Professional Documents
Culture Documents
Acls Studypack
Uploaded by
bethchaygwapaOriginal Description:
Original Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Acls Studypack
Uploaded by
bethchaygwapaCopyright:
Available Formats
2005 ACLS OVERVIEW & STUDY GUIDE
Vanderbilt Resuscitation Program
ACLS is a course dedicated to sharing a core of advanced information regarding respiratory and cardiac
emergencies. It is taught according to the most current guidelines approved by the American Heart Association as
a uniform approach to the treatment of these emergencies.
Because of the volume of materials to be covered in this course, the following skills are STRONGLY recommended
as prerequisites to attending ACLS:
(a) BLS - it is highly recommended that you have attended a BLS course within the last two years. You will be
expected to perform BLS during the case studies and you must be able to perform BLS flawlessly during
the Mega VF and BLS/AED evaluation stations.
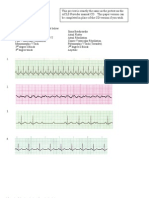
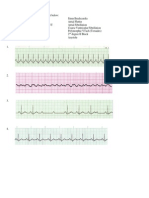
(b) Arrhythmia recognition - you MUST be able to easily recognize arrhythmias to successfully complete
ACLS. If you do not work with arrhythmias on a regular basis, it is STRONGLY suggested that you
consider attending Essentials of Resuscitation and a Basic Arrhythmia Course prior to attending ACLS.
(c) Pharmacology - you MUST be comfortable with the drugs used in ACLS. If you do not work with these
drugs on a regular basis, it is STRONGLY suggested that you spend time reviewing a pharmacology text.
SUCCESSFUL ACLS COURSE COMPLETION
One ACLS course requirement is completion of the enclosed multiple choice and ECG exams.
Bring your completed exams with you—they are your “entrance tickets” into class.
The other course completion criteria are:
1. Active participation in ALL stations, including demonstrated knowledge of ACLS principles. Inability
to demonstrate mastery of these "ACLS essentials" would require that you be remediated and re-evaluated:
a. Assure that the patient’s ABCs are intact, either spontaneously or with your assistance.
i. Airway: open it, keep it open
ii. Breathing: make sure it is adequate at ALL times---give oxygen as a first-line drug
iii. Circulation: make sure it is adequate at ALL times---begin and continue CPR as needed
b. Assess and reassess the patient's condition frequently and intervene as indicated
c. Perform early, safe, and effective defibrillation for VF or pulseless VT.
d. Know and use appropriate pharmacological agents---which drug, which route, which dose
2. Mega-VF evaluation. You will manage the first 10 minutes of resuscitation for a patient in ventricular
fibrillation or pulseless ventricular tachycardia. You will be functioning as the team leader, and must direct all care
provided for the "patient".
3. Automated External Defibrillation. You will properly attach and safely use an automated external
defibrillator. This may be a separate station or could be incorporated into your Mega VF evaluation, depending on
your experience with an AED.
4. ACLS Post-test. A post-test, very similar in content to the pre-test, will be given at the end of class. You will
be expected to complete this exam with a score of 84% or greater.
TEXTS
The following texts are required for all ACLS Provider Courses and recommended but optional for all ACLS
Renewal Courses:
ACLS Provider Manual
Handbook of Emergency Cardiovascular Care (ECC Handbook)
Created by Kim Chunn 9/01
Revised 12/04
1
THE 10 ACLS CASES
Respiratory Arrest w/ Pulse VF/Pulseless VT
Bradycardia Stable Tachycardia
Acute Coronary Syndromes Unstable Tachycardia
Asystole Pulseless Electrical Activity (PEA)
Acute Ischemic Stroke Automated External Defibrillation
THE ACLS SKILLS
1. Airway/Breathing
a. Provide oxygen
i. Nasal cannula 2-6 liters/minute
ii. 100% non-rebreather mask
b. Open the airway/keep it open
i. Head-tilt/chin-lift
ii. Jaw thrust
iii. Oral airway
iv. Nasal airway
v. Suction
vi. Endotracheal Intubation
vii. Alternative Devices/Techniques
1. LMA
2. Combitube
3. Needle Cricothyrotomy
c. Ventilate
i. Mouth-to-Mask
ii. Bag-Mask
1. with oral airway
2. 2-person technique
2. Circulation
3. Dysrhythmia Recognition
a. Non-perfusing (arrest) rhythms
i. Shockable
1. VF
2. Pulseless VT
ii. Non-shockable
1. PEA
2. Asystole
b. Perfusing (peri-arrest) rhythms
i. Symptomatic Bradycardia
ii. Tachycardia, Stable and Unstable
4. Electrical Therapy
a. Defibrillation
b. Synchronized cardioversion
c. Transcutaneous pacing
5. Peripheral IV access
6. Pharmacology
Created by Kim Chunn 9/01
Revised 12/04
2
PHARMACOLOGY
The following drugs are part of the ACLS algorithms and are the ones you are expected to know readily
(drug, dose, route(s), indications, contraindications):
** DRUGS ACCEPTABLE VIA ETT ROUTE: Drugs given via endotracheal tube should be given at 2 to 2.5
times the IV dose and diluted in 10 ml. of saline.
IV PUSH DRUGS: INFUSIONS:
Epinephrine** Lidocaine
1 mg q. 3-5 min. 2-4 mg/min. Mix 1-2 gm/250 cc. of D5W
Vasopressin Procainamide
40 units, single dose, one time only (VF only) 1-4 mg/min. Mix 1-2 gm/250 cc of D5W
Atropine** Dopamine
0.5-1 mg q. 3-5 min, up to a total of 0.04 mg/kg 5-10 mcg/kg/min. Mix 400 mg/250 cc of D5W
Amiodarone Epinephrine
(VF/VT) 300 mg, consider repeating 150 mg in 3- 2-10 mcg/min. Mix 1-2 mg/250 cc of D5W
5 min.
Amiodarone
Lidocaine** Rapid infusion (non-VF): 150 mg over 10 min, may
1-1.5 mg/kg; repeat at 0.5-1.5 mg/kg q. 5-10 min. repeat every 10 mins prn.
up to 3 mg/kg max Maintenance infusion: 1 mg/min for 6 hrs
decreasing to 0.5 mg/min for 18 hrs.
Procainamide Max cumulative dose 2.2 gm IV/24 hrs.
20-50 mg/min, up to a total of 17 mg/kg
Magnesium Sulfate
1-2 gm in 10 ml of D5W over 1-2 min.
Sodium Bicarbonate
1 mEq/kg; repeat at 0.5 mEq/kg q. 10 mins.
Adenosine
6 mg over 1-3 sec. followed by saline bolus to
flush; repeat at 12 mg. after 1-2 min. twice (30
mg total)
Further information on ACLS Pharmacology can be found in the ECC Handbook, pgs. 54-72.
Created by Kim Chunn 9/01
Revised 12/04
3
UNIVERSAL PULSELESS RHYTHM MANAGEMENT
V-FIB ASYSTOLE PEA
Shock
Shock
Shock
C CPR
O Oxygen
T Tubes: ET, IV
E Epinephrine 1 mg Q 3-5 minutes
Acceptable to use Vasopressin
40 U IV, single dose, 1 time only as
alternative to epinephrine and may
return to epinephrine 1 mg Q 3-5
mins if no response after 10-20
mins.
Shock Atropine Etiology
Drug 1 mg q3min x 3 Atropine (if HR<60)
Shock
Drug
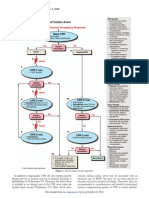
The central concept is that the COTE mnemonic is the core treatment of all non-perfusing rhythms with the
additions listed in line with each particular rhythm. Remember:
1) V-Fib rhymes with Defib and there should be a direct neurologic synapse between them. Next go to COTE
then think Defib - Drug - Defib - Drug - etc.
2) Asystole goes straight to COTE then out to Atropine, which also begins with an A.
3) PEA goes straight to COTE then out to Etiology and then to Atropine if the rate is less than 60.
Created by Kim Chunn 9/01
Revised 12/04
4
AUTOMATED EXTERNAL DEFIBRILLATION
(pending the arrival of EMS)
Unresponsive—911---AED:
• Check if unresponsive
• Call 911
• Get AED
• Identify and respond to special situations
Unresponsive
Start ABCDs:
• Airway: open airway, hold it open
• Breathing: look, listen and feel for breathing
Breathing Not Breathing
• Provide 2 slow breaths
• Breathing adequate? Place in recovery position • Circulation: check for carotid pulse
• Breathing inadequate? Start rescue breathing:
1 breath every 5 seconds
• Monitor signs of circulation every 30-60 seconds: pulse, color,
movement, return or remaining presence of normal breathing
No Circulation
pattern, coughing
Circulation
Perform CPR until AED arrives and is
• Start rescue breathing: 1 breath every 5 seconds ready to attach:
• Monitor signs of circulation every 30-60 seconds: pulse, color, • Chest compressions 100/minute
movement, return of normal breathing pattern, coughing • 15 compressions to 2 breaths (1 or 2
rescuers)
Attempt Defibrillation (when AED arrives)
• POWER ON AED first
• ATTACH AED electrode pads (stop CPR)
• ANALYZE (“all clear!”)
• SHOCK (“all clear!”) up to 3 times if advised
After 3 shocks or “No shock indicated”:
• Recheck ABCs
• No Pulse? Begin CPR
• Leave AED on and attached to victim for
repeat analysis at automatically preset
intervals
Created by Kim Chunn 9/01
Revised 12/04
5
Respiratory Emergencies
Is the patient breathing?
YES NO
Allow pt. to assume position of comfort
Provide oxygen prn Attempt to ventilate patient:
Suction prn Does chest rise with ventilation?
Monitor respirations:
Depth, bilateral chest rise, resp. rate
Begin ventilations as indicated
YES NO
ACT QUICKLY!
PATIENT WILL DIE
IF NO AIRWAY
IS ESTABLISHED
Reposition airway---head-tilt/chin-lift
Continue ventilations w/ 100% oxygen Consider oral airway, use 2 people
Squeeze bag slowly and gently, use 2 people Rapidly assess for airway obstruction
Maintain head-tilt/chin-lift, consider oral airway Immediately intubate if no obstruction
Consider quickly reversible causes of apnea: Prepare for alternative airway access:
narcotic OD, hypoglycemia, hypercarbia, hypoxia LMA, Combitube, needle cricothyrotomy,
Consider intubation by most experienced person emergent tracheotomy @ bedside
Continue bag-mask ventilation and call anesthesia
if no experienced person present
Created by Kim Chunn 9/01
Revised 12/04
6
SYMPTOMATIC BRADYCARDIA
Assess ABCs
Oxygen—IV access—monitor—fluids
Vital signs, pulse oximetry, monitor
BP
Type II second-degree AV Sinus Bradycardia
block Junctional Rhythm
or Type I second-degree AV
Third-degree AV block block (Wenckebach)
Atropine 0.5 - 1.0 mg q 3-5 min (up to 0.04 mg/kg)
Transcutaneous pacing if available
Dopamine 5 - 20 µg/kg per minute
Epinephrine 2 - 10 µg/min
Isoproterenol 2 - 10 µg/min
Transcutaneous pacer ---may try
Atropine until transcutaneous pacer
arrives. Reassess ABCs—Blood pressure
preferred circulatory assessment
Created by Kim Chunn 9/01
Revised 12/04
7
STABLE TACHYCARDIAS
Assess ABCs
Oxygen—IV—Monitor
Narrow-complex Wide-complex
May go directly
Consider vagal maneuvers to cardioversion
Adenosine 6 mg rapid IV push + flush, may
amiodarone 150 mg over 10 mins
be repeated in 1 to 2 mins at 12 mg x 2.
lidocaine 1.0-1.5 mg/kg, may repeat at ½
original dose in 5 mins x 2
procainamide 20-50 mg/min up to 17 mg/kg
amiodarone 150 mg over 10 mins magnesium 1-2 gm over 1-2 mins
β blockers
calcium channel blockers Additional options if Torsades suspected:
digoxin overdrive pacing
procainamide isoproterenol drip
phenytoin
lidocaine
Sedation with short-acting agent
Synchronized cardioversion
100 J
200 J
300 J
360 J
Created by Kim Chunn 9/01
Revised 12/04
8
UNSTABLE TACHYCARDIAS
Assess ABCs
Oxygen—IV—Monitor
Sedate if possible
DO NOT DELAY CARDIOVERSION!
Have ready:
Functional suction unit
Bag-valve-mask
Intubation equipment
Synchronized cardioversion
• Ventricular Tachycardia
• Paroxysmal supraventricular 100 J
tachycardia (PSVT) 200 J
300 J
• Atrial fibrillation 360 J
• Atrial flutter
Considerations:
Effective regimens have included a sedative (eg, diazepam, midazolam, barbiturates, etomidate,
ketamine, methohexital) with or without an analgesic agent (eg, fentanyl, morphine, meperidine). Many
experts recommend anesthesia if service is readily available.
NOTE POSSIBLE NEED TO RESYNCHRONIZE AFTER EACH ENERGY DELIVERY.
If delays in synchronization occur and clinical condition is critical, go immediately to unsynchronized
shocks.
Treat polymorphic ventricular tachycardia (irregular form and rate) like ventricular fibrillation: see
VF/pulseless VT algorithm.
PSVT and Atrial flutter often respond to lower energy levels (50 J).
Created by Kim Chunn 9/01
Revised 12/04
9
PULSELESS ELECTRICAL ACTIVITY
CPR—call for monitor-defibrillator
Ventilate/oxygenate, IV access, fluids
Intubate: hyperoxygenate, confirm tube placement, secure
Rhythm on monitor without detectable pulse
Rule out causes
• POTENTIALLY FAST or EASY • PROBABLY UNTREATABLE
TO DIAGNOSE/TREAT • Massive MI
• Hypoxia • Massive PE
• Tension PTX
• Cardiac Tamponade
• Hypovolemia
• Hyper/hypokalemia
• Acidosis
• Hypothermia
• Drug Overdose
epinephrine 1 mg every 3 mins
Atropine 1 mg every 3 mins x 3 for HR < 60
Created by Kim Chunn 9/01
Revised 12/04
10
ASYSTOLE
CPR—call for defibrillator
Confirm Asystole in two leads
Rapid scene survey: any evidence personnel should not attempt resuscitation?
If the use of electricity is considered, trancutaneous pacing should be performed immediately upon
diagnosis of asystole. Insufficient data to support use of defibrillation to rule out “ultra-fine” VF.
Ventilate, oxygenate, IV access
Intubate: hyperoxygenate, confirm placement, secure tube
Rule out potentially reversible causes:
Hypoxia Hypovolemia Hypo-/hyperkalemia Acidosis
Hypothermia Drug Overdose Cardiac Tamponade
Tension Pneumothorax Massive Acute MI Massive PE
epinephrine 1 mg every 3 mins
atropine 1 mg every 3 mins x 3
If asystole persists:
Cease resuscitation efforts?
• Consider quality of resuscitation/Reassess
ABCs/Recheck end-tidal CO2 detector
• Consider termination if no response after 10 mins
• Atypical clinical features present?
• Hypothermia
• Drug OD
• Near Drowning
• In the field: termination protocols in place?
Created by Kim Chunn 9/01
Revised 12/04
11
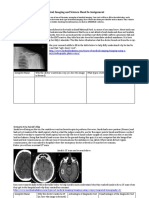
SUSPECTED STROKE
(Pre-hospital to ED arrival)
Immediate general assessment: <10 mins from arrival Immediate neuro assessment: <25 mins from arrival
Assess ABCs, vital signs Review patient history
Oxygen—IV--Monitor Establish onset (<3 hours required for fibrinolytics)
LABS: CBC, Lytes, coag studies Physical examination
Check blood sugar; treat if indicated Perform neurological examination:
*check level of consciousness (Glasgow Coma Scale)
*check level of stroke severity (NIH Stroke Scale or
Hunt and Hess Scale)
12-lead EKG; check for arrhythmias Urgent noncontrast CT
Alert Stroke Team --door-to-CT performed goal: <25 minutes
Read CT scan
--door-to-CT read goal: <45 minutes
Perform lateral cervical spine xray (pt.comatose/hx of trauma)
CT indicates non-hemorrhagic stroke CT indicates hemorrhagic stroke
• Consider fibrinolytics—TPA only approved • Consult Neurosurgery
drug for stroke: door-to-treatment goal <60 • Reverse any anticoagulants
mins • Reverse any bleeding disorder
• Lytics contraindicated for rapidly improving • Monitor neurological condition
symptoms • Treat hypertension in awake patients
• Emergent CT if deterioration
• No anticoagulant or antiplatelet therapy for 24 hrs
• Treat hypertension
Cincinnati Prehospital Stroke Scale (72% probability with one positive marker)
Facial Droop: Have patient smile or show teeth
Arm Drift: Have patient hold both arms straight out for 10 seconds with eyes closed
Abnormal Speech: Have patient repeat the phrase, “You can’t teach an old dog new tricks.”
Created by Kim Chunn 9/01
Revised 12/04
12
ISCHEMIC CHEST PAIN
Immediate assessment (<10 minutes) Immediate general assessment
• Vital signs • Oxygen
• IV access • Aspirin
• 12-lead ECG (physician reviews) • Nitroglycerin SL or spray
• Brief, targeted H&P; focus on eligibility for • Morphine IV (if pain not relieved w/
fibrinolytics nitroglycerin)
• LABS: serum cardiac markers, electrolytes, coag
studies Remember: “MONA” greets all patients
• CXR (<30 minutes) (Morphine, Oxygen, Nitroglycerin,
Aspirin)
EMS personnel can perform
immediate assessment/treatment
(“MONA”), incl. initial 12-lead ECG
and review for fibrinolytic therapy
indications and contraindications.
Start treatment as indicated
• Aspirin
• β blockers IV
• Nitroglycerin IV
• Consider ACE inhibitors
• Heparin (unfractionated or low
molecular weight) IV
• Glycoprotein IIb/IIIa inhibitors
Select a reperfusion strategy based on resources:
Lytics Interventional Cath Lab
-many choices -experienced operators (>75/year)
-rule out absolute contraindications -high-volume center (>250/year)
-major surgery or trauma (incl. -cardiac surgical back up
traumatic CPR) in last 21-30 days
-stroke of any kind in last 6 months GOAL: door-to-balloon inflation 60-120 mins.
-presence of head lesions
-known active bleeding
-bleeding disorder: plts <150,000
-uncontrolled HTN (>180/100)
GOAL: door-to-drug <30 minutes
Created by Kim Chunn 9/01
Revised 12/04
13
VENTRICULAR FIBRILLATION/
PULSELESS VENTRICULAR TACHYCARDIA
CPR—call for defibrillator
Defibrillate ASAP
200 J
200 J (BIPHASIC)
200 J
Check pulse/Resume CPR
Ventilate, oxygenate, IV access
Intubate: hyperoxygenate, confirm tube placement, secure tube
epinephrine 1 mg every 3 mins
OR
Vasopressin 40 units IV x 1 only (may resume epinephrine after 10 mins)
Defibrillate 200 J (BIPHASIC)
ANTIARRHYTHMIC CHOICES:
amiodarone: 300 mg, consider repeating 150 mg in 5 mins
lidocaine: 1 to 1.5 mg/kg, may repeat in 5 mins up to 3 mg/kg
magnesium: 1 to 2 gm in 10 ml D5 W over 1 to 2 mins, may repeat in 5 mins
procainamide: 20 to 50 mg/minute, up to 17 mg/kg
Defibrillate 200 J (BIPHASIC)
Created by Kim Chunn 9/01
Revised 12/04
14
You might also like
- ACLS Study Guide NewDocument35 pagesACLS Study Guide NewNIRANJANA SHALININo ratings yet
- Advanced Cardiac Life Support Quick Study Guide 2015 Updated GuidelinesFrom EverandAdvanced Cardiac Life Support Quick Study Guide 2015 Updated GuidelinesRating: 4 out of 5 stars4/5 (6)
- American Heart Association: Precourse Written Examination May 2001Document10 pagesAmerican Heart Association: Precourse Written Examination May 2001Ericka SwordNo ratings yet
- Pediatric Advanced Life Support Quick Study Guide 2015 Updated GuidelinesFrom EverandPediatric Advanced Life Support Quick Study Guide 2015 Updated GuidelinesRating: 5 out of 5 stars5/5 (2)
- Acls - Megacode - UpdatedDocument4 pagesAcls - Megacode - UpdatedDivine Dela Pena100% (1)
- Haemodynamic Monitoring & Manipulation: an easy learning guideFrom EverandHaemodynamic Monitoring & Manipulation: an easy learning guideNo ratings yet
- ACLS Test PrintscreenedDocument13 pagesACLS Test Printscreenedhellfireomega67% (9)
- ACLS Cheat SheetDocument8 pagesACLS Cheat SheetLenTheRN85% (27)
- ACLS Advanced Cardiovascular Life Support Provider Manual 2023From EverandACLS Advanced Cardiovascular Life Support Provider Manual 2023No ratings yet
- American Heart Association Acls Post Test AnswersDocument4 pagesAmerican Heart Association Acls Post Test AnswersArun Jude Alphonse0% (9)
- ACLS PrecourseAssessmentDocument19 pagesACLS PrecourseAssessmentBrigitte Elaine81% (21)
- Advance Cardiac Life Support: Short, Sweet and to the PointFrom EverandAdvance Cardiac Life Support: Short, Sweet and to the PointRating: 3 out of 5 stars3/5 (2)
- ACLS Practice TestDocument5 pagesACLS Practice Testprettynpink0867% (3)
- ACLS Precourse Test AnswersDocument60 pagesACLS Precourse Test AnswersTip Piraya60% (5)
- ACLS Test BankDocument13 pagesACLS Test BankSofiaSheikh94% (51)
- ACLS PharmacologyDocument6 pagesACLS PharmacologyEunice Angela Fulgueras80% (5)
- Ccrn Certification Examination Practice Questions and Answers with Rationale: First EditionFrom EverandCcrn Certification Examination Practice Questions and Answers with Rationale: First EditionRating: 5 out of 5 stars5/5 (1)
- Acls Study GuideDocument24 pagesAcls Study GuideMohammad Gita100% (17)
- 2021 ACLS Study GuideDocument20 pages2021 ACLS Study GuideShane Brown83% (12)
- ACLS Memory AidsDocument2 pagesACLS Memory Aidsmaur_jmp78% (9)
- Acls Cheat Sheet PDFDocument3 pagesAcls Cheat Sheet PDFDarren Dawkins100% (4)
- Acls Test: 1. Start CPR, Beginning With Chest CompressionsDocument15 pagesAcls Test: 1. Start CPR, Beginning With Chest CompressionsBoby Jomol100% (11)
- ACLS Answer KeyDocument23 pagesACLS Answer KeyKirana Budhiarta94% (17)
- ACLS Post Test (Copy) 낱말 카드 - QuizletDocument18 pagesACLS Post Test (Copy) 낱말 카드 - Quizlet김민길No ratings yet
- ACLS 2020 Algorithms: American Heart Association 2020 GuidelinesDocument8 pagesACLS 2020 Algorithms: American Heart Association 2020 GuidelinesNofi Nurina100% (4)
- ACLS Review TestDocument5 pagesACLS Review Testtostc60% (5)
- ACLS Exam ADocument8 pagesACLS Exam AAgil Rumboko Sumitro100% (3)
- Acls Pre Course Self Assessment Study GuideDocument7 pagesAcls Pre Course Self Assessment Study Guidenova939100% (5)
- ACLS Exams A and B 3-30-16Document67 pagesACLS Exams A and B 3-30-16bevjsn95% (64)
- ACLS Post TestDocument6 pagesACLS Post TestSheila Tolentino-Belanio73% (77)
- ACLS Exam ADocument8 pagesACLS Exam ASean Johnson83% (30)
- ACLS Rhythms Practice Test 2020 Recognition Rhythm Strips (PDF)Document11 pagesACLS Rhythms Practice Test 2020 Recognition Rhythm Strips (PDF)김민길100% (2)
- ACLS Study Guide JULY 2021 UPDATEDocument3 pagesACLS Study Guide JULY 2021 UPDATENina Morada100% (2)
- ACLS Pretest Exam AnnotatedDocument21 pagesACLS Pretest Exam AnnotatedMOLLYNo ratings yet
- Tips For PALS ExamDocument3 pagesTips For PALS ExamAy Men Alej91% (11)
- ACLS - Precourse Questions and AnswersDocument18 pagesACLS - Precourse Questions and Answerssuperdockk58% (12)
- AHA ACLS Megacode ScenariosDocument6 pagesAHA ACLS Megacode ScenariosChad Sanford78% (18)
- Test Questions - Com Test QuestionsDocument3 pagesTest Questions - Com Test QuestionsSiti Nabila20% (5)
- Cals ReviewbjvjvjDocument14 pagesCals ReviewbjvjvjCarl Jay M Ocariza100% (1)
- AclsDocument20 pagesAclsqueennita69100% (4)
- 2011 ACLS Pretest Annotated Answer KeyDocument19 pages2011 ACLS Pretest Annotated Answer KeyMohammed Abdou92% (13)
- ACLS AlgorithmsDocument4 pagesACLS Algorithmsmonickams100% (1)
- ACLS Rhythms Cheat SheetDocument21 pagesACLS Rhythms Cheat SheetShannon Hagan Wilson100% (8)
- Pharmacological Tools: Doses, Routes, and Uses of Common DrugDocument1 pagePharmacological Tools: Doses, Routes, and Uses of Common DrugApuntesdemedicinaa blogNo ratings yet
- ACLS PrecourseAssessmentDocument19 pagesACLS PrecourseAssessmentRaiedKhaled100% (1)
- Aha Acls Prep Packet 2020Document69 pagesAha Acls Prep Packet 2020VP The Hacker100% (2)
- TestDocument11 pagesTestzenagit123456100% (1)
- PALS Written Exam ADocument12 pagesPALS Written Exam AFooz Sroor91% (11)
- Study Guide: MandatoryDocument24 pagesStudy Guide: Mandatorybooksir86% (7)
- ACLS2Document7 pagesACLS2Jennifer Kaye L. DucaoNo ratings yet
- Checklist & Algoritma ACLSDocument16 pagesChecklist & Algoritma ACLSNadhif JovaldyNo ratings yet
- Acls QuestionsDocument28 pagesAcls QuestionsDsd100% (1)
- AHA ACLS Megacode ScenariosDocument6 pagesAHA ACLS Megacode ScenariosVitor Hugo G Correia86% (7)
- 2016 Updated ACLS HandoutsDocument24 pages2016 Updated ACLS Handoutskarenjlazarus86% (14)
- Medical Imaging WebquestDocument8 pagesMedical Imaging Webquestapi-262193618No ratings yet
- Standard Practice For Magnetic Particle Testing For AerospaceDocument16 pagesStandard Practice For Magnetic Particle Testing For AerospaceSaul RuizNo ratings yet
- Yumiko@Document2 pagesYumiko@api-25886263No ratings yet
- Pre Commissioning Check List of GeneratorDocument26 pagesPre Commissioning Check List of GeneratorSUROHMAN ROHMANNo ratings yet
- Measurement LabDocument4 pagesMeasurement LabHenessa GumiranNo ratings yet
- Matter and Change 2008 Chapter 14Document40 pagesMatter and Change 2008 Chapter 14cattmy100% (1)
- Anthropocene Working Group PDFDocument6 pagesAnthropocene Working Group PDFRuth Stacy EmmanuelNo ratings yet
- Finding Clara: Establishing The Biographical Details of Clara Peeters (Ca. 1587-After 1636)Document15 pagesFinding Clara: Establishing The Biographical Details of Clara Peeters (Ca. 1587-After 1636)victoriagalapedroNo ratings yet
- Chan vs. ChanDocument2 pagesChan vs. ChanMmm GggNo ratings yet
- TNEB Thermal Power PlantDocument107 pagesTNEB Thermal Power Plantvicky_hyd_130% (1)
- Drug StudyDocument4 pagesDrug Studysnowyfingers100% (1)
- French Pharmacopoeia PDFDocument15 pagesFrench Pharmacopoeia PDFHasan Abu AlhabNo ratings yet
- Chrono Biology SeminarDocument39 pagesChrono Biology SeminarSurabhi VishnoiNo ratings yet
- Top AttorneysDocument7 pagesTop AttorneysArlington MagazineNo ratings yet
- ACED Murugadoss PPT TAFEDocument91 pagesACED Murugadoss PPT TAFEMarikya GuptaNo ratings yet
- Epididymo OrchitisDocument18 pagesEpididymo OrchitisRifqi AlridjalNo ratings yet
- National Federation OF Sugar Workers (NFSW), Petitioner, vs. ETHELWOLDO R. OVEJERA Et. Al., RespondentsDocument32 pagesNational Federation OF Sugar Workers (NFSW), Petitioner, vs. ETHELWOLDO R. OVEJERA Et. Al., RespondentsRon GawatNo ratings yet
- Bituminous MixesDocument13 pagesBituminous MixesRanjit SinghNo ratings yet
- FACSDocument8 pagesFACSKarthick ThiyagarajanNo ratings yet
- Quick Guide To Cardiopulmonary Care 4th EditionDocument185 pagesQuick Guide To Cardiopulmonary Care 4th EditionLorenzo Romero AlbarranNo ratings yet
- Sail ProjectDocument28 pagesSail ProjectShahbaz AlamNo ratings yet
- Chapter 1 Section 6 Spoon Feeding BasicsDocument9 pagesChapter 1 Section 6 Spoon Feeding Basicskenneth mayaoNo ratings yet
- 04 TitrimetryDocument7 pages04 TitrimetryDarwin Fetalbero ReyesNo ratings yet
- D435L09 Dental Trauma-2C Cracked Teeth - 26 Root FractureDocument73 pagesD435L09 Dental Trauma-2C Cracked Teeth - 26 Root FractureD YasIr MussaNo ratings yet
- HSE TBT Schedule - Apr 2022Document1 pageHSE TBT Schedule - Apr 2022deepak bhagatNo ratings yet
- Turbo Lab 1Document10 pagesTurbo Lab 1Seng SoonNo ratings yet
- FPGA-based System For Heart Rate Monitoring PDFDocument12 pagesFPGA-based System For Heart Rate Monitoring PDFkishorechiyaNo ratings yet
- Biecco Lawrie Ece Gec Reyrolle Burn Jyoti SwitchgearDocument18 pagesBiecco Lawrie Ece Gec Reyrolle Burn Jyoti SwitchgearSharafat AliNo ratings yet
- Wound Dressing ChecklistDocument3 pagesWound Dressing ChecklistBUAHIN JANNA100% (1)
- Pressure MeasurementDocument293 pagesPressure MeasurementGlen Lauren PerezNo ratings yet