Professional Documents
Culture Documents
28 C.fracture of Spine
Uploaded by
Noor Hazilla WatyOriginal Description:
Original Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
28 C.fracture of Spine
Uploaded by
Noor Hazilla WatyCopyright:
Available Formats
28.d.
Fracture of spine: first aid, classification and therapy
First Aid: Fracture of the Spine spinal cord may be crushed, cut, or otherwise damaged so severely that death or paralysis will result.However, if the fracture occurs in such a way that the spinal cord is not seriously damaged, there is a very good chance of complete recoveryPROVIDED the victim is properly cared for. Any twisting or bending of the neck or back, whether due to the original injury or carelessness from handling later, is likely to cause irreparable damage to the spinal cord. The primary symptoms of a fractured spine are pain, shock, and paralysis. o PAIN is likely to be acute at the point of fracture. It may radiate to other parts of the body. SHOCK is usually severe, but (as in all injuries) the symptoms maybe delayed for some time. o PARALYSIS occurs if the spinal cord is seriously damaged. If the vic-tim cannot move the legs, feet, or toes, the fracture is probably in the back; if the fingers will not move, the neck is probably broken. Remember that a spinal fracture does not always injure the spinal cord, so the victim is not always paralyzed.Any person who has an acute pain in the back or the neck following an injury should be treated as though there is a fractured spine, even if there are no other symptoms. First aid treatment for all spinal fractures,whether of the neck or of the back, has two primary purposes: o (1) to minimize shock and o (2) toprevent further injury to the spinal cord. Keep the victim comfortably warm. Do not attempt to keep the victim in the position ordinarily used for the treatment of shock, because it might cause further damage to the spinal cord. Just keep the victim lying flat and do NOT attempt to lower the head. To avoid further damage to the spinal cord,DO NOT MOVE THE VICTIM UNLESS IT IS ABSOLUTELY ESSENTIAL. If the victims life is threatened in the present location or transportation is necessary to receive medical attention,then of course you must move the victim.However, if movement is necessary, be sure that you do it in a way that will cause the least possible damage. DO NOT BEND OR TWIST THEVICTIMS BODY, DO NOT MOVE THE HEADFORWARD, BACKWARD, OR SIDEWAYS,AND DO NOT UNDER ANY CIRCUM-STANCES ALLOW THE VICTIM TO SIT UP. If it is necessary to transport a person who has suffered a fracture of the spine, follow these general rules:1.2.3.If the spine is broken at the NECK, the vic-tim must be transported lying on the back,FACE UP. Place pillows or sandbagsbeside the head so that it cannot turn toeither side. Do NOT put pillows or pad-ding under the neck or head.If you suspect that the spine is fracturedbut do not know the location of the break,treat the victim as though the neck isbrokeni.e., keep the victim supine. Ifboth the neck and the back are broken,keep the victim supine.No matter where the spine is broken, USEA FIRM SUPPORT IN TRANSPORT-ING THE VICTIM. Use a rigid stretcher,or a door, shutter, wide board, etc. Padthe support carefully and put blankets bothunder and over the victim. Use cravatbandages or strips of cloth to secure the vic-tim firmly to the support. o
CLASSIFICATION AND MANAGEMENT OF SPINAL AND SPINAL CORD INJURIES General points In cases of neurological injury, initial intervention is aimed at reducing the secondary injury, preventing further deterioration and allowing return of neurological function in some cases. Most spinal trauma centres no longer use steroids in cases of spinal cord injury as there is no evidence that they work.
Basic management principles Spinal realignment In cases of cervical spine subluxation or dislocation, skull tongs are used to apply traction. The alternative is open reduction and operative realignment using internal fixation . A halo brace can be used to perform a closed realignment of cervical fractures . Stabilisation If a spinal fracture or dislocation is unstable (moves abnormally when stressed) there is a risk of new or further neurological injury as well as painful post-traumatic deformity. Many spinal injuries can be managed non-operatively with external support but, when possible, internal fixation should be used. The only absolute indication for surgery in spinal trauma is deteriorating neurological function. All other indications are relative. Early stabilisation has the advantage that it allows early mobilisation of the patient. Decompression of the neural elements Spinal realignment is important in this regard. Compression of the cord by bone and/or disc material requires surgical removal SPECIFIC SPINAL INJURIES Upper cervical spine (skull to C2) Craniocervical dislocation This injury is the consequence of high-energy trauma and is usually fatal. It may be anterior, posterior or vertical (Fig. 24.23). Powers ratiois used to assess skull translation. In survivors, careful occipitocervical fusion is required. A halo braceshould be applied before surgery to prevent intraoperative dislocation. Atlantoaxial instability The most common form is a rotatory subluxation in children. This is usually of spontaneous onset but can be traumatic. The 3 months followed by flexionextension stress radiography to check stability. Persistent C1/2 instability will need C1/2 or occiputC2 fusion. Odontoid fractures There are three types of odontoid fracture (Fig. 24.27). o Type I fractures are uncommon and are usually stable, requiring no immobilisation. o Type II fractures may fail to unite, particularly those with significant displacement on presentation and those in the elderly. o Type III fractures extend into the C2 vertebral body and usually readily unite. Neurological injury is rare. The majority of acute injuries are treated non-operatively in a halo jacket for 3 months. Internal fixation with an anterior compression screw is indicated in displaced fractures in younger patients with good bone quality (Fig. 24.28). Posterior C1/2 fusion is required in cases of non-union. Elderly patients often develop a fibrous pseudoarthrosis that is relatively stable and does not require surgery. Hangmans fracture This injury can be considered as a traumatic spondylolisthesis of C2/3 resulting from bilateral C2 pedicle fractures secondary to hyperextension (Fig. 24.29). The majority can be treated nonoperatively in a halo jacket or brace. Those with significant displacement or associated facet dislocation are treated operatively,usually with posterior stabilisation. Subaxial cervical spine (C3C7) The pattern of lower cervical spine injury depends on the mechanism of trauma. Many of the more severe injuries are associated with spinal cord injury. Wedge fracture This results from hyperflexion and is usually stable without neurological injury. It is treated in a brace or halo for 3 months.
Burst fracture This occurs secondary to axial loading of the cervical spine. Bony fragments may explode into the spinal canal and cause neurological injury (Fig. 24.30a). Surgical intervention may be required to remove the fractured vertebral body, decompress the spinal cord and then stabilise with internal fixation (Fig. 24.30b). Burst fractures without neurological deficit can be treated non-operatively in a halo jacket. Tear-drop fracture The mechanism of injury is hyperextension. Unstable fractures require operative treatment. Facet subluxation/dislocation The pattern of injury ranges from facet subluxation, through unifacetal dislocation to bifacetal dislocation (Fig. 24.31). Bifacetal dislocation is associated with spinal cord injury in the majority of cases. The mechanism of injury is a combination of axial loading and flexion leading to compression at the anterior aspect of the spine and distraction of the posterior elements. The majority are pure ligamentous injuries with associated disruption of the intervertebral intervertebral disc. Surgical stabilisation is required in most cases; awake, closed reduction with skeletal traction is recommended when possible. In cases of incomplete paralysis or normal neurology, a pre-traction MRI should be considered to identify disc herniations that may then press on the cord and damage it during reduction (Summary box 24.8). Thoracic and thoracolumbar fractures Fractures that are highly unstable with an associated risk of neurological deficit should be fixed surgically. The AO (Arbeitsgemeinschaft fr Osteosynthesefragen) classifies fractures into three main types, A, B and C, with injuries becoming progressively more unstable from A to C. There is also an increasing risk of associated neurological injury. o Type A fractures primarily involve the vertebral body. o Type B injuries have additional distraction/disruption of the posterior elements and o type C injuries are rotational. The majority of type B and type C injuries require surgical stabilisation. Burst fractures are included in type A. Thoracic spine (T1T10) Osteoporotic wedge compression fractures in the elderly are the most common injury in this group. These are stable so can be treated symptomatically. Fractures that remain symptomatic for more than 6 weeks can be treated with percutaneousbone cement augmentation, known as vertebroplasty.Specialised balloons can also be inserted and inflated in an attempt to restore vertebral height (kyphoplasty) and relieve pain (Fig. 24.32). The combination of thoracic spine disruption and a sterna fracture (Fig. 24.33) carries a significant risk of aortic rupture. Multiple posterior rib fractures and rib dislocations above and below a thoracic spinal injury signify a major rotational injury to the chest and are associated with vascular injury and significant pulmonary contusion (Fig. 24.34). Upper thoracic spinal column injuries can be difficult to diagnose with plain radiography. High-quality CT sagittal reformats are best. Posterior instrumentation is indicated in almost all unstable thoracic spinal injuries as braces do not provide adequate stability and the risk of neurological deterioration can be considerable. Thoracolumbar spinal fractures (T11S1) The thoracolumbar junction is prone to injury as it represents a transition zone from fixed to mobile segments. There is a wide spectrum of possible injuries, ranging from minor wedge fractures to spinal dislocation (Fig. 24.35). Burst fractures o These are comminuted fractures of the vertebral body. The distance between the pedicles is widened and bone is retropulsed into the spinal canal (Fig. 24.36). o Many of these fractures can be treated non-operatively.
Surgical intervention is indicated when there is neurological compromise or the fracture is unstable. Chance fractures o These are flexiondistraction injuries and are classically associated with the use of lap belts (Fig. 24.38). o They may be bony or soft tissue in nature and predominantly occur at the thoracolumbar junction. o Duodenal, pancreatic and/or aortic rupture can occur in these injuries and there must be a high index of suspicion
You might also like
- Neck Trauma, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsFrom EverandNeck Trauma, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsNo ratings yet
- Principles of Spine Trauma and Spinal Deformities PDFDocument34 pagesPrinciples of Spine Trauma and Spinal Deformities PDFVirlan Vasile CatalinNo ratings yet
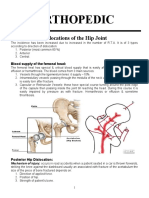
- Orthopedic: Dislocations of The Hip JointDocument16 pagesOrthopedic: Dislocations of The Hip JointAnmarNo ratings yet
- Spine InjuriesDocument58 pagesSpine InjuriesVinwin777No ratings yet
- Hip Joint DislocationDocument19 pagesHip Joint Dislocationshaoib.grandyNo ratings yet
- REFERAT Lumbar Compression FractureDocument25 pagesREFERAT Lumbar Compression FractureTaufik Ghockil ZlaluwNo ratings yet
- Seminar On Upper Limb FractureDocument166 pagesSeminar On Upper Limb FractureArko dutta100% (1)
- Upper Limb Fracture GuideDocument90 pagesUpper Limb Fracture Guideatikah_jamilNo ratings yet
- Orthopedic: Lec.11 DR - Hasan Abdulhadi.MDocument10 pagesOrthopedic: Lec.11 DR - Hasan Abdulhadi.MninaNo ratings yet
- Mode of InjuryDocument48 pagesMode of InjuryirfanzukriNo ratings yet
- Clavicle FractureDocument33 pagesClavicle FractureNitin AggarwalNo ratings yet
- Broken Neck (Hangman's Fracture): Causes, Symptoms and TreatmentDocument5 pagesBroken Neck (Hangman's Fracture): Causes, Symptoms and TreatmentFatima RizwanNo ratings yet
- Hip DislocationDocument4 pagesHip DislocationcrunkestNo ratings yet
- Fracture FemurDocument28 pagesFracture FemurKulsoom ShahNo ratings yet
- LBM 4 - Signs, Classification, Diagnosis and Complications of Pelvic FracturesDocument6 pagesLBM 4 - Signs, Classification, Diagnosis and Complications of Pelvic FracturesindahsariNo ratings yet
- Spinalinjuries 180518121456Document40 pagesSpinalinjuries 180518121456Akash KoulNo ratings yet
- Frienchzel Joy A. Asis Group 3 BSN 3-ADocument14 pagesFrienchzel Joy A. Asis Group 3 BSN 3-AKenneth Louis GalizaNo ratings yet
- Upper Extremity Injuries in Youth Sports: Jorge E. Go Mez, MS, MDDocument34 pagesUpper Extremity Injuries in Youth Sports: Jorge E. Go Mez, MS, MDАлексNo ratings yet
- Disorders of The Sternoclavicular Joint: SoulderDocument14 pagesDisorders of The Sternoclavicular Joint: SoulderFillipe AgraNo ratings yet
- Elbow Dislocation: Severe Dislocations, The Blood Vessels and Nerves That Travel Across The Elbow May Be Injured. IfDocument15 pagesElbow Dislocation: Severe Dislocations, The Blood Vessels and Nerves That Travel Across The Elbow May Be Injured. IftelefixeroNo ratings yet
- CHAPTER 2 Injuries of The PelvisDocument19 pagesCHAPTER 2 Injuries of The PelvisNabeelNo ratings yet
- Cedera Medulla SpinalisDocument49 pagesCedera Medulla SpinalisDimas Nugroho NugrohoNo ratings yet
- Fractures: Mary Grace B. Gutierrez Resti Mariano Ma. Cindy O. BautistaDocument50 pagesFractures: Mary Grace B. Gutierrez Resti Mariano Ma. Cindy O. BautistaJustin Ahorro-DionisioNo ratings yet
- Spinal Cord Injury ManagementDocument49 pagesSpinal Cord Injury ManagementAtika NajlaNo ratings yet
- Fractures of Clavicle AserDocument44 pagesFractures of Clavicle AserHeba ElgoharyNo ratings yet
- Elbow Pain.Document47 pagesElbow Pain.salmankhan09215No ratings yet
- Adult Hip Fracture-Dislocation GuideDocument69 pagesAdult Hip Fracture-Dislocation GuideKaizar Ennis100% (1)
- Surgical Stabilization of SpineDocument4 pagesSurgical Stabilization of SpineMaria Jonnalin SantosNo ratings yet
- Acetabulum FractureDocument32 pagesAcetabulum FracturePhysiotherapist AliNo ratings yet
- Spinal Cord InjuryDocument9 pagesSpinal Cord Injuryta CNo ratings yet
- ORIF Radius and Ulna ProcedureDocument7 pagesORIF Radius and Ulna ProcedurealcojonicNo ratings yet
- Лекция № 12 англDocument31 pagesЛекция № 12 англchai rinNo ratings yet
- Hip Fractures-Orthoinfo - AaosDocument9 pagesHip Fractures-Orthoinfo - Aaosapi-228773845No ratings yet
- Pathology Mechanism: Jefferson Fracture Is The Eponymous Name Given To A Burst Fracture ofDocument25 pagesPathology Mechanism: Jefferson Fracture Is The Eponymous Name Given To A Burst Fracture ofAtikah FairuzNo ratings yet
- Lower Limb InjuriesDocument47 pagesLower Limb InjuriesDaisyyhyNo ratings yet
- Traumatic Hip Dislocation: A ReviewDocument6 pagesTraumatic Hip Dislocation: A ReviewAna HurtadoNo ratings yet
- OrifDocument24 pagesOrifkier khierNo ratings yet
- Trauma - Intertrochanteric Fracture - RustiniDocument7 pagesTrauma - Intertrochanteric Fracture - Rustinidedyalkarni08No ratings yet
- Dislocations: Diagnosis, Management, and Complications: Marvin H. Meyers, M.D.Document12 pagesDislocations: Diagnosis, Management, and Complications: Marvin H. Meyers, M.D.Unoscientris StupaNo ratings yet
- ScoliosisDocument18 pagesScoliosisMj EnofnaNo ratings yet
- 018 OrthopedicsDocument16 pages018 OrthopedicsAhmed Zaghw92% (13)
- Upper Cervical Injuries Diagnosis and TreatmentDocument36 pagesUpper Cervical Injuries Diagnosis and TreatmentesterhsNo ratings yet
- Shoulder DislocationDocument28 pagesShoulder DislocationQueen SofiaNo ratings yet
- Introduction of FractureDocument80 pagesIntroduction of Fracturealsead798No ratings yet
- تروما محاضرة 1Document58 pagesتروما محاضرة 1202003339No ratings yet
- Gadline PrsentationDocument12 pagesGadline PrsentationsumardiNo ratings yet
- Clavicle AO Surgery Reference (2023)Document399 pagesClavicle AO Surgery Reference (2023)Wael GabrNo ratings yet
- Understanding Intertrochanteric Fractures of the FemurDocument12 pagesUnderstanding Intertrochanteric Fractures of the FemurEinz Nur Amalyah IdrusNo ratings yet
- Pelvic Injruies 2Document57 pagesPelvic Injruies 2King salehNo ratings yet
- Anatomy of Spinal CordDocument43 pagesAnatomy of Spinal CordGargi MPNo ratings yet
- Pelvic Injruies 1Document43 pagesPelvic Injruies 1King salehNo ratings yet
- Exogenous Spinal Trauma-Surgical Therapy and AftercareDocument8 pagesExogenous Spinal Trauma-Surgical Therapy and Aftercaretaner_soysurenNo ratings yet
- Introduction To Fracture: Parathyroid Hormone CalcitoninDocument36 pagesIntroduction To Fracture: Parathyroid Hormone CalcitoninArlene Ferrer100% (1)
- Sport Injury in Children (Short)Document3 pagesSport Injury in Children (Short)Ribka TheodoraNo ratings yet
- Intertrochanter Femur Fracture: M.Akhyar Baharuddin 20194010011Document23 pagesIntertrochanter Femur Fracture: M.Akhyar Baharuddin 20194010011Muhammad AkhyarNo ratings yet
- Schwartz Ortho NotesDocument16 pagesSchwartz Ortho Notesfsf50% (2)
- Cervical Radiculopathy Symptoms, Causes, and TreatmentDocument15 pagesCervical Radiculopathy Symptoms, Causes, and TreatmentRandi SukmanaNo ratings yet
- Orthopaedic Surgery Fractures and Dislocations: Tomas Kurakovas MF LL Group 29Document13 pagesOrthopaedic Surgery Fractures and Dislocations: Tomas Kurakovas MF LL Group 29Tomas Kurakovas100% (1)
- Spinal Immobilization: By: Hatem AlsrourDocument16 pagesSpinal Immobilization: By: Hatem Alsrourhatem alsrour100% (2)
- Broken Neck GuideDocument7 pagesBroken Neck GuideSulla FelixNo ratings yet
- Anatomy Physiology and Disease For The Health Professions 3rd Edition Booth Test Bank Full Chapter PDFDocument63 pagesAnatomy Physiology and Disease For The Health Professions 3rd Edition Booth Test Bank Full Chapter PDFrelatermotifef4oq100% (12)
- 0070412359Document470 pages0070412359Victor Galvez100% (11)
- Key Topics in Ortho Surgry PM 2Document352 pagesKey Topics in Ortho Surgry PM 2sharu429167% (3)
- The Anatomy of the Face and NeckDocument74 pagesThe Anatomy of the Face and Neckhazell_aseronNo ratings yet
- Blood Supply To The Human Spinal Cord. I. Anatomy and HemodynamicsDocument13 pagesBlood Supply To The Human Spinal Cord. I. Anatomy and HemodynamicsAnusha SebastianNo ratings yet
- Mrcs Part B Anatomy Stations 11 16 Compilation With Solution 2022Document68 pagesMrcs Part B Anatomy Stations 11 16 Compilation With Solution 2022Pritam RoyNo ratings yet
- Peifu Tang (editor), Hua Chen (editor) - Orthopaedic Trauma Surgery_ Volume 3_ Axial Skeleton Fractures and Nonunion (2023, Springer) - libgen.liDocument226 pagesPeifu Tang (editor), Hua Chen (editor) - Orthopaedic Trauma Surgery_ Volume 3_ Axial Skeleton Fractures and Nonunion (2023, Springer) - libgen.liThiago Longo MoraesNo ratings yet
- Skull PositioningDocument10 pagesSkull PositioningShionna MandyNo ratings yet
- Massage Therapy School ProgramDocument270 pagesMassage Therapy School ProgramLimarOrravanNo ratings yet
- Brachial Plexus InjuriesDocument346 pagesBrachial Plexus InjuriesvinaymanNo ratings yet
- Acute Spinal Cord Injuries - PDFDocument9 pagesAcute Spinal Cord Injuries - PDFEmanuel31No ratings yet
- Clinical DX in PMR Case by CaseDocument143 pagesClinical DX in PMR Case by CaseNayem comNo ratings yet
- Anatomy and Physiology Test 2 PrepDocument21 pagesAnatomy and Physiology Test 2 PrepNicholas SirunoNo ratings yet
- Assessment Question 1. All Are True About Vertebrae Levels EXCEPTDocument13 pagesAssessment Question 1. All Are True About Vertebrae Levels EXCEPTDevsya DodiaNo ratings yet
- Traumatic Spinal Cord Injury 2018Document16 pagesTraumatic Spinal Cord Injury 2018LEONARDO ANTONIO CASTILLO ZEGARRANo ratings yet
- Form 5 Biology (Chapter 2: Locomotion & Support)Document15 pagesForm 5 Biology (Chapter 2: Locomotion & Support)Gerard Selvaraj100% (23)
- Anatomy of ScoliosisDocument6 pagesAnatomy of ScoliosisDaniel MañalacNo ratings yet
- Animal Anatomy For Artist PDFDocument257 pagesAnimal Anatomy For Artist PDFGioteya95% (20)
- Gross Comparative Anatomy of Domestic AnimalsDocument51 pagesGross Comparative Anatomy of Domestic AnimalsLila Loureen AlkuinoNo ratings yet
- Muscle Origins, Insertions, Actions, and InterventionsDocument15 pagesMuscle Origins, Insertions, Actions, and InterventionsJoseph Kachelman100% (3)
- Jurnal FixnDocument8 pagesJurnal FixnummulNo ratings yet
- Ayush 5418206Document5 pagesAyush 5418206ਅਰਪਣਸਿੰਘNo ratings yet
- Anatomy of The Spine: Cervical (Neck) - The Main Function of The CervicalDocument5 pagesAnatomy of The Spine: Cervical (Neck) - The Main Function of The Cervicalid_pandianNo ratings yet
- Rom MMT Trunk Study Sheet 1Document3 pagesRom MMT Trunk Study Sheet 1api-242889989No ratings yet
- Week 1 and 2 PCP Workbook QuestionsDocument4 pagesWeek 1 and 2 PCP Workbook Questionsapi-479717740100% (1)
- Star Health Premier - Version 1.0 - Mar - 22Document33 pagesStar Health Premier - Version 1.0 - Mar - 22Anoop AravindNo ratings yet
- General Safety Guidelines For Yoga ClassesDocument2 pagesGeneral Safety Guidelines For Yoga Classescarmen13vmcNo ratings yet
- 1201 PDFDocument6 pages1201 PDFHARIKRISHNAN RNo ratings yet
- St. Paul University Philippines: Head-To-Toe Physical AssessmentDocument33 pagesSt. Paul University Philippines: Head-To-Toe Physical AssessmentKeith AquinoNo ratings yet
- Spinal Cord ExternalDocument33 pagesSpinal Cord ExternalCosplay AccountNo ratings yet