation to the molecular
weight of drugs. J Pharm Pharmacol 47:379–384, 1995.
61. Y Wang, R Aun, FLS Tse. Brain uptake of dihydroergotamine after intravenous
and nasal administration in the rat. Biopharm Drug Dispos 19:571–575, 1998.
62. T Sakane, S Yamashita, N Yata, H Sezaki. Transnasal delivery of 5-fluorouracil
to the brain in the rat. J Drug Target 7:233–240, 1999.
63. AN Fisher, K Brown, SS Davis, GD Parr, DA Smith. The effect of molecular size
on the nasal absorption of water-soluble compounds in the albino rat. J Pharm
Pharmacol 39:357–362, 1987.
64. A De Ascentüs, R Bettini, G Caponetti, PL Catellani, MT Peracchia, P Santi, P
Colombo. Delivery of nasal powders of β-cyclodextrin by insufflation. Pharm Res
13:734–738, 1996.
65. D Corbo, J Liu, YW Chien. Drug absorption through mucosal membranes: effect
of mucosal route and penetrant hydrophilicity. Pharm Res 6:848–852, 1989.
66. T Ohwaki, H Ando, S Watanabe, Y Miyake. Effects of dose, pH, and osmolarity
on the nasal absorption of secretin in rats. J Pharm Sci 74:550–552, 1985.
67. T Ohwaki, H Ando, F Kakimoto, K Uesugi, S Watanabe, Y Miyake, M Kayano.
Copyright © 2003 Marcel Dekker, Inc.
744 Wermeling and Miller
Effects of dose, pH, and osmolarity on nasal absorption of secretin in rats. II. Histo-
logical aspects of the nasal mucosa in relation to the absorption variation due to
the effects of pH and osmolarity. J Pharm Sci 76:695–698, 1987.
68. CR Behl, HK Pimplaskar, AP Sileno, J deMeireles, VD Romeo. Effects of physio-
chemical properties and other factors on systemic nasal drug delivery. Adv Drug
Del Rev 29:89–116, 1998.
69. N Shimoda, Y Maitani, Y Machida, T Nagai. Effects of dose, pH and osmolarity
on intranasal absorption of recombinant human erythropoietin in rats. Biol Pharm
Bull 18:734–739, 1995.
70. P Valensi, P Zirinis, P Nicolas, G Perret, D Sandre-Banon, JR Attali. Effect of
insulin concentration on bioavailability during nasal spray administration. Path Biol
44:235–240, 1996.
71. AA Hussain, R Bawarshi-Nassar, CH Huang. Physiochemical consideration in in-
tranasal drug administrations. In: YW Chein, ed. Transnasal Systemic Medications.
Amsterdam: Elsevier, 1985, pp. 121–137.
72. AW Proetz. Applied Physiology of the Nose. St. Louis: Annals Publishing Com-
pany, 1953.
73. AS Harris, M Ohlin, S Lethagen, IM Nilsson. Effects of concentration and volume
on nasal bioavailability and biological response to desmopressin. J Pharm Sci 77:
337–339, 1988.
74. HJM van de Donk, FWHM Merkus. Decreases in ciliary beat frequency due to
intranasal administration of propanolol. J Pharm Sci 71:595–596, 1982.
75. IL Bernstein. Is the use of benzalkonium chloride as a preservative for nasal formu-
lations a safety concern? A cautionary note based on compromised mucocilliary
transport. J Allergy Clin Immunol 105:39–44, 2000.
76. G Hillardal. Adverse reaction to locally applied preservatives in nose drops. ORL
J Otorhinolaryngol Relat Spec 47:278–279, 1985.
77. H Hallén, P Graf. Benzalkonium chloride in nasal decongestive sprays has a long-
lasting adverse effect on the nasal mucosal of healthy volunteers. Clin Exp Allergy
25:401–405, 1995.
78. P Graf, H Hallén. Effect on the nasal mucosa of long-term treatment with oxymeta-
zoline, benzalkonium chloride, and placebo nasal sprays. Laryngoscope 106:605–
609, 1996.
79. P Graf, H Hallén, J-E Juto. Benzalkonium chloride in a decongestant nasal spray
aggravates rhinitis medicamentosa in healthy volunteers. Clin Exp Allergy 25:395–
400, 1995.
80. M Quadir, H Zia, TE Needham. Development and evaluation of nasal formulations
of ketorolac. Drug Deliv 7:223–229, 2000.
81. N Griffith, S Howell, DG Mason. Intranasal midazolam for premedication of chil-
dren undergoing day-case anaesthesia: comparison of two delivery systems with
assessment of intra-observer variability. Br J Anaesth 81:865–869, 1998.
82. SF Conley. Comparative trial of acceptability of beclomethasone dipropionate and
a new formulation of flunisolide. Ann Allergy 72:829–832, 1994.
83. EO Meltzer, HA Orgel, RK Bush, JR Haltom, J Metzger, BA Moss, DQ Mitchell,
ZK Ballas, JM Seltzer, GG Shapiro, JH Van Bavel. Evaluation of symptom relief,
Copyright © 2003 Marcel Dekker, Inc.
Intranasal Drug Delivery 745
nasal airflow, nasal cytology, and acceptability of two formulations of flunisolide
nasal spray in patients with perennial allergic rhinitis. Ann Allergy 64:536–540,
1990.
84. S Denyer. Pharmaceutical properties of fluticasone propionate nasal drops: a new
formulation. Allergy 54:17–20, 1999.
85. MI Ugwoke, N Verbeke, R Kinget. The biopharmaceutical aspects of nasal mu-
coadhesive drug delivery. J Pharm Pharmacol 53:3–22, 2001.
86. E Marttin, JC Verhoef, FWHM Merkus. Efficacy, safety and mechanism of cyclo-
dextrins as absorption enhancers in nasal delivery of peptide and protein drugs. J
Drug Target 6:17–36, 1998.
87. E Marttin, JC Verhoef, F Spies, J van der Meulen, JF Nagelkerke, HK Koerten,
FWHM Merkus. The effect of methylated β-cyclodextrins on the tight junctions
of the rat nasal respiratory epithelium: electron microscopic and confocal laser
scanning microscopic visualization studies. J Control Rel 57:205–213, 1999.
88. K Matsubara, K Abe, T Irie, K Uekema. Improvement of nasal bioavailability of
luteinizing hormone-releasing hormone agonist, burserelin, by cyclodextrin deriva-
tives in rats. J Pharm Sci 84:1295–1300, 1995.
89. C Agerholm, L Bastholm, PB Johansen, MH Nielsen, F Elling. Epithelial trans-
port and bioavailability of intranasally administered human growth hormone formu-
lated with the absorption enhancers didecanoyl-l-α-phosphatidylcholine and α-
cyclodextrin in rabbits. J Pharm Sci 83:1706–1711, 1994.
90. FWHM Merkus, JC Verhoef, SG Romeijn, NGM Schipper. Absorption enhancing
effect of cyclodextrins on intranasally administered insulin in rats. Pharm Res 8:
588–592, 1991.
91. Y Watanabe, Y Matsumoto, K Kawamoto, S Yazawa, M Matsumoto. Enhancing
effect of cyclodextrins on nasal absorption of insulin and its duration in rabbits.
Chem Pharm Bull 40:3100–3104, 1992.
92. Z Shao, R Krishnamoorthy, A Mitra. Cyclodextrins as nasal absorption promoters
of insulin: mechanistic evaluations. Pharm Res 9:1157–1163, 1992.
93. NGM Schipper, SG Romeijn, JC Verhoef, FWHM Merkus. Nasal insulin delivery
with dimethyl-β-cyclodextrin as an absorption enhancer in rabbits: powder more
effective than liquid formulations. Pharm Res 10:682–686, 1993.
94. NGM Schipper, JC Verhoef, LM De Lannoy, SG Romeijn, JH Brakkee, VM Wie-
gant, WH Gispen, FWHM Merkus. Nasal administration of an ACTH(4-9) peptide
analogue with dimethyl-β-cyclodextrin as an absorption enhancer: pharmacokinet-
ics and dynamics. Br J Pharmacol 110:1334–1340, 1993.
95. NSM Schipper, JC Verhoef, SG Romeijn, FWHM Merkus. Methylated β-cyclodex-
tins are able to improve the nasal absorption of salmon calcitonin. Calcif Tissue
Int 56:280–282, 1995.
96. M Machida, K Sano, M Arakawa, M Hayashi, S Awazu. Effects of surfactants and
protease inhibitors on nasal absorption of recombinant human granulocyte colony-
stimulating factor (rhG-CSF) in rats. Biol Pharm Bull 17:1375–1378, 1994.
97. K Morimoto, H Yamaguchi, Y Iwakura, M Miyazaki, E Nakatani, T Iwamoto, Y
Ohashi, Y Nakai. Effects of proteolytic enzyme inhibitors on the nasal absorption
of vasopressin and an analogue. Pharm Res 8:1175–1179, 1991.
Copyright © 2003 Marcel Dekker, Inc.
746 Wermeling and Miller
98. K Drejer, A Vaag, K Bech, P Hansen, AR Sørensen, N Mygind. Intranasal adminis-
tration of insulin with phospholipid as absorption enhancer: pharmacokinetics in
normal subjects. Diabet Med 9:335–340, 1992.
99. BJ Aungst, NJ Rogers. Site dependence of absorption-promoting actions of laureth-
9, Na salicylate, Na2EDTA, and aprotinin on rectal, nasal, and buccal insulin deliv-
ery. Pharm Res 5:305–308, 1988.
100. S Kagatani, T Shinoda, M Fukui, T Ohmura, S Hasumi, T Sonobe. Enhancement
of nasal salmon calcitonin absorption by lauroylcarnitine chloride in rats. Pharm
Res 13:739–743, 1996.
101. M Mishima, S Okada, Y Wakita, M Nakano. Promotion of nasal absorption of
insulin by glycyrrhetinic acid derivatives. I. J Pharmacobio-Dyn 12:31–36, 1989.
102. C Baglioni, RJ Phipps. Nasal absorption of interferon: enhancement by surfactant
agents. J Interferon Res 10:497–504, 1990.
103. MJM Duerloo, WAJJ Hermens, SG Romeyn, JC Verhoef, FWHM Merkus. Absorp-
tion enhancement of intranasally administered insulin by sodium taurodihydrofusi-
date (STDHF) in rabbits and rats. Pharm Res 6:853–856, 1989.
104. K Hosoya, H Kubo, T Akutsu, H Natsume, K Sugibayashi, Y Morimoto. Effect
of sodium taurodihydrofusidate on nasal drug delivery: differences in its concentra-
tion and penetrant molecular weight. Arch Pharm Res 17:57–59, 1994.
105. A Donnelly, IW Kellaway, G Taylor, M Gibson. Absorption enhancers as tools to
determine the route of nasal absorption of peptides. J Drug Target 5:121–127,
1997.
106. L Illum. Bioadhesive formulations for nasal peptide delivery. In: E Mathiowitz,
DE Chickering III, C Lehr, eds. Bioadhesive Drug Delivery Systems. New York:
Marcel Dekker, 1999, pp. 507–541.
107. KA Janes, P Calvo, MJ Alonso. Polysaccharide colloidal particles as delivery sys-
tems for macromolecules. Adv Drug Del Rev 47:83–97, 2001.
108. P Tengamnuay, A Sahamethapat, A Sailasuta, AK Mitra. Chitosans as nasal absorp-
tion enhancers of peptides: comparison between free amine chitosans and soluble
salts. Int J Pharm 197:53–67, 2000.
109. EA McNeela, D O’Connor, I Jabbal-Gill, L Illum, SS Davis, M Pizza, S Peppoloni,
R Rappuoli, KHG Mills. A mucosal vaccine against diphtheria: formulation of cross
reacting material (CRM197) of diphtheria toxin with chitosan enhances local and
systemic antibody and Th2 responses following nasal delivery. Vaccine 19:1188–
1198, 2001.
110. C Sankar, M Rani, AK Srivastava, B Mishra. Chitosan based pentazocine micro-
spheres for intranasal systemic delivery: development and biopharmaceutical evalu-
ation. Pharmazie 56:223–226, 2001.
111. L Illum, NF Farraj, SS Davis. Chitosan as a novel nasal delivery system for peptide
drugs. Pharm Res 11:1186–1189, 1994.
112. J Woodley. Bioadhesion new possibilities for drug administration? Clin Pharma-
cokinet 40:77–84, 2001.
113. R Fernández-Urrusono, P Calvo, C Remuñán-López, JL Vila-Jato, MJ Alonso. En-
hancement of nasal absorption of insulin using chitosan nanoparticles. Pharm Res
16:1576–1581, 1999.
Copyright © 2003 Marcel Dekker, Inc.
Intranasal Drug Delivery 747
114. RJ Soane, M Frier, AC Perkins, NS Jones, SS Davis, L Illum. Evaluation of the
clearance characteristics of bioadhesive systems in humans. Int J Pharm 178:55–
65, 1999.
115. H Critchley, SS Davis, NF Farraj, L Illum. Nasal absorption of desmopressin in
rats and sheep. Effect of a bioadhesive microsphere delivery system. J Pharm Phar-
macol 46:651–656, 1994.
116. P Edman, E Bjork, L Ryden. Microspheres as a nasal delivery system for peptide
drugs. J Control Rel 21:165–172, 1992.
117. MI Ugwoke, E Sam, G Van Den Mooter, N Verbeke, R Kinget. Nasal mucoadhe-
sive delivery systems of the anti-parkinsonian drug, apomorphine: influence of
drug-loading on in vitro and in vivo release in rabbits. Int J Pharm 181:125–138,
1999.
118. MI Ugwoke, RU Agu, M Jorissen, P Augustijns, R Sciot, N Verbeke, R Kinget.
Nasal toxicological investigations of carbopol 971P formulation of apomorphine:
effects on ciliary beat frequency of human nasal primary cell culture and in vivo
on rabbit nasal mucosa. Eur J Pharm Sci 9:387–396, 2000.
119. JS Chu, R Chandrasekharan, GL Amidon, ND Weiner, AH Goldberg. Viscometric
study of polyacrylic acid systems as mucoadhesive sustained-release gels. Pharm
Res 8:1408–1412, 1991.
120. MI Ugwoke, RU Agu, M Jorissen, P Augustijns, R Sciot, N Verbeke, R Kinget.
Toxicological investigations of the effects carboxymethylcellulose on ciliary beat
frequency of human nasal epithelial cells in primary suspension culture and in vivo
of rabbit nasal mucosa. Int J Pharm 205:43–51, 2000.
121. MI Ugwoke, G Kaufmann, N Verbeke, R Kinget. Intranasal bioavailability of apo-
morphine from carboxymethylcellulose-based drug delivery systems. Int J Pharm
202:125–131, 2000.
122. K Nakamura, Y Maitani, AM Lowman, K Takayama, NA Peppas, T Nagai. Uptake
and release of budesonide from mucoadhesive, pH-sensitive copolymers and their
application to nasal delivery. J Control Rel 61:329–335, 1999.
123. M Singh, M Briones, DT O’Hagan. A novel bioadhesive intranasal delivery system
for inactivated influenza vaccines. J Control Rel 70:267–276, 2001.
124. LE Bromberg. Enhanced nasal retention of hydrophobically modified polyelectro-
lytes. J Pharm Pharmacol 53:109–114, 2001.
125. K Morimoto, H Katsumata, T Yabuta, K Iwanaga, M Kakemi, Y Tabata, Y Ikada.
Evaluation of gelatin microspheres for nasal and intramuscular administrations of
salmon calcitonin. Eur J Pharm Sci 13:179–185, 2001.
126. B Brime, MP Ballesteros, P Frutos. Preparation and in vitro characterization of
gelatin microspheres containing levodopa for nasal administration. J Microencapsul
17:777–784, 2000.
127. K Aikawa, K Matsumoto, H Uda, S Tanaka, H Shimamura, Y Aramaki, S Tsuchiya.
Prolonged release of drug from O/W emulsion and residence in rat nasal cavity.
Pharm Dev Technol 3:461–469, 1998.
128. TW Kim, H Chung, IC Kwon, HC Sung, SY Jeong. In vivo gene transfer to the
mouse nasal cavity mucosa using a stable cationic lipid emulsion. Mol Cells 10:
142–147, 2000.
Copyright © 2003 Marcel Dekker, Inc.
748 Wermeling and Miller
129. TT Kararli, TE Needham, G Schoenhard, DA Baron, RE Schmidt, B Katz, B Be-
lonio. Enhancement of nasal delivery of a renin inhibitor in the rat using emulsion
formulations. Pharm Res 9:1024–1028, 1992.
130. SL Law, KJ Huang, HY Chou. Preparation of desmopressin-containing liposomes
for intranasal delivery. J Control Rel 70:375–382, 2001.
131. BH Jung, BC Chung, S Chung, M Lee, C Shim. Prolonged delivery of nicotine in
rats via nasal administration of proliposomes. J Control Rel 66:73–79, 2000.
132. D Betbeder, S Spérandio, J Latapie, J de Nadaı́, A Etienne, J Zajac, B Frances.
Biovector nanoparticles improve antinociceptive efficacy of nasal morphine. Pharm
Res 17:743–748, 2000.
133. M Tobı́o, R Gref, A Sánchez, R Langer, MJ Alonso. Stealth PLA-PEG nanopar-
ticles as protein carriers for nasal administration. Pharm Res 15:270–275, 1998.
134. JE Nally, S Artiushin, AS Sheoran, PJ Burns, B Simon, RM Gilley, J Gibson, S
Sullivan, JF Timoney. Induction of mucosal and systemic antibody specific for
SeMF3 of Streptococcus equi by intranasal vaccination using a sucrose acetate iso-
butyrate based delivery system. Vaccine 19:492–497, 2001.
Copyright © 2003 Marcel Dekker, Inc.
You might also like
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeFrom EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeRating: 4 out of 5 stars4/5 (5794)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreFrom EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreRating: 4 out of 5 stars4/5 (1090)
- Never Split the Difference: Negotiating As If Your Life Depended On ItFrom EverandNever Split the Difference: Negotiating As If Your Life Depended On ItRating: 4.5 out of 5 stars4.5/5 (838)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceFrom EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceRating: 4 out of 5 stars4/5 (894)
- Grit: The Power of Passion and PerseveranceFrom EverandGrit: The Power of Passion and PerseveranceRating: 4 out of 5 stars4/5 (587)
- Shoe Dog: A Memoir by the Creator of NikeFrom EverandShoe Dog: A Memoir by the Creator of NikeRating: 4.5 out of 5 stars4.5/5 (537)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureFrom EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureRating: 4.5 out of 5 stars4.5/5 (474)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersFrom EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersRating: 4.5 out of 5 stars4.5/5 (344)
- Her Body and Other Parties: StoriesFrom EverandHer Body and Other Parties: StoriesRating: 4 out of 5 stars4/5 (821)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)From EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Rating: 4.5 out of 5 stars4.5/5 (119)
- The Emperor of All Maladies: A Biography of CancerFrom EverandThe Emperor of All Maladies: A Biography of CancerRating: 4.5 out of 5 stars4.5/5 (271)
- The Little Book of Hygge: Danish Secrets to Happy LivingFrom EverandThe Little Book of Hygge: Danish Secrets to Happy LivingRating: 3.5 out of 5 stars3.5/5 (399)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyFrom EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyRating: 3.5 out of 5 stars3.5/5 (2219)
- The Yellow House: A Memoir (2019 National Book Award Winner)From EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Rating: 4 out of 5 stars4/5 (98)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaFrom EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaRating: 4.5 out of 5 stars4.5/5 (265)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryFrom EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryRating: 3.5 out of 5 stars3.5/5 (231)
- Team of Rivals: The Political Genius of Abraham LincolnFrom EverandTeam of Rivals: The Political Genius of Abraham LincolnRating: 4.5 out of 5 stars4.5/5 (234)
- On Fire: The (Burning) Case for a Green New DealFrom EverandOn Fire: The (Burning) Case for a Green New DealRating: 4 out of 5 stars4/5 (73)
- The Unwinding: An Inner History of the New AmericaFrom EverandThe Unwinding: An Inner History of the New AmericaRating: 4 out of 5 stars4/5 (45)
- Non-symbiotic Nitrogen FixersDocument21 pagesNon-symbiotic Nitrogen Fixersrajiv pathakNo ratings yet
- Regular Evaluation Test I Maths+Sc IXDocument7 pagesRegular Evaluation Test I Maths+Sc IXB.L. Indo Anglian Public School, Aurngabad, BiharNo ratings yet
- Determination of Lethal Dose Ld50of Venom of Four Different Poisonous Snakes Found in PakistanDocument4 pagesDetermination of Lethal Dose Ld50of Venom of Four Different Poisonous Snakes Found in PakistanSutirtho MukherjiNo ratings yet
- Noscapine - British PharmacopoeiaDocument3 pagesNoscapine - British PharmacopoeiaSocial Service (V)No ratings yet
- 8 Cell - The Unit of Life-NotesDocument6 pages8 Cell - The Unit of Life-NotesBhavanya RavichandrenNo ratings yet
- Biofuels Bioprod Bioref - 2022 - Souza - Bioenergy Research in Brazil A Bibliometric Evaluation of The BIOEN ResearchDocument16 pagesBiofuels Bioprod Bioref - 2022 - Souza - Bioenergy Research in Brazil A Bibliometric Evaluation of The BIOEN Researchdeborah151No ratings yet
- Ssac 2104Document100 pagesSsac 2104Amrutha amrNo ratings yet
- Natamycin Story - What You Need to KnowDocument13 pagesNatamycin Story - What You Need to KnowCharles MardiniNo ratings yet
- Jurnal Perkecambahan Biji PDFDocument14 pagesJurnal Perkecambahan Biji PDFKinad Danik50% (2)
- Chapter 5Document14 pagesChapter 5Caitlin G.No ratings yet
- 1 s2.0 S0141022999001556 MainDocument21 pages1 s2.0 S0141022999001556 MainRenata ScoralickNo ratings yet
- E-Techno: Cbse Class-Ix - E6 - E-Techno JEE TEST DATE: 17-11-2020Document16 pagesE-Techno: Cbse Class-Ix - E6 - E-Techno JEE TEST DATE: 17-11-2020Himanshu ThakurNo ratings yet
- MDU Open Elective 3rd Sem Date Sheet May 2019Document1 pageMDU Open Elective 3rd Sem Date Sheet May 2019Ratan DeshNo ratings yet
- Rife S Fundamental Resonance Enhancement A 100 Effective Cure For CancersDocument28 pagesRife S Fundamental Resonance Enhancement A 100 Effective Cure For CancersDimitar LevskiNo ratings yet
- 02 Anatomy and Histology PLE 2019 RatioDocument69 pages02 Anatomy and Histology PLE 2019 RatioPatricia VillegasNo ratings yet
- Candida Tropicalis - ACMGDocument12 pagesCandida Tropicalis - ACMGSergio Iván López LallanaNo ratings yet
- Characterization of Polydimethylsiloxane (PDMS) PropertiesDocument13 pagesCharacterization of Polydimethylsiloxane (PDMS) PropertiesEsteban ArayaNo ratings yet
- Morphology of Flowering PlantsDocument13 pagesMorphology of Flowering Plantschiragbhaskar16No ratings yet
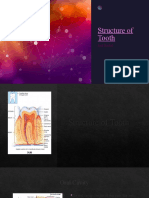
- Structure of Tooth m121Document13 pagesStructure of Tooth m121amirhossein vaeziNo ratings yet
- Mejasco, Bianca Isabelle A. - Block H - SGD #1Document2 pagesMejasco, Bianca Isabelle A. - Block H - SGD #1Bianca MejascoNo ratings yet
- Behaviour of Great Apes Studied by Three Female ScientistsDocument12 pagesBehaviour of Great Apes Studied by Three Female ScientistsSani AhmadNo ratings yet
- Introduction To Bioinformatics: Database Search (FASTA)Document35 pagesIntroduction To Bioinformatics: Database Search (FASTA)mahedi hasanNo ratings yet
- Agilent ASMS 2019 ThP762 PosterDocument4 pagesAgilent ASMS 2019 ThP762 PostersppNo ratings yet
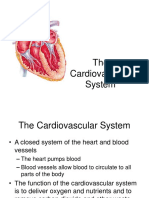
- Cardiovascular SystemDocument40 pagesCardiovascular SystemMudasir Hussain TuriNo ratings yet
- Lesson Plan No 5Document6 pagesLesson Plan No 5hafeez ahmedNo ratings yet
- Advanced Level Biology 2015 Marking SchemeDocument29 pagesAdvanced Level Biology 2015 Marking SchemeAngiee FNo ratings yet
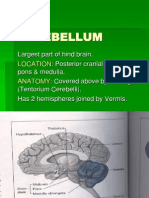
- Physiology of Cerebellum Lec Foe 2nd Year by DR Sadia Uploaded by ZaighamDocument61 pagesPhysiology of Cerebellum Lec Foe 2nd Year by DR Sadia Uploaded by ZaighamZaigham HammadNo ratings yet
- Pengantar Mikrobiologi LingkunganDocument28 pagesPengantar Mikrobiologi LingkunganAhmad SyahrulNo ratings yet
- 421 Reproduction Developmental Toxicity Screening TestDocument10 pages421 Reproduction Developmental Toxicity Screening TestAshishNo ratings yet
- 1oksidative Stress TestDocument34 pages1oksidative Stress TestDian WijayantiNo ratings yet