Professional Documents
Culture Documents
Local Anesthetic Techniques
Uploaded by
Zcsba AldehidOriginal Description:
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Local Anesthetic Techniques
Uploaded by
Zcsba AldehidCopyright:
Available Formats
Long Buccal Nerve
Long Buccal nerve passes between the two heads of the lateral pterygoid muscle and crosses in front of the anterior border of the ramus Provides sensory innervation to the buccal gingiva of the mandibular molars
Masseter and Auriculotemporal Nerves
Auriculotemporal Nerve The masseter nerve passes in front of the temporomandibular joint and enters the masseter muscle The auriculotemporal nerve passes behind the condylar neck to provide sensory innervation to the skin of the external auditory canal and anterior temple
Inferior Alveolar and Mental Nerves
Inferior Alveolar and Mental Nerves
IAN is the largest branch of the mandibular division Accompanied by the inferior alveolar artery which is branch of the internal maxillary artery Provides pulpal anesthesia to all teeth of the quadrant Exits the mandible via the mental foramina Divides into the mental and incisive branches Incisive branch provides pulpal anesthesia to the mandibular premolars, canines and incisors Mental nerve innervates skin of the chin and mucous membranes of the lower lip
Mylohyoid Branch
Mylohyoid nerve branches from the IAN prior to entry into the mandibular canal Runs forward in the mylohyoid groove to the mylohyoid muscle Motor to the mylohyoid muscle and anterior belly of the digastric Provides some fibers to skin of the mental protuberance May provide some innervation to mandibular incisors and possibly to the molars
Lingual Nerve
Lingual nerve branches off the mandibular nerve before entering the bone to reach the base of the tongue Proceeds anteriorly and loops medial to the Whartons duct of the submandibular gland Sensory to the anterior 2/3 of the tongue as well as taste via the chorda tympani nerve
TECHNIQUE
Local Anesthetic Injection Techniques
Do Not Inject Under the Periosteum PAINFUL!!!
Maxillary Infiltration Technique
Maxillary Infiltration Technique
Supraperiosteal Placement of Local Anesthetic
Posterior Superior Alveolar Nerve Block
Useful block for third, second and distobuccal root of first molar Risk of hematoma No bony landmarks Second injection required for mesiobuccal root of first molar
Target for PSA Injection
Middle Superior Alveolar Nerve
MSA nerve present in about 28% population Anesthetizes the maxillary premolars Used when infraorbital nerve block fails distal to the canine
Infraorbital Nerve Blockade
Not popular due to operator familiarity Highly successful and very safe technique Provides pulpal and buccal soft tissue anesthesia in 72% of patients Also anesthetizes lower eyelid, lateral nose and upper lip
Infraorbital Nerve Blockade
Palpate the inferior orbital rim and move inferiorly until reaching the infraorbital foramina Maintain finger position over the foramina and orient needle into the mucobuccal fold over the first premolar Approximate depth of insertion is 16 mm
Infraorbital Nerve Blockade
Greater Palatine Nerve Block
Nerve block will provide anesthesia to the posterior portion of the hard palate and overlying soft tissues as far as the first premolar Use a cotton swab to find the depression of the foramina Apply pressure to blanch tissue prior to injection Not necessary to deposit local anesthetic within the foramina
Area Anesthetized by Infraorbital Nerve Block
Nasopalatine Nerve Block
Will anesthetize the hard and soft tissues of the premaxilla including the area between the canines Single injection technique places needle directly into the incisive papilla Soft tissue is very adherent to bone and the region of the incisive papilla is very sensitive Multiple needle penetration technique first deposits local anesthetic into the labial frenum Second injection through the labial papilla between the central incisors towards the incisive foramina Third injection adjacent to the incisive foramina only if necessary
Maxillary Division Nerve Block
Also called Second Division Block Effective method of achieving profound anesthesia of hemimaxilla Approached by either the high tuberosity technique or the greater palatine approach Not indicated in children High incidence of hematoma from the high tuberosity approach No true bony landmarks Needle inserted to depth of 30 mm Aim for pterygopalatine fossa
Maxillary Division Nerve Block
Areas anesthetized:
maxillary teeth in quadrant overlying bone periodontium soft tissues of the hard palate and part of soft palate skin of the lower eyelid, side of nose, cheek and upper lip
Maxillary Division Nerve Block
Greater palatine approach can also be used Potential trauma to nerve from needle insertion More difficult to locate the greater palatine foramina Advance needle to depth of 30 mm 5 to 15% of canals will have obstructions that prevent passage of needle
Mandibular Infiltration
Useful predominately for the mandibular incisors and buccal tissues Effective because of thin alveolar bone Not reliable for anesthesia of the canine due to thicker cortical bone
Mandibular Infiltration
Mandibular Infiltration
Mental Nerve Block
Provides mostly sensory innervation to the buccal soft tissues anterior to the foramina of the lip/chin Least frequently used block Unreliable anesthesia of the premolars No need to enter foramina Pull tissue taut and may be able to visualize nerve branches
Mental Nerve Block
Long Buccal Nerve Block
Branch of the anterior division of V3 Required for surgical procedures involving the buccal soft tissues adjacent to the molars Success rate of nearly 100% due to location just below mucosa Low incidence of hematoma formation which can be controlled with direct pressure
Long Buccal Nerve Block
Inferior Alveolar Nerve Block: Direct Technique
Most frequently used nerve block in dentistry 15 to 20% rate of clinical failure Positive aspiration 10 to 15% Anesthetizes:
mandibular teeth to midline anterior 2/3 of tongue (Lingual n.) lingual soft tissues mental n. soft tissue distribution
Average depth of penetration is 20 to 25 mm
Inferior Alveolar Nerve Block: Direct Technique
Inferior Alveolar Nerve Block: Direct Technique
Zone of Injection for IAN Block Deposition of Local Anesthetic in the Pterygomandibular Space
Lingual Nerve Block
Lingual nerve block usually made in conjunction with the inferior alveolar nerve block Deposition of anesthetic upon withdrawal of needle Inject anesthetic when approximately half the needle length has been withdrawn Local from the IAN block will usually diffuse to the lingual nerve as well
Lingual Nerve Block
Akinosi Closed Mouth Mandibular Block
Used primarily in patients with trismus who require mandibular anesthesia Contraindicated in patients with infection or acute inflammation in region of injection Will provide sensory and motor nerve blockade if administered properly
Akinosi Closed Mouth Mandibular Block
Orient bevel away from bone Barrel of syringe held parallel with the maxillary occlusal plane Height of needle above the mucogingival junction of the maxillary third molar Advance needle about 25 mm into tissue measured from the maxillary tuberosity to the mid portion of the pterygomandibular space
Gow-Gates Mandibular Block GowTrue mandibular nerve block since it provides:
inferior alveolar lingual mylohyoid mental incisive auriculotemporal long buccal
Gow-Gates Mandibular Block GowNeedle is inserted at the distal of the maxillary second molar directed towards the tragus Advance the needle until bone is contacted at the neck of the mandibular condyle Average depth of penetration is 25 mm If bone is not contacted, withdraw and re-direct the reneedle Do not deposit local if bone has not been contacted
Higher rate of failure due to operator unfamiliarity Complications include hematoma formation and CN III, IV, and VI temporary paralysis
Extraoral Mandibular Block
Useful in cases of severe trismus when unable to perform a Direct IAN or Gow-Gates block GowCan be administered via the sigmoid notch or inferiorly from the chin
Local Complications of Local Anesthetics
Needle breakage Pain on injection Burning on injection Persistent anesthesia Trismus Hematoma Infection Sloughing of tissues Facial nerve paralysis Post-anesthetic intraoral lesions Post-
Systemic Complications of Local Anesthetics
Allergy Epinephrine effects Overdose (progression of symptoms)
slurred speech disorientation vomiting elevated heart and respiratory rate visual disturbances (blurring) auditory disturbances (tinnitus) loss of consciousness tonic clonic seizure activity depressed blood pressure, heart rate and breathing
The End
You might also like
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)From EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Rating: 4.5 out of 5 stars4.5/5 (119)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaFrom EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaRating: 4.5 out of 5 stars4.5/5 (265)
- The Little Book of Hygge: Danish Secrets to Happy LivingFrom EverandThe Little Book of Hygge: Danish Secrets to Happy LivingRating: 3.5 out of 5 stars3.5/5 (399)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryFrom EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryRating: 3.5 out of 5 stars3.5/5 (231)
- Grit: The Power of Passion and PerseveranceFrom EverandGrit: The Power of Passion and PerseveranceRating: 4 out of 5 stars4/5 (587)
- Never Split the Difference: Negotiating As If Your Life Depended On ItFrom EverandNever Split the Difference: Negotiating As If Your Life Depended On ItRating: 4.5 out of 5 stars4.5/5 (838)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeFrom EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeRating: 4 out of 5 stars4/5 (5794)
- Team of Rivals: The Political Genius of Abraham LincolnFrom EverandTeam of Rivals: The Political Genius of Abraham LincolnRating: 4.5 out of 5 stars4.5/5 (234)
- Shoe Dog: A Memoir by the Creator of NikeFrom EverandShoe Dog: A Memoir by the Creator of NikeRating: 4.5 out of 5 stars4.5/5 (537)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyFrom EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyRating: 3.5 out of 5 stars3.5/5 (2219)
- The Emperor of All Maladies: A Biography of CancerFrom EverandThe Emperor of All Maladies: A Biography of CancerRating: 4.5 out of 5 stars4.5/5 (271)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreFrom EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreRating: 4 out of 5 stars4/5 (1090)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersFrom EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersRating: 4.5 out of 5 stars4.5/5 (344)
- Her Body and Other Parties: StoriesFrom EverandHer Body and Other Parties: StoriesRating: 4 out of 5 stars4/5 (821)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceFrom EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceRating: 4 out of 5 stars4/5 (894)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureFrom EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureRating: 4.5 out of 5 stars4.5/5 (474)
- Acupressure Points For Weight LossDocument17 pagesAcupressure Points For Weight Lossconsaldradoo100% (2)
- The Unwinding: An Inner History of the New AmericaFrom EverandThe Unwinding: An Inner History of the New AmericaRating: 4 out of 5 stars4/5 (45)
- Efficient Strength Training by Matt BrzyckiDocument5 pagesEfficient Strength Training by Matt Brzyckigregorio919100% (2)
- The Yellow House: A Memoir (2019 National Book Award Winner)From EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Rating: 4 out of 5 stars4/5 (98)
- On Fire: The (Burning) Case for a Green New DealFrom EverandOn Fire: The (Burning) Case for a Green New DealRating: 4 out of 5 stars4/5 (73)
- Revised Manual Ligament Therapy - FoundationDocument38 pagesRevised Manual Ligament Therapy - FoundationKleberBattaglia100% (4)
- Body For Life - Abs TrainingDocument9 pagesBody For Life - Abs Trainingzulu22No ratings yet
- Anatomy of The Facial NerveDocument75 pagesAnatomy of The Facial NerveSerene Batra100% (2)
- Hip Arthroscopy Recovery ExercisesDocument5 pagesHip Arthroscopy Recovery ExercisesbekchievagNo ratings yet
- Head InjuriesDocument9 pagesHead InjuriesQasim HaleimiNo ratings yet
- Chest X Ray Techniques and PositioningDocument67 pagesChest X Ray Techniques and PositioningSandeep ChaudharyNo ratings yet
- Chapter 4. Muscular - System JeDocument55 pagesChapter 4. Muscular - System JeIvonike Lim100% (2)
- Cast and MoldsDocument11 pagesCast and Moldskaliente0118No ratings yet
- College of Physical Therapy Sem2Document10 pagesCollege of Physical Therapy Sem2karen magallanesNo ratings yet
- Exocad Brochure Anteriors ZRS-EnDocument23 pagesExocad Brochure Anteriors ZRS-EnAnderson Macena de Araujo100% (1)
- Mobility Aids With VideoDocument92 pagesMobility Aids With VideoRadha KrishnanNo ratings yet
- Range of Motion Exercises &Document47 pagesRange of Motion Exercises &Nikita Sharma100% (1)
- Brunnstrom ApproachDocument26 pagesBrunnstrom ApproachMohaChebiNo ratings yet
- Approaches in NeurosurgeryDocument226 pagesApproaches in NeurosurgeryJavier Andres Jacobo100% (2)
- Core Stix Instructional RoutinesDocument11 pagesCore Stix Instructional RoutinesAmber Riley100% (1)
- Párpado Duane'sDocument34 pagesPárpado Duane'sLuis Miguel Salazar AmatureNo ratings yet
- Safe exposure of the cervical esophagusDocument11 pagesSafe exposure of the cervical esophagusRoxa777No ratings yet
- Physical Examination in Orthopedi DR - ThomasDocument54 pagesPhysical Examination in Orthopedi DR - Thomasyulia manaweanNo ratings yet
- RPG Na Hernia DiscalDocument6 pagesRPG Na Hernia DiscalJoseph Dos SantosNo ratings yet
- 2.08 Brachial Region (Arm) - Compartments, Muscles, Nerves, and VesselsDocument3 pages2.08 Brachial Region (Arm) - Compartments, Muscles, Nerves, and VesselsDi CanNo ratings yet
- Rapid Entire Body Assessment (REBA) : General Result 12 Very HighDocument11 pagesRapid Entire Body Assessment (REBA) : General Result 12 Very HighflorentinoNo ratings yet
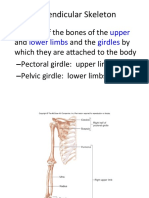
- Appendicular Skeleton: Upper Lower Limbs GirdlesDocument37 pagesAppendicular Skeleton: Upper Lower Limbs GirdlesAprilSensengNo ratings yet
- Spinal Cord Reflexes Protect the BodyDocument2 pagesSpinal Cord Reflexes Protect the BodyriyanNo ratings yet
- BY DR Jahangir Hammad BDS, FcpsDocument110 pagesBY DR Jahangir Hammad BDS, FcpsAtika Iftikhar MirNo ratings yet
- Normal PE Sample Write-UpDocument5 pagesNormal PE Sample Write-UpMikie BausinNo ratings yet
- Carly Green Bench Press Journal 2007Document5 pagesCarly Green Bench Press Journal 2007RosaneLacerdaNo ratings yet
- Constraints On Somatotopic Organization in The Primary Motor CortexDocument19 pagesConstraints On Somatotopic Organization in The Primary Motor CortexYnahatNo ratings yet
- p3 Science Summary Chapter 1 and 2Document2 pagesp3 Science Summary Chapter 1 and 2wilson0% (1)