Professional Documents
Culture Documents
Testis Tuberculosis Case Without Pulmonary or Renal Involvement
Uploaded by
ntambik21Original Description:
Original Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Testis Tuberculosis Case Without Pulmonary or Renal Involvement
Uploaded by
ntambik21Copyright:
Available Formats
Kathmandu University Medical Journal (2006), Vol. 4, No.
1, Issue 13, 98-99
Case Note
Isolated tuberculosis of testis
Biswas M1, Rahi R2, Tiwary SK3, Khanna R4, Khanna AK5 1,2 Resident in Surgery, 3Senior Resident in Surgery, 4Reader in Surgery, 5Professor of Surgery, Department of General surgery Institute of Medical Sciences Banaras Hindu University Varanasi-221005, INDIA Abstract Isolated epididymo-orchitis is an uncommon presentation of tuberculosis. We report a case of left sided epididymoorchitis and scrotal involvement due to tuberculosis in a young male patient. The diagnosis was suspected on clinical examination of scrotum and confirmed by FNAC of scrotal and testis. Patient improved after taking antitubercular treatment. Key words: infection, scrotum, treatment enitourinary tuberculosis is one of the most common manifestations of extrapulmonary tuberculosis and represents 2-4% of cases of tuberculosis or approximately 15% of non-pulmonary manifestations of tuberculosis, although genitourinary involvement has been noted in 7 % of the patients with tuberculosis at autopsy1. The prostate, epididymis and seminal vesicles are the most commonly affected sites while involvement of the testis is very rare. The isolated epididymo-orchitis is an unusual presentation of tuberculosis and may produce diagnostic difficulty while excluding a possible testicular neoplasm2. We present a case of isolated epididymo-orchitis with scrotal involvement due to tuberculosis with no evidence of tuberculous foci elsewhere in the body. Case report A 18 year male, nonsmoker, farmer presented with complaints of pain and ulcer in scrotum. He had small nodular swelling on the left scrotal wall six weeks earlier, which subsequently enlarged and ruptured. These were followed by increase in pain and diffuse swelling of the left scrotum. There were no other constitutional or systemic symptoms. He denied dysuria, frequency, urgency of micturition and history of any sexually transmitted or urological disease. His past medical history was also negative. On examination an ulcerative wound over left scrotum 4x4 cms in size fixed to testis, with undermined edges was found. There was diffuse swelling of the left sided scrotum with left thickened
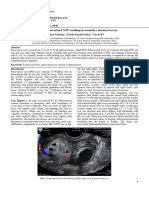
cord. The right testis was normal on examination (fig-1). The systemic examination was essentially normal. Investigations revealed haemoglobin 10.0 gm%, total leucocytes count 5,900/mm3, differential count polymorphs 58%, lymphocytes 40%, eosinophils 1%, basophils 1%, ESR 15 mm after one hour, fasting blood sugar 94 mg% and normal urine examination on routine and microscopic evaluation. VDRL and HIV were seronegative. FNAC suggested tuberculous orchitis with tuberculous granulomatous lesion. To find out tuberculous lesions elsewhere in the body, patient was investigated by skiagram chest, sputum examination for AFB, ultrasonography of abdomen, intravenous urography, urine smear and culture for Mycobacterium tuberculosis etc. but none of these tests revealed positive results. Anti-tuberculous treatment with Isoniazid 300mg, Rifampicin 450mg, Ethambutol 1000mg and Pyrazinamide 1500mg was started as directly observed therapy (Category I). The swelling disappeared within four weeks and ulcer healed subsequently.
Correspondence Prof A K Khanna Department of General Surgery Institute of Medical Sciences, Banaras Hindu University, Varanasi, U.P.-221005, India Email: akk_dr@sify.com
98
Fig. 1: pre-treatment clinical photograph
Fig. 2: post-treatment (after 1month) clinical photograph
Discussion Genital tuberculosis is usually a disease of sexually active males and most commonly occurs between the ages of 20 and 40 years, although it has been reported in children also. Extra-genital involvement including pulmonary and renal tuberculosis can be documented in 50 % and 80 to 85 % respectively of the patients with genital tuberculosis. The spread of tuberculosis to the epididymis is thought to occur haematogenously or by retrocanalicular descent of organisms from the haematogenously infected prostate. Distal spread through the genitourinary tract from a renal source also may occur. A rare possibility of female to male transmission (veneral transmission of tuberculosis) has also been suggested. Testicular involvement is usually as a result of local invasion from the epididymis, retrograde seeding from the epididymis and rarely by haematogenous spread2. The involvement of scrotal wall in our case suggests local extratesticular extension of disease process. Genital tuberculosis commonly presents as unilateral scrotal swelling, pain, discharging sinuses. The presence of abscess or sinus formation indicates advanced widespread scrotal disease. The most characteristic feature is its edge which is thin, reddish blue and undermined. There is pale granulation tissue with scanty serosanguineous discharge in the floor and slight induration at the base which indicates that this ulcer is a chronic one. The urinary symptoms and sterile pyuria strongly suggest associated renal involvement which was not evident in our case. High resolution sonography is currently the best technique for imaging the scrotum and its contents4. Tuberculous epididymo-orchitis has considerable effect on the fertility. The sperm counts and motility
may be reduced due to blockage of the vas and/or secondary atrophy3. Our case demonstrates unusual presentation of genital tuberculosis with no evidence of associated pulmonary or renal tuberculosis, bilateral involvement of epididymis, diffuse involvement of left testis with ulceration of the scrotum. Tuberculous epididymo-orchitis must be considered in the differential diagnosis of a scrotal swelling apart from testicular tumour, acute infection and inflammatory orchitis5. All attempts must be made for early diagnosis and treatment of this condition to avoid unnecessary epididymectomy and effect on fertility. References 1. Rosenberg S. Has chemotherapy reduced the incidence of genitourinary tuberculosis: A comparison based on necropsy material from Bellevue Hospital. J Urol 1963; 90: 317. 2. Hetal Shah Isolated Tuberculous Epididymo-Orchitis. Indian J Tuberc 2004; 51:159-62. 3. Gorse GJ, Belshe RB. Male genital tuberculosis: a review of the literature with instructive case reports. Rev Infect Dis 1985; 7: 511-2. 4. Chung JJ, Kim MJ, Lee T, et al. Sonographic findings in Tuberculous epididymitis and epididymo-orchitis. J Clin Ultrasound 1997; 25: 390-4. 5. Kundu S, Sengupta A, Dey A, Thakur SB. Testicular tuberculosis mimicking testicular malignancy. J Indian Med Assoc. 2004 May; 102(5):270.
99
You might also like
- Unusual Case of Tuberculous Pleural Effusion and Abdominal MassDocument4 pagesUnusual Case of Tuberculous Pleural Effusion and Abdominal MassRofi IrmanNo ratings yet
- Case Report Prostate Tuberculosis-RD - 1-1Document6 pagesCase Report Prostate Tuberculosis-RD - 1-1GemiNo ratings yet
- 13 - Case Report - 5 (OK Final) Tuberculosis of Cervix - A Rare Clinical EntityDocument3 pages13 - Case Report - 5 (OK Final) Tuberculosis of Cervix - A Rare Clinical EntityAnisa Prima Justica MustikyantoroNo ratings yet
- Delay in Diagnosis of Extra-Pulmonary Tuberculosis by Its Rare Manifestations: A Case ReportDocument5 pagesDelay in Diagnosis of Extra-Pulmonary Tuberculosis by Its Rare Manifestations: A Case ReportSneeze LouderNo ratings yet
- Chapter-47 - Genitourinary Tuberculosis in MaleDocument7 pagesChapter-47 - Genitourinary Tuberculosis in MalemanaNo ratings yet
- Female Genital Tuberculosis-PatelDocument37 pagesFemale Genital Tuberculosis-PatelLionel BaniquedNo ratings yet
- 44 Danfulani EtalDocument3 pages44 Danfulani EtaleditorijmrhsNo ratings yet
- Jurnal UrolithiasisDocument6 pagesJurnal UrolithiasisAliimah KhairiyahNo ratings yet
- Gonorrhoeae in East-European Countries: Guidelines For Laboratory Diagnosis of NeisseriaDocument10 pagesGonorrhoeae in East-European Countries: Guidelines For Laboratory Diagnosis of NeisseriaGunay AliyevaNo ratings yet
- 1-S2.0-S1726490112000895-Main Baru - En.idDocument5 pages1-S2.0-S1726490112000895-Main Baru - En.idHenandwita Fadilla PravitasariNo ratings yet
- Jurnal 7 PulmoDocument7 pagesJurnal 7 Pulmomisra lailaNo ratings yet
- Clinical Predictors of Ileocecal Tuberculosis: A Case SeriesDocument14 pagesClinical Predictors of Ileocecal Tuberculosis: A Case SeriesChristopher AsisNo ratings yet
- A Clinical Study of Generalised Peritonitis and ItDocument9 pagesA Clinical Study of Generalised Peritonitis and ItafifahNo ratings yet
- Osteomyelitis DG HivDocument4 pagesOsteomyelitis DG HivLiina Lo Ne Ly IINo ratings yet
- Squamous Cell Carcinoma of the Anal Canal: Causes, Diagnosis and TreatmentDocument12 pagesSquamous Cell Carcinoma of the Anal Canal: Causes, Diagnosis and TreatmentGabriela Zavaleta CamachoNo ratings yet
- Sterile PyuriaDocument7 pagesSterile PyuriaLuiggi D. Chambi MaidaNo ratings yet
- 1 s2.0 S0302283822026252 MainDocument6 pages1 s2.0 S0302283822026252 MainjuanmisqjNo ratings yet
- Women Genital Tuberculosis: A Study of Two Cases at Mohammed Vi University Hospital in MarrakechDocument5 pagesWomen Genital Tuberculosis: A Study of Two Cases at Mohammed Vi University Hospital in MarrakechIJAR JOURNALNo ratings yet
- 2006 Etiologies of Nongonococcal Urethritis. Bacteria, Viruses, and The Association With Orogenital ExposureDocument10 pages2006 Etiologies of Nongonococcal Urethritis. Bacteria, Viruses, and The Association With Orogenital Exposurebiocbc08No ratings yet
- Management of The Urologic Sepsis SyndromeDocument10 pagesManagement of The Urologic Sepsis SyndromeNur Syamsiah MNo ratings yet
- Case Report: A Case Report of Peritoneal Tuberculosis: A Challenging DiagnosisDocument4 pagesCase Report: A Case Report of Peritoneal Tuberculosis: A Challenging DiagnosisDumitru RadulescuNo ratings yet
- Filaria PDFDocument3 pagesFilaria PDFArdanta Dat Topik TariganNo ratings yet
- Uretritis GonoreDocument16 pagesUretritis GonoreUswatun HasanahNo ratings yet
- ArchIntSurg Adult IntuDocument5 pagesArchIntSurg Adult IntusinghalbmNo ratings yet
- Chapter-48 - Genitourinary Tuberculosis in FemaleDocument7 pagesChapter-48 - Genitourinary Tuberculosis in FemalemanaNo ratings yet
- Bacterial Uropathogenic Factors & Host DefensesDocument7 pagesBacterial Uropathogenic Factors & Host DefensesAtma AdiatmaNo ratings yet
- Tuberculosis of The Urogenital TractDocument3 pagesTuberculosis of The Urogenital TractIan HuangNo ratings yet
- Ou Sumber4Document14 pagesOu Sumber4AnggaNo ratings yet
- 2 5 21 861 PDFDocument3 pages2 5 21 861 PDFAhmed ZidanNo ratings yet
- True Hermaphroditism With Seminoma, Case ReportDocument4 pagesTrue Hermaphroditism With Seminoma, Case ReportJesahias Trejo MartínezNo ratings yet
- 16 3 2010 0350 0351 PDFDocument2 pages16 3 2010 0350 0351 PDFSandi ApriadiNo ratings yet
- Ijahs Vol 1 Issue 4 4Document5 pagesIjahs Vol 1 Issue 4 4A A Ngurah Wisnu Adiputra CNo ratings yet
- Spontaneous Perforated Pyometra With An Intrauterine Device in Menopause: A Case ReportDocument2 pagesSpontaneous Perforated Pyometra With An Intrauterine Device in Menopause: A Case ReportTomy SaputraNo ratings yet
- doi- 10.1111:j.1525-1438.2006.00209.x.Document6 pagesdoi- 10.1111:j.1525-1438.2006.00209.x.Sulaeman Andrianto SusiloNo ratings yet
- Usg PidDocument13 pagesUsg PidHisbulloh syarifNo ratings yet
- GTI InfectionsDocument13 pagesGTI InfectionsFrancis GacheruNo ratings yet
- AMasculine PresentingFemaleAdolescentaRareCaseofPoorly DifferentiatedSertoli LeydigCellTumorDocument15 pagesAMasculine PresentingFemaleAdolescentaRareCaseofPoorly DifferentiatedSertoli LeydigCellTumorDaniella Ashley BaltesNo ratings yet
- Krukenberg Tumour Simulating Uterine Fibroids and Pelvic Inflammatory DiseaseDocument3 pagesKrukenberg Tumour Simulating Uterine Fibroids and Pelvic Inflammatory DiseaseradianrendratukanNo ratings yet
- Review of The Journal Enterobius Vermicularis in Tubo-Ovarian Abscess: A Rare and Interesting Incidental Finding-A Case ReportDocument2 pagesReview of The Journal Enterobius Vermicularis in Tubo-Ovarian Abscess: A Rare and Interesting Incidental Finding-A Case ReportalfikaNo ratings yet
- International Archives of Urology and Complications Iauc 8 086Document6 pagesInternational Archives of Urology and Complications Iauc 8 086Ikhsan PrialaksanaNo ratings yet
- Is Surveillance Necessary For Inverted Papilloma in The Urinary Bladder and Urethra?Document5 pagesIs Surveillance Necessary For Inverted Papilloma in The Urinary Bladder and Urethra?Денис КрахоткинNo ratings yet
- Tuberculous Lymphadenopathy Diagnosis and Treatment ReviewDocument6 pagesTuberculous Lymphadenopathy Diagnosis and Treatment ReviewAnonymous OktIZHNo ratings yet
- Ovarian TorsionDocument4 pagesOvarian TorsionRiko KuswaraNo ratings yet
- Primary Umbilical Endometriosis. Case Report and Discussion On Management OptionsDocument7 pagesPrimary Umbilical Endometriosis. Case Report and Discussion On Management Optionsari naNo ratings yet
- Iaat 12 I 9 P 187Document8 pagesIaat 12 I 9 P 187Maniak LuckNo ratings yet
- A Rare Germ-Cell Tumor Site: Vaginal Endodermal Sinus Tumor: CasereportDocument3 pagesA Rare Germ-Cell Tumor Site: Vaginal Endodermal Sinus Tumor: CasereportmonicamoniccNo ratings yet
- Prostatitis PDFDocument3 pagesProstatitis PDFWidya PuspitaNo ratings yet
- Case ReportDocument3 pagesCase Reportyena hillNo ratings yet
- Case StudiesDocument6 pagesCase StudiesPatricia CruzNo ratings yet
- Manajemen UTI Pada ElderlyDocument4 pagesManajemen UTI Pada ElderlyTrismi IstianaNo ratings yet
- Rare Primary Tuberculosis in TonsilsDocument3 pagesRare Primary Tuberculosis in Tonsilsmanish agrawalNo ratings yet
- Radiology Case Report - Splenic AbscessDocument6 pagesRadiology Case Report - Splenic AbscessAbeebNo ratings yet
- Pancreatic Tuberculosis Diagnosis UpdateDocument24 pagesPancreatic Tuberculosis Diagnosis UpdatesamudraandiNo ratings yet
- Renal Disease in TuberculosisDocument10 pagesRenal Disease in TuberculosismiguelNo ratings yet
- Hiller 2015Document7 pagesHiller 2015Muhamad Ilhamsyah DandungNo ratings yet
- Case 16-2014: A 46-Year-Old Woman in Botswana With Postcoital BleedingDocument10 pagesCase 16-2014: A 46-Year-Old Woman in Botswana With Postcoital BleedingDesi HutapeaNo ratings yet
- International Journal of Pharmaceutical Science Invention (IJPSI)Document3 pagesInternational Journal of Pharmaceutical Science Invention (IJPSI)inventionjournalsNo ratings yet
- Art09 PDFDocument7 pagesArt09 PDFJulio BarrantesNo ratings yet
- Clinical Images: A Quarterly ColumnDocument3 pagesClinical Images: A Quarterly ColumnAustine OsaweNo ratings yet
- Guide to Pediatric Urology and Surgery in Clinical PracticeFrom EverandGuide to Pediatric Urology and Surgery in Clinical PracticeNo ratings yet
- SAWFCC Micro Teaching PDFDocument34 pagesSAWFCC Micro Teaching PDFdipjsamNo ratings yet
- Group-Work - Disaster - ManagementDocument35 pagesGroup-Work - Disaster - Managementntambik21No ratings yet
- 4mgdskmlswg6dvazveij Signature Poli 150701080131 Lva1 App6892 PDFDocument42 pages4mgdskmlswg6dvazveij Signature Poli 150701080131 Lva1 App6892 PDFsaurabh chaturvediNo ratings yet
- Chison ECO1 CatalogueDocument3 pagesChison ECO1 Cataloguentambik21No ratings yet
- Machine Learning Intro: Prob, Density Est, PerceptronsDocument271 pagesMachine Learning Intro: Prob, Density Est, Perceptronssri1991nivasNo ratings yet
- Blooms Taxononmy (Autosaved)Document26 pagesBlooms Taxononmy (Autosaved)ntambik21No ratings yet
- Foundations or Determinants of A CurriculumDocument86 pagesFoundations or Determinants of A Curriculumntambik21No ratings yet
- Pharmacist - ResumeDocument2 pagesPharmacist - Resumentambik21No ratings yet
- Useful Mathematical & Physical FormulaeDocument35 pagesUseful Mathematical & Physical Formulaentambik21No ratings yet
- Mindray DP6600Document113 pagesMindray DP6600ntambik21No ratings yet
- D AND C SET - #98-1014: Number Description QtyDocument1 pageD AND C SET - #98-1014: Number Description Qtyntambik21No ratings yet
- Stages of ImplantationDocument5 pagesStages of Implantationntambik21No ratings yet
- ABCAUS Help FileDocument7 pagesABCAUS Help Filentambik21No ratings yet
- C.D.H.L Progress Report 2014Document5 pagesC.D.H.L Progress Report 2014ntambik21No ratings yet
- Tea Cup Reading and FortuneDocument4 pagesTea Cup Reading and Fortunentambik21No ratings yet
- Atlas of OceansDocument257 pagesAtlas of Oceansntambik2192% (12)
- Uganda Dental ReportDocument44 pagesUganda Dental Reportntambik21No ratings yet
- DentalDocument2 pagesDentalntambik210% (1)
- Handbook of Goat FarmingDocument25 pagesHandbook of Goat FarmingZubair Ali Bhutto100% (2)
- Handbook of Goat FarmingDocument25 pagesHandbook of Goat FarmingZubair Ali Bhutto100% (2)
- HerniationDocument8 pagesHerniationntambik21No ratings yet
- Renal ScintigraphyDocument6 pagesRenal Scintigraphyntambik21No ratings yet
- Nursing Satisfaction AnecoDocument34 pagesNursing Satisfaction Anecontambik21No ratings yet
- Clark S Positioning in Radiography 12th EditionDocument532 pagesClark S Positioning in Radiography 12th EditionWisdom Patrick Enang95% (63)
- Atlas of OceansDocument257 pagesAtlas of Oceansntambik2192% (12)
- ABCAUS Help FileDocument7 pagesABCAUS Help Filentambik21No ratings yet
- Proper Circumcision Techniques for Infants and AdultsDocument6 pagesProper Circumcision Techniques for Infants and Adultsntambik21No ratings yet
- MantouxDocument1 pageMantouxntambik21No ratings yet
- Ivory CoastDocument1 pageIvory Coastntambik21No ratings yet
- CaseDocument3 pagesCasebLessy_july16No ratings yet
- Fever in The Neurointensive Care UnitDocument9 pagesFever in The Neurointensive Care UnitDiayanti TentiNo ratings yet
- Hepatitis A VaccineDocument5 pagesHepatitis A VaccineHåíthãm KhãtïßNo ratings yet
- Skin Hydrating and Whitening Effects of Vitamin C and Glutathione in Asian Skin Types - PRIME JournalDocument9 pagesSkin Hydrating and Whitening Effects of Vitamin C and Glutathione in Asian Skin Types - PRIME JournalNovia SaragihNo ratings yet
- The many benefits of music. Listening to and creating music helps children learn numeracy, literacy and emotional skillsDocument5 pagesThe many benefits of music. Listening to and creating music helps children learn numeracy, literacy and emotional skillsHarold JimenezNo ratings yet
- Psychological Aspects of Rehabilitation in Cases of Brain Injury (Zangwill, 1947)Document10 pagesPsychological Aspects of Rehabilitation in Cases of Brain Injury (Zangwill, 1947)Cyberterton4No ratings yet
- CP PPTDocument58 pagesCP PPTKatherine 'Chingboo' Leonico LaudNo ratings yet
- Johanes Hardjono: Problematik Fisioterapi Dan Diagnose FisioterapiDocument30 pagesJohanes Hardjono: Problematik Fisioterapi Dan Diagnose FisioterapisulaimanNo ratings yet
- Bronchitis: Kelompok IDocument14 pagesBronchitis: Kelompok ILinda Permata Sari100% (1)
- Brief Strategic Family TherapyDocument12 pagesBrief Strategic Family Therapymichelle458No ratings yet
- Dossier RPG EnglishDocument15 pagesDossier RPG EnglishtetevoNo ratings yet
- Presentation On StressDocument31 pagesPresentation On StressDr. Smita Choudhary100% (1)
- LIST OF REGISTERED DRUGS DECEMBER 2012Document18 pagesLIST OF REGISTERED DRUGS DECEMBER 2012Benjamin Tantiansu100% (1)
- 2018 07 04 UpToDate - Anemia in Pregnancy (18157)Document20 pages2018 07 04 UpToDate - Anemia in Pregnancy (18157)Kharisma RosaNo ratings yet
- Tranquil Eyes Kit User ManualDocument27 pagesTranquil Eyes Kit User ManualJj TreyNo ratings yet
- Phenergan (Promethazine)Document1 pagePhenergan (Promethazine)E100% (1)
- Brexpiprazole: A Review of A New Treatment Option For Schizophrenia and Major Depressive DisorderDocument6 pagesBrexpiprazole: A Review of A New Treatment Option For Schizophrenia and Major Depressive DisorderLuis Pablo HsNo ratings yet
- Labor and Delivery QuizDocument7 pagesLabor and Delivery QuizAmy50% (2)
- Model Curriculum Handbook RadiotDocument157 pagesModel Curriculum Handbook RadiotYuda FhunkshyangNo ratings yet
- Risk Management Sample PlanDocument13 pagesRisk Management Sample PlanSARAH JOY JAGNA-ANNo ratings yet
- 7 Simple Yoga Stretches To Soothe Sciatica Back Pai1Document31 pages7 Simple Yoga Stretches To Soothe Sciatica Back Pai1Nemanja Peric100% (1)
- Art Therapy AssessmentDocument7 pagesArt Therapy Assessmentreighn_21100% (4)
- Management of Medically Compromised PatientsDocument70 pagesManagement of Medically Compromised PatientsPriyanka WadhawanNo ratings yet
- CTG classification 2015 FIGO guidelines fetal monitoringDocument1 pageCTG classification 2015 FIGO guidelines fetal monitoringHerry SasukeNo ratings yet
- CDC guidelines for treating syphilisDocument27 pagesCDC guidelines for treating syphilisGabrielaGushikenNo ratings yet
- Cyclosporine PharmaDocument2 pagesCyclosporine PharmaflagaacNo ratings yet
- Stress Management at Workplace Through SpiritualityDocument84 pagesStress Management at Workplace Through SpiritualityKiran Sakroji100% (3)
- MRK - Spring 2019 - PSYI619 - 8 - MC170401426Document42 pagesMRK - Spring 2019 - PSYI619 - 8 - MC170401426Amara AhmadNo ratings yet
- Health Guard Customer Information Sheet: Bajaj Allianz General Insurance Company LimitedDocument3 pagesHealth Guard Customer Information Sheet: Bajaj Allianz General Insurance Company LimitedKumud GandhiNo ratings yet
- Komunikasi Profesional dalam KeperawatanDocument100 pagesKomunikasi Profesional dalam KeperawatanyaminmuhNo ratings yet