Professional Documents
Culture Documents
Visual Disturbances
Uploaded by
Bobbie Sison0 ratings0% found this document useful (0 votes)
30 views15 pagesCataracts can develop in one or both eyes at any age Ior a variety oI causes. The extent oI visual impairment depends on the size, density, and location in the lens. People with the highest levels oI sunlight exposure have twice the risk oI developing cortical cataracts than those with low-level sunlight exposure.
Original Description:
Copyright
© Attribution Non-Commercial (BY-NC)
Available Formats
DOCX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCataracts can develop in one or both eyes at any age Ior a variety oI causes. The extent oI visual impairment depends on the size, density, and location in the lens. People with the highest levels oI sunlight exposure have twice the risk oI developing cortical cataracts than those with low-level sunlight exposure.
Copyright:
Attribution Non-Commercial (BY-NC)
Available Formats
Download as DOCX, PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
30 views15 pagesVisual Disturbances
Uploaded by
Bobbie SisonCataracts can develop in one or both eyes at any age Ior a variety oI causes. The extent oI visual impairment depends on the size, density, and location in the lens. People with the highest levels oI sunlight exposure have twice the risk oI developing cortical cataracts than those with low-level sunlight exposure.
Copyright:
Attribution Non-Commercial (BY-NC)
Available Formats
Download as DOCX, PDF, TXT or read online from Scribd
You are on page 1of 15
MANILA TYTANA COLLEGES
Manila Doctors College of Nursing
President Diosdado Macapagal Boulevard, Metropolitan Park
Pasay City
Passed by:
Leader: Teologo, Marilyn A.
Members: Santos, Cienna Mae S.
Sison, Bobbie Jo
Santos, Maryrose B.
Sison, Robert Joseph
Group 9
Passed to:
Dr. Romyr Cajucom
CA2 ProIessor
'ISUAL DISTURBANCES
I. CATARACT
DEFINITION:
CATARACTS - a lens opacity or cloudiness; cataract is the leading cause oI blindness in the
world (World Health Organization,).
PATHOPHYSIOLOGY:
O Cataracts can develop in one or both eyes at any age Ior a variety oI causes
O The extent oI visual impairment depends on the size, density, and location in the
lens
O More than one type can be present in one eye.
The three most common types oI senile (age-related) cataracts are deIined by their location in the
lens:
1. Nuclear
2. cortical
3. posterior subcapsular.
1. A nuclear cataract
O associated with myopia (ie, nearsightedness),
O the cataract severely blurs vision.
O Periodic changes in prescription eyeglasses help manage this problem.
2. A cortical cataract
O involves the anterior, posterior, or equatorial cortex oI the lens
O 'ision is worse in very bright light.
O Studies show that people with the highest levels oI sunlight exposure have
twice the risk oI developing cortical cataracts than those with low-level
sunlight exposure (West et al., 1998).
3. Posterior subcapsular cataracts
O occur in Iront oI the posteriorcapsule.
O typically develops in younger people and, in some cases, is associated
with prolonged corticosteroid use, inIlammation, or trauma.
O Near vision is diminished, and the eye is increasingly sensitive to glare
Irom bright light (eg, sunlight,headlights).
CLINICAL MANIFESTATIONS
O Painless, blurry vision is characteristic oI cataracts
O Other eIIects include myopic shiIt, astigmatism,monocular diplopia (ie,
double vision), color shiIt (ie, the aginglens becomes progressively more
absorbent at the blue end oI thespectrum), brunescens (ie, color values
shiIt to yellow-brown),and reduced light transmission.
ASSESSMENT AND DIAGNOSTIC FINDINGS
1.The Snellen visual acuity test
2. Ophthalmoscopy
3. Slitlamp biomicroscopic examination
O used to establish the degree oI cataract Iormation.
O The degree oI lens opacity does not always ncorrelate with the patient`s Iunctional
status.
O Others with less lens opaciIication have a disproportionate decrease in visual
acuity; hence, visual acuity is an imperIect measure oI visual impairment.
MEDICAL MANAGEMENT
O No nonsurgical treatment cures cataracts.
O Ongoing studies are investigating ways to slow cataract progression:
O intake oI antioxidants (eg, vitamin C, beta-carotene, vitamin E) (Age-Related Eye
Disease Research Study Group, 2001).
O n the early stages oI cataract development, glasses, contact lenses, strong
biIocals, or magniIying lenses may improve vision.
O Reducing glare with proper light and appropriate lighting can Iacilitate reading.
O Mydriatics can be used as short-term treatment to dilate the pupil.
SURGICAL MANAGEMENT
O Surgery is perIormed on an outpatient basis and usually takes less than 1 hour,
with the patient being discharged in 30 minutes or less aIterward.
O Restoration oI visual Iunction through a saIe and minimally invasive procedure is
the surgical goal
O which is achieved:
1. topical anesthesia
applied to the surIace oI the eye, eliminates the hazards oI regional
anesthesia, such as ocular perIoration, retrobulbar hemorrhage, optic
injuries, diplopia, and ptosis
ideal Ior patients receiving anticoagulants.
2. smaller wound incision (ie, clear cornea incision)
3. lens design (ie, Ioldable and more accurate intraocular lens measurements).
O When both eyes have cataracts:
one eye is treated Iirst, with at least several weeks, preIerably months,
separating the two operations.
1. Intracapsular Cataract Extraction.
The entire lens (ie, nucleus, cortex, and capsule) is removed, and Iine sutures
close the incision.
ndicated when there is a need to remove the entire lens, such as with a subluxated
cataract (ie, partially or completely dislocated lens).
2. Extracapsular Surgery.
achieves the intactness oI smaller incisional wounds (less trauma to the eye) and
maintenance oI the posterior capsule oI the lens, reducing
postoperative complications, particularly aphakic retinal detachment
and cystoid macular edema.
n ECCE, a portion oI the anterior capsule is removed, allowing extraction oI the
lens nucleus and cortex. The posterior capsule and zonular support are
leIt intact.
An intact zonular-capsular diaphragm provides the needed saIe anchor Ior the
posterior chamber intraocular lens (OL).
a viscoelastic substance (clear gel) is injected into the space between the cornea
and the lens.
This prevents the space Irom collapsing and Iacilitates insertion oI the OL.
. Phacoemulsification
&ses an ultrasonic device that liqueIies the nucleus and cortex, which are then
suctioned out through a tube.
The posterior capsule is leIt intact
wound heals more rapidly, and there is early stabilization oI reIractive error and
less astigmatism.
. Lens Replacement.
AIter removal oI the crystalline lens, the patient is reIerred to as ,5,.(ie,
without lens).
The lens, which Iocuses light on the retina, must be replaced Ior the patient to see
clearly.
three lens replacement options:
1. aphakic eyeglasses
eIIective but heavy
Objects are magniIied by 25, making them appear closer
than they actually are.
Objects are magniIied unequally, creating distortion.
Peripheral vision is also limited
binocular vision is impossible iI the other eye is phakic
(normal).
2. contact lenses
provide patients with almost normal vision
contact lenses need to be removed occasionally, the patient
also needs a pair oI aphakic glasses
not advised Ior patients who have diIIiculty inserting,
removing, and cleaning them
requent handling and improper disinIection increase the
risk Ior inIection.
3. OL implants.
the usual approach to lens replacement
AIter CCE, the surgeon implants an anterior chamber
OL in Iront oI the iris.
Posterior chamber lenses, generally used in ECCE, are
implanted behind the iris
contraindicated in patients with recurrent uveitis
proliIerative diabetic, retinopathy, neovascular
glaucoma, or rubeosis iridis
NURSING MANAGEMENT
1. PRO'DNG PREOPERAT'E CARE
anticoagulation therapy is withheld
Aspirin should be withheld Ior 5 to 7 days, nonsteroidal
anti-inIlammatory medications (NSADs) Ior 3 to 5 days
warIarin (Coumadin) until the prothrombin time oI 1.5 is almost reached.
Dilating drops are administered
10 minutes Ior Iour doses at least 1 hour beIore surgery.
Additional dilating drops may be administered in the operating
room (immediately beIore surgery)
iI the aIIected eye is not Iully dilated. Antibiotic, corticosteroid,
and NSAD drops may be administered prophylactically
2. PRO'DNG POSTOPERAT'E CARE
4 the patient receives verbal and written instruction regarding how to protect the
eye, administer medications, recognize signs oI complications, and obtain
emergency care
4 explains that there is minimal discomIort aIter surgery and instructs the patient to
take a mild analgesic agent, such as acetaminophen, as needed. Antibiotic, anti-
inIlammatory, and corticosteroid eye drops or ointments are prescribed
postoperatively
3. PROMOTNG HOME AND COMM&NTY-BASED CARE
4 Teaching Patients Self-Care.
4 patient wears a protective eye patch
4 To prevent accidental rubbing or poking oI the eye
4 Worn Ior 24 hours aIter surgery
4 Iollowed by eyeglasses worn during the day
4 a metal shield worn at night Ior 1 to 4 weeks.
4 The nurse instructs the patient and Iamily in applying and caring
Ior the eye shield.
4 Sunglasses should be worn while outdoors during the day because
the eye is sensitive to light.
4 Slight morning discharge, some redness, and a scratchy Ieeling
may be expected Ior a Iew days.
4 A clean, damp washcloth may be used to remove slight morning
eye discharge
4 the patient must know to notiIy the surgeon iI new Iloaters (ie,
dots) in vision, Ilashing lights, decrease in vision, pain, or increase
in redness occurs.
4 Continuing Care.
O The eye patch is removed aIter the Iirst Iollowup appointment.
O Patients may experience blurring oI vision Ior several days to weeks.
O Sutures leIt in the eye alter the curvature oI the cornea, resulting in
temporary blurring and some astigmatism.
O 'ision gradually improves as the eye heals.
O Patients with OL implants have visual improvement Iaster than those
waiting Ior aphakic glasses or contact lenses.
O 'ision is stabilized when the eye is completely healed, usually within 6 to
12 weeks
O 'isual correction is needed Ior any remaining nearsightedness or
Iarsightedness (even in patients with OL implants).
II. GLAUCOMA
DEFINITION:
Glaucoma used to reIer to a group oI ocular conditions characterized by optic nerve damage.
Was seen more as a condition oI elevated OP than oI optic neuropathy.
Second leading cause oI blindness in &S.
More prevalent in people older than 40 years oI age and third most common age-related
eye disease in &S.
AIrican Americans~Caucasians
No cure but can be controlled
PATHOPHYSIOLOGY:
1.) Direct Mechanical Theory high OP damages retinal layer as it passes through the optic
nerve.
2.) Indirect Ischemic Theory high OP compresses the microcirculation in the optic nerve
head, resulting in cell injury and death.
DIAGNOSTIC FINDINGS:
Purpose: to establish diagnostic category, assess optic nerve damage and Iormulate treatment
plan.
MA1OR TYPES OF EXAMINATIONS:
1.) TONOMETRY used to measure OP
2.) OPHTHALMOSCOPY to inspect optic nerve
3.) GONOSCOPY to examine Iiltration angle oI the anterior chamber
4.) PERMETRY to assess visual Iields
MEDICAL MANAGEMENT:
Goal: to maintain OP within range unlikely to cause Iurther damage.
PHARMACOLOGIC THERAPY
O Ocular Medications: used to treat glaucoma
Medication Action Side Effects Nursing
Implications
CHOLINERGICS
(MIOTICS) -
pilocarpine, carbachol
ncrease aqueous
Iluid outIlow by
contracting the ciliary
muscle and causing
miosis (constriction
oI the pupil) and
opening o trabecular
meshwork
Periorbital pain,
blurry vision,
diIIiculty seeing the
dark
Caution patients about
diminished vision in
dimly lit areas
ADRENERGIC
AGONISTS -
dipiveIrin, epinephrine
Reduces production
oI aqueous humor and
increases outIlow
Eye redness and
burning; can have
systemic eIIects
including palpitations,
elevated blood
pressure, tremor,
headaches and anxiety
Teach patients punctal
occlusion to limit
systemic eIIects
BETA BLOCKERS -
betaxolol, timolol
Decreases aqueous
humor production
Can have systemic
eIIects including
bradycardia,
exacerbation oI
pulmonary disease
and hypotension
Contraindicated in
patients with asthma,
COPD, second or
third degree A'
block, bradycardia or
cardiac Iailure. Teach
patients punctal
occlusion to limit
systemic eIIects
ALPHA
2
-
AGONISTS -
apraclonidine,
brimonidine
Decreases aqueous
humor
Eye redness, dry
mouth and nasal
passages
Teach patients punctal
occlusion to limit
systemic eIIects
CARBONIC
ANHYDRASE
INHIBITORS -
acetazolamide,
methazolamide,
dorzolamide
Decreases aqueous
humor production
Oral medications
(acetazolamide and
methazolamide)
associated with
serious side eIIects
including
anaphylactic
reactions, electrolyte
loss, depression,
lethargy,
gastrointestinal upset,
impotence and weight
Do not administer to
patients with sulIa
allergies; monitor
electrolyte levels
loss; side eIIects oI
topical Iorm
(dorzolamide)
include topical allergy
PROSTAGLANDINS
- latanoprost,
bimatoprost
ncreases uveoscleral
outIlow
Darkening oI the iris,
conjunctival redness
and possible rash
&sed once a day and
do not aIIect pupil
size
SURGICAL MANAGEMENT
1.) Laser Trabeculoplasty - laser burns are applied to inner surIace oI trabecular meshwork to
open intrabecular spaces and widen canal oI Schlemm, promoting outIlow oI aqueous humor and
decrease OP.
COMPLCATON: transient elevated OP (2 hours aIter surgery) may become persistent
2.) Laser Iridotomy - Ior papillary block glaucoma, an opening is made in iris to eliminate
papillary block
CONTRANDCATON: patients with corneal edema which interIeres with laser targeting and
strength
POTENTAL COMPLCATONS: burns to cornea, lens or retina; transient elevated OP;
closure oI iridotomy; uveitis; blurring
Pilocarpine prescribed to prevent closure oI iridotomy
.) Filtering Procedures for Chronic Glaucoma - used to create an opening or Iistula in
trabecular meshwork to drain aqueous humor Irom the anterior chamber to subconjunctival space
into a bleb (Iluid collection on the outside oI the eye), bypassing usual drainage structures
Trabeculectomy standard Iiltering technique used to remove part oI trabecular meshwork
COMPLCATONS: hemorrhage, extremely low(hypotony) or extremely elevated OP, uveitis,
cataracts, bleb Iailure, bleb leak and endophthalmitis
.) Trabectome Surgery - Ior those patients whom pharmacologic treatment and laser
trabeculoplasty do not control OP; minimal invasive treatment; improve Iluid drainage Irom
eye to balance OP; to restore eye`s natural Iluid balance, this stabilizes optic nerve and
minimizes Iurther age; small incision and does not create permanent hole in the eye wall or
external Iiltering bleb or implant.
NURSING MANAGEMENT:
O Teaching patients self-care
4 nclude nature oI the disease and importance oI strict adherence to the medical
regimen in the teaching plan
Rationale: to help ensure compliance
4 Thoroughly discuss medical regimen, particularly interactions oI glaucoma-
control medications with other medications
4 Explain eIIects oI glaucoma-control medications on vision
RATONALE: patients need to be cautious in navigating surroundings
4 Discuss the inIormation about instilling ocular medications and prevent systemic
absorption with punctal occlusion
4 Assess Ior knowledge level and compliance with therapeutic regimen
O Patient Education: Managing Glaucoma
4 now OP measurement and desired range
4 nIorm about extent oI vision loss and optic nerve damage
4 Emphasize importance oI keeping a record oI eye pressure measurements and
visual Iield test results to monitor own progress
4 Encourage to have a review oI all medications whether it is over-the-counter or
herbal medicine with ophthalmologist and mention side eIIects upon visit
4 Ask about potential side eIIects and drug interactions oI eye medications
4 Ask whether generic or less costly Iorms oI eye medications are available
4 Encourage to review dosing schedule with ophthalmologist and inIorm him or her
iI troubled Iollowing the schedule
4 Encourage to participate in decision-making. Let the doctor know dosing schedule
that works Ior the patient and other preIerences about eye care
4 Allow the nurse to observe the patient to in instilling eye medications to
determine whether patient administers it properly
4 Have an awareness about glaucoma medications that can cause adverse eIIects iI
used inappropriate eye drops ( administered as prescribed not when eyes are
irritated)
4 nstruct to ask the ophthalmologist to send report to doctor aIter each appointment
4 Emphasize the need oI a Iollow up check up
O Continuing care
4 Patients with severe glaucoma and impaired Iunction reIer to services that assist
patient in perIorming ADLs, loss oI vision impairs mobility
4 ReIer Ior low vision and rehabilitation services
4 Patients with legal blindness oIIer reIerrals to agencies to obtain Iederal
assistance
4 Reassurance and emotional support
4 amily members are encouraged to undergo examinations at least once every 2
years to detect glaucoma early
III. RETINAL DETACHMENT
DEFINITION:
t is deIined as the separation oI the retinal pigment epithelium (RPE)
There are Iour ways that it may become separated
4 Rhegmatogenous detachment
The most common Iorm
A hole or tear develops in the sensory retina, allowing some oI the liquid
vitreous to seep through the sensory retina and detach it Irom the RPE
People at risk would be those people with
O high myopia or aphakia aIter cataract surgery
O recent trauma
5-10 oI all rhematogenous retinal detachments are associated with
proliIerative retinopathy (a retinopathy related with diabetic
neovascularization)
4 Traction
Tension or pulling Iorce is responsible Ior traction retinal detachment
An ophthalmologist must ascertain all oI the areas oI retinal break and
identiIy and release the scars or bands oI Iibrous material providing
traction on the retina
Generally, patients with this condition have developed Iibrous tissue Irom
conditions such as:
O diabetic retinopathy
O vitreous hemorrhage
O retinopathy oI prematurity
hemorrhages and Iibrous proliIeration associated with these conditions
exert a pulling Iorce on the delicate retina
4 A combination oI both Rhegmatogenous and Traction detachment
Some cases detachment was caused both by rhegmatogenous and traction
detachment
4 Exudative
the result oI the production oI a serous Iluid under the retina Irom the
choroid
conditions such as uveitis and macular degeneration may cause the
production oI this serous Iluid
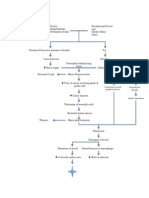
PATHOPHYSIOLOGY
Rhegmatogenous detachment
A break or tear in the retina usually
due to retinal atrophy
luid Irom vitreal space Ilows into the subretinal
space between the retina and RPE
The Iluid causes the retina to slowly to
detach Irom the RPE resulting
in Rhegmatogenous detachment
Traction
ormation oI Iibrous materials due to an
injury, inIlammation or neovascularisation
ibrous proliIeration along with possible
hemorrhages causes a pulling Iorce on the retina
Over time the pulling Iorce detaches the retina Irom RPE
A combination oI both Rhegmatogenous and Traction detachment
Tension Retinal Detachment starts to occur
This starts to cause hemorrhaging in the
RPE which results in rhegmatogenous
Both conditions then help contribute to the
detachment oI the retina Irom the RPE
Exudative
nIlammation, injury or vascular abnormalities
that results in Iluid accumulating underneath
the retina without the presence oI a hole, tear, or break
The presence oI this Iluid causes pressure in the eye
which then over time separates the retina Irom the RPE
CLINICAL MANIFESTATIONS
This may include verbalization Irom the patient that there is:
a sensation oI a shade or curtain coming across the vision oI one eye
a presence oI cobwebs within their vision
bright Ilashing lights
The sudden onset oI a great number oI 'Iloaters
4 Small particles in the eye that are perceived as small Iibers Iloating in the air
DIAGNOSTIC TESTS
Dilated Iundus examination
4 AIter visual acuity is determined the patient must undergo a dilated Iundus
examination
4 &ses an indirect opthalmosccope as well as a slit-lamp biomicroscopy
4 Stereo Iundus photography and Iluorescein angiography are also commonly used
during this examination
4 Mydriatic Eye Drops are used in order to dilate the pupil, so that (with the help oI
the equipment stated) a better view oI the Iundus can be obtained
Optical coherence tomography and ultrasound
4 Are used Ior the complete retinal assessment
4 Especially used when the view is obscured by a dense cataract or vitreal
hemorrhage
4 Through this all retinal breaks, all Iibrous bands that may be causing traction on
the retina, and all degenerative changes must be identiIied
MEDICAL MANAGEMENT
n detachment, an attempt is made to surgically reattach the sensory retina to the RP
n traction detachment, the source oI traction must be removed and the sensory retina can
then be reattached
The most commonly used surgical interventions include the:
4 Scleral buckle
The retinal surgeon compresses the sclera to indent the scleral walls Irom
the outside oI the wall Irom the outside oI the eye and bring th two retinal
layers in contact with each other
Has a high success rate iI done by an experienced retinal surgeons
Some risks include diplopia, myopia and increased postoperative pain
4 Pars Plana 'itrectomy
A vitrectomy is an intraocular procedure in which 1mm to 4mm incisions
are made at the pars plana
One incision allows the introduction oI a light source while another
incision serves as the portal Ior the vitrectomy instrument
The surgeon then dissects preretinal membranes under direct visualization
while the retina is stabilized by an intraoperative vitreous substitute
'itrectomy can also be used in the removal oI Ioreign bodies, vitreous
opacities such as blood, and dislocated lenses
'itrectomy can be combined scleral buckling to repair retinal breaks
Treatment oI macular holes includes citrectomy, laser photocoagulation,
air-Iluid-gas exchanges and the use oI the growth Iactor.
4 Pneumatic Retinopexy
This technique is used Ior the repair oI a rhegmatogenous retinal
detachment.
s is the least invasive oI the three procedures mentioned
The vitreous Iluid is Iirst drained
A gas bubble, silicone oil, or perIluoro-carbons and liquids is then injected
into the vitreous cavity to help push the sensory retina up against the RPE
Post operational position is critical, due to the need that the injected
bubble must Iloat into a position overlying the area oI detachment, so that
a consistent pressure is provided to reattach the sensory retina
Argon laser photocoagulation or cryotherapy is also used to 'spot-weld
small holes
NURSING INTER'ENTIONS
Promote ComIort
4 I a gas tomponade is used to Ilatten the retina, the patient may have to specially
positioned to make the gas bubble Iloat into the best position
4 Some patients must lie Iace down or on their side Ior days
Teaching about complications
4 n many cases, vitreoretinal procedures are perIormed on an outpatient basis, and
the patient is seen the next day Ior a Iollow-up examination and closely monitored
thereaIter as required
4 Postoperative complications may include increased:
nceased op
Endophthalmitis
Development oI other retinal detachments
Development oI cataracts
Loss oI turgor oI the eye
4 Patients must be taught the signs oI symptoms oI complications, with an emphasis
on increased OP and Postoperative inIection
You might also like
- NeuroexamDocument7 pagesNeuroexamBobbie SisonNo ratings yet
- Pa Tho PhysiologyDocument2 pagesPa Tho PhysiologyBobbie SisonNo ratings yet
- Case Study - HPN OsMunDocument37 pagesCase Study - HPN OsMunBobbie SisonNo ratings yet
- NCM104 012111Document8 pagesNCM104 012111Bobbie SisonNo ratings yet
- NCM104 012111Document8 pagesNCM104 012111Bobbie SisonNo ratings yet
- Final Drug Study.Document20 pagesFinal Drug Study.Bobbie Sison67% (3)
- Drug StudyDocument8 pagesDrug StudyBobbie SisonNo ratings yet
- Drug StudyDocument8 pagesDrug StudyBobbie SisonNo ratings yet
- AaronDocument1 pageAaronBobbie SisonNo ratings yet
- AaronDocument1 pageAaronBobbie SisonNo ratings yet
- AaronDocument1 pageAaronBobbie SisonNo ratings yet
- AnaphysiogallbladderDocument2 pagesAnaphysiogallbladderBobbie SisonNo ratings yet
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeFrom EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeRating: 4 out of 5 stars4/5 (5794)
- Shoe Dog: A Memoir by the Creator of NikeFrom EverandShoe Dog: A Memoir by the Creator of NikeRating: 4.5 out of 5 stars4.5/5 (537)
- The Yellow House: A Memoir (2019 National Book Award Winner)From EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Rating: 4 out of 5 stars4/5 (98)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceFrom EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceRating: 4 out of 5 stars4/5 (895)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersFrom EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersRating: 4.5 out of 5 stars4.5/5 (344)
- The Little Book of Hygge: Danish Secrets to Happy LivingFrom EverandThe Little Book of Hygge: Danish Secrets to Happy LivingRating: 3.5 out of 5 stars3.5/5 (399)
- Grit: The Power of Passion and PerseveranceFrom EverandGrit: The Power of Passion and PerseveranceRating: 4 out of 5 stars4/5 (588)
- The Emperor of All Maladies: A Biography of CancerFrom EverandThe Emperor of All Maladies: A Biography of CancerRating: 4.5 out of 5 stars4.5/5 (271)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaFrom EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaRating: 4.5 out of 5 stars4.5/5 (266)
- Never Split the Difference: Negotiating As If Your Life Depended On ItFrom EverandNever Split the Difference: Negotiating As If Your Life Depended On ItRating: 4.5 out of 5 stars4.5/5 (838)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryFrom EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryRating: 3.5 out of 5 stars3.5/5 (231)
- On Fire: The (Burning) Case for a Green New DealFrom EverandOn Fire: The (Burning) Case for a Green New DealRating: 4 out of 5 stars4/5 (73)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureFrom EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureRating: 4.5 out of 5 stars4.5/5 (474)
- Team of Rivals: The Political Genius of Abraham LincolnFrom EverandTeam of Rivals: The Political Genius of Abraham LincolnRating: 4.5 out of 5 stars4.5/5 (234)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyFrom EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyRating: 3.5 out of 5 stars3.5/5 (2259)
- The Unwinding: An Inner History of the New AmericaFrom EverandThe Unwinding: An Inner History of the New AmericaRating: 4 out of 5 stars4/5 (45)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreFrom EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreRating: 4 out of 5 stars4/5 (1090)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)From EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Rating: 4.5 out of 5 stars4.5/5 (120)
- Her Body and Other Parties: StoriesFrom EverandHer Body and Other Parties: StoriesRating: 4 out of 5 stars4/5 (821)
- MetLife CaseDocument4 pagesMetLife Casekatee3847No ratings yet
- Maven MCQDocument55 pagesMaven MCQANNAPUREDDY ANIL KUMAR REDDY CSENo ratings yet
- Thom22e ch03 FinalDocument44 pagesThom22e ch03 FinalDionisius AlvianNo ratings yet
- Arrhythmia - WikipediaDocument76 pagesArrhythmia - WikipediaJamesNo ratings yet
- Letter of Intent Date: 18-Feb-2019 Mr. Ravi Mishra,: For Multiplier Brand Solutions PVT LTDDocument2 pagesLetter of Intent Date: 18-Feb-2019 Mr. Ravi Mishra,: For Multiplier Brand Solutions PVT LTDRavi MishraNo ratings yet
- Architecture of Neural NWDocument79 pagesArchitecture of Neural NWapi-3798769No ratings yet
- Advancement of SGDocument2 pagesAdvancement of SGkailasasundaramNo ratings yet
- Trend Trading StocksDocument64 pagesTrend Trading Stockssasi717100% (1)
- AMX Prodigy Install ManualDocument13 pagesAMX Prodigy Install Manualsundevil2010usa4605No ratings yet
- International Rice Research Newsletter Vol12 No.4Document67 pagesInternational Rice Research Newsletter Vol12 No.4ccquintosNo ratings yet
- El Nino 3Document8 pagesEl Nino 3nisAfiqahNo ratings yet
- BF254 BF255Document3 pagesBF254 BF255rrr2013No ratings yet
- 1.6 FSI Inlet Manifold Removal Guide - Audi A2 Owners' ClubDocument3 pages1.6 FSI Inlet Manifold Removal Guide - Audi A2 Owners' Clubdusan jovanovicNo ratings yet
- Summary of The Pilot ProjectDocument46 pagesSummary of The Pilot ProjectSrinivasan JeganNo ratings yet
- No Experience ResumeDocument2 pagesNo Experience ResumeNatalia PantojaNo ratings yet
- Molecules of Life PDFDocument113 pagesMolecules of Life PDFArpit Pradhan100% (1)
- Fbla Scavenger Hunt 1Document3 pagesFbla Scavenger Hunt 1api-472648158No ratings yet
- EPA NCP Technical Notebook PDFDocument191 pagesEPA NCP Technical Notebook PDFlavrikNo ratings yet
- Scale Aircraft Modelling 01.2019Document100 pagesScale Aircraft Modelling 01.2019Nikko LimuaNo ratings yet
- Probecom 11.3M Antenna System Datasheet 2Document2 pagesProbecom 11.3M Antenna System Datasheet 2Hugo MateoNo ratings yet
- Chapter 7odeDocument29 pagesChapter 7odeRoberto NascimentoNo ratings yet
- Job Sheet 1Document5 pagesJob Sheet 1Sue AzizNo ratings yet
- UniFi Quick GuideDocument2 pagesUniFi Quick GuideAndhika TharunaNo ratings yet
- Avanquest Perfect Image V.12 User GuideDocument174 pagesAvanquest Perfect Image V.12 User GuideShafiq-UR-Rehman Lodhi100% (1)
- Corporate Profile of Multimode GroupDocument6 pagesCorporate Profile of Multimode GroupShaheen RahmanNo ratings yet
- Practice Quiz Reflection Project Initiation and Key ComponentsDocument3 pagesPractice Quiz Reflection Project Initiation and Key ComponentsFalastin Tanani67% (3)
- Professional Development Objectives Related To Modalities Specific TopicsDocument3 pagesProfessional Development Objectives Related To Modalities Specific TopicsCris100% (1)
- H I Ôn Thi Aptis & Vstep - Tài Liệu - Anna MaiDocument4 pagesH I Ôn Thi Aptis & Vstep - Tài Liệu - Anna Maihanh.mt2022No ratings yet
- FO - Course Transition Info - Acknowledgement - SIT50422 - Dip Hospitality Management - V1Document2 pagesFO - Course Transition Info - Acknowledgement - SIT50422 - Dip Hospitality Management - V1nitesh.kc06No ratings yet
- Review Problems On Gas TurbineDocument9 pagesReview Problems On Gas TurbinejehadyamNo ratings yet