Professional Documents
Culture Documents
Swchwanoma
Uploaded by
hockteo77Original Description:
Original Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Swchwanoma
Uploaded by
hockteo77Copyright:
Available Formats
DOI 10.3349/ymj.2010.51.6.
938
Original Article pISSN: 0513-5796, eISSN: 1976-2437 Yonsei Med J 51(6):938-942, 2010
Schwannoma in Head and Neck: Preoperative Imaging
Study and Intracapsular Enucleation
for Functional Nerve Preservation
Si Hong Kim, Na Hyun Kim, Kyung Rok Kim, Ja Hyun Lee, and Hong-Shik Choi
Department of Otorhinolaryngology, Institute of Logopedics & Phoniatrics, Yonsei University College of Medicine,
Gangnam Severance Hospital, Seoul, Korea.
Received: March 3, 2010 Purpose: In treating schwannoma patients, it is critical to determine the origin of the
Revised: April 28, 2010 tumor to preserve nerve function. We evaluated the validity of preoperative imaging
Accepted: May 17, 2010 studies in distinguishing the neurological origin of the schwannomas of the head and
Corresponding author: Dr. Hong-Shik Choi, neck, and the efficacy of intracapsular enucleation in preserving nerve function.
Department of Otorhinolaryngology, Yonsei Materials and Methods: In 7 cases of schwannomas in the head and neck region,
University College of Medicine, Gangnam we predicted whether the tumor originated from the vagus nerve or the cervical
Severance Hospital, Gangnam-gu,
sympathetic chain through imaging studies including computed tomography (CT)
712 Eonju-ro, Seoul 135-270, Korea.
and magnetic resonance imaging (MRI). All patients were performed intracapsular
Tel: 82-2-2019-3461, Fax: 82-2-3463-4750
enucleation, and the function of the vagus nerve and the sympathetic nerve was
E-mail: hschoi@yuhs.ac
evaluated preoperatively and postoperatively. Results: Preoperative imaging studies
∙The authors have no financial conflicts of
showed 6 cases where the tumor was located between the carotid artery and the
interest. internal jugular vein, and 1 case where the tumor was located posteriorly, displacing
the carotid artery and the internal jugular vein anteriorly. At the time of operation,
we confirmed schwannoma originating from the vagus nerve on the first 6 cases, and
schwannoma originating from the sympathetic nervous system on the last case. All
patients went through successful intracapsular enucleation, and of the seven schwan-
noma cases, 6 patients maintained normal postoperative neurological function
(85.7%). Conclusion: Preoperative imaging studies offer valuable information
regarding the location and origination of the tumor, and intracapsular enucleation
helped us to preserve the nerve function.
Key Words: Schwannoma, vagus nerve, sympathetic nerve, intracapsular enuclea-
tion, nerve function
INTRODUCTION
Schwannoma is a benign neural sheath tumor, and it occurs as a single entity in
many cases. It also occurs in overall body areas including the head and neck
© Copyright: region. As a slowly-growing benign tumor, it has been reported to occur in the
Yonsei University College of Medicine 2010 head and neck region in approximately 25-40% of total schwannoma cases.1 It
This is an Open Access article distributed under the
terms of the Creative Commons Attribution Non-
involves the cranial nerves such as V, VII, IV, X, XI, and XII or the sympathetic
Commercial License (http://creativecommons.org/ and peripheral nerves.2 Schwannomas surround many kinds of cranial nerves or
licenses/by-nc/3.0) which permits unrestricted non- other nerves could occur in the head and neck region, it is known that most
commercial use, distribution, and reproduction in any
medium, provided the original work is properly cited. schwannomas occurring in the head and neck region generally originate from the
938 Yonsei Med J http://www.eymj.org Volume 51 Number 6 November 2010
Preoperative Imaging Study and Intracapsular Enucleation in Schwannoma
vagus nerve or sympathetic nervous system, and various
preoperative image studies are used to distinguish its loca-
tion and origin.3 The accepted treatment of schwannoma is
surgical resection, and several surgical modalities have
been introduced to preserve the neurological functions.4-6
Recently, intracapsular enucleation has been introduced
for the preservation of the neurological functions. In this
study, we evaluated the validity of preoperative imaging
studies in distinguishing the neurological origin of the
schwannomas of the head and neck, and the efficacy of
intracapsular enucleation in preserving the nerve function. Fig. 1. Neck CT image of a vagal schwannoma patient. Tumor (asterisk) is
separating the common carotid artery (white arrow) anteriorly and internal
jugular vein (arrow head) posteriorly.
MATERIALS AND METHODS
This study was conducted on seven patients who were
suspected with schwannoma at the Department of
Otorhinolaryngology Gangnam Severance Hospital from
March 2003 to September 2009. All the patients compl-
ained of a neck mass as a major symptom. Six patients had
normal nerve function, the other one complained of ptosis.
There were three men and four women, whose ages ranged
Fig. 2. Neck CT image of a sympathetic schwannoma patient. Tumor (asterisk)
between 46 and 71. Computed tomography (CT) and mag-
is anteriorly displacing the common carotid artery (white arrow) and internal
netic resonance imaging (MRI) were performed to examine jugular vein (arrow head) together without separating them.
the location of the tumor and its correlation with the
carotid artery and the internal jugular vein. Whether the confirmed schwannoma originating from the vagus nerve
tumor displaced the internal jugular vein and carotid artery on the first 6 cases, and schwannoma originating from the
to the same direction or to the opposite directions was sympathetic nervous system on the last case (Table 1). The
evaluated. tumor was surrounded by the nerve fibers in all 7 cases,
After informed consent, all patients underwent intra- and an incision was made on the capsule. The tumor was
capsular enucleation via the transcervical approach under carefully dissected from the capsule while preserving the
general anesthesia. After exposing the tumor in the carotid nerve fibers, and intracapsular enucleation was performed
sheath, a vertical incision parallel to the direction of the (Figs. 3 and 4). The preoperative and postoperative neurol-
nerve was made on the capsule, after confirming that the ogical functions were evaluated. Of the six vagal schwan-
nerve fibers surrounded the tumor. Then intracapsular nomas, five cases maintained normal postoperative neurol-
enucleation was performed as the tumor was carefully ogical function. In the case of sympathetic schwannoma,
dissected from the capsule without any damages given to there were no aggravated neurological deficits except for
the nerve fibers. Special attention was paid to preserve the the ptosis which was observed preoperatively (Table 2).
lymphovascular structure within the nerve sheath. The
function of the vagus nerve and the sympathetic nerve was
evaluated preoperatively and postoperatively by examining
DISCUSSION
vocal cord mobility with laryngoscope and symptoms of
Hornor’s syndrome. It is well-known that schwannoma occurring in the head and
neck region mostly originates from the vagus nerve or sym-
pathetic nervous system. It is also known that the incidence
RESULTS of vagal schwannoma is 2 to 3 times higher than that of
sympathetic schawannoma.7 Schwannoma can compress
Preoperative imaging studies showed 6 cases where the the maternal nerve fibers which go over the tumor capsule
tumor located between the carotid artery and the internal as its size is gradually increased. Therefore, nerve paralysis
jugular vein, and 1 case where the tumor located posterio- may occur preoperatively. Vagal schwannoma is typically
rly displacing the carotid artery and the internal jugular characterized by dysphagia and hoarseness. Sympathetic
vein anteriorly (Figs. 1 and 2). At the time of operation, we schwannoma is characterized by Horner’s syndrome. In
Yonsei Med J http://www.eymj.org Volume 51 Number 6 November 2010 939
Si Hong Kim, et al.
most cases, however, there are no symptoms, thus it is dif- In making a differential diagnosis of the intracranial
ficult to identify the neurological origin based on the physi- tumors, imaging studies play a key role. Particularly in cases
cal examination.8,9 in which schwannoma was suspected, CT is routinely
Table 1. Imaging Findings and Probable Nerves of Origin vs. Diagnosis (n = 7) (Schwannoma in Head and
Neck Case at Gangnam Severance 2003 - 2009)
Patient Probable nerve
Imaging findings Diagnosis
no. origin
1 2 3 6 cm Tumor separates the ICA and IJV Vagus Vagus
2 1 2 4 cm Tumor separates the ICA and IJV Vagus Vagus
3 3 3 4 cm Tumor separates the ICA and IJV Vagus Vagus
4 6 6 4 cm Tumor separates the ICA and IJV Vagus Vagus
5 2 3 6 cm Tumor displaces the ICA and IJV Sympathetic Sympathetic
anteriorly trunk trunk
6 3 3.5 5.5 cm Tumor separates the ICA and IJV Vagus Vagus
7 4 3 5.5 cm Tumor separates the ICA and IJV Vagus Vagus
ICA, internal carotid artery; IJV, internal jugular vein.
Table 2. Neural Function Outcome after Tumor Intracapsular Enucleation (n = 7) (Schwannoma in Head and
Neck Case at Gangnam Severance 2003 - 2009)
Patient no. Nerve Preoperative status Postoperative status
1 Vagus Normal Normal
2 Vagus Normal Vocal fold paralysis
3 Vagus Normal Normal
4 Vagus Normal Normal
5 Sympahtic trunk Ptosis Ptosis (no interval change)
6 Vagus Normal Normal
7 Vagus Normal Normal
A B C
Fig. 3. Operative findings (A and B) and specimen (C) of a vagal schwannoma patient. (A) A vagal schwannoma that surrounded the capsule
exposed. (B) After confirming that the nerve fibers surrounded the tumor, intracapsular enucleation was performed as the tumor was carefully
dissected from the capsule without any damages given to the nerve fibers. (C) A photograph of the schwannoma specimen. About 1cm sized
rounded mass without the capsule is observed.
A B C D
Fig 4. Operative findings (A-C) and specimen (D) of a sympathetic schwannoma patient. (A) A sympathetic schwannoma that surrounded the capsule exposed. (B) A
vertical incision parallel to the direction of the nerve was made on the capsule. (C) Tumor was enucleated by preserving the neural pathway using the microsurgical
technique. (D) A photograph of multiple schwannoma specimens. About 6 cm sized yellowish mass like fat tissue without the capsule is observed.
940 Yonsei Med J http://www.eymj.org Volume 51 Number 6 November 2010
Preoperative Imaging Study and Intracapsular Enucleation in Schwannoma
performed, and such imaging diagnostic modalities as Previous studies reported the preservation rate of the
MRI, Dyanimc MRI, and angiography may be performed neurological functions following the intracapsular enuclea-
additionally. Imaging diagnostic modalities like CT and tion to be 30-80%. In our series, the neurological function
MRI offer great help in identifying the tumor and its cor- was preserved in 6 out of 7 cases. Only a minimum longi-
relations with surrounding vascular structures, muscles, tudinal incision in the capsule was made during the opera-
and nerves.3 From an anatomical perspective, the carotid tion and the capsule was not connected to the nerve fibers.
sheath contains the carotid artery, the internal jugular vein, When the tumor was removed after making an incision,
and the vagus nerve. The carotid sympathetic ganglion additional damages around the capsule did not occur. Mo-
descends medioposteiror aspect to the carotid sheath. reover, when the tumor was not isolated from the capsule,
Accordingly, when a vagal schwannoma is enlarged, the we used our fingers to remove the tumor from the capsule.
internal jugular vein is displaced laterally, and the carotid These cautious intracapsular enucleations could have led to
artery is displaced medially, displaying each other. In the maintaining of 86% of their nerve function after the
contrast, when a sympathetic schwannoma is enlarged, the operation. In the case of patient #2, intracapsular enuclea-
carotid sheath is displaced anteriolaterally, not displaying tion was performed routinely; however, multiple schwan-
the internal jugular vein and the carotid artery.10-12 nomas directly connected to the nerve fiber were observed
In 1996, Furukawa, et al. performed imaging studies on intraoperatively. This suggests the possibility of perineu-
nine schwannoma patients, and suggested their neurologi- rium or endoneurium origin schwannoma, and it may have
cal origin prior to surgery. These authors reported an ac- caused the vocal cord paralysis examined postoperatively.
curate diagnostic rate of 100%.3 In 2007, Saito, et al. also Many controversies exist regarding the recurrence rate
made an accurate diagnosis at a rate of 83% prior to surgery between the total tumor resection including nerve fibers
in 12 schwannoma patients.12 In this study, with the criteria and the intracapsular enucleation. According to Zbären, et
proposed by Furukawa, et al. imaging studies were per- al., there was no significant difference in the recurrence
formed on all seven cases, and an accurate diagnosis was rate between the total tumor resection including nerve
made in all cases when confirmed with later surgeries.3 fibers and the intracapsular enucleation. In cases where
Preoperative diagnosis based on imaging studies offered partial removal of the tumor was performed, however, the
better understanding of the anatomical correlation between recurrence rate has been reported to rise.19 In this study, the
the nerve and vascular structures intraoperatively. We mean follow-up period after the surgery was 3.42 years,
were also able to explain to the patients each complication and no recurrence has yet been noted. However, further
of vagal schwannoma and sympathetic schwannoma long-term regular follow-up imaging studies are needed in
which may follow the surgery preoperatively. As the this series.
authors had just experienced only one case of the schwan- In conclusion, in cases of schwannoma arising in the
noma of sympathetic origin, the follow-up studies are head and neck region, surgical resection may cause fatal
needed for the accuracy of this study. nerve damage unlike other tumors. Therefore, treatments
Schwannoma is a benign tumor that originates from the assuring the preservation of neurological functions are
neural sheath of Schwann cells. Previously, to prevent the needed. In the current study, the neurological origins of
recurrence of tumors, radical dissection including the neuro- schwannomas were predicted through preoperative imag-
progenitor cells was performed. Even in cases in which ing studies, before the surgical procedure, and we were
recovery was achieved following the nerve transplantation able to explain the possible nerve damages to patients.
or primary anastomosis, preservation of the neurological Intracapsular enucleation was performed in all cases, and
function was not to be expected. Most of the neuropro- the postoperative neurological functions were preserved in
genitor fibers do not run through schwannoma and they most cases without recurrence. Thus, we report our treat-
pass over the tumor capsule.13,14 ment outcomes with a review of literature that preoperative
Most schwannomas are encapsulated. In cases where the imaging studies were effective for making an accurate
nerve fibers surround the surface of tumors, the intracap- diagnosis, and intracapsular enucleation was effective for
sular enucleation can be performed while preserving the preserving the neurological functions.
nerve fibers. According to the study by Valentino, et al.,
intracapsular enucleation while preserving the nerve fibers
preserved its function by more than 30% when compared
REFERENCES
to tumor resection with primary anastomsosis.15 The neurol-
ogical functions can also be monitored using a nerve 1. Ducatman BS, Scheithauer BW, Piepgras DG, Reiman HM,
stimulator or under a microscope in performing the intraca- Ilstrup DM. Malignant peripheral nerve sheath tumors. A clinico-
pathologic study of 120 cases. Cancer 1986;57:2006-21.
psular enucleation.15-18
Yonsei Med J http://www.eymj.org Volume 51 Number 6 November 2010 941
Si Hong Kim, et al.
2. Colreavy MP, Lacy PD, Hughes J, Bouchier-Hayes D, Brennan nance imaging and the management of parapharyngeal space
P, O’Dwyer AJ, et al. Head and neck schwannomas: a 10 year tumors. Head Neck 1996;18:67-77.
review. J Laryngol Otol 2000;114:119-24. 12. Saito DM, Glastonbury CM, El-Sayed IH, Eisele DW. Parap-
3. Furukawa M, Furukawa MK, Katoh K, Tsukuda M. Differen- haryngeal space schwannomas: preoperative imaging determina-
tiation between schwannoma of the vagus nerve and schwan- tion of the nerve of origin. Arch Otolaryngol Head Neck Surg
noma of the cervical sympathetic chain by imaging diagnosis. 2007;133:662-7.
Laryngoscope 1996;106:1548-52. 13. Chang SC, Schi YM. Neurilemmoma of the vagus nerve. A case
4. Fujino K, Shinohara K, Aoki M, Hashimoto K, Omori K. Intracap- report and brief literature review. Laryngoscope 1984;94:946-9.
sular enucleation of vagus nerve-originated tumors for preserva- 14. Saydam L, Kizilay A, Kalcioglu T, Gurer I. Ancient cervical
tion of neural function. Otolaryngol Head Neck Surg 2000;123: vagal neurilemmoma: a case report. Am J Otolaryngol 2000;21:
334-6. 61-4.
5. Fornaro R, Frascio M, Stabilini C. Excision of a schwannoma of 15. Valentino J, Boggess MA, Ellis JL, Hester TO, Jones RO. Ex-
the head and neck: surgical technique. G Chir 2006;27:428-32. pected neurologic outcomes for surgical treatment of cervical
6. Moukarbel RV, Sabri AN. Current management of head and neck neurilemomas. Laryngoscope 1998;108:1009-13.
schwannomas. Curr Opin Otolaryngol Head Neck Surg 2005;13: 16. Charles D, Yingling CD. Intraoperative monitoring of cranial
117-22. nerves in neurotologic surgery. In: Cummings CW, Fredrickson
7. Wax MK, Shiley SG, Robinson JL, Weissman JL. Cervical JM, Harker LA, Krause CJ, Schuller DE, editors. Otolaryngol-
sympathetic chain schwannoma. Laryngoscope 2004;114:2210-3. Head and Neck Surgery. St. Louis:Mosby year Book; 1996.
8. Gilmer-Hill HS, Kline DG. Neurogenic tumors of the cervical p.3331-55.
vagus nerve: report of four cases and review of the literature. 17. Pesavento G, Ferlito A, Recher G. Benign solitary schwannoma
Neurosurgery 2000;46:1498-503. of the cervical vagus nerve. A case report with a review of the
9. de Araujo CE, Ramos DM, Moyses RA, Durazzo MD, Cernea literature. J Laryngol Otol 1979;93:307-16.
CR, Ferraz AR. Neck nerve trunks schwannomas: clinical fea- 18. Langner E, Del Negro A, Akashi HK, Araújo PP, Tincani AJ,
tures and postoperative neurologic outcome. Laryngoscope 2008; Martins AS. Schwannomas in the head and neck: retrospective
118:1579-82. analysis of 21 patients and review of the literature. Sao Paulo
10. Wang CP, Hsiao JK, Ko JY. Splaying of the carotid bifurcation Med J 2007;125:220-2.
caused by a cervical sympathetic chain schwannoma. Ann Otol 19. Zbären P, Markwalder R. Schwannoma of the true vocal cord.
Rhinol Laryngol 2004;113:696-9. Otolaryngol Head Neck Surg 1999;121:837-9.
11. Miller FR, Wanamaker JR, Lavertu P, Wood BG. Magnetic reso-
942 Yonsei Med J http://www.eymj.org Volume 51 Number 6 November 2010
You might also like
- TFN Declaration FormDocument6 pagesTFN Declaration FormTim DunnNo ratings yet
- The Pentester BlueprintDocument27 pagesThe Pentester Blueprintjames smith100% (1)
- Break Free - Nathaniel BrandenDocument16 pagesBreak Free - Nathaniel Brandennbckudxtkudkuf50% (2)
- Presentation On Data Integrity in PharmaDocument80 pagesPresentation On Data Integrity in Pharmaskvemula67% (3)
- Colreavy 2000Document6 pagesColreavy 2000Yi-Hung SungNo ratings yet
- 2008 TWPRMLinDocument8 pages2008 TWPRMLinVictor_id077No ratings yet
- Cervical Sympathetic Chain Ganglioneuroma: Case Report and Review of LiteratureDocument4 pagesCervical Sympathetic Chain Ganglioneuroma: Case Report and Review of LiteratureIOSR Journal of PharmacyNo ratings yet
- A Rare Case of Optic Nerve Schwannoma: Case Report and Review of The LiteratureDocument5 pagesA Rare Case of Optic Nerve Schwannoma: Case Report and Review of The LiteratureloversockfulNo ratings yet
- Paraganglioma of Neck in Middle Aged Male: A Case ReportDocument4 pagesParaganglioma of Neck in Middle Aged Male: A Case ReportIJAR JOURNALNo ratings yet
- 5thDocument17 pages5thMohamed MohammedNo ratings yet
- The Long Term Outcome After Resection Of.20 PDFDocument9 pagesThe Long Term Outcome After Resection Of.20 PDFDragos IftimieNo ratings yet
- Facial UltrassomDocument7 pagesFacial UltrassomcarlosNo ratings yet
- SaudiMedJ 36 1363Document4 pagesSaudiMedJ 36 1363Lý TưởngNo ratings yet
- Meningeal SarcomaDocument4 pagesMeningeal SarcomaFebrina RamadhaniNo ratings yet
- Atretic Cephaloceles May Indicate Underlying Brain AbnormalitiesDocument6 pagesAtretic Cephaloceles May Indicate Underlying Brain AbnormalitiesAhmed H. Ali ElbestaweyNo ratings yet
- Headache After Removal of Vestibular Schwannoma Via The Retrosigmoid Approach: A Long-Term Follow-Up-StudyDocument9 pagesHeadache After Removal of Vestibular Schwannoma Via The Retrosigmoid Approach: A Long-Term Follow-Up-StudySebastian GiovanniniNo ratings yet
- Vol-1, Issue-1 Prospective Study of Peripheral Nerve Tumors Over A Period of 2 YearsDocument4 pagesVol-1, Issue-1 Prospective Study of Peripheral Nerve Tumors Over A Period of 2 YearsijhrmimsNo ratings yet
- World Journal of Radiology PDFDocument8 pagesWorld Journal of Radiology PDFniluhNo ratings yet
- Rare Subglottic SchwannomaDocument2 pagesRare Subglottic Schwannomaaraila123No ratings yet
- Bahan 3Document11 pagesBahan 3Adam JohnsonNo ratings yet
- 1 s2.0 S0967586817300024 MainDocument10 pages1 s2.0 S0967586817300024 MainFabianto SantosoNo ratings yet
- Epidermoid Cysts TNEDocument10 pagesEpidermoid Cysts TNEbello_england_209552No ratings yet
- SANCHEZ GONZALEZ FEDERICO. White Matter Topographic Anatomy Applied To Temporal Lobe Surgery. WORLD NEUROSURGERY 2019Document10 pagesSANCHEZ GONZALEZ FEDERICO. White Matter Topographic Anatomy Applied To Temporal Lobe Surgery. WORLD NEUROSURGERY 2019Federicos Sánchez GonzálezNo ratings yet
- Facial Nerve Diameter Reference Values in Healthy AdultsDocument5 pagesFacial Nerve Diameter Reference Values in Healthy AdultsCarlinhosdadeep DeepWebNo ratings yet
- Systematic Ultrasound Identification of The Dorsal Scapular and Long Thoracic Nerves During Interscalene BlockDocument4 pagesSystematic Ultrasound Identification of The Dorsal Scapular and Long Thoracic Nerves During Interscalene BlockWidya AriatyNo ratings yet
- Neurol J Southeast Asia 1999 4: 83 - 88: LCS Tan, YY Sitoh, HTL TjiaDocument6 pagesNeurol J Southeast Asia 1999 4: 83 - 88: LCS Tan, YY Sitoh, HTL Tjiarani suwadjiNo ratings yet
- Articol ORLDocument6 pagesArticol ORLSabina BădilăNo ratings yet
- Spinal Epidural Cavernous Hemangiomas in The 2024 International Journal of SDocument3 pagesSpinal Epidural Cavernous Hemangiomas in The 2024 International Journal of SRonald QuezadaNo ratings yet
- (10920684 - Neurosurgical Focus) Surgical Management of Trigeminal Schwannomas - Defining The Role For Endoscopic Endonasal ApproachesDocument9 pages(10920684 - Neurosurgical Focus) Surgical Management of Trigeminal Schwannomas - Defining The Role For Endoscopic Endonasal ApproachesasiyazaidiaNo ratings yet
- Case Series - A Radiological Spectrum of Cranial Nerve SchwannomasDocument11 pagesCase Series - A Radiological Spectrum of Cranial Nerve SchwannomasInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- The Roof of The Labyrinthine Facial Nerve Canal and The Geniculate Ganglion Fossa On High-Resolution Computed Tomography - Dehiscence Thickness and PneumatizationDocument11 pagesThe Roof of The Labyrinthine Facial Nerve Canal and The Geniculate Ganglion Fossa On High-Resolution Computed Tomography - Dehiscence Thickness and PneumatizationSa'Deu FondjoNo ratings yet
- Alwahab2017 Article OccipitalMeningoencephaloceleC PDFDocument4 pagesAlwahab2017 Article OccipitalMeningoencephaloceleC PDFOvamelia JulioNo ratings yet
- Clinical Features and Outcomes in Patients With Non-Acoustic Cerebellopontine Angle TumoursDocument4 pagesClinical Features and Outcomes in Patients With Non-Acoustic Cerebellopontine Angle TumoursRikizu HobbiesNo ratings yet
- Neonatal Neurosonography: A Pictorial Essay: Venkatraman Bhat, Varun BhatDocument19 pagesNeonatal Neurosonography: A Pictorial Essay: Venkatraman Bhat, Varun BhatHeitor Bittencourt Netto0% (1)
- 127 - Case Report - Complicanza Iniezione Faccette CervicaliDocument3 pages127 - Case Report - Complicanza Iniezione Faccette CervicaliMarco PeroliNo ratings yet
- Idiopathic Cervical Spinal Subdural Haematoma: A Case Report and Literature ReviewDocument10 pagesIdiopathic Cervical Spinal Subdural Haematoma: A Case Report and Literature ReviewSelfa YunitaNo ratings yet
- Surgical Outcome of Primary Intradural Surgical Outcome of Primary IntraduralDocument6 pagesSurgical Outcome of Primary Intradural Surgical Outcome of Primary Intraduralmazen alkarrasNo ratings yet
- Medicine: Brachial Plexus Schwannoma Mimicking Cervical LymphadenopathyDocument4 pagesMedicine: Brachial Plexus Schwannoma Mimicking Cervical LymphadenopathykalixinNo ratings yet
- Pon XDocument6 pagesPon XMillerNo ratings yet
- Neurosonography in The Neonate FinalDocument9 pagesNeurosonography in The Neonate FinalCh RajeshNo ratings yet
- TMP 33 BFDocument6 pagesTMP 33 BFFrontiersNo ratings yet
- Meningioma of The Internal Auditory Canal Case ReportDocument4 pagesMeningioma of The Internal Auditory Canal Case ReportStanley KambeyNo ratings yet
- Spinal Tumour Surgery OutcomesDocument5 pagesSpinal Tumour Surgery OutcomesNouman Safdar AliNo ratings yet
- Spinal Tumors ArticleDocument5 pagesSpinal Tumors ArticleMariaLakhaniNo ratings yet
- V69n2a17 PDFDocument5 pagesV69n2a17 PDFK'RiBo Siahaan PaRt IINo ratings yet
- Al-Gahtany2003 Article PrimaryCentralNervousSystemSarDocument10 pagesAl-Gahtany2003 Article PrimaryCentralNervousSystemSarNadia Ximena Rodríguez VargasNo ratings yet
- NeuroDocument6 pagesNeuroAkhdan AufaNo ratings yet
- Implications For The Treatment of Chronic HeadachesDocument5 pagesImplications For The Treatment of Chronic HeadachesCloé SzcNo ratings yet
- Overview of Intraoperative Neurophysiological Monitoring During Spinal Surgery - 2016 PDFDocument7 pagesOverview of Intraoperative Neurophysiological Monitoring During Spinal Surgery - 2016 PDFAndrea RoesnerNo ratings yet
- Vestibular Neuritis Affects Both Superior and Inferior Vestibular NervesDocument10 pagesVestibular Neuritis Affects Both Superior and Inferior Vestibular NervesSabina BădilăNo ratings yet
- Microsurgical Anatomy Brainstem Safe Entry Zones, Jns 2016Document18 pagesMicrosurgical Anatomy Brainstem Safe Entry Zones, Jns 2016Andrés SeguraNo ratings yet
- 1009 Case 2Document4 pages1009 Case 2willygopeNo ratings yet
- Neonatal Neurosonography: A Pictorial Essay: EuroradiologyDocument13 pagesNeonatal Neurosonography: A Pictorial Essay: EuroradiologyAnom RahartoNo ratings yet
- Imaging Findings of Vascular Lesions in The Head and NeckDocument7 pagesImaging Findings of Vascular Lesions in The Head and NeckSLMC-QC IRNo ratings yet
- kerasnoudis2014Document10 pageskerasnoudis2014Laura A M MNo ratings yet
- causas neuropatia cranel multpile hivDocument4 pagescausas neuropatia cranel multpile hivBatgirl xoxoNo ratings yet
- NeuroradiologyCurrent and Future Imaging of The Peripheral NervoussystemDocument10 pagesNeuroradiologyCurrent and Future Imaging of The Peripheral NervoussystemRyanNo ratings yet
- Intrasphenoidal Encephalocele: An Incidental Finding in Emergency DepartmentDocument3 pagesIntrasphenoidal Encephalocele: An Incidental Finding in Emergency DepartmentRinda AndreanditaNo ratings yet
- Clinical Features of Intracranial Vestibular SchwannomasDocument6 pagesClinical Features of Intracranial Vestibular SchwannomasIndra PrimaNo ratings yet
- Resection of Gliomas With and Without Neuropsychological Support During Awake Craniotomy-Effects On Surgery and Clinical OutcomeDocument8 pagesResection of Gliomas With and Without Neuropsychological Support During Awake Craniotomy-Effects On Surgery and Clinical OutcomeHellen SantosNo ratings yet
- EmailingMedPulse 2 5 8Document4 pagesEmailingMedPulse 2 5 8Satyaja KinnaraNo ratings yet
- 2019 - Chung Et Al-AnnotatedDocument6 pages2019 - Chung Et Al-AnnotatedCemal GürselNo ratings yet
- Aaid Joi D 13 00346Document8 pagesAaid Joi D 13 00346na huNo ratings yet
- Ultrasonography Diagnosis of Peripheral Nerves: Cases and IllustrationsFrom EverandUltrasonography Diagnosis of Peripheral Nerves: Cases and IllustrationsDingzhang ChenNo ratings yet
- Catalogo Unidad Enfriadora Trane R-407C PDFDocument8 pagesCatalogo Unidad Enfriadora Trane R-407C PDFJUAN FRANCISCO AYALANo ratings yet
- App 17 Venmyn Rand Summary PDFDocument43 pagesApp 17 Venmyn Rand Summary PDF2fercepolNo ratings yet
- To 1 BUMN 2023 Bahasa Inggris StructureDocument5 pagesTo 1 BUMN 2023 Bahasa Inggris StructureKukuh Perkasa WirayudaNo ratings yet
- Chemistry CHM 1311C 2012 Test 1 BlankDocument6 pagesChemistry CHM 1311C 2012 Test 1 BlankSimon HagosNo ratings yet
- Edna Adan University ThesisDocument29 pagesEdna Adan University ThesisAbdi KhadarNo ratings yet
- Recombinant DNA TechnologyDocument14 pagesRecombinant DNA TechnologyAnshika SinghNo ratings yet
- Darnell's Father Goes StrictDocument2 pagesDarnell's Father Goes StrictDavid Theodore Richardson IIINo ratings yet
- Vacuum Conveyin 5.0Document56 pagesVacuum Conveyin 5.0Mostafa AtwaNo ratings yet
- Arecaceae or Palmaceae (Palm Family) : Reported By: Kerlyn Kaye I. AsuncionDocument23 pagesArecaceae or Palmaceae (Palm Family) : Reported By: Kerlyn Kaye I. AsuncionNamae BacalNo ratings yet
- MPQ2908 - 48V Buck Converter Automotive Reference DesignDocument4 pagesMPQ2908 - 48V Buck Converter Automotive Reference DesignShubham KaklijNo ratings yet
- Rawat Inap Rumah Sakit Santa Elisabeth Medan Englin Moria K. Tinambunan, Lindawati F. Tampubolon, Erika E. SembiringDocument14 pagesRawat Inap Rumah Sakit Santa Elisabeth Medan Englin Moria K. Tinambunan, Lindawati F. Tampubolon, Erika E. SembiringafrilianaNo ratings yet
- Lesson 8 - Philippine Disaster Risk Reduction and Management SystemDocument11 pagesLesson 8 - Philippine Disaster Risk Reduction and Management SystemMary Joy CuetoNo ratings yet
- Power Systems-III Ditital NotesDocument102 pagesPower Systems-III Ditital NotesSimranNo ratings yet
- Atomic and Molecular PhysicsDocument28 pagesAtomic and Molecular PhysicsAvinash GuptaNo ratings yet
- 12 2022 Salary Slip SintexDocument1 page12 2022 Salary Slip SintexpathyashisNo ratings yet
- Company Law AssignmentDocument5 pagesCompany Law AssignmentABISHEK SRIRAM S 17BLA1008No ratings yet
- PTA Resolution for Donation to School WashroomDocument2 pagesPTA Resolution for Donation to School WashroomMara Ciela CajalneNo ratings yet
- Final Project Report 2Document8 pagesFinal Project Report 2Mallesh MaranurNo ratings yet
- Rise School of Accountancy Test 08Document5 pagesRise School of Accountancy Test 08iamneonkingNo ratings yet
- Mechanical Thrombectomy For Acute Ischemic StrokeDocument19 pagesMechanical Thrombectomy For Acute Ischemic StrokeCarlos Alfredo Vargas QuinteroNo ratings yet
- 2022 TESAS PublicationDocument103 pages2022 TESAS PublicationNathan LakaNo ratings yet
- Edinburgh Postnatal Depression Scale. Detection of Postnatal Depression. Development of The 10-ItemDocument6 pagesEdinburgh Postnatal Depression Scale. Detection of Postnatal Depression. Development of The 10-ItemKyze LQNo ratings yet
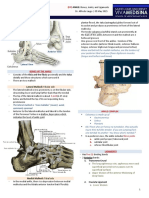
- (9F) Ankle - Bones, Joints, Tendons and LigamentsDocument4 pages(9F) Ankle - Bones, Joints, Tendons and LigamentsJeffrey RamosNo ratings yet
- Vietnam Snack Market Grade BDocument3 pagesVietnam Snack Market Grade BHuỳnh Điệp TrầnNo ratings yet
- Naskah PublikasiDocument14 pagesNaskah PublikasiNirmala malaNo ratings yet
- Causes of DyspneaDocument9 pagesCauses of DyspneaHanis Afiqah Violet MeowNo ratings yet