Professional Documents
Culture Documents
Definition of JVP
Uploaded by
Mimi ChukwuOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Definition of JVP
Uploaded by
Mimi ChukwuCopyright:
Available Formats
The jugular venous pressure (JVP, sometimes referred to as jugular venous pulse) is the indirectly observed pressure over
the venous system via visualization of the internal jugular vein. It can be useful in the differentiation of different forms of heart and lung disease. Classically three upward deflections and two downward deflections have been described.
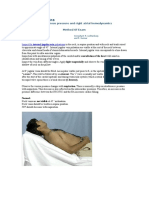
Visualization The veins of the neck, viewed from in front. The patient is positioned under 45, and the filling level of the jugular vein determined. Visualize the internal jugular vein when looking for the pulsation. In healthy people, the filling level of the jugular vein should be less than 3 centimetres vertical height above the sternal angle. A pen-light can aid in discerning the jugular filling level by providing tangential light.
Above, it lies upon the rectus capitis lateralis, behind the internal carotid artery and the nerves passing through the jugular foramen; lower down, the vein and artery lie upon the same plane, the glossopharyngeal and hypoglossal nerves passing forward between them; the vagus descends between and behind the vein and the artery in the same sheath (the carotid sheath), and the accessory runs obliquely backward, superficial or deep to the vein. At the root of the neck, the right internal jugular vein is a little distance from the common carotid artery, and crosses the first part of the subclavian artery, while the left internal jugular vein usually overlaps the common carotid artery. The left vein is generally smaller than the right, and each contains a pair of valves, which are placed about 2.5 cm above the termination of the vessel.
The JVP is easiest to observe if one looks along the surface of the sternocleidomastoid muscle, as it is easier to appreciate the movement relative to the neck when looking from the side (as opposed to looking at the surface at a 90 degree angle). Like judging the movement of an automobile from a distance, it is easier to see the movement of an automobile when it is crossing one's path at 90 degrees (i.e. moving left to right or right to left), as opposed to coming toward one.
Pulses in the JVP are rather hard to observe, but trained cardiologists do try to discern these as signs of the state of the right atrium.
The mean pressure in the right atrium is normally <7mmhg (9cm="" h2o);="" as="" the="" sternal="" angle="" is="" approximately="" 5cm="" above="" the="" right="" atrium,="" the="" normal="" jugular="" pressure="" pulse="" should="" not="" be="">4cm (9cm-5cm) above the sternal angle. Therefore, in a healthy patient with normal right atrial pressure: - Sitting at a 45 degs angle - the transition point between the distended vein and the collapsed vein may or may not be visible; if it is visible, the pulsation will be seen just above the clavicle; - Lying flat - the jugular vein will be distended and the pulsation will not be visible; - Sitting upright - the upper part of the vein will be collapsed and the transition point between it and the distended vein will be obscured, so the pulsation will not be seen
THE PROCEDURE - Explain the procedure to the patient. - Ensure there is adequate lighting. - Adopt a position on the patients right. - While ensuring privacy and maintaining the patients dignity, expose the upper chest. Remove any restrictive clothing from around the patients neck and chest. - Position the patient at an angle of 45 degs, leaving one pillow under the head . - Ask the patient to turn her or his head to the left . - Observe the level of the jugular venous pulsations just above the clavicle. - Measure the vertical distance (cm) between the sternal angle (manubrio sternal joint or angle of Louis) and the highest visible level of jugular vein pulsation. The normal distance is <4cm; add="" 5cm="" to="" this="" because="" the="" right="" atrium="" is="" 5cm="" below="" the="" sternal="">
- If it is difficult to see the jugular venous pulsation, shine a bright light directly onto the patients neck. - If it is still difficult to see jugular venous pulsation or there is uncertainty whether the pulsation is venous or arterial, some authorities recommend gentle compression on the right upper quadrant of the abdomen. This will transiently increase venous pressure resulting in a more prominent internal jugular vein. Venous pulsation usually returns to normal after a few seconds (even with continued abdominal pressure); if it remains elevated this suggests right-sided heart failure. - Document the findings of whether the jugular venous pulsation is visible and, if so, whether it is normal or elevated
The JVP and carotid pulse can be differentiated several ways:
multiphasic - the JVP "beats" twice (in quick succession) in the cardiac cycle. In other words, there are two waves in the JVP for each contractionrelaxation cycle by the heart. The first beat represents that atrial contraction (termed a) and second beat represents venous filling of the right atrium against a closed tricuspid valve (termed v) and not the commonly mistaken 'ventricular contraction'. These wave forms may be altered by certain medical conditions; therefore, this is not always an accurate way to differentiate the JVP from the carotid pulse. The carotid artery only has one beat in the cardiac cycle.
non-palpable
- the JVP cannot be palpated. If one feels a pulse in the neck, it is generally the common carotid artery. occludable - the JVP can be stopped by occluding the internal jugular vein by lightly pressing against the neck. It will fill from above. varies with head-up-tilt (HUT) - the JVP varies with the angle of neck. If a person is standing, his JVP appears to be lower on the neck (or may not be seen at all because it is below the sternal angle). The carotid pulse's location does not vary with HUT.
varies
with respiration - the JVP usually decreases with deep inspiration. Physiologically, this is a consequence of the FrankStarling mechanism as inspiration decreases the thoracic pressure and increases blood movement into the heart (venous return), which a healthy heart moves into the pulmonary circulation.
The jugular venous pulsation has a biphasic waveform.
The " a " wave corresponds to right Atrial contraction and ends synchronously with the carotid artery pulse. The peak of the 'a' wave demarcates the end of atrial systole. The " c " wave corresponds to right ventricular Contraction causing the triCuspid valve to bulge towards the right atrium. The " x " descent follows the 'a' wave and corresponds to atrial relaXation and rapid atrial filling due to low pressure.
JVP Waveform
The " x' " (x prime) descent follows the 'c' wave and occurs as a result of the right ventricle pulling the tricuspid valve downward during ventricular systole. The x' (x prime) descent can be used as a measure of right ventricle contractility. The " v " wave corresponds to Venous filling when the tricuspid valve is closed and venous pressure increases from venous return - this occurs during and following the carotid pulse. The " y " descent corresponds to the rapid emptYing of the atrium into the ventricle following the opening of the tricuspid valve.
Certain wave form abnormalities, include "Cannon awaves", or increased amplitude 'a' waves, are associated with AV dissociation (third degree heart block), when the atrium is contracting against a closed tricuspid valve, or even in ventricular tachycardia. Another abnormality, "c-v waves", can be a sign of tricuspid regurgitation. The absence of 'a' waves may be seen in atrial fibrillation.
An
elevated JVP is the classic sign of venous hypertension (e.g. right-sided heart failure). JVP elevation can be visualized as jugular venous distension, whereby the JVP is visualized at a level of the neck that is higher than normal. The paradoxical increase of the JVP with inspiration (instead of the expected decrease) is referred to as the Kussmaul sign, and indicates impaired filling of the right ventricle. The differential diagnosis of Kussmaul's sign includes constrictive pericarditis, restrictive cardiomyopathy, pericardial effusion, and severe right-sided heart failure.
Raised
JVP, normal waveform Bradycardia Fluid overload Heart Failure Raised JVP, absent pulsation Superior vena cava syndrome Large 'a' wave (increased atrial contraction pressure) tricuspid stenosis Right heart failure Pulmonary hypertension Cannon 'a' wave (atria contracting against closed tricuspid valve) Atrial flutter Premature atrial rhythm (or tachycardia) third degree heart block Ventricular ectopics Ventricular tachycardia Absent 'a' wave (no unifocal atrial depolarisation) atrial fibrillation
Large
'v' wave (c-v wave) Tricuspid regurgitation Slow 'y' descent Tricuspid stenosis Cardiac Tamponade Prominent & Deep 'y' descent Constrictive pericarditis Parodoxical JVP (Kussmaul's sign: JVP rises with inspiration, drops with expiration) Pericardial effusion Constrictive pericarditis Pericardial tamponade
You might also like
- Jugular Venous PressureDocument5 pagesJugular Venous PressureYusran YusoffNo ratings yet
- Jugular Venous PressureDocument9 pagesJugular Venous Pressuremoh86-No ratings yet
- Jugular Venous Pressure: Congestive Heart FailureDocument5 pagesJugular Venous Pressure: Congestive Heart FailureKrisSentosaNo ratings yet
- Jugular Venous Pressure: Syed Farrukh UmairDocument30 pagesJugular Venous Pressure: Syed Farrukh UmairsfumairNo ratings yet
- JVP Rajesh - 2Document16 pagesJVP Rajesh - 2bminor7No ratings yet
- JVPDocument5 pagesJVPYhr YhNo ratings yet
- Cardiovascular System, Questioning and Examination of Patients With Pathology of The Cardiovascular System.Document20 pagesCardiovascular System, Questioning and Examination of Patients With Pathology of The Cardiovascular System.ASAP teleNo ratings yet
- JVP Examination For GPDocument43 pagesJVP Examination For GPNovenZefanyaNo ratings yet
- Peripheral Arterial Pulse and JVP: Sweta Sah Intern JMCTHDocument40 pagesPeripheral Arterial Pulse and JVP: Sweta Sah Intern JMCTHsahsweta67No ratings yet
- Examination of Neck VeinsDocument6 pagesExamination of Neck VeinsCaleb biiNo ratings yet
- Lung Physical DiagnosisDocument68 pagesLung Physical DiagnosisfaberNo ratings yet
- Jugular VeinsDocument13 pagesJugular VeinsstudymedicNo ratings yet
- JVP and HS .-2Document93 pagesJVP and HS .-2Sahithi ChittepuNo ratings yet
- 42020E58E9FE69687The20Jugular20Venous20Pressure20and20Pulse20Contour20 20Clinical20Methods20 20NCBI20BookshelfDocument6 pages42020E58E9FE69687The20Jugular20Venous20Pressure20and20Pulse20Contour20 20Clinical20Methods20 20NCBI20BookshelfMayda MendozaNo ratings yet
- Cardiovascular System ExaminationDocument20 pagesCardiovascular System ExaminationAditya CherukuriNo ratings yet
- Cardio 2Document2 pagesCardio 2Erika De JesusNo ratings yet
- CardiologyDocument62 pagesCardiologysee yinNo ratings yet
- Cardiovascular System: By: S@JDocument35 pagesCardiovascular System: By: S@JD TekNo ratings yet
- Aortic Valve DiseaseDocument25 pagesAortic Valve Diseasesagungw93No ratings yet
- Pericardial Disease: Adel Hasanin Ahmed 1Document5 pagesPericardial Disease: Adel Hasanin Ahmed 1Shaz ChindhyNo ratings yet
- Cardiovascular ExaminationDocument13 pagesCardiovascular ExaminationBitu JaaNo ratings yet
- Emergency UltrasoundDocument32 pagesEmergency UltrasoundChoga ArlandoNo ratings yet
- Physical Assessment of Patient With Cardiovascular DisorderDocument3 pagesPhysical Assessment of Patient With Cardiovascular Disordermichelle marquezNo ratings yet
- JVP Examination For GPDocument43 pagesJVP Examination For GPYonathanHasudunganNo ratings yet
- 0 ECG - 1st - Book GLOSSARY (12 21.1 2014) LOCKDocument16 pages0 ECG - 1st - Book GLOSSARY (12 21.1 2014) LOCKShehnaaz KhanNo ratings yet
- Angelina A Joho MSC in Critical Care and TraumaDocument50 pagesAngelina A Joho MSC in Critical Care and TraumaZabron LuhendeNo ratings yet
- 04-The Cardiac Cycle - Wigger's Diagram (J Swanevelder)Document6 pages04-The Cardiac Cycle - Wigger's Diagram (J Swanevelder)Patrick WilliamsNo ratings yet
- Valvular Heart DiseaseDocument27 pagesValvular Heart DiseaseOwen J. WieseNo ratings yet
- Jugular Venous PulseDocument21 pagesJugular Venous Pulsevidishmalaviya300No ratings yet
- BST Dr. AnnaDocument12 pagesBST Dr. AnnaKomang AryaNo ratings yet
- JVP Examination For GP Interna NewDocument43 pagesJVP Examination For GP Interna NewAlexander Lukky SugondoNo ratings yet
- Approach To Cardiac MurmursDocument11 pagesApproach To Cardiac Murmurstouthang0074085No ratings yet
- Cardiovascular Exam: Examination Includes The FollowingDocument37 pagesCardiovascular Exam: Examination Includes The FollowingyayayanizaNo ratings yet
- Valsalva ManeuverDocument4 pagesValsalva ManeuverjyotimaheshwariNo ratings yet
- Non-Invasive Cardiac ImagingDocument9 pagesNon-Invasive Cardiac Imagingoddone_outNo ratings yet
- Acyanotic Heart DiseaseDocument18 pagesAcyanotic Heart DiseaseShishir ShresthaNo ratings yet
- Immediate Life Support for healthcare Practitioners: A Step-By-Step GuideFrom EverandImmediate Life Support for healthcare Practitioners: A Step-By-Step GuideNo ratings yet
- 1077 CMCNCHDocument11 pages1077 CMCNCHمحمد عقيليNo ratings yet
- TUGAS Ventricular Septal DefectDocument8 pagesTUGAS Ventricular Septal DefectMohammad NafisNo ratings yet
- Diagnostic Methods in Cardiac DisordersDocument29 pagesDiagnostic Methods in Cardiac Disordersmanzoor bhatNo ratings yet
- Clinical Examination of CVSDocument33 pagesClinical Examination of CVSmahnoorNo ratings yet
- Cvs2-k1 (JP-PJB Pada Dewasa)Document81 pagesCvs2-k1 (JP-PJB Pada Dewasa)32 sebastian Josia N.No ratings yet
- Physical DiagnosisDocument42 pagesPhysical DiagnosisKhim Yalong100% (1)
- CVS ExaminationDocument32 pagesCVS ExaminationDurr E SAJALNo ratings yet
- Aortic Regurgitation: Group IvDocument28 pagesAortic Regurgitation: Group IvKim Michael PabatangNo ratings yet
- Cardiac Cycle - Atrial Contraction (Phase 1) : A-V Valves Open Semilunar Valves ClosedDocument10 pagesCardiac Cycle - Atrial Contraction (Phase 1) : A-V Valves Open Semilunar Valves ClosedFatima KhanNo ratings yet
- JVP MedicineDocument27 pagesJVP MedicinesarathNo ratings yet
- Cardiovascular Notes - Paediatrics ExaminationDocument5 pagesCardiovascular Notes - Paediatrics ExaminationPraveenNo ratings yet
- Cardiac Cycle JVPDocument70 pagesCardiac Cycle JVPAstrid PramudyaaNo ratings yet
- IM 3A PE Cardiology Dr. JumangitDocument12 pagesIM 3A PE Cardiology Dr. JumangitCzara DyNo ratings yet
- The ABCs of Heart Disease William HerringDocument14 pagesThe ABCs of Heart Disease William HerringHerchell Sayo SantosNo ratings yet
- Y2 Week 2 Aortic StenosisDocument4 pagesY2 Week 2 Aortic Stenosissurreal_blankNo ratings yet
- CVS ExaminationDocument72 pagesCVS ExaminationPrashanthBhatNo ratings yet
- Congenital Heart Disease: Kriti Puri, MD Hugh D. Allen, MD Athar M. Qureshi, MDDocument30 pagesCongenital Heart Disease: Kriti Puri, MD Hugh D. Allen, MD Athar M. Qureshi, MDhari ilman toniNo ratings yet
- Clinical Examination of The Cardiovascular SystremDocument12 pagesClinical Examination of The Cardiovascular Systremsahsweta67No ratings yet
- Valve SurgeriesDocument13 pagesValve SurgeriesShreeja SajitNo ratings yet
- Assessment Cardiac SystemDocument51 pagesAssessment Cardiac Systemejarnmd100% (2)
- Phases PPT 2Document34 pagesPhases PPT 2victorfoxiNo ratings yet
- Cardiothoraxic and Vascular ExaminationDocument4 pagesCardiothoraxic and Vascular ExaminationPreetha PANo ratings yet
- Case ReportDocument15 pagesCase ReportMimi ChukwuNo ratings yet
- 10 Management of Patient With Hypoglycemic Coma. Management of Patient With Hyperglycemic (Ketoacidotic) ComaDocument59 pages10 Management of Patient With Hypoglycemic Coma. Management of Patient With Hyperglycemic (Ketoacidotic) ComaMimi ChukwuNo ratings yet
- The Hellraiser - Rhonda Nelson (Blaze)Document125 pagesThe Hellraiser - Rhonda Nelson (Blaze)Mimi ChukwuNo ratings yet
- Personal Hygiene Hygiene and Ecology DepartmentDocument17 pagesPersonal Hygiene Hygiene and Ecology DepartmentMimi ChukwuNo ratings yet
- The Wrong Bed Bundle (Blaze)Document1,202 pagesThe Wrong Bed Bundle (Blaze)Mimi ChukwuNo ratings yet
- Cookies, Frosting, PieDocument9 pagesCookies, Frosting, PieMimi ChukwuNo ratings yet
- Brownies RecipeDocument7 pagesBrownies RecipeMimi ChukwuNo ratings yet
- Chocolate RecipesDocument24 pagesChocolate RecipesMimi ChukwuNo ratings yet
- Examination of Cardiovascular System: IAP UG Teaching Slides 2015-16Document76 pagesExamination of Cardiovascular System: IAP UG Teaching Slides 2015-16Abdullah Mohammad Ibne Haider100% (1)
- CHAPTER 11: The History and Physical Examination: An Evidence Based ApproachDocument5 pagesCHAPTER 11: The History and Physical Examination: An Evidence Based ApproachReda SoNo ratings yet
- Ingurgitacion YugularDocument6 pagesIngurgitacion YugularValeria BejarNo ratings yet
- Lecture On Atrial Pressure Changes and JVP by Dr. RoomiDocument9 pagesLecture On Atrial Pressure Changes and JVP by Dr. RoomiMudassar Roomi100% (2)
- Pathophysiology of Pericardial DiseaseDocument36 pagesPathophysiology of Pericardial DiseaseivaniNo ratings yet
- Signs NotesDocument22 pagesSigns NotesVaidehi guptaNo ratings yet
- Cardiac Cycle: Mechanical Event and Their Electrical and Clinical CorrelationDocument28 pagesCardiac Cycle: Mechanical Event and Their Electrical and Clinical Correlationhawas muhammed100% (1)
- Clinical Examination of The Cardiovascular SystemDocument2 pagesClinical Examination of The Cardiovascular SystemPeter 'Pierre' Robson100% (1)
- 4th Year Part 2 End of TermDocument10 pages4th Year Part 2 End of TermKekelwa Mutumwenu SnrNo ratings yet
- History & Examination - FullDocument65 pagesHistory & Examination - FullCharithe Lakshithe ChandanayakeNo ratings yet
- Introduction To Clinical ExaminationDocument153 pagesIntroduction To Clinical ExaminationBnB UsmleNo ratings yet
- Concise CardiologyDocument354 pagesConcise CardiologyAtish_Mathur_9874No ratings yet
- Format (Practical Examination / OSPE) : MBBS First Professional Examination (Part-I)Document2 pagesFormat (Practical Examination / OSPE) : MBBS First Professional Examination (Part-I)Rani MobilinkNo ratings yet
- Assessing Heart and Neck VesselsDocument7 pagesAssessing Heart and Neck VesselsJae TyNo ratings yet
- 1.2.1 Cardio History Taking and Physical Examination Part 1Document53 pages1.2.1 Cardio History Taking and Physical Examination Part 1Abanoub AwadallaNo ratings yet
- Cardiology Consult Manual 2018 PDFDocument450 pagesCardiology Consult Manual 2018 PDFmepimplolabotellas100% (2)
- Count To Ten Allowing YourselfDocument1 pageCount To Ten Allowing YourselfwisgeorgekwokNo ratings yet
- The Arterial PulseDocument66 pagesThe Arterial PulseMohit JainNo ratings yet
- HA Rle Mid 2Document571 pagesHA Rle Mid 2Faith madayagNo ratings yet
- IVMS Physiology and Pathophysiology Flash FactsDocument4,648 pagesIVMS Physiology and Pathophysiology Flash FactsMarc Imhotep Cray, M.D.No ratings yet
- Definition of JVPDocument16 pagesDefinition of JVPMimi ChukwuNo ratings yet
- A Clinical Guide in SurgeryDocument107 pagesA Clinical Guide in SurgerySumayyah AhmadNo ratings yet
- C - Cardiovascular PhysiologyDocument61 pagesC - Cardiovascular PhysiologyMohamad Zekry ZuhairyNo ratings yet
- NCLEX Exam 2 Prioritization QuestionsDocument5 pagesNCLEX Exam 2 Prioritization QuestionsParallelNo ratings yet
- Cardio Vascular HISTORY AND PHYSICAL EXAMINATIONDocument18 pagesCardio Vascular HISTORY AND PHYSICAL EXAMINATIONDan FabrosNo ratings yet
- Pe Fill in BlankDocument34 pagesPe Fill in BlankDhrithiNo ratings yet
- Cardiovascular System Physical AssessmentDocument6 pagesCardiovascular System Physical Assessmentpulsating humNo ratings yet
- Skill: Assessing The Heart and Central VesselsDocument2 pagesSkill: Assessing The Heart and Central VesselsDr. Abiola KomolafeNo ratings yet
- MCQ Internal Medicine PDFDocument448 pagesMCQ Internal Medicine PDFAyaa Yousef100% (5)
- RN Fundamentals Online Practice 2016 A Study Online at QuizletDocument14 pagesRN Fundamentals Online Practice 2016 A Study Online at QuizletDerek Scott Tripp100% (1)