Professional Documents
Culture Documents
Chapter 2
Uploaded by
Shoroq El BeshbeshyOriginal Description:
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Chapter 2
Uploaded by
Shoroq El BeshbeshyCopyright:
Available Formats
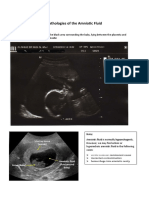
_/+e:.- I.-.. -, :.:.-+:-.
4HNlB1lC FLLlB
DeIinition:
he amniotic fluid is the normally clear fluid that
collects within the amniotic cavity increases as
pregnancy progresses until about 34 weeks, when there is a
decrease in volume. An average volume of about 1000 mL is
found at term, although this may vary widely from a few
milliliters to many liters in abnormal conditions (Barss VA et
al., 1984).
EmbryoIogy of amniotic membranes & amniotic cavity:
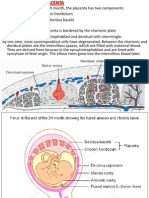
Amnion
%he amnion at term is a tough and tenacious but
pliable membrane. t is the innermost fetal membrane and is
contiguous with amnionic fluid. %his particular avascular
structure occupies a role of incredible importance in human
pregnancy. n many obstetrical populations, preterm
prematurely ruptured fetal membranes are the single most
common antecedent of preterm delivery. %he amnion is the
tissue that provides almost all of the tensile strength of the
fetal membranes. %herefore, the development of the
components of the amnion that protect against its rupture or
tearing is vitally important to successful pregnancy outcome
(Piantelli et al., 2004).
%
_/+e:.- I.-.. -, :.:.-+:-.
Amnion Structure
Bourne (1962) described five separate layers of
amnion tissue. %he inner surface, which is bathed by
amnionic fluid, is an uninterrupted, single layer of cuboidal
epithelial cells, believed to be derived from embryonic
ectoderm. %his epithelium is attached firmly to a distinct
basement membrane that is connected to the acellular
compact layer, which is composed primarily of interstitial
collagens. On the outer side of the compact layer, there is a
row of fibroblast-like mesenchymal cells, which are widely
dispersed at term. %hese are probably derived from
mesoderm of the embryonic disc. %here also are a few fetal
macrophages in the amnion. %he outermost layer of amnion
is the relatively acellular zona spongiosa, which is
contiguous with the second fetal membrane, the chorion
laeve. %he human amnion lacks smooth muscle cells,
nerves, lymphatics, and importantly, blood vessels.
Amnion DeveIopment
Early in the process of implantation, a space develops
between the embryonic cell mass and adjacent trophoblasts.
Small cells that line this inner surface of trophoblasts have
been called amniogenic cells, the precursors of amnionic
epithelium. %he human amnion is first identifiable about the
seventh or eighth day of embryo development. nitially a
minute vesicle, the amnion develops into a small sac that
covers the dorsal surface of the embryo. As the amnion
enlarges, it gradually engulfs the growing embryo, which
prolapses into its cavity (Benirschke et al., 2000).
_/+e:.- I.-.. -, :.:.-+:-.
omposition of amniotic fIuid:
Water (99%) and solids (1%) which include (1) organic
constituents: carbohydrates (as glucose and fructose),
proteins (as albumin and globulin), lipids, enzymes, and
hormones (2) inorganic constituents: sodium, potassium,
chloride, copper are found as in plasma (3) vernix caseosa,
lanugo hair, and desquamated epithelial cells and
sometimes meconium.
Amniotic fIuid formation:
etal Urine:
%he main source of AF is fetal urination. n the human, the
fetal kidneys begin to make urine before the end of the first
trimester, and production of urine continues from this point,
ever increasing, until term gestation. Efforts to measure
human fetal urine production have been accomplished by
ultrasound measuring the change in fetal bladder volume
over time.
Wladimiroff and Campbell initially measured three
dimensions of the fetal bladder every 15 minutes and
reported a human fetal urine production rate of 230 ml/day at
36 weeks of gestation, which increased to 655 ml/day at
term. Others found similar volumes using the same
technique.
More recently, Rabinowitz et al., using the same
technique as Wladimiroff and Campbell but measuring the
change in volume every 2 to 5 minutes, found fetal urine
production to be much greater than previously predicted,
1,224 ml/day.
_/+e:.- I.-.. -, :.:.-+:-.
n Figure 1, the fetal urine production rates of several
studies are shown, with the greatest volume being that of
Rabinowitz et al., who measured at the most frequent
intervals.
Clearly, the human fetal urine production rate can
be seen to be approximately 1,000 to 1,200 ml/day at term,
suggesting that the entire AFV is replaced more frequently
than every 24 hours (Tomoda et al., 1985).
Figure (1): ormal changes in Ietal urine Ilow rates across
gestation. Lines represent mean values Ior six studies in the
literature. %he individual Iirst authors are shown in the Iigure itselI.
%he highest line is data Irom Rabinowitz et al and represents
bladder volume measurements every 5 minutes instead oI every 15
minutes, as is the case Ior the other Iive studies (Reproduced with
_/+e:.- I.-.. -, :.:.-+:-.
permission from Cilbert WM, Brace RA: Amniotic fluid volume
and normal flows to and from the amniotic cavity. Semin
Perinatol 7:15, 1993) (Cabbe et al., 27).
ung iquid:
Although rarely even contemplated by the practicing
clinician, fetal lung liquid plays an important role in AF
formation. n fact, there is normally an outward rather than
inward movement of fluid from the lungs. %hroughout
gestation, the fetal lungs produce fluid that exits the trachea
and is either swallowed, or leaves the mouth, and enters the
amniotic compartment. n humans, we know that fetal lung
liquid enters the amniotic compartment owing to the
presence of surfactant within the AF, both near and at term,
as measured by amniocentesis for lung maturity.
During normal fetal life, the fetus performs breathing
movements that provide a "to-and-fro movement of AF into
and out of the trachea, upper lungs and mouth. Although AF
may move back and forth, there is a net outward movement
of fetal lung liquid. Clearly, the fetal lungs provide a volume
of liquid to the AF, which adds to that of the fetal urine
(Duenhoelter et al., 1976).
Amniotic fIuid removaI:
etal Swallowing:
_/+e:.- I.-.. -, :.:.-+:-.
n the human, fetal swallowing begins early in gestation.
Sherman et al. have reported that the ovine fetus swallows
in episodes lasting 2 minutes and at volumes of 100 to 300
ml/kg/day. n the term ovine fetus, that volume represents a
daily swallowing rate of 350 to 1,000 ml/day for a 3.5 kg
fetus (Sherman et al., 1990).
Human fetal swallowing was studied by injecting
radioactive chromiumlabeled erythrocytes and hypaque into
the amniotic compartment, and swallowing rates of 72 to 262
ml/kg/day were found.
Abramovich injected colloidal gold into
the human amniotic compartment and found that fetal
swallowing increased with advancing gestational age. He
also found similar swallowing rates to those reported by
Pritchard.
Obviously similar studies could not be performed
today, but the information is helpful in our understanding of
human fetal swallowing. Clearly, fetal swallowing could not
remove the entire volume of fluids entering the amniotic
compartment from fetal urine production and lung liquid, and
therefore, other mechanisms for AF removal must occur
(Tomoda et al., 1985).
Intramembranous Absorption:
_/+e:.- I.-.. -, :.:.-+:-.
A second route for AF removal has been suggested,
namely the intramembranous pathway.
%his process
describes the movement of water and solutes between the
amniotic compartment and the fetal blood, which circulates
through the fetal surface of the placenta. %he large osmotic
gradient (Fig. 2) between AF and fetal blood provides a
substantial driving force for the movement of AF into the fetal
blood.
n separate publications, Heller and Renaud et al. each
injected labeled amnio acids into the amniotic compartments
of women, who were shortly thereafter delivered by
cesarean section. Both groups found high levels of the
amino acids concentrated in the placenta within 45 minutes
of injection. %hey concluded that the amino acids had to be
absorbed by some route other than swallowing in order to
explain the rapid absorption into the fetal circulation within
the placenta. ntramembranous absorption could easily
explain this movement. %his route of absorption is now being
actively investigated, and researchers have noted that 200 to
500 ml/day leaves the amniotic compartment under normal
physiologic conditions.
Figure 3 demonstrates the summation of all currently
identified avenues for fluid entry and exit from the amniotic
compartment, along with their measured or estimated
values. With the identification of intramembranous
absorption as a significant route for the removal of amniotic
water and solutes, it appears that all routes of entry and
removal from the amniotic compartment have possibly been
_/+e:.- I.-.. -, :.:.-+:-.
identified, and the equation of input and outflow has finally
been balanced ( Fig. 3 ) (Gilbert et al., 1989).
Figure ( hange in maternal and Ietal plasma and in amniotic
Iluid osmolality across gestation (Reproduced with permission
from Gilbert WM, Moore TR, Brace RA. Amniotic fluid volume
dynamics. etal Med Review 3:89, 1991) (Cabbe et al., 27).
Figure (: All known pathways Ior Iluid and solute entry and exit
Irom the amniotic Iluid in the Ietus near term. Arrow size is
relative to associated Ilow rate. %he solid red arrows represent
directly measured Ilows, whereas the blue arrows represent
estimated Ilows. %he numbers represent volume Ilow in milliliters
per day. %he curved portion oI the double arrow represents lung
Iluid that is directly swallowed aIter leaving the trachea, whereas
the straight portion represents lung Iluid that enters the amniotic
cavity Irom the mouth and nose Reproduced with permission
_/+e:.- I.-.. -, :.:.-+:-.
from Cilbert WM, Moore 1R, Brace RA: Amniotic fluid volume
dynamics. etal Med Review 3:89, 1991) (Cabbe et al., 27).
ormal amniotic fluid volume:
As a result of various limitations, attempts to measure
actual AFV are difficult. t is not easy to get near, or into, the
amniotic compartment. %o enter the amniotic cavity, an
invasive procedure such as an amniocentesis must be
performed. %o measure the volume of AF, an inert dye must
be injected, which dilutes to fill the amniotic cavity. Follow-up
samples of amniotic fluid are then obtained to determine a
dilution curve. Obviously, an amniocentesis has a small but
real risk of interrupting the pregnancy, and any substance
injected into the uterus can cause infection despite every
precaution being taken. %he dye injection technique is
considered the "gold standard for determining actual AFV
and is compared with other methods of estimating AFV, such
as ultrasound (Magann et al., 1992).
Despite these measurement limitations, Brace and Wolf
identified all published measurements of AFV in 12 studies
with 705 individual AFV measurements. %heir findings are
demonstrated in Figure 4 . From this figure, it can be seen
that for each week of gestation, there can be widely varying
amounts of AF, which increase with advancing gestational
age. %he largest variation occurs at 32 to 33 weeks of
gestation. At this time, the normal range (5th to 95th percent)
is from 400 to 2100 ml. %his represents a wide "normal
range. One of the most interesting findings of the Brace and
Wolf study is that from 22 weeks through 39 weeks of
gestation, the average volume of AF (black dots on Fig. 1 )
_/+e:.- I.-.. -, :.:.-+:-.
remained unchanged. At a time when the fetus weighed, on
average, about 500 g at 22 weeks, up to term gestation
when it weighed 3,500 g, a 7-fold increase in weight, the
mean AFV was the same. %his would suggest that AFV was
being carefully regulated (Brace et al., 1989).
Figure (4): omogram showing amniotic Iluid volume as a Iunction
oI gestational age. %he black dots are the mean Ior each 2-week
interval. Percentiles calculated Irom polynomial regression
equation and standard deviation oI residuals (Reproduced with
permission from Brace RA, Wolf E1: Aormal amniotic fluid
volume throughout pregnancy. Am 1 Obstet Cynecol 11:382,
1989) (Cabbe et al., 27).
UItrasound measurements of amniotic fIuid voIume:
Measuring true AFV is not only difficult but clinically
impractical as well. %he advent of ultrasound has afforded us
_/+e:.- I.-.. -, :.:.-+:-.
the ability of looking, noninvasively, into the human uterus to
examine both the fetus and AFV. Early ultrasound
estimations of AFV were made by measuring the largest
vertical pocket (LVP) of AF. Other researchers have
examined the LVP, and then considered the horizontal plain,
if the LVP was less than 1 cm.
Chamberlain et al. and Mercer et al. found that with
the LVP of AF less than 1 cm or 0.5 cm, respectively,
perinatal morbidity and the PMR were increased. %hese
lower values of the LVP certainly identified at-risk fetuses,
but the sensitivity for identifying the majority of pregnancy
complications associated with oligohydramnios, was not as
strong, causing others to choose higher values as a cutoff
point (Manning et al., 1981).
As the quality of ultrasound improved, investigators
expanded their measurements to include the LVP in each of
the four quadrants of the uterus throughout gestation. %he
uterus at any gestational age beyond 20 weeks is divided
into four equal quadrants, %he deepest clear pocket of AF is
then measured, making sure that the ultrasound transducer
is perpendicular to the floor. %his four-quadrant
measurement was termed the Amniotic Fluid ndex (AF) by
Phelan et al. and has been described by others as well.
%he clearest graphic presentation of the AF ( Fig. 5) is
that of Moore and Cayle, who described their population of
791 normal pregnant women. %heir cross-sectional study
obtained only one AF measurement from each pregnancy
with a normal outcome. %he 5th and 95th percentile of the
AF varied for each gestational age, suggesting that what
_/+e:.- I.-.. -, :.:.-+:-.
may be normal for one gestational age period, may be
abnormal for another. %he 95th percentile for 35 to 36 weeks
of gestation was a value of 24.9 cm, whereas the 95th
percentile for 41 weeks of gestation was 19.4 cm. %he
variation in the AF at the 5th percentile was less than that of
the 95th percentile, but it still varied by as much as 2.5 cm.
Finally, the investigators reported the interobserver and
intraobserver variation to be 3.1 percent and 6.7 percent,
respectively, which is acceptable for this commonly
performed procedure. Comparing the ultrasound estimation
of the AFV by the AF with the actual measured volume
demonstrates very similar-appearing curves (Phelan et al.,
1987).
Figure (5): Amniotic Iluid index in millimeters plotted with
gestational age weeks. %he solid line denotes the 50th percentile;
dashed lines, the 5th and 95th percentiles; and the dotted lines, 2
_/+e:.- I.-.. -, :.:.-+:-.
standard deviations 2.5th and 97.5th percentiles (Reproduced
with permission from Moore 1R, Cayle 1E: 1he amniotic fluid
index in normal human pregnancy. Am 1 Obstet Cynecol
2:118, 199) (Cabbe et al., 27).
Magann et al. have published several studies comparing
the LVP with the AF and dye dilution techniques, to
determine which test is superior for predicting actual AFV, or
perinatal morbidity or mortality.
Consistently, they reported
that both ultrasound methods (LVP and AF) poorly predicted
actual AFV. n addition, they found an observed sensitivity
for an AF measurement of less than 5 cm of 10 percent
(specificity of 96 percent), whereas the LVP was worse
(sensitivity 5 percent, specificity 98 percent).
When examining cases of suspected polyhydramnios,
an AF greater than 20 cm had a sensitivity of 29 percent
(specificity 97 percent), which was equal to the LVP method
(sensitivity of 29 percent, specificity of 94 percent). When the
LVP method was compared with the AF method, the former
had fewer false-positive tests than the latter, suggesting the
LVP was the superior method. n comparison, Moore found
the AF superior to the LVP for identifying cases of
oligohydramnios but found the two methods similar at
predicting polyhydramnios (Horsager et al., 1994).
Measurement of the AF can also vary widely depending
upon the technique used. Flack et al. reported that they
could increase the AF (13 percent) by using low pressure
with the ultrasound transducer on the maternal abdomen, as
compared with moderate pressure, or decrease the AF (21
percent) with high pressure on the maternal abdomen.
Clearly technique is important to prevent overestimating or
_/+e:.- I.-.. -, :.:.-+:-.
underestimating the ultrasound measurement of the AF.
Despite the fact that the actual measurement of AFV by
Brace and Wolf roughly superimposes upon the graph of the
normal AF of Moore and Cayle, it does not mean that they
will necessarily correlate well with each other (lack et al.,
1994).
For many years, investigators have tried, with mixed
success, to demonstrate the utility and applicability of
ultrasound estimation of AFV in relation to perinatal
outcome. Early work by Chamberlain et al. found that with
the LVP smaller than 1 cm, there was a marked increase in
perinatal morbidity and mortality, which persisted even after
correcting for birth defects. Despite overwhelming evidence
that any ultrasound method for predicting AFV is poor at
best, clinical practice continues to include the use of weekly
or biweekly AFV estimation by ultrasound (Chamberlain et
al., 2004).
_/+e:.- I.-.. -, :.:.-+:-.
Pulyhydramnius
With the increasing use of real-time ultrasound, the
diagnosis of polyhydramnios has been on the rise.
Previously, the diagnosis of polyhydramnios was made when
the uterus was large for gestational age or the fetus could
not be easily palpated by Leopold's maneuvers. %he
diagnosis was often not made until the time of delivery, when
large gushes of AF preceded or followed the delivery of the
newborn. Polyhydramnios has an impact on perinatal
morbidity and mortality based largely on the amount of fluid
present, and when in gestation it presents. %he earlier in
gestation it occurs and the greater the amount of fluid, the
higher the morbidity and mortality.
%he incidence of polyhydramnios has been reported to
be about 1 percent in large population-based studies.
%he
most common cause for severe polyhydramnios in
midgestation is congenital malformations, with or without
aneuploidy, and monozygotic twins (Wier et al., 1979).
_/+e:.- I.-.. -, :.:.-+:-.
FetaI and MaternaI auses of PoIyhydramnios
etal conditions
O Congenital anomalies
4 Gastrointestinal obstruction
4 CNS abnormalities
4 Cystic hygromas
4 Nonimmune hydrops
4 Sacrococcygeal teratoma
4 Aneuploidy
O %win-to-twin transfusion syndrome
O Muscular dystrophy syndromes
Maternal conditions
4 diopathic
4 Poorly controlled diabetes mellitus
4 CNS, central nervous system.
Early ultrasound studies examining polyhydra-mnios used
the LVP method for measuring AFV. Most authors report an
LVP of greater than 8 cm to define polyhydramnios. Hill et al.
divided their patients with polyhydramnios into three groups:
mild (LVP 8 to 11 cm, 79 percent of cases), moderate (LVP
12 to 15 cm, 16.5 percent cases), and severe (LVP 16+ cm,
5 percent of cases). Overall the perinatal mortality rate was
127.5/1,000, which corrected to 58.8/1,000 when lethal
malformations were removed. %his value is markedly
increased over the background rate.
_/+e:.- I.-.. -, :.:.-+:-.
Hill et al. found that with mild polyhydramnios, a
specific diagnosis for the cause of polyhydramnios could
only be found 16 percent of the time. %his diagnosis
increased to a rate of 90 percent for moderate
polyhydramnios, and 100 percent for severe
polyhydramnios. n a follow-up study, Many et al. examined
275 women with polyhydramnios to determine if the degree
of polyhydramnios had an impact on the rate of prematurity.
Although excessive amniotic fluid did not impact the rate of
prematurity, the presence of anomalies or diabetes mellitus
was associated with an increased risk of preterm delivery
(Hill et al., 1987).
Later in pregnancy, with milder degrees of polyhydramnios,
the cause is usually idiopathic or related to diabetes. At
present, there are no uniformly accepted criteria for making
the diagnosis of polyhydramnios. Brace and Wolf defined
polyhydramnios as being present when the actual fluid
volume was greater than 2,100 ml (2.5 percent incidence),
but an actual measurement of AFV is difficult and clinically
impractical (Golan et al., 1994).
Using the four-quadrant AF, Moore and Cayle reported the
AF for varying gestational ages (see Fig. 5) and concluded
that one value for the AF cannot be used throughout
gestation but must be referenced to gestational age. %he
study found the 97.5 percentile at 35 weeks of gestation to
be 27.9 cm, which represents the upper limits of normal for
that gestational age. %his value would clearly be abnormally
increased for earlier and later measurements in gestation
(see Fig. 5) (Moore et al., 1990).
_/+e:.- I.-.. -, :.:.-+:-.
Midgestation PoIyhydramnios:
%he pregnant woman who presents with a rapidly enlarging
uterus in midpregnancy, or who presents in preterm labor,
will most likely have a fetus with a congenital malformation
or aneuploidy, or both. Severe polyhydramnios in the second
trimester has a significant PMR, which is most commonly
due to prematurity or aneuploidy.
%he more common
congenital malformations associated with severe
polyhydramnios include the host of defects associated with
gastrointestinal obstruction. Esophageal atresia with or
without tracheoesophageal fistula can present with early-
onset severe polyhydramnios owing to the blockage of fetal
swallowing.
With certain malformations, AFV may still be normal
because a tracheoesophageal fistula, for example, provides
for the movement of fluid into the stomach, and thus,
polyhydramnios may not develop. Other gastrointestinal
obstructions such as duodenal atresia may result in
polyhydramnios. Whenever a structural defect is seen in a
fetus, consideration should be given to performing a
karyotype owing to the dramatic increase in aneuploidy seen
with one or more structural defects. Knowing the karyotype
of the fetus with a defect may allow for further treatment
options, or possible pregnancy termination. %he fetus with
polyhydramnios and trisomy 18 would be a candidate for
pregnancy termination at any point in the pregnancy owing
to the lethal nature of trisomy 18 (Pauer et al., 2003).
Another common cause of acute, severe,
polyhydramnios in the second trimester is the condition
_/+e:.- I.-.. -, :.:.-+:-.
associated with the twin-to-twin transfusion syndrome (%%S).
%his may be found in single placenta, monozygotic twin
pregnancies. With identical twins who share a single
placenta, 90 percent of the fetuses will have vascular
connections between the arteries and veins on the surface of
the placenta. %he most common connection is the artery-to-
artery connection, followed by the vein-to-vein connection.
%he least common connection is the artery of one twin
connecting to the vein of the other. %his can lead to
oligohydramnios of the twin with the arterial connection, and
polyhydramnios in the twin with the venous connection. f the
polyhydramnios/ oligohydra-mnios is severe enough, the
PMR can approach 100 percent without treatment. However,
survival improves to 50 to 70 percent with intervention
(Benirschke et al., 2000).
%hird-%rimester PoIyhydramnios:
When polyhydramnios occurs in the third trimester of
pregnancy, it is usually mild and not associated with a
structural defect. Despite the fact that a diagnosis can be
determined for the majority of early-onset cases, for the vast
majority of cases in the third trimester, a diagnosis cannot be
found. %hus, these cases are given the diagnosis of
idiopathic. Despite this, however, the other causes of
polyhydramnios must be ruled out before the idiopathic label
can be applied (Hill et al., 1987).
n many cases, polyhydramnios may be transient.
Golan et al. examined 113 cases of polyhydramnios. On
repeated examination, patients separated into two groups:
%hose cases in which the polyhydramnios worsened or the
_/+e:.- I.-.. -, :.:.-+:-.
AFV remained markedly elevated, and those whose AFV
returned to normal, or decreased to mild polyhydramnios. n
the former group, all complications of pregnancy were
greater, including preterm delivery (2.7-fold increase),
preeclampsia (2.7-fold increase), UFD (7.7-fold increase),
and neonatal demise (7.7-fold increase). n the latter group
in which the polyhydramnios improved or AFV returned to
normal, the most common diagnosis was idiopathic and
showed a favorable outcome. %his study would suggest that
if polyhydramnios is persistent, the fetus should be
examined closely for congenital malformations and
aneuploidy, and monitored to prevent an UFD. n addition,
the mother should be watched closely for other medical
complications of pregnancy (Golan et al., 1994).
MaternaI and FetaI hazards:
Maternal complications of polyhydramnios mainly relate
to distention of the uterus and include preterm labour,
abdominal discomfort and utrine atony postpartum. Unstable
lie, placental abruption and an increased incidence of
caesarean section also result from severe polyhydramnios
(Many et al., 1995).
Perinatal mortality in cases of polyhydramnios is increased
10-30 percent and is secondary to the presence of
congenital malformations and preterm delivery (Hill et al.,
1987).
%reatment of PoIyhydramnios:
_/+e:.- I.-.. -, :.:.-+:-.
%reatment options for patients with polyhydramnios are
usually tailored to the underlying cause of the
polyhydramnios. With mild idiopathic polyhydramnios, in
which the work-up is negative, and follow-up ultrasound
demonstrates persistent poly-hydramnios, the only possible
intervention might be antepartum testing with fetal kick
counts, or nonstress tests. When poorly controlled diabetes
mellitus is the cause of the polyhydramnios, proper glycemic
control may be beneficial as a treatment option.
With the
current aggressive management of diabetes in pregnancy, it
is rare to see severe polyhydramnios associated with
diabetes. Usually, if the diabetes is not well controlled, then
the mother will undergo antepartum testing to assess fetal
well-being (Bartha et al., 2003).
Polyhydramnios associated with a fetal structural
abnormality such as an obstruction to swallowing, usually
requires invasive testing by amniocentesis to rule out
aneuploidy. Often, the degree of polyhydra-mnios in these
cases is severe and the resulting overdistention of the uterus
causes preterm labor long before the due date. n these
cases, one medical treatment option involves the
administration of a prostaglandin inhibitor such as
indomethacin, which works by decreasing fetal urine
production.
Prostaglandin inhibitors have been shown to
decrease fetal urine output significantly. %his effect occurs
within 5 hours of starting the medication and decreases AFV
within 24 hours.
Although indomethacin has been shown to be
relatively safe when given over a short period of time, such
_/+e:.- I.-.. -, :.:.-+:-.
as 72 hours, prolonged usage may be associated with risks
to the fetus. Prolonged use has been shown to cause
premature closure, or narrowing, of the ductus venosus
within the fetal heart and renal abnormalities in the newborn
period.
Complications related to indomethacin use worsen
with advancing gestational age, and such treatment beyond
31 to 32 weeks of gestation should be avoided. Because of
the adverse effects on the fetus associated with the long-term
use of indomethacin, it probably has limited use in pregnancy
for the treatment of severe polyhydramnios (Stevenson et al.,
1992).
For those pregnancies complicated by the %%S, or for
the fetus with obstructed swallowing, repetitive
amnioreductions may be required to reduce the AFV until the
fetus reaches viability.
Severe cases of %%S, if left untreated,
can have a PMR approaching 100 percent. Repetitive
amnioreductions, in which an amniocentesis is performed
and AF is withdrawn until the AF is normal, can reduce the
PMR from 100 percent to about 50 percent.
Further options
for the treatment of the %%S include the ablation of the
connecting blood vessels by laser photocoagulation via
fetoscopy.
A recent large prospective trial found that the laser
ablation of the connecting blood vessels resulted in better
outcomes for the twin pregnancy as compared with
amnioreduction alone. A major problem with laser ablation is
that only certain centers perform the procedure, and most
insurance companies will not pay for the procedure. %his is
not the case with amnioreductions, which can be performed
_/+e:.- I.-.. -, :.:.-+:-.
anywhere and, therefore, are usually covered by insurance.
Although laser ablation treatment may "cure the cause of
the %%S, amnioreduction only treats the symptoms. As a
result, the amnioreduction method of treatment may require
repeated procedures every 1 to 2 weeks for the remainder of
the pregnancy (Reisner et al., 1993).
You might also like
- Last Minute Embryology: Human embryology made easy and digestible for medical and nursing studentsFrom EverandLast Minute Embryology: Human embryology made easy and digestible for medical and nursing studentsNo ratings yet
- The Amnion and Amniotic FluidDocument7 pagesThe Amnion and Amniotic FluidMerina FirmansahNo ratings yet
- Stem CellsDocument15 pagesStem CellsDelia Andreia ȘveduneacNo ratings yet
- Sin Título 2Document16 pagesSin Título 2Anilu ApNo ratings yet
- Physiology of Amniotic Fluid Volume RegulationDocument8 pagesPhysiology of Amniotic Fluid Volume RegulationYosep SutandarNo ratings yet
- Amniotic PhysioDocument3 pagesAmniotic PhysiobjfieroNo ratings yet
- Hydra Mi NosDocument8 pagesHydra Mi NosSudha DeviNo ratings yet
- Amniotic Fluid As A Vital Sign For Fetal Wellbeing: ReviewDocument9 pagesAmniotic Fluid As A Vital Sign For Fetal Wellbeing: ReviewMeska AmeliaNo ratings yet
- Fetal Membranes IMBBSDocument26 pagesFetal Membranes IMBBSSubham YadavNo ratings yet
- Romzan Alfiriza R (2018) Maryo Juan L.T (2018) Sarah Safrilia (201810401011007)Document22 pagesRomzan Alfiriza R (2018) Maryo Juan L.T (2018) Sarah Safrilia (201810401011007)SarahNo ratings yet
- 2006 7 E292-E299 William M. Gilbert: Amniotic Fluid DynamicsDocument10 pages2006 7 E292-E299 William M. Gilbert: Amniotic Fluid DynamicsMel MurNo ratings yet
- Pathologies of The Amniotic Fluid: Gyneco Naji HajjDocument13 pagesPathologies of The Amniotic Fluid: Gyneco Naji HajjHassan KawtharanyNo ratings yet
- Fetal MembranesDocument17 pagesFetal MembranesQaiser InayatNo ratings yet
- Anatomy and Embryology of Umbilicus in Newborns ADocument8 pagesAnatomy and Embryology of Umbilicus in Newborns AAubrey PerezNo ratings yet
- Amniotic Fluid Water Dynamics: M.H. Beall, J.P.H.M. Van Den Wijngaard, M.J.C. Van Gemert, M.G. RossDocument8 pagesAmniotic Fluid Water Dynamics: M.H. Beall, J.P.H.M. Van Den Wijngaard, M.J.C. Van Gemert, M.G. RossCorín AnelNo ratings yet
- Amniotic FluidDocument33 pagesAmniotic FluidElsa Aprillia SujadiNo ratings yet
- Wvith: ExchangedDocument10 pagesWvith: ExchangedJessica StephanieNo ratings yet
- OLIGOHIDRAMNIOSDocument20 pagesOLIGOHIDRAMNIOSJorge Luis Sánchez AlarcónNo ratings yet
- Perkembangan Plasenta (Autosaved) .En - IdDocument18 pagesPerkembangan Plasenta (Autosaved) .En - IdFATIMAHNo ratings yet
- 11th Lecture Amnion& Amniotic FluidDocument35 pages11th Lecture Amnion& Amniotic FluidHussein Al Saedi100% (1)
- Balance de Agua en El Feto y El Recién NacidoDocument5 pagesBalance de Agua en El Feto y El Recién NacidoCarlos ReveloNo ratings yet
- Selaput EmbrioDocument25 pagesSelaput EmbrioMartupa SidabutarNo ratings yet
- Pathophysiology Hidrop FetalisDocument25 pagesPathophysiology Hidrop FetalisPandu Nugroho KantaNo ratings yet
- Amniocentrices (From The Greek Amnion For "Sac" and KenteDocument5 pagesAmniocentrices (From The Greek Amnion For "Sac" and KenteJohn Paolo Tamayo OrioNo ratings yet
- Amniotic FluidDocument55 pagesAmniotic FluidRoselle Joy D. RosalejosNo ratings yet
- Stages of Fetal Growth and DevelopmentDocument10 pagesStages of Fetal Growth and DevelopmentGrant KhangabNo ratings yet
- Embryology, Yolk Sac - StatPearls - NCBI BookshelfDocument10 pagesEmbryology, Yolk Sac - StatPearls - NCBI Bookshelfr9fch8mws7No ratings yet
- Fetal Membranes and PlacentaDocument48 pagesFetal Membranes and Placentaveegeer100% (4)
- Fallopian Tube PresentationDocument41 pagesFallopian Tube PresentationReena Ross Nathan100% (3)
- CA RationaleDocument8 pagesCA RationaleNursing LectureNo ratings yet
- Amnion 1Document2 pagesAmnion 1Oryza SativaniNo ratings yet
- Extraembryonic MembraneDocument41 pagesExtraembryonic MembraneDangkoNo ratings yet
- Sofie R Krisnadi, Dr. SpogDocument82 pagesSofie R Krisnadi, Dr. SpogYogi OktiandiNo ratings yet
- Anatomy and Physiology FinalDocument2 pagesAnatomy and Physiology FinalChloé Jane Hilario100% (1)
- Fertilization: Glora P. de Leon, RN, RM, ManDocument103 pagesFertilization: Glora P. de Leon, RN, RM, ManJoan VillafrancaNo ratings yet
- SAQ EmbryologyDocument9 pagesSAQ EmbryologyShilpa DuttaNo ratings yet
- Picture of The Month: What Is Amniotic Fluid Sludge'?Document6 pagesPicture of The Month: What Is Amniotic Fluid Sludge'?Luis InostrozaNo ratings yet
- Disorders in Amniotic FluidDocument5 pagesDisorders in Amniotic FluidLatansa DinaNo ratings yet
- Embryology, Pathophysiology, and Ultrasound Characteristics of The Placenta ObjectivesDocument13 pagesEmbryology, Pathophysiology, and Ultrasound Characteristics of The Placenta ObjectivesAudrey100% (5)
- Extra-Embryonic MembranesDocument60 pagesExtra-Embryonic MembranesDaniel MendozaNo ratings yet
- TTN AafpDocument9 pagesTTN Aafpsiti nur rachmaniNo ratings yet
- Amniotic FluidDocument7 pagesAmniotic FluidCherralaine CorderoNo ratings yet
- Anatomy and Embryology of Umbilicus in Newborns: A Review and Clinical CorrelationsDocument7 pagesAnatomy and Embryology of Umbilicus in Newborns: A Review and Clinical Correlationsbayu pamungkasNo ratings yet
- OB Definition of TermsDocument9 pagesOB Definition of TermsWarrenSandovalNo ratings yet
- PlacentaDocument11 pagesPlacentasubashikNo ratings yet
- Extraembryonic MembranesDocument4 pagesExtraembryonic MembranesShafiullah Habib LitonNo ratings yet
- Fetal CirculationDocument28 pagesFetal CirculationNelai GoNo ratings yet
- Mere A: SyncytiotrophoblastDocument6 pagesMere A: SyncytiotrophoblastMere MujeresNo ratings yet
- FertilizationDocument6 pagesFertilizationKristine Castillo100% (1)
- Congenital Abnormalities of The UterusDocument7 pagesCongenital Abnormalities of The Uterusمحمود الموسويNo ratings yet
- Transient Tachypnea of The Newborn: Pediatrics in Review December 2008Document10 pagesTransient Tachypnea of The Newborn: Pediatrics in Review December 2008Haneen Dabbas2019No ratings yet
- Neo-Natal Physiology and Post-Natal AdaptationsDocument27 pagesNeo-Natal Physiology and Post-Natal Adaptationskiflie derejeNo ratings yet
- Fertilization and Fetal DevelopmentDocument50 pagesFertilization and Fetal DevelopmentMark Ludwig Labastida100% (1)
- EmbryologyDocument26 pagesEmbryologyBryan Mae H. Degorio100% (1)
- Amniotic Fluid and Cord Abnormalities: DR - Saswati Tripathy Professor ObgyDocument46 pagesAmniotic Fluid and Cord Abnormalities: DR - Saswati Tripathy Professor ObgySaranya BalamuruganNo ratings yet
- NCLEX Review of Maternity NursingDocument34 pagesNCLEX Review of Maternity NursingAlain Chery100% (2)
- Bovine Reproduction Booklet UK A5 16pp Text 10Document20 pagesBovine Reproduction Booklet UK A5 16pp Text 10lenn chandNo ratings yet
- Unit 2 - Fertilization, Impantation, Development of Placenta and Its Function, AbnormalityDocument62 pagesUnit 2 - Fertilization, Impantation, Development of Placenta and Its Function, AbnormalityN. Siva100% (1)
- OSCE On 14/3/2008: Describe Gynaecoid PelvisDocument82 pagesOSCE On 14/3/2008: Describe Gynaecoid PelvisKahing LiNo ratings yet
- A. Paracervical Block C. Give Spinal Block D. Pudendal BlockDocument48 pagesA. Paracervical Block C. Give Spinal Block D. Pudendal BlockMae Rose Charlene MendozaNo ratings yet
- Amniotic Fluid DisordersDocument22 pagesAmniotic Fluid Disordersvictor onapaNo ratings yet
- Hilaria Sas 8Document3 pagesHilaria Sas 8Christy Mae Batucan HilariaNo ratings yet
- Post MaturityDocument5 pagesPost MaturityBa BamNo ratings yet
- GRP 7 Partograph BSN - 2DDocument13 pagesGRP 7 Partograph BSN - 2DCzarina Mae Quinones Tadeo0% (1)
- High Risk Pregnancy Part 2Document12 pagesHigh Risk Pregnancy Part 2Kenneth Noveno100% (1)
- Case Study On Breech BirthDocument65 pagesCase Study On Breech BirthSujan Shrestha94% (32)
- MCN Lec Fetal DevpDocument580 pagesMCN Lec Fetal DevpknotstmNo ratings yet
- Case 5Document41 pagesCase 5Trisha Mae Marquez100% (2)
- Fertilization & Fetal DevelopmentDocument23 pagesFertilization & Fetal DevelopmentDimple CosNo ratings yet
- OB FC Nov 2021 NLEDocument9 pagesOB FC Nov 2021 NLEAlyssa SaibiNo ratings yet
- Lesson Plan Preparing For Parenthood Pregnancy and Labor-1Document12 pagesLesson Plan Preparing For Parenthood Pregnancy and Labor-1Ting AlqNo ratings yet
- A Clinical Study On Oligohydramnios in The ThirdDocument23 pagesA Clinical Study On Oligohydramnios in The ThirdDickyNo ratings yet
- Midterm NotesDocument28 pagesMidterm NotesGen FranchesKyle Cortez ErigbuagasNo ratings yet
- Physical Examination For OBDocument63 pagesPhysical Examination For OBQuolette Constante87% (77)
- Maternal & Child Nursing: NNCM 107 Lilia B. DungalaDocument176 pagesMaternal & Child Nursing: NNCM 107 Lilia B. DungalaagentcasperNo ratings yet
- Case StudyDocument5 pagesCase StudyJui Perano100% (2)
- Amniotiv Fluid DisorderDocument22 pagesAmniotiv Fluid DisorderLiangkiuwiliu100% (1)
- AmniocentesisDocument10 pagesAmniocentesisDane Orilla100% (1)
- AbbreviationsDocument7 pagesAbbreviationsPallaviNo ratings yet
- Chapter 26Document84 pagesChapter 26Johanna Erazo Padilla100% (1)
- 648-672 CH21 Lowdermilk PDFDocument25 pages648-672 CH21 Lowdermilk PDFMark Anthony EspirituNo ratings yet
- Nursing Staff Development DepartmentDocument15 pagesNursing Staff Development DepartmentJohnmer AvelinoNo ratings yet
- TerminologyDocument38 pagesTerminologypandem soniyaNo ratings yet
- Amniotic Fluid DisordersDocument16 pagesAmniotic Fluid DisordersLytiana Williams100% (2)
- Partogram Case StudiesDocument6 pagesPartogram Case StudiesnyangaraNo ratings yet
- Assessment of Fetal Lung MaturityDocument16 pagesAssessment of Fetal Lung MaturitybenNo ratings yet
- Maternal and Child NursingDocument11 pagesMaternal and Child NursingKSY JanedoeNo ratings yet
- Partograph: By. Ronalyn A. Fabrigas, RN., MN Credits ToDocument36 pagesPartograph: By. Ronalyn A. Fabrigas, RN., MN Credits ToJmarie Brillantes Popioco100% (1)
- Research Article Risk Factors For Meconium Stained Amniotic Fluid and Its ImplicationsDocument4 pagesResearch Article Risk Factors For Meconium Stained Amniotic Fluid and Its ImplicationsAnonymous s8YWSzNo ratings yet